The Market You’re Actually Competing In

The generic drug industry saves the U.S. healthcare system more than $445 billion per year. Generics fill over 90% of all prescriptions dispensed domestically. Globally, the market was valued at roughly $491 billion in 2024 and is projected to reach $926 billion by 2034, driven by aging demographics, chronic disease prevalence, and relentless pressure from payers and governments to reduce drug spend. These numbers make generics look like a growth industry. In practice, for the companies inside it, large portions of the market are a slow-motion margin collapse.
The data is precise about how brutal the commodity dynamic gets. A single generic entrant cuts the brand’s price by 30% to 39%. Two or three generics push prices down 50% to 70%. Ten or more generics, and the price drops as much as 95% from the brand’s peak. At those economics, the cost of manufacturing and regulatory compliance often exceeds the per-unit revenue, and the result has been documented drug shortages in dozens of therapeutic categories. The Association for Accessible Medicines has stated plainly that the sustainability of the generics industry ‘remains fragile.’ The Guardian reported in January 2024 that generic drugs in the U.S. are in some categories ‘too cheap to be sustainable.’
This commoditization is not random. It is the predictable consequence of the legislative design of the Hatch-Waxman Act working exactly as intended, creating competition that pushes prices to marginal cost. For companies that understood this dynamic early, the strategic response was clear: move up the complexity curve, toward products that cannot be commoditized quickly because the science, the IP, and the manufacturing know-how required to replicate them create natural barriers.
That pivot is now industry-wide. The products commanding sustainable margins are modified-release oral solids, long-acting injectables (LAIs), transdermal drug delivery systems, ophthalmic suspensions and emulsions, and biosimilars. These product categories share one characteristic: their performance is not determined solely by the identity and quantity of their ingredients. It is determined by the physical structure, microarchitecture, and dynamic behavior of the final dosage form. Replicating that structure requires systematic reverse engineering, which the industry calls deformulation.
Mastering deformulation is the central competency separating companies that will grow profitably through the rest of this decade from those that will continue racing to the bottom on oral tablets. This document covers every dimension of that competency, from the regulatory framework that creates the financial incentive, to the specific analytical techniques that generate the data, to the IP intelligence strategy that turns lab results into market exclusivity.
Key Takeaways: Market Context
The simple generics race to commoditization is a structural feature, not a temporary disruption. The only exit is up the complexity curve. Complex formulations, including modified-release products, LAIs, transdermal patches, and biosimilars, require systematic deformulation to develop. Deformulation is not a lab function; it is the strategic lever connecting market intelligence to ANDA filing to 180-day exclusivity capture. Companies that treat it as a cost center will continue losing ground to those that treat it as a core competitive function.
The Hatch-Waxman Rulebook: Every Provision That Matters
The Drug Price Competition and Patent Term Restoration Act of 1984 (universally called the Hatch-Waxman Act) created the modern generic pharmaceutical industry. It resolved a prior regulatory failure: before 1984, a generic manufacturer had to conduct full clinical trials to prove safety and efficacy for a drug whose active ingredient had already been proven safe and effective by the brand company. That requirement was redundant and expensive. Hatch-Waxman eliminated it by creating the Abbreviated New Drug Application (ANDA) pathway.
The ANDA Pathway and Bioequivalence
Under the ANDA pathway, a generic applicant relies on the FDA’s prior finding of safety and efficacy for the Reference Listed Drug (RLD). The applicant’s scientific burden shifts entirely to demonstrating bioequivalence: proving that the generic product delivers the same amount of active pharmaceutical ingredient (API) into the bloodstream over the same period as the RLD. The FDA defines bioequivalence using the statistical 90% confidence interval of the generic’s pharmacokinetic parameters falling within 80% to 125% of the RLD’s. If you hit that window, FDA considers the products therapeutically equivalent, and pharmacists can substitute one for the other.
The direct consequence for development strategy is this: a generic company does not need to re-prove that the drug works. It needs to prove its product performs the same as the version already proven to work. That makes the RLD the entire analytical reference point. Every formulation decision, every manufacturing parameter, and every stability study is calibrated against the RLD’s observed behavior. Reverse engineering the RLD is not preparatory work; it is the core scientific activity of ANDA development.
Paragraph IV Certification: The Strategic Challenge Filing
When submitting an ANDA, a generic applicant must address every Orange Book-listed patent for the RLD. The Orange Book (officially the FDA’s Approved Drug Products with Therapeutic Equivalence Evaluations) contains brand companies’ self-disclosed patent portfolios for each listed drug. A Paragraph IV (PIV) certification declares that a listed patent is either invalid, unenforceable, or will not be infringed by the proposed generic product.
Filing a PIV certification is, by legal construction, an act of patent infringement. Federal statute (35 U.S.C. § 271(e)(2)) makes filing itself the infringing act, which triggers the brand company’s right to sue. The applicant must notify the patent holder and NDA holder within 20 days of the ANDA receiving a filing date. The brand company then has 45 days to initiate litigation. If it files suit within that window, the FDA is automatically barred from approving the ANDA for 30 months unless the court resolves the case first. This 30-month stay is the brand company’s most powerful defensive tool, granting up to two-and-a-half additional years of effective market exclusivity at zero cost beyond the filing fee for the lawsuit.
The data on Paragraph IV litigation is instructive. The FDA Center for Drug Evaluation and Research has recorded that brand companies sue on roughly 75% of first-to-file PIV challenges. Generic applicants prevail outright or reach settlement in the large majority of cases, but the litigation itself typically runs 18 to 36 months. Understanding the claim language of every Orange Book-listed patent before filing is not optional; it is the determinant of whether a PIV challenge is viable or financially ruinous.
180-Day Exclusivity: The Financial Architecture of First-to-File
The 180-day marketing exclusivity provision is the financial engine that drives the entire PIV challenge ecosystem. The first generic company to file a substantially complete ANDA with a valid PIV certification for a given drug is awarded 180 days during which the FDA cannot approve any other generic versions of that product.
The financial mechanics of this exclusivity period are well understood inside the industry. During 180-day exclusivity, the first generic entrant competes only against the high-priced brand in a temporary duopoly. The generic can price its product at a discount to the brand, typically 20% to 30%, capture significant formulary position, and collect margins far above the commodity-level prices that emerge after the exclusivity period expires. For large-revenue drugs, the first-to-file prize can be worth hundreds of millions of dollars. Historical analysis across multiple blockbuster patent cliffs suggests that 60% to 80% of a generic product’s total lifetime profit can be captured within this six-month window.
That financial structure is what makes precision and speed in deformulation directly valuable to the executive suite. The faster and more accurately a company can characterize the RLD, design a bioequivalent formulation, build the patent challenge strategy, and file the ANDA, the greater its probability of capturing first-to-file status. Laboratory efficiency is not a scientific nicety; it translates directly into a competitive legal position and a specific dollar advantage.
The 30-Month Stay and Its Strategic Use by Brand Companies
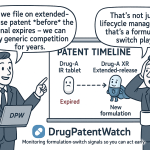
Brand companies have learned to use the 30-month stay as a component of their commercial lifecycle management. By constructing layered patent portfolios with multiple patents covering different aspects of the drug product (the API, the formulation, the dosage form, the manufacturing process, the polymorph, metabolite, methods of treatment), they can generate multiple distinct PIV challenges and, in theory, multiple overlapping 30-month stays. The FTC and Congress have addressed some of the most egregious stay-stacking through the 2003 Medicare Modernization Act amendments to Hatch-Waxman, but the strategic use of formulation and polymorph patents to extend effective exclusivity remains standard practice.
