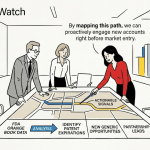
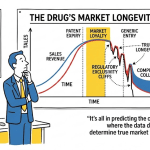
When generic competition arrives, it arrives fast. Within the first 12 months of a major brand losing exclusivity, generic entrants can strip 80% to 90% of its revenue. For a deal team evaluating an in-licensing target, that single statistic reframes the entire analytical problem. The core question is not whether a drug is commercially attractive today. It is whether its exclusivity is structurally durable enough to make it commercially attractive three, five, or eight years from now.
That question requires a framework far more sophisticated than checking a patent expiration date in the Orange Book. A truly defensible asset sits behind a series of concentric protective layers: a patent fortress built by the innovator, a regulatory moat granted by the FDA, structural barriers inherent to the drug’s manufacturing and market, and a litigation posture capable of withstanding the near-certain Paragraph IV challenge that comes with any commercially meaningful product. This pillar page works through each layer in technical depth, adds IP valuation frameworks missing from the original analysis, and closes with a deal-structuring and life cycle management roadmap built for the analysts and portfolio managers who will actually execute these decisions.
Part One: Market Exclusivity Architecture
How a Drug’s Monopoly Is Actually Built
Pharmaceutical market exclusivity is a dual-system construct. The first system is patent law, administered by the USPTO, which grants time-limited monopoly rights in exchange for public disclosure of an invention. The second is regulatory exclusivity, administered by the FDA, which grants marketing protection periods as a statutory incentive to encourage development in specific areas. These two systems run in parallel, interact in complex ways, and together determine the effective exclusivity window that an in-licensing team must model.
A common due diligence error is treating these systems as redundant. They are not. A composition of matter patent can be challenged and invalidated. A 7-year Orphan Drug Exclusivity cannot be bypassed regardless of patent status. A drug that loses its composition patent to an Inter Partes Review (IPR) petition but retains two years of Orphan Drug Exclusivity (ODE) has two years of guaranteed market isolation that no generic can touch legally. The deal team that fails to model this interaction will both underprice and under-protect itself.
The Patent Fortress: Structure, Valuation, and Strategic Depth
Composition of Matter Patents: The Foundational Asset
A composition of matter patent on an active pharmaceutical ingredient is the highest-value single IP asset in pharma. It covers the molecular entity itself, which means a generic competitor cannot legally manufacture the drug in any form during the patent’s life without risking infringement. For valuation purposes, a composition of matter patent with substantial remaining life (eight-plus years) on a drug generating $500M or more in annual revenue justifies a discounted cash flow (DCF) premium versus a drug with equivalent revenue but only secondary patent protection remaining.
The practical valuation question for an in-licensing team is not just ‘does this drug have a composition patent’ but ‘what is the remaining adjusted term after Patent Term Extension (PTE)?’. Under 35 U.S.C. Section 156, the FDA review period can be partially added back to the patent term, up to a maximum of five additional years, with total adjusted term capped at 14 years post-approval. A drug approved after a lengthy NDA review may have a PTE-adjusted composition patent that extends meaningfully beyond its nominal expiration date. This adjusted term, not the filed expiration, is the correct input for any revenue-at-risk model.
IP Valuation: The Rents-Based and Risk-Adjusted Approaches
Two methodologies dominate pharmaceutical patent valuation, and a serious due diligence process uses both as a cross-check. The first is the relief-from-royalty method, which estimates the value of the patent portfolio by calculating the royalty stream the company would have to pay if it did not own the IP. Industry royalty rates for pharmaceutical composition patents typically range from 3% to 8% of net sales for small molecules, and 8% to 15% for complex biologics, though specific terms vary widely by therapeutic area and market exclusivity remaining. Applying these rates to the risk-adjusted net present value of projected revenues produces a patent portfolio value estimate.
The second approach is the income method with a probability-adjusted patent cliff. This model forecasts revenue under two scenarios: a ‘patent held’ scenario where full exclusivity is maintained, and a ‘patent lost’ scenario where generic entry occurs at a specified future date. Each scenario receives a probability weight based on the litigation risk assessment described in Part Three. The weighted average of the two discounted revenue streams yields the risk-adjusted asset value. The delta between that figure and a naive ‘no generic entry’ valuation quantifies exactly what you are paying for IP durability, which is the number that belongs in every board-level deal memo.
Secondary Patent Portfolios: Building and Reading the Thicket
Beyond the composition patent, a well-protected drug carries a dense secondary portfolio covering formulations, methods of use, polymorphs, metabolites, dosing regimens, patient selection methods, manufacturing processes, and delivery device components. The strategic logic is straightforward. A generic challenger must ‘clear the path’ by either waiting for every relevant patent to expire or by litigating each one. A portfolio with a composition patent expiring in 2029 but carrying formulation patents through 2033 and a method-of-use patent through 2035 forces a generic developer to win at multiple legal fronts simultaneously, dramatically raising its cost of entry.
Reading a target’s patent thicket requires more than counting Orange Book listings. Many relevant patents are not listed in the Orange Book because they are not directly tied to the approved formulation or use code, yet they can still support infringement claims. A complete patent landscape must include USPTO database searches, PCT filings at the World Intellectual Property Organization (WIPO), and European Patent Office (EPO) records. Platforms like DrugPatentWatch surface non-Orange Book patents that would be invisible to a team relying solely on the FDA’s public database.
The density and diversity of secondary patents correlate strongly with an innovator’s institutional commitment to a franchise. A company that has filed 12 patents across six distinct categories for a single drug (formulation, method, polymorph, device, dosing regimen, manufacturing) is telling you something specific: this product is a priority asset, they have assigned dedicated IP counsel and R&D resources to it, and they intend to fight for it. That commitment is not just a legal asset; it is an organizational signal that reduces the risk of the licensor abandoning defense litigation after your deal closes.
Key Takeaways: Patent Fortress Assessment
When screening in-licensing targets on patent strength, prioritize composition of matter patents with PTE-adjusted terms exceeding five years from deal close. Calculate patent portfolio IP value using both the relief-from-royalty and probability-weighted income methods, and flag any gap larger than 20% between the two estimates as a valuation risk requiring additional legal review. Treat secondary patent count and category diversity as a proxy for the innovator’s institutional commitment, not merely as a count of legal obstacles. Any target where secondary patents were filed more than two years after the original composition filing warrants extra scrutiny on whether those patents were prosecuted with a clear litigation strategy in mind or were filed reactively as an afterthought.
