The single most valuable regulatory asset in the U.S. generic pharmaceutical industry is not a patent. It is the absence of competition for exactly 180 days. That window, created by the 1984 Hatch-Waxman Act and refined by the 2003 Medicare Modernization Act (MMA), concentrates the bulk of a generic product’s lifetime profit into six months. Companies that execute flawlessly during that window can generate returns that fund the next five years of pipeline investment. Companies that stumble, through operational failure, forfeiture, or a poorly negotiated settlement, watch hundreds of millions in projected revenue evaporate.
This pillar page is a comprehensive operational and strategic reference for generic pharmaceutical IP teams, ANDA portfolio managers, business development leads, and institutional analysts who cover the sector. It deconstructs the Hatch-Waxman regulatory architecture, maps every forfeiture tripwire with mitigation tactics, quantifies the first-mover financial premium with granular market data, dissects the authorized generic (AG) threat and post-‘Actavis’ settlement mechanics, and extracts actionable lessons from the Ranbaxy/Teva atorvastatin disaster and Mylan’s EpiPen AG maneuver. Where specific drugs and corporate actors appear, this analysis extends into IP valuation, because the patent portfolio is not background context; it is the core asset being contested.
Part I: The Regulatory Architecture of Generic Competition
What the Hatch-Waxman Act Actually Did
The Drug Price Competition and Patent Term Restoration Act of 1984 resolved a market failure that had persisted since the Federal Food, Drug, and Cosmetic Act first required clinical proof of safety and efficacy. Before 1984, a generic manufacturer had to run its own full clinical trial program even when the active ingredient was identical to an already-approved reference product, a scientific redundancy that made generic entry prohibitively expensive. The Act eliminated that requirement, allowing generics to demonstrate bioequivalence to a Reference Listed Drug (RLD) rather than repeat the innovator’s clinical work.
The tradeoff for innovators was twofold. Patent term restoration under 35 U.S.C. 156 compensates for time lost during FDA review, up to five years of restoration with a post-restoration term cap of 14 years from approval. Hatch-Waxman also created a five-year data exclusivity period for New Chemical Entities (NCEs), blocking ANDA submissions entirely for that window regardless of patent status. These provisions were designed to preserve R&D incentive by guaranteeing innovators meaningful time in market before generic entry.
The numbers validate the framework’s effect on access. In 1984, generics held 19% of prescription volume in the United States. By 2024 that share exceeded 90%. The Association for Accessible Medicines calculated that first generics alone generated nearly $20 billion in healthcare savings in 2020, a figure that excludes the downstream savings from subsequent competitive entrants. But those numbers obscure how unevenly the value of generic entry is distributed across time: the overwhelming majority of the economic prize goes to the company that moves first.
The ANDA Pathway: Mechanics and Cost Structure
The Abbreviated New Drug Application (ANDA) is the operational backbone of the generic industry. Where a full New Drug Application (NDA) requires phase I, II, and III clinical trials that routinely cost $800 million to $2.6 billion and take ten or more years, an ANDA requires bioequivalence studies that typically cost $1 million to $4 million and can be completed in two to three years. The core standard is rate and extent of absorption: the generic must demonstrate that its pharmacokinetic profile, measured by area under the curve (AUC) and maximum concentration (Cmax), falls within the FDA’s 80-125% confidence interval relative to the RLD.
For most oral solid dosage forms, this is a well-characterized process. The complexity scales sharply for complex generics: locally-acting drugs like inhaled corticosteroids or topical dermatologics require product-specific bioequivalence guidance because systemic pharmacokinetics do not adequately predict local drug delivery. Injectable depots, liposomal formulations, and transdermal systems present similar challenges. The FDA’s Product-Specific Guidance (PSG) database, which now covers over 1,700 reference products, is the primary technical roadmap for ANDA formulation development, and a company’s ability to read and execute on a PSG is a direct competitive differentiator.
The Orange Book: IP Inventory and Strategic Weapon
The FDA’s ‘Approved Drug Products with Therapeutic Equivalence Evaluations’, known universally as the Orange Book, is a dual-function document. Publicly, it is a database of FDA-approved drug products with therapeutic equivalence ratings that enable pharmacist substitution. Strategically, it is the IP battleground where innovators declare their patent positions and generic challengers identify attack vectors.
NDA holders must list all patents claiming the drug substance (active ingredient), drug product (formulation or composition), or method of use. Process patents are explicitly excluded from Orange Book listing under 21 U.S.C. 355(b)(1). This exclusion matters: a process patent not listed in the Orange Book can still be asserted in district court but cannot trigger the 30-month stay mechanism, reducing its tactical value as a delay instrument. Brand companies have repeatedly pushed the boundaries of what qualifies as a ‘drug product’ patent, listing packaging, metabolite, and enantiomer patents, sometimes successfully, sometimes not. The FDA’s listing standard requires only that the company certify the patent claims the drug product or method of use for which approval is sought, a relatively low bar that has led to Orange Book inflation.
For generic challengers, the Orange Book listing is the starting inventory for freedom-to-operate (FTO) analysis. Every listed patent requires a certification, and every certification choice carries different commercial and legal consequences.
The Four Patent Certifications: Strategic Implications
An ANDA filer must certify to each Orange Book-listed patent under one of four paragraphs of 21 U.S.C. 355(j)(2)(A)(vii).
A Paragraph I certification states that no patent has been filed for the RLD. A Paragraph II certification states the relevant patent has expired. Both allow the FDA to approve the ANDA on its scientific merits without triggering patent litigation. A Paragraph III certification commits the applicant to a delayed market entry date equal to the patent expiration, which is the lowest-risk path but forfeits any claim to 180-day exclusivity and hands the full remaining patent term to the brand company.
The Paragraph IV (P-IV) certification is the operative mechanism for accessing exclusivity. It asserts that the listed patent is invalid, unenforceable, or will not be infringed by the proposed generic. This is not a mere procedural declaration; under 35 U.S.C. 271(e)(2), the filing of an ANDA with a P-IV certification constitutes a technical act of patent infringement, giving the brand manufacturer immediate standing to sue in federal district court. The generic company is challenging the validity or scope of a granted patent before making a single commercial sale, accepting that exposure to full patent litigation is the cost of admission to the exclusivity race.
A fifth certification type, the ‘Section viii’ carve-out or ‘method-of-use’ carve-out, allows a generic to file without a P-IV if it simply excludes from its labeling the patented method of use. This avoids litigation on that use patent but limits the generic’s labeling, which can restrict formulary positioning if major indications are carved out. Brand companies have extended Orange Book listings specifically to foreclose the section viii option.
