Section 1: The 505(b)(2) Value Proposition — Pricing Incremental Innovation
1.1 Why the Pathway Exists and What It Actually Does

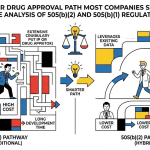
The 505(b)(2) NDA is a product of the Drug Price Competition and Patent Term Restoration Act of 1984 — the Hatch-Waxman Amendments — and it remains one of the most commercially consequential provisions in U.S. pharmaceutical law. Its core mechanism is simple: a sponsor can submit a full New Drug Application containing complete reports of safety and effectiveness while relying, at least in part, on studies that were not conducted by or for that sponsor and for which they hold no right of reference. In practice, this means a company can build on the FDA’s own prior findings for a Reference Listed Drug (RLD) or on published scientific literature, avoiding duplicative research that adds cost without adding clinical value.
The result is a hybrid approval pathway that sits between a 505(b)(1) NDA for a genuine New Chemical Entity (NCE) and a 505(j) Abbreviated New Drug Application for a generic. Development costs are typically 40-50% lower than a traditional 505(b)(1) program, and timelines compress accordingly. But unlike a 505(j) generic, a successful 505(b)(2) application generates its own market exclusivity — three years for a new clinical investigation, five years for a new molecular entity in certain configurations, or seven years for an orphan designation. That exclusivity period is the structural basis for premium pricing.
The ‘scientific bridge’ is the technical heart of every 505(b)(2) application. It consists of sponsor-conducted studies that link the new product to the RLD, demonstrating that the proposed modification does not negatively affect safety or efficacy. For a simple formulation change, a comparative pharmacokinetic study showing bioavailability equivalence or superiority may suffice. A new route of administration, or a new indication involving a distinct patient population, typically requires a more extensive bridging data package. The complexity of this bridge is the primary variable in forecasting development cost.
1.2 The Commercial Architecture: What Types of Innovation the Pathway Supports
The 505(b)(2) route accommodates a wide range of modifications, and each carries a distinct value profile. The pathway is routinely used for new dosage forms and formulations, extended-release mechanisms, novel routes of administration, new fixed-dose combinations (FDCs), new therapeutic indications applied to previously approved active moieties, prodrugs, and ready-to-use injectables that replace complex compounding or reconstitution steps.
Each modification maps to a specific commercial logic. A once-monthly subcutaneous formulation of a previously daily oral drug addresses adherence as a primary disease-management failure mode, particularly in conditions like schizophrenia, opioid use disorder, or osteoporosis. An FDC that collapses a three-pill regimen to one targets pill burden and adherence in polypharmacy populations, often elderly patients with cardiovascular or metabolic disease. A ready-to-dilute oncology formulation that reduces infusion time from 60 minutes to 10 minutes targets provider workflow, chair utilization, and pharmacy safety in infusion centers. The pricing case for each product flows directly from the specific problem the modification solves.
The critical insight is that the pricing exercise for a 505(b)(2) product is not about setting a price for a molecule. It is about setting a price for the modification. The active moiety is, by definition, already known, already off-patent in most cases, and already subject to generic pricing. The incremental value layer — the formulation engineering, the adherence benefit, the safety improvement, the operational efficiency — is the sole basis for any price above the generic floor. If that incremental layer cannot be quantified, demonstrated, and communicated to payers in concrete clinical and economic terms, there is no sustainable commercial case for a premium price.
1.3 Candidate Assessment: The Phase Where Pricing Potential Is Made or Lost
Commercial viability analysis must begin at the candidate assessment stage, before an Investigational New Drug (IND) application is filed. This pre-IND evaluation should explicitly address three questions that will determine the product’s pricing trajectory.
First: is there a measurable, payer-relevant clinical benefit to the proposed modification? Improved adherence is only valuable if it can be linked, with data, to better outcomes or lower total cost of care. A formulation that reduces pill burden from two tablets to one will not command a significant premium unless there is evidence that the reduction materially affects compliance rates and downstream healthcare resource utilization (HCRU). ‘Convenience’ without a connected outcomes story does not clear payer formulary committees.
Second: what is the competitive trajectory of the RLD and its generics at the projected approval date? A 505(b)(2) product targeting a market where the RLD’s net price has already collapsed 80-90% due to multi-source generic competition faces a dramatically compressed pricing corridor. Timing the launch to precede the most severe phase of generic price erosion — or to target a patient sub-population that is not adequately served by the commoditized generic — is a commercial strategy that must be decided before significant development capital is committed.
Third: what is the most likely reimbursement path, and does the product’s value story match what the relevant payer tier actually evaluates? A hospital system pharmacy and therapeutics (P&T) committee evaluates products differently than a national PBM formulary committee. An oncology practice administrator cares about J-code clarity and infusion chair throughput. A Medicaid managed care plan cares about total cost of care and rebate magnitude. The evidence package the development program must generate is determined by answering this question before Phase I starts, not after NDA approval.
Key Takeaways: Section 1
The 505(b)(2) pathway’s commercial value derives entirely from the incremental benefit of the modification, not from the underlying molecule. Development cost reduction of 40-50% versus a 505(b)(1) program creates capital efficiency, but that efficiency is only realizable if the modification generates a defensible value proposition for payers. The candidate assessment phase, pre-IND, is when pricing potential is built or forfeited. Teams that treat pricing as a launch-year activity will consistently underperform against those that integrate commercial modeling into the initial asset selection decision.
Section 2: IP Valuation as a Core Commercial Asset
2.1 The 505(b)(2) IP Stack: Patents, Exclusivities, and the Orange Book
For a 505(b)(2) product, intellectual property protection is not a legal formality. It is the structural foundation of the entire commercial thesis. Without a clearly defined and legally defensible exclusivity wall, every premium pricing strategy discussed in this document collapses within 180 days of the first generic ANDA filing.
The IP stack for a 505(b)(2) asset typically has four layers, each with distinct durations and strategic functions.
The first layer is FDA regulatory exclusivity — specifically, the three-year new clinical investigation exclusivity that attaches to new approvals requiring new clinical studies, or five-year NCE exclusivity in cases involving genuinely new active moieties. These periods run from the date of NDA approval and block the FDA from approving a competing ANDA or 505(b)(2) application that relies on the same submitted data. They are granted by statute, require no active prosecution, and are not invalidatable in litigation.
The second layer is Orange Book-listed patents. A 505(b)(2) sponsor lists all patents that claim the drug product or a method of using it in the FDA’s Orange Book. Any ANDA or 505(b)(2) filer that references the same RLD and seeks approval before those patents expire must certify against each listed patent. A Paragraph IV certification — which alleges that the listed patent is invalid, unenforceable, or will not be infringed by the generic product — triggers a 30-month stay of FDA approval and, almost always, patent infringement litigation. That litigation process, even when the innovator ultimately loses, typically adds 18-30 months of market protection beyond the regulatory exclusivity period.
The third layer is patent portfolio depth. A sophisticated 505(b)(2) sponsor does not rely on a single compound or formulation patent. They build a portfolio covering the specific modified formulation, the drug delivery system, the manufacturing process, polymorphic forms of the active ingredient, and the specific patient population sub-indications identified in the clinical program. Each additional patent in the Orange Book is a separate Paragraph IV certification required of any generic challenger, increasing the litigation surface and the cumulative time and cost burden on potential competitors.
