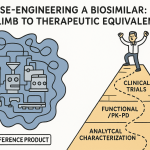
The Molecular Reality: Why Biosimilars Cannot Be Generics
The entire strategic, regulatory, and commercial architecture around biosimilars flows from one inescapable biochemical fact: living cells cannot be copy-pasted. A biologic is produced in a proprietary cell line under tightly controlled culture conditions, then extracted, purified, and formulated through a manufacturing process that can span dozens of steps, each introducing potential micro-variation. The final molecule that reaches a patient is not a single chemical entity. It is a heterogeneous population of protein isoforms, each shaped by post-translational events that no two manufacturers can control identically.
Aspirin has 21 atoms. A monoclonal antibody like adalimumab or pembrolizumab has roughly 25,000. That scale difference is not just a chemistry curiosity. It means that the three-dimensional fold of a therapeutic protein, the glycosylation pattern on its Fc region, and the charge variants present in a given batch all influence receptor binding, half-life, and immunogenicity. Small shifts in any of these attributes can matter clinically. The manufacturer of the originator product cannot itself produce an identical copy from one lot to the next, and it does not need to: regulators accept intra-product batch variation because the totality of data from clinical trials anchors the safety and efficacy profile.
Core Concept The phrase ‘highly similar’ in biosimilar regulation is not a hedge. It is the scientifically accurate ceiling of what biological manufacturing can achieve. ‘Identical’ is a standard that no biologic anywhere in the world meets, including the originator’s own consecutive lots.
This impossibility of exact replication has a second-order consequence that shapes the entire competitive landscape: it gives originator companies a legitimate scientific argument that any difference between their molecule and a biosimilar requires scrutiny. The argument has been weaponized in misinformation campaigns, but it originates in real science. Biosimilar developers must therefore invest in an analytical characterization program that does not just characterize their own molecule. It characterizes both molecules, simultaneously, to demonstrate that the biosimilar falls within the natural variation band of the reference product across all critical quality attributes.
The Analytical Toolbox: What Characterization Actually Involves
A modern biosimilar analytical package runs to hundreds of pages of data. Primary structure confirmation comes via peptide mapping with mass spectrometry. Higher-order structure analysis uses circular dichroism, differential scanning calorimetry, and hydrogen-deuterium exchange mass spectrometry to compare protein folding and stability. Glycan profiling via LC-MS documents N-linked and O-linked glycosylation patterns, which directly affect Fc receptor binding and serum half-life. Charge variant analysis by capillary isoelectric focusing identifies deamidation and oxidation differences. Receptor binding assays with SPR (surface plasmon resonance) or ELISA quantify on-target and Fc-effector function. In aggregate, these techniques are more sensitive to structural differences than most clinical endpoints. A well-executed analytical package is therefore the primary argument for biosimilarity, not just a supporting exhibit.
The regulatory and commercial implication is direct: biosimilar developers that invest heavily in analytical characterization upfront can reduce the size and scope of required clinical studies, compressing both timelines and costs. Developers that rush past analytics and rely on clinical data to carry the application face longer review cycles and greater regulatory uncertainty. The science at the molecule level dictates the strategic path at the development level.
Key Takeaways: Section 01
- Biologic manufacturing produces heterogeneous protein populations; exact replication is physically impossible, which is why ‘highly similar’ is the correct and complete regulatory standard.
- A biosimilar developer must characterize both molecules against each other, not just describe their own product.
- Advanced analytical investment reduces downstream clinical data requirements, shortening timelines and cutting development spend.
- The same scientific complexity that makes biosimilars hard to develop also makes them hard for originators to defend against with purely legal arguments once analytical equivalence is established.
Section 02
The Regulatory Spectrum: Biologic, Biosimilar, Interchangeable
The U.S. regulatory lexicon for biologics has three distinct tiers, each carrying different evidentiary requirements, market access mechanics, and commercial implications. Conflating them, or allowing payors and prescribers to conflate them, costs biosimilar manufacturers market share.
The originator biologic earns licensure through a standalone Biologics License Application (BLA) under Section 351(a) of the Public Health Service Act. The manufacturer submits full preclinical and clinical data packages, including Phase 1, 2, and 3 trial results across each intended indication. This is the innovator’s burden, and the exclusivity periods it earns, 4 years of data exclusivity and 12 years of market exclusivity under the BPCIA, compensate for it. Those 12 years represent the legal horizon within which no biosimilar can reach market regardless of scientific readiness.
A biosimilar earns licensure under Section 351(k), which allows the applicant to reference the originator’s approval history rather than re-running de novo efficacy trials. The evidentiary standard is ‘no clinically meaningful differences’ from the reference product in safety, purity, and potency. The totality-of-evidence framework, discussed in the analytical context above, governs this assessment. Critically, a 351(k) biosimilar approval is as legally complete as a 351(a) approval for the indications covered. A physician prescribing a biosimilar prescribes an FDA-licensed product backed by the same regulatory scrutiny framework as any originator.
The interchangeable designation adds a third, U.S.-specific layer. An interchangeable product satisfies additional statutory requirements confirming that it will produce the same clinical result in any given patient and, for products administered more than once, that switching carries no additional risk compared to continuous use of the reference product. The commercial value of this designation is narrow but tactically important: it enables automatic pharmacy-level substitution without prescriber intervention, subject to state pharmacy board rules. In practice, the designation is most valuable in retail pharmacy channels where pharmacists exercise substitution authority. In hospital and specialty pharmacy settings, the distinction matters less because substitution decisions pass through clinical committees regardless of interchangeability status.
Analyst Note The FDA has been explicit, repeatedly, that a biosimilar without the interchangeable designation is not inferior in safety or efficacy. The designation is a dispensing logistics designation, not a quality ranking. Any originator marketing material that implies otherwise is misinformation, and former FDA Commissioner Scott Gottlieb said so directly in 2018.
Key Takeaways: Section 02
- The 12-year market exclusivity clock under the BPCIA is the hard outer boundary for U.S. biosimilar entry, regardless of patent status.
- Section 351(k) approval is a full FDA license, not a conditional or second-tier approval.
- The interchangeable designation matters most in retail pharmacy; its strategic value in hospital or specialty channels is limited.
- Originator messaging that exploits the tiered terminology to imply quality differences is a documented commercial tactic, not a scientific argument.
