The premise sounds straightforward enough: a blockbuster biologic loses patent protection, a competitor copies it at lower cost, patients save money. That is how generics work. Biologics do not work that way, and neither does the $36 billion biosimilar industry that has grown up around them.
Getting a biosimilar to market requires reverse-engineering a 140,000-Dalton protein made inside a living cell, satisfying regulators on three continents, surviving a legally mandated patent disclosure process that hands your trade secrets to the company you are trying to compete with, and then convincing a Pharmacy Benefit Manager (PBM) to put your product on formulary even when keeping the originator is more profitable for them. Do all of that correctly and you might capture meaningful market share. Fail at any one stage and you have written off $100 to $300 million and five to nine years of development time.
This guide covers each of those stages in full technical depth: manufacturing science, global regulatory pathways (FDA, EMA, and beyond), the BPCIA patent dance and patent thicket economics, commercial access dynamics including the PBM rebate wall, and the technology and policy shifts reshaping the decade ahead. It is written for IP teams, portfolio managers, R&D leads, and institutional investors who need to understand not just what the challenges are, but what the specific failure modes look like and how leading developers are engineering around them.
Part I: The Science — Why ‘The Process Is the Product’ Changes Everything
What Makes a Biologic Fundamentally Different From a Small Molecule
The distinction between a conventional generic drug and a biosimilar is not regulatory nuance. It is molecular reality. Aspirin has a molecular weight of 180 Daltons and 21 atoms. Its structure is fixed, reproducible, and fully characterizable by standard analytical chemistry. Infliximab (Remicade) has a molecular weight of approximately 149,000 Daltons, contains over 18,000 atoms, and is folded into a three-dimensional quaternary structure that is produced by, and depends on, the behavior of a living Chinese Hamster Ovary (CHO) cell line under tightly controlled culture conditions. Change the cell line, the pH, the dissolved oxygen set-point, or the nutrient feed strategy, and the molecule that comes out the other end is measurably different — not a copy of the original, but a close relative.
This is why the FDA’s statutory definition of a biosimilar is ‘highly similar’ rather than ‘identical.’ Identity is not chemically achievable. The regulatory and scientific challenge is to demonstrate that any differences between the biosimilar and its reference product are analytically detectable but clinically inactive — that they fall within the range of batch-to-batch variation the originator itself produces.
Molecular Complexity: Post-Translational Modifications and the Glycosylation Problem
Every monoclonal antibody and most therapeutic proteins carry post-translational modifications (PTMs) that are added by the host cell after the primary amino acid chain is assembled. The most commercially consequential of these is N-linked glycosylation: the attachment of branched sugar chains at specific asparagine residues on the Fc region of IgG antibodies.
Glycosylation patterns are not encoded in DNA. They emerge from the interaction between the protein sequence and the enzymatic machinery of the cell, and that machinery responds to culture conditions. Core fucosylation levels on the Fc region directly modulate antibody-dependent cellular cytotoxicity (ADCC) activity. High-mannose glycoforms affect serum half-life through mannose receptor-mediated clearance. Terminal sialylation affects immunogenicity risk. A biosimilar developer who produces a molecule with a fucosylation profile shifted even slightly from the reference product must demonstrate through biological assays — not just structural data — that this shift does not translate into a functional difference detectable in a clinical setting.
The glycosylation challenge is compounded by the fact that the reference product itself is not a single glycoform. Every batch of Humira, Herceptin, or Enbrel contains a heterogeneous mixture of glycoforms within a defined specification range. The biosimilar developer must characterize this heterogeneity across multiple commercially sourced reference lots — including lots from different markets, since the European and U.S. versions of the same biologic are sometimes manufactured differently — before they can define their own quality target product profile (QTPP). This multi-lot characterization exercise, often consuming 30 or more reference product batches, is expensive and time-consuming before a single cell line has been chosen.
Beyond glycosylation, PTMs include oxidation of methionine residues (which can reduce potency and increase immunogenicity), deamidation of asparagine and glutamine (which can alter charge heterogeneity and stability), C-terminal lysine clipping (which affects charge variants), and disulfide bond formation (which governs tertiary structure). Each of these must be profiled and compared head-to-head using orthogonal analytical methods.
Cell Line Development: Screening Hundreds to Find One
Because the originator’s cell line and upstream process are protected as trade secrets rather than by patents — they are typically never published — the biosimilar developer starts from a blank slate. The first task is generating a new proprietary cell line capable of producing a protein with the right analytical fingerprint.
The standard approach uses CHO cells transfected with the target gene, followed by single-cell cloning and a screening cascade. Starting from thousands of individual clones, developers apply multiple rounds of selection — first for productivity (titer in shake flask), then for product quality (glycosylation profile, charge heterogeneity, aggregation propensity), then for genetic stability over extended culture periods. Reaching a single lead clone suitable for IND-enabling studies typically takes 12 to 18 months and costs $5 to $15 million before any bioreactor development begins.
The productivity-quality trade-off is a real constraint. High-expressing clones frequently produce protein with a different glycosylation profile than lower-expressing clones, because the glycosylation machinery of the cell becomes saturated at high specific productivity rates. A developer optimizing purely for titer can inadvertently select a clone whose product quality attributes diverge from the reference product in ways that require substantial reformulation work downstream.
Scale-Up and the Manufacturing Consistency Imperative
Once a lead cell line is selected and a process is developed at laboratory scale (1 to 10 liters), the developer must demonstrate that the process is scalable — that a 2,000-liter or 15,000-liter commercial bioreactor will produce protein with the same critical quality attributes (CQAs) as the bench-scale runs used for analytical similarity comparisons.
Scale-up failure is common and poorly publicized. Changes in bioreactor geometry alter the shear stress environment that cells experience. Larger vessels have different mixing times, meaning nutrients and pH-correcting agents are distributed less uniformly. Dissolved CO2 accumulates differently at scale, affecting intracellular pH and glycosylation enzyme activity. Each of these variables can shift CQAs. A developer who achieves a beautiful glycan profile at 10 liters may find their fucosylation or galactosylation pattern drifts when they transfer to a 2,000-liter GMP bioreactor.
Process Analytical Technology (PAT) — the deployment of real-time in-process sensors for parameters like dissolved oxygen, pH, metabolite concentrations, and cell viability — is now considered best practice for managing this scale-up risk. By building a detailed mechanistic model of how CQAs respond to process parameters (a ‘design space’ in ICH Q10 terminology), developers can use PAT data to make real-time adjustments that hold the product within its target quality range, giving regulators confidence that consistency is engineered into the process rather than hoped for.
