Full drug development — from first synthesis of a new chemical entity to FDA approval — costs, on average, $2.6 billion and takes ten to fifteen years [1]. That figure is not a secret, and it is not inflated. It accounts for the cost of failure, the capital deployed on compounds that never reach approval, the clinical trial infrastructure, the manufacturing scale-up, and the regulatory apparatus required to demonstrate safety and efficacy from scratch.
The 505(b)(2) New Drug Application pathway does not eliminate those costs. What it does is let you avoid paying most of them by relying on safety and efficacy data that already exists — data generated by the original developer of an active pharmaceutical ingredient, and data that the FDA has already accepted as valid. Done correctly, 505(b)(2) development compresses a fifteen-year process into three to five years and cuts total investment from $2.6 billion to somewhere between $20 million and $300 million, depending on the nature of the innovation and the complexity of the required clinical program [2].
That is not an approximation. Companies including Jazz Pharmaceuticals, Supernus Pharmaceuticals, Noven Pharmaceuticals, and dozens of smaller specialty pharma operations have built franchises worth hundreds of millions of dollars by developing 505(b)(2) products — reformulations, new delivery systems, new dosing regimens, new salt forms, new patient populations — without synthesizing a single novel molecule. They navigated a regulatory structure that most pharmaceutical executives have heard of but relatively few understand well enough to exploit fully.
This article explains exactly how 505(b)(2) works, what it takes to build a successful product on the pathway, how the intellectual property strategy connects to the regulatory strategy, where the approach breaks down and why, and how competitive intelligence tools like DrugPatentWatch are essential for identifying which molecules and market positions are worth pursuing in the first place.
Part One: What 505(b)(2) Actually Is — And What It Is Not
The Three NDA Pathways and Why the Middle One Gets Ignored
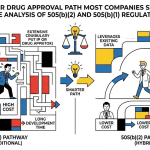
The Federal Food, Drug, and Cosmetic Act provides three routes to FDA drug approval for small-molecule drugs. Understanding the differences is not bureaucratic detail — it is the foundation of every strategic decision that follows.
The 505(b)(1) pathway is the full NDA. The applicant submits complete safety and efficacy data from studies conducted or sponsored by the applicant. Every preclinical package, every Phase I, II, and III trial, every manufacturing validation study — the applicant owns or licenses all of it. This is the pathway for genuine new chemical entities, and it carries the $2.6 billion price tag.
The 505(j) pathway is the ANDA — the Abbreviated New Drug Application used by generic drug manufacturers. The applicant does not submit new clinical data at all. Instead, it demonstrates that its product is pharmaceutically equivalent (same active ingredient, same strength, same dosage form, same route of administration) and bioequivalent to the reference listed drug. No independent clinical evidence required. The cost runs $1 to $5 million. The catch is that the product must be identical to the reference drug in its formulation and dosage form, leaving no room for clinical differentiation.
The 505(b)(2) pathway sits between these two. The applicant submits an NDA that relies, at least in part, on data or information from studies that were not conducted by or for the applicant — and for which the applicant has not obtained a right of reference [3]. That “right of reference” qualifier matters enormously. The applicant does not need the original developer’s permission to rely on FDA’s finding of safety and efficacy for the referenced drug. The FDA’s prior approval constitutes the evidentiary basis, and the applicant supplements it with whatever new studies are required to support the specific changes being made.
The practical result: a 505(b)(2) applicant developing a novel extended-release formulation of a well-characterized molecule does not need to prove the molecule’s basic safety profile in a 500-patient Phase III trial. The original sponsor did that. The 505(b)(2) applicant needs to prove that its specific formulation is safe, delivers the molecule with the pharmacokinetic profile claimed, and — if a new indication is sought — demonstrates efficacy in that indication. That is a much narrower clinical program.
What “Relying On” FDA’s Prior Findings Actually Means
The mechanism that makes 505(b)(2) work is the FDA’s acknowledgment that its prior approval of a referenced drug constitutes evidence of that drug’s safety and efficacy. When a 505(b)(2) applicant lists a reference listed drug (RLD), it is essentially saying: “The FDA has already found this active ingredient to be safe and effective for certain purposes. My product uses the same active ingredient, and I am making specific modifications. Here is my evidence that those modifications are safe and effective.”
The FDA does not require the 505(b)(2) applicant to repeat the clinical history of the referenced molecule. It requires only the bridging studies needed to connect the RLD’s established profile to the new product’s specific attributes — typically bioavailability and bioequivalence studies that demonstrate how the new formulation compares to the RLD in terms of pharmacokinetic exposure, plus any safety data required to support the specific modification.
This “reliance” framework has three important limits. First, if the 505(b)(2) product differs from the RLD in ways that introduce new safety concerns — a new indication, a new patient population with different metabolic profiles, a new dosage form with different absorption characteristics — the FDA will require safety data adequate to characterize those new concerns, regardless of the RLD’s established profile. Second, the applicant must address every listed Orange Book patent for the RLD through Paragraph II, III, or IV certification, precisely as any ANDA filer must. Third, data exclusivity attached to the RLD may block 505(b)(2) approval for a defined period, even if all patent issues are resolved.
The Spectrum of 505(b)(2) Products
The FDA has approved 505(b)(2) applications for a wide range of product types. The list is longer than most practitioners assume:
New salt forms and polymorphs of established active ingredients, where a different physical form delivers improved bioavailability, stability, or manufacturing characteristics.
New dosage forms of existing molecules — converting an injectable to an oral solid, a tablet to a transdermal patch, an immediate-release to an extended-release formulation.
New strengths outside the approved range, particularly when the new strength enables a dosing regimen with clinical advantages over available doses.
New combinations of established active ingredients in a single dosage form (fixed-dose combinations), where the combination itself is the innovation.
New indications for established molecules, relying on the existing safety profile and supplementing it with efficacy data for the new use.
New patient populations — pediatric, geriatric, renally impaired, hepatically impaired — where dosing characterization for the population is the primary scientific contribution.
Drug-device combination products, where the active ingredient is established but the delivery device — an autoinjector, an inhaler, a prefilled syringe — is the meaningful innovation.
The 505(b)(2) pathway is not intended for “me-too” products with no genuine medical advance. But the FDA’s threshold for “genuine medical advance” is lower than commercial judgment might suggest — improved bioavailability that enables lower dosing, reduced pill burden that improves adherence, elimination of food effects that complicates dosing, or a new route of administration that benefits specific patient populations all qualify, provided the applicant generates adequate evidence.
Part Two: The Economics — Where the 90% Cost Reduction Actually Comes From
Decomposing the $2.6 Billion NDA Cost
The $2.6 billion average cost of new molecular entity development is a composite that disguises significant internal variation. Breaking it down reveals where the cost actually resides and, by extension, where the 505(b)(2) savings are largest [1]:
Preclinical and discovery costs account for roughly $450 million on average, primarily because this stage’s cost is inflated by the high failure rate of novel compounds. The compounds that make it to IND are supported by a mountain of preclinical work on compounds that never did.
Phase I clinical trials (first-in-human safety and pharmacokinetic studies) typically cost $4 to $20 million per study, with most NME programs running multiple Phase I studies across different populations, doses, and formulations.
Phase II clinical trials (proof-of-concept efficacy and dose-ranging) cost $15 to $50 million per trial and carry a high failure rate — only about 40 percent of compounds entering Phase II advance to Phase III [4].
Phase III clinical trials (pivotal efficacy and safety trials) are the dominant cost driver, typically consuming $150 to $400 million per trial, with most NME programs requiring at least two adequate and well-controlled Phase III studies.
Chemistry, manufacturing, and controls (CMC) development — designing the commercial manufacturing process, validating it, and demonstrating that it consistently produces a product meeting specifications — costs $50 to $300 million depending on the complexity of the synthesis and dosage form.
Regulatory and post-approval studies add another $50 to $100 million across the NDA assembly, submission, review, and any post-market commitment studies.
A 505(b)(2) applicant eliminates essentially all of the preclinical and discovery costs, because the molecule is already characterized. It eliminates most of the Phase I cost, because basic pharmacology and toxicology are established. It eliminates Phase II in many cases, because the dose-response relationship is already understood. It dramatically reduces Phase III, because the scope of the required clinical evidence is narrowly targeted to the specific change being made rather than the full therapeutic indication from scratch. CMC costs are real but compressed by the availability of published formulation literature and the shorter manufacturing timeline.