Key Takeaways: Regulatory Architecture
The Hatch-Waxman Act is a deliberate incentive structure, not just a regulatory framework. The ANDA pathway makes generic entry scientifically cheap but legally expensive. The Orange Book converts patent portfolios into public declarations of IP scope. The P-IV certification is the only mechanism that unlocks 180-day exclusivity, and its filing is simultaneously the opening shot in federal patent litigation. Generic companies that treat the regulatory and legal tracks as separate workflows almost always lose to those that run them as a single integrated campaign.
Part II: The Paragraph IV Race: Filing Mechanics and the First-to-File Standard
What ‘First Applicant’ Actually Means
The 180-day exclusivity reward goes to the ‘first applicant,’ defined under 21 U.S.C. 355(j)(5)(B)(iv) as any applicant that submitted a substantially complete ANDA containing a P-IV certification on the first day that any such application was submitted. The word ‘any’ in the statute is load-bearing: if two companies file on the same day, both qualify as first applicants and share the exclusivity. If three companies file on Day 1 and a fourth files on Day 2, the fourth is categorically excluded from the exclusivity benefit regardless of the quality of its scientific package.
The FDA has published detailed guidance on same-day filing scenarios. In cases where multiple applicants share first-applicant status, each holds a blocking right: one company’s exclusivity is not triggered until it launches or forfeits, and during that period, subsequent applicants cannot receive final approval. This creates a coordination problem when multiple first applicants settle with the brand at different times, sometimes leaving an exclusivity block in place that delays patient access without conferring commercial benefit on anyone.
The ‘Substantially Complete’ Standard and Refuse-to-Receive Risk
‘Substantially complete’ is an FDA term of art that operates as a de facto quality gate on first-applicant status. A substantially complete ANDA is one that contains bioequivalence data, a complete chemistry, manufacturing, and controls (CMC) section, a signed application form, patent certifications for every listed patent, and all other information required by 21 C.F.R. Part 314. An ANDA that the FDA refuses to receive (RTR) is not considered ‘submitted’ for purposes of establishing the filing date.
This creates a straightforward but consequential failure mode. A company that rushes an ANDA to beat a competitor to the first-applicant date, but submits a package with material deficiencies, may receive an RTR letter while the competitor’s complete application goes through. The competitor becomes the sole first applicant with no shared exclusivity obligation. Quality and speed are not competing priorities in this context; they are jointly necessary conditions.
The FDA also has the authority to deem an ANDA ‘withdrawn’ if an applicant fails to meet certain ongoing requirements after submission, including failure to respond to a Complete Response Letter (CRL) within the required timeframe. A deemed-withdrawn ANDA can trigger the forfeiture provisions discussed in Part IV.
The Paragraph IV Notice Letter: Laying Your Hand on the Table
Within 20 days of FDA acceptance of an ANDA containing a P-IV certification, the applicant must send a notice letter to the NDA holder and patent owner. The notice letter is a legally mandated disclosure of the generic company’s invalidity or non-infringement arguments. Under 21 C.F.R. 314.52(c), it must include a detailed statement of the factual and legal basis for the opinion that the patent is invalid, unenforceable, or not infringed.
In practice, a well-drafted P-IV notice letter runs 30 to 100 pages and constitutes the opening brief in what will become a multi-year patent dispute. It must address claim construction, prior art for invalidity arguments, and the specific structural or functional differences between the proposed generic and the claimed invention for non-infringement arguments. Courts have found that an inadequate notice letter can defeat first-applicant status entirely. In ‘Teva Pharmaceuticals USA v. Sebelius’ (D.D.C. 2009), the court evaluated whether a notice letter provided sufficient detail to start the brand’s 45-day clock. Generic companies that treat the notice letter as a formality rather than a legal brief take on avoidable risk.
The 45-Day Window and the 30-Month Stay: The Delay Mechanism
The brand company has 45 days from receipt of the notice letter to file a patent infringement lawsuit. Filing within that window triggers an automatic 30-month stay on FDA final approval of the ANDA under 21 U.S.C. 355(j)(5)(B)(iii). The stay runs from the date the brand received the notice letter, not from the filing of the lawsuit.
The 30-month stay was conceived as a safe harbor for litigation, a protected period during which courts could adjudicate the patent dispute before a generic entered the market. Its actual function is frequently more mechanical than judicial. Brand companies routinely file infringement suits within the 45-day window regardless of their patent’s underlying strength, because the stay itself is worth hundreds of millions of dollars in continued monopoly revenue independent of any litigation outcome. An FDA analysis of Paragraph IV litigation found that a substantial proportion of stays expire before the underlying litigation concludes, confirming that the stay operates as a standalone delay instrument rather than purely as litigation protection.
Congress addressed this in the 2003 MMA by limiting the number of 30-month stays to one per patent, eliminating the pre-MMA practice of ‘daisy-chaining’ successive stays by listing new patents in the Orange Book after an ANDA was filed.
Key Takeaways: Filing Mechanics
First-applicant status is won or lost on process discipline, not scientific merit alone. A complete, high-quality ANDA filed on the critical date beats a scientifically superior package filed one day later. The notice letter is a legal document, not a courtesy, and inadequate notice letters have cost generic companies their exclusivity. The 30-month stay is a reliable, legally mandated delay instrument for brand companies; generic challengers must build stay duration into their financial models as the most probable scenario, not an outlier.
Part III: Quantifying the 180-Day Financial Premium
Market Share Dynamics: Why the First Position Is Durable
The economic case for pursuing 180-day exclusivity rests on one empirical finding: the first generic to market captures market share that is disproportionate to its period of exclusivity and that decays far more slowly than intuition suggests. Data published by the Association for Accessible Medicines and corroborated by FDA analyses shows first movers achieving up to 90% market share advantage over later generic entrants measured across the product’s full commercial life. The first entrant holds approximately an 80% share advantage over the second generic to enter, and roughly 225% over the third.
The durability of this advantage reflects several compounding factors. Pharmacies and pharmacy benefit managers (PBMs) establish preferred supplier agreements during the exclusivity period when there is no alternative generic source. Drug utilization patterns shift during that window: physicians and pharmacists substitute from brand to the first generic, and patients refill on that product. Switching costs for subsequent entrants are real: convincing a chain pharmacy to replace an established generic supplier involves contract renegotiation, formulary paperwork, and inventory disruption that most procurement managers prefer to avoid absent a meaningful price incentive.
Generic atorvastatin (Lipitor) illustrates the magnitude at scale. Atorvastatin was the highest-grossing drug in pharmaceutical history before its November 2011 patent expiration, generating approximately $13 billion in annual U.S. brand sales. Ranbaxy’s first-generic launch captured over 70% of the genericized atorvastatin market within weeks, a share that partially eroded only after Ranbaxy’s manufacturing problems forced a production halt and gave other entrants an opening.
