A strategic analysis for pharmaceutical companies, generic manufacturers, investors, and policy professionals
The Indian Clock

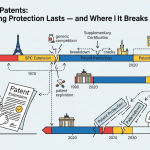
In most patent systems, the question ‘how long does a patent last?’ has a simple answer: 20 years from the filing date. In India, that answer is technically correct but operationally misleading. The statutory term is 20 years, but the actual commercial exclusivity a drug company can expect in India is shaped by a thicket of provisions that exist nowhere else in the developed world: a unique anti-evergreening clause, no patent term extensions, no data exclusivity, active compulsory licensing, pre-grant and post-grant opposition proceedings, and a judiciary that has repeatedly ruled against multinational pharmaceutical companies on questions that would go the other way in the United States or Europe.
For a foreign pharmaceutical company entering India with a blockbuster drug, the effective exclusivity period can range from zero (if the compound patent is rejected under Section 3(d) of the Patents Act) to the full 20 years from the priority date, minus development time, minus regulatory approval delays, and minus any time lost to opposition proceedings. Understanding which of these applies to your drug, and why, is one of the most commercially important questions in global pharmaceutical strategy.
India is not a minor market. It has 1.4 billion people, a rapidly expanding middle class, and one of the world’s fastest-growing pharmaceutical sectors, forecast to reach $130 billion in annual market value by 2030 [1]. It is simultaneously the world’s largest producer of generic medicines by volume, supplying approximately 20 percent of global generic drug exports by value and more than 60 percent of global vaccine supply [2]. Every decision India’s patent system makes about how long a drug patent lasts reverberates through the pricing and access calculations of every other country on earth.
This guide builds a complete picture of drug patent duration in India: the legal architecture, the exceptions, the litigation landscape, how Indian courts have applied these rules to specific drugs, what happens when a patent runs out, and what companies on both sides of the innovator-generic divide should be doing right now to protect their positions.
The Legal Architecture: Patents Act 1970 and the 2005 Amendment
Why 1970 Matters
India’s Patents Act 1970 was drafted deliberately to favor generic manufacturing. The government of the time recognized that pharmaceutical prices under a full product patent regime would be unaffordable for most of the population, so it eliminated product patents on pharmaceutical substances entirely, permitting only process patents. This meant that as long as a generic manufacturer could find a different route to synthesize the same active pharmaceutical ingredient (API), it could produce and sell the drug freely, regardless of what patents existed elsewhere in the world.
The practical consequence was the creation of the Indian generic pharmaceutical industry as a global force. Companies like Cipla, Ranbaxy (now Sun Pharmaceutical Industries), Dr. Reddy’s Laboratories, and Aurobindo Pharma built their businesses under a framework that treated pharmaceutical patents as barriers to public health rather than rewards for innovation. By the 1990s, Indian generic manufacturers were exporting to more than 150 countries, supplying the anti-retroviral drugs that made HIV treatment accessible in sub-Saharan Africa and other low-income regions at a fraction of the branded price.
That system was legally consistent with the General Agreement on Tariffs and Trade (GATT) framework that preceded the World Trade Organization. But India’s accession to the WTO in 1995, and its obligations under the Agreement on Trade-Related Aspects of Intellectual Property Rights (TRIPS), required it to amend its patent law to permit product patents on pharmaceutical substances. The transition period for developing countries extended to January 1, 2005.
The 2005 Amendment: TRIPS Compliance With Indian Characteristics
The Patents (Amendment) Act 2005 introduced product patents on pharmaceutical and agrochemical substances for the first time since 1970, bringing India formally into compliance with TRIPS. The amendment was not optional. WTO dispute settlement mechanisms backed by the threat of trade sanctions gave the Indian government no realistic alternative.
But the government embedded in the amendment a provision that has no equivalent in any other TRIPS-compliant patent system: Section 3(d). This clause, inserted into the list of subject matter not patentable in India, states that ‘the mere discovery of a new form of a known substance which does not result in the enhancement of the known efficacy of that substance’ is not patentable. New polymorphs, isomers, esters, ethers, salts, metabolites, prodrugs, and combinations of known substances are all presumptively excluded from patentability unless the applicant can demonstrate a significant improvement in known therapeutic efficacy.
The pharmaceutical industry’s reaction was immediate and hostile. Multinational companies argued that Section 3(d) violated TRIPS by restricting the scope of patentable subject matter beyond what the agreement permitted. The WTO’s TRIPS Council considered the issue. India argued, correctly as it turned out, that TRIPS Article 27 permits member states to exclude certain inventions from patentability for reasons of public interest, and that the scope of the word ‘invention’ in Article 27 does not mandate patentability of minor modifications to known substances. No formal WTO dispute panel has ruled against Section 3(d) to date.
The Text of Section 3(d) and What It Covers
Section 3(d) of the Patents Act 1970 (as amended in 2005) reads in relevant part: ‘the mere discovery of a new form of a known substance which does not result in the enhancement of the known efficacy of that substance’ is not an invention. The section includes an explanatory note that salts, esters, ethers, polymorphs, metabolites, pure form, particle size, isomers, mixtures of isomers, complexes, combinations, and other derivatives of a known substance shall be considered the same substance unless they differ significantly in properties with regard to efficacy.
In pharmaceutical terms, this covers the most common evergreening strategies used by multinational pharmaceutical companies in markets without this restriction. Filing patents on new polymorphs of existing APIs, on new salts or esters that offer better bioavailability but not enhanced efficacy in the clinical sense, on prodrug forms of known compounds, or on new crystalline structures all face rejection under Section 3(d) in India. The clause effectively resets the patent clock for known pharmaceutical compounds and prevents the incremental extension strategies that have generated billions of dollars in extended exclusivity in the United States and Europe.
The Novartis Glivec Case: Section 3(d) Defined
The definitive interpretation of Section 3(d) came in Novartis AG v. Union of India, decided by the Supreme Court of India in April 2013 [3]. Novartis had applied for a patent on the beta crystalline form of imatinib mesylate, the active ingredient in Gleevec (known as Glivec in India), its treatment for chronic myelogenous leukemia (CML). Imatinib itself had been synthesized and patented in the 1990s. The compound patent, filed under a then-existing mechanism called a ‘mailbox application,’ was pending. Novartis sought a separate product patent on the specific crystalline form.
The Indian Patent Office rejected the application on Section 3(d) grounds. Novartis appealed through the Intellectual Property Appellate Board and ultimately to the Supreme Court, where a two-judge bench spent years on the case before issuing a unanimous 112-page decision rejecting Novartis’s application. The court held that the beta crystalline form of imatinib mesylate was a known substance within the meaning of Section 3(d), that the claimed improvement in bioavailability did not constitute enhanced therapeutic efficacy as required by the statute, and that Novartis had failed to demonstrate any clinical benefit beyond what was already known from the free base form of the compound.
The Novartis decision established three principles that have governed Indian pharmaceutical patent law since. First, ‘efficacy’ in Section 3(d) means therapeutic efficacy, not pharmacokinetic properties like bioavailability or solubility. Improvements in the latter category do not satisfy the requirement. Second, the burden of demonstrating enhanced efficacy rests squarely on the patent applicant, with no presumption in favor of patentability for new forms of known substances. Third, the section applies retrospectively to all applications in the patent pipeline, including those filed before the 2005 amendment. The case set the standard by which all subsequent pharmaceutical patent applications in India are evaluated.
Mailbox Applications: Pre-2005 Pipeline Patents
The TRIPS agreement required India to create a ‘mailbox’ system for pharmaceutical product patent applications filed between 1995 and 2004, while the country completed its transition to full TRIPS compliance. Approximately 8,900 mailbox applications were on file when the 2005 amendment took effect [4]. Each application was then examined against the new patentability standards, including Section 3(d). The vast majority were rejected, either for failing the Section 3(d) test or for being anticipated by prior art. A small number of applications on genuinely novel compounds approved for marketing after 1995 received product patents.
The mailbox application system is now closed and its pipeline exhausted. But it remains historically significant because it explains why many drugs that received product patents in the United States in the mid-to-late 1990s have no product patents in India. For drugs approved in the U.S. before 1995 and still patented there through patent term extensions and supplementary protection certificates, India has had generic versions available for decades.
The 20-Year Term: What the Clock Actually Measures
Filing Date vs. Priority Date
Under Section 53 of the Patents Act 1970, the term of an Indian patent is 20 years from the date of filing the patent application in India. For applications claiming priority from an earlier foreign application under the Paris Convention or PCT, the 20-year term runs from the Indian filing date, not the priority date. This is an important distinction. A company that files a patent application in the United States in 2010, then files in India in 2011 claiming Paris Convention priority, receives a 20-year term from the 2011 Indian filing date — meaning the patent expires in 2031 regardless of what happens to the U.S. patent.