The FDA’s Process Validation Guidance (2011) and the EMA’s equivalent guidelines require manufacturers to demonstrate consistency across at least three consecutive commercial-scale validation batches. For a biosimilar, each of these batches must meet both internal CQA specifications and the analytical similarity criteria established for comparison to the reference product.
Analytical Similarity: Building the ‘Totality of the Evidence’ Foundation
The analytical similarity package is the foundation of a biosimilar regulatory dossier. It is where biosimilarity is first established and where the argument for reduced clinical requirements is anchored. The FDA’s tiered approach, outlined in its 2015 guidance on statistical approaches to analytical similarity, places CQAs into three tiers based on their clinical relevance and risk to patients.
Tier 1 attributes — those with the highest clinical impact, typically biological activity assays and binding assays for the drug’s primary mechanism of action — require a formal equivalence testing framework using prespecified acceptance criteria. The biosimilar must demonstrate that its mean attribute value is within 1.5 standard deviations of the reference product’s mean, with a 90% confidence interval that falls entirely within that margin. This is a strict standard. Failing Tier 1 is effectively a program-stopping event.
Tier 2 attributes use a quality range approach: the biosimilar’s values must fall within the range observed across reference product lots. Tier 3 attributes require only a fingerprint analysis with a qualitative discussion of any differences. A typical biosimilar submission contains data for 40 to 60 individual attributes across these tiers, generated using techniques including size exclusion chromatography (SEC), ion exchange chromatography (IEX), capillary electrophoresis (CE-SDS), peptide mapping with liquid chromatography-mass spectrometry (LC-MS), surface plasmon resonance (SPR) for binding kinetics, cell-based potency assays, and Fc receptor binding assays.
The sophistication of this characterization package is one area where the biosimilar industry has clearly advanced beyond what was required for the original innovator approvals. Many reference products approved in the 1990s and early 2000s were approved with analytical packages that by today’s standards look thin. A biosimilar developer today often knows more about the molecular heterogeneity of Humira or Herceptin than AbbVie or Roche’s own regulatory teams documented at the time of approval.
Immunogenicity Assessment: The Risk That Cannot Be Fully Characterized Pre-Clinically
Immunogenicity — the generation of anti-drug antibodies (ADAs) against a biologic — is the primary safety risk specific to protein therapeutics. ADAs can reduce efficacy by binding and clearing the drug faster than it can act. They can cause hypersensitivity reactions. In rare cases they cause neutralization of endogenous proteins, as occurred with pure red cell aplasia in patients receiving certain epoetin formulations.
For biosimilar developers, the immunogenicity challenge is twofold. First, they must demonstrate that their product is no more immunogenic than the reference product, a comparison that is confounded by the fact that many reference products were approved using older, less sensitive ADA assay technologies. A bridging study comparing ADA incidence between a biosimilar and its reference using modern electrochemiluminescence (ECL)-based assays will detect ADAs that older ELISA assays would have missed, potentially creating a misleading appearance of higher immunogenicity for the biosimilar simply because the assay is more sensitive.
Second, animal models for immunogenicity prediction are unreliable. Human proteins are fully tolerated by most animal immune systems because the proteins are identical or nearly identical to the animal’s endogenous equivalent. The only reliable immunogenicity data comes from human studies, meaning this risk cannot be fully characterized until the Phase I or Phase III clinical program.
Key manufacturing-related drivers of immunogenicity include protein aggregates (particularly soluble oligomers in the 100 nm to 10 micron size range), host cell protein (HCP) impurities from the CHO cell line, and the formulation excipient profile. A developer who achieves a clean analytical similarity package but has a higher HCP impurity level than the reference product — perhaps due to differences in their purification platform — may face higher ADA rates in clinical studies even if the protein itself is identical at the amino acid level. The HCP profile is increasingly treated as a critical quality attribute in its own right, requiring deep characterization by 2D mass spectrometry rather than reliance on generic ELISA-based HCP assays.
Key Takeaways: Manufacturing and Science
A biosimilar development program is structurally front-loaded. The decisions made in the first 18 months — cell line selection, process design, glycosylation targeting — cascade through every subsequent stage. A cell line that produces a molecule with a high-mannose glycan enrichment, for example, may clear faster from the bloodstream than the reference product, creating a pharmacokinetic difference that regulatory reviewers will flag and that must be resolved either through process change (expensive, time-consuming) or clinical justification (even more expensive). Front-loading investment in world-class analytical science, PAT infrastructure, and multi-lot reference product characterization is the highest-return risk mitigation available at the program initiation stage. Developers who cut corners here typically pay multiples of the savings later in clinical programs or regulatory review.
Part II: IP Valuation of Reference Biologics — What Biosimilar Developers Are Actually Competing Against
Before assessing the regulatory pathway, IP teams need to understand the IP asset structure of the reference product they are targeting. A biologic’s patent estate is a core financial asset, capitalized on the originator’s balance sheet and managed as deliberately as any manufacturing asset. Miscalculating the strength or breadth of that estate is one of the most common and expensive errors biosimilar programs make.
How Biologic Patent Estates Are Structured: The Four-Layer Architecture
Originator companies build biologic patent protection in layers, and each layer has a distinct commercial function.
The first layer is the composition-of-matter patent on the molecule itself — the amino acid sequence, the CDR regions for an antibody, or the specific protein structure for a fusion protein. These are the highest-value patents and typically expire 20 years from the filing date, though patent term extension (PTE) under the Hatch-Waxman framework can add up to five additional years to compensate for regulatory review time. The molecule patent is what biosimilar developers watch most closely when assessing market entry timing.
The second layer covers manufacturing process patents: the specific cell line (though cell lines themselves are not patentable, methods of using them are), fermentation conditions, purification sequences, and formulation composition. These patents are filed after initial development work and often post-approval. They are generally weaker than composition-of-matter patents because the inventive step is harder to establish for process improvements, but they are cheaper to litigate around through design-around strategies.
The third layer consists of formulation and device patents: citrate-free formulations (as AbbVie developed for adalimumab to reduce injection-site pain), high-concentration subcutaneous formulations, pre-filled syringe designs, and autoinjector mechanisms. These patents have significant commercial value because they protect the product form that patients actually use and that payers sometimes specify in formulary contracts. A biosimilar that matches the molecule but cannot access the device platform may face formulary exclusion in markets where the device is bundled with the drug benefit.
The fourth layer is indication-specific and method-of-treatment patents covering specific dosing regimens, patient populations, or combination therapy protocols. These are the hardest patents for biosimilar developers to avoid because using the approved product in its approved indications can constitute infringement even when the compound itself is off-patent.
