Target Audience: Pharma/biotech IP counsel, ANDA portfolio managers, R&D leads, CMC directors, and institutional investors tracking complex generics pipelines.
1. Why Generic Formulation Is Harder Than It Looks

The economics of generic pharmaceuticals are well understood. When a brand-name drug’s market exclusivity expires, generic entry typically drives prices down by 80% or more within the first year. In the United States, generic drugs filled roughly 90% of all prescriptions in 2023 while accounting for approximately 18% of total prescription drug spend. The Association for Accessible Medicines estimates generics saved the U.S. healthcare system $408 billion in 2022 alone.
What analysts and even many R&D executives consistently underestimate is the technical cost of capturing that value. Developing a successful ANDA is not a reverse-engineering exercise in the casual sense of the term. It is a full-scale pharmaceutical development program constrained by three forces that do not apply to innovator development: patent avoidance requirements, bioequivalence mandates, and the economics of compressed timelines.
A new molecular entity developer has the luxury of iterating formulation strategy over a decade, with clinical data constantly feeding back into the design. A generic developer has 18 to 36 months to replicate the performance of that decade of work, without access to the innovator’s process data, excipient grade specifications, or manufacturing know-how. The product must perform identically in the human body. The process to make it can differ entirely. That tension between identical output and completely different input is the core technical problem of generic formulation.
For extended-release oral products, the degree of difficulty is another order of magnitude higher. For sterile injectables, transdermal systems, and complex inhalers, it rises again. Understanding why requires starting where the project starts: the patent landscape.
2. The Patent Estate: What IP Teams Miss When Targeting an RLD
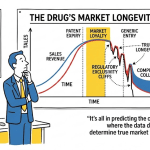
2.1 The Patent Cliff Is Not One Date. It Is a Sequence.
The term ‘patent cliff’ is shorthand that has caused more strategic errors in generic portfolio planning than any other simplification in the industry. The phrase implies a single drop-off point. In reality, the IP protection around any commercially significant drug product is a layered set of barriers that expire on different dates, cover different aspects of the product, and respond differently to legal challenge.
The typical patent estate for a blockbuster small-molecule product includes a composition-of-matter patent on the API molecule itself, one or more polymorph patents covering specific crystalline forms, formulation patents describing the drug delivery system, process patents covering synthesis or manufacturing methods, and method-of-use patents tied to specific therapeutic indications. The FDA’s Orange Book lists the patents the innovator has certified as covering the approved product. What the Orange Book does not tell you is which of those patents are actually enforceable, which are weak on prior art grounds, and which cover the specific approved dosage form versus the molecule generally.
Generic teams that plan entry based on the earliest Orange Book expiration date and ignore the full estate regularly find themselves facing injunctions that push commercial launch years past their modeled date. The 30-month stay triggered by a Paragraph IV certification filing means any litigation initiated within 45 days of ANDA receipt can delay approval regardless of scientific readiness.
2.2 Patent Intelligence Tools: What Competent IP Analysis Looks Like
Platforms like DrugPatentWatch provide structured access to Orange Book listings, Paragraph IV litigation histories, exclusivity period tracking, and patent claim-level analysis for both brand and ANDA filers. For any target product, a complete IP analysis should answer at least seven questions before formulation work begins:
Which composition-of-matter patents cover the approved API, and when do they expire with and without Patent Term Restoration? Which polymorph patents exist, and has the innovator actually validated those polymorphs in the approved product? Has the formulation technology been separately patented, and does that patent describe functional elements our proposed formulation would necessarily replicate? Have other ANDA filers already challenged these patents under Paragraph IV, and what were the outcomes? Are there process patents that would restrict API sourcing from specific manufacturers? Do any SPCs (Supplementary Protection Certificates) extend protection in EU jurisdictions that affect parallel market strategy? What pediatric exclusivity periods exist, and are they stacked behind other exclusivities?
The answers to these questions define the actual entry window and, critically, the technological constraints within which formulators must work. A formulator who does not know the patent landscape cannot design around it.
2.3 The Toprol-XL Patent Estate: A Worked Example
AstraZeneca’s Toprol-XL (metoprolol succinate extended-release tablets) illustrates how a patent estate shapes every downstream technical decision. The innovator’s core delivery technology relied on a multi-particulate system built around controlled-release pellets. The specific architecture of those pellets, the polymer systems used for coating, and the compression process that assembled them into a tablet were all protected by formulation and process patents layered beyond the core API coverage.
Any generic developer targeting Toprol-XL had to answer one question before designing a single experiment: can we achieve the same pharmacokinetic profile through a structurally different drug delivery mechanism? The answer was yes. Hydrophilic matrix technology, built around swellable HPMC polymers rather than coated pellets, could produce a bioequivalent dissolution profile. But that determination required patent claim-level reading, not just expiration date monitoring.
2.4 IP Valuation of the Toprol-XL Franchise
For portfolio managers and deal teams, the IP valuation of the Toprol-XL franchise at the time of generic entry illustrates how patent structure translates into revenue modeling. The product peaked at roughly $1 billion in annual U.S. sales. The multi-layered patent estate supported approximately five years of post-composition-of-matter protection via formulation and pediatric exclusivity extensions.
For the first generic filer, the 180-day exclusivity period under Hatch-Waxman created a revenue window estimated at $200 to $400 million in the U.S. market depending on launch timing and competitive dynamics. That exclusivity, however, was only accessible to companies that: filed a Paragraph IV certification, prevailed in or settled the subsequent patent litigation, and had a technically defensible non-infringing formulation ready at approval. Companies that failed on the technical dimension lost the exclusivity period entirely, even when they won the legal battle.
The calculation reinforces a structural reality in generic portfolio strategy: IP analysis and formulation capability are not sequential workstreams. They are parallel dependencies. A company that wins in court but cannot manufacture a bioequivalent product is out of the money.
Key Takeaways: Patent Strategy
IP teams should treat the Orange Book as a starting point, not a complete picture. Every target product requires claim-level patent analysis across composition, polymorph, formulation, process, and method-of-use categories. The formulation team should receive the IP analysis before beginning pre-formulation work, so that technological constraints are incorporated from day one. Exclusivity period valuation should stress-test for litigation delay scenarios. A 30-month stay on a product with 180-day FTF exclusivity can convert a projected $300 million revenue window into a $50 million residual.
3. Toprol-XL and Metoprolol Succinate ER: The Case Study Anchor
3.1 Why This Product Is the Standard Teaching Case
Metoprolol succinate extended-release tablets occupy a specific position in the generic formulation literature: they are difficult enough to be instructive but well-characterized enough to be tractable. The therapeutic category (cardiovascular, beta-blockade) has tolerably well-understood PK-PD relationships. The innovator product was a commercial blockbuster with years of clinical and real-world data. And the formulation challenge, matching a 24-hour release profile for a highly water-soluble BCS Class I drug without copying the innovator’s multi-particulate architecture, captures almost every major principle of ER generic development in a single product.
The drug itself is a beta-1 selective adrenergic receptor blocker approved for hypertension, stable angina, heart failure with reduced ejection fraction, and post-MI management. The succinate salt form was chosen for the extended-release product precisely because of its superior aqueous solubility and stability versus the tartrate salt used in immediate-release formulations. That high solubility, approximately 500 mg/mL at 25 degrees Celsius, is exactly what makes ER formulation difficult. The drug wants to dissolve immediately. The formulation has to prevent it from doing so over 24 hours.
3.2 The Toprol-XL Multi-Particulate System: What the Innovator Built
AstraZeneca’s Toprol-XL uses a system in which metoprolol succinate is loaded onto inert pellets or beads via layering, followed by application of a rate-controlling polymer film coat. The coated pellets are then compressed into a tablet with suitable excipients. Upon ingestion, the tablet disintegrates in the GI tract, releasing the individual pellets. Each pellet then functions as an independent drug delivery unit, releasing metoprolol at a rate determined by the permeability and thickness of its polymer coat.
