Somewhere in a regulatory affairs department right now, a development team is arguing about whether to run a comparative clinical efficacy study for their biosimilar candidate. The analytical data looks good. The PK bridging is solid. But the default answer — the safe answer — has always been to run the trial. That answer is no longer default. In 2025, the regulatory floor shifted under the entire biosimilar industry, and the teams that understand exactly what changed, and why, will reach the market two to four years faster than those who don’t.
This article is a ground-level account of how biosimilar clinical efficacy trials actually work, what regulators across the FDA, EMA, PMDA, and Health Canada now require, and what the seismic changes in 2024 and 2025 mean for development strategy, patent intelligence, and competitive positioning. It covers the science without burying the business logic.
Part I: The Economics That Drive Everything
The Market Is Not Hypothetical
The global biosimilars market was valued at USD 21.8 billion in 2022 and is projected to reach USD 76.2 billion by 2030, a compound annual growth rate of 15.9% [1]. More aggressive estimates push that figure to USD 171–185 billion by 2033 [2]. Those numbers are worth treating with some skepticism — biosimilar market projections have historically outrun actual adoption — but even the conservative range represents one of the most reliably large growth opportunities in pharmaceutical commercial history.
The mechanism behind that growth is arithmetic, not speculation. A single 100-mg vial of Remicade (infliximab) carried a retail price around USD 1,600. Avsola, an FDA-approved infliximab biosimilar, entered the market priced around USD 500 [1]. That 69% gap exists across dozens of reference biologics whose patents are either expiring now or will expire within the next decade. The IQVIA Institute estimated in a widely cited analysis that biosimilar entry into the U.S. biologics market would save approximately USD 38.4 billion in biologic expenditure between 2021 and 2025 [3]. The savings are real and they are already materializing.
North America held 40.4% of global biosimilar revenue in 2022 [2]. Europe, which built its biosimilar regulatory framework roughly a decade earlier than the United States, held 50.44% of global market share that same year [2]. The gap between those two figures tells you something important: early regulatory clarity creates market scale. Europe figured out the clinical evidence standard for biosimilars before the U.S. did, and European patients got cheaper biologics faster as a result. The U.S. is now doing something similar, and the window to position ahead of that shift is closing. <blockquote> ‘A review of over 600 published biosimilar studies found that no biosimilar with proven analytical similarity has ever failed a comparative efficacy study.’ — Scientific Justification and Policy Recommendations to the U.S. Food and Drug Administration for Waiving Comparative Efficacy Studies, published in <em>Pharmaceutics</em>, 2025 [4] </blockquote>
That single statistic reframes the entire clinical trial debate. If the outcome is preordained by the analytical data, then the comparative efficacy study becomes an expensive formality — and that is exactly how both the FDA and EMA have begun to treat it.
What a Biosimilar Actually Is (And Why It Matters for Trial Design)
The standard definition calls a biosimilar a biological medicine that is ‘highly similar’ to an already-approved reference product with ‘no clinically meaningful differences’ in safety, purity, and potency [5]. That definition is precise to the point of being strategic. Every word in it has regulatory consequence.
‘Highly similar’ is not ‘identical.’ Biologics are produced in living cells — mammalian, bacterial, or yeast — and biological manufacturing is inherently variable. Batch-to-batch variation is a feature of originator biologics, not just biosimilars. The post-translational modifications that give a monoclonal antibody its three-dimensional shape, its glycosylation pattern, its effector function — these are never precisely reproduced even by the same manufacturer using the same cell line across time [6]. The FDA has approved multiple variants of reference biologics’ own manufacturing process changes under its comparability framework. Biosimilar development operates by an analogous scientific logic.
‘No clinically meaningful differences’ is the phrase that drives clinical trial design. It does not mean no differences at all. It means no differences that a patient would experience in terms of how well the drug works or how likely it is to harm them. Quantifying that threshold is the entire technical challenge of running a biosimilar efficacy trial.
The distinction from generics is not semantic. A generic is the same molecule as the brand-name drug. A biosimilar is not the same molecule — it is a large, complex protein produced by a different cell line in a different facility, and the two molecules differ in ways that can be measured analytically but may not manifest clinically. That gap between ‘analytically detectable’ and ‘clinically meaningful’ is where biosimilar science lives.
Why Clinical Trials Cost So Much and Why Regulators Are Rethinking Them
A standard comparative efficacy trial for a biosimilar costs USD 30–100 million to execute and takes three to five years from IND filing to final data [7]. The FDA’s own October 2025 draft guidance cites the objective of halving biosimilar development timelines from 5–8 years down to 2–4 years and reducing per-product costs by ‘tens of millions of dollars’ [8]. That goal cannot be achieved without changing how clinical data requirements are structured.
The irony is that the clinical trial is usually the least informative part of the biosimilar development package. An analytical characterization program using hydrogen deuterium exchange mass spectrometry, high-resolution glycan mapping, and functional binding assays detects differences between a biosimilar and its reference product with far greater sensitivity than a 300-patient equivalence trial. The FDA said this explicitly in its October 2025 draft guidance: ‘A comparative analytical assessment is generally more sensitive than a comparative efficacy study to detect differences between two products, should any exist, that may preclude a demonstration of biosimilarity’ [9].
The question is not whether biosimilar clinical efficacy trials matter — they do, in cases where analytical and PK data leave residual uncertainty. The question is which trials are scientifically necessary versus bureaucratically inherited. That distinction is now at the center of a global regulatory reckoning.
Part II: The ‘Totality of Evidence’ Framework
What It Means in Practice
The phrase ‘totality of evidence’ appears in virtually every biosimilar regulatory guidance document issued by the FDA, EMA, PMDA, and WHO. It refers to the integrated weight of analytical, functional, non-clinical, pharmacokinetic, and clinical data, evaluated as a whole to determine whether a proposed biosimilar is sufficiently similar to its reference product [10].
The framework is both philosophically sound and practically difficult. It is sound because no single study type can prove biosimilarity on its own. Analytical data establishes structural and functional comparability at the molecular level but cannot account for complex interactions within a patient’s immune system. Clinical PK data demonstrates that the drug behaves comparably in human subjects but is limited by the small sample sizes typical of PK studies. Comparative efficacy studies add large-sample clinical validation but are statistically powered to detect only large differences. Put them all together and you get a coherent picture.
It is difficult because ‘weighing totality’ is inherently judgmental. Different regulators weigh the same package of evidence differently, and the same regulator may weigh similar packages differently across product classes or over time. Managing that uncertainty is the core regulatory strategy challenge in biosimilar development.
The practical implication is that the strength of your early-stage analytical work determines how much clinical work you need to do. Invest heavily in characterization and you de-risk the clinical program. Cut corners on characterization and you create residual uncertainties that must be resolved with additional, expensive clinical studies.
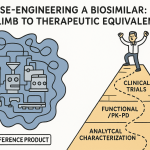
Stepwise Development: The Logic of the Pyramid
Biosimilar development is structured as a cascade. You start with the most information-rich, lowest-cost studies and use those results to determine what additional work is needed. The logical flow is:
- Physicochemical and structural characterization comparing the biosimilar and multiple batches of the reference product
- Functional assays — binding, cell-based, and mechanistic — confirming that the two products engage their targets identically
- Non-clinical assessments, increasingly in vitro rather than in vivo, to bridge the mechanistic data to human biology
- Clinical PK/PD studies in healthy volunteers or patients to demonstrate that the drug behaves comparably in the human body
- Comparative efficacy and safety studies in patients, if and only if residual uncertainty remains after the prior steps
At each stage, the goal is to ask: does this data resolve the question of biosimilarity, or does residual uncertainty require the next step? If the analytical and functional data are sufficiently robust, you may not need animal studies. If the analytical, functional, and PK data taken together are convincing, you may not need a comparative efficacy trial. That conditional logic is the architecture of modern biosimilar regulatory strategy.
Residual Uncertainty: The Decision Variable That Drives Everything
Every regulatory decision in biosimilar development comes back to residual uncertainty. Regulators ask: after considering all the data assembled at this stage, what uncertainty remains about whether the biosimilar will perform like the reference product in patients? If that uncertainty is negligible — which an increasing body of science and regulatory experience suggests it often is, once analytical and PK similarity is established — then requiring a large-scale clinical trial serves no scientific purpose.
This framing is useful for development teams because it provides a concrete decision criterion. The question to ask at every development stage is not ‘have we done enough studies?’ but rather ‘what uncertainty remains, and what study, if any, would resolve it?’ A team that can answer that question precisely and document it clearly is in a position to have a productive conversation with regulators about waiving unnecessary requirements.
Platforms like DrugPatentWatch are valuable at this stage not just for patent intelligence but for understanding precedent: which biosimilars in a given therapeutic class have been approved with reduced clinical data packages, what analytical thresholds those approvals established, and what arguments successfully supported clinical trial waivers. That historical approval data is a primary input for a scientifically defensible justification of reduced clinical requirements.
Part III: Analytical Characterization — Where the Real Work Happens
The Toolkit Has Changed Dramatically
Twenty years ago, biosimilar developers worked primarily with basic chromatographic methods and gel-based protein analysis. Today’s characterization toolkit is sophisticated enough to detect single-site glycosylation differences and map protein folding dynamics in solution. This analytical revolution is the primary scientific justification for reduced clinical requirements.
The key techniques in a modern characterization program include:
Structural analysis: X-ray crystallography and cryo-electron microscopy establish the three-dimensional conformation of the protein at atomic resolution. Circular dichroism spectroscopy assesses secondary structure. Hydrogen deuterium exchange mass spectrometry probes conformational dynamics and identifies structural differences that static crystallography would miss [11].
