A technical deep dive for IP teams, portfolio managers, R&D leads, and institutional investors in biologics and biosimilar development.
Why Regulatory Strategy Is Now a Core Competitive Asset
The FDA’s biosimilar approval rate, once accepted for full review under the 351(k) pathway, consistently exceeds 90%. That number is counterintuitive to anyone who treats regulatory affairs as a back-office function. It means the decisive work, the work that actually determines whether a biosimilar program succeeds or fails commercially, happens well before the Biologics License Application lands on an agency reviewer’s desk.
Regulatory affairs in biologics has shifted from a compliance cost center to a front-line strategic function. Portfolio decisions that once lived entirely in R&D, such as which molecule to pursue, which manufacturing process to lock in, which patient population to enroll, now require regulatory input at inception. Miss that window and you spend the next decade paying for it.
This is not a claim unique to highly capitalized originators. Amgen’s experience filing the first FDA-approved biosimilar in the U.S. (Zarxio, approved 2015) demonstrated that navigating agency expectations early, aligning on analytical methodology, and controlling the narrative in pre-IND meetings produced a cleaner and faster review than programs that waited for deficiency letters. For smaller biosimilar developers, the stakes are even higher because they rarely have the balance sheet to absorb a Complete Response Letter that demands a full clinical comparability study they had assumed could be waived.
The practical implication: regulatory strategy must be capitalized, not expensed. It is an investment in accelerating time-to-market, protecting patent-window revenue, and reducing the probability of late-stage failure.
Key Takeaways: Why Regulatory Strategy Matters
Regulatory excellence is not about avoiding mistakes. It is about compressing the 7-to-10-year biosimilar development timeline by months, which, against a $83.6 billion market growing at a 23.4% CAGR, can represent hundreds of millions in first-mover revenue. The companies earning outsized returns in biosimilars are the ones treating each agency interaction as a revenue event.
The Global Biosimilar Market: Size, Trajectory, and What the Numbers Actually Mean
Market Size and Growth Projections
The global biosimilar market sits at approximately $36 billion in 2024 and carries credible projections to $83.6 billion by 2029, representing a 23.4% CAGR. Separate forecasting from MarketsandMarkets places the figure closer to $72.3 billion by 2035 at a 7.5% CAGR on a larger base estimate. The variance in projections reflects genuine disagreement on uptake velocity, particularly in the U.S. market, where biosimilar substitution rates have lagged European counterparts by a wide margin despite the 2010 BPCIA framework having been in place for fifteen years.
Adalimumab biosimilars tell the most instructive story. AbbVie’s Humira ($20.7 billion in 2022 U.S. revenue) faced a wave of biosimilar entrants after its primary composition patent expired in January 2023. Sandoz (Hyrimoz), Coherus (Yusimry), Pfizer (Abrilada), Organon (Hadlima), Samsung Bioepis/Biogen (Hadlima, Imraldi), and several others entered the market. By mid-2024, biosimilar market share for adalimumab in the U.S. had reached roughly 25% by volume, a substantially slower adoption curve than European markets where biosimilar penetration crossed 85% within two years of entry. That gap traces directly to U.S.-specific market access dynamics: formulary exclusion arrangements, PBM contracting, and patient assistance programs that AbbVie employed to retain Humira on preferred formulary positions.
The lesson for regulatory strategists is that approval is necessary but not sufficient. A biosimilar that clears the FDA’s 351(k) pathway without a parallel market access strategy is commercially vulnerable, even against a technically weaker originator defense.
Therapeutic Area Dynamics
Oncology, immunology, and diabetes represent the highest-value biosimilar target categories, housing the majority of aging blockbuster biologics. Specific molecules with large global revenue exposure include etanercept (Enbrel), trastuzumab (Herceptin), bevacizumab (Avastin), rituximab (Rituxan), infliximab (Remicade), and insulin glargine (Lantus). Each carries a distinct patent and exclusivity profile, distinct interchangeability considerations, and distinct immunogenicity characterization requirements.
Ophthalmology biosimilars have recently attracted serious capital. Ranibizumab (Lucentis) and aflibercept (Eylea) biosimilars are entering U.S. and European markets, driven by the ocular administration route’s immunogenicity nuances and the concentrated prescriber base. The regulatory path for intravitreal biosimilars involves additional physicochemical scrutiny given the sensitivity of the target tissue.
Investment Strategy: Interpreting Market Signals
For institutional investors, the 23.4% CAGR on a base that remains U.S. substitution-constrained suggests there is structural upside if U.S. policy evolves toward stronger pharmacy-level substitution mandates or if PBM contracting practices change under continued political pressure. Monitoring biosimilar interchangeability designations, CMS reimbursement policy, and formulary transparency regulations provides a leading indicator for which companies’ biosimilar pipelines are likely to convert approvals into durable revenue.
Foundational Regulatory Science: Totality of Evidence, Biosimilarity, and the Stepwise Framework
Defining ‘Highly Similar’ and ‘No Clinically Meaningful Differences’
Both the FDA and EMA define a biosimilar as a biological product demonstrated to be ‘highly similar’ to a reference biologic with ‘no clinically meaningful differences’ in safety, purity, and potency. These phrases are not marketing language. They are legal and scientific thresholds that govern the entire development program.
‘Highly similar’ means that observed differences in structure or activity must be rigorously characterized and scientifically justified as incapable of affecting clinical outcomes. A glycan profile variation that a developer attributes to manufacturing process differences must be accompanied by receptor binding data, effector function assays, and potentially in vivo pharmacodynamic data demonstrating the difference is clinically inert. Agencies do not accept ‘highly similar except for’ as an analytic conclusion. They require the scientific argument for why the exception does not affect the clinical equivalence claim.
‘No clinically meaningful differences’ sets a clinical bar, not just an analytical one. It frames the evidentiary question: given that some structural heterogeneity is inevitable between a biosimilar and its reference product (because complex biologics are defined by their manufacturing process), at what threshold does structural difference become clinically consequential? The answer depends on the mechanism of action, the therapeutic window, the patient population’s immune sensitivity, and the dosing regimen. An infliximab biosimilar used in Crohn’s disease (where immunogenicity drives secondary non-response) faces a stricter immunogenicity comparability bar than a biosimilar used in ankylosing spondylitis.
Totality of Evidence: The Evidentiary Architecture
The ‘Totality of Evidence’ principle means that no single dataset is dispositive. A biosimilar cannot fail on analytical grounds alone if every other data domain demonstrates comparability. Conversely, a program with near-perfect analytical similarity but a signal of elevated anti-drug antibody (ADA) formation in a Phase 1 PK study will face intense agency scrutiny regardless of the upstream data package.
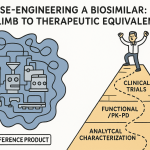
The practical architecture of a totality of evidence submission runs through four evidentiary layers:
The first layer is analytical and physicochemical characterization. This is the densest and most data-rich section of the submission, covering primary amino acid sequence confirmation, higher-order structure (HOS) analysis using techniques such as hydrogen-deuterium exchange mass spectrometry (HDX-MS), circular dichroism (CD), and Fourier-transform infrared spectroscopy (FTIR), post-translational modifications including N- and O-linked glycan profiling, charge variant analysis, aggregate and particle quantification, and in vitro biological activity assays.