The Pricing Window: Duopoly Economics and Margin Structure
During the 180-day exclusivity period, the market structure for the drug in question converts from a brand monopoly to a duopoly or, when the brand launches an authorized generic simultaneously (discussed in Part V), a triopoly. This structure allows the first-filer to price at a meaningful discount to the brand, typically 15-25% below brand WAC, while capturing the vast majority of prescriptions that payers and PBMs redirect from brand to generic. The financial result is the capture of high volume at margins that are radically better than post-Day-181 market conditions.
Industry analysis consistently places 60-80% of a generic product’s total lifetime profit within the first 180 days. For a brand with $1 billion in annual U.S. sales, the first-generic exclusivity window can generate $200-400 million in gross profit for the first-filer, depending on the presence or absence of an authorized generic. For blockbuster brands with multi-billion-dollar sales, the numbers scale proportionally, which is why Paragraph IV challenges against drugs like atorvastatin, esomeprazole, and clopidogrel attracted five, seven, or more simultaneous first-day filers.
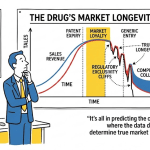
The Day 181 Cliff: Quantifying Price Erosion by Competitor Count
On Day 181, the FDA is free to grant final approval to all other pending ANDAs for the same drug. The influx of multiple generic suppliers triggers rapid, severe price competition. The HHS ASPE analysis of generic drug market entry established the following price reduction benchmarks relative to brand price:
| Number of Generic Competitors | Average Price vs. Brand | Notes |
|---|---|---|
| 1 (Exclusivity Period) | ~61% of brand price (39% discount) | Duopoly or triopoly if AG present |
| 2 competitors | ~46% of brand price (54% discount) | Post-exclusivity early entry |
| 3-5 competitors | ~30% of brand price (~70% discount) | Rapid commoditization phase |
| 6+ competitors | Below 5% of brand price (>95% discount) | Full commodity market |
These figures explain why the first-mover’s revenue advantage over second and third entrants is so large: by the time later entrants launch, market price has often dropped below their cost of goods, particularly for foreign API-sourced small molecules where the cost floor is very low but not zero. The Day 181 cliff is not gradual; ANDAs are approved in batches and multiple new entrants often hit the market simultaneously, compressing the erosion timeline.
IP Valuation: The Patent Portfolio as Core Asset
Any financial model of 180-day exclusivity must begin with an IP valuation of the brand’s patent position. The commercial value of first-generic exclusivity is directly tied to the duration and enforceability of the patents being challenged: a company that successfully invalidates a primary compound patent with eight years remaining captures a fundamentally different prize than one that challenges a method-of-use patent with two years remaining on a drug already genericized in three European markets.
The key IP valuation inputs for a P-IV target are: patent expiration date (adjusted for any term restoration under 35 U.S.C. 156), patent scope relative to the proposed generic formulation, litigation history and claim construction rulings in prior cases, and the Orange Book listing’s relationship to actual commercial embodiments of the brand product. A narrow compound patent that fails to capture all clinically relevant polymorphs is a weaker target than a broad claim, but it may be easier to design around. A formulation patent with explicit working examples closely matching the brand’s commercial product is likely to be litigated aggressively and is less likely to settle early.
For portfolio managers evaluating generic companies, the IP attack portfolio, the collection of P-IV challenges currently in litigation or filed, is the primary driver of earnings optionality. A company with three or four high-quality first-applicant positions against blockbuster drugs represents a materially different risk-adjusted earnings profile than one with a larger number of lower-value challenges. The challenge-to-revenue conversion rate, the fraction of filed P-IVs that result in a launched exclusivity period, is a key operating metric that institutional analysts should track alongside pipeline metrics like FDA approval rates.
Investment Strategy: Paragraph IV as an Asset Class
Institutional investors can extract measurable alpha from tracking Paragraph IV filings against drugs approaching primary patent expiration. The filing of a P-IV challenge is public information, disclosed in the brand company’s SEC filings upon receipt of the notice letter (brand companies are required to disclose material litigation). For generic company shareholders, first-applicant status on a high-revenue drug is a binary option: the upside (successful launch, hundreds of millions in exclusivity revenue) is large relative to the downside (litigation loss, with the main cost already sunk in ANDA development and legal fees).
Key signals to monitor: the volume and quality of P-IV filers against a specific RLD; the speed of district court litigation; the presence or absence of a consent judgment or settlement; and the brand’s public disclosures about authorized generic plans. An AG commitment in a settlement agreement fundamentally changes the first-filer’s revenue model and should be reflected in any earnings estimate.
Key Takeaways: Financial Quantification
The 180-day exclusivity period is where generic pharmaceutical economics concentrate. First movers capture 60-80% of a product’s lifetime gross profit in six months. Price erosion post-Day-181 is rapid and severe, dropping to less than 5% of brand price once six or more competitors enter. The brand’s patent portfolio is the primary driver of exclusivity value, and IP valuation, including patent scope, expiration, and prior litigation outcomes, should precede any commercial projection. For investors, first-applicant positions against high-revenue brands are material, quantifiable assets that can be tracked through public disclosures.
Part IV: The Forfeiture Minefield
Why the MMA 2003 Forfeiture Provisions Exist
Before the 2003 Medicare Modernization Act, the 180-day exclusivity structure had an exploitable flaw: a first-applicant generic could file a P-IV challenge, secure first-applicant status, settle with the brand for a delayed entry date, and thereby hold a blocking position that prevented any subsequent generic from receiving FDA approval indefinitely. This ‘exclusivity parking’ kept markets closed to cheaper generic competition while the first-filer collected settlement value without actually marketing its product.
Congress responded with six specific forfeiture triggers under 21 U.S.C. 355(j)(5)(D)(i). Triggering any one of them strips the first applicant of its 180-day exclusivity, allowing the FDA to approve subsequent ANDAs. The forfeiture provisions are the most complex and consequential provisions in the exclusivity framework, and misreading them is among the most expensive mistakes a generic company can make.
Forfeiture Trigger 1: Failure to Market
Failure to Market is the most commonly triggered forfeiture event. The statute requires the first applicant to begin commercial marketing by the later of two ‘bookend’ dates. The first is 75 days after the first applicant receives final FDA approval or 30 months after it receives tentative approval, whichever is earlier. The second is 75 days after a final court decision finding all relevant patents invalid, unenforceable, or not infringed, or 75 days after a district court consent judgment to that effect.
