1. The Market Imperative: Biologics Cost 46% of U.S. Drug Spend at Less Than 2% of Volume
Biologic drugs generated more than $461 billion in global revenue in 2023. Forecasters project that figure will exceed $700 billion by 2030. In the United States, biologics account for approximately 46% of total drug expenditures while being used by less than 2% of the patient population. That ratio, the most frequently cited and least frequently unpacked number in pharmaceutical policy, is the foundation upon which the entire biosimilar reimbursement debate rests.
The $461 billion figure is not a single market. It is a collection of distinct therapeutic categories, each with its own pricing architecture, reimbursement channel, and competitive dynamics. Oncology biologics, predominantly physician-administered via infusion, route through Medicare Part B and the buy-and-bill model. Autoimmune biologics, predominantly patient-injected, route through Medicare Part D and commercial pharmacy benefit plans managed by PBMs. The reimbursement rules, the pricing incentives, and the barriers to biosimilar adoption differ substantially across these two channels. Analysts who apply a single-market model to biologic LOE events will consistently mis-forecast both biosimilar penetration rates and originator revenue trajectories.
The Association for Accessible Medicines estimated biosimilars could save the U.S. healthcare system $133 billion by 2025. As of year-end 2024, total biosimilar savings since 2015 reached approximately $36 billion. The gap between the projected savings and the realized savings is not primarily a scientific failure; biosimilars work. It is a reimbursement architecture failure. The science delivered the products. The reimbursement system failed to absorb them efficiently.
The biosimilar market’s structural problems are fixable, and policymakers, large employers, and PBMs under regulatory pressure are actively working to fix them. But the solutions require precise technical understanding of where the economic distortions originate: in the ASP-plus-add-on formula under Medicare Part B, in the rebate-driven formulary economics of the three dominant PBMs, in the 340B program’s site-of-care incentives, and in the patient-level coinsurance structures that can inadvertently penalize biosimilar use. Each of these distortions is addressable, and each is in motion.
Key Takeaways: Section 1
Biologics consume 46% of U.S. drug spending while serving less than 2% of patients. The $36 billion in actual biosimilar savings through 2024 falls dramatically short of the $133 billion projected by 2025. The gap is a reimbursement architecture problem, not a science problem. Two distinct reimbursement channels, Medicare Part B buy-and-bill for physician-administered biologics and PBM-managed pharmacy benefit for self-administered biologics, require separate analytical frameworks.
2. Biologic Manufacturing Complexity and Its Direct Reimbursement Consequences
The pricing and reimbursement dynamics of biologics and biosimilars trace directly back to the science of how these molecules are made. Understanding manufacturing complexity is not background reading; it is the analytical foundation for understanding why biosimilar development costs run $100 million to $250 million, why initial price discounts are 15% to 50% rather than 80% to 90%, and why multiple manufacturers cannot simultaneously flood the market the way they do with small molecules after LOE.
2a. What Makes a Biologic Different
A small-molecule drug is a defined chemical structure, typically below 1,000 daltons in molecular weight, produced through repeatable synthetic chemistry. The active pharmaceutical ingredient is identically reproducible batch to batch. Bioequivalence can be established by measuring plasma concentration in healthy volunteers.
A biologic is produced in living cell systems, typically Chinese hamster ovary (CHO) cells, yeast, or bacterial expression systems, depending on the molecule. The product is a protein, antibody, or nucleic acid construct with a molecular weight that can reach 150,000 daltons or higher for monoclonal antibodies. The three-dimensional folding of the protein, its glycosylation pattern (the sugar chains attached to specific amino acid residues), its charge variants, and its aggregation profile all affect clinical performance and immunogenicity. These structural attributes are not determined solely by the DNA sequence encoding the protein; they are determined by the cell line, the fermentation conditions, the purification process, and the formulation. They cannot be fully specified in advance and cannot be identically reproduced even by the original manufacturer from batch to batch, a property called inherent variability.
This inherent variability is not a deficiency. It is a fundamental property of biological expression systems. The FDA and EMA both acknowledge it and build it into their approval standards by specifying acceptable ranges for critical quality attributes (CQAs) rather than exact molecular identity. An originator biologic’s approved specifications define a range. A biosimilar’s approved specifications define a different but overlapping range that is close enough to produce no clinically meaningful differences.
2b. Manufacturing Complexity as a Market Entry Barrier
The manufacturing barriers for biosimilars translate directly into competitive dynamics that differ from generic small molecules in several quantifiable ways.
A generic small molecule ANDA applicant needs to establish a pharmaceutical manufacturing process, conduct bioequivalence studies, and submit an abbreviated dossier. Total investment: $1 million to $4 million, 18 to 36 months.
A biosimilar applicant must establish a cell bank, develop and validate a cell culture and fermentation process, develop and validate a downstream purification process, characterize the biosimilar and reference product using a state-of-the-art analytical battery that typically includes mass spectrometry, X-ray crystallography, hydrogen-deuterium exchange (HDX-MS), surface plasmon resonance (SPR), and cell-based functional assays, conduct comparative nonclinical studies, conduct a comparative pharmacokinetic study, often conduct a comparative efficacy and safety trial, and prepare a totality-of-evidence dossier for FDA or EMA submission. Total investment: $100 million to $250 million, 7 to 9 years.
The practical consequence of this cost differential is that far fewer manufacturers can participate in any given biosimilar market compared to generic markets. At a $1 billion peak revenue threshold, a generic market might attract 12 to 20 ANDA filers. A biosimilar market for a $5 billion biologic might attract 5 to 10 BLA filers, and only 2 to 5 will achieve commercial launch before competition has already compressed prices to levels that make the investment difficult to recover. This is the economic engine behind modest initial biosimilar price discounts and the relatively slow price floor erosion compared to small molecules.
2c. Cell Line Proprietary Status and Its IP Implications
The cell line used to produce a biologic is itself a proprietary asset protected by a combination of trade secrets, utility patents, and biological material transfer agreements. A biosimilar developer cannot obtain the originator’s cell bank. It must develop its own cell line that expresses a protein highly similar to the reference product’s structural and functional profile.
This cell line development requirement has two important commercial implications. First, it means that the process patents surrounding cell line selection, optimization, and cell culture media composition can be independently licensed or litigated, adding another layer to the patent thicket that biosimilar developers must navigate. Second, it means that two biosimilar manufacturers producing the same reference biologic will have structurally different manufacturing processes and potentially different CQA profiles, even if both products meet the FDA’s biosimilarity standard. This structural divergence between biosimilars is a clinical and regulatory fact that prescribers sometimes cite when expressing hesitancy about switching between biosimilars, a legitimate but frequently overstated concern.
Key Takeaways: Section 2
Biologic manufacturing complexity is the direct cause of biosimilar development costs that are 30-to-100 times higher than small molecule generic costs. Higher development costs produce fewer market entrants, more modest initial price discounts, and slower price floor erosion. Cell line proprietary status creates an independent IP protection layer beyond standard composition-of-matter patents. Inherent manufacturing variability is a feature of biological production systems, not a deficiency, and is built into both FDA and EMA approval standards through CQA ranges rather than exact molecular identity requirements.
3. The ‘Highly Similar, Not Identical’ Standard: Regulatory Science and Its Commercial Weaponization
The FDA’s definition of a biosimilar, ‘highly similar to the reference product with no clinically meaningful differences in safety, purity, and potency,’ is technically precise and scientifically supported. It is also the phrase that originator manufacturers have most aggressively exploited to slow biosimilar adoption.
3a. What ‘Highly Similar’ Actually Means Analytically
‘Highly similar’ is not a vague aspiration. It has a specific technical meaning within the biosimilar approval framework. A biosimilar must demonstrate structural similarity at the primary amino acid sequence level (typically 100% identity for monoclonal antibodies), comparability in higher-order structure including secondary and tertiary folding, comparable glycosylation profiles within an acceptable range, similar functional activity in receptor binding assays and cell-based potency assays, comparable pharmacokinetic profiles in clinical studies, and a safety and immunogenicity profile with no clinically meaningful differences from the reference product.
The analytical methods used to characterize biosimilarity have advanced substantially over the past decade. Modern biosimilar characterization packages routinely include mass spectrometric peptide mapping, capillary electrophoresis for charge variant profiles, size-exclusion chromatography for aggregates, dynamic light scattering for particle size distribution, and multiple cell-based functional assays covering the molecule’s primary and secondary mechanisms of action. The totality of this analytical evidence, when it clearly establishes high similarity, dramatically reduces the clinical uncertainty that would otherwise require large confirmatory trials.
3b. The ‘Nocebo Effect’ and Prescriber Inertia as Commercial Phenomena
The nocebo effect, the phenomenon in which a patient experiences adverse outcomes or loss of efficacy after switching products due to negative expectations rather than pharmacological differences, is real and documented in the biosimilar literature. Studies of patients switched from originator infliximab to its biosimilar CT-P13 (Inflectra/Remsima) have found nocebo-related discontinuation rates of 5% to 10% in some populations, predominantly among patients who were aware of the switch and who expressed concerns about it beforehand. In contrast, blinded switch studies, where patients do not know whether they have been switched, show discontinuation rates equivalent to the originator.
The nocebo effect is a clinical reality. It is also a commercially exploitable narrative. Originator manufacturers have funded and publicized research on nocebo effects, sponsored patient advocacy organizations to raise concerns about switching, and provided educational materials to prescribers that emphasize the ‘highly similar, not identical’ language in ways that imply clinical risk without scientific support. The FTC and CMS have both noted this pattern.
The regulatory community’s response has been to accumulate real-world evidence that switching is safe. Over 100 randomized and observational studies of biosimilar switching have now been published. The EMA’s safety monitoring database includes over one million patient-treatment years of biosimilar data. The aggregate evidence does not support clinically meaningful risks from a single switch between an originator and an approved biosimilar or between two biosimilars of the same reference product.
3c. Extrapolation: The Most Commercially Valuable Regulatory Principle
Extrapolation, the regulatory principle by which a biosimilar approved in one indication can receive approval for all indications of the reference product without conducting separate clinical trials in each indication, is the single most important economic concept in biosimilar development.
Without extrapolation, a biosimilar developer would need to conduct separate comparative clinical trials in each of a reference biologic’s approved indications. For adalimumab, which has approximately 11 FDA-approved indications across rheumatology, gastroenterology, and dermatology, this would require 11 clinical programs. At $10 million to $30 million per comparative trial, the development cost would increase from $150 million to $300 million to $600 million to $900 million, making most biosimilar programs economically unviable. Extrapolation compresses this cost to a single or small number of comparative trials in a scientifically sensitive indication where differences, if any existed, would be most likely to manifest.
Originator manufacturers have challenged extrapolation in FDA advisory committee proceedings and in Citizen Petitions for specific molecules, arguing that mechanism-of-action differences across indications mean that biosimilarity in one indication cannot be scienturally extrapolated. The FDA has consistently rejected these challenges when the scientific justification for extrapolation is adequate, but each case requires specific defense and contributes to the perception among some clinicians that extrapolation is scientifically uncertain. It is not. The FDA’s and EMA’s handling of extrapolation reflects a scientifically mature framework built on two decades of data.
Key Takeaways: Section 3
‘Highly similar’ has a specific technical meaning encompassing structural characterization, functional assay data, pharmacokinetics, and immunogenicity profiles. The nocebo effect is real but has been strategically amplified by originator manufacturers beyond its actual clinical incidence. Blinded switching studies consistently show no clinically meaningful differences from originator use. Extrapolation is scientifically sound, commercially essential, and consistently upheld by both the FDA and EMA despite repeated originator challenges.
4. IP Valuation Framework: Pricing a Biologic Patent Thicket as the Primary Asset
For pharma IP teams and institutional investors, a biologic’s patent portfolio is not a legal appendix to the product profile. It is the product’s primary commercial asset. For a drug generating $5 billion in annual revenue, a two-year delay in biosimilar entry through patent thicket enforcement is worth $10 billion in protected sales. Understanding how to quantify that value, and how to assess the probability that it will hold, is a core analytical skill.
4a. Revenue-Duration NPV for Biologic IP Portfolios
The standard approach to biologic patent portfolio valuation uses a discounted cash flow model with probability-weighted revenue duration. The key inputs differ from small molecule models in several respects.
