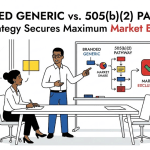
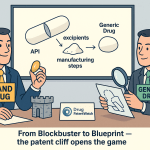
1. What a Generic Drug Actually Is, Legally and Commercially
The Regulatory Definition and Why It Is a Legal Construct, Not Just a Scientific One

A generic drug is a bioequivalent copy of an already-approved brand-name drug, the Reference Listed Drug (RLD), that contains the same active pharmaceutical ingredient (API), in the same dosage form and strength, administered by the same route, and labeled for the same indications. The FDA codifies this under 21 CFR 314.92 and its global counterparts operate on broadly similar principles. That much is well-established.
What is less appreciated is how deliberately this definition functions as a legal trigger rather than a purely scientific designation. ‘Sameness’ is not a casual term in pharmaceutical regulation. It is a precisely scoped construct that determines which approval pathway a company may use, which patents it must address, which exclusivities block it, and ultimately, when it can sell its product. Every word in that definition carries commercial weight.
The abbreviated approval pathway created by that sameness requirement is the financial engine of the entire industry. Instead of running multiphase clinical trials to prove safety and efficacy from scratch, a generic applicant cites the FDA’s prior finding on the innovator drug. The burden shifts from demonstrating clinical benefit to demonstrating scientific equivalence. This is accomplished through bioequivalence (BE) studies, which show that the generic delivers the same amount of active ingredient into systemic circulation over the same period as the brand-name drug. In theory, this removes billions of dollars in development cost. In practice, the FDA holds generic manufacturers to identical cGMP manufacturing standards, impurity limits, and analytical rigor as innovator companies. The savings are real but not unconstrained.
One persistent complexity is the gap between regulatory ‘sameness’ and patient perception. U.S. trademark law prevents a generic from replicating a brand drug’s physical appearance. This means generics can and regularly do differ in inactive ingredients, colorants, fillers, and tablet geometry. The FDA requires proof that these differences do not affect performance, but it also acknowledges receiving post-market reports from patients who perceive differences after switching from brand to generic or from one generic to another. This ‘trust deficit’ is not merely a public relations issue. It is an ongoing regulatory obligation that requires robust post-market pharmacovigilance and, in some therapeutic areas with narrow therapeutic index (NTI) drugs, specialized bioequivalence standards with tighter confidence interval limits.
IP Valuation: The RLD Designation as a Core Asset
For brand-name manufacturers, the RLD designation is itself an IP-adjacent asset, not listed in the Orange Book but operationally equivalent in strategic value. A drug loses its RLD status only when it is withdrawn from sale for reasons of safety or efficacy, a threshold the FDA applies narrowly. As long as the RLD remains listed, it anchors every generic ANDA and every bioequivalence study. Brand companies that discontinue a product for commercial rather than safety reasons can trigger an FDA ‘discontinued from sale’ finding, and the FDA will designate another listed drug as the reference standard. Brands that have tried to remove their RLD from the market to block generic development have faced legal challenges and FDA policy pushback. The RLD listing, in short, is an asset that the innovator cannot simply take off the table.
For generic companies, understanding which product holds RLD status and whether that product is actually available for procurement for reference-standard BE studies is a genuine operational risk. Several developers have lost months of program time when the brand company restricted sample availability through Risk Evaluation and Mitigation Strategy (REMS) programs. Teva, Amneal, and others have successfully sued to compel sample access, establishing that REMS programs cannot be weaponized to block BE study procurement. That litigation created useful precedent, but it adds legal cost to what should be a straightforward R&D step.
Key Takeaways: Section 1
The generic drug’s legal definition is the foundation of every downstream regulatory, IP, and commercial decision. The RLD designation is not inert background information. It governs which products are valid reference standards, which exclusivities apply, and whether REMS-related access restrictions can delay a development program. Generic teams that treat this as administrative boilerplate rather than strategic terrain consistently underestimate the first source of competitive differentiation: knowing which exact product to reference, in which market, at which time.
2. The Global Market: $487 Billion, Thinning Margins, and a Supply Chain Under Siege
Market Scale and the Affordability Paradox
The global generic drug market reached approximately $487 billion in 2024 and is on a trajectory toward $816 billion by 2034, driven by a wave of compound patent expirations on high-revenue biologics and small molecules, demographic pressure from aging populations with chronic disease burdens, and sustained government pressure to reduce pharmaceutical expenditure. These are structural tailwinds that no near-term policy headwind is likely to fully reverse.
In the United States, the numbers are equally arresting. Generic medicines represent more than 90% of all prescriptions dispensed but only 17.5% of total prescription drug spending. The Association for Accessible Medicines (AAM) reported $408 billion in documented savings to the U.S. healthcare system in 2022 alone, with cumulative decade-long savings exceeding $2.9 trillion. These figures recur in every policy debate about drug pricing, and they should. They are the strongest argument for the existence of the generic model.
The paradox embedded in that success, however, is structural and intensifying. The competitive dynamics that generate those savings also destroy the financial conditions under which they can be sustained. When eight or ten generic manufacturers enter the market for the same small-molecule oral tablet, average selling prices can fall 90% or more within 12 to 18 months of launch. Profit margins compress to single digits. Contract manufacturing costs, API procurement, packaging, and quality systems still have to be paid for. The resulting economics disincentivize continued investment in manufacturing capacity and, critically, in the production of lower-volume but medically essential generic drugs.
David Gaugh, who served as Interim President and CEO of the AAM, described the situation plainly: the sustainability of the industry remains fragile. That is a carefully worded warning from a trade group whose job is to promote the generic sector. It deserves to be taken seriously.
Drug Shortages: The Commercial Consequence of Price Erosion
The most visible downstream effect of sustained price erosion is the drug shortage crisis. As of 2024, the FDA’s shortage list routinely included hundreds of products, with injectable generics, oncology supportive care agents, and anesthetics consistently among the most affected categories. The causes are systemic. When a manufacturer’s margin on a generic injectable falls below the cost of maintaining FDA-compliant manufacturing infrastructure, the rational response is to exit the market. When enough manufacturers exit, shortage follows.
The 2023 shortage of amoxicillin suspension, a drug that has been off-patent for decades, illustrated this dynamic precisely. It is not a failure of innovation but of economic sustainability. The FDA’s Drug Shortage Staff (DSS) has limited tools to compel continued production. It can expedite inspections, facilitate alternative supplier approvals, and issue shortage guidance to prioritize distribution. It cannot force a manufacturer to stay in a market where it loses money on every unit sold.
The 2025 tariff environment introduced additional volatility. Proposed pharmaceutical tariffs from the Trump administration’s executive orders targeted active ingredients manufactured outside the United States, with particular exposure for India and China, which together supply the majority of API volume for U.S. generic products. Industry analysts at IQVIA estimated that tariffs at proposed levels would add between $7 billion and $14 billion annually to U.S. generic drug costs, a figure that would flow either to higher consumer prices, further manufacturer consolidation, or both. The precise tariff structure remained in regulatory flux through mid-2025, but the directional pressure on supply chain economics is clear.
The Consolidation Response and Its IP Implications
The generic industry has responded to margin pressure through sustained M&A activity. Teva’s acquisition of Allergan Generics for $40.5 billion in 2016, Mylan’s merger with Pfizer’s Upjohn division to form Viatris in 2020, and smaller bolt-on acquisitions by Sun Pharma, Aurobindo, and Hikma have progressively concentrated market power in fewer hands. In this context, IP portfolio valuation has become a critical input to deal economics, not a secondary diligence consideration.
When Viatris was formed, its combined ANDA portfolio of over 1,400 approved applications and its pipeline of complex generics under development were the central IP assets underwriting the merger’s strategic rationale. The ANDA itself, as a regulatory authorization, has a quantifiable asset value: it represents the right to sell a product in the world’s largest pharmaceutical market, protected from new competition through FDA review timelines, and potentially through 180-day exclusivity if a Paragraph IV challenge was successful. Portfolio managers evaluating generic company M&A need to understand ANDA valuation methodology, patent expiry schedules on remaining brand competition, and the quality of the pipeline ANDA filings as development-stage assets.
Investment Strategy: Global Generic Market Positioning
For institutional investors, the generic drug market in 2025 presents a bifurcated opportunity set. The commodity end of the market, simple oral small-molecule generics with multiple competitors, is a volume and cost-efficiency play. Margin expansion is limited; competitive moats are narrow. The more defensible investment thesis lies in companies that have built capabilities in complex generics (transdermal patches, inhaled products, injectable liposomes, drug-device combinations) and biosimilars, where development barriers are higher, approved competitor counts are lower, and pricing holds longer. Companies with established pre-ANDA meeting track records at FDA’s Office of Generic Drugs (OGD), proprietary in vitro testing capabilities for locally acting drugs, and demonstrated Quality by Design (QbD) implementation are better positioned to defend margins in a consolidating market.
Key Takeaways: Section 2
The generic market’s growth trajectory is real, but margin sustainability is not guaranteed. Price erosion, API supply chain vulnerability, tariff exposure on imported ingredients, and shortage-driven regulatory scrutiny are converging pressures. Companies that treat these as operational challenges rather than strategic ones will underinvest in the quality infrastructure and IP capabilities that determine long-term competitive position. The shortage crisis and the tariff debate are both symptoms of the same underlying problem: a market structure that prices generics below the true cost of sustainable, high-quality domestic production.
3. The U.S. Regulatory Gauntlet: Mastering the FDA ANDA Pathway
The Hatch-Waxman Act: A Litigation Framework Disguised as a Regulatory Statute
The Drug Price Competition and Patent Term Restoration Act of 1984, universally referenced as the Hatch-Waxman Act, did not merely create an abbreviated approval pathway for generic drugs. It created a structured legal ecosystem in which patent litigation is the intended and primary mechanism for determining when a generic may enter the market before all brand patents expire. This is the single most important conceptual point for any regulatory or legal team working in the U.S. generic space.