The remaining cost — primarily the bridging bioavailability studies, a focused clinical program demonstrating the benefit of the reformulation or new indication, and CMC development — typically runs between $20 million for a straightforward formulation change and $300 million for a new indication with a full Phase III program. Against the $2.6 billion baseline, that is a cost reduction ranging from 88 to 99 percent depending on program complexity.
The Timeline Compression: Why Five Years Beats Fifteen
Cost compression matters, but timeline compression may matter more for most development programs. The ten-to-fifteen-year NDA timeline for an NME includes two to four years of discovery and lead optimization, two to three years of preclinical development, and six to ten years of clinical development. Each of these phases carries capital cost, but the more significant cost is opportunity cost — the time during which the patent clock is running without commercial revenues.
A drug’s composition-of-matter patent is typically filed at or before IND, well before the first clinical trial. By the time an NME receives FDA approval ten to fifteen years later, the patent has consumed most of its life, leaving an average of twelve years of commercial exclusivity. A company that spends fifteen years developing a drug to get twelve years of commercial life has a commercial window that is itself pressured from day one.
A 505(b)(2) applicant starts from the molecule’s known pharmacology, skips discovery and most preclinical work, and enters development with a formulation hypothesis grounded in published scientific literature. The development timeline from project initiation to NDA approval runs three to five years for a straightforward reformulation, four to seven years for a new indication requiring a Phase III program. The resulting product can have new formulation patents filed early in development with ten-plus years of commercial patent life remaining when approved.
The economic difference is not subtle. A product approved in year four with twelve years of patent life remaining and $200 million in development cost has a fundamentally different NPV profile than a product approved in year thirteen with seven years of patent life remaining and $2.6 billion in development cost — even if the two products address the same clinical need and generate the same peak revenues.
The Risk Profile Shift: Eliminating Phase II Attrition
Drug development failure rates are high and heavily concentrated in clinical development. The probability of a drug entering Phase I ultimately reaching approval is roughly ten percent for NMEs [4]. The majority of those failures occur during Phase II and Phase III, after significant capital has already been deployed.
The specific cause of most Phase II failures is inadequate proof of concept — the molecule does not demonstrate the efficacy signal in humans that preclinical models predicted. This is the translational gap, and it is the single largest driver of NME development cost and failure rate. A molecule that fails Phase II has cost $50 to $100 million in preclinical and Phase I investment without generating any return.
A 505(b)(2) program eliminates this failure mode for the molecular component. The molecule’s efficacy in humans has already been proven. The uncertainty in a reformulation program is not “does this molecule work?” but “does this specific formulation deliver the molecule with the pharmacokinetic profile we need?” and “does delivering it this way generate clinical benefit over existing options?” These are narrower, better-defined questions with better-characterized risk profiles.
This risk shift has significant financing implications. A 505(b)(2) program can be financed by mid-tier specialty pharma companies, private equity-backed platforms, and even well-capitalized startups because the capital requirement and failure probability are both manageable on a balance sheet that could not support an NME program. The 505(b)(2) opportunity is genuinely accessible to a wider range of developers than full NME development.
Part Three: Finding the Right Target — The Molecule Selection Framework
What Makes a Molecule a Good 505(b)(2) Candidate
Not every established molecule with a patent cliff or a suboptimal formulation is a good 505(b)(2) target. The development program has to deliver something that prescribers will choose over existing options, that payers will pay for at a premium over generic alternatives, and that can be protected with a patent position strong enough to justify the development investment. All three conditions must hold simultaneously.
A good 505(b)(2) target has four characteristics:
Established safety with a known and acceptable adverse effect profile. The FDA requires adequate characterization of the new formulation’s safety, but it does not require the applicant to re-establish that the molecule is not a carcinogen or genotoxin. If the molecule has regulatory safety concerns that were inadequately characterized in the original approval, those concerns will resurface in the 505(b)(2) review, and the program will face unexpected requirements that erode the cost advantage.
A clear pharmacokinetic improvement opportunity. The most defensible clinical rationale for a 505(b)(2) reformulation is a demonstrable improvement in the pharmacokinetic profile of the drug — reduced peak-to-trough variability, elimination of food effects, extended duration of action, improved bioavailability, or reduced dose requirements. These are measurable, the FDA can evaluate them objectively, and they translate directly to clinical benefit claims that support formulary positioning.
A market position where the improvement justifies premium pricing. If an extended-release formulation of a molecule will be priced at $200 per month against a generic immediate-release formulation at $15 per month, the clinical differentiation must be compelling enough that prescribers and payers accept the premium. This is a commercial judgment that must be made before committing to development, not after. Many 505(b)(2) programs fail commercially — not at the FDA — because the development team did not rigorously test whether prescribers would actually prefer the new formulation over the generic at the anticipated price differential.
A patentable formulation innovation. The 505(b)(2) product needs its own intellectual property to generate commercial life beyond the referenced drug’s remaining exclusivity. A 505(b)(2) product approved using an obvious modification of an off-patent molecule, with no independently patentable formulation attributes, competes against both the original brand and the generics of the original product. It can win in that environment, but only if the clinical differentiation is compelling enough to maintain formulary position without patent protection — a much harder commercial challenge.
How to Use DrugPatentWatch to Identify Opportunities
The practical starting point for 505(b)(2) target identification is a systematic analysis of the pharmaceutical patent landscape — specifically, finding molecules where the composition-of-matter patent has expired or is approaching expiration, where the original formulation has known clinical limitations, and where no competitor has already filed a 505(b)(2) application for the obvious reformulation.
DrugPatentWatch provides exactly the data structure needed for this analysis. Its patent expiration database tracks every Orange Book-listed patent by product, active ingredient, and expiry date — allowing developers to identify molecules where the primary patent has recently expired or will expire within two to four years, the window in which development for the reformulation can be completed and launched before generic erosion of the original formulation is total. Its Paragraph IV litigation database shows which products are already under active generic challenge, signaling that the primary patent may fall earlier than its nominal expiry date. Its ANDA filing database shows which generic manufacturers have already filed for the base formulation, indicating that commodity generic competition is imminent or underway.
The combination of these data sources produces a shortlist of molecules where: the base molecule is becoming or has become generic (eliminating the need to compete on price for the original formulation), the original formulation has known limitations (providing the clinical rationale for the reformulation), and no 505(b)(2) application has yet been approved for the obvious improvement. This is the target list for a 505(b)(2)-focused developer.
The analysis requires judgment, not just data retrieval. The “obvious improvement” question is both a commercial judgment and a patent strategy question. A modification obvious enough to be commercially compelling may also be obvious enough to face an obviousness challenge at the USPTO — an argument that the formulation innovation was within the ordinary skill of the relevant art given the state of knowledge at the time of filing. The formulation scientist and the patent attorney need to evaluate the same opportunity from both perspectives simultaneously.
Case Study: The Extended-Release Opportunity Map
Immediate-release formulations of many CNS, cardiovascular, and endocrine drugs were developed and approved in an era when extended-release technology was less sophisticated and less well-understood. Many of these drugs have adverse effect profiles driven by peak plasma concentrations — CNS stimulants cause cardiovascular effects at Cmax, antiepileptics cause sedation and ataxia at peak, cardiovascular drugs cause hypotension at peak. Extended-release formulations that smooth the plasma concentration-time curve can reduce those peak-related adverse effects while maintaining trough efficacy.
This pharmacokinetic rationale has driven a substantial proportion of successful 505(b)(2) approvals. Concerta (methylphenidate extended-release) was approved via 505(b)(2) and built a franchise worth over $1 billion annually, competing against the generic immediate-release formulation of the same molecule by delivering a distinct pharmacokinetic profile suited to the ADHD treatment paradigm [5]. Vyvanse (lisdexamfetamine), while technically a new molecular entity (the prodrug structure differentiated it from existing amphetamine salts), exemplifies the same commercial logic: a delivery innovation that extended commercial life and franchise value well beyond what the underlying pharmacology alone would have supported.
