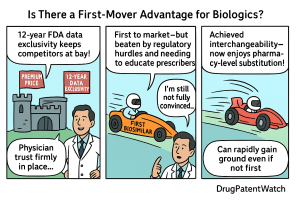
The biosimilar first-mover question has a clean theoretical answer and a messy empirical one. Theory says: get to market first, lock up formularies, and collect the premium. The adalimumab data says something more specific, and more useful — that timing matters less than which lever you pull, and that the innovator’s patent architecture can make the question of ‘first’ entirely academic for years.
This guide works through the mechanics of biosimilar market entry from the patent estate backward through launch sequencing, payer contracting, interchangeability strategy, and real-world evidence generation. It is written for IP teams, portfolio managers, and R&D leads who need to move past the high-level narrative and into actionable frameworks.
Part I: Framing the Question
What ‘First Mover’ Actually Means in Biosimilars
The phrase ‘first-mover advantage’ gets borrowed from consumer technology markets, where network effects and switching costs can lock in early users for years. Biosimilars work differently. The ‘market’ is not one homogeneous population of buyers — it is a layered decision architecture involving the FDA’s interchangeability determination, PBM formulary committees, hospital P&T committees, specialty-specific physician prescribing habits, and state pharmacy substitution laws. Being first in time does not translate automatically into being first at any of those decision points.
That distinction matters because the two most frequently cited benefits of early biosimilar entry — early market share capture and favorable payer contracts — are not guaranteed by regulatory approval. They require active commercial execution against a set of institutional inertias that, without the right strategy, can hold total biosimilar market share below 5% for more than a year post-launch, exactly as happened with adalimumab through most of 2023.
The more precise question is not whether a first-mover advantage exists, but under what conditions it materializes, how durable it is, and what destroys it. The adalimumab saga answers all three.
Key Takeaways for Part I:
- ‘First mover’ in biosimilars is defined not at FDA approval but at the formulary and prescriber level.
- Early market share capture requires active PBM contracting, not just regulatory clearance.
- Market inertia can suppress even a first-to-market biosimilar to single-digit share for 12 months or more.
- Understanding which lever drives adoption (payer vs. physician vs. interchangeability) determines the value of timing.
Part II: The Biologic IP Estate
The Biologic IP Estate: What You’re Competing Against
Any analysis of biosimilar market entry must start with the innovator’s IP position, because that is the constraint set inside which all timing and strategy decisions are made.
Biologics operate under a different IP framework than small-molecule drugs. Under the Hatch-Waxman Act, small-molecule generics face a defined patent list in the Orange Book, and the Paragraph IV certification process gives generics a structured litigation pathway with a 30-month stay. The Biologics Price Competition and Innovation Act of 2009 (BPCIA) established the analogous pathway for biosimilars, but with a critical architectural difference: the BPCIA places no statutory cap on the number of patents a reference product sponsor can assert in BPCIA litigation. There is no biosimilar equivalent of the Orange Book’s finite listed patents. That omission is the single largest structural reason why biologic patent thickets are denser and more litigation-intensive than anything in the small-molecule world.
The composition of a mature biologic IP estate typically has several layers. The primary composition-of-matter patent covers the active molecule. Secondary patents cover formulations, including excipient choices, concentration levels, and citrate content. Manufacturing process patents cover cell line selection, purification steps, and production conditions. Method-of-use patents cover each approved indication individually. Delivery device patents cover auto-injectors, prefilled syringes, and pen configurations. Finally, continuation patents — filed long after market launch — extend the filing date of the original application while claiming progressively narrower and more specific embodiments.
This layering is not incidental. It is a deliberate IP lifecycle management strategy, sometimes called ‘evergreening,’ in which a company files continuation applications continuously to maintain a stream of patents with different expiry dates, ensuring that no single patent expiry opens a clean window for biosimilar entry.
IP Valuation: Why the Patent Estate Is a Financial Asset, Not Just a Legal One
For innovator companies, the patent portfolio around a blockbuster biologic is not simply a defensive legal instrument. It is a revenue-generating asset with a quantifiable present value equal to the discounted cash flows attributable to years of exclusivity preserved through patent enforcement.
AbbVie’s Humira portfolio makes this concrete. Humira launched in 2002. Its primary composition-of-matter patent expired in the U.S. in 2016. Yet biosimilars did not enter the U.S. market until January 2023, a gap of nearly seven years. During that interval, Humira generated over $150 billion in cumulative global revenue. The secondary and tertiary patents that filled the gap between composition-of-matter expiry and actual biosimilar entry were, in financial terms, worth an estimated 60–70% of the drug’s total U.S. lifetime revenue. That is what a patent estate does when it is managed as a core asset.
For biosimilar developers, the inverse calculation matters equally. Before committing $100–$300 million in development capital to a biosimilar program, the team needs a granular read on the innovator’s IP estate: which patents are likely invalid on obviousness grounds, which are litigation-resistant, which are pure continuation filings linked by terminal disclaimers to an already-expired parent, and which manufacturing patents extend the effective exclusivity window past the formulation patent expiry.
This analysis is precisely what tools like DrugPatentWatch are built for — tracking the full patent estate, litigation history, regulatory exclusivity layers, and settlement terms that define the actual market entry window, as opposed to the theoretical window suggested by the primary composition patent date alone.
Key Takeaways for Part II:
- The BPCIA’s absence of a patent cap is the structural root cause of dense biologic patent thickets.
- A biologic’s IP estate has at least five distinct layers; each must be analyzed independently.
- Secondary and continuation patents represent a quantifiable financial asset for innovators and a quantifiable risk for biosimilar entrants.
