Part 1: The Market Reality Behind Analytical Similarity
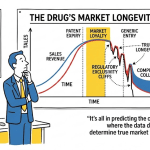
The Patent Cliff Driving a $185 Billion Opportunity
The global biosimilar market was valued at approximately $26.5 billion in 2024. Forecasters at IMARC Group project it reaches $185.1 billion by 2033, a compound annual growth rate above 24%. That number is not speculative optimism; it is arithmetic. A specific set of biologic drugs, each with annual revenues ranging from $3 billion to $21 billion, is losing patent protection on a known schedule, and biosimilar developers are lined up to compete for each one.
The blockbusters at the center of this shift include adalimumab (AbbVie’s Humira), bevacizumab (Roche/Genentech’s Avastin), trastuzumab (Roche/Genentech’s Herceptin), etanercept (Pfizer/Amgen’s Enbrel), rituximab (Roche/Genentech’s Rituxan), and ustekinumab (Janssen’s Stelara). Together, these six molecules generated well over $50 billion in combined annual revenue at their peak. Their IP estates are either expired, actively litigating, or scheduled to expire before 2030. Each represents a distinct risk profile, competitive landscape, and analytical development challenge.
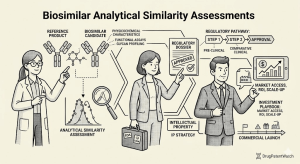
For an IP team or institutional investor, the analytical similarity assessment is not a regulatory technicality. It is the primary determinant of whether a biosimilar reaches the market at all, and how quickly. A poorly executed analytical package generates regulatory deficiency letters, extends timelines by 12 to 24 months, and can collapse the net present value of a program that required $150 million or more to build. A well-executed one compresses the clinical development burden, enables extrapolation of approval across multiple indications without separate trials, and creates a dossier strong enough to enter patent litigation from a position of scientific authority.
Key Takeaways: Part 1
The biosimilar opportunity is structurally real and quantifiable. The analytical similarity assessment controls the path to that opportunity more directly than any other single activity. Every decision in the analytical development program, from reference lot procurement to tier classification of quality attributes, carries direct financial consequences that compound through the full commercial lifecycle of the product.
Part 2: Foundational Science: Why Biosimilars Are Not Generic Biologics
Molecular Complexity as the Core Regulatory Problem
A small-molecule drug like ibuprofen has a molecular weight of 206 daltons and a structure that can be completely specified by a single chemical formula. Any chemist with the right reagents and equipment can reproduce it atom-for-atom. A generic ibuprofen is, by any meaningful scientific standard, identical to the brand.
Monoclonal antibodies operate in a different universe. A full-length IgG1 antibody like infliximab has a molecular weight of approximately 149,000 daltons and a structure that is not fully specified by its amino acid sequence alone. The gene tells you the sequence. The cell line, the bioreactor conditions, the pH gradients, the dissolved oxygen levels, the temperature profiles, and the purification steps determine everything else: the glycosylation pattern on Asn-297 in the Fc region, the ratio of acidic to basic charge variants, the percentage of high-mannose glycoforms, the degree of C-terminal lysine clipping, the level of methionine oxidation, the distribution of disulfide bond configurations, and the propensity of the molecule to form soluble oligomers or submicron aggregates.
None of these attributes are incidental. Each has a documented or plausible relationship to the molecule’s pharmacokinetics, its immune effector functions, or its immunogenic potential in patients. Glycosylation at Asn-297 directly modulates Fc receptor binding, which in turn controls antibody-dependent cell-mediated cytotoxicity (ADCC) and complement-dependent cytotoxicity (CDC). High-mannose glycoforms are cleared faster by the liver, shortening half-life. Aggregates are consistently associated with elevated immunogenicity risk, which is the primary safety concern for any biologic therapy.
The regulatory consequence of this complexity is direct: it is not scientifically defensible to call a biologic from a different manufacturer ‘identical’ to the originator. Two manufacturers using independently developed processes will produce molecules with measurable differences in these attributes, even if the amino acid sequence is identical. The regulatory framework must therefore substitute a different standard for identity. That standard is ‘high similarity with no clinically meaningful differences,’ and the analytical similarity assessment is the scientific instrument used to establish it.
The ‘Highly Similar’ Standard: FDA vs. EMA Definitions Compared
The FDA, operating under the Biologics Price Competition and Innovation Act of 2009, defines a biosimilar as a biological product that is ‘highly similar to the reference product notwithstanding minor differences in clinically inactive components’ and for which there are ‘no clinically meaningful differences between the biological product and the reference product in terms of the safety, purity, and potency of the product.’
The EMA, which established its framework in 2004 and approved the first biosimilar in 2006, defines a biosimilar as a biological medicine that is ‘highly similar to a reference medicine already approved in the EU in terms of structure, biological activity and efficacy, safety and immunogenicity profile.’
The practical difference matters for global development strategy. The FDA’s explicit carve-out for ‘minor differences in clinically inactive components’ creates a specific, bounded regulatory space for formulation flexibility. A developer can, in principle, use a different buffer system or a different stabilizer than the originator, provided it demonstrates that the excipient change has no clinical consequence. The EMA’s language is more holistic; it focuses on the overall profile rather than parsing component-level differences, which places greater analytical burden on building a complete and coherent similarity narrative across all quality dimensions.
A developer running a simultaneous global program must construct a data package capable of satisfying both standards. This is not as simple as combining two separate programs. Certain analytical methodologies accepted as state-of-the-art in Europe may not carry the same weight at the FDA, and vice versa. The statistical frameworks differ. The reference product sourcing requirements differ. Designing a program that is genuinely dual-purpose from day one, rather than adapting a single-agency submission for a second filing, is the most cost-efficient approach and also the most analytically demanding.
Why Manufacturing Variability Is Not a Bug
One of the most important concepts for any non-scientist engaging with this field: the originator biologic has its own lot-to-lot variability, and regulators accept this as inherent to the biology. The target for a biosimilar is not a single point; it is a distribution. Demonstrating biosimilarity means showing that the biosimilar’s attribute distributions are comparable to the originator’s distributions, not that the biosimilar’s mean matches the originator’s mean on a one-time measurement.
This has a major practical implication: a biosimilar developer who fails to characterize the originator’s variability thoroughly, by sourcing too few lots or lots from too narrow a manufacturing period, is operating without a reliable target. They may design their process to hit a target that does not represent the true commercial range of the reference product, which will become apparent when regulatory reviewers compare the developer’s narrow reference range to the wider range they see in the originator’s own manufacturing records. Resolving that discrepancy after a submission has been filed is expensive and slow.
Key Takeaways: Part 2
Biological complexity is not an obstacle to be minimized; it is the scientific foundation of the entire regulatory framework. The ‘highly similar’ standard exists because identity is unachievable, not because regulators are being lenient. Developers who internalize this distinction build analytically coherent programs. Those who treat it as bureaucratic language tend to underpowered their reference product characterization and overpromise on similarity claims they cannot fully defend at review.
Part 3: The Totality-of-the-Evidence Pyramid: Analytical Work as the Primary Asset
Inverting the Traditional Drug Development Logic
In conventional new drug development, clinical trials are the primary evidence-generating activity. Phase 3 data establishes efficacy and safety from scratch for a molecule with no prior human experience. Analytical characterization supports quality control and provides mechanistic context, but the regulatory decision rests on what happened in patients.
For biosimilars, the logic runs in the opposite direction. The reference product has already established efficacy and safety in humans across years of clinical experience. The biosimilar program’s question is not ‘does this work?’ but ‘is this the same thing?’ Answering that question with the most sensitive tools available, before any patient is enrolled, is the foundational task.
The FDA and EMA both use the phrase ‘totality of the evidence’ to describe this approach. In practice, it means that a highly persuasive analytical package can reduce or eliminate the need for extensive clinical data at the top of the pyramid. The more completely an analytical program demonstrates structural and functional equivalence, the less residual uncertainty remains for a clinical trial to resolve. A clinical trial in 300 or 500 patients has limited statistical power to detect small differences in immunogenicity or PK variability. A mass spectrometer measuring glycopeptide abundance across 30 lots of both products has no such limitation.
This creates a direct financial incentive for analytical investment. A full comparative efficacy trial for a complex monoclonal antibody can cost $40 million to $100 million and take 18 to 36 months to complete. If an analytical package is sufficiently comprehensive and the molecule has a measurable pharmacodynamic endpoint, regulators may accept PK/PD bridging studies in healthy volunteers as adequate clinical confirmation. The difference in cost and time between those two scenarios is the financial return on analytical excellence.
The Pyramid’s Five Layers
The totality-of-the-evidence structure has five functional layers, each addressing a specific dimension of similarity. Each layer builds on the one below it.
The base layer, covering the broadest surface area of the pyramid, is the comprehensive analytical characterization. This includes primary structure confirmation, higher-order structure assessment, post-translational modification profiling, purity and impurity characterization, and a full panel of functional assays. This layer uses the largest number of lots, the greatest variety of orthogonal techniques, and the most rigorous statistical treatment.
The second layer, if required, is non-clinical testing. Regulatory guidance from both the FDA and EMA has moved consistently toward eliminating dedicated animal toxicology studies for biosimilars, on the grounds that such studies are not sufficiently sensitive to detect clinically relevant differences between a biosimilar and its reference. Where residual safety questions remain after analytical characterization, targeted in vitro cytotoxicity or receptor binding studies are generally more informative and less costly than rodent or primate studies.
The third layer is clinical pharmacology, specifically comparative PK and PD studies. These are typically conducted in healthy volunteers and are designed to show that the biosimilar reaches the same exposures as the reference product and produces the same biological effect at those exposures. For a granulocyte colony-stimulating factor like filgrastim, the PD marker is absolute neutrophil count, which is directly measurable and has a well-characterized relationship to clinical outcomes. For a monoclonal antibody without a validated PD marker, this layer relies primarily on PK equivalence.
The fourth layer, which is becoming progressively less common for well-characterized molecules, is a confirmatory clinical efficacy study in patients. This is still required for complex molecules where residual uncertainty about immunogenicity or mechanism-dependent efficacy exists after the lower layers of the pyramid are complete.
The fifth layer, often overlooked but critically important, is post-marketing pharmacovigilance. Regulators expect biosimilar developers to maintain robust pharmacovigilance programs that can detect rare immunogenic events or safety signals that would not be apparent in pre-approval clinical programs.
Key Takeaways: Part 3
Analytical investment has a direct and quantifiable return in the form of reduced clinical development burden. The pyramid structure means that every marginal improvement in analytical package quality is worth more than its face value, because it potentially eliminates entire clinical studies that would otherwise sit above it. Developers who approach analytical development as a cost center are systematically undervaluing their most powerful tool for accelerating time to market.