The ‘grand bargain’ the Act struck gave generic manufacturers the Abbreviated New Drug Application (ANDA) pathway, allowing reliance on an innovator’s prior clinical findings, and a ‘safe harbor’ provision permitting bioequivalence testing during the patent term without triggering infringement liability. In exchange, brand companies received patent term restoration (up to five years of patent life lost to FDA review) and several periods of marketing exclusivity tied to the novelty of their clinical data.
The numbers on the Act’s impact are definitive. Generic prescription share in the U.S. stood at roughly 19% in 1984. It now exceeds 90%. That shift is almost entirely attributable to Hatch-Waxman’s approval pathway. But the litigation machinery embedded in the Act is where the real strategic action occurs, and where most regulatory teams still underweight their preparation.
Patent Term Restoration: The IP Valuation Mechanics
Patent term restoration under 35 U.S.C. 156 allows a brand company to apply to the USPTO for restoration of patent life lost to FDA regulatory review, up to a five-year extension. The maximum total patent term with restoration is 14 years from product approval. For high-revenue compounds, this extension can be worth billions of dollars in protected market exclusivity, making it a primary IP asset to model in any competitive entry timeline.
The calculation is specific: the restoration period equals half the time spent in clinical development plus the full time spent in FDA review, minus any period where the applicant did not act with due diligence. A drug that spent four years in Phase II and III trials and two years in FDA review could, in principle, recover four years of patent life (two years for the clinical half plus two years for the full regulatory period). This restoration applies to only one patent per product, and the patent holder must apply within 60 days of product approval. For generic teams assessing a target drug’s true patent expiry date, the restoration-adjusted term, not the nominal patent filing date, is the number that matters.
Deconstructing the ANDA: What the Application Actually Requires
The ANDA, governed under 21 CFR Part 314 Subpart C, requires a comprehensive body of evidence across four primary domains.
Pharmaceutical equivalence data must show that the generic contains the same API at the same strength, in the same dosage form, delivered by the same route. This sounds straightforward. For drugs with complex salt forms, polymorphic API variants, or combination products, it is not.
Bioequivalence data, discussed in depth in Section 5, must demonstrate through in vivo pharmacokinetic studies or acceptable alternatives that the generic delivers the same systemic drug exposure as the RLD. The FDA publishes Product-Specific Guidances (PSGs) specifying exactly what study design it expects for each drug.
Chemistry, Manufacturing, and Controls (CMC) data is the largest and most technically demanding section of a typical ANDA. It encompasses the characterization of the API (including identification of all process impurities and degradation products), the formulation, the manufacturing process, analytical method validation, container-closure system testing, and the stability data demonstrating the product’s shelf life under defined storage conditions. The Drug Master File (DMF) submitted by the API supplier is referenced by the ANDA and reviewed in parallel. A deficient DMF stops the ANDA.
Labeling must be identical to the RLD’s FDA-approved labeling, with only narrow permissible differences: the generic’s own manufacturer name and contact information, and any carve-outs of patented indications (the ‘skinny label’ strategy, discussed in Section 6). The FDA’s labeling review is more granular than most teams expect. Formatting, section ordering, and even specific clinical pharmacology language must track the RLD label precisely.
The ANDA Review Lifecycle: Filing to Approval
Once submitted, the ANDA undergoes a filing review within 60 days. A Refuse-to-Receive (RTR) letter issues if the application is not substantially complete. RTR grounds include missing or incorrect FDA forms, inadequate patent certifications, failure to comply with eCTD electronic submission standards, and incomplete bioequivalence data packages. These are largely preventable errors, but the FDA’s 2024 and 2025 monthly statistical reports continue to show RTR rates in the mid-single-digit percentage range, indicating that submission quality problems persist across the industry.
If accepted for review, the ANDA proceeds through discipline-specific review cycles covering bioequivalence, chemistry, labeling, and manufacturing facility inspection. The FDA issues Information Requests (IRs) and Discipline Review Letters (DRLs) throughout this process. Under GDUFA III performance goals, the standard first-cycle review goal is 10 months for original ANDAs. In practice, the average number of review cycles for approval has historically exceeded one, with complex products often requiring two or three cycles. Each additional cycle adds six to ten months of review time.
A Complete Response Letter (CRL) issues when the FDA identifies deficiencies that preclude approval. The CRL must be addressed by amending the ANDA with the requested data or argumentation, and the amendment restarts a review clock. The FDA has committed under GDUFA III to specific review timelines for amendments categorized by workload impact. Tier 1 amendments (minor changes) receive a six-month review goal. Tier 2 (moderate) receive a ten-month goal. Major amendments may be treated as new cycles with extended timelines.
IP Valuation: The ANDA as a Regulatory Asset
An approved ANDA is a licensable, transferable, and acquirable regulatory asset with a quantifiable market value. Buyers and sellers of ANDA portfolios use several valuation frameworks. The most common is a risk-adjusted net present value (rNPV) model that discounts projected revenue (product of volume, price, and market share assumptions) by the probability of maintaining approval and by the patent and exclusivity risk that might block commercial launch.
Pending ANDAs with first-to-file Paragraph IV status carry a significant premium over later-filed ANDAs for the same product, because the 180-day exclusivity period creates a temporary duopoly that supports materially higher pricing. For blockbuster drugs, the NPV of 180-day exclusivity alone has been estimated in the hundreds of millions of dollars. Teva’s 2011 generic launch of atorvastatin (Lipitor) is the canonical example. Teva held first-to-file status and earned an estimated $600 million to $1 billion in its 180-day exclusivity period, before the market moved to multi-generic competition and prices collapsed.
For M&A diligence, ANDA portfolio valuation requires assessing not just the number of approved applications but their commercial quality: the patent expiry schedule on remaining brand protection, the number of existing generic competitors already in the market, the product’s price trajectory under multi-generic competition, and the regulatory maintenance burden (ongoing stability testing, annual reports, potential post-approval change supplements). A portfolio of 50 approved ANDAs in highly competed therapeutic categories with 12 or more competitors per product may have lower intrinsic value than a portfolio of 15 complex generic ANDAs with only one or two competitors each.
Common ANDA Deficiencies: Where Programs Break Down
The FDA’s Office of Generic Drugs (OGD) has published data on the leading causes of CRLs and delayed approvals. Data integrity issues topped the list in a 2025 FDA analysis, accounting for 75% of ANDAs that missed their GDUFA goal date by more than 60 days. The FDA defines data integrity failures broadly: they include falsification of bioequivalence study records, inconsistent analytical data across batches, unresolved discrepancies between raw and reported data, and inadequate audit trails in electronic data systems. The agency has shown particular focus on data generated by contract research organizations (CROs) conducting bioequivalence studies, where oversight and auditing responsibilities rest with the ANDA sponsor, not the CRO.
CMC deficiencies consistently appear as the second major category. The most frequent involve inadequate process validation (particularly for products with complex manufacturing steps like wet granulation, lyophilization, or sterile fill-finish), insufficient impurity characterization against ICH Q3A/Q3B thresholds, incomplete analytical method validation per ICH Q2(R1), and failures during FDA pre-approval inspection (PAI) of manufacturing facilities. A single 483 observation at the manufacturing site during a PAI can generate a CRL even when the chemistry data package is otherwise complete.
Bioequivalence study failures round out the major deficiency categories. These range from study design problems (wrong fed/fasted conditions, incorrect sampling schedule, inadequate washout period) to statistical analysis errors (incorrect mixed-effects model specification, failure to apply reference-scaled average bioequivalence for highly variable drugs) to analytical issues in the bioanalytical method used to measure drug concentrations in plasma.
The most expensive type of CRL is one that requires a new in vivo BE study, because that typically adds 12 to 24 months and $2 million to $5 million to the development timeline. The most avoidable type is the RTR, which addresses formatting, form completion, and submission standard compliance. The industry’s continued rate of preventable RTRs reflects under-investment in submission quality systems, not scientific complexity.
Key Takeaways: Section 3
The ANDA pathway is not just a scientific hurdle but a litigation system, a financial asset class, and an operational discipline. Companies that treat it as purely scientific get CRLs. Companies that treat it as purely legal miss the CMC and data integrity traps that stop programs before they reach the patent fight. The most successful ANDA programs run regulatory, legal, CMC, and commercial functions in parallel from product selection through launch. Patent term restoration, first-to-file Paragraph IV status, and the ANDA’s transferable asset value are all material inputs to portfolio economics that should appear in business case models, not footnotes.
4. The European Framework: Multi-Track Market Access as a Commercial Strategy
The EMA’s Approval Pathways for Generic Medicines
The European Medicines Agency (EMA) does not offer a single pathway equivalent to the FDA’s ANDA. It offers a structured menu of options, each with distinct timelines, risk profiles, market coverage, and cost structures. Selecting among them is a commercial strategy decision that requires input from market access, pricing, regulatory, and supply chain functions simultaneously. Regulatory teams that make this choice without commercial alignment routinely produce the wrong answer.
The Centralised Procedure (CP) submits a single dossier directly to the EMA. The Committee for Medicinal Products for Human Use (CHMP) performs a scientific review over a statutory 210-day clock (not including ‘clock stops’ for applicant questions). A positive CHMP opinion leads to a European Commission decision granting a Marketing Authorisation valid in all 27 EU member states and the three European Economic Area (EEA) countries. The CP is mandatory for certain innovator categories and is available, though not mandatory, for generics of CP-approved drugs.
The Decentralised Procedure (DCP) is the most commonly used pathway for generics. The applicant submits an identical dossier simultaneously to the competent authorities of multiple chosen member states. One country is designated the Reference Member State (RMS), which leads the scientific assessment and prepares an assessment report. The remaining Concerned Member States (CMSs) review that report and raise objections during a defined coordination phase. If consensus is reached, each country issues a national Marketing Authorisation. If disagreements arise, a coordination group referral process applies.