Table 1: Hatch-Waxman Provisions and Their Strategic Implications
| Provision | Trigger | Brand Weapon | Generic Weapon | Role of Deformulation |
|---|---|---|---|---|
| ANDA Pathway | Generic ANDA filing | N/A | Eliminates need for clinical trials | RLD characterization defines the bioequivalence target |
| PIV Certification | ANDA filing with patent challenge | Lawsuit within 45 days activates 30-month stay | First-to-file wins 180-day exclusivity | Analytical data builds the non-infringement or invalidity argument |
| 30-Month Stay | Brand lawsuit within 45 days of PIV notification | Up to 2.5 years of additional de facto exclusivity | Aggressive litigation strategy; seek summary judgment | Deformulation data quality determines the strength of early settlement leverage |
| 180-Day Exclusivity | First substantially complete ANDA with PIV | None (cannot be blocked by brand) | Temporary duopoly with the brand; captures majority of lifetime profit | Deformulation speed determines first-to-file probability |
Patent Thickets, Evergreening, and the IP Valuation of Your Target Drug
How Innovators Build Patent Fortresses
Brand pharmaceutical companies do not rely on a single patent to protect a blockbuster drug. They construct what IP practitioners call a patent thicket: a layered stack of patents, each covering a different aspect of the product, timed to expire at different points in the future. The result is that even after the original compound patent expires, a generic company faces dozens of additional patents on formulations, dosage forms, manufacturing processes, polymorphic forms, particle size specifications, specific excipient combinations, and methods of treatment.
The tactic is called evergreening, and it is systematic. The typical lifecycle of a blockbuster small-molecule drug involves four or five distinct patent protection waves. The base compound patent (often filed during early discovery) provides the initial protection window, typically 20 years from filing date, often reduced to an effective market exclusivity of 12 to 14 years by the time FDA approval arrives. Patent Term Extensions (PTEs) under Hatch-Waxman itself can restore up to five years of patent life lost to the regulatory review period, capped at a remaining term of 14 years post-approval.
After the compound patent, the brand files formulation patents covering the specific dosage form (e.g., the extended-release matrix or the microparticle suspension). These routinely add three to seven years of exclusivity beyond the compound patent cliff. Next come polymorph patents covering the specific crystal form used in the commercial product. API manufacturers and brand companies alike file these, and they have been the subject of prolific litigation, most notably AstraZeneca’s patent strategy on omeprazole (Prilosec to Nexium) and Pfizer’s campaigns around atorvastatin (Lipitor). Active metabolite patents on pharmacologically active breakdown products of the parent API represent another layer, as do salt form patents and patents claiming specific particle size ranges for the API or excipient.
Beyond the product itself, brand companies file method-of-treatment patents covering the approved indications, sometimes with specific dosing schedules. Teva’s extended-release formulation of glatiramer acetate (Copaxone 40 mg/mL, dosed three times weekly) generated a rich pattern of method-of-use patents that complicated generic entry well after the core compound patents expired.
IP Valuation Framework for Target Drug Assessment
Before a generic company commits R&D resources to deformulation of an RLD, its business development team and IP counsel must conduct a rigorous IP valuation. This is not simply counting the number of Orange Book-listed patents. It requires assessing the economic and legal weight of each patent individually.
The IP valuation framework for a target drug should include at least the following analytical components.
The first component is patent term mapping: plotting every Orange Book-listed patent against its expiration date, distinguishing between compound patents, formulation patents, polymorph patents, and method patents. This establishes the patent cliff structure. A drug with a compound patent expiring in 2025 but formulation patents running to 2031 is a very different proposition from one whose entire portfolio expires simultaneously.
The second component is claim scope analysis: reading the independent claims of each formulation and polymorph patent to understand how broadly or narrowly the claims are drawn. A formulation patent that claims ‘a sustained-release composition comprising [API] and a hydroxypropyl methylcellulose polymer in a ratio of 1:0.5 to 1:2.0’ is significantly narrower than one that claims ‘a sustained-release composition comprising [API] and a cellulosic polymer.’ Narrow claims are easier to design around.
The third component is litigation history review: examining prior Paragraph IV challenges to the same drug, their outcomes, and settlement terms. Multiple generic companies may have already cleared some of the patent claims through prior litigation or settlements, reducing the risk for a later filer. DrugPatentWatch and commercial IP databases like Derwent Innovation and Anaqua aggregate this litigation history in machine-readable form.
The fourth component is market exclusivity residual value analysis: modeling the revenue that would be captured during 180-day exclusivity for the target drug, discounted by the probability of winning first-to-file status given current competitive intelligence on which other companies are likely developing generic versions.
The fifth component is Freedom to Operate (FTO) assessment of the proposed formulation approach: once the deformulation team has characterized the RLD’s composition and structure, the IP team must confirm that the proposed generic formulation does not reproduce the specific combinations claimed in the surviving formulation patents.
Case Examples: IP Stacking in Complex Generics
Risperdal Consta (risperidone extended-release injectable microspheres) illustrates the IP complexity facing a generic developer targeting an LAI. Johnson & Johnson’s Janssen Pharmaceuticals built a portfolio covering the base compound, the PLGA microsphere formulation, specific polymer molecular weight and end-group specifications, the solvent evaporation manufacturing process, and the reconstitution kit configuration. The result was a product that remained largely insulated from generic competition for years beyond the primary compound patent expiration. The deformulation challenge is not merely to characterize the microsphere composition; it is to understand the precise PLGA grade, molecular weight distribution, and drug loading that are claimed in the surviving formulation patents, then either match the non-claimed aspects or design a novel microsphere system with equivalent release kinetics.
Concerta (methylphenidate HCl, 18 mg to 72 mg, OROS formulation) offers a different architecture. Alza Corporation’s OROS osmotic pump system was protected by a dense cluster of device and formulation patents. IMPAX Laboratories filed a PIV challenge and developed what it called an ‘extended-release’ formulation that technically delivered methylphenidate over a similar duration but with a different release mechanism, an immediate-release bead/extended-release bead combination rather than an osmotic pump. The FDA initially granted bioequivalence, but the formulation later became the subject of controversy when clinical pharmacists questioned its interchangeability in practice. The OROS system’s precise push-pull osmotic pump architecture can only be replicated through manufacturing processes protected by the original device patents; any ‘design-around’ will produce a different Q3 structure and must be assessed for true bioequivalence independently.
Deformulation: What Q1, Q2, and Q3 Sameness Actually Require
The Regulatory Architecture of the Q-Framework
The FDA’s Q1/Q2/Q3 framework is the regulatory lingua franca of generic formulation development. These three designations organize the hierarchy of analytical requirements for demonstrating sameness to the RLD, and their relative importance shifts dramatically depending on the complexity of the dosage form.
Q1, qualitative sameness, requires that the proposed generic contain the same inactive ingredients as the RLD. This seems straightforward, but several complications arise in practice. First, the FDA’s Inactive Ingredient Database and the RLD’s prescribing information often list excipient names at varying levels of specificity. ‘Hydroxypropyl methylcellulose’ is a class name; the commercial grade used could be Methocel K4M, K15M, or K100M, each with a different viscosity and different drug release characteristics when used in a hydrophilic matrix tablet. Second, confirming Q1 requires analytical identification, not just reference to public sources, because errors in public documentation exist and because the grade of an excipient matters as much as its identity.
Q2, quantitative sameness, requires that the concentration of each inactive ingredient in the generic match the RLD within an acceptable range, typically plus or minus 5% of the total formulation weight. This is where the analytical complexity escalates. Determining that microcrystalline cellulose constitutes 38.5% of a tablet’s total weight, in the presence of magnesium stearate, croscarmellose sodium, hypromellose, titanium dioxide, polyethylene glycol, and the API, requires a carefully designed separation and quantification strategy. There is no single method that quantifies all excipient classes simultaneously with acceptable precision. The analytical team must build a multi-method approach.
Q3, physicochemical sameness, is where the science becomes sophisticated enough to constitute a competitive moat. For complex generics, Q3 encompasses the solid-state form of the API, the particle size distribution of the API and key excipients, the microstructure of the dosage form (how the API and rate-controlling polymers are spatially arranged), viscosity, rheological behavior, pH, osmolality, drug release kinetics, and the colligative properties of the vehicle for liquids and semisolids.
The key strategic insight is this: for simple immediate-release oral tablets, achieving Q1 and Q2 sameness usually produces a Q3-equivalent product automatically, and bioequivalence follows. For every complex dosage form on the high-margin end of the market, Q3 sameness is the dominant constraint. A developer can perfectly reproduce the Q1 and Q2 composition of a PLGA microsphere LAI and still fail spectacularly if the manufacturing process creates microspheres with different size distribution, porosity, or polymer crystallinity. The Q3 failure will manifest as a different in vitro drug release profile and, ultimately, a different in vivo pharmacokinetic profile. Q3 is not a checkbox; it is the performance specification.