In practice, most major pharmaceutical companies file PCT (Patent Cooperation Treaty) applications simultaneously with or shortly after their first national filings, then enter the national phase in India within the 30-month window the PCT provides. The Indian filing date under this scenario is typically 30 months after the priority date. For a priority date of January 2010, the Indian filing date might be July 2012, giving a patent term running to July 2032. This is modestly later than the priority country’s expiry date but does not provide any meaningful commercial advantage, since the drug’s approval and marketing timeline in India is independent.
How Regulatory Delay Erodes the Commercial Term
India does not have a patent term extension mechanism equivalent to the U.S. Patent Term Extension or the European Supplementary Protection Certificate. There is no provision in the Patents Act for extending the 20-year term to compensate for time spent awaiting regulatory approval from the Central Drugs Standard Control Organisation (CDSCO). This is not an oversight. The Indian government has consistently declined to introduce PTEs, viewing them as instruments that would primarily benefit multinational pharmaceutical companies at the expense of Indian patients and generic manufacturers.
The practical consequence is significant. A drug whose Indian patent is filed in 2010 and that receives CDSCO approval in 2016 has only 14 years of patent-protected commercial life, not 20. If regulatory approval takes 8 years from filing, the effective commercial exclusivity shrinks to 12 years. In the United States, the same drug might receive a 3-to-5-year PTE to compensate for exactly this delay, extending commercial exclusivity to 17 to 19 years. In India, no such compensation exists. The company absorbs the entire cost of regulatory delay in the form of reduced commercial exclusivity time.
This asymmetry is one of the principal reasons multinational companies argue that the Indian patent system is structurally unfavorable to innovation investment. The TRIPS agreement does not require patent term extensions, so India is under no legal obligation to provide them. But the absence of PTEs, combined with Section 3(d) restrictions on the types of patents that can be obtained, means that the maximum effective commercial patent life for a new chemical entity in India is materially shorter than in every other major pharmaceutical market.
PCT National Phase and the Filing Date Question
When a company files a PCT application and then enters the Indian national phase, it must understand how the Indian Patent Office (IPO) calculates the filing date. The IPO treats the international filing date of the PCT application as the Indian filing date for purposes of the 20-year term calculation under Section 53. This means that a PCT application with an international filing date of March 2008 that enters national phase in India in September 2010 has a 20-year term running from March 2008, expiring in March 2028, not September 2030.
Companies sometimes misunderstand this and assume the national phase entry date starts the clock. The error has commercial consequences because patent monitoring systems that use national phase entry dates rather than international filing dates will overestimate the remaining term. Patent intelligence platforms, including DrugPatentWatch, which covers Indian patent data alongside its global pharmaceutical IP database, use the international filing date as the reference point for Indian PCT-based patents, ensuring that expiration projections are accurate [5].
Patent of Addition: Extending and Restricting
The Patents Act 1970 provides for a ‘patent of addition’ under Section 54, which covers improvements or modifications to an invention already the subject of a pending or granted patent. A patent of addition does not have an independent term. It expires on the same date as the main patent, regardless of when the patent of addition was granted. If the main patent expires, the patent of addition expires with it. If the main patent is surrendered or revoked, the patent of addition may be converted into an independent patent, which then carries its own 20-year term from its own filing date.
From a pharmaceutical perspective, patents of addition can cover incremental formulation improvements, dosage regimen refinements, or new methods of manufacture, provided they represent genuine improvements over the main patent invention. The Section 3(d) restrictions apply equally to patents of addition: a new form of a known substance claimed in a patent of addition must demonstrate enhanced efficacy to qualify. This prevents the use of patents of addition as a backdoor to evergreening after the main patent’s Section 3(d) application fails.
What Can and Cannot Be Patented: India’s Unique Scope Restrictions
Section 3: The Exclusions List
Section 3 of the Patents Act lists what is not an invention for the purposes of Indian patent law. For pharmaceutical companies, four exclusions are commercially significant. Section 3(d), already discussed, excludes new forms of known substances without enhanced efficacy. Section 3(e) excludes ‘a substance obtained by a mere admixture resulting only in the aggregation of the properties of the components thereof,’ which affects combination drug patents unless the combination demonstrates a synergistic effect beyond the sum of its individual components. Section 3(i) excludes ‘any process for the medicinal, surgical, curative, prophylactic, diagnostic, therapeutic or other treatment of human beings,’ which restricts pure method-of-treatment patents. Section 3(p) excludes traditional knowledge, effectively preventing patents on compounds or processes already in the public domain under traditional medicine systems like Ayurveda, Siddha, and Unani.
Together, these four exclusions create a significantly narrower patentable space for pharmaceutical compounds in India than exists in the United States or Europe. A drug company that holds 15 patents on the same compound in the United States — covering the compound, new polymorphs, extended-release formulations, pediatric dosages, new indications, and treatment methods — may hold only two or three valid Indian patents covering the underlying compound and genuinely novel formulations.
Product Patents vs. Process Patents Post-2005
Before 2005, India permitted only process patents on pharmaceutical substances. A process patent gave the patent holder the right to exclude others from using the specific synthesis route described in the patent but not from using other routes to the same API. Indian generic manufacturers became highly skilled at designing around process patents, developing alternative synthesis pathways that were sometimes more efficient than the original patented process.
Post-2005, product patents on pharmaceutical substances are fully available, subject to the Section 3 exclusions. A product patent on a new chemical entity covers the compound regardless of how it is synthesized. Generic manufacturers cannot legally manufacture or market the compound in India during the patent term, regardless of the synthesis route they use. This is the fundamental change the 2005 amendment made. Process patents on pharmaceutical synthesis routes are still available and still filed, but they are no longer the primary mode of pharmaceutical patent protection in India for post-2005 drugs.
Biologics and Large Molecule Patenting
Biological products — including monoclonal antibodies, fusion proteins, therapeutic peptides, and biosimilars — present distinct patentability questions in India. The Patents Act does not explicitly exclude biologics from patentability, and the IPO grants product patents on novel biologic molecules. However, Section 3(j) excludes ‘plants and animals in whole or any part thereof other than microorganisms,’ and Section 3(c) excludes ‘the mere discovery of a scientific principle or the formulation of an abstract theory.’ The interaction of these exclusions with biologic drug patents, particularly claims covering cell lines, biological production processes, and genetic sequences, has generated significant uncertainty.
For biosimilar manufacturers, the absence of data exclusivity in India is at least as important as the biologic patent landscape. In the United States, a biologic reference product receives 12 years of data exclusivity under the BPCIA, preventing biosimilar approval regardless of patent status. India has no equivalent data exclusivity framework. A biosimilar manufacturer in India can apply to the CDSCO for approval of a biosimilar product immediately upon demonstration of similarity, without waiting for any data exclusivity period to expire. The CDSCO’s 2016 guidelines on similar biologics set out the regulatory pathway. The patent position of the reference product determines whether the biosimilar can be marketed, but the regulatory approval pathway itself faces no data exclusivity barrier.
Traditional Knowledge and the TKDL
India maintains the Traditional Knowledge Digital Library (TKDL), a database of approximately 900 traditional formulations and Ayurvedic, Unani, and Siddha medicinal practices documented in five languages. The TKDL was created specifically as a prior art resource to defeat pharmaceutical patent applications on traditional remedies that had entered the international patent system without acknowledgment of their traditional origins.
The TKDL has been shared with patent offices in the United States, the European Patent Office, the United Kingdom, Canada, Australia, and Germany under access agreements. Patent examiners in these offices use it as a search resource for prior art in pharmaceutical applications. The Indian Patent Office uses it extensively. It has contributed to the rejection of dozens of patent applications internationally, including applications by major pharmaceutical companies on compounds or preparations with documented traditional medicine histories.
For drug patent duration in India, the TKDL matters because it creates a category of compounds that are permanently non-patentable in India regardless of the 2005 amendment. Any pharmaceutical substance that can be traced to traditional Indian medicinal knowledge is subject to prior art challenge based on TKDL documentation. Companies that discovered pharmaceutical activity in compounds with traditional medicine backgrounds — a significant category in natural product drug discovery — face a higher bar for patentability in India than they do in markets without the TKDL resource.
Data Exclusivity: The Gap That Matters Most
Why India Has No Data Exclusivity
Data exclusivity is the protection given to the clinical trial data submitted to a regulatory authority to support a new drug approval. In the United States, a new chemical entity receives five years of data exclusivity under the Hatch-Waxman Act. In the European Union, reference products receive eight years of data exclusivity plus two years of market protection plus one additional year for new indications, commonly called the ‘8+2+1’ framework. During these exclusivity periods, generic applicants cannot rely on the originator’s data to support their own applications, regardless of the patent position.