Section 03
Two Agencies, Two Playbooks: FDA vs. EMA Compared
The EMA approved the first biosimilar, Omnitrope (somatropin), in 2006. By the time the FDA approved Zarxio in 2015, European regulators had nearly a decade of post-market safety surveillance data across multiple molecules and therapeutic classes. That head start created systematic differences in regulatory philosophy, exclusivity structures, and commercial outcomes that U.S.-focused biosimilar developers cannot afford to ignore.
Regulatory Architecture: Where the Frameworks Diverge
Both agencies apply the totality-of-evidence principle, but the EMA has historically moved faster toward a ‘comparability exercise’ model that minimizes duplicative clinical work. The EMA’s ‘tailored clinical approach’ has long held that if analytical and PK/PD data are sufficiently convincing, a separate comparative efficacy trial is unnecessary. The FDA has been moving toward this position but started from a more conservative baseline, historically expecting a Phase 3 comparative trial for most complex molecules. Recent FDA guidance on eliminating switching study requirements for interchangeability is the clearest signal yet that the two agencies are converging on methodology.
Exclusivity terms differ meaningfully. The EU gives originator biologics 8 years of data exclusivity and 10 years of market exclusivity, with a possible 11th year for a new indication approved within the first 8 years. The BPCIA’s 12-year U.S. market exclusivity is the longest among major pharmaceutical markets, a deliberate legislative choice to protect the biologic innovation ecosystem. From a portfolio planning perspective, a molecule that faces EU competition in year 10 may not face U.S. competition until year 12 or 13, creating a two-to-three-year revenue protection gap that originators price into their global revenue models.
| Feature | U.S. FDA (BPCIA / 351k) | European EMA (Centralized Procedure) |
|---|---|---|
| Framework established | 2010 | 2005 |
| First approval | 2015 (Zarxio) | 2006 (Omnitrope) |
| Approval standard | Highly similar; no clinically meaningful differences | Similar in quality, safety, and efficacy |
| Phase 3 comparative trial | Historically expected; now increasingly optional for well-characterized molecules | Tailored approach; often waived if analytical and PK/PD data are robust |
| Data exclusivity | 4 years | 8 years |
| Market exclusivity | 12 years | 10 years (+1 for new indication) |
| Interchangeability designation | Yes, separate statutory designation | None; all approved biosimilars are scientifically interchangeable |
| Substitution authority | Federal designation; state pharmacy law governs implementation | Delegated entirely to individual EU member states |
| Approval scope | Product-specific BLA; extrapolation to other indications reviewed case-by-case | Centralized MA valid across all EU member states; extrapolation accepted for well-justified cases |
Extrapolation: The High-Leverage Approval Strategy
One of the most consequential and often misunderstood regulatory concepts in biosimilar development is extrapolation: the regulatory grant of approval for an indication that was not directly studied in a comparative clinical trial, based on the totality of evidence from other studied indications. Both the FDA and EMA accept extrapolation, but the scientific justification must address mechanism of action in each indication, receptor and target similarity, patient population differences, and any indication-specific safety signals.
For a multi-indication blockbuster like adalimumab or infliximab, where the reference product has approvals across rheumatoid arthritis, psoriatic arthritis, ankylosing spondylitis, Crohn’s disease, ulcerative colitis, and psoriasis, extrapolation is not a regulatory shortcut. It is the primary mechanism by which a biosimilar developer can access the full commercial market without running a separate Phase 3 trial for each indication. Without extrapolation, the economics of biosimilar development would be fundamentally broken: the cost of replicating every indication-specific trial would approach or exceed the originator’s original development program, eliminating the cost advantage entirely. Developers must therefore invest in building airtight extrapolation justifications, not as a compliance exercise but as a core commercial strategy.
Key Takeaways: Section 03
- The EU’s 8-year data exclusivity versus the U.S.’s 12-year market exclusivity creates a systematic 2-to-3-year gap in competitive entry across markets, with major revenue implications for both originator and biosimilar revenue models.
- Regulatory convergence between FDA and EMA on reduced clinical data requirements is the single biggest cost-reduction driver for biosimilar development over the next five years.
- Extrapolation to unstu died indications is not optional strategy; it is the mechanism by which multi-indication biologics become economically viable biosimilar targets.
- In Europe, the scientific question of interchangeability is settled at approval; the commercial battle shifts immediately to national health authority reimbursement and substitution policy.
Section 04
Interchangeability: The U.S.-Specific Strategic Differentiator
The interchangeability framework is the arena where regulatory science, commercial strategy, and originator misinformation converge most visibly. Understanding the precise mechanics, the history of how the designation was used as a marketing weapon, and where the FDA’s policy is heading gives biosimilar teams a meaningful strategic edge.
The History of the Switching Study Requirement
The BPCIA’s statutory language for interchangeability requires that a biosimilar show it produces the same clinical result as the reference product in any given patient, and that switching carries no additional risk. The FDA initially interpreted this to require dedicated switching studies, typically a randomized crossover design in which patients alternate between the biosimilar and the reference product multiple times, then are evaluated for loss of efficacy, new adverse events, or immunogenicity signals. These studies were expensive, took 18 to 24 months to complete, and added $20 to $50 million to a biosimilar’s development cost. They also provided the originator community with a narrative: if the FDA requires switching studies, something about switching must be risky.
That narrative was never supported by European data. Over the 15 years since the EU began approving biosimilars, national registries in Norway (NOR-SWITCH), Denmark (DANBIO), and the Netherlands tracked hundreds of thousands of patients switched from originator biologics to biosimilars. The data showed no clinical signal of increased risk. Switching was as safe and effective as continuous treatment. The FDA, citing this accumulated evidence, issued draft guidance indicating it no longer intends to require switching studies as a default condition for interchangeability. This policy shift, if finalized, will halve the regulatory cost of achieving interchangeability for most molecules.
State-Level Substitution Rules: The Commercial Implementation Layer
Even with an interchangeable designation from the FDA, automatic pharmacy substitution is not guaranteed. Each U.S. state operates its own pharmacy practice act, and substitution rules vary. As of mid-2025, all 50 states have enacted biosimilar substitution laws, but the specific mechanics differ. Some states require pharmacist notification to the prescriber before substituting. Some require patient notification. Some mandate documentation in the pharmacy record. Some allow the prescriber to block substitution by writing ‘brand medically necessary’ or an equivalent directive. For a biosimilar developer building a U.S. commercial strategy, state-by-state policy mapping is not optional compliance work. It is a market access planning input that determines which states will generate volume from automatic substitution and which will require direct physician detailing regardless of FDA designation.