- Biosimilar ROI modeling that starts only with primary patent expiry will systematically overestimate the addressable entry window.
Part III: The Patent Dance and Settlement Mechanics
The Patent Dance: Strategy, Not Procedure
The BPCIA’s pre-litigation information exchange process, colloquially called the ‘patent dance,’ requires the biosimilar applicant (the 351(k) applicant) to share its abbreviated Biologics License Application (aBLA) and manufacturing information with the reference product sponsor. The sponsor then identifies patents it believes would be infringed. The parties negotiate which patents to litigate immediately in a first wave and which to reserve. Litigation follows, and settlements are common.
The critical strategic insight is that the patent dance functions less as a dispute resolution mechanism and more as a structured business negotiation with litigation as the credible threat. Approximately 67% of BPCIA cases terminate through settlements or stipulated dismissals rather than judicial decisions on the merits. Settlements typically include a negotiated market entry date, sometimes a royalty on post-entry sales, and a license to the patents at issue.
For biosimilar developers, the dance creates two distinct strategic choices. Engage and reveal manufacturing details, gaining information about the patent list but exposing proprietary process data. Or opt out, as Sandoz did in the original Zarxio (filgrastim) dispute that went to the Supreme Court in 2017, protecting process data at the cost of triggering more aggressive litigation. The Supreme Court in Sandoz Inc. v. Amgen Inc. confirmed that the dance is not mandatory, resolving the opt-out question in favor of the biosimilar developer’s discretion, but the strategic tradeoffs remain product-specific.
Settlement dynamics mean that in a crowded reference product (one with multiple biosimilar programs), the first company to settle sets the market entry date benchmark for all subsequent settlements. AbbVie negotiated staggered entry dates with nine biosimilar manufacturers for Humira, all centered on 2023. The first settlement, with Amgen, effectively defined the floor below which subsequent entrants could not go. Amgen’s six-month exclusivity window before the July 2023 cohort launched was a direct product of being first to settle, not first to receive FDA approval — Amgevita/Amjevita was approved in September 2016, nearly seven years before its U.S. commercial launch.
The Settlement-Entry Date as the True First-Mover Metric
This reframing is important for portfolio strategy. In markets with dense patent thickets and multiple biosimilar programs, the ‘first mover’ is most accurately defined as the company that negotiates the earliest market entry date in its settlement agreement, not the one that filed its aBLA earliest or received FDA approval first. Those earlier milestones matter for the settlement negotiation — a company with FDA approval in hand has stronger leverage — but they do not map directly to launch timing.
For biosimilar developers, this means that patent litigation strategy and settlement timing should be explicitly modeled as market entry levers, not just legal costs. A company that settles early and alone may secure a meaningful exclusivity window before the next wave of entrants. A company that litigates aggressively and loses may find itself launching simultaneously with five competitors, eliminating any timing advantage.
Key Takeaways for Part III:
- The patent dance is a negotiation mechanism, not a pure litigation process.
- Settlement market entry dates, not aBLA filing dates, determine actual launch sequencing.
- First-to-settle with a leading exclusivity window is the operationally meaningful definition of ‘first mover’ in densely patent-protected markets.
- Process data exposure during the dance is a strategic cost that must be weighed against the litigation leverage gained.
Part IV: The AbbVie Humira Portfolio — A Case Study in IP Defense
Case Study: AbbVie’s Humira Patent Portfolio as the Definitive Evergreening Model
No reference biologic has been studied more thoroughly as an IP defense case study than Humira. The numbers are striking enough to cite directly: AbbVie filed over 250 patents related to adalimumab. Of those, approximately 130 were granted in the U.S. alone, with many linked by terminal disclaimers — a legal mechanism that allows continuation patents to co-expire with a parent patent while still claiming novel, narrower subject matter. Independent analysis has found that approximately 80% of the patents in Humira’s U.S. portfolio were non-patentably distinct from each other, meaning they existed primarily to expand the litigation surface area rather than to protect genuinely novel inventions.
In BPCIA litigation, AbbVie placed 61 to 80 patents on its list in individual ‘patent dances’ with each biosimilar manufacturer. The volume alone was coercive: no biosimilar company could economically litigate 60-plus patents simultaneously, even if many of those patents were of questionable validity. The rational response — and the response all nine manufacturers eventually took — was to settle for delayed entry rather than litigate an impassable patent thicket. Biosimilar companies that settled explicitly acknowledged they had no viable alternative to accepting 2023 launch dates, years after the primary composition patent had expired.
The financial consequence for AbbVie: Humira held roughly 99% of the U.S. adalimumab market through November 2023, ten months after the first biosimilar launched. Even in 2024, with ten biosimilars commercially available, AbbVie still held 96% of market share as late as February 2024. The patent estate, functioning as designed, delivered approximately seven additional years of near-monopoly pricing in the world’s largest pharmaceutical market.
IP Valuation: The Humira Patent Estate in Financial Terms
AbbVie’s Humira generated $14.4 billion in global net revenues in 2023, down 32% from the prior year but still the world’s top-selling drug. By 2024, global Humira net revenues reached approximately $9 billion, with biosimilar erosion accelerating particularly in the U.S., where the drug still accounted for roughly 34% of AbbVie’s immunology portfolio revenues.