The Biowaiver Path: When Q3 Eliminates In Vivo Studies
For specific dosage form categories, the FDA allows a biowaiver: the applicant can demonstrate bioequivalence without conducting an in vivo pharmacokinetic study if the formulation achieves Q1/Q2/Q3 sameness. This is explicitly available for ophthalmic and otic solutions and for certain nasal sprays and oral inhalation products. The logic is that if two sterile solutions contain the same active and inactive ingredients at the same concentrations, with the same physicochemical properties, they will deliver drug to the site of action in an identical manner, and no blood sampling study can meaningfully measure that comparison anyway.
For oral solid dosage forms, Class I BCS (Biopharmaceutics Classification System) drugs with rapid dissolution and high solubility qualify for a biowaiver under FDA’s BCS-based guidance if Q1/Q2 is demonstrated. Achieving a biowaiver for either category saves between $1 million and $3 million in clinical study costs and six to twelve months of development time. That is the direct economic value of comprehensive, accurate deformulation.
Key Takeaways: Q1/Q2/Q3 Framework
For simple oral tablets, Q1/Q2 is the decisive challenge. For modified-release, parenteral, transdermal, ophthalmic, and other complex dosage forms, Q3 sameness is the rate-limiting step. The analytical investment required scales with product complexity: a standard oral tablet requires perhaps four to six primary analytical techniques; a long-acting injectable requires a dozen or more, many of them highly specialized. A correctly executed deformulation program eliminates the guesswork from formulation development and provides the technical basis for the biowaiver applications and PIV litigation support that multiply the economic return.
The Systematic Deformulation Workflow
Step 1: Strategic RLD Procurement and Multi-Lot Assessment
Deformulation does not start at the instrument. It starts with a deliberate procurement strategy for the RLD. Best practice calls for acquiring a minimum of three distinct lots: a freshly manufactured lot with maximum remaining shelf life, a lot at mid-shelf-life, and a lot approaching expiration. Comparing freshly manufactured and aged lots reveals the degradation chemistry of the formulation, the identity and growth rate of degradation products, and the physical changes that occur over time, such as polymorph conversion or particle size shifts in suspension-based products.
This multi-lot analysis is commercially significant in two ways. First, it enables the generic developer to design a formulation with at least equivalent stability, reducing the risk of costly late-stage stability failures. Second, it sometimes reveals that the innovator’s own product has a poorly controlled quality attribute, which can be used to argue for broader acceptance criteria in the ANDA or, in some cases, as part of a patent invalidity argument based on lack of enablement.
Procurement also covers packaging characterization. The closure system (e.g., a specific glass or HDPE container with a particular oxygen permeability and moisture vapor transmission rate) can be integral to the product’s stability performance. For products sensitive to light, oxygen, or moisture, the container-closure system must be treated as a functional component of the formulation.
Step 2: Physical and Functional Baseline Characterization
Before any separation or spectroscopic analysis occurs, the team conducts a complete physical and functional characterization of the RLD. For oral solid dosage forms, this includes weight, dimensions, hardness, friability, and disintegration time. For modified-release tablets, the dissolution profile at multiple pH values and in multiple dissolution media is the defining functional target. Every formulation and process decision downstream must be traceable back to matching this profile.
For liquids and semi-solids, the baseline includes pH, osmolality, viscosity at one or more shear rates, turbidity, color, and, for suspensions, sedimentation rate. For injectables, the initial assessment covers syringeability, which involves measuring the force required to push the product through the intended needle gauge, and for depot formulations, the visual and textural characteristics of the depot that forms immediately after injection. These physical assessments are both Q3 targets and regulatory requirements for the ANDA submission.
Step 3: Component Separation
Component separation is the technical heart of the deformulation workflow. The objective is to reduce the complexity of the mixture enough that individual components can be identified and quantified without interference from other ingredients. No separation strategy is universal; the correct approach depends on the physical state of the dosage form and the physicochemical properties of the target components.
For solid dosage forms, the separation typically begins with a selective dissolution strategy. If the API is highly soluble in a specific organic solvent in which most excipients are not, an initial extraction can isolate the API. Residual solid material can then be subjected to sequential extractions in solvents of increasing polarity, separating lipophilic excipients (waxes, glycerides, hydrogenated vegetable oils) from hydrophilic polymers (celluloses, povidone, copovidone) and inorganic fillers (calcium phosphate, silicon dioxide, magnesium silicate). For coated dosage forms, the coating must first be physically removed, characterized separately, and then the core subjected to the same sequential extraction strategy.
For parenteral products, the separation strategy depends on whether the product is a solution, a suspension, or a microparticle system. For aqueous solutions, direct chromatographic injection after appropriate dilution and filtration often suffices. For microparticle systems like PLGA microspheres, the particles must first be isolated by filtration or centrifugation, the polymer matrix dissolved in a compatible solvent, and the drug content released and quantified before the polymer itself is characterized for molecular weight and end-group composition.
Step 4: Identification and Quantification
Once components are separated or isolated, identification (Q1) and quantification (Q2) proceed in parallel using a suite of orthogonal techniques. The principle of analytical orthogonality means using methods based on different physical or chemical phenomena so that each confirms the others rather than repeating the same measurement. If HPLC-UV and HPLC-MS both identify the same compound independently, the identification confidence is substantially higher than either alone.
The standard protocol deploys Fourier-transform infrared spectroscopy (FTIR) or Raman spectroscopy for rapid qualitative identification against reference libraries, HPLC with selective detection for quantification of organic excipients, ion chromatography or capillary electrophoresis for ionic species, thermogravimetric analysis for moisture content and volatile components, and XRPD for solid-state form identification. For complex formulations, at least eight to twelve distinct analytical methods typically contribute to the complete Q1/Q2 profile.
Step 5: Data Synthesis and the Deformulation Blueprint
The output of all the analytical work is a single comprehensive document: the deformulation blueprint. This document is the key deliverable that drives everything downstream: formulation development, patent challenge strategy, regulatory submissions, and manufacturing process design. A well-constructed deformulation blueprint includes the complete Q1 ingredient list with analytical confidence ratings for each identification, Q2 quantitative data with precision and accuracy estimates, Q3 characterization data covering solid-state properties, particle size distributions, release profiles, and structural observations, and stability-indicating information from the multi-lot comparison.
The blueprint also identifies gaps: components that resist identification, quantities that cannot be precisely determined, or structural features that require additional characterization. These gaps inform the next phase of investigation and are documented as open items in the development risk register.
The Analytical Arsenal: Technique-by-Technique Reference Guide
API Characterization: Confirming the Cornerstone
Nuclear Magnetic Resonance (NMR) Spectroscopy
NMR probes the magnetic environments of specific atomic nuclei within molecules. In a strong magnetic field, nuclei like hydrogen (1H) and carbon (13C) absorb radiofrequency energy at frequencies that depend on their local electronic environment. The resulting chemical shifts and coupling patterns map the molecular connectivity with a precision no other technique matches.
In pharmaceutical deformulation, NMR plays three distinct roles. For API structural confirmation, a 1H NMR spectrum of the isolated API compared against the reference standard provides unambiguous identity proof. The FDA considers NMR the gold standard for structural elucidation of unknown impurities, precisely because the spectrum encodes every carbon and proton environment in the molecule. For quantification, quantitative NMR (qNMR) exploits the direct proportionality between peak area and nuclear count to determine absolute purity without requiring a matched reference standard for every analyte. This is particularly useful in early development when certified reference standards for all expected impurities are not yet available. For solid-state characterization, solid-state NMR (SSNMR) can detect polymorphic transitions, amorphous content, and drug-polymer interactions in the final dosage form, providing complementary evidence to XRPD.