Part 4: Regulatory Pathways: FDA vs. EMA, Structure, History, and Key Divergences
The EMA’s Two-Decade Head Start and What It Means Practically
The EMA approved its first biosimilar, a somatropin product (Omnitrope, Sandoz), in April 2006. By the time the FDA approved its first biosimilar in March 2015, the EMA had nearly a decade of accumulating real-world experience, approved more than 20 products, and built a substantial body of post-marketing safety data demonstrating that its framework was scientifically sound.
This head start has had several concrete effects on how the two agencies approach the science. The EMA has published dozens of product-class-specific guidance documents covering monoclonal antibodies, erythropoietins, granulocyte colony-stimulating factors, follicle-stimulating hormones, low-molecular-weight heparins, and recombinant insulin products, among others. Each document provides molecule-class-specific guidance on which analytical attributes are most critical, which clinical designs are acceptable, and what immunogenicity monitoring is required. The specificity of this guidance reduces regulatory uncertainty substantially for developers operating in those classes.
The FDA, starting from a later base, initially published fewer product-class-specific guidances and relied more heavily on a set of general scientific principles articulated in its 2015 guidance documents. This created more uncertainty for early US biosimilar developers, who had to infer regulatory expectations from the agency’s feedback letters and approval decisions rather than from explicit written guidance. The FDA has since moved toward greater specificity, but the EMA’s catalog of class-specific guidances remains more comprehensive.
The EMA’s centralized procedure is also a structural advantage. A single application, a single scientific committee evaluation, and a single approval decision grant marketing authorization across all EU member states. The FDA covers only the United States, and each separate market (Canada, Japan, Australia, emerging markets) requires its own regulatory strategy.
FDA-Specific Requirements: the 351(k) Pathway and Its Unique Features
The BPCIA created the 351(k) pathway for biosimilar applications. Several features of this pathway have no EMA equivalent and require specific attention from developers pursuing a US approval.
The 12-year data exclusivity period for reference products is the first. Under the BPCIA, the FDA cannot approve a 351(k) application referencing a biological product until 12 years after the reference product’s first approval date. This is longer than the typical 10-year EU exclusivity period and creates a hard timeline constraint that affects program initiation decisions.
The interchangeability designation is the second. No EMA equivalent exists. Under the BPCIA, a biosimilar that meets the additional statutory standard for interchangeability can be substituted for the reference product at the pharmacy level without prescriber intervention, subject to state pharmacy laws. The practical consequence for retail pharmacy-dispensed biologics is substantial: an interchangeable biosimilar can be dispensed automatically when a prescriber writes for the reference product, without requiring a separate prescriber authorization for the switch. For products like adalimumab or etanercept, which are dispensed through specialty pharmacy channels, achieving the interchangeability designation is commercially essential.
The FDA’s June 2024 draft guidance on interchangeability, proposing to eliminate the requirement for dedicated switching studies, has significantly lowered the analytical and clinical bar for achieving this designation. The agency’s position is that the totality of the biosimilarity evidence itself, if sufficiently comprehensive, demonstrates that switching is safe. This represents a major policy evolution and has direct implications for development program design, cost projections, and competitive strategy.
The ‘patent dance’ provisions of the BPCIA are the third unique feature. These provisions establish a structured exchange of patent information between the biosimilar applicant and the reference product sponsor that triggers specific litigation timelines and a period during which the biosimilar cannot be marketed even after receiving FDA approval. A detailed treatment of this mechanism follows in Part 5.
The EMA’s ‘Tailored Clinical Approach’ and Its Forward Implications
The EMA published a reflection paper in 2022 exploring a ‘tailored clinical approach’ for biosimilar development. This document represents the most significant signal from any major regulatory agency about the future direction of the field. It proposes a framework under which, for certain well-characterized molecules and molecule classes, the confirmatory comparative clinical efficacy study could be waived entirely if the analytical and PK evidence package meets a set of elevated criteria.
The EMA’s reasoning is straightforward. For a molecule whose structure-activity relationships are thoroughly understood, whose PK is accurately predictable from structural data, and whose clinical effects are tightly linked to its mechanism of action, a large randomized controlled trial adds limited additional confidence beyond what analytical and PK data already provide. The trial is expensive, slow, and, by the agency’s own assessment, less sensitive than modern analytical tools at detecting clinically relevant differences between two products.
If this framework is formalized and extended to broad molecular classes, it will compress biosimilar development timelines by 18 to 36 months for applicable products and reduce development costs by $40 million to $100 million per program. The downstream effect on competition will be substantial: more developers will be able to afford to enter markets for complex molecules, accelerating the price erosion that benefits payers and patients.
For developers currently planning programs for monoclonal antibodies with validated PD endpoints or well-established PK-efficacy relationships, monitoring the EMA’s evolution on this topic and engaging proactively in public consultation processes is worth prioritizing.
Key Takeaways: Part 4
The FDA and EMA share foundational science but diverge on specific requirements in ways that can make or break a global development strategy. The FDA’s interchangeability pathway, the BPCIA patent dance, and the 12-year exclusivity period are US-specific features with major commercial consequences. The EMA’s longer track record translates into more specific, more predictable guidance, particularly for established molecular classes. Developers running simultaneous global programs should treat regulatory strategy as a primary function, not a submission-stage afterthought.
Part 5: The BPCIA ‘Patent Dance’ and Its Commercial Consequences
Anatomy of the Patent Dance
The BPCIA’s patent exchange mechanism, colloquially called the ‘patent dance,’ is a formal, step-by-step legal process that determines which patents covering the reference product will be litigated before the biosimilar reaches the market. Understanding its mechanics is essential for any investor or IP team modeling the commercial timeline of a US biosimilar.
The process begins when the FDA accepts the biosimilar application for review. Within 20 days, the applicant must provide the reference product sponsor with a copy of the 351(k) application and all manufacturing information. The reference product sponsor then has 60 days to review this material and provide a list of patents it believes are potentially infringed by the biosimilar product, process, or use.
The applicant can then respond with its own patent list and, critically, provide a statement for each patent on the sponsor’s list explaining why the patent is invalid, unenforceable, or not infringed by the biosimilar. This is the equivalent of the Paragraph IV certification in the small-molecule Hatch-Waxman world, but the mechanism is more complex and operates on a more compressed timeline.
The two parties then have 15 days to agree on which patents from the exchanged lists will be the subject of immediate litigation. If they cannot agree, the reference product sponsor can select up to one-half of the total number of patents on its list for immediate litigation, and the applicant can select the same from its list. Litigation on the selected patents must be filed within 30 days. Regardless of the outcome of this first round of litigation, the applicant must give 180 days’ notice before commercial launch, and any patents not included in the first round of litigation can be asserted in a second-wave action.
Strategic Implications: When to Dance and When to Opt Out
The ‘patent dance’ is optional. A biosimilar applicant can decline to provide the reference product sponsor with its application and manufacturing information. The consequence of opting out is that the reference product sponsor loses certain procedural advantages, specifically the right to an automatic 30-day preliminary injunction period. The applicant, however, is still subject to patent infringement claims after launch, which can result in an injunction and substantial damages liability.
The decision to participate or opt out depends heavily on the specific patent landscape for the target molecule. For a reference product surrounded by a dense patent thicket, the structured dance may be preferable because it surfaces all patent disputes before launch, creating legal certainty. For a reference product with a thin or expiring IP estate, opting out and accepting the litigation risk may be the faster path to market.
AbbVie’s management of the Humira biosimilar patent thicket is the most instructive case study in the field. AbbVie held more than 130 US patents related to adalimumab, covering the molecule itself, its formulation, manufacturing methods, dosing regimens, and methods of use. This thicket was assembled through a deliberate strategy of filing continuation applications and new formulation patents over the 20-year commercial lifecycle of Humira. The result was that every biosimilar developer entering the US market faced a multi-front patent war. AbbVie settled with each of them on licensing terms that allowed staggered entry, with Amgen’s Amjevita entering the US market in January 2023 and several others following throughout 2023.
The commercial impact was unambiguous: AbbVie extracted an additional six years of substantially unchallenged US market exclusivity for Humira after the molecule’s core composition-of-matter patent expired. During those six years, Humira generated approximately $20 billion annually in US revenue alone. The analytical similarity assessment had nothing to do with this delay; it was entirely a function of IP architecture and litigation settlement strategy.
Key Takeaways: Part 5
A biosimilar program that clears the analytical similarity hurdle still faces a patent litigation gauntlet in the United States that can delay commercial launch by years. IP teams modeling US market entry timelines must account for the full patent thicket, not just the composition-of-matter patent. Settlement licensing, staggered entry, and the litigation costs embedded in the dance process are all financially material inputs to any program NPV model.
Part 6: Originator IP Valuation: Remicade, Humira, Neupogen, and Herceptin as Case Studies
How to Value a Biologic’s IP Estate
The intellectual property surrounding a blockbuster biologic functions as a set of layered exclusive rights, each with its own expiration date, litigation history, and commercial consequence. Standard pharmaceutical IP valuation assigns a probability-adjusted present value to each right, discounted by both time and litigation risk. For biosimilar developers, the inverse calculation is equally important: understanding what the originator’s IP estate is worth tells you what the originator will spend to defend it, which in turn calibrates realistic timelines for market entry.
A biologic’s IP estate typically contains four types of assets: composition-of-matter patents covering the molecule itself, formulation patents covering the drug product, manufacturing process patents covering production methods and cell lines, and method-of-use patents covering specific dosing regimens or indications. Each has a different litigation profile and a different evidentiary burden for a Paragraph IV-equivalent challenge.
Remicade (Infliximab): IP Valuation and the Biosimilar Entry Timeline
Remicade reached peak US sales of approximately $5.4 billion in 2014. Janssen’s core composition-of-matter patent for infliximab expired in September 2018. However, a series of formulation and manufacturing patents extended effective protection well past that date, and the clinical trial precedent established by PLANETRA and PLANETAS for Inflectra shaped the evidentiary standard for every subsequent infliximab biosimilar.
By mid-2023, six infliximab biosimilars had received FDA approval: Inflectra (Celltrion/Pfizer), Renflexis (Samsung Bioepis/Merck), Avsola (Amgen), Ixifi (Pfizer), Hyrimoz (Sandoz), and Hadlima (Samsung Bioepis). US market penetration by biosimilars in the infliximab class has been meaningfully slower than in European markets, where payer systems have actively promoted substitution. This divergence illustrates that IP expiration and analytical approval are necessary but not sufficient conditions for commercial success.
The residual IP value of Remicade-related patents at the time of the first US biosimilar launch in 2016 was significant enough that Janssen and its parent company Johnson & Johnson pursued active litigation strategies that settled on licensing terms, allowing controlled biosimilar entry while preserving a portion of their branded revenue through rebate contracting with pharmacy benefit managers.