The fourth layer is trade dress and data package complexity. While not strictly IP, the combination of proprietary delivery technology (e.g., a polymer depot injection system), complex manufacturing know-how, and a deep clinical data package creates practical barriers to entry that extend commercial exclusivity beyond the nominal patent expiration dates.
2.2 Valuing the IP Asset: Methodologies for Portfolio Managers
Three established valuation methodologies apply to a 505(b)(2) IP asset, each suited to different stages of the product lifecycle.
The risk-adjusted net present value (rNPV) approach is the standard for pre-launch or early-stage assets. It discounts projected post-launch cash flows back to a present value, applying probability weights at each development milestone — IND, Phase I completion, NDA submission, NDA approval — and at each stage of the commercial model. The IP exclusivity period directly governs the duration of the premium-priced revenue window in the model. A product with a three-year exclusivity period and a single formulation patent expiring in year five of commercialization will have a dramatically shorter high-revenue window than a product with layered IP extending protection to year twelve. In DCF terms, the difference between a five-year and a twelve-year exclusivity window, at a 10% discount rate and $300M peak annual revenue, can exceed $700M in net present value.
The comparable transaction approach benchmarks the asset against precedent transactions involving similar 505(b)(2) assets in the same therapeutic class. Licensing deal structures, upfront payments, milestone schedules, and royalty rates from publicly disclosed transactions provide market-derived evidence of what buyers and licensors have historically assigned to comparable IP positions. This method is most useful in M&A due diligence or licensing negotiations.
The real options approach is appropriate for early-stage 505(b)(2) candidates where a key commercial decision — most critically, whether to pursue a Therapeutic Equivalence rating — has not yet been made. Real options modeling explicitly values the flexibility to make that decision conditional on future data, treating the commercial pathway choice as an option with calculable value.
2.3 Orange Book Listing Strategy and Paragraph IV Exposure
The decision of which patents to list in the Orange Book is itself a strategic commercial decision with direct pricing consequences. Listing every defensible patent, including method-of-use patents for specific indications and extended-release formulation patents, maximizes the Paragraph IV certification burden on would-be generic challengers. Each additional listing requires a separate certification, a separate notice letter, and a separate litigation track.
However, over-listing carries risk. Listing a weak patent that a generic challenger successfully invalidates in Paragraph IV litigation can accelerate generic entry rather than delay it, and can expose the sponsor to antitrust scrutiny if the listing is found to be objectively baseless. The Orange Book listing strategy must therefore be calibrated by patent counsel with specific expertise in Hatch-Waxman litigation, coordinated with the commercial team’s pricing and exclusivity timeline modeling.
The interaction between Orange Book listing strategy and the J-code decision (discussed in Section 4) is particularly important. A product that seeks and receives a Therapeutic Equivalence ‘AB’ rating will likely face generic substitution pressure more quickly. A product that intentionally avoids a TE rating to secure a unique J-code must rely more heavily on its patent portfolio to maintain commercial exclusivity, because the reimbursement protection of the unique J-code does not substitute for IP-based market protection in the retail pharmacy channel.
2.4 Evergreening via the 505(b)(2) Pathway
Evergreening — the practice of extending the commercial life of a pharmaceutical franchise through sequential line extensions — is a defined strategic use of the 505(b)(2) pathway. The mechanics are straightforward: a sponsor holds a branded drug facing patent expiration and/or generic entry, and uses the 505(b)(2) pathway to develop and approve a modified version of the same active moiety with its own new IP stack and exclusivity period. The commercial objective is to migrate patients from the original formulation to the new one before generic entry, capturing the existing patient base in the new protected product.
Common evergreening vectors include moving from immediate-release to extended-release (the most common), moving from oral to transdermal, moving from IV to subcutaneous, adding an approved pediatric indication to reset or extend exclusivity, and creating an FDC with a complementary agent. The Pediatric Research Equity Act (PREA) and the Best Pharmaceuticals for Children Act (BPCA) create a specific evergreening mechanism: completing required pediatric studies can generate an additional six months of exclusivity layered on top of existing patent and regulatory exclusivity periods. For a product generating $2 billion annually, six additional exclusivity months represents approximately $1 billion in protected revenue.
The regulatory and commercial risks of evergreening are real. The FTC has scrutinized ‘product hopping’ cases where branded manufacturers withdrew original formulations to prevent generic substitution, arguing this constitutes anticompetitive conduct. The legal standard in U.S. courts has not uniformly condemned product hopping, but the litigation risk is non-trivial and must be weighed in the commercial model.
Key Takeaways: Section 2
A 505(b)(2) product’s commercial value is inseparable from its IP position. The regulatory exclusivity clock starts at NDA approval; the patent exclusivity clock is governed by the filing and prosecution decisions made years earlier. Portfolio managers should model the full IP stack — regulatory exclusivity, Orange Book patents, litigation outcomes, and pediatric exclusivity opportunities — as the primary driver of revenue duration in any DCF analysis. Evergreening via sequential 505(b)(2) applications is a documented commercial strategy with significant upside but measurable regulatory and antitrust risk.
Investment Strategy Note: When evaluating a 505(b)(2) asset for acquisition or licensing, request a full Freedom-to-Operate opinion alongside the Orange Book listing analysis. Assess the litigation history of each listed patent, particularly any prior Paragraph IV challenges that may have narrowed the scope of enforceable claims. A patent that has survived litigation is worth materially more in an IP valuation model than one that has never been tested.
Section 3: Competitive Triangulation — RLD, Generics, and Market Analogs
3.1 The RLD as a Pricing Ceiling, Not a Pricing Target
The Reference Listed Drug establishes the upper bound of a practical pricing corridor for its 505(b)(2) counterpart in most commercial scenarios. Payers will not, as a rule, reimburse a 505(b)(2) product at a price significantly exceeding the RLD’s net price unless the sponsor can demonstrate quantifiable superiority — not just FDA-approved labeling differences, but payer-relevant clinical and economic outcomes that close the value gap.
The RLD analysis for pricing purposes must focus on net price, not Wholesale Acquisition Cost (WAC). The spread between WAC and net price — the gross-to-net gap driven by rebates, chargebacks, and government price calculations — has widened substantially over the past decade. For mature branded products in competitive therapeutic classes, gross-to-net gaps of 50-65% are not unusual. A 505(b)(2) product that sets its WAC at a 20% premium to the RLD’s WAC may actually be priced below the RLD’s net price once its own rebate commitments are modeled. Anchoring the competitive analysis to net price throughout the model avoids this analytical error.
The RLD analysis must also track the patent and exclusivity timeline. A product whose RLD is three years from multi-source generic entry faces a very different pricing environment than one whose RLD holds another eight years of protection. The pricing corridor narrows rapidly as generic entry approaches and the RLD itself begins aggressively rebating to maintain formulary position ahead of the generic wave.