For a biologic, the composition-of-matter patent on the molecule typically provides the narrowest commercial protection because the structural complexity of the molecule makes it inherently difficult for a competitor to infringe it directly. The more commercially significant patents are often the process patents covering cell line development, fermentation conditions, purification methods, and formulation specifications. These process patents protect the specific way the originator makes its molecule, and a biosimilar developer must either design around them (producing its own distinct manufacturing process) or challenge them (through PTAB IPR or district court litigation).
Quantifying the value of a biologic process patent portfolio requires: identifying which patents the biosimilar developer must infringe to produce a commercially competitive product (the ‘unavoidable’ patents), identifying which patents can be designed around at acceptable cost and development timeline (the ‘designable’ patents), assessing the probability that each unavoidable patent survives a PTAB IPR challenge (historically 30-50% invalidation rate in final written decisions for pharmaceutical patents), and modeling the launch delay generated by the time required for litigation or design-around development.
The product of these inputs, multiplied by annual branded revenue and discounted at an appropriate rate, generates the NPV of the patent thicket as a commercial asset. For Humira’s thicket of 250+ patents, this NPV exceeded $80 billion by the time biosimilar developers were pursuing U.S. entry in the 2018-2022 period.
4b. The Patent Dance as an IP Asset Discovery Process
The BPCIA’s ‘patent dance’ (discussed in detail in Section 19) functions as a structured discovery process for both parties. The biosimilar developer’s disclosure of its manufacturing process to the reference product sponsor forces the sponsor to identify which of its patents it believes are relevant and infringed. This disclosure, while compelled by statute, reveals the sponsor’s assessment of its own patent portfolio’s strength, because the sponsor that over-claims infringement faces early dispositive motions that can invalidate that position.
For IP analysts, tracking the patent dance docket in BPCIA litigation provides direct insight into which process and formulation patents the originator considers commercially essential. If an originator lists 120 patents in its initial disclosure but ultimately asserts only 12 in litigation, the 108 non-asserted patents either do not cover the biosimilar’s manufacturing process or were assessed as too vulnerable to assert. That gap between listed and asserted patents is an IP portfolio quality signal that analysts can track and use to assess the actual depth of the thicket versus its nominal size.
4c. PTAB IPR as a Biosimilar IP Strategy Tool
Inter partes review at the PTAB is a less expensive, faster alternative to district court litigation for challenging the validity of specific biosimilar-relevant patents. A PTAB petition costs approximately $200,000 to $500,000 to file and pursue through final written decision, compared to $5 million to $25 million for district court litigation through trial. Institution rates for pharmaceutical patents run 60% to 70%, and final invalidation rates for instituted petitions are approximately 75%.
Biosimilar developers have used PTAB IPR to systematically challenge the weakest patents in a reference product’s thicket, selectively removing barriers rather than challenging the entire portfolio at once. AbbVie successfully defended many Humira patents at PTAB, but the IPR threat forced it into settlement negotiations with biosimilar developers and produced the structured entry date agreements that ultimately brought biosimilars to the U.S. market in January 2023.
For biologic IP teams, the PTAB IPR threat from biosimilar developers should be modeled into patent portfolio valuation. A secondary patent that faces a credible IPR threat carries a materially lower probability of survival than one that has already survived or been declined institution. Portfolio managers should track biosimilar developer PTAB filings as a direct signal of which patent positions competitors consider vulnerable.
Investment Strategy: Biologic IP Valuation
Investors should construct three scenario NPVs for each major biologic approaching biosimilar entry: (1) ‘thicket holds’ scenario in which all asserted patents survive litigation and the last settlement date defines the LOE; (2) ‘core defense’ scenario in which process and formulation patents are invalidated or designed around and LOE occurs at the composition-of-matter expiry or after a single successful biosimilar settlement; (3) ‘contested market entry’ scenario in which one or more biosimilar developers launches before all litigation is resolved, producing injunction proceedings and a contracted at-risk period. Probability-weight each scenario using PTAB docket data, settlement history for the reference product, and the number of BPCIA litigation actions filed. The gap between scenario (1) and scenario (2) NPVs is the quantifiable value of the patent thicket as a management-controlled asset.
Key Takeaways: Section 4
Biologic patent portfolio value is driven primarily by process patents, not composition-of-matter patents. The NPV of AbbVie’s Humira patent thicket exceeded $80 billion, making it the most commercially valuable single patent portfolio in pharmaceutical history. BPCIA patent dance disclosures reveal which patents an originator considers commercially essential, and the gap between listed and asserted patents signals portfolio quality. PTAB IPR is a cost-effective selective challenge tool for biosimilar developers that forces originator companies into NPV reassessments and settlement negotiations.
5. The BPCIA 351(k) Pathway: Totality of Evidence, Extrapolation, and Development Cost Architecture
The Biologics Price Competition and Innovation Act of 2009, which created the 351(k) abbreviated licensure pathway for biosimilars, established the regulatory framework that determines development cost, timeline, and the degree of clinical evidence required for biosimilar approval. Understanding the 351(k) pathway’s structure is essential for modeling biosimilar development programs and assessing the cost basis that determines pricing strategy at launch.
5a. The Stepwise Evidence Package
The 351(k) pathway builds a biosimilar application in sequential tiers of evidence, with each tier designed to resolve residual uncertainty from the prior tier.
The analytical tier is the foundation. A biosimilar developer conducts state-of-the-art structural and functional characterization comparing its product to the reference at the molecular level. This package typically includes primary sequence confirmation, higher-order structure analysis, glycosylation profiling, charge variant characterization, aggregation assessment, and cell-based functional assays. The goal is to minimize residual uncertainty about structural similarity before any clinical work begins.
If the analytical tier leaves residual uncertainty about in vivo performance, the developer proceeds to nonclinical studies, typically animal pharmacokinetic and pharmacodynamic studies and, for certain molecules, toxicology studies. These studies are designed not to establish safety and efficacy independently but to provide additional comparative data.
If nonclinical data leaves further residual uncertainty, clinical pharmacokinetic and pharmacodynamic (PK/PD) studies follow. A comparative PK study in healthy volunteers (where appropriate) or in patients (for molecules where healthy volunteer administration is not ethical) establishes that the biosimilar’s pharmacokinetics overlap adequately with the reference product. This study is typically the most expensive and time-consuming clinical element in the development program.
A confirmatory comparative efficacy and safety trial follows if the PK/PD studies do not resolve all residual uncertainty. For highly complex molecules, such as pegylated proteins or antibody-drug conjugates, the FDA may require this step even when analytical and PK data are strong. For simpler monoclonal antibodies, the stepwise package may terminate at the PK level if the totality of the analytical evidence is sufficiently compelling.
An immunogenicity assessment, comparing rates of anti-drug antibody (ADA) formation between the biosimilar and the reference product, is required as part of every 351(k) package. ADA formation can affect efficacy (through drug neutralization), safety (through immune complex-mediated reactions), and pharmacokinetics (through antibody-mediated clearance). Demonstrating comparable immunogenicity profiles is essential to establishing no clinically meaningful differences.
5b. Extrapolation: Technical Requirements and Originator Challenges
For extrapolation to be granted, the biosimilar developer must provide a scientific justification demonstrating that the mechanism(s) of action responsible for each proposed extrapolated indication involve the same molecular target or pathway, that the safety and immunogenicity profile established in the studied indication is reasonably predictive of the profile in the extrapolated indications, and that no unique patient population considerations in the extrapolated indications would alter the safety or efficacy profile in ways not captured by the studied indication data.
The scientific justification for extrapolation is typically most robust for monoclonal antibodies targeting a single molecular target (e.g., anti-TNF antibodies, where the mechanism of action across rheumatoid arthritis, Crohn’s disease, and psoriasis is the same TNF-alpha neutralization). It is more technically demanding for antibodies with multiple binding epitopes or multiple mechanisms of action, and for molecules whose activity in different indications involves different Fc-receptor interactions or different effector functions.
Originator manufacturers have challenged extrapolation for specific molecules by arguing that mechanism differences across indications make cross-indication inference scientifically unjustified. The FDA has addressed these arguments in draft guidance documents, reaffirming that extrapolation is scientifically appropriate when the justification addresses the specific mechanisms relevant to each indication. The key regulatory principle is that extrapolation decisions are made based on scientific evidence, not administrative convenience, and neither on commercial preference from either party.
5c. The 12-Year Reference Product Exclusivity Period
The BPCIA grants reference biological products 12 years of exclusivity from the date of first licensure, during which the FDA cannot approve a 351(k) application referencing the innovator’s data. This exclusivity period is separate from and often extends beyond patent protection. For a biologic approved after undergoing a lengthy clinical development program, the 12-year exclusivity period may expire before or around the same time as the composition-of-matter patent, depending on development timeline.
The 12-year exclusivity period cannot be shortened by patent challenges. A biosimilar applicant can file a 351(k) application and even begin the patent dance during the exclusivity period, but FDA approval cannot occur until the exclusivity expires. This is distinct from the Hatch-Waxman framework, where a Paragraph IV challenge can potentially produce FDA approval before the patent’s nominal expiry through a finding of invalidity or non-infringement.
The interplay between 12-year exclusivity and patent thicket enforcement is the defining strategic question in biologic lifecycle management. A biologic whose composition-of-matter patent expires before its 12-year exclusivity ends is fully protected by the exclusivity regardless of patent status. A biologic whose 12-year exclusivity expires before its most valuable process or formulation patents expire must rely on those patents to sustain its market protection.
Key Takeaways: Section 5
The 351(k) pathway’s stepwise evidence structure allows analytical data to reduce clinical study requirements, and high analytical similarity can sometimes satisfy FDA without a full comparative efficacy trial. Extrapolation is scientifically justified for molecules with consistent mechanisms across indications and is commercially essential: without it, biosimilar development costs for multi-indication biologics would be prohibitive. The 12-year BPCIA reference product exclusivity is a hard regulatory floor that cannot be shortened by patent challenges and must be tracked separately from patent expiry dates in LOE modeling.
6. The Interchangeability Conundrum: FDA’s Two-Tier System and Its Impending Collapse
The FDA’s interchangeability designation has been the most commercially consequential and scientifically contested element of the U.S. biosimilar regulatory framework. It was designed to facilitate pharmacy-level substitution. Instead, it has functioned primarily as a source of confusion that slowed biosimilar adoption.
6a. What Interchangeability Requires and What It Grants
The BPCIA defines an interchangeable biosimilar as one that ‘can be expected to produce the same clinical result as the reference product in any given patient,’ and for products administered more than once, ‘the risk in terms of safety or diminished efficacy of alternating or switching between use of the biological product and the reference product is not greater than the risk of using the reference product without such alternation or switching.’
To meet this standard, the FDA historically required manufacturers to conduct switching studies, typically randomized crossover trials in which patients alternate between the reference product and the biosimilar over multiple treatment periods. The FDA recommended a minimum of three treatment periods (ABB or ABAB design) to assess the immunogenicity and pharmacokinetic effects of switching. These studies added 12 to 24 months to the development timeline and $20 million to $50 million in additional cost.
The commercial benefit of interchangeability is the right to automatic pharmacy substitution. Under state pharmacy practice laws, a pharmacist can substitute an interchangeable biosimilar for a prescribed brand-name biologic without contacting the prescriber, in the same way that a pharmacist can substitute a generic for a brand-name small molecule. As of 2025, virtually all states have enacted legislation permitting automatic substitution of FDA-designated interchangeable biosimilars, with notification requirements that vary by state.
6b. The Two-Tier Perception Problem
The practical problem with interchangeability is that it created a perceived hierarchy that the underlying science does not support. A physician or patient who sees two biosimilars on a formulary, one labeled ‘interchangeable’ and one without that designation, reasonably assumes the interchangeable product is safer or more effective for switching. The FDA’s own research on prescriber and patient understanding of the distinction confirmed this misconception is widespread.
The two-tier system was also commercially exploited. The first biosimilar to receive an interchangeable designation for a given reference product earned a 12-month period of marketing exclusivity during which no other biosimilar could receive an interchangeable designation for the same reference product. This created a race for interchangeable status that was driven more by competitive commercial positioning than by scientific need. Several adalimumab biosimilar developers pursued interchangeability studies specifically to gain this exclusivity period, spending tens of millions of dollars on switching studies whose clinical value was scientifically marginal but whose commercial value was real.