Post-translational modification mapping: Glycosylation is the most therapeutically significant PTM for most monoclonal antibodies. High-resolution glycan mapping using liquid chromatography coupled with mass spectrometry can quantify differences in glycan composition at individual sites. Deamidation, oxidation, and disulfide bond variants are mapped using peptide mapping with tandem mass spectrometry [6].
Functional assays: Binding affinity measurements using surface plasmon resonance or biolayer interferometry quantify target engagement at the molecular level. Cell-based assays assess downstream pharmacological effects, including antibody-dependent cellular cytotoxicity, complement-dependent cytotoxicity, and FcRn binding — all of which are directly relevant to efficacy and immunogenicity [12].
Together, these techniques produce a comprehensive molecular portrait of the biosimilar and the reference product. When that portrait shows high similarity across all measured attributes, the probability that clinical differences will emerge in a comparative trial is extremely low. The FDA, EMA, and MHRA have all now explicitly recognized this probability in their guidance frameworks.
Batch-to-Batch Variability: The Analytical Argument
One of the most compelling analytical arguments for reduced clinical requirements is the observation that approved originator biologics already exhibit measurable batch-to-batch variation. AbbVie’s Humira, for example, has shown documented glycosylation variability across manufacturing batches that was approved by regulators as not clinically meaningful [13]. If the FDA is comfortable with the originator’s own product varying in measurable ways between batches without requiring new clinical trials, it follows logically that a biosimilar showing similar or smaller variability from a well-characterized reference batch should not automatically require a full comparative efficacy trial.
This argument is now institutionalized in regulatory guidance. The FDA’s September 2025 final guidance on comparative analytical assessment specifies factors for determining when analytical similarity is sufficiently robust to reduce clinical requirements, including the number of reference product batches tested, the range of variability observed in the reference product, and the margin of difference between the biosimilar and reference product on key quality attributes [14].
The Investment Calculus
Building a comprehensive analytical characterization capability is expensive. High-resolution mass spectrometry instruments run USD 500,000 to several million dollars each. The scientists who operate them and interpret the data command salaries at the upper end of the pharmaceutical compensation scale. The analytical program for a single biosimilar candidate can cost USD 5–20 million and take two to three years to complete fully [15].
That investment looks different in the context of the clinical trial costs it can displace. A comparative efficacy trial that costs USD 80 million and takes four years is a far larger expenditure than the analytical program that might make it unnecessary. The expected value of front-loading analytical investment is strongly positive for companies with biosimilar pipelines of more than a few candidates, because analytical platforms are partially shared across programs while clinical trials are entirely program-specific.
This is the core strategic argument for building or acquiring analytical capabilities early. Companies that treat characterization as a checkbox requirement rather than a strategic asset will find themselves running clinical trials that better-equipped competitors do not need to run.
Part IV: Non-Clinical Studies — A Shrinking Requirement
The Regulatory Trajectory on Animal Studies
In early biosimilar regulation, comparative animal toxicology studies were a standard expectation. The logic was straightforward: before you expose patients to a biosimilar, confirm in animals that the product has no unexpected toxic effects relative to the reference product. That logic has been substantially eroded by accumulated evidence and scientific progress.
The FDA and EMA now largely waive comparative animal toxicology studies when biosimilarity is well-established by structural, functional, and in vitro mechanistic data [16]. The scientific rationale is that modern in vitro assays are more sensitive than animal studies at detecting biologically relevant differences for therapeutic proteins, and that the same accumulated experience showing no clinically meaningful differences in human PK/PD data has consistently corroborated in vitro similarity assessments.
Animal models present additional complications for biosimilar assessment. Most therapeutic biologics act through mechanisms that are species-specific, meaning animal pharmacology does not directly translate to human pharmacology. A comparative animal study that shows no toxicological difference between a biosimilar and its reference product in mice or rats has limited predictive value for the human immune response — particularly for immunogenicity, which is the primary safety concern unique to biologics. Cell-based assays using human immune cells are more informative.
The Remaining Regional Requirements
Not all regulatory authorities have moved at the same pace. Brazil’s ANVISA, China’s NMPA, and the Republic of Korea’s MFDS have historically retained requirements for comparative animal toxicology data that major Western agencies have waived [17]. Companies developing biosimilars for global markets — and most commercially viable biosimilars are developed with global launch in mind — must account for this divergence in their development timelines and budgets.
The practical implication is that ‘one regulatory package fits all markets’ is not achievable. A biosimilar development plan must explicitly map each market’s requirements and identify studies that serve multiple regulatory submissions versus studies that must be conducted specifically for regional compliance. DrugPatentWatch’s market intelligence tools are useful here for identifying which markets have approved specific reference biologic biosimilars, what clinical packages were accepted in each market, and where regulatory precedent exists for reduced data requirements [18].
The good news is that the regulatory trajectory runs in one direction: toward reduced animal study requirements. Regional outlier requirements are becoming progressively harder to defend in the context of accumulated clinical experience with biosimilars globally, and international harmonization efforts through ICH and the WHO are pushing agencies toward convergence.
Part V: PK and PD Studies — The Clinical Foundation
Why PK Studies Do the Heavy Lifting
Pharmacokinetic studies measure how the biosimilar moves through the body: absorption, distribution, metabolism, and elimination. They answer the question ‘does this drug behave the same way in the body?’ without needing to observe clinical outcomes. For most therapeutic proteins, PK equivalence is a strong predictor of clinical equivalence, because the mechanism of action operates through the same concentration-response relationship.
The standard design for a biosimilar PK study is a single-dose, randomized, two-period or parallel-group crossover study measuring key exposure parameters: AUC (area under the concentration-time curve from zero to infinity, AUCinf), maximum concentration (Cmax), and half-life (t½). Biosimilarity is concluded when the 90% confidence interval for the ratio of geometric means falls within predefined equivalence bounds — most commonly 80–125%, consistent with bioequivalence standards [19].
The choice of study population is a clinical strategy decision with direct cost implications. Healthy volunteers are preferred for most PK studies because they eliminate disease-state variability and concomitant medication effects, increasing the statistical sensitivity to detect PK differences between products. Larger variability in patient populations means larger sample sizes are needed to achieve equivalent statistical power. For a biosimilar where PK similarity is expected, recruiting healthy volunteers — when ethically permissible — typically produces the same regulatory conclusion with a smaller, faster, cheaper study than a patient-based design [19].
There are exceptions. When the reference biologic’s PK profile is substantially altered by the disease state — as can happen with some monoclonal antibodies targeting soluble antigens that are shed at different rates in diseased versus healthy tissue — a patient-based PK study is scientifically more appropriate and regulatorily expected.
PK Bridging: The Multi-Market Complexity
Companies seeking approval in both the U.S. and European markets face a specific complication: the FDA requires that biosimilarity be demonstrated against a U.S.-licensed reference product, and the EMA requires demonstration against an EU-authorized reference product. These are the same molecule from the same originator, but they may have been manufactured at different facilities or at different time periods, producing products with measurable but not clinically meaningful differences between them.
The solution is a PK bridging study: a three-arm PK comparison of the biosimilar, the U.S. reference product, and the EU reference product, which simultaneously establishes biosimilarity to each regional reference and demonstrates that the regional reference products are themselves equivalent. This bridging design adds cost and complexity but is now well-established regulatory practice and typically the most efficient path to multi-regional approval [20].
Bridging strategy requires careful reference product sourcing. The U.S. reference product, legally required to be purchased through U.S. commercial channels, carries a significant cost premium due to its originator price. Regulatory timelines must account for reference product procurement, comparability testing, and the bridging study itself. Companies that have not secured reference product supply before designing their clinical programs often encounter timeline delays that erode first-mover advantages.
PD Biomarkers: The Path to Fewer Trials
Pharmacodynamic studies measure the drug’s biological effect — receptor engagement, downstream signaling, relevant biomarker changes. Where a validated PD biomarker exists that correlates reliably with the reference product’s clinical mechanism of action, a PD study can provide additional biosimilarity evidence beyond PK data without requiring a full comparative efficacy trial.
The FDA has been explicit about its interest in PD biomarkers as a tool for reducing clinical trial burden. The agency has explicitly stated that it is assessing whether conventional Phase III comparative studies can be replaced with robust PD biomarker data in appropriate contexts [21]. The EMA’s 2025 reflection paper similarly identifies ‘sensitive functional assays’ as one of the prerequisites for waiving a comparative efficacy study [22].
The strategic implication is clear: investment in biomarker validation is investment in clinical trial efficiency. Companies with validated PD biomarkers for their target class, developed through their own research or through partnerships with academic groups or CROs, are in a materially better position to negotiate reduced clinical requirements with regulators.
A particularly well-documented case is the use of erythropoietin-stimulating agents, where hemoglobin response is a validated PD endpoint that has long been accepted as a basis for demonstrating biosimilarity without large equivalence trials in full patient populations. The same logic applies to G-CSF biosimilars using absolute neutrophil count, and to some TNF-alpha inhibitor classes where validated composite inflammatory biomarkers are available.
Part VI: The Comparative Efficacy Study — When It’s Required and When It Isn’t
The Regulatory Shift of 2025
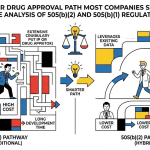
For the first decade of biosimilar regulation in the U.S., the expectation was that biosimilar applicants would include at least one comparative clinical efficacy study in their data package. The burden of proof ran in one direction: if you wanted to waive the study, you had to justify it scientifically, and FDA was not frequently convinced. The default was to run the trial.