3.2 Generic Price Erosion: The Floor, the Curve, and the Timing Window
Generic entry follows a predictable price decay curve that is the most important external variable in the 505(b)(2) commercial model. The data are consistent: when six or more generic manufacturers compete in a market, the generic price settles at approximately 5-15% of the original branded WAC. With one or two generics, prices may hold at 30-50% of brand pricing for a transitional period. The decay from one generic to six generics typically occurs within 24-36 months of the first ANDA approval.
For a 505(b)(2) sponsor, this curve creates a specific timing opportunity. A 505(b)(2) applicant is not bound by the 180-day first-filer exclusivity that governs ANDA competition — that 180-day period belongs to the first Paragraph IV ANDA filer and blocks other generic entrants, but does not block a 505(b)(2) product. A 505(b)(2) application can theoretically receive approval and launch into a market that still has only one or two generic competitors, capturing a pricing window before the full erosion cycle completes. This timing arbitrage requires a precise understanding of the ANDA pipeline for the relevant molecule, which is exactly the kind of intelligence that structured patent and filing databases are designed to provide.
The practical floor for a 505(b)(2) product in a multi-source generic market is determined not by the generic WAC, but by the generic net price, which in a highly competitive market approaches manufacturing cost plus distribution margin. Any 505(b)(2) price above this floor requires a positive answer to the question payers will always ask: what am I getting for the additional cost?
3.3 Market Analog Analysis: The Real-World Test of Payer Willingness to Pay
Market analog analysis — studying the commercial performance of comparable 505(b)(2) products — is the most direct way to calibrate payer willingness to pay for specific types of incremental value. The analysis should focus on products with similar modification types, similar site-of-care profiles, and similar RLD competitive situations.
The analog analysis should specifically reconstruct each product’s formulary history: when payers granted preferred coverage, at what price premium over the RLD or generics, and with what utilization management requirements (prior authorization, step therapy, quantity limits). This reconstructed access history is more commercially useful than peak sales figures because it reflects the terms on which each premium price was actually sustained.
One consistent finding from analog analysis is that site of care is a stronger predictor of pricing success than modification type. Products reimbursed under the medical benefit — specifically, provider-administered injectables billed under a HCPCS code — have historically sustained far larger price premiums than products dispensed through the retail pharmacy channel under the pharmacy benefit. The structural reasons for this are explained fully in Section 4, but the competitive intelligence implication is that analogs in a provider-administered infusion setting are not directly comparable to analogs in a retail oral therapy setting, even if both share similar modification profiles.
Key Takeaways: Section 3
Competitive triangulation for a 505(b)(2) product requires simultaneous analysis of three reference points: the RLD’s net price trajectory (the ceiling), the post-generic-entry price floor (the floor), and market analog pricing and access history (the calibration data). The single most common error in 505(b)(2) pricing analysis is using the RLD’s WAC as the ceiling and ignoring the net price. This produces a model that overstates the available pricing corridor and underestimates the rebate commitments required to achieve formulary access.
Section 4: The J-Code Revolution — How CMS Rewired the Commercial Calculus
4.1 The Pre-2022 Reimbursement Problem
Before 2022, CMS’s default policy was to group a 505(b)(2) injectable product under the same Healthcare Common Procedure Coding System (HCPCS) J-code as its RLD and any therapeutically equivalent generic alternatives. This multisource J-code practice meant that a provider who administered a premium-priced 505(b)(2) product was reimbursed at an Average Sales Price calculated across all products sharing that code — a blend heavily influenced by the cheap generics. The ASP blending destroyed the commercial rationale for a ‘Differentiated Brand’ pricing strategy, because the provider had no reimbursement incentive to choose the 505(b)(2) over the generic, and in many cases would lose money by doing so under the ASP+6% model.
This structural problem was not a theoretical concern. It actively suppressed adoption of 505(b)(2) products in provider-administered settings, particularly oncology and infusion centers, even when those products offered genuine workflow or safety improvements over their generic counterparts.
4.2 The 2022 Policy Shift and Its Commercial Consequences
In 2022, following a complaint by a pharmaceutical manufacturer, CMS re-evaluated its coding policy against the Social Security Act’s statutory definition of a ‘sole-source drug.’ The agency concluded that a 505(b)(2) product not rated as therapeutically equivalent to its RLD in the FDA’s Orange Book qualifies as sole-source. Effective January 1, 2023, CMS began assigning unique, product-specific J-codes to non-TE 505(b)(2) products.
This change has three direct commercial consequences. First, a non-TE 505(b)(2) injectable product is now reimbursed at its own ASP+6% under Medicare Part B, completely decoupled from the RLD’s or generic’s ASP. Second, providers receive a clear, profitable reimbursement signal for using the 505(b)(2) product: they buy at acquisition cost, bill at ASP+6%, and capture the 6% spread as margin. Third, pricing negotiations with hospital GPOs and specialty distributors are restructured around the product’s standalone price, not a blended pool.
The commercial scale of this policy change is visible in the data from published Medicare claims analyses. Bendeka (bendamustine) reached a reimbursement level of 459% of its reference drug’s price in Medicare Part B data. Pemfexy (pemetrexed) reached 2,055% of its reference drug’s reimbursement level. These are not pricing anomalies; they are the predictable commercial output of a unique J-code in a market where providers have strong financial and operational incentives to adopt the differentiated product.
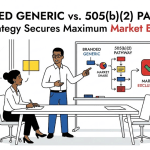
4.3 The Strategic Bifurcation: Branded Generic vs. Differentiated Brand
The 2022 CMS policy created a formal strategic fork in the road for 505(b)(2) commercialization. Every development team must now make an explicit, early-stage choice between two distinct commercial architectures.
Path A is the Branded Generic strategy. The sponsor requests a Therapeutic Equivalence rating from the FDA — typically an ‘AB’ designation — which certifies the product as substitutable for the RLD at the pharmacy level. If granted, the product shares a multisource J-code (or a multisource NDC in the retail channel) with the RLD and its generics. The commercial strategy becomes volume-driven: the sponsor competes on net price, contracting depth, supply reliability, and the practical benefit of substitutability to gain market share rapidly. The price premium above generics is modest. This path is appropriate for modifications with limited clinical differentiation or for sponsors whose primary objective is market penetration over margin maximization.
Path B is the Differentiated Brand strategy. The sponsor does not request a TE rating, or the FDA declines to grant one based on the nature of the modification. The product is classified as sole-source and receives its own unique J-code. The sponsor sets a premium WAC that reflects the product’s specific clinical and operational benefits, and builds a market access strategy around demonstrating the value of that premium to payers, P&T committees, and providers. The required evidence package — particularly the HEOR data discussed in Section 6 — is substantially more intensive than Path A requires.
The FDA does not automatically evaluate 505(b)(2) products for therapeutic equivalence. The sponsor must actively request the evaluation, and Congress has now mandated a 180-day review period for such requests, providing schedule certainty. The TE decision is therefore not a passive regulatory outcome; it is a commercial strategy decision with an explicit timeline and a clear trigger point that must be planned for in the development program.
4.4 The Formulary Implications: Medical Benefit vs. Pharmacy Benefit
The J-code architecture applies specifically to provider-administered products reimbursed under the medical benefit — primarily Medicare Part B injectables and infusibles. The distinction between medical benefit and pharmacy benefit reimbursement is one of the most consequential variables in the 505(b)(2) commercial model.