Key Takeaways: Section 04
- The FDA’s shift away from mandatory switching studies for interchangeability removes $20 to $50 million from development budgets and eliminates the originator’s ability to use the requirement as a misinformation anchor.
- Even with federal interchangeability, commercial substitution volume depends on state pharmacy laws, each of which must be mapped individually in market access planning.
- In hospital and specialty pharmacy channels, the interchangeable designation is largely irrelevant; formulary committee decisions drive substitution regardless of designation status.
Section 05
The Economic Equation: Savings, Price Erosion, and the Rebate Wall
The theoretical case for biosimilar savings is well-established. Biologics represent 2% of U.S. prescriptions and 46% of pharmaceutical spending. Any sustainable path to bending the drug cost curve runs through biosimilar competition. The actual realization of those savings, however, depends on market mechanics that are far less elegant than the theory.
Price Dynamics: What Competition Actually Does
Biosimilars typically launch at 15% to 50% below the reference product’s Wholesale Acquisition Cost (WAC). This range is narrow compared to small-molecule generic discounts of 80% to 85%, reflecting the higher development costs and more complex competitive dynamics. But WAC discounts overstate the actual pricing pressure in markets where net price, after rebates, governs formulary decisions. The more important data point is what happens to net prices over time as biosimilar competition matures. Weighted-average inflation-adjusted prices for biologics with biosimilar competition declined 56% over a five-year window, while prices for biologics without competition increased. In oncology infusion settings, where buy-and-bill economics and ASP (Average Sales Price) reimbursement govern purchasing, multiple biosimilar entrants have driven net prices to 60% to 70% of pre-competition reference product levels.
The Rebate Wall: How Originators Suppress Competition Without Patents
The rebate wall is the dominant commercial barrier in the U.S. biosimilar market. Understanding its mechanics is essential for any biosimilar commercial team, because no price point and no regulatory designation defeats it without a direct market access strategy.
Pharmacy Benefit Managers (PBMs) control drug formularies for most U.S. commercial insurance plans. Their revenue model is partially tied to the rebates they negotiate from manufacturers. Originator biologic manufacturers, facing the prospect of losing market share to lower-list-price biosimilars, can offer PBMs large rebates as a condition of maintaining preferred formulary position. Because PBMs’ revenue is often calculated as a percentage of list-price rebates rather than net savings, a high-list-price originator offering a 40% rebate can generate more PBM revenue than a low-list-price biosimilar offering a 10% rebate, even if the biosimilar’s net cost to the plan is lower. The PBM is financially incentivized to keep the high-rebate product preferred.
‘Of the 118 biologics set to lose exclusivity in the coming decade, only 10% currently have biosimilars in the development pipeline.’Dracey Poore, Cardinal Health (2024 Biosimilar Market Analysis)
The adalimumab market provides the clearest case study. AbbVie’s Humira generated U.S. revenues of $18.6 billion in 2022. Multiple biosimilars launched in 2023 with WAC discounts as steep as 85%. In their first full year of competition, those biosimilars captured approximately 3% of the market. The primary explanation was not physician hesitancy or patient resistance. Major PBMs maintained Humira on preferred formulary positions because AbbVie’s rebate structure made the originator more financially attractive to the plan than the cheaper biosimilars. Patients covered by those plans had no choice but to use the higher-cost product unless they paid out of pocket for the biosimilar. The result: a lower-cost, equally effective medicine was effectively excluded from the majority of the commercial market by financial intermediary incentives.
At-Risk Biosimilar Revenue: A Framework for Modelers
Biosimilar revenue models that project penetration solely from WAC price advantages will systematically overestimate market share in rebate-wall environments. A more accurate modeling framework accounts for the following inputs. First, the formulary position of the originator at time of biosimilar launch, which reflects the strength of the existing rebate structure. Second, the biosimilar’s ability to participate in the rebate game, which requires a list price high enough to offer meaningful rebates even if the net price is competitive. Third, payer mix by channel, since Medicare Part B buy-and-bill dynamics, Medicare Part D formulary construction, and commercial insurance rebate walls operate under different rules. Fourth, the number and timing of competing biosimilar entrants, since a market with six biosimilar competitors compresses prices faster but also fragments the share available to any individual entrant.
Investment Strategy: Economics
What Institutional Investors Should Watch
The rebate wall dynamic means that biosimilar commercial success is not a simple function of price or approval date. Investors should evaluate: (1) the biosimilar developer’s PBM contracting infrastructure and track record, (2) formulary position of the originator at the time of the biosimilar’s planned launch, (3) penetration in Medicare Part B, where ASP-based reimbursement creates different economics than commercial PBM channels, and (4) the pipeline of competing biosimilar entrants for the same reference product. A biosimilar with a robust PBM strategy and early Medicare penetration can outperform a rival with a lower launch price but no contracting infrastructure.
Key Takeaways: Section 05
- WAC list price discounts of 15% to 50% understate the real competitive dynamic; net price erosion in mature biosimilar markets reaches 56% or more over five years.
- PBM rebate wall mechanics can suppress biosimilar uptake even when the biosimilar is lower-cost at WAC, as the adalimumab launch made starkly visible.
- Revenue models for biosimilar programs must account for payer mix, PBM contracting capacity, channel economics, and competitor entry timing, not just price differential.
- Medicare Part B buy-and-bill channels behave differently from commercial PBM-managed markets and often offer earlier, more predictable biosimilar penetration.
Section 06
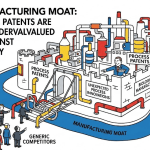
Patent Thicket Anatomy: How Originators Build Legal Fortresses
If the rebate wall is the dominant commercial barrier, the patent thicket is the dominant legal barrier. The two often work in concert: originator companies use litigation timelines to buy time for PBM contracting, and they use PBM revenue dependence to fund the legal campaign. Understanding how a thicket is constructed, patent class by patent class, is a prerequisite for building a credible challenge strategy.
The Composition-of-Matter Patent: The Clock That Starts the Race
Every biologic has a primary composition-of-matter patent that protects the molecule itself. This is the foundational IP asset. Its expiration is the event that theoretically opens the market to competition. In practice, the primary patent expiration is only the starting gun, not the finish line. For most blockbuster biologics, the primary patent expires years before the market exclusivity period ends, and secondary patents maintain legal coverage well beyond both dates.