In October 2025, the FDA inverted that presumption. Its draft guidance on ‘Scientific Considerations in Demonstrating Biosimilarity: Updated Recommendations for Assessing the Need for Comparative Efficacy Studies’ states that for therapeutic protein products manufactured from clonal cell lines, where the products are highly purified and can be well-characterized analytically, a comparative efficacy study ‘may not be necessary’ [9]. The new default, for products meeting those criteria, is that a CES is unnecessary unless the sponsor can identify scientific justification for why one is required.
That is a structural reversal of FDA’s historical stance. The agency explained its reasoning: a decade of biosimilar approvals and post-market experience has produced no evidence that any biosimilar with demonstrated analytical and PK similarity has shown clinically meaningful differences in comparative efficacy trials. The trials have been uniformly confirmatory — they have confirmed what the analytical data already showed. Running them anyway serves no patient safety purpose while costing hundreds of millions of dollars in aggregate development expense across the industry.
The EMA moved in parallel. In April 2025, the agency published its draft reflection paper on a ‘tailored clinical approach in biosimilar development,’ formally proposing that comparative efficacy studies may be waived when the following prerequisites are met:
- The active substance’s mechanism of action is well understood
- Analytical similarity is demonstrated across all key quality attributes
- Sensitive functional assays are available and show comparable results
- The manufacturing process is validated and controlled
- PK studies demonstrate comparable exposure profiles [22]
The EMA reflection paper received approximately 400 comments during its consultation period, which ran through September 2025. The feedback was broadly supportive [23]. Implementation is targeted for 2026. The FDA’s October 2025 draft guidance is expected to be finalized in early 2026 [24].
Together, these changes represent the most significant structural reform of biosimilar clinical development requirements since the FDA issued its foundational 2012 biosimilar guidance.
When a CES Is Still Required
The shift away from routine comparative efficacy studies does not mean these trials are obsolete. There are specific circumstances where regulators will continue to require them, and development teams that misread the guidance scope will face nasty surprises at pre-BLA meetings.
A comparative efficacy study remains necessary when:
The mechanism of action differs meaningfully across the reference product’s indications, and the clinical data from one indication cannot be extrapolated to others without some clinical validation in a second indication. This scenario is discussed in detail in the extrapolation section below.
Analytical and functional similarity data leave residual uncertainty about specific quality attributes that are known to be clinically relevant for the product class. An example would be a biosimilar where glycosylation patterns are significantly different from the reference product in ways that could affect either efficacy or immunogenicity, and where in vitro functional assays cannot fully resolve whether those differences are clinically meaningful.
The reference product’s mechanism of action is not sufficiently understood to support a scientific assessment of whether analytical differences would translate to clinical differences. This situation is more common for complex biologics with multiple simultaneous targets or poorly characterized downstream signaling pathways.
The sponsor is seeking interchangeable designation in the U.S. under the historical standard, where additional clinical evidence may add weight to the safety assessment, though this is now far less likely to require a dedicated efficacy study following the June 2024 interchangeability guidance update [25].
Equivalence vs. Non-Inferiority: A Statistical Choice With Commercial Consequences
When a comparative efficacy study is required, the trial must be designed around either an equivalence or non-inferiority statistical framework, and that choice has both scientific and commercial implications.
Non-inferiority trials are designed to show that the test product is not worse than the comparator by more than a predefined margin. They are the standard design for most active-controlled clinical trials. For biosimilars, however, non-inferiority design alone is generally insufficient. A biosimilar that is non-inferior to its reference product could theoretically also be superior, and regulatory authorities require that biosimilars not demonstrate superiority because superiority would imply meaningful differences that could have unforeseen safety implications, including immunogenicity effects [26].
Equivalence trials use a two-sided approach: the biosimilar must be neither worse nor better than the reference product by more than the equivalence margin. This requires larger sample sizes than non-inferiority trials but produces cleaner biosimilarity conclusions. The FDA preference for equivalence designs in biosimilar efficacy trials is well-established in its 2015 scientific considerations guidance and has been reaffirmed in subsequent guidance documents [27].
A more nuanced design, described in the biostatistical literature, uses asymmetric margins: a standard non-inferiority margin on the lower end and a tighter non-superiority margin on the upper end. This acknowledges the practical reality that detecting clinically meaningful superiority is less important than detecting clinically meaningful inferiority, while still requiring that large apparent efficacy differences in either direction be investigated [28].
The equivalence margin itself — the boundary that defines ‘no clinically meaningful difference’ — must be derived from the reference product’s historical clinical data, typically using a meta-analysis of the originator’s pivotal trials. This derivation is itself a major analytical undertaking. It requires access to the originator’s published clinical trial data, proprietary unpublished data where available, and sophisticated meta-analytic methodology. The resulting margin must be clinically justified, not merely statistically convenient.
A poorly chosen equivalence margin can sink an otherwise well-executed biosimilar program. Set the margin too tight and the trial is underpowered, requiring an enormous sample size. Set it too wide and regulators will reject the comparison as insufficiently sensitive. Getting the margin right requires biostatistical expertise that goes well beyond standard phase III trial design competency.
Patient Population Selection: The ‘Most Sensitive Model’ Principle
The FDA’s guidance explicitly directs biosimilar sponsors to conduct comparative efficacy studies in the patient population and indication that provides the most sensitive detection of clinically meaningful differences — the ‘most sensitive model’ [29]. The scientific rationale is that a less sensitive population would allow real differences to go undetected, making the study meaningless as a biosimilarity demonstration.
A well-documented example is adalimumab (Humira) biosimilar development. The key clinical questions were: which indication among Humira’s 13 approved uses would provide the most sensitive signal for detecting efficacy differences? Analysis of the originator’s clinical data identified psoriasis (PsO) as the most sensitive model, for two reasons: PsO trials showed higher placebo-adjusted response rates (61–64%) than RA or Crohn’s disease trials, maximizing the statistical signal-to-noise ratio; and PsO patients are typically not on concomitant immunosuppressive therapy, which in RA patients can mask immunogenicity-related efficacy differences [30].
Several adalimumab biosimilar sponsors ran their comparative efficacy studies in PsO, then sought extrapolation to Humira’s other approved indications. That strategy succeeded, producing approvals that covered the full label of the reference product from a single clinical study in a single indication.
The commercial consequence of selecting the wrong patient population goes beyond regulatory approval risk. Recruiting patients with the relevant disease from specialist centers, running them through a comparative trial design with mandatory washout periods and frequent monitoring, and following them long enough to see meaningful endpoint data all cost money that is proportional to the trial size. A study in the most sensitive population achieves the same regulatory conclusion with fewer patients and less time than a study in a less sensitive population.
Part VII: Immunogenicity — The Safety Question That Never Goes Away
Why Anti-Drug Antibodies Matter
All therapeutic proteins carry some risk of eliciting an immune response in patients. The body’s immune surveillance system treats large foreign proteins with suspicion, and even fully human monoclonal antibodies — which are structurally identical to proteins the immune system naturally produces — can trigger anti-drug antibody (ADA) development in a meaningful fraction of patients.
The clinical consequences of ADA formation range from trivial to severe. In the least concerning scenario, ADAs form but do not bind to the drug’s active site and have no detectable clinical effect. In the most severe scenario, neutralizing antibodies bind directly to the drug’s mechanism-of-action domain, completely blocking its efficacy, while simultaneously cross-reacting with the patient’s own endogenous protein — a potentially life-threatening autoimmune response. This last scenario, while rare, has occurred with erythropoietin products and drove the regulatory framework that now mandates comprehensive immunogenicity assessment for all biologics [31].
For biosimilar development, immunogenicity assessment serves a dual purpose. First, it assesses whether the biosimilar’s structural attributes — particularly any differences in glycosylation, protein aggregates, or host cell proteins compared to the reference product — increase the patient’s risk of developing ADAs relative to the reference product. Second, it generates comparative data that regulators use to confirm that the immunogenicity profile is ‘no worse than’ the reference product, which is the applicable standard.
The Assay Technology Challenge
Immunogenicity assessment requires validated, sensitive assays capable of detecting the full spectrum of ADA responses: non-neutralizing antibodies (detected in screening assays), neutralizing antibodies (detected in specialized Nab assays that measure the drug’s functional activity in the presence of patient serum), and cross-reactive antibodies to endogenous proteins.
Assay technology for immunogenicity has advanced enormously in the past two decades. Current electrochemiluminescence-based bridge assays can detect ADAs at concentrations several orders of magnitude lower than the radioimmunoassays used in the early regulatory era. This creates a practical compliance challenge for biosimilar developers: the FDA and EMA now expect biosimilar immunogenicity assays to use contemporary, highly sensitive methods, even though the reference product’s ADA data was generated with older, less sensitive assays.
The result is that a biosimilar developer using state-of-the-art assays may detect low-level ADAs that the originator’s clinical trials would have missed entirely — not because the biosimilar is more immunogenic, but because the detection threshold has moved. Regulators understand this, and FDA guidance explicitly addresses the issue by asking sponsors to evaluate the clinical relevance of any detected ADAs and assess whether the rates and titers are clinically meaningfully different from the reference product’s profile [32].
Study Design for Immunogenicity
The standard recommendation for comparative immunogenicity assessment is a parallel-arm clinical study in a patient population sensitive to ADA development [33]. Several design elements are specified in FDA and EMA guidance:
The patient population should be treatment-naïve and not receiving concomitant immunosuppressive therapy, since immunosuppressants reduce ADA formation rates and could mask real differences in immunogenicity between products.
The follow-up duration should be at least one year for products that are chronically administered. Neutralizing ADAs can develop weeks to months after initial exposure, and delayed-onset immune responses would be missed by shorter follow-up windows.
Sampling should be frequent enough to capture the timing and kinetics of ADA development, not merely whether ADAs are present at a single endpoint.