Products dispensed through retail pharmacies under the pharmacy benefit — oral tablets, capsules, most topical formulations — are managed by PBMs. PBM formularies are structured around therapeutic alternatives, step-therapy requirements, and rebate economics. In this channel, a premium-priced 505(b)(2) faces direct formulary competition from low-cost generics. The PBM has strong financial incentives — rebate capture, spread pricing — to route patients to the cheapest available product in a given therapeutic class. Securing preferred formulary status in a PBM-managed benefit requires either substantial rebate commitments that compress the net price dramatically, or clinical differentiation compelling enough that a P&T committee places restrictive utilization management controls on the generic alternatives.
Products administered in a clinical setting and billed under the medical benefit operate under a different logic. The provider, not the PBM, is the primary decision-maker. The provider’s incentives are shaped by reimbursement margin, operational efficiency, patient outcomes, and liability risk. A unique J-code that generates a positive buy-and-bill margin for the provider, combined with a formulation that reduces chair time or pharmacy preparation burden, can drive adoption without the PBM rebate negotiation. This is why the most dramatic 505(b)(2) pricing outcomes — Bendeka, Pemfexy — have occurred in oncology infusion settings rather than retail pharmacy channels.
Key Takeaways: Section 4
The 2023 sole-source J-code policy is the most commercially significant regulatory development for 505(b)(2) products in at least a decade. It has created a bifurcated market where Differentiated Brand products in provider-administered settings can command prices that bear little relationship to the underlying generic cost. However, this pricing power is channel-specific. It applies to the medical benefit and is effectively inaccessible in the retail pharmacy benefit without a wholly different market access strategy. The J-code path decision is a commercial strategy decision, not a regulatory classification, and it must be made during candidate assessment.
Investment Strategy Note: When evaluating a 505(b)(2) asset, the first commercial due-diligence question should be: is this a medical benefit or pharmacy benefit product? If it is a provider-administered injectable with a plausible sole-source J-code pathway, the pricing ceiling is materially higher than standard competitor-based models would suggest. Failure to model the J-code pathway will systematically undervalue medical benefit 505(b)(2) assets in transaction analysis.
Section 5: Payer Architecture — PBMs, Formularies, and the AMCP Dossier
5.1 How Payers Actually Evaluate a 505(b)(2) Product
FDA approval does not obligate a payer to cover a drug. Every major commercial payer and PBM runs its own internal formulary review process, and for a premium-priced 505(b)(2) entering a market with existing, lower-cost alternatives, that process begins with institutional skepticism.
The payer evaluation follows a consistent logic. The clinical pharmacist or Medical Director assigned to the review will assess whether the product’s labeled improvements represent a clinically meaningful advantage over available generics for the specific patient population the payer covers. ‘Clinically meaningful’ is not a synonym for ‘statistically significant’ — a payer may acknowledge that a modified formulation shows a 15% adherence improvement in a controlled trial and still conclude that the improvement does not justify the price premium given the real-world complexity of their population. The burden of proof falls entirely on the sponsor.
Payers are increasingly demanding ‘hard’ economic evidence — reductions in measurable HCRU events, particularly hospitalizations, emergency department visits, and disease-related complications — rather than surrogate endpoints like pharmacokinetic parameters or patient satisfaction scores. A budget impact model that demonstrates net healthcare cost savings when the 505(b)(2) product replaces a cheaper but less adherence-friendly alternative is the most commercially useful evidence type in a payer submission.
5.2 PBM Dynamics: The Opaque Intermediary
The three largest PBMs — Express Scripts, CVS Caremark, and OptumRx — manage the pharmacy benefit for an estimated 289 million Americans. Their influence over formulary placement is enormous. Their economics are complex. PBMs generate revenue through multiple mechanisms simultaneously: administrative fees from plan sponsors, rebates negotiated from manufacturers, retained spread between what they pay pharmacies and what they charge plan sponsors, and in some configurations, revenue from affiliated specialty pharmacies. These mechanisms create incentives that do not always align with minimizing net drug costs for payers or patients.
For a 505(b)(2) sponsor, the practical implication is that PBM formulary access comes at a price. The rebate required to achieve preferred formulary status for a premium-priced product in a therapeutic class with available generics can easily reach 50-70% of WAC in competitive classes. Modeling the gross-to-net gap is therefore not an accounting exercise; it is the core of the revenue forecasting model. A product with a $400/month WAC and a 60% gross-to-net gap generates $160/month in net revenue — a number that must cover not only cost of goods and SG&A, but also the R&D cost recovery embedded in the price and the return on capital expected by investors.
5.3 AMCP Dossier: Structure, Content, and Tactical Deployment
The AMCP Format for Formulary Submissions — version 4.1, most recently updated — is the primary vehicle for presenting a drug’s clinical and economic value proposition to U.S. payers. For a 505(b)(2) product, the dossier must accomplish something that a standard branded NDA dossier does not need to: it must affirmatively explain why the product’s incremental improvement over an available generic justifies its premium price.
The dossier’s clinical section must present the full evidence base for the specific modification, including the bridging study data, any pivotal clinical trials, and a direct comparison of outcomes versus the most relevant available alternatives — which, for a 505(b)(2) product, means the generic, not just the RLD. The economic section must contain a budget impact model tailored to the payer’s population characteristics (commercial, Medicare, Medicaid) and a cost-effectiveness analysis that positions the product against the current standard of care. The HEOR section should present all available evidence on HCRU offsets — hospitalizations, ED visits, disease complications — and include sensitivity analyses that show how the economics shift under different adherence or outcome assumptions.
Payer engagement should begin 18-24 months before NDA submission. Early advisory board meetings with medical directors from large national payers and regional Blue Cross Blue Shield plans allow the sponsor to test the value proposition, refine the evidence requirements, and identify the specific objections that the AMCP dossier will need to address. This iterative pre-launch engagement is not a marketing activity; it is evidence development strategy.
Key Takeaways: Section 5
Payers are the commercial gatekeepers for 505(b)(2) products, and their evaluation framework is fundamentally different from the FDA’s. The FDA asks whether the modification is safe and effective. The payer asks whether the modification is worth the added cost for their specific enrolled population. Answering that question requires HCRU data, budget impact modeling, and a gross-to-net financial model that accurately reflects the rebate environment. PBM formulary access in the retail channel requires rebate commitments that compress net price substantially, and those commitments must be built into the revenue model from the beginning.
Section 6: Building the Hybrid Pricing Model — HEOR as Commercial Currency
6.1 Value-Based Pricing Applied to Incremental Innovation
Value-based pricing (VBP) links a product’s price to the clinical, economic, and humanistic value it delivers. For a full 505(b)(1) NCE, VBP is applied against the backdrop of no existing therapeutic equivalent — the value is the entire benefit of the new medicine. For a 505(b)(2) product, VBP is applied to the delta between the new product and what is already available, often including cheap generics. This narrows the value foundation substantially, which is why the HEOR evidence base must be especially rigorous.