The pattern extends across therapeutic areas. Coreg CR (carvedilol extended-release) was approved via 505(b)(2), offering once-daily dosing versus the original twice-daily immediate-release. Bupropion XL extended the bupropion franchise well past the generic IR competition. Diltiazem, nifedipine, verapamil, metoprolol — virtually every major cardiovascular drug with an immediaterelease heritage now has extended-release variants that were developed and approved via 505(b)(2) or its predecessor pathways, and that have maintained meaningful market share against the generic immediate-release formulations for years.
The systematic identification of molecules where this opportunity has not yet been exploited — where the IR formulation is generating generic erosion but no ER product exists — is precisely the analysis that DrugPatentWatch’s patent and ANDA filing databases support.
Part Four: The Regulatory Strategy — Getting the FDA to Work With You
The Pre-NDA Meeting: Why You Cannot Skip It
The single most important investment a 505(b)(2) developer can make before committing to a full clinical program is a Type B pre-NDA meeting with the FDA [6]. This is a formal meeting at which the applicant presents its proposed development program — the reference listed drug, the modifications being made, the proposed clinical and CMC data package — and receives FDA feedback on whether the proposed approach is adequate to support approval.
The meeting is not a negotiation. The FDA does not commit to approving a product in a Type B meeting. What it does commit to is clarity: it tells the applicant what studies it will require to approve the application, what the regulatory standard is for the specific type of 505(b)(2) being pursued, and what questions from the literature review or the proposed clinical design need to be resolved. An applicant that conducts a Type B meeting before starting clinical work has materially lower execution risk than one that designs its studies in isolation and files the NDA without FDA input.
The preparation for a Type B pre-NDA meeting requires a substantial investment of scientific work. The briefing document — the written summary of the proposed program that the FDA reviews before the meeting — should address the regulatory basis for the 505(b)(2) approach (identifying the RLD and the specific data being relied upon), the proposed bridging studies (bioavailability and bioequivalence studies connecting the new formulation to the RLD), any additional clinical data proposed to support the modifications being made, and a CMC summary demonstrating that the manufacturing process is controlled and reproducible.
Companies that submit thin pre-NDA meeting packages receive thin FDA feedback. The investment in a rigorous briefing document pays for itself many times over in the precision of the FDA’s guidance.
Bioavailability and Bioequivalence Studies: The Scientific Core
The clinical bridge between a 505(b)(2) product and its reference listed drug is typically a series of bioavailability and bioequivalence studies. These studies measure the pharmacokinetic parameters of the new product — primarily area under the concentration-time curve (AUC) and maximum concentration (Cmax) — and compare them to the RLD under defined conditions [7].
For a product seeking to demonstrate bioequivalence to the RLD (common in new salt forms, new polymorphs, or minor formulation changes), the standard is the 80-125% confidence interval criterion: the 90% confidence intervals for the ratio of test to reference AUC and Cmax must both fall within 80 to 125 percent. Meeting this standard demonstrates that the new formulation delivers the drug to the systemic circulation in essentially the same manner as the reference.
For a product intentionally designed to deliver the drug differently — an extended-release formulation with a lower Cmax and extended Tmax, an abuse-deterrent formulation with a blunted intranasal pharmacokinetic profile, an oral formulation of a molecule previously only available by injection — the question is not bioequivalence but adequate characterization of the new pharmacokinetic profile. The applicant must demonstrate that the new PK profile is safe, that it delivers adequate drug exposure to achieve the therapeutic effect claimed, and that it does not create new safety concerns.
Food effect studies are a routine component of the bioavailability package. Many oral formulations have meaningful food effects — the presence or absence of food in the stomach changes the rate and extent of absorption. If the RLD has a known food effect that the new formulation is designed to eliminate (a genuine clinical benefit in drugs where co-administration with food is burdensome), the food-effect bioavailability study provides the evidence. If the new formulation has a new food effect not present in the RLD (a potential safety concern in drugs where food-effect-driven overexposure could cause harm), the FDA will require characterization of that interaction.
The Clinical Bridge for New Indications
When a 505(b)(2) application seeks approval for a new indication not held by the reference listed drug, the clinical data requirement is more substantial. The applicant cannot rely on the RLD’s clinical evidence for the new indication — the FDA has not previously evaluated the molecule for that purpose — and must generate adequate and well-controlled clinical evidence for it.
The scope of that evidence depends on the indication. For an indication that is closely related pharmacologically to an established indication of the RLD (treating Type 2 diabetes with a novel formulation of a molecule previously approved only for Type 1, for instance), the FDA may accept a smaller clinical program if the pharmacology is well understood and the safety profile in the new population is adequately characterized.
For a genuinely new indication, the applicant typically needs at least one adequate and well-controlled Phase III trial demonstrating efficacy, plus safety data from a population large enough to characterize the adverse effect profile in the new indication. This is more than a bioavailability study, but it is still substantially less than the two-to-three Phase III trials typically required for NME approval, because the underlying pharmacology of the molecule is established and the FDA focuses its review on the indication-specific evidence rather than the molecule’s entire clinical profile.
The most important 505(b)(2) clinical program I have reviewed was Jazz Pharmaceuticals’ program for sodium oxybate in idiopathic hypersomnia — a condition for which no approved treatment existed and for which the existing literature supported sodium oxybate’s mechanism of action. The 505(b)(2) approach allowed Jazz to reference the established safety profile of sodium oxybate (already approved for narcolepsy as Xyrem) and focus its clinical investment on an indication-specific Phase III trial rather than a full NME development program. The resulting approval of Lumryz (a different formulation of sodium oxybate, once-nightly rather than twice-nightly) extended the franchise further, demonstrating the layered 505(b)(2) strategy in practice [8].
Navigating the Data Exclusivity Bars and Patent Certifications
A 505(b)(2) application faces two potential timing obstacles that are absent from the ANDA pathway but that must be addressed before the FDA can approve it: data exclusivity attached to the reference listed drug and Orange Book patent certifications.
Data exclusivity arises when the RLD was approved with NCE exclusivity (five years) or with exclusivity for new clinical investigations (three years). For a five-year NCE exclusivity, the FDA cannot accept a 505(b)(2) application until four years after the RLD’s approval date (with the possibility of Paragraph IV certification triggering the 30-month stay, precluding final approval before the five-year mark). For a three-year data exclusivity on a new formulation or new indication, approval is blocked until the three years expire.
The practical implication is that a 505(b)(2) developer targeting a recently approved RLD must plan its development timeline around the exclusivity expiry. A drug approved in 2023 with NCE exclusivity cannot have a 505(b)(2) application accepted until 2027. If development takes three years and takes a further year through FDA review, the earliest possible approval is 2028 — by which time the NCE exclusivity has expired and the formulation innovation alone must justify the market position.
Patent certifications follow the same structure as ANDA patent certifications. The 505(b)(2) applicant must make one of four certifications for each Orange Book patent listed for the RLD: Paragraph I (the patent has expired), Paragraph II (the patent will expire before the approval date requested), Paragraph III (the applicant will wait until the patent expires), or Paragraph IV (the patent is invalid or will not be infringed by the 505(b)(2) product) [9]. A Paragraph IV certification triggers the same 30-month stay mechanism available against ANDAs, and the same litigation dynamics — the brand files infringement suits, the 30-month clock runs, and the 505(b)(2) applicant either litigates, settles, or waits.
A well-designed 505(b)(2) product should, where possible, be formulated to non-infringe relevant Orange Book patents through product design rather than patent certification litigation. If the reformulation approach inherently avoids the specific claims of the RLD’s formulation patents — using different excipients, different release mechanisms, different particle engineering approaches — a Paragraph IV certification asserting non-infringement may be technically supportable without the costs and timeline risks of full patent litigation.
Part Five: The Intellectual Property Architecture for 505(b)(2) Products
Why You Need Your Own Patents — The Commercial Logic
A 505(b)(2) product that relies entirely on the RLD’s patent position for market protection is a product whose commercial life is constrained by someone else’s IP strategy. The developer that builds a 505(b)(2) product without its own patents is building a product that can, in principle, be copied by another 505(b)(2) applicant as soon as the RLD’s data exclusivity and patents expire — and that is subject to Paragraph IV challenge by ANDA filers against the reformulated product’s own Orange Book listings.