AbbVie’s humira provides the canonical example. The core adalimumab composition patent expired in December 2016 in the U.S. The 12-year market exclusivity period under BPCIA, calculated from Humira’s 2002 approval, had already expired. But biosimilar entry did not occur until January 2023. The intervening seven years of monopoly protection came not from a single primary patent but from a fortress of over 100 secondary patents, each requiring individual assessment and potential challenge, all filed and maintained by a company with deep litigation resources and a strategic imperative to delay competition.
Secondary Patent Categories: The Thicket’s Building Blocks
Formulation patents cover specific concentrations of the active ingredient, excipient compositions, pH ranges, and buffer systems. These are particularly powerful barriers because a biosimilar manufacturer who develops a formulation that is analytically and clinically equivalent to the reference product may still infringe a formulation patent even if the proteins themselves are not patented. The FDA’s approval of a biosimilar for clinical equivalence does not create a safe harbor from formulation patent infringement claims.
Manufacturing process patents protect proprietary upstream cell culture conditions, purification steps, and quality control methods. Because the manufacturing process directly determines protein quality attributes, a biosimilar developer who independently optimizes their process for the same protein target may inadvertently replicate a patented step. Assessing freedom to operate on process patents requires deep process development knowledge combined with IP analysis expertise.
Delivery device patents protect the autoinjector pens, pre-filled syringes, and on-body injectors used to administer subcutaneous biologics. Device patents are often underestimated in thicket analyses because they seem peripheral to the drug itself, but they can be highly durable and technically difficult to design around. A biosimilar that uses the same drug but a different delivery device may require additional device-specific clinical or human factors studies to demonstrate equivalent usability and patient outcomes.
Method-of-use and dosing regimen patents cover specific therapeutic applications or administration schedules. These create the most complex ‘skinny labeling’ considerations for biosimilar developers. A biosimilar can, in some cases, launch for non-patented indications while omitting patented indications from its label. But carving out an indication carries its own commercial cost, as formularies and prescribers who manage patients across multiple indications prefer a product with a complete label.
The Patent Filing Roadmap: Evergreening in Practice
The technology roadmap for biologic patent evergreening follows a predictable lifecycle pattern that competitive intelligence teams can map and anticipate. Early in the biologic’s lifecycle, the originator files composition-of-matter patents and initial manufacturing patents. As the product reaches commercial maturity and generates revenue sufficient to fund lifecycle management, formulation and device patents proliferate. As the primary patent expiration approaches and biosimilar developers become visible in regulatory filings, a second wave of patents covers new indications, combination therapies, and refined dosing regimens. Some originators have used this pattern to file patents on improvements that were actually developed in response to biosimilar pressure, specifically because those improvements would apply to the originator’s own product and create additional infringement exposure for biosimilars already under development.
1
Year 0-3: Core IP Filing
Composition-of-matter, initial manufacturing process, and primary formulation patents filed around IND submission and Phase 1 data. These anchors define the molecule’s basic IP footprint and typically have the longest remaining life at product launch.
2
Year 4-8: Commercial Expansion
Device patents for specific autoinjector designs, indication-specific dosing regimens, and pediatric formulations. Second-generation formulations with improved stability or concentration. Patient registry patents in some jurisdictions.
3
Year 9-12: Defensive Clustering
High-concentration formulation patents targeting the subcutaneous self-injection market. Combination therapy patents. Biomarker-based patient selection patents. New manufacturing optimization patents. Filed specifically to extend coverage beyond primary patent expiration.
4
Year 13+: Evergreening Under Pressure
Next-generation molecule filing (biosuperiors or biobetters with reformulation). Pediatric indication expansions. Co-formulation patents with other biologics or small molecules. Filing pace typically accelerates as biosimilar Paragraph IV equivalents appear in BPCIA filings.
Key Takeaways: Section 06
- The primary composition-of-matter patent expiration is the beginning of the legal battle, not the end. For Humira, the primary patent expired in 2016; biosimilar entry did not occur until 2023.
- A thicket typically includes four distinct patent classes: composition-of-matter, formulation, manufacturing process, delivery device, and methods of use. Each requires separate freedom-to-operate and invalidity analysis.
- The originator’s patent filing timeline follows a predictable lifecycle pattern. Competitive intelligence teams can anticipate when new patent clusters will appear and prepare challenge strategies in advance.
- Skinny labeling, carving out patented indications from the biosimilar label, is a viable but commercially costly strategy that requires careful commercial impact modeling before adoption.
Section 07
IP Valuation: Quantifying the Fortress Asset-by-Asset
For pharma IP teams and institutional investors alike, a patent thicket is not just a legal obstacle. It is a balance sheet asset on the originator’s side and a liability-quantification challenge on the biosimilar developer’s side. Accurate IP valuation changes how deals are structured, how litigation budgets are allocated, and how biosimilar developers communicate portfolio risk to their own investors.
The Three Valuation Frameworks IP Teams Use
The income approach to patent valuation estimates the net present value of the cash flows attributable to the patent’s exclusionary power. For a primary composition-of-matter patent on a $10 billion revenue biologic in year 11 of its lifecycle, the income approach requires modeling the revenue erosion curve under a biosimilar competition scenario (which can be derived from empirical data in analogous markets), subtracting that from the continued monopoly revenue, and discounting the result at an appropriate risk-adjusted rate. This approach is most accurate for primary patents and weakens as you move to secondary patents, where attributing specific revenue to a single formulation or device patent requires assumptions that can vary widely.
The market approach uses transaction comparables: licensing agreements, litigation settlements, patent sale prices, and M&A transactions where specific IP portfolios were valued as part of the deal. The biosimilar settlement landscape provides a rich dataset. When an originator settles BPCIA litigation with a biosimilar developer and grants a delayed-entry license, the settlement terms (specifically, the authorized entry date and any royalty rate) imply a value for the contested patents. A settlement that delays entry by 4 years for a $2 billion market implies that the patents were worth approximately $400 million to $600 million in NPV terms, depending on assumptions about post-entry market share. This reverse-engineered valuation data is accessible through public settlement disclosures and litigation records.
The cost approach estimates replacement value: what would it cost to develop, file, and maintain an equivalent IP portfolio? This is most relevant for manufacturing process patents, where the cost approach translates directly into the biosimilar developer’s freedom-to-operate investment. If avoiding a process patent requires redesigning a purification step, the cost of that redesign, multiplied by the probability that the patent is valid and infringed, is the floor valuation of that patent from the challenger’s perspective.