The complexity lies in the word ‘later.’ For a drug with multiple listed patents in different litigation postures, the triggering bookend date requires careful legal analysis. Companies that receive final approval but are waiting for appellate resolution of a patent dispute face the starkest version of this problem: they must decide whether to launch at risk before the appeal concludes or risk triggering the failure-to-market forfeiture if the bookend date passes while they wait.
Mitigation requires launch readiness infrastructure maintained on a live basis, not built from scratch when approval arrives. Commercial inventory, distribution agreements, PBM contracts, and pharmacy stocking programs must be executable within days of approval, not weeks or months.
Forfeiture Trigger 2: Withdrawal of Application
If the first applicant withdraws its ANDA, or if the FDA deems it withdrawn for failure to respond to an FDA request within the required timeframe, exclusivity is forfeited. The ‘deemed withdrawn’ mechanism is the more dangerous variant: a slow-moving regulatory affairs function that misses a CRL response deadline can trigger forfeiture without any affirmative decision by the company. Integrated project management linking regulatory timelines to commercial planning is the operative mitigation.
Forfeiture Trigger 3: Amendment of Certification
If the first applicant amends or withdraws its P-IV certification for all patents that qualified it for first-applicant status, exclusivity is forfeited. The critical word is ‘all.’ If a first applicant filed P-IVs against three listed patents, losing litigation on two and changing those certifications to Paragraph III does not forfeit exclusivity as long as the P-IV on the third patent is maintained. This creates an asymmetric incentive to preserve at least one P-IV certification regardless of litigation outcomes on other patents.
The practical implication: when structuring a settlement with the brand, a generic company must analyze which P-IV certifications anchor its first-applicant status and avoid settling on terms that require amendment of all qualifying certifications. Some settlements have included explicit provisions where the generic amends all certifications and receives a specified entry date directly from the brand, functionally trading exclusivity for settlement value. The FTC has characterized some of these arrangements as potential antitrust violations.
Forfeiture Trigger 4: Failure to Obtain Tentative Approval
The FDA must grant tentative approval to the first applicant’s ANDA within 30 months of the application’s submission date, or exclusivity is forfeited. Tentative approval signifies that the ANDA meets all FDA requirements except for those that cannot be finalized before the expiration of the 30-month stay or other blocking exclusivity.
Failure to achieve tentative approval within 30 months is typically caused by manufacturing quality issues, incomplete or deficient CMC data, or unresolved bioequivalence questions. The FDA will accept a ‘review-ready’ ANDA that front-loads all necessary data, but an application that requires multiple amendment cycles can run out of time. Regulatory affairs teams must build tentative approval probability into the P-IV commercial model and trigger internal escalation procedures when FDA information requests suggest the 30-month deadline is at risk.
Forfeiture Trigger 5: Antitrust Violation
If the FTC or DOJ finds that the first applicant entered into an agreement that violates antitrust laws, exclusivity is forfeited. This provision was added to address reverse payment settlements but is written broadly enough to cover any agreement that regulators characterize as exclusivity parking. Post-‘FTC v. Actavis’ (2013), all settlement agreements between brand and generic companies in P-IV litigation carry antitrust risk and require explicit legal review under the ‘rule of reason’ standard before execution.
Forfeiture Trigger 6: Patent Expiration
If all patents that formed the basis of first-applicant status expire before the exclusivity period is triggered, the exclusivity is forfeited. This provision primarily affects challenges where the patent at issue has a near-term expiration and the litigation runs past that date. It creates an incentive to prioritize challenges against patents with longer remaining terms, both because the commercial value of early generic entry is higher and because the expiration forfeiture risk is lower.
Forfeiture Risk Summary Table
| Forfeiture Event | Primary Cause | Mitigation Priority |
|---|---|---|
| Failure to Market | Delay in commercial launch readiness | Build launch infrastructure in parallel with litigation |
| Withdrawal of Application | Missing FDA response deadlines | Dedicated regulatory timeline monitoring |
| Amendment of Certification | Settling all qualifying P-IV certifications | Structure settlements to retain at least one qualifying P-IV |
| Failure to Obtain Tentative Approval | Manufacturing or CMC deficiencies | Submit review-ready ANDA; escalate FDA requests early |
| Antitrust Agreement | Reverse payment or no-AG settlement | Mandatory antitrust review of all settlement terms |
| Patent Expiration | Litigation extends past patent expiry | Prioritize challenges against longer-dated patents |
Key Takeaways: Forfeiture
The six forfeiture provisions are the operational risk layer of the 180-day exclusivity framework. Companies that fail to market on time, miss FDA deadlines, improperly structure settlements, or challenge dying patents lose exclusivity they spent years and millions of dollars acquiring. Every forfeiture trigger has a corresponding mitigation tactic, but mitigation requires proactive planning, not reactive response. The failure-to-market provision is the most frequently triggered and the most preventable.
Part V: The Brand’s Countermove: Authorized Generics, No-AG Agreements, and Post-‘Actavis’ Settlements
The Authorized Generic: Mechanism and Market Impact
An authorized generic (AG) is a version of the brand-name drug distributed under the brand company’s existing NDA, without the brand name on the label and typically at a lower price. Because it is licensed under the NDA rather than approved through an ANDA, it is not subject to the 180-day exclusivity block. The brand can launch an AG on the same day the first-filing generic enters the market, immediately converting the expected duopoly into a three-player market.
The FTC’s 2011 comprehensive study on authorized generics remains the most rigorous analysis of AG market effects. The FTC found that AG competition during a first-filer’s 180-day period reduces the first-filer’s revenues by 40-52% on average. Retail prices are 4-8% lower and wholesale prices are 7-14% lower when an AG is present. The FTC noted that despite this revenue impact, the total volume of P-IV challenges had not measurably declined, suggesting that generic companies discount the AG threat or expect to recover enough volume to justify the challenge even with an AG present.
The AG is typically marketed through a subsidiary or a separate marketing agreement, allowing the brand to capture revenue at a generic price point without formally reducing brand WAC, which would affect PBM rebate calculations tied to brand pricing. Pfizer used this structure for Lipitor: it authorized a generic through Greenstone, its generic subsidiary, simultaneously with Ranbaxy’s launch, ensuring that Pfizer retained economic interest in the atorvastatin market regardless of which generic supplier dominated pharmacy shelves.
The Greenstone/Atorvastatin AG: IP Valuation in Practice
Pfizer’s Orange Book position on atorvastatin at the time of patent expiration included a compound patent (U.S. Patent No. 4,681,893, claiming the atorvastatin molecule, expired November 2011), a crystalline form patent (U.S. Patent No. 5,969,156, claiming the hemicalcium salt form, expiration contested and ultimately resolved in Ranbaxy’s favor through litigation), and formulation patents covering the commercial tablet. The compound patent was the primary barrier; its expiration opened the market. The crystalline form patent was Ranbaxy’s primary litigation target and the central IP asset at risk.