For investors evaluating infliximab biosimilar programs today, the relevant questions are no longer primarily analytical; they are commercial. The reference product’s IP has largely run its course. The competitive dynamics now turn on manufacturing cost structure, formulary positioning, and the ability to execute on hospital and specialty pharmacy contracting.
Humira (Adalimumab): The World’s Most Valuable Patent Thicket
Humira generated $21.2 billion in global revenue in 2022, making it, at its peak, the highest-revenue drug in the history of pharmaceuticals. AbbVie’s IP strategy around adalimumab is a masterclass in evergreening, patent thicket construction, and settlement licensing that deserves detailed analysis as both a commercial phenomenon and a regulatory case study.
The core composition-of-matter patent for adalimumab, US Patent 6,090,382, expired in December 2016. AbbVie then asserted more than 130 additional US patents, covering a high-concentration citrate-free formulation (which allowed subcutaneous self-injection with reduced injection site pain), specific manufacturing processes including Chinese hamster ovary cell line conditions, dosing regimens for specific indications including rheumatoid arthritis and Crohn’s disease, and specific methods of use including combination with methotrexate.
The high-concentration, citrate-free formulation patent, US Patent 8,895,009, is the most commercially important secondary patent in this estate. It covers the 100 mg/mL formulation of Humira that became the standard commercial presentation. Any biosimilar that wanted to offer an equivalent patient experience, specifically the same injection volume with lower injection site discomfort, had to either license this patent or develop a different formulation that provided comparable tolerability without infringing it.
AbbVie’s patent thicket had an estimated IP estate value, on a probability-adjusted basis, of $20 billion to $30 billion in extended US exclusivity when the settlement licenses were negotiated. The analytic consequence for biosimilar developers was that their formulation development programs had to be designed from the outset around freedom-to-operate constraints. Samsung Bioepis, Amgen, Sandoz, and others each developed high-concentration adalimumab formulations that avoided the patented citrate-free system, using alternative excipient combinations to achieve comparable stability and tolerability.
This is a concrete example of the relationship between patent intelligence and analytical development strategy. The CQA risk assessment for adalimumab biosimilars had to include an explicit evaluation of how formulation differences, specifically the excipient system, affected the product’s physical stability and injection site tolerability profile. These attributes became analytically critical not because of their biological mechanism but because of the IP landscape.
Neupogen (Filgrastim): A Simpler Molecule, a Clearer Valuation Picture
Filgrastim is the first molecule to go through the 351(k) pathway in the United States. Amgen’s core patent on Neupogen expired in December 2013. The molecule is non-glycosylated, relatively small at 18.8 kDa, and thoroughly characterized by the scientific literature accumulated during more than two decades of clinical use.
The IP estate for Neupogen was thin by the standards of modern biologics. Amgen held patents on the manufacturing process and certain formulation aspects, but the absence of complex glycosylation removed the entire layer of post-translational modification patents that make complex biologics like monoclonal antibodies so difficult to surround with secondary IP. The biosimilar development program for Zarxio, as a result, was primarily an analytical and clinical pharmacology challenge rather than an IP navigation challenge.
From a valuation standpoint, the residual IP value of Neupogen-related patents at first biosimilar entry was modest. The commercial consequence was a relatively orderly market transition: Zarxio launched in September 2015 at a roughly 15% discount to Neupogen’s list price, and market share shifted gradually rather than abruptly, in part because Amgen had strong formulary relationships and a well-established biosimilar brand of its own.
For developers considering similar molecules, the Neupogen/Zarxio case establishes a benchmark: a non-glycosylated protein with expired core patents, a well-understood mechanism, a validated PD endpoint, and a thin secondary IP estate can be developed analytically with a streamlined toolkit and approved with a PK/PD-based clinical package. The total development cost for Zarxio has been estimated in the range of $100 million to $150 million, compared to the $200 million to $300 million typically required for a complex mAb biosimilar program.
Herceptin (Trastuzumab): Glycosylation Complexity and a Multi-Wave IP Defense
Trastuzumab, sold as Herceptin by Roche/Genentech, generated peak annual revenues of approximately $7 billion globally. It targets HER2, a receptor overexpressed in approximately 20% of breast cancers. The molecule is a glycosylated IgG1 monoclonal antibody, and glycosylation at Asn-297 directly affects its Fc-receptor-mediated ADCC activity, which is an important component of its anti-tumor mechanism.
The analytical challenge for trastuzumab biosimilars is more demanding than for simpler molecules because the ADCC-relevant glycosylation must be demonstrated to be highly similar. Fucosylation levels, specifically the proportion of afucosylated glycoforms, correlate with FcgRIIIa binding affinity and ADCC potency. A biosimilar with meaningfully lower afucosylation than the originator would have stronger ADCC activity. Higher afucosylation would produce weaker ADCC. Either direction could be clinically relevant, and both would require clinical justification or process correction.
Roche’s IP estate around trastuzumab included composition-of-matter patents, manufacturing process patents covering CHO cell culture conditions and purification sequences, and formulation patents. The core US composition-of-matter patent, US Patent 5,821,337, expired in June 2019. Roche’s secondary patents were litigated by multiple biosimilar developers, with settlement licenses allowing entry for Samsung Bioepis (Ontruzant), Celltrion (Herzuma), Pfizer (Trazimera), Mylan/Biocon (Ogivri), and Amgen (Kanjinti) in the US market between 2019 and 2020.
The analytical consequence of this IP landscape is that trastuzumab biosimilar development programs had to include rigorous glycoform profiling as a primary analytical activity. Cell-based ADCC assays became Tier 1 functional attributes for these programs, and any formulation or manufacturing process difference that shifted the fucosylation profile required explicit justification in the submission.
Investment Strategy: IP Valuation and Target Selection
For institutional investors evaluating biosimilar development programs, the IP valuation of the reference product is a critical input that most standard pharma equity models underweight. A program that has solved the analytical similarity problem but underestimated the residual IP estate of the originator will fail to reach commercial launch on the modeled timeline, destroying the NPV that justified the investment.
A rigorous IP valuation for any biosimilar target should assess the probability of successfully challenging or designing around each material patent, weighted by the commercial consequences of success or failure. The relevant inputs include the number and quality of secondary patents in the estate, the originator’s historical litigation behavior and settlement terms, the regulatory approval timeline projections from the analytical development program, and the commercial market dynamics that determine whether litigation delay is financially survivable.
Programs targeting molecules with thin or expired IP estates, validated PD endpoints, and non-glycosylated structures offer the most predictable development timelines and the clearest NPV modeling. Programs targeting complex glycoproteins with dense secondary patent estates require a materially higher discount rate on projected launch timelines and a litigation budget that is explicitly modeled as a cost of revenue.
Part 7: The Evergreening Technology Roadmap: How Originators Extend Exclusivity
Taxonomy of Evergreening Strategies for Biologics
Evergreening, in the pharmaceutical context, describes any strategy used by an originator to extend market exclusivity beyond the expiration of the primary composition-of-matter patent. For small molecules, the classic tactics include new polymorph patents, new formulation patents for modified-release systems, and new indication filings that reset exclusivity clocks. For biologics, the strategies are more varied, more technically complex, and often more difficult to challenge.
A complete taxonomy of biologic evergreening strategies includes at least six distinct approaches.
The first is formulation evolution. The originator makes a clinically meaningful improvement to the drug product, typically the development of a subcutaneous self-injection formulation from an intravenous infusion product, or the development of a high-concentration formulation that reduces injection volume. These improvements generate new patents while also changing the commercial product to one that biosimilar developers must now match analytically. AbbVie’s transition of Humira from 50 mg/mL to 100 mg/mL and from citrate-buffered to citrate-free is the canonical example.
The second is device integration. The originator develops an auto-injector or prefilled syringe for a product that was previously available only in vials. The device itself generates patent protection, as does the drug-device combination. A biosimilar developer wishing to compete on patient experience must match the device, which requires its own engineering development and patent clearance, or accept a potentially disadvantageous presentation format.
The third is indication expansion. By filing for and obtaining approval for new clinical indications, the originator generates method-of-use patents and additional exclusivity periods for those indications. These patents are frequently listed in the FDA’s ‘Purple Book’ (the biological equivalent of the Orange Book for small molecules), and while they can be challenged in Paragraph IV-equivalent proceedings, each one extends the litigation surface that a biosimilar developer must navigate.
The fourth is new dosing regimen patents. The originator generates clinical data supporting a less frequent dosing schedule, a weight-based dosing algorithm, or a loading dose regimen, and patents these methods of administration. These patents can be asserted against any biosimilar developer that includes the new dosing regimen in its prescribing information.
The fifth is manufacturing process innovation. The originator patents improvements to its cell culture conditions, purification sequences, or quality control methods. These patents are difficult for biosimilar developers to infringe directly if they have independently developed their own process, but they can complicate freedom-to-operate analysis if the biosimilar’s process happens to use similar approaches.
The sixth is follow-on biologic development. The originator develops a second-generation version of the molecule, typically an antibody-drug conjugate, a bispecific antibody, or a PEGylated version with improved pharmacokinetics, and positions this as the clinical successor to the originator product. This strategy does not extend exclusivity for the original molecule, but it shifts prescriber behavior away from the original toward the new product before biosimilar entry, effectively migrating the revenue base to a product with fresh IP protection.
The Continuation Application Strategy: Manufacturing the Thicket
The most technically sophisticated evergreening tactic involves the systematic use of continuation patent applications to generate a large number of related but distinct patents from a single original application. The US patent system allows an applicant to file a continuation of a pending application, claiming a different but related invention while benefiting from the priority date of the original filing. This means that a single drug can be surrounded by dozens of patents, all claiming priority to an application filed before the molecule was approved, but each with a different expiration date based on when the continuation was granted.
For biologics with long development histories, this tactic can generate a patent thicket in which expiration dates are staggered over a 10-to-15-year period beyond the primary patent. Each continuation adds a new patent to the portfolio, each potentially requires its own litigation or design-around effort by biosimilar developers, and each can support a new infringement claim in the ‘patent dance’ process.
AbbVie’s Humira patent portfolio, which ultimately comprised more than 130 US patents, was assembled largely through this continuation strategy. Some of the patents in the portfolio shared the same or similar claims as earlier patents; their primary value was adding litigation complexity rather than protecting genuinely distinct inventions.
Regulatory Pathway Switching as an Exclusivity Strategy
In certain cases, originators have pursued regulatory pathway changes as an exclusivity strategy. The most relevant example involves the transition of insulin products from small-molecule drug status under the Federal Food, Drug, and Cosmetic Act to biological product status under the Public Health Service Act, which occurred in March 2020. This transition reset the exclusivity clock under the BPCIA’s 12-year provision for any insulin product that had not previously received a BLA. The practical effect was to create new exclusivity periods for established insulin products that had already been on the market for decades.