The Regulatory Moat: Statutory Exclusivities in Detail
New Chemical Entity (NCE) Exclusivity
NCE exclusivity grants five years of protection from the date of FDA approval for drugs containing an active moiety never previously approved. The FDA will not accept an ANDA or 505(b)(2) application for four years (or five years if no Paragraph IV challenge is filed). NCE exclusivity runs from the approval date regardless of patent status. For a drug approved on January 1, 2023, with a composition patent that theoretically expired in 2021 due to prior litigation, NCE exclusivity alone would bar generic entry through January 1, 2027. This is why regulatory moat analysis must always run in parallel with, not downstream of, patent analysis.
Orphan Drug Exclusivity (ODE): The Niche Market Premium
ODE grants seven years of marketing exclusivity for drugs approved to treat diseases affecting fewer than 200,000 Americans. The bar for a competing application during ODE is extraordinarily high. A second manufacturer can only obtain approval for the same drug in the same orphan indication by demonstrating clinical superiority, a regulatory standard that has historically been difficult to meet. The economic logic of ODE aligns with the natural market structure of rare disease treatment: small patient populations, no meaningful generic entry incentive, and formulary dynamics driven by clinical differentiation rather than price.
For in-licensing purposes, an ODE-protected rare disease drug is among the most durable available targets. The combination of regulatory exclusivity and natural market economics makes generic entry both legally improbable and commercially unattractive. The 2024 orphan drug market exceeded $200 billion globally, with average net price per patient year in the range of $150,000 to over $500,000 for ultra-rare conditions. A licensed ODE asset in this space carries a fundamentally different risk profile than a primary-care blockbuster with similar topline revenue.
IP Valuation Note: ODE as a Standalone Asset
An ODE remaining term should be valued as a distinct cash flow-generating asset separate from the patent portfolio. Because it cannot be challenged or invalidated through IPR or Paragraph IV proceedings, it carries a near-zero legal risk discount, unlike patent-based exclusivity. A two-year ODE tail after the last patent expiry on a drug with $300M in annual rare disease sales represents roughly $600M in guaranteed brand-protected revenue (before discounting), with minimal probability of dilution. That figure belongs explicitly in the deal valuation model, labeled separately from patent-protected revenue.
Biologic Exclusivity Under the BPCIA
The Biologics Price Competition and Innovation Act (BPCIA) grants 12 years of reference product exclusivity from first licensure, during which the FDA cannot approve a biosimilar application for that reference biologic. An additional one-year exclusivity attaches to a newly approved indication for a previously approved biologic. The 12-year term is longer than any other FDA exclusivity type and reflects the genuine complexity of biosimilar development.
A biosimilar manufacturer faces development timelines of 7 to 8 years and costs typically between $100 million and $250 million, compared to under $10 million for a standard small-molecule generic. The analytical and manufacturing demands of demonstrating biosimilarity, including extensive comparability studies across physicochemical, functional, and clinical endpoints, filter the competitive field to a small number of well-capitalized players. As of 2025, fewer than 20 companies globally have the technical infrastructure to advance a biosimilar through U.S. approval on their own. This structural reality makes a biologic in the first half of its BPCIA exclusivity window one of the most defensible in-licensing targets in the market.
Pediatric Exclusivity and QIDP: The Additive Extensions
Pediatric exclusivity adds six months to all existing patents and exclusivities upon completion of an FDA-requested pediatric study. For a blockbuster drug with multiple remaining patents, six months of extended monopoly pricing can represent several hundred million dollars in incremental revenue, making it a meaningful deal consideration even though it is procedurally a ‘bonus’ rather than a core IP right.
The Qualified Infectious Disease Product (QIDP) designation for antibacterial and antifungal drugs adds five years to any other exclusivity, turning a standard 5-year NCE exclusivity into 10 years. Combined with an orphan designation for a rare infectious disease, QIDP can create total exclusivity periods that push well past a decade from approval. Any in-licensing target in the infectious disease space should be screened for these additive designations before the core valuation is established.
Regulatory Exclusivity Interaction: The Gap-Filling Strategy
The most overlooked application of regulatory exclusivity analysis is identifying how exclusivity periods can ‘fill gaps’ created by patent weakness. Consider a drug where the composition patent expires in 2027, a formulation patent expires in 2030, and a 7-year ODE runs through 2031. A generic manufacturer could theoretically challenge the composition patent today but cannot obtain FDA approval for any competing product until ODE expires in 2031. By that date, the formulation patent has only one year remaining. The expected window between patent defeat and effective generic market entry is compressed to a single year, a scenario that most generic developers would judge uneconomical given their sunk litigation costs. This gap-filling dynamic fundamentally de-risks the asset, and a deal team that models it correctly will assign a materially higher probability-weighted value to the franchise than one that treats patents and exclusivity as independent protections.
Key Takeaways: Regulatory Moat Assessment
Build a parallel regulatory exclusivity timeline alongside the patent expiration schedule for every in-licensing target. Identify all active exclusivities (NCE, ODE, BPCIA, Pediatric, QIDP) and map their remaining durations against the patent cliff. Flag any ODE remaining terms as near-zero legal risk cash flow and value them separately from patent-protected revenue. Screen all infectious disease and rare disease targets for QIDP and orphan designations before finalizing the DCF model. Run a ‘gap-fill’ analysis to determine the minimum realistic window between a successful patent challenge and actual FDA generic approval, the compressed economic opportunity left for a generic developer is the correct risk metric, not simply patent expiration.
Part Two: Evergreening as Signal and Strategy
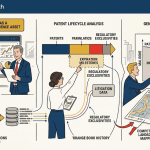
What an Innovator’s Life Cycle Management History Tells You
Evergreening is the systematic use of secondary IP filings to extend a drug’s commercial monopoly beyond its original composition patent. Critics frame it as delay of generic competition. For a business development team evaluating an in-licensing target, it is a clinical indicator of how aggressively the innovator manages its franchises.