IP Spotlight: AbbVie’s Humira (Adalimumab) Patent Portfolio
Anatomy of a 100-Patent Fortress
Humira’s IP portfolio is the most analyzed in biosimilar history. AbbVie amassed 132 U.S. patents covering adalimumab by 2022. Core composition-of-matter patents expired as early as 2016. The remaining portfolio spanned high-concentration subcutaneous formulations (which created the 40 mg/0.4 mL prefilled pen central to the self-injection market), manufacturing processes for reducing tungsten-induced protein aggregation, antibody purification methods, methods of treatment for specific plaque psoriasis subtypes, and the autoinjector device design. The high-concentration formulation patents were particularly valuable: they covered the product form that generated the majority of Humira’s U.S. revenue. Any biosimilar using a 40 mg/0.4 mL concentration needed either a license or an invalidity strategy for those specific claims. AbbVie’s settlement agreements with biosimilar developers, including Amgen, Sandoz, Mylan, Samsung Bioepis, and Fresenius Kabi, all included authorized entry provisions tied to specific launch dates rather than patent-by-patent validity determinations. The royalty and entry terms from those settlements imply an aggregate portfolio value in the $8 to $12 billion range, based on the revenue protection they secured between 2016 and 2023.
Key Takeaways: Section 07
- Patent portfolio valuation for biosimilar litigation targets requires all three approaches, income, market, and cost, applied class-by-class across the thicket, not as a single aggregate estimate.
- Settlement terms in BPCIA litigation are public record and provide an empirical market for patent value that IP teams can mine for comparable valuation inputs.
- For originators, the IP portfolio’s economic value is not just the discounted monopoly cash flows it protects. It is also the basis for authorized entry licensing revenue from settled biosimilar challengers, which can total billions in aggregate across multiple settlements.
- Biosimilar developers should calculate the ‘cost of avoidance’ for each patent class when building freedom-to-operate assessments, as this number directly inputs into the go/no-go economics of the development program.
Section 08
BPCIA Litigation Strategy: The Patent Dance and At-Risk Launches
The BPCIA’s patent resolution mechanism, the patent dance, is a uniquely structured information exchange and litigation sequencing process with no parallel in small-molecule Hatch-Waxman litigation. It has been litigated to the Supreme Court, strategically gamed by both originators and biosimilar developers, and regularly circumvented when the dance’s costs outweigh its benefits. Understanding the mechanics and the game theory gives biosimilar legal and commercial teams a tactical map.
The Patent Dance: Mechanics and Optionality
The dance begins when a biosimilar applicant submits its 351(k) application to the FDA. The applicant then has 20 days to notify the originator of its filing, triggering the exchange period. The biosimilar applicant provides the originator with a detailed copy of its application. The originator responds with a list of patents it believes could be infringed. The biosimilar applicant then provides detailed validity and non-infringement arguments for each listed patent. The parties negotiate to produce a list of patents for the first wave of litigation. All of this happens under confidentiality, making the process opaque to third-party competitive intelligence.
The Supreme Court’s 2017 decision in Sandoz v. Amgen confirmed that the patent dance is optional for the biosimilar applicant: a developer can bypass the exchange process and simply notify the originator of its intent to launch 180 days before doing so. Bypassing the dance accelerates the litigation timeline but removes the strategic advantage of narrowing the patent list before litigation commences. For a developer facing a 50-patent thicket, bypassing the dance means all 50 patents arrive in district court simultaneously rather than being sequenced. The choice depends on confidence in the validity and non-infringement positions on each patent class.
PTAB Challenges: The Pre-Litigation Weapon
Inter partes review (IPR) proceedings at the Patent Trial and Appeal Board (PTAB) are a parallel and often complementary strategy to district court litigation. A biosimilar developer can file IPR petitions against the weakest patents in the thicket before the BPCIA litigation commences, using the PTAB’s faster and more patent-challenger-friendly institution process to invalidate or narrow the most problematic claims. PTAB success rates for patent challengers in IPR proceedings have historically run above 60% on instituted petitions. For formulation and manufacturing process patents with extensive prior art in academic and industry literature, IPR petitions are a lower-cost, faster path to clearing specific obstacles than district court invalidity defenses.
At-Risk Launches: The High-Stakes Endgame
An at-risk launch is a biosimilar market entry that occurs before all BPCIA litigation is resolved, accepting the legal risk that a court might subsequently find infringement and impose damages or injunctive relief. The decision to launch at risk is the highest-stakes strategic choice in the biosimilar commercial lifecycle. The first-mover advantage in a biosimilar market can be worth hundreds of millions of dollars in net revenue, since each month of solo or duopoly competition before other biosimilars enter generates disproportionate share. But the downside risk, a court ordering an injunction and awarding lost profits or reasonable royalty damages, can wipe out several years of accumulated biosimilar revenue.
At-risk launches are more defensible when the biosimilar developer has strong invalidity and non-infringement positions on the most economically critical patents, when PTAB proceedings have already resulted in institution or cancellation of key claims, when the originator’s litigation posture suggests prioritizing settlement over maximum damages, and when the commercial window for first-mover advantage is particularly large. The decision requires a formal expected-value calculation that integrates legal probability estimates from patent counsel, commercial revenue projections, and downside loss scenarios, all reviewed by senior leadership and the board.
Key Takeaways: Section 08
- The patent dance is optional. Bypassing it accelerates litigation timelines but removes the ability to narrow the dispute before filing. The decision depends on thicket density and confidence in freedom-to-operate positions.
- PTAB IPR proceedings are a faster and cheaper mechanism to clear specific weak patents than district court litigation and should be initiated in parallel with, not after, BPCIA litigation preparation.
- At-risk launch decisions require a formal expected-value analysis that integrates patent counsel probability estimates, commercial revenue projections, and scenario-based downside modeling.
- Settlement authorized entry agreements, where the biosimilar developer accepts a fixed future launch date in exchange for dropping all patent challenges, are the most common resolution. Understanding the originator’s financial incentives for settlement versus continued litigation is a key negotiating input.
Section 09
Competitive Intelligence Playbook: From Data to Market Entry
A biosimilar developer that treats competitive intelligence as a late-stage activity, something to run once the molecule is in Phase 3, has already made its most expensive strategic mistake. The CI program should start at target selection and run continuously through launch, integrating patent, regulatory, clinical, and commercial data streams into a single decision-support system.