The multi-particulate architecture has three distinct advantages over a monolithic matrix. First, drug release is not dependent on tablet orientation or GI transit variability, because hundreds of individual units are simultaneously active throughout the GI tract. Second, the risk of catastrophic dose dumping is low, because failure of the coat on a subset of pellets does not release the entire dose. Third, the system is relatively insensitive to food-induced changes in gastric emptying, because the small pellets empty from the stomach at a rate more similar to liquids than to solid tablets.
All three of those advantages create equivalence hurdles that the generic developer must address, either by matching them with an alternative technology or by demonstrating through clinical data that their different mechanism does not produce clinically meaningful differences in the fed-state PK profile.
3.3 The BCS Classification and What It Means for ER Strategy
Metoprolol succinate is BCS Class I: high solubility, high permeability. The BCS classification is most commonly invoked in the context of biowaiver opportunities for immediate-release products. For extended-release formulations, the BCS classification has a different strategic implication. High solubility means the API will dissolve rapidly in almost any aqueous environment the GI tract provides. The rate-limiting step for ER performance is therefore the drug release mechanism itself, not dissolution of the dissolved drug particle. This shifts all formulation focus onto the delivery system.
For BCS Class I ER products, the dissolution test is a direct surrogate for in vivo release, because once the drug is released from the dosage form, absorption is essentially complete. This makes IVIVC establishment more tractable for Class I products than for Class II or IV drugs, and the FDA has historically accepted Level A IVIVC as a basis for post-approval change management for products in this category.
4. Pre-Formulation Science: The Analytical Foundation
4.1 API Characterization: Beyond USP Compliance
Meeting the United States Pharmacopeia monograph for metoprolol succinate is the floor, not the ceiling, of API characterization for a complex ER development program. The USP monograph establishes identity, assay, and impurity limits. It says nothing about particle size distribution, polymorphic form, hygroscopicity index, true density, bulk and tapped density, or the thermal behavior of the API under processing conditions. Each of those properties will affect either the manufacturing process, the dissolution profile, or both.
Particle size distribution (PSD) for metoprolol succinate in an ER matrix is less critical for dissolution rate than for a poorly soluble API, but it is still consequential for blend uniformity and granulation behavior. A bimodal PSD with a significant fines fraction will behave differently in a high-shear granulator than a narrow monomodal distribution centered at the same D50. The formulator needs to know what PSD the API supplier consistently delivers, set it as a controlled critical material attribute, and verify supplier capability across multiple commercial lots, not just development batches.
Hygroscopicity matters because water uptake during storage or processing can alter the API’s physical form, affect granulation dynamics, and cause tablet hardness to drift over time as the matrix partially hydrates. Differential scanning calorimetry (DSC) and thermogravimetric analysis (TGA) together define the thermal fingerprint of the API, identify any hydrate or solvate transitions, and confirm that the chosen processing temperatures will not inadvertently convert the API to an undesired physical form.
4.2 Polymorphism: The Variable That Has Crashed Commercial Programs
Polymorphism is the crystallographic phenomenon in which a single compound can adopt multiple solid-state structures with distinct thermodynamic stability, solubility, and dissolution rates. For metoprolol succinate specifically, the literature identifies at least two crystalline forms, with Form I being the thermodynamically stable polymorph under ambient conditions and the form used in commercial products.
The risk in generic development is not always that the wrong polymorph is selected knowingly. More commonly, manufacturing process parameters, particularly solvent selection, temperature during crystallization, and drying conditions, inadvertently produce a metastable polymorph or a mixture of forms. If that metastable form has higher solubility than the stable form, the dissolution rate will be faster than expected and the product may fail BE by exceeding the Cmax upper boundary. If the metastable form converts to the more stable, less soluble form on storage, the dissolution profile will slow over time and the product will fail its shelf-life dissolution specification.
The canonical industry example of a polymorph failure is ritonavir. Abbott’s antiviral Norvir was formulated as a capsule using a metastable polymorph. Years after commercial launch, the more stable Form II polymorph spontaneously nucleated in manufacturing environments globally, rendering the existing formulation unable to dissolve sufficiently. The resulting recall and full reformulation cost hundreds of millions of dollars and temporarily removed the product from the market. A generic developer entering ritonavir today would need to demonstrate polymorphic control across the entire manufacturing and storage lifecycle, not just at batch release.
For Metoprolol Succinate ER, the generic formulator must: screen all accessible polymorphic and solvate forms using XRPD, DSC, and Raman spectroscopy; confirm that the API used in pivotal bioequivalence batches is the same polymorphic form as in commercial production batches; and validate that granulation, drying, and compression steps do not induce form conversion.
4.3 Solubility Profiling Across pH
Because the tablet travels from the acidic stomach environment (pH approximately 1.2) to the near-neutral duodenum (pH approximately 6.0) to the more alkaline distal intestine (pH approximately 7.4), solubility must be profiled across the full physiological pH range. For a BCS Class I drug like metoprolol succinate, solubility is more than adequate throughout this range. The exercise confirms what is expected but also establishes baseline data for dissolution method development and IVIVC modeling.
The solubility data feeds directly into selection of dissolution media for the discriminating dissolution test. A dissolution method is only useful to a generic developer if it can distinguish between a bioequivalent formulation and one that would fail in vivo. Selecting media that all give complete release within 30 minutes for a 24-hour ER product provides no discriminating power. The formulator needs media conditions where the drug release is rate-limited by the delivery system, not by solubility. For Metoprolol Succinate ER, this typically means running multi-point dissolution profiles at pH 1.2, 4.5, and 6.8 with timed sampling out to 24 hours.
5. Reverse Engineering the RLD: Deformulation Strategy and Tools
5.1 The Analytical Battery for Deformulation
Deformulation of Toprol-XL is not a single experiment. It is a systematic analytical program whose goal is a semi-quantitative compositional model of the innovator product, a structural understanding of its drug delivery architecture, and a target dissolution fingerprint that the generic formulation must replicate.
The analytical sequence typically begins with physical examination of the tablet under optical microscopy and SEM. For Toprol-XL, SEM cross-sections reveal the pellet-in-tablet architecture: individual coated spheroids visible within the compressed tablet matrix. This structural observation immediately confirms that the drug delivery mechanism is multi-particulate and directs the deformulation team toward characterizing individual pellet coatings rather than a continuous matrix polymer.
HPLC with UV and mass spectrometric detection quantifies the API and identifies any co-formulated materials. FTIR and Raman spectroscopy provide functional group fingerprints that identify specific polymers by comparing spectra against reference libraries of pharmaceutical excipients. XRPD confirms the physical form of the API and, if crystalline excipients are present, can identify them as well.
Thermogravimetry and DSC characterize the water content of the product and the thermal transitions of any polymers, which helps identify the grade of materials like HPMC or ethylcellulose by comparing measured onset temperatures against known grade-specific values.
The dissolution profile of the RLD, measured across multiple pH conditions and multiple lot numbers of the commercial product, establishes the quantitative bioequivalence target. Analyzing multiple commercial lots is important because the generic developer needs to characterize natural batch-to-batch variability in the RLD. If Toprol-XL lots show a dissolution range of, say, 20% drug released at 2 hours versus 27% drug released at 2 hours across commercial lots, the generic developer knows that their product needs to consistently fall within that natural variability window, not just hit a single point.
5.2 Identifying Excipient Identity and Function
Through the combined analytical program, the deformulation team will identify the key excipients in Toprol-XL: the rate-controlling polymer on the pellet coat (most likely ethylcellulose or a blend of ethylcellulose and hydroxypropyl cellulose), the pellet substrate (likely microcrystalline cellulose or sugar spheres), plasticizers in the coating film (such as dibutyl sebacate or triethyl citrate), and tablet matrix excipients including fillers, binders, disintegrants, and lubricants.