The key value metrics for a 505(b)(2) payer submission, in rough order of payer impact, are: HCRU reduction (hospitalizations, ED visits, readmissions), Quality-Adjusted Life Year (QALY) gain versus standard of care, medication adherence improvement with an established link to clinical outcomes, patient-reported outcome (PRO) improvement in symptom burden or functional status, and healthcare provider time or cost savings. Each metric must be quantified using data specific to the sponsor’s product — not extrapolated from analogs or inferred from the modification’s theoretical benefits.
The Institute for Clinical and Economic Review (ICER) increasingly functions as an informal reference body for U.S. payer formulary decisions. ICER’s willingness-to-pay threshold for a cost-effective intervention is typically framed as $100,000-$150,000 per QALY gained. For a 505(b)(2) product priced at a significant premium to available generics, an ICER review that finds the cost-per-QALY substantially above this range creates formulary headwinds that can persist for years after launch. Sponsors should model their product against ICER’s methodology proactively, before launch, and develop counter-evidence or pricing concessions before a critical ICER assessment is published.
6.2 The Budget Impact Model: Structure and Payer-Specific Customization
A Budget Impact Model (BIM) is required in every AMCP dossier submission. For a 505(b)(2) product, the BIM has two components that must be modeled simultaneously.
The first is the drug acquisition cost differential — the difference in pharmacy or drug purchasing cost between the 505(b)(2) product and the generics it displaces, net of applicable rebates. For a premium-priced product, this component is always negative (i.e., it increases drug spend). The second component is the medical cost offset — the reduction in HCRU-associated medical costs attributable to the 505(b)(2) product’s improved adherence, safety, or efficacy profile. If the medical cost offset exceeds or approaches the drug acquisition cost differential, the product’s payer value story is very strong. If the drug cost increase substantially exceeds the medical cost savings, the payer must decide whether the patient benefit justifies the net cost, which is a harder argument to win.
The BIM should be built and presented in payer-specific versions. A large self-insured employer plan with a commercially insured population skews younger and healthier than a Medicare Advantage plan. The HCRU rates for the same condition, and therefore the magnitude of the potential medical cost offset, differ substantially between these populations. A BIM calibrated to the payer’s own claims data, or at minimum to published HCRU rates for a demographically similar population, is more persuasive than a generic national-average model.
6.3 Cost-Effectiveness Analysis and the QALY Question
Cost-effectiveness analysis (CEA) in the U.S. context is a supporting tool rather than the primary decision driver, in contrast to HTA-governed single-payer systems like the UK’s NHS where NICE QALY thresholds directly determine reimbursement. Nevertheless, U.S. payers increasingly reference cost-per-QALY data when justifying formulary tier placement decisions or when communicating with plan sponsor clients about coverage rationale.
For a 505(b)(2) product, the CEA compares the incremental cost per QALY gained by the 505(b)(2) product versus the current standard of care — typically the cheapest available generic in the same therapeutic class. The QALY gain must be derived from the product’s clinical trial data or from a validated health state utility model. The cost denominator includes the product’s net price plus any additional costs of administration, minus the medical cost offsets attributable to the clinical benefit.
A CEA that yields an incremental cost-effectiveness ratio (ICER) in the range of $50,000-$100,000/QALY against the generic standard of care is broadly considered favorable by U.S. payers. An ICER above $150,000/QALY will generate formulary access challenges across multiple payer segments.
6.4 Real-World Evidence Strategy: Pre-Launch Planning for Post-Launch Value
Real-world evidence (RWE) generated after launch is now a standard component of the ongoing market access strategy for premium-priced 505(b)(2) products. Payers who grant conditional preferred formulary access at launch often require RWE commitments — typically registry studies, claims-based retrospective analyses, or electronic health record (EHR) cohort studies — to confirm that the HCRU benefits demonstrated in clinical trials replicate in the payer’s actual population.
The RWE plan should be designed before launch. The primary endpoints of post-launch RWE studies must align with the primary value claims in the AMCP dossier: if the dossier claims a 30% reduction in hospital admissions, the RWE study must measure hospitalization rates. If the claim is improved medication adherence, the RWE study must use prescription refill data or pharmacy claims to measure medication possession ratio (MPR) or proportion of days covered (PDC).
A robust post-launch RWE dataset also provides a renewable evidence base for formulary contract renegotiations, typically conducted every 12-24 months. Each renewal cycle is an opportunity to present new data reinforcing the product’s value and defending against payer attempts to reclassify the product to a non-preferred tier or subject it to new utilization management restrictions.
Key Takeaways: Section 6
HEOR is the commercial currency of the 505(b)(2) market access model. It is not a post-NDA marketing activity; it is a pre-IND strategic investment that determines whether the premium price the commercial team sets can actually be defended at the payer level. The budget impact model and cost-effectiveness analysis must reflect the payer’s population and cost structure, not generic national averages. Post-launch RWE strategy should be planned before launch to support formulary contract renewals and defend against access erosion.
Section 7: Evergreening Mechanics and the 505(b)(2) Life Cycle Extension Toolkit
7.1 The Patent Cliff and the 505(b)(2) Response
The ‘patent cliff’ — the precipitous revenue decline that follows multi-source generic entry — is the defining commercial risk in pharmaceutical portfolio management. The 505(b)(2) pathway is one of the pharmaceutical industry’s primary tools for extending the commercial life of a molecule franchise beyond the original patent expiration.
The mechanics of a life cycle extension (LCE) via 505(b)(2) follow a predictable sequence. Two to four years before the primary compound patent on the RLD expires, the sponsor files a new 505(b)(2) NDA for a modified version — most commonly an extended-release formulation, a new delivery system, or a new FDC. If approved, the new product receives its own three-year (or, in certain cases, five-year) regulatory exclusivity period and generates a new Orange Book patent listing. The commercial team begins the patient migration from the original formulation to the new one ahead of generic entry on the original, capitalizing on the existing prescriber relationships, brand recognition, and patient base.
The commercial success of an LCE depends heavily on execution timing and formulary strategy. If the original formulation remains on the market after generic entry, PBMs will simply tier the generic to preferred status and apply step-therapy requirements for the LCE, forcing patients through the cheaper alternative before the new product is approved. Successful LCE strategies typically involve a coordinated formulary contracting approach that establishes preferred access for the new formulation before the generic versions of the old one are widely available.
7.2 The Pediatric Exclusivity Play
Pediatric exclusivity is among the most reliable and predictable of the life cycle extension tools available through the 505(b)(2) pathway. Under the Best Pharmaceuticals for Children Act (BPCA), a sponsor that completes a Written Request from the FDA for pediatric studies receives an additional six months of exclusivity layered on top of all existing patents and regulatory exclusivities. This six-month extension applies to every Orange Book-listed patent for the drug, regardless of how many patents exist.
For a large-revenue asset — any drug generating over $1 billion annually — six months of additional exclusivity has a net present value of approximately $400-600 million at a 10% discount rate. For a drug generating $3 billion annually, the pediatric exclusivity value approaches $1.5 billion. The cost of the required pediatric clinical program rarely exceeds $30-80 million. The risk-adjusted return on pediatric exclusivity investment is among the highest in pharmaceutical commercial development.