The second layer is non-clinical comparability, typically comprising in vitro pharmacology studies (receptor binding, Fc effector function assays, cell-based potency), and, where warranted, in vivo pharmacology or toxicology studies. Regulatory agencies have increasingly accepted in vitro non-clinical packages without in vivo animal studies when the analytical data are compelling, particularly for monoclonal antibodies with well-understood mechanisms.
The third layer is clinical pharmacology, primarily comparative PK and PD studies in healthy volunteers or sensitive patient populations. These studies typically measure area under the curve (AUC), peak concentration (Cmax), and bioequivalence margins (90% CI within 80-125%), along with immunogenicity endpoints.
The fourth layer is confirmatory clinical efficacy and safety data in a sensitive patient population, often the originator’s pivotal indication. This layer is increasingly compressible when the three upstream layers are robust, but it is rarely fully eliminated for complex molecules.
Key Takeaways: Regulatory Science Fundamentals
The stepwise nature of the biosimilar framework creates a direct relationship between the quality of upstream data and the cost of downstream trials. Every dollar invested in state-of-the-art analytical characterization in Year 1 of a biosimilar program can eliminate multiple millions in clinical trial costs in Year 5. The analytics-first investment thesis is not aspirational. It is mechanistically grounded in how agencies weigh totality of evidence.
FDA’s 351(k) Pathway: Mechanics, Interchangeability, and IP Valuation
BPCIA Framework: What Section 351(k) Actually Created
The Biologics Price Competition and Innovation Act of 2009 (BPCIA), enacted as Title VII of the Affordable Care Act, amended the Public Health Service Act to add Section 351(k), creating the abbreviated licensure pathway for biosimilars. Before BPCIA, there was no statutory route to reference a previously approved biologic product in a new BLA. Every biologic required a full standalone package. BPCIA changed that by allowing biosimilar applicants to rely on the FDA’s prior finding of safety and effectiveness for the reference product, provided the applicant could demonstrate biosimilarity through the comparability framework.
Key structural elements of the 351(k) pathway include a 12-year reference product exclusivity period (running from the date of first licensure of the reference product, not from patent expiry), a 4-year exclusivity period before which a 351(k) application cannot even be submitted (the ‘first licensure’ date triggers the clock), and the patent dispute resolution procedures that constitute the ‘patent dance.’
The distinction between a standard biosimilar and an interchangeable biosimilar is commercially consequential. An interchangeable biosimilar must meet the biosimilarity standard plus an additional requirement: the applicant must demonstrate that the product can be expected to produce the same clinical result as the reference product in any given patient, and for products administered more than once, must show that the risk in safety or diminished efficacy from alternating or switching between the interchangeable product and the reference product is no greater than the risk of using the reference product without such alternation. This standard is typically supported by ‘switching studies,’ which randomize patients between the biosimilar and the reference product across multiple switch cycles.
IP Valuation: The 351(k) Reference Product as a Core Asset
For originators, the reference product’s regulatory exclusivity is a distinct IP asset that sits alongside, and in some cases outlasts, the patent estate. This is worth quantifying precisely.
Humira (adalimumab), approved in December 2002, carried its 12-year reference product exclusivity through December 2014. AbbVie’s primary composition patent, U.S. 6,090,382, expired in December 2016, and the broader patent thicket (discussed below) extended meaningful protection into the 2030s for some claims. For biosimilar developers, the 12-year exclusivity period was the binding constraint, not the primary patent, which had to be cleared in parallel through the patent dance.
Investors valuing a biosimilar developer’s pipeline should treat the reference product exclusivity expiry as the floor for market entry timing analysis, not the primary patent expiry. A biosimilar targeting a molecule still within its 12-year exclusivity window can file its 351(k) application (after 4 years), can even receive tentative approval, but cannot receive a final effective approval until the exclusivity expires.
For biosimilar developers, the practical IP asset to quantify is the total window of patent exposure remaining after the exclusivity expiry. A molecule where the primary patent expires simultaneously with or shortly after the 12-year exclusivity presents a relatively clean entry scenario. A molecule where the originator has built a 50-patent ‘thicket’ around manufacturing processes, formulations, dosing regimens, and devices presents a different risk calculus entirely, and requires patent-by-patent invalidity and non-infringement analysis.
Investment Strategy: Reading FDA Biosimilar Approvals
FDA biosimilar approval data has predictive value for portfolio managers. When the FDA grants interchangeability designation, it signals that switching studies were conducted and passed, which means the biosimilar has a credible claim to pharmacy-level auto-substitution in states with permissive substitution laws. Tracking interchangeability grants by molecule tells an analyst which biosimilar companies have invested in the clinical work required for formulary access, not just regulatory approval.
Semglee (insulin glargine-yfgn, Biocon/Viatris) received the first FDA interchangeable biosimilar designation in July 2021. Cyltezo (adalimumab-adbm, Boehringer Ingelheim) received interchangeable designation for Humira in October 2021. The downstream formulary and PBM dynamics for these products relative to non-interchangeable adalimumab biosimilars are a natural experiment in the commercial value of the interchangeability designation.
EMA Centralized Procedure: Scientific Advice, CHMP Dossier Architecture, and National Substitution Divergence
The Centralized Procedure’s Scope and Commercial Reach
The EMA’s centralized procedure, governed by Regulation (EC) No 726/2004 and EU Directive 2001/83/EC, produces a single marketing authorization valid in all 27 EU member states plus Iceland, Liechtenstein, and Norway. For biologics, including biosimilars, the centralized procedure is mandatory.
The EMA’s Committee for Medicinal Products for Human Use (CHMP) conducts the scientific assessment and issues an opinion that forms the basis of the European Commission’s marketing authorization decision. Assessment timelines run 210 active days (with clock stops for questions), though complex applications routinely stretch longer.
The EMA published its first biosimilar guideline in 2005, making Europe the global leader in articulating the regulatory framework for follow-on biologics. The framework’s core documents include the overarching biosimilar guideline (EMEA/CHMP/74562/2006), product-class-specific guidelines (for monoclonal antibodies, EPO, G-CSF, insulins, etc.), and the reflection paper on immunogenicity.
Scientific Advice: Mechanics and Strategic Value
The EMA’s scientific advice mechanism is arguably the most valuable regulatory tool available to European biosimilar developers. Unlike FDA meetings, which are limited to specific procedural types (pre-IND, Type B, Type C), EMA scientific advice can be requested at any stage of development and can cover any aspect of the development program, from the design of the analytical comparability exercise to the statistical approach for the confirmatory clinical trial.
Scientific advice is provided in writing after a CHMP rapporteur team reviews the company’s briefing document. For complex questions, a scientific advice meeting may be convened. The output, a Scientific Advice letter, is not legally binding, but it constitutes the agency’s position at the time of issuance and creates a reasonable expectation that advice followed in good faith will not generate deficiency letters on the same points at marketing authorization review.
Companies that use scientific advice poorly, by asking yes/no questions when the agency needs to understand the full data context, or by submitting incomplete briefing documents, extract limited value. Companies that use it as a genuine dialogue mechanism, presenting their working scientific rationale and asking the CHMP to identify gaps, create a feedback loop that de-risks the program at each development stage.