The assays must include screening, confirmatory, and Nab tests, applied in a validated tiered algorithm.
Meeting all of these requirements within a feasible trial design requires careful planning. Adding immunogenicity assessments to a PK or comparative efficacy study — collecting additional blood samples for ADA testing alongside PK samples — is typically more efficient than running a separate immunogenicity study, and regulators generally prefer this integrated approach.
Post-Market Immunogenicity: The Long Tail
Pre-market immunogenicity data has inherent limitations. Clinical trials are too small and too short to detect rare delayed-onset immune responses. Post-marketing surveillance is the mechanism through which these events are identified and characterized.
FDA’s naming convention for biosimilars — a core nonproprietary name plus a four-letter distinguishing suffix, such as adalimumab-adaz for Hyrimoz — was specifically designed to enable precise pharmacovigilance. When an adverse event report mentions a biologic product by name, the suffix allows exact identification of which product was involved. Without that specificity, safety signals cannot be reliably attributed to individual products, and pharmacovigilance data becomes noise rather than signal.
European regulators have implemented similar traceability requirements through mandatory brand-name recording at the point of dispensing. The underlying principle is identical: you cannot monitor biosimilar safety effectively if you cannot identify which biosimilar a patient received.
Part VIII: Indication Extrapolation — The Commercial Multiplier
The Logic of Extrapolation
A blockbuster biologic like adalimumab is approved for 13 separate indications spanning rheumatology, gastroenterology, and dermatology. Running a separate comparative efficacy trial for each of those indications would cost roughly USD 1 billion in aggregate — a number that would make biosimilar economics unworkable for most of them.
Extrapolation solves that problem. If a biosimilar is demonstrated to be comparable to its reference product in one indication through a well-designed comparative study (or, increasingly, through analytical and PK data alone), and if the mechanism of action is the same across all of the reference product’s indications, then regulators will extrapolate the biosimilarity finding to the other indications without requiring separate clinical proof in each [34].
The FDA, EMA, PMDA, Health Canada, and WHO all accept the principle of extrapolation, though they have historically differed in the specific requirements they impose [34]. That convergence at the level of principle, with some divergence at the level of implementation detail, is exactly what makes this area navigable for a development team with strong regulatory intelligence capabilities.
What Justifies Extrapolation
The scientific case for extrapolation rests on four pillars, all of which must be defensible:
The mechanism of action must be the same — or at minimum, scientifically well understood — across all proposed indications. An antibody that blocks TNF-alpha in rheumatoid arthritis blocks TNF-alpha in Crohn’s disease and psoriasis by the same molecular mechanism. If the mechanism of action is incompletely characterized or differs meaningfully between indications, extrapolation requires additional scientific justification [35].
The PK/PD relationship must be similar in the relevant patient populations. If the drug’s behavior in the body differs substantially between, say, patients with rheumatoid arthritis and patients with pediatric Crohn’s disease — in ways that could affect whether the biosimilar and reference product remain comparable — then extrapolation to the pediatric population requires additional PK data in that population.
The immunogenicity risk must be comparable across indications. If an indication involves a patient population with fundamentally different immune characteristics — for example, immunocompromised oncology patients versus otherwise healthy RA patients — regulators may require immunogenicity data in the population being extrapolated to [36].
No safety signals should differ between indications in ways that are attributable to product characteristics rather than disease-specific factors. Extrapolation of a safety profile to an indication with substantially different patient vulnerabilities requires clinical justification.
The PMDA and Health Canada Positions
Japan’s PMDA is explicit in its biosimilar guidelines: extrapolation is acceptable if clinical comparability in one indication can be demonstrated and pharmacological effects are expected to be comparable across other indications [37]. However, PMDA requires that if the mechanism of action is unclear or differs across indications, comparability must be demonstrated separately for each indication. This is more conservative than the FDA’s current stance following the October 2025 draft guidance, which would allow waiving of clinical comparability altogether in appropriate cases.
Health Canada allows sponsors to apply for all indications held by the Canadian-authorized reference biologic, provided a sound scientific justification for extrapolation is submitted with the application [38]. The Canadian framework does not require that the justification come from a completed comparative clinical trial; robust analytical and PK data can support extrapolation to the full label.
Understanding these regional variations is essential for companies developing global biosimilar dossiers. A regulatory strategy that works for FDA and EMA submissions may require supplementation for the PMDA filing if the mechanism of action documentation is insufficient, or for certain emerging market submissions that have not yet adopted the global consensus position on extrapolation.
Part IX: Interchangeability — The U.S.-Specific Designation and Its Transformation
What Interchangeability Means
Interchangeability is a regulatory designation that exists almost exclusively in the United States. An interchangeable biosimilar may be substituted for its reference product at the pharmacy level without the prescriber’s prior authorization, subject to state pharmacy laws [39]. In practical terms, a pharmacist filling a prescription for the reference product can substitute an interchangeable biosimilar without calling the doctor’s office — just as a pharmacist can substitute a generic for a small-molecule brand-name drug.
The economic value of interchangeability is primarily operational, not clinical. Interchangeable biosimilars tend to achieve faster formulary placement and higher rates of pharmacy-level substitution. Payers and pharmacy benefit managers can drive formulary substitution more aggressively for interchangeable products than for biosimilars without that designation.
In Europe, this question does not arise. The EMA considers all approved biosimilars scientifically interchangeable with their reference products, meaning regulatory approval itself confers interchangeability. No separate designation, no additional data package, no switching study required — biosimilar approval and interchangeable status are the same thing.
The June 2024 Draft Guidance: Removing Switching Studies
In June 2024, the FDA issued draft guidance proposing to remove the requirement for a clinical switching study as a prerequisite for interchangeable designation [25]. This followed a decade of data showing that switching between reference products and biosimilars produces no detectable immunogenicity or efficacy differences. Of the 13 biosimilars designated interchangeable as of mid-2024, 9 had been approved without switching study data — demonstrating that the agency had already been applying a de facto waiver policy before formalizing it [40].
FDA’s Sarah Yim, director of the Office of Therapeutic Biologics and Biosimilars, stated that the draft guidance, when finalized, would ‘provide clarity and transparency about the FDA’s thinking and align the review and approval process with existing and emerging science.’
The Federal Trade Commission endorsed the FDA’s draft guidance in August 2024, stating that the new draft would streamline the approval process by reducing administrative burden and lowering the cost of demonstrating that switching between a biologic and a biosimilar is safe and effective.
The practical consequence is that companies seeking interchangeable designation can now submit an analytical assessment of why their existing comparative analytical and clinical data supports the interchangeability standard, rather than conducting a dedicated switching study. For companies with robust analytical packages and clinical PK/immunogenicity data, this route may require no additional clinical work.
Merging Biosimilarity and Interchangeability
The October 2025 FDA draft guidance on comparative efficacy studies, taken together with the June 2024 interchangeability guidance, points toward a near-complete collapse of the distinction between biosimilar and interchangeable biosimilar status. As the Jones Day analysis of these developments noted, if the draft guidances are finalized as written, high-quality analytical comparability paired with pharmacokinetic and immunogenicity assessments will generally suffice; clinical efficacy and switching studies would become the exception, at least for therapeutic proteins.
The first-mover implication of this structural change is significant and underappreciated. Under the old framework, the first biosimilar to achieve interchangeable designation — which required switching study data — held a first-interchangeable exclusivity period of one year before a second biosimilar could be designated interchangeable. If all biosimilars are effectively deemed interchangeable upon approval, the basis for that exclusivity period may erode. FDA plans to finalize the guidance documents in early 2026 to align the biosimilar pathway more with the generics model, and may begin approving all non-vaccine biosimilars as interchangeable products.
Companies that had been building clinical programs around winning first-interchangeable exclusivity need to re-evaluate that strategy now, before the guidance finalizes and the strategic landscape is locked in.
Part X: Post-Market Surveillance — The Regulatory Commitment That Lasts Forever
Pharmacovigilance Is Not Optional
FDA approval or EMA marketing authorization is not the end of a biosimilar’s regulatory obligations; it is the beginning of the post-market phase. Biosimilar manufacturers are required to maintain comprehensive pharmacovigilance programs throughout the product’s commercial life, with the primary objectives of detecting safety signals not identified in pre-approval clinical trials and confirming that the safety and immunogenicity profile observed in clinical development is consistent with real-world experience [41].
The specific obligations include: expedited 15-day alert reports for serious and unexpected adverse experiences; periodic safety update reports (PSURs in Europe, periodic benefit-risk evaluation reports in the U.S.) submitted on fixed schedules; and active surveillance programs targeting known areas of risk.
For biologics, the primary known area of risk is immunogenicity. The tiered post-market immunogenicity monitoring program should include systematic ADA surveillance in the treated population, with mechanisms for linking detected ADAs to clinical outcomes (reduced efficacy, infusion reactions, cross-reactive autoimmunity). The naming convention and traceability systems discussed earlier are the infrastructure that makes this surveillance possible.
Risk Management Plans
The EMA requires a detailed Risk Management Plan (RMP) as part of the biosimilar marketing authorization application. The RMP identifies all known and potential safety concerns, proposes specific monitoring activities and risk minimization measures for each concern, and establishes criteria for evaluating the effectiveness of those measures [42].
For biosimilars, the RMP typically focuses on:
Immunogenicity monitoring, including the methodology for ADA detection and classification.
Monitoring for any safety signals specific to the biosimilar’s manufacturing process — host cell proteins, process-related impurities, or aggregation profiles that differ from the reference product.
Signals specific to the therapeutic class — for example, neutropenia risk for G-CSF biosimilars or infection risk for TNF-alpha inhibitor biosimilars.