The pediatric exclusivity strategy requires early planning. The FDA’s Written Request process has a defined timeline, and the pediatric studies themselves — particularly if they involve distinct formulations suitable for children (e.g., oral liquids, chewable tablets) — may require separate 505(b)(2) NDA submissions. A pediatric formulation submitted under a separate 505(b)(2) NDA can generate its own new clinical investigation exclusivity in addition to triggering the BPCA six-month extension on the parent molecule’s patents.
7.3 The New Indication Play: Repurposing as a Pricing Reset
New indication development via the 505(b)(2) pathway is a specific type of life cycle extension that has the additional commercial effect of a pricing reset. When a drug approved for indication A is developed and approved for indication B, the pricing for the product in indication B is benchmarked against the standard of care in indication B, not against the original price in indication A.
This matters particularly when the new indication is in a therapeutic area with a higher prevailing price level than the original. A molecule approved as an antifungal that is repurposed as an oncology adjunct can be repriced against oncology standards. A cardiovascular drug shown to reduce kidney disease progression in diabetic patients — as demonstrated with certain SGLT-2 inhibitors, though those were 505(b)(1) approvals — can be repriced against the renal care market. The 505(b)(2) pathway is the mechanism for making the regulatory and commercial case for that repricing.
The IP implications of a new indication filing deserve specific attention. A new indication claimed in an Orange Book-listed method-of-use patent provides Hatch-Waxman protection against ANDA challengers seeking approval for that indication — but generic ANDA filers can, and routinely do, carve out the new indication from their generic labeling in a ‘skinny label’ strategy. The scope of protection provided by a method-of-use patent for a new indication is therefore narrower than the commercial team may assume, and the repricing benefit must be modeled with realistic assumptions about skinny-label generic competition.
7.4 FDC Strategy: The Combination Play
Fixed-dose combination (FDC) development is one of the most commercially durable forms of 505(b)(2) life cycle extension. An FDC that combines the sponsor’s original branded compound with a complementary agent into a single dosage form creates a new product with its own IP stack, its own Orange Book listing, and its own exclusivity period. From a commercial standpoint, the FDC competes against the individual components taken separately, not against a generic of either component.
The pricing logic for an FDC reflects this positioning. The standard approach prices the FDC at a modest discount to the combined WAC of both individual components taken separately but at a substantial premium to the cost of either generic alternative alone. This pricing structure creates a compelling health economic argument — patients who would otherwise be prescribed two separate pills (potentially with separate co-pays and adherence complexities) can access both active ingredients in a single pill at a lower combined cost than the two brands separately.
The commercial durability of an FDC depends on the IP position of both component molecules. If one or both components have already faced generic entry, the FDC’s price premium over the cheapest available treatment option narrows considerably. The strongest FDC commercial positions occur when the FDC is launched while both component brands still hold meaningful market exclusivity, capturing the clinical rationale for combination therapy before generic fragmentation of either component disrupts the pricing anchor.
Key Takeaways: Section 7
The 505(b)(2) pathway is the primary mechanism for pharmaceutical life cycle extension. The pediatric exclusivity play, executed with proper planning, consistently delivers among the highest risk-adjusted returns in pharmaceutical development. New indication development via 505(b)(2) can reset pricing benchmarks when the new indication occupies a higher-value therapeutic category. FDC strategy creates durable IP positions that bridge the patent cliffs of both component molecules. None of these LCE strategies is passive; each requires coordinated IP, regulatory, and commercial planning that should begin at the inception of the original asset’s development program.
Section 8: Case Studies in 505(b)(2) Commercialization
8.1 Bendeka and Pemfexy: The Oncology Pricing Paradox
Bendeka (bendamustine HCl Injection, 100 mg/20 mL) is Eagle Pharmaceuticals’ 505(b)(2) formulation of Cephalon’s Treanda. The modification was straightforward: Bendeka is a ready-to-use, pre-mixed liquid in a 50 mL bag that infuses over 10 minutes, compared to Treanda’s lyophilized powder requiring reconstitution, dilution, and a 30-60 minute infusion in a 500 mL bag. The formulation change eliminated a cytotoxic handling step for pharmacy staff, reduced infusion chair time per patient by approximately 30-50 minutes, and removed the reconstitution error risk inherent in the Treanda preparation process.
Bendeka received FDA approval in December 2015 and was not rated therapeutically equivalent to Treanda. It received a unique J-code (J9034) effective January 2016. Eagle set the WAC at a substantial premium to Treanda. When Teva’s generic bendamustine entered the market, Bendeka’s price relative to the generic rose to approximately 459% at its peak in Medicare Part B reimbursement data, according to a 2025 ASCO presentation analyzing the 505(b)(2) price paradox.
The commercial mechanism is reproducible and instructive. Oncology practices operate under a buy-and-bill reimbursement model for Medicare Part B drugs. They purchase the drug, administer it, and bill Medicare at ASP+6%. When Bendeka carried a unique J-code reimbursed at its own ASP+6%, practices that used Bendeka received a larger absolute dollar margin per administration than they would from using the cheaper generic billed under a multisource code. This created a direct financial incentive for the provider to choose Bendeka, independent of the price level. The clinical rationale — reduced staff exposure to a cytotoxic agent, faster chair throughput — reinforced the financial incentive.
Pemfexy (pemetrexed for injection, Fresenius Kabi) follows the same structural template as a ready-to-dilute formulation of Eli Lilly’s Alimta (pemetrexed). The modification eliminated the multi-step reconstitution required for Alimta, providing a concentrated liquid vial that pharmacists can directly draw from and dilute without the powder-handling step. Pemfexy received a unique J-code and reached 2,055% of its reference drug’s Medicare reimbursement level according to the same ASCO dataset — an extraordinary commercial outcome for a product whose clinical modification was almost entirely operational rather than therapeutic.
The critical lesson is that payer resistance, which drives down 505(b)(2) prices in the retail pharmacy channel, operates differently in the buy-and-bill medical benefit setting. In the infusion center, the ‘payer’ in the traditional sense does not review the formulary at the point of dispensing. The provider is both the clinical decision-maker and the billing entity, and the unique J-code aligns that decision-maker’s financial incentives with the 505(b)(2) product’s adoption.
IP Valuation Note for Analysts: Eagle’s commercial model for Bendeka was built on a combination of Orange Book-listed formulation patents (protecting the specific low-volume, low-concentration liquid formulation chemistry), the non-TE classification (blocking generic substitutability), and the unique J-code structure. The effective commercial moat was not any single IP element but the combination of all three. When assessing Bendeka-type transactions, value the non-TE classification and J-code access as assets with economic lives approximating the term of the relevant Orange Book patents.
8.2 Sublocade and Vivitrol: The Adherence Premium in Addiction Medicine
Sublocade (buprenorphine extended-release injection) is Indivior’s once-monthly subcutaneous buprenorphine formulation approved via 505(b)(2) in 2017. The RLD is oral buprenorphine/naloxone (Suboxone). The modification converts daily sublingual dosing to monthly subcutaneous injection using Braeburn’s (now Indivior’s) ATRIGEL polymer depot delivery system, guaranteeing continuous buprenorphine blood levels and eliminating the possibility of diversion — a primary clinical and regulatory concern with oral buprenorphine.