Identifying the grade of polymer is more difficult than identifying its type. Ethylcellulose is available in multiple viscosity grades (N7, N10, N14, N22, N45, N100), and the dissolution rate of a coated pellet is highly sensitive to the film-forming properties of the specific grade used. The team can narrow the grade range by comparing the coating film’s dissolution behavior and mechanical properties against reference standards, but some ambiguity typically remains.
That ambiguity is actually strategically acceptable, because the generic company is not trying to copy the innovator’s process. They are trying to match its output. They are free to use a different polymer system entirely, provided their formulation passes bioequivalence. The deformulation data informs their starting formulation design, particularly the target dissolution profile, not a replication blueprint.
5.3 Building the Deformulation Report as a Regulatory Document
The deformulation report is not just a scientific record. It becomes part of the ANDA CMC section as evidence supporting the generic developer’s formulation rationale. FDA reviewers expect to see a credible scientific basis for the choice of formulation approach. A formulation that uses a completely different delivery mechanism from the RLD, with no documentation of why that mechanism was selected or how it was validated as bioequivalent, invites a deficiency letter.
The deformulation report should document: the analytical methods used to characterize the RLD, the identified components and their approximate quantification, the target dissolution profile derived from multi-lot RLD testing, and the scientific rationale for the proposed generic delivery mechanism. When the generic developer writes the pharmaceutical development section of the ANDA, that rationale becomes the narrative backbone of the submission.
6. The Extended-Release Problem: Polymer Physics, IVIVC, and Dose Dumping
6.1 Why High Solubility Makes ER Formulation Harder
Conventional wisdom in formulation science holds that BCS Class II drugs (low solubility, high permeability) are the hardest to develop because getting them into solution is the rate-limiting step for absorption. For ER formulations, the opposite problem is more challenging: BCS Class I drugs need their release actively throttled by the delivery system, because if the system fails, the full dose reaches systemic circulation immediately.
The thermodynamic driver for dissolution is concentration gradient. Metoprolol succinate dissolves so readily that even a small breach in a rate-controlling film coat creates a steep concentration gradient that pulls drug out rapidly. The formulator’s job is to design a delivery system where that gradient is managed deliberately and consistently across a 24-hour period, across varying GI environments, and across patients with different fed-state gastric pH, transit times, and GI motility.
6.2 Hydrophilic Matrix Technology: Mechanism, Polymer Selection, and Failure Modes
The hydrophilic matrix tablet is the most widely adopted alternative to the multi-particulate architecture for BCS Class I ER products. Its operating principle relies on the surface hydration of swellable polymers, primarily hydroxypropyl methylcellulose, to form a viscous gel layer that controls drug diffusion to the tablet surface.
When the tablet contacts aqueous fluid, HPMC chains on the tablet surface hydrate and swell. This creates a gel layer of increasing viscosity. Drug dissolved at the gel-tablet interface must diffuse through this tortuous hydrated network to reach the dissolution medium. The flux is described by Fick’s first law: J = -D(dC/dx), where D is the diffusion coefficient of the drug in the gel and dC/dx is the concentration gradient. As the outer gel erodes and new HPMC is exposed to hydration, the system maintains an approximately constant diffusion path length and constant flux, producing the desired zero-order or near-zero-order release kinetics.
HPMC grade selection is the primary lever for controlling release rate. The relevant grades for ER matrices are HPMC K-series (hydroxypropyl substitution dominant), available in viscosity grades from approximately 100 mPas to over 100,000 mPas in 2% aqueous solution at 20 degrees Celsius. Higher viscosity grades produce stronger, more erosion-resistant gels and slower drug release. The polymer concentration in the tablet matrix is the secondary lever. Typical ER matrices use HPMC concentrations between 20% and 40% by weight, with higher concentrations required for stronger drug retention.
A single HPMC grade often cannot produce the precise biphasic dissolution profile that matches the RLD. Formulators frequently blend two grades, for example K100M (very high viscosity) and K15M (medium viscosity), to achieve an initial lag phase followed by near-linear release over the 24-hour window. The ratio of the two grades and their combined concentration defines the formulation’s ‘knobs’, the variables that the DoE strategy will optimize against the target dissolution profile.
The failure modes for hydrophilic matrix systems are dose dumping in the fed state, incomplete release in 24 hours (drug retention in the matrix remnant), and dissolution profile sensitivity to tablet hardness. Fed-state dose dumping occurs when high-fat meal-induced changes in gastric pH and viscosity disrupt the HPMC gel layer before adequate drug has been released. Because Toprol-XL’s multi-particulate system is relatively insensitive to fed-state conditions, the generic hydrophilic matrix product must demonstrate fed-state bioequivalence through actual clinical study, not inference from fasting data alone.
Incomplete release is a risk when the HPMC concentration is too high or the grade too viscous. The matrix remnant, a swollen, partially eroded tablet ghost, can pass through the GI tract still containing 10% to 20% of the labeled dose. This reduces AUC in vivo relative to the RLD, a bioequivalence failure on the extent dimension. Formulating at a lower HPMC concentration resolves the retention problem but risks sacrificing the rate control needed to prevent dose dumping. This trade-off is the central optimization problem of BCS Class I ER matrix formulation.
6.3 IVIVC Development: The Level A Model and Its Regulatory Utility
An In Vitro-In Vivo Correlation at Level A is a point-to-point relationship between the in vitro dissolution fraction dissolved at time t and the in vivo fraction absorbed at the same time point. A validated Level A IVIVC has direct regulatory utility: FDA guidance allows companies with an established Level A IVIVC to use dissolution testing as a surrogate for in vivo BE studies when making certain post-approval manufacturing changes, avoiding the cost and delay of conducting new human PK studies.
For Metoprolol Succinate ER, establishing a Level A IVIVC requires at minimum three formulations with meaningfully different dissolution profiles (a slow, a medium, and a fast formulator) plus in vivo PK data for each formulation in the same study. The deconvolution method converts the observed plasma concentration-time profile from each formulation into a fraction-absorbed-versus-time curve, which is then correlated against the corresponding dissolution profile. If the mathematical relationship is consistent across all three formulations, the IVIVC is considered established.
The internal predictability of the IVIVC is validated by confirming that the in vivo PK profile predicted from the dissolution data of each formulation matches the actual observed PK profile within 10% for Cmax and 10% for AUC, the standard FDA acceptance criteria. External predictability is then confirmed by demonstrating that the correlation successfully predicts the in vivo performance of one or two additional formulations not used to build the model.
A validated Level A IVIVC is a competitive asset. It accelerates post-approval change management, reduces the cost of lifecycle management activities, and provides a more defensible basis for the dissolution specification in the ANDA. Companies that invest in IVIVC development early gain regulatory flexibility that competitors without the correlation cannot access.
7. Excipient Control: Why ‘Inactive’ Ingredients Collapse Submissions
7.1 Excipient Variability Is a Supply Chain Problem, Not Just a Chemistry Problem
The pharmaceutical industry describes excipients as ‘inactive’ ingredients for labeling and regulatory classification purposes. The classification is a legal convenience, not a scientific description. Every excipient in a formulation has a functional role, and every functional role depends on physical and chemical properties that vary between suppliers, between manufacturing sites within a single supplier, and between production lots at the same site.
Microcrystalline cellulose is illustrative. It is produced by acid hydrolysis of cellulose to its level-off degree of polymerization, typically in the range of 220 to 270. The resulting material is available in multiple grades (PH-101, PH-102, PH-200, PH-301, PH-302) that differ in particle size, bulk density, and moisture content. MCC PH-101 has a mean particle size of approximately 50 microns. MCC PH-102 has a mean particle size of approximately 100 microns. These two grades will behave differently in a wet granulation process. PH-102’s coarser particles produce a different granule structure, different compressibility, and different tablet hardness at the same compression force.
For a hydrophilic matrix tablet where tablet hardness is a critical quality attribute that directly controls dissolution rate, substituting one MCC grade for another without revalidation of the compression parameters can shift the dissolution profile outside the acceptance criteria. The change appears minor on paper, a different particle size grade of the same compendial material. In practice, it can trigger a dissolution failure in the first commercial batch.