India has no data exclusivity framework. The Drugs and Cosmetics Act 1940, which governs pharmaceutical regulation in India, and the rules made under it, including the New Drugs and Clinical Trials Rules 2019, do not provide for data exclusivity protection. A generic manufacturer in India can submit an abbreviated dossier to the CDSCO citing the reference originator’s data immediately upon the originator’s approval, subject only to demonstrating bioequivalence. The CDSCO does not require the generic applicant to generate its own clinical data, and it does not delay generic approvals out of deference to any exclusivity period.
This means that in India, the only barrier to generic entry from day one of a new drug’s approval is patent protection. If the drug’s compound patent is valid and enforceable in India, generics must wait for it to expire or successfully challenge it. If the compound patent was rejected under Section 3(d), or if no Indian product patent was ever filed, there is no regulatory barrier to immediate generic entry. There is no data exclusivity backstop.
TRIPS Article 39.3 and the Indian Position
TRIPS Article 39.3 requires member states to protect undisclosed test data submitted to government authorities for new pharmaceutical or agrochemical products against ‘unfair commercial use.’ India’s position has been that this obligation can be satisfied through existing trade secret and unfair competition laws, without creating a specific data exclusivity framework. The government has argued that Article 39.3 does not require a time-limited exclusivity period of the type found in the United States or Europe, but only prevents direct copying of confidential data submitted to regulators.
This interpretation has been consistently contested by the United States and European Union in trade negotiations and in the TRIPS Council. The USTR’s annual ‘Special 301’ report on intellectual property protection has placed India on its ‘Priority Watch List’ repeatedly, citing the absence of data exclusivity as a market access barrier for U.S. pharmaceutical companies [6]. India has consistently declined to change its position. No WTO dispute settlement panel has formally adjudicated Article 39.3’s requirements in a way that would require India to introduce data exclusivity, and the political cost of doing so domestically — given the public health implications — has prevented successive Indian governments from acting.
The Commercial Impact of No Data Exclusivity
For a pharmaceutical company launching a new drug in India, the absence of data exclusivity means that generic competition can begin the moment the original product patent expires, or immediately if no valid product patent exists. There is no two-year, five-year, or eight-year safety net. A company that spends $1 billion developing a drug, receives regulatory approval in India in 2024, and holds a product patent expiring in 2030 has exactly six years of patent-protected revenue in India, after which generic manufacturers can freely enter. A company in the same situation in Europe has eight years of data exclusivity independent of any patent, meaning that even if the patent were successfully invalidated, generic approval would be delayed by the data exclusivity period.
The practical effect is to make patent protection in India more commercially critical than it is in markets with data exclusivity backstops. If a company’s Indian patent is challenged and successfully invalidated, there is no regulatory safety net of any kind. The market opens completely. This makes the quality of Indian patent prosecution — the rigor of the application, the breadth of the claims, the choice of patents to protect — more commercially significant in India than the same decisions are in the United States or Europe, where data exclusivity provides a floor of protection even in a worst-case patent scenario.
Compulsory Licensing: The Override Mechanism
Section 84 and the Three-Year Rule
Section 84 of the Patents Act permits any person to apply to the Controller of Patents for a compulsory licence on any patent after three years from the date of grant, if the applicant can satisfy one or more of three conditions. First, the reasonable requirements of the public with respect to the patented invention have not been satisfied. Second, the patented invention is not available to the public at a reasonably affordable price. Third, the patented invention is not worked in the territory of India.
The three conditions are each independently sufficient to trigger the grant of a compulsory licence. Condition two, unreasonable pricing, has been the basis for the most commercially significant compulsory licence in India’s post-2005 history. Condition three, lack of working in India, requires domestic manufacture rather than importation. This provision reflects a policy preference for local pharmaceutical manufacturing and has been used to pressure foreign patent holders to either manufacture in India, license Indian companies, or face compulsory licence applications.
The Natco v. Bayer Decision: The First Post-2005 Compulsory Licence
In March 2012, the Controller of Patents granted India’s first post-2005 compulsory licence to Natco Pharma Limited for the manufacture and sale of sorafenib tosylate, the active ingredient in Bayer’s cancer drug Nexavar, used to treat kidney and liver cancer [7]. Bayer held a product patent on sorafenib in India granted under the post-2005 regime. Natco applied for a compulsory licence under Section 84, arguing that Nexavar was priced at approximately 280,000 Indian rupees per month (roughly $5,600 at the time), placing it beyond the reach of the vast majority of Indian patients with renal and hepatocellular carcinoma. Natco proposed to manufacture and sell a generic version at approximately 8,800 rupees per month.
The Controller granted the licence, finding that all three conditions of Section 84 were satisfied. Bayer appealed to the Intellectual Property Appellate Board and then to the Bombay High Court, both of which upheld the Controller’s decision. The compulsory licence required Natco to pay Bayer a royalty of 6 percent of net sales, a figure well below the TRIPS guideline range for compulsory licences in situations of non-commercial public interest, but applied in a commercial context. Bayer’s sorafenib patent in India was not revoked. It remained in force and continued to be enforceable against any other generic manufacturer that did not hold a licence. The compulsory licence was specific to Natco.
The Natco v. Bayer decision sent a clear message to multinational pharmaceutical companies about the price levels at which Section 84 compulsory licence applications become viable. It established that a patented drug priced at roughly 30 times the generic price, treating a life-threatening illness, with low penetration among patients who could benefit, will face compulsory licence risk in India regardless of the patent’s legal validity. Pricing strategy in India must account for this floor.
Section 92: Government Use Without Compulsory Licence Application
Section 92 of the Patents Act provides an expedited pathway for compulsory licensing in circumstances of national emergency, extreme urgency, or for non-commercial public use. Unlike Section 84, Section 92 allows the Central Government to authorize a government undertaking or third party to use a patented invention by notification in the Official Gazette, without requiring the three-year waiting period or the individual application process. The royalty payable is determined by the High Court in the event of dispute.
Section 92 has been invoked rarely but is theoretically available for any public health emergency. During the COVID-19 pandemic, there were significant calls for the Indian government to use Section 92 to authorize generic production of COVID-19 treatments and vaccines. The government ultimately did not invoke Section 92 explicitly, but it used voluntary licensing negotiations as leverage to obtain favourable terms from vaccine manufacturers. The existence of Section 92 as a credible threat was part of that leverage.
The Doha Declaration Context
India’s compulsory licensing provisions are consistent with the Doha Declaration on TRIPS and Public Health, adopted by WTO member states in November 2001. The Doha Declaration affirmed that each WTO member has the right to grant compulsory licences and the freedom to determine the grounds on which such licences are granted. It confirmed that member states with insufficient domestic manufacturing capacity in the pharmaceutical sector can issue compulsory licences for importation. India, with substantial domestic pharmaceutical manufacturing capacity, does not need to rely on this importation provision, but it shaped the international consensus that India’s Section 84 mechanism is legally permissible under WTO rules.
The Doha Declaration also affirmed that public health concerns can override intellectual property interests when the two come into conflict. This principle is embedded in India’s compulsory licensing jurisprudence, and any analysis of how long a drug patent effectively lasts in India must account for the possibility that Section 84 or Section 92 reduces the commercial value of the patent term even when the patent itself remains legally valid.
Voluntary Licensing as a Compulsory Licence Substitute
Several multinational pharmaceutical companies have preemptively negotiated voluntary licences with Indian generic manufacturers on patented drugs, partly to forestall compulsory licence applications. Gilead Sciences has entered into voluntary licence agreements with multiple Indian generic manufacturers for its HIV, hepatitis C, and COVID-19 treatments. AstraZeneca negotiated voluntary licences for its COVID-19 vaccine, Vaxzevria. Bristol Myers Squibb has voluntary licence arrangements for HIV drugs including atazanavir and efavirenz.
Voluntary licences typically include royalty payments, quality requirements, and geographic restrictions. They allow branded companies to maintain some revenue stream from India while permitting affordable generic versions. From a patent duration perspective, voluntary licences do not affect the patent term itself, but they change the commercial exclusivity that the patent provides. A drug with a valid 2030 expiry patent generating revenue through a voluntary licence at 5 percent royalty on generic sales has substantially less commercial exclusivity than the same patent without any voluntary licence would theoretically provide.
The Evergreening Battle: How Companies Try and How India Stops Them
What Evergreening Means in the Indian Context
Evergreening refers to the practice of extending effective pharmaceutical exclusivity beyond the original patent term by filing and obtaining patents on minor modifications to a known drug: new salt forms, new polymorphs, new dosage strengths, extended-release formulations, or new combinations with other known compounds. In markets without Section 3(d) equivalents, this practice extends effective exclusivity by several years per iteration, allowing companies to collect branded revenues well past the original compound patent’s expiry.