Sublocade’s WAC is approximately $2,117 per monthly dose (as disclosed on the manufacturer’s WAC pricing page). Oral generic buprenorphine/naloxone 8mg/2mg films are available at approximately $50-80 per month at retail pharmacies. The 26-30x price premium is sustained entirely by the adherence and diversion-prevention value proposition.
The commercial strategy targets specific institutional settings where that value is most operationally significant: opioid treatment programs (OTPs), federally qualified health centers (FQHCs), the correctional health system, and organized health systems managing high-risk OUD populations. In these settings, confirmed monthly dosing has direct administrative and clinical value — providers know the patient has received the medication, courts and parole systems can verify treatment compliance, and healthcare systems can attribute downstream cost reductions (fewer overdose-related ED visits, fewer readmissions) to the intervention. Indivior’s investor presentations explicitly highlight the correctional health channel as a high-value institutional target precisely because the value of verifiable adherence is maximized in that setting.
Vivitrol (naltrexone for extended-release injectable suspension, Alkermes) is a once-monthly intramuscular injection for both alcohol use disorder (AUD) and opioid use disorder (OUD). The RLD is oral naltrexone. Vivitrol’s list price runs approximately $1,000-$1,500 per monthly dose versus oral naltrexone at approximately $30-60/month.
The FDA’s Perseris (risperidone extended-release injectable suspension, Braeburn) case is instructive for the limits of the adherence premium. Perseris is a once-monthly subcutaneous LAI for schizophrenia, referencing oral risperidone (Risperdal). The primary adherence benefit is real, but Canada’s CADTH HTA review concluded that without head-to-head evidence against other available LAI antipsychotics, including Risperdal Consta (IM) and the paliperidone palmitate LAIs, Perseris should not command a price premium above the least costly LAI alternative. This is the payer principle that analogs matter: a 505(b)(2) formulation that shares a core benefit with an already-available branded product is benchmarked against that product, not only against the original oral RLD. The pricing corridor narrows further when the market already has ‘differentiated brand’ competition.
8.3 Key Cross-Case Takeaways
Four patterns emerge from these case studies. First, site of care is the strongest predictor of 505(b)(2) pricing power. Provider-administered products in the medical benefit can sustain price premiums that retail pharmacy channel products cannot. Second, the unique J-code is a commercial asset as valuable as a patent when the product is administered in a buy-and-bill setting. Third, the value proposition must match the actual decision-maker’s incentive structure. For oncology infusion products, that is the practice administrator. For addiction medicine products, it is the institutional health system or correctional authority. For retail pharmacy products, it is the PBM formulary committee. Fourth, head-to-head data against the most relevant comparator — which may be another formulation in the same class, not just the original oral RLD — is increasingly required to defend a premium position at payer renewal.
Section 9: The Pre-IND-to-Launch Roadmap — Phase-Gated Pricing Decisions
9.1 Phase 1: Candidate Assessment (Pre-IND)
The pre-IND candidate assessment phase is the most commercially consequential decision point in the entire 505(b)(2) lifecycle. All subsequent investment is predicated on the commercial viability conclusions reached here.
The value proposition must be stated in quantifiable terms from the outset. Not ‘improved adherence,’ but ‘an expected 25-35% improvement in medication possession ratio based on published adherence data from analogous LAI versus oral comparisons in this indication, translating to an estimated 18% reduction in annual hospitalization rate per retrospective registry study methodology.’ That level of specificity determines whether the HEOR plan can generate the evidence required to support a premium price.
The J-code pathway decision — Differentiated Brand (Path B) or Branded Generic (Path A) — must be made here, with full awareness of its implications for the evidence package, the patent filing strategy, and the commercial model. The RWE strategy and HEOR plan must align with the chosen path.
Preliminary competitive triangulation at this stage should model three scenarios: best case (no meaningful generic entry before launch, strong J-code access), base case (moderate generic penetration, J-code access with rebate requirements), and downside case (rapid generic erosion, TE rating required by FDA, retail channel pricing constraints). Each scenario should yield a distinct revenue forecast that informs the go/no-go investment decision.
9.2 Phase 2: IND Through NDA Submission — Evidence Building
The clinical development program must be designed to generate both the regulatory bridging data and the payer-oriented outcomes data. These are not always the same studies. The FDA bridging study may require only comparative pharmacokinetic data. The payer outcomes data — hospitalization rates, adherence measures, HCRU cost offsets — may require a separate registry study, a real-world cohort analysis, or additional clinical trial endpoints.
Payer advisory boards should be running in parallel with Phase II data generation, testing emerging data with formulary decision-makers and refining the commercial evidence requirements. These boards are not marketing events; they are structured primary research activities that should yield specific insights about the evidence gaps that, if filled, would change a payer’s formulary decision.
The AMCP dossier is a living document that should be initiated in Phase II and continuously updated. The budget impact model framework should be built before pivotal data is available so that the final clinical data can be dropped in and the economic conclusions generated rapidly for the NDA submission period.
9.3 Phase 3: NDA Submission Through Launch — Price Setting and Access Preparation
The launch price (WAC) is set in this phase, based on the synthesis of the HEOR evidence package, the payer research findings, the competitive triangulation, and the J-code determination. The WAC must be modeled alongside its gross-to-net implication across all relevant payer segments — commercial, Medicare Part B, Medicare Part D, Medicaid, and, where applicable, the VA Federal Supply Schedule.
The HCPCS J-code application to CMS should be submitted with the NDA or shortly thereafter. The application must explicitly support the non-TE classification (if Path B is chosen) and provide all necessary clinical and regulatory documentation to support the sole-source determination. CMS’s 180-day review timeline means that a product approved in January can receive a unique J-code assignment effective by mid-year, which is typically the first quarter where the code becomes operationally billable.
Patient support programs — co-pay assistance cards for commercially insured patients, patient assistance programs for uninsured or underinsured patients — must be designed and operational at launch. For a premium-priced 505(b)(2) product, co-pay assistance is not optional. Without it, patient out-of-pocket costs under non-preferred formulary placement can reach hundreds to thousands of dollars per month, directly suppressing adoption.
Key Takeaways: Section 9
The pre-IND candidate assessment phase builds or destroys the commercial case. By NDA submission, the price has been determined by the evidence that was — or was not — generated during development. Teams that run pricing in parallel with clinical development, integrating payer advisory research into evidence gap analysis, consistently achieve better formulary access outcomes than teams that build the payer strategy after regulatory approval.
Section 10: Investment Strategy for Portfolio Managers and Analysts
10.1 Screening Criteria for 505(b)(2) Asset Evaluation
When screening 505(b)(2) assets for acquisition, licensing, or investment, six variables determine the quality of the commercial opportunity.
The first is the nature of the modification. Modifications that directly prevent a high-cost medical event — hospitalization, relapse, overdose — generate the most durable payer value stories. Modifications that improve convenience or reduce pill burden, without a connected HCRU data set, face significantly more formulary resistance.