Case Study: AbbVie’s Humira (Adalimumab) IP Estate and the $7-Year Extension
Humira is the most extensively documented example of strategic patent portfolio construction in the biopharmaceutical industry. The adalimumab molecule patent expired in the U.S. in December 2016. AbbVie held patent exclusivity until January 2023 — a 7-year extension achieved entirely through the patent thicket. The core numbers are stark: 247 patent applications filed, more than 130 granted U.S. patents, and approximately 89% of those applications filed after Humira’s initial FDA approval. The I-MAK analysis of the Humira estate found that AbbVie’s average patent filing occurred 13 years after the original molecule patent was filed, creating a layered exclusivity structure that extended market protection well into the 2030s for some patents.
The financial impact of this structure is quantifiable. In Europe, where biosimilars launched in 2018 following patent expiration (European patent law does not permit the same thicket construction as U.S. law), prices fell 40 to 80% within two years. In the U.S., Humira retained more than 96% market share through 2023 despite multiple FDA-approved biosimilars existing from 2016 onward. The delta between European and U.S. pricing represents billions of dollars annually transferred from U.S. health plans and patients to AbbVie’s earnings — a direct financial consequence of patent thicket strategy.
For biosimilar developers assessing the adalimumab opportunity in retrospect, the correct analytical framework was not ‘when does the molecule patent expire?’ but ‘what is the litigation settlement leverage of AbbVie given its 130-patent portfolio, and what licensed entry date can we negotiate?’ Every adalimumab biosimilar that launched in the U.S. did so under a negotiated license from AbbVie, not through successful patent invalidation.
Valuing a Biologic’s IP Estate for Competitive Intelligence
For portfolio managers and IP teams, the practical question is how to value a reference biologic’s patent estate as a barrier to entry. Several analytical frameworks apply.
The litigation-adjusted NPV model discounts a projected market entry date by the probability-weighted outcomes of patent challenge scenarios. A patent thicket of 50 patents with an average challenge success rate of 30% at the PTAB represents a very different risk profile than a thicket of 10 patents with a 60% challenge success rate. The expected value of market entry is a function of the number of blocking patents, their individual vulnerability scores (based on claim breadth, prior art density, and prosecution history estoppel), and the time cost of each challenge pathway.
The freedom-to-operate (FTO) landscape analysis, updated continuously using platforms like DrugPatentWatch, maps every active patent against the biosimilar developer’s intended product and process. A robust FTO report does not just identify blocking patents — it identifies design-around opportunities. A formulation patent covering a citrate buffer can sometimes be designed around by using a histidine buffer system. A device patent covering a specific autoinjector mechanism can be designed around by developing an alternative delivery system. These design-around investments, typically $5 to $20 million depending on complexity, are often far cheaper than PTAB challenges or litigation.
The settlement option value analysis recognizes that for highly complex patent estates like Humira’s, the expected outcome is not litigation victory but a negotiated license with a defined entry date. The value of a biosimilar program under this model is the NPV of revenues starting from the licensed entry date, discounted by the probability that the license negotiation succeeds and by the royalty rate the originator will demand. Companies entering a crowded thicket late — after two or three other biosimilar developers have already negotiated licenses — typically face more favorable terms because the originator’s negotiating leverage declines as it grants more licenses.
Investment Strategy: Targeting the Patent Cliff
For institutional investors, the biologic patent cliff represents one of the most analyzable value creation events in healthcare. Unlike clinical trial binary events, patent expiration dates are public information, and the period of market exclusivity erosion is predictable within a 12 to 36-month window (adjusted for litigation outcomes).
The strategically attractive targets for new biosimilar investment share several characteristics: they have molecule patents expiring within 3 to 5 years, relatively thin formulation and device patent layers, regulatory precedent from a first-wave biosimilar that has already run the analytical similarity gauntlet, and commercial markets large enough to support at least two or three profitable biosimilar entrants. Keytruda (pembrolizumab, $25 billion in 2023 global sales) has its core patent expiring in 2028 in the U.S. and will face a wave of biosimilar development. Stelara (ustekinumab, approximately $10 billion in peak sales) has already seen its first biosimilar approvals. Entyvio (vedolizumab) and Dupixent (dupilumab) are on similar trajectories for the early 2030s.
The caution flag for investors is that nominal patent expiration is not market entry. The Humira case set a precedent for litigation-based delay that originator companies will attempt to replicate. Investors should build patent litigation timeline analysis into their biosimilar investment models, treating the originator’s stated ‘negotiating posture’ — whether they have filed preemptive suits, how many PTAB petitions have been filed against their secondary patents, how many biosimilar developers have signed licensing agreements — as leading indicators of market entry probability.
Part III: The Global Regulatory Architecture — Totality of Evidence, Interchangeability, and the Harmonization Gap
The ‘Totality of the Evidence’ Standard: How the Evidentiary Pyramid Works in Practice
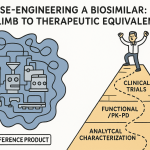
The totality of evidence framework, shared by the FDA, EMA, Health Canada, and most stringent regulatory authorities, is structured as a hierarchical evidence package where each layer resolves residual uncertainty left by the layer below it. The framework’s practical effect is to front-load the evidentiary burden onto analytical and PK/PD studies, which are far cheaper than Phase III trials.
At the base of the pyramid, analytical similarity data must demonstrate that the biosimilar and reference product are indistinguishable at the molecular level for clinically relevant attributes. If this base is solid — meaning all Tier 1 attributes pass equivalence testing and no Tier 2 attributes fall outside the reference product’s quality range — the developer needs only a relatively small PK/PD comparability study to move up the pyramid. The confirmatory clinical efficacy trial, if required at all, is designed around a pre-agreed clinical endpoint margin that presupposes analytical similarity has already been established.
The corollary of this structure is that a developer who arrives at Phase I with a weak analytical package — perhaps because they compressed the characterization timeline to hit a filing deadline — will face a much heavier clinical burden. FDA reviewers who see unexplained differences in Tier 1 functional assays will demand clinical data to resolve that uncertainty, at a cost that can add $50 to $100 million to the development program.
The extrapolation principle compounds this dynamic. A developer who can demonstrate biosimilarity in one sensitive patient population may receive approval for all indications of the reference product without running indication-specific trials. Rituximab biosimilars, for example, have been approved for both oncology (diffuse large B-cell lymphoma) and immunology (rheumatoid arthritis) indications based on PK/PD data primarily collected in RA patients, with a scientific justification that the mechanism of action is the same across indications. The extrapolation argument, however, requires a clean analytical package. If the biosimilar shows meaningful differences in Fc receptor binding, the regulator may require oncology-specific data because ADCC — Fc-dependent — is more important in the oncology mechanism of action than in RA.