The control strategy for excipients in a complex ER product must therefore specify not just identity and purity per compendial standards, but also the material attributes that drive formulation performance. For MCC, those attributes are particle size (D10, D50, D90), moisture content, bulk density, and tapped density. For HPMC, the critical attributes are viscosity (specified grade and in-house measured viscosity of each incoming lot), degree of substitution, and moisture content. These specifications go beyond what compendial monographs require and must be established by the formulator based on characterization data and risk assessment.
7.2 Excipient-API Compatibility: Systematic Screening Protocol
The Maillard reaction between primary amine functional groups in APIs and reducing sugars in excipients like lactose is the best-known example of excipient-API incompatibility. Metoprolol succinate contains a secondary amine group that is potentially reactive, though the risk with lactose is lower for succinate salt than for some other amine-containing APIs. The formulator cannot assume safety based on precedent. Every potential excipient requires systematic compatibility screening.
The standard protocol mixes the API with each excipient at 1:1 and 1:5 ratios (API:excipient and excipient:API) in open and closed containers, stored at 40 degrees Celsius and 75% relative humidity (accelerated condition), and at 25 degrees Celsius and 60% relative humidity (long-term condition). Samples are pulled at 1-week, 2-week, 1-month, and 3-month time points and analyzed by HPLC for API purity. Visual examination for color change, physical state change, or gas evolution accompanies the analytical testing.
Any excipient that produces greater than 0.5% total impurity increase relative to the API control at the accelerated condition at any time point is flagged as potentially incompatible and either rejected from the formulation or advanced only with additional mechanistic investigation. The compatibility data is included in the ANDA pharmaceutical development section as evidence that excipient selection was science-based.
Peroxide content in excipients is a separate but related concern. Polyvinylpyrrolidone (povidone), polysorbates, and some grades of polyethylene glycol contain trace levels of hydrogen peroxide and organic peroxides from their manufacturing processes. These oxidants can degrade APIs with oxidation-sensitive functional groups, including thioethers, thiols, and tertiary amines. For metoprolol specifically, oxidative degradation of the isopropylamine side chain can occur under peroxide stress. Any formulation including these excipients should specify a maximum peroxide content limit in the excipient specification and require suppliers to test and certify each lot.
7.3 The Cost of Excipient Failures: ANDA Deficiency Letter Statistics
FDA has published data on ANDA deficiency rates across CMC categories. Chemistry and manufacturing deficiencies are consistently the leading cause of Complete Response Letters for generic applications, accounting for a substantial fraction of first-cycle non-approvals. Within CMC deficiencies, excipient-related issues, including inadequate specifications, undisclosed variability, and missing compatibility data, appear in a material fraction of CRLs for complex dosage forms.
The commercial cost is concrete. A CRL that requires three months of additional stability data before resubmission delays commercial launch by at minimum six months after factoring in data generation, internal review, and FDA review of the resubmission. For a product with a $200 million first-year revenue opportunity and 180-day exclusivity, a six-month delay to exclusivity launch effectively eliminates the exclusivity value. The market will have already been seeded by other generic entrants who either filed later but received first-cycle approval, or who aggressively negotiated authorized generic agreements.
8. Quality by Design: From QTPP to Design Space
8.1 The QbD Framework: What It Actually Requires
Quality by Design for generic drug products is described in ICH Q8(R2), Q9, and Q10. The FDA’s 2011 guidance on scale-up and post-approval changes for controlled-release solid oral dosage forms incorporates QbD principles as the framework for justifying manufacturing flexibility. The core of QbD is establishing the linkage between input variables (material attributes and process parameters) and output quality attributes (the CQAs of the drug product).
The implementation sequence is well established in the literature but still inconsistently applied in practice. The QTPP defines the desired profile of the finished product: dosage form, strength, route of administration, pharmacokinetic target (bioequivalent to the RLD), release profile, stability, and container-closure system. The CQAs are then identified as the attributes of the drug product that must be within defined limits to achieve the QTPP. For Metoprolol Succinate ER tablets, the CQAs are assay (98.0% to 102.0% of label claim), content uniformity (AV not more than 15 per ICH Q6A), the dissolution profile at specified time points across pH conditions, total impurities (not more than 0.5% by HPLC), tablet hardness (14 kP to 20 kP, for example), and friability (not more than 1.0%).
The CMAs and CPPs are identified through risk assessment, typically using an Ishikawa (fishbone) diagram or a failure mode effects analysis (FMEA) to systematically map the potential impact of every input variable on every CQA. Variables assessed as having high impact or high uncertainty are designated critical and become the subjects of controlled experimentation. Low-risk variables are controlled by specification without further study.
8.2 Design of Experiments: Efficient Mapping of the Formulation Space
DoE replaces the one-factor-at-a-time (OFAT) experimental approach that dominated pharmaceutical development for decades. OFAT is inefficient because it cannot detect interaction effects between variables, and it systematically underestimates the true complexity of the formulation space. A formulation where HPMC concentration and tablet hardness interact to affect dissolution cannot be optimized by varying each parameter independently.
For the Metoprolol Succinate ER hydrophilic matrix, a three-factor, two-level full factorial design studying HPMC K100M concentration (25% vs. 35% w/w), HPMC K15M concentration (5% vs. 10% w/w), and compression force (8 kN vs. 12 kN) requires eight experimental runs and generates data that captures all main effects and all two-way interaction effects. Adding center points (two or three replicates at mid-range values for all factors) enables estimation of curvature and confirms whether the linear model is adequate or whether a more complex response surface design is needed.
The response surface methodology produces contour plots and three-dimensional surface maps showing how the key CQA (dissolution at 2h, 8h, and 24h) responds to the studied factors. The region of factor space that consistently meets all CQA specifications defines the Design Space. Within the Design Space, the formulator can demonstrate that manufacturing variability, within the Design Space boundaries, does not produce out-of-specification product. This is the regulatory basis for proposing enhanced manufacturing flexibility in the ANDA: changes within the Design Space can be made without prior regulatory approval, because the Design Space itself was approved.
8.3 PAT Integration with DoE: Real-Time Data as the Control Strategy
Process Analytical Technology closes the loop between the DoE-derived Design Space and commercial manufacturing execution. Near-infrared spectroscopy probes positioned in the blender can monitor blend uniformity in real time and generate a stop-criterion (when the blend endpoint is reached) rather than a fixed mixing time. This replaces a static time-based control with a quality-based control, accommodating natural batch-to-batch variability in the incoming material properties.
Moisture content sensors in the fluid bed dryer replace fixed drying time with a moisture endpoint, ensuring that every batch is dried to the same water activity regardless of incoming moisture content of the granulation or ambient humidity in the production facility. Inline tablet hardness measurement on the compression press enables real-time closed-loop adjustment of compression force to maintain tablet hardness within the target range as the granule properties naturally drift during the press run.
The integration of PAT into the control strategy is documented in the ANDA as part of the process description and control strategy sections. FDA reviewers have increasingly expected PAT systems for complex dosage forms, and the absence of real-time controls for a product whose CQAs are sensitive to process parameter variability can generate a deficiency question.
9. Scale-Up and Manufacturing: Where Lab Success Goes to Die
9.1 The Physics of Scale: Why 500x Is Not 500x
The failure mode of scale-up is dimensional. At laboratory scale, a 1 kg blender processes material in a vessel where the ratio of particle size to vessel diameter allows efficient convective mixing. At production scale, a 500 kg bin blender operates in a geometric regime where convective mixing is less efficient and the risk of segregation by particle density or size is substantially higher. Powder flow patterns do not scale linearly with vessel volume.
The engineering principle used to guide scale-up of mixing processes is the Froude number, Fr = (N squared times D) / g, where N is the impeller speed in rotations per second, D is the impeller diameter, and g is gravitational acceleration. Maintaining a constant Froude number across scales preserves the hydrodynamic similarity of the mixing process, ensuring that the relative magnitudes of centrifugal force and gravity acting on particles remain constant. This guides the selection of impeller speed at production scale from lab-scale parameters.