A company with a documented track record of successful evergreening on multiple products has demonstrated specific institutional capabilities: a dedicated pharmaceutical IP strategy function, established relationships with patent litigation counsel, in-house formulation R&D capable of generating defensible incremental innovations, and a corporate willingness to commit the legal budget to defend those innovations in court. These capabilities do not disappear when a licensing deal is signed. They continue to operate in service of the franchises those companies protect, including the asset you are licensing.
Product Hopping: The Most Commercially Potent Tactic
Product hopping involves launching a patent-protected next-generation formulation, typically a new extended-release version or a novel delivery system, and then systematically migrating the patient base from the original formulation to the new one before the original’s patents expire. The migration depletes the commercial market for the incoming generic, which is designed to be bioequivalent to the original formulation, not the new improved version. By the time the first generic of the original enters the market, a substantial fraction of prescriptions have shifted to the new formulation where no generic yet exists.
AstraZeneca’s execution of this strategy between Prilosec (omeprazole) and Nexium (esomeprazole) is the canonical reference case. Prilosec was the world’s best-selling drug in 2000 with over $6 billion in U.S. revenue. Rather than simply defending the Prilosec franchise against the incoming generic, AstraZeneca began aggressively marketing Nexium, the S-enantiomer of omeprazole, in 2001. By the time Prilosec went generic in late 2001, the company had already repositioned a significant portion of its prescribing base. Nexium went on to peak at nearly $6 billion in U.S. revenue. The company did not simply defend a franchise; it replaced it with a patent-protected successor.
For in-licensing analysis, this case yields a specific investigative question: has the innovator already initiated the R&D or regulatory work for a next-generation version of the target asset? A Phase II trial registered on ClinicalTrials.gov for an extended-release formulation, a recent patent filing on a drug-device combination, or an FDA 505(b)(2) application in progress are all signals that the innovator is already executing a product hop strategy. If that successor product is included in the licensing deal, its incremental IP value must be valued separately. If it is not included, the deal team must understand exactly where the rights to that next-generation asset sit and whether the licensor retains the ability to execute a competing product hop post-deal close.
Case Study: Revlimid’s 18-Year Exclusivity Extension
Celgene’s management of Revlimid (lenalidomide) is the most thoroughly documented example of an extended patent thicket defense in contemporary pharmaceutical history. Between 1994 and 2019, Celgene obtained 27 additional patents on Revlimid beyond the original composition of matter patent, along with eight separate orphan drug exclusivities covering different hematological malignancies. The net effect was to push meaningful generic entry to 2026, 18 years beyond when it would have occurred based on the original patent alone.
From a portfolio valuation standpoint, this IP architecture created enormous shareholder value and justified Bristol Myers Squibb’s $74 billion acquisition of Celgene in 2019. The market priced the deal in part on confidence that Revlimid’s exclusivity was genuinely durable through the late 2020s. The subsequent settlement with generic manufacturers that allowed limited volume entry starting in 2022, stepping up gradually rather than a cliff-like full generic launch, demonstrated exactly the kind of controlled exclusivity unwind that a deep patent and ODE portfolio enables a company to negotiate.
An in-licensing team looking at an asset with a similarly dense patent portfolio should analyze whether the thicket structure makes a settlement-based ‘soft landing’ likely in the event of litigation, rather than a sudden generic cliff. That distinction has direct implications for how the revenue tail is modeled in any DCF.
Case Study: GlaxoSmithKline and Lamictal
GlaxoSmithKline extended Lamictal’s (lamotrigine) total protection period to 32 years, 12 years beyond the original compound patent, through a series of patents on new formulations including chewable dispersible tablets. The key IP move was combining formulation innovation with a method-of-use patent for the orally disintegrating tablet in specific patient subpopulations (pediatric and dysphagic patients) who had previously had difficulty tolerating the standard tablet. This is not trivial patent padding. The formulation had a genuine clinical rationale, which made it substantially more defensible in court and made physician-driven brand loyalty a real commercial factor.
The Lamictal case illustrates a broader principle: the strongest evergreening strategies are those where the secondary innovation has a legitimate clinical value proposition, because physicians who believe the new formulation is meaningfully better for their patients will resist substitution even after the original goes generic. Physician inertia among specialists managing severe epilepsy patients on stable regimens is a commercially real phenomenon. The patents protect the revenue; the clinical evidence protects market share when the patents eventually expire.
Key Takeaways: Evergreening Analysis
Before valuing any in-licensing target, build a complete timeline of the innovator’s historical patent filings on the asset and identify every product hop or formulation extension they have attempted. Cross-reference this history against the innovator’s other major franchises to identify whether this level of IP activity is characteristic of the company’s standard operating procedure or whether this particular asset has received unusual strategic attention. Search ClinicalTrials.gov and recent patent databases for any next-generation formulation work that may already be in progress. If a product hop is underway, negotiate explicit rights to the successor asset in the deal structure, or obtain a clear first right of negotiation, before closing.
Investment Strategy. For institutional investors evaluating a pharma company’s deal announcement, the disclosure that a newly in-licensed asset has an active next-generation program already in development at the licensor is a material positive signal. It suggests the licensee may be acquiring a pipeline of two products, not one, and that the life cycle management architecture is already being built, rather than being a future plan dependent on licensee R&D investment.
Part Three: Structural Barriers Beyond IP
Manufacturing Complexity as a Competitive Moat
Patent protection and regulatory exclusivity are legal constructs that can be challenged, circumvented, or invalidated. Manufacturing complexity is a technical barrier that exists regardless of legal outcomes. A generic manufacturer can win a Paragraph IV challenge against every one of a drug’s listed patents and still be unable to enter the market for years if it cannot replicate the manufacturing process.
Biologics: The Technical Replication Problem
Monoclonal antibodies, fusion proteins, and other large-molecule biologics cannot be chemically synthesized from a recipe the way a small molecule can. They are produced in living cell systems, typically mammalian cell lines such as Chinese Hamster Ovary (CHO) cells, under tightly controlled bioreactor conditions. Minute variations in cell line selection, nutrient media composition, dissolved oxygen levels, temperature cycling, and downstream purification chromatography steps all affect the post-translational modification profile of the resulting protein, particularly glycosylation patterns. These modifications directly influence immunogenicity, half-life, and efficacy. A biosimilar developer must characterize all of these attributes for the reference product, design and validate a manufacturing process capable of producing a molecule with a comparable profile, run comparability studies across analytical, functional, and clinical endpoints, and then generate clinical data in patients, all without access to the innovator’s proprietary cell line or process know-how.