This tactic is specific to the transitional provisions of the BPCIA and has limited applicability to newly approved biologics. However, it illustrates the depth of the regulatory expertise required to fully map the exclusivity landscape for any given target molecule, and reinforces that the analytical similarity assessment is only one component of a biosimilar program’s regulatory risk profile.
Key Takeaways: Part 7
Evergreening is not a single tactic; it is a systematic strategy implemented across multiple patent prosecution tracks over the full commercial lifecycle of a biologic. Biosimilar developers who analyze only the primary composition-of-matter patent when selecting targets are systematically underestimating IP risk. A complete freedom-to-operate analysis must cover all six evergreening categories described above, quantify the probability of successful challenge or design-around for each material patent, and incorporate that analysis directly into the program’s cost and timeline models.
Part 8: Critical Quality Attributes: Identification, Risk Stratification, and Tier Classification
Building the CQA Risk Matrix
A critical quality attribute is a physical, chemical, biological, or microbiological property or characteristic that should be within an appropriate limit, range, or distribution to ensure the desired product quality. In biosimilar development, ‘desired product quality’ specifically means matching the reference product’s clinical performance profile, covering activity, PK, safety, and immunogenicity.
The process of identifying CQAs begins with a comprehensive characterization of the reference product using a broad panel of analytical methods applied without prior prioritization. The objective at this stage is to generate a complete attribute inventory, not to evaluate importance. Common attributes measured at this stage for a monoclonal antibody include primary sequence, disulfide bonding pattern, N-linked glycan profile, O-linked glycosylation if present, sialic acid content, C-terminal lysine clipping, deamidation at Asn and Gln residues, oxidation at Met and Trp residues, aggregation and fragmentation levels by multiple orthogonal methods, charge variant distribution, hydrodynamic size by dynamic light scattering, thermal stability by differential scanning calorimetry, target binding affinity by surface plasmon resonance, FcRn binding affinity, FcgRIIIa binding affinity, complement component C1q binding, ADCC activity by cell-based assay, and complement-dependent cytotoxicity if relevant to the molecule’s mechanism.
This initial inventory is then subjected to a two-dimensional risk assessment. The first dimension is the attribute’s known or potential impact on clinical performance, scored on a numerical scale. The second dimension is the uncertainty in that impact assessment, also scored numerically. Attributes that score high on both dimensions, meaning they have a significant potential impact but limited published data to characterize that impact precisely, represent the highest analytical development risk and require the most extensive characterization work.
Attributes that score high on impact but low on uncertainty, where the literature clearly establishes their clinical relevance, are the most straightforward CQAs. They require rigorous analytical attention, but their importance is not contested. The uncertainty dimension is where scientific judgment and proprietary data generation provide competitive differentiation.
FDA Tier Classification: The Complete Decision Framework
The FDA’s three-tier system for analytical similarity assessment is described in its guidance document ‘Development of Therapeutic Protein Biosimilars: Comparative Analytical Assessment and Other Quality-Related Considerations’ (2019). The tier structure organizes CQAs by clinical risk and specifies the appropriate statistical treatment for each.
Tier 1 contains the attributes with the highest potential to impact clinical outcomes. These are typically attributes directly linked to the molecule’s primary mechanism of action. For a TNF-alpha inhibitor, this would include TNF-alpha binding affinity, as measured by SPR with full kinetic characterization. For an anti-CD20 antibody, it would include CD20 binding affinity and cell-based CDC activity. For any Fc-bearing antibody, FcgRIIIa binding, which drives ADCC, is typically Tier 1. The statistical requirement for Tier 1 attributes is formal equivalence testing using the Two One-Sided Tests procedure.
The FDA recommends an equivalence acceptance criterion of plus or minus 1.5 times the standard deviation of the reference product, estimated from the lots tested in the comparability study. This margin is data-driven rather than pre-specified, which creates a statistical dependency on the reference lot sample. If the specific lots sampled happen to show unusually low variability, the resulting narrow margin may be statistically difficult to meet even for a well-matched biosimilar. This is not a flaw to be exploited; it is a design challenge to be managed through aggressive reference lot procurement strategy.
Tier 2 contains attributes with moderate clinical risk, where the mechanism of action is understood but the magnitude of clinical impact from moderate attribute variation is not precisely established. The recommended statistical approach is the quality range method: a range of mean plus or minus k times the standard deviation of the reference product, where k is selected based on the attribute’s criticality and the analytical method’s precision. The biosimilar demonstrates similarity by showing that a pre-specified percentage of its lot values, typically 90%, fall within this range.
Tier 3 contains attributes with low clinical risk or attributes that are not quantifiable with sufficient precision to support formal statistical testing. Side-by-side graphical comparison and summary statistics are sufficient for these attributes. The analytical effort here is focused on presentation quality: generating clear, interpretable graphics that make the similarity narrative visually compelling to a regulatory reviewer.
EMA Comparability Exercise: Principles Without Prescription
The EMA does not use the FDA’s tier nomenclature, but it applies equivalent scientific logic through its ‘comparability exercise’ framework. The core EMA requirement is that the biosimilar developer establishes a reference range for each relevant quality attribute based on sufficient lots of the reference product to capture its inherent variability, and then demonstrates that the biosimilar’s attribute values are within that range.
The EMA’s approach is more narrative in character than the FDA’s statistical framework. Rather than specifying a particular statistical test for high-risk attributes, the EMA asks sponsors to provide a scientific justification for any observed difference and explain why that difference does not translate into a clinically meaningful change. This places more weight on the scientific argumentation in the submission document and less on the formal statistical test results.
A concrete implication: a minor difference in a charge variant profile that would fail the FDA’s quality range test might be accepted by the EMA if the developer can demonstrate, through functional assay data, that the charge variant with the different level has no relevant biological activity, or that the quantitative difference is too small to affect any downstream pharmacological parameter. The FDA’s statistical gate is binary; the EMA’s scientific narrative is more flexible but also more demanding of the underlying data.
Key Takeaways: Part 8
CQA identification is the intellectual backbone of the entire analytical development program. Errors at this stage propagate through every subsequent step. Overly narrow CQA lists generate regulatory deficiency letters. Overly broad lists waste capital on low-value analytical work. The optimal list, produced through a rigorous and well-documented risk assessment, defines a development program that is both comprehensive and efficient. Tier classification decisions have direct statistical consequences that must be understood and actively managed throughout the reference lot procurement process.
Part 9: The Scientist’s Full Toolbox: State-of-the-Art Characterization Techniques
Primary Structure: Confirming the Amino Acid Sequence
The primary structure of a biosimilar must match the reference product exactly. Any difference in the amino acid sequence means the product is a distinct molecule, not a biosimilar. Confirming sequence identity requires peptide mapping combined with liquid chromatography-tandem mass spectrometry.
In a standard peptide mapping experiment, the protein is first denatured and reduced to break disulfide bonds, then digested with a sequence-specific protease, most commonly trypsin, which cleaves at the C-terminal side of lysine and arginine residues. The resulting peptide fragments are separated by reversed-phase HPLC and analyzed by high-resolution mass spectrometry. Modern instruments, including Orbitrap-based systems from Thermo Fisher and quadrupole time-of-flight instruments from Waters and Agilent, can measure peptide masses with sub-ppm accuracy and generate MS/MS fragmentation spectra that confirm the amino acid sequence of each peptide.
A complete sequence coverage of 100% is the target and is generally achievable for monoclonal antibodies with a combination of multiple enzymes, such as trypsin and Glu-C, and multiple chromatographic conditions. Any region of the sequence not covered by the standard digest must be addressed with alternative digestion strategies or electron transfer dissociation MS approaches.
Post-Translational Modifications: Glycosylation as the Core Complexity
Glycosylation is analytically the most complex and commercially the most important PTM category for monoclonal antibodies. N-linked glycosylation at Asn-297 in the Fc region is present in virtually all IgG antibodies and is the primary glycan position relevant to effector function. Afucosylation at this position enhances FcgRIIIa binding by approximately 10-to-50-fold, depending on the FcgRIIIa allotype, and proportionally increases ADCC activity.
The glycan profile at Asn-297 is a mixture of complex biantennary structures with variable sialylation, galactosylation, and fucosylation. The specific composition of this mixture is determined by the host cell line, the culture conditions, and the purification process. CHO cells, which are the standard production system for most monoclonal antibodies, produce predominantly complex biantennary glycans with high core fucosylation. The exact ratio of G0F, G1F, G2F, Man5, and other glycoform species varies with culture conditions and is a process-sensitive attribute.
Characterizing the glycan profile requires multiple methods. Released glycan analysis by HPLC with fluorescence detection or by mass spectrometry provides the overall glycoform distribution. Intact mass analysis by native mass spectrometry resolves the antibody into its major glycoform species at the intact molecule level. Peptide mapping with glycopeptide enrichment provides site-specific information confirming that the glycan distribution at specific sites matches between the biosimilar and the reference product.
Oxidation at methionine residues, particularly Met252 and Met428 in the Fc region, is another analytically critical PTM. Oxidation at these positions reduces FcRn binding affinity, which shortens the molecule’s half-life by increasing its clearance rate from the circulation. A biosimilar with systematically higher levels of Met oxidation than the reference product would have different PK, which is a clinically meaningful difference. Quantifying oxidation levels requires peptide mapping with careful sample handling to avoid artifactual oxidation during sample preparation.
Deamidation at Asn residues, particularly in the complementarity-determining regions of the antibody, converts Asn to Asp or isoAsp and can affect antigen binding affinity. Deamidation in the Fc region is generally lower clinical risk. The rate of deamidation in solution depends on local sequence context, pH, temperature, and ionic strength, and is therefore a stability-relevant attribute that must be monitored under accelerated and real-time stability conditions.
Higher-Order Structure: The Multi-Technique Mandate
Higher-order structure assessment requires a panel of orthogonal techniques because no single method provides complete information about protein conformation in solution. The selection of methods depends on the information needed, and regulators expect a combination that covers secondary, tertiary, and quaternary structure assessment.
Circular dichroism spectroscopy measures the differential absorption of left and right circularly polarized light by chiral molecules, including the peptide bond. Far-UV CD spectra (180-260 nm) provide quantitative information on secondary structure content: alpha-helix, beta-sheet, beta-turn, and random coil proportions. Near-UV CD spectra (250-320 nm) provide information on the tertiary environment of aromatic amino acids (phenylalanine, tyrosine, tryptophan) and disulfide bonds. For a biosimilar comparison, both spectra must be highly similar.
Fourier-transform infrared spectroscopy provides complementary information on secondary structure through the amide I band (1600-1700 cm-1), which reflects the C=O stretching vibration of the peptide bond. FTIR is particularly useful for detecting differences in beta-sheet content and for comparing samples in different formulation buffers where CD measurements may be compromised.