The valuation of Pfizer’s exclusivity position at atorvastatin patent expiry was approximately $4-5 billion in annual U.S. brand sales. Greenstone’s AG captured roughly 30% of the generic atorvastatin market during the Ranbaxy exclusivity period. This outcome, loss of 30% of the genericized market to an AG while also managing a manufacturing recall, reduced Ranbaxy’s actual exclusivity period revenue to well below projections. The Greenstone AG was not a defensive measure; it was an offensive income preservation strategy that Pfizer had prepared years before the patent expiration.
The No-AG Agreement: Exclusivity by Contract
The no-AG agreement is the most significant post-‘Actavis’ settlement innovation. In a no-AG agreement, the brand company contractually commits not to launch its own authorized generic during the first-filer’s 180-day exclusivity period. In exchange, the generic company typically agrees to a delayed market entry date relative to what a patent invalidation verdict would have allowed.
The FTC has treated no-AG agreements as a form of payment warranting antitrust scrutiny. The economic logic is direct: an AG reduces first-filer revenues by 40-52%, so a promise of no AG is worth, in the FTC’s estimate, hundreds of millions of dollars on high-revenue drugs. When a brand pays that promise in exchange for a delayed entry date, the economic structure mirrors a reverse cash payment, which ‘Actavis’ held subject to rule-of-reason antitrust review.
A 2025 Health Affairs study found that the prevalence of no-AG commitments in Paragraph IV settlements has been declining since approximately 2020, as generic companies and brand companies have both internalized the antitrust risk of explicit no-AG terms. Some settlements now use ‘most favored entry’ clauses instead, which guarantee the first-filer a specified launch date without an explicit no-AG commitment. The FTC has begun scrutinizing these structures as well.
‘FTC v. Actavis’: What the Decision Actually Held
The 2013 Supreme Court decision in ‘FTC v. Actavis, Inc.’ addressed a settlement in the AndroGel (testosterone gel) P-IV litigation in which AbbVie and Besins Healthcare agreed to pay Actavis and other generic companies substantial sums in exchange for delayed generic entry. The FTC challenged the arrangement under Section 5 of the FTC Act.
The Court’s holding, written by Justice Breyer in a 5-3 decision, rejected the ‘scope of the patent’ test that several circuit courts had applied. That test held that settlement agreements were per se lawful as long as the delayed entry date did not exceed the patent’s remaining term, reasoning that the patent holder was simply enforcing rights it already had. The Court found instead that large, unexplained reverse payments create an inference of anticompetitive harm sufficient to trigger rule-of-reason analysis. The patent’s existence does not immunize the agreement from antitrust scrutiny.
Critically, the Court did not hold reverse payment settlements per se illegal, nor did it require that they be proven unlawful by the FTC. It sent the case back for rule-of-reason analysis in which the FTC would need to demonstrate anticompetitive effects. In practice, ‘Actavis’ made explicit cash reverse payments from brand to generic nearly extinct in new settlements, while creating substantial ambiguity about the permissibility of non-cash forms of compensation.
Crafting Compliant Settlement Structures Post-‘Actavis’
Legal counsel advising on P-IV settlement structure must now work within a framework where any form of value transfer from brand to generic, including no-AG commitments, co-promotion rights, API supply agreements at below-market prices, or licensing fees, can be characterized as a reverse payment subject to antitrust scrutiny.
The compliance framework requires demonstrating that any value transfer is legitimately attributable to a business rationale independent of delayed entry. An API supply agreement at fair market prices survives scrutiny. A co-promotion deal at economic terms consistent with market rates survives. A no-AG commitment paired with a multi-year entry delay is at high risk. Settlement counsel should document the business rationale for each element of the agreement contemporaneously and avoid structuring terms in ways that are most naturally explained by their delay effect rather than their independent commercial value.
Key Takeaways: AGs and Settlements
The authorized generic is the brand company’s most effective single countermeasure to 180-day exclusivity. It requires no FDA action, can launch the same day as the first-filer, and cuts first-filer revenues by 40-52% on average. No-AG agreements are the primary negotiated protection against this threat, but they carry antitrust risk under ‘FTC v. Actavis’ when paired with delayed entry commitments. Post-‘Actavis’ settlements require contemporaneous business-rationale documentation for every value element. Companies that build AG probability assumptions into their exclusivity revenue models perform systematically better than those that model a clean duopoly.
Part VI: The Strategic Launch Playbook
Phase 1: Target Identification and Portfolio Strategy
A disciplined P-IV program begins with the selection of targets that meet a coherent set of financial, legal, and operational criteria. The commercial threshold is brand sales sufficient to generate a meaningful return after litigation costs of $5-15 million per case and ANDA development costs of $1-5 million for a typical oral solid. As a practical floor, most generic companies require $250-500 million in annual brand U.S. sales to justify a contested P-IV challenge. Below that level, the risk-adjusted return is frequently insufficient relative to the company’s cost of capital.
The legal threshold is a patent position that has identifiable vulnerabilities: prior art that anticipates or renders obvious key claims, a claim scope that the proposed formulation can design around, or a history of inconsistent claim construction in prior litigation. A patent with a strong record, especially one that has survived prior P-IV challenges and been upheld in inter partes review (IPR) at the Patent Trial and Appeal Board (PTAB), should be viewed with appropriate skepticism regardless of its commercial appeal.
The competitive threshold is a race landscape that is not so saturated that the exclusivity economics collapse before launch. A drug that attracts 15 simultaneous first-day filers is not necessarily more valuable than one that attracts three; it may simply be more widely recognized as attractive, with more parties sharing exclusivity and more AGs in play by the time litigation resolves.
Evergreening and Its Implications for P-IV Target Selection
Brand companies use patent evergreening to extend effective market exclusivity beyond the primary compound patent. Common mechanisms include: extended-release formulation patents covering a new dosage form, polymorph or salt form patents covering the specific crystalline structure of the commercial product, enantiomer patents where a racemic drug has been separated into its active enantiomer, metabolite patents covering the active metabolite of a prodrug, and pediatric exclusivity, which adds six months to all patent protections when the brand conducts FDA-requested pediatric studies.
For P-IV challengers, evergreening creates a layered patent landscape that must be navigated with precision. A challenge to the compound patent alone may leave secondary patents in place that restrict the generic’s ability to match the brand’s market-leading formulation, particularly for extended-release products where the patent-protected delivery mechanism is central to clinical positioning. A full P-IV strategy maps the entire Orange Book listing for the target drug, identifies which patents can be challenged, which can be designed around through section viii carve-outs, and which represent genuine blocking barriers that require litigation.