The second is the reimbursement channel. Medical benefit products with a plausible unique J-code pathway have a structurally higher pricing ceiling than retail pharmacy benefit products. Evaluate the site of care at the earliest stage of due diligence.
The third is the IP stack depth. Count the number of Orange Book-listed patents, their expiration dates, and their litigation history. A product with a single formulation patent expiring in year three of commercialization has a very different revenue duration profile than one with a layered portfolio extending to year ten.
The fourth is the regulatory exclusivity clock. Note the NDA approval date and calculate the remaining exclusivity runway. For an older product, a pediatric exclusivity play or a new indication filing may be the most immediately value-accretive development option.
The fifth is the competitive analog landscape. Identify the three to five most commercially comparable 505(b)(2) products in the same or adjacent therapeutic areas and reconstruct their formulary access histories. The analog set is the most direct evidence of payer willingness to pay for the type of incremental value the asset offers.
The sixth is the gross-to-net model. Payers will negotiate. The sustainable revenue from a 505(b)(2) product is the net price after all rebates, not the WAC. Model gross-to-net at 20%, 40%, and 60% to understand the revenue resilience of the asset across a range of payer negotiation outcomes.
10.2 Valuation Framework for 505(b)(2) Assets
The rNPV model for a 505(b)(2) asset should explicitly map the commercialization path choice (Path A vs. Path B) and model each path separately. In most cases, Path B generates a higher rNPV if the J-code is secured, but carries higher risk if the FDA requires a TE rating or if payers resist the premium price at scale.
The model’s revenue driver is the net price times the captured patient volume. Patient volume is a function of formulary access — specifically, the proportion of the relevant patient population covered by plans that grant preferred or at least covered status. A product with preferred access in plans covering 60% of commercially insured patients and Part B coverage under its own J-code will generate materially more volume than a product with non-preferred access across all payer segments.
Sensitivity analyses should test: (a) the impact of one or two years of delayed J-code assignment, (b) the impact of a competitor 505(b)(2) product entering the same market with a competing J-code, (c) the impact of IRA drug price negotiation if the product reaches blockbuster scale, and (d) the impact of a generic Paragraph IV challenge that successfully invalidates the primary Orange Book patent.
10.3 Red Flags in 505(b)(2) Commercial Due Diligence
Four red flags should prompt deeper scrutiny or a revised valuation.
The first is a weak or unpublished HEOR data package at the time of commercialization. If a product has been on the market for two or more years without published cost-effectiveness or HCRU data, it typically means the outcomes data does not support the premium price, and payers have already begun restricting access.
The second is a gross-to-net gap that has widened in consecutive annual disclosures. Widening gross-to-net reflects escalating rebate commitments required to maintain formulary position, signaling that payer acceptance of the premium price is eroding.
The third is a TE rating granted after launch. If the FDA grants a TE rating subsequent to approval — which can occur if the sponsor requests it or if a generic challenge establishes bioequivalence — the unique J-code basis may be challenged, and the product’s pricing position in the medical benefit channel weakens materially.
The fourth is a product that relies exclusively on the buy-and-bill mechanism for its commercial model, with no established pharmacy benefit access. A regulatory or CMS policy change that modifies the ASP+6% model or the sole-source J-code criteria would eliminate the primary commercial foundation of the product with no fallback channel.
Key Takeaways: Section 10
505(b)(2) assets in the medical benefit channel, with unique J-codes and deep IP stacks, have generated some of the highest risk-adjusted returns in pharmaceutical commercial development over the past decade. The pricing ceiling in the buy-and-bill setting is structurally higher than standard competitor-based models capture. However, that pricing power is dependent on three conditions holding simultaneously: the non-TE classification, the unique J-code assignment, and the absence of a meaningful clinical comparator that breaks the sole-source commercial argument. Assess all three conditions with current data, not historical precedent.
Appendix: Comparison Tables
Table 1: FDA Approval Pathway Comparative Analysis
| Feature | 505(b)(1) NDA | 505(b)(2) NDA | 505(j) ANDA |
|---|---|---|---|
| Purpose | New Chemical Entity | Modified version of approved drug | Generic copy of approved drug |
| Data Package | Full preclinical/clinical, sponsor-generated | Full safety/efficacy reports, relies in part on RLD data plus sponsor bridging studies | Bioequivalence data only |
| Innovation Scope | High: novel molecule, new mechanism | Moderate: clinically meaningful modifications | None: bioequivalent copy |
| Development Cost | >$1B typical | 40-50% lower than 505(b)(1) | Lowest |
| Exclusivity Types | 5-yr NCE, 7-yr Orphan, 3-yr new clinical investigation | 3-yr new clinical investigation, 5-yr NCE (select cases), 7-yr Orphan | 180-day first-filer only |
| Pricing Power | Highest | Moderate to high, modification-dependent | Minimal, competition-driven |
Table 2: 505(b)(2) J-Code Strategy Decision Matrix
| Strategic Variable | Path A: Seek TE Rating | Path B: Forgo TE Rating |
|---|---|---|
| Reimbursement Mechanism | Multisource J-code; ASP blended with generics | Unique J-code; ASP based solely on product’s own price |
| Pricing Logic | Volume-driven; modest premium to generics | Value-based; premium justified by clinical/economic differentiation |
| Primary Payer Objection | ‘Why cover this over a substitutable generic?’ | ‘Prove the incremental benefit justifies the cost premium’ |
| Required Evidence Package | Bioequivalence, supply chain reliability | Robust HEOR: BIM, CEA, HCRU offset data |
| Competitive Vulnerability | Price erosion if rebates are non-competitive | Payer rejection if value story is thin or unsupported |
| Best Fit Profile | Modest modification; market share is the primary goal | Significant modification with a measurable outcomes advantage |
Table 3: 505(b)(2) Life Cycle Extension Mechanisms
| LCE Type | Regulatory Mechanism | Exclusivity Generated | Key Commercial Risk |
|---|---|---|---|
| Extended-Release Reformulation | New 505(b)(2) NDA for new dosage form | 3-yr new clinical investigation | PBM step-therapy to cheaper IR generic |
| New Indication | 505(b)(2) NDA with clinical efficacy data | 3-yr new clinical investigation | Skinny-label generic carve-out limits IP protection |
| Pediatric Studies (BPCA) | Written Request completion | +6 months on all listed patents | Requires FDA Written Request; program must be designed to FDA specification |
| FDC Development | 505(b)(2) NDA for combination product | 3-yr new clinical investigation, new Orange Book listing | Both components must maintain pricing anchor; generic fragmentation of either component erodes FDC premium |
| Subcutaneous vs. IV Switch | 505(b)(2) NDA for new route of administration | 3-yr new clinical investigation | Head-to-head vs. competing SC products required by payers |
This analysis draws on publicly disclosed regulatory filings, FDA Orange Book data, CMS HCPCS coding decisions, published HEOR literature, and peer-reviewed pricing analyses including ASCO 2025 presentation data on the 505(b)(2) price paradox. It does not constitute investment advice. All pricing data reflects publicly disclosed WAC and published Medicare claims analyses; net prices reflect estimated gross-to-net adjustments based on market analogs and may differ from actual negotiated prices.