1. Why ‘Inactive’ Is a Dangerous Word: The Strategic Case for Excipient Scrutiny
The Myth That Costs Billions
The word ‘excipient’ derives from the Latin excipere, meaning ‘other than.’ That etymology has done more damage to pharmaceutical R&D economics than almost any other linguistic accident in the industry’s history. Derived from that root, the field spent decades treating excipients, the non-API components that constitute an average of 90% of a finished dosage form, as inert scaffolding. They were the background. The filler. The stuff you use so the pill holds together.
That framing is wrong, and the industry now knows it. What the industry still struggles with is acting on that knowledge early and systematically, before clinical trials lock in a formulation that will cost eight figures to revisit after approval.
Excipients govern drug stability, bioavailability, manufacturing process behavior, immunological tolerability, and shelf life. They interact chemically with the API, physically with each other, and biologically with the patient. A single poor excipient choice can trigger a Maillard degradation cascade that destroys potency over 18 months of storage, cause anaphylaxis in a patient with an unrecognized PEG sensitivity, or produce a tablet with dissolution kinetics so misaligned from the reference listed drug (RLD) that bioequivalence studies fail twice before the problem is correctly diagnosed.
The cost of these failures is not abstract. Late-stage clinical failures attributable to formulation issues can run $50 million to $300 million depending on the development stage. Post-approval reformulation requiring a Prior Approval Supplement (PAS) to FDA can add 18 to 36 months to a product’s timeline. For a drug generating $1 billion in annual revenue, each month of delay represents approximately $83 million in foregone sales.
This report presents the Excipient Exclusion Filter framework: a systematic, science-driven methodology for proactively screening and eliminating problematic excipients at the earliest stages of development. It is not a checklist. It is a disciplined risk management system that aligns formulation science with regulatory strategy, commercial objectives, and intellectual property creation.
Patient-Centricity Is Not a Tagline, It Is a Commercial Variable
The business case for patient-centric formulation is quantifiable. Analysis from Arthur D. Little found that drugs developed using patient-centric processes were 20% more likely to launch successfully than those developed without systematic patient input. A drug that a lactose-intolerant patient cannot tolerate, that a Muslim patient will not take because of porcine-derived gelatin, or that a clinician refuses to prescribe to a neonate because it contains benzyl alcohol, is not a complete therapeutic product. It is a partial one. Incomplete products lose market share to complete ones.
The ‘free-from’ formulation category, including lactose-free, gelatin-free, alcohol-free, and dye-free products, is the most technically rigorous and commercially potent expression of patient-centricity in pharmaceutical manufacturing. The Excipient Exclusion Filter is the operational roadmap to get there without sacrificing product quality, bioavailability, or regulatory clarity.
Key Takeaways: Section 1
Excipients constitute roughly 90% of the final dosage form by mass and govern stability, bioavailability, and patient tolerability. The ‘inactive ingredient’ designation is a regulatory classification, not a pharmacological one. Late-stage reformulation driven by excipient failures costs tens to hundreds of millions of dollars per program. Patient-centric formulation, specifically ‘free-from’ products targeting defined exclusion criteria, improves commercial launch probability by a documented 20%. The highest-leverage intervention point is at pre-formulation, before pivotal clinical studies begin.
2. The Excipient Risk Landscape: Hidden Liabilities in Your Formulation
Three Categories of Risk That Define the Exclusion Logic
Excipient risk operates in three distinct but often overlapping domains. A robust exclusion framework must address all three simultaneously, because a formulation that avoids patient hypersensitivity risks but ignores API degradation risks will still fail, just at a different point in the development timeline.
Domain 1: Direct Patient Reactions
Adverse reactions to excipients range from mild gastrointestinal intolerance to IgE-mediated anaphylaxis. Research published in PLOS One found that 92.8% of oral medicines contain at least one ingredient with allergen potential. That statistic reframes excipient risk from a niche concern to a near-universal formulation problem.
The most clinically significant offenders by mechanism:
Lactose (filler, diluent): Causes dose-dependent gastrointestinal symptoms in lactase-deficient patients. Global lactase non-persistence runs 65-80% in adults, with near-total penetrance in East Asian, West African, and Native American populations. While pharmaceutical lactose doses are typically sub-threshold for symptom induction in most patients (the gastrointestinal symptom threshold sits around 12 grams; a standard tablet rarely exceeds 400 mg), patients with severe intolerance or those on high-pill-count regimens can accumulate clinically relevant doses across a dosing day.
Benzyl alcohol (preservative, injectable solvent): Documented as the causative agent in ‘gasping syndrome’ in neonates, a condition characterized by metabolic acidosis, CNS depression, and cardiovascular collapse. The mechanism is accumulation of benzyl alcohol’s metabolite, benzoic acid, which cannot be conjugated to hippuric acid at the rate required in neonates due to immature hepatic glucuronidation. This excipient is a hard exclusion for any neonatal or infant parenteral formulation.
Polyethylene glycol (PEG) and polysorbates: PEG sensitivity received substantial clinical attention during the 2020-2021 COVID-19 mRNA vaccine rollout, where PEG-coated lipid nanoparticles were identified as the antigen in a subset of anaphylactic reactions. The underlying immunological mechanism involves pre-existing anti-PEG IgG and IgM antibodies, which are present at low levels in a non-trivial proportion of the general population due to exposure through cosmetics, food additives, and prior medications. For injectable formulations and lipid nanoparticle-based delivery systems, PEG and polysorbate sensitivity requires specific pre-screening strategies and emergency response protocols.
Tartrazine (FD&C Yellow No. 5): Azo dye with a well-characterized association with urticaria, angioedema, and aspirin-exacerbated respiratory disease. FDA mandates label disclosure for any product containing tartrazine, which is itself a meaningful signal of the agency’s view of its risk profile. One analysis estimated that up to one-third of marketed medications contain at least one dye associated with allergic reactions, making colorant exclusion a high-yield filter for sensitive populations.
Carmine: Red dye derived from the crushed cochineal insect (Dactylopius coccus). Documented to cause anaphylaxis. Non-trivially, carmine is simultaneously a vegan/vegetarian exclusion target and an anaphylaxis risk, illustrating how multiple exclusion filters can reinforce each other.
Lanolin and arachis (peanut) oil: Topical sensitizer and parenteral anaphylaxis trigger, respectively. Arachis oil used in some oil-based injectables and softgel fills is highly refined, but the UK’s MHRA advises avoidance in patients with confirmed peanut allergy due to residual protein risk, and cross-reactivity with soy must be assessed given the botanical proximity of peanut and soybean.
Domain 2: API-Excipient Incompatibility
The most economically damaging excipient risks are often not direct patient reactions but silent API degradation reactions that compound over the drug’s shelf life and go undetected until a stability batch fails or, worse, until post-market surveillance catches a potency decline in distributed product.
The Maillard reaction is the canonical example. A primary or secondary amine on the API reacts with the carbonyl group of a reducing sugar to form Schiff base intermediates, which rearrange into Amadori products and ultimately melanoidin pigments. The product discolors, API potency drops, and degradation products of unknown toxicological profile accumulate. Lactose is the most common reducing sugar trigger, but glucose, maltose, and reducing sugar impurities in nominally non-reducing excipients like microcrystalline cellulose (MCC) can initiate the same cascade. Heat and moisture act as rate multipliers. Any API with a primary or secondary amine (a large fraction of CNS, cardiovascular, and antibiotic drugs) carries Maillard risk with lactose-containing formulations.
Oxidative degradation via excipient impurities: Polymers including povidone, crospovidone, and various polyethylene glycol grades can contain residual peroxide impurities generated during manufacturing and storage. These peroxides act as oxidants for susceptible APIs, particularly those containing thioether, phenol, or catechol functionalities. The risk is not simply the excipient identity but the excipient’s peroxide value at the grade level being sourced. A ‘pharmaceutical grade’ povidone from two different suppliers can have meaningfully different peroxide levels, and only one may push a sensitive API past its stability specification at 36 months.
Aldehyde interactions: Trace aldehydes, including formaldehyde, are common impurities across a wide range of excipients: lactose, MCC, starch, and PEG-based polymers all have documented aldehyde contamination profiles. Aldehydes react readily with hydroxyl, amine, and thiol groups on drug molecules, forming adducts that alter the API’s pharmacological activity and can create immunogenic conjugates in protein-based drugs.
Physical incompatibilities: Magnesium stearate, the near-universal tablet lubricant, presents a subtle but significant risk when mixed with certain formulations. Extended blending creates a hydrophobic film around API and excipient particles (‘over-lubrication’) that retards water penetration and delays dissolution, potentially compromising bioequivalence for BCS Class II drugs without any change in chemical identity.
Domain 3: Excipient Impurities and Concomitant Components
The International Pharmaceutical Excipients Council (IPEC) classifies non-primary substances in excipient materials as ‘concomitant components,’ which include residual solvents, catalyst traces, unreacted monomers, and manufacturing byproducts. The reference case is the 1980s discovery of hydrazine contamination in pharmaceutical-grade povidone. Hydrazine, a carcinogen and potent toxin, was a polymerization byproduct. The discovery required process modifications and, subsequently, pharmacopeial monograph updates specifying a hydrazine test method and upper limit. The timeline from discovery to pharmacopeial control spanned years, during which patient exposure occurred at levels above what would later be deemed acceptable.
The regulatory infrastructure for controlling excipient impurities has strengthened considerably since then, but the risk class persists. ICH Q3C and Q3D guidelines govern residual solvents and elemental impurities in drug products respectively, and their requirements apply to impurities regardless of whether they originate from the API or an excipient. A formulation team sourcing a new excipient must assess the full impurity profile, not merely confirm the primary substance identity.