The Mutual Recognition Procedure (MRP) starts from an existing national Marketing Authorisation in one member state, which then requests recognition in additional countries. This is typically used for products already marketed in one EU market seeking expansion.
The National Procedure produces a Marketing Authorisation in only a single member state and is most commonly used for products with very limited EU market scope.
The ‘8+2+1’ EU Data and Market Exclusivity Formula
Understanding the EU exclusivity framework precisely is the prerequisite for knowing when a generic dossier can be submitted and when the product can actually enter the market. The formula, colloquially called ‘8+2+1’, works as follows.
The innovator has eight years of data exclusivity from the date of the first EU marketing authorization. During this period, a generic company may not file its marketing authorization application relying on the innovator’s clinical data, even as a reference.
The innovator then has two additional years of market exclusivity, for a total of ten years of protected market. A generic may receive approval after the eight-year data exclusivity period expires but cannot sell the product until the ten-year market exclusivity has passed.
A one-year extension of market exclusivity applies if, within the first eight years, the innovator gains a marketing authorization for a new therapeutic indication that represents a ‘significant clinical benefit.’ This brings the potential protected period to eleven years.
The practical implication for generic development timelines is significant. Under the U.S. system, a generic manufacturer can file an ANDA at any time (though approval is blocked by exclusivities), and the Paragraph IV mechanism allows litigation to resolve patent disputes before exclusivity expires. Under the EU system, the generic cannot even submit its dossier until the eight-year data exclusivity expires. There is no EU equivalent of the Paragraph IV challenge that allows early filing and litigation-driven entry. Generic entry in Europe is therefore more predictable in timing but offers no analog to the 180-day exclusivity reward that makes U.S. Paragraph IV challenges so valuable.
Strategic Pathway Selection: The Commercial Decision Behind the Regulatory Choice
The CP is the fastest theoretical route to the broadest market, a single CHMP opinion covering 30 countries. For a generic of a high-volume blockbuster approved via the CP, this can maximize first-mover advantage in a multi-country simultaneous launch. The risk is binary: a negative CHMP opinion forecloses the entire EU market in a single decision. For companies with limited regulatory resources or products with heterogeneous market potential across member states, this concentration of risk is a real concern.
The DCP provides a lower-risk but more operationally complex alternative. Targeting a first wave of RMS and CMS countries with favorable regulatory track records, efficient national procedures, and strong reimbursement environments (Germany, the Netherlands, and the Nordic countries are frequently chosen) allows a company to sequence its market entry. The product generates revenue in early-launch markets while broader EU coverage is built through subsequent MRP applications. This phased approach also aligns better with supply chain buildout, which rarely supports a simultaneous 27-country launch.
What makes this strategic calculation genuinely difficult is the EU’s fragmented pricing and reimbursement landscape. Germany operates under the AMNOG reference pricing system, which applies mandatory price reductions after a benefit assessment. France negotiates prices with the Comite Economique des Produits de Sante. Spain operates a national formulary with regional variation. Italy has a multi-tier formulary with negotiations at both national and regional levels. A generic authorized via the CP but unable to secure reimbursement in three or four of the largest EU markets has paid for CP-wide approval without capturing CP-wide revenue. This misalignment between regulatory and commercial strategy is common and expensive.
FDA vs. EMA: A Strategic Comparison
| Feature | FDA (U.S.) | EMA (EU) | Strategic Implication |
|---|---|---|---|
| Application Type | ANDA | MA via CP, DCP, or MRP | EU multi-track enables phased or broad entry strategies |
| Legal Basis | Hatch-Waxman Act (1984) | Directive 2001/83/EC | U.S. system is structurally designed to produce patent litigation |
| BE Standard | 90% CI for Cmax and AUC within 80.00-125.00% | Same for AUC; Cmax interval may be widened for highly variable drugs under RSABE | Standards are harmonized enough to support single global BE programs for most products |
| Data Exclusivity | 5 years (NCE), 3 years (new clinical studies) | 8 years | EU provides a longer, fixed protection window; generic submission timing is more predictable |
| Market Exclusivity | 180-day exclusivity for first P-IV challenger | 2 years after 8-year data exclusivity (extendable to 3 years with new indication) | U.S. rewards litigation risk-taking with duopoly pricing; EU provides fixed non-litigation protection |
| Submission Timeline | GDUFA goal: 10 months first cycle; multiple cycles common | CP: 210 days statutory (excl. clock stops) | EMA CP timeline is often more predictable; FDA timelines are subject to review cycle variability |
| User Fees | GDUFA fees: ANDA submission, DMF, facility, and program participation fees | EMA fees for CP scientific assessment | GDUFA fees represent a significant entry barrier for smaller companies and niche products |
| Labeling | ‘Same as’ RLD; skinny label carve-outs permitted for off-patent indications | Consistent with RLD Summary of Product Characteristics (SmPC); carve-outs permitted | GSK v. Teva has added U.S. inducement liability risk to skinny labels not yet replicated in EU case law |
| Post-Approval Changes | Major (PAS), Moderate (CBE), Minor (Annual Report) | Type IA (minor, do-and-tell), Type IB (minor, tell-and-do), Type II (major, prior approval) | Both systems are risk-tiered, but specific classification criteria and timelines differ |
| Parallel Scientific Advice | Pre-ANDA meeting program (GDUFA II/III) | FDA/EMA Parallel Scientific Advice program for complex generics | Joint advice allows a single interaction to align both agencies on complex development questions |
The FDA/EMA Parallel Scientific Advice program for complex generics, formally launched in 2019, is an underused tool. It allows developers of difficult products such as orally inhaled products, locally acting topicals, and complex injectables to present their development plan to both agencies simultaneously and receive coordinated feedback. For companies building global complex generic pipelines, one well-prepared parallel advice session can eliminate redundant development work and reduce total global program cost by 20% to 40%.
Key Takeaways: Section 4
The EU regulatory pathway choice is a commercial and operational strategy decision that must involve market access and supply chain functions, not just regulatory affairs. The ‘8+2+1’ data and market exclusivity formula provides precise, litigation-free timelines that should anchor all EU launch planning. The FDA/EMA Parallel Scientific Advice program is a material cost reduction tool for complex generic developers that most companies underutilize.
5. The Science of Sameness: Bioequivalence for Simple and Complex Generics
Standard Bioequivalence: The Pharmacokinetic Framework
Bioequivalence establishes, through in vivo pharmacokinetic measurement, that a generic drug product delivers the same systemic exposure as the RLD. The FDA’s statutory definition in 21 CFR 320.1(e) requires an ‘absence of a significant difference in the rate and extent to which the active ingredient becomes available at the site of drug action.’ For most systemically acting drugs, the site of action is pharmacologically distal from the gastrointestinal tract, and systemic plasma concentration is an acceptable surrogate for drug availability at the site of action.
The standard BE study uses a two-period, two-sequence, crossover design in a panel of healthy adult volunteers. Volunteers receive either the test generic or the reference brand in one period and cross over to the alternative in the second period, separated by a washout interval sufficient to eliminate residual drug from the first period (typically five or more half-lives). Plasma samples are collected at specified intervals and analyzed for drug concentration using a validated bioanalytical method, typically LC-MS/MS. From the concentration-time profiles, two primary pharmacokinetic endpoints are derived:
Cmax, the peak plasma concentration, quantifies the rate of absorption. AUC(0-t) and AUC(0-inf), the area under the concentration-time curve to the last measured time point and extrapolated to infinity, quantify the total extent of systemic drug exposure.
The regulatory acceptance criterion requires that the 90% confidence interval for the geometric mean ratio (Test/Reference) for each endpoint falls entirely within the predefined bounds of 80.00% to 125.00%. This is not a 20% margin of error, as it is sometimes mischaracterized. The logarithmic transformation of the data means that 80-125% represents roughly plus or minus 22% around the geometric mean ratio of 1.00 on the log scale, and the confidence interval constraint requires that the ratio is close to 1.00 with high statistical confidence. Products meeting this criterion are expected to produce clinical outcomes equivalent to the RLD.
Product-Specific Guidances: The Double-Edged Tool
The FDA publishes PSGs for hundreds of drugs under its GDUFA commitments, specifying recommended BE study design, statistical approach, waiver eligibility for lower strengths, and supplemental in vitro requirements for specific products. PSGs are, in principle, the most efficient pathway to BE study design certainty. In practice, they have become a double-edged tool for the generic industry.
When a PSG exists and is current, it provides a clear and predictable development roadmap. When no PSG exists, developers must rely on FDA’s general BE guidance, published scientific literature, and formal FDA interaction through Controlled Correspondence or pre-ANDA meetings to reach the same clarity. When a PSG exists but is revised during development, companies that designed their studies to the old guidance may face the choice between costly redesign and the risk of a CRL under the new standard.
The FDA issued over 500 new or revised PSGs in 2019 and 2020 under GDUFA II-era commitments. The pace slowed materially in 2023 and 2024, a development that Amarex Clinical Research and other regulatory consultancies flagged as creating development uncertainty particularly for complex products where PSG guidance is most needed. For regulatory intelligence teams, tracking PSG publication and revision activity is not an occasional literature review. It is a continuous monitoring function with direct program risk implications.
ICH M13A: Global BE Harmonization for Oral Solids
In October 2024, the FDA adopted ICH M13A, a harmonized guideline on bioequivalence for immediate-release solid oral dosage forms. M13A introduces global alignment on several BE principles, including criteria for waiving in vivo BE studies for lower strengths of a product when higher strength BE data are available (strength waivers), and alignment on the use of in vitro dissolution data as a surrogate for in vivo BE (the biopharmaceutics classification system, or BCS, waiver). For regulatory teams managing multi-market submissions, ICH M13A meaningfully reduces the possibility of having to design country-specific BE studies for the same product. A single, well-designed BE program aligned with M13A should, for most BCS Class I and III immediate-release solid oral products, support simultaneous ANDA and EMA submissions without protocol modification.