No EU-Level Interchangeability: The National Substitution Patchwork
The EMA does not grant an interchangeability or substitutability designation. The 2019 CHMP and CMHV statement on the scientific rationale supporting biosimilar interchangeability confirmed that biosimilars approved in the EU are safe to use interchangeably, but the operational decision on pharmacy-level substitution is left to individual member states.
The resulting patchwork is complex. Germany, France, and Denmark have adopted automatic substitution policies under specific conditions. Several Central and Eastern European markets lack formal substitution frameworks, requiring a prescriber action to switch patients. The U.K. (post-Brexit, regulated by the MHRA) has its own evolving substitution guidance.
For biosimilar commercial teams, this means market access strategy must run 27 distinct regulatory playbooks in parallel with the central CHMP approval. The country-level work on formulary positioning, physician education, and national health authority engagement is not an afterthought to the EMA submission; it must run concurrently.
IP Valuation: EMA Data Exclusivity and Reference Biologic Protection in Europe
The EU grants biologics an 8+2+1 year market exclusivity structure: 8 years of data exclusivity (during which no competitor can reference the originator’s clinical data), 2 additional years of market protection (during which the biosimilar can receive approval but cannot be commercialized), and a possible additional 1 year for a new therapeutic indication approved within the 8-year data exclusivity period.
This 10-year minimum exclusivity period (8+2) is the binding constraint for biosimilar European market entry, layered against any surviving patent claims. Biosimilar developers targeting European markets must model both the EU exclusivity clock and the European patent estate, which is governed by the European Patent Office (EPO) and national patent offices, to construct an accurate earliest-launch-date estimate.
Health Canada, PMDA, TGA, and Emerging Markets: Regional Nuances That Sink Timelines
Health Canada: Subsequent Entry Biologics (SEB) Framework
Health Canada uses the term ‘Subsequent Entry Biologics’ (SEBs) rather than biosimilars. The SEB guidance (2010, updated 2016) aligns closely with the FDA and EMA approach on totality of evidence and stepwise development but contains some specific Canadian requirements worth flagging. The reference biologic for Canadian SEB submissions must typically be a product approved and marketed in Canada, which means foreign-approved reference product data may require bridging to a Canadian-authorized reference product. For molecules approved in Canada through the FDA or EMA approval reliance pathway, this bridging requirement is often manageable. For molecules with limited Canadian market presence, it adds complexity.
Health Canada’s Biologics and Genetic Therapies Directorate (BGTD) offers a Pre-Submission Meeting program comparable to FDA’s Type B meeting mechanism. Companies developing SEBs for the Canadian market should request pre-submission meetings on the comparative clinical program design, as the BGTD has issued specific guidance on the use of foreign-collected reference product data that interacts with the bridging question.
PMDA: Japan’s Biosimilar Framework and Ethnic Bridging Requirements
Japan’s Pharmaceuticals and Medical Devices Agency (PMDA) has operated a biosimilar framework since 2009. Japan’s regulatory approach emphasizes ethnic sensitivity; the PMDA has historically required Japanese clinical data for many new molecular entities due to concerns about pharmacokinetic or pharmacodynamic differences in Japanese versus Western populations.
For biosimilars, the ethnic bridging requirement is typically addressed by including Japanese subjects in the comparative PK study or by conducting a standalone Japanese PK bridging study. The PMDA’s position has evolved: for molecules with a strong global biosimilar data package and well-characterized PK that is not expected to differ by ethnicity (typically non-immunological PK drivers), it has accepted Western data with a smaller Japanese safety and immunogenicity dataset. Companies should obtain PMDA scientific advice (Consultation for New Drug Approval) early to clarify current expectations, as PMDA positions on bridging data requirements have shifted meaningfully over the past five years.
TGA: Australia’s Biosimilar Pathway
The Therapeutic Goods Administration (TGA) follows a pathway closely aligned with EMA guidelines, reflecting the formal regulatory reliance framework Australia applies to EMA-approved products. For biosimilars already authorized by the EMA, the TGA abbreviated assessment pathway can substantially compress Australian review timelines. Australia does not have a separate interchangeability designation; substitution decisions are made at the state/territory level.
Emerging Markets: ANVISA, WHO Prequalification, and Regulatory Reliance
Latin America, Southeast Asia, and Sub-Saharan Africa represent the next frontier for biosimilar market expansion. Brazil’s ANVISA has a formal biosimilar pathway (RDC 55/2010, updated through subsequent resolutions) that distinguishes between ‘individual development’ (full non-clinical and clinical package) and ‘comparative development’ (totality of evidence approach). ANVISA’s comparability route requires the reference product to be registered in Brazil, which has historically meant the originator’s Brazilian-approved product must serve as the comparator, creating logistical challenges when global reference product supplies differ from Brazilian-marketed formulations.
The WHO Prequalification Programme for biosimilars has gained importance for developers targeting low-income country markets or multinational procurement (e.g., PAHO, UNICEF). WHO PQ operates on a totality of evidence framework aligned with EMA/FDA principles and accepts data packages prepared for major regulatory authorities, reducing the marginal cost of achieving WHO qualification once a major-market dossier is complete.
Regulatory reliance, where a national authority formally relies on another authority’s assessment without conducting a full independent review, is increasingly common in emerging markets. Singapore’s HSA, Canada’s Health Canada, Switzerland’s Swissmedic, and several others have formal reliance frameworks. Biosimilar developers can design their global regulatory strategy to sequence submissions through jurisdictions in an order that maximizes reliance opportunities, compressing total global submission costs substantially.
Pre-Submission Strategy: Scientific Advice, Type 2 Meetings, and BPD Program Mechanics
FDA Meeting Types: Matching the Mechanism to the Question
The FDA’s biosimilar-specific meeting program operates under the framework established in the BPCIA and elaborated in FDA’s 2015 and 2018 guidance on biosimilar development meetings. The key meeting types for biosimilar programs are:
Biosimilar Initial Advisory (BIA) meetings are available early in development, before an IND is filed, to discuss general questions about whether a proposed comparability exercise is scientifically appropriate for the reference product and proposed indication. BIAs are informational rather than binding.
Type 2 meetings address specific clinical, non-clinical, or manufacturing questions and are the workhorses of FDA-company dialogue during biosimilar development. A well-executed Type 2 meeting on the design of the confirmatory clinical trial can resolve endpoint selection disputes, sample size assumptions, and sensitivity analyses before the study is enrolled, eliminating the most common source of late-stage deficiency letters.
The Biosimilar Product Development (BPD) program is a formal feedback mechanism that provides written FDA feedback on biosimilar development questions in lieu of or in addition to meetings. BPD submissions are tiered by type (I through IV), with Type 1 being requests for meetings and Types 2-4 covering specific data and scientific questions. Companies have found that submitting BPD Type 2 or 4 packages with detailed scientific rationale and data elicits more actionable FDA feedback than broadly worded questions.
Pre-BLA meetings (equivalent to a pre-NDA meeting for small molecules) should be requested approximately 6-12 months before a planned BLA submission to confirm submission readiness, agree on the format and content of the dossier, and identify any known agency concerns.