Pediatric exclusivity deserves special attention because it is not a patent and cannot be challenged through ANDA proceedings. It attaches to all Orange Book-listed patents and must be modeled as a fixed delay on top of any patent challenge timeline. A successful P-IV challenge that resolves two years before the compound patent expiration, combined with six months of pediatric exclusivity, gives the first-filer an entry date that is 18 months ahead of secondary-patent expiration but potentially only months ahead of subsequent generic entrants if other patents create no further obstacles.
Building the Legal Case: FTO Analysis and Litigation Strategy
Freedom-to-operate analysis for a P-IV target requires a structured evaluation of each listed patent across three analytical dimensions. First, claim construction: what do the claims actually cover when read through the lens of the specification and prosecution history? Second, invalidity: is there prior art that anticipates or renders obvious the claims, or does the patent have written description, enablement, or definiteness problems that would support invalidity? Third, non-infringement: does the proposed generic product fall outside the scope of the claims under proper construction?
The PTAB provides an alternative invalidity venue through inter partes review (IPR) and post-grant review (PGR). IPR petitions are filed as standalone proceedings independent of district court litigation, but the two venues interact: a PTAB institution decision on an IPR petition may affect district court willingness to stay parallel litigation, and a final PTAB written decision has estoppel effects on the petitioner’s ability to raise the same invalidity arguments in district court. Generic companies now routinely file coordinated IPR petitions alongside P-IV filings, using PTAB proceedings to pressure brand companies into settlement while maintaining district court litigation as a backup.
Manufacturing Readiness: The Ranbaxy Lesson
The Ranbaxy atorvastatin launch is the canonical example of manufacturing failure negating litigation success. Ranbaxy spent years litigating the atorvastatin crystalline form patent, reached a settlement with Pfizer allowing a November 2011 launch, and received FDA approval from its Ohm Laboratories facility in New Jersey. Within weeks of launch, FDA inspections of other Ranbaxy facilities and an ongoing DOJ investigation into data integrity fraud at its Indian manufacturing sites created regulatory pressure that culminated in a recall of generic atorvastatin tablets in November 2012, attributed to glass particle contamination. A second recall followed.
The recalls forced Ranbaxy to halt production temporarily, creating supply gaps that subsequent entrants exploited. The partnership with Teva, structured as a contingency arrangement where Teva would receive a share of Ranbaxy’s atorvastatin profits in exchange for agreement not to challenge Ranbaxy’s first-applicant status, became public and attracted antitrust scrutiny from state attorneys general who characterized it as market allocation.
The operational lesson is not subtle. A first-applicant that cannot supply the market loses the exclusivity value it spent years acquiring. Manufacturing validation, cGMP compliance, and API supply security must be treated as commercially critical investments, not back-office functions. Quality systems failures are not independent of commercial strategy; they are commercial catastrophes.
Payer Engagement and Formulary Access
During the 180-day exclusivity period, the primary commercial lever is formulary positioning. PBMs manage formulary tier assignments for the majority of insured prescription drug volume in the United States. A first-generic that achieves preferred formulary status, meaning it is on Tier 1 or Tier 2 with minimal patient cost-sharing, captures the bulk of pharmacy substitution volume rapidly. A generic that has not negotiated PBM contracts before launch spends weeks or months fighting for formulary access while the exclusivity clock runs.
Pre-launch PBM engagement should begin 12-18 months before the anticipated launch date for high-revenue targets. The generic company must provide PBMs with pricing commitments, volume guarantees, and supply security assurances. Payers want a single source they can rely on during the exclusivity period; they are not primarily interested in maximizing short-term price savings at the cost of supply disruption. A credible supply chain story is a competitive asset in PBM negotiations.
Specialty pharmacy and hospital formulary channels require separate engagement strategies. Hospital formulary committees evaluate therapeutic equivalence documentation, bioequivalence data quality, and FDA approval status. For complex generics where bioequivalence is demonstrated through in vitro or device-based endpoints rather than systemic PK studies, clinician education on the FDA’s determination of equivalence is a necessary part of the launch program.
Phase 3: Post-Day-181 Market Defense
The structural shift on Day 181 from exclusivity to open competition does not eliminate the first-mover’s advantage; it changes the nature of the competition required to maintain it. The first-mover’s embedded supplier relationships, established distribution flows, and PBM contract coverage create switching costs for competitors, but not insurmountable ones.
Long-term supply agreements with guaranteed volume and pricing are the primary defense mechanism. A chain pharmacy or PBM that has signed a two-year preferred supplier agreement with the first-filer will not switch to a new entrant unless the price differential is large enough to justify the administrative cost of the switch. The first-filer must be prepared to reduce margin post-Day-181 to hold contracts, and that margin reduction should be anticipated in the original financial model rather than treated as an unexpected erosion.
Portfolio diversification is the longer-term structural defense. The profits from a successful 180-day exclusivity launch fund the next P-IV campaign. Companies that treat each exclusivity window as the end of a cycle rather than the funding mechanism for the next cycle cannot sustain growth in the generic business. The generic industry’s most durable operators, measured by sustained free cash flow generation, are those with a rolling portfolio of P-IV challenges at various stages of litigation and regulatory review, providing a pipeline of exclusivity windows spread across multiple years.
Key Takeaways: Strategic Playbook
Target selection must integrate commercial, legal, and competitive criteria simultaneously. Evergreening creates patent landscapes that require a full-portfolio FTO analysis, not a single-patent challenge. Manufacturing readiness is a commercial prerequisite, not an operational afterthought. PBM engagement before launch determines the revenue capture rate during exclusivity. Post-Day-181 defense requires pre-committed pricing strategy and contractual relationships established during the exclusivity period.
Part VII: Case Studies
Case Study A: Ranbaxy and Teva on Atorvastatin: Operational Risk at Scale
Ranbaxy Laboratories secured first-applicant status on generic atorvastatin calcium (brand: Lipitor) through a Paragraph IV challenge to Pfizer’s crystalline form patent, U.S. Patent No. 5,969,156. The litigation outcome, a 2007 settlement with Pfizer that allowed Ranbaxy a November 30, 2011 launch date, was commercially extraordinary given atorvastatin’s status as the highest-grossing pharmaceutical product in history.
Ranbaxy’s IP position was, on paper, the most valuable first-applicant position the generic industry had seen. The compound patent (4,681,893) expired in June 2011 with pediatric exclusivity extending to November 2011, the date of Ranbaxy’s authorized launch. The crystalline form patent was the contested asset; Ranbaxy’s challenge succeeded in establishing a pathway to market for its non-infringing polymorph formulation. That IP victory, worth hundreds of millions of dollars in exclusivity revenue, was the asset.