Risk minimization measures can range from standard product labeling updates to structured educational programs for healthcare providers. In cases where serious risks require active management, regulators may impose Risk Evaluation and Mitigation Strategies (REMS) — specific safety programs that go beyond standard labeling to require prescriber certification, patient enrollment in registries, or specific monitoring requirements before each prescription can be filled [43].
The FDA’s June 2025 decision to remove REMS requirements for certain autologous CAR T-cell immunotherapies illustrates that REMS can evolve and be removed as safety evidence accumulates. Biosimilar manufacturers should view their RMPs as living documents, updated on the basis of accumulating real-world data, and should engage proactively with regulators when post-market data supports relaxing monitoring requirements.
Part XI: The Patent Landscape — Turning Intelligence Into Advantage
Beyond the Core Patent
A common misunderstanding among executives new to biosimilar strategy is that biosimilar market entry becomes possible when the reference product’s core composition-of-matter patent expires. In practice, originator companies routinely file dozens to hundreds of secondary patents covering manufacturing processes, specific formulations, methods of use, dosing regimens, and delivery devices. These secondary patents extend practical market exclusivity well beyond the expiration of the foundational molecular patent.
Humira (adalimumab) is the textbook case. AbbVie’s core adalimumab composition-of-matter patent expired years before biosimilars entered the U.S. market. But AbbVie maintained a portfolio of more than 130 additional patents covering formulations, manufacturing methods, methods of treatment, and the auto-injector device. That portfolio created a patent thicket that delayed U.S. biosimilar entry until 2023, roughly a decade after the first Humira biosimilar received FDA approval [44].
The lesson is that patent expiry dates matter, but they are only the starting point for a realistic market entry timeline. The full IP landscape — including formulation patents, manufacturing process patents, device patents, and any regulatory exclusivity periods layered on top of patent protection — must be mapped comprehensively before committing to a development program.
Data Exclusivity: A Separate Clock
In the U.S., biosimilars are subject to a 12-year regulatory exclusivity period from the date of the reference product’s first FDA approval. This exclusivity is independent of patent protection: even if every relevant patent has expired or been invalidated, a biosimilar applicant cannot receive full FDA approval until 12 years have elapsed from the reference product’s approval [45]. A 4-year exclusivity period prevents biosimilar applications from even being submitted before that point.
In Europe, the relevant periods are shorter: 8 years of data exclusivity (during which a biosimilar application can be submitted but not approved) plus 2 years of additional market protection, for a 10-year total [46]. This difference in exclusivity periods between U.S. and European markets is one reason European biosimilars historically entered the market earlier.
Understanding the interaction between patent expiry and exclusivity periods requires tracking both clocks simultaneously. A biosimilar that becomes eligible for approval from a patent standpoint before the 12-year exclusivity period expires is stuck waiting regardless of its clinical development progress. Conversely, a biosimilar that could theoretically enter the market from an exclusivity standpoint may still face patent litigation that delays actual launch.
The ‘Patent Dance’ Under BPCIA
The Biologics Price Competition and Innovation Act (BPCIA) of 2009 established a structured information exchange process between biosimilar applicants and reference product sponsors — colloquially called the ‘patent dance’ — designed to facilitate early identification and resolution of patent disputes [47].
Under the original framework, a biosimilar applicant who files an abbreviated Biologics License Application (aBLA) must provide the reference product sponsor with detailed information about the biosimilar’s manufacturing process, and the two parties then engage in a structured exchange identifying patents that the sponsor believes are potentially infringed and that the applicant believes can be challenged. The intent was to resolve patent disputes before biosimilar launch, avoiding the disruption of market entry followed by injunctive relief.
The Supreme Court’s 2017 ruling in Sandoz Inc. v. Amgen Inc. held that the patent dance is optional — a biosimilar applicant may choose not to participate, though doing so carries specific procedural consequences for later patent litigation. This ruling gave biosimilar applicants more strategic flexibility but did not resolve the underlying reality: originator companies use their patent portfolios aggressively to delay biosimilar entry, and biosimilar companies must decide whether to challenge those patents proactively through PTAB proceedings, wait for natural expiration, or negotiate licensing agreements.
Research published in the Journal of Law and the Biosciences estimated that allowing biosimilar firms to initiate patent litigation earlier — specifically, at the start of Phase 3 clinical trials rather than after their completion — could reduce market entry delays by approximately 1.8 years on average [48]. Given that typical Phase 3 biosimilar trials take 4–5 years to complete, the litigation timeline under BPCIA creates a substantial gap between regulatory approval readiness and actual market entry.
Using DrugPatentWatch for Competitive Intelligence
Navigating this landscape requires structured patent intelligence, not ad hoc searching. DrugPatentWatch provides systematic patent tracking for pharmaceutical products, including biosimilar reference products, with data on patent expiry dates, patent linkage to FDA-approved products, litigation history, and inter partes review proceedings at the Patent Trial and Appeal Board [49].
Practically, a biosimilar development team using DrugPatentWatch can do several things that improve decision quality. They can identify the complete patent portfolio protecting a reference product and determine which patents represent genuine market entry barriers versus weak patents likely to be invalidated on challenge. They can track PTAB proceedings initiated by other biosimilar companies against the same patent portfolio, anticipating whether key patents might be narrowed or invalidated before their own product reaches the market. They can monitor reference product label changes, which sometimes trigger new regulatory exclusivity periods. They can identify ‘biosimilar voids’ — reference products approaching the end of both patent and data exclusivity where no biosimilar candidate is currently in late-stage development — representing potential market opportunities with limited near-term competition.
This kind of systematic competitive intelligence is the difference between entering a market against eight competitors and entering with two. Both scenarios are possible with the same reference product; the difference is knowing, years in advance, which competitors are serious and which will drop out, and planning development timelines and commercial strategies accordingly.
Part XII: Global Regulatory Harmonization — Progress and Persistent Gaps
Where the Major Agencies Agree
The good news for global biosimilar developers is that the major regulatory agencies — FDA, EMA, PMDA, Health Canada, TGA — converge on the most important scientific principles. The ‘totality of evidence’ approach is universally accepted. Extrapolation of indications is accepted by all of them. Reduced clinical requirements based on robust analytical data are increasingly accepted by all of them. The direction of travel, in every major market, is toward streamlined clinical development [50].
The EMA-FDA Parallel Scientific Advice program formalizes this convergence for individual product development programs. Companies can engage both agencies simultaneously on a single development plan, receiving coordinated feedback that reduces the risk of designing studies that meet one agency’s requirements but not another’s. Availability of this joint advice is limited, and applications are competitive, but companies with complex biosimilar programs should actively pursue it.
Where the Gaps Remain
The less welcome reality is that implementation details diverge in ways that create real additional costs and complexity for global programs.
Reference product sourcing requirements create forced duplication. The FDA requires comparability data against U.S.-sourced reference product; the EMA requires it against EU-sourced product. In markets like Japan, Brazil, and some emerging economies, locally sourced reference product may be required, adding yet another supply chain and analytical comparison exercise [51].
Clinical study design expectations differ in detail even where they converge in principle. Some emerging market regulators expect confirmatory clinical data in local patient populations, citing ethnic pharmacogenomic differences or disease pattern variations that may affect how the drug behaves. These requirements are scientifically questionable for most well-characterized monoclonal antibodies but are regulatory reality in markets that represent significant commercial opportunity — particularly China, Brazil, and India.
Good Manufacturing Practice standards — the manufacturing compliance framework that governs how the biosimilar is produced — vary in specific requirements across markets. A manufacturing facility approved by FDA and EMA may still need supplementary inspection by PMDA or by China’s NMPA before those markets will approve the product. Each additional inspection adds timeline risk and resource requirements.
ICH and the WHO: Moving the Floor
The International Council for Harmonisation of Technical Requirements for Pharmaceuticals for Human Use (ICH) produces guidelines that, when adopted by member agencies, create genuine regulatory harmonization. ICH Q5E, which governs the comparability of biotechnological products following manufacturing process changes, is foundational to biosimilar development science and is implemented by all major agencies [52]. ICH E6 good clinical practice standards govern biosimilar clinical trial conduct globally.
The WHO’s Collaborative Procedure for Accelerated Registration — which allows emerging market regulators to rely on the scientific review conducted by FDA, EMA, or other WHO-listed authorities — is particularly relevant for biosimilar market access in resource-limited settings. A biosimilar approved by the FDA can receive expedited review in WHO collaborative procedure countries by submitting the FDA’s full assessment report. This mechanism substantially reduces the duplication of regulatory review burden and has been actively promoted by the WHO as a tool for expanding biosimilar access in lower-income markets [53].
The cumulative effect of these harmonization mechanisms is that a biosimilar development program designed to meet FDA and EMA requirements is substantially aligned with the requirements of most other major markets. The residual divergences are manageable, but they require active regulatory intelligence to anticipate and address early enough in development to avoid costly last-minute modifications to the data package.
Part XIII: Development Economics — The Business Case in Numbers
The Cost Structure of Biosimilar Development
Biosimilar development is expensive by any pharmaceutical standard, but it is substantially cheaper than developing a new biologic from scratch. A novel therapeutic biologic drug costs USD 2.6 billion or more to develop through to approval, by the widely cited DiMasi analysis [54]. A biosimilar development program for a well-characterized monoclonal antibody has historically cost USD 100–250 million, a fraction of that figure, but still a commitment that requires careful economic analysis.