How to Structure a Briefing Document That Actually Works
FDA meeting briefing documents for biosimilar programs are commonly deficient in three ways: they are too long, they ask questions the agency cannot answer without seeing data, and they fail to present the scientific rationale before the question.
A briefing document that performs well in FDA review follows a specific architecture. It opens with a concise product and development history that confirms the reader’s orientation to the program. It then presents the specific data or rationale relevant to each question, followed by the question itself, formatted as a specific query with a yes/no or choose-from-options answer structure that makes agency response efficient. Appendices contain the detailed analytical or clinical data.
Questions framed as ‘Does FDA agree that…’ followed by a clearly articulated scientific position are processed faster and more usefully than ‘What does FDA recommend…’ questions, which require the agency to generate a position without any proposed framework to react to. The agency’s time is a constraint. Briefing documents that respect that constraint by doing the scientific work upfront get better meetings.
Key Takeaways: Pre-Submission Strategy
A pre-IND meeting with FDA is not bureaucratic overhead. It is the single highest-leverage regulatory investment available to a biosimilar developer in the first two years of a program. Developers who skip pre-submission engagement to save time discover, at BLA review, that they have spent 7 years building a comparability package that does not match the agency’s current expectations, often on clinical trial endpoints or immunogenicity assay validation.
Analytical Characterization: The Front-Loaded Investment That Determines Clinical Scope
Critical Quality Attributes and the Analytical Comparability Matrix
Analytical comparability begins with defining the reference product’s critical quality attributes (CQAs): the physicochemical and biological properties that have a demonstrated or potential impact on safety or efficacy. CQAs for a monoclonal antibody typically span primary structure (peptide mapping, disulfide bond connectivity, free sulfhydryl groups), glycosylation profile (N-glycan site occupancy, glycan antennae, sialylation, fucosylation), charge heterogeneity (deamidation, oxidation, C-terminal lysine processing), size heterogeneity (aggregates, fragments), Fc receptor binding (FcRn, FcgRIIIa, FcgRII), Fab-mediated activity (antigen binding by SPR, ELISA), and cell-based biological activity (ADCC, CDC, apoptosis, depending on mechanism).
The analytical comparability matrix is the structured document that maps each CQA against its analytical method, the method’s qualification/validation status, the acceptance criteria for similarity, and the outcome of the comparison. This matrix becomes the scientific spine of the quality module in the BLA or MAA submission.
Methods used in the comparability matrix must be validated for their intended purpose. The FDA and EMA have both issued guidance making clear that analytical methods used to claim similarity must be shown to be capable of detecting relevant differences. An HPLC method that cannot distinguish a glycan variant known to affect Fc effector function is not adequate for claiming glycan comparability relevant to ADCC-dependent mechanisms of action.
Higher-Order Structure: The Technical Frontier of Biosimilar Characterization
Higher-order structure (HOS) analysis has become a differentiating analytical capability for biosimilar developers. Techniques including hydrogen-deuterium exchange mass spectrometry (HDX-MS), X-ray crystallography, cryo-electron microscopy (cryo-EM), and nuclear magnetic resonance (NMR) spectroscopy provide increasingly detailed views of protein conformation and dynamics that were inaccessible a decade ago.
The regulatory expectation for HOS characterization has risen substantially since the first wave of biosimilar approvals. The FDA’s guidance on analytical procedures for biosimilars (2019) explicitly calls for ‘state-of-the-art’ analytical techniques, and the agency has cited inadequate HOS characterization as a deficiency in Complete Response Letters for biosimilar applications.
For biosimilar developers, investment in HDX-MS capability, either in-house or through contract analytical laboratories, is now essentially a table-stakes requirement for complex monoclonal antibody programs. Developers who rely solely on circular dichroism and intrinsic fluorescence for secondary and tertiary structure characterization will encounter pushback from FDA and EMA reviewers on HOS sufficiency.
Fingerprint Similarity: The Statistical Framework
The ‘analytical fingerprint’ approach, where the biosimilar and reference product are compared across a comprehensive attribute panel and evaluated for similarity using quality range (QR) methods, has become a widely used framework in biosimilar analytical submissions. The QR approach defines similarity boundaries based on the natural variability of the reference product (typically across multiple lots, markets, and time points) and evaluates whether biosimilar attribute values fall within those boundaries.
The FDA’s 2022 draft guidance on establishing similarity through analytical procedures endorsed a statistical framework for the fingerprint approach that requires developers to use multiple reference product lots, conduct measurements across relevant release and characterization timepoints, and report biosimilar data relative to the reference product’s range of natural variability.
Sourcing adequate reference product lots for the fingerprint analysis requires careful planning. The FDA expects originator product from the U.S. market. EMA expects EU-marketed product. For global programs, this often means procuring and characterizing reference product from multiple markets, confirming lot-to-lot consistency across regions before using the combined dataset to establish similarity ranges.
Key Takeaways: Analytical Characterization
The return on investment for analytical characterization is direct and quantifiable. A biosimilar program with a comprehensive, validated analytical comparability package can justify a streamlined clinical program to regulators, often replacing a full Phase 3 efficacy trial with a comparative PK study plus safety and immunogenicity data. At a cost differential of $50-100 million between a full Phase 3 and a PK-only confirmatory program, the analytics investment is not a science question. It is a capital allocation decision.
Clinical Comparability Programs: PK/PD Study Design, Immunogenicity, and Confirmatory Trial Architecture
Comparative PK Studies: Design Standards and Bioequivalence Margins
The comparative PK study is typically the first and most structurally determinative clinical study in a biosimilar program. Its primary objective is to demonstrate that the systemic exposure of the biosimilar and the reference product are equivalent within pre-specified margins, using a 90% confidence interval framework that mirrors small-molecule bioequivalence standards (80-125% on log-transformed AUC and Cmax, or alternative metrics agreed with the agency for non-linear PK molecules).
Study population selection is a strategic variable. Healthy volunteers offer the most sensitive population for detecting PK differences because disease-related factors (inflammation, altered distribution, elevated drug clearance) that are present in patients can mask exposure differences. However, for molecules with significant immunogenicity concerns in healthy volunteers (e.g., certain fusion proteins or ADAs with clinical consequences in healthy subjects), a patient population may be required or preferred.
Crossover versus parallel designs require careful consideration for biosimilar PK studies. Crossover designs are statistically powerful for highly variable PK compounds but are only appropriate for molecules where carryover effects and washout periods are manageable, and where immunogenicity from a single dose is unlikely to confound the second period. Parallel designs are more conservative statistically (require larger sample sizes) but are necessary when immunogenicity concerns preclude repeated dosing in the same subject.
Immunogenicity Comparability: The Highest-Stakes Clinical Question
Immunogenicity comparability is the clinical question that generates the most regulatory scrutiny and the most litigation risk in biosimilar programs. Anti-drug antibodies (ADAs) can affect PK (neutralizing or clearing antibodies alter drug exposure), safety (immune complex-mediated reactions, cross-reactivity with endogenous proteins), and efficacy (secondary non-response). For molecules where immunogenicity drives clinical outcomes, the FDA and EMA require a direct head-to-head immunogenicity comparison between the biosimilar and reference product in the confirmatory clinical study.