Target Selection: The CI-Driven Go/No-Go
Four data inputs should govern which molecules enter a biosimilar development program. The first is peak sales and remaining commercial life of the reference product, which sets the upper bound on market revenue available to biosimilars. The second is thicket density: total patent count, clustering of expiration dates, and prior invalidation history. A molecule with 15 secondary patents clustered in 2028 to 2032 is a different risk profile than one with 60 patents spanning 2025 to 2038. The third is the competitive pipeline: how many other biosimilar developers are already in clinical development, at what stage, and with what projected approval dates. The fourth is the channel and payer mix of the reference product, which determines how the rebate wall will be structured at the time of biosimilar entry.
Platforms like DrugPatentWatch aggregate these four data streams into a queryable intelligence environment. A CI team can pull the patent landscape for a target molecule, overlay it with competitor pipeline data, and build a probability-weighted revenue model for a potential biosimilar program in a single research session. Without that infrastructure, the same analysis requires weeks of manual patent database searches, regulatory filing reviews, clinical trial registry queries, and commercial data purchases.
Competitor Monitoring: Reading the Signals Before They Become Public
Biosimilar developers file with the FDA under the 351(k) pathway without public disclosure until the agency publishes the biosimilar product information. But multiple earlier signals reveal competitor activity. ClinicalTrials.gov registrations for ‘biosimilar’ studies with the reference product’s INN (International Nonproprietary Name) identify programs that have entered clinical development, often 18 to 24 months before an FDA application is submitted. Patent assignment records at the USPTO track manufacturing and formulation patent filings by potential competitors, indicating development activity before clinical work begins. SEC filings and investor presentations by publicly traded biosimilar developers include pipeline disclosures. Conference presentations at ASCO, EULAR, and ACR, the major clinical meetings for oncology and rheumatology, often include early biosimilar comparative data that reveals development stage.
Case Study: Applying CI to a Pembrolizumab (Keytruda) Biosimilar Program
Pembrolizumab is the world’s best-selling oncology drug by revenue, with 2024 sales exceeding $25 billion. Its core patents begin expiring in 2028, creating one of the largest biosimilar market opportunities in pharmaceutical history. A development team evaluating entry would begin a CI program today, not in 2026 or 2027.
The initial patent landscape assessment would identify the primary anti-PD-1 antibody composition patents, secondary patents covering the specific CDR sequences that define pembrolizumab’s unique binding profile, manufacturing process patents for the CHO cell line, protein A purification, and viral inactivation steps, and formulation patents for the histidine-buffered, polysorbate 80-stabilized liquid formulation. Any developer whose manufacturing process uses protein A affinity chromatography with similar elution conditions needs a specific freedom-to-operate analysis on those process claims.
The competitor landscape as of early 2025 already includes more than 14 programs in clinical development, with Samsung Bioepis SB27 in Phase 3 and multiple others in Phase 1 to 2. A developer entering now is entering a market that will likely have three to five approved biosimilars by 2030. The commercial planning question is not ‘can we get approved’ but ‘what market position and price point generates acceptable returns given the competitive density by our projected approval date.’ That calculation requires ongoing monitoring of competitor progress, not a one-time baseline assessment.
Investment Strategy: Competitive Intelligence
Portfolio Manager Framework for Biosimilar Pipeline Assessment
When evaluating a company’s biosimilar pipeline for investment purposes, the CI infrastructure is itself a valuation input. Companies with systematic CI programs, reflected in their target selection history, litigation outcomes, and market timing track records, generate higher risk-adjusted returns than companies that rely on in-house legal and regulatory teams working in isolation. Specific due diligence questions: Does the company have a documented process for patent thicket analysis before committing development resources? Have they used IPR proceedings offensively, and what were the outcomes? What is their track record on at-risk launch decisions? What percentage of their pipeline has entered markets within 12 months of patent expiration versus 24 or 36 months? These operational metrics are more predictive of future performance than the pipeline molecule list alone.
Key Takeaways: Section 09
- CI program launch should coincide with target identification, not Phase 3 enrollment. The further upstream the analysis, the greater the impact on development strategy and cost.
- Four data inputs drive target selection: peak reference product sales, patent thicket density and expiration clustering, competitor pipeline density, and channel payer mix at projected entry date.
- Competitor development activity becomes visible through ClinicalTrials.gov, USPTO patent assignments, SEC filings, and conference presentations well before FDA applications are submitted.
- For investors, CI program maturity is an operational proxy for management quality in biosimilar development companies and should be evaluated explicitly in diligence.
Section 10
Real-World Evidence as a Commercial Weapon
Real-world evidence (RWE) is the accumulated clinical data from patients treated outside the controlled conditions of a randomized trial: national patient registries, insurance claims databases, electronic health records, and observational cohort studies. For biosimilars, RWE has graduated from a post-marketing surveillance obligation to a primary commercial asset. The developer that builds a strong RWE program early, generates robust switching data, and disseminates that data effectively through medical affairs channels will outcompete rivals on physician confidence even when list prices are equivalent.
Infliximab: The Proving Ground
Infliximab biosimilars were the first major test of switching confidence in clinical practice. The NOR-SWITCH trial, a Norwegian government-funded randomized controlled trial published in The Lancet in 2017, enrolled 481 patients on reference infliximab (Remicade) across six diagnoses and randomized them to either continue on the originator or switch to the biosimilar CT-P13 (Remsima/Inflectra). After 52 weeks, disease worsening occurred in 26.2% of the CT-P13 arm versus 29.6% of the Remicade arm, meeting the pre-defined non-inferiority margin. The study was designed specifically to address switching safety, not just comparative efficacy, and its design directly countered the originator narrative that switching was clinically risky. Combined with DANBIO registry data from Denmark tracking thousands of patients switched under national health service protocols, the NOR-SWITCH findings gave formulary committees across Europe and the U.S. the evidence base to mandate switching and capture the cost savings. Denmark alone saved over 60 million Euros in the first two years of infliximab biosimilar adoption.