This three-domain risk framework establishes the intellectual basis for the Excipient Exclusion Filter. Risk is not a property of an excipient in isolation. It is a function of the excipient in combination with a specific API, in a specific dosage form, for a specific patient population, manufactured under specific process conditions. Generic exclusion lists are insufficient. The framework must be dynamic, contextual, and applied at the interface of all three risk domains simultaneously.
Key Takeaways: Section 2
92.8% of oral medicines contain at least one ingredient with allergen potential. Excipient risk operates across three domains: direct patient reactions, API-excipient incompatibility, and impurity-related toxicity. The Maillard reaction, oxidative degradation via peroxide impurities, and aldehyde-adduct formation are the most common and economically damaging incompatibility mechanisms. Excipient risk is context-dependent; no universal ‘safe’ or ‘unsafe’ list exists. Impurity profiles at the grade and supplier level, not just excipient identity, determine actual risk.
3. The Excipient Exclusion Filter: A Four-Step Operational Framework
From Reactive Troubleshooting to Proactive Risk Architecture
The Excipient Exclusion Filter reframes excipient selection from an empirical, trial-and-error process into a structured risk management methodology aligned with Quality by Design (QbD). ICH Q8(R2) defines QbD as systematic development beginning with predefined objectives, emphasizing product and process understanding and control based on sound science and quality risk management. The Excipient Exclusion Filter is the application of QbD principles specifically to excipient risk.
Step 1: Define the Target Product Profile (TPP) and Patient Population
Every exclusion decision must originate from a clearly defined Target Product Profile. The TPP specifies the drug’s intended clinical use, route of administration, target patient population, and performance requirements. These parameters directly determine which exclusion filters apply.
Patient population definition is the primary driver. Pediatric formulations, particularly those intended for neonates and infants under two years of age, trigger an extensive list of automatic exclusions. Benzyl alcohol (gasping syndrome), ethanol (immature alcohol dehydrogenase activity, with neonatal ADH concentrations below 20% of adult levels), propylene glycol (CNS toxicity at high doses, caution below age four per EMA guidance), and parabens (contact sensitizer, endocrine disruption concerns in neonates) all require either hard exclusion or severe dose restriction. EMA’s Guideline on Excipients in Medicinal Products for Human Use and FDA’s recommendations for pediatric OTC products both provide formal dose limits by age band that must be incorporated into the TPP as design constraints, not post-hoc label additions.
Geriatric populations introduce a different exclusion logic. Dysphagia affects an estimated 15% of community-dwelling elderly patients and up to 68% of nursing home residents. Standard tablet sizes and coating systems that require intact swallowing function become formulation liabilities in this demographic. The TPP for a geriatric-focused product should specify patient-appropriate size limits, and exclusion filters should target excipients that prevent alternative dosage form options, favoring approaches compatible with orally disintegrating tablet (ODT), liquid, or modified-release pellet formats.
Route of administration establishes the baseline excipient safety standard. Parenteral formulations bypass mucosal and hepatic first-pass barriers, eliminating most detoxification mechanisms that protect patients from oral excipient risks. This demands ultra-high purity grades with specified endotoxin and bioburden limits. Intravenous formulations exclude essentially all excipients not validated for systemic exposure. Ophthalmic formulations carry specific pH, osmolality, and preservative constraints that exclude large swaths of the standard oral excipient toolkit.
Step 2: Characterize the API and Map Incompatibility Risks
Pre-formulation studies generate the data that populates the exclusion filter’s incompatibility logic. The API’s molecular structure, pKa profile, solubility characteristics, solid-state behavior, and stability profile under stress conditions must be fully characterized before excipient selection begins.
Structural alerts for excipient incompatibility:
An API containing a primary or secondary amine group activates a reducing sugar exclusion filter. Lactose, maltose, glucose, and excipients with reducing sugar impurity profiles move to the exclusion list. Preferred alternatives include mannitol, sorbitol, sucrose, and trehalose for low-moisture systems.
An API with oxidation-sensitive functionalities, thioethers, catechols, phenols, and certain tertiary amines, activates a peroxide impurity exclusion filter. Povidone and polysorbate grades must have specified low peroxide values from the supplier, or the excipient class requires exclusion in favor of alternatives with cleaner oxidant profiles.
An API with poor aqueous solubility (BCS Class II or IV) activates a dissolution-impact exclusion filter. Excipients that reduce tablet porosity, increase hydrophobicity, or alter wettability, including high concentrations of magnesium stearate or hydrophobic waxy excipients, carry heightened bioequivalence risk and must be carefully staged in the design space.
Hygroscopic APIs require excipients with low hygroscopicity and minimal free moisture content. Highly hygroscopic excipients like sorbitol or certain grades of MCC can accelerate moisture-driven degradation.
Step 3: Screen Against Regulatory Databases and Precedent
The FDA’s Inactive Ingredient Database (IID) is the foundational tool for regulatory risk stratification in the US market. For each excipient, the IID specifies the dosage forms and administration routes in which it has previously been approved and the maximum potency observed in an approved product for each context.
The IID’s risk stratification logic:
If the intended excipient and concentration fall within IID precedent for the target route, the regulatory burden is standard. No additional safety package is required beyond the normal formulation characterization.
If the intended concentration exceeds the IID’s maximum potency for that route, or if the excipient has no IID listing for the target route, it is classified as a ‘novel excipient’ under FDA’s framework. Novel excipient status triggers a requirement for a standalone safety package, typically including repeated-dose toxicity studies, genotoxicity assessment, and a toxicological risk assessment. This adds 12-24 months and several million dollars to the development timeline.
The European Medicines Agency’s Annex to the Guideline on Excipients in the Labelling and Package Leaflet provides a parallel reference for the European market, specifying excipients with recognized effects that require mandatory label disclosure and patient-information text. Building these labeling requirements into the TPP at the outset prevents late-stage label negotiations with the agency.
The IID should not function as an innovation ceiling. Novel APIs with extreme physicochemical challenges, such as highly lipophilic small molecules requiring lipid-based drug delivery systems, or macromolecular biologics requiring specialized cryoprotectant systems, often require excipients or concentration levels without IID precedent. In these cases, the exclusion framework documents the risk-benefit decision and the data package supporting the novel use.
Step 4: Integrate Exclusion Outputs into the QbD Control Strategy
The outputs of Steps 1-3 feed directly into the QbD architecture. Exclusion decisions become Quality Target Product Profile (QTPP) attributes. If lactose is excluded because of amine Maillard risk, ‘free of reducing sugars’ becomes a CQA of the formulation. The alternative excipient’s critical material attributes (CMAs), particle size distribution, bulk density, flowability, and compressibility index for a filler replacement, become process design space parameters that must be controlled within validated ranges to ensure the QTPP is met batch-to-batch.
This integration converts excipient selection from a one-time screening decision into a continuous control point across the product’s lifecycle. It also generates the formal documentation trail that supports regulatory filings and post-approval change management when excipient suppliers are qualified, substituted, or when material specifications need updating.
Key Takeaways: Section 3
The Excipient Exclusion Filter is a four-step framework: define TPP and patient population, characterize API risks, screen against regulatory databases, and integrate outputs into QbD. Pediatric formulations trigger automatic exclusions for benzyl alcohol, ethanol, propylene glycol, and parabens based on EMA and FDA guidance. The FDA’s IID determines whether an excipient use is precedented (standard regulatory burden) or novel (requires a full toxicology package and 12-24 months additional development time). Exclusion decisions documented within the QbD framework become enforceable QTPP attributes and CQA-linked CMAs, not just informal formulator preferences.
4. The Lactose-Free Filter: Navigating the Industry’s Most Common Technical Hurdle
The Scale of the Challenge
Lactose is the most widely used pharmaceutical excipient in oral solid dosage forms. Its functional properties, specifically its compressibility, flowability, low hygroscopicity, and cost-effectiveness, make it the default filler and diluent for direct compression and wet granulation tablets. Approximately 70% of global tablet and capsule products contain lactose in some form.
Lactose intolerance (lactase non-persistence) affects an estimated 65-80% of the adult global population. The geography is heavily skewed. Northern European populations show 5-10% prevalence; Scandinavian countries sit at the low end of that range. East Asian populations show 70-100% prevalence. West African descent populations and Native Americans average 80% or above. In the United States, the Lactose Intolerance NIH Consensus Panel estimated 30-50 million affected adults.
The clinical threshold for symptom induction from lactose in pharmaceutical preparations deserves careful analysis. A randomized, double-blind, placebo-controlled study of 77 lactose-intolerant subjects found that a 400 mg lactose dose (approximately the amount in a standard tablet) did not produce a statistically significant increase in gastrointestinal symptoms versus placebo. The established symptom threshold sits around 12 grams. For the majority of lactose-intolerant patients on single-product regimens, pharmaceutical lactose loads likely fall sub-threshold.
However, this threshold analysis does not end the case for lactose-free formulation. Patients on high-pill-count polypharmacy regimens, particularly in geriatric and oncology settings, can accumulate lactose loads across multiple concurrent medications that aggregate into symptom-inducing ranges. Patients with severe or total lactase deficiency operate at lower thresholds than study medians. The ‘free-from’ market pull is commercial and not purely clinical: growing consumer demand for transparent labeling and the ‘clean label’ trend in both food and pharma creates prescribing preference for lactose-free options even among tolerant patients.