The IP strategy for a 505(b)(2) product has a specific objective: generate formulation patents that are independently valid, that directly cover the commercial product as approved, and that expire significantly later than the RLD’s original patent position. If executed well, the 505(b)(2) product has more effective remaining exclusivity than the RLD it references — because the formulation patents were filed late in the development timeline and expire fifteen to twenty years from that filing date, while the RLD’s composition-of-matter patent was filed at or before IND years earlier.
The categories of patents typically available to a 505(b)(2) developer track the product’s innovations:
Formulation patents covering the specific composition, process, or structural attributes of the new dosage form. Extended-release matrices, nanoparticle suspensions, abuse-deterrent systems, drug-device combinations — these all generate patentable formulation inventions if designed with patent protection in mind from the start of development.
Method-of-use patents covering the therapeutic application enabled by the new formulation’s specific pharmacokinetic profile. A once-weekly oral formulation that enables dosing regimens not achievable with the daily oral or injectable, a transdermal patch that maintains stable plasma concentrations sufficient to support a new indication — these generate method-of-use claims independent of the underlying molecule.
Method-of-manufacture patents covering the manufacturing process for the novel formulation, particularly relevant when the process is non-obvious given the published state of formulation science and when it enables the specific product characteristics that make the formulation clinically valuable.
Device patents covering the delivery mechanism when the 505(b)(2) product is a drug-device combination — the specific autoinjector design, the dry powder inhaler configuration, the prefilled syringe with specific safety features.
The filing strategy should layer these categories with staggered expiration dates, precisely as described for large-molecule franchise management in the prior analysis. The goal is a patent portfolio that provides meaningful protection at the commercial product level even after the earliest-filed formulation patents expire.
The Obviousness Problem: When Your Formulation Innovation Is Too Clean
The primary IP challenge for 505(b)(2) developers is that the best formulation innovations — the ones that generate the clearest clinical rationale and the easiest regulatory path — are sometimes also the most obvious from a patent perspective. An extended-release formulation of a drug with a known half-life that requires twice-daily dosing is a commercially compelling development target, but it is also the exact kind of project that ANDA filers and IPR petitioners will attack as obvious: “Given the known pharmacokinetics of compound X and the well-developed state of extended-release matrix technology at the time of filing, formulating compound X as an extended-release matrix was within the ordinary skill of the art.”
The defense against this obviousness challenge requires building into the formulation evidence of unexpected results — specific technical challenges encountered in formulating the compound in the claimed manner, specific performance attributes of the formulation that exceeded what the art would have predicted, or a specific combination of formulation attributes that the prior art taught away from. The FDA approval itself can provide supporting evidence: if the FDA required specific studies to characterize unexpected pharmacokinetic behavior of the new formulation, that is evidence that the formulation’s attributes were not predictable from the prior art.
This means that the patent strategy for a 505(b)(2) program needs to be integrated into the clinical development program from the beginning, not appended as an afterthought at the end. The scientists designing the formulation and the clinical program should be aware of what technical data will later be needed to support the patent claims — and should be collecting that data in the course of normal development work rather than scrambling to generate it post hoc.
Data Exclusivity as a Patent Supplement — Not a Replacement
When a 505(b)(2) application is approved, the new product qualifies for three years of data exclusivity for the information in the application that required new clinical investigations conducted by or for the applicant — typically the bioavailability studies and any additional clinical trials [10]. This three-year exclusivity is protection for the specific clinical data package, not for the reference molecule itself. It means that no other 505(b)(2) applicant can, for three years, rely on the data generated in the approved application to support its own application — a competitor must generate its own clinical data package or wait out the exclusivity.
The three-year exclusivity is not a substitute for formulation patents. It blocks direct copying of the specific data package for three years, but it does not prevent a competitor from developing a different formulation of the same molecule, generating a separate clinical package, and filing a competing 505(b)(2) application. And three years is a short commercial window — long enough to establish market position but not long enough to build a sustainable franchise without the patent protection described above.
The most secure commercial position for a 505(b)(2) product combines three-year data exclusivity (active during the early commercial period) with formulation patents (providing protection for fifteen to twenty years from filing date) with Orange Book listing of those patents (triggering 30-month stays against Paragraph IV challenges from future ANDA or 505(b)(2) filers). Each layer fills a different temporal gap in the exclusivity architecture.
Part Six: CMC Strategy — Where Most 505(b)(2) Programs Actually Fail
The Chemistry, Manufacturing, and Controls Challenge
The 505(b)(2) pathway reduces the clinical burden substantially, but it does not reduce the chemistry, manufacturing, and controls (CMC) requirements. The FDA expects the same manufacturing quality standards for a 505(b)(2) product as for any other approved drug. The applicant must demonstrate that the manufacturing process consistently produces a product meeting its specifications, that the product is stable throughout its proposed shelf life, and that the analytical methods used to characterize the product are validated and suitable for their purpose.
For novel dosage forms — extended-release matrices, nanoparticle suspensions, transdermal systems — the CMC challenge can be as significant as the clinical challenge. Extended-release matrix formulations require rigorous in vitro dissolution method development and correlation with in vivo pharmacokinetic data; the FDA’s approval of the product is premised on a correlation between the in vitro dissolution profile and the in vivo pharmacokinetic exposure that must be demonstrated and validated. Nanoparticle formulations require characterization of particle size distribution, surface charge, and physical stability under conditions that may not be fully developed in the scientific literature for a given compound.
The most common cause of 505(b)(2) application rejection — or delay — is not clinical inadequacy. It is CMC deficiency: inadequate analytical method validation, insufficient stability data, manufacturing process variability that was not characterized before the NDA was filed, or in vitro-in vivo correlations that the FDA finds insufficiently robust to support the claims made about the product’s performance.
The implication is that CMC investment should not be deferred or under-resourced relative to clinical investment. A $50 million 505(b)(2) program that spends $35 million on clinical work and $15 million on CMC may fail at the CMC stage, wasting the clinical investment. A better-balanced program invests adequately in manufacturing process development, analytical characterization, and stability studies from the beginning — even though this investment is less visible and less exciting than clinical trial enrollment.
Contract Development and Manufacturing Organizations (CDMOs): The Infrastructure Advantage
One of the structural advantages of 505(b)(2) development relative to NME development is the availability of sophisticated contract development and manufacturing organizations (CDMOs) with existing expertise in the specific dosage form being developed. Extended-release systems, transdermal patches, nanotechnology-based formulations, modified-release pellets — the major CDMOs (Lonza, Catalent, Thermo Fisher/Patheon, Samsung Biologics) have built deep technical expertise in each of these technologies and have developed these formulations for many drugs already.
Partnering with a CDMO that has previously developed a similar dosage form means accessing accumulated process knowledge that would otherwise take years to build internally. The CDMO has solved the dissolution method development problem, the physical stability challenge, and the scale-up characterization for similar products before. The 505(b)(2) developer benefits from that accumulated expertise without having to build it from scratch.
The CDMO relationship requires active management. The developer must clearly specify the target product profile — the pharmacokinetic targets, the desired in vitro dissolution profile, the stability requirements — before the CDMO begins formulation work. A poorly specified target product profile produces a CDMO-designed formulation that may not meet the clinical objectives, requiring expensive reformulation cycles that erode the timeline advantage of the 505(b)(2) pathway.
Early engagement with the CDMO — before the pre-NDA meeting, not after — allows the developer to incorporate manufacturing feasibility considerations into the development plan and to identify potential CMC challenges before they become program-stopping obstacles. The CDMO’s formulation experience is most valuable when it is integrated into the development strategy from the beginning.
Part Seven: Commercial Strategy — Turning a 505(b)(2) Approval into a Franchise
Formulary Access: The Biggest Challenge No One Talks About
FDA approval is not commercial success. It is a license to compete. The actual commercial challenge for a 505(b)(2) product is gaining formulary access at a tier that enables patient access at a co-pay that drives prescribing.
Pharmacy benefit managers and managed care organizations have become increasingly sophisticated in their evaluation of 505(b)(2) products. The standard they apply is clinical differentiation: does this new formulation deliver meaningful clinical benefit over the generic immediate-release formulation that costs 90 percent less? If the answer is “modestly improved pharmacokinetics in pharmacokinetic studies but no demonstrated outcomes benefit,” the payer will place the 505(b)(2) product on a high co-pay tier or require prior authorization, effectively limiting market penetration regardless of FDA approval.