Differential scanning calorimetry measures the heat absorption of a protein as temperature increases. The resulting thermogram shows one or more transitions representing the unfolding of different structural domains. For a monoclonal antibody, the Fab and Fc domains have distinct unfolding transitions at characteristic temperatures. The melting temperatures (Tm) and the shape and area of these transitions are sensitive to structural differences, and a highly similar DSC thermogram provides strong evidence of comparable structural integrity.
Hydrogen-deuterium exchange mass spectrometry has become a front-line technique for higher-order structure comparison in biosimilar programs. HDX-MS measures the rate at which backbone amide hydrogens exchange with deuterium from a deuterium-containing solvent. This exchange rate is highly sensitive to the local protein structure: residues in stable hydrogen-bonded secondary structures exchange slowly, while residues in flexible or solvent-exposed regions exchange rapidly. By digesting the protein into peptides after controlled deuterium labeling, the level of deuterium incorporation at each peptide segment can be determined by mass spectrometry, generating a map of structural dynamics across the entire protein sequence.
Comparing the HDX-MS profiles of a biosimilar and reference product provides high-resolution, site-specific information about conformational similarity. Differences in exchange rates at specific peptide segments, even if they do not affect overall secondary structure content as measured by CD, can indicate local conformational differences in regions critical for function or stability. HDX-MS data has been increasingly referenced in FDA review documents as a key piece of the higher-order structure case.
Cryo-electron microscopy represents the frontier of structural characterization for biosimilar development. Unlike X-ray crystallography, which requires protein crystals, cryo-EM resolves protein structures in near-native solution conditions frozen in vitreous ice. Modern cryo-EM instruments with direct electron detectors can resolve protein structures to 2-to-3 angstrom resolution for large complexes, and to 4-to-6 angstrom resolution for IgG-sized molecules without the target being in a complex. While cryo-EM is not yet routinely used as a required characterization tool in biosimilar submissions, it is being employed by leading developers as a supplemental HOS technique, and its regulatory acceptance is expected to grow as the technology becomes more accessible and as the field accumulates examples of its sensitivity to conformational differences.
Potency and Binding Assays: Translating Structure to Function
The functional assay panel for a biosimilar program serves two purposes: it directly demonstrates biological activity equivalence, and it provides functional context for any minor structural differences observed during characterization. A structural difference that has no functional consequence in multiple orthogonal assays is a structural difference with low clinical risk.
Surface plasmon resonance is the gold standard for quantitative binding kinetics. The target antigen is immobilized on a sensor chip, and the biosimilar or reference product is flowed over it in solution. The SPR instrument measures changes in the refractive index of the sensor surface in real time, which is proportional to the mass of protein binding or dissociating. The resulting sensorgrams provide the association rate constant (kon), the dissociation rate constant (koff), and the equilibrium dissociation constant (KD) calculated as koff/kon. For a biosimilar to be considered highly similar, all three kinetic parameters should be within the established equivalence margins for the assay. SPR is preferred over equilibrium binding assays like ELISA for Tier 1 attributes because it provides mechanistically richer information and is more sensitive to subtle differences in binding affinity.
Cell-based potency assays are required for all functional attributes that directly reflect the molecule’s clinical mechanism. For an anti-TNF antibody, this means a cell-based neutralization assay measuring the ability of the drug to prevent TNF-alpha from activating a downstream reporter in a cell line that expresses the TNF receptor. For an anti-VEGF antibody, it might be an endothelial cell proliferation inhibition assay. For any antibody with Fc effector function relevant to its mechanism, a cell-based ADCC assay measuring the ability of the drug to direct NK cell-mediated killing of target cells is required.
Cell-based assays are the most variable analytical method in a biosimilar program. They depend on the biological behavior of living cells, which introduces sources of variability that are not present in instrument-based methods. Managing the variability of cell-based potency assays requires extensive assay development work, including cell line selection and stability testing, assay format optimization, reference standard preparation, and statistical validation. The coefficient of variation for a well-developed cell-based ADCC assay might be 15 to 25%, compared to 5% or less for an SPR-based binding assay. This inherent variability must be accounted for in the statistical design of the similarity assessment for Tier 1 cell-based attributes.
Impurity Profiling: The Manufacturing Process Fingerprint
The purity and impurity profile of a biosimilar is not just a quality attribute; it is an indirect readout of the manufacturing process. Two products with highly similar purity profiles are likely the products of manufacturing processes that share fundamental design principles, even if the specific details differ. Conversely, a biosimilar with a new impurity not present in the reference product provides evidence that the manufacturing process differs in a way that requires additional characterization and safety justification.
Size exclusion chromatography with multi-angle light scattering detection (SEC-MALS) is the primary method for quantifying aggregates and fragments. SEC separates species by hydrodynamic radius, and MALS measures the absolute molecular weight of each peak, allowing aggregates to be distinguished from the monomer and precisely sized. This method can detect aggregates above approximately 10 nm in size; larger aggregates and particulates require orthogonal methods.
Analytical ultracentrifugation, specifically sedimentation velocity experiments, resolves protein species by their sedimentation coefficient in a centrifugal field. AUC-SV is more sensitive than SEC for detecting small amounts of soluble aggregates and is not affected by matrix interactions that can cause retention artifacts in SEC. The FDA and EMA both expect AUC-SV to be used as an orthogonal confirmation of SEC results for aggregate quantification.
Dynamic light scattering measures the intensity fluctuations of laser light scattered by particles in solution due to their Brownian motion. DLS provides the hydrodynamic size distribution of the sample and is particularly useful for detecting large aggregates and proteinaceous particles in the 10 nm to 10 micron range. DLS is sensitive to contamination and sample preparation conditions, and results must be interpreted in the context of the overall particle characterization strategy.
Charge variant analysis by capillary isoelectric focusing or ion-exchange HPLC resolves the protein into acidic, main, and basic variant peaks. The distribution of charge variants is a sensitive marker of the overall chemical modification state of the molecule, reflecting deamidation, oxidation, C-terminal lysine clipping, and sialylation levels in a composite readout. Matching the charge variant distribution is a standard expectation in all biosimilar programs, and the FDA’s quality range approach is commonly applied to the acidic and basic variant peak areas.
Host cell protein analysis by ELISA using antibodies raised against the production cell line proteins quantifies the total residual HCP burden in the drug substance. HCP specifications for monoclonal antibodies are typically in the range of 1 to 100 ppm by mass relative to the drug substance. Individual HCP species that are present at high relative abundance, or that have known enzymatic activities that could degrade the drug product, require specific attention. Next-generation HCP analysis by mass spectrometry-based proteomics can identify and quantify individual HCP species at low ppm levels, providing a much more detailed safety picture than antibody-based total HCP assays.
Key Takeaways: Part 9
The analytical toolbox for a modern biosimilar program is broad, technically demanding, and rapidly evolving. No single technique is sufficient for any major structural or functional attribute; orthogonal methods are the standard. Investment in state-of-the-art instrumentation, including HDX-MS, native mass spectrometry, and cryo-EM, provides both scientific and regulatory advantages: it generates more comprehensive data, detects differences that simpler methods would miss, and produces the kind of thorough analytical narrative that earns regulatory confidence and reduces clinical burden.
Part 10: Statistical Frameworks: Equivalence Testing, Quality Ranges, and Global Bridging
The TOST Procedure for Tier 1 Attributes: A Technical Deep Dive
The Two One-Sided Tests procedure is the statistical method recommended by the FDA for demonstrating equivalence between a biosimilar and reference product on Tier 1 critical quality attributes. Understanding its mechanics is essential for any analyst building a statistical analysis plan.
The TOST procedure begins with specifying the equivalence acceptance criterion (EAC). The FDA recommends the EAC be set as the mean of the reference product plus or minus 1.5 times the standard deviation of the reference product, estimated from the comparability study lots. This creates a symmetric zone of equivalence centered on the reference mean.
The procedure then performs two one-sided tests. The first tests whether the biosimilar mean is greater than the lower bound of the equivalence zone. The second tests whether the biosimilar mean is less than the upper bound of the equivalence zone. If both tests are statistically significant at the pre-specified alpha level (typically 0.05), the procedure concludes equivalence. This is mathematically equivalent to constructing a 90% confidence interval for the difference between the biosimilar and reference means and verifying that the entire interval falls within the EAC bounds.
The statistical power of the TOST procedure depends on four factors: the true difference between the biosimilar and reference means, the within-group variability of both products, the width of the EAC (which is determined by the reference product’s standard deviation), and the sample size (the number of lots of each product included in the comparability study). The sensitivity of this relationship to the reference product’s variability creates the practical challenge described earlier: a reference product with low inter-lot variability generates a narrow EAC, which requires either a very precise biosimilar (low variability and a mean very close to the reference mean) or a large number of biosimilar lots to achieve adequate power.
Developers should perform power calculations during the protocol design phase of the comparability study, with sensitivity analyses varying the assumed reference product variability over a plausible range. If the power calculation indicates that the study is underpowered under the low-variability scenario, the protocol should either increase the number of biosimilar lots or modify the reference lot procurement strategy to better capture the reference product’s true long-term variability.
The Quality Range Method: Calibrating the ‘k’ Factor
The quality range method for Tier 2 attributes sets a statistical acceptance range based on the reference product’s distribution. The range is defined as the reference mean plus or minus k times the reference standard deviation, where k is chosen by the developer and must be justified to the agency.
The selection of k involves a trade-off between analytical stringency and operational feasibility. A k of 2 covers approximately 95% of the reference product’s distribution under normality assumptions; a k of 3 covers approximately 99.7%. The FDA has not prescribed a specific k value but expects the selection to reflect the clinical risk of the attribute being assessed. For an attribute with a clear, well-documented relationship between variability and clinical outcome, k should be smaller, indicating a tighter standard. For an attribute whose clinical relevance at the margins of its distribution is not well characterized, k can be larger.
In practice, k values of 2 and 3 are most commonly used in biosimilar submissions. The choice is justified in the statistical analysis plan with reference to the attribute’s clinical risk assessment, its role in the CQA tier classification, and the precision of the analytical method used to measure it.
Global Bridging Statistics: Controlling Multiplicity in 3-Way Comparisons
A biosimilar program targeting both US and EU approvals requires a study comparing three products: the biosimilar, the US-sourced reference product, and the EU-sourced reference product. This 3-way comparison structure generates multiple simultaneous statistical hypotheses, and standard hypothesis testing without multiplicity correction inflates the overall Type I error rate.
Three comparisons in a 3-way bridging study: biosimilar versus US reference, biosimilar versus EU reference, and US reference versus EU reference. If each comparison is tested at a 5% significance level, the probability of at least one false positive across the three tests is approximately 14%, not 5%. Regulatory reviewers are aware of this problem and expect sponsors to address it explicitly in the statistical analysis plan.