Why Lactose Is Hard to Replace: Technical Properties
Lactose’s dominance derives from a combination of functional properties that very few single alternative excipients can match simultaneously:
Spray-dried lactose (SDL) offers a particle morphology, specifically spherical, porous agglomerates with enclosed fines, that provides both excellent flowability (low Carr Index, Hausner Ratio near 1.15) and good compressibility without granulation. Anhydrous lactose provides even better compressibility and is preferred for moisture-sensitive APIs. Both forms are non-hygroscopic under typical warehouse conditions and have low water activity.
Replacing lactose requires replicating or exceeding these combined properties. No single standard excipient does this. The challenge is multiplied because the primary alternative candidates each solve one problem while creating others: mannitol has good compressibility for ODTs but lower cohesivity for direct compression tablets above certain API loads; MCC has excellent binding and tablet strength but poor flow requiring granulation or blending with glidants; dicalcium phosphate has good flow but low compactibility, yielding brittle tablets with high friability.
Biopharmaceutical Risk: The BCS Framework for Lactose Replacement Decisions
The Biopharmaceutics Classification System (BCS) provides the most operationally useful framework for stratifying bioequivalence risk in lactose replacement projects. The key variable is dissolution-rate dependency: excipient changes that alter how quickly the API dissolves from the dosage form will affect systemic exposure for drugs whose absorption is dissolution-limited.
For BCS Class I drugs (high solubility, high permeability), dissolution is rapid under all physiologically relevant conditions. The probability that lactose replacement will alter bioavailability is low. A well-characterized substitute maintaining similar porosity and disintegration behavior can be selected with confidence that bioequivalence is preserved.
For BCS Class II drugs (low solubility, high permeability), dissolution rate is the absorption rate-limiting step. The excipient matrix controls dissolution kinetics. Any change in filler solubility, porosity contribution, or tablet disintegration mechanism carries medium-to-high bioequivalence risk. This class requires comparative in vitro dissolution profiling across multiple pH conditions (1.2, 4.5, 6.8) before any in vivo study decision, and a formal risk assessment determining whether an in vivo bioequivalence study is required to support regulatory approval of the reformulation.
For BCS Class IV drugs (low solubility, low permeability), both dissolution and membrane permeability limit absorption, making these drugs extraordinarily sensitive to formulation changes. Lactose replacement in a BCS Class IV drug is a high-risk project that requires in vivo bioequivalence demonstration in most regulatory jurisdictions, with the full associated cost and timeline implications.
BCS Class III drugs (high solubility, low permeability) present medium risk from lactose replacement, primarily because permeability limits absorption rather than dissolution, but atypical excipient interactions with transporters are possible for certain compounds.
Formulator’s Toolkit: Alternatives to Lactose
Mannitol is the strongest direct compression alternative for moisture-sensitive and temperature-sensitive APIs. Its non-hygroscopicity (equilibrium moisture content near 0.3% at 65% RH), pleasant taste, and good compressibility in coarser particle grades make it the dominant choice for ODTs and moisture-critical products. Its limitations include higher cost than lactose (typically 3-5x) and lower cohesivity at fine particle sizes, which can result in capping and lamination during compression if not adequately compensated by a compatible binder.
Microcrystalline cellulose (MCC) provides excellent binding and tablet hardness, and its self-disintegrating properties at 5-15% concentrations are well characterized. It is the most common co-excipient in lactose-free wet granulation formulations. Its deficits are poor flowability in fine grades, sensitivity to over-lubrication with magnesium stearate, and moisture uptake that can compromise APIs sensitive to hydrolysis.
Dicalcium phosphate (DCP), specifically the dihydrate (dibasic calcium phosphate dihydrate, DCPD) and anhydrous (DCPA) grades, offers excellent flow and low cost. It is the preferred alternative when bulk density matching is required and tablet hardness requirements are moderate. Its compactibility is low compared to lactose or MCC, limiting its use to applications where a binder can compensate.
Dextrates (e.g., Emdex) are partially hydrolyzed dextrose polymers with particle morphology and bulk density profiles closely matching spray-dried lactose. Published data on cetirizine tablet reformulation showed that a 1:1 Emdex substitution for SDL produced tablets with statistically equivalent powder flow, hardness, friability, and dissolution profiles to both the lactose control and the marketed reference product. Emdex represents the lowest-risk direct replacement strategy for SDL-based direct compression formulations.
Co-processed excipients are the most technically sophisticated option. These multi-component particles, produced via spray drying or co-granulation of two or more standard excipients, engineer multiple functional properties into a single ingredient. Examples include MCC-mannitol, MCC-calcium carbonate, and lactose-free combinations pairing a binder with a disintegrant. Their advantages: superior and consistent compressibility, flowability, and disintegration; reduced total excipient count; simplified formulation development. Their disadvantages: higher cost, proprietary sourcing from single manufacturers creates supply chain concentration risk, and documentation requirements for co-processed excipient qualification are more complex than for single-entity excipients.
Case Studies
Cetirizine (Reactine) Lactose-Free Reformulation
Objective: Produce a bioequivalent lactose-free version of a marketed antihistamine for lactose-intolerant patients using direct compression.
Approach: 1:1 substitution of spray-dried lactose with Emdex dextrates, maintaining all other excipient identities and concentrations.
Results: Equivalent powder flow (angle of repose, Carr Index), tablet hardness (>80 N), friability (<0.5%), and dissolution profiles (f2 similarity factor >80 at pH 1.2, 4.5, and 6.8) versus lactose control and marketed RLD. No bioequivalence study was required. A low-cost, low-risk development program delivered a patient-relevant product differentiation.
Rivaroxaban (Xarelto, BCS Class II) Lactose-Free Reformulation
Objective: Develop lactose-free tablet and MUPS (Multiple-Unit Pellet System) formulations of a poorly soluble anticoagulant without compromising dissolution or stability.
Approach: Anhydrous dicalcium phosphate (DCPA) as primary filler, with optimized binder and disintegrant concentrations. MUPS format to maximize surface area and dissolution potential.
Results: Tablets and MUPS formulations met mechanical specifications and demonstrated comparable in vitro dissolution profiles to the marketed Xarelto reference across the physiological pH range. Chemical stability at accelerated conditions (40°C/75% RH) was equivalent to the reference. The project demonstrated that lactose replacement in BCS Class II drugs is achievable with appropriate formulation strategy, though the comparative dissolution data required to support this conclusion were substantially more extensive than those required for the cetirizine project.
IP Landscape: Lactose-Free Formulation Patents
Lactose-free formulation patents represent a growing and commercially significant IP category. A January 2022 PCT filing (WO2022180444A1) covers a lactose-free empagliflozin formulation produced by direct compression using specifically engineered co-processed excipients. The patent’s claims are narrow enough in their combination of excipient identities and process parameters that they represent genuine protectable territory rather than evergreening of trivial modifications.
For generic developers targeting SGLT2 inhibitors, a patent landscape analysis using tools such as DrugPatentWatch will reveal formulation patent coverage extending beyond the API patent expiry. Understanding these filing dates, claim scope, and expiry timelines is required before investing in lactose-free generics development.
Investment Strategy Note: Lactose-Free Formulation
The lactose-free pharmaceutical excipient market is a sub-segment within the broader pharmaceutical excipients market projected to reach approximately $15.49 billion by 2034. Mannitol, co-processed excipients, and dextrate producers are direct beneficiaries of the lactose-free trend. For branded pharmaceutical companies, lactose-free line extensions targeting BCS Class I drugs represent low technical risk and straightforward regulatory paths; they merit aggressive commercial development. BCS Class II and IV lactose-free reformulations require in vivo bioequivalence studies and carry higher development cost, but they also carry higher IP defensibility because the technical barrier to replication is proportionally higher.
Key Takeaways: Section 4
65-80% of the global adult population has lactase non-persistence, but the clinical relevance of pharmaceutical lactose doses requires case-by-case analysis based on patient population, pill burden, and intolerance severity. Lactose’s functional excellence (compressibility, flowability, non-hygroscopicity) means replacement is a multi-attribute engineering problem, not a simple substitution. BCS class determines bioequivalence risk level: Class I is low risk, Class II is medium-to-high, Class IV is high and typically requires an in vivo study. Dextrates offer the most direct 1:1 replacement for SDL in direct compression formulations. Co-processed excipients offer superior performance at higher cost and with supply chain concentration risk. Lactose-free formulation patents are an active and growing IP category relevant to both branded lifecycle management and generic entry strategy.
5. The Animal-Free Filter: Gelatin, HPMC, and the Ethics-Driven Market Shift
Gelatin’s Dominance and Its Structural Vulnerabilities
Gelatin has been the capsule material of choice since the mid-19th century because it works exceptionally well: it forms strong, flexible films, dissolves rapidly at body temperature (37°C), and processes efficiently on high-speed encapsulation equipment. Derived from the collagen of bovine or porcine skin and bones, it is both functionally superior and commercially dominant. The global hard gelatin capsule market is enormous; it underpins virtually all oral liquid-fill and powder-fill capsule dosage forms at scale.
Four structural vulnerabilities make gelatin a formulation risk that cannot be ignored:
First, its animal origin excludes it from vegetarian, vegan, Halal, and Kosher markets. Porcine gelatin is categorically prohibited under Islamic dietary law. Bovine gelatin from non-ritually slaughtered animals is similarly excluded. The global Muslim population exceeds 1.8 billion people. Even a 10% prescription non-adherence rate among patients who object to animal-derived formulations represents a meaningful commercial and clinical problem.
Second, gelatin’s moisture content (13-16%) renders it incompatible with hygroscopic APIs and moisture-sensitive fill materials. It actively transfers moisture to enclosed powder fills under humidity cycling, potentially destabilizing the API.