The FDA’s totality-of-evidence standard for biosimilar approval, established under the BPCIA’s Section 351(k) pathway, requires this extensive characterization. It takes 7 to 8 years and costs $100 million to $250 million. Even after approval, the biosimilar must navigate the distinction between biosimilarity and interchangeability. An interchangeable designation, which allows pharmacist-level substitution without physician sign-off, requires additional switching studies demonstrating that alternating between the reference product and the biosimilar produces no additional risk versus continued use of either. As of early 2026, only a handful of biologics have achieved interchangeability designation, limiting the automatic substitution dynamic that drives rapid market share erosion in the small-molecule generic world.
IP Valuation Note: Biologic Manufacturing Know-How
In a biologic in-licensing transaction, the licensed IP extends beyond patents to include trade secrets: cell line construction methods, media formulations, purification protocols, and analytical methods for characterizing the drug substance. These trade secrets often hold more commercial value than the listed patents, particularly if the manufacturing process patent landscape is sparse. The deal structure must include comprehensive technology transfer provisions and, ideally, a transition services agreement (TSA) that keeps the innovator’s manufacturing team engaged long enough to validate the licensee’s internal capabilities. A failed biologic technology transfer is not just an operational setback; it is a catastrophic destruction of the asset’s commercial value.
Complex Small-Molecule Formulations: Where Bioequivalence Fails
Beyond biologics, a substantial category of small-molecule drugs resists generic replication due to formulation complexity. Long-acting injectable (LAI) formulations for antipsychotics, liposomal encapsulation systems used in oncology, and drug-in-adhesive transdermal patch systems all require manufacturing capabilities far beyond those of a standard oral solid dosage generics facility.
For LAIs, bioequivalence is governed by a hybrid standard that requires both pharmacokinetic studies and sometimes in vitro release rate testing. Particle size distribution and microparticle morphology matter for ensuring that the release profile from the depot injection is replicated. A generic developer cannot simply dissolve an API in suspension and call it bioequivalent.
Liposomal formulations present their own distinct challenge. Encapsulation efficiency, vesicle size distribution, lamellar structure, and drug-to-lipid ratio all affect the pharmacokinetic profile and toxicity of the final product. The FDA has issued detailed product-specific guidance for several liposomal drugs, acknowledging that standard bioequivalence approaches are insufficient and requiring product-specific study designs that substantially raise the development cost and timeline.
Drug-device combinations, including metered-dose inhalers, auto-injectors, and prefilled syringes, add a regulatory dimension that extends into the Center for Devices and Radiological Health (CDRH), not just the Center for Drug Evaluation and Research (CDER). For inhaled products, the generic must demonstrate device equivalence through in vitro aerosol characterization, cascade impaction, and, for some products, pharmacokinetic or pharmacodynamic clinical studies. Human factors studies for auto-injectors must show comparable ease of use across diverse patient populations. These requirements create substantial additional development time and cost that most generic developers have historically avoided.
Narrow Therapeutic Index Drugs: Regulatory Friction as a Moat
For drugs where small differences in plasma concentration produce either therapeutic failure or toxicity, NTI bioequivalence standards are tightened. The FDA’s standard bioequivalence acceptance criterion is a 90% confidence interval (CI) for the ratio of test-to-reference AUC and Cmax falling within 80% to 125%. For NTI drugs, the FDA may apply a scaled average bioequivalence (SABE) criterion that is more stringent, sometimes narrowed to 90% to 111%. This tightening substantially raises the probability that a generic candidate will fail bioequivalence testing, require reformulation and retesting, and face additional development delays.
Beyond the regulatory hurdle, NTI drugs benefit from a clinical inertia effect among prescribers. A neurologist managing a patient on stable carbamazepine or phenytoin therapy has a strong professional incentive not to introduce a formulation change. A single breakthrough seizure from a subtle difference in absorption kinetics carries severe consequences for the patient. This prescriber reluctance acts as a soft market barrier that persists even after generic approval, extending the brand’s effective market share retention beyond what pure bioequivalence data would predict.
API Supply Chain Concentration
The global API supply chain for most pharmaceutical products is highly concentrated. A significant proportion of APIs and their key starting materials (KSMs) for both branded and generic drugs are manufactured in China and India. For a generic developer, securing a qualified, cGMP-compliant API source is a prerequisite for any ANDA submission. For complex molecules with limited supplier bases, this is a genuine bottleneck. If only one or two API manufacturers globally have the synthetic chemistry capability to produce a specific compound at commercial scale, the generic developer must either secure supply from an existing manufacturer (potentially a direct competitor’s supplier) or develop an independent synthesis route, a process that can take two to three years and cost tens of millions of dollars.
The FDA’s post-pandemic enforcement posture on drug manufacturing quality has also raised the compliance bar for API sourcing. A manufacturing warning letter or import alert on a key API supplier can halt an entire ANDA program. For branded drugs with complex APIs, the probability that a would-be generic developer’s API source runs into compliance problems is non-trivial, particularly when sourcing from a small number of contract manufacturers with high industry volume.
Key Takeaways: Structural Barrier Assessment
When evaluating a biologic in-licensing target, obtain a full accounting of proprietary manufacturing trade secrets and ensure comprehensive technology transfer rights are included in the deal before any exclusivity payment is made. For complex small-molecule targets, use FDA product-specific bioequivalence guidance documents to assess whether the agency has already flagged the product as requiring non-standard BE approaches, those guidance documents are a direct indicator of the technical difficulty a generic developer faces. NTI status should be verified through clinical literature and the FDA’s published NTI drug lists, and its impact on prescriber switching behavior should be reflected in the brand’s projected post-generic market share model. API supply chain risk cuts both ways, a narrow supplier base deters generics but also creates operational risk for the licensee; demand full supply chain disclosure before deal close.
Investment Strategy. Institutional investors should screen pharma deal announcements involving complex biologics or drug-device combination products for the presence of a technology transfer provision in the disclosed term sheet. Deals announced without a defined technology transfer mechanism carry meaningful operational risk that is often not priced into initial market reactions.