The EMA Framework: 20 Years of Regulatory Precedent
The EMA approved its first biosimilar, Omnitrope (somatropin), in 2006. Its current framework has been refined through four generations of product-specific guidelines covering growth hormones, epoetins, granulocyte colony-stimulating factors (G-CSFs), monoclonal antibodies, recombinant FSH, and insulin. As of early 2026, the EMA has recommended approval for more than 100 biosimilar products.
The EMA’s Biosimilar Medicines Working Party (BMWP), within the Committee for Medicinal Products for Human Use (CHMP), has consistently pushed for reduced clinical data requirements as analytical methods have improved. The EMA now accepts biosimilar MAA submissions for monoclonal antibodies without confirmatory clinical efficacy data when the analytical and PK/PD package is strong, a position that the FDA has been slower to adopt formally.
The centralized procedure through the EMA grants marketing authorization across all EU member states simultaneously, which is a significant efficiency advantage over bilateral national approvals. A single CHMP assessment, lasting approximately 210 active review days, results in a Day 1 approval valid in all 27 member states plus Norway, Iceland, and Liechtenstein. Post-approval labeling harmonization through the EMA also simplifies pharmacovigilance obligations compared to managing country-specific variation files.
The EMA’s position on interchangeability is clear in principle and complex in practice. The CHMP and Heads of Medicines Agencies (HMA) issued a joint statement in 2022 confirming that all EMA-approved biosimilars are considered interchangeable with their reference product from a scientific standpoint. Substitution decisions at the pharmacy level, however, remain with national competent authorities. France, Germany, Italy, and most Nordic countries have implemented policies permitting non-medical switching from reference biologic to biosimilar, and in some cases mandating it for new patients. The variation between national substitution policies creates market access complexity for commercial teams, even within the ‘harmonized’ European regulatory framework.
The FDA Pathway Under the BPCIA: Key Features and Evolving Requirements
The Biologics Price Competition and Innovation Act, enacted in 2010 as part of the Affordable Care Act, created the 351(k) pathway for biosimilar applications and the separate pathway for interchangeable biosimilar designation. The FDA approved its first biosimilar, Zarxio (filgrastim-sndz, Sandoz), in March 2015.
The FDA’s reviewdivision responsible for biosimilar applications is the Office of Therapeutic Biologics and Biosimilars (OTBB) within the Center for Drug Evaluation and Research (CDER), though biologics licensed under the Public Health Service Act are reviewed by CBER. The FDA has issued product-specific guidance documents for over 30 reference products, covering acceptable analytical methods, study designs for comparative PK/PD studies, and the scope of required immunogenicity data. These guidance documents are essential reading for any development team entering a biosimilar program for a specific molecule.
A key difference between FDA and EMA approaches is the FDA’s emphasis on large, well-controlled confirmatory clinical trials for monoclonal antibodies. While the FDA has approved some biosimilars using PK/PD data only — Cyltezo (adalimumab-adbm) and several more recently — the default expectation for complex monoclonal antibodies has historically included a comparative efficacy trial with an adequate power to detect a pre-specified clinical equivalence margin. This requirement has been a significant cost driver and a source of debate, since most statisticians and regulatory scientists agree that these trials are rarely the most sensitive tool for detecting clinically meaningful differences between two analytically similar products.
The FDA’s June 2024 draft guidance on interchangeability signaled a meaningful shift in this position. The guidance proposed eliminating the default requirement for switching studies as a condition for the interchangeable biosimilar designation, citing accumulated real-world evidence from Europe and the U.S. demonstrating the safety of switching. If finalized in its proposed form, this change would remove a $15 to $50 million barrier that previously separated biosimilar designation from interchangeable biosimilar designation and would remove the implied quality hierarchy between the two labels.
Interchangeability: What the Designation Does and Does Not Mean
The interchangeable biosimilar designation under U.S. law is a logistical classification for pharmacy dispensing, not a clinical quality tier. Under the BPCIA, a product designated as interchangeable may be substituted for the reference product at the pharmacy counter without intervention by the prescribing physician, subject to state pharmacy substitution laws. As of early 2026, all 50 states have enacted statutes governing biosimilar substitution, with most requiring pharmacist notification to the prescriber within some specified period after substitution.
The first interchangeable biosimilar designation was granted to Semglee (insulin glargine-yfgn, Viatris/Biocon) in July 2021. Subsequent interchangeable designations have been granted to several adalimumab biosimilars, bevacizumab biosimilars, and trastuzumab biosimilars.
The FDA’s recent moves to update biosimilar product labeling are also consequential here. In 2023, the FDA revised its labeling guidance to remove the explicit ‘interchangeable’ statement from product labels, replacing it with the Biosimilar Product Information box that communicates approval standards to prescribers without creating a tiered quality impression. This was a deliberate effort to address the persistent misperception — documented in prescriber surveys from 2019 through 2022 — that a biosimilar without the interchangeable designation is somehow clinically inferior.
The commercial reality is that interchangeable designation has concrete formulary access value in the U.S., independent of any clinical differentiation. PBMs and health plans use interchangeable designation as a formulary management criterion. A biosimilar with interchangeable status can be placed on a formulary with automatic substitution enabling, allowing the PBM to switch patients at the point of dispensing without prescriber action. This mechanism drives volume efficiently. A biosimilar without the designation requires either prescriber conversion or step therapy protocols, which are slower and more resource-intensive commercially.
Global Regulatory Divergences: Where Duplication Costs the Most
Beyond the FDA and EMA, biosimilar developers targeting global markets face divergent requirements in Japan (PMDA), Canada (Health Canada), Australia (TGA), Brazil (ANVISA), India (CDSCO), China (NMPA), and South Korea (MFDS). The aggregate cost of managing these divergences across a single global program can reach $30 to $60 million in bridging studies, local clinical trials, and regulatory dossier variations.
Several specific divergences stand out for their cost impact. The PMDA requires a Japanese PK bridging study for most biosimilars, citing ethnic sensitivity as justification. For a monoclonal antibody with well-established population PK, this requirement — which adds 18 to 24 months and $8 to $15 million — is increasingly difficult to justify scientifically given the absence of clinically meaningful ethnic differences in PK parameters for IgG antibodies. The NMPA in China previously required local clinical trials for most biosimilars; regulatory reform since 2020 has reduced this burden for products approved by the FDA or EMA that use a globally sourced reference product, but the reform is inconsistently applied in practice.