The analytical limitation of solution-state NMR is its relatively poor sensitivity for trace impurities compared to mass spectrometry. A typical 600 MHz NMR instrument in quantitative mode has a detection limit around 0.1% to 0.5% of the major component, which is adequate for excipient quantification but insufficient for ICH Q3B-compliant impurity profiling at the 0.05% reporting threshold.
Mass Spectrometry: Impurity Profiling and Molecular Confirmation
Mass spectrometry ionizes molecules and measures their mass-to-charge ratio (m/z) with exceptional sensitivity and specificity. The technique is almost always deployed in a hyphenated configuration: liquid chromatography-mass spectrometry (LC-MS) for non-volatile analytes, or gas chromatography-mass spectrometry (GC-MS) for volatile or semi-volatile compounds.
High-resolution mass spectrometry (HRMS), using instruments such as Orbitrap or time-of-flight analyzers, measures accurate mass to within a few parts per million. This precision is sufficient to determine the exact elemental formula of an unknown compound directly from its molecular ion. A peak at m/z 306.0534 in positive ion mode corresponds unambiguously to C16H10FNO4 when measured with a modern Orbitrap, providing the first step in structural identification of an unknown impurity without requiring a reference standard.
Tandem MS (MS/MS or MSn) fragments ions inside the mass spectrometer, generating product ion spectra that reveal connectivity and functional group positions. Combined with HRMS and chromatographic retention time matching, MS/MS provides sufficient structural evidence for definitive identification of process-related and degradation impurities at concentrations well below ICH reporting thresholds.
For deformulation specifically, LC-HRMS deployed against a matrix digest of the complete dosage form can detect and identify not just the API but multiple excipients simultaneously, provided appropriate chromatographic conditions are used. This so-called ‘untargeted’ metabolomic approach, borrowed from clinical bioanalysis, has begun appearing in complex generic development pipelines as a tool for initial, comprehensive Q1 screening before targeted quantitative methods are built.
X-Ray Powder Diffraction (XRPD) and Polymorph Strategy
XRPD is the primary instrument for polymorphic form identification. When a crystalline powder is irradiated with monochromatic X-rays, the crystal lattice diffracts the X-rays at angles defined by Bragg’s Law (nλ = 2d sin θ), where d is the interplanar spacing specific to the crystal structure. The resulting diffractogram is a fingerprint of the crystal form, reproducible from any sample of the same polymorph regardless of particle size or sample history.
The pharmaceutical importance of polymorphism cannot be overstated. The FDA’s regulatory experience is littered with bioequivalence failures traced to polymorphic form discrepancies. Abbott’s ritonavir (Norvir) manufacturing crisis in 1998, when Form II of ritonavir precipitated from capsule formulations designed around Form I, caused a temporary product withdrawal that cost tens of millions of dollars. The more soluble Form I had been accidentally replaced by a less soluble, thermodynamically stable Form II. For a generic developer, this history translates into a clear operational requirement: identify the polymorph in the RLD with XRPD, confirm it with DSC, and then decide whether to replicate it or deliberately develop a non-infringing alternative.
Differential Scanning Calorimetry (DSC) complements XRPD by measuring thermal events as a function of temperature. A crystalline polymorph melts at a specific temperature with a characteristic enthalpy; the DSC trace shows a sharp endotherm at that temperature. An amorphous material does not melt but exhibits a glass transition temperature (Tg) and may crystallize on heating before eventually melting. The combination of XRPD and DSC can quantify amorphous content in a nominally crystalline sample, which is critical because amorphous regions are typically more soluble but less physically stable than crystalline regions.
From an IP strategy perspective, the polymorph identified in the RLD must be cross-referenced against the Orange Book patent portfolio. If a polymorph patent is in force, the generic developer has two choices: design around to a non-claimed polymorph (a ‘design-around’ strategy) while ensuring bioequivalence, or file a PIV challenge arguing that the polymorph patent is invalid or not infringed. Both paths require definitive characterization of the RLD’s polymorphic form as the analytical foundation.
Particle Size Analysis: Laser Diffraction and Electron Microscopy
Particle size is a Critical Quality Attribute (CQA) for APIs with poor aqueous solubility (BCS Class II and IV), for API suspensions, and for excipients where size affects compaction or release kinetics. Laser diffraction (LD), also called laser diffraction particle size analysis, measures the angular distribution of light scattered by a particle ensemble and uses Mie theory calculations to derive a volume-weighted particle size distribution.
The industry-standard output is the D10, D50, and D90 values representing the 10th, 50th, and 90th percentiles of the cumulative volume distribution. An RLD’s suspension might specify D90 less than 10 micrometers for a specific API; a generic that achieves D50 match but fails D90 will have a different dissolution rate and potentially different bioavailability.
Scanning Electron Microscopy (SEM) provides direct visual confirmation of particle morphology that LD cannot deliver. LD reports all particles as equivalent spheres; SEM shows whether they are acicular (needle-like), platelet, agglomerated, or genuinely spherical. This distinction matters because particle shape affects powder flow, compressibility, and the specific surface area available for dissolution. An API that appears mono-modal in LD data but is actually a bimodal mixture of needles and spheres will behave differently in a tablet press and in a dissolution vessel than a truly mono-modal spherical particle distribution of the same D50.
Excipient Deformulation: Chromatographic and Spectroscopic Approaches
HPLC and GC: The Quantification Workhorses
High-Performance Liquid Chromatography (HPLC) is the single most widely used technique for Q2 quantification in deformulation. The diversity of detection options makes it applicable to nearly every excipient class. UV-Vis detection covers UV-absorbing compounds including many preservatives, antioxidants, and pH adjusters. Evaporative Light Scattering Detection (ELSD) and Charged Aerosol Detection (CAD) cover non-UV-absorbing compounds including sugars, sugar alcohols, polyols, and lipids. Refractive Index detection works for simple carbohydrates and polyethylene glycols. Coupling HPLC to a mass spectrometer (LC-MS) provides both quantification and definitive structural identification simultaneously, which is the most information-rich configuration for unknown excipients.
Gas Chromatography (GC) is the method of choice for volatile analytes: residual solvents from manufacturing processes, volatile flavors, volatile plasticizers, and short-chain fatty acids. GC coupled to flame ionization detection (FID) provides broad quantitative coverage of organic volatiles. GC-MS provides structural identification. The FDA’s ICH Q3C residual solvent guidance defines permitted daily exposure limits for Class 1, 2, and 3 solvents; GC analysis of the RLD’s residual solvent profile can reveal the manufacturing process used by the innovator, which in some cases is itself patent-protected.
FTIR and Raman Spectroscopy: Chemical Identity and Spatial Mapping
Fourier-Transform Infrared Spectroscopy (FTIR) and Raman spectroscopy probe the vibrational modes of chemical bonds. Both techniques generate spectra that are specific enough to identify excipient classes and in many cases specific grades when compared against well-maintained reference libraries. The key difference in application is that Raman’s laser can be focused to a sub-micron spot, enabling chemical imaging of solid dosage forms with spatial resolution unavailable to FTIR.
Raman chemical imaging (also called Raman mapping or hyperspectral Raman microscopy) collects a full Raman spectrum at each pixel of a two-dimensional raster scan across a tablet cross-section. Processing this data cube with multivariate analysis tools (principal component analysis, partial least squares) generates false-color maps showing the spatial distribution of each chemical species across the scanned area. For a hydrophilic matrix modified-release tablet, such a map immediately reveals whether the API is uniformly distributed through the polymer matrix or concentrated in specific domains, whether the rate-controlling polymer forms a continuous phase or is dispersed, and whether multiple polymer layers are present.
This capability is commercially decisive for complex generics. A competitor trying to develop a modified-release tablet without Raman imaging must guess at the release mechanism from dissolution data alone; the search space of possible mechanisms and compositions is enormous. A team with Raman imaging data knows, from direct observation, whether the innovator used a matrix design, a coated core design, or a reservoir design. That knowledge compresses the formulation search space from months of trial-and-error to a targeted development effort with a defined endpoint.