In India, Section 3(d) specifically targets evergreening by requiring that any new form of a known substance demonstrate enhanced therapeutic efficacy to qualify for a patent. ‘Enhanced efficacy’ has been interpreted strictly by Indian courts to mean clinical or therapeutic improvement in the treatment of disease, not pharmacokinetic improvements like better absorption or longer half-life. A new salt form that has better bioavailability but produces the same clinical outcomes as the original compound fails Section 3(d). A new polymorph that is more stable in tropical climates but no more effective therapeutically also fails. Only genuine therapeutic improvements qualify.
This standard eliminates most of the commonly used evergreening strategies at the first examination stage. Indian patent examiners are trained to apply Section 3(d) analysis to pharmaceutical applications, and the rate of rejection for pharmaceutical patent applications in India is substantially higher than in the United States or Europe for exactly this reason. For a multinational company accustomed to building a layered patent portfolio of 20 to 50 patents on a single drug, the Indian system may yield two to five valid patents, covering the genuinely novel compound and perhaps one or two truly innovative formulations.
Pre-Grant Opposition: Any Person Can Object
Section 25(1) of the Patents Act 1970 permits any person to file a pre-grant opposition to a pending patent application. The opposition can be filed at any time after the application is published but before the patent is granted. Importantly, there is no standing requirement: any person, anywhere in the world, can file a pre-grant opposition in India, not just competitors or parties with commercial interests. This has enabled civil society organizations, patient advocacy groups, health NGOs, and generic manufacturers to challenge pharmaceutical patent applications at the examination stage.
The pre-grant opposition system has been actively used against pharmaceutical patent applications in India. The Lawyers Collective, MSF (Medecins Sans Frontieres), and various Indian patient groups have filed pre-grant oppositions against applications by Novartis, Roche, Bristol Myers Squibb, Gilead Sciences, and others. The grounds for opposition under Section 25(1) include anticipation by prior publication, obviousness, non-patentability under Section 3, and lack of novelty.
Pre-grant oppositions can delay patent grant by months or years while the IPO processes the opposition and responds to written arguments from both the applicant and the opponent. For a company counting on its patent to provide exclusivity protection from the date of drug approval, a pre-grant opposition that delays grant until well after regulatory approval directly reduces the effective commercial patent term. It does not extend the 20-year term from the filing date; the patent, if ultimately granted, expires at the same time it would have without the opposition. But the period during which the patent is not yet granted, and therefore not yet enforceable against specific generic products, represents commercial exclusivity lost.
Post-Grant Opposition: Five Years to Challenge
Section 25(2) of the Patents Act permits any interested person to file a post-grant opposition within one year of the patent grant. Unlike the pre-grant opposition, the post-grant opposition requires the opponent to be an ‘interested person,’ which includes generic manufacturers with commercial interests in the subject matter. The grounds for post-grant opposition are broader than pre-grant grounds, including insufficiency of description, failure to disclose best mode, and obtaining by fraud.
Post-grant oppositions are heard by an Opposition Board constituted by the IPO, which provides recommendations to the Controller of Patents. The Controller’s decision can then be appealed to the High Court. The process can take three to five years from filing, during which the challenged patent remains in force unless a court grants an interim injunction suspending its enforcement. Generic manufacturers who anticipate filing post-grant oppositions typically seek to coordinate the timing so that the opposition proceedings conclude before they plan to launch their generic product.
Revocation Petitions: The High Court Route
Separately from the opposition system, any person may seek revocation of a granted patent directly before the relevant High Court under Section 64 of the Patents Act, or before the IPO under Section 63. The High Court route is commonly used by generic manufacturers as a defensive measure when a brand company has initiated infringement proceedings: the generic files a revocation petition as a counterclaim, forcing the brand company to defend the patent’s validity while simultaneously pursuing the infringement case.
The revocation proceedings and the opposition proceedings can run simultaneously, creating a complex multi-forum litigation environment that significantly increases the cost and uncertainty for both sides. Brand companies defending their Indian patents against coordinated opposition, revocation, and infringement counterclaims in multiple High Courts simultaneously face litigation costs that, while modest by U.S. standards, represent meaningful strategic resources in a market where branded revenues may be substantially lower than in the United States or Europe.
India in Practice: How Major Drug Patents Have Played Out
Imatinib (Gleevec/Glivec): The Case That Defined the System
Novartis’s imatinib mesylate, marketed globally as Gleevec or Glivec, is the most extensively litigated pharmaceutical patent in Indian legal history. Novartis filed a mailbox application in 1998 for the beta crystalline form of imatinib mesylate and filed separately for the free base form. The free base form was covered by a process patent granted in India before the 2005 amendments. Indian generic manufacturers, including Cipla, Natco, and Ranbaxy, were producing and selling generic imatinib from the mid-2000s based on the process patent limitations in pre-2005 law and the absence of a product patent on the compound.
When Novartis’s mailbox application for the crystalline form was examined under post-2005 standards, the IPO rejected it under Section 3(d). Novartis pursued appeals through the IPAB and the Supreme Court, which issued its final rejection in April 2013. The decision confirmed that Novartis could not obtain a product patent on the imatinib crystalline form in India. Generic manufacturers continued to produce imatinib freely. Patients in India could access generic imatinib at approximately one percent of the price charged in the United States.
The broader significance for patent duration is direct: the 20-year term of a product patent is irrelevant if the patent is not granted. For imatinib in India, the effective patent term on the compound was zero, not 20 years. The lesson for pharmaceutical companies is that the nominal term and the effective term are fundamentally different questions, and Section 3(d) analysis must precede any calculation of expected Indian exclusivity.
Sofosbuvir (Sovaldi): The Hepatitis C Access Battle
Gilead Sciences’ sofosbuvir, the nucleotide analog that transformed treatment of Hepatitis C, received approval in India in 2015. Gilead had filed a patent application on sofosbuvir in India. Multiple pre-grant oppositions were filed, including by Medecins Sans Frontieres (MSF) and the Initiative for Medicines, Access, and Knowledge (I-MAK). The IPO rejected Gilead’s patent application on the compound in January 2015 [8]. Gilead appealed. Separately, the IPAB revoked a related patent on sofosbuvir’s phosphoramidate prodrug form.
In parallel, Gilead negotiated voluntary licences with seven Indian generic manufacturers, anticipating that it would not secure comprehensive patent protection in India. The voluntary licences permitted Indian generics to manufacture and sell sofosbuvir-based treatments in India and to export to certain lower-income countries. The generic versions launched in India at approximately $900 for a 12-week treatment course, compared to $84,000 for the same course in the United States.
The sofosbuvir story illustrates a specific dynamic in Indian pharmaceutical patent duration: a company that loses its primary patent application can still extract value through voluntary licensing, converting what would have been a total exclusivity loss into a revenue-sharing arrangement. But the commercial exclusivity the company originally expected — 20 years of sole right to sell the drug at branded prices — was never realized in India.
Bedaquiline (Sirturo): Tuberculosis and the 2023 Revocation
Bedaquiline, developed by Janssen (Johnson & Johnson) and approved in the United States in 2012 for drug-resistant tuberculosis, received Indian regulatory approval in 2019. The drug was the first new TB treatment in 40 years with a genuinely novel mechanism of action. Janssen held an Indian product patent on bedaquiline. In July 2023, the IPO granted post-grant oppositions filed by MSF, the TB Alliance, and others, revoking the bedaquiline patent in India [9].
The revocation was based primarily on findings of lack of inventive step and anticipation by prior art published before the Indian patent’s priority date. The IPO determined that the compound’s activity against TB bacteria had been sufficiently disclosed in earlier scientific literature to deprive the Janssen application of novelty and inventive step. Janssen appealed to the Delhi High Court, where the case remained pending as of 2024.
The bedaquiline revocation, if upheld on appeal, means that a drug approved as recently as 2019 in India has already lost its patent protection, giving it an effective exclusivity term of approximately four years in the Indian market before competition from generic manufacturers. At the bedaquiline case proceedings, generic manufacturers were preparing to launch generic versions as soon as the revocation was confirmed. For a drug treating a disease with enormous prevalence in India — the country carries approximately 27 percent of the global TB burden — the patent’s validity was always contested from a public health perspective.
Lenalidomide: Evergreening Attempts in Oncology
Bristol Myers Squibb’s lenalidomide, marketed as Revlimid for multiple myeloma, illustrates the evergreening restriction in practice. BMS and its predecessor Celgene filed multiple patent applications on lenalidomide in India, covering the compound, polymorphs, and specific formulations. Pre-grant oppositions were filed by multiple generic manufacturers, and the IPO significantly narrowed the granted claims. The primary compound patent on lenalidomide itself was ultimately granted but with narrowed claims that gave generic manufacturers more room to design around.