The ‘global comparator’ problem compounds these costs. Many biosimilar developers use a U.S.-sourced reference product as the primary comparator, since U.S. market launch is the primary commercial target. A regulator that accepts only locally sourced reference product may require a separate bridging study comparing U.S.-sourced and locally sourced reference product to establish quality equivalence before accepting the development data. This adds a study that can cost $5 to $10 million and delays market entry by 12 to 18 months.
WHO’s prequalification program for biosimilars offers a partial solution for emerging markets, providing a technical assessment that national authorities can rely on as an alternative to conducting their own full review. WHO prequalification has been completed for several epoetins and G-CSFs and is being extended to monoclonal antibodies, which could meaningfully improve access in lower-income countries that lack the regulatory capacity for independent biosimilar assessment.
Key Takeaways: Regulatory Strategy
The most expensive regulatory mistake a biosimilar developer can make is treating the clinical trial program as the primary evidence-generation vehicle. Developers who front-load analytical characterization, negotiate with the FDA (via Type B meetings) on the evidentiary standard before committing to a clinical study design, and leverage extrapolation principles to minimize indication-specific trials consistently produce more efficient development programs. The trend toward reducing confirmatory clinical data requirements — visible in both FDA and EMA policy evolution — rewards developers who can generate a compelling, high-confidence analytical package. The companies that master analytical similarity science are structurally advantaged in a world where regulators are moving to accept more chemistry and less clinical.
Part IV: The BPCIA Patent Dance — Mechanics, Strategy, and the Real Cost of the Thicket
The Patent Dance: A Mandatory Disclosure of Your Trade Secrets to Your Competitor
The BPCIA’s patent dispute resolution process begins within 20 days of FDA acceptance of a biosimilar Biologics License Application (BLA). The biosimilar applicant must provide the reference product sponsor (RPS, i.e., the originator) with its complete application and detailed manufacturing process information. This disclosure is compelled by statute and is broader than anything required in Paragraph IV small-molecule patent litigation. The originator company receives the biosimilar’s cell line development data, upstream and downstream process parameters, formulation composition, and analytical methods — essentially the core proprietary knowledge that the biosimilar developer spent years generating.
The intended purpose of this disclosure is to enable an informed patent list to be compiled. The RPS then provides a list of patents it believes could be infringed, to which the applicant responds with detailed claim-by-claim invalidity and non-infringement contentions. The parties then negotiate a list of patents to be included in the first wave of ‘immediate patent litigation,’ with any remaining patents placed on a ‘second list’ that can be asserted after market launch.
The Supreme Court’s 2017 ruling in Sandoz Inc. v. Amgen Inc. established that the biosimilar applicant may decline to participate in the patent dance. If the applicant provides notice of commercial marketing no earlier than 180 days before launch (the ‘180-day notice’ requirement), the RPS can sue for infringement immediately upon receiving that notice, but the RPS cannot compel disclosure of the application through BPCIA mechanisms. The trade-off for opting out is that the RPS files suit against a less-defined target — it must identify potentially infringed patents without the detailed process information the dance would have provided — which can result in a broader initial complaint but may actually narrow the final dispute as the RPS learns more through litigation discovery.
Patent Dance Strategic Decision Matrix
The decision whether to engage in the patent dance is a function of four variables: the size and quality of the originator’s patent estate, the strength of the biosimilar developer’s freedom-to-operate position, the developer’s tolerance for disclosure risk, and the desired timeline to market entry.
Engaging in the dance is typically advantageous when the originator’s patent estate is large but the developer has strong invalidity contentions for most patents. The structured timeline of the dance forces the originator to narrow its claims early, limiting the scope of first-wave litigation and allowing the developer to focus its legal resources. For a 50-patent thicket where 40 patents are vulnerable to IPR or obviousness challenges, the dance provides a structured mechanism to identify and eliminate weak patents before they can be asserted at launch.
Opting out makes strategic sense when the originator’s blocking patents are few, the developer’s non-infringement position is strong, and rapid launch is commercially critical. In the adalimumab case, several biosimilar developers who had already secured licenses from AbbVie chose to minimize dance participation because the license already defined their rights and obligations, making the formal dance process largely redundant.
The decision is irreversible. Once a developer engages in the dance and provides its BLA, the disclosure has occurred. The risk calculus must account for the possibility that the disclosed information reveals process details the originator was unaware of — potentially enabling the originator to file new continuation patents covering the biosimilar’s specific manufacturing approach before the dance concludes.
Patent Thickets: Construction, Cost, and the Antitrust Frontier
Patent thickets are constructed systematically, and the pattern is detectable through patent database analysis years before a biologic approaches patent expiration. The filing cadence of secondary patents typically accelerates 5 to 8 years before the molecule patent expires, as originator companies begin formalizing their life-cycle management strategy. Developers watching a biologic 10 years out from its molecule patent expiry can observe this filing acceleration in real time and model the expected scope of the eventual thicket.
The economic logic of thicket construction is straightforward. Filing a patent application costs approximately $30,000 to $100,000 in prosecution fees. If even one secondary patent in a 100-patent portfolio survives PTAB challenge and holds up in district court, it can delay market entry by two to four years, generating billions in protected revenue for the originator. The expected return on investment for thicket construction is extraordinarily high, which is why major biologic sponsors continue to pursue it aggressively.
The antitrust challenge to thickets has largely failed in U.S. courts. The Seventh Circuit’s 2022 decision in Mayor & City Council of Baltimore v. AbbVie affirmed dismissal of antitrust claims against AbbVie’s Humira patent estate on the grounds that filing and asserting valid patents, even in large numbers, is protected petitioning activity under the Noerr-Pennington doctrine. Only ‘objectively baseless’ patent assertions — a very high legal bar — can constitute anticompetitive conduct. Legislative solutions are therefore the primary mechanism for constraining thickets, and several bills have been introduced in Congress that would limit the number of patents an originator can assert in BPCIA first-wave litigation.
The PTAB represents the most effective current tool for thicket reduction. Inter Partes Review (IPR) petitions challenge issued patents on grounds of anticipation or obviousness over prior art, using an expedited 12-month timeline and a lower burden of proof (preponderance of evidence) compared to district court litigation (clear and convincing evidence). PTAB institution rates for pharmaceutical patents have historically been above 60%, and the cancellation rate for petitioned claims is approximately 75% in instituted trials. For a biosimilar developer facing a 50-patent thicket, a coordinated PTAB campaign targeting the 20 to 25 most commercially blocking patents — while simultaneously pursuing district court litigation on the remainder — is the standard litigation strategy.