The Reference-Scaled Average Bioequivalence Framework for Highly Variable Drugs
Certain drugs exhibit high within-subject pharmacokinetic variability, defined as an intra-subject coefficient of variation (CV) exceeding 30% for Cmax or AUC. For these highly variable drugs (HVDs), the standard 90% CI/80-125% acceptance criterion is scientifically inappropriate because it would require an unrealistically large sample size to achieve the statistical power needed for approval, or would fail despite the drug being therapeutically equivalent.
Both the FDA and EMA accept reference-scaled average bioequivalence (RSABE) for HVDs. Under RSABE, the acceptance criterion scales with the variability of the reference product. If the reference Cmax CV is high enough, the effective acceptance limits for Cmax can widen, potentially to 69.84% to 143.19% at the maximum. The EMA applies the RSABE approach only to Cmax when AUC is not highly variable, while the FDA applies it to both Cmax and AUC independently depending on each parameter’s variability.
The strategic implication for generic developers is that HVD classification of a target drug requires advance analysis of published PK data for the reference product to estimate within-subject variability. This analysis should happen during target selection and development planning, not after a BE study has already been designed and initiated. RSABE designs require a replicate crossover design (each subject receives the reference product twice across four periods), which increases study size and duration but reduces the risk of a false failure.
Complex Generics: Where Standard BE Fails
The FDA defines complex generics as products with complex drug substances, complex formulations, complex routes of delivery, or complex drug-device combinations. None of these categories are amenable to standard blood-level BE studies alone, and many require fundamentally different approaches to demonstrating therapeutic equivalence.
Complex Formulations: Liposomes, Emulsions, and Microspheres
Liposomal drug products present a unique characterization challenge because the pharmacological activity of the encapsulated API depends critically on the physical characteristics of the lipid bilayer: vesicle size distribution, encapsulation efficiency, drug release rate, and membrane fluidity. These structural properties determine the product’s pharmacokinetic behavior, its biodistribution to target tissues, and its tolerability profile. Standard BE between a generic liposome and the reference liposome requires not just equivalence in plasma concentration but equivalence in structural attributes that govern release kinetics.
The FDA’s PSG for liposomal doxorubicin (the generic equivalent of Doxil) requires characterization of lipid composition, particle size, zeta potential, in vitro drug release, and drug-to-lipid ratio, in addition to standard PK endpoints. This is effectively a partial-characterization approach that attempts to ensure the generic liposome has the structural attributes necessary to reproduce the clinical behavior of the reference. Developing these analytical methods and demonstrating comparability within acceptable bounds requires specialized equipment and expertise not commonly found in standard generic formulation labs.
Locally Acting Drug Products: The Absence of a Systemic PK Surrogate
For topical dermatological products, ophthalmic solutions, intranasally administered drugs, and orally inhaled products, the site of drug action is local tissue, not systemic circulation. Measuring plasma drug concentration after application of a topical cream or inhalation of a respiratory product provides no pharmacologically relevant information about drug availability at the mucosa, skin, or airway epithelium. Standard PK BE is therefore scientifically inapplicable.
The FDA has developed a toolbox of alternative equivalence approaches for these products.
In vitro release testing (IVRT) uses a membrane diffusion cell system (typically Franz cell apparatus) to measure the rate of drug release from a topical formulation under standardized conditions. IVRT is sensitive to formulation differences that could affect drug release from the vehicle. The FDA accepts IVRT as an element of the equivalence evidence package for many topical products but rarely accepts it as the sole equivalence demonstration.
In vitro permeation testing (IVPT) uses human cadaver skin or other membrane models as the diffusion barrier to measure drug permeation through the skin under conditions approximating in vivo application. The FDA’s 2022 IVPT draft guidance provided updated methodology standards, including use of flow-through diffusion cells and quantitative method validation requirements. IVPT using human skin is closer to a clinical measurement than IVRT but still falls short of direct pharmacodynamic or clinical endpoint data.
Pharmacodynamic (PD) studies use a measurable biological response as a surrogate for drug activity at the site of action. For topical corticosteroids, the vasoconstriction assay (skin blanching test) is the established PD surrogate accepted by both FDA and EMA. The test subject applies the test or reference corticosteroid to defined skin areas and the degree of skin blanching is measured chromametrically as a proxy for local glucocorticoid receptor activation. This approach works well for the vasoconstriction-competent corticosteroid class but has limited applicability to other topical drug categories.
Comparative clinical endpoint studies, in which patients are randomized to test generic or reference brand and evaluated on a clinical outcome measure (reduction in lesion count, symptom score improvement), are the most direct form of equivalence evidence but also the most expensive, slowest, and statistically least sensitive. A clinical endpoint study for a topical acne treatment typically requires 600 to 1,200 patients across 8 to 12 weeks, at a cost of $20 million to $50 million, and the study’s power to detect formulation differences that are smaller than clinically relevant depends on having a sufficiently sensitive primary endpoint. The FDA strongly prefers to avoid requiring these studies and funds regulatory science research specifically aimed at developing validated in vitro alternatives.
Orally Inhaled Products: The Drug-Device Interaction Problem
Metered-dose inhalers (MDIs), dry powder inhalers (DPIs), and nebulized inhalation solutions combine a pharmaceutical formulation with a drug delivery device in which device performance and patient interface characteristics are co-determinants of drug delivery. A generic MDI with a bioequivalent formulation but a different actuator, canister geometry, or valve configuration will deliver a different aerosol particle size distribution with potentially different lung deposition, even if the nominal dose per actuation is identical.
The FDA’s current approach to orally inhaled product BE requires a weight-of-evidence package that includes in vitro aerodynamic particle size distribution (APSD) comparisons across multiple flow rates and actuation conditions, extracted actuation profile comparisons, in vitro dose uniformity data, and device characteristic comparisons. For MDIs, the FDA also expects in vivo BE data through lung deposition studies using gamma scintigraphy or pharmacokinetic studies, though the specific study design depends on whether the drug is locally or systemically active.
The development cost of a complex orally inhaled generic is substantially higher than a simple oral tablet ANDA. Total development costs, including device engineering, analytical method development, and in vivo studies, routinely reach $30 million to $100 million per product, closer to a 505(b)(2) new drug application than a traditional ANDA. This creates a high barrier to entry that supports more durable pricing and smaller competitor counts, which is precisely why players like Mylan (now Viatris), Teva, and Cipla have invested heavily in respiratory complex generic capabilities.
Physiologically Based Pharmacokinetic Modeling as Regulatory Evidence
Physiologically Based Pharmacokinetic (PBPK) modeling integrates drug-specific physicochemical properties (solubility, permeability, protein binding, metabolic clearance) with anatomical and physiological parameters (tissue volumes, blood flow rates, enzyme expression) to simulate drug absorption, distribution, metabolism, and elimination in silico. The FDA has accepted PBPK modeling as supportive evidence for a growing range of regulatory decisions, including drug interaction labeling, dose adjustments in renal and hepatic impairment, and pediatric extrapolation.
For complex generics, the FDA has accepted PBPK modeling as a component of the equivalence evidence package for certain topically applied and inhaled products where direct clinical measurement is impractical. A well-validated PBPK model for a transdermal product, for example, can predict local skin drug concentrations from formulation properties such as drug solubility in the vehicle, vehicle-skin partition coefficients, and skin diffusivity parameters. If the model predicts equivalent local drug concentrations for the test and reference formulations, and the model has been validated against available PK data, this constitutes meaningful mechanistic evidence in support of equivalence.
The FDA’s use of PBPK in complex generic approvals remains selective and case-by-case. Regulatory teams should not treat PBPK modeling as a substitute for robust in vitro data or, where needed, in vivo data. It is most powerful as a mechanistic bridge that makes sense of the totality of a diverse equivalence evidence package and that allows sponsors to justify waiving certain studies based on mechanistic reasoning rather than empirical precedent.
IP Valuation: Complex Generic Development as a Patent-Creating Activity
Complex generic development does more than create an ANDA. It often generates patentable improvements in manufacturing, analytical methods, device components, or formulation approaches. These can be filed as patents in their own right, creating an IP estate that has value independent of the ANDA. A generic company that develops a novel in vitro permeation testing method for topical products, for example, owns that method and can license it, use it defensively to demonstrate non-infringement of brand patents on testing methodology, or use it offensively against biosimilar competitors who use inferior methods.
The strategic implications are significant. Companies investing in complex generic development should have a deliberate IP capture process running in parallel with regulatory development. Every novel analytical method, every non-obvious formulation innovation, and every device improvement should be evaluated by IP counsel for patentability. The resulting patent portfolio increases asset valuation in M&A contexts and creates licensing revenue potential. Teva, Perrigo, and Mylan all maintain substantial patent portfolios derived from generic development activities, portfolios that provide defensive value against brand company infringement suits and offensive value in cross-licensing negotiations.
Key Takeaways: Section 5
BE for standard oral generics is a well-mapped scientific process, but one where ICH M13A harmonization now offers material multi-market study consolidation opportunities. For complex generics, the regulatory equivalence standard is product-specific, methodology-dependent, and frequently higher cost than the brand-equivalent NDA that preceded it. PBPK modeling, IVRT, IVPT, and PD studies are not alternatives to choose among freely. They are complementary layers of evidence, and the FDA’s expectation for each product is specified in its PSG, or must be established through pre-ANDA engagement when no PSG exists. RSABE for HVDs is a technical area that must be assessed during target selection, not during study design. Complex generic development generates patentable innovations that should be systematically captured by IP counsel.