Natco Pharma, which had experience navigating Indian pharmaceutical patent law from the Nexavar compulsory licence, filed a pre-grant opposition on lenalidomide and introduced a generic version in India that it began exporting to certain markets. BMS initiated litigation in multiple jurisdictions. In India, the litigation confirmed that the Section 3(d) restrictions effectively limited BMS’s patent portfolio on lenalidomide to a narrower set of claims than it had hoped to maintain.
Key Indian Patent Decisions (2012-2024)
| Drug | Company | Legal Basis | Outcome | Year |
|---|---|---|---|---|
| Imatinib (Gleevec) | Novartis | Sec. 3(d) rejection | Patent denied | 2013 |
| Sofosbuvir | Gilead | Pre-grant opposition | Patent rejected | 2015 |
| Sorafenib (Nexavar) | Bayer | Sec. 84 CL petition | CL granted to Natco | 2012 |
| Bedaquiline | J&J (Janssen) | Post-grant opposition | Patent revoked | 2023 |
| Dasatinib (Sprycel) | BMS | Sec. 3(d) challenge | Patent refused | 2015 |
| Lenalidomide (Revlimid) | Celgene/BMS | Pre-grant opposition | Narrowed claims | 2018 |
| Baricitinib (Olumiant) | Eli Lilly | Post-grant opposition | Patent upheld | 2022 |
Sources: Indian Patent Office records, IPO Official Gazette, reported High Court and Supreme Court decisions, DrugPatentWatch [5].
Effective Exclusivity: What the Numbers Actually Show
The Range of Outcomes
A systematic analysis of drug patent outcomes in India since 2005 shows that the effective commercial exclusivity period varies enormously depending on the type of compound, the strength of the patent application, the speed of regulatory approval, and whether opposition proceedings intervene. The following scenarios represent the range of outcomes a pharmaceutical company can expect for a new drug launched in India post-2005.
| Scenario | Filing Year | Approval Year | Patent Expires | Effective Term |
|---|---|---|---|---|
| Standard NCE, fast approval | 2005 | 2010 | 2025 | 15 yrs total / 15 yrs commercial |
| NCE with PCT delay, slow approval | 2004 | 2012 | 2024 | 20 yrs total / 12 yrs commercial |
| Sec. 3(d) rejected, process patent only | 2005 | 2010 | 2025 (process) | Generic API legal from day 1 |
| Compulsory licence granted | 2005 | 2010 | 2025 | Generic available mid-term |
| Pre-grant opposition delays grant | 2005 | 2012 | 2025 | Effective term reduced to 13 yrs |
Analysis based on IPO data, regulatory approval timelines from CDSCO records, and patent term calculations under Section 53 of the Patents Act. Sources: IPO, CDSCO, DrugPatentWatch [5].
The scenario with the most favorable outcome for an innovator company — a genuinely novel compound that passes Section 3(d) review, receives an Indian product patent, obtains CDSCO approval quickly, and faces no successful opposition — may deliver 12 to 15 years of effective commercial exclusivity. This is substantially shorter than the 17 to 19 years that might be available in the United States for the same drug after a patent term extension, but it is not trivial. For a drug in a therapeutic category where Indian generic manufacturers are not yet strong competitors, 12 years of branded sales at significant price premium may still generate substantial returns.
Comparing India to Major Pharmaceutical Markets
| Feature | India | USA | EU | China |
|---|---|---|---|---|
| Statutory patent term | 20 years | 20 years | 20 years | 20 years |
| Patent term extension (PTE/SPC) | None | Up to 5 yrs | Up to 5 yrs SPC | 5 yrs (drugs) |
| Data exclusivity | None | 5 yrs NCE | 8+2+1 yrs | 6 yrs |
| Evergreening restriction (Sec. 3(d)) | Yes (strict) | No | No | Partial |
| Pre-grant opposition | Yes | No | No | No |
| Compulsory licensing (CL) | Yes (active) | Rare | Rare | Yes (active) |
| Product patents on APIs (post-2005) | Yes | Yes | Yes | Yes |
Sources: 35 U.S.C. Section 156 (U.S. PTE); EU SPC Regulation (EC) No. 469/2009; China Patent Law Amendment 2020; India Patents Act 1970 as amended 2005. DrugPatentWatch covers patent expiry data across all these jurisdictions [5].
“India accounts for approximately 20% of global generic medicine exports by value and over 60% of global vaccine supply, making its patent regime one of the most consequential in global health policy.”
— India Brand Equity Foundation (IBEF), Pharmaceuticals Sector Report 2024 [2]
The Generic Manufacturing Ecosystem: India as the World’s Pharmacy
Why Indian Generics Are a Global Force
India’s generic pharmaceutical industry is not an accident of patent policy. It is the product of 50 years of deliberate industrial policy, engineering talent, process chemistry expertise, and regulatory navigation capability. Companies like Sun Pharmaceutical Industries (the world’s fifth-largest specialty generic pharmaceutical company by revenue), Dr. Reddy’s Laboratories, Cipla, Aurobindo Pharma, Lupin, and Zydus Lifesciences collectively supply more than 150 countries with generic medicines across essentially every therapeutic category.
The industry produces approximately 60,000 approved generic formulations, runs more than 500 FDA-approved manufacturing facilities (more than any other country outside the United States), and supplies 40 percent of generic medicines used in the United States by volume [10]. The FDA regularly inspects Indian manufacturing sites, and the industry has faced scrutiny for quality compliance issues at specific facilities. But the scale, sophistication, and cost competitiveness of Indian generics production is structurally irreplaceable in the global pharmaceutical supply chain.
API Patents vs. Formulation Patents: Two Different Clocks
In India, as in most patent systems, pharmaceutical companies file patents at multiple levels of the product: on the active pharmaceutical ingredient (API) itself, on specific formulations (tablet, capsule, injectable), on manufacturing processes for the API, on the finished dosage form manufacturing process, and on specific delivery systems or devices. Each of these patent types has a separate 20-year term from its own filing date.
For generic manufacturers, the practical question is which patents stand between them and legal market entry. If the API patent expires in 2028 but a formulation patent expires in 2032, the generic cannot legally market a product that falls within the formulation patent’s claims even after the API patent expires. Designing a generic formulation that avoids the formulation patent, while bioequivalent to the reference product, requires significant formulation chemistry expertise. This is a field in which major Indian generics have invested heavily, specifically because it enables earlier entry into post-API-patent markets.
PatentWatch data aggregated by platforms including DrugPatentWatch shows that Indian pharmaceutical patent portfolios are typically shallower than U.S. or European portfolios on the same drug, reflecting Section 3(d) rejections, successful pre-grant and post-grant oppositions, and narrowed claims. The average number of valid Indian patents per branded drug is substantially lower than the average in the United States, which directly affects the strategic importance of each remaining Indian patent [5].
The Hatch-Waxman Equivalent in India: No Formal Equivalent
The United States has an explicit statutory framework under Hatch-Waxman for managing the generic drug approval process, patent certifications, and the resolution of patent disputes before generic launch. India has no equivalent framework. The CDSCO approves generic drugs through a simplified application process that does not require formal patent certifications of the type required under U.S. law. Indian generic manufacturers do not certify in their regulatory applications that they believe the reference product’s patents are invalid or will not be infringed by their product.
The absence of a Hatch-Waxman equivalent means that patent disputes between brand and generic companies in India are resolved entirely through civil litigation in the High Courts, not through a formal pre-market patent dispute resolution process integrated into the regulatory framework. A brand company that discovers a generic manufacturer is selling a product it believes infringes its Indian patent must seek an injunction in the relevant High Court. The generic manufacturer can counterclaim with a revocation petition. The litigation can take years. During that period, depending on the court’s decision on interim injunctions, the generic may or may not be on the market.
Interim Injunctions and the Balance of Convenience Test
Indian courts apply a three-part test for interim injunctions in patent infringement cases: the plaintiff must show a prima facie case of infringement, demonstrate that the balance of convenience favors granting the injunction, and show that irreparable harm would result from refusal. In pharmaceutical patent cases, the balance of convenience analysis frequently weighs the potential harm to the patent holder against the public interest in access to affordable medicines.
Indian High Courts, particularly the Delhi High Court which handles most pharmaceutical patent litigation, have been relatively reluctant to grant interim injunctions that would remove an already-launched generic product from the market. The courts are aware that restoring a product to the market after an injunction is lifted is commercially complicated, and that patients who have started treatment on a generic product may be disrupted by sudden unavailability. This judicial posture reduces the practical enforcement value of Indian pharmaceutical patents compared to their theoretical legal value.
TRIPS, Free Trade Agreements, and the Pressure to Change
India’s TRIPS Compliance: Genuine but Minimal
India’s patent system is formally TRIPS-compliant. The WTO’s TRIPS Council has considered India’s implementation multiple times, and no formal dispute settlement case has resulted in a ruling requiring India to change its Section 3(d) provision, its absence of data exclusivity, or its compulsory licensing framework. India’s legal position on each of these points has been carefully constructed to sit within the flexibilities that TRIPS expressly provides to developing country members.