Third, gelatin is susceptible to cross-linking, a chemical reaction between gelatin’s lysine residues and aldehyde-containing compounds that stiffens the shell, reduces solubility, and can create a pellicle, a partially insoluble membrane, on dissolution testing. The cross-linking risk is not hypothetical; it has caused bioavailability failures for marketed products with aldehyde-generating fill ingredients. FDA’s dissolution test limits for gelatin capsules acknowledge this risk via the two-tier dissolution approach that allows for the use of enzymes in acceptance criteria.
Fourth, gelatin’s biological origin creates supply chain vulnerability tied to animal disease outbreaks (BSE/TSE concerns), geopolitical events affecting livestock supply chains, and the disruptions exposed during the COVID-19 pandemic when raw material availability tightened globally.
HPMC: Technical Profile and Market Position
Hydroxypropyl methylcellulose (HPMC, hypromellose) is the market-leading plant-derived alternative to gelatin for capsule manufacturing. Produced from pine or spruce tree cellulose through etherification, it is classified as Halal, Kosher, and vegan-compliant, and it carries none of gelatin’s animal-origin risks.
HPMC’s technical advantages over gelatin are specific and quantifiable:
Moisture content is 3-8% versus gelatin’s 13-16%. For hygroscopic APIs or moisture-sensitive fill matrices (e.g., lipid-based drug delivery systems, moisture-activated drug release systems), this is a decisive advantage that directly reduces API degradation risk.
Cross-linking risk is essentially zero. HPMC has no protein structure, no lysine residues, and therefore no chemical mechanism by which aldehyde contaminants in the fill or the environment can stiffen the shell. This makes dissolution behavior more predictable and consistent across the product’s shelf life.
Gelling temperature behavior differs from gelatin in a clinically relevant way: HPMC gels at room temperature rather than at body temperature, which can produce a slower dissolution profile in vivo compared to gelatin. For immediate-release formulations, this difference requires explicit characterization during development and may necessitate in vivo bioequivalence confirmation. The difference is manageable with appropriate formulation optimization but cannot be assumed to be equivalent to gelatin without data.
HPMC capsule manufacturing cost is approximately 3-4x that of gelatin capsules at equivalent scale. This cost premium is the primary barrier to universal adoption and is the reason gelatin retains dominance in price-sensitive generic markets.
The HPMC capsule market growth rate is projected at 8.5-9.7% CAGR through 2030, driven by new product launches in biologics, nutraceuticals, and sensitive specialty pharmaceuticals, all segments where HPMC’s technical advantages justify the cost premium.
Pullulan: The Alternative for Oxygen-Sensitive APIs
Pullulan capsules, derived from the fermentation of tapioca starch by Aureobasidium pullulans, represent a third option specifically suited for oxygen-sensitive APIs. Pullulan films have extremely low oxygen permeability compared to both gelatin and HPMC, making them the capsule material of choice for formulations where oxidative degradation via atmospheric oxygen is the primary stability threat. They are plant-derived, Halal and Kosher compliant, and mechanically robust. Their cost exceeds even HPMC, limiting their use to high-value specialty applications where the oxygen-barrier advantage justifies the premium.
Beyond the Capsule Shell: The Full Animal-Free Excipient Audit
Applying a comprehensive animal-free filter requires a systematic audit of every excipient in the formulation, not just the capsule shell.
Magnesium stearate and stearic acid, the near-universal tablet lubricants, are commonly derived from beef tallow or pork-derived fat fractions. Vegetable-derived grades sourced from palm oil are commercially available and must be explicitly specified with supplier certification if animal-free compliance is required. The supplier certificate of origin is a regulatory document in Halal and Kosher certification; it cannot be assumed from the generic chemical name.
Glycerin is a byproduct of biodiesel production (vegetable-derived) or soap manufacturing (historically animal-derived). Synthetic glycerin is also available. The correct grade and origin must be specified at the time of excipient qualification.
Lactose is milk-derived, excluding it from vegan formulations. Its compliance with Kosher certification depends on the specific manufacturing facility’s certification status, as dairy-derived ingredients require separate Kosher-dairy designation that affects product labeling and market positioning.
Shellac, used in modified-release coating systems, is a resin secreted by Laccifer lacca (lac bug) and is thus excluded from vegan formulations. Alternative coating polymers include cellulose acetate phthalate, HPMC phthalate (HPMCP), and Eudragit-series methacrylate polymers, all of which are fully synthetic and animal-origin-free.
Halal, Kosher, and Vegan Certification: Distinct Frameworks Requiring Distinct Strategies
Many formulators treat Halal, Kosher, and vegan requirements as interchangeable. They are not. Each framework has distinct ingredient restrictions, processing requirements, and cross-contamination controls.
Halal compliance prohibits pork and pork derivatives in any form, blood and blood products, alcohol in functional concentrations, and any meat from animals not slaughtered according to Islamic law. It requires documentation of the entire supply chain and, for some certifying bodies, facility-level audits verifying that prohibited substances are not manufactured on shared equipment without validated cleaning procedures. Certifying bodies include IFANCA in North America, JAKIM in Malaysia, and MUIS in Singapore.
Kosher compliance prohibits the mixing of meat and dairy in the same product or on the same equipment. This means a kosher-dairy product (lactose-containing) cannot be produced on the same line as a kosher-meat product (containing animal-derived gelatin or stearates from non-dairy animal sources) without full kosherization of the equipment between runs. Certifying bodies include the Orthodox Union (OU), Star-K, and OK Kosher Certification.
Vegan compliance, as defined by organizations like The Vegan Society, prohibits all animal-derived ingredients, animal-derived processing aids (e.g., bone char used in sugar refining), and ingredients tested on animals. It has no intrinsically religious dimension, which means the certification framework is less standardized than Halal or Kosher but can be stringently enforced by activist consumer groups and retail category managers in natural product channels.
Pharmaceutical companies pursuing multi-market animal-free certification should engage Halal, Kosher, and vegan certification bodies early in the formulation process, ideally at the excipient qualification stage, because retrofitting certification requirements onto an established formulation frequently requires ingredient or supplier changes that trigger regulatory post-approval change filings.
IP Considerations: HPMC Capsule Formulations
HPMC-based formulations, particularly those combining plant-derived capsule shells with specialized fill matrices for moisture-sensitive or oxygen-sensitive APIs, represent patentable formulation inventions where the combination of capsule material, fill excipients, and API performance attributes produces non-obvious technical advantages. A patent landscape review of the HPMC capsule space reveals active filings in extended-release, enteric, and pulsatile release applications. Generic developers evaluating HPMC-based innovator products should conduct freedom-to-operate analyses covering both the capsule material’s use in the specific dosage form context and any manufacturing process patents covering fill-capsule interaction management.
Key Takeaways: Section 5
Gelatin’s four structural vulnerabilities are animal origin exclusion, high moisture content (13-16%), cross-linking susceptibility, and supply chain concentration risk. HPMC capsules eliminate all four at 3-4x the capsule manufacturing cost, with the trade-off of requiring bioequivalence characterization versus gelatin for immediate-release applications. Pullulan capsules provide the lowest oxygen permeability of any standard capsule material, serving oxygen-sensitive APIs at premium cost. A comprehensive animal-free formulation audit extends to lubricants (magnesium stearate origin), plasticizers (glycerin origin), coating materials (shellac), and diluents (lactose). Halal, Kosher, and vegan certifications have distinct, non-interchangeable requirements and should be engaged at the excipient qualification stage, not post-approval.
6. The Alcohol-Free Filter: Solubilization Without the Safety Compromise
Ethanol’s Functional Role and Its Clinical Costs
Ethanol performs two distinct functions in liquid pharmaceutical formulations that make it difficult to replace with a single alternative. As a cosolvent, its semi-polarity bridges the solubility gap between water and hydrophobic APIs, enabling clear solutions that would otherwise be unstable suspensions. As a preservative, at concentrations above 15% it inhibits the full spectrum of bacterial and fungal contaminants relevant to multi-dose products; for preparations with neutral or alkaline pH, effective antimicrobial preservation typically requires 18% or above.
The clinical costs of these functional benefits are concentrated in specific patient populations. Understanding the mechanistic basis for those costs is essential for building a rational alternative strategy.
In neonates, alcohol dehydrogenase (ADH) concentrations are less than 20% of adult levels at birth. CYP2E1, the cytochrome P450 isoform that metabolizes ethanol at higher concentrations, is similarly underdeveloped. This metabolic immaturity means that ethanol ingested from a medicated syrup cannot be cleared at adult rates, leading to systemic accumulation. CNS depression, hypothermia, and severe hypoglycemia, including seizures and coma at toxic doses, are the documented consequences. Long-term neurological effects from chronic low-level ethanol exposure during critical developmental windows are a recognized concern in pediatric neuroscience, though the dose-response relationship in the pharmaceutical context is not fully established.
EMA’s guidance specifies that ethanol should be avoided in pediatric medicines unless technically unavoidable. FDA recommends that OTC products for children under six be ethanol-free, with concentration limits of less than 5% for children ages 6-12 and less than 10% for children over 12. These limits are designed for OTC self-medication; prescription products require case-by-case assessment with explicit risk-benefit documentation.
Beyond pediatrics, ethanol exclusion filters apply to pregnant patients (fetal alcohol syndrome risk at any dose level), patients with liver disease (reduced metabolic clearance), patients recovering from alcohol use disorder (relapse risk from even small ethanol doses), and patients taking CNS depressants including opioids, benzodiazepines, and certain antihistamines where ethanol has synergistic sedative and respiratory-depressant effects.