Table 2: The Deformulation Analytical Toolbox
| Technique | Primary Q-Target | Key Information | Strategic Application |
|---|---|---|---|
| LC-HRMS | Q1, Q2 | Exact mass, molecular formula, structure | Definitive identification of unknowns; untargeted excipient screening |
| HPLC-UV/ELSD/CAD | Q2 | Quantification of most excipient classes | Core Q2 workhorse across all dosage forms |
| GC-MS | Q2 | Volatile excipients, residual solvents | Manufacturing process inference; solvent classification under ICH Q3C |
| NMR (1H, 13C, qNMR) | Q1 | Structural confirmation, absolute purity | FDA gold standard for API identity; purity without reference standards |
| SSNMR | Q3 | Polymorph, drug-polymer interaction | API solid state in finished form; complements XRPD |
| XRPD | Q3 | Crystal form fingerprint | Polymorph identification; patent strategy foundation |
| DSC/TGA | Q3 | Melting, Tg, water content, crystallinity | Amorphous content detection; stability risk assessment |
| Laser Diffraction | Q3 | Particle size distribution (D10/D50/D90) | CQA quantification for suspensions, poorly soluble APIs |
| SEM | Q3 | Particle morphology, surface texture, microstructure | Visual confirmation of Q3 attributes; internal tablet architecture |
| Raman Imaging | Q3 | Spatial distribution of API and excipients | Decoding modified-release mechanisms; competitor intelligence |
| Rheology | Q3 | Viscosity, viscoelasticity, yield stress | Syringeability, spreadability, patient-relevant physical performance |
| Dynamic Light Scattering | Q3 | Nanoparticle/colloidal size and polydispersity | Nanosuspensions, emulsions, liposomes |
| TEM | Q3 | Internal nanoparticle structure, liposome bilayer | Advanced characterization of nanoparticle drug delivery systems |
Complex Dosage Forms: Specialized Analytical Playbooks
Modified-Release Oral Solids: Decoding the Release Architecture
The deformulation of modified-release (MR) oral solids, including extended-release (ER), sustained-release (SR), delayed-release (DR), and controlled-release (CR) tablets and capsules, is a fundamentally different challenge from immediate-release counterparts. The therapeutic performance of these products is controlled not by the API itself but by the physical architecture of the delivery system. The innovator’s IP frequently resides in that architecture, and the generic developer’s goal is to replicate the performance while either replicating the architecture (if legally permissible) or constructing a different architecture that achieves the same pharmacokinetic outcome.
The three primary release mechanisms found in commercial MR oral solids are hydrophilic matrix systems, insoluble matrix systems, and coated particle or multiparticulate systems.
In a hydrophilic matrix system (exemplified by Hypromellose-based ER tablets like the original Glucophage XR or Concerta’s osmotic layer), the API is dispersed in a tablet compressed with one or more water-swellable polymers. On contact with gastrointestinal fluid, the polymer swells and forms a viscous gel layer. The drug diffuses through this gel layer and erodes from the tablet surface over an extended time. The release rate is governed by the viscosity grade of the polymer, its concentration, the particle size of the API, and the tablet’s surface area. Raman imaging of a hydrophilic matrix tablet cross-section reveals the API distribution within the polymer matrix and whether a single polymer or a blend of polymers controls release, directly informing the formulation design.
An insoluble matrix system uses polymers that do not dissolve in gastrointestinal fluid, such as ethylcellulose, polyvinyl acetate, or certain acrylates. The API dissolves out of the matrix via a pore-diffusion mechanism. SEM of tablet cross-sections often shows the characteristic pore network left behind as drug dissolves, and DSC can quantify the amount of porous filler (typically microcrystalline cellulose or lactose) that creates the pore network.
Multiparticulate systems, including pellets, beads, and granules coated with functional membranes and filled into capsules, offer the most flexible and sophisticated release architectures. Each particle consists of a drug-loaded core coated with a rate-controlling membrane of defined thickness and composition. HPMC phthalate, Eudragit L, and Eudragit S are common enteric or pH-dependent coating polymers; ethylcellulose and Eudragit RS/RL are common time-controlled coating polymers. The coating thickness is precisely controlled to achieve the target release profile. Cross-sectional SEM of the particles reveals the coating architecture; FTIR or Raman identifies the coating polymer; mercury porosimetry or nitrogen adsorption measurements quantify coating porosity.
The complete analytical workflow for an MR oral solid must include dissolution testing in at least four pH conditions (1.2, 4.0, 4.5, and 6.8) and at multiple time points to map the entire release profile. The profile must be compared to RLD data at every time point, not just at a single endpoint, to ensure the release kinetics are genuinely matched throughout the dosing interval.
Long-Acting Injectables: The Q3 Frontier
Long-acting injectables represent the highest-margin, most technically defensible segment of the complex generics landscape. A single injection providing four weeks (risperidone microspheres), one month (paliperidone palmitate), three months (buprenorphine), or even six months of therapeutic coverage eliminates the patient adherence problem entirely. The clinical value is exceptional; the manufacturing complexity to replicate it is correspondingly high.
The two dominant technology platforms for LAIs are PLGA-based microsphere systems and prodrug-based crystalline nanosuspensions.
PLGA microsphere systems encapsulate the API within poly(lactic-co-glycolic acid) polymer microspheres typically 10 to 100 micrometers in diameter. On injection, the polymer degrades hydrolytically, releasing drug over weeks to months. The release profile is determined by the PLGA copolymer ratio (which controls the degradation rate), the molecular weight and molecular weight distribution of the polymer, the end-group chemistry (acid-terminated vs. ester-terminated, the latter degrading more slowly), the particle size distribution and morphology, the drug loading and distribution within the particles, and the presence of any excipients that modify degradation or hydration.
Deformulating a PLGA microsphere product requires the full analytical battery described earlier, but with several specialized additions. Gel permeation chromatography (GPC) or size exclusion chromatography (SEC) determines the PLGA molecular weight distribution and polydispersity index. NMR in deuterated chloroform or DMSO quantifies the lactide-to-glycolide ratio (e.g., 75:25 vs. 50:50) and the end-group composition. TGA quantifies residual solvent content. SEM of particle cross-sections (prepared by cryo-sectioning or ion-beam milling) reveals the internal drug distribution: is the drug uniformly distributed through the polymer matrix, or is it concentrated near the surface? The answer has major implications for the burst release profile (the initial rapid release in the first 24 hours after injection) and the patent claim analysis.
Prodrug-based crystalline nanosuspensions, exemplified by paliperidone palmitate (Invega Sustenna, Invega Trinza), involve an API modified as an ester prodrug that is essentially water-insoluble and can be milled to a nanosuspension of crystalline drug particles in an aqueous vehicle. After injection, the prodrug slowly dissolves from the particle surface and is converted to the active drug by plasma esterases. The release rate is governed by the particle size distribution (smaller particles dissolve faster), the polymorphic form of the prodrug crystal, and the concentration of stabilizing excipients that prevent particle growth. Dynamic Light Scattering (DLS) and nanoparticle tracking analysis (NTA) characterize particle size; XRPD identifies the polymorphic form of the prodrug crystal; rheology characterizes the injectability of the nanosuspension.
IP Valuation: Risperidone LAI (Risperdal Consta)
Janssen’s Risperdal Consta launched in 2003 at a price that generated peak annual U.S. sales exceeding $1.5 billion. The original compound patent on risperidone expired, but Janssen layered formulation patents covering the PLGA microsphere delivery system, the polymer composition, the particle size specification, and the manufacturing process that extended effective exclusivity. The first generic risperidone LAI, from Mylan (now Viatris), did not reach the U.S. market until 2020, nearly 17 years after Consta’s launch. The accumulative effect of the patent thicket on a single LAI product translated into billions of dollars in protected revenue. For a generic developer targeting the next-generation atypical antipsychotic LAIs (aripiprazole lauroxil, currently marketed as Aristada), the playbook is to map the patent portfolio, identify the thinnest formulation claims, and conduct deformulation to determine whether a design-around microparticle system is achievable within a commercially relevant timeline.