Under the regulatory frameworks taking shape in 2025 and 2026 — where CES requirements and switching study requirements are being substantially reduced — the upper end of that cost range should fall significantly. ICON’s analysis of the FDA’s draft CES guidance estimates that the objective of reducing development timelines from 5–8 years to 2–4 years implies substantial cost reductions on the order of tens of millions of dollars per program [8]. A more optimistic analysis published in Pharmaceutics suggests that if the U.S. adopted an EMA-MHRA-style approach of waiving CES requirements when scientifically justified, approximately USD 4.5 billion in annual healthcare savings could be realized through expanded biosimilar competition — reflecting both faster market entry and lower development costs [4].
The cost structure within a biosimilar development program allocates resources roughly as follows. Analytical characterization and process development collectively represent 20–30% of total program costs. Clinical PK studies represent 10–20%. Comparative efficacy studies, when required, represent 30–50%. Regulatory strategy and documentation, manufacturing scale-up, and commercial preparation make up the remainder. Eliminating or substantially reducing the comparative efficacy study shifts the cost distribution toward the analytical and manufacturing components, which are more amenable to platform efficiencies and shared costs across programs.
The Portfolio Argument
Individual biosimilar economics are challenging. Biosimilars typically enter markets at a 15–30% discount to the reference product, though competition between multiple biosimilars for the same reference product can drive discounts to 50–80% in U.S. Medicaid and VA formularies, and to similar levels in European tender markets [55]. Capturing meaningful commercial value requires achieving significant market penetration quickly, before other biosimilars erode price points further.
The economics improve substantially for companies with biosimilar portfolios rather than single programs. Analytical platform capabilities, regulatory expertise, manufacturing infrastructure, and commercial relationships are partially shared across multiple programs. A company running 10 biosimilar programs simultaneously amortizes its analytical platform investment across 10 revenue streams rather than one. Its regulatory affairs team builds expertise and relationships with FDA and EMA review divisions that carry over from program to program. Its manufacturing facilities run at higher utilization.
This portfolio logic explains the market structure of the global biosimilar industry. The largest biosimilar developers — Sandoz, Celltrion, Samsung Bioepis, Biocon, Pfizer — are companies with portfolios of 10 or more programs, backed by manufacturing infrastructure capable of supporting multiple products simultaneously. Single-program biosimilar developers face structural cost disadvantages that make commercial success increasingly difficult.
Commercial Strategy: Pricing, Contracting, and Channel
The commercial challenge for biosimilars is less about regulatory approval and more about market access and utilization. Even with FDA approval and favorable formulary placement, biosimilar uptake in the U.S. has lagged European adoption rates substantially for years, driven by:
Rebate dynamics. Originator companies offer pharmacy benefit managers deep rebates on reference products that, in some cases, make the reference product’s net cost to the PBM comparable to or lower than the biosimilar’s list price. This perverse incentive has suppressed biosimilar uptake in certain categories, including adalimumab, where biosimilars have struggled to achieve rapid penetration despite significant list price discounts.
Physician hesitancy. Despite accumulating evidence that biosimilars perform identically to their reference products, some physicians remain reluctant to initiate biosimilar therapy in patients who have been stable on the reference product. The nocebo effect — reduced therapeutic response attributable to patient expectation of reduced efficacy, rather than actual pharmacological differences — is real and documented [56].
Coverage and access requirements. Hospital formulary committees, specialty pharmacy benefit managers, and payer prior authorization processes each add friction to biosimilar adoption, friction that the reference product does not face because it is already established on formulary.
Interchangeability designation addresses some of these barriers by enabling pharmacy-level substitution for new prescriptions. The FDA’s proposed regulatory changes in 2024 and 2025, which will effectively make all approved biosimilars interchangeable, should accelerate formulary adoption by removing the administrative distinction between biosimilars and reference products at the pharmacy level.
Part XIV: Recent Case Studies in Biosimilar Clinical Development
Adalimumab: The Largest Patent Thicket in Pharmaceutical History
The adalimumab biosimilar experience is the most thoroughly documented and commercially significant case study in biosimilar development history. AbbVie’s Humira was the world’s best-selling drug for more than a decade, generating peak annual revenues exceeding USD 20 billion. Its biosimilar development story illustrates nearly every challenge discussed in this article.
On the clinical side, multiple adalimumab biosimilar sponsors ran comparative efficacy studies in rheumatoid arthritis or psoriasis, establishing the design precedents discussed above. Several sponsors used the psoriasis-as-most-sensitive-model approach, achieving FDA approval for the full Humira label from a single clinical program. Sandoz’s Hyrimoz, for example, received EMA approval with a clinical package weighted toward analytical and PK data, representing an early example of EMA’s flexibility in reducing comparative efficacy requirements for a product where structural and functional similarity was comprehensively demonstrated [22].
On the IP side, AbbVie’s 130+ patent portfolio delayed U.S. biosimilar entry until January 2023, at which point more than a year of settlement agreements with biosimilar developers came into effect. The first biosimilar launches occurred simultaneously from multiple manufacturers — Boehringer Ingelheim, Sandoz, Pfizer, Amneal, and others — producing immediate intense price competition that drove reference product net prices down substantially. The patent thicket strategy succeeded in its core objective: it extracted approximately eight additional years of exclusivity revenue in the U.S. market beyond what the core patents would have supported [44].
Ustekinumab: The First Approved CES Waiver
The FDA granted a waiver of clinical studies for a biosimilar version of the monoclonal antibody ustekinumab (Stelara). This was the first reported instance of the FDA exercising its waiver authority under the Food, Drug, and Cosmetic Act to reduce the evidence normally required for biosimilarity, and to the authors’ knowledge at the time of publication, the first biosimilar monoclonal antibody approved without any clinical efficacy study.
This approval — whose timing in 2025 immediately preceded the FDA’s draft CES guidance — functioned as a proof of concept for the broader guidance that followed. It demonstrated that the FDA’s internal scientific review process was capable of concluding, in a specific case, that comprehensive analytical and PK data removed the need for a comparative efficacy study. The October 2025 draft guidance then codified that case-by-case reasoning into a formal framework.
The ustekinumab precedent has direct implications for companies developing biosimilars to other IL-12/23 antibodies and, more broadly, to any well-characterized therapeutic protein where the structure-function relationship is comprehensively understood.
Infliximab in Europe: 15 Years of Real-World Switching Evidence
The first infliximab biosimilar (Remsima, developed by Celltrion) received EMA approval in 2013. The European experience since then has produced the most extensive real-world dataset on biosimilar switching and post-market safety of any biosimilar class [57].
The NOR-SWITCH study — a Norwegian randomized controlled trial of patients switching from originator infliximab to Remsima — remains the most rigorous switching study conducted for any biosimilar. It found no clinically meaningful differences in disease control across all five approved indications in the study population. Several subsequent European observational datasets confirmed those findings in larger, less controlled real-world populations.
This body of evidence was directly cited by the FDA in its reasoning for the June 2024 interchangeability guidance change. Europe’s willingness to run large, high-quality switching studies in the early biosimilar period produced the evidence that ultimately made switching studies unnecessary going forward — by proving conclusively that switching is safe, the European experience made further testing redundant.
Part XV: Strategic Recommendations
For Biosimilar Developers
Re-evaluate whether your pipeline programs still require comparative efficacy studies. The October 2025 FDA draft guidance and EMA’s 2025 reflection paper create a credible path to CES waivers for well-characterized therapeutic proteins. Programs that had CES built into their development plans as a default requirement should be reviewed against the criteria in both guidance documents before those trials are initiated. Starting a CES that is not scientifically necessary is equivalent to spending USD 50–100 million on data that will not change the regulatory outcome.
Invest in analytical infrastructure before clinical infrastructure. The regulatory shift toward analytical-data-driven approvals makes analytical characterization capabilities a primary competitive asset, not a supporting function. Companies with state-of-the-art analytical platforms and skilled scientists capable of generating and interpreting comprehensive comparability data are in a structurally better regulatory position than companies that contract analytical work out to CROs without building internal expertise.
Build regulatory intelligence into your pipeline selection process. Not every reference biologic represents an equally attractive biosimilar opportunity. The patent landscape, data exclusivity period, existing and emerging biosimilar competition, and each market’s regulatory requirements all need to be assessed systematically before a program is initiated. Tools like DrugPatentWatch provide the structured patent and approval data needed to make that assessment rigorously, rather than relying on general knowledge of a drug’s commercial profile.
Plan for global from Day 1. A biosimilar development program designed solely for U.S. or European approval will face costly retrofitting if the program’s commercial success depends on additional markets. The PK bridging strategy, reference product sourcing plan, and manufacturing quality systems should be designed with the full intended market list in mind from the outset.
Engage regulators early and often. Both the FDA and EMA have pre-consultation programs specifically designed for biosimilar development questions. Using these programs — including the FDA’s Biosimilar Initial Advisory (BIA) meetings — to align on development strategy before completing analytical studies saves time that is otherwise spent re-running experiments after receiving unexpected feedback at formal review meetings.
For Business Development and Investment Professionals
The biosimilar market is entering its most productive regulatory phase since the BPCIA was passed in 2009. Reduced clinical development requirements, faster approval timelines, and a more favorable interchangeability landscape all point toward higher returns on biosimilar investment over the next 5–10 years — but only for companies with the right analytical capabilities and regulatory expertise.
The reference biologics reaching patent and exclusivity expiry over the 2025–2030 period include several large-market products in oncology and immunology. IQVIA’s biosimilar void analysis identifies categories where patent expiry is approaching but biosimilar pipelines are thin, representing opportunities with reduced near-term competition [58].
The margin compression that comes with multiple biosimilar entrants in a reference product class is real. The strategic response — either move faster than competitors through superior analytical and regulatory execution, or position in less competitive reference product classes — requires the kind of real-time competitive intelligence that patent tracking platforms provide.