Solubilization Strategies for Alcohol-Free Liquid Formulations
Replacing ethanol’s solubilization function requires selecting an alternative strategy based on the API’s specific physicochemical properties:
Cosolvency with alternative solvents: Glycerin, propylene glycol, and low-molecular-weight PEGs are water-miscible cosolvents with similar mechanistic action to ethanol. Glycerin is the safest for pediatric use and carries no significant toxicity at pharmaceutical doses. Propylene glycol is effective but carries EMA caution for use in children under four years old and requires dose-based risk assessment for neonates. PEGs introduce the PEG-sensitivity risk discussed in Section 2. The practical formulation approach often involves a blend of cosolvents at sub-toxic individual concentrations to achieve target solubility without exceeding any single solvent’s safety threshold.
pH manipulation and salt formation: For ionizable APIs (weak acids and weak bases, which comprise a large majority of marketed drugs), solubility is a strong function of pH, as described by the Henderson-Hasselbalch relationship. Adjusting the formulation pH to the ionized form of the API dramatically increases aqueous solubility without any organic cosolvent. Buffering agents including citrate, phosphate, acetate, and tartrate systems provide pH stability across the product’s shelf life. This is the highest-preference strategy where the API’s pKa allows it, because it introduces no additional solvent risk.
Micellar solubilization via surfactants: Polysorbates, poloxamers, and d-alpha-tocopheryl polyethylene glycol succinate (TPGS) form micelles that solubilize hydrophobic APIs in their hydrophobic core. Surfactant-based systems are particularly relevant for pediatric oral liquids when pH manipulation is insufficient. The risk-benefit analysis requires evaluating the surfactant’s own safety profile in the target age group; polysorbate 80 carries the PEG-related sensitization risk noted above, and its use in neonatal products requires specific justification.
Cyclodextrin complexation: Beta-cyclodextrins, particularly hydroxypropyl-beta-cyclodextrin (HPβCD), form inclusion complexes with poorly water-soluble APIs by enclosing the hydrophobic drug molecule in the cyclodextrin’s internal cavity. The resulting host-guest complex has dramatically improved aqueous solubility (often 10-100x the uncomplexed API). HPβCD is FDA-approved for parenteral use and has an established safety record in both adult and pediatric populations. The key technical challenge is that complexation requires stoichiometric amounts of cyclodextrin, which can substantially increase the formulation’s mass and manufacturing cost.
Suspension formulation: When none of the solubilization strategies can achieve a stable solution without unacceptable excipient risks, a well-formulated suspension is a viable alternative. Published stability data for alcohol-free furosemide suspensions prepared in Ora-Blend and Ora-Blend SF vehicles demonstrated physical and chemical stability for 30 days, with equivalent potency to the ethanol-containing reference preparation. Suspension development requires careful management of settling rate (via viscosity-imparting suspending agents such as xanthan gum, microcrystalline cellulose-carboxymethylcellulose combinations, or methylcellulose), particle size distribution, and wettability (via low-concentration surfactant addition).
The Preservative Cascade: A Systems-Level Formulation Problem
Removing ethanol’s preservative function activates a secondary selection problem. The replacement preservative must be effective against the relevant microbial challenge for that dosage form and route, must be safe for the target patient population, and must not conflict with the other exclusion filters already applied.
This creates what is usefully framed as a formulation cascade: the decision to exclude ethanol forces a choice among available preservatives, and many of those preservatives carry their own exclusion flags.
Parabens are effective and widely used in oral liquids and topical preparations, but they are known contact sensitizers and appear on EMA and WHO caution lists for pediatric use due to concerns about estrogenic activity at high doses in neonates. Applying both an alcohol-free and a pediatric safety filter simultaneously may exclude parabens as well.
Benzyl alcohol, effective as a preservative in some topical and injectable formulations, is a hard exclusion for neonatal products due to gasping syndrome risk.
Benzalkonium chloride, common in ophthalmic and inhalation products, causes bronchoconstriction in asthmatic patients when used in nebulizer solutions and carries ocular toxicity concerns with long-term ophthalmic use.
Sodium benzoate and sorbic acid are generally considered the preferred alternatives in alcohol-free, pediatric-appropriate oral liquids, but their efficacy is pH-dependent and their concentrations must be validated against relevant USP/Ph. Eur. antimicrobial effectiveness test criteria for the specific dosage form.
The practical conclusion: alcohol-free formulation for pediatric populations requires a systems approach, not an ingredient-by-ingredient swap. The entire preservation strategy must be re-engineered simultaneously with the solubilization strategy, with each component evaluated against the same patient-population-specific exclusion criteria that triggered the alcohol-free requirement in the first place.
Key Takeaways: Section 6
Ethanol serves as both cosolvent and antimicrobial preservative in liquid formulations, and both functions must be replaced when the exclusion filter is applied. Neonatal ADH concentrations below 20% of adult levels create dose-dependent ethanol toxicity risk at therapeutic exposures. EMA guidance recommends ethanol avoidance in pediatric medicines unless technically unavoidable; FDA specifies age-banded concentration limits for OTC products. Replacement solubilization strategies in order of safety preference for pediatric use: pH adjustment and salt formation, cyclodextrin complexation, alternative cosolvent blends (glycerin preferred over propylene glycol), then micellar surfactant systems. Replacing ethanol’s preservative function triggers a secondary excipient selection problem (‘formulation cascade’) where many standard preservatives carry their own pediatric exclusion flags.
7. The Allergen and Sensitizer Filter: Dyes, Preservatives, and Reactive Excipients
The Colorant Problem: Risk-Benefit Is Not Simple
Pharmaceutical colorants perform two functions that exist in tension when a sensitizer filter is applied. First, they make products visually identifiable, providing a safety function that reduces medication errors in polypharmacy settings and institutional pharmacy environments. Second, a subset of commonly used colorants, specifically synthetic azo dyes, causes hypersensitivity reactions in sensitive individuals. Removing colorants eliminates the allergen risk but introduces the medication identification risk. Both risks are real. A rational filter must weigh them against each other for the specific product and patient population.
Tartrazine (FD&C Yellow No. 5, E102) is the best-characterized sensitizing dye. Hypersensitivity reactions including urticaria, angioedema, and aspirin-exacerbated respiratory disease occur in susceptible individuals, particularly those with underlying aspirin sensitivity or atopic disease. FDA requires mandatory label disclosure for tartrazine in any drug product. The EU requires label disclosure and warning text for a broader set of azo dyes under the EMA Annex guideline. One published analysis estimated that up to one-third of marketed medications contain at least one dye with documented allergy associations.
Sunset Yellow (FD&C Yellow No. 6, E110), Allura Red (FD&C Red No. 40, E129), and other azo dyes carry smaller but non-trivial allergenic risk profiles. Carmine (E120), the insect-derived red colorant, has caused anaphylaxis and is excluded under both vegan and allergen-sensitizer filters simultaneously.
The practical approach:
A tiered colorant exclusion strategy, rather than blanket dye-free formulation, serves most patient populations better than total elimination. Tier 1: hard exclusion of tartrazine and other azo dyes with documented high-sensitivity incidence, specifically in products intended for patients with aspirin-exacerbated respiratory disease, atopic disease, or known dye hypersensitivity. Tier 2: use of synthetic dyes with lower sensitization profiles (FD&C Blue No. 1, FD&C Red No. 3) or replacement with naturally sourced colorants (iron oxides, titanium dioxide for opacity, beta-carotene) for products targeting health-conscious or pediatric markets. Tier 3: complete dye-free formulation for products where the therapeutic indication or patient population makes any sensitization risk unacceptable.
For dye-free formulations, API stability implications of removing titanium dioxide must be explicitly assessed. Titanium dioxide in film coatings reduces light transmission to 1-3% of incident radiation, protecting photolabile APIs. Its removal requires either alternative photoprotective coating excipients or upgraded primary packaging with UV-barrier properties, both of which add cost and may require process revalidation.
Sulfites and Asthmatics
Sodium metabisulphite (E223) and potassium metabisulphite (E224), used as antioxidant preservatives in liquid injections and oral solutions, are potent bronchospasm triggers in sulfite-sensitive patients, a population with significant overlap with severe asthmatics. EMA’s excipient guideline requires label warnings and package leaflet information for sulfite-containing products. For any product whose clinical indication or target patient population includes asthmatic or COPD patients, sulfite exclusion is effectively mandatory. Alternative antioxidants with lower sensitization risk include ascorbic acid, sodium ascorbate, and citric acid, though each has different chemical reducing capacity and must be selected based on the specific API’s oxidation vulnerability.
Peanut Oil and Cross-Allergen Risk
Arachis (peanut) oil appears in oil-based injectable formulations and softgel fills because of its lipid composition and oxidative stability. Pharmaceutical-grade arachis oil undergoes extensive refining that reduces the allergenic peanut protein (Ara h 2 and related 2S albumins) to levels typically below ELISA detection limits. Despite this, UK MHRA guidance advises that peanut-allergic patients should avoid products containing peanut oil, and product labeling must declare its presence. Cross-reactivity with soy is clinically documented; patients with confirmed peanut allergy should be evaluated for soy sensitivity before prescribing soy-excipient-containing products.
Aspartame and Phenylketonuria
Aspartame (E951), used as a sweetener in chewable and orally disintegrating tablets and some oral liquid formulations, is metabolized to phenylalanine. Phenylketonuria (PKU), a genetic deficiency in phenylalanine hydroxylase, results in accumulation of phenylalanine and its metabolites to neurotoxic levels. PKU prevalence runs approximately 1 in 10,000 to 1 in 15,000 births in most European and North American populations. For products containing aspartame, FDA and EMA both require mandatory phenylalanine content disclosure on the label, and clinicians managing PKU patients must actively exclude aspartame-containing formulations from all prescriptions.