The critical TRIPS provisions relevant to Indian patent law are Articles 27 (patentable subject matter), 28 (rights conferred), 30 (exceptions to rights conferred), 31 (other use without authorization, i.e., compulsory licensing), and 39 (protection of undisclosed information). India has argued successfully that each of its distinctive provisions falls within the explicit or implicit flexibilities in these articles. The Novartis decision at the WTO level was essentially a non-event because no formal dispute was ever brought.
U.S. and EU Trade Pressure: Special 301 and FTA Negotiations
The absence of formal WTO dispute settlement does not mean India has been free from trade pressure. The USTR’s Office of the United States Trade Representative places India on its Special 301 Priority Watch List annually, alongside countries like China and Russia, citing inadequate intellectual property protection including the absence of data exclusivity, the compulsory licensing framework, and what the USTR describes as the unpredictable patent grant environment created by Section 3(d) [6].
The European Union has been engaged in bilateral free trade agreement (FTA) negotiations with India intermittently since 2007. Earlier rounds of negotiations stalled partly over IP provisions. The EU sought TRIPS-plus commitments on data exclusivity and patent linkage that India refused to provide. Negotiations resumed in 2021 and remain ongoing. The pharmaceutical IP chapter of any India-EU FTA is expected to be among the most contested provisions. The EU has sought the same data exclusivity protections it has secured in FTAs with other countries. India’s negotiating position has been that its domestic patent law reflects a legitimate balancing of public health and innovation incentives that it will not alter for trade purposes.
Patent Linkage: The Regulatory-Patent Connection India Rejects
Patent linkage refers to the practice, standard in the United States under Hatch-Waxman, of formally connecting the drug regulatory approval process to the patent status of the reference product. Under patent linkage, a regulatory authority will not approve a generic product if a valid patent covering the reference product remains in force, unless the generic has a valid legal basis to launch (such as a successful patent challenge).
India explicitly rejects patent linkage. The CDSCO approves generic drugs on the basis of pharmaceutical quality, safety, and bioequivalence data alone, without reference to patent status. An April 2009 circular from the Department of Pharmaceuticals directed regulatory authorities not to reject generic approvals on patent grounds. The practical effect is that a generic manufacturer can receive CDSCO approval for a product that infringes a valid Indian patent. It cannot legally sell that product without the patent holder’s permission or a court order, but regulatory approval and patent clearance are entirely separate processes.
The rejection of patent linkage is consistent with India’s broader approach to pharmaceutical IP: the public health system and the intellectual property system are treated as parallel but independent frameworks. The consequences of infringement are legal and commercial, not regulatory. This approach maximizes the speed and ease of generic regulatory approval, which serves the public interest in access to affordable medicines, while leaving intellectual property disputes to the courts.
The India-EU FTA and the Data Exclusivity Stalemate
The current India-EU FTA negotiations are the most commercially significant ongoing trade discussion affecting Indian pharmaceutical patent law. EU pharmaceutical companies, through the European Federation of Pharmaceutical Industries and Associations (EFPIA), have lobbied aggressively for data exclusivity, patent linkage, and stronger enforcement commitments as part of the FTA. Indian generic manufacturers, through the Indian Pharmaceutical Alliance and the Pharmaceuticals Export Promotion Council of India (Pharmexcil), have lobbied equally aggressively against all three provisions.
The political economy of this dispute is asymmetric in India’s favor. The Indian government controls both the FTA negotiation and the domestic pharmaceutical policy framework. The generic industry is a major employer, a significant export earner ($27.7 billion in pharmaceutical exports in FY2023-24), and a politically popular sector given its association with affordable medicines and global vaccine access [11]. Any Indian government that agreed to data exclusivity provisions in an FTA would face immediate domestic political opposition from patient groups, public health NGOs, and the generic industry simultaneously.
Patent Intelligence in the Indian Market: What You Need to Track
The Data Landscape for Indian Pharmaceutical Patents
Tracking Indian pharmaceutical patent status requires navigating multiple data sources. The Indian Patent Office publishes patent grants, oppositions, and revocations in an official journal published weekly. The Controller General of Patents, Designs and Trade Marks maintains the Indian Patent Advanced Search System (InPASS), a public database that allows searches by patent number, applicant name, inventor name, and keyword. The CDSCO publishes drug approvals in the Central Licensing Authority’s drug approvals database. High Court judgments are available through the e-Courts system and legal databases like Manupatra and SCC Online.
The challenge is that none of these systems are integrated. A pharmaceutical company or investor trying to understand the complete patent and exclusivity position of a specific drug in India must check InPASS for patent grants and oppositions, the IPO journal for recent changes, the CDSCO database for regulatory approval dates (which determine the effective commercial term), the relevant High Court databases for ongoing litigation, and the IPO’s records for any compulsory licence applications or grants.
DrugPatentWatch integrates Indian patent data alongside its global pharmaceutical patent database, providing a consolidated view of Indian drug patent status, opposition proceedings, and expiration dates alongside U.S. PTE data, European SPC information, and global litigation histories [5]. For pharmaceutical companies and investors who need to understand competitive exclusivity globally, including in India, consolidated intelligence of this type is more efficient than navigating each national database separately. The Indian market’s increasing commercial significance has driven demand for precisely this kind of integrated coverage.
Monitoring Pre-Grant and Post-Grant Opposition Activity
Pre-grant and post-grant oppositions in India can significantly affect the commercial value of a pharmaceutical patent portfolio. A patent application that is granted without opposition has higher certainty of validity than one that has survived an opposition, which in turn has higher certainty than one that has not yet been tested. Conversely, an application with multiple pending pre-grant oppositions from well-resourced opponents faces genuine risk of rejection or substantial claim narrowing.
For generic manufacturers, monitoring pre-grant opposition activity on competitor patents in their therapeutic areas is basic competitive intelligence. If a generic manufacturer sees that a pre-grant opposition has been filed against a patent that it would otherwise have to wait for, it knows that the market entry timeline is uncertain. If the opposition succeeds, entry may be possible immediately upon drug approval. If the opposition fails, the patent term runs its full course.
For brand manufacturers, monitoring opposition filings against their own pending applications allows them to prepare substantive responses. The quality of the response to a pre-grant opposition, including the presentation of comparative efficacy data to satisfy Section 3(d), can determine whether the patent is granted with full claims, granted with narrowed claims, or rejected entirely. These outcomes have direct commercial consequences measured in years of exclusivity.
The Role of Parallel Import Rights
India’s patent law includes provisions on exhaustion of rights that are relevant to the question of how long a patent’s commercial effect lasts. Section 107A of the Patents Act permits parallel importation of patented pharmaceuticals from any country where the drug was legally marketed with the patent holder’s authorization. This is international exhaustion, meaning that once the patent holder sells a product anywhere in the world, it cannot use Indian patent rights to prevent the reimportation of that product into India.
In pharmaceutical terms, this means that if a brand company sells a patented drug in a lower-priced market — say, South Africa or Vietnam — and that product finds its way to India through parallel trade, the Indian patent cannot be used to stop its sale. Parallel imports are uncommon in practice because the logistics and quality verification challenges are significant, but the legal framework creates a theoretical ceiling on the price premium that Indian patent protection can support. If branded prices in India rise significantly above international reference prices, parallel import pressure increases.
Investment and Commercial Implications: Pricing Your Indian Position
How Multinational Companies Value Indian Patent Protection
Indian revenues for major multinational pharmaceutical companies typically represent a small fraction of global revenues. For a blockbuster drug generating $10 billion globally, Indian revenues may be $50 million to $200 million — between 0.5 and 2 percent of global sales. At those revenue levels, the commercial case for investing heavily in Indian patent prosecution, opposition defense, and enforcement litigation may appear marginal.
This calculation changes when you account for the precedential and access effects of Indian patent decisions. A compulsory licence granted in India creates a template that other countries in the global south may follow. A successful pre-grant opposition in India may provide factual record that opponents in other jurisdictions can use. A Supreme Court decision on Section 3(d) receives global attention and shapes negotiations in multiple FTA contexts simultaneously. Indian pharmaceutical IP decisions have effects that are disproportionate to India’s direct revenue contribution, which is why multinational companies consistently fight Indian patent cases all the way to the Supreme Court even when the Indian revenue at stake is modest.
Generic Companies: The Timeline That Matters
For Indian generic manufacturers, the question of how long a drug patent lasts in India is a direct input to their launch planning models. A patent with a confirmed expiry of 2028 tells a generic company that if it plans to launch a generic version in India in 2028, it needs to have its CDSCO abbreviated dossier ready, its manufacturing capacity validated, and its API supply chain secured roughly two to three years in advance. If it plans to challenge the patent through a pre-grant or post-grant opposition, it needs to assess the strength of the opposition grounds and the timeline of proceedings.