Key Takeaways
The regulatory framework for biosimilar clinical efficacy trials underwent its most consequential structural changes in a generation during 2024 and 2025. Here is what matters most:
The default clinical evidence standard has shifted. The FDA’s October 2025 draft guidance and the EMA’s 2025 finalized reflection paper both establish that comparative efficacy studies are no longer the default requirement for therapeutic protein biosimilars. For products meeting specific analytical and PK criteria, regulatory approval can be sought on the basis of analytical and PK evidence alone. Development programs built around the old default should be re-evaluated.
Analytical investment is now the primary driver of development efficiency. Robust characterization can eliminate the need for comparative efficacy trials — the single largest cost item in most biosimilar development programs. Analytical platform capabilities have become a core strategic asset, not a supporting function.
Interchangeability is being effectively universalized in the U.S. The FDA’s June 2024 guidance removing switching study requirements, combined with proposals to deem all approved biosimilars interchangeable, will erode the commercial significance of the interchangeable designation. Companies that have built commercial strategies around first-interchangeable exclusivity need to revise those strategies.
The patent landscape is as important as the clinical development plan. Patent expiry dates are the starting point, not the conclusion. Formulation, process, device, and method-of-use patents can extend effective exclusivity by years beyond core patent expiry. Competitive intelligence on patent portfolios, PTAB proceedings, and litigation history — available through platforms like DrugPatentWatch — is essential for realistic market entry planning.
Global development requires a global regulatory strategy. FDA and EMA convergence at the level of principle does not eliminate regional divergence at the level of detail. Reference product sourcing requirements, animal study mandates, ethnic population data requirements, and GMP inspection procedures vary in ways that add cost and timeline risk to programs designed with only one market in mind.
Extrapolation is the commercial multiplier. A single well-designed comparative study in the most sensitive indication, supported by a rigorous scientific justification of the mechanism of action’s consistency across indications, can generate regulatory approval for the full reference product label. The economics of biosimilar development depend on this extrapolation working, and it requires front-loading the analytical and MOA characterization work that supports the scientific argument.
Post-market pharmacovigilance is not a regulatory formality. Immunogenicity monitoring, product traceability through naming conventions, and responsive Risk Management Plans are the systems that maintain the safety record on which continued biosimilar adoption depends. Underinvestment in pharmacovigilance infrastructure creates both regulatory risk and commercial risk.
FAQ
Q1: Can a biosimilar be approved in the U.S. today without any comparative clinical efficacy study?
Yes, and this was not reliably possible before 2025. The FDA’s October 2025 draft guidance established that for therapeutic proteins produced from clonal cell lines, where the product is highly purified and well-characterized analytically, a comparative efficacy study ‘may not be necessary.’ The approval of a ustekinumab biosimilar — the first monoclonal antibody biosimilar approved without a clinical efficacy study — preceded that guidance and demonstrated that the agency’s review process could support such a conclusion. The guidance, when finalized, codifies that reasoning into an expected pathway rather than an exceptional one. Companies should initiate pre-BLA meetings with the FDA’s Office of Therapeutic Biologics and Biosimilars to determine whether their specific program qualifies under the streamlined approach.
Q2: How does the FDA’s June 2024 interchangeability guidance change commercial strategy for biosimilar developers?
The removal of switching study requirements reduces the cost and timeline to achieve interchangeable designation, making it achievable for more biosimilars and faster. But the more significant commercial implication is the FDA’s associated proposal to deem all approved biosimilars interchangeable upon approval, eliminating the designation as a distinct regulatory category. If finalized, this effectively makes the U.S. regulatory framework more similar to the European model, where all biosimilars are already treated as interchangeable. For companies that had planned to capture first-interchangeable exclusivity as a commercial differentiator, this regulatory change eliminates that strategy. Commercial positioning will need to shift toward market share capture speed, formulary contracting, and channel relationships rather than regulatory designation.
Q3: What is ‘biosimilar void analysis’ and how does it identify market opportunities?
A biosimilar void is a reference biologic product for which patent protection and regulatory exclusivity are expiring, but where no biosimilar candidate is in advanced (Phase 2/3) clinical development to enter the market at the time of exclusivity lapse. IQVIA’s analysis of these voids identifies product classes where the originator’s pricing power will not face immediate competitive challenge, because the expected biosimilar entry wave will arrive later than the expiry date would suggest. For biosimilar developers, identifying voids early means entering a less competitive market — fewer biosimilars competing for the same formulary position means higher sustainable market prices and better long-term returns. DrugPatentWatch’s patent expiry tracking, combined with pipeline databases tracking clinical development stage by reference product, provides the two primary inputs for this analysis.
Q4: Why is the EMA’s extrapolation framework considered more straightforward to navigate than the FDA’s?
The EMA has an extensive published record of positive scientific opinions on extrapolation, covering multiple therapeutic classes, and its product-specific guidelines explicitly address which indications can be extrapolated from a clinical study in which indication. This published precedent makes the regulatory expectation for extrapolation more predictable. The FDA has also accepted extrapolation broadly, but published guidance on extrapolation is less product-specific, and FDA feedback on specific extrapolation arguments is more frequently sought through formal pre-BLA consultation than through published guidance. Additionally, EMA’s July 2025 and subsequent finalized reflection paper on tailored clinical approaches explicitly establishes conditions under which clinical studies across multiple indications can be fully replaced by analytical and PK data — a more explicit policy position than the FDA’s October 2025 draft guidance, which is less specific about indication-level extrapolation in the absence of any clinical study.
Q5: How should biosimilar companies use patent intelligence platforms during the development process, not just at program initiation?
Patent intelligence is typically treated as a one-time due diligence exercise during program selection. It should be a continuous input throughout development. During the clinical development period — which lasts three to five years — reference product sponsors file new patents, PTAB proceedings resolve or escalate, litigation settlements establish market entry dates for other biosimilar competitors, and regulatory exclusivity periods run their course. A company that conducted a thorough patent analysis at program initiation but did not monitor subsequent patent filings may find that the reference product sponsor has secured new formulation or manufacturing patents after the development program began. DrugPatentWatch and similar platforms provide ongoing patent monitoring that supports mid-program strategy adjustments — including decisions to accelerate clinical timelines, alter product formulation to avoid a newly filed patent claim, or initiate PTAB challenges against patents identified as vulnerable. Treating competitive intelligence as a continuous process rather than a project-start activity gives development teams substantially more strategic flexibility.
References
[1] DrugPatentWatch. (2025, August 21). Regulatory considerations for biosimilar clinical efficacy trials. DrugPatentWatch Blog. https://www.drugpatentwatch.com/blog/regulatory-considerations-for-biosimilar-clinical-efficacy-trials/
[2] Grand View Research. (2023). Biosimilars market size, share & trends analysis report. https://www.grandviewresearch.com/industry-analysis/biosimilars-market
[3] IQVIA Institute for Human Data Science. (2022). Assessing the biosimilar void in the U.S. https://www.iqvia.com/insights/the-iqvia-institute/reports-and-publications/reports/assessing-the-biosimilar-void-in-the-us
[4] Niazi, S. K., et al. (2025). Scientific justification and policy recommendations to the U.S. Food and Drug Administration for waiving comparative efficacy studies. Pharmaceutics, 18(6), 779. https://pmc.ncbi.nlm.nih.gov/articles/PMC12196284/
[5] Health Canada. (2023). Biosimilar biologic drugs. https://www.canada.ca/en/health-canada/services/drugs-health-products/biologics-radiopharmaceuticals-genetic-therapies/biosimilar-biologic-drugs.html
[6] European Medicines Agency. (2014). Guideline on similar biological medicinal products containing biotechnology-derived proteins as active substance: Non-clinical and clinical issues — Revision 1 (EMA/CHMP/BMWP/289894/2014). https://www.ema.europa.eu/en/documents/scientific-guideline/guideline-similar-biological-medicinal-products-containing-biotechnology-derived-proteins-active-substance-non-clinical-and-clinical-issues-revision-1_en.pdf
[7] Biopharm International. (2022). The evolving cost-benefit landscape of biosimilar drug development. https://www.biopharminternational.com/view/the-evolving-cost-benefit-landscape-of-biosimilar-drug-development
[8] ICON plc. (2025, November 24). The changing regulatory requirements for biosimilar drug development: More nuanced than they initially appear. https://www.iconplc.com/insights/blog/2025/11/24/changing-regulatory-requirements-biosimilar-drug-development-more-nuanced
[9] U.S. Food & Drug Administration. (2025, October 29). Scientific considerations in demonstrating biosimilarity to a reference product: Updated recommendations for assessing the need for comparative efficacy studies [Draft Guidance]. https://www.hoganlovells.com/en/publications/fda-rethinks-need-for-comparative-efficacy-studies-for-certain-biosimilars
[10] U.S. Food & Drug Administration. (2015). Scientific considerations in demonstrating biosimilarity to a reference product: Guidance for industry. https://www.fda.gov/regulatory-information/search-fda-guidance-documents/scientific-considerations-demonstrating-biosimilarity-reference-product-guidance-industry
[11] Evidentic GmbH. (2024). Biosimilar comparability exercise. https://evidentic.com/biosimilar-comparability-exercise/
[12] Amgen Oncology. (2023). Biosimilars: Determining immunogenic potential (USA-BIO-80007). https://www.amgenoncology.com/resources/biosimilars-determining-immunogenic-potential-USA-BIO-80007.pdf
[13] Cohen, H. P., et al. (2018). Switching reference medicines to biosimilars: A systematic literature review of clinical outcomes. Drugs, 78, 463–478.