6. The Patent Battlefield: Paragraph IV, Evergreening, and the IP Endgame
The Paragraph IV Certification: Mechanics and Strategic Logic
When a generic applicant prepares to file an ANDA for a drug with unexpired patents listed in the FDA’s Orange Book (the FDA’s ‘Approved Drug Products with Therapeutic Equivalence Evaluations’), it must certify its position with respect to each listed patent. The four certification options, Paragraphs I through IV, define the legal relationship between the ANDA and the patent.
Paragraph I and II certifications (no patent listed, or patent already expired) allow approval without litigation. Paragraph III certification (patent has not yet expired; applicant will wait for expiry) leads to Tentative Approval and a scheduled commercial launch date. Paragraph IV certification is categorically different. It asserts that the listed patent is invalid, unenforceable, or will not be infringed by the generic product as described in the ANDA. Filing a Paragraph IV certification is itself a technical act of patent infringement under 35 U.S.C. 271(e)(2), a legal fiction specifically created by Hatch-Waxman to allow infringement disputes to be resolved before the generic enters the market.
Once the ANDA with a Paragraph IV certification is filed, the applicant must send a detailed notice letter to the patent owner and the NDA holder within 20 days. The notice must set out the factual and legal basis for the applicant’s claim that the patent is invalid or not infringed. This starts a 45-day window during which the patent owner can file a patent infringement lawsuit. Filing the lawsuit within that window triggers the 30-month automatic stay: the FDA is barred from granting final approval to the ANDA for up to 30 months from the date the brand received the notice letter, unless the court resolves the patent dispute favorably for the generic applicant before that period elapses.
The 30-Month Stay: Strategic Implications for Both Sides
For brand companies, the 30-month stay is a guaranteed period of insulation from generic competition following any Paragraph IV challenge. During those 30 months, the brand can continue to earn monopoly-level revenue on the challenged product, fund its own litigation defense, and, critically, deploy its evergreening patent strategy. For blockbuster drugs, this stay is worth hundreds of millions or billions of dollars in protected revenue. A study published in PubMed Central analyzing first generics between 2013 and 2020 found that the timing of stay expirations strongly predicted generic entry timing, confirming that the stay functions largely as intended as an automatic delay mechanism for the generic.
For generic companies, the 30-month stay is a guaranteed period of pre-launch investment: litigation costs, manufacturing scale-up, market preparation, and continued regulatory compliance obligations, all without commercial revenue. For a complex generic with high development costs, this can represent a substantial cash burn period. The company must balance this against the expected value of 180-day exclusivity if it wins the litigation, or the expected return from a Paragraph III later entry if it decides not to fight.
The 180-Day Exclusivity: The Financial Prize and Its Pathologies
The 180-day marketing exclusivity period for the first ANDA applicant to file a substantially complete Paragraph IV challenge is the most powerful financial incentive in the generic drug industry. It creates a temporary duopoly in which only the brand-name drug and the first generic compete. This duopoly period typically supports generic pricing at 20% to 40% below the brand price, dramatically higher than the 80% to 90% discounts that emerge in multi-generic markets. For a drug with $1 billion in annual U.S. brand revenue, 180-day exclusivity can generate $200 million to $400 million in gross profit for the first generic manufacturer.
The mechanics of exclusivity eligibility are precise. First applicant status requires filing a substantially complete ANDA with a Paragraph IV certification on the same day as the earliest Paragraph IV filer for the same RLD and strength. All companies that file on that first date share first applicant status and share the exclusivity if they each succeed in triggering it. Exclusivity is triggered by either commercial marketing or a court decision holding the challenged patent invalid or not infringed, whichever comes first for any first applicant.
Two pathologies have emerged from this system. The first is ‘exclusivity parking,’ where a first filer enters a reverse payment settlement with the brand company and agrees to delay commercial marketing. Because exclusivity is not triggered until marketing begins, the first filer’s exclusivity ‘parks’ while later ANDA filers are blocked from approval. This effectively extends the brand’s protected period at the expense of subsequent generic competitors and, ultimately, patients. The Medicare Modernization Act of 2003 introduced forfeiture provisions that cause a first applicant to forfeit exclusivity under defined circumstances, including failure to market within certain timeframes after approval or after a favorable patent outcome. These provisions have constrained the most egregious parking arrangements but have not eliminated them.
The second pathology is the race to file Paragraph IV challenges on drugs that are not yet ready for development, simply to secure first applicant status. This incentive can encourage submission of ANDAs before CMC development is complete, bioequivalence data is solid, or manufacturing scale-up has been validated, producing the RTR and early-stage CRL issues that inflate FDA review resources and delay eventual market entry for everyone.
The Evergreening Roadmap: How Brand Companies Extend Patent Life
Patent evergreening is the systematic practice of obtaining secondary patents on modifications, reformulations, or new uses of an existing drug compound, with the objective of extending effective market exclusivity beyond the expiry of the original compound patent. It is not illegal. It is not inherently anticompetitive. It is a rational IP strategy that any innovator company with a successful product will pursue. Generic teams that fail to understand the full depth and mechanics of an evergreening campaign will consistently underestimate the true patent clearance horizon for a target drug.
The following roadmap describes the typical multi-layer evergreening architecture deployed by innovator companies against blockbuster small-molecule drugs.
Layer 1: Compound Patent The original composition-of-matter patent covers the API itself. This is typically the narrowest claim in scope but the strongest in validity. It typically expires 20 years from filing. Hatch-Waxman patent term restoration can extend it by up to five years.
Layer 2: Formulation Patents After the compound patent issues, the innovator invests in developing formulations with improved patient convenience or clinical properties: extended-release (ER) formulations, once-daily dosing, abuse-deterrent coatings, or taste-masked pediatric forms. Each new formulation is patented separately. By the time the compound patent expires, the innovator may have a substantial portfolio of formulation patents extending five to fifteen years beyond it. These formulation patents are listed in the Orange Book and must be challenged via Paragraph IV certifications.
Layer 3: Method-of-Use Patents New clinical indications for approved drugs are pursued and patented. A drug originally approved for hypertension may receive new patents on its use for heart failure, diabetic nephropathy, or cardiorenal protection. These method-of-use patents are also Orange Book-listable and must be addressed by generic ANDAs seeking approval for those indications, or carved out using a skinny label.
Layer 4: Metabolite and Prodrug Patents Active metabolites or prodrug forms of the parent compound are developed and patented as separate chemical entities. The innovator then transitions its marketing emphasis to the new formulation, creating a new product lifecycle even as the parent compound patent expires. AstraZeneca’s transition from omeprazole (Prilosec) to esomeprazole (Nexium) is the canonical example. The base compound was generic; the active enantiomer was a new patented entity with a fresh 20-year patent clock.
Layer 5: Crystalline Form and Polymorph Patents The physical solid-state form of an API (crystal packing arrangement, or polymorph) can significantly affect manufacturing processing and dissolution properties, and each polymorph can be patented separately. An innovator that patents every known polymorph of its API creates a defensive thicket that requires any generic API supplier to either use the patented form (and risk infringement) or develop and validate an alternative polymorph (requiring additional development work and IP clearance analysis).
Layer 6: Process Patents Manufacturing processes for both the API and the finished formulation are patentable independently of the product itself. A patented stereoselective synthesis route, a specific purification method, or a specialized particle engineering technique can create infringement risk even for a generic that avoids all product patents.
Layer 7: Pediatric and Orphan Extensions Pediatric testing under the Best Pharmaceuticals for Children Act (BPCA) grants an additional six months of exclusivity beyond all existing patents and exclusivities. Orphan drug designation for a narrow indication grants seven years of market exclusivity. Both are pursued by innovators as legitimate extensions of commercial protection that also generate genuine clinical value.
The practical effect of this multi-layer architecture on a generic development timeline is substantial. AbbVie’s strategy for adalimumab (Humira), the world’s best-selling drug by revenue from 2012 to 2022, is the most analyzed modern example. AbbVie built a portfolio exceeding 250 patents around adalimumab, covering formulations, methods of use, dosing regimens, delivery devices, and manufacturing processes. The compound patent expired in 2016, but AbbVie’s patent thicket prevented U.S. biosimilar entry until 2023, seven years after compound patent expiry, through a combination of litigation settlements and licensing arrangements with biosimilar manufacturers. The IP asset value of that thicket, measured as the present value of the protected revenue stream it preserved, was estimated by analysts at over $100 billion.
The Skinny Label After GSK v. Teva: A Compromised Strategy
The skinny label, or Section viii carve-out, allows a generic applicant to seek approval only for non-patented uses of a drug when some method-of-use patents remain in force. The generic’s labeling carves out any mention of the patented indication, and the ANDA includes a Section viii statement rather than a Paragraph IV certification for those use patents. This avoids triggering the 30-month stay on the patented indication while allowing the generic to market for off-patent uses.
For decades, the skinny label was a reliable tool for early market entry. The Federal Circuit’s GlaxoSmithKline v. Teva decision, initially issued in 2020 and substantially affirmed in 2021 after en banc reconsideration, introduced material new risk. The court found that Teva’s press releases and marketing communications describing its carvedilol generic (the generic of Coreg) as equivalent to Coreg, a drug then approved for three indications including one still patent-protected, could constitute inducement of infringement. The skinny label itself carved out the patented indication, but Teva’s commercial messaging encouraged prescribers to use the product for all Coreg indications, including the patented one.
The ruling has generated significant concern. A 2025 analysis published in the Journal of Managed Care and Pharmacy found that skinny label approvals have continued post-Teva but that companies have adopted substantially more conservative marketing communications for skinny-label products. Some companies have chosen Paragraph IV certification over Section viii carve-outs for indications where the patented use is likely to drive the majority of prescriptions, accepting the litigation risk of a Paragraph IV challenge in preference to the inducement risk of a skinny label launch. For regulatory and legal teams, the post-Teva skinny label requires integration of marketing communications review into the regulatory and legal clearance process before any promotional materials go out. This is a functional integration that most organizations have not yet achieved.