Several approaches are used in practice. The Bonferroni correction applies a stricter significance level to each individual test (0.05/3 = 0.0167 for three tests), which controls the family-wise error rate but reduces statistical power. The Holm-Bonferroni step-down method provides better power while still controlling the family-wise error rate by applying a sequentially stricter correction based on the ordered p-values. Simultaneous confidence band methods construct a joint confidence region for all comparisons and require the entire region to fall within the acceptance margins for all comparisons to pass.
For PK parameters in bridging clinical studies, the EMA’s standard 80% to 125% acceptance margin for the geometric mean ratio applies to each pairwise comparison, and the statistical analysis plan must specify how the multiplicity across comparisons is handled. The FDA applies similar logic for bridging PK studies, though the specific margin depends on the pharmacological context and the molecule’s PK variability.
Key Takeaways: Part 10
Statistical planning for a biosimilar analytical similarity assessment is not a standard activity that can be delegated to a general biostatistician with small-molecule experience. The TOST procedure’s dependence on estimated reference product variability, the k-factor selection problem for quality range analyses, and the multiplicity challenges of global bridging studies all require specific expertise in biosimilar statistical methodology. Statistical analysis plans should be finalized before study execution begins, not after data collection, and early consultation with regulatory biostatisticians at both the FDA and EMA is a standard risk-mitigation practice.
Part 11: Manufacturing Scale-Up: The Hidden Destroyer of Programs
Why Lab-Scale Success Does Not Predict Commercial Performance
The engineering and biological differences between a 50-liter development bioreactor and a 15,000-liter commercial-scale tank are more consequential than most non-manufacturing scientists appreciate. The fluid dynamics of large-scale stirred tanks create shear stress environments substantially different from smaller vessels. Oxygen transfer rates scale non-linearly with vessel size. The heat transfer surface area to volume ratio decreases dramatically at scale, affecting the precision of temperature control. Carbon dioxide accumulation in the liquid phase, which affects pH and can inhibit cell growth and alter glycosylation, is a common and underappreciated scale-up problem.
Each of these factors can affect the biology of the production cell line and, through the cell biology, affect the quality attributes of the protein product. A cell culture process optimized at 50-liter scale to produce a specific glycoform distribution may, at 15,000-liter scale, produce a meaningfully different distribution if the oxygen transfer or carbon dioxide clearance conditions are not correctly controlled. The resulting product may have different levels of high-mannose glycoforms, different fucosylation ratios, or different charge variant distributions than the development-scale material.
If the commercial-scale product differs from the development-scale material used in the initial analytical similarity studies and early clinical pharmacology studies, the developer must conduct an internal comparability exercise under ICH Q5E guidance to demonstrate that its own pre-scale and post-scale materials are comparable before the final submission can be completed. This exercise requires the same battery of analytical methods, the same statistical rigor, and the same scientific argumentation as the comparison to the reference product. A failed internal comparability exercise can require manufacturing process re-optimization, which in the worst case means restarting the analytical characterization program from the beginning with the new process.
Quality by Design in Scale-Up: The CPP-CQA Relationship
Quality by Design principles require the developer to explicitly understand and document the relationship between critical process parameters and critical quality attributes. A CPP is a process parameter whose variability has an impact on a CQA, and therefore must be monitored and controlled within a defined range to ensure consistent product quality.
For a monoclonal antibody manufacturing process, key CPPs in the upstream cell culture stage include temperature (both set point and shift timing if a temperature shift strategy is used), pH, dissolved oxygen, agitation rate, nutrient feed composition and timing, and cell density at harvest. Each of these parameters has documented effects on glycosylation, oxidation, and aggregation levels in the published scientific literature and in the body of in-house development data accumulated during process development.
The QbD approach requires the developer to define a ‘design space,’ a multi-dimensional range of CPP values within which the process reliably produces product that meets all CQA specifications. Operating within the design space should not require regulatory approval for process changes; moving outside it does. Demonstrating the robustness of the design space through designed experiments, typically fractional factorial or central composite designs, is a key part of the commercial manufacturing process validation package.
For biosimilar developers, the design space must produce not just product that meets in-house specifications, but product that falls within the similarity ranges established relative to the reference product. The target for process development is therefore externally constrained, which is more demanding than the target for a novel biologic, where the developer has full flexibility to design for any attribute values that meet the clinical requirements.
CDMO Partner Selection: Criteria for Outsourced Manufacturing
Many biosimilar developers, particularly those without legacy biologics manufacturing infrastructure, outsource clinical and commercial manufacturing to contract development and manufacturing organizations. The CDMO selection decision is both a capability decision and a risk management decision, and the specific capabilities required for a biosimilar program differ from those required for a novel biologic program in several important ways.
A CDMO selected for biosimilar manufacturing must have established analytical capabilities for the full range of characterization methods described in Part 9, not just quality control release testing. The ability to perform HDX-MS, native mass spectrometry, AUC-SV, cell-based ADCC assays, and advanced glycan profiling in-house is a significant differentiator, because relying on multiple specialized CROs for these analyses adds coordination complexity, sample handling risk, and timeline uncertainty.
The CDMO must also have a robust reference lot management program, including the capability to acquire, properly store, and maintain documentation for dozens of lots of the reference product over the course of a multi-year development program. Reference lots stored at incorrect conditions or with incomplete chain-of-custody documentation will not be accepted in regulatory submissions.
Platform cell lines and platform formulations represent another important CDMO selection criterion. A CDMO with an established CHO cell expression platform can provide a starting cell line, a defined set of cell culture conditions known to produce well-behaved glycosylation profiles, and preliminary formulation knowledge that substantially compresses the early development timeline compared to a CDMO that must start entirely from scratch for each new molecule.
Key Takeaways: Part 11
Manufacturing scale-up is the phase of biosimilar development most frequently underestimated in project plans and financial models. The timeline and budget contingencies associated with a failed scale-up must be explicitly incorporated into NPV models and investor communications. CDMO selection is a scientific and regulatory decision, not just a cost decision. The specific analytical and manufacturing capabilities of the CDMO partner directly affect the quality of the analytical similarity package and the probability of a successful regulatory submission.
Part 12: Case Studies: Zarxio, Inflectra, and the Adalimumab Biosimilar Wave
Zarxio (Filgrastim-sndz): The Pathfinder Case
Sandoz’s Zarxio received FDA approval in March 2015 as the first US biosimilar under the BPCIA pathway. Amgen’s Neupogen (filgrastim), a recombinant G-CSF with annual US revenues of approximately $1.3 billion at the time of biosimilar entry, was the reference product.
Filgrastim is a 175-amino-acid, non-glycosylated protein produced in E. coli. Its molecular weight of approximately 18.8 kDa makes it substantially simpler than any monoclonal antibody, and the absence of glycosylation removes the most technically demanding PTM characterization requirement. The molecule’s mechanism of action, stimulating neutrophil production by binding the G-CSF receptor, is well understood and has a validated pharmacodynamic endpoint: absolute neutrophil count, measured by a routine complete blood count.
Sandoz’s analytical package for Zarxio covered 22 orthogonal analytical methods applied to 19 quality attributes comparing 19 lots of the biosimilar against 12 lots of the reference product. Primary sequence was confirmed by peptide mapping LC-MS with full sequence coverage. Higher-order structure was assessed by CD, FTIR, and DSC. Biological activity was confirmed by a cell-based proliferation assay and a receptor binding assay. Purity was characterized by SEC, IEX, and capillary electrophoresis.
The clinical program consisted of comparative PK/PD studies in healthy volunteers, demonstrating pharmacokinetic equivalence and equivalent pharmacodynamic response (ANC increase) relative to Neupogen. No comparative efficacy trial was conducted. The approval was granted for all five of Neupogen’s indications through the scientific principle of extrapolation: if the molecule is analytically and pharmacokinetically equivalent, and if the mechanism of action is the same across all indications, there is no scientific basis to require a separate clinical trial for each indication.
The commercial trajectory of Zarxio illustrates both the opportunity and the limits of first-mover advantage in biosimilars. Zarxio launched at approximately 15% below Neupogen’s list price and has captured a substantial share of the US G-CSF market. However, market share accumulation was slower than in EU markets for analogous molecules, reflecting differences in payer incentives and prescriber familiarity with biosimilar products.
Inflectra (Infliximab-dyyb): The First US mAb Biosimilar
Celltrion’s Inflectra received FDA approval in April 2016, establishing the evidentiary standard for complex monoclonal antibody biosimilars in the United States. The reference product, Janssen’s Remicade (infliximab), is a chimeric IgG1 antibody used in rheumatoid arthritis, Crohn’s disease, ulcerative colitis, plaque psoriasis, and ankylosing spondylitis.
The analytical package for Inflectra was substantially more complex than for Zarxio, reflecting infliximab’s greater molecular complexity. Celltrion compared 26 lots of Inflectra against 36 lots of Remicade for core analytical attributes, accumulating a reference dataset large enough to robustly characterize the originator’s natural variability. Primary sequence identity was confirmed. Higher-order structure was assessed by CD, FTIR, DSC, and HDX-MS. Glycan profiles were characterized by released glycan HPLC and intact mass LC-MS. Charge variant distributions were compared by IEX and cIEF. Aggregation was quantified by SEC and AUC-SV.
Minor analytical differences were detected. The charge variant distribution of Inflectra differed slightly from Remicade, with a somewhat different ratio of acidic and basic variants. A small difference in the level of protein dimers was observed. Both differences were thoroughly characterized and judged by the FDA not to be clinically meaningful, based on functional assay data demonstrating that the observed differences had no impact on binding affinity, cell-based neutralization activity, or ADCC potency.
The clinical package included two randomized controlled trials: PLANETRA in rheumatoid arthritis patients and PLANETAS in ankylosing spondylitis patients. Both trials demonstrated equivalent efficacy and comparable safety and immunogenicity profiles. These clinical data, combined with the analytical foundation, supported extrapolation to Remicade’s additional indications without dedicated trials in each condition.
Inflectra’s US commercial launch was complicated by Janssen’s aggressive rebate contracting strategy, which maintained Remicade’s market position at the expense of gross margin. The lesson here is that an approved biosimilar with a solid analytical foundation can still face commercial barriers that have nothing to do with its scientific quality.
The Adalimumab Wave: Anatomy of the Most Complex Biosimilar Market
The US adalimumab biosimilar market began in earnest in 2023 after years of patent settlement negotiations. At peak, Humira had US annual revenues of approximately $18 billion, making its biosimilar market the largest single commercial opportunity in biosimilar history. The analytical and IP challenges of this market deserve detailed examination.