The IP defense strategy’s value can be estimated by comparing U.S. biosimilar entry timing with Europe. In Europe, where the patent thicket was less dense and regulatory frameworks differ, the first Humira biosimilar (Samsung Bioepis’ Imraldi) entered in October 2018 — five years before the U.S. The resulting price erosion in Europe was immediate and steep. AbbVie had already written down European revenues substantially by the time U.S. biosimilars entered. The U.S. revenue preserved between 2018 and 2023 by the patent estate, at Humira’s average annual U.S. net revenue of approximately $12–15 billion per year, represents an IP-derived value in the range of $60–75 billion. That is the asset value of a well-executed biologic patent strategy.
For biosimilar developers, Humira’s IP architecture functions as both a warning and a template. The warning: do not model market entry timing based on the composition-of-matter expiry. The template: understand that manufacturing and formulation patents with late expiry dates (Humira has manufacturing patents extending to 2034) can create residual litigation exposure even for post-settlement entrants.
Investment Strategy Note: AbbVie’s share price held surprisingly well through the 2023 biosimilar entry wave precisely because the market had already priced in the settlement-negotiated timeline years in advance. The patent estate provided time for AbbVie to develop replacement revenue drivers — specifically Skyrizi (risankizumab) and Rinvoq (upadacitinib) — that now anchor the immunology franchise as adalimumab erodes. IP teams at biosimilar-targeted innovators should benchmark their lifecycle management strategy against this model: use patent exclusivity time not just to delay competitors but to build the successor portfolio.
Key Takeaways for Part IV:
- AbbVie deployed over 250 patents, roughly 80% of which were non-patentably distinct, to create litigation-coercive volume rather than individually strong IP positions.
- The U.S. vs. Europe biosimilar entry timing gap for Humira represents an IP-derived financial benefit in the range of $60–75 billion in preserved revenues.
- Manufacturing patents extending to 2034 create residual litigation exposure for adalimumab biosimilar entrants even after all settlement windows have opened.
- Innovator companies should model patent estate value as a transition financing mechanism for successor product development.
Part V: Regulatory Pathways
Regulatory Pathways and the Interchangeability Asymmetry
The FDA’s biosimilar approval framework under the BPCIA has two distinct endpoints. Biosimilarity approval means the product has demonstrated no clinically meaningful differences from the reference product in terms of safety, purity, and potency. Interchangeability designation means the product has additionally demonstrated through a switching study that alternating between the reference product and the biosimilar produces no additional risk relative to using the reference product alone.
The distinction has direct commercial consequences. A biosimilar without interchangeability can be prescribed by physicians as an alternative to the reference product, but pharmacists cannot substitute it at the dispensing level without a new prescription. A biosimilar with interchangeability can be auto-substituted by the pharmacist in states that permit pharmacy-level substitution — the majority of U.S. states — without contacting the prescriber.
The interchangeability switching study requirement is operationally significant. It requires a randomized controlled trial comparing pharmacokinetics, efficacy, immunogenicity, and safety between patients who switch multiple times between the reference product and the biosimilar against those who remain on continuous treatment. The VOLTAIRE-X study that earned Boehringer Ingelheim’s Cyltezo (adalimumab-adbm) the first interchangeability designation for Humira enrolled 238 patients with moderate-to-severe chronic plaque psoriasis in a multiple-switch design. Cyltezo received FDA interchangeability approval in October 2021 — two full years before its negotiated commercial launch date of July 1, 2023.
That sequencing is strategically relevant. Boehringer Ingelheim had interchangeability in hand before launch, giving it a designation that no other adalimumab biosimilar held at the time of entry. Amjevita, which launched six months earlier in January 2023, did not carry the interchangeability label. The question — which proved commercially important — was whether interchangeability translated into meaningful market share.
The Interchangeability Exclusivity Provision
The BPCIA provides the first interchangeable biosimilar for a given reference product with a period of interchangeability exclusivity during which no other biosimilar can receive interchangeability designation for the same reference product. The exclusivity period has a complex calculation based on timing benchmarks, but the net effect is that Cyltezo held a period of exclusivity as the first and only interchangeable adalimumab biosimilar in the U.S. market.
Sandoz’s Hyrimoz (adalimumab-adaz) received interchangeability designation for its prefilled syringe presentation in April 2024, but not for its autoinjector formulation, illustrating the FDA’s presentation-specific application of the interchangeability determination. As of mid-2025, seven adalimumab biosimilars hold interchangeability designation: Amjevita, Cyltezo, Hyrimoz (prefilled syringe), Abrilada, Hulio, Yuflyma, and Simlandi.
The proliferation of interchangeable designations across the adalimumab class has diluted the competitive value of any single company’s interchangeability status. This was predictable. Interchangeability exclusivity provides a meaningful window only if the first-interchangeable biosimilar can convert formulary and prescriber adoption before competitors close the designation gap.
EMA Framework: No Interchangeability Designation, Different Substitution Dynamics
The European Medicines Agency evaluates biosimilars solely on biosimilarity criteria. There is no EU-level interchangeability designation. Individual member states determine substitution policy, and practice varies considerably: some northern European countries permit pharmacy-level substitution of biosimilars, while others require a new prescription. This regulatory heterogeneity across 27 member states creates a fragmented commercial landscape in which the same biosimilar may be substitutable in Denmark and not in Germany.
For biosimilar developers building global strategies, this means the commercial advantage of interchangeability is geographically specific to the U.S. and a subset of markets that have adopted similar frameworks. The ROI calculation for a dedicated switching study must account for the U.S.-only or limited-market applicability of the resulting designation.
Key Takeaways for Part V:
- Interchangeability requires a dedicated switching study and confers auto-substitution rights at the pharmacy level in most U.S. states.
- First interchangeability exclusivity provides a competitive window, but the adalimumab market shows that the window narrows quickly as competitors file for the same designation.