The Indian generic industry has institutionalized patent monitoring as a core business function. Companies like Sun Pharmaceutical, Dr. Reddy’s, and Cipla have dedicated IP teams that track patent expirations, file oppositions on strategically important applications, manage revocation petitions, and time their regulatory submissions to align with anticipated patent expiry. For complex patent situations involving multiple patents on the same drug, these teams develop a product-specific patent cliff analysis that looks similar in structure to the analysis that drives M&A valuations in the Western pharmaceutical industry, but operates on Indian legal terrain with Indian rules.
The Export Dimension: Voluntary Licences and Access Programs
Indian generic manufacturers do not produce only for the domestic Indian market. They are major exporters to low-income countries in Africa, Asia, and Latin America, often under voluntary licence or compulsory licence frameworks that permit them to export to these markets. The Medicines Patent Pool (MPP), established by UNITAID and endorsed by the WHO, negotiates voluntary licences with originator companies on critical medicines — HIV/AIDS, hepatitis C, tuberculosis, COVID-19 — and sub-licenses them to Indian generic manufacturers for production and export.
For Indian generic companies, MPP licences represent a commercially significant supplement to their domestic sales. For originator companies, MPP agreements provide a structured alternative to compulsory licensing in lower-income markets, providing some royalty income while avoiding the reputational damage of a forced licence. For Indian patent duration purposes, an MPP voluntary licence does not affect the domestic patent term. But it changes the commercial relationship between the originator and the Indian generic industry from adversarial to quasi-cooperative on specific products, which can affect the intensity of domestic patent litigation.
Recent Developments: The 2020-2025 Landscape
COVID-19’s Effect on Indian Patent Policy
The COVID-19 pandemic tested the Indian pharmaceutical patent system’s public health provisions in real time. As COVID-19 treatments and vaccines entered development and approval processes, civil society groups, government officials, and international health organizations called for waivers of intellectual property protections to enable maximum global production. India and South Africa co-sponsored a proposal at the WTO in October 2020 for a TRIPS waiver covering COVID-19 medical technologies.
The TRIPS waiver proposal was ultimately adopted in a limited form in June 2022, covering COVID-19 vaccines but not treatments or diagnostics. In India, the government did not invoke Section 92 emergency compulsory licensing for COVID-19 medicines, but the credible threat of doing so was reflected in the speed with which originator companies, including AstraZeneca, Johnson & Johnson, Pfizer, and Serum Institute of India, negotiated voluntary licences for domestic and export production.
The COVID-19 experience reinforced the structural features of India’s patent system: no data exclusivity meant generic manufacturers could enter COVID-19 drug markets quickly once regulatory approval was obtained, compulsory licensing provisions provided leverage in voluntary licence negotiations, and the pre-grant opposition system allowed civil society groups to challenge pending pharmaceutical patent applications on COVID-19 treatments before they were granted.
The National IPR Policy 2016 and Its Limits
India’s National IPR Policy 2016, approved by the Cabinet in May 2016, articulated the government’s commitment to strengthening intellectual property rights as a tool for economic development [12]. The policy emphasized enforcement, awareness, and infrastructure development, and signaled a more development-oriented approach to IP that could benefit both innovators and the domestic IP-intensive industries. The policy was received positively by multinational pharmaceutical companies as a sign of greater receptiveness to IP concerns.
In practice, the National IPR Policy has not produced the changes that multinational pharmaceutical companies sought most urgently: data exclusivity, patent linkage, or significant reforms to Section 3(d). Successive governments have reaffirmed the policy’s general orientation toward IP development while declining to implement the specific provisions that would affect pharmaceutical patent duration and commercial exclusivity.
The Draft National Pharmaceutical Policy and Patent Concerns
India’s Draft National Pharmaceutical Policy, circulated in 2023, addressed pharmaceutical pricing, domestic manufacturing, and access to essential medicines. The policy reflected the government’s continued prioritization of affordable medicine access as a primary objective. It did not propose changes to patent law but reinforced the government’s readiness to use compulsory licensing and pricing controls to maintain affordable access where patent protection raises prices beyond what the government considers acceptable.
For pharmaceutical companies considering long-term India investments, the draft policy confirmed that patent protection in India is commercially significant but not inviolable. The government’s public health toolkit — Section 84 and 92 compulsory licensing, drug price controls under the National Pharmaceutical Pricing Authority (NPPA), and preferential procurement policies — means that even a valid, fully enforceable Indian patent does not guarantee the same commercial exclusivity that the same patent would provide in the United States or a European market.
The Delhi High Court as the Dominant IP Forum
The Delhi High Court has emerged as the primary forum for pharmaceutical patent litigation in India. Its Intellectual Property Division, established in 2021 with dedicated IP judges, handles a large volume of pharmaceutical patent infringement cases, revocation petitions, and compulsory licence appeals. The court has developed specialized expertise in pharmaceutical patent law, and its judgments are the most closely watched in the Indian pharmaceutical IP landscape.
Several Delhi High Court decisions in the 2020-2024 period have refined the application of Section 3(d), the scope of process patent protection, and the standards for interim injunctions in pharmaceutical patent cases. The court’s decisions on claim construction for biotechnology and biologic patents have been particularly important as biosimilar litigation increases. Its approach to pharmaceutical patent disputes increasingly resembles that of specialized IP courts in the United States and Europe in procedural sophistication, though the substantive law remains distinctly Indian.
What Companies Should Do: A Strategic Checklist
For Originators and Multinational Pharma Companies
The single most important strategic reality for multinational pharmaceutical companies in India is this: the nominal 20-year patent term and the effective commercial exclusivity period may be radically different. Section 3(d), the absence of PTEs, the absence of data exclusivity, pre-grant and post-grant oppositions, and compulsory licensing all operate independently, and any one of them can eliminate or dramatically shorten the protection you expected. Building an India strategy around the assumption that your U.S. or European patent portfolio translates directly to India will produce incorrect financial models and incorrect market planning.
The practical checklist for originators entering or operating in India has four components. First, conduct a Section 3(d) freedom assessment before filing any pharmaceutical patent application in India. The assessment should evaluate whether each patent in your portfolio claims a genuinely novel compound or a modification to a known compound that meets the enhanced efficacy standard. Patents that fail this analysis should not be counted in your India revenue model. Second, price your drug at a level that makes a Section 84 compulsory licence application implausible. The Natco v. Bayer case provides the factual benchmark: a drug priced at more than 10 to 15 times the generic manufacturing cost, treating a serious illness, with low patient reach, faces compulsory licence risk. Third, monitor pre-grant and post-grant opposition filings on your key Indian patent applications. Opposition by well-resourced opponents with strong prior art requires substantive engagement and top-tier Indian patent counsel. Ignoring an opposition is not a viable strategy. Fourth, develop a voluntary licensing strategy for essential medicines before one is forced on you. Voluntary licences negotiated on your terms, with quality controls, royalty rates, and geographic restrictions, are commercially superior to compulsory licences granted by the Controller on his terms.
For Generic Manufacturers
For Indian generic manufacturers, the question of when a drug becomes available for generic production in India depends on which of the following events occurs first: patent expiry (the 20-year term from the filing date), successful pre-grant opposition defeating the patent application before grant, successful post-grant opposition or revocation petition after grant, successful compulsory licence application under Section 84, or the originator entering into a voluntary licence that includes the generic manufacturer.
The strategic priority is to identify, as early as possible, which of these pathways is most likely for each target drug. The answer determines where to invest legal and regulatory resources. For drugs with weak Section 3(d) positions, pre-grant opposition is often the most efficient pathway. For drugs with granted patents that have significant prior art problems, post-grant opposition or revocation may be more appropriate. For drugs with valid patents but extreme pricing, Section 84 is available after three years from the grant date. Patent intelligence platforms provide the data foundation for these assessments, tracking patent status, opposition filings, compulsory licence applications, and expiry dates in a consolidated format.
For Investors and Payers
Investors in Indian generic pharmaceutical companies need to understand which pipeline products depend on patent expiries in India, and whether those expiries are certain, contested, or uncertain. A generic company that has filed a successful pre-grant opposition against a major patent has a significantly earlier entry date than one that is simply waiting for a 2030 patent expiry. A company with a compulsory licence has different commercial economics than one manufacturing under voluntary licence.
Payers — government health schemes like Ayushman Bharat, state health authorities, and insurance companies — use Indian patent expiry data to forecast when generic versions of currently branded medicines will become available and at what price. The National Pharmaceutical Pricing Authority uses this analysis to plan drug price controls and to determine which drugs should be included on the National List of Essential Medicines at government-mandated price ceilings. Patent expiration forecasts feed directly into health budget planning at both the central and state government levels.