Inter Partes Review: The Administrative Patent Challenge
Inter partes review (IPR) is an administrative proceeding at the USPTO Patent Trial and Appeal Board (PTAB) that allows any party to challenge the validity of an issued patent on grounds of anticipation or obviousness based on prior art patents and printed publications. IPR proceedings are cheaper, faster, and often more likely to succeed than district court patent challenges. The petitioner need only show that there is a ‘reasonable likelihood that it would prevail’ on at least one challenged claim to have the IPR instituted. The burden of proof at trial is preponderance of the evidence, lower than the clear and convincing evidence standard required to invalidate a patent in district court.
For generic companies facing a patent thicket, IPR is not a substitute for Paragraph IV litigation but a complement to it. An IPR filed against a key Orange Book patent while Paragraph IV litigation is pending in district court creates dual pressure on the innovator. If the PTAB institutes the IPR, the innovator must defend its patent on two fronts simultaneously. A favorable PTAB decision invalidating even a single key claim can reshape the litigation dynamics in district court and drive settlement at better terms for the generic.
The America Invents Act (AIA) of 2011 created IPR and related proceedings (post-grant review, or PGR) as patent quality improvement tools. The pharmaceutical industry has used them extensively. Between 2012 and 2024, the PTAB instituted IPRs against Orange Book-listed pharmaceutical patents at meaningful rates, with institution rates for pharmaceutical patents generally running below the overall PTAB average but with high claim cancellation rates among instituted proceedings. For generic IP teams, maintaining a systematic IPR candidate identification program, running in parallel with ANDA development and Paragraph IV strategy, is an integral part of the patent clearance toolkit.
Patent Intelligence: The Foundational Data Layer
None of the strategies described in this section, from Paragraph IV timing to evergreening defense to IPR targeting, can be executed without comprehensive, current, and structured patent intelligence. The Orange Book is the starting point but not the endpoint. It lists patents that the NDA holder has certified as claiming the drug or method of use. It does not list all patents that may be relevant to manufacturing, formulation, or analytical method, and patent listings can be contested as improper by generic challengers.
Tools like DrugPatentWatch consolidate Orange Book listings, FDA exclusivity data, ANDA filing records, Paragraph IV certification histories, litigation outcomes, and patent expiry schedules into a single queryable database. This integration allows development and legal teams to answer the questions that actually drive portfolio decisions: Which patents have already been successfully challenged for this drug? What was the theory of invalidity that succeeded? Which companies have already filed ANDAs? Which patents have been licensed in prior settlement agreements? What is the earliest date on which a generic can credibly enter the market given all current IP and exclusivity constraints?
The value of this intelligence is not limited to the legal team. Business development uses it for target identification and deal valuation. R&D uses it to design around problematic formulation or process patents. Finance uses it to model launch timing probability distributions for revenue forecasts. Regulatory uses it to determine which Paragraph certifications are needed and in what order. In this sense, patent intelligence is not a support function. It is the shared analytical infrastructure on which every commercial decision in the generic drug business ultimately rests.
Investment Strategy: Patent Risk and Generic Company Equity
For institutional investors in generic pharmaceutical companies, patent risk is among the most significant drivers of equity valuation uncertainty. A company’s forward earnings depend heavily on which products it can launch, at what time, and at what price. All three variables are functions of the patent and exclusivity landscape for each pipeline product.
Three analytical frameworks are particularly useful for investor diligence.
The patent cliff exposure analysis identifies which products in a company’s revenue base are currently protected by brand patents nearing expiry, and whether the company has the ANDA development capability and Paragraph IV filing history needed to be a first-or-early-entry generic. Companies with a track record of successful P-IV litigation and established relationships with leading Hatch-Waxman law firms (Robins Kaplan, Duane Morris, Goodwin Procter) signal higher capability.
The pipeline IP quality assessment evaluates pending ANDA filings for their patent certification status. First-applicant P-IV ANDAs are premium assets. Later-filed P-IV ANDAs for the same drug, if first-applicant status is already taken, are lower-value assets with earlier-stage market entry probability dependent on the success of the first filer’s litigation. Third-party patent challenge databases can identify how many companies have already filed and whether any have settled.
The evergreening vulnerability map asks, for each marketed brand drug that is a generic development target, how many layers of secondary patent protection remain after compound patent expiry. Drugs with thin secondary patent portfolios (few formulation or method-of-use patents, no pediatric exclusivity) represent lower-barrier generic opportunities. Drugs with dense multi-layer patent architectures, like adalimumab’s biosimilar space, require sustained litigation investment and may have compressed exclusivity windows even for successful challengers.
Key Takeaways: Section 6
Paragraph IV litigation is not an optional strategy for companies targeting high-value U.S. generics. It is the mechanism by which early market entry is achieved. The 180-day exclusivity reward system creates genuine financial incentive to challenge patents aggressively, but also creates pathological incentives for parking and premature filing. Evergreening is a systematic multi-layer brand IP strategy that generic teams must map in full, not just at the compound patent level. GSK v. Teva has materially complicated skinny label risk management and requires marketing communications to be reviewed as part of the legal clearance process. IPR at the PTAB is a faster, lower-cost patent validity challenge tool that should run in parallel with Paragraph IV litigation strategy. Structured patent intelligence is not a legal support tool but the foundational data layer for every commercial decision in the generic business.
7. The Proactive Playbook: Pre-ANDA Meetings, QbD, and AI-Driven Regulatory Affairs
Pre-ANDA Meetings: Front-Loading Regulatory Clarity
The traditional generic drug development model placed regulatory affairs at the end of the process: formulate the product, run the BE studies, manufacture the clinical batches, compile the data, and submit. Any disagreement with the FDA on the approach surfaced in a CRL, weeks or months after the study was done and the money was spent. For simple generics with clear PSG guidance, this model is tolerable. For complex generics with ambiguous regulatory pathways, it is financially catastrophic.
The GDUFA II pre-ANDA meeting program, expanded and formalized under GDUFA III, specifically addresses complex products where the regulatory path is unclear. Product Development (PDEV) meetings allow early-stage developers to present a proposed development strategy to OGD and receive specific scientific feedback before committing to a study design. Pre-Submission (PSUB) meetings, held closer to submission, allow a company to walk through its completed data package with OGD and identify any obvious deficiencies before the ANDA is formally filed.
The FDA’s 2024 guidance on pre-ANDA meetings specifies that PDEV meeting requests should include a clear statement of the development question, a summary of relevant scientific background, and proposed development approaches with their scientific rationale. Vague or underprepared meeting packages generate vague FDA responses. Teams that invest in detailed, scientifically rigorous meeting packages receive correspondingly more actionable feedback.
The strategic value of a well-executed PDEV meeting goes beyond the information exchanged. For complex generic products where the first company to achieve approval gains a near-permanent competitive position, the intelligence advantage from a PDEV meeting is measured in years of development time saved or redirected. If the FDA confirms that a company’s proposed in vitro permeation testing approach is adequate, the company can commit its full formulation optimization resources to that approach with confidence. If the FDA indicates that in vivo data will also be required, better to know that in year one of the program than in year three, after the formulation is locked and the IVPT data package is complete.
Companies that have built systematic pre-ANDA engagement programs, including dedicated teams for meeting preparation and follow-up, have measurably shorter first-cycle approval rates for complex products than those that avoid agency contact until submission. OGD’s own data from GDUFA performance reports confirms that pre-ANDA meetings are associated with higher submission quality and fewer major amendment requests.
Quality by Design: The Architecture of Regulatory Flexibility
Quality by Design (QbD) is a pharmaceutical development philosophy originating from the FDA’s 2004 Pharmaceutical cGMPs for the 21st Century initiative and formalized through ICH guidelines Q8(R2) (Pharmaceutical Development), Q9 (Quality Risk Management), and Q10 (Pharmaceutical Quality System). Its core premise is that quality cannot be reliably tested into a finished product. It must be designed in through a systematic understanding of how formulation and process variables affect product performance.
The QbD framework begins with defining the Quality Target Product Profile (QTPP), a prospective summary of the quality characteristics that the drug product should have to achieve the desired clinical outcome. For a generic immediate-release tablet, the QTPP might specify bioequivalence to the RLD, a dissolution profile matching the RLD across pH conditions, acceptable hardness and friability for coating and packaging, and a two-year shelf life under ICH Zone II stability conditions.
From the QTPP, the development team identifies Critical Quality Attributes (CQAs), the physical, chemical, biological, or microbiological properties of the drug product that must be within specified limits to ensure product quality. Dissolution rate and API assay are almost always CQAs for oral products. Particle size distribution of the API may be a CQA if it affects dissolution. Moisture content may be a CQA if it affects stability.
Critical Material Attributes (CMAs) of the API and excipients, and Critical Process Parameters (CPPs) of the manufacturing process, are then characterized through systematic experimentation, typically using design of experiments (DoE) to understand their effect on CQAs. This builds a multi-dimensional knowledge space, sometimes called a Design Space, within which process variations can be shown not to adversely affect product quality.
How QbD Creates Regulatory Flexibility
The commercial value of a QbD development program is its post-approval flexibility. Under 21 CFR 314.70, post-approval changes to an ANDA must be reported as Prior Approval Supplements (PAS), Changes Being Effected supplements (CBE-30 or CBE-0), or in Annual Reports, depending on the potential impact on product quality. The more a company can demonstrate, using validated process knowledge, that a proposed change falls within the established design space where quality is maintained, the less burdensome the required reporting category.
A company operating within a validated design space can often report API particle size specification adjustments (within the proven acceptable range) in a CBE-30 supplement or Annual Report, rather than a PAS that would require months of FDA review before implementation. In a world of API supply chain disruptions, where switching to an alternative supplier or adjusting a process parameter may be operationally necessary on short notice, this flexibility is not a regulatory abstraction. It is a direct contributor to supply continuity.