Part Four: The Niche Market Economics of Generic Entry
Why Market Size Determines Competitive Intensity
Generic drug development is an investment decision. A generic company commits $2 million to $10 million to develop and file an ANDA for a standard oral solid dosage drug, factoring in development costs, clinical studies if required, and FDA filing fees. The economic return depends entirely on the size of the market and the number of competitors who also enter. As generic competitors accumulate, price erosion is rapid and severe.
The HHS ASPE analysis quantifies this precisely. A single generic entrant causes an average branded price reduction of 30% to 39%. Two entrants push the reduction to 54%. At six or more entrants, prices fall by 80% to 95% relative to the pre-generic branded price. The branded manufacturer retains a diminishing share of a rapidly shrinking pie. In large markets, the first-filer’s 180-day exclusivity remains valuable, but the post-exclusivity period becomes a race to the bottom among multiple competitors each fighting for volume at marginal cost.
This dynamic creates a clear economic screen for in-licensing teams. Markets with annual revenues above $1 billion attract a median of close to 10 generic applicants. Markets between $50 million and $200 million attract an average of three entrants. Below $50 million, the market is frequently not worth a single generic developer’s time to pursue. For an in-licensing team, a drug with $150 million in stable rare disease revenue protected by ODE and served by a complex manufacturing process often represents a more durable commercial position than a $1 billion primary care drug with a straightforward formulation and an approaching patent cliff.
The Orphan Drug Economics Model
Orphan drug pricing operates under a fundamentally different logic than primary care drug pricing. With patient populations capped at fewer than 200,000 in the United States by definition, and often in the range of 5,000 to 50,000 for ultra-rare conditions, a manufacturer must price per patient at a premium to justify R&D recovery. Average net prices for orphan drugs range from $150,000 to over $500,000 per patient per year, with the most severe rare diseases commanding over $1 million annually. This pricing premium is sustained by the ODE’s legal prohibition on competing products, the clinical complexity of switching stable patients, and the limited negotiating leverage of insurers who face political and regulatory pressure not to deny coverage for rare disease treatments.
For in-licensing due diligence, an orphan drug target with several years of ODE remaining and a genuine rare disease indication (small, well-characterized, and genetically defined patient population) warrants a lower risk discount on projected revenues than its topline numbers might suggest to an analyst applying generic pharmaceutical modeling assumptions.
The Inflation Reduction Act: A Counterintuitive Effect on Generic Entry Risk
The IRA’s drug price negotiation provisions, implemented through the Center for Medicare and Medicaid Services (CMS), allow the government to negotiate maximum fair prices (MFPs) for a defined list of high-spend Medicare drugs each year. Initial negotiations targeted small-molecule drugs that have been on the market for more than nine years post-BPCIA exclusivity, or nine years post-approval for small molecules, without generic or biosimilar competition. This eligibility window effectively targets the exact scenario that in-licensing teams seek to avoid: long-standing branded drugs with no competitive pressure.
The counterintuitive implication is that IRA negotiations reduce the net price of some branded drugs that generic developers were counting on for a large price differential. If a drug’s MFP is negotiated down to $80 per month from $300, the generic developer’s opportunity at, say, $60 per month is considerably less attractive than it was at the original price. The generic capture margin narrows, the ROI on ANDA development compresses, and some marginal investment decisions tip toward not filing. This dynamic is still early, and the evidence base is limited, but any in-licensing deal involving a drug with substantial Medicare exposure and potential IRA eligibility must model this policy effect explicitly.
Key Takeaways: Market Economics and Generic Entry Incentives
Screen in-licensing targets against the generic economic model explicitly. For each target, estimate the number of likely ANDA filers based on market size and formulation complexity, and model the revenue trajectory under the expected number of entrants. Targets with annual revenues below $200 million, complex formulations or BE hurdles, and ODE protection are among the least economically attractive markets for generic investment. For larger-market targets, run a probability-weighted analysis of the 180-day first-filer incentive to determine whether the economic prize is large enough to attract aggressive first-filer challengers.
Investment Strategy. Analysts covering branded pharma should model the IRA’s MFP negotiations as a variable in generic entry probability assessments, not just as a direct revenue headwind. A negotiated MFP that compresses the generic price premium below the typical ANDA-justification threshold for a given market size is a de facto extension of branded pricing power, even without legal exclusivity protection.
Part Five: The Paragraph IV Litigation Gauntlet
How Patent Challenges Work, What They Cost, and How to Read Them
For any branded drug with meaningful commercial sales, a Paragraph IV certification challenge is effectively inevitable. The Hatch-Waxman framework was designed to create this outcome by offering the first-filer a 180-day generic exclusivity period as a reward for successfully challenging a brand’s patents. The financial math is compelling enough that generic companies have built entire business models around identifying and attacking branded drug IP.
A due diligence team that frames PIV risk as ‘possible’ rather than ‘probable’ or ‘certain’ for any commercial-scale asset is making a modeling error. The correct framework is to assess the strength of the brand’s defense, not the likelihood of a challenge.
The Mechanics of the 30-Month Stay
When an NDA holder receives notice of a Paragraph IV certification against any of its Orange Book-listed patents, it has 45 days to file suit in federal district court. Filing suit automatically triggers a 30-month stay on FDA final approval of the ANDA. During those 30 months, the generic cannot enter the market regardless of the scientific merits of its application. For a drug with $1 billion in annual sales, the stay alone preserves roughly $2.5 billion in gross revenue. That is not a side effect of the litigation process; it is a discrete, calculable financial asset. Its value is captured in the brand’s stock price on the day a PIV filing is disclosed, as investors price in the extended exclusivity period the stay guarantees.
The asymmetric financial stakes in PIV litigation are documented in the legal economics literature. A 2020 analysis in the Journal of Law and Economics estimated average brand-side stakes per PIV decision at $4.3 billion versus average generic-side stakes of $204.3 million. This 20-to-1 ratio explains why brand manufacturers invest heavily in litigation strategy and why settlements, which allow both parties to achieve certainty and avoid the winner-take-all outcome of a court decision, are common.