6c. FDA’s Proposed Reform: Eliminating the Designation
The FDA released two draft guidance documents in 2023 and 2024 signaling a fundamental rethinking of interchangeability. The first proposed eliminating the requirement for dedicated switching studies to obtain an interchangeability designation. The second, more consequential, proposed removing the ‘interchangeable’ designation from product labeling entirely and replacing it with a unified ‘biosimilarity statement’ applying to all approved biosimilars. Under this proposed framework, all FDA-approved biosimilars would be considered interchangeable as a matter of regulatory science, and state-level pharmacy substitution laws would need to adapt accordingly.
If finalized, this reform would align the U.S. regulatory framework with the EMA’s approach and eliminate the two-tier perception that has complicated prescriber education for a decade. It would also eliminate the $20-to-$50 million switching study cost from the development program of every biosimilar that would otherwise have pursued interchangeability, reducing the total cost of biosimilar development and potentially encouraging entry into markets that are currently considered economically marginal.
The FDA has been cautious about timeline. Finalizing the guidance requires addressing state pharmacy substitution laws that reference the specific ‘interchangeable’ designation, and it may require Congressional action to fully harmonize the legal framework. Nevertheless, the direction is clear: the FDA has concluded that the interchangeability distinction has created more regulatory complexity than clinical benefit, and it intends to eliminate it.
Investment Strategy: Interchangeability Reform
For biosimilar developers with programs currently pursuing interchangeability designation, the expected value of the 12-month exclusivity period should be discounted against the probability that FDA finalizes its reform before the product reaches market. If the designation is eliminated, the exclusivity period disappears with it. Developers should conduct explicit scenario modeling: what is the value of the exclusivity period if the reform is not finalized, versus the cost savings from not conducting switching studies if it is?
Key Takeaways: Section 6
The interchangeability designation’s primary legacy has been to create a two-tier perception system that slows biosimilar adoption without corresponding clinical benefit. FDA’s proposed reform to eliminate the distinction from labeling and align with the European scientific consensus would reduce development costs by $20-to-$50 million per program and remove a major source of prescriber confusion. Biosimilar developers with interchangeability programs underway should model the expected value of the 12-month marketing exclusivity against the probability that the designation is eliminated before their product reaches market.
7. EMA Regulatory Architecture: What Europe Built in Two Decades and What the U.S. Can Borrow
The European Medicines Agency approved the world’s first biosimilar (somatropin) in 2006. Eighteen years of regulatory experience, more than one million patient-treatment years of safety data, and over 100 approved biosimilar products have produced a regulatory and market access framework that the U.S. is now beginning to deliberately emulate.
7a. The EMA’s Centralized Procedure and Its Efficiency Advantages
The EMA’s centralized procedure grants marketing authorization across all EU member states via a single application. This contrasts with the U.S. system, where FDA approval grants a single national authorization. The EMA procedure’s efficiency advantage over the U.S. is not primarily in the regulatory review itself, which is comparable in scientific rigor and timeline, but in the market access that follows approval. A biosimilar approved by the EMA can, in principle, immediately access 27 national markets, though each country’s reimbursement and pricing frameworks operate independently.
The EMA has been refining its biosimilar guidelines continuously since 2006. Its 2014 overarching biosimilar guideline established the totality-of-evidence framework. Product-specific annexes provide molecule-level technical requirements. The EMA’s 2024 draft reflection paper proposing to waive comparative efficacy studies when sufficient analytical and PK/PD evidence is available represents the most significant efficiency improvement in the EMA framework since 2006 and reflects the accumulation of scientific confidence built on two decades of biosimilar approval experience.
7b. The EMA’s Scientific Consensus on Interchangeability
The EMA does not issue an ‘interchangeable’ designation because, from a scientific standpoint, it does not need to. All EMA-approved biosimilars are considered interchangeable with their reference products by the agency’s Committee for Medicinal Products for Human Use (CHMP). The agency’s position is that if a product has passed the totality-of-evidence standard and has been approved, it is scientifically appropriate to use it in place of the originator in any approved indication.
Whether automatic pharmacy-level substitution is permitted is left to each member state’s national medicine agency and pharmacy laws. This decentralization has produced variability: France, the Netherlands, and Finland permit automatic substitution under specific conditions. Germany and most other states do not mandate substitution but permit it with prescriber notification. The absence of a formal EMA interchangeability step has not prevented the rapid biosimilar penetration seen in most EU markets, because the primary driver of adoption is national reimbursement policy rather than pharmacy-level substitution.
7c. National Tendering and Its Price Mechanism
National tendering, in which a government health authority issues a competitive tender for the supply of a specific biologic product, is the most powerful single mechanism for biosimilar adoption in Europe. Under a winner-takes-all or sole-source tender, a biosimilar manufacturer that wins the tender captures essentially the entire public market for that molecule in that country for the tender period, typically one to three years. The price competition between biosimilar manufacturers competing for the tender can be fierce, driving discounts of 70% to 80% off the originator’s pre-biosimilar price.
The Nordic countries (Norway, Denmark, Sweden, Finland) have been the most aggressive users of national tendering for biologics. Norway’s tender for infliximab in 2015 produced a winning biosimilar price that was approximately 70% below the originator’s pre-biosimilar price and led to biosimilar market share above 90% within 12 months. The Nordic model has been widely cited as proof that rapid, deep biosimilar adoption is achievable when the reimbursement framework creates unambiguous financial incentives.
The U.S. has no direct equivalent to national tendering. The Federal Supply Schedule (FSS) and the VA’s National Acquisition Center conduct tendering for government payers, but commercial markets operate through PBM-negotiated formulary contracts that produce very different competitive dynamics. Understanding the tendering mechanism is therefore not about directly importing it to the U.S. context but about identifying which U.S. policy tools, particularly formulary exclusion and mandatory biosimilar step therapy in Medicare, can produce functionally comparable financial incentives for biosimilar adoption.
Key Takeaways: Section 7
The EMA’s 18 years of biosimilar regulatory experience have produced a scientifically mature framework that treats all approved biosimilars as interchangeable without a separate designation, and the absence of a two-tier system has not impeded adoption. National tendering in the Nordic countries produces biosimilar market shares above 90% within 12 months of launch, demonstrating that rapid adoption is achievable when reimbursement incentives are unambiguous. The U.S. cannot directly import national tendering, but Medicare formulary exclusion and mandatory step therapy produce functionally comparable directional effects.
8. Buy-and-Bill: The Mechanics, the Margins, and the Perverse Incentive Structure
The buy-and-bill model is the dominant reimbursement mechanism for physician-administered biologics in the United States, covering drugs dispensed in oncology practices, rheumatology infusion suites, hospital outpatient departments, and specialty infusion centers. It is the system that most directly creates the perverse incentive to prescribe higher-priced biologics over lower-priced biosimilars.
8a. Operational Mechanics of Buy-and-Bill
In the buy-and-bill model, a healthcare provider acquires a specialty drug directly from a specialty distributor or directly from the manufacturer. The provider takes legal title to the drug, stores it (often under temperature-controlled conditions), administers it to the patient, and then submits a claim for reimbursement from the patient’s insurer.
The provider’s economic position in this model is that of a pharmaceutical mini-distributor. They assume inventory risk (spoilage, theft, waste), cash flow risk (the lag between acquisition payment and reimbursement receipt), and reimbursement risk (prior authorization denials, claim audits, clawbacks). In exchange, they earn a margin on the drug that is the difference between their acquisition cost and their reimbursement.
For a practice operating on tight margins, this drug margin can represent a material fraction of total revenue. Studies of oncology practices found that drug-related revenue, including both the drug margin and administration fees, accounts for 40% to 70% of total practice revenue for some practice types. In this context, the financial consequences of switching from a higher-margin to a lower-margin product are not abstract; they determine whether a practice can meet payroll.
8b. Acquisition Cost vs. Reimbursement: The Gap That Determines Prescribing Behavior
The margin available to a provider under buy-and-bill is determined by the gap between their acquisition cost and their reimbursement. Under Medicare Part B, reimbursement is set at ASP plus a 6% add-on. A provider’s acquisition cost is typically at or near the ASP, because ASP is calculated as the average of all manufacturer prices to all commercial purchasers, net of most discounts and rebates.
When ASP reflects a single product in a class (the originator biologic), the margin mechanics are straightforward. When a lower-priced biosimilar enters the class, the margin mechanics create an immediate disadvantage for the biosimilar.
Originator biologic reimbursement: (ASP $1,000) + (6% x $1,000) = $1,060. Provider margin: $60. Biosimilar reimbursement: (ASP $700) + (6% x $700) = $742. Provider margin: $42.
The provider earns $18 more per dose by prescribing the originator. At 100 infusions per month, this is $1,800 in monthly margin difference, $21,600 per year. For a practice managing hundreds of biologic patients, the annual margin impact of switching is material. This is the quantitative foundation of the perverse incentive, and it operates identically across every physician-administered biologic market.
8c. Site-of-Care Economics and the 340B Program
The buy-and-bill perverse incentive is dramatically amplified in hospitals and outpatient departments participating in the 340B Drug Pricing Program. The 340B program, created by Congress in 1992, requires pharmaceutical manufacturers to provide outpatient drugs at steeply discounted prices, up to 50% below non-340B prices, to qualifying covered entities, including disproportionate share hospitals (DSH), cancer centers, children’s hospitals, and certain federally qualified health centers.
A 340B-participating hospital acquires a biologic at 340B prices, which can be 25% to 50% of WAC, then bills Medicare at the standard ASP-plus-6% rate. The margin is not 6% of ASP; it is the full difference between the discounted 340B acquisition cost and the ASP-based reimbursement, which can be 30% to 50% of the drug’s WAC on an originator biologic priced above $100,000 per year.
When a biosimilar enters the market, the 340B hospital faces the same directional perverse incentive as a physician practice but at a higher absolute dollar magnitude. If the originator biologic generates a 40% margin over acquisition cost in a 340B context, and the biosimilar generates a 20% margin (its lower ASP reduces both the reimbursement ceiling and the absolute 340B discount), the hospital loses substantially more margin per dose by switching to the biosimilar than a non-340B practice does. The Government Accountability Office and CMS’s Office of Inspector General have both documented this dynamic, and it is a significant contributor to the slow biosimilar uptake in hospital outpatient settings.
Key Takeaways: Section 8
The buy-and-bill model’s ASP-plus-add-on reimbursement formula creates a direct financial disincentive for providers to prescribe lower-priced biosimilars, quantifiable at $18 or more per dose in the model example. The 340B program amplifies this disincentive by generating margins that are proportional to the drug’s absolute price, making high-priced originator biologics even more financially attractive to participating hospitals. Site-of-care economics are a major contributor to slow biosimilar uptake in hospital outpatient settings and cannot be addressed by the ASP+8% fix alone.
9. ASP+6% and the Provider’s Financial Calculus: A Quantitative Model
The ASP-plus-6% reimbursement formula is the most frequently cited cause of biosimilar adoption resistance in the physician-administered channel. Building a quantitative model of its effects clarifies both the scale of the distortion and the limits of the IRA’s policy correction.
9a. How ASP Is Calculated and Reported
Average Sales Price is a manufacturer-reported figure submitted to CMS quarterly. The calculation includes all U.S. sales to all purchasers, minus certain price concessions including cash discounts, free goods, chargebacks, rebates, and other price adjustments. The net ASP reflects the average realized price across the manufacturer’s entire distribution network.
ASP is calculated per billing unit (typically per milligram or per milliliter) and is published by CMS quarterly on a six-month lag. A drug administered in Q1 2026 is reimbursed based on the ASP from Q3 2025. This lag has commercial implications: if a biosimilar launches with a substantially lower price, the originator’s ASP will decline over subsequent quarters as the biosimilar’s market penetration grows (because the biosimilar’s lower prices appear in the originator manufacturer’s net sales calculations if they are the same manufacturer, or because the competition forces originator net price reductions). This ASP decline then reduces the absolute dollar amount of the 6% add-on in future quarters, compressing the originator’s margin advantage over time.