Key Takeaways
The most important conclusions from this analysis of drug patent duration in India:
• The statutory patent term in India is 20 years from the filing date, with no patent term extensions or supplementary protection certificates. Every day of regulatory delay directly reduces the commercial term without any compensation mechanism.
• Section 3(d) of the Patents Act is the most commercially significant provision in Indian pharmaceutical patent law. It excludes new forms of known substances from patentability unless they demonstrate enhanced therapeutic efficacy. Most evergreening strategies that work in the United States and Europe fail at this threshold in India.
• India has no data exclusivity framework. Generic manufacturers can apply for and receive CDSCO regulatory approval immediately after the originator, relying on the originator’s safety and efficacy data. Patent protection is the only barrier to generic entry; there is no regulatory safety net.
• Compulsory licensing under Section 84 is available three years after patent grant if reasonable public requirements are not met, the drug is not affordable, or it is not manufactured locally. The Natco v. Bayer decision confirms that extreme pricing of life-saving drugs triggers Section 84 applications. Pricing strategy must account for this risk.
• Pre-grant and post-grant opposition proceedings allow any person (pre-grant) or any interested person (post-grant) to challenge pharmaceutical patent applications and granted patents. Opposition by civil society groups and generic manufacturers has successfully blocked or narrowed patents on drugs including imatinib, sofosbuvir, bedaquiline, and lenalidomide.
• The effective commercial exclusivity period for a new drug in India typically ranges from zero (if the compound patent is rejected under Section 3(d)) to approximately 12 to 15 years for a genuinely novel compound with a fast regulatory approval timeline — substantially shorter than comparable U.S. or European exclusivity.
• India’s pharmaceutical IP environment is formal TRIPS-compliant. No WTO dispute panel has ruled against Section 3(d), the absence of data exclusivity, or the compulsory licensing framework. Multinational pressure through Special 301 and FTA negotiations has not resulted in statutory change.
• Patent intelligence platforms covering India, including DrugPatentWatch, integrate IPO patent data, CDSCO regulatory approvals, opposition proceedings, and compulsory licence records to provide a complete picture of a drug’s exclusivity status. Manual monitoring of multiple separate databases is the alternative, and it is inferior in speed and coverage.
FAQ
1. Can a foreign pharmaceutical company apply for a drug patent in India even if it already has patents in the United States and Europe?
Yes. A foreign company can file a patent application in India claiming priority from its U.S. or European application under the Paris Convention or the PCT. The Indian Patent Office will examine the application independently against Indian patentability standards, including Section 3(d). The fact that the same compound received patent protection in the United States or Europe does not mean it will receive protection in India. The EPO and USPTO apply different patentability standards, neither of which includes a Section 3(d) equivalent. Many pharmaceutical patents that are valid in the United States have been rejected in India on Section 3(d) grounds after being granted in every other major market. Foreign companies should treat Indian patent prosecution as an entirely separate exercise, requiring independent assessment of the Indian legal standards rather than reliance on foreign grant histories.
2. If a drug has no valid patent in India because of a Section 3(d) rejection, can the originator company prevent generic manufacturers from selling the drug in India?
No. If a patent application is rejected under Section 3(d), or if a granted patent is subsequently revoked, the originator company has no patent-based right to prevent generic manufacturers from producing and selling the drug in India. Without a valid patent, and without data exclusivity (which India does not have), there is no legal barrier to generic entry from a pharmaceutical IP perspective. The originator may still have trademark protection over its brand name, but generic manufacturers will sell under their own generic names and are not affected by trademark restrictions. This is the fundamental outcome in the imatinib, sofosbuvir, and bedaquiline cases: once the patent challenge succeeded, generics entered freely. The only remedy available to the originator in this scenario is to appeal the rejection or revocation decision through the court system while the challenge proceeds, which may involve seeking an interim injunction to maintain the status quo during the appeal.
3. Is a compulsory licence in India limited to domestic sales, or can Indian generic manufacturers export drugs produced under a compulsory licence?
Compulsory licences granted under Section 84 of the Indian Patents Act are issued primarily for the domestic Indian market. Section 84 is designed to address domestic supply and pricing conditions, and the Controller’s determination of what is required to satisfy the three conditions of Section 84 is based on the Indian market’s needs. However, Section 92A of the Patents Act implements the TRIPS amendment on compulsory licensing for export to countries with insufficient manufacturing capacity. Under Section 92A, a compulsory licence for export can be granted to manufacture a patented pharmaceutical product exclusively for export to a country that has issued or intends to issue a compulsory licence for the product, or has provided by notification that it intends to import from India. In practice, Section 92A has rarely been invoked. Voluntary licences, including through the Medicines Patent Pool, have been the more commonly used mechanism for enabling Indian generic export of medicines under IP frameworks.
4. How does India handle biosimilar regulatory approval and biologic patent protection differently from the United States?
India’s approach to biosimilar regulation and biologic patent protection differs from the United States in two fundamental respects. First, India has no data exclusivity for biologics. The BPCIA in the United States grants 12 years of reference product exclusivity to biologics, preventing biosimilar approval regardless of patent status. India has no equivalent provision. The CDSCO’s similar biologics guidelines set out a clinical comparability pathway for biosimilar approval, and biosimilar manufacturers can apply for approval as soon as they can demonstrate comparability, without any wait for a data exclusivity period. Second, India’s patent system applies Section 3(d) to biologic-related patents and may reject patents on new formulations or biosimilar manufacturing process improvements that would be patentable in the United States. The combination of no data exclusivity and strict patentability standards for biologics means that biosimilar entry in India can occur much earlier than in the United States for the same reference product. Indian companies like Biocon Biologics, Dr. Reddy’s, and Zydus have built significant biosimilar portfolios partly because the domestic Indian regulatory and patent framework makes early biosimilar development economically viable.
5. What is India’s position on patent linkage, and what does it mean practically for a generic company that wants to launch a drug before its Indian patent expires?
India explicitly rejects patent linkage. The CDSCO approves generic drugs based on pharmaceutical quality, bioequivalence, and safety data alone, without examining the patent status of the reference product. A generic company that wants to launch before a branded drug’s Indian patent expires can obtain CDSCO approval freely, but it cannot legally sell the product without the patent holder’s permission or a valid legal basis such as a successful patent challenge or a compulsory licence. The practical sequence is: the generic company obtains CDSCO approval (using the abbreviated pathway, citing the reference product’s regulatory data), then either waits for the patent to expire, challenges the patent through pre-grant or post-grant opposition proceedings, files a revocation petition in the High Court, or applies for a compulsory licence if the three-year post-grant period has passed and the Section 84 conditions are met. The absence of patent linkage means the regulatory and patent timelines are entirely independent, and a generic company can have its product approved and ready to launch on the day the patent expires, minimizing the delay to market entry.
References
[1] IBEF. (2024). Pharmaceuticals industry in India — sector report. India Brand Equity Foundation. https://www.ibef.org/industry/pharmaceutical-india
[2] India Brand Equity Foundation. (2024). Pharmaceuticals sector report 2024. IBEF. https://www.ibef.org/exports/pharmaceutical-exports-from-india
[3] Novartis AG v. Union of India & Others, (2013) 6 SCC 1. Supreme Court of India. https://main.sci.gov.in
[4] Watal, J., & Taubman, A. (2015). The WTO, intellectual property and pharmaceuticals. Cambridge University Press.
[5] DrugPatentWatch. (2024). Global pharmaceutical patent database, including India IPO data. https://www.drugpatentwatch.com
[6] Office of the United States Trade Representative. (2024). 2024 Special 301 report. USTR. https://ustr.gov/about-us/policy-offices/press-office/reports-and-publications/2024/2024-special-301-report
[7] Natco Pharma Ltd. v. Bayer Corporation, C.L.A. No. 1 of 2011 (Controller of Patents, Mumbai, March 9, 2012). Indian Patent Office.
[8] Medecins Sans Frontieres. (2015). MSF access campaign: Gilead’s hepatitis C drug sofosbuvir — India patent decision. MSF. https://msfaccess.org
[9] MSF Access Campaign & TB Alliance. (2023). Bedaquiline patent revoked by Indian Patent Office. https://msfaccess.org/indian-patent-office-revokes-bedaquiline-patent
[10] Pharmaceuticals Export Promotion Council of India. (2024). Annual performance review FY2023-24. Pharmexcil. https://www.pharmexcil.com/statistics
[11] Ministry of Commerce and Industry, Government of India. (2024). Pharmaceutical exports statistics FY2023-24. Department of Pharmaceuticals. https://pharmaceuticals.gov.in
[12] Department for Promotion of Industry and Internal Trade. (2016). National IPR Policy 2016. DPIIT, Ministry of Commerce and Industry. https://dipp.gov.in/policies/national-ipr-policy