Pharmaceutical Quality Management Systems (QMS) governed by ICH Q10 provide the organizational framework that sustains QbD throughout a product’s commercial lifecycle. A QMS defines the procedures for document control, training, deviation management, corrective and preventive action (CAPA) implementation, change control, and supplier qualification. It is the operational infrastructure that ensures a company’s Quality by Design intentions are consistently executed at the manufacturing level, day after day, batch after batch.
For generic manufacturers competing on cost, the temptation to minimize QMS investment is real. The consequences of that minimization, in FDA warning letters, import alerts, manufacturing site shutdowns, and recall-driven revenue losses, are visible in the FDA enforcement database every year. Sun Pharma’s Halol facility received an import alert in 2014 that disrupted product supply for over two years and depressed the company’s U.S. revenue significantly. Ranbaxy’s multi-site data integrity and cGMP failures resulted in the most extensive enforcement action in the FDA’s generic drug history, ultimately costing the company $500 million in criminal and civil settlements and permanent loss of several U.S. product approvals.
AI and Machine Learning in Generic Drug Development
Artificial intelligence and machine learning are at various stages of practical deployment across the generic development lifecycle. The technology is sufficiently mature in some applications to generate material ROI today, while in others it remains in early-stage development or validation.
Formulation Development: AI-Guided Excipient Selection
AI-driven formulation optimization uses historical datasets of drug-excipient compatibility studies, dissolution profiles, and stability outcomes to train predictive models that recommend optimal formulation compositions for new API targets. Platforms from companies including Molecular Forecaster, Chemaxon, and Schrödinger, as well as internally built ML tools at larger generic companies, can reduce the number of experimental formulation screening iterations needed to achieve a target dissolution profile or stability specification.
The data quality problem is substantial. Most generic manufacturers maintain formulation development data in electronic lab notebooks (ELNs) and LIMS systems that were not designed with ML data feeding in mind. Schema inconsistencies, free-text fields, variable unit conventions, and incomplete batch records undermine the ability to train reliable models. Before investing in ML formulation platforms, companies typically need 12 to 24 months of data standardization work to achieve the data quality baseline required for meaningful model training.
Stability Prediction: Accelerated Development Through ML
Formal stability programs for ANDA submissions require real-time stability data at the time of submission under ICH Q1A(R2) conditions (25C/60% RH for Zone I/II markets, 30C/65% RH for Zone III/IV). This typically requires 12 months of real-time data at the time of submission for products with proposed 24-month shelf lives. ML models trained on physicochemical properties of the API and formulation, historical stress test data from accelerated stability conditions (40C/75% RH), and analogous product stability databases can generate early predictions of real-time stability performance, allowing teams to identify high-risk formulations and redirect development before the 12-month stability clock becomes a program constraint.
Regulatory Submission Automation: NLP and Document QC
Natural language processing tools can automate the review of ANDA draft documents for compliance with FDA formatting requirements, cross-document consistency (e.g., batch numbers referenced in BE reports must match those in the CMC section), and alignment with the specific PSG guidance for the product. Several regulatory technology companies, including Saama Technologies, Certus, and Regulatory Compliance Associates, offer NLP-based submission QC platforms. The FDA itself has deployed AI tools internally to assist in ANDA review, and the agency’s 2024 AI Action Plan for drugs and biologics signals continued investment in AI-assisted regulatory review.
The FAIR Data Infrastructure: The Prerequisite for AI Success
The most common reason AI initiatives in pharmaceutical regulatory affairs fail is not algorithmic. It is architectural. Regulatory data in most pharmaceutical companies exists in isolated functional silos: formulation data in R&D’s ELN, manufacturing data in the operations MES, stability data in a quality-controlled LIMS, and patent and competitive intelligence data in a separate legal database. AI models trained on data from one silo cannot make the cross-functional connections that generate the highest value insights.
FAIR data principles (Findable, Accessible, Interoperable, Reusable), promoted by the Research Data Alliance and increasingly adopted by pharmaceutical regulatory agencies as part of data integrity expectations, provide the framework for the data infrastructure needed to support cross-functional AI. Implementing FAIR principles requires governance decisions about data standards, metadata schemas, data owner roles, and cross-system interoperability that span multiple functions and require executive sponsorship.
The FDA’s current expectations for AI in regulatory submissions, articulated in its 2023 draft guidance on AI-assisted drug development submissions, focus on transparency about model inputs, validation documentation for model performance, and clear articulation of where AI outputs are used in the submission versus where traditional experimental data remains the primary evidence. Companies that build FAIR data infrastructure now will be materially better positioned to meet these evolving expectations as AI use in submissions becomes standard rather than exceptional.
Key Takeaways: Section 7
Pre-ANDA meetings, particularly PDEV meetings for complex generics, provide development guidance whose value is measured in years of avoided rework. QbD is not a quality compliance exercise but a regulatory flexibility strategy that pays commercial dividends when supply chain disruptions or process optimization opportunities require post-approval changes. AI in generic regulatory affairs is past the proof-of-concept stage for formulation prediction, stability modeling, and submission QC automation, but its effectiveness depends entirely on the quality and organization of the underlying data infrastructure. Companies that invest in FAIR data governance before deploying AI will extract meaningfully higher ROI than those that bolt AI tools onto siloed, inconsistent data systems.
8. Investment Strategy for Portfolio Managers and Institutional Analysts
Valuing Generic Drug Companies: The IP and Regulatory Metrics That Matter
Generic pharmaceutical company equity valuation is frequently anchored to revenue multiples and EBITDA, which are lagging indicators of competitive position. The leading indicators, the ones that predict whether a company’s revenue will grow, contract, or hold over the next three to five years, are almost entirely IP and regulatory in nature. Portfolio managers and buy-side analysts who do not build these metrics into their models are working with systematically incomplete information.
Key leading indicators for long-term generic company value:
First-to-file Paragraph IV ANDA count and win rate in subsequent litigation. Companies with a high ratio of first-to-file P-IV ANDAs to total ANDA pipeline, and a strong track record of either winning litigation or entering favorable settlements, have a structurally advantaged revenue pipeline. This data is publicly available through Orange Book filings, ANDA approval announcements, and court docket searches.
FDA facility inspection profile. A company whose manufacturing sites have received FDA warning letters or import alerts in the preceding 24 months will face approval delays, potential consent decrees, and ongoing remediation cost burdens. The FDA’s enforcement database tracks all warning letters and import alerts publicly. A clean, multi-site manufacturing network with well-documented GMP compliance is worth a meaningful premium in valuation.
ANDA cycle rate. The average number of review cycles required to achieve ANDA approval, data the FDA reports in its annual performance reports and which can be approximated for individual companies through FDA approval date analysis relative to submission date, is a proxy for submission quality. Companies with low average cycle rates maintain more predictable launch timelines and lower regulatory management costs.
Complex generic and biosimilar pipeline proportion. As discussed throughout this piece, complex generics carry higher development costs but support more durable pricing. A company transitioning its pipeline toward complex generics is a company investing in margin sustainability. Biosimilar pipeline proportion matters similarly: the global biosimilar market is projected to reach $100 billion by 2030, and companies with demonstrated biologics manufacturing capability and established regulatory interchangeability designations are positioning for a different competitive dynamic than the small-molecule generic market.
Case Study: Adalimumab Biosimilars and IP Valuation
The adalimumab biosimilar space provides the most instructive recent case study in IP-driven market timing and valuation. AbbVie’s Humira generated peak U.S. revenues exceeding $20 billion annually. Its compound patent expired in 2016. AbbVie’s multi-layer patent estate, combined with litigation settlements that included licensing arrangements with biosimilar manufacturers (Amgen, Sandoz, Boehringer Ingelheim, Fresenius Kabi, and others) in exchange for delayed U.S. entry until 2023, preserved an extraordinarily valuable revenue stream for seven years beyond compound patent expiry.
When U.S. biosimilar entry began in earnest in 2023, nine biosimilars launched in rapid succession. AbbVie had already repositioned its U.S. Humira franchise to Skyrizi and Rinvoq, newer immunology drugs with patent protection extending into the 2030s. The biosimilar manufacturers that entered in 2023 are competing in a market where the innovator has already actively migrated its patient population to patent-protected successors. The revenue available to biosimilar entrants is structurally smaller than it would have been with earlier entry, a direct consequence of AbbVie’s seven-year IP-driven delay. Analysts at SVB Securities and TD Cowen revised biosimilar revenue forecasts downward through 2023 and 2024 as this dynamic became apparent.
The lesson for investors is that patent expiry date does not equal market entry date, and market entry date does not equal market opportunity. The IP strategy deployed by the innovator between patent expiry and actual generic/biosimilar entry is the critical intervening variable.
Sector-Level Investment Themes for 2025-2030
The generic pharmaceutical sector presents several distinct investment themes over the medium term.
The GLP-1 patent cliff is the most discussed upcoming generic opportunity. Semaglutide (Ozempic, Wegovy) holds compound patent protection through approximately 2032 in the United States, with formulation and method-of-use patents extending potentially further. The molecule’s extraordinary commercial scale and strong formulary entrenchment create an exceptional generic opportunity for any company that succeeds in developing a bioequivalent formulation and navigating the IP landscape. The technical challenges are significant: subcutaneous injection formulations with specific viscosity, pH, and long-term stability requirements, combined with an auto-injector device platform. Companies investing now in semaglutide-related ANDA development are building a multi-year option on a potentially massive revenue opportunity.
The oncology complex generic space, particularly for targeted therapies and liposomal formulations, offers durable competitive differentiation. Drugs like liposomal doxorubicin, nab-paclitaxel (Abraxane), and branded topotecan formulations have high scientific barriers to generic development that keep competitor counts low and pricing supportable even in multi-generic markets.