First-Filer Economics: The 180-Day Jackpot
The first generic applicant to file a substantially complete ANDA with a Paragraph IV certification receives 180 days of generic exclusivity upon market entry. During those six months, the first-filer is the only generic competitor. It can price at a 15% to 25% discount to the brand rather than the 80% to 95% discount that arrives when six or more generics compete. For a multi-billion-dollar drug, 180 days of near-duopoly pricing can generate $500 million or more in high-margin revenue for the first-filer. Barr Laboratories’ 2001 fluoxetine launch after winning its PIV challenge to Eli Lilly’s Prozac patents is the canonical example: during its 180-day period, Barr captured the majority of the generic market at a fraction of the price erosion seen in later multi-generic scenarios, and the resulting profitability nearly doubled the company’s gross margin for that period.
This prize drives behavior. It ensures that for any commercially significant drug, at least one generics company will run the financial calculus, determine that the PIV litigation gamble has a positive expected value, and file. The in-licensing team’s job is to evaluate whether, if that challenge succeeds, the rest of the drug’s IP and exclusivity architecture is robust enough to limit the damage.
Inter Partes Review (IPR): The Parallel Attack
Since the America Invents Act of 2011 established the Patent Trial and Appeal Board (PTAB), generic manufacturers have a second litigation track available to them. An IPR petition challenges patent validity before the USPTO itself rather than in federal district court, using a ‘preponderance of the evidence’ standard (rather than the ‘clear and convincing evidence’ standard required to invalidate a patent in district court). This lower evidentiary bar, combined with a technical panel of patent judges rather than a generalist district court judge and jury, has made IPR a powerful tool for challengers. Studies have shown that 60% to 70% of challenged patent claims are either amended or canceled in IPR proceedings.
Generic firms now routinely file IPR petitions in parallel with their district court litigation. A successful IPR on a key patent significantly changes the settlement negotiation dynamics, as a brand with one of its key patents rendered invalid or substantially amended by PTAB has lost a major piece of its bargaining position. Deal teams evaluating older patent portfolios, those filed and granted before 2011 and not yet tested in an IPR, face a different risk profile than those evaluating patents drafted with IPR anticipation in mind. Post-2011 patents are typically prosecuted with IPR-style prior art and claim scope arguments already considered during prosecution, which tends to produce claims more narrowly tailored but more defensible under the IPR standard.
Reading the Innovator’s Litigation DNA
An innovator’s historical patent defense record is among the most useful data inputs in PIV due diligence, and it is systematically underweighted in most standard analyses. There are two dimensions to evaluate.
First, how has the company handled PIV challenges on this specific asset? A drug whose key patents have already been challenged and affirmed valid and infringed in a final court decision has the strongest possible IP validation. That judicial affirmation is an asset with a specific dollar value: it eliminates the uncertainty discount that attaches to untested patents.
Second, how does the company handle PIV challenges across its entire portfolio? A company known for early settlement on unfavorable terms, granting generous ‘authorized generic’ rights to challengers in exchange for peace, is telling you something important about how it will defend your licensed asset. Conversely, a company that has a track record of litigating to the Federal Circuit and winning, investing whatever legal fees are required, is signaling institutional commitment that provides meaningful downside protection to the licensee.
The use of FDA citizen petitions is a related signal. Brand manufacturers file citizen petitions raising scientific objections to pending generic applications, often arguing that the standard bioequivalence framework is inadequate for their product’s complexity. The FDA denies the vast majority of these petitions, and courts have increasingly treated them as delay tactics. But their existence indicates a brand that is willing to use every available tool, legal and regulatory, to delay competition. That posture reduces the licensee’s risk.
‘Soft Landing’ Settlements: Modeling the Controlled Entry
Many PIV cases resolve through negotiated settlement rather than a court decision. Settlements frequently take the form of a ‘pay-for-delay’ or authorized generic arrangement, in which the brand grants the first-filer a limited entry date well in advance of full generic market opening. The Celgene-Revlimid settlement, which allowed specific generic manufacturers to enter with capped volume in 2022 and step up in subsequent years, is a sophisticated version of this structure. Rather than a cliff where brand revenue drops 80% in year one, the agreement created a graduated volume ramp that preserved significant brand-level pricing for several additional years.
For in-licensing deal modeling, the probability of a ‘soft landing’ settlement versus a full generic cliff should be modeled explicitly for each drug’s likely litigation trajectory. Assets with dense patent portfolios and sympathetic ODE protections are more likely to achieve favorable settlement terms, because the generic developer knows the expected value of winning outright is limited by the remaining exclusivity runway. Drugs with a single vulnerable composition patent and no other protections face a genuine binary: win everything or lose everything in litigation.
Key Takeaways: Litigation Risk Assessment
For every in-licensing target with more than $100 million in annual revenue, treat a Paragraph IV challenge as a baseline assumption, not a tail risk. Quantify the value of the 30-month stay as a discrete, near-certain asset and include it explicitly in the deal valuation. Run a patent-vintage analysis to identify which listed Orange Book patents predate the 2011 IPR system and flag them for detailed legal review. Obtain the innovator’s full PIV litigation history across all products, and weight it as a predictor of their likely defense posture on the target asset. For assets with multi-patent portfolios and ODE protection, model the probability and expected terms of a ‘soft landing’ settlement as a distinct revenue scenario in addition to the ‘full defense wins’ and ‘full generic cliff’ base cases.
Part Six: The Integrated Due Diligence Framework
Building the Multi-Factor Risk Assessment
No single data point determines whether a branded drug is a durable in-licensing target. The composition patent might be strong but the ODE is expired. The ODE might be active but the manufacturing complexity is low and a generic developer with deep pockets has already filed. The niche market might naturally deter generics but the regulatory exclusivity has lapsed and the first PIV was filed last quarter. The analytical task is to synthesize all of these factors into a single risk-adjusted view of the asset’s exclusivity durability.
The Multi-Factor Risk Assessment Scorecard provides the structure for this synthesis. It is not a black-box scoring algorithm. It is a disciplined framework that forces the deal team to generate a specific score and specific qualitative notes across every material domain, creating a documented analytical record that can be defended to a deal committee or an investment committee.