Transdermal Drug Delivery Systems: Layer-by-Layer Deconstruction
A transdermal patch is a multilayer laminate device, not a simple formulation. Characterizing it requires both pharmaceutical analytical skills and materials science capability. A typical drug-in-adhesive patch consists of a backing film (polyester, polyethylene, or polyurethane), a drug-containing pressure-sensitive adhesive layer (acrylate, silicone, or polyisobutylene-based), optionally a rate-controlling membrane (microporous or dense polymer film), and a release liner (siliconized polyester or polyethylene). Each layer must be separately characterized.
For the drug-in-adhesive layer, the critical questions are the identity and quantity of the adhesive polymer, the concentration and physical state of the API (dissolved vs. suspended as crystals vs. in a thermodynamic supersaturated state), the presence and identity of penetration enhancers (fatty acids, terpenes, propylene glycol, or oleyl alcohol), and the presence of any crystallization inhibitors. DSC detects crystalline drug as a melting endotherm; polarized light microscopy directly visualizes drug crystals in the adhesive. FTIR and Raman identify adhesive polymer type and penetration enhancer chemistry.
The most critical performance test for a transdermal patch is In Vitro Permeation Testing (IVPT), using Franz diffusion cells with human cadaver skin or, where validated, synthetic membrane substitutes. IVPT measures the cumulative amount of drug that crosses the skin barrier over a 24 to 48-hour period and provides the pharmacokinetic surrogate for in vivo permeation. The FDA’s product-specific guidances for several transdermal products explicitly require IVPT data in the ANDA submission. Matching the RLD’s IVPT profile is a direct Q3 requirement for the release membrane and adhesive layer design.
Adhesion testing is a regulatory requirement documented in FDA’s guidance ‘Assessing Adhesion with Transdermal and Topical Delivery Systems.’ Tack testing (probe tack, rolling ball tack), peel adhesion testing (90-degree or 180-degree peel at defined speeds), and shear testing (time to failure under constant load) collectively characterize the adhesive performance profile. These tests are not cosmetic; inadequate adhesion is a safety issue because a partially detached patch delivers unpredictable drug amounts.
Ophthalmic and Otic Formulations: The Biowaiver Opportunity
For sterile solutions intended for ocular or otic administration, the FDA’s guidance on demonstrating bioequivalence through Q1/Q2/Q3 sameness explicitly allows a waiver of in vivo bioequivalence studies when Q1/Q2 sameness is demonstrated and the physicochemical properties (pH, osmolality, viscosity, surface tension, preservative system, and buffer capacity) are matched. This biowaiver pathway reduces the development cost of these products by $1 million to $3 million compared to products requiring in vivo studies.
The deformulation challenge for ophthalmic solutions is primarily analytical precision at low concentrations. Many ophthalmic preservatives (benzalkonium chloride at 0.01% to 0.02%, polyhexamethylene biguanide at 0.001%), tonicity agents (sodium chloride, mannitol, glycerin), and viscosity enhancers (hydroxypropyl methylcellulose, carbomer, polyvinyl alcohol, hyaluronic acid) must be precisely quantified. Ion chromatography quantifies sodium, chloride, potassium, phosphate, and borate. HPLC with UV or CAD detection quantifies preservatives and surfactants. Viscometry or cone-and-plate rheology measures viscosity, and an osmometer measures tonicity. The combination of these physical measurements with the chemical quantification data constitutes the complete Q3 package for the biowaiver application.
Biosimilar Analytics: Large Molecule Characterization
Biologics are produced in living cells rather than synthesized via chemical reactions, which means the manufacturer cannot produce two batches with literally identical molecular populations. Every batch contains a distribution of molecular species, glycoforms, charge variants, and structural isoforms. The goal for a biosimilar developer is not to produce an identical copy but to produce a product that is ‘highly similar’ with no clinically meaningful differences in safety, purity, or potency. The FDA’s biosimilar approval framework, established under the Biologics Price Competition and Innovation Act (BPCIA) of 2009, is built entirely on this analytical comparability concept.
The analytical characterization of a biosimilar reference product is orders of magnitude more complex than any small-molecule deformulation program. A reference monoclonal antibody like adalimumab (Humira, whose composition patents have generated extensive biosimilar litigation) must be characterized for its primary amino acid sequence (confirmed by peptide mapping with LC-HRMS), its higher-order structure (secondary structure by circular dichroism or FTIR, tertiary structure by intrinsic fluorescence and hydrogen-deuterium exchange MS), its glycosylation pattern (N-glycan site occupancy and glycoform distribution by glycan analysis LC-MS), its charge variant profile (by cation exchange chromatography or capillary isoelectric focusing), its aggregation state (by size exclusion chromatography and dynamic light scattering), and its functional activity (by Fc receptor binding assays, complement activation assays, and cell-based potency assays).
The biosimilar developer must demonstrate that the totality of this evidence supports a conclusion that the proposed biosimilar is highly similar to the reference biologic. The analytical comparison must account for reference product lot-to-lot variability, which requires characterizing multiple RLD lots to define the natural range of variability before the biosimilar can be judged against it.
IP Valuation: Adalimumab (Humira) Biosimilar Market
Adalimumab holds the record as the world’s highest-selling drug for multiple consecutive years, with global peak sales exceeding $21 billion annually. AbbVie’s patent portfolio on Humira comprised over 100 patents in the U.S. alone, covering the drug substance, formulation, manufacturing processes, methods of treatment, and device (prefilled syringe and autoinjector). AbbVie licensed Humira biosimilars to launch in Europe in 2018 and in the U.S. in 2023 under settlement agreements that gave biosimilar developers their own periods of exclusivity in exchange for patent peace. By 2024, nine FDA-approved adalimumab biosimilars had entered the U.S. market. The combined analytical investment across all biosimilar programs for a single reference biologic can be estimated at $50 million to $200 million per developer, reflecting the extraordinary analytical complexity of the characterization program required for BPCIA regulatory approval.
Quality by Design: Turning Deformulation Data into a Bulletproof ANDA
QbD Principles in Generic Development
Quality by Design (QbD) is the FDA’s preferred development philosophy for both new drug applications and ANDAs. The agency’s Process Analytical Technology (PAT) initiative and its ICH Q8, Q9, and Q10 guidances collectively define QbD as a systematic approach to development that begins with predefined objectives and uses prior knowledge and scientific understanding to design the product and process. In generic development, the ‘predefined objective’ is explicit: replicate the RLD’s performance as defined by the Q1/Q2/Q3 analysis.
The deformulation blueprint feeds directly into the first formal QbD deliverable: the Quality Target Product Profile (QTPP). The QTPP is a prospective summary of the quality characteristics the generic product must achieve to be considered equivalent to the RLD. It includes the dosage form, route of administration, drug release mechanism, dosing strength, container-closure system, and all relevant CQA targets. Every target value in the QTPP can be traced directly to a measurement made during RLD characterization.
From RLD Characterization to Critical Quality Attributes
The RLD characterization data identifies which product attributes matter most for therapeutic equivalence. These become the Critical Quality Attributes (CQAs): the properties whose variation outside a defined range would compromise safety, efficacy, or quality. For a modified-release tablet, CQAs might include the dissolution rate at pH 6.8 (linked to in vivo drug absorption from the colon), the crystalline form of the API (linked to solubility and bioavailability), the D90 particle size of the API (linked to dissolution kinetics), and the weight uniformity of the tablet (linked to dosing accuracy). For a long-acting injectable, CQAs include the particle size distribution of the microspheres, the polymer molecular weight distribution, the drug loading, and the initial burst release.
Each CQA target is derived from the RLD characterization data. The range of acceptable values for each CQA is then established through designed experiments, typically using Design of Experiments (DoE) methodology, that systematically vary the formulation composition and manufacturing parameters to determine how each input variable affects each output CQA. The region of input variable combinations that consistently produces CQAs within their acceptable ranges constitutes the design space.
Manufacturing Process Design and Control Strategy
The design space concept is where QbD translates analytical data into manufacturing robustness. A well-defined design space means that any combination of formulation and process parameters within the space will produce a product that meets all CQAs. The FDA allows manufacturers to operate anywhere within their design space without triggering a regulatory filing; this flexibility is a commercial advantage because it enables process optimization, scale-up, and site transfer without the delays associated with ANDA supplement filings.