The immunogenicity assay package requires substantial method validation work. Screening assays (typically ECL-based or ELISA) must be validated for sensitivity, drug tolerance, selectivity, and precision. Confirmatory assays to rule out false positives and neutralizing antibody (NAb) assays to characterize the functional consequence of ADA formation must also be validated against the reference product. The FDA’s 2019 immunogenicity guidance for therapeutic proteins specifies a risk-based approach to the scope of the immunogenicity assessment, with complex molecules in long-term patient exposures requiring the most comprehensive package.
The timing of ADA sampling relative to dosing is a common source of protocol deficiencies. Pre-dose, end-of-treatment, and follow-up samples are the minimum. For molecules with delayed-onset immunogenicity (certain fusion proteins, products with manufacturing process-related impurities as potential drivers), extended follow-up beyond the active treatment phase is warranted and agencies will ask for it if the protocol does not include it.
Extrapolation: The Mechanism That Makes Biosimilars Commercially Viable
Extrapolation of biosimilarity from one indication to all approved indications of the reference product is one of the most powerful and most contested elements of the biosimilar regulatory framework. If a biosimilar is approved on the basis of clinical data in one indication, extrapolation allows the marketing authorization to cover other indications of the reference product without requiring separate clinical trials in each indication.
The scientific justification for extrapolation requires the developer to demonstrate that the mechanism of action is the same or sufficiently similar across extrapolated indications, that the safety and efficacy data generated are relevant to the extrapolated indications, and that the patient populations and disease contexts do not introduce unique risks not captured by the studied population.
Infliximab biosimilars provide the canonical extrapolation case. Remicade’s FDA-approved indications include rheumatoid arthritis, Crohn’s disease, ulcerative colitis, ankylosing spondylitis, psoriatic arthritis, and plaque psoriasis. Biosimilar programs typically generate clinical data in RA or Crohn’s disease, then extrapolate to the remaining indications based on shared TNF-alpha neutralization mechanism. Both the FDA and EMA have accepted this extrapolation rationale for multiple infliximab biosimilars, establishing a precedent framework that subsequent programs reference.
Extrapolation is not automatic. The developer must make the scientific case. Agencies have declined extrapolation requests where the mechanism of action varies by indication (e.g., a molecule with both immunosuppressive and direct cytotoxic mechanisms in different disease contexts) or where the patient population for the extrapolated indication is immunologically distinct in a way that raises unique immunogenicity concerns.
IP Valuation of Reference Biologic Assets: Patent Thickets, Exclusivity Stacking, and Paragraph IV Economics
Patent Thicket Architecture: How Originators Build Layered IP Protection
The term ‘patent thicket’ describes the accumulation of multiple overlapping patents surrounding a single drug product that collectively delay generic or biosimilar entry beyond the expiry of the primary composition-of-matter patent. For biologics, patent thickets are substantially more complex than in small molecules because biologics are manufactured (not synthesized), meaning the manufacturing process itself, formulation, delivery device, dosing regimen, and specific therapeutic use can each be separately patented.
AbbVie’s Humira portfolio is the most extensively studied patent thicket in biopharmaceutical history. AbbVie accumulated over 130 U.S. patents related to adalimumab, covering the antibody composition, its crystalline form, its low-viscosity high-concentration formulation (critical for the prefilled syringe device), the citrate-free formulation, the prefilled syringe device itself, and methods of treating specific conditions at specific doses. The practical effect was that even after the primary composition patent expired in December 2016, biosimilar developers could not launch the citrate-free formulation (which patients preferred, as citrate causes injection-site pain) without clearing or licensing the formulation patents.
AbbVie executed settlement agreements with every major biosimilar developer that included license grants to the patent thicket in exchange for delayed launch dates, ranging from January 2023 (Alvotech, Coherus, Samsung Bioepis) to January 2024 (other agreements). The settlements effectively extended AbbVie’s commercial exclusivity by approximately 6 years beyond the primary patent expiry in the U.S., worth an estimated $80 billion in cumulative U.S. Humira revenue during that period.
Exclusivity Stacking: The Regulatory and IP Layering Strategy
Exclusivity stacking refers to the strategic sequential or overlapping grant of regulatory exclusivities that extends the effective commercial protection period beyond any single exclusivity grant. For biologics, the toolkit includes the 12-year reference product exclusivity under BPCIA, orphan drug exclusivity (7 years in the U.S., 10 years in the EU) for a designated orphan indication, pediatric exclusivity (6-month extension of any existing exclusivity or patent protection on any listed patent upon completion of FDA-requested pediatric studies), and new formulation or manufacturing process patents that can receive additional market exclusivity if they qualify as a ‘new’ licensure rather than a supplement.
The most aggressive exclusivity stacking strategies layer orphan drug exclusivity on top of the 12-year reference product exclusivity for biologics that treat a disease affecting fewer than 200,000 U.S. patients, then use the orphan exclusivity period to conduct pediatric studies that generate a further 6-month extension. For a biologic with broad adult indications that also happens to have an orphan pediatric indication, this can extend regulatory exclusivity to 13+ years while the broader patent estate does its work.
For biosimilar developers conducting IP due diligence on a target molecule, exclusivity stacking analysis requires reviewing not just the primary BPCIA exclusivity but all supplementary grants. Tools like DrugPatentWatch allow systematic mapping of all exclusivity periods associated with an NDA or BLA number, including orphan and pediatric grants, presenting the full exclusivity profile in a queryable format that patent attorneys can use to construct an earliest-launch-date analysis.
Evergreening Tactics: A Biosimilar Developer’s Counter-Intelligence Map
Evergreening, the practice of making incremental modifications to a drug to generate new patents and extend commercial exclusivity beyond the primary patent, takes several specific forms in biologics:
Device patents are among the most effective and least-appreciated evergreening tools. AstraZeneca’s Fasenra (benralizumab), administered via a prefilled syringe or autoinjector pen, generated device-specific patents covering the prefilled accessorized injector system that outlast the antibody composition patent. A biosimilar developer seeking to compete on a patient-preferred device must either design a functionally equivalent device that does not infringe the originator’s device patents (complex) or launch with a less preferred device format while pursuing device patent challenges.
Formulation patents covering specific excipient compositions, pH ranges, or tonicity agents that improve product stability or reduce immunogenicity can block biosimilar entry even when the molecule itself is freely copyable. The citrate-free adalimumab formulation discussed above is the canonical case, but similar dynamics apply across dozens of high-value biologics.
Method-of-treatment patents covering specific dosing regimens (e.g., a specific weight-based dosing algorithm) or specific patient sub-populations (e.g., patients with a specific genetic marker) can create infringement risk for biosimilars that include these methods in their proposed label. The solution is a ‘skinny label,’ where the biosimilar label omits the patented indication or dosing method. The FDA has approved skinny labels for biosimilars where the patented use is separable from the approved biosimilar indications, but the legal risk around induced infringement in skinny-label contexts remains contested.
Biosimilar development teams should conduct patent landscape analysis at target selection, not at BLA preparation. By the time a clinical program is underway, the development investment creates sunk-cost pressure to proceed even when the patent thicket analysis should prompt reconsideration. DrugPatentWatch’s patent expiration and patent family databases allow development teams to run preliminary thicket analyses on candidate molecules within hours, flagging the number and nature of secondary patents before committing to a full IND.