For wet granulation in a high-shear mixer, the relevant scale-up parameter is tip speed (the velocity of the impeller blade tip), which drives granule growth kinetics. Constant tip speed translates to lower impeller rotational speed at production scale (because the impeller diameter is larger), but the same linear velocity at the granule-impeller contact point. Temperature rise in the granulation mass scales differently from tip speed, however, because the ratio of mixer volume to heat-dissipating surface area increases with scale. Production-scale batches frequently run hotter than lab-scale batches at nominally equivalent tip speeds, which can accelerate granule drying during the wet phase and produce harder, denser granules than expected.
9.2 Technology Transfer Package: What Must Be Documented
The technology transfer package is the formal knowledge object that moves a product from R&D control to manufacturing control. Its adequacy determines whether scale-up succeeds in three consecutive validation batches or requires multiple development cycles at production scale, each adding six months to the project timeline.
A complete technology transfer package for a complex ER solid oral product includes the master batch record with all processing steps, equipment specifications, in-process controls, and acceptance criteria; a complete set of validated analytical methods with system suitability requirements and reference standard management protocols; the development report documenting the QbD work, including the QTPP, CQAs, risk assessment, DoE studies, and the established Design Space; the CPP and CMA specifications with statistical justification; the stability data from development and registration batches; the equipment qualification status of all production equipment to be used; and the cleaning validation rationale for the API and product residue limits.
The manufacturing team needs to be involved in the technology transfer process at least 12 months before the planned validation campaign, not when the development report arrives. This gives manufacturing engineers time to assess whether the proposed process is executable on their installed equipment base, to raise concerns about specific steps that may require equipment modification, and to train operators on the unique requirements of the new process before the high-stakes validation batches begin.
9.3 Validation Batches: What the Data Must Demonstrate
The three validation batches, also called pivotal batches or registration batches, must be manufactured at commercial scale, in the commercial facility, using commercial equipment, with commercial-grade raw materials, operated by commercial production personnel under commercial cGMP conditions. Any deviation from these requirements compromises the regulatory value of the batches.
The validation protocol must pre-specify the CQAs to be tested, the sampling plan (how many tablets from how many locations in the batch), the acceptance criteria for each attribute, and the statistical basis for those criteria. Process hold time studies, conducted during or alongside the validation campaign, establish the maximum allowable hold times for granulation wet mass before drying, dry granules before compression, and compressed tablets before coating, without adverse impact on CQA performance.
Accelerated stability data from the validation batches (3 months at 40 degrees Celsius and 75% relative humidity) is required for ANDA submission. Long-term stability data from 12 months at 25 degrees Celsius and 60% relative humidity is typically available at the time of submission for applications filed 12 or more months after validation batch manufacture. The ANDA committing to the 24-month shelf life requires extrapolation of the 12-month data per ICH Q1E, which FDA reviewers scrutinize closely for ER products where dissolution drift on stability is a known risk.
10. ANDA CMC Strategy: Building a Submission That Survives Review
10.1 The Pharmaceutical Development Section: Making the Scientific Case
The pharmaceutical development section (formerly called Section 3.2.P.2 in CTD format) is where ANDA applicants explain, in narrative form, why they made the formulation and process decisions they made. It is not a compendium of tables. It is a scientific argument, and its persuasiveness matters.
A weak pharmaceutical development section states facts without interpretation: ‘HPMC K100M was used as the extended-release polymer at a concentration of 30% w/w.’ A strong pharmaceutical development section contextualizes the decision: ‘HPMC K100M was selected as the primary release-controlling polymer following screening of six HPMC grades at concentrations of 20%, 25%, and 30% w/w. The screening data, shown in Figure 3.2.P.2-4, demonstrated that K100M at 30% produced the dissolution profile most closely matching the multi-point RLD target at pH 1.2, 4.5, and 6.8. Lower viscosity grades at equivalent concentrations produced faster release at pH 6.8, inconsistent with the RLD profile, and were excluded.’
The FDA reviewer reading that section can reconstruct the development logic, evaluate its soundness, and make an approval decision with confidence. The reviewer reading the weak version has to guess whether the choice was scientifically justified or arbitrary, which is grounds for a deficiency question.
10.2 GDUFA Performance Goals and First-Cycle Approval Strategy
GDUFA III, the current reauthorization cycle covering fiscal years 2023 to 2027, commits the FDA to reviewing 90% of standard ANDAs within 10 months of receipt. The priority review goal for products with public health importance is 6 months. These commitments have materially improved approval predictability since GDUFA I’s implementation in fiscal year 2013, when a backlog of over 4,000 applications had accumulated.
First-cycle approval, meaning approval without any interim deficiency letters or complete response, is the highest-value outcome in ANDA strategy. A company that achieves first-cycle approval in 10 months launches 10 to 18 months before a company that receives a CRL and requires two complete review cycles. For a product with 180-day FTF exclusivity, that timing difference often determines whether the exclusivity is captured at all.
The structural drivers of first-cycle failure are identifiable and largely controllable. Manufacturing facility inspection findings (Warning Letters, import alerts) are the hardest to control because they depend on facility-wide cGMP compliance, not just the specific product’s CMC quality. CMC deficiencies related to dissolution specification justification, stability data gaps, and excipient specification inadequacy are addressable through rigorous internal review before submission. Having the pharmaceutical development section reviewed by a consultant with FDA review experience before submission is a cost-effective intervention for any application with a significant market opportunity.
10.3 Paragraph IV Certifications: The 180-Day Exclusivity Race
A Paragraph IV certification declares that a listed patent in the Orange Book is either invalid, unenforceable, or will not be infringed by the proposed generic product. Filing such a certification triggers a 45-day window in which the patent holder can initiate infringement litigation. If litigation is initiated within that window, a 30-month stay of approval automatically applies.
The business logic of a Paragraph IV filing depends on three variables: the strength of the invalidity or non-infringement argument, the size of the market opportunity during the 180-day exclusivity period, and the cost and risk tolerance of sustained patent litigation. Companies that file Paragraph IV certifications without credible non-infringement arguments, hoping to settle for a reverse-payment agreement, operate in a legally constrained environment following FTC v. Actavis (2013), which held that reverse-payment patent settlements can violate antitrust law.
The formulation strategy and the legal strategy are inseparable in a Paragraph IV program. A credible non-infringement argument requires a formulation that genuinely avoids the patent claims, not a formulation that marginally distinguishes from the claims but would likely be found to infringe under doctrine of equivalents analysis. Legal counsel must review the technical formulation design at multiple stages of development to confirm that the patent avoidance argument remains valid as the formulation evolves from concept to ANDA.
11. Bioequivalence Study Design: Fasting, Fed, and Statistical Traps
11.1 The Two-Period Crossover Design and Its Statistical Requirements
The standard bioequivalence study design for a single-dose, oral, solid dosage form is a two-treatment, two-period, two-sequence (2x2x2) crossover in healthy adult volunteers. Each subject receives the Test product (the generic) and the Reference product (the RLD) in separate periods, separated by a washout period adequate to ensure complete drug elimination from the prior period. For metoprolol succinate with a half-life of approximately 3 to 7 hours, a washout of 5 to 7 days is standard.
The primary PK parameters are AUC0-inf (total drug exposure extrapolated to infinity) and Cmax (peak concentration). The statistical criterion for bioequivalence is that the 90% confidence interval for the geometric mean ratio (GMR) of Test to Reference for both parameters must fall entirely within 80.00% to 125.00%. This criterion derives from a two one-sided tests (TOST) procedure and is not equivalent to saying that the point estimate must be near 100%. A study with a point estimate GMR of 95% but a wide confidence interval (for example, 78% to 120%) fails, because the lower boundary falls below 80%.