The Scorecard Domain Architecture
The scorecard operates across five domains. Patent Fortress covers the composition patent’s remaining PTE-adjusted term, the density and category diversity of secondary patents, the expiration timeline across all listed patents, and the litigation history specific to the asset. Regulatory Moat covers the type and remaining duration of all active FDA exclusivities, including additive pediatric and QIDP extensions. Structural Barriers covers manufacturing complexity category (biologic, complex small molecule, or standard oral solid), API supply chain concentration, and whether the drug has NTI status or complex bioequivalence requirements. Market Dynamics covers annual revenue position relative to the generic entry incentive curve, orphan or niche status, and IRA exposure. Litigation Posture covers the innovator’s defense history across its entire portfolio.
Each factor receives a score from 1 (high risk) to 5 (low risk) and a category weight that reflects its relative importance to the overall durability assessment. The weighted total score is the primary screening metric. Any domain with a score of 1 or 2 should generate a specific investigation task in the legal, technical, or regulatory due diligence workstream, regardless of how high the other domain scores are. A single catastrophic vulnerability, a composition patent with prior art that was never fully examined, a manufacturing process with known cGMP violations, or an ODE that was inadvertently abandoned, can render an otherwise high-scoring asset uninvestable.
Dynamic Scorecard Maintenance
The scorecard must be updated each time material new information becomes available during the due diligence process. An initial review might assign a Patent Fortress score of 4, reflecting a dense and apparently robust portfolio. If subsequent legal review by outside patent counsel identifies a specific prior art reference that one of the key formulation patents did not address during prosecution, and that reference would likely succeed in an IPR petition, the Patent Fortress score drops and the overall durability score changes accordingly. That revised score should immediately trigger a renegotiation of the milestone payment structure linked to patent validity, or a reconsideration of the deal entirely.
This dynamic feedback loop is what separates a real due diligence process from a box-checking exercise. The scorecard is a live document that translates new legal and technical findings into direct consequences for deal economics.
Data Sources and Intelligence Tools
The FDA Orange Book is the baseline source for patent listings, exclusivity types, and approved formulation data. It is freely accessible and searchable, but it captures only patents that the NDA holder has listed, and listing is voluntary for many patent types. Platforms like DrugPatentWatch extend this coverage to unlisted patents, international filings, PCT applications, and European Patent Office records, and provide automated monitoring for new PIV filings and PTAB petitions against specific assets.
ClinicalTrials.gov is the primary source for identifying in-progress next-generation formulation or indication expansion programs that might signal either an ongoing product hop or, conversely, a new clinical indication that could yield additional method-of-use patent protection. Scientific literature searches via PubMed or Embase can surface recent publication of clinical data that either strengthens or weakens the drug’s competitive position relative to emerging alternatives. Market research databases provide commercial forecasts and physician prescribing pattern data that inform the market dynamics portion of the scorecard.
No single tool provides a complete picture. The analytical process that generates genuine insight is one that cross-references patent litigation outcomes with financial disclosures, clinical trial registrations with recent patent filings, and physician prescribing inertia with ODE remaining duration. The synthesis is where the competitive intelligence becomes decision-relevant.
Mandatory External Counsel
The due diligence framework generated by internal analysis and commercial intelligence tools is a screening and prioritization instrument. It is not a legal opinion. Before any material in-licensing transaction closes, two formal external engagements are mandatory.
A patent law firm with pharmaceutical Hatch-Waxman expertise must provide a Freedom-to-Operate (FTO) opinion confirming that the licensee’s manufacturing, marketing, and commercialization activities will not infringe valid third-party patents. The same firm must provide a patent validity and enforceability opinion assessing the defensibility of the target’s own Orange Book patents against anticipated PIV and IPR challenges. These opinions should be based on the complete prosecution history of the patents, not just their claims as issued.
Technical and regulatory due diligence requires a separate engagement with process chemistry and pharmaceutical manufacturing experts who can assess the innovator’s manufacturing facilities and process documentation for cGMP compliance and technology transfer feasibility. Regulatory affairs consultants with NDA review experience should verify the integrity of the clinical data package and identify any unresolved FDA commitments or post-marketing study requirements that represent future cost and risk liabilities.
Key Takeaways: Due Diligence Architecture
Run all five scorecard domains simultaneously, not sequentially. Sequential due diligence delays insights that might have changed the screening decision. Treat any domain score of 1 or 2 as a deal condition that must be resolved or priced into the deal structure before close. Never substitute internal analysis for the FTO and patent validity opinions from external patent counsel. Establish a scorecard update protocol that specifies the conditions under which the deal committee must be reconvened to assess material changes in the risk score, and write that protocol into the deal team’s operating procedures before due diligence begins.
Part Seven: Deal Architecture and Post-Licensing Life Cycle Management
Translating Due Diligence into a Resilient Deal Structure
Due diligence findings have direct and specific implications for deal economics. A high-scoring asset with a PTE-adjusted composition patent running eight more years, an active ODE with four years remaining, complex manufacturing that has already deterred PIV filings, and an innovator with a documented track record of aggressive litigation defense justifies a larger upfront payment and a standard royalty structure. A lower-scoring asset with a vulnerable composition patent, no active regulatory exclusivity, and an innovator known for early settlement requires a fundamentally different payment structure that protects the licensee against the financial consequences of earlier-than-modeled generic entry.
Risk-Adjusted Deal Structures
Tiered royalties, linked to actual market exclusivity status, are the primary risk-transfer mechanism in pharmaceutical licensing. A standard royalty tier applies while the brand maintains full branded market status with no generic competition. A reduced tier activates automatically upon generic entry, sharing the revenue erosion proportionally between licensor and licensee. The royalty reduction percentage and the trigger definition (first generic ANDA approval? first generic commercial launch? generic market share exceeding a threshold?) must be negotiated precisely in the licensing agreement.
Exclusivity-contingent milestone payments defer a portion of the deal’s value to future dates tied to specific IP events. A milestone paid upon the successful defense of the composition patent in PIV litigation, or upon a specific patent’s validity being affirmed by the Federal Circuit, ensures that the licensor receives that value only if the protection it represented as durable actually proves durable. Similarly, a milestone linked to the product remaining generic-free through a specified date ties licensor compensation directly to the outcome the licensee is paying for.