The destruction of value was operational. Ranbaxy’s manufacturing infrastructure had been under FDA scrutiny since 2006, when inspectors found data integrity problems at its Paonta Sahib facility in India. By the time of the atorvastatin launch, Ranbaxy was operating under a 2008 FDA import ban covering products from multiple Indian facilities and was in active DOJ investigation for alleged drug application fraud. Its Ohm Laboratories facility in New Jersey, which would manufacture generic atorvastatin for the U.S. market, was the only compliant production site available.
The Teva back-up agreement, by which Teva received a share of atorvastatin exclusivity revenue in exchange for agreeing not to challenge Ranbaxy’s first-applicant status, was disclosed in Teva’s SEC filings and later became the subject of an antitrust action by the Connecticut and Louisiana attorneys general. The states alleged that the agreement was an illegal market allocation scheme under which Ranbaxy and Teva agreed not to compete against each other in atorvastatin to the detriment of subsequent generic entrants and consumers. The case ultimately settled without a public finding of liability, but the legal exposure confirmed that back-up arrangements structured as profit-sharing agreements between first-applicants and competing ANDA holders carry antitrust risk.
The manufacturing recall of November-December 2012, driven by glass particle contamination from a glass-lined reactor vessel, forced a production halt that allowed competitors including Watson (later Actavis) to capture market share that Ranbaxy had held. The episode illustrates an irony specific to the 180-day exclusivity structure: a company’s IP position can be commercially irreplaceable, while its manufacturing infrastructure, which is replaceable in principle but not quickly in practice, determines whether the IP value is actually realized.
Case Study B: Mylan and the EpiPen Authorized Generic: Pricing Strategy as Public Relations
Mylan N.V. acquired the U.S. marketing rights to EpiPen (epinephrine injection, 0.3mg auto-injector) as part of its 2007 acquisition of Merck KGaA’s generics business. Between 2007 and 2016, Mylan increased EpiPen’s list price from approximately $100 for a two-pack to over $600, a 500% increase driven by a combination of inflation-adjusted pricing, rebate strategy optimization against PBMs, and the absence of direct generic competition.
The absence of generic competition was itself IP-driven. The EpiPen device was covered by multiple device patents owned by Pfizer subsidiary King Pharmaceuticals (which Pfizer acquired in 2011), and separately by formulation and method-of-use patents assigned to Mylan’s licensor. The auto-injector mechanism, not the epinephrine formulation (which is off-patent), was the primary barrier to generic entry. Teva filed an ANDA for a generic EpiPen and received a Complete Response Letter from the FDA in 2016 citing device-related deficiencies, blocking its launch and leaving Mylan as the sole supplier of the reference product.
In August 2016, facing congressional investigation and the possibility of price control legislation, Mylan announced the launch of an authorized generic EpiPen at $300 for a two-pack, half the brand list price. Because the AG was distributed under Mylan’s existing NDA, it required no additional FDA approval and could launch within weeks. The strategic logic of the AG launch operated on four levels simultaneously.
First, it allowed Mylan to address public pressure on pricing without reducing the list price of branded EpiPen, preserving the rebate structure that PBMs and hospital group purchasing organizations had negotiated based on brand WAC. Second, the AG captured the price-sensitive market segment, including cash-pay patients, high-deductible plan members, and Medicaid patients in states with restrictive formulary management, without cannibalizing the insured, rebate-generating brand revenue. Third, by establishing a generic price floor at $300, Mylan reduced the commercial incentive for a competing generic entrant, particularly Teva, to enter at a price that would need to undercut $300 to capture market share. Fourth, the AG generated revenue and market share data that Mylan could use in PBM negotiations, demonstrating that it controlled both sides of the market.
The EpiPen AG was subsequently reviewed by the FTC as part of a broader investigation into Mylan’s pricing practices, and some healthcare economists argued that the AG launch was a form of product hopping designed to complicate generic competition rather than genuinely lower prices. Whether characterized as a crisis response, a pricing strategy, or a competitive defense, the EpiPen AG remains the clearest example in the modern generic landscape of an authorized generic deployed as a multidimensional strategic instrument rather than a simple pricing concession.
Key Takeaways: Case Studies
Ranbaxy’s atorvastatin experience establishes that IP victory and commercial success are not the same thing. Manufacturing quality is a revenue-determining variable. The Teva back-up arrangement illustrates that cooperation between ANDA holders to manage exclusivity sharing can constitute antitrust exposure. The EpiPen AG demonstrates that brand companies with no generic competition threat can use an AG proactively to manage public pricing pressure, control market segmentation, and set floor prices that reduce the commercial attractiveness of future independent generic entry.
Part VIII: The Evolving Frontier
FDA’s Proposed Exclusivity Trigger Reform
In its FY2023 budget justification, the FDA proposed amending the 180-day exclusivity provisions to adopt a ‘trigger-on-marketing’ model analogous to the Competitive Generic Therapy (CGT) exclusivity framework created by the FDA Reauthorization Act of 2017. Under the proposed model, the 180-day exclusivity period would begin only when the first applicant commences commercial marketing. Subsequent ANDA applicants would be eligible for tentative or final FDA approval during the first applicant’s exclusivity, but could not begin commercial sales until the first applicant launched or forfeited.
The practical effect of this change would be to eliminate the blocking effect of a non-marketing first applicant. Under current law, an ANDA holder with first-applicant status and no current intention to launch can hold the market closed to all other generics indefinitely, an outcome that serves neither patients nor the public health goals of the Hatch-Waxman Act. Under the proposed model, subsequent applicants would receive approval and could launch the day the first-applicant’s exclusivity is triggered, creating a much more competitive Day 1 market.
Critics from the generic industry argue that the proposal devalues the exclusivity incentive by eliminating the first-applicant’s ability to plan a launch with certainty about the competitive landscape. If five other generics are already fully approved when the first applicant launches, the Day 1 pricing and formulary environment resembles a Day 181 market, which substantially erodes the first-mover premium. As of April 2026, the proposal has not been enacted but remains active in FDA’s legislative agenda discussions.
Complex Generics: Scientific Barriers as Market Defense
The generic industry’s most significant strategic shift over the past decade is the reallocation of R&D investment from oral solid dosage forms toward complex generics. Complex generics include sterile injectable formulations (particularly long-acting injectables and liposomal drugs), inhaled drug products (metered-dose and dry-powder inhalers), transdermal systems, topical products with locally-acting ingredients, and ophthalmics. What these categories share is that bioequivalence demonstration is technically difficult, FDA review is more demanding, and manufacturing scale-up requires specialized equipment and expertise.