The commercial strategy for a 505(b)(2) product must therefore generate clinical evidence of meaningful benefit — not just regulatory evidence of safety and adequate pharmacokinetic characterization. This means designing the clinical program to generate outcomes data that payers find compelling, not just bioavailability data that satisfies the FDA’s regulatory standard.
The gap between regulatory adequacy and commercial adequacy is one of the most common miscalculations in 505(b)(2) development. A company can spend $50 million developing a product that receives FDA approval and then fail commercially because the payer community refuses to differentiate it from the generic on formulary. This is not a regulatory failure — it is a market failure driven by insufficient investment in generating the clinical evidence needed to justify formulary access.
The companies that succeed with 505(b)(2) products consistently generate this additional clinical evidence — responder analyses showing improved outcomes in specific patient populations, quality-of-life studies showing adherence advantages, real-world evidence studies showing reduced hospitalization rates — and invest in medical affairs programs that communicate this evidence to formulary committees and prescribers. The FDA approval gets you in the door. The payer evidence keeps you there.
Pricing Strategy for 505(b)(2) Products
Pricing a 505(b)(2) product requires balancing two competing pressures: capturing a premium sufficient to justify the development investment and fund the commercial launch, and maintaining a price differential over the generic that does not become the primary objection in formulary negotiations.
The standard pricing framework for a 505(b)(2) product prices the new formulation at a premium to the branded RLD (if the branded RLD is still on the market) and at a substantial premium to the generic RLD, justified by the clinical differentiation evidence. The exact premium is determined by the strength of that evidence and by the competitive landscape in the therapeutic class.
For CNS drugs — ADHD, epilepsy, anxiety, depression — where patient-specific dosing variability and tolerability differences drive substantial prescriber preference, 505(b)(2) products have historically maintained premiums of 3x to 10x the generic immediate-release formulation. The clinical rationale (peak-related adverse effects, adherence benefits, once-daily versus multiple-daily dosing) is well understood by prescribers and by payers in high-prescribing specialties, enabling formulary access at preferred branded tiers.
For cardiovascular and metabolic drugs, where outcomes data is more rigorous and payer scrutiny more intense, the premium is typically smaller and the formulary access requirement for evidence is higher. A 505(b)(2) cardiovascular drug that cannot demonstrate outcomes benefit over the generic IR in a reasonably sized outcomes study will struggle to maintain a premium beyond the first contract cycle.
The Geographic Expansion Opportunity
A frequently underused dimension of 505(b)(2) strategy is geographic expansion. The 505(b)(2) pathway is a U.S. regulatory concept, but the underlying logic — relying on established scientific literature and prior regulatory findings to reduce the clinical data package required for new formulation approval — has equivalents in other jurisdictions:
The EU’s Article 10(3) “hybrid application” pathway allows applicants to reference the established safety profile of an approved active substance while providing new data to support a different formulation or new indication [11]. The bridging data requirements are similar to U.S. 505(b)(2), though the specific standards for what constitutes an adequate bridge differ.
Japan’s regulatory framework has Partial Change Approval applications for modifications to approved drugs that follow a similar logic, with requirements calibrated to the nature and magnitude of the change.
Health Canada’s hybrid approach to new drug submissions mirrors the 505(b)(2) structure closely, with established drug submissions relying on previously published safety and efficacy data.
A 505(b)(2) product with a strong clinical package approved in the U.S. often has a credible path to approval in the EU, Canada, Japan, and key emerging markets using the U.S. clinical data as the primary evidence base, supplemented by smaller bridging studies in local populations where required by local authorities. The marginal cost of these additional approvals, relative to the U.S. development cost, is low — primarily regulatory affairs costs and bridging study costs.
The developer that plans the clinical program with international regulatory requirements in mind from the beginning — collecting data across diverse patient populations, using internationally recognized reference standards, filing investigational new drug applications in multiple jurisdictions in parallel — can achieve multi-jurisdictional approval at modest incremental cost over the U.S. program.
Part Eight: The Competitive Intelligence Discipline
Monitoring the 505(b)(2) Pipeline to Protect Your Position
Once a 505(b)(2) product is approved and commercially launched, the company holding the NDA must actively monitor for competing 505(b)(2) and ANDA filings against its own product. This monitoring is not optional — it is operational intelligence that drives patent strategy, pricing strategy, and commercial resource allocation.
The FDA’s drugs@FDA database provides public access to all approved NDA and ANDA applications, including 505(b)(2) approvals. New ANDA filings that reference a 505(b)(2) product’s NDA as the RLD appear as Paragraph IV certification notices sent to the NDA holder. The 45-day window to file an infringement suit and trigger the 30-month stay is measured from receipt of that notice.
DrugPatentWatch automates the monitoring process that would otherwise require daily manual review of FDA databases, patent assignment records, and PTAB docket filings. Its alert system can notify a 505(b)(2) NDA holder when a new ANDA is filed referencing its product, when an IPR petition is filed challenging a key formulation patent, when a competitor files a 505(b)(2) application for a competing reformulation of the same active ingredient, or when a patent in the Orange Book for the product is approaching a triggering expiration date. For a mid-sized specialty pharma company managing a portfolio of 505(b)(2) products, this kind of automated intelligence infrastructure is what separates proactive IP defense from reactive crisis management.
The Paragraph IV Defense Strategy for 505(b)(2) Products
A successful 505(b)(2) product will receive Paragraph IV challenges from ANDA filers. This is predictable and should be planned for, not treated as a surprise when it arrives. The 505(b)(2) NDA holder has the same tools available as any NDA holder: the 45-day suit filing window, the 30-month stay, and the substantive patent litigation that follows.
The specific vulnerabilities of 505(b)(2) formulation patents in Paragraph IV litigation are worth understanding in advance. Formulation patents are typically challenged on two grounds: obviousness (the formulation was within the ordinary skill of the art given the prior published formulation literature) and non-infringement (the generic’s formulation does not use the same components or mechanisms claimed in the patent).
Obviousness challenges to formulation patents succeed at higher rates than obviousness challenges to composition-of-matter patents, because formulation science is highly developed and the prior art for common dosage form technologies is rich. An extended-release matrix patent that does not adequately distinguish the claimed formulation from the prior art by generating unexpected results evidence is vulnerable. A matrix patent supported by data demonstrating unexpected in vitro-in vivo correlation improvements, unexpected stability advantages, or unexpected tolerability improvements is more defensible.
The pre-litigation preparation that matters most is the same internal analysis that should have been conducted before filing the patent: identifying the most challenging prior art, preparing the narrative of unexpected results, retaining expert witnesses with relevant formulation science backgrounds, and documenting the evidence of non-obviousness that was generated during development. Companies that maintain rigorous scientific documentation of development work — not just the data required for the NDA, but the technical decision history and the experiments that led to the final formulation — have substantially better litigation records.
Watching Your Competitors’ Filings
The 505(b)(2) market is not a secret. Every NDA approval is public. The FDA’s drug approval database lists every approved NDA, including 505(b)(2) approvals, with the date of approval, the reference listed drug, and the proprietary name of the approved product. ANDA filings, when made public through Paragraph IV notice letters, reveal which generic manufacturers are targeting specific 505(b)(2) products.
What is less visible — but still trackable through systematic patent monitoring — is the pre-approval pipeline of competing 505(b)(2) products. A competitor developing its own reformulation of the same active ingredient will be filing patent applications covering its formulation eighteen months before those applications publish. Systematic monitoring of published patent applications in the relevant formulation technology space, filtered by the active ingredients of strategic interest, provides advance warning of competitive reformulation programs before they reach the NDA filing stage.
This intelligence has direct strategic value. If a competitor is filing patents covering a once-monthly extended-release formulation of a molecule for which you have a once-weekly formulation, it signals a competitive threat to your market position that will arrive in three to five years. The strategic response — filing continuation patents that expand your own coverage, accelerating a second-generation reformulation program, or strengthening commercial relationships with key prescribers — is best initiated early, not at the moment the competitive NDA is filed.