The lag also means that a new biosimilar’s ASP at initial launch may be calculated from limited sales data, producing a less stable ASP figure in early quarters. Providers should model ASP trajectories quarterly rather than using static ASP figures for cost analysis.
9b. The Competitive Cascade Effect on ASP Trajectories
When multiple biosimilars of the same reference product are on the market and actively competing, the ASP trajectories of both the originator and the biosimilars decline over time. This creates a ‘race to the bottom’ dynamic in which the margin available to providers from any product in the class compresses.
CMS data on Medicare Part B biosimilars documented this cascade clearly. For the trastuzumab class, the launch of multiple biosimilars produced a 50.3% average reduction in biosimilar reimbursement rates over a five-year period post-launch, while the originator trastuzumab reimbursement rates fell 32.7% over the same period. The total Medicare Part B expenditure reduction attributable to biosimilar competition in the oncology class was estimated at 62% versus the counterfactual of no biosimilar entry.
The cascade effect has a secondary consequence: it compresses manufacturer gross margins on the biosimilar itself. A biosimilar that launches with a 30% discount to originator ASP and then experiences an additional 50% ASP decline over five years ends up priced at 35% of the originator’s pre-launch price. At that price level, the cost-of-goods for manufacturing a complex biologic may approach or exceed the realized net price, particularly for later-entering biosimilar manufacturers who did not recoup fixed development costs during the period of higher prices. This compression is the primary cause of market exit by some biosimilar manufacturers and the primary risk factor for the ‘biosimilar void’ phenomenon described in Section 22.
Key Takeaways: Section 9
ASP is a lagged, realized-price metric that declines over time as biosimilar competition intensifies, creating a compounding margin compression effect for all products in a biologic class. The competitive cascade effect on ASP trajectories produces a ‘race to the bottom’ that can threaten the long-term economic viability of later-entering biosimilar manufacturers, risking market exit and reduced competition. Providers should model ASP trajectories quarterly rather than statically for financial planning purposes.
10. The Inflation Reduction Act’s ASP+8% Fix: Mechanism, Limitations, and 340B Complications
The Inflation Reduction Act of 2022 included a direct legislative intervention in the ASP-plus-add-on formula for qualifying biosimilars under Medicare Part B. It is the most significant federal policy action to address the buy-and-bill perverse incentive since the original Hatch-Waxman Act established the pharmacy benefit equivalents.
10a. The Mechanism: ASP+8% of Reference Product ASP
Effective October 1, 2022, a ‘qualifying biosimilar’ under the IRA receives reimbursement equal to the biosimilar’s ASP plus 8% of the reference product’s ASP. A qualifying biosimilar is defined as one whose ASP does not exceed the reference product’s ASP, which automatically excludes any biosimilar that has adopted a high-list/high-rebate pricing strategy above the originator’s WAC.
The critical distinction from the standard formula is that the add-on is computed from the reference product’s ASP, not the biosimilar’s own ASP. Because the reference product carries a higher ASP, 8% of reference ASP produces a larger absolute dollar add-on than 6% of the biosimilar’s lower ASP. Using the earlier quantitative model:
Standard biosimilar reimbursement: $700 + (6% x $700) = $742. Provider margin: $42. IRA-adjusted biosimilar reimbursement: $700 + (8% x $1,000) = $780. Provider margin: $80. Originator reimbursement: $1,000 + (6% x $1,000) = $1,060. Provider margin: $60.
The policy inversion is clear: the provider now earns $20 more per dose from the biosimilar than from the originator. At 100 infusions per month, this is $2,000 per month, $24,000 per year in incremental margin from switching. The IRA provision mathematically resolves the perverse incentive for non-340B providers.
10b. Why Real-World Impact Has Been ‘Modest’ So Far
Despite the correct theoretical direction of the IRA’s formula change, early analyses describe its real-world impact on biosimilar adoption as modest rather than transformative. Several structural factors explain the gap between the policy’s mechanical logic and its market outcomes.
Commercial payer inertia: the IRA’s ASP+8% provision applies to Medicare Part B. Commercial payers use their own reimbursement formulas, which they negotiate with providers in physician network contracts. Most commercial payers reimburse provider-administered drugs at a percentage of WAC or at contracted rates that do not automatically incorporate the IRA formula. For providers whose patient populations are predominantly commercially insured rather than Medicare, the IRA change has limited direct impact on prescribing economics.
Prior authorization barriers: even when the biosimilar is the more financially attractive option for the provider, a commercial payer may require the patient to use the originator or undergo step therapy protocols that override the provider’s preference. Prior authorization requirements at the commercial level can block the biosimilar regardless of the provider’s financial incentive to use it.
340B complication: the IRA provision did not modify 340B program mechanics. A 340B-participating hospital continues to earn substantially higher margins on high-priced originator biologics acquired at steeply discounted 340B prices and billed at ASP-based rates. The IRA’s formula change is insufficient to reverse the 340B margin advantage for originator products in hospital settings. Addressing the buy-and-bill perverse incentive in 340B hospitals requires either separate 340B program reform or site-of-care reimbursement adjustments, neither of which was included in the IRA.
Transition friction: prescribing behavior does not respond instantly to reimbursement formula changes. Practice managers and physicians need time to understand the new economics, update their formulary preferences, and execute contracting changes with their specialty distributors. The modest impact observed in the first year post-implementation likely reflects this adoption lag rather than a fundamental failure of the policy direction.
Investment Strategy: IRA Impact Modeling
Investors modeling biosimilar market share dynamics under Medicare Part B should apply the IRA incentive primarily to the non-340B provider segment. For the 340B segment, model continued originator preference until separate 340B reform occurs, as the IRA formula change provides insufficient margin incentive to overcome the 340B math. Commercial payer dynamics remain independent of the IRA provision and should be modeled based on individual PBM formulary position trajectories.
Key Takeaways: Section 10
The IRA’s ASP+8% formula correctly inverts the buy-and-bill perverse incentive for non-340B Medicare Part B providers, generating $20 more per dose from the biosimilar than from the originator in the model scenario. Real-world impact has been modest because the change applies only to Medicare Part B, commercial payers use independent reimbursement formulas, prior authorization can block biosimilar use regardless of provider financial preference, and the 340B program’s margin mechanics are not addressed by the IRA provision. Site-of-care reform and 340B program reform are the remaining policy levers required to complete the reimbursement incentive correction.
11. PBM Architecture: Formulary Tiers, Rebate Economics, and the Rebate Wall
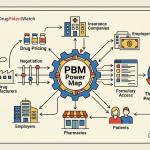
For self-administered biologics covered under the pharmacy benefit, the dominant force shaping biosimilar market penetration is not physician-level economics but the formulary decisions of the three PBMs that collectively process approximately 80% of U.S. prescription claims: CVS Caremark, Express Scripts (Cigna), and OptumRx (UnitedHealth Group).
11a. Formulary Tier Architecture and Its Volume Consequences
A drug formulary is a tiered list of covered medications in which tier assignment determines the patient’s out-of-pocket cost-sharing obligation. For specialty biologics, tier placement is the primary commercial determinant of market share, often exceeding the influence of clinical evidence or manufacturer price.
Tier 1 (preferred generic): typically $0-$10 copay. Tier 2 (preferred brand): typically $30-$60 copay. Tier 3 (non-preferred brand): typically $70-$100 or higher copay. Specialty tier (for biologics): coinsurance of 20%-33% rather than a flat copay, producing patient cost-sharing that can reach thousands of dollars per month.
A biosimilar placed on the specialty tier at a 20% coinsurance rate while the originator is placed on a preferred specialty tier at 10% coinsurance creates a substantial patient cost differential even if the biosimilar’s list price is lower. On a drug with a $30,000 annual cost, the patient on the originator at 10% coinsurance pays $3,000 per year; the patient on the biosimilar at 20% pays $6,000 per year, assuming the biosimilar list price is 20% lower than the originator and coinsurance applies to the actual cost.
The patient cost-sharing structure is therefore a tool that PBMs can deploy in either direction: to accelerate biosimilar uptake (by placing the biosimilar on a lower tier with lower patient cost-sharing) or to suppress it (by requiring higher patient cost-sharing for the biosimilar while the originator benefits from lower coinsurance and a manufacturer copay assistance card that effectively eliminates out-of-pocket cost).
11b. The Rebate Architecture: WAC, Gross-to-Net, and the PBM Revenue Model
A PBM’s core financial model depends on rebate revenue from pharmaceutical manufacturers. A manufacturer pays a rebate, typically expressed as a percentage of the drug’s WAC, in exchange for preferred formulary position. The PBM negotiates these rebates with manufacturers, retains a portion, and passes the remainder to its clients (health plans and employers). The proportion retained by the PBM is not disclosed publicly; estimates range from 5% to 30% of gross rebates depending on the PBM and the contract structure.
The gross-to-net gap for a high-priced biologic with a large rebate can be enormous. An originator biologic with a WAC of $60,000 per year and a 50% net rebate has a net price of $30,000. A biosimilar with a WAC of $42,000 (30% below originator WAC) and a 10% rebate has a net price of $37,800. Despite the biosimilar’s lower list price, its net price is actually higher than the rebated originator, at least from the PBM’s perspective. This arithmetic is the precise mechanism of the rebate wall: the PBM cannot simultaneously maximize rebate revenue and adopt the lower-list-price biosimilar.
The health plan that the PBM serves may or may not share this conflict of interest, depending on the pass-through structure of their PBM contract. Under a guaranteed net cost (GNC) or pass-through contract, the health plan receives 100% of rebates and the biosimilar’s lower net price is unambiguously better for the plan. Under a traditional retained-rebate model, the plan receives only a portion of rebates, and the comparative economics may favor the originator from the plan’s perspective as well, depending on the pass-through rate.
11c. The Rebate Wall: Structural Definition and FTC Analysis
The FTC defined ‘rebate walls’ in its 2023 staff report on PBMs as contractual arrangements in which a manufacturer pays large rebates contingent on the payer granting the manufacturer’s product exclusive or dominant formulary position, with the rebate either disappearing or substantially declining if the payer adds a biosimilar or places the originator in a non-preferred tier.
The economic mechanism is a volume-linked all-or-nothing rebate structure. The originator’s rebate is calculated on total volume of the originator product, not per unit. If the payer switches 30% of patients to a biosimilar, the rebate applies only to the remaining 70% originator volume, but the payer may lose the favorable rebate rate entirely if biosimilar coverage triggers a contract renegotiation clause. The total rebate loss on 70% of a $60,000-per-patient drug across 50,000 patients at a 50% rebate rate is substantial.
The FTC characterized rebate wall arrangements as potentially anticompetitive under FTC Act Section 5 in its 2023 report, and referred six large originator manufacturers for potential enforcement consideration. The report documented practices that the FTC concluded could harm competition by foreclosing lower-cost alternatives from formulary access without a clinical justification.
Key Takeaways: Section 11
The PBM’s financial model depends on retaining a portion of manufacturer rebates, and the rebate wall creates a structural misalignment between PBM financial incentives and lower net drug cost for the health plan. The gross-to-net gap can make a lower-list-price biosimilar appear more expensive than the rebated originator from the PBM’s net revenue perspective. The FTC’s 2023 staff report characterized rebate wall arrangements as potentially anticompetitive and referred six manufacturers for enforcement consideration, signaling increased regulatory scrutiny of this practice.
12. The Rebate Wall in Detail: How AbbVie Built It, How CVS Caremark Broke It
The adalimumab rebate wall is the defining case study of both the construction and eventual dismantling of the rebate barrier to biosimilar adoption. Understanding its architecture and the mechanism of its collapse provides the template for forecasting equivalent dynamics in the Stelara, Keytruda, and Dupixent biosimilar markets.
12a. AbbVie’s Rebate Wall Construction: The Contract Engineering
AbbVie’s Humira generated $21.2 billion in global revenue in 2022, with approximately $18.6 billion in the U.S. The U.S. price, approximately $6,900 per 28-day carton at WAC, was among the highest in the world. European Humira prices after biosimilar entry in 2018 were 70% to 85% lower.