Adalimumab is a fully human IgG1 antibody targeting TNF-alpha. Its mechanism involves direct neutralization of soluble TNF-alpha, binding to transmembrane TNF-alpha, and complement-dependent lysis of TNF-alpha-expressing cells. All three mechanisms are analytically relevant: TNF-alpha neutralization requires intact antigen binding, Fc-mediated effector functions require characterization of FcgR binding and ADCC activity, and CDC requires characterization of complement C1q binding.
The formulation challenge for adalimumab biosimilars was the high-concentration citrate-free formulation covered by AbbVie’s secondary patents. The marketed Humira presents at 100 mg/mL in a citrate-free system, which reduces injection site pain compared to earlier citrate-containing formulations. Any biosimilar seeking to match this patient experience without infringing the citrate-free patents had to develop alternative formulations. Amgen (Amjevita), Samsung Bioepis (Hadlima), Sandoz (Hyrimoz), and others each developed proprietary formulation systems that achieved comparable stability and injectability profiles through different excipient combinations, which then required characterization as part of the analytical similarity package.
The analytical consequence was that the formulation difference between each biosimilar and the reference product had to be assessed as a potential clinically inactive component difference under the FDA’s definition. Each developer had to demonstrate that its different buffer or excipient system did not affect the drug’s stability, its release kinetics from the formulation, or any relevant quality attribute at the time of injection.
Key Takeaways: Part 12
The three case studies span the complexity spectrum from a simple non-glycosylated protein to the most commercially important monoclonal antibody in pharmaceutical history. The analytical rigor required scales with molecular complexity, and the commercial outcomes are shaped by IP landscape as much as by analytical quality. Developers approaching any new target should use these cases as benchmarks for analytical scope, clinical program design, and commercial risk assessment.
Part 13: Patent Intelligence as a Development Tool: Mining IP for Competitive Advantage
Converting Originator Patents into Analytical Blueprints
The intellectual property around a reference product contains detailed technical information that originators spent years and hundreds of millions of dollars generating. Formulation patents describe the stability challenges that had to be overcome and the excipient combinations that resolved them. Manufacturing process patents describe the cell culture conditions, purification sequences, and quality control methods that produced a commercially successful product. Method-of-use patents describe the clinical evidence supporting specific dosing regimens and indications.
A systematic mining of this patent literature, using a structured analytical framework, can convert the originator’s proprietary R&D history into an analytical roadmap for the biosimilar developer. The process begins with identifying all patents in the estate using a comprehensive database search that covers not just the primary compound patent but the full family of continuation applications, divisional applications, international counterparts, and any relevant third-party patents that might read on the development program.
For each patent, the ‘Background of the Invention’ section is the primary source of analytical intelligence. It describes the technical problem the inventors were trying to solve, which directly reveals which quality attributes caused them difficulty and which properties of the molecule they found hardest to control. A formulation patent that opens by describing the challenge of maintaining monomer integrity at high protein concentrations under refrigerated storage is explicitly telling the reader that aggregation under those conditions is a CQA that requires specific attention.
The ‘Examples’ section is the second key resource. It describes the specific experiments conducted, the formulations or process conditions tested, and the analytical methods used to evaluate them. This is primary experimental data, generated and validated by the originator’s own scientists, describing the relationship between specific excipients or process parameters and the quality attributes they affect. It is, in effect, a published structure-activity relationship for the formulation or process, and it provides a starting point for the biosimilar developer’s own experimental design.
Freedom-to-Operate Analysis as an Analytical Development Constraint
Freedom-to-operate analysis determines whether specific development activities or commercial activities would infringe any in-force patents. For a biosimilar developer, FTO analysis is not a one-time activity conducted before program initiation; it is a continuous process that evolves as the development program progresses and as new patents are granted or challenged.
The most analytically consequential FTO constraint is the formulation patent. If the originator holds valid, enforceable patents on the only formulation system capable of maintaining the molecule’s stability at commercial concentrations, the biosimilar developer has two options: license the patent or develop an alternative formulation that provides comparable performance without infringing. The second option requires its own formulation development program and, critically, its own analytical characterization to demonstrate that the alternative formulation system does not introduce any new quality attribute differences relative to the reference product.
A biosimilar developer who has not systematically analyzed the formulation IP landscape before beginning formulation development may invest 12 to 18 months in optimizing a formulation system that turns out to infringe a core patent, requiring a complete restart with a non-infringing excipient system. This failure mode is entirely preventable with adequate upfront patent analysis.
Tools like DrugPatentWatch provide structured access to drug patent databases, patent expiration calendars, litigation histories, and regulatory exclusivity information in a format that enables efficient, systematic analysis of the full IP estate around any target molecule. The ability to rapidly screen a patent portfolio for relevant technical claims, track litigation outcomes, and monitor continuation application filings is operationally essential for biosimilar development teams managing multiple programs simultaneously.
Competitive Pipeline Intelligence: Monitoring Biosimilar Developer Activity
Beyond the originator’s IP estate, biosimilar developers need continuous intelligence on the activities of their competitors in the same molecule class. IND filings, BLA application dates, clinical trial registrations, partnership announcements, and manufacturing facility FDA inspections are all publicly available signals that, when tracked systematically, provide a picture of the competitive development timeline for any given molecule.
A biosimilar developer who enters the market second or third for a given molecule faces a materially different commercial landscape than the first entrant. Payer contracts negotiated by the first biosimilar entrant may have exclusivity provisions that block subsequent competitors for defined periods. Hospital formulary decisions tend toward single-source biosimilar adoption. The first entrant’s pharmacovigilance data accumulates real-world safety and efficacy evidence that reinforces prescriber confidence in that specific product.
The financial consequence of being the third biosimilar to market for a given molecule versus the first can easily exceed $200 million in NPV terms, depending on the molecule’s market size and the competitive dynamics of the specific therapeutic class. Tracking competitor development timelines using all available public information is therefore a material component of portfolio strategy for any company with multiple biosimilar programs.
Key Takeaways: Part 13
Patent intelligence is a scientific tool, not just a legal one. The originator’s IP portfolio is a documented history of the molecule’s development challenges and the solutions that worked, available for systematic analysis by any developer willing to invest the time and expertise to extract its technical content. Failing to conduct this analysis before beginning formulation development or CQA risk assessment leaves a material source of competitive advantage unused, and creates the risk of late-stage program failures that patent analysis would have predicted and prevented.
Part 14: Investment Strategy: NPV Frameworks, Risk Factors, and Portfolio Construction
The NPV Model for a Biosimilar Program: Key Inputs and Common Errors
Net present value modeling for biosimilar programs involves a set of inputs that differ materially from those used for novel drug development programs. The most common errors in biosimilar NPV models stem from underestimating development cost, overestimating market penetration, and mismodeling the IP litigation timeline.
Development cost for a complex mAb biosimilar program runs from $150 million to $300 million in total direct costs. This range reflects the variability in analytical program scope, the presence or absence of a confirmatory clinical efficacy trial, manufacturing scale-up complexity, and CDMO fees. Programs that expect to rely on PK/PD bridging without a confirmatory efficacy trial should model the lower end of this range contingent on a successful analytical package and a supportive regulatory outcome. Programs that anticipate a full comparative efficacy trial should model the upper end and extend the timeline by 18 to 30 months.
Development cost for a simpler non-glycosylated protein like filgrastim runs from $75 million to $150 million, reflecting the reduced analytical scope and the availability of validated PK/PD endpoints that support a PK/PD-only clinical strategy.
Market penetration rates for biosimilars vary dramatically by molecule class, therapeutic area, therapeutic setting (hospital vs. retail pharmacy), payer system, and competitive dynamics. A naive model that assumes biosimilar penetration will follow the trajectory of small-molecule generics (rapid and near-complete within two to three years) consistently overestimates biosimilar revenues. Hospital-administered oncology biologics have seen faster penetration than physician-administered immunology biologics because hospital pharmacy and therapeutics committees make formulary decisions centrally and have strong incentives for cost reduction. Retail pharmacy-dispensed biologics depend on pharmacy benefit manager formulary tier decisions and prescriber willingness to authorize substitution, both of which move more slowly.
IP litigation timeline errors are the most consequential modeling mistakes. A model that assumes the reference product’s composition-of-matter patent expiration date is the correct market entry timeline, without accounting for secondary patent litigation, settlement negotiation, and the BPCIA patent dance process, will consistently overestimate NPV by placing commercial cash flows years ahead of their actual timing. The Humira case established that secondary patent estates can effectively extend exclusivity by six to eight years beyond the primary patent expiration. This is an extreme case, but secondary patent litigation adding two to four years to biosimilar market entry is common for complex biologics with active IP management programs.
Portfolio Construction: Diversification Across Molecule Complexity and IP Risk
For an investor or company building a biosimilar portfolio, the most effective risk management strategy combines programs across the complexity-IP risk spectrum. A portfolio concentrated entirely in complex mAbs with dense secondary patent estates carries high correlated risk: if the IP litigation environment becomes more hostile, multiple programs are affected simultaneously. A portfolio that includes simpler molecules with thin IP estates provides downside protection while the complex mAb programs work through their litigation timelines.
The ideal portfolio structure, from a risk-return perspective, includes some combination of the following. First, one or two complex mAb programs targeting molecules with high commercial values (above $5 billion in annual global revenue) where the analytical investment is large but the commercial prize justifies it. Second, two or three programs targeting molecules in the intermediate complexity range, including glycoproteins with some secondary IP complexity but where the patent estate is manageable and the development timeline is more predictable. Third, one or two simpler molecules with thin IP estates where the development cost is lower and the timeline to market is shorter, providing earlier cash flows to offset the longer development cycles of the complex programs.
Platform approaches to biosimilar development, where the same analytical methodology, the same cell expression system, and the same CDMO infrastructure are applied to multiple molecules in sequence, provide cost advantages that justify portfolio approaches over single-program strategies. A developer who has built the analytical team, the reference lot procurement infrastructure, and the CDMO relationships required for one mAb biosimilar can typically initiate a second program at 60 to 70 cents on the dollar relative to the first program’s cost, because the fixed investments in capability have already been made.
Signals to Monitor: Leading Indicators of Biosimilar Program Risk
Several observable signals indicate elevated risk in a biosimilar development program before the risk materializes in a regulatory deficiency letter or clinical trial failure.
Reference product manufacturing changes by the originator are a leading indicator of analytical risk. If the originator announces a manufacturing process change or a change in the commercial product specification, the biosimilar developer’s existing analytical comparison may become partially obsolete. Regulatory submissions must be based on comparison to the currently marketed reference product, not the product as it existed when the program began. Originators sometimes make these changes strategically, knowing they complicate the biosimilar comparability exercise.
Regulatory complete response letters for competitor biosimilars targeting the same molecule are the most direct available intelligence about specific regulatory expectations. When the FDA or EMA issues a CRL for a biosimilar program and the deficiency letter is made public, it describes exactly what the agency found inadequate. This is a specific, actionable signal for any other developer working on the same molecule.