The result is a smaller field of ANDA applicants per product, which translates directly into better exclusivity economics. A complex generic facing two or three ANDA competitors on Day 181 maintains pricing at 40-60% of brand for years, versus the 5% of brand that a commodity oral solid achieves within 18 months of patent expiration. The FDA’s Product-Specific Guidance program is the primary roadmap for complex generic development: companies that invest early in PSG interpretation and work closely with the FDA during development have demonstrably higher approval rates than those that file without PSG engagement.
Biosimilars Under the BPCIA: A Different Exclusivity Architecture
The Biologics Price Competition and Innovation Act (BPCIA) of 2009 created a biosimilar approval pathway under 351(k) of the Public Health Service Act, separate from the ANDA pathway. The exclusivity structures under the two acts are fundamentally different and create distinct strategic paradigms.
| Feature | Hatch-Waxman (Small Molecules) | BPCIA (Biologics) |
|---|---|---|
| Approval Standard | Bioequivalence to RLD | ‘Highly similar’ with no clinically meaningful differences |
| Reference Product Data Exclusivity | 5 years (NCE) | 12 years |
| First-Mover Exclusivity | 180 days (P-IV first applicant) | 12 months (first interchangeable biosimilar) |
| Interchangeability Standard | Automatic for AB-rated generics | Separate demonstration required; additional clinical studies |
| Patent Dispute Mechanism | 30-month stay triggered by P-IV litigation | ‘Patent Dance’ information exchange under 42 U.S.C. 262(l) |
| Regulatory IP Listing | Orange Book (FDA-administered) | Purple Book (does not contain patents) |
The 12-month interchangeable biosimilar exclusivity is awarded to the first biosimilar granted interchangeable status by the FDA, a designation that allows pharmacist-level substitution without physician intervention. Interchangeability requires demonstration that the biosimilar can be switched with the reference product without increased risk, a clinical and analytical burden that substantially exceeds the biosimilarity standard alone.
The strategic implication is that the biosimilar first-mover reward is tied to a scientific and regulatory investment larger than that required for a standard biosimilar, and the 12-year data exclusivity on reference biologics creates a much longer, more formidable market entry barrier than the 5-year NCE exclusivity in the small-molecule framework. Companies entering the biosimilar market must evaluate interchangeability as a discrete investment decision, not an automatic extension of biosimilar development.
The 2025-2030 Patent Cliff and Market Opportunity
Branded drugs generating more than $200 billion in annual U.S. sales face primary patent expiration or data exclusivity expiration by 2030. The drugs contributing most significantly to this cliff include several GLP-1 receptor agonists, monoclonal antibodies approaching biologic data exclusivity expiration, and established blockbuster small molecules with primary patents expiring in the 2025-2028 window.
Global generic market revenues are projected to grow from approximately $450 billion in 2025 to over $700-775 billion by 2030-2033, driven primarily by this patent cliff and by biosimilar market development in the United States and European Union. For generic companies, the opportunity is real but competitive intensity is intensifying in parallel: the largest generic manufacturers, including Teva, Viatris, Sun Pharma, and Aurobindo, are all scaling complex generic and biosimilar programs to capture higher-margin exclusivity periods as the oral solid commodity market continues to compress margins.
Investment Strategy: Patent Cliff as a Systematic Signal
Institutional investors can use patent expiration data systematically. The analytical framework has two components. On the brand side, primary patent expiration and data exclusivity loss are well-defined, quantifiable revenue cliff events. For brand companies with high revenue concentration in products approaching patent expiration, the cliff is a negative catalyst that is predictable in timing if not always in magnitude. On the generic side, the same data identifies the commercial opportunity pipeline.
Key metrics to track for generic companies include: the number and quality of first-applicant P-IV positions currently held; the approximate launch timing for each (based on litigation status and stay expiration); the revenue exposure of the target brand (a direct proxy for the exclusivity prize); and whether the brand has disclosed plans for an authorized generic or a consent judgment settlement with an entry date. These variables, collectively, provide a basis for building adjusted earnings scenarios that incorporate exclusivity upside without relying on management guidance alone.
Key Takeaways: The Evolving Frontier
The FDA’s proposed trigger-on-marketing reform would reduce the value of non-marketing first-applicant positions, shifting the balance of power toward brands that can prepare multiple generic approvals for simultaneous launch on the exclusivity trigger date. Complex generics maintain better exclusivity economics because scientific barriers limit the ANDA filer pool. Biosimilar exclusivity is structured differently from Hatch-Waxman exclusivity, with interchangeability as the key value-determining designation. The 2025-2030 patent cliff is the largest pipeline of generic opportunity in the market’s history, but it is not uniform; its value is concentrated in high-revenue brands with defensible exclusivity positions.
Conclusion: The Execution Imperative
The 180-day generic exclusivity is a structured commercial opportunity with a known mechanism, a known duration, and a known set of rules. What separates companies that consistently extract its value from those that repeatedly fall short is not access to information, the regulatory framework is public, or scientific capability, bioequivalence is well-understood. It is execution quality across every functional domain simultaneously.
Legal teams must file complete, well-crafted ANDAs with robust P-IV notice letters. Patent litigators must build invalidity and non-infringement cases with sufficient depth to survive appellate review, not just district court adjudication. Regulatory affairs must manage FDA review timelines with the urgency of a commercial deadline. Manufacturing must deliver cGMP-compliant product at commercial scale before the launch date, not after it. Business development must negotiate settlements that preserve exclusivity rather than trade it away. Commercial teams must have PBM contracts executed and distribution networks loaded before the approval arrives.
The Ranbaxy atorvastatin experience is in the record not because Ranbaxy’s legal strategy was flawed, it was not, but because manufacturing failure negated a legally successful first-applicant position worth hundreds of millions of dollars. The EpiPen case is instructive not because Mylan had a better patent position than anyone expected, but because it shows how a brand company, controlling both NDA and authorized generic simultaneously, can use the AG as a commercial instrument that shapes competitive dynamics years into the future.
For portfolio managers and institutional analysts, the 180-day exclusivity period remains the most concentrated earnings event in the generic pharmaceutical industry. A single successful exclusivity launch against a major brand can represent 20-40% of an annual earnings forecast for a mid-size generic company. Tracking P-IV filings, litigation outcomes, manufacturing compliance records, and settlement structures provides a systematic edge in modeling earnings scenarios that company guidance typically underspecifies.
The companies that will sustain leadership in this space through 2030 are those that combine legal sophistication in P-IV strategy, operational discipline in manufacturing and regulatory affairs, commercial precision in payer engagement, and financial discipline in portfolio selection. The exclusivity window is fixed at 180 days. Everything else is a choice.