AbbVie maintained this U.S. price and market position through a contract engineering strategy that tied Humira’s rebate payments to formulary exclusivity. AbbVie offered PBMs and health plans escalating rebate rates in exchange for two specific formulary protections: placement of Humira on the preferred specialty tier (typically the lowest coinsurance tier for specialty drugs) and exclusion of Humira biosimilars from the plan’s specialty formulary. Rebate rates on Humira were reported in various analyses to range from 40% to 60% of WAC.
The mathematics of the rebate wall for a PBM with 10 million Humira-treated lives: at $6,900 WAC, $830 per 2-week injection, 26 injections per year, total WAC per patient per year approximately $21,580. A 50% rebate generates approximately $10,790 per patient per year in gross rebate revenue. At 100,000 Humira patients under management, total gross rebate revenue from Humira alone: approximately $1.08 billion per year.
A biosimilar at $1,700 WAC (75% discount) with a 10% rebate generates $170 per patient per year in rebate revenue. Switching 100,000 patients to the biosimilar produces $17 million in rebate revenue, versus $1.08 billion from Humira. The PBM’s rebate revenue would fall by over $1 billion. From a pure rebate revenue perspective, the decision to add an $1,700 WAC biosimilar to the preferred formulary was the equivalent of electing to lose $1 billion per year in PBM revenue. The rebate wall held precisely because the math was unambiguous.
12b. The Commercial Pressure That Broke the Wall
The rebate wall held through all of 2023. Biosimilar market share at year-end 2023 was approximately 2%, confirming that AbbVie’s contract engineering had successfully maintained formulary exclusivity for Humira across most major commercial formularies.
The wall broke in 2024 for three compounding reasons. First, the FTC’s increased scrutiny of PBM rebate practices and its characterization of rebate walls as potentially anticompetitive raised legal risk for PBMs that continued to block FDA-approved, lower-cost biosimilars without justification. Second, large self-insured employers, who negotiate directly with PBMs and who increasingly demand transparent, pass-through rebate contracts that align PBM incentives with lower net cost, began threatening to change PBMs or demand biosimilar coverage as a contract condition. Third, CVS Health’s Cordavis subsidiary, which co-markets Sandoz’s Hyrimoz adalimumab biosimilar under CVS branding, created a direct financial incentive for CVS Caremark to shift formulary position from Humira to Cordavis/Hyrimoz.
CVS Caremark’s January 2024 announcement that it would remove Humira from major commercial formularies effective mid-2024, making Cordavis/Hyrimoz the preferred adalimumab option, was the event that broke the wall. The competitive consequences were immediate. AbbVie’s U.S. Humira revenues declined from approximately $12.2 billion in 2023 to approximately $7.1 billion in 2024. Adalimumab biosimilar market share climbed from 2% at year-end 2023 to above 20% by Q3 2024.
The CVS Caremark move was followed by analogous formulary restructuring at other major PBMs for Humira and, increasingly, for ustekinumab (Stelara) biosimilars. The pattern, once one major PBM breaks ranks, competitive dynamics force the others to follow or risk losing large employer clients who demand biosimilar access, appears to be the mechanism by which rebate walls ultimately collapse in competitive PBM markets.
Investment Strategy: Rebate Wall Collapse Timing
For investors modeling biosimilar market share inflection points, the rebate wall collapse event is a binary catalyst. Biosimilar market share typically remains in low single digits until the first major PBM formulary exclusion of the originator, at which point it inflects sharply upward. The timing of this catalyst can be estimated by tracking: (1) the number of available biosimilars in the market (more competitors give PBMs more negotiating leverage and formulary options); (2) the level of FTC regulatory pressure on the specific originator’s rebate contracts; (3) the originator’s rebate escalation pattern in its most recent PBM contract cycle (escalating rebates signal defensive positioning); (4) large employer public statements about biosimilar demand.
Key Takeaways: Section 12
AbbVie’s Humira rebate wall was maintained by contractual rebate rates of 40%-60% of WAC that generated approximately $1 billion per year in PBM rebate revenue per 100,000 patients, making biosimilar coverage financially irrational under the retained-rebate model. The wall broke in 2024 under the combined pressure of FTC scrutiny, employer demand, and CVS Caremark’s creation of a direct financial interest in biosimilar success through the Cordavis joint venture. Once a major PBM breaks ranks, competitive dynamics force the others to follow, producing a step-change in biosimilar market share.
13. Patient Cost-Sharing: Coinsurance Burden, Prescription Abandonment, and the Copay Coupon Distortion
Patient out-of-pocket costs for specialty biologics are the most visible manifestation of the biologic affordability crisis. For a drug priced at $20,000 per year, a standard 30% coinsurance produces a $6,000 annual patient obligation. Studies show that monthly out-of-pocket costs exceeding $100 directly correlate with increased prescription abandonment rates. At $500 per month, abandonment rates are substantial enough to produce measurable treatment gaps and downstream healthcare costs from uncontrolled disease.
13a. Coinsurance Structures and Their Biosimilar Implications
The shift from flat-dollar copays to percentage-based coinsurance for specialty biologics, which accelerated after the Affordable Care Act and the expansion of specialty drug tiers, theoretically benefits from biosimilar price reductions. A 30% coinsurance on a $15,000 biosimilar produces a $4,500 annual patient obligation versus $6,000 on a $20,000 originator. The patient saves $1,500 per year, and their cost is proportionally lower.
In practice, this straightforward calculation is disrupted by three factors. First, if the biosimilar is placed on a higher-coinsurance tier than the originator (as occurs when the PBM maintains the originator on a preferred tier), the patient’s cost for the biosimilar can exceed the originator cost despite the biosimilar’s lower list price. Second, originator manufacturers offer copay assistance cards that eliminate or reduce patient out-of-pocket costs for commercially insured patients. A patient on the originator with a copay assistance card paying $0 per month has no financial incentive to switch to a biosimilar, even a free one. Third, Medicare beneficiaries cannot use manufacturer copay assistance cards, which means the coinsurance dynamics for Medicare patients are different from commercial patients, and biosimilar pricing is more directly relevant to patient affordability in the Medicare channel.
13b. The Copay Coupon Distortion: How Manufacturer Assistance Cards Preserve Originator Market Share
Manufacturer copay assistance programs, colloquially called copay cards, are typically offered for commercially insured patients and reduce or eliminate the patient’s out-of-pocket cost for the originator drug. A patient on Humira with AbbVie’s myAbbVie Assist program may pay $5 per month regardless of the plan’s stated coinsurance rate.
The commercial logic for the originator manufacturer is straightforward: eliminating the patient’s cost differential removes the financial signal that would otherwise drive patients to request biosimilar switches. The patient’s insurance plan bears the full cost of the high-priced originator (minus the rebate), while the patient faces no cost motivation to switch. This is effective because patient cost-sharing is one of the most reliable behavioral levers for driving medication changes; when it is neutralized, the transition to biosimilars slows substantially.
Payers and PBMs have attempted to address copay card distortions through ‘copay accumulator’ or ‘copay maximizer’ programs, which do not count manufacturer assistance payments toward the patient’s annual deductible or out-of-pocket maximum. Under accumulator programs, the patient’s cost-sharing resets when the copay card’s annual maximum benefit is exhausted, potentially exposing the patient to full coinsurance during the remainder of the plan year. This creates an unpredictable mid-year cost spike and has generated litigation from patient advocacy organizations. CMS limited accumulator programs for Medicare Part D plans effective 2025.
Key Takeaways: Section 13
Patient coinsurance on specialty biologics is a behavioral lever that drives medication switching when the cost differential is meaningful. Manufacturer copay assistance cards neutralize this lever for commercially insured patients by eliminating out-of-pocket cost differences, significantly slowing biosimilar adoption in the commercial channel. Medicare patients cannot use copay cards, making reimbursement-driven price differences more directly impactful in the Medicare channel. Copay accumulator programs attempted to restore cost sensitivity but generated significant patient backlash and regulatory restrictions.
14. Utilization Management as Competitive Weapon: Step Therapy, Prior Authorization, and Formulary Exclusion
Payers deploy utilization management (UM) tools not merely to control costs in the aggregate but to direct specific patients to specific products. In the biosimilar context, UM tools are the primary mechanism through which payers execute their formulary strategy at the individual patient level.
14a. Step Therapy and Fail-First Protocols
Step therapy requires a patient to demonstrate that a lower-cost medication is ineffective or not tolerated before the payer will approve coverage for a more expensive alternative. In the biosimilar context, step therapy can be implemented in two opposite directions.
A payer deploying ‘biosimilar-first’ step therapy requires new patients to initiate treatment on a formulary-preferred biosimilar and document failure or intolerance before the originator will be covered. This protocol rapidly shifts new-patient initiations to the biosimilar without requiring any existing patient to switch. For a biologic with high new-patient volume (treatment-naive patients entering therapy), biosimilar-first step therapy can capture the majority of the incident patient population within 12 to 18 months of implementation.
Retrospective claims analyses of UM-driven biosimilar adoption in the filgrastim and trastuzumab markets found that payer policies incorporating step therapy or mandatory substitution accounted for a large fraction of the biosimilar market share gains observed in the first three years post-launch. In oncology specifically, where prescribing is highly concentrated among a relatively small number of large practices, step therapy implementation is efficiently communicated to the prescriber base and consistently executed.
14b. Prior Authorization as a Directed Prescribing Tool
Prior authorization (PA) requires prescribers to obtain pre-approval before a specific drug is covered. PA can be structured to favor biosimilars by requiring PA only for the originator, making the biosimilar a covered-without-PA ‘preferred’ product. Conversely, PA applied only to the biosimilar (a common early approach in some plans) creates administrative friction that suppresses biosimilar use simply by making it harder to prescribe.
The direction of PA implementation has shifted decisively toward biosimilar promotion as payers have internalized the cost advantages. By mid-2024, major national commercial plans were implementing PA requirements for originator biologics in classes where approved biosimilars were available, with biosimilars as the non-PA-required alternative. This administrative asymmetry is functionally equivalent to the Nordic tendering model in its directional effect: the originator becomes the high-friction, high-documentation choice, and the biosimilar is the path of least resistance.
14c. Formulary Exclusion: The Nuclear Option
Complete formulary exclusion, removing a product from a plan’s covered drug list, is the most aggressive UM tool available to payers and PBMs. An excluded product is not merely non-preferred; it is not covered at all, requiring patients to either switch to the preferred alternative or pay entirely out-of-pocket.
The major national PBMs issue annual formulary exclusion lists that collectively remove hundreds of drugs from coverage, typically those for which lower-cost alternatives (including biosimilars) are available. CVS Caremark’s 2025 national commercial formulary excluded brand-name Humira and several Stelara presentations where biosimilar alternatives had received FDA approval and were available at materially lower net prices. Express Scripts and OptumRx followed with comparable exclusions.
Formulary exclusion is powerful but generates patient and prescriber friction. Patients on stable biologic therapy who are mandated to switch products, even to clinically equivalent biosimilars, experience disruption and uncertainty that can temporarily increase contact with healthcare providers and create adverse event report generation that biosimilar manufacturers must carefully monitor and communicate. Managing the clinical and operational transition of existing patients is as important a commercial capability for biosimilar manufacturers as winning formulary access in the first place.
Key Takeaways: Section 14
Step therapy implementing a biosimilar-first protocol efficiently captures new-patient initiations without forcing existing patient switches, and retrospective evidence confirms it is a major driver of biosimilar market share gains in oncology. Prior authorization asymmetry (requiring PA for the originator, waiving it for the biosimilar) functions as an administrative incentive to prescribe the biosimilar and is increasingly implemented by major commercial payers. Formulary exclusion is the most powerful UM tool but requires active management of patient transitions to avoid adverse event generation that can undermine biosimilar adoption momentum.
15. Case Study: Adalimumab (Humira) – IP Valuation, Rebate Wall Construction, and Market Share Chronology
15a. IP Asset Profile
AbbVie’s adalimumab (Humira) is the highest-grossing pharmaceutical product in history, with approximately $200 billion in cumulative global revenue. The U.S. composition-of-matter patents expired in 2016. AbbVie maintained U.S. market exclusivity through January 2023, seven years after molecular patent expiry, through a patent thicket that eventually encompassed more than 250 related patents. AbbVie executed settlement agreements with all major U.S. biosimilar developers specifying structured entry dates beginning January 31, 2023.