The litigation control clause is among the most operationally critical provisions in any licensing agreement. It must specify: which party controls the patent infringement litigation strategy; how legal costs are shared across the 30-month stay period, district court trial, Federal Circuit appeal, and PTAB proceedings; what level of technical and documentary cooperation the licensor is obligated to provide; and what happens if the licensor decides to settle on terms the licensee considers unfavorable. A licensor that can settle a PIV case on whatever terms it chooses, without the licensee’s consent, holds the power to unilaterally determine when generic competition arrives. That is not an acceptable deal structure.
Royalty stacking provisions protect against a specific risk: the discovery post-close that additional third-party patent licenses are required to commercialize the product without infringement exposure. A royalty stacking clause allows the licensee to reduce the royalty paid to the licensor by a fraction of the additional royalties required, up to a defined cap, preventing the total royalty burden from becoming commercially prohibitive.
Life Cycle Management Begins at Close
Signing the licensing agreement does not pause the competitive clock. The moment the deal closes, the licensee becomes responsible for the ongoing defense and enhancement of the asset’s exclusivity. This requires a LCM plan developed during due diligence, not after, so that the necessary R&D commitments, regulatory strategies, and IP filing programs are funded and staffed from day one.
The first LCM priority is to assess the feasibility of a next-generation formulation program. Can the drug be reformulated as an extended-release product, a fixed-dose combination, a subcutaneous version of an IV product, or a drug-device combination that would generate new patent protection and create the conditions for a product hop? The timeline for this kind of program is typically three to five years for an extended-release reformulation, longer for a drug-device combination requiring device design validation and human factors studies. A program initiated at deal close with an eight-year patent horizon has a realistic chance of generating a patent-protected successor before the original expires.
The second LCM priority is indication expansion. Every approved drug has a label that defines its approved use. Beyond that label lies a set of potential indications that the clinical and scientific literature may support. A new indication, validated in a randomized controlled trial and submitted in a supplemental NDA, generates a new method-of-use patent and a new three-year period of clinical investigation exclusivity. If the new indication qualifies for orphan designation, the licensee also gains seven years of ODE for that indication. Indication expansion is simultaneously a commercial growth strategy and an IP fortification strategy.
Post-marketing data generation is the third priority. Real-world evidence studies, comparative effectiveness analyses, and health outcomes research can document specific advantages of the branded product versus its generic alternative in terms of formulation consistency, patient adherence, or clinical outcomes in narrow patient subgroups. This data does not prevent generic entry, but it gives payers, pharmacy benefit managers, and clinicians a clinical rationale for maintaining branded product on preferred formulary tiers even after generic entry, which reduces market share erosion relative to what purely price-driven substitution would produce.
Portfolio Construction: The Strategic Synthesis
No individual in-licensing deal operates in isolation. Each asset should be evaluated not only on its standalone durability profile but also on its contribution to a diversified portfolio that balances risk across exclusivity types, market sizes, therapeutic areas, and litigation exposure timelines. A portfolio that consists entirely of primary-care blockbusters approaching patent cliffs is maximally exposed to the Paragraph IV ecosystem. A portfolio balanced across orphan disease assets with ODE protection, complex biologics with BPCIA exclusivity and high biosimilar development costs, and two or three primary-care assets with strong litigation-tested composition patents is substantially more durable in aggregate.
The data on in-licensing’s role in portfolio construction is unambiguous. As of 2025, 68% of blockbuster pharmaceutical products originated from external licensing deals rather than purely in-house discovery. In-licensing is not a supplement to internal R&D; it is the primary channel through which late-stage commercial assets reach the market for most mid-size and large pharma companies. The analytical rigor applied to in-licensing decisions is therefore among the highest-leverage activities in pharmaceutical business development.
Key Takeaways: Deal Structure and LCM
Price risk explicitly into deal economics by using tiered royalties, exclusivity-contingent milestones, and a clearly defined litigation control clause. Never allow a licensor to settle PIV litigation unilaterally without licensee consent or at minimum, without a defined process for licensee participation. Develop the LCM plan during due diligence, before deal close, and fund it at day one rather than treating it as a future initiative. Prioritize next-generation formulation programs and indication expansion as the two highest-return LCM investments for any asset with an eight-plus-year exclusivity runway. Evaluate every in-licensing opportunity against the existing portfolio’s risk concentration profile, not only on its standalone merits.
Investment Strategy. For institutional investors in pharmaceutical companies, the sophistication of a company’s in-licensing due diligence and LCM execution is a durable source of alpha that is not fully captured in near-term earnings models. A company that consistently identifies durable assets, structures deals with appropriate risk-sharing provisions, and executes LCM programs that produce next-generation product launches compounds its portfolio value in ways that become visible only over multi-year holding periods. These capabilities are disclosed implicitly in the structure of deals announced, the track record of managed patent cliffs, and the frequency with which in-licensed assets generate LCM-driven line extensions. Analysts should build these as distinct evaluation criteria in their company-level research frameworks.
Conclusion: The Competence Is in the Framework
The pharmaceutical in-licensing decision is not a single judgment call. It is the output of a systematic process that generates a clear, documented view of an asset’s exclusivity durability across legal, regulatory, structural, and market dimensions. The companies that execute this process well, building the analytical infrastructure, engaging the right legal and technical counsel, and pricing risk into deal structures with precision, consistently outperform those that treat in-licensing as a qualitative bet on a commercial opportunity.
The framework presented here is designed to make that process explicit and repeatable: patent analysis grounded in PTE-adjusted term calculations and IP valuation methods; regulatory exclusivity modeling that treats ODE and BPCIA protection as distinct, non-overlapping cash flow assets; structural barrier assessment that distinguishes between legal protections that can be challenged and technical barriers that simply exist; market economics analysis that accounts for the generic entry incentive curve and the IRA’s counterintuitive effect on competition; and litigation risk assessment that prices the 30-month stay as an asset and reads the innovator’s corporate DNA as a predictor of defense posture.
A drug protected by a dense patent thicket, active ODE protection, a biologic manufacturing process no competitor has yet replicated, and an innovator with a documented record of litigating PIV challenges to the Federal Circuit is not just commercially attractive today. It is the closest thing to a durable, long-term revenue-generating asset that the pharmaceutical industry can produce. Finding those assets, understanding why they are durable, and structuring deals that capture that durability without overpaying for it, is the competence that separates world-class pharmaceutical business development from the rest.