For complex generics, the manufacturing process itself is a critical variable that QbD must characterize. A PLGA microsphere manufacturer must understand how spray-dryer inlet temperature, feed rate, polymer concentration, and emulsification parameters each affect the particle size distribution, drug loading efficiency, and polymer morphology of the final microspheres. This process understanding cannot be assumed; it must be generated through experimental work that is informed by the deformulation analysis of the RLD. The deformulation data tells you what the target looks like; the QbD experimental work tells you how to build a process that reliably produces that target.
Key Takeaways: QbD and Deformulation Integration
Deformulation without QbD produces a recipe. QbD without deformulation data produces a process without a defined target. The combination produces a product that matches the RLD, can be consistently manufactured at commercial scale, and can withstand regulatory scrutiny. The QTPP derived from RLD characterization is the architectural blueprint. The CQAs identified from Q3 analysis are the load-bearing specifications. The design space developed through DoE is the engineering tolerance that ensures every batch meets those specifications. Companies that execute this integrated approach consistently have shorter ANDA review cycles, fewer Complete Response Letters, and higher commercial batch success rates.
The Intelligence Feedback Loop: Patent Data, Lab Data, Legal Strategy
Competitive Intelligence as the Development Trigger
Generic product selection is a competitive decision before it is a scientific decision. The probability of winning first-to-file status, the risk profile of the PIV litigation, the likely settlement terms, and the eventual commoditization timeline all depend on competitive intelligence gathered before a single milligram of RLD is purchased.
The ideal intelligence stack for a generic product selection decision includes: complete patent term analysis from the Orange Book and supplementary patent searches (branded drugs sometimes have relevant formulation or method patents that are not Orange Book-listed), litigation tracking data showing all prior PIV challenges and their outcomes for the target drug, competitive ANDA pipeline information from the FDA’s Paragraph IV Drug Product List (which discloses all approved first-to-file applications and all applications currently under 30-month stay), market revenue data for the brand product and any existing generic competition, and regulatory complexity signals from FDA product-specific guidances and previous ANDA Complete Response Letters.
Platforms like DrugPatentWatch integrate patent expiration data, Orange Book listings, litigation history, and ANDA approval status into a single searchable interface. The competitive intelligence workflow starts with screening that platform for drugs with approaching patent cliffs, dense PIV challenge activity (indicating competitive interest but also high litigation risk), and revenue profiles that justify the development investment.
The Go/No-Go Decision Framework
The go/no-go decision for a complex generic product should be structured as a sequential filter with explicit criteria at each stage. The first filter is market attractiveness: does the brand product generate enough revenue, and is the patent cliff close enough, that a 180-day exclusivity prize would be commercially meaningful? A drug with $50 million in U.S. annual sales generates a very different 180-day prize than one with $500 million. The second filter is IP feasibility: given the patent portfolio structure, is a PIV challenge viable within the target filing timeline, or would the 30-month stay arithmetic delay approval until after the compound patent expires anyway? The third filter is technical feasibility: given what is known about the dosage form complexity, does the company have the analytical capabilities and formulation expertise to execute the deformulation and development program in the required time?
Only products that pass all three filters warrant the full investment in deformulation. Products that pass market attractiveness but fail IP feasibility might be worth developing as post-patent-expiry generic entrants without a PIV challenge, accepting a later launch in exchange for reduced litigation risk.
Lab Data as Legal Evidence
The analytical data generated during deformulation is dual-purpose. It guides formulation development, and it constitutes the technical evidence for the PIV challenge. When the legal team files a PIV certification asserting non-infringement of a formulation patent, the assertion must be backed by the analytical characterization of the generic product showing that it does not contain the specifically claimed combination of ingredients, the specifically claimed particle size, or the specifically claimed structural feature that defines the brand’s patent.
Conversely, when the PIV challenge asserts patent invalidity, the analytical data can be the evidence of prior art or the basis for a written description argument. If the innovator’s patent claims a ‘sustained-release composition wherein the rate-controlling polymer constitutes 20% to 40% by weight of the formulation’ but the deformulation analysis of the actual commercial RLD shows the polymer at 18%, the generic company’s patent attorneys have a documented argument that the commercial product itself does not practice the patent claims, which bears on the patent’s validity and scope.
The quality, precision, and documentation discipline of the deformulation analytical work directly determines the strength of these legal arguments. A deformulation report prepared under GLP conditions, with traceable methods, certified reference standards, and documented chain of custody for the RLD samples, carries substantially more weight in litigation than informal development data. Companies that treat their deformulation reports as legal documents from inception are better positioned in Paragraph IV litigation.
Technology Roadmap: Where Complex Generics Are Heading
2025 to 2028: The LAI and Transdermal Buildout
The near-term pipeline of patent cliffs in complex generics is well-populated with LAI and transdermal products. Buprenorphine monthly injection (Brixelle, CAM2038), aripiprazole lauroxil (Aristada, Aristada Initio), and paliperidone palmitate 6-month formulation (Invega Hafyera) all represent multi-hundred-million-dollar annual revenue products with patent portfolios that become challengeable in the 2025 to 2028 window. Each requires the full suite of LAI analytical capabilities described above: PLGA molecular weight analysis, particle size characterization, drug loading quantification, and in vitro release method development.
Transdermal systems entering the challenge window include several fentanyl patch formulations where remaining formulation patents are narrow and potentially vulnerable, rivastigmine transdermal (Exelon Patch) follow-on systems, and newer products like blonanserin transdermal. The analytical playbook for each is patch deconstruction, IVPT characterization, and adhesion profiling.
2028 to 2032: Inhalation and Nasal Systems
The inhaled and intranasal complex generic space is the next major frontier after LAIs. Fluticasone propionate/salmeterol (Advair Diskus), budesonide/formoterol (Symbicort), and indacaterol/glycopyrronium (Ultibro Breezhaler) represent combined annual revenues exceeding $10 billion globally. Generic versions of these products require characterization of drug particle size in the aerosol, emitted dose uniformity, device aerodynamic performance, and formulation properties for the specific inhaled system. The FDA’s guidance for orally inhaled and nasal drug products (OINDPs) makes demonstrating bioequivalence for these products exceptionally complex; companies that invest in the particle engineering and aerosol characterization capabilities now will be positioned to file first-to-file ANDAs in this window.
The Automation and AI Layer
The analytical workflows described throughout this document are already being partially automated. Robotic sample preparation systems reduce analyst error and throughput time for serial dissolution testing and chromatographic sample preparation. High-throughput XRPD screening platforms can analyze dozens of polymorph samples per day. Automated dissolution testing systems with inline UV fiber optic probes eliminate the manual sample collection that traditionally made dissolution testing a bottleneck.
Artificial intelligence and machine learning are entering the deformulation workflow in two ways. Predictive formulation models, trained on databases of pharmaceutical excipient properties and their effects on drug release, can suggest candidate formulations for a target release profile before any physical batches are made. These models compress the initial design space exploration from bench experiments to computational screening. The second application is automated spectral interpretation: ML models trained on reference FTIR and Raman spectra can identify excipients in a complex mixture faster and more consistently than manual spectral matching, reducing the time required for the Q1 identification phase of deformulation from days to hours.
The legal application of ML to patent analytics is equally compelling. Models trained on the full text of issued patents and their litigation outcomes can predict the probability that a given patent will be found invalid or not infringed in Paragraph IV litigation, providing the business development team with a quantitative risk score for each patent in a target drug’s portfolio. DrugPatentWatch’s structured patent and litigation database is the type of data infrastructure that feeds these predictive models.
Investment Strategy for Analysts and Portfolio Managers
Framework for Evaluating Complex Generic Companies
An institutional investor evaluating generic pharmaceutical companies should assess the following five dimensions, in order of strategic importance.
The first is the complexity mix of the pipeline. A company with 80% of its late-stage pipeline in complex generics (LAIs, transdermals, inhalation, complex oral) has a structurally different earnings outlook from one with 80% in standard oral solids. Complexity mix is the single most predictive indicator of future margin sustainability, because complex products take longer to commoditize and typically enter markets with fewer competitors.