15b. IP Valuation at Thicket Enforcement
The value of the Humira patent thicket, measured as protected revenue attributable to the thicket beyond the composition-of-matter patent expiry, can be quantified using AbbVie’s own reported U.S. revenue. AbbVie reported U.S. Humira revenues of approximately $14.9 billion in 2017, $13.7 billion in 2018, $14.9 billion in 2019, $16.1 billion in 2020, $17.3 billion in 2021, and $18.6 billion in 2022. Total U.S. Humira revenue from the composition-of-matter patent expiry in 2016 through the biosimilar entry date in January 2023: approximately $95 billion.
The EU comparator, where biosimilars entered in October 2018 following the EU composition-of-matter patent expiry, experienced rapid price erosion. European Humira revenues declined approximately 30% in the first year of biosimilar availability and continued declining at 15%-20% annually. Applying the EU erosion trajectory to the U.S. market from 2017 (the first full year after U.S. composition-of-matter expiry) produces a counterfactual U.S. revenue of approximately $50-55 billion for the 2017-2022 period. The thicket protected approximately $40-45 billion in additional U.S. revenue beyond the counterfactual.
This is a conservative estimate because it assumes EU-equivalent biosimilar penetration in the U.S. without a rebate wall. The actual U.S. market structure would likely have produced slower erosion even without the thicket, due to buy-and-bill and PBM dynamics. The thicket’s isolated contribution to revenue protection was approximately $30-40 billion.
15c. Biosimilar Market Share Chronology
| Date | Adalimumab Biosimilar Market Share | Key Event |
|---|---|---|
| Jan. 2023 | 0% | Amgen’s Amjevita (adalimumab-apat) first U.S. launch at $1,318/carton WAC (55% discount) |
| Q1 2023 | ~0.5% | Multiple biosimilars launch at high-WAC/high-rebate and low-WAC/no-rebate dual price points |
| Q2-Q3 2023 | ~1-2% | Rebate wall intact; major PBMs maintain Humira on preferred formulary |
| Q4 2023 | ~2% | Year-end biosimilar share confirms rebate wall holding despite 85% list price discounts |
| Q1 2024 | ~4-6% | PBM formulary renegotiation cycle begins; CVS Caremark signals Humira removal |
| Q2 2024 | ~10-15% | CVS removes Humira from major commercial formularies; Cordavis/Hyrimoz gains preferred position |
| Q3 2024 | >20% | Express Scripts and OptumRx biosimilar position shifts; AbbVie U.S. revenues decline sharply |
| Q4 2024 | ~25-30% | Continued acceleration; AbbVie full-year 2024 U.S. Humira: ~$7.1 billion vs. $12.2 billion in 2023 |
Key Takeaways: Section 15
The Humira patent thicket protected approximately $30-40 billion in U.S. revenues beyond the composition-of-matter patent expiry. Biosimilar market share remained below 2% for 12 full months after biosimilar entry despite 85% list price discounts, confirming the rebate wall’s operational effectiveness. CVS Caremark’s formulary exclusion of Humira in 2024 was the singular catalyst that produced a step-change in biosimilar market share from ~2% to >20% within two quarters. AbbVie’s U.S. Humira revenues declined from $12.2 billion to $7.1 billion in a single year following the formulary shift.
16. Case Study: Infliximab (Remicade) – The U.S.-vs.-EU Adoption Gap in Detail
16a. The Reference Product and Its Market Position
Infliximab (Remicade), a chimeric anti-TNF-alpha monoclonal antibody marketed by Johnson & Johnson (Janssen) and sold in the U.S. through a distribution partnership with Merck, is a physician-administered therapy used for Crohn’s disease, ulcerative colitis, rheumatoid arthritis, ankylosing spondylitis, and plaque psoriasis. It is administered by IV infusion, making it a buy-and-bill product covered under medical benefit rather than pharmacy benefit. This distinction is central to understanding why its U.S. biosimilar adoption trajectory differed from adalimumab’s.
16b. The EU Adoption Story
Biosimilar infliximab (Remsima/Inflectra, CT-P13, developed by Celltrion) launched in the EU in 2013, followed by additional biosimilars. Norway’s national tender for infliximab in 2015 produced a biosimilar winning price approximately 70% below Remicade’s pre-biosimilar price. National health systems across Scandinavia, the Netherlands, and the UK rapidly mandated or financially incentivized biosimilar infliximab use. By 2017, biosimilar market share in Norway exceeded 90%. The UK’s NHS implemented prescribing incentives and achieved comparable penetration.
The EU infliximab market demonstrated that a product with an established patient base, strong physician familiarity with the originator, and active patient advocacy community could nonetheless achieve rapid biosimilar penetration when national reimbursement policy was aligned. The critical enabling factor was not patient or physician preference but payer financial architecture: governments controlled procurement, governments directed the switch, and the switch happened.
16c. The U.S. Adoption Story
In the U.S., biosimilar infliximab (Inflectra, launched 2016) faced the buy-and-bill perverse incentive directly. Infliximab is one of the most commercially significant drugs in rheumatology and gastroenterology practices. The margin on Remicade in large practices, particularly those with 340B status, was substantial, and the economic case for switching to Inflectra, priced at approximately 15% below Remicade initially, was weak. Four years after the first U.S. biosimilar infliximab launch, market share remained below 10%.
The contrast with the EU is stark and instructive. The U.S. lacked the top-down procurement authority that European national health systems exercised. American physicians in buy-and-bill practices had a direct financial incentive to maintain originator use. Janssen executed a sophisticated originator defense that included competitive contracting with PBMs and hospitals and vigorous physician education emphasizing the ‘high similarity’ language.
The U.S. infliximab market did eventually shift as additional biosimilars entered (Renflexis, Avsola, Ixifi, Hyrimoz-SC) and as payer step therapy and prior authorization policies mandated biosimilar trial. By 2024, U.S. biosimilar infliximab market share had risen to approximately 30-40% of volume, driven primarily by payer UM policy rather than provider financial preference.
Key Takeaways: Section 16
Infliximab’s U.S.-vs.-EU adoption gap, less than 10% U.S. share at four years post-launch versus more than 70% EU share, is the quantitative evidence most frequently cited in policy discussions about U.S. biosimilar adoption failures. The primary cause was the buy-and-bill perverse incentive in U.S. physician practices, amplified by 340B program margin dynamics. European adoption was driven by national procurement authority, not physician preference. U.S. infliximab market share eventually climbed to 30-40% by 2024, driven by payer UM policies, demonstrating that payer tools can partially compensate for the buy-and-bill structural barrier even without the IRA’s formula change.
17. Case Study: Trastuzumab (Herceptin) – Why Oncology Biosimilars Penetrate Faster
17a. Why Trastuzumab Is Different
Trastuzumab (Herceptin, Genentech/Roche) is an anti-HER2 monoclonal antibody approved for HER2-positive breast cancer and HER2-positive metastatic gastric or gastroesophageal junction adenocarcinoma. Six biosimilar trastuzumab products received FDA approval between 2019 and 2021. By 2022, biosimilars had captured the majority of the U.S. trastuzumab market, a penetration rate substantially faster than either infliximab or adalimumab achieved in comparable timeframes.
17b. Structural Factors Enabling Faster Penetration
Several structural characteristics of the oncology market accelerated biosimilar trastuzumab adoption beyond what was observed in rheumatology and gastroenterology.
Treatment setting concentration: oncology drug administration is highly concentrated in a smaller number of large academic medical centers, cancer network hospitals, and integrated oncology practices compared to the fragmented community infusion center landscape for rheumatology biologics. When a major oncology network or academic cancer center adopts a trastuzumab biosimilar as its formulary standard, that decision covers thousands of patients. A single formulary decision by a major GPO (Group Purchasing Organization) can move more volume than hundreds of individual practice-level decisions in rheumatology.
GPO leverage: oncology practices disproportionately use GPO contracts for drug procurement, and GPOs have been active drivers of biosimilar trastuzumab adoption by negotiating GPO-level preferred biosimilar pricing that creates compelling acquisition cost advantages for member practices even under the buy-and-bill formula.
Treatment-naive new patients: breast cancer has high incidence and relatively short treatment durations compared to chronic autoimmune diseases. A large fraction of trastuzumab-treated patients are initiating therapy for a new diagnosis rather than continuing long-term maintenance therapy. New-patient initiations are the easiest to direct toward biosimilars because there is no existing treatment to disrupt.
IRA incentive relevance: trastuzumab is Medicare-heavy (breast cancer incidence peaks in older demographics). The IRA’s ASP+8% provision is more commercially relevant for trastuzumab than for adalimumab, which has a broader age distribution.
Key Takeaways: Section 17
Trastuzumab biosimilars achieved majority U.S. market share within three years of launch due to GPO leverage, high treatment-naive new-patient volume, concentrated prescribing in large oncology networks, and an older patient population where Medicare reimbursement dynamics (including the IRA provision) are more relevant. The oncology biosimilar model is structurally more favorable for rapid adoption than the rheumatology/autoimmune model. Investor models for oncology biosimilars should reflect this and apply different penetration rate assumptions than for self-administered autoimmune biologics.
18. Case Study: Ustekinumab (Stelara) – The Second Major Biologic LOE and What It Signals
18a. IP and Market Position
Johnson & Johnson’s ustekinumab (Stelara), an anti-IL-12/23 monoclonal antibody, had peak global revenues of approximately $9.7 billion in 2022, with approximately $6.5 billion in the U.S. Its primary U.S. patents expired in late 2023, and the first U.S. biosimilar ustekinumab products received FDA approval and began commercial launch in early 2024. Stelara is self-administered (subcutaneous injection) and covered under the pharmacy benefit, making its reimbursement dynamics more analogous to Humira than to Remicade.
18b. What Stelara’s LOE Tests
Stelara’s biosimilar entry is the second major pharmacy-benefit biologic LOE after adalimumab and provides a test of whether the structural changes observed in the adalimumab market, PBM formulary exclusions, private-label biosimilar partnerships, and accelerated step therapy implementation, are generalizing to new molecules.
Early evidence suggests the transition to biosimilar ustekinumab is proceeding faster than the adalimumab transition did in its first year. PBMs had 12 months of observational learning from the adalimumab market by the time biosimilar ustekinumab launched. CVS Caremark, Express Scripts, and OptumRx were all prepared with formulary strategies for Stelara biosimilars that reflected their acquired experience from the Humira market shift. The ‘rebate wall build, hold, break’ cycle that took 18 months to complete for adalimumab appears to be compressing for ustekinumab.
18c. IP Valuation at Stelara LOE
J&J’s Stelara patent thicket was thinner than AbbVie’s Humira portfolio. J&J listed approximately 145 patents in the Purple Book, compared to AbbVie’s 250+. Settlement agreements with biosimilar developers specified entry dates in late 2023 through mid-2024, a shorter delay beyond the composition-of-matter patent expiry than AbbVie achieved. J&J’s LOE preparation strategy was more reliant on its pipeline successor Tremfya (guselkumab, an anti-IL-23 antibody) than on patent thicket defense, a different lifecycle management posture than AbbVie’s.
Key Takeaways: Section 18
Stelara’s biosimilar transition appears to be accelerating faster than adalimumab’s due to PBM market learning, pre-positioned formulary strategies, and a thinner patent thicket that produced a shorter delay beyond composition-of-matter expiry. J&J’s lifecycle management posture relied more on successor product positioning (Tremfya) than on patent thicket defense, suggesting differentiated strategic approaches among originator manufacturers facing biologic LOE. The rate of the Stelara biosimilar transition relative to adalimumab will be closely monitored as a calibration data point for Keytruda and Dupixent LOE modeling.
19. The BPCIA Patent Dance: Litigation Architecture, Settlement Economics, and IPR Interaction
The BPCIA’s patent dispute resolution mechanism, colloquially called the ‘patent dance,’ is a multi-step compelled disclosure and negotiation process that governs how biosimilar manufacturers and reference product sponsors (RPSs) exchange information and resolve patent disputes before a biosimilar launch.