- The EMA has no interchangeability framework; substitution policy is determined at the member-state level, creating commercial heterogeneity across Europe.
- Interchangeability’s ROI must be modeled against the cost of the switching study, the duration of the exclusivity window, and the speed at which competing programs can close the designation gap.
Part VI: Market Dynamics — What the Adalimumab Data Actually Shows
The Adalimumab Market: What Amjevita’s Launch Window Actually Bought
Amgen’s Amjevita entered the U.S. market on January 31, 2023, as the first Humira biosimilar. Its settlement agreement with AbbVie provided six months of exclusive commercial presence before the July 2023 cohort — including Cyltezo, Hadlima, Yusimry, Hyrimoz, Idacio, Hulio, and Abrilada — could launch.
That six-month window was structurally valuable. Amjevita set the pricing template for the class: a dual-price strategy offering a 5% discount to list price for payers who continued taking AbbVie rebates, and a 55% discount for payers who were willing to forgo the rebate structure. This pricing architecture acknowledged the dominant commercial reality: AbbVie had pre-contracted massive rebates with PBMs and payers that made Humira’s effective net price substantially lower than its list price. A biosimilar at a 15–20% list price discount could be more expensive on a net-cost basis than Humira at a 40–50% rebated discount. The biosimilar first-mover problem, uniquely in the adalimumab market, was not clinical hesitancy — it was the rebate structure.
The result: despite a six-month exclusivity window, Amjevita held less than 1% of the U.S. adalimumab market by November 2023, ten months after launch. Humira maintained 99% market share through that period. The first-mover advantage, in this case, was structurally neutralized by the innovator’s contracting strategy, not by any failure of Amgen’s commercial execution.
The PBM Formulary Shift: How Adoption Actually Accelerated
Biosimilar adalimumab market share reached approximately 5% at the start of 2024 and then jumped to 36% within five days of CVS Caremark removing Humira from certain formulary positions in favor of Hyrimoz. That single formulary decision, driven by the PBM rather than by prescriber education or clinical outcomes data, produced a market share shift that twelve months of biosimilar commercial activity had failed to generate.
The competitive beneficiary was Sandoz’s Hyrimoz, not Amgen’s Amjevita — the company that had been first to market by six months. By mid-2024, Hyrimoz held approximately 13% of the U.S. adalimumab market, while the remaining nine biosimilars combined held less than 5%. Hyrimoz’s position was a product of Sandoz’s contracting and co-marketing strategy with Cordavis (a CVS Health subsidiary created specifically to market Hyrimoz), not of its temporal position in the market entry sequence.
By Q4 2024, total adalimumab biosimilar market share reached 22–23%, with Hyrimoz and Hadlima driving the majority of gains. Adalimumab biosimilars went from 2% market share in early 2024 to 22%, driven primarily by biosimilar uptake through private-label brands as payers and PBMs began prioritizing biosimilars over the reference product.
Amgen recorded a year-over-year 22% increase in Amjevita sales to $761 million for its first full U.S. commercial year in 2024, while Sandoz’s biosimilar portfolio reached $2.9 billion for 2024, with Hyrimoz contributing to a 30% increase in biosimilar portfolio sales.
The Rebate Wall Problem and Its Structural Causes
The Humira biosimilar adoption timeline illustrates what market analysts call the ‘rebate wall’ — the mechanism by which an innovator biologic’s contracted rebates with PBMs create a net-cost barrier to biosimilar adoption that is independent of list price. AbbVie reportedly offered PBMs rebates of 40–60% on Humira’s list price. A biosimilar priced at 20% below list, before any rebate, produces a higher net cost for the payer than the rebated Humira — a counterintuitive outcome that the rebate architecture produces deliberately.
Breaking through the rebate wall requires either a biosimilar discount steep enough to undercut the net rebated innovator price (85–86% WAC discounts, as seen with Hadlima, Yusimry, and Simlandi), or formulary decisions by PBMs to remove the reference product entirely and replace it with a biosimilar preferred tier. CVS Caremark’s 2024 formulary action achieved the latter. The rebate wall problem is not unique to adalimumab — it will recur for every major biologic biosimilar launch in a market where the innovator has had years to build PBM rebate contracts.
Key Takeaways for Part VI:
- Amjevita’s six-month first-mover window produced less than 1% market share before the rebate wall made biosimilar adoption financially irrational for most payers.
- The PBM formulary decision (CVS Caremark removing Humira) produced more market share movement in five days than twelve months of biosimilar commercial activity.
- The competitive winner in the adalimumab class was the company (Sandoz/Cordavis) best positioned in PBM contracting, not the one first to market.
- Biosimilar developers must model net-cost competition against innovator rebate structures, not gross list price discounts, in their market access planning.
Part VII: PBM Contracting and Formulary Architecture
PBM Contracting and Formulary Dynamics
The three largest PBMs by covered lives — CVS Caremark, Express Scripts (Evernorth), and OptumRx — collectively manage formulary access for well over 200 million Americans. Their formulary decisions, particularly their choices about preferred tier placement, prior authorization requirements, and step therapy protocols, are the single most powerful determinant of biosimilar adoption in the U.S. pharmacy benefit channel.
For the majority of self-injectable biologics dispensed through the pharmacy benefit, PBM formulary placement determines whether a biosimilar reaches the patient at all. A biosimilar on a non-preferred tier with a high patient cost-sharing requirement will see minimal uptake regardless of its clinical profile or its position in the market entry sequence. A biosimilar on the preferred tier with zero or low co-pay drives immediate switching.