Key Takeaways: Section 7
Up to one-third of marketed medications contain at least one dye associated with allergic reactions. Tartrazine is the highest-risk synthetic azo dye and requires mandatory FDA label disclosure; blanket dye-free formulation may introduce medication error risk in polypharmacy settings, requiring a tiered colorant exclusion strategy rather than total elimination. Titanium dioxide removal for opacity/photoprotection purposes requires compensatory packaging or coating changes. Sulfite antioxidants are hard exclusions for asthmatic patient populations. Peanut oil requires label disclosure and avoidance guidance regardless of refining degree. Aspartame requires phenylalanine content disclosure and is a hard exclusion for phenylketonuria patients.
8. Manufacturing and Scale-Up: From Lab Bench to Commercial Reality
The Ripple Effect: How One Excipient Change Propagates
Post-approval reformulation is one of the most underestimated financial risks in pharmaceutical portfolio management. The direct cost of the reformulation project itself, covering analytical development, stability studies, manufacturing validation, and regulatory submission, is only the visible portion. The larger costs are indirect: timeline delay, manufacturing line downtime, inventory write-offs for the transitioning product, and potential market share loss if supply gaps occur during the transition.
Understanding how a single excipient substitution propagates through manufacturing is essential for accurate project scoping:
Replacing a free-flowing excipient like spray-dried lactose with a cohesive material like fine-grade MCC affects powder flow from the hopper to the die, die fill uniformity, tablet weight variability, and content uniformity. If the blend’s Carr Index moves from below 20 (free-flowing) to above 25 (cohesive, poor flow), the manufacturing process must shift from direct compression to granulation to restore acceptable powder flow. This is not a formulation tweak; it is a manufacturing process change requiring full process validation, updated batch records, and potentially equipment qualification for the granulation unit operation.
Replacing a binder or filler that contributes significantly to tablet compressibility can shift the compression force required to achieve target tablet hardness outside the equipment’s validated operating range. This may necessitate a press speed reduction (reducing throughput and increasing cost per batch), a change in punch/die geometry, or a switch to a higher-capacity press with different validated parameters.
The biopharmaceutical consequences of excipient replacement require equal attention. Switching from a soluble filler (lactose) to an insoluble one (MCC) changes the mechanism of tablet disintegration from dissolution-driven erosion to swelling-driven rupture. This alters both the rate and pattern of drug release, and the difference may be invisible in dissolution testing at a single pH but visible in the biorelevant dissolution conditions (fasted-state simulated intestinal fluid, FeSSIF/FaSSIF) relevant to predicting in vivo performance. For any BCS Class II or IV drug, this mechanistic change in disintegration behavior requires formal dissolution modeling and likely an in vivo bioequivalence study before the reformulation can be approved.
Regulatory Mechanics of Post-Approval Changes
In the United States, post-approval changes to an approved NDA or ANDA are governed by FDA’s SUPAC (Scale-Up and Post-Approval Changes) guidance documents. Excipient changes are categorized by their potential impact on product quality:
A change in the type or grade of an excipient typically qualifies as a Level 2 or Level 3 change under SUPAC-IR (immediate release) or SUPAC-MR (modified release) depending on the magnitude of change. Level 2 changes require a CBE-30 supplement (Changes Being Effected in 30 Days), allowing the change to be implemented 30 days after submission if FDA does not object. Level 3 changes require a Prior Approval Supplement (PAS), which must be approved by FDA before implementation, typically requiring 6-18 months of review time.
A reformulation that changes a ‘critical’ excipient for immediate-release tablets, defined as one that significantly affects bioavailability, or that changes the type of modified-release polymer in a controlled-release system, almost always requires a PAS with full in vivo bioequivalence data. This is the most resource-intensive and time-consuming regulatory pathway for post-approval changes in solid oral dosage forms.
In the European Union, the equivalent framework is the Variations Regulation (EC) No. 1234/2008. A change in the qualitative and/or quantitative composition of excipients is typically a Type II variation (requiring a full assessment procedure) or a Type IB variation (requiring 30 days notification), depending on its potential impact on safety and efficacy.
Excipient Variability: The Under-Recognized Scale-Up Risk
Published research on excipient variability documents a consistent finding: the same excipient from different suppliers, or different lots from the same supplier, can have sufficiently different physical properties (particle size distribution, surface area, bulk density, crystallinity) to produce tablets with meaningfully different dissolution profiles and mechanical properties when all other process parameters are held constant.
This variability is not a quality failure; it reflects the inherent complexity of excipient manufacturing from natural or semi-synthetic feedstocks. Its risk management implication is that excipient specifications in the regulatory filing must go beyond identity and assay to include physical attribute limits that are directly linked to the formulation’s design space. Incoming material testing must verify these physical attributes, not just chemical identity, for every incoming lot.
For novel or co-processed excipients available from a single manufacturer, supply concentration risk adds a dimension beyond variability. A quality or regulatory issue at the sole supplier halts supply of the excipient and, consequently, production of the drug product. This scenario, which occurred for several specialty excipients during COVID-19 supply chain disruptions, argues for dual-sourcing excipient qualification programs as part of supply chain risk management for any excipient that is both critical to the formulation’s performance and available from a limited supplier base.
The Formulation Lock-In Effect: Why Early Is Always Better
Post-approval reformulation’s regulatory, technical, and commercial costs create a powerful inertia against change once a product is approved. For generic products with thin margins, the cost of a PAS submission and supporting bioequivalence study can exceed the product’s annual profit, making reformulation economically unviable regardless of the clinical rationale. For branded products, the opportunity cost of diverting formulation development resources away from pipeline programs toward reformulating approved products is a constant competitive pressure.
These dynamics establish a clear strategic principle: the Excipient Exclusion Filter must be applied during initial development, before pivotal clinical studies begin. A formulation that is optimized for patient-centricity, IP defensibility, and regulatory efficiency from the outset will substantially outperform one that achieves these objectives through costly post-approval retrofitting. The pre-clinical and Phase I formulation development window, typically 18-36 months in a standard development program, is where the exclusion filter delivers its highest return on investment.
Key Takeaways: Section 8
A single excipient substitution can cascade into manufacturing process changes (direct compression to granulation), equipment qualification updates, new stability studies, and in vivo bioequivalence studies. FDA SUPAC classifies excipient changes as Level 2 (CBE-30) or Level 3 (PAS) based on potential bioavailability impact; PAS requires FDA approval before implementation with 6-18 months typical review time. Excipient variability between suppliers and lots is a documented source of product performance variability; physical attribute specifications and incoming material testing must be included in the control strategy. Single-source specialty excipients require dual-source qualification programs to manage supply chain concentration risk. The pre-pivotal clinical development window delivers the highest ROI from the Excipient Exclusion Filter; post-approval reformulation costs make early application economically essential.
9. Formulation as IP: Using Exclusion Filters to Build a Multi-Layered Patent Fortress
The IP Value of Formulation Patents
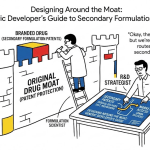
The composition of matter patent on an API is the most valuable intellectual property asset in a pharmaceutical portfolio. But it is also the most time-limited and the hardest to extend. Formulation patents, which claim the specific combination of an API with excipients, dosage form design, release mechanisms, or manufacturing processes, are the primary mechanism for extending meaningful market exclusivity beyond primary patent expiry. They constitute the second and third walls of the patent fortress that sophisticated pharma IP teams construct around successful products.
The commercial value of formulation patent coverage is directly observable in Paragraph IV litigation statistics. Between 2000 and 2024, formulation and method-of-use patents were the subject of the majority of Paragraph IV challenges and Orange Book patent disputes, precisely because they represent the last line of patent protection standing between a branded product and generic entry at a time when the API patent has expired or been invalidated.
DrugPatentWatch data on multi-patent drug products consistently shows that products with three or more formulation patents listed in the Orange Book maintain significantly longer periods of exclusivity after primary API patent expiration than products with composition-of-matter-only protection. The quantitative value of each additional formulation patent, measured in months of market exclusivity maintained, runs into hundreds of millions of dollars for high-revenue products.
How the Exclusion Filter Generates Patentable Inventions
The most counterintuitive insight in excipient strategy is that the constraint imposed by an exclusion filter is itself an IP opportunity. When a formulator is barred from using the standard, obvious excipient combination and is forced to find an alternative, the resulting solution is more likely to be non-obvious, the core patentability requirement, than a formulation that simply uses the industry default.
The formal analysis of a lactose-free formulation for a primary amine drug that achieves bioequivalent dissolution through a specific combination of mannitol grades, a co-processed binder, and a novel disintegrant is a potentially patentable combination, because the selection rationale, the technical problem it solves, and the specific combination of elements chosen to solve it may not be obvious to a person of ordinary skill in the art from the prior art. The same API formulated with lactose, MCC, and magnesium stearate, the default combination, would not be patentable as a formulation because it is obvious.
The exclusion filter’s constraint, the demand to formulate without a standard ingredient, thus functions as an innovation forcing function that generates non-obvious technical solutions, and non-obvious solutions are the raw material of patent prosecution.
Patent Intelligence Tools: DrugPatentWatch for Competitive Formulation Analysis
Effective formulation IP strategy requires systematic competitive intelligence on the patent landscape. DrugPatentWatch provides the operational infrastructure for this analysis, aggregating Orange Book listings, FDA regulatory filings, global patent databases, and market exclusivity data into a searchable intelligence platform.