19a. The Statutory Dance Steps
The patent dance proceeds in a structured sequence. Within 20 days of FDA acceptance of a 351(k) application, the biosimilar applicant must provide the RPS with a copy of its complete manufacturing process description, including cell culture, purification, formulation, and quality control procedures. This ‘aBLA package’ disclosure is compelled by statute and is the most commercially sensitive information a biosimilar developer possesses. It reveals the specific process the developer has designed, which the RPS uses to assess which of its process patents may be infringed.
Within 60 days of receiving the aBLA package, the RPS must provide the biosimilar applicant with a list of all patents it believes could be asserted against the applicant’s product and process. Within 60 days of receiving the RPS’s list, the applicant provides a claim-by-claim explanation of why each listed patent is invalid, unenforceable, or not infringed. The parties then negotiate, within 15 business days, which patents to litigate in the first phase of litigation (‘immediate patent resolution’). Any patents not selected for immediate litigation are subject to a ‘second notice’ lawsuit at 180 days before commercial launch.
The patent dance is optional for biosimilar applicants: a developer can choose to skip all steps except the 180-day notice and sue-on-notice provision. The consequence of skipping the dance is losing the benefit of the ‘immediate patent resolution’ process but avoiding the compelled disclosure of manufacturing process information. Developers with novel processes that they prefer to keep confidential have chosen this path, accepting the later and less structured litigation posture.
19b. Settlement Economics in BPCIA Litigation
The vast majority of BPCIA patent disputes resolve through settlement rather than trial. Settlement economics in biosimilar patent litigation are determined by the RPS’s and biosimilar developer’s respective NPVs under three scenarios: settlement with a negotiated entry date, litigation outcome (win/loss), and at-risk launch.
From the RPS’s perspective, a settlement that secures a defined entry date well into the future (providing multiple additional years of branded revenue) is economically superior to trial outcome uncertainty, even if the RPS believes its patents are strong. The calculus changes if multiple biosimilar developers are simultaneously in patent dance negotiations: settlements with each developer individually, at staggered entry dates, can maintain an orderly market introduction that manages price erosion more predictably than a single adverse court decision that could enable simultaneous entry by all biosimilar applicants.
AbbVie’s adalimumab settlement strategy, which produced staggered U.S. entry dates negotiated individually with each biosimilar developer, was a masterclass in using settlement timing to control the competitive entry sequence. No single biosimilar received a day-one market entry advantage; all were bound by negotiated entry dates that AbbVie had some influence over through the settlement terms.
19c. At-Risk Launch and Injunction Dynamics
An at-risk launch in the biosimilar context carries different risk characteristics than in the small molecule context. If a biosimilar launches at risk and the court subsequently issues a preliminary or permanent injunction, the developer must immediately cease distribution and may face destruction-of-inventory orders for product already in the supply chain. The damages calculation in a successful BPCIA infringement case is the RPS’s lost profits attributable to the at-risk period, which can be substantial for a high-revenue biologic even over a short commercial period.
The structural complexity of biologic supply chains amplifies the at-risk launch risk. Biologic manufacturing requires long lead times (3 to 6 months from cell culture initiation to final product release), meaning a biosimilar developer that suspends commercial supply under an injunction cannot quickly restart it. The supply gap created by an injunction can permanently damage commercial relationships with specialty pharmacies and infusion centers that have already transitioned patients to the biosimilar.
Key Takeaways: Section 19
The BPCIA patent dance’s compelled disclosure of manufacturing process information is the most commercially sensitive element of the biosimilar litigation process, and developers with novel processes rationally choose to skip the dance to protect that information. Settlement economics strongly favor negotiated entry dates over trial for both parties, and RPS settlement strategies that stage entry dates for multiple biosimilar developers can manage competitive entry dynamics more effectively than relying on litigation outcomes. At-risk biosimilar launch carries supply chain complications beyond financial damages that small molecule at-risk launch models do not capture.
20. Value-Based Care as the Long-Term Reimbursement Solution: EOM, APMs, and the Incentive Alignment Problem
The ASP-plus-add-on formula and the PBM rebate model are both products of fee-for-service (FFS) reimbursement architecture. Their shared deficiency is that they reward the use of high-cost products rather than the achievement of efficient, high-quality patient outcomes. The long-term structural solution to biosimilar adoption resistance is the replacement of FFS mechanics with value-based care (VBC) frameworks that align provider financial incentives with the goal of delivering equivalent clinical outcomes at the lowest total cost of care.
20a. CMS’s Enhancing Oncology Model
CMS’s Enhancing Oncology Model (EOM), launched July 1, 2023, is the most commercially significant current VBC model for biologic reimbursement. Under the EOM, oncology practices receive monthly enhanced payments for attributed Medicare beneficiaries with cancer who are undergoing chemotherapy, in exchange for accountability for the total cost of care for those beneficiaries’ cancer episodes. Practices that keep total episode costs below a benchmark receive a shared savings payment. Practices that exceed the benchmark pay a performance penalty.
The EOM creates a direct financial incentive to prescribe lower-cost biosimilars in place of higher-cost originator biologics for every indication where biosimilars are available. A practice that switches from originator trastuzumab to a biosimilar for all eligible breast cancer patients reduces its per-episode total drug cost. If that reduction contributes to the practice staying below its benchmark, the practice earns a shared savings payment that exceeds any margin it would have earned from the higher-priced originator under FFS buy-and-bill.
The EOM model covers seven cancer types: breast, chronic leukemia, small intestine/colorectal, lung, lymphoma, multiple myeloma, and prostate cancer. Participation is voluntary, and early reports on participation rates suggest that larger, better-resourced practices with strong data infrastructure are overrepresented in the EOM participant pool, while smaller community practices (which collectively represent a large fraction of Medicare oncology volume) are underrepresented. Broadening VBC model participation to include smaller practices is a structural priority for CMS.
20b. APM Design Principles for Biosimilar Adoption
For a VBC model to function as a biosimilar adoption accelerator, it must satisfy several design conditions.
Drug cost must be within the accountable cost perimeter. If drug costs are carved out of the episode cost benchmark, provider groups have no financial accountability for drug spend and no incentive to select lower-cost biologics. The EOM includes drug costs in the total episode cost benchmark, which is the correct design for biosimilar adoption incentives.
Quality measures must confirm clinical equivalence of biosimilars. If a VBC model’s quality metrics reward specific clinical outcomes without distinguishing between originator and biosimilar achievement of those outcomes, providers who use biosimilars receive equivalent quality credit. Quality metric design that inadvertently penalizes biosimilar use (for example, by measuring outcomes in ways that the historical originator experience has calibrated but biosimilar real-world data has not yet matched) would undermine adoption.
Transition support must address the administrative costs of switching existing patients. Moving a practice’s established biologic patient population to biosimilars requires EHR updates, pharmacy reprogramming, patient communication, and clinical monitoring protocols. VBC models should either include transition support payments or build transition costs into the benchmark calculation.
Key Takeaways: Section 20
The Enhancing Oncology Model creates a direct financial incentive for participating oncology practices to prescribe biosimilars by including drug costs in the total episode cost benchmark. VBC model design must include drug costs within the accountable perimeter, apply quality metrics that do not inadvertently penalize biosimilar use, and provide transition support for patient switching. Voluntary participation limits EOM impact: smaller community practices are underrepresented, and broadening participation is the primary CMS policy priority for extending VBC biosimilar incentives to the full Medicare oncology patient population.
21. Global Reimbursement Comparative Framework: U.S., Germany, France, UK, and Japan
21a. Germany: AMNOG and Reference Pricing
Germany’s Act on the Reform of the Market for Medicinal Products (AMNOG), enacted in 2011, subjects all newly approved drugs to a mandatory benefit assessment within 12 months of launch. The assessment determines whether the drug provides an ‘additional benefit’ over the appropriate comparator therapy. If no additional benefit is established, the drug is priced at the level of the comparator (reference pricing). If additional benefit is established, the manufacturer and the National Association of Statutory Health Insurance Funds (GKV-SV) negotiate a price capped by the benefit assessment outcome.
For biosimilars, Germany’s framework combines AMNOG reference pricing with a robust tendering system operated by individual statutory health insurance funds (Krankenkassen). A Krankenkasse can issue a tender for a specific biologic class, and the winning biosimilar captures the insured population of that fund for the tender period. Competition among biosimilar manufacturers for tender contracts drives prices to levels well below those achievable in the U.S. market.
Germany’s biosimilar infliximab penetration exceeded 80% within three years of first biosimilar launch, driven primarily by tender-based procurement that the U.S. equivalent (GPO contracting) partially but imperfectly replicates.
21b. UK: NHS Prescribing Incentives and ‘Best Value Biologics’
The UK’s National Health Service introduced the ‘Best Value Biologics’ (BVB) framework in 2020 to accelerate biosimilar adoption by creating explicit financial incentives for prescribers and NHS trusts to switch from originator biologics to biosimilars when clinically appropriate. Under BVB, NHS integrated care systems (ICSs) receive financial benefit from the cost savings generated by biosimilar prescribing, aligning local NHS financial accountability with biosimilar uptake.
The NHS also implemented a specific switching protocol that requires NHS trusts to develop patient communication materials, training for clinical staff, and clear clinical governance frameworks for biosimilar transitions. This operational support reduced prescriber and patient hesitancy and contributed to UK biosimilar penetration rates that consistently rank among the highest in the EU.
21c. Japan: Prescribing Targets and NHI Reimbursement
Japan’s Ministry of Health, Labour, and Welfare (MHLW) set a national target of 80% generic/biosimilar utilization as a share of total volume, a policy explicitly designed to drive cost containment in Japan’s aging population health system. NHI reimbursement prices for biosimilars are set at a defined percentage of the originator’s NHI price, with the percentage varying by product type and level of competition.
Physician incentives in Japan are structured differently from U.S. buy-and-bill: physicians in Japan do not profit from drug margins in the same way because most drugs are dispensed by independent pharmacies rather than administered in-office. This structural absence of the buy-and-bill margin dynamic makes physician-level adoption incentives less financially distorted than in the U.S., contributing to a more straightforward policy implementation pathway for biosimilar prescribing targets.
Global Reimbursement Comparative Table
| Feature | U.S. | Germany | UK | Japan |
|---|---|---|---|---|
| Procurement Model | Fragmented, PBM-mediated + buy-and-bill | Statutory fund tenders (GKV) + AMNOG | NHS Best Value Biologics framework | NHI price list, pharmacy dispensing |
| Biosimilar Price Mechanism | Market-negotiated (PBM rebate) + ASP | Tender + AMNOG reference pricing | Negotiated NHS national price | NHI administrative price setting |
| Pharmacy Substitution | Interchangeable designation required | Permitted for all approved biosimilars | Permitted within NHS BVB protocols | Permitted with prescriber notification |
| Buy-and-Bill Perverse Incentive | Present and material | Minimal (drug margin not a physician revenue driver) | Minimal (NHS employment model) | Minimal (pharmacy dispensing separate) |
| Biosimilar Penetration Speed | Slow (pharmacy-benefit), Moderate (oncology) | Fast (tender-driven) | Fast (BVB-incentivized) | Moderate (policy-target-driven) |
| Infliximab Biosimilar Share (3yr) | <10% | >70% | >70% | ~40-50% |
Key Takeaways: Section 21
Germany’s AMNOG-plus-tender framework and the UK’s NHS Best Value Biologics program are the international models that most closely approximate what comprehensive U.S. biosimilar adoption policy reform would need to produce. Japan’s separation of physician prescribing from pharmacy dispensing removes the buy-and-bill perverse incentive at the source. The common feature of all high-adoption markets is procurement authority either at the national level (tenders) or institutional level (NHS trust formularies) that overrides individual prescriber financial preference.
22. The Biosimilar Void: 90% of LOE Biologics Will Have No Biosimilar Challenger
IQVIA’s analysis of the biosimilar development pipeline against the universe of biologics expected to face LOE over the next decade identified a striking gap: approximately 90% of reference biological products losing exclusivity will have no biosimilar competitor. This ‘biosimilar void’ is not primarily a regulatory or scientific failure. It is a market economics failure.