The cost of this campaign is substantial: $2 to $5 million per PTAB petition filed, multiplied by the number of petitions, plus district court litigation costs that can reach $50 million per case through trial. For a biosimilar developer targeting a market worth $2 billion annually, this investment is rational. For one targeting a market worth $200 million annually, the litigation economics may be negative — which is precisely why some important biologics never attract biosimilar competition.
Negotiated Licenses: When Settlement Is the Optimal Strategy
Most U.S. biosimilar market entries for products with complex patent estates conclude not with a court verdict but with a negotiated license from the originator. The terms of these licenses are generally confidential, but the public record reveals their structure: a defined launch date, a royalty rate (typically 5 to 15% of net sales), and sometimes field-of-use restrictions or supply constraints during an exclusivity period.
The negotiated license reflects a specific game theory equilibrium. The originator knows that if it litigates aggressively against all biosimilar developers, some will eventually win at the PTAB or in district court, potentially invalidating its most valuable secondary patents and triggering open market entry. By licensing the first two or three developers at defined entry dates, the originator buys time, collects royalties, and reduces the risk of outright patent invalidation. The biosimilar developers, facing the prospect of $100 million+ in litigation costs with uncertain outcomes, accept the certainty of a defined launch date in exchange for the royalty burden.
Understanding this equilibrium is essential for any developer entering a market with a complex patent estate. The practical question is not ‘can we win in court?’ but ‘what is the originator’s minimum acceptable license term, and can we build a business at that royalty rate?’ Developers who enter a crowded thicket with strong PTAB petitions filed early improve their negotiating leverage because they impose real legal risk and cost on the originator, which shifts the settlement equilibrium toward a more favorable entry date and lower royalty rate.
Part V: Commercial Strategy — Formulary Access, the PBM Rebate Wall, and the European Contrast
The U.S. Market Access Problem Is Structural, Not Price-Based
The conventional assumption about biosimilar commercial strategy — that a lower price drives market share — is wrong for the U.S. market. Price is a necessary condition but not a sufficient one. The U.S. biopharmaceutical reimbursement system routes volume through PBMs and health plan formularies, and those formulary decisions are driven by rebate economics, not list price comparisons.
The structure of the problem is as follows. An originator biologic with a $60,000 annual list price provides the PBM with a 30 to 50% rebate — $18,000 to $30,000 per patient-year — in exchange for preferred formulary placement. A biosimilar launching at a 30% list price discount ($42,000 annual list price) may offer the PBM a smaller absolute rebate, both because the price base is lower and because the biosimilar developer lacks the margin to match the originator’s rebate commitment. The net cost to the health plan of the originator, after rebates, may actually be lower than the biosimilar’s list price, depending on rebate rates. The PBM therefore has an economic incentive to give the originator preferred status, even though the biosimilar carries a lower list price.
This dynamic played out precisely with adalimumab in 2023. Despite biosimilars launching with list price discounts as steep as 80%, the major PBMs — CVS Caremark, Express Scripts, and OptumRx — maintained Humira on preferred commercial formularies through most of 2023 and into 2024, citing the value of AbbVie’s rebate commitments. The cumulative biosimilar market share remained below 5% for the first 12 months post-launch, a result that shocked analysts who had projected 20 to 30% uptake based on list price economics.
The dam broke in April 2024 when CVS Caremark announced that it would remove Humira from its primary commercial formularies and substitute Sandoz’s Hyrimoz (adalimumab-adaz) as the preferred biosimilar, via CVS’s Cordavis subsidiary. Within 30 days, biosimilar adalimumab’s share of new prescriptions rose to approximately 36%. The formulary decision — not the drug’s FDA approval, not its analytical similarity, not its list price — was the commercial inflection point.
Commercial Models for Biosimilar Market Access
The Cordavis/CVS model represents a structural evolution in biosimilar commercialization. Rather than competing for formulary placement through standard contracting, Sandoz effectively partnered with a major PBM to create a captive distribution relationship. CVS Caremark, through Cordavis, has a direct financial interest in Hyrimoz’s commercial success, aligning the PBM’s incentives with biosimilar uptake rather than against it. This is a significant model innovation and one that other biosimilar developers are studying carefully.
Alternative commercial models gaining traction include direct-to-employer contracting, where biosimilar manufacturers bypass PBMs entirely and contract with self-insured employers (who cover approximately 60% of commercially insured U.S. patients) at net prices that reflect the true biosimilar discount rather than the list-price-plus-rebate structure. Cigna’s Express Scripts launched similar direct contracting arrangements for adalimumab biosimilars in late 2023. Hospital group purchasing organizations (GPOs), which have historically been more price-sensitive than commercial PBMs, have shown higher biosimilar uptake rates for physician-administered biologics (the ‘buy-and-bill’ channel), where hospital formulary committees make the primary prescribing decision and the institution captures the margin between acquisition cost and reimbursement.
The buy-and-bill channel deserves particular attention for IV-administered biologics like infliximab, rituximab, and trastuzumab. In this channel, hospitals and oncology practices purchase biologics at negotiated acquisition prices and bill payers at the Average Sales Price (ASP) plus a 6% margin. When a biosimilar has a lower ASP than the reference product, the absolute dollar margin on the 6% add-on is smaller, but the net acquisition cost savings to the provider are larger. CMS’s reimbursement structure has been modified to provide a higher ASP add-on for biosimilars (ASP+8% versus ASP+6% for reference biologics) as an incentive for provider adoption, a policy that meaningfully improved biosimilar penetration in the oncology buy-and-bill market.
European Market Access: Tendering, Reference Pricing, and What Actually Works
European biosimilar market dynamics differ substantially from the U.S. because European health systems are structured to capture the lowest net cost at the formulary or procurement level, rather than managing a multi-party rebate system. Two mechanisms dominate.
National tendering is used in Nordic countries, the U.K. (through NHS England’s Commercial Medicines Unit), and increasingly in Italy and Spain. In a tender, health authorities issue a call for bids from all suppliers of a given biologic (reference product and biosimilars), commit to purchasing a specified volume over a defined contract period, and award the contract to the lowest bidder or to a basket of bidders using a framework that allocates volume in exchange for price commitments. Norway’s national tender for infliximab in 2017 resulted in biosimilar Remsima winning approximately 90% of market share within six months of the tender result, at a price 72% below the originator’s previous list price. This represents a speed and depth of penetration that has never been achieved in the U.S. commercial market.