Cyltezo, despite being the first interchangeable adalimumab biosimilar at launch, secured preferred formulary placement at OptumRx at launch on July 1, 2023 — a positioning that Amjevita, the market’s first entrant by six months, had not achieved. OptumRx covers more than 66 million patients. That formulary decision was worth more, commercially, than the interchangeability designation or the temporal first-mover position.
The mechanics of a biosimilar PBM contracting strategy require several elements: a competitive WAC (wholesale acquisition cost) discount, a rebate offer that is transparent and predictable (unlike the rebate maze that Humira’s contracting created), and in many cases a co-pay assistance program that eliminates patient cost-sharing friction. Companies that entered the adalimumab market with high WAC discounts (85–86% below Humira’s list price) were explicitly pricing to the net-cost level at which they could beat Humira’s rebated effective price without requiring the PBM to restructure its Humira contract.
Hospital P&T Committee Dynamics for IV-Administered Biologics
For biologics administered in outpatient infusion centers or hospital settings — infliximab, bevacizumab, trastuzumab — the formulary decision moves from the PBM to the hospital Pharmacy and Therapeutics (P&T) committee. P&T committees evaluate biosimilars on clinical evidence, cost-effectiveness, supply reliability, and operational factors such as drug information support and pharmacist training resources.
A biosimilar company seeking to be first-to-preferred in the hospital channel must engage P&T committees proactively before launch, provide comprehensive drug information dossiers, and offer contracting terms that reflect the hospital’s volume and formulary exclusivity value. Celltrion’s Inflectra (infliximab-dyyb), the first infliximab biosimilar in the U.S., built its hospital market position through this channel — earlier and more systematically than its competitors — and established institutional adoption that created switching costs for later entrants.
Investment Strategy Note: PBM and IDN contracting capability is now a core underwriting criterion for biosimilar program valuation. A development-stage company without an established PBM relationship or a commercial partner with one faces a structural market access disadvantage that no amount of clinical data superiority will overcome. Investors should assess the quality of the commercial infrastructure attached to any biosimilar program alongside the clinical and regulatory pathway.
Part VIII: Physician Adoption and Specialty-Specific Behavior
Physician Adoption: Specialty-Level Prescribing in the Adalimumab Market
Biosimilar prescribing behavior varies substantially by physician specialty, and the adalimumab data makes this concrete. Rheumatologists have leaned toward Hyrimoz, with approximately one-third of rheumatology adalimumab scripts going to Sandoz’s biosimilar, while dermatologists prefer Amjevita for psoriasis prescriptions, capturing about 25% of the market in that specialty. Gastroenterologists favor Amjevita with 26% of scripts, followed by unbranded adalimumab and Hyrimoz.
These specialty-specific preferences are not driven by clinical differentiation — all approved adalimumab biosimilars have demonstrated biosimilarity. They are driven by payer dynamics and specialty-specific familiarity, as BioSpace has reported. That distinction matters for commercial strategy: if specialist prescribing preferences are a product of formulary economics rather than clinical preference, they are malleable through contracting, not entrenched through efficacy.
The implication for biosimilar commercial teams is that specialty detailing and KOL engagement should be targeted and evidence-driven rather than broadcast. A rheumatology-specific medical education campaign that addresses immunogenicity concerns and provides real-world evidence from rheumatoid arthritis populations will produce better adoption than a general biosimilar education effort. Companies that invested in specialty-specific education early in the adalimumab launch cycle built stronger prescriber relationships that PBM formulary shifts subsequently translated into durable volume.
Overcoming Prescriber Inertia: The Role of Real-World Evidence
Physician inertia in switching from a known biologic to a biosimilar is real and quantifiable. The most effective tool for overcoming it is real-world evidence — pharmacovigilance data, electronic health record analyses, and registry studies that demonstrate equivalent outcomes across large, diverse patient populations in routine clinical practice.
A first-mover biosimilar has a temporal advantage in generating this evidence: it accumulates post-marketing data before competitors and can publish outcomes data that competitors cannot match. Samsung Bioepis has leveraged its quarterly U.S. biosimilar market reports to keep Hadlima in the clinical conversation despite not being first to market. Amgen’s real-world pharmacovigilance program for Amjevita — drawing on its Amgevita European experience dating to 2018 — provided a depth of safety data at U.S. launch that no competitor could match.
Immunogenicity: The Physician Concern That Matters Most
The immunogenicity question — whether the body develops neutralizing antibodies to a biosimilar, potentially reducing efficacy or causing adverse events — remains the primary clinical concern driving physician hesitancy. It is also, in the context of approved biosimilars, a concern that the regulatory data package has already addressed: FDA approval requires demonstration of a comparable immunogenicity profile to the reference product.
The physician education task is not to prove that the biosimilar is safe on immunogenicity, but to communicate that the regulatory approval process already required that proof. That educational gap is the one that first movers have the greatest opportunity to close, and the one that benefits most from early, sustained investment in specialist-targeted medical education.
Part IX: Manufacturing as Competitive Moat
Manufacturing Quality as a Market Entry Asset
Biosimilar manufacturing is technically demanding in ways that have no direct analog in small-molecule generics. The active molecule is produced in living cell systems — Chinese hamster ovary cells, yeast, or bacterial expression systems — whose output is inherently variable. Post-translational modifications, including glycosylation patterns, affect the drug’s potency and immunogenicity profile. A biosimilar’s analytical similarity package must demonstrate that its molecular structure, including these post-translational modifications, falls within the comparability range established for the reference product.