22a. Why the Void Exists
The biosimilar development economics that enable competition depend on a market size threshold that most biologics do not meet. Developing a biosimilar costs $100-$250 million and takes 7-9 years. To achieve an acceptable return on this investment, the target market must be large enough, and the biosimilar’s expected market share and price must be high enough, to generate net revenues sufficient to cover development costs plus cost of goods plus commercial expenses.
For a biologic with $200 million in annual U.S. revenue (far below blockbuster scale), a biosimilar manufacturer that achieves 40% market share at a 30% discount would generate approximately $56 million in annual U.S. revenue. At a 30% gross margin, this produces $16.8 million in annual gross profit, requiring 6 to 15 years to recoup a $100-250 million development investment. In a market with two or three biosimilar competitors, the individual market share would be lower, the price competition more severe, and the payback period longer. The biosimilar economics are simply unworkable below a market size threshold of approximately $500 million to $1 billion in annual U.S. revenue for most standard-complexity monoclonal antibodies.
This leaves the patients who rely on biologics with revenues below that threshold facing continued originator monopoly pricing indefinitely after LOE, with no realistic prospect of biosimilar-driven price relief. For rare disease biologics with small patient populations and high per-patient costs, the void is particularly acute: high unit costs combined with small total markets produce economics that do not support biosimilar development even when per-patient pricing is extreme.
22b. Policy Responses to the Void
Several policy approaches have been proposed to address the biosimilar void. The FDA’s Center for Biologics Evaluation and Research (CBER) has worked to reduce regulatory burden and development costs for biosimilars in underserved markets through product-specific development guidances that clarify exactly what evidence the FDA requires, reducing the uncertainty premium that developers must build into development budgets.
The IRA’s drug price negotiation provision, which targets high-revenue biologics, perversely reduces the biosimilar development incentive for the most commercially significant molecules by reducing the originator’s price to a level closer to what a biosimilar would offer, thereby compressing the market opportunity for the biosimilar developer. The IRA does not create any compensating incentive for biosimilar development in smaller markets.
Academic and policy proposals have included a government-funded or subsidized biosimilar development program for rare disease biologics, analogous to the NIH-supported development of certain orphan drugs. No such program has been enacted, but the biosimilar void represents a growing policy gap that limits the healthcare system’s ability to use biosimilar competition as a cost-containment tool for the full range of high-cost biological therapies.
Key Takeaways: Section 22
Approximately 90% of biologics facing LOE will not attract a biosimilar developer, because market size economics do not support the $100-250 million development investment for most non-blockbuster molecules. The IRA’s drug price negotiation provision, while reducing originator prices, also reduces the market opportunity for biosimilar developers, potentially worsening the void for major biologics selected for negotiation. No current U.S. policy program addresses the biosimilar void for rare disease or low-revenue biologics. This structural gap represents the most significant unaddressed market failure in U.S. biosimilar policy.
23. Investment Strategy: Patent Expiry, Formulary Events, and the LOE Alpha Signal
23a. Building the Biologic LOE Calendar
The Purple Book, the FDA’s equivalent of the Orange Book for biological products, lists all approved biological products and their biosimilars. Unlike the Orange Book, the Purple Book does not list patent information directly. Patent surveillance for biologics requires tracking the BPCIA patent dance dockets in federal district court, monitoring PTAB IPR petition filings, and tracking Orange Book listings for any biologic-small molecule combinations.
The analytically useful LOE calendar for any biologic requires at minimum: the 12-year BPCIA reference product exclusivity expiry date, the date of first 351(k) application filing (publicly visible through FDA’s biologics licensing database), the existence and terms of any disclosed settlement agreements specifying entry dates, any pending PTAB IPR petitions on process or formulation patents, and the number of 351(k) BLA applications currently under FDA review or approved.
23b. Formulary Change as a Discrete Investable Catalyst
The adalimumab market demonstrated that formulary change events are discrete, dateable, and produce quantifiable market share responses. CVS Caremark’s formulary change announcement preceded the effective date by several months, providing investors with an advance signal. The market share response was measurable within two quarters of the effective date.
For investors monitoring the biosimilar market, tracking PBM formulary change announcements, which are communicated to plan members and prescribers and are partially disclosed through plan benefits documentation, is a leading indicator of market share inflections. PBMs typically announce formulary changes for the following calendar year in September and October. Monitoring these announcements for originator exclusions or biosimilar preferred-tier placements provides a six-to-nine-month advance signal for market share inflections.
23c. Short-Side and Long-Side Positioning
On the short side: originator biologic manufacturers whose leading products face a combination of (1) thin patent thickets with multiple BPCIA settlements already executed and entry dates within 24 months, (2) PBM contract cycles expiring within 12 months, and (3) FTC rebate wall scrutiny are in the highest risk quadrant. Revenue model over-reliance on a single biologic facing these combined pressures, as AbbVie was with Humira by 2022, creates a short-side opportunity in the 12-to-24 months before the rebate wall collapses.
On the long side: biosimilar manufacturers with early formulary exclusivity for a major biologic class, either through first-mover Paragraph IV-equivalent settlement terms or through PBM private-label partnerships, are positioned for step-change revenue events. Sandoz’s Cordavis relationship with CVS Caremark for adalimumab is the prototype. Monitoring similar PBM-biosimilar manufacturer partnership announcements for ustekinumab, mepolizumab, dupilumab, and eventually pembrolizumab biosimilar programs is the key intelligence priority for the long side.
23d. IRA Drug Negotiation Interaction with Biosimilar Valuations
The IRA’s selection of specific drugs for Medicare price negotiation creates a direct interaction with biosimilar development valuations. A biologic selected for IRA negotiation before biosimilars have achieved significant market penetration will have its Medicare price reduced to the ‘maximum fair price’ (MFP). This MFP reduces the market opportunity for biosimilar developers, because the biosimilar’s competitive price advantage over the IRA-negotiated originator is compressed. In extreme cases, the MFP could be set at a level close to what biosimilar manufacturers would need to charge to recover development costs, making the biosimilar program economically unviable.
The race between IRA negotiation timelines and biosimilar development timelines is a new variable in biologic LOE modeling that did not exist before 2022. For any biologic in biosimilar development programs that is also a potential IRA negotiation candidate, the probability and expected timing of IRA selection should be explicitly modeled as a downside scenario to the biosimilar’s expected net present value.
Key Takeaways: Section 23
The biologic LOE calendar requires Purple Book exclusivity tracking, BPCIA court docket monitoring, and PTAB petition surveillance, as the Purple Book does not include patent expiry dates directly. PBM formulary change announcements in September and October each year are leading indicators of the following year’s biosimilar market share inflections, providing investors with a 6-to-9-month advance signal. The IRA’s drug price negotiation creates a new downside scenario for biosimilar NPV models by compressing the price advantage that a biosimilar can offer over an IRA-negotiated originator.
24. Master Key Takeaways and Glossary
Master Key Takeaways
Biologics account for 46% of U.S. drug spending while serving less than 2% of patients. Total biosimilar savings through 2024 were approximately $36 billion against a projected $133 billion by 2025. The gap is a reimbursement architecture problem, not a science problem.
The buy-and-bill model’s ASP-plus-6% formula financially penalizes biosimilar prescribing for every physician-administered biologic, quantifiable at $18 or more per dose in standard scenarios. The 340B program amplifies this perverse incentive in hospital outpatient settings to a degree that the IRA’s ASP+8% formula change cannot overcome.
PBM rebate walls held adalimumab biosimilar market share at 2% for 12 full months despite 85% list price discounts. A single PBM formulary exclusion event by CVS Caremark produced a market share inflection from 2% to above 20% within two quarters.
The FDA’s proposed elimination of the interchangeability designation from biosimilar labeling would remove a two-tier perception system that has impeded adoption without clinical justification and would reduce development costs by $20-50 million per biosimilar program.
Approximately 90% of biologics facing LOE will attract no biosimilar competition because their market size economics do not support $100-250 million development investments. This biosimilar void is the most significant unaddressed market failure in U.S. biosimilar policy.
Value-based care models that include drug costs within the accountable cost perimeter, such as CMS’s Enhancing Oncology Model, are the structural long-term solution to the buy-and-bill perverse incentive. Their limited voluntary participation rate constrains their near-term market impact.
The IRA’s drug price negotiation provision creates a new downside scenario for biosimilar NPV models by potentially compressing the price advantage biosimilars can offer over IRA-negotiated originators. Biosimilar developers should scenario-model IRA selection timing for each target molecule.
The BPCIA patent dance’s compelled manufacturing process disclosure is the most commercially sensitive element of biosimilar patent litigation, and developers with novel processes rationally skip the dance to protect that information.
Glossary
ASP (Average Sales Price): Manufacturer-reported average realized price per billing unit, net of most discounts and rebates, used by CMS as the basis for Medicare Part B drug reimbursement. Published quarterly on a six-month lag.
BPCIA (Biologics Price Competition and Innovation Act): The 2009 statute creating the 351(k) abbreviated licensure pathway for biosimilars, the 12-year reference product exclusivity, and the patent dance dispute resolution mechanism.
Buy-and-Bill: The reimbursement model for physician-administered drugs in which the provider purchases the drug, administers it, and bills the payer for both the drug cost and an administration fee. Dominant for oncology and IV-administered rheumatology biologics.
Copay Accumulator/Maximizer: A payer program that does not count manufacturer assistance payments toward the patient’s annual deductible or out-of-pocket maximum, preventing copay cards from eliminating the patient’s cost-sharing exposure to high-priced biologics.
EOM (Enhancing Oncology Model): CMS’s value-based care model for oncology practices that creates two-sided financial accountability for total episode costs, incentivizing use of lower-cost biosimilars to stay below the episode cost benchmark.
Extrapolation: The regulatory principle allowing a biosimilar approved in one indication to receive approval for all indications of the reference product without separate clinical trials in each indication, based on scientific justification of consistent mechanism of action.
Gross-to-Net Gap: The difference between a drug’s WAC (list price) and its net realized price after accounting for all rebates, chargebacks, and discounts. For high-rebate biologics, the gross-to-net gap can exceed 50% of WAC.
Inherent Variability: The natural, batch-to-batch structural variation in biological products produced in living cell systems. Present in both originator biologics and biosimilars; accepted within specified ranges in regulatory approval.
Interchangeability: The FDA designation for a biosimilar that has met additional evidence requirements allowing automatic pharmacy substitution without prescriber intervention. Under proposed FDA reform, this designation would be eliminated from product labeling.
Patent Dance: The BPCIA’s multi-step compelled information exchange and patent dispute negotiation process between a biosimilar applicant and the reference product sponsor.
Purple Book: The FDA’s registry of approved biological products and their biosimilars. Unlike the Orange Book, does not include patent expiry information.
Rebate Wall: A contractual arrangement in which an originator manufacturer pays volume-linked rebates to a PBM or payer contingent on the payer granting the originator exclusive or dominant formulary position, financially penalizing the adoption of lower-cost biosimilars.
Reference Product Exclusivity: The 12-year period under BPCIA during which the FDA cannot approve a 351(k) biosimilar application referencing the innovator’s data. Cannot be shortened by patent challenges.
Step Therapy: A utilization management protocol requiring patients to try a preferred (typically lower-cost) medication before a more expensive alternative is covered. Can be directed toward biosimilars (biosimilar-first step therapy) to accelerate adoption.
Totality of the Evidence: The FDA’s regulatory standard for biosimilar approval, requiring a comprehensive analytical, nonclinical, and clinical data package demonstrating no clinically meaningful differences from the reference product across all relevant quality attributes.
WAC (Wholesale Acquisition Cost): The manufacturer’s published list price to wholesalers. The starting point for rebate calculations and the reference price for most PBM contracting. Does not reflect net prices after rebates.
340B Program: A federal program requiring pharmaceutical manufacturers to provide outpatient drugs at steeply discounted prices (up to 50% below non-340B) to qualifying covered entities including hospitals. Creates amplified buy-and-bill perverse incentives for high-priced originator biologics.
This analysis is intended for pharmaceutical IP professionals, managed care strategists, health economics teams, and institutional investors. It reflects publicly available data and policy analysis. Reimbursement formulas, FDA guidance positions, and PBM formulary decisions are subject to change. All financial figures are sourced from company disclosures, CMS databases, and published academic analyses unless otherwise noted.