Sample size calculation for the BE study requires an estimate of the intrasubject coefficient of variation (CV) for Cmax and AUC in the study population, and a target power of at least 80%. For metoprolol, published BE study data suggests intrasubject CVs for Cmax in the range of 20% to 30%, which is relatively high for an oral product and requires sample sizes of 36 to 60 subjects to achieve 80% power at a GMR assumption of 0.95.
11.2 Fed-State BE: The Most Common Failure Point for ER Products
FDA’s guidance on food effect studies for extended-release products requires that the fed-state study use a high-fat, high-calorie standardized meal (approximately 800 to 1000 kilocalories, 50% from fat) consumed 30 minutes before dosing. The rationale is that a high-fat meal produces the largest and most consistent effect on GI physiology, providing the most discriminating test condition for food effect.
For Toprol-XL and its generic versions, the fed-state condition is particularly challenging for hydrophilic matrix formulations because: the high-fat meal delays gastric emptying, extending the time the tablet resides in the acidic stomach environment; increased gastric fluid volume from the meal promotes faster surface hydration of the HPMC matrix; and the presence of dietary fats may interact with the polymer gel layer in ways that alter its diffusion barrier properties.
The clinical consequence can be a food effect manifesting as either faster release (fed-state dose dumping) or, less commonly, slower release leading to reduced fed-state AUC. Either direction represents a bioequivalence failure relative to the RLD, which by virtue of its multi-particulate architecture is more robust to fed-state variability.
Companies that perform a fasting study first and find bioequivalence should not delay the fed-state study. A fasting BE pass followed by fed BE failure is a common and costly outcome. The formulation strategy must specifically address fed-state performance from the first DoE work. Accelerated in vitro screening using dissolution testing in simulated fed-state media (FeSSIF, Fed State Simulated Intestinal Fluid) can identify formulations at elevated risk of fed-state failure before committing to an in vivo study.
11.3 Highly Variable Drugs and the Scaled Average BE Approach
Metoprolol is classified as a highly variable drug (HVD), meaning intrasubject variability in Cmax exceeds 30% in replicate-design studies. FDA guidance permits a scaled average bioequivalence (SABE) approach for HVD products, where the 80/125 acceptance limits are widened proportionally to the within-subject variability of the reference product.
SABE studies require a replicate design, typically a four-period, two-sequence (RTRT/TRTR) design where each subject receives the Reference in two periods and the Test in two periods. The within-subject standard deviation of the Reference (sWR) is estimated from the replicate Reference periods and used to scale the acceptance limits. For metoprolol products where sWR exceeds the threshold of 0.294, the Cmax acceptance limits can expand beyond the standard 80/125 window, up to a regulatory cap.
The SABE approach reduces the required sample size for products with high within-subject variability, because the wider acceptance limits are easier to achieve. However, the replicate design adds protocol complexity and study cost (four periods versus two), and the statistical analysis is more involved. The decision to use SABE versus standard average BE must be made at the study design stage, because the study design determines which statistical approach applies.
12. Complex Generics: Long-Acting Injectables, Topicals, and Inhalers
12.1 The FDA Complex Drug Products Framework
FDA’s Complex Drug Products program, established under GDUFA II and expanded under GDUFA III, recognizes that a subset of generic products require novel bioequivalence approaches, device-specific performance standards, or enhanced analytical characterization beyond what the standard ANDA framework addresses.
The complex drug products category includes: drug-device combination products (metered-dose inhalers, dry powder inhalers, nasal sprays, auto-injectors); products with complex drug substances (proteins, polysaccharides, oligonucleotides); products with complex formulations (liposomes, emulsions, microspheres); and products with complex routes of delivery (ophthalmic, local transdermal, topical dermatological). For each category, FDA has published or is developing product-specific guidance documents that describe the recommended BE approach.
12.2 Long-Acting Injectables: Formulation-Dependent PK and In Vitro Release Testing
Long-acting injectable (LAI) products based on biodegradable microsphere technology, such as risperidone microspheres (Risperdal Consta) or paliperidone palmitate (Invega Sustenna), present a BE challenge that standard plasma-level studies cannot fully address. The release rate of drug from the microsphere depot is controlled by polymer degradation kinetics (for PLGA-based systems), particle size distribution of the microspheres, drug loading, and the physical form of the drug within the polymer matrix.
Demonstrating BE through a plasma-level study alone is problematic because: in vivo PK from a LAI product integrates the effects of injection site distribution, lymphatic transport, microsphere degradation, and drug permeation through tissue, making the plasma profile a poor surrogate for formulation equivalence; standard 90% CI criteria based on two-period crossover designs are not applicable to LAI products where the drug releases over weeks to months; and the large sample sizes and long washout periods required for comparative clinical PK studies are not practically feasible.
FDA’s approach for LAI microsphere generics requires demonstration of sameness across multiple dimensions: an identical polymer composition and molecular weight distribution, equivalent microsphere particle size distribution and surface morphology by SEM, equivalent drug loading and encapsulation efficiency, equivalent in vitro release profiles in the FDA-specified dissolution test method, and equivalent residual solvent content. When all these attributes are matched, an abbreviated clinical pharmacology study (comparing steady-state PK after multiple administrations) supplements the formulation characterization data rather than replacing it.
The IP architecture around LAI products tends to be particularly dense. Alkermes’s PLGA microsphere technology has been the basis for multiple products and multiple patent estates. Generic developers targeting LAI products must navigate composition-of-matter patents on the polymer, formulation patents on the specific PLGA grade and drug loading range, manufacturing process patents on the microencapsulation technique (typically emulsion-solvent evaporation or spray drying), and in some cases device patents on the reconstitution and delivery system.
12.3 Topical Dermatological Products: Q1/Q2/Q3 Sameness and IVPT
For topical semisolid products (creams, ointments, gels, lotions), bioequivalence cannot be measured by plasma levels because the drugs are designed to act locally at the skin surface and, for most indications, minimal systemic absorption is desired. FDA has established a qualitative (Q1) and quantitative (Q2) sameness approach, supplemented by physical characterization and in vitro permeation testing (IVPT).
Q1 sameness means the generic contains the same inactive ingredients as the RLD. Q2 sameness means the inactive ingredients are present in substantially the same concentrations, within a 5% proportional variation. For creams and emulsions, the physical microstructure (Q3 sameness) must also be demonstrated, because the thermodynamic activity of the drug in the vehicle, which drives skin permeation, depends on the microstructure of the emulsion and not just its composition.
IVPT using human skin mounted in diffusion cells (typically Franz diffusion cells) measures the flux of drug from the test formulation versus the RLD through excised skin tissue. FDA’s draft guidance on topical BE has defined acceptance criteria based on the cumulative amount permeated per unit area at specified time points, with a 90% CI for the Test/Reference geometric mean ratio falling within 80/125, analogous to systemic BE criteria.
The skin itself is a biological variable. Human skin from different donors shows substantial variability in permeation rates, driven by differences in stratum corneum thickness, lipid composition, and integrity. IVPT studies must use skin from multiple donors, balanced across test and reference groups, and the statistical model must account for the skin-as-blocking-factor. IVPT study designs that ignore donor variability are routinely rejected by FDA reviewers.
13. Biosimilars: The Formulation Challenge at the Molecular Level
13.1 Why Biosimilars Are Not Generic Biologics
The statutory framework for biosimilar approval in the United States is the Biologics Price Competition and Innovation Act of 2009, which established the 351(k) pathway. The standard is not bioequivalence but biosimilarity: ‘highly similar to the reference product notwithstanding minor differences in clinically inactive components, and no clinically meaningful differences in the safety, purity, and potency of the product.’
The reason the standard is different is physical chemistry. A monoclonal antibody like adalimumab (Humira) has a molecular weight of approximately 148,000 daltons, compared to approximately 300 daltons for metoprolol succinate. The primary structure of an antibody is a specific amino acid sequence, but its biologic activity depends on higher-order structure, post-translational modifications (particularly glycosylation), and the three-dimensional folding of the protein. All of these are determined by the cell line and the bioprocessing conditions used to manufacture the protein. Because biological manufacturing systems are inherently variable, it is impossible to manufacture an exact molecular copy of a reference biologic. The biosimilar manufacturer produces a product that is highly similar but not identical.