Manufacturing quality problems have derailed biosimilar programs at the FDA review stage with consequences for market entry timing. Alvotech’s high-concentration adalimumab biosimilar AVT02 received two complete response letters (CRLs) related to manufacturing facility deficiencies during FDA inspection, delaying its approval by over a year. That delay had direct commercial consequences: AVT02 launched after the July 2023 cohort, entering a market in which ten competitors were already competing for payer contracts.
For biosimilar developers, manufacturing facility quality is therefore a market entry timeline asset, not just a compliance requirement. A company with a manufacturing site that has a strong FDA inspection history and robust change control processes can commit to launch dates with confidence. A company with unresolved facility deficiencies cannot. The difference in launch timing can determine whether a program enters a relatively open market or a saturated one.
Supply Chain Reliability as a Formulary Selection Criterion
P&T committees and PBMs explicitly evaluate supply reliability as a formulary selection criterion, particularly for biologics where treatment discontinuity creates clinical risk. A biosimilar company that has demonstrated consistent supply at commercial scale, without shortages or lot failures, has a formulary positioning advantage over a competitor whose manufacturing reliability is less established.
This is not theoretical. Several early European biosimilar launches were undermined by supply disruptions that led hospital systems to revert to the reference product. The reputational cost of a supply failure in the first year of commercial launch can persist for the product’s lifetime. Biosimilar developers should plan manufacturing scale-up to commercial demand well before launch, not in parallel with it.
Part X: Real-World Evidence and Post-Launch IP Value
Real-World Evidence and Post-Launch IP Strategy
Real-world evidence (RWE) — generated from electronic health records, insurance claims databases, and patient registries rather than randomized controlled trials — has become a standard component of biosimilar lifecycle management. Its commercial value has two dimensions: it builds prescriber confidence by demonstrating outcomes in diverse populations, and it supports label expansion applications by providing evidence of effectiveness in patient subgroups not fully represented in the pivotal trials.
For first-mover biosimilars, RWE generation is both an opportunity and a differentiator. A company that launches January 2023 and publishes a 12-month real-world pharmacovigilance analysis in Q1 2024 has data that no competitor, regardless of development quality, can match. That temporal advantage in evidence accumulation is the one dimension of first-mover advantage that cannot be neutralized by contracting strategy or formulary decisions.
The commercial monetization of RWE operates through payer value dossiers and medical literature. Payers increasingly require RWE as a component of formulary renewal discussions — demonstrating not just that the biosimilar is approved, but that its real-world performance matches the clinical trial data. A biosimilar with two years of RWE at formulary renewal time is in a stronger negotiating position than a competitor with only approval data.
Post-Launch Indication Expansion and Its IP Implications
Biosimilars are approved for the same indications as the reference product, either automatically (extrapolation) or through specific clinical evidence. In the U.S., the FDA permits extrapolation of biosimilarity data across indications if the mechanism of action is the same and the clinical findings support it. Most adalimumab biosimilars received approval across all of Humira’s labeled indications through extrapolation.
However, the innovator may hold method-of-use patents on specific indications that extend beyond the primary composition patent. If a method-of-use patent on a particular indication is not yet expired or successfully challenged, a biosimilar may be at risk for infringement if it promotes that indication, even if the molecule is approved for it. This creates a carve-out labeling strategy in which the biosimilar’s label omits the indication protected by a valid method-of-use patent.
Biosimilar developers must audit each indication in the reference product’s label against the innovator’s method-of-use patent estate. Indications with unexpired patent protection require either carve-out labeling or a separate litigation strategy to clear the patent before promotion. DrugPatentWatch’s indication-level patent mapping allows development teams to conduct this analysis systematically before aBLA submission, rather than discovering exposure at the litigation stage.
Part XI: Emerging Targets and Entry Window Analysis
Emerging Biosimilar Targets and Entry Window Analysis
The next wave of major biosimilar launches will center on several blockbuster biologics whose primary patents are approaching or have recently expired. The analytical framework is: primary composition patent expiry minus realistic patent thicket litigation duration minus manufacturing development and regulatory review timeline equals the practical entry window, which may be years narrower than the nominal patent expiry date suggests.
Ustekinumab (AbbVie/J&J’s Stelara) represents one of the highest-value targets, with its U.S. composition patent expiring in September 2023 and biosimilar launches beginning in early 2025. The ustekinumab patent thicket is materially thinner than Humira’s; AbbVie did not have ten years to build secondary patent layers for a drug it licensed from J&J. The class already has multiple FDA-approved biosimilars, and the PBM formulary shift dynamics observed in adalimumab are already visible in ustekinumab contracting discussions.
Dupilumab (Sanofi/Regeneron’s Dupixent) sits at the frontier of the next major biosimilar opportunity. The primary composition patent extends to approximately 2031, but the commercial scale of the asset — projected to reach $20+ billion in annual sales — makes it an attractive development target despite the timeline. Biosimilar developers who begin analytical development and cell line work now will be positioned to file aBLAs shortly after patent expiry, while those who wait will face a crowded field.
Pembrolizumab (Merck’s Keytruda) is the most discussed future biosimilar target given its status as the world’s top-selling drug. The composition patent expires in the early 2030s depending on jurisdiction. The complexity of the reference product — an IgG4 monoclonal antibody with a specific PD-1 binding profile — means that analytical similarity demonstration will be technically demanding. The indication breadth (dozens of approved cancer indications) creates both an opportunity and a method-of-use patent risk landscape that requires careful mapping.
The global biosimilar market reached $30.3 billion in 2024, growing at a 14% CAGR, with adalimumab, infliximab, and bevacizumab together capturing 45% of the market. The FDA approved 18 biosimilars in 2024 and the EMA approved a record 28 — a regulatory pipeline that signals accelerating competition across reference products, not just the blockbuster molecules.