Reference pricing operates in Germany (through the GKV-Spitzenverband framework), France, and several other markets. In Germany, the GKV sets a reference price for each therapeutic cluster — including the originator biologic and all its biosimilars — and reimburses patients up to that reference price. If the originator’s list price exceeds the reference price, patients pay the difference out-of-pocket, creating a direct financial incentive to use the biosimilar. The originator can either lower its price to match the reference or accept reduced market share as cost-sensitive patients shift to biosimilars. AbbVie responded to this mechanism in Germany by lowering Humira’s list price significantly, and biosimilars still captured the majority of new prescriptions because their prices were lower still.
The practical lesson from European experience is that reimbursement system design is the primary driver of biosimilar uptake speed and depth. No amount of physician education, patient communication, or commercial excellence can overcome a reimbursement architecture that financially rewards originator prescribing. U.S. payers who genuinely want to capture biosimilar savings need to restructure formulary contracting to align PBM incentives with net cost reduction rather than rebate maximization.
Overcoming Prescriber Inertia and the Nocebo Effect
Even in markets with favorable reimbursement structures, physician prescribing inertia can slow biosimilar uptake, particularly for patients already stable on a reference biologic. Two factors drive this inertia: genuine uncertainty about the safety of switching (which is scientifically unjustified but pervasive among non-specialist prescribers) and the nocebo effect, where patients who are informed that they are being switched to a ‘different’ medication report subjective adverse events at higher rates than patients switched without this framing.
The nocebo effect is not trivial. Studies of infliximab and etanercept switching in inflammatory bowel disease and rheumatology patients have documented nocebo-related discontinuation rates of 5 to 15%, despite no pharmacological basis for differential response. Physician communication strategy — specifically, framing the switch as a routine formulary change rather than a medical substitution — can meaningfully reduce nocebo rates. The NOR-SWITCH study, a randomized controlled trial of switching from Remicade to Remsima in Norwegian IBD patients, found no meaningful difference in disease control outcomes, but this landmark data was published in 2017 and remains underutilized in U.S. prescriber education programs.
The real-world evidence base for biosimilar switching safety has now reached a scale that removes most legitimate clinical uncertainty. A 2023 meta-analysis covering more than 150,000 patient-switch events across multiple biologics and therapeutic areas found no statistically significant difference in efficacy or safety outcomes between patients who switched to a biosimilar and those who continued on the reference product. This body of evidence is the most powerful educational asset available to biosimilar commercial teams, and it has not been used effectively in most U.S. go-to-market strategies.
Investment Strategy: Commercial Due Diligence for Biosimilar Programs
For investors evaluating biosimilar commercial programs, the key due diligence variables are formulary access strategy, channel mix, and time-to-profitability assumptions.
A biosimilar program without a credible formulary access strategy — specific PBM contracting relationships or direct employer contracting commitments in place before launch — should be discounted heavily in commercial projections. Historical U.S. launch data shows that biosimilars that launched without PBM formulary commitments captured median market share of less than 5% in year one, compared to 15 to 20% for biosimilars that launched with at least one major PBM formulary commitment.
Channel mix matters for gross margin analysis. The buy-and-bill oncology channel typically generates higher gross margins per unit than specialty pharmacy channels because reimbursement is at ASP and the 8% add-on provides a floor for profitability. Specialty pharmacy-dispensed biologics (self-injectable subcutaneous products like adalimumab or etanercept) face more complex margin dynamics because the gross-to-net discount required to achieve formulary placement in commercial PBM channels can reduce realized net price to 40 to 60% of list price.
Time-to-profitability for U.S. biosimilar programs with complex patent litigation and PBM contracting requirements averages 4 to 7 years from IND filing to positive EBITDA, assuming commercial launch in years 5 to 7. Programs that achieve formulary placement at launch can reach profitability faster, but the contracting cost of that placement reduces gross margin in early years.
Part VI: Emerging Technologies Reshaping Biosimilar Development Economics
AI and Machine Learning in Upstream Process Development
Machine learning applications in biosimilar development are moving from pilot to production across several areas. In cell line screening, supervised learning models trained on historical datasets of clone productivity, product quality, and genetic stability can narrow the screen from thousands of candidates to dozens within weeks, compressing the cell line development timeline by 30 to 50%. The input features for these models include transcriptomic profiles of clones at early passage, in-process metabolite trajectories, and early glycan profiling data.
In upstream process optimization, neural network models trained on historical bioreactor datasets can predict how changes in feeding strategy, temperature shift timing, or agitation rate will affect product quality attributes. These models enable in silico process optimization — testing hundreds of process parameter combinations computationally before committing to experimental runs — which reduces the number of bioreactor experiments required to develop a commercial-scale process. Lonza, Sartorius, and several biosimilar developers including Celltrion and Samsung Bioepis have published data on ML-accelerated process development timelines.
In the analytical domain, deep learning models applied to mass spectrometry datasets can detect subtle glycoform distribution differences between biosimilar and reference product lots with sensitivity beyond human expert interpretation. These models, when validated and submitted as part of an analytical similarity package, could eventually support reduced clinical study requirements by demonstrating a higher degree of molecular confidence than conventional analytical approaches provide.
Continuous Bioprocessing and Its Implications for Biosimilar Economics
Traditional biopharmaceutical manufacturing uses fed-batch bioreactors followed by batch capture chromatography, with the process stopped and the harvest tank emptied between each production cycle. Continuous bioprocessing — specifically the use of perfusion bioreactors coupled to continuous capture chromatography (periodic counter-current or simulated moving bed systems) — changes the economics of biologic production fundamentally.
In a perfusion bioreactor, cells are retained inside the bioreactor while spent culture media is removed and fresh media added continuously. Cell densities 10 to 50 times higher than fed-batch are achievable, with a corresponding increase in volumetric productivity. A 200-liter perfusion bioreactor can match the output of a 2,000-liter fed-batch bioreactor, with dramatically lower facility capital investment. The consistency advantage is equally important: a continuous process operates at steady state, with CQAs more tightly controlled than in a fed-batch process that traverses multiple metabolic phases during a 14-day production run.
For biosimilar economics, continuous manufacturing at smaller scale changes the minimum viable market size calculation. Under conventional fed-batch manufacturing, the capital cost of building and validating a commercial-scale facility (typically $200 to $400 million) is only justified for markets with peak annual biosimilar revenue potential of $300 million or more. A continuous manufacturing platform capable of meeting commercial supply requirements from a $50 million capital investment potentially enables biosimilar development for biologics with annual market sizes of $100 to $200 million, opening competition in markets that are currently uncontested.