Key Takeaways: IP Valuation
The IP asset value of a reference biologic cannot be summarized by its primary composition patent. Analysts and IP teams who model biosimilar market entry using only the composition patent expiry date will systematically underestimate the duration of commercial protection and the complexity of market access. The complete IP valuation requires mapping the reference product exclusivity period, every secondary patent family with potential relevance to the biosimilar program, any orphan or pediatric exclusivity grants, and any device or delivery system patents that could constrain preferred formulation development.
The Patent Dance Under BPCIA: Procedural Mechanics and Litigation Strategy
How the Patent Dance Actually Works
The BPCIA’s patent dispute resolution mechanism, colloquially the ‘patent dance,’ is one of the most complex procedural constructs in pharmaceutical law. Its mechanics are worth understanding precisely because strategic decisions made during the dance have irreversible consequences for market entry timing.
After the FDA accepts a 351(k) application for review, the biosimilar applicant must provide the reference product sponsor with a confidential copy of its application. The sponsor then has 60 days to provide a list of patents it believes could reasonably be asserted against the biosimilar, along with its contentions on infringement. The applicant responds with its own list of patents it thinks should be litigated and its non-infringement or invalidity contentions. The parties then negotiate to identify a subset of patents for immediate litigation (Phase I patents) and agree to a list of patents reserved for later litigation (Phase II patents).
For patents in Phase I, the reference product sponsor must file suit within 30 days or lose its right to sue on those patents before approval. The 30-month stay provision that operates in Paragraph IV Hatch-Waxman litigation for small molecules does not apply directly in the BPCIA context, but patent infringement suits during the pre-approval period have the practical effect of delaying biosimilar market entry.
The Supreme Court’s 2017 decision in Amgen Inc. v. Sandoz established that the patent dance information exchange is optional for the biosimilar applicant, not mandatory. A biosimilar applicant can choose not to provide its application to the reference product sponsor, bypassing the dance entirely, at the cost of potentially accelerating litigation uncertainty. In practice, most sophisticated biosimilar applicants engage the dance procedurally while making strategic choices about which patents to contest and in which forums.
Litigation Strategy: Inter Partes Review and District Court Coordination
The Patent Trial and Appeal Board (PTAB) inter partes review (IPR) mechanism allows biosimilar developers to challenge the validity of originator patents on prior art grounds through an administrative proceeding that is typically faster and less expensive than district court patent litigation. An IPR petition must be filed within one year of service of a patent infringement complaint in district court.
The coordination of IPR filings with district court litigation defense is the primary tactical challenge in biosimilar patent litigation. Developers want to use IPR to invalidate the strongest originator patents while managing estoppel risk (a losing IPR petitioner is estopped from asserting in district court any invalidity ground that was raised or could have been raised in the IPR). This requires careful selection of IPR targets and grounds.
Biosimilar developers that have executed this strategy effectively (e.g., Pfizer’s challenge to Remicade-related Janssen patents) have created paths to early market entry that bypassed settlements and avoided the drawn-out settlement negotiations that characterized the Humira biosimilar experience.
Global Regulatory Submission Architecture: eCTD, Module Structure, and Dossier Quality Control
eCTD and the Common Technical Document
All major regulatory authorities, including the FDA, EMA, Health Canada, PMDA, and TGA, now require biosimilar BLAs or MAAs to be submitted in the electronic Common Technical Document (eCTD) format. The CTD structure organizes the dossier into five modules: Module 1 (regional administrative information), Module 2 (summaries), Module 3 (quality/CMC), Module 4 (non-clinical reports), and Module 5 (clinical study reports).
For biosimilar submissions, the Module 3 quality section carries disproportionate weight relative to most new drug applications because the comparability exercise is primarily a quality event. The analytical comparability data, reference product lot information, critical quality attribute summary, and process characterization data all reside in Module 3 and are frequently the subject of detailed questions during review.
The Module 2 Quality Overall Summary (QOS) and the Overarching Biosimilarity Summary (OBS) or equivalent summary documents in biosimilar submissions are the narrative spine of the dossier. These documents must present the totality of evidence narrative in a coherent form that allows the agency reviewer to follow the scientific argument across modules. Poorly written summaries, even when the underlying data is strong, generate questions simply because the reviewer cannot efficiently navigate the evidence.
Dossier QC: The Deficiency Prevention Checklist
The most expensive regulatory outcome in biosimilar development is a Complete Response Letter (CRL) from the FDA or a Day 120 List of Questions from the EMA that requires additional data or studies. CRLs typically add 1-3 years to a program’s timeline, depending on whether they require new clinical studies. Preventing deficiency letters through rigorous pre-submission dossier quality control is the most cost-effective investment a regulatory team can make in the 12 months before submission.
A dossier QC process should include a structured cross-reference audit confirming that all data summarized in Module 2 are traceable to source reports in Modules 3-5, a method consistency audit confirming that analytical methods referenced in Module 3 are described, validated, and consistently named, a clinical-analytical consistency review confirming that the totality of evidence narrative in the clinical overview accurately represents the analytical comparability conclusions, and a regulatory readiness review where an external regulatory expert simulates agency review by attempting to identify gaps before submission.
Post-Approval Lifecycle: Pharmacovigilance, RMP/REMS, and Manufacturing Variation Management
Pharmacovigilance Requirements for Biosimilars: European Risk Management Plans and U.S. REMS
Regulatory approval triggers a post-approval pharmacovigilance obligation that runs for the commercial life of the product. For biosimilars, the pharmacovigilance challenge is more complex than for small-molecule generics because the long-term immunogenicity profile of the biosimilar must be monitored separately from the reference product. The EMA requires a Risk Management Plan (RMP) for all approved biosimilars specifying the post-approval safety monitoring commitments, including any enhanced pharmacovigilance activities (EPVAs) or post-authorization safety studies (PASS) required by the CHMP.
The FDA’s equivalent is the Risk Evaluation and Mitigation Strategy (REMS), though many biosimilars do not require a REMS unless they involve a product with a significant identified safety concern. The FDA may require biosimilar sponsors to participate in a shared REMS with the reference product sponsor, particularly for high-risk biologics.
A central challenge in biosimilar post-market surveillance is attributability in spontaneous adverse event reports. When a patient experiences a serious adverse event while on a biosimilar, the prescribing physician’s report may not reliably identify whether the product administered was the originator or the biosimilar, particularly in markets with pharmacy-level substitution. Regulatory agencies have pushed for improved biosimilar product traceability through nonproprietary naming conventions (the FDA’s biosimilar suffix system, e.g., ‘-awwb’ for the adalimumab biosimilar Hadlima) that allow adverse events to be attributed to the specific product administered.
Post-Approval Manufacturing Changes: Comparability Under ICH Q5E
Manufacturing changes are inevitable across a biosimilar’s commercial life. Process scale-up, site transfers, raw material sourcing changes, and process improvements generate post-approval variations that require regulatory filings. The regulatory pathway for post-approval manufacturing changes in biosimilars is governed by ICH Q5E (Comparability of Biotechnological/Biological Products Subject to Changes in Their Manufacturing Process) and its regional implementing guidance.