Technology Roadmap: Next-Generation Biosimilar Development
The next generation of biosimilar programs will not simply replicate existing development approaches. Several technical advances are changing both the development cost structure and the competitive differentiation opportunities.
Cell line engineering has advanced substantially. CRISPR-based genome editing allows for more precise glycosylation control in CHO cell lines, reducing batch-to-batch variability and improving the precision of the analytical similarity package. This tightens the comparability range and reduces the risk of analytical similarity failures during FDA review.
Continuous bioprocessing is moving from development into commercial manufacturing at several large CDMOs. Unlike traditional batch processing, continuous manufacturing produces a steady output from a single production run, reducing cycle time, batch failure risk, and capital footprint. A biosimilar developer that operates a continuous manufacturing platform can reduce cost of goods by 20–40% relative to batch competitors, creating pricing flexibility that is directly relevant to the WAC discount strategies needed to break through rebate walls.
Analytical characterization technology has improved to the point where some developers are building what they call ‘totality of evidence’ packages that go beyond the minimum regulatory requirement — providing a comprehensive multi-attribute monitoring dataset that demonstrates not just biosimilarity but structural identity at a resolution the reference product sponsor’s own characterization may not match. This approach has been used to pre-empt innovator arguments about analytical differences during BPCIA patent dance exchanges.
Subcutaneous formulation development for biologics traditionally delivered intravenously is creating a new category of product differentiation. A biosimilar that can be administered subcutaneously in a setting where the reference product requires IV infusion offers a genuine clinical convenience advantage — one that physicians and patients can observe directly, independent of any analytical similarity argument. This formulation differentiation sits outside the strict definition of biosimilarity but can support a competitive moat in certain reference product classes.
Key Takeaways for Part XI:
- Ustekinumab represents the near-term high-value biosimilar opportunity with a thinner patent thicket than Humira.
- Dupilumab and pembrolizumab are longer-horizon targets where development investment now positions companies for early entry at patent expiry.
- Continuous manufacturing offers a 20–40% COGS advantage that translates directly into WAC discount headroom.
- Subcutaneous reformulation of IV-administered biologics creates a clinical convenience differentiator that complements the biosimilarity argument.
Part XII: Investment Strategy for Biosimilar Portfolio Managers
Investment Strategy: Framework for Biosimilar Portfolio Evaluation
For institutional investors evaluating biosimilar programs or companies, the analytical framework requires a different set of inputs than standard pharmaceutical company analysis. The key variables are: patent estate clearance probability, regulatory pathway risk, manufacturing platform quality, PBM contracting capability, and the competitive cohort size at expected launch.
Patent Estate Clearance Probability is the most specialized input. It requires analysis of the innovator’s patent estate beyond the primary composition patent — formulation patents, manufacturing patents, method-of-use patents, and continuation filings. Companies with in-house IP analytics or access to patent intelligence platforms that track the full estate, litigation status, and terminal disclaimer linkages are better positioned to estimate this probability than those relying on publicly available summary data.
Regulatory Pathway Risk includes both the FDA’s scientific review of the analytical similarity package and the manufacturing inspection outcome. Programs with complete response letter history (as Alvotech experienced with its adalimumab program) represent delayed-but-not-dead scenarios. The key analytical question is whether the CRL reflected addressable manufacturing deficiencies or fundamental analytical similarity gaps. The former is resolvable; the latter may require a reformulated development strategy.
Manufacturing Platform Quality is assessed through the contract development and manufacturing organization (CDMO) relationship, facility inspection history, and the platform’s track record across multiple reference products. A development company without its own manufacturing capability is dependent on its CDMO partner’s inspection standing — a dependency that should be reflected in the risk-adjusted valuation.
PBM Contracting Capability is either a first-party asset (the company has its own PBM relationship and contracting team) or a partnership asset (the company has partnered with a commercial organization that has the relationship). The adalimumab market provides a clear case study: Sandoz’s Hyrimoz became the market leader not through temporal priority or interchangeability status but through its Cordavis relationship with CVS Health. Investors should evaluate commercial partnership quality as rigorously as clinical program quality.
Competitive Cohort Size at Expected Launch determines the pricing and contracting environment into which a biosimilar enters. A program expected to launch with fewer than three competitors has meaningfully different economics than one that enters a 10-competitor market, even if the molecule is the same. The adalimumab market, with ten biosimilars, has produced 85–86% WAC discounts at the low end of pricing — margin structures that are viable only for large-volume manufacturers with low COGS.
Valuation Multiples for Biosimilar Programs: Biosimilar programs are typically valued on a risk-adjusted net present value (rNPV) basis, discounting projected net revenues by the probability of patent clearance, regulatory approval, and commercial success. Discount rates for biosimilar programs should be higher than for branded pharmaceutical programs due to the combinatorial risk stack — patent litigation, manufacturing, regulatory review, and market access each carry independent probability of failure or delay. Programs in the 351(k) pathway with filed aBLAs and clean manufacturing inspection histories trade at materially lower risk premiums than pre-filing programs.
Part XIII: Comprehensive Key Takeaways by Segment
Key Takeaways: The Patent and IP Dimension
The biologic patent thicket is the primary constraint on biosimilar market entry timing. Primary composition patent expiry does not equal market entry opportunity. The BPCIA’s absence of a patent cap allows reference product sponsors to construct litigation-coercive patent volumes that drive settlement-based entry dates years after composition patent expiry. Patent estate analysis — across formulation, manufacturing, method-of-use, and continuation layers — is a prerequisite for credible market entry modeling, not an optional input. AbbVie’s Humira strategy, which preserved an estimated $60–75 billion in U.S. revenue through secondary patent enforcement, is the benchmark against which all biologic IP defense strategies are now measured. For biosimilar developers, the settlement market entry date is the commercially operative first-mover metric, not the aBLA filing date or FDA approval date.