The totality-of-evidence approach required for biosimilar approval includes analytical characterization (structural, functional, and purity), non-clinical studies (in vitro receptor binding, in vivo pharmacology if needed), and clinical studies (PK/PD similarity and, for most products, at least one adequately powered comparative efficacy study). Formulation contributes to biosimilarity in a specific and critical way: the biosimilar drug product formulation must maintain the protein in its native, active conformation throughout its shelf life, must not introduce novel impurities or degradation products absent from the reference product, and must present the protein to the immune system in a way that does not alter its immunogenicity profile.
13.2 Formulation Challenges Specific to Protein Drug Products
Protein stability is the central formulation problem for any biologic product. Proteins are susceptible to multiple degradation pathways that have no analog in small-molecule formulation: aggregation (the association of individual protein molecules into dimers, oligomers, or insoluble particles); deamidation (chemical modification of asparagine residues that can alter biological activity); oxidation (particularly of methionine and tryptophan residues in the Fc region of antibodies); and fragmentation (hydrolytic cleavage of peptide bonds).
Aggregation is particularly problematic because protein aggregates can be immunogenic. Patients who develop antibodies against a biosimilar’s aggregate impurities can develop antibodies against the reference product as well, with clinical consequences ranging from loss of therapeutic response to anaphylaxis. The formulation must suppress aggregation throughout the product’s shelf life (typically 18 to 24 months) across the range of storage and handling conditions specified in the label.
The excipient toolkit for protein formulation differs entirely from small-molecule tablet formulation. Stabilizers such as sucrose, trehalose, and mannitol act as preferential exclusion agents, reducing thermodynamic activity for protein unfolding. Surfactants such as polysorbate 20 and polysorbate 80 reduce protein adsorption to surfaces (glass vials, rubber stoppers, plastic tubing) and protect against shear-induced aggregation. Buffering systems maintain pH in the range where the protein is most conformationally stable, typically pH 5 to 7 for most therapeutic antibodies.
For a biosimilar developer, the challenge is not just optimizing a stable formulation but demonstrating that the formulation does not introduce differences in protein structure, function, or immunogenicity relative to the reference product. The formulation comparison data, comparing biosimilar versus reference product physical stability profiles, must be included in the biosimilar BLA (Biologics License Application).
13.3 Biosimilar Interchangeability: The Regulatory and Commercial Stakes
Biosimilar interchangeability is a distinct regulatory designation under the BPCIA that permits pharmacist-level substitution of the biosimilar for the reference product without prescriber intervention, in states with automatic substitution laws. Achieving interchangeability designation requires demonstrating that switching between the reference product and the biosimilar does not produce greater immunogenicity or safety risk than continued use of the reference product.
The commercial value of interchangeability is substantial. In the U.S. market, the majority of prescriptions for drugs like adalimumab, etanercept, and insulin are dispensed through pharmacy benefit management plans that incentivize pharmacist substitution at the point of dispensing. A biosimilar without interchangeability designation is limited to prescriber-level uptake, a slower and more sales-force-intensive market penetration pathway. A biosimilar with interchangeability can access the pharmacy substitution channel, which has historically driven rapid volume uptake for small-molecule generics and is increasingly important for biologics as formulary management practices evolve.
The IP complexity of the biosimilar landscape exceeds even the complexity of complex small-molecule generics. AbbVie’s patent thicket around Humira comprised over 100 U.S. patents at its peak, covering the antibody sequence, formulation, device, and manufacturing process. Multiple biosimilar developers (Amgen, Sandoz, Pfizer, Samsung Bioepis, Mylan/Viatris) litigated or settled with AbbVie before achieving U.S. market entry. The settlement agreements, which permitted biosimilar entry on agreed dates rather than patent expiration dates, collectively delayed U.S. market entry by roughly six years relative to EU entry, at an estimated cost to the U.S. healthcare system measured in tens of billions of dollars.
14. AI and Machine Learning in Formulation Development
14.1 Where ML Is Generating Quantifiable Value Today
Artificial intelligence applications in pharmaceutical formulation have moved from proof-of-concept studies in academic literature to production deployment at several large generics and CDMOs in the past three years. The applications generating measurable value fall into three categories: predictive formulation design, process optimization, and regulatory intelligence.
Predictive formulation design uses supervised machine learning models trained on historical development databases to predict the dissolution profile, stability outcome, or processability of a candidate formulation before synthesis. The models require structured training data, specifically batches where the input variables (excipient types, grades, concentrations, and process parameters) and the output CQA results are both recorded in a queryable database format. Most generic pharmaceutical companies have this data in their laboratory information management systems (LIMS) but have not structured it for ML consumption. The data preparation step, standardizing excipient nomenclature, normalizing concentration units, and curating out failed experiments that may have been terminated prematurely, is the most labor-intensive part of the ML implementation.
Process optimization using ML draws on the PAT data stream from manufacturing equipment. Models trained on time-series data from granulator temperature sensors, torque measurements, and moisture probes can predict granule endpoint properties (size distribution, bulk density) from process signatures rather than relying on offline analytical testing. This enables adaptive process control: the manufacturing system adjusts CPPs in real time based on the predictive model output rather than waiting for offline QC results.
Regulatory intelligence tools, some built on large language model foundations, can analyze FDA deficiency letter databases, ANDA approval histories, and product-specific guidances to identify the most common review issues for a given dosage form category and flag potential CMC vulnerabilities in a draft submission before filing. This is not automated compliance. It is structured risk identification that the human CMC team then prioritizes and addresses.
14.2 The Data Infrastructure Prerequisite
AI-driven formulation development cannot substitute for data quality or data volume. The minimum training data set size for a meaningful predictive dissolution model is typically 200 to 500 distinct formulation batches with fully characterized input and output data. Most generic companies with active ER pipelines have this data in some form, but it is frequently distributed across multiple LIMS instances, paper lab notebooks, and project-specific spreadsheets that cannot be queried uniformly.
The investment required to build a consolidated, structured formulation data repository is a pre-competitive infrastructure cost. Companies that make this investment gain a compounding advantage: every new development batch adds to the model training data, making predictions more accurate over time. Companies that do not make the investment cannot access ML-driven formulation tools, regardless of the sophistication of the algorithms available, because the algorithms are only as useful as the data they run on.
14.3 The Regulatory Position on AI-Generated Evidence in ANDA Submissions
FDA has not yet published definitive guidance on the use of AI-generated predictions or models as supporting evidence in ANDA submissions. The agency’s framework for software as a medical device (SaMD) guidance and its discussion documents on AI in drug development establish the principle that AI outputs must be validated against empirical data and that the validation methodology must be transparently documented.
For formulation development purposes, the practical implication is that an ML model’s prediction of a dissolution profile does not replace the experimental dissolution data. It can, however, reduce the number of experiments required to navigate the design space, provided the model’s predictive accuracy is documented in the pharmaceutical development section of the ANDA. FDA reviewers are increasingly familiar with DoE-based development; AI-assisted DoE, where the model selects the next most informative experimental point rather than the formulator selecting it manually, is a natural extension that fits within the existing framework.
15. Investment Strategy for Analysts
15.1 How to Value a Generic ANDA Pipeline
Institutional investors and portfolio managers evaluating generic pharmaceutical companies routinely undervalue or overvalue ANDA pipelines because they apply standard discounted cash flow methodology to revenue projections that ignore the technical and regulatory risk embedded in formulation complexity.
A sound valuation framework for an ANDA pipeline adjusts for four risk dimensions: technical risk (probability of achieving bioequivalence), regulatory risk (probability of first-cycle approval given the CMC quality and facility compliance history), competitive risk (number of other filers targeting the same product and their estimated timeline), and market risk (price erosion dynamics after generic entry given the number of eventual entrants).