The ICH Q5E framework requires that manufacturing changes be accompanied by a comparability study comparing the pre- and post-change product across relevant quality attributes. If the comparability study confirms unchanged quality, and if the change is within the established design space, the variation may be submitted as a minor variation (EU) or as a Changes Being Effected (CBE) supplement (U.S.). Changes that affect product quality in a material way require prior approval variations (EU) or Prior Approval Supplements (PAS, U.S.) and may require clinical comparability data.
For biosimilar manufacturers, the discipline of process validation and manufacturing consistency is directly connected to the ease and cost of managing post-approval changes. A manufacturer with a well-characterized process, a robust control strategy, and a validated multivariate analytical control system will navigate post-approval variations more efficiently than a manufacturer operating close to the edge of its process understanding.
Building the Agile Regulatory Organization: Talent, Cross-Functional Integration, and Intelligence Systems
Regulatory Intelligence as a Competitive Function
Regulatory intelligence, the systematic monitoring of guidance documents, agency advisory committee meetings, court decisions, competitor submissions, and scientific literature to anticipate regulatory evolution, is the highest-leverage investment a regulatory affairs function can make outside of direct program work.
The FDA holds public advisory committee meetings for biosimilar-related policy questions that telegraph agency thinking months or years before formal guidance is issued. Biosimilar companies with staff assigned to monitor and synthesize advisory committee transcripts, FDA workshop proceedings, and public docket comments from scientific advisors consistently respond to evolving agency expectations faster than those that wait for final guidance.
EMA scientific guidelines, when published in draft form for public comment, represent an opportunity for industry input. Companies that engage the EMA’s public consultation process with well-reasoned scientific comments, supported by data, can influence final guidance language. This is not a passive observation process; it is a regulatory affairs strategy.
Cross-Functional Architecture: Embedding Regulatory Into R&D
The organizational structure that best supports biosimilar regulatory success embeds regulatory affairs personnel within the development team from preclinical IND-enabling studies through post-approval lifecycle management, rather than engaging regulatory affairs as a handoff function at the submission stage.
The practical model places a regulatory affairs lead as a core member of each biosimilar program team, participating in CMC strategy meetings where comparability study designs are being set, in clinical protocol development meetings where endpoints are selected, and in IP strategy meetings where patent landscapes are reviewed. The regulatory lead’s function in these meetings is not to approve decisions post-hoc but to surface agency perspective in real time, asking ‘how will the FDA read this design choice’ before the design is locked.
Companies that operate with this embedded model generate fewer late-cycle surprises and fewer Complete Response Letters, because the regulatory view is applied continuously rather than as a final checkpoint. The cost of embedding regulatory expertise in program teams is substantially lower than the cost of a single CRL-driven program delay.
Key Takeaways: Agile Regulatory Organization
Regulatory agility is a talent and process investment, not a budget line item that can be cut without downstream program cost. The regulatory teams that deliver the fastest biosimilar approvals are not the largest teams. They are the teams with the deepest scientific training, the most current agency intelligence, and the organizational mandate to engage program decisions at inception rather than at submission.
Investment Strategy for Analysts: Reading Regulatory Signals and Patent Data for Alpha Generation
How to Use Regulatory Milestones as Trading Signals
For institutional investors in biopharmaceuticals, biosimilar regulatory milestones generate both event-driven trading opportunities and longer-duration structural theses. The key events and their market implications are specific.
FDA acceptance of a BLA (which triggers a PDUFA date) confirms that the agency found the application sufficiently complete for review. This is a positive signal but not a guarantee of approval. Between 10-15% of accepted BLAs receive CRLs on first review, typically for CMC or clinical deficiencies identified during review. The announcement of a PDUFA date for a biosimilar BLA tells an analyst that the company cleared the administrative threshold; the stock’s implied probability of approval at that point should incorporate the product-specific and company-specific regulatory track record.
FDA advisory committee meetings for biosimilar applications signal that the agency has identified questions it wants public scientific input on, which typically indicates the agency has concerns not resolved by the standard review process. A biosimilar that goes to an advisory committee is statistically at higher risk of a CRL or approval with labeling restrictions than one that proceeds to approval without advisory committee review.
FDA interchangeable biosimilar designations, announced in approval letters, are not directly priced by the market efficiently because many analysts do not track the commercial consequences of interchangeability (pharmacy-level substitution access) versus standard biosimilar status. Stocks of companies receiving interchangeable designations for products in large markets (adalimumab, insulin) merit a positive re-rating if the product’s commercial model depends on volume-driven substitution rather than direct-to-physician selling.
Using Patent Expiration Data for Biosimilar Pipeline Valuation
The conventional approach to biosimilar pipeline valuation applies a probability-of-approval estimate (typically 70-80% for late-stage biosimilar programs with adequate analytical packages) and a market penetration curve estimate to projected reference product revenue. This approach systematically undervalues programs targeting molecules with weak secondary patent protection and overvalues programs targeting molecules with strong patent thickets.
A more precise approach layers patent expiry data from DrugPatentWatch or equivalent sources onto the basic pipeline model. For each biosimilar target, the analyst should map the primary patent expiry, the secondary patent families with remaining life (segmented by composition, formulation, device, process, and method of treatment), the reference product exclusivity period (FDA and EU), and any outstanding litigation that could either accelerate or block market entry.
Programs targeting molecules where the primary patent has expired, exclusivity has expired or is expiring within 12 months, and no material secondary patents remain should receive higher probability-of-timely-market-entry estimates than programs where a significant secondary patent thicket remains unresolved. Conversely, programs where the developer has successfully challenged or designed around key secondary patents, even before approval, should receive a premium for patent-clearance risk reduction.
Monitoring Biosimilar Market Adoption for Long-Duration Thesis Construction
The structural thesis that U.S. biosimilar adoption rates will converge toward European rates over a 5-10 year horizon depends on several policy variables: CMS reimbursement policy for Part B biosimilars (which has moved toward biosimilar payment parity), formulary transparency regulation (pending), PBM contracting reform (politically active), and physician/patient education progress. Investors with long-duration horizons should monitor leading indicators including biosimilar prescription fill rates by NDC at the pharmacy level (available through IQVIA or Symphony Health data), biosimilar formulary placement changes in the top-10 PBM formularies, and CMS finalizing interchangeable biosimilar reimbursement parity in Medicare Part D.
The adalimumab biosimilar market in the U.S., with 10+ approved competitors and a branded originator that aggressively defended formulary position, is the natural experiment that will determine whether U.S. biosimilar adoption can reach 50%+ penetration within a 3-year post-entry window. By 2025, that experiment had not yet resolved in favor of the biosimilar thesis on a volume basis, though net price competition had materially reduced adalimumab unit economics for AbbVie.
Key Takeaways by Segment
For IP Teams and Patent Counsel
The reference biologic IP landscape requires analysis across five distinct protection layers: the primary composition-of-matter patent, secondary formulation and device patents, regulatory data exclusivity and reference product exclusivity periods, orphan and pediatric exclusivity stacking, and method-of-treatment patents that drive skinny-label strategy. Managing biosimilar market entry without a complete map of all five layers is the most common source of costly surprises in biosimilar litigation.