Part Nine: Special Cases — Abuse-Deterrent Formulations, Combination Products, and Biosimilar-Adjacent Strategies
Abuse-Deterrent Formulations: The 505(b)(2) Pathway’s Highest-Profile Application
No category of 505(b)(2) product has generated more commercial attention, more policy debate, or more litigation than abuse-deterrent formulations (ADFs) of opioid analgesics. The FDA’s ADF guidance establishes a framework in which a new formulation of an opioid that incorporates physical or chemical barriers to abuse — making it resistant to crushing, dissolving, or other preparation for non-oral routes of administration — can be approved via 505(b)(2) and can carry labeling stating that it “has properties that are expected to deter abuse” [12].
The commercial logic is clear: an abuse-deterrent opioid can be positioned as a differentiated product in a market saturated by generics of the original formulation, justified by a genuine public health rationale (deterring diversion and misuse) and supported by the FDA’s formal recognition of the ADF category. Purdue Pharma’s reformulated OxyContin — the extended-release, polyethylene oxide matrix version — is the most widely cited example, generating billions in revenue after the original composition-of-matter patent expired, primarily because the FDA’s 2013 decision to deny approval to generic versions of the original formulation (on the grounds that the original formulation was no longer marketed and therefore no appropriate reference existed) effectively created a protected market for the ADF version for several years.
The Purdue OxyContin ADF strategy generated substantial criticism from public health and antitrust perspectives, and the FDA has since refined its guidance on when it will decline to approve generics of non-ADF opioids. The broader 505(b)(2) ADF strategy, however — developing genuinely differentiated opioid formulations with physical abuse deterrence — remains a legitimate development approach for companies with the technical capability and the clinical development infrastructure to pursue it.
The key requirement is that the ADF properties be genuine. The FDA requires clinical evidence — typically human abuse potential studies comparing routes of administration between the ADF and the non-ADF reference, plus in vitro manipulation studies — that the formulation actually deters the specific abuse behaviors it claims to address. A formulation that merely changes the tablet coating without incorporating functional abuse deterrence will not receive ADF labeling and will not command the associated market position.
Fixed-Dose Combinations: The Adherence-Driven 505(b)(2)
Fixed-dose combination (FDC) products — single dosage forms combining two or more established active ingredients — represent one of the clearest 505(b)(2) value propositions available. The clinical rationale is adherence: patients who take one pill per day adhere to their therapy at higher rates than patients taking two or three separate pills per day, and improved adherence in chronic conditions translates directly to improved outcomes [13].
The FDA’s FDC approval framework under 505(b)(2) requires the applicant to demonstrate the contribution of each component to the claimed therapeutic effect — typically through a factorial study design that compares the combination to each component alone. This requirement adds clinical program cost relative to a simple reformulation 505(b)(2), but it is substantially less expensive than establishing two entirely new agents in a new indication from scratch.
The commercial history of FDCs in HIV, cardiovascular disease, and diabetes management is unambiguously positive. Gilead’s Atripla, Stribild, and Genvoya built a multi-billion-dollar HIV franchise through sequential FDC development. The cardiovascular FDC space has produced numerous successful products — amlodipine/olmesartan (Azor), amlodipine/valsartan (Exforge), and many others — that maintained market position well past the individual components’ patent expirations by combining components into products with independent formulation patent protection.
The target identification framework for FDC development is slightly different from single-agent reformulation: the developer is looking for therapeutic areas where multiple guideline-recommended therapies are used concurrently, where pill burden is clinically meaningful, where the pharmacokinetic profiles of the candidate components are compatible (similar half-lives, no problematic food interactions in combination, no pharmacokinetic interactions that complicate dosing), and where no FDC of those specific components yet exists.
DrugPatentWatch’s combination product database is a useful starting point for this analysis, flagging approved FDCs, pending FDC applications, and the patent positions of the individual components being combined — giving developers a map of what has already been done and where the remaining white space exists.
Prodrug Development: The 505(b)(2) Gateway to NCE Economics at 505(b)(2) Cost
A prodrug is an inactive compound that converts to an active drug in the body through metabolic processes. When the active drug — the parent molecule — is an established, off-patent compound, a prodrug of that compound may qualify as a new chemical entity (receiving NCE exclusivity) while relying on the parent compound’s established safety and efficacy profile through the 505(b)(2) pathway.
This dual status is not a contradiction — it is a specific feature of the regulatory framework, confirmed by FDA guidance. A prodrug that is itself a new chemical entity can receive five years of NCE exclusivity while its NDA relies, in part, on the FDA’s prior findings for the parent compound. This gives the prodrug developer the cost advantages of 505(b)(2) development (no need to re-establish the parent’s basic pharmacology and toxicology) and the exclusivity advantages of NCE status (five years of data protection rather than three).
Vyvanse is the clearest modern example. Lisdexamfetamine dimesylate, the active ingredient in Vyvanse, is a prodrug of d-amphetamine. D-amphetamine is an established molecule with decades of regulatory history. Lisdexamfetamine itself is a new chemical entity. Shire’s development program relied on the established pharmacology of d-amphetamine while generating new clinical evidence for the prodrug’s specific pharmacokinetic profile and clinical performance [14]. The resulting NDA received NCE exclusivity, and the formulation innovation (the prodrug structure inherently limiting the drug’s manipulability for abuse) was separately patented.
The prodrug approach requires genuine chemical innovation — a prodrug that simply esterifies an active molecule without generating a stable, manufacturable, non-toxic prodrug with the desired pharmacokinetic characteristics is not commercially viable. But for developers with medicinal chemistry capabilities, the prodrug strategy can produce products with the commercial durability of NCEs at development costs closer to standard 505(b)(2) programs.
Part Ten: The Future of 505(b)(2) — Where the Opportunity Is Largest
The IRA Patent Cliff and the Window It Creates
The Inflation Reduction Act’s drug price negotiation provisions — discussed in the prior analysis of pharmaceutical patent strategy — create a specific opportunity window for 505(b)(2) developers. As small-molecule drugs approach their nine-year negotiation eligibility threshold, the commercial value of those products decreases, reducing the incentive for the original NDA holder to invest in lifecycle management. Products that the original developer has chosen not to reformulate — because the IRA’s pricing constraints reduce the return on lifecycle management investment — become available targets for independent 505(b)(2) developers.
The 505(b)(2) developer is not subject to the IRA’s negotiation provisions for its own product until nine years after its own approval date. A 505(b)(2) product approved in 2027, for a molecule where the original NDA holder’s product became negotiation-eligible in 2025, has nine additional years of free-pricing exclusivity from 2027 — a meaningful commercial advantage over the referenced product whose price is now constrained by the negotiated ceiling.
This dynamic is not yet fully priced into the market’s evaluation of 505(b)(2) opportunities. As the IRA’s negotiation provisions are implemented and their pricing effects become visible in specific therapeutic classes, the molecules where original NDA holder lifecycle management investment has stalled will become identifiable — and DrugPatentWatch’s commercial analytics can help developers track which products are approaching or have already crossed the negotiation eligibility threshold without significant reformulation activity.
Gene and Cell Therapy Delivery: The Next 505(b)(2) Frontier
The 505(b)(2) pathway has historically been applied to small-molecule drugs. Its extension to gene therapy and cell therapy delivery platforms is an emerging area that could significantly expand the pathway’s scope. Gene therapies and RNA-based medicines face substantial delivery challenges — in vivo delivery to target tissues, endosomal escape, immunogenicity, manufacturing scale — that are, in principle, the kind of formulation problems the 505(b)(2) pathway was designed to address when those problems exist in the context of an established active ingredient or mechanism.
The FDA’s guidance on 505(b)(2) applications for complex drug products — including drug-device combinations, nanoparticle formulations, and liposomal formulations — has been expanding, and the agency has approved 505(b)(2) applications for increasingly complex drug products. As RNA therapeutics and gene therapies targeting validated mechanisms (PCSK9, TTR, HIF2α) become established, novel delivery formulations of these validated mechanisms could theoretically follow the 505(b)(2) model: rely on the established pharmacology of the target mechanism, provide new data demonstrating the delivery system’s safety and pharmacokinetic performance, and build the commercial product around the delivery innovation.