The second is the analytical infrastructure depth. Companies with validated in-house capabilities in XRPD, solid-state NMR, Raman imaging, rheology, IVPT, and in vitro aerosol testing have a durable competitive advantage in identifying and executing complex generic opportunities faster than competitors who outsource this work. Analytical infrastructure is expensive to build and slow to replicate; it is a genuine moat. Look for capital expenditure patterns, patent filings on analytical methods, and scientific publication track records as proxy indicators of this capability depth.
The third is the first-to-file rate in PIV challenges. A company that consistently files first-to-file PIV challenges on large-revenue drugs is one that has mastered the intelligence-to-lab-to-legal pipeline described in this document. First-to-file rate is directly measurable from the FDA’s Paragraph IV Drug Product List. Companies with high first-to-file rates on large-revenue drugs are likely to capture disproportionate profits during 180-day exclusivity windows.
The fourth is ANDA approval cycle time and complete response letter rate. Shorter approval cycles and lower CRL rates indicate a company whose ANDA submissions are well-prepared, analytically rigorous, and bioequivalence studies are executed correctly the first time. CRL rates are disclosable events for public companies, and patterns across multiple ANDAs reveal the quality of the underlying development process.
The fifth is the patent litigation win rate. A company with a track record of winning or favorably settling Paragraph IV litigation is demonstrating that its technical and legal teams are genuinely integrated, that its deformulation data is of sufficient quality to support strong legal positions, and that it can execute on the high-risk/high-reward first-to-file strategy effectively.
Valuation Considerations: 180-Day Exclusivity as an NPV Event
The financial modeling of a first-to-file generic launch should treat the 180-day exclusivity period as a discrete, high-probability-adjusted net present value event rather than blending it into a generic market share projection. The standard approach is to model the 180-day window as a separate cash flow stream assuming a pricing premium of 20% to 30% relative to eventual steady-state generic pricing, a market share capture rate of 40% to 60% of the brand’s prescriptions, and a risk-adjustment reflecting the probability of winning litigation or reaching a favorable settlement before the launch date.
For a drug with $500 million in annual U.S. brand revenue, a first-to-file generic with 50% market share during 180-day exclusivity at a price 25% below brand generates roughly $60 million to $80 million in contribution over the exclusivity period. After deducting the development cost (typically $5 million to $25 million for a complex generic) and the litigation cost, the net value is still substantially positive for most large-revenue drugs. The key variable is timing: each year of delay in filing reduces the NPV by the annual carrying cost of the development investment plus the opportunity cost of the delayed revenue. This is precisely why analytical speed in deformulation is financially quantifiable, and why the senior management of any serious generic company should view its analytical science function as a revenue accelerator.
Key Takeaways: Investment Strategy
Companies with deep complex generic pipelines, proprietary analytical infrastructure, and demonstrated first-to-file rates in PIV challenges are the most defensible long-term positions in the generic sector. IP valuation of target drugs, specifically the layered patent portfolio analysis described earlier, is the correct framework for assessing near-term pipeline risk and competitive positioning. The LAI and transdermal segments represent the highest near-term complex generic opportunity, with biosimilars representing the highest-value long-term opportunity for companies willing to build the biological characterization infrastructure. The 180-day exclusivity cash flow model should be a standard analytical tool for any institutional investor with exposure to generic pharmaceutical equities.
FAQ: Operational Questions from the Field
Q1. What is the single biggest mindset shift required when moving from simple oral solid development to long-acting injectable development?
The shift is from composition-centric thinking to process-centric thinking. For an immediate-release tablet, if you correctly identify all ingredients and replicate their quantities, the product generally performs as expected because the manufacturing process for a straightforward direct-compression tablet has limited ability to alter the API’s release behavior. For a PLGA microsphere LAI, the manufacturing process does not merely assemble the ingredients; it creates the product. The spray-drying conditions, solvent evaporation rate, emulsification parameters, and annealing conditions each directly determine the particle size distribution, the polymer morphology, and the drug distribution within the particles, which in turn determine the release profile over weeks or months. Replicating the RLD’s Q1/Q2 composition but using a different manufacturing process will produce Q3-different microspheres. The analytical question shifts from ‘What does the product contain?’ to ‘What does the product’s structure look like, and what manufacturing process is consistent with producing that structure?’
Q2. How should a generic company make the capital expenditure case to leadership for building in-house Raman imaging capability versus continuing to outsource?
Frame it as a risk-adjusted cost comparison on a per-product basis. A Raman mapping instrument (confocal Raman microscope with imaging software) costs approximately $300,000 to $600,000. A single complex modified-release product development program that requires multiple rounds of outsourced Raman imaging studies at a CRO costs $50,000 to $150,000 per analytical campaign. Across four to six complex generic programs per year, the outsourcing cost equals or exceeds the instrument cost within 12 to 24 months. The qualitative argument, that in-house capability allows iterative, rapid experimental feedback rather than waiting two to four weeks for outsourced results, is equally important: each iteration cycle saved is worth one to two months of development time, which translates directly into earlier filing and a higher probability of first-to-file status.
Q3. How do we structure the relationship between our R&D and legal teams for Paragraph IV challenges?
Create a formal cross-functional Product Strategy Team with defined membership from R&D, regulatory affairs, IP/legal, and business development. This team should hold a joint patent review at the outset of every PIV product selection, where patent attorneys explain the specific claims of each formulation patent and R&D leads assess the analytical feasibility of characterizing the corresponding feature. This meeting forces explicit conversation about which claims are potentially most vulnerable to invalidity arguments (prior art, lack of written description, obviousness) and which claims require a design-around formulation approach. The output is a shared development brief that aligns the R&D analytical program with the specific legal arguments the PIV certification will assert. Without this alignment, R&D teams frequently generate data that is thorough but not legally targeted, and legal teams make arguments that are not fully supported by the available analytical evidence.
Q4. What is the most common and costly avoidable mistake in deformulation programs?
Insufficient RLD procurement and characterization at the start of the program. Teams under schedule pressure often cut this phase short, acquiring a single RLD lot and conducting a limited initial characterization before beginning formulation development. The consequence is that the development team discovers a critical Q3 attribute, a specific polymorphic form, a bimodal particle size distribution in the API, or a specific excipient grade that requires a sourced material not in the standard supply chain, only after multiple failed bioequivalence studies. A comprehensive initial RLD characterization phase, including multiple lots and the full analytical battery described in this document, requires two to three months and costs $200,000 to $500,000. It routinely prevents six to twelve months of failed development iterations that cost ten times that amount.
Q5. How does the biosimilar development framework affect strategy for a company currently focused on complex small-molecule generics?
The biosimilar regulatory framework represents the highest analytical standards currently in effect for any category of pharmaceutical product. The totality-of-evidence approach, the requirement for comprehensive structural characterization, the expectation that analytical similarity data will support extrapolation of clinical data, and the rigorous comparative analytical studies required by the BPCIA are raising the bar for what FDA expects from complex product developers across the board. FDA’s increasing sophistication in reviewing Q3 data for complex small-molecule generics, particularly for LAIs and nasal inhalation products, reflects this trend. Companies that invest in the analytical capabilities needed for today’s complex small-molecule generics, particularly mass spectrometry platforms, advanced physical characterization, and biofunctional testing systems, are simultaneously building toward the analytical infrastructure required to enter biosimilars. The two pipelines are not as technically distant as they might appear.
About DrugPatentWatch
DrugPatentWatch provides fully integrated pharmaceutical intelligence combining patent expiration data, Orange Book listings, Paragraph IV litigation history, ANDA approval timelines, market revenue data, and exclusivity tracking across the full U.S. generic drug landscape. The platform is used by IP teams, portfolio managers, business development leads, and institutional investors to identify generic drug opportunities, map patent fortress structures, track competitor ANDA activity, and build data-driven product selection strategies.
For a detailed analysis of any drug’s patent portfolio, Paragraph IV history, and generic pipeline status, visit DrugPatentWatch.com.
This analysis draws on public FDA data, Orange Book listings, published Paragraph IV litigation records, peer-reviewed literature on pharmaceutical analytical methods, and publicly disclosed company financials. It does not constitute legal or investment advice.