The biosimilar interchangeability designation, granted by the FDA when a biosimilar meets additional switching study requirements demonstrating that patients can switch between the originator and biosimilar without increased risk, creates a meaningful commercial advantage in states where pharmacist-level substitution (without prescriber intervention) is permitted for interchangeable products. Companies with interchangeability designations, currently a small subset of approved biosimilars, are positioned for higher market penetration rates in the U.S. retail pharmacy channel.
9. FAQ: What Generic Drug Teams Actually Ask
How should a mid-sized generic firm choose between simple and complex generic targets?
The decision is a capability assessment, not a market size analysis. A high-volume simple generic (blockbuster oral tablet) offers scale but guarantees price collapse and requires operational cost efficiency as the primary competitive moat. A complex generic (transdermal system, inhaled powder, liposomal injectable) offers a higher-barrier market with fewer competitors and more durable pricing, but requires R&D capabilities, specialized manufacturing infrastructure, and regulatory expertise that most mid-sized generic firms do not currently possess.
A mid-sized firm should assess honestly whether its core competencies are operational (low-cost manufacturing, supply chain scale, commercial execution speed) or scientific (advanced formulation capability, analytical chemistry expertise, regulatory science innovation). Operational strengths point toward optimizing within the simple generic category while building selectivity around products with longer competitive protection due to complexity of manufacture even if not complex from an FDA definitional standpoint. Scientific strengths point toward investment in complex generic development, with realistic expectations of a four-to-seven-year program timeline and $20 million to $100 million in development investment per product before an ANDA can be filed.
What are the steps after receiving a Complete Response Letter with major CMC deficiencies?
The immediate response is to assemble a cross-functional triage team with leadership from Regulatory Affairs, Manufacturing/CMC, Analytical Chemistry, Quality Assurance, and Legal. The first task is not to begin remediation but to read the CRL with the level of precision the FDA used in drafting it. Every deficiency statement is a legal document. The agency’s language in a CRL defines the scope of the required response, and misinterpreting that language can produce a second CRL.
The second step is to request a post-CRL Type A meeting with the FDA. Type A meetings are reserved for critical program issues including CRL responses for ANDAs. The request must be submitted within 30 days of the CRL to be granted by FDA within 30 business days. The objective is not to argue with the FDA’s conclusions but to confirm the agency’s precise expectations for the amendment, identify whether any alternative data or approaches would be acceptable, and establish a submission timeline. Companies that skip this step and proceed directly to remediation based on their own interpretation of the CRL consistently produce second CRLs.
The third step is an integrated project plan with explicit task ownership, dependencies mapped between CMC workstreams (stability studies feeding analytical method revalidation, process validation batches feeding updated batch analysis data), and a realistic submission date that accounts for FDA review cycles, not just internal completion dates.
What non-litigation strategies exist for navigating a patent thicket?
Four approaches have material strategic value before committing to full Paragraph IV litigation on all thicket patents.
Structured validity analysis using prosecution history estoppel is the most cost-efficient starting point. The prosecution history of each Orange Book patent, publicly available through the USPTO Patent Center, records the arguments the applicant made to overcome examiner rejections. Applicants who argued their patent claims narrowly to avoid prior art are often estopped from later claiming a broader scope in litigation. An experienced Hatch-Waxman patent litigator reviewing prosecution histories can identify patents where the claims are effectively narrower than their face text and where a non-infringement argument is strong before any litigation begins.
Formulation design-around is the cleanest strategic outcome when it is achievable. If the strongest thicket patents claim specific excipient combinations, polymer grades, or manufacturing process steps, a formulation chemistry team working in close coordination with patent counsel may be able to develop an alternative formulation that achieves bioequivalence to the RLD through a different technical approach. Design-around eliminates the litigation exposure entirely.
Inter Partes Review (IPR) at the PTAB is the fastest administrative route to invalidating weak or narrow patents in the thicket. The cost of a single IPR petition is approximately $300,000 to $600,000 in total legal fees, compared to $5 million to $20 million or more for district court litigation. The PTAB’s institution rate for well-supported IPR petitions in the pharmaceutical space has historically been significant, and claim cancellation rates in instituted proceedings are high. Strategically timing IPR petitions to coincide with the 30-month stay period allows the generic challenger to pursue validity attacks administratively while district court litigation proceeds in parallel.
Licensing negotiations with the brand company, particularly for products where the generic challenger has significant financial resources and litigation credibility, sometimes produce settlement terms that allow generic entry before all patents expire. These negotiations require demonstrating that the Paragraph IV challenge is credible and well-funded, that litigation will be sustained regardless of the brand’s counter-strategy, and that the economic terms of a licensing settlement are preferable for both parties to the cost and uncertainty of protracted multi-year litigation.
What is the single most important change for successful AI implementation in regulatory affairs?
Establish unified data governance before deploying any AI model. Regulatory AI fails almost universally not because the algorithms are inadequate but because the training data is incomplete, inconsistent, or inaccessible. Formulation data lives in R&D’s ELN. Batch manufacturing data lives in the operations MES. Stability data is managed by the quality unit in a separate LIMS. API characterization data is often embedded in PDF attachments to paper-based DMF submissions. None of these systems talk to each other in a structured, machine-readable way.
Building FAIR data infrastructure requires two to three years of disciplined governance work: defining data standards for each functional data type, assigning data ownership and stewardship roles, implementing cross-system interoperability protocols, and shifting organizational culture toward treating data as a strategic asset requiring active curation. Companies that invest this foundation will find AI tools become meaningfully more powerful and their FDA submissions involving AI components become more defensible. Companies that skip this step will find that AI tools produce inconsistent, unvalidatable outputs that cannot support regulatory submissions and generate more compliance risk than they resolve.
10. Future Outlook: Five Forces Reshaping Generic Regulation by 2030
Force 1: Global Regulatory Harmonization Accelerating
The FDA’s Global Generic Drug Affairs program, the ICH Generic Drug Working Group, and the EMA’s international cooperation activities are all moving toward greater harmonization of generic drug standards. ICH M13A on immediate-release solid oral BE is the most recent and most significant output. ICH M13B, covering modified-release products, and M13C, covering other dosage forms, are in various stages of development. For multi-market generic companies, harmonization reduces duplicative study burdens and should eventually allow a single global ANDA/MA dossier for most standard product categories.
Force 2: Biosimilar Regulatory Science Maturing
The FDA’s Purple Book equivalent of the Orange Book now lists biosimilar approvals alongside interchangeability designations. Post-2023 experience with the adalimumab biosimilar class and the ongoing development of biosimilar versions of other high-revenue biologics (ustekinumab, dupilumab, pembrolizumab) is generating real-world evidence on switching behavior, immunogenicity outcomes, and market uptake dynamics. This evidence base will progressively refine the FDA’s and EMA’s analytical expectations for biosimilar interchangeability demonstration, making the pathway more predictable and eventually more accessible.
Force 3: GLP-1 Generics Reshaping the Competitive Landscape
The expiry of semaglutide’s core patents in the early 2030s will likely produce the most commercially significant generic drug launch in history, assuming demand for GLP-1 receptor agonists remains at or above current levels. The regulatory, manufacturing, and IP challenges are substantial. Developing injectable peptide generics requires peptide synthesis capability, lyophilization or sterile fill-finish manufacturing, complex device integration, and reference-scaled BE approaches that the FDA has not yet fully standardized for injectable peptides. Companies that begin this development program in 2025 or 2026 are working on realistic timelines for first launch windows.
Force 4: Tariff and Supply Chain Policy Creating New Domestic Manufacturing Incentives
U.S. pharmaceutical tariff policy, whatever form it ultimately takes, is generating meaningful interest from generic manufacturers in domestic API production and finished drug manufacturing. The FDA’s recently enhanced domestic pharmaceutical manufacturing incentive framework and Congressional proposals for preferential procurement of domestically manufactured generics for federal programs create a potential structural shift in the economics of U.S. API supply. Companies with domestic manufacturing footprints may gain both regulatory and commercial advantages over the medium term.
Force 5: AI-Driven Regulatory Submissions Becoming the New Standard
The FDA’s 2024 AI Action Plan and the EMA’s ongoing reflection paper on AI in medicines development signal that both agencies are developing frameworks for AI-generated data in regulatory submissions. The trajectory is toward acceptance of AI-assisted formulation development data, AI-predicted stability outcomes, and AI-assisted bioequivalence assessment as supporting evidence in ANDA packages, with appropriate validation documentation. Companies that develop AI capabilities and the validation frameworks the FDA expects will submit faster, more complete, higher-quality ANDAs. Those that rely solely on traditional development methods will face systematic disadvantage against AI-equipped competitors who produce equivalent evidence packages at lower cost and in shorter time.
Final Perspective
The generic drug regulatory environment in 2025 is not simply more complex than it was in 1984 when Hatch-Waxman passed. It operates on a fundamentally different logic. The original framework assumed that most generics were straightforward chemical replicas of simple oral drugs, that patent litigation was an exceptional rather than routine feature of market entry, and that the primary regulatory challenge was proving scientific equivalence. All three of those assumptions have been invalidated by the evolution of the industry.
Modern generic drug regulatory strategy integrates patent law, advanced formulation science, complex manufacturing, global market access, and AI-driven data systems in a single coherent program. The companies that succeed over the next decade will be those that treat regulatory affairs not as a compliance function at the end of the development chain, but as a strategic and commercial function running from the first day of target identification through the last day of a product’s commercial lifecycle.
The margin for error is tighter than it has ever been. The opportunity for those who get it right remains substantial.
This analysis is intended for pharmaceutical IP teams, regulatory strategy functions, R&D leadership, and institutional investors in the pharmaceutical sector. Patent and exclusivity data should be verified against current Orange Book listings and USPTO records prior to any investment or development decision. This document does not constitute legal or investment advice.
Data sources include FDA Orange Book, GDUFA performance reports, AAM savings reports, EMA guidance documents, PTAB statistics, IQVIA market data, PubMed Central, and public company disclosures.