For branded pharmaceutical companies executing lifecycle management, the workflow is:
Identify the primary API patent’s expiration date and any granted pediatric exclusivity or orphan drug extensions. Map all Orange Book-listed formulation and method-of-use patents, their claim scope, expiration dates, and any pending Paragraph IV challenges. Identify the technical problems that the existing approved formulation does not address: sensitivity populations it excludes, administration challenges it creates, stability limitations it imposes. Use the exclusion filter framework to develop a reformulated product that addresses one or more of these unmet needs. File formulation patents on the new formulation before any clinical or regulatory work begins, to establish priority date.
This sequence creates a new Orange Book-listed patent with a later expiration date than the primary composition-of-matter patent, extending the period during which generic entry requires Paragraph IV certification and provides the innovator with a 30-month stay of generic approval. Done correctly across multiple line extensions, this approach can maintain meaningful market exclusivity for five to ten years beyond primary patent expiry.
For generic and 505(b)(2) companies, the workflow is:
Identify the innovator’s formulation patent claims in detail, understanding both the literal claim scope and the range of equivalents that might be asserted. Apply the exclusion filter framework in reverse: instead of excluding excipients for patient-safety reasons, exclude the innovator’s patented excipient combinations from the design space. This ‘design-around’ strategy guides R&D toward formulations that are bioequivalent to the RLD but non-infringing on the innovator’s formulation patents. For 505(b)(2) applicants, the design-around formulation can be improved relative to the RLD on patient-centricity dimensions (lactose-free, gelatin-free, alcohol-free), creating a differentiated product with its own patentable features and commercial positioning.
White-space analysis is the complement to design-around. By mapping all existing patents in a therapeutic area’s formulation space, including both the innovator’s patents and those of other generic and specialty pharma players, a company can identify formulation approaches that are unprotected. If all existing patents for a given API claim solid oral tablets, and the target patient population has significant swallowing difficulties (dysphagia is prevalent in neurological conditions), a patent application on a novel orally disintegrating tablet or oral suspension formulation occupies unprotected territory. This is not incremental IP; it is foundational IP on an unserved patient need.
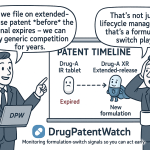
Formulation Patent Lifecycle: Technology Roadmap for a Branded Product
Year 0-5 (Pre-approval to Launch): File composition-of-matter patent (or confirm in-license). Begin pre-clinical formulation development applying the Excipient Exclusion Filter for the primary indication and primary patient population. File formulation patent on the specific clinical trial formulation, including excipient identities, concentrations, manufacturing process, and demonstrated performance characteristics.
Year 3-7 (Post-launch, Market Establishment): Initiate line extension programs targeting secondary patient populations identified during Phase III (pediatric, geriatric, renal impairment populations often requiring dose adjustments and formulation adaptations). File formulation patents on each line extension.
Year 7-12 (Pre-LOE Lifecycle Management): Launch line extensions. Initiate Paragraph IV defense strategy for any innovator formulation patents being challenged. File additional patents on manufacturing process improvements, new analytical methods, or combination products if relevant. Identify 505(b)(2) opportunities for delivery system upgrades (extended release, ODT, transdermal).
Year 12-20 (Post-LOE): Authorized generics strategy where formulation IP remains protective. Biosimilar formulation patents if applicable. New formulation IP on combination products or novel delivery systems.
Key Takeaways: Section 9
Formulation patents are the primary mechanism for extending commercial exclusivity beyond primary API patent expiration; products with three or more Orange Book-listed formulation patents maintain substantially longer exclusivity periods than API-patent-only protected products. The exclusion filter’s design constraint generates non-obvious technical solutions, making formulation IP filing more defensible than obvious, default-excipient formulations. DrugPatentWatch and similar patent intelligence platforms provide the operational infrastructure for competitive landscape mapping, design-around strategy, and white-space identification. A structured formulation IP roadmap covering pre-approval through post-LOE phases maximizes the commercial return on formulation investment.
10. The Future of Excipient Science: Smart Materials, AI, and Precision Formulation
Co-processed and Multifunctional Excipients: The Near-Term Frontier
The pharmaceutical excipient market is projected to reach $15.49 billion by 2034, and the fastest-growing segment within it is co-processed and multifunctional excipients. These engineered materials, produced by spray drying, hot melt extrusion, or fluid bed granulation of two or more standard excipients, offer a combination of functional attributes that no single-entity excipient can match.
A co-processed mannitol-MCC particle, for example, engineers the compressibility of MCC and the flowability of coarse-grade mannitol into a single particle morphology that enables robust direct compression tableting without the segregation risk inherent in blending the two separate powders. The co-processing creates composite particles where the component excipients are physically integrated at the particle level, not merely mixed. This integration produces superior and more consistent functional performance, reducing lot-to-lot variability from the physical blending step.
For the Excipient Exclusion Filter framework, co-processed excipients offer a specific advantage: they can provide turnkey lactose-free, vegan-compliant, or low-moisture solutions for formulation challenges that would otherwise require complex multi-excipient optimizations. The trade-off is that single-source availability creates supply chain concentration risk that requires explicit management through supplier qualification programs and safety stock strategies.
Artificial Intelligence in Formulation Development
Machine learning applications in pharmaceutical formulation development are advancing rapidly from research interest to commercial deployment. The computational approach addresses the core inefficiency of traditional formulation development: the combinatorial explosion of possible excipient combinations, concentration ranges, and manufacturing process parameters that make comprehensive experimental exploration economically impossible.
Current AI formulation platforms apply neural networks and Gaussian process regression to datasets of API physicochemical properties, excipient material attributes, and historical stability and performance outcomes. The models predict which excipient combinations are most likely to achieve target dissolution profiles, stability specifications, and manufacturing process robustness metrics without requiring exhaustive experimental screening.
For the Excipient Exclusion Filter, AI integration offers a specific capability: predictive exclusion. Instead of requiring the formulator to manually identify all potential API-excipient incompatibilities from literature and structural analysis, an AI model trained on large datasets of incompatibility observations can automatically flag potential Maillard, oxidation, and aldehyde-adduct risks for a given API structure, effectively automating Step 2 of the four-step framework described in Section 3.
Early implementations of this approach have demonstrated reduction in the number of formulation screening experiments required before identifying an optimal candidate by 40-60% compared to traditional design of experiments approaches. This is not marginal efficiency gain; it is a compression of the formulation development timeline that can move a candidate from API selection to first-in-human trial formulation in significantly less time.
Smart Excipients and Stimuli-Responsive Drug Delivery
‘Smart’ excipient technology refers to polymers and materials that modify drug release behavior in response to physiological stimuli, specifically pH, temperature, enzyme activity, redox potential, or mechanical force. These materials convert the dosage form from a passive container to an active participant in drug delivery.
pH-responsive polymers, including Eudragit L100 (dissolves above pH 6.0) and Eudragit S100 (dissolves above pH 7.0), are already commercially deployed in enteric coating systems. Their next-generation successors target even more precise pH thresholds corresponding to specific disease states; tumor microenvironments are characteristically acidic (pH 6.0-6.5), and pH-responsive release targeted to this microenvironment is an active oncology delivery research area.
Temperature-responsive polymers based on poly(N-isopropylacrylamide) chemistry undergo a sharp solubility transition near body temperature, enabling injectable in-situ gelling depot systems that transition from free-flowing liquid at room temperature (easy to administer) to solid depot at 37°C (providing controlled release over days to weeks). This approach eliminates the solubilization challenges of poorly water-soluble long-acting injectable APIs without requiring organic cosolvents or complex lipid vehicles.
Enzyme-responsive systems exploit the overexpression of specific enzymes in disease tissue (proteases in tumor stroma, phospholipases at inflammatory sites) to trigger drug release selectively at the pathological site. These systems are predominantly in pre-clinical and early clinical development but represent a direction where excipient design directly determines therapeutic precision.
The Generative Formulation Model: From Exclusion to Creation
The Excipient Exclusion Filter, as currently practiced, is a process of elimination: a defined set of exclusion criteria removes problematic excipients from the candidate space, and the formulator then optimizes within the remaining design space. This approach is effective but inherently reactive to existing excipient options.
The next generation of formulation design will likely invert this logic. A generative AI model, trained on the full corpus of excipient science, formulation performance data, patient biology data, and regulatory precedent, will accept as inputs the API’s molecular structure, the target clinical performance profile, and the patient population’s biological characteristics (genetic profile, microbiome composition, relevant disease biomarkers). The model will not simply exclude problematic options from an existing catalog; it will propose novel excipient combinations, or even flag gaps where new excipients need to be developed, to achieve a specific performance objective for a specific patient.
This represents a shift from formulation optimization within a fixed excipient toolkit to formulation design as a generative creative process constrained by biology, chemistry, and regulation simultaneously. The companies building the data infrastructure for this generative approach today, by systematically collecting and curating formulation performance data across their development programs, will have a significant advantage in the next decade of pharmaceutical development.
Key Takeaways: Section 10
Co-processed excipients are the highest-growth segment of the pharmaceutical excipients market and provide turnkey solutions for multi-attribute formulation challenges at the cost of supply chain concentration risk. AI formulation platforms demonstrate 40-60% reduction in required experimental screening efforts, compressing development timelines and reducing pre-clinical costs. Smart excipients that respond to pH, temperature, and enzyme activity are the enabling technology for precision drug delivery; commercial deployment is advancing from enteric coatings to injectable depots to early-stage tumor-targeted systems. The future formulation paradigm shifts from exclusion-based elimination to generative algorithmic design, where patient-specific biological parameters drive excipient selection rather than the reverse.
11. Investment Strategy for Portfolio Managers and Institutional Analysts
How to Value Excipient IP in a Pharmaceutical Portfolio
Excipient strategy is a material valuation variable for pharmaceutical portfolios that is routinely underweighted by generalist analysts. The following framework provides a structured approach to excipient IP valuation.