Adalimumab: RWE’s Commercial Role in the Post-Rebate-Wall Environment
In the U.S. adalimumab market, where the rebate wall limited biosimilar access through commercial PBM-managed channels, RWE played a different but equally strategic role. Biosimilar developers used European registry data showing equivalent disease control, equivalent drug survival rates, and high patient and physician satisfaction after switching to support payer arguments that Humira biosimilars should receive non-inferior formulary positioning. Published data from a cross-sectional European study covering over 1,200 patients treated with adalimumab biosimilar ABP 501 (Amjevita) found equivalent clinical outcomes in both new-start and switched patients, with high physician and patient-reported satisfaction. That data, distributed through a systematic medical affairs program, gave employers and health plans the evidence to challenge PBM formulary decisions that kept Humira in exclusive preferred positions.
Etanercept: Drug Survival as the Key RWE Metric
Drug survival, defined as the proportion of patients still on treatment at a given time point, is a composite real-world effectiveness and tolerability measure that is particularly relevant for biosimilar switching assessments. A patient who discontinues a biosimilar after switching, for any reason including loss of efficacy, adverse event, or patient preference, represents a commercial failure regardless of clinical trial equivalence. Data from a Frontiers in Pharmacology cohort study comparing reference etanercept to its biosimilar GP2015 in rheumatoid arthritis patients found 52-week drug survival rates of 82% for the originator and 80% for the biosimilar, a clinically non-meaningful difference. DAS28-CRP remission rates and low disease activity rates were also statistically equivalent across the 52-week follow-up. Drug survival data of this quality, consistently replicated across multiple cohorts and registries, is the RWE that turns a physician who is ‘cautiously open’ to biosimilars into one who switches patients proactively.
Key Takeaways: Section 10
- RWE generation should be planned before launch, not after. A medical affairs RWE strategy is a commercial infrastructure investment with a 3 to 5-year payback horizon.
- Switching study data, specifically designed RCTs like NOR-SWITCH and registry cohorts with explicit switching protocols, are the highest-value RWE assets for physician confidence building.
- Drug survival is a more persuasive real-world metric for prescribers than disease activity scores alone, because it integrates efficacy, tolerability, and patient acceptance into a single number.
- European registry data has direct commercial utility in U.S. market access arguments, particularly when challenging PBM formulary decisions that cite clinical uncertainty to justify originator preference.
Section 11
Pipeline Targets: The Next Decade’s Battleground Molecules
| Reference Product | Active Ingredient | Indication | 2024 Global Revenue (approx.) | U.S. Primary Patent Expiry | Biosimilar Pipeline | Key IP Risk |
|---|---|---|---|---|---|---|
| Keytruda (Merck) | Pembrolizumab | Oncology (multiple) | $25.0B | 2028 | 14+ programs; Samsung Bioepis SB27 in Phase 3 | CDR sequence patents; subcutaneous formulation patents |
| Dupixent (Regeneron/Sanofi) | Dupilumab | Atopic dermatitis; asthma | $11.0B | ~2031 | 0 in clinical development as of 2025 | Composition and formulation; bispecific mechanism complexity |
| Opdivo (BMS) | Nivolumab | Oncology (multiple) | $9.2B | 2028 | Early-stage programs; no Phase 3 as of early 2025 | Anti-PD-1 composition; manufacturing process |
| Stelara (J&J) | Ustekinumab | Psoriasis; IBD | $10.4B | 2023 (expired) | 5+ approved U.S. biosimilars as of 2024 | Remaining formulation patents; rebate wall primary barrier |
| Eylea (Regeneron) | Aflibercept | Wet AMD; diabetic macular edema | $6.0B | 2023 (expired) | 2 approved (Yesafili, Opuviz); ophthalmology-specific delivery challenges | High-dose formulation patents; intravitreal delivery device |
| Prolia / Xgeva (Amgen) | Denosumab | Bone health; oncology bone metastases | $5.8B | 2025 (expiring) | 2 approved (Jubbonti, Wyost) | Formulation patents; osteoporosis indication-specific dosing |
| Entyvio (Takeda) | Vedolizumab | Ulcerative colitis; Crohn’s disease | $4.9B | 2026 | Multiple in Phase 2/3 | Anti-integrin mechanism; SC formulation patents |
Pembrolizumab: The $25 Billion Battleground
Pembrolizumab is a structurally and mechanistically complex molecule. As a fully humanized IgG4 monoclonal antibody targeting PD-1, it works by releasing a brake on the patient’s own T-cell immune response. That mechanism makes immunogenicity assessment particularly challenging in biosimilar development: differences in the molecule that alter T-cell modulation could produce clinical effects not captured by standard binding assays or even PK/PD studies. Merck’s patent portfolio for Keytruda covers the core anti-PD-1 antibody sequences, multiple formulation variants (including the lyophilized vial and the liquid formulation), CHO cell manufacturing processes, and a growing array of combination therapy methods of use. The combination therapy patents are particularly strategic. As Keytruda generates its revenue primarily from use in combination regimens with chemotherapy, targeted agents, and other immunotherapies, a biosimilar whose label excludes combination indications is commercially neutered in the most profitable market segments.
Key Takeaways: Section 11
- The pembrolizumab opportunity represents the largest single biosimilar revenue target in pharmaceutical history. The 14+ programs already in development will produce an intensely competitive market by 2030, compressing per-product returns significantly.
- Dupilumab’s absence of biosimilar development activity as of 2025 creates a first-mover opportunity for developers willing to invest now for a 2031 to 2032 entry window.
- Ophthalmology biosimilars (aflibercept) carry unique regulatory requirements: sterility standards for intravitreal injection and device compatibility with standard clinical delivery systems must both be addressed in development design.
- Molecules facing primary patent expiration within 24 months but with thin biosimilar pipelines, like vedolizumab and denosumab, represent underserved commercial opportunities where competitive density will be lower than in the heavy-investment oncology targets.
Section 12
Sustainability, Policy Risk, and the Road Ahead
The next decade will bring approximately $234 billion in biologic sales to patent expiration. But the fraction of that revenue that translates into viable biosimilar commercial programs depends on resolving structural threats to market sustainability that, if left unaddressed, could replicate the quality and shortage problems that now characterize parts of the generic small-molecule market.
Market Concentration Risk: The Generic Precedent
The generic drug market offers a cautionary precedent. Intense price competition drove generic drug prices toward or below manufacturing cost for many molecules, triggering market exits, manufacturing consolidation, and eventually chronic drug shortages. The FDA’s Drug Shortages Staff database consistently lists dozens of critical generic medications in shortage. The biosimilar market has not yet reached that level of consolidation, but the trajectory of per-unit price erosion in mature biosimilar markets, particularly for filgrastim and trastuzumab, where six or more competitors have driven prices down 70% or more from the reference product WAC, shows the same competitive dynamic at work. A biosimilar market that is uneconomical to supply does not serve patients or payers.
