Executive Summary

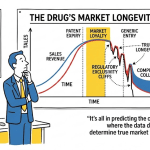
The pharmaceutical industry’s revenue engine runs on a single legal mechanism: the patent. Strip away the marketing language about pipelines and innovation platforms, and what you have is a business that sells a commodity molecule at a monopoly price for a finite period, then watches that price collapse by 80 to 90 percent within twelve months of generic entry. Every strategic decision the industry makes, from discovery spend to acquisition multiples to pipeline sequencing, traces back to that expiration date.
Between 2025 and 2030, the global industry faces the steepest patent cliff in its history. Somewhere between $200 billion and $400 billion in branded drug revenue sits in the crosshairs as statutory monopolies expire on a cohort of blockbusters that includes Merck’s pembrolizumab (Keytruda), Bristol Myers Squibb’s apixaban (Eliquis), Johnson & Johnson’s ustekinumab (Stelara), and Regeneron’s aflibercept (Eylea). These are not marginal assets. Keytruda alone generated $29.5 billion in 2024, making its 2028 loss of exclusivity (LOE) the largest single revenue-erosion event in the history of the pharmaceutical industry.
The “date on the patent” is almost never the operative date. The real number, the one that determines when a generic manufacturer can walk product onto pharmacy shelves, is the result of compounding variables: Patent Term Extensions (PTEs) granted under 35 U.S.C. Section 156, regulatory exclusivities granted by the FDA under the Federal Food, Drug, and Cosmetic Act, Pediatric exclusivity add-ons under PREA/BPCA, litigation outcomes under Hatch-Waxman’s 30-month stay provision, and the settlement terms of any Paragraph IV challenges.
Since 2022, a fifth variable has entered the calculation: the Inflation Reduction Act (IRA). For small-molecule drugs, Medicare price negotiation eligibility arrives just nine years after approval. That date now functions as a de facto secondary LOE, compressing the commercially viable period of a drug’s life regardless of what the USPTO certificate says.
This guide provides a granular technical analysis of all these variables, structured for pharma IP counsel, business development teams, and institutional investors who need to do more than read a headline. It does not summarize. It maps the mechanism.
Part I: The 20-Year Illusion: Statutory vs. Effective Patent Life
The Basic Arithmetic of Attrition
A U.S. utility patent has a statutory term of 20 years from the earliest effective filing date. For pharmaceutical compounds, that term begins during early discovery, often years before anyone has dosed a human. From that filing date, the drug must travel through preclinical toxicology (four to seven years), Phase I through Phase III clinical trials (six to eight years), and FDA review of the New Drug Application or Biologics License Application (six months to two years). The math is ruthless.
By the time FDA approval arrives, a molecule that filed its first patent application at year zero has consumed 10 to 15 years of its 20-year term. The “effective patent life,” meaning the period during which the drug can be sold at a monopoly price under patent protection, runs to somewhere between five and ten years in many cases, though it varies widely by therapeutic area and development timeline. Oncology drugs, which often qualify for Priority Review and Breakthrough Therapy designation, can exit clinical development faster; complex biologics targeting rare diseases sometimes take longer. The averages disguise enormous variance.
The structural consequence of this attrition is well-understood but worth stating plainly: it compresses the window during which a company must recoup sunk R&D costs that, according to the Tufts Center for the Study of Drug Development, now average over $2.6 billion per approved drug when accounting for the cost of failures. That number has no intellectual honesty unless paired with the effective years of exclusivity available to monetize it.
How the IP Portfolio Gets Filed: The Discovery-to-Filing Sequence
The filing sequence matters for anyone doing IP valuation, because it determines not just expiration dates but patent layering, the strategic architecture that allows lifecycle management to work.
The first patent filed is almost always a composition-of-matter (COM) patent. It covers the molecule itself, the active pharmaceutical ingredient (API), its salts, its enantiomers, and sometimes a genus of structurally related analogs. This is the strongest patent, the one generics most want to challenge, and the one that expires first in the absence of a Patent Term Extension. Its filing date precedes human trials.
As the molecule advances into clinical development, a second wave of patents covers formulation: specific dosage forms, excipient combinations, particle sizes, crystalline polymorphs, and drug delivery mechanisms. These are filed when the final commercial formulation is locked in, typically during Phase II or early Phase III. Their filing dates are later, meaning their 20-year terms extend further.
A third wave covers manufacturing processes, particularly for biologics where the production process is tightly coupled to the product’s identity. A fourth wave covers methods of use, claims that the molecule treats a specific disease at a specific dose by a specific route. Each new indication produces a fresh method-of-use filing with a later expiration date.
This sequential filing architecture is not incidental. It is the deliberate engineering of a patent portfolio designed so that even as the earliest COM patent expires, subsequent layers maintain Orange Book listings and sustain infringement claims against Paragraph IV challengers.
Patent Term Extension (PTE) Mechanics: The 35 U.S.C. Section 156 Calculus
Congress codified the basic PTE mechanism in the Drug Price Competition and Patent Term Restoration Act of 1984, the Hatch-Waxman Act. Under 35 U.S.C. Section 156, a drug sponsor may apply to the USPTO for an extension of a single patent per product, calculated as:
Full clinical testing period x 0.5, plus the full regulatory review period.
Two hard statutory caps apply. First, the extension cannot exceed five years. Second, the remaining term of the patent after extension (the period from FDA approval to patent expiration) cannot exceed 14 years. The five-year cap and the 14-year cap interact to produce a range of outcomes depending on development timeline, and the arithmetic of this interaction is a discrete analytical skill that IP teams need to perform correctly before a drug launches.
Consider the financial consequence of an error. A drug generating $8 billion annually that qualifies for a full 24-month PTE but receives only 18 months due to a calculation error loses roughly $4 billion in protected revenue. PTE applications have time limits, require precise records of regulatory review periods, and can be challenged by generic manufacturers. The USPTO’s published PTE records show a non-trivial rate of disputed applications, particularly where the clinical testing period is ambiguous or where multiple regulatory submissions are involved.
The PTE is available only for the first commercial marketing of the active ingredient. A drug that has been previously approved, even for a different indication in a different patient population, does not qualify. New combination products may qualify if the combination itself has not been marketed before. These distinctions require careful analysis during due diligence.
Key Takeaways: Statutory vs. Effective Patent Life
The 20-year statutory term is a ceiling, not a guarantee. Effective patent life typically runs five to ten years after drug approval. PTEs under Section 156 can restore up to five years of lost time, subject to the 14-year total remaining term cap. The entire value of a PTE for a $5 billion