Formulation patent expiration mapping: For any product under coverage, map the full Orange Book patent listing including formulation patents. A product with primary API patent expiry in 2027 but formulation patents expiring in 2033 has a meaningful additional exclusivity window that must be discounted for generic entry risk, but represents real value if those formulation patents are defensible. DrugPatentWatch’s patent expiry data and Paragraph IV challenge tracking provide the operational basis for this analysis.
Patient population access analysis: A product with a standard excipient formulation (lactose-containing, gelatin capsule) that serves a therapeutic area with high prevalence of lactose intolerance, religious dietary restrictions, or alcohol sensitivity has a quantifiable addressable market reduction relative to a patient-centric alternative formulation. For CNS products targeting East Asian markets where lactase non-persistence exceeds 90%, a lactose-free reformulation is not a niche play; it is a market access strategy.
Line extension pipeline valuation: Pharmaceutical companies with active lifecycle management programs built on patient-centric reformulation (pediatric-appropriate formulations, gelatin-free alternatives, alcohol-free liquids) have identifiable revenue upside from these programs that is sometimes disclosed in pipeline reports but more often requires bottom-up valuation from clinical trial registries, patent filings, and regulatory submissions. When a 505(b)(2) NDA for a line extension is filed, it typically adds 3-5 years of market exclusivity on the new formulation, with addressable market size depending on the specificity of the patient population being targeted.
Excipient company equity considerations: The HPMC capsule market, co-processed excipient segment, and cyclodextrin market are all growing at CAGRs that exceed the broader pharmaceutical excipients market average of approximately 6-7%. Companies with leading positions in these segments, including Lonza, ACG Capsules, Roquette, IMCD, and ABITEC, have revenues directly tied to the growing demand for patient-centric and technically sophisticated excipient solutions.
Generic entry risk assessment: For covered innovator products approaching loss of exclusivity (LOE), the defensibility of remaining formulation patents is the key variable in generic entry timing models. A formulation patent with narrow, clearly-drafted claims that covers a specific technical solution to a well-defined formulation problem is more defensible than a broad formulation patent with claims that may not be novel or non-obvious over the prior art. Patent invalidity via inter partes review (IPR) at the USPTO has invalidated a significant fraction of formulation patents challenged in the past decade; the prosecution history and claim specificity of each formulation patent must be assessed before using it as a major exclusivity assumption in a loss-of-exclusivity model.
12. Key Takeaways
Excipients constitute approximately 90% of a finished dosage form by mass and govern stability, bioavailability, immunological tolerability, and manufacturing processability. The ‘inactive ingredient’ designation is a regulatory classification, not a pharmacological one, and treating it as the latter has cost the industry billions in late-stage formulation failures.
The Excipient Exclusion Filter is a four-step proactive risk management framework: define the TPP and patient population, characterize the API’s incompatibility risk profile, screen candidates against regulatory databases (FDA IID, EMA Annex), and integrate outputs into the QbD control strategy as formal CQA-linked CMAs.
92.8% of oral medicines contain at least one ingredient with allergen potential. The highest-risk excipients by mechanism include reducing sugars (Maillard reaction with amine APIs), benzyl alcohol (neonatal gasping syndrome), tartrazine (azo dye hypersensitivity), PEG and polysorbates (anaphylaxis in sensitized patients), sulfites (bronchospasm in asthmatics), and porcine/bovine gelatin (religious and ethical exclusions).
Lactose replacement for a BCS Class II or IV API is a high-stakes project requiring comparative in vitro dissolution profiling across multiple pH conditions and typically an in vivo bioequivalence study. Dextrates provide the lowest-risk 1:1 replacement for spray-dried lactose in direct compression. Co-processed excipients provide superior performance at higher cost and supply chain concentration risk.
HPMC capsules eliminate gelatin’s four structural liabilities (animal origin, high moisture, cross-linking susceptibility, supply chain vulnerability) at 3-4x the capsule manufacturing cost. Pullulan capsules provide superior oxygen barrier performance for oxygen-sensitive APIs at further cost premium.
Alcohol-free formulation for pediatric products requires simultaneous resolution of solubilization (preferred: pH adjustment, cyclodextrin complexation, alternative cosolvents) and preservation (preferred: sodium benzoate, sorbic acid in pH-appropriate systems) without triggering secondary exclusion flags for the replacement preservatives.
Formulation patents are the primary post-primary-patent exclusivity mechanism. Products with three or more Orange Book-listed formulation patents maintain significantly longer exclusivity periods than API-patent-only products. The exclusion filter’s design constraints generate non-obvious technical solutions with stronger IP defensibility than default-excipient formulations.
Post-approval reformulation carries enormous regulatory, technical, and commercial costs. The highest ROI from the Excipient Exclusion Filter comes from its application in the pre-pivotal clinical development window, before first-in-human studies lock in the formulation.
AI formulation platforms currently demonstrate 40-60% reduction in required experimental screening, and the near-term trajectory points toward generative formulation design where patient-specific biological data drives excipient selection.
13. Frequently Asked Questions
Q: What is the first operational step when tasked with a lactose-free reformulation of an approved tablet?
A: Characterize both the current formulation and the API before touching an excipient catalog. Document the functional role lactose plays in the existing product, whether it is the primary filler in a direct compression process, a co-binder in a wet granulation, or a flow enhancer at lower concentrations. Determine the API’s BCS class, because this single variable sets the level of bioequivalence risk and determines the scope of the development program. A BCS Class I reformulation with a 1:1 dextrates replacement is a straightforward project. A BCS Class IV reformulation requires a full dissolution modeling program and almost certainly an in vivo bioequivalence study, which means a materially different budget, timeline, and risk profile. Those project parameters need to be established before the first kilogram of alternative excipient is ordered.
Q: Is HPMC always the right choice over gelatin for a new capsule product?
A: For new products where the API is moisture-sensitive, where the fill contains aldehyde-generating ingredients, or where the commercial strategy requires Halal, Kosher, or vegan compliance, HPMC is generally the correct choice on technical merits, and the cost premium is justified by risk reduction. For a robust, non-hygroscopic API in a price-sensitive generic market where dietary compliance is not a label claim, gelatin’s cost and machinability advantages may make it the better commercial decision. The decision should be a documented risk-benefit analysis against the specific API and commercial context, not a default either way.
Q: How do we justify the higher cost of co-processed or specialty excipients to management?
A: Frame the justification in total value, not unit cost. A co-processed excipient that enables direct compression (eliminating a granulation step) reduces capital expenditure, energy cost, batch cycle time, and cleaning validation scope. The cost comparison is not ‘expensive excipient vs. cheap excipient’ but ‘expensive excipient plus simple process vs. cheap excipient plus expensive process.’ The second comparison often favors the specialty excipient on total cost of goods. Additionally, a formulation that requires a specialty excipient is less easily replicated by generic competitors, providing IP and market defensibility that has quantifiable revenue value.
Q: Our API is BCS Class II and poorly water-soluble. How do we formulate an alcohol-free pediatric oral liquid?
A: This is the hardest case in pediatric formulation. The preferred sequence: first, check whether pH manipulation can achieve the required solubility. If the API is a weak base, acidifying the formulation to below its pKa will dramatically increase solubility; citrate or acetate buffers at pH 3.5-5.0 often suffice for basic APIs and are well-tolerated in pediatric populations. If pH manipulation is insufficient, evaluate HPβCD complexation; its safety record in pediatric populations is established, and its solubilization capacity for lipophilic APIs is substantial. If complexation does not achieve target concentration, a cosolvent blend using glycerin as the primary cosolvent with minimal propylene glycol may be necessary, with explicit dose-based safety assessment against EMA pediatric propylene glycol limits. If none of these approaches achieves a stable solution at the required dose concentration, develop a suspension: a validated wetting agent plus suspending agent combination (xanthan gum or microcrystalline cellulose-carboxymethylcellulose systems) will provide physical stability; preservative selection from sodium benzoate or sorbic acid based on target pH; and re-suspend instructions on the label. Document every step of this decision tree in the pre-formulation report.
Q: We are a generic company. How does the exclusion filter framework apply to our development strategy?
A: Two applications, each with distinct commercial logic. For standard ANDA targets, analyze the innovator’s Orange Book-listed formulation patents before committing to a formulation approach. Apply the exclusion filter in reverse: exclude the innovator’s patented excipient combinations from your design space. This is not about patient-centricity initially; it is about freedom-to-operate. The design-around formulation must be bioequivalent and non-infringing. For 505(b)(2) opportunities, patient-centricity becomes the commercial differentiator. Identify the unmet patient need in the current approved formulation. A lactose-free version of a blockbuster tablet, a vegan-certified version of a gelatin-capsule product, or an alcohol-free pediatric version of an adult oral liquid each addresses a documented market need. The 505(b)(2) pathway allows you to rely on the innovator’s safety and efficacy data while differentiating on formulation. A successful 505(b)(2) application for a patient-centric reformulation can carry three years of new clinical investigation exclusivity, providing market protection in a segment where the original product does not adequately compete.
This report is prepared for pharmaceutical and biotech IP teams, portfolio managers, R&D leadership, and institutional investors in the life sciences sector. It reflects publicly available regulatory guidance, published scientific literature, and patent database information as of April 2026. It does not constitute legal advice or investment recommendation. Drug patent and exclusivity data referenced herein should be verified against current DrugPatentWatch filings and official regulatory agency databases before commercial decision-making.
Copyright © DrugPatentWatch. Originally published at https://www.drugpatentwatch.com/blog/