[14] U.S. Food & Drug Administration. (2025, September). Development of therapeutic protein biosimilars: Comparative analytical assessment and other quality-related considerations [Final Guidance]. https://www.fda.gov/regulatory-information/search-fda-guidance-documents/development-therapeutic-protein-biosimilars-comparative-analytical-assessment-and-other-quality
[15] Parexel. (2023). Biosimilar development: Optimizing PK/PD studies [White paper]. https://www.parexel.com/insights/whitepaper/biosimilar-development-optimizing-pkpd-studies
[16] Taylor & Francis. (2025). Evolving global regulatory landscape for approval of biosimilars: Current challenges and opportunities for convergence. Expert Opinion on Biological Therapy. https://www.tandfonline.com/doi/full/10.1080/14712598.2025.2507832
[17] PMC. (2025). Global harmonization of biosimilar development by overcoming existing differences in regional regulatory requirements. https://pmc.ncbi.nlm.nih.gov/articles/PMC11880096/
[18] DrugPatentWatch. (2025). Biosimilar patent dance: Leveraging PTAB challenges for strategic advantage. https://www.drugpatentwatch.com/blog/biosimilar-patent-dance-leveraging-ptab-challenges-for-strategic-advantage/
[19] Aragen Life Sciences. (2024). Accelerating biosimilar approval with PK data and PD biomarkers. https://www.aragen.com/article/accelerating-the-regulatory-approval-process-of-biosimilars-by-leveraging-precise-and-reliable-pk-data-and-pd-biomarker-data/
[20] U.S. Food & Drug Administration. (2020). Biosimilar development, review, and approval [Fact sheet]. https://www.fda.gov/drugs/biosimilars/industry-information-and-guidance
[21] U.S. Food & Drug Administration. (2023). Increasing the efficiency of biosimilar development [Public workshop proceedings]. https://www.fda.gov/drugs/biosimilars/industry-information-and-guidance
[22] European Medicines Agency. (2025). Reflection paper on a tailored clinical approach in biosimilar development (EMA/CHMP/BMWP/60916/2025). https://www.ema.europa.eu/en/reflection-paper-tailored-clinical-approach-biosimilar-development
[23] RAPS. (2025, April). Euro roundup: EMA finalizes reflection paper on biosimilar comparative efficacy studies. https://www.raps.org/resource/euro-roundup-ema-finalizes-reflection-paper-on-biosimilar-comparative-efficacy-studies.html
[24] Jones Day. (2025, December 3). FDA’s biosimilar playbook: Merging biosimilarity with interchangeability. https://www.jonesday.com/en/insights/2025/12/fda-biosimilar-playbook-merging-biosimilarity-with-interchangeability
[25] U.S. Food & Drug Administration. (2024, June). Considerations in demonstrating interchangeability with a reference product: Update [Draft Guidance]. https://www.fda.gov/drugs/drug-safety-and-availability/fda-updates-guidance-interchangeability
[26] PubMed. (2012). Statistical considerations in biosimilar clinical efficacy trials with asymmetrical margins. https://pubmed.ncbi.nlm.nih.gov/22991275/
[27] Amgen Oncology. (2023). Statistical considerations for biosimilar equivalence trials (USA-BIO-80179). https://www.amgenoncology.com/resources/biosimilars-statistical-considerations-for-biosimilar-equivalence-tests-USA-BIO-80179.pdf
[28] EMWA Journal. (2022). Statistical principles in biosimilar development. https://journal.emwa.org/generics-and-biosimilars/statistical-principles-in-biosimilar-development/
[29] U.S. Food & Drug Administration. (2015). Guidance for industry: Clinical pharmacology data to support a demonstration of biosimilarity to a reference product. https://www.fda.gov/regulatory-information/search-fda-guidance-documents/clinical-pharmacology-data-support-demonstration-biosimilarity-reference-product
[30] RMD Open. (2016). Principles of clinical efficacy trials for biosimilars. RMD Open, 2(1), e000154. https://rmdopen.bmj.com/content/2/1/e000154
[31] BioAgilytix. (2023). Immunogenicity testing for biosimilars. https://www.bioagilytix.com/blog/immunogenicity-testing-for-biosimilars/
[32] U.S. Food & Drug Administration. (2019). Immunogenicity testing of therapeutic protein products — developing and validating assays for anti-drug antibody detection: Guidance for industry. https://www.fda.gov/regulatory-information/search-fda-guidance-documents/immunogenicity-testing-therapeutic-protein-products-developing-and-validating-assays-anti-drug
[33] Cognizant. (2023). Pharmacovigilance considerations for biologics and biosimilars. https://www.cognizant.com/en_us/industries/documents/pharmacovigilance-considerations-for-biologics-and-biosimilars.pdf
[34] PMC. (2017). Biosimilars and the extrapolation of indications for inflammatory conditions. Biologics: Targets and Therapy, 11, 5–11. https://pmc.ncbi.nlm.nih.gov/articles/PMC5322938/
[35] Pharmaceuticals and Medical Devices Agency (PMDA). (2021). Guideline for biosimilars. https://www.pmda.go.jp/files/000267474.pdf
[36] DrugPatentWatch. (2024). Regulatory considerations for biosimilar extrapolation of indications. https://www.drugpatentwatch.com/blog/regulatory-considerations-for-biosimilar-extrapolation-of-indications/
[37] Pharmaceuticals and Medical Devices Agency (PMDA). (2023). Biosimilars: Review services overview. https://www.pmda.go.jp/english/review-services/reviews/0005.html
[38] Health Canada. (2023). Guidance document: Information and submission requirements for biosimilar biologic drugs. https://www.canada.ca/en/health-canada/services/drugs-health-products/biologics-radiopharmaceuticals-genetic-therapies/biosimilar-biologic-drugs.html
[39] Sandoz. (2023). Biosimilar development pathway overview. https://www.us.sandoz.com/our-work/biosimilars/biosimilar-development-process/
[40] Center for Biosimilars. (2024, June 20). FDA draft guidance removes switching study requirements for biosimilar interchangeability. https://www.centerforbiosimilars.com/view/fda-draft-guidance-removes-switching-study-requirements-for-biosimilar-interchangeability
[41] U.S. Food & Drug Administration. (2022). Postmarketing requirements and commitments: Reports. https://www.fda.gov/drugs/postmarketing-requirements-and-commitments-introduction/postmarketing-requirements-and-commitments-reports
[42] European Medicines Agency. (2022). Guideline on good pharmacovigilance practices (GVP) Module V — Risk management systems. https://www.ema.europa.eu/en/documents/regulatory-procedural-guideline/guideline-good-pharmacovigilance-practices-gvp-module-v-risk-management-systems-rev-2_en.pdf
[43] U.S. Food & Drug Administration. (2023). Risk evaluation and mitigation strategies (REMS): Overview. https://www.fda.gov/drugs/drug-safety-and-availability/risk-evaluation-and-mitigation-strategies-rems
[44] IPWatchdog. (2023). AbbVie’s Humira biosimilar patent portfolio. https://ipwatchdog.com/tag/biosimilars/
[45] U.S. Food & Drug Administration. (2023). Implementation of the Biologics Price Competition and Innovation Act of 2009. https://www.fda.gov/drugs/guidance-compliance-regulatory-information/implementation-biologics-price-competition-and-innovation-act-2009
[46] European Medicines Agency. (2023). Biosimilar medicines: Overview. https://www.ema.europa.eu/en/human-regulatory-overview/biosimilar-medicines-overview
[47] DrugPatentWatch. (2023). Biosimilar patent dance: Leveraging PTAB challenges for strategic advantage. https://www.drugpatentwatch.com/blog/biosimilar-patent-dance-leveraging-ptab-challenges-for-strategic-advantage/
[48] Beall, R. F., et al. (2024). Biosimilar market entry delays under BPCIA patent litigation framework. Journal of Law and the Biosciences, 12(1), lsae030. https://academic.oup.com/jlb/article/12/1/lsae030/7942247
[49] DrugPatentWatch. (2024). The importance of pharmaceutical competitor analysis. https://www.drugpatentwatch.com/blog/the-importance-of-pharmaceutical-competitor-analysis/
[50] World Health Organization. (2022). WHO guidelines on evaluation of similar biotherapeutic products (SBPs). https://www.who.int/publications/i/item/9789241504874
[51] PMC. (2025). Global harmonization of biosimilar development. https://pmc.ncbi.nlm.nih.gov/articles/PMC11880096/
[52] International Council for Harmonisation. (2004). ICH Q5E: Comparability of biotechnological/biological products subject to changes in their manufacturing process. https://www.ich.org/page/quality-guidelines
[53] World Health Organization. (2023). WHO collaborative procedure for accelerated registration. https://www.who.int/publications
[54] DiMasi, J. A., et al. (2016). Innovation in the pharmaceutical industry: New estimates of R&D costs. Journal of Health Economics, 47, 20–33.
[55] Fortune Business Insights. (2023). U.S. biosimilars market. https://www.fortunebusinessinsights.com/industry-reports/u-s-biosimilars-market-100990
[56] The Rheumatologist. (2024, August). Draft FDA guidance no longer requires biosimilar switching studies. https://www.the-rheumatologist.org/article/draft-fda-guidance-no-longer-requires-biosimilar-switching-studies/
[57] GeneOnline. (2024). DrugPatentWatch analysis: Biosimilars offer potential cost savings, but adoption rates differ sharply between U.S. and Europe. https://www.geneonline.com/drugpatentwatch-analysis-biosimilars-offer-potential-cost-savings-but-adoption-rates-differ-sharply-between-u-s-and-europe/
[58] IQVIA Institute for Human Data Science. (2022). Assessing the biosimilar void in the U.S. https://www.iqvia.com/insights/the-iqvia-institute/reports-and-publications/reports/assessing-the-biosimilar-void-in-the-us