For R&D Leads
The analytical characterization investment at the front of a biosimilar program is the most capital-efficient development expenditure available. A program with a comprehensive critical quality attribute profile, validated HDX-MS HOS data, and a rigorous fingerprint similarity matrix enters pre-IND meetings with the FDA with a scientific position that can credibly justify a streamlined clinical program. That justification, if accepted, converts an $80-120 million clinical investment into a $20-40 million comparative PK study. The mathematics of front-loading are unambiguous.
For Portfolio Managers
Biosimilar portfolio value is not additive across programs without adjustment for patent thicket exposure. Two biosimilar programs targeting molecules with identical revenue opportunities but different secondary patent landscapes carry materially different risk-adjusted values. Patent thicket analysis at the program-selection stage is not legal overhead; it is portfolio management.
For Institutional Investors
Regulatory milestones in biosimilar development are less informative as discrete events than as signals within a program’s regulatory track record. A company that has obtained two or more biosimilar approvals through efficient, CRL-free review processes has demonstrated systematic regulatory execution capability that should be assigned a premium over a single-program biosimilar developer with no prior FDA approval history. The FDA’s cumulative experience with specific companies’ regulatory teams is a real, if difficult to quantify, factor in the pace and friction of subsequent BLA reviews.
For Key Decision-Makers
The organizational decision that most determines biosimilar regulatory outcomes is whether regulatory affairs is embedded in program teams from preclinical inception or engaged as a handoff function at BLA submission. The former produces systematically better outcomes. The latter produces CRLs, program extensions, and delayed ROI. This is an organizational design choice, not a headcount question.
Frequently Asked Questions
What is the practical difference between a biosimilar and an interchangeable biosimilar in the U.S. market?
A biosimilar approved under Section 351(k) may be prescribed and dispensed as a biosimilar but requires prescriber action for substitution in most pharmacy contexts. An interchangeable biosimilar can be substituted by the pharmacist for the reference product without prescriber intervention, in states that have enacted permissive automatic substitution laws, which now includes the majority of U.S. states. The commercial consequence is that interchangeable biosimilars have access to the pharmacy-level substitution channel, which drives volume at scale in high-refill therapeutic categories like insulin and long-term immunotherapy.
How does the patent dance create market entry risk for biosimilar developers?
The BPCIA patent dance creates risk primarily through the Phase I litigation mechanism, where the reference product sponsor can file a patent infringement suit within 30 days of receiving the biosimilar’s patent list and contentions, potentially enjoining market entry during litigation. The risk is manageable through pre-suit patent invalidity analysis (including IPR petitions), design-around strategies for key formulation or device patents, and settlement negotiations that include launch date agreements. The largest risk is underestimating the secondary patent estate and entering the dance without a clear litigation strategy for each patent on the originator’s list.
What analytical methods does the FDA currently consider state-of-the-art for higher-order structure characterization?
The FDA’s 2019 guidance on analytical procedures for biosimilars identifies a suite of complementary methods as appropriate for HOS characterization. Hydrogen-deuterium exchange mass spectrometry (HDX-MS) has emerged as the most comprehensive single technique for characterizing backbone dynamics and conformational similarity. It is complemented by orthogonal techniques including circular dichroism (CD) for secondary structure, intrinsic fluorescence spectroscopy and extrinsic dye-based assays for tertiary structure, and size-exclusion chromatography with multi-angle light scattering (SEC-MALS) for quaternary structure and aggregation. For glycoproteins, site-specific glycan mapping by LC-MS is expected. Relying on CD and intrinsic fluorescence alone is no longer considered sufficient for monoclonal antibody HOS packages.
How should biosimilar developers approach scientific advice at the EMA versus FDA Type 2 meetings?
EMA scientific advice and FDA Type 2 meetings serve the same strategic purpose, obtaining agency feedback on development plan design, but they operate differently in form. EMA scientific advice is written and produced after CHMP rapporteur deliberation, typically within 70 days of the request. FDA Type 2 meetings are face-to-face (or video conference) discussions with the review division, producing meeting minutes agreed by both parties. EMA scientific advice is generally more comprehensive (covers all aspects of the dossier in a single response) while FDA Type 2 meetings are typically focused on a specific set of questions. For programs targeting both markets, simultaneous EMA scientific advice and FDA pre-IND requests covering aligned questions can generate a comparative agency perspective that identifies areas of regulatory divergence before the development program is locked.
What is the earliest date a biosimilar can launch in the U.S. market?
The earliest U.S. launch date for a biosimilar is the later of three constraints: the expiry of the 12-year reference product exclusivity period (running from the date of first FDA licensure of the reference product), the resolution of any patent disputes that have resulted in a court-ordered injunction against market entry, and the receipt of FDA final approval of the 351(k) application. A biosimilar application can be submitted after 4 years from reference product first licensure, can receive tentative approval before the 12-year exclusivity expires, but cannot receive final effective approval until the 12-year period ends (absent a successful patent challenge that unlocks earlier entry). For products where the primary patent and the 12-year exclusivity expire simultaneously or close together, the FDA approval timeline becomes the rate-limiting constraint.
How does the EU data exclusivity period interact with biosimilar market entry in Europe?
The EU 8+2 exclusivity structure means a biosimilar MAA cannot be submitted until 8 years after the reference product’s first EU marketing authorization. The biosimilar can receive approval during the 10-year market protection period (8+2) but cannot be commercialized until the full 10 years elapse. An additional 1-year market protection extension applies if the reference product sponsor obtained approval for a new indication within the first 8 years that brings significant clinical benefit. For drugs approved in Europe in the late 1990s and early 2000s (the first wave of major biologics), most EU exclusivity periods have already expired, meaning the primary constraint on European biosimilar entry is now the patent estate, not regulatory exclusivity.
References and Data Sources
All regulatory citations in this article reflect the frameworks in place as of April 2026. Specific guidance documents and legislative provisions referenced include:
- Biologics Price Competition and Innovation Act (BPCIA) of 2009, codified at 42 U.S.C. 262(k)
- FDA Guidance: Scientific Considerations in Demonstrating Biosimilarity to a Reference Product (2015, revised 2019)
- FDA Guidance: Formal Meetings Between the FDA and Biosimilar Biological Product Sponsors or Applicants (2018)
- FDA Guidance: Considerations in Demonstrating Interchangeability with a Reference Product (2019)
- EMA Guideline on Similar Biological Medicinal Products (CHMP/437/04 Rev 1)
- EMA Guideline on Similar Biological Medicinal Products Containing Monoclonal Antibodies (EMA/CHMP/BMWP/403543/2010 Rev 1)
- ICH Q5E: Comparability of Biotechnological/Biological Products Subject to Changes in Their Manufacturing Process
- Amgen Inc. v. Sandoz Inc., 137 S.Ct. 1664 (2017)
- MarketsandMarkets Biosimilars Market Report (2024 edition)
- DrugPatentWatch patent expiration and exclusivity databases
This article was prepared for informational purposes for IP teams, portfolio managers, and institutional investors in the biopharmaceutical sector. It does not constitute legal advice. Consult qualified IP counsel for Paragraph IV and patent dance strategy specific to individual programs.