This application of 505(b)(2) logic to complex biologics and gene therapies is not currently codified in FDA guidance, and the specific regulatory requirements for such applications have not been definitively established. But the conceptual framework — reducing clinical development cost by relying on established scientific findings and focusing the clinical program on the specific innovation — is consistent with the FDA’s general approach to development efficiency.
Personalized Medicine and the 505(b)(2) Specific Patient Population Strategy
One of the most commercially interesting applications of the 505(b)(2) pathway for the next decade is the development of reformulations specifically optimized for patient populations poorly served by existing formulations: pediatric patients, geriatric patients, patients with renal or hepatic impairment, patients with swallowing difficulties, and patients with specific pharmacogenomic profiles that alter drug metabolism.
The pediatric 505(b)(2) opportunity is particularly well-defined. Many widely used drugs were originally developed for adult populations, with pediatric dosing characterized through off-label use rather than formal pediatric clinical programs. The FDA’s pediatric exclusivity and pediatric study requirement framework creates incentives for developers to generate formal pediatric pharmacokinetic and safety data. A developer that creates a pediatric-specific formulation of an established drug — liquid formulation, orally disintegrating tablet, age-appropriate flavoring and dosing precision — and files a 505(b)(2) application with a pediatric clinical program qualifies for pediatric exclusivity and for three years of data exclusivity on the pediatric formulation.
The commercial size of individual pediatric indications is small relative to adult indications, but the competitive landscape is also less crowded, payer scrutiny is somewhat less intense (there is greater tolerance for branded pediatric formulations without generic equivalents), and the regulatory pathway is well-defined. A portfolio strategy focused on developing pediatric-specific formulations of established drugs across multiple therapeutic areas can build a defensible franchise at aggregate development costs significantly below NME-focused development.
Part Eleven: Building a 505(b)(2) Franchise — The Organizational Requirements
What Kind of Company Succeeds at 505(b)(2)
The organizational capabilities required for 505(b)(2) success differ from those required for NME development. The competencies that matter most are formulation science, regulatory strategy, and commercial market access — not the basic research and early clinical capabilities that drive NME pipelines.
A successful 505(b)(2)-focused company has a formulation science function capable of designing and iterating on dosage forms with the technical sophistication required to generate both an approvable NDA and a defensible patent position. It has regulatory affairs professionals with deep 505(b)(2) experience — specifically, experience writing the briefing documents for pre-NDA meetings, managing the FDA correspondence during the review, and responding to the CMC deficiencies that are most likely to delay approval. It has a commercial function capable of executing in the managed care environment, generating the payer evidence described earlier, and building the medical affairs infrastructure required to differentiate a 505(b)(2) product in a market that already has generics.
What this company does not need, relative to an NME-focused organization, is a large discovery research organization, a clinical pharmacology group running first-in-human studies, or the Phase I clinical unit infrastructure required for NME safety escalation studies. These costs — which are among the most significant fixed cost drivers of large pharmaceutical R&D organizations — are not required for a 505(b)(2) strategy executed correctly.
The private equity-backed specialty pharma model has been particularly successful at building these organizations. Companies like Jazz Pharmaceuticals, Supernus Pharmaceuticals, and Patheon (before its CDMO acquisition) were built specifically around the 505(b)(2) development and commercialization model, with organizational structures and talent profiles calibrated to the actual competencies the strategy requires.
Deal Structures: In-Licensing, Partnerships, and Asset Acquisition
Many 505(b)(2) programs are not built from scratch internally. They are assembled through partnerships, licensing transactions, and asset acquisitions — buying or licensing the rights to a 505(b)(2)-stage asset from an academic institution, a discovery stage startup, or a large pharmaceutical company that has decided the asset does not fit its pipeline strategy.
The valuation of a 505(b)(2)-stage asset — a formulation concept with published proof-of-concept pharmacokinetic data and a proposed regulatory strategy, but no IND and no FDA interaction — is substantially lower than the valuation of an NME at the same stage of development. This reflects both the smaller peak revenue expectations of most 505(b)(2) products and the residual regulatory and commercial risk before approval. The discount also creates acquisition opportunities for developers who have the regulatory and commercial execution capabilities that the asset’s prior holder lacked.
The key due diligence questions for a 505(b)(2) asset acquisition are analogous to the target selection criteria discussed earlier: Is the clinical rationale for the reformulation strong enough to generate payer-acceptable differentiation? Is the formulation innovation patentable in a way that provides durable exclusivity? Has the reference listed drug’s patent and data exclusivity position been fully mapped? Have competing 505(b)(2) applications for similar reformulations been filed or published?
Getting rigorous answers to these questions before closing an asset acquisition requires exactly the kind of patent and regulatory landscape analysis that DrugPatentWatch’s patent expiration tracking, Orange Book database, and Paragraph IV litigation history are designed to support. Due diligence on a 505(b)(2) asset without systematic patent landscape analysis is incomplete due diligence.
Conclusion
The 505(b)(2) pathway does not eliminate pharmaceutical development risk, and it does not guarantee commercial success. What it does is restructure the economic proposition of drug development so radically that a category of products — reformulations, new delivery systems, new indications for established molecules — can be developed at a cost and timeline that opens the opportunity to a much wider range of developers and investors than the full NME model permits.
The $2.6 billion average NME development cost is a real number, but it is the right number only for the right strategy. For a company that is not trying to synthesize a new chemical entity and prove it from first principles, the reference number is $20 million to $300 million for a 505(b)(2) program, with a three-to-five-year timeline for straightforward reformulations. The difference between these numbers is not a shortcut or a regulatory loophole. It is a different definition of what you are trying to accomplish — improving how an established molecule is delivered, not discovering a new molecule.
The companies that execute this strategy best — Jazz, Supernus, and a tier of less-visible specialty pharma operators — share several characteristics. They select targets rigorously, using competitive intelligence infrastructure to identify molecules where the clinical rationale is compelling, the payer environment supports differentiation, and the formulation innovation is patentable. They invest in CMC development with the same seriousness as clinical development. They engage the FDA early and specifically, through pre-NDA meetings that clarify the clinical data requirements before the clinical work is done. And they build IP portfolios that protect the 505(b)(2) product’s commercial life well beyond the referenced drug’s original patent position.
The 505(b)(2) opportunity is not a niche. The pharmaceutical market is full of molecules with established safety profiles and suboptimal formulations, with generic competition reducing incentive for the original NDA holders to invest in reformulation, and with clinical needs unmet by the existing commercial products. Finding those molecules, building the case for the improvement, and executing the development program at the cost and speed the pathway permits — that is where the real 90% cost reduction lives.
Key Takeaways
- The 505(b)(2) pathway cuts drug R&D costs from $2.6 billion to $20-300 million by relying on the FDA’s prior safety and efficacy findings for the referenced drug. The applicant does not reproduce the original molecule’s clinical development history — it supplements it with evidence for the specific innovation being made.
- Target selection is the highest-leverage decision in a 505(b)(2) program. A molecule with established safety, a clear pharmacokinetic improvement opportunity, a patentable formulation innovation, and a payer environment that supports clinical differentiation can support a commercial franchise worth far more than the development cost. A molecule that lacks any one of those characteristics is a commercial risk that patent protection cannot fully offset.
- The pre-NDA meeting with FDA is not optional — it is the single most risk-reducing investment available before clinical work begins. A Type B meeting that produces clear FDA guidance on the required clinical package eliminates the most common category of 505(b)(2) failure: building the wrong clinical program.
- CMC failure is more common than clinical failure in 505(b)(2) programs. The formulation science, analytical characterization, and stability work required to support a novel dosage form NDA require the same investment rigor as the clinical program.
- A 505(b)(2) product without its own formulation patents is a commercial asset without durable protection. Three years of data exclusivity provides a commercial launch window, not a franchise. The layered patent portfolio — formulation, method-of-use, device — is what converts an FDA approval into a multi-year revenue stream.
- Payer access requirements are more stringent than FDA approval requirements for commercial success. The clinical evidence needed to justify formulary position at a meaningful premium over the generic often exceeds the evidence required for FDA approval. Plan the clinical program for the payer, not just the regulator.