Key Takeaways: Regulatory and Interchangeability Strategy
Interchangeability designation confers auto-substitution rights at the pharmacy level and carries a first-interchangeable exclusivity period that bars competitors from receiving the designation for a defined window. The switching study investment is material (typically a dedicated Phase III RCT) and the commercial ROI depends on capturing the exclusivity window before competitors close the designation gap. The adalimumab market demonstrates that interchangeability is necessary but not sufficient for market leadership: Cyltezo held interchangeability from July 2023, but Hyrimoz became the market share leader through PBM contracting, not regulatory status. The EMA’s lack of an interchangeability framework means the designation’s commercial value is geographically specific to the U.S. and markets with similar pharmacy substitution frameworks.
Key Takeaways: Commercial Strategy and Market Access
PBM formulary decisions drive more biosimilar market share movement than any other single variable in the U.S. pharmacy benefit channel. The rebate wall — the mechanism by which innovator rebates to PBMs make the net cost of the reference product lower than a nominally discounted biosimilar — can suppress biosimilar adoption to near-zero for years after regulatory approval. Breaking through the rebate wall requires either extreme WAC discounts (85–86% below list) or exclusive formulary positioning by the PBM. Commercial partnership quality (Sandoz/Cordavis with CVS Health) is a stronger market access driver than temporal priority or regulatory designation alone. Hospital P&T committee adoption for IV-administered biologics requires proactive engagement, supply reliability evidence, and comprehensive drug information support.
Key Takeaways: Manufacturing and Supply Chain
Manufacturing quality directly affects launch timing through FDA inspection outcomes. A complete response letter related to manufacturing deficiencies delays launch into a more competitive market cohort — a compounding disadvantage. Supply chain reliability is a formulary selection criterion, not just a compliance matter. Continuous manufacturing platforms offer COGS advantages that translate into WAC discount headroom, directly relevant to the economics of breaking through rebate walls. Biosimilar developers without their own manufacturing capability carry a dependency risk on their CDMO partner’s inspection standing that should be reflected in program risk assessments.
Key Takeaways: Real-World Evidence and Lifecycle Management
RWE generation is the one dimension of temporal first-mover advantage that compounds over time rather than eroding. A first-to-launch biosimilar that systematically generates real-world pharmacovigilance data builds an evidence asset that competitors cannot replicate through contracting or pricing. Post-launch immunogenicity surveillance data is specifically valuable for overcoming physician inertia in specialties with high clinical risk aversion (oncology, transplant medicine). Indication-level method-of-use patent analysis is required before commercial promotion of any indication in the reference product’s label. Subcutaneous formulation development for traditionally IV-administered biologics creates a genuine clinical differentiation opportunity that operates outside the strict biosimilarity definition.
Appendix: Glossary of Key Terms
aBLA (abbreviated Biologics License Application): The regulatory submission used by biosimilar developers under the BPCIA 351(k) pathway.
BPCIA (Biologics Price Competition and Innovation Act, 2009): The U.S. law establishing the biosimilar approval pathway and the associated patent dance litigation framework.
Biosimilarity: The FDA standard requiring that a biosimilar have no clinically meaningful differences from its reference product in safety, purity, and potency.
Continuation Patent: A patent application that claims priority to an earlier parent application, using the parent’s filing date, while claiming narrower or more specific subject matter. Used to extend patent family coverage through multiple filing cycles.
Evergreening: The practice of filing secondary and continuation patents on formulations, manufacturing processes, methods of use, and delivery devices to extend effective market exclusivity beyond composition patent expiry.
Interchangeability: The FDA designation for a biosimilar that has demonstrated, through a switching study, that alternating between the reference product and the biosimilar produces no additional risk. Allows pharmacy-level auto-substitution in states that permit it.
P&T Committee (Pharmacy and Therapeutics Committee): The institutional body within a hospital or health system responsible for formulary management and drug utilization decisions.
Paragraph IV Filing: The small-molecule generic drug equivalent of the biosimilar’s BPCIA challenge; a Paragraph IV certification asserts that a listed patent is invalid or will not be infringed.
Patent Dance: The BPCIA’s pre-litigation information exchange process between a biosimilar applicant and the reference product sponsor.
Patent Thicket: A dense network of overlapping patents covering multiple aspects of a reference product, designed to create litigation volume that is economically coercive for biosimilar developers.
PBM (Pharmacy Benefit Manager): An intermediary that manages prescription drug benefits for health plans, negotiating rebates with manufacturers and determining formulary placement.
RWE (Real-World Evidence): Clinical evidence generated from sources outside randomized controlled trials, including EHRs, claims data, and patient registries.
Terminal Disclaimer: A legal instrument filed with the USPTO in which a patent applicant disclaims any portion of the patent term that would extend beyond the term of a related patent, used to overcome obviousness-type double patenting rejections in continuation patent filings.
WAC (Wholesale Acquisition Cost): The manufacturer’s published list price for a drug before rebates, discounts, and other price concessions.
This analysis draws on public regulatory filings, published clinical trial data, commercial market reports from IQVIA, Samsung Bioepis, Alira Health, and Vizient, peer-reviewed literature from PMC and AJMC, and patent data from public USPTO records. Patent intelligence cited in the context of DrugPatentWatch capabilities reflects the analytical categories tracked by that platform.