Sartorius’s ambr 250 perfusion system and Repligen’s continuous bioprocessing portfolio are enabling contract development and manufacturing organizations (CDMOs) to offer continuous manufacturing services that smaller biosimilar developers can access without building proprietary infrastructure.
The Next Wave: Monoclonal Antibody Biosimilars for Immuno-Oncology and Beyond
The biologics approaching patent expiration over the 2026 to 2035 period represent a fundamentally more complex development challenge than first-wave biosimilars. Keytruda (pembrolizumab, anti-PD-1) and Opdivo (nivolumab, anti-PD-1) are checkpoint inhibitors whose mechanism of action is not fully characterized at the molecular level — specifically, the relationship between Fc effector function, PD-1 binding affinity, and clinical efficacy in each indication has not been cleanly defined. A biosimilar developer targeting pembrolizumab must demonstrate functional similarity for a mechanism that involves T-cell receptor complex interactions and tumor microenvironment signaling that cannot be fully modeled in cell-based assays.
Stelara (ustekinumab) biosimilars are already in late-stage development and early approvals (Samsung Bioepis’s Pyzchiva received FDA approval in 2023, and Hikma/Biocon’s product followed), with a commercial inflection expected as Johnson & Johnson’s Paragraph IV litigation settlements define market entry dates. Ustekinumab targets both IL-12 and IL-23 via binding to the shared p40 subunit; its dual-cytokine mechanism means that Tier 1 functional assays must cover both pathways, making the analytical package more complex than for a single-target antibody.
Dupilumab (Dupixent, anti-IL-4Ra), with global 2024 sales approaching $14 billion across atopic dermatitis, asthma, and COPD indications, will become one of the highest-value biosimilar targets as its core patents expire in the early 2030s. Sanofi and Regeneron’s extensive patent estate will require the same thicket-management strategy as Humira, and the commercial launch will be complicated by the high patient population overlap between atopic dermatitis (managed in dermatology) and asthma (managed in pulmonology/allergy), requiring multi-specialty commercial execution.
Key Takeaways: Technology and Future Landscape
The structural economics of biosimilar development are changing in a direction favorable to new entrants with technology capabilities. AI-accelerated process development compresses the most capital-intensive pre-IND phase. Continuous manufacturing reduces the facility capital barrier for commercial supply. Regulatory evolution toward reduced clinical data requirements lowers the probability-weighted expected cost of the clinical phase. The combination of these trends will not transform biosimilar development into generic drug development — the molecular complexity and regulatory rigor will remain qualitatively different — but they are shifting the minimum viable investment from $150 to $300 million toward $75 to $150 million for straightforward monoclonal antibody targets. That shift opens the market to a broader range of companies and makes a wider range of biologic targets commercially viable.
Conclusion: The Integrated Strategy Imperative
The biosimilar industry’s core insight is that development excellence in any single domain is insufficient. A developer with world-class bioprocess engineering who fails to anticipate the patent thicket will miss its market window by years. A developer with a clean analytical similarity package who launches without formulary access commitments will capture single-digit market share despite FDA approval. A developer with both scientific and regulatory capability who underestimates the nocebo effect will spend $50 million on a commercial launch that moves less volume than a competitor who invested half as much in prescriber education.
What separates durable competitors in this space is an integrated capability — the ability to run scientific, regulatory, legal, and commercial processes in parallel rather than sequentially, with each function informing the others continuously. The biosimilar development timeline is not eight years of sequential gate-based decisions; it is eight years of parallel workstreams that must be coordinated in real time. Process decisions made in year one have patent design-around implications that IP counsel needs to assess in year one. Regulatory precedent established by a competitor’s FDA advisory committee in year three informs the confirmatory clinical study design the team commits to in year four. PBM contracting discussions that begin in year five shape the list price architecture that finance locked down in year three.
The companies succeeding in this environment — Sandoz, Celltrion, Samsung Bioepis, Amgen Biosimilars, Pfizer Biosimilars — share this integration capability. They are not the cheapest manufacturers or the best lawyers or the most experienced regulatory teams. They are the organizations that have built systems for coordinating all three domains under a unified development strategy.
For newer entrants, the path to competitive viability runs through specialization in one of three directions: technology differentiation (continuous manufacturing, AI-accelerated development, or novel formulation capabilities that create design-around options for thicket management); market focus (targeting therapeutic areas or geographies where the originator’s commercial infrastructure is weaker and formulary access is less contested); or partnering (licensing cell lines or process technology from established CDMOs, partnering with PBMs or health systems for commercial access, or co-developing with regional market specialists who bring local regulatory and commercial capabilities).
The $180 billion in projected cumulative savings by 2027 is not automatic. It is the output of investment decisions made by developers, health system design choices made by payers, and patent policy choices made by legislators. Every actor in this system is making decisions under uncertainty with incomplete information. The developers and investors who build the best information advantage — through rigorous patent analysis, regulatory intelligence, and commercial access data — will capture a disproportionate share of both the savings and the returns.
Investment Strategy Summary for Biosimilar Portfolio Managers
Target selection criteria for high-probability returns should weight four factors: molecule patent expiration within 3 to 5 years with limited secondary patent overhang; reference product annual revenue above $1.5 billion in the target market; existing regulatory precedent from at least one prior biosimilar approval that resolved the most complex analytical comparability questions; and a commercial market structure in which at least one major payer has expressed interest in formulary conversion.
Red flags that warrant additional due diligence include: a patent thicket with more than 50 active secondary patents filed after approval (Humira-pattern risk); a mechanism of action that depends on incompletely characterized immune cell interactions (risk of Phase III clinical requirement); a reference product primarily dispensed through a single specialized pharmacy network with long-term exclusive distribution contracts (formulary access barrier); and a developer without prior commercial-scale biologics manufacturing experience (scale-up risk that inflates probability of CMC delays).
The most asymmetric near-term opportunities lie in second-wave biosimilars where a first entrant has already incurred the analytical development and regulatory precedent costs, reducing the evidentiary burden for subsequent applicants. In established biosimilar markets (infliximab, rituximab, trastuzumab), the cost of development for a third or fourth market entrant is materially lower than for the first, because prior FDA biosimilar approvals define the acceptable analytical comparability package and the clinical study design. These ‘fast-follower’ programs can sometimes be developed for $60 to $90 million, placing them within the reach of mid-sized specialty pharma companies or well-capitalized private equity-backed platforms.
The decade ahead belongs to developers who treat biosimilar development as an integrated scientific, legal, and commercial investment thesis rather than a manufacturing challenge with a regulatory wrapper. The companies that internalize that framing — and build organizations accordingly — will define the next generation of this market.