- DrugPatentWatch and equivalent patent analytics platforms are essential infrastructure for 505(b)(2) target identification, competitive monitoring, and patent litigation preparation. Systematic monitoring of Orange Book listings, ANDA filings, and competitor patent publications is the intelligence foundation on which specific development and IP strategy decisions are made.
- The IRA’s drug price negotiation provisions are creating new 505(b)(2) windows. As small-molecule drugs approach their nine-year negotiation eligibility threshold, original NDA holders’ incentive to invest in lifecycle management decreases, leaving reformulation opportunities for independent 505(b)(2) developers whose approval timelines reset the negotiation eligibility clock.
Frequently Asked Questions
Q1: Can a 505(b)(2) application reference a drug that is only approved outside the United States?
Yes, under FDA regulations and guidance, a 505(b)(2) applicant can rely on published literature describing foreign clinical experience with a drug, even if that drug has never been approved in the U.S. [3]. The applicant cannot reference a foreign approved drug the way it references a U.S. reference listed drug (triggering the Orange Book patent certification requirements), but it can include that foreign data as part of the published literature on which the application relies. In practice, this means a drug approved in the EU or Japan but not the U.S. can form part of the scientific basis for a U.S. 505(b)(2) application, provided the applicant can adequately characterize how the foreign clinical experience supports the safety and efficacy of the U.S. product being developed. This is particularly relevant in therapeutic areas where regulatory approval timelines differ materially between the U.S. and Europe, and where a U.S. developer wants to reference European clinical experience rather than starting from scratch.
Q2: How does a 505(b)(2) product qualify for pediatric exclusivity, and is it worth pursuing?
A 505(b)(2) NDA holder can receive a Written Request from the FDA asking it to conduct pediatric studies of the 505(b)(2) product, and if it conducts and submits those studies, it receives six months of pediatric exclusivity attached to all currently listed Orange Book patents [7]. The commercial value of pediatric exclusivity on a 505(b)(2) product is proportional to the product’s annual revenues and to the length of remaining patent life to which the exclusivity attaches. On a product generating $500 million annually, six months of exclusivity is worth roughly $250 million in preserved revenues — a compelling return on a pediatric study investment of $20 to $50 million. The timing requirement is the same as for any NDA holder: the study must be completed and submitted before the last Orange Book patent expires. 505(b)(2) developers who file formulation patents late in development, extending their patent position into the product’s commercial years, are in the best position to capture pediatric exclusivity’s full value because the exclusivity attaches to patents with significant remaining life.
Q3: What happens if the FDA asks for more clinical data during the NDA review than the pre-NDA meeting guidance indicated?
This happens, and it is one of the more frustrating aspects of 505(b)(2) development, because the pre-NDA meeting is not a binding commitment by the FDA to accept the proposed data package. The FDA’s Complete Response Letter (CRL) can ask for additional studies — typically additional bioavailability data, more robust dissolution characterization, or additional safety data in a specific subpopulation — even if the pre-NDA meeting briefing did not explicitly identify those requirements. The best protection against unexpected CRL requirements is comprehensive pre-NDA meeting preparation: raise every potential data gap proactively in the briefing document, ask explicitly whether the proposed package is adequate, and document the FDA’s specific responses. A CRL that requests studies not mentioned in the pre-NDA meeting can sometimes be challenged through formal dispute resolution if the applicant believes the FDA’s position is inconsistent with its prior guidance. More practically, the risk of unexpected clinical data requests is lower in therapeutic areas with well-established 505(b)(2) precedent — multiple prior approvals — and higher in novel delivery system categories where the FDA is establishing requirements for the first time.
Q4: Is there an advantage to filing a 505(b)(2) application rather than pursuing a full NDA for a new prodrug of an established molecule?
The choice between a 505(b)(2) application and a full 505(b)(1) NDA for a new prodrug involves a specific trade-off. The 505(b)(2) route is available when the application relies, at least in part, on published literature or FDA’s prior findings for the parent compound, reducing the clinical data package required. The full 505(b)(1) route generates a purely self-referencing application and does not require the patent certification step for the parent compound’s Orange Book patents — but it requires a complete clinical data package independent of the parent. For most prodrug development programs, the 505(b)(2) route is preferable: it reduces development cost by leveraging the parent compound’s established pharmacology, and the patent certification requirement, while adding an additional step, is manageable through either design-around formulation or Paragraph IV litigation strategy. The full 505(b)(1) route is worth considering when the parent compound has extensive Orange Book listings that would trigger a large number of Paragraph IV certifications and associated 30-month stays — a scenario where the litigation cost and timeline risk of the certification process could materially delay approval or complicate the development program.
Q5: How should a 505(b)(2) developer think about the 180-day generic exclusivity when its own product eventually faces ANDA challenges?
When a 505(b)(2) NDA holder’s product faces its first Paragraph IV ANDA challenge, the generic’s first-filer exclusivity dynamic applies to the 505(b)(2) product’s Orange Book patents exactly as it applies to any NDA. The first Paragraph IV ANDA filer receives 180 days of generic exclusivity — a period during which no other generic can be approved for the same product. From the 505(b)(2) NDA holder’s perspective, this means the first generic entry is followed by a 180-day period of brand plus one-generic competition, before the market opens fully to multiple generic entrants. The authorized generic strategy — launching an authorized generic of the 505(b)(2) product during the first filer’s 180-day exclusivity period — is as available to a 505(b)(2) NDA holder as to any other NDA holder, and can capture meaningful market share during the transition. The more important preparation, however, is ensuring that the 505(b)(2) product’s formulation patents are strong enough to sustain the Paragraph IV litigation, because the value of the authorized generic strategy depends on the brand maintaining enough market share to make the authorized generic worth launching. A product that loses the Paragraph IV case quickly and loses most of its market share immediately is not worth the operational complexity of an authorized generic program.
Citations
[1] DiMasi, J. A., Grabowski, H. G., & Hansen, R. W. (2016). Innovation in the pharmaceutical industry: New estimates of R&D costs. Journal of Health Economics, 47, 20–33. https://doi.org/10.1016/j.jhealeco.2016.01.012
[2] Gottlieb, S. (2002). Examining the FDA’s 505(b)(2) pathway. Journal of Generic Medicines, 1(1), 55–60.
[3] 21 C.F.R. § 314.54 (2023). Procedure for submission of a 505(b)(2) application requiring investigations for approval of a new condition of use or new dosage form. Code of Federal Regulations.
[4] Hay, M., Thomas, D. W., Craighead, J. L., Economides, C., & Rosenthal, J. (2014). Clinical development success rates for investigational drugs. Nature Biotechnology, 32(1), 40–51. https://doi.org/10.1038/nbt.2786
[5] SHIRE US INC. (2000). Concerta (methylphenidate HCl) extended-release tablets NDA 021121. U.S. Food and Drug Administration.
[6] U.S. Food and Drug Administration. (2017). Formal meetings between the FDA and sponsors or applicants of PDUFA products: Guidance for industry. FDA.
[7] U.S. Food and Drug Administration. (2014). Bioavailability and bioequivalence studies submitted in NDAs or INDs: General considerations: Guidance for industry. FDA.
[8] Jazz Pharmaceuticals. (2022). Lumryz (sodium oxybate) NDA 214755 approval letter. U.S. Food and Drug Administration.
[9] 21 C.F.R. § 314.52 (2023). Notice of certification of invalidity or noninfringement of a patent. Code of Federal Regulations.
[10] 21 U.S.C. § 355(c)(3)(E)(iii) (2023). Three-year exclusivity for new clinical investigations. United States Code.
[11] Directive 2001/83/EC of the European Parliament and of the Council of 6 November 2001 on the Community code relating to medicinal products for human use, Article 10(3). Official Journal of the European Union.
[12] U.S. Food and Drug Administration. (2015). Abuse-deterrent opioids: Evaluation and labeling: Guidance for industry. FDA.
[13] Bangalore, S., Kamalakkannan, G., Parkar, S., & Messerli, F. H. (2007). Fixed-dose combinations improve medication compliance: A meta-analysis. The American Journal of Medicine, 120(8), 713–719. https://doi.org/10.1016/j.amjmed.2006.08.033
[14] Shire BioPharma. (2007). Vyvanse (lisdexamfetamine dimesylate) NDA 021977 approval letter. U.S. Food and Drug Administration.