Patent Paragraph IV certification filings and litigation outcomes for competitor programs are directly relevant to any developer’s IP risk model. A successful invalidity argument by a competitor against a key secondary patent opens the path for all biosimilar developers. A failed invalidity argument, or an unfavorable preliminary injunction ruling, indicates that the patent will remain in force and will need to be designed around or licensed.
Manufacturing inspection outcomes, specifically FDA Form 483 observations and warning letters issued to CMO facilities used by biosimilar competitors, are publicly available and provide intelligence about the state of manufacturing quality in the biologics CDMO ecosystem.
Key Takeaways: Part 14
Biosimilar NPV modeling requires specific inputs and assumptions that differ substantially from novel drug development models. The most common and most financially consequential modeling errors involve development cost underestimation, IP litigation timeline errors, and overly optimistic market penetration rates. Portfolio construction benefits from explicit diversification across the complexity-IP risk spectrum. Program risk monitoring should incorporate signals from competitor regulatory outcomes, originator product changes, and IP litigation developments.
Part 15: The Future of the Field: Interchangeability, Harmonization, and the End of Confirmatory Efficacy Trials
The Interchangeability Redesign: What the FDA’s 2024 Guidance Means for Commercial Strategy
The FDA’s June 2024 draft guidance proposing to eliminate switching studies as a requirement for interchangeability designation is the most commercially significant regulatory document for the US biosimilar market in several years. The full implications for development program design and commercial strategy merit careful analysis.
The scientific basis for the FDA’s position is solid. The agency reviewed post-marketing surveillance data from multiple years of biosimilar use in the United States and in Europe, where automatic substitution has been practiced in some member states since the early days of biosimilar regulation. This review found no evidence of increased adverse events, immunogenic reactions, or loss of efficacy in patients who switched from a reference product to a biosimilar or between biosimilars. The conclusion is consistent with the scientific prediction: if two products are analytically highly similar and pharmacokinetically equivalent, the clinical risk of switching between them is not meaningfully different from the inherent variability of continuing on the same product.
The practical consequence for developers is that the additional clinical study previously required for interchangeability, which was a multi-arm pharmacokinetic study with alternating dosing periods typically requiring 100 to 200 subjects and costing $15 million to $30 million, can likely be eliminated from the development plan. This is a direct and immediate cost reduction.
The commercial consequence is more nuanced. If interchangeability becomes effectively automatic for any biosimilar with an adequate analytical and PK package, the first-interchangeable exclusivity period that BPCIA creates becomes commercially less valuable. Multiple biosimilars in the same class may achieve interchangeability within months of each other, rather than the previous pattern where one developer invested in the switching study and held the exclusivity. The result is faster competition among interchangeable products, faster price erosion, and greater market share for the payer systems and patients who benefit from lower prices.
For developers currently planning programs, the implication is to design the analytical and PK package to the highest achievable quality from the outset, treating interchangeability as an outcome that follows from scientific rigor rather than from a specific additional study. This is both the scientifically correct approach and the strategically optimal one under the new regulatory framework.
Global Harmonization: Progress, Obstacles, and the Path Forward
The global regulatory landscape for biosimilars remains fragmented in ways that add significant cost and delay to development programs with ambitions beyond the US and EU. Japan’s Pharmaceuticals and Medical Devices Agency has its own guidance framework, which has historically required demonstration of biosimilarity relative to Japanese-licensed reference products rather than accepting non-Japanese reference product comparisons. China’s National Medical Products Administration has a rapidly evolving biosimilar framework that has been moving toward greater alignment with international standards but retains specific data requirements that differ from the FDA and EMA. Emerging markets in Southeast Asia, Latin America, and the Middle East each have their own regulatory frameworks at various stages of development.
The most impactful harmonization progress in the near term is likely to come from bilateral or multilateral agreements between major regulatory agencies to mutually recognize biosimilar approvals under certain conditions. Pilot programs for reliance on foreign regulatory decisions already exist in various forms; extending this principle to biosimilar approvals could substantially reduce the data generation burden for developers pursuing multi-regional launches.
The WHO’s biosimilar evaluation guidelines provide a scientific foundation for regulatory convergence in emerging markets, and the WHO’s Collaborative Registration Procedure allows member states to rely on WHO recommendations for product approval without conducting a full independent evaluation. Expanding the scope and uptake of these collaborative procedures would meaningfully accelerate biosimilar access in markets where the regulatory infrastructure for independent review is limited.
For developers, the practical strategy in the current environment is to design the global development program around the most demanding regulatory requirements, which is generally the FDA’s analytical framework and the EMA’s clinical PK requirements, and then build regional filing strategies that adapt the core submission for each additional market. This approach is more expensive upfront than a single-market strategy, but it produces a dossier with the scientific depth and technical comprehensiveness to withstand regulatory review in any jurisdiction.
AI and Machine Learning in Analytical Development: Current Applications and Near-Term Trajectory
Artificial intelligence and machine learning are already deployed in operational biosimilar development programs, though the applications are currently more concentrated in data analysis and process optimization than in the analytically creative functions that define competitive programs.
Mass spectrometry data from biosimilar characterization programs is a natural application domain for machine learning. A single LC-MS/MS run on a peptide digest can produce hundreds of thousands of spectral data points. Automated peak identification, charge state deconvolution, and glycopeptide assignment are all functions where machine learning algorithms outperform manual analysis in speed and, for well-trained models, in accuracy. Vendors including Thermo Fisher, Waters, and Agilent are embedding ML-based data processing tools into their commercial software platforms. These tools reduce the analyst time required for routine data processing but do not yet fully replace the scientific judgment required for complex cases or unusual findings.
In manufacturing process development, ML models trained on historical bioreactor data can predict quality attribute outcomes from process parameter inputs with sufficient accuracy to guide process optimization decisions without exhaustive confirmatory experiments. A model trained on the relationship between pH, dissolved oxygen, agitation rate, and N-linked glycan distribution across hundreds of bioreactor runs can suggest process conditions likely to produce a target glycan profile, reducing the number of experimental runs required during scale-up optimization.
The near-term trajectory is toward integration of analytical data streams from multiple sources, including real-time bioreactor monitoring, at-line spectroscopic measurements, and offline chromatographic analyses, into unified data models that can detect process deviations and predict their downstream quality attribute consequences before the batch is harvested. This is not AI creativity; it is sophisticated pattern recognition applied to high-dimensional manufacturing data, and it has a well-defined path to clinical and commercial utility.
The Scientific Case for Eliminating Confirmatory Efficacy Trials in Well-Characterized Molecule Classes
The accumulated evidence from more than a decade of biosimilar approvals supports a clear scientific argument: for molecules with well-characterized structure-activity relationships, validated pharmacodynamic endpoints, and no known mechanism-dependent immunogenic risks that are not captured by analytical assessment, a confirmatory comparative efficacy trial adds negligible information about biosimilarity relative to what an excellent analytical and PK package already provides.
The EMA’s ‘tailored clinical approach’ reflection paper articulates this argument in regulatory language. The FDA has operationalized it, at least partially, through its acceptance of PK/PD-only programs for molecules like filgrastim and insulin, and its evolving position on the minimum clinical evidence required for interchangeability.
The extension of this principle to complex monoclonal antibodies is the logical next step, and the scientific community is building the evidentiary foundation to support it. For molecules like infliximab and trastuzumab, where the clinical indications are diverse and the mechanisms are well understood, the case for a waiver of confirmatory efficacy trials based on comprehensive analytical and PK data is scientifically defensible. Regulators have not yet formally adopted this position for all mAb classes, but the direction of travel is clear and the scientific arguments supporting it are becoming harder to dispute.
For the biosimilar industry, the commercial consequence of widespread adoption of this principle is transformative. Average development costs would fall by $50 million to $100 million per program. Development timelines would compress by 18 to 30 months. The number of competitors able to enter any given biosimilar market would increase, accelerating price competition. Healthcare systems and patients would benefit from faster access to more affordable medicines.
For investors, this trend means that the barriers to entry in biosimilar markets will continue to decline over the next decade. Programs that are currently too expensive to justify for molecules with moderate market sizes will become financially viable as the clinical development burden shrinks. The competitive advantage will shift progressively from the ability to fund large clinical programs to the ability to execute excellent analytical development with speed and precision.
Key Takeaways: Part 15
The regulatory direction for biosimilar development is consistently toward greater reliance on analytical data and less on confirmatory clinical evidence. The FDA’s interchangeability guidance change, the EMA’s tailored clinical approach, and the global harmonization momentum all point in the same direction. Developers who build their core competencies around analytical excellence, statistical rigor, and global regulatory strategy are positioned to benefit from this trend. Those who continue to rely on traditional clinical trial-centric development models will find themselves at a systematic cost and timeline disadvantage.
Summary: Key Takeaways Across All Sections
The biosimilar analytical similarity assessment is the primary scientific and commercial differentiator in a market projected to exceed $100 billion in annual revenues within the next decade. The following points synthesize the core findings across this analysis:
The totality-of-the-evidence pyramid places analytical assessment at the foundation. The more comprehensive and technically convincing the analytical package, the lower the clinical development burden and the shorter the time to market.
CQA identification and tier classification are strategic decisions with direct financial consequences. Errors in CQA scoping cause regulatory deficiency letters. Accurate tier classification with well-justified statistical plans enables the most efficient allocation of analytical resources.
Reference product characterization is the most common point of failure in biosimilar programs. Insufficient lot procurement, too narrow a manufacturing date range, and inadequate analytical method development for the reference product propagate errors through every subsequent stage of development.
IP valuation is a primary input to biosimilar target selection. The originator’s patent estate, specifically the secondary formulation, manufacturing, and method-of-use patents, determines the realistic market entry timeline more accurately than the primary composition-of-matter expiration date.
Evergreening strategies extend effective exclusivity well beyond the primary patent. A systematic taxonomy of evergreening tactics, applied to every target molecule before program initiation, is the minimum required analysis for any credible investment decision.
Manufacturing scale-up is a material source of program risk that is consistently undermodeled in development plans and investor projections. Explicit contingency budgets and timeline buffers for scale-up challenges should be standard inputs in program financial models.
The regulatory landscape is moving consistently toward greater analytical reliance and reduced clinical burden. Developers who invest in the most sensitive analytical platforms and build the regulatory science expertise to maximize the value of those investments are aligned with the trajectory of the field. Those who do not will find regulatory expectations moving away from their capabilities.
This analysis was prepared for informational purposes for pharmaceutical industry professionals, IP counsel, and institutional investors. It does not constitute legal, regulatory, or investment advice. Patent landscapes, regulatory guidance, and market data are subject to continuous change. All program-specific decisions should be made in consultation with qualified legal, regulatory, and scientific advisors.