Technical risk is highest for complex dosage forms. Long-acting injectables, topical semisolids, and inhalation products have historically failed at BE at rates substantially higher than standard oral solid products. A pipeline that appears diverse may be heavily concentrated in high-technical-risk complex products. Investors should ask specifically about the number of failed BE studies in a company’s development history, the reasons for those failures, and whether the company has the in-house expertise to address the failure modes most common in its target product categories.
Regulatory risk is increasingly quantifiable through GDUFA performance data. Companies with active FDA Warning Letters covering their manufacturing facilities face systematic delays regardless of the quality of their CMC submissions. A Warning Letter can add 12 to 18 months to approval timelines for all ANDAs associated with the affected facility. Investors should monitor FDA’s facility inspection database and cross-reference manufacturing sites against ANDA portfolios.
15.2 The Economics of 180-Day FTF Exclusivity
The 180-day exclusivity period for the first Paragraph IV filer is the most economically significant event in the generic pharmaceutical calendar for any given product. The value of the exclusivity is a function of four variables: the size of the brand-name market at the time of generic entry, the rate of generic conversion during the exclusivity period, the price premium achievable relative to post-exclusivity generic pricing, and whether the exclusivity is shared (if multiple companies file simultaneously and are deemed co-first filers).
For large primary care markets, the 180-day exclusivity window can generate revenues of $100 million to $500 million for the first filer, depending on product and market conditions. For specialty or hospital markets, the economics are different. Brand-name drugs with limited market size, strong physician brand loyalty, or complex reimbursement dynamics may see slower generic conversion during the exclusivity period, compressing the financial benefit.
The critical valuation insight for portfolio managers is that exclusivity value is highly sensitive to timing. A six-month delay in ANDA approval, caused by a CRL, can convert a $400 million exclusivity opportunity to a $0 exclusivity outcome if a competitor achieves approval and commercial launch first. The risk-adjusted value of an ANDA in Paragraph IV litigation must therefore be discounted not just for the probability of losing the patent case but for the probability of being first to launch conditional on winning.
15.3 Biosimilar Pipeline Valuation: Reference Product IP and Interchangeability Premium
Biosimilar pipeline valuation requires the same IP-adjusted analysis applied to small-molecule generics, amplified by the greater complexity of the reference product patent estate and the binary commercial value of interchangeability designation.
Investors should assess: the reference product’s U.S. revenue and its trajectory (growing, stable, or declining due to disease area competition); the settlement landscape (have other biosimilar developers already negotiated entry dates, and do those dates provide an implied market entry window?); the interchangeability status of competing biosimilars (a biosimilar with interchangeability designation entering a market where other biosimilars lack that designation has a structural market access advantage); and the clinical indication scope of the biosimilar license (biosimilars approved for all reference product indications through extrapolation have a broader commercial footprint than those with restricted indication approvals).
The IP valuation of the reference product is a specific asset for the innovator company and a specific liability for the biosimilar developer. AbbVie’s patent thicket strategy for Humira added approximately $50 billion in cumulative U.S. revenues beyond what would have accrued under a thinner IP estate. The biosimilar developers who settled for post-2023 U.S. entry dates effectively agreed to pay AbbVie the time-value of those delayed revenues in the form of foregone market opportunity.
16. Key Takeaways by Segment
For Formulation Scientists and CMC Leads
Bioequivalence for extended-release oral products is not achieved by matching API content. It requires matching the pharmacokinetic profile in both fed and fasting states. For BCS Class I products, the delivery mechanism is the critical design element, and every material attribute and process parameter that affects the mechanism must be identified, studied, and controlled. Excipient variability is a legitimate source of formulation failure and must be managed at the supplier qualification level, not the batch release level. Establishing a Level A IVIVC is worth the investment for any ER product with post-approval lifecycle management potential. PAT integration improves batch consistency and provides a real-time control strategy that strengthens the ANDA submission.
For IP Teams and Patent Counsel
The Orange Book is the starting point, not the complete picture. A full patent estate analysis covering composition, polymorph, formulation, process, and method-of-use patents must precede formulation design. Formulation strategy and Paragraph IV strategy are not independent. The technical design must be reviewed by patent counsel at multiple development stages to ensure non-infringement arguments remain valid as the formulation evolves. Biosimilar patent thickets require specialized IP analytics. Reference product settlement histories and shared exclusivity positions significantly affect the commercial modeling for any biosimilar development program.
For Portfolio Managers and Business Development
Product selection for complex ER and complex generic programs must weigh technical risk explicitly, not just market size and patent expiry. BE failure rates for topical, inhaled, and LAI products are substantially higher than for oral solid products. First-cycle ANDA approval rate should be a tracked KPI for any generics-focused company. A persistent below-industry approval rate is a leading indicator of CMC quality problems that will depress the commercial value of the pipeline. Biosimilar interchangeability designation commands a premium market access position that should be separately valued in pipeline models.
For Institutional Investors
The economic value of a generic drug ANDA is a function of patent risk, technical risk, regulatory risk, and competitive timing, in roughly equal measure. The technical risk component is systematically underanalyzed because it requires formulation science expertise that most investment teams do not maintain in-house. Companies with documented QbD development programs, validated IVIVC libraries, and strong first-cycle approval track records are less likely to face the timeline disruptions that destroy exclusivity value. The biosimilar market represents the next major value creation opportunity in the generic pharmaceutical sector. IP thicket analysis and interchangeability strategy will determine which companies capture that value and which fund the reference product manufacturer’s extended exclusivity through their own delayed entry.
References
- Association for Accessible Medicines. 2023 Generic Drug & Biosimilars Access & Savings in the U.S. Report.
- IQVIA Institute for Human Data Science. The Use of Medicines in the U.S. 2023.
- Hatch-Waxman Amendments to the Federal Food, Drug, and Cosmetic Act, 21 U.S.C. 355(j).
- 21 CFR Part 320 – Bioavailability and Bioequivalence Requirements.
- Sandberg A, et al. Pharmacokinetic and pharmacodynamic properties of a new controlled-release formulation of metoprolol: a comparison with a conventional tablet. Eur J Clin Pharmacol. 1988;33(Suppl):S9-S14.
- Amidon GL, et al. A theoretical basis for a biopharmaceutic drug classification: the correlation of in vitro drug product dissolution and in vivo bioavailability. Pharm Res. 1995;12(3):413-420.
- Bauer J, et al. Ritonavir: an extraordinary example of conformational polymorphism. Pharm Res. 2001;18(6):859-866.
- FDA Inactive Ingredient Database. accessdata.fda.gov/scripts/cder/iig.
- Colombo P, et al. Swellable matrices for controlled drug delivery: gel-layer behaviour, mechanisms and models. PSTT. 2000;3(6):198-204.
- FDA Guidance for Industry: Extended Release Oral Dosage Forms: Development, Evaluation, and Application of In Vitro/In Vivo Correlations. 1997.
- ICH Harmonised Guideline Q8(R2): Pharmaceutical Development. 2009.
- FDA Guidance for Industry: PAT – A Framework for Innovative Pharmaceutical Development, Manufacturing, and Quality Assurance. 2004.
- FDA Guidance for Industry: Bioequivalence Studies With Pharmacokinetic Endpoints for Drugs Submitted Under an ANDA. 2021.
- FDA Complex Drug Products. fda.gov/drugs/generic-drugs/complex-generic-drugs.
- FDA Guidance for Industry: Scientific Considerations in Demonstrating Biosimilarity to a Reference Product. 2015.
- FTC v. Actavis, Inc., 570 U.S. 136 (2013).
- FDA GDUFA III Commitment Letter. 2022.
Copyright notice: This article draws on publicly available regulatory guidance, academic literature, and industry data. It does not constitute legal or investment advice. Patent analysis and portfolio decisions should be made in consultation with qualified patent counsel and financial advisors.