IRA Medicare Negotiation: The Policy Wildcard
The Inflation Reduction Act’s Medicare Drug Price Negotiation Program, fully operational as of 2026, allows the Department of Health and Human Services to negotiate direct prices for high-spend Medicare Part D and Part B drugs. The first 10 drugs selected for negotiation included several small molecules. The second and third selection cycles will likely include biologics. The implications for biosimilar development economics are complex. On one hand, a negotiated Medicare price for an originator biologic compresses the originator’s revenue base, which reduces the absolute value of IP protection and could make originator patent litigation posture more settlement-oriented. On the other hand, the negotiated price creates a new price floor for the market that may limit how low biosimilar prices can go before the program’s own design undermines the economic rationale for developing biosimilars to compete with it. The interaction between IRA negotiated prices and biosimilar development incentives is the most consequential policy uncertainty in the sector.
Regulatory Evolution: The Next Frontier
The elimination of switching study requirements for interchangeability is the regulatory change with the most immediate commercial impact. But longer-term regulatory evolution will reshape development economics more fundamentally. FDA and EMA are both working toward greater use of platform data, where characterization and clinical data from one molecule in a class of biosimilars can partially support applications for subsequent molecules from the same manufacturer in the same class. This concept, analogous to platform licensing in vaccine manufacturing, could dramatically reduce per-program development costs for companies with established biosimilar manufacturing platforms. It is the structural analog to what mRNA platform manufacturing did for vaccine development timelines.
Complex biosimilars, including oligonucleotide-based biologics, cell-derived products, and next-generation bispecific antibodies, will require new analytical methodologies and regulatory frameworks that neither the FDA nor EMA has fully specified. Early engagement with regulators through pre-IND meetings, Type B meeting requests, and participation in FDA’s Biosimilar Product Development (BPD) program gives developers the opportunity to help shape those frameworks and reduce regulatory uncertainty for their specific programs.
Key Takeaways: Section 12
- Generic drug shortages are a structural outcome of price-driven market consolidation. The biosimilar market is at an earlier stage of the same cycle, and developers should plan for pricing discipline that preserves manufacturing margins, not just market share maximization.
- IRA Medicare negotiation creates a new policy variable in biosimilar revenue modeling. Programs targeting drugs likely to enter Medicare negotiation should build scenario models for the negotiated price environment, not just the current market structure.
- Platform manufacturing advantages will increasingly differentiate biosimilar manufacturers. Developers with established CHO cell culture platforms, robust analytical infrastructure, and regulatory relationships will compress per-program development costs as regulatory science matures.
- Early FDA engagement through the BPD program for novel or complex biosimilar targets is a strategic investment, not an optional compliance step, because it creates regulatory pathway clarity that compresses timelines and reduces late-stage uncertainty.
Master Summary: The Biosimilar Decision Matrix
Biosimilar development is a $100 to $300 million bet on a sequence of scientific, regulatory, legal, and commercial decisions that span a decade. The developers that consistently generate positive returns are not those with the best chemistry or the most experienced regulatory team in isolation. They are the ones that integrate all four capability domains: analytical development excellence that reduces regulatory risk upfront; IP intelligence that identifies patent thicket vulnerabilities before committing development capital; commercial infrastructure that can navigate both the FDA approval process and the PBM contracting environment; and real-world evidence programs that convert regulatory approval into durable market access.
The biosimilar market in 2025 is not the market of 2015. The science is validated. The regulatory pathways are mature. The real-world evidence base is overwhelming. The barriers that remain are structural, commercial, and legal, not scientific. That means the competitive advantage in this market belongs to organizations with strategic intelligence, commercial sophistication, and IP warfare capability, not just laboratory and manufacturing excellence.
Final Investment Strategy Note
What Separates Winners from Casualties in Biosimilar Development
Four characteristics distinguish the biosimilar developers that generate consistent investor returns from those that generate write-downs. First, target selectivity: the winners choose molecules with the right combination of market size, patent thicket manageability, and competitive pipeline density. They do not chase the largest market regardless of legal complexity. Second, patent intelligence as a core competency: they have in-house or deeply integrated external IP analysis infrastructure that runs from target selection through launch, not just during litigation. Third, PBM and payer contracting muscle: in the U.S., commercial success is more dependent on formulary strategy than approval date. Companies without PBM contracting experience are structurally disadvantaged. Fourth, RWE commitment: developers that invest in post-launch clinical programs generate the physician confidence data that translates market access into durable market share. The market will deliver $234 billion in opportunity over the next decade. The distribution of that opportunity will be highly unequal.
Tags
BiosimilarsPatent ThicketBPCIAInterchangeabilityRebate WallPTAB IPRReal-World EvidenceParagraph IV
Key Data Points
Biosimilars account for 2% of U.S. prescriptions but reference products that generate 46% of pharmaceutical spend.
Development cost: $100M to $300M. Timeline: 6 to 9 years. Price discount at launch: 15% to 50%.
Adalimumab biosimilars captured ~3% U.S. market share in Year 1 despite 85% WAC discount, due to PBM rebate wall dynamics.
Key Frameworks
Totality of Evidence, BPCIA Patent Dance, IPR at PTAB, At-Risk Launch Decision Framework, IP Valuation (Income / Market / Cost), Rebate Wall Analysis, RWE Commercial Strategy
Competitive intelligence transforms raw patent and regulatory data into a market entry decision with quantified legal and commercial risk.
Major Cases Covered
Sandoz v. Amgen (2017 SCOTUS) / Humira (adalimumab) patent fortress / NOR-SWITCH trial / DANBIO registry / Keytruda pipeline / IRA Medicare negotiation impact
This analysis is produced for informational and strategic planning purposes. It does not constitute legal advice. Patent status, regulatory guidance, and market data change continuously.
Sources: FDA, EMA, BPCIA statutory text, Sandoz v. Amgen (2017), NOR-SWITCH (Lancet 2017), Cardinal Health 2022 Biosimilars Report, RAND Corporation, IQVIA Institute, Matrix Global Advisors patent thicket analysis, DrugPatentWatch database, Center for Biosimilars, JMCP, Frontiers in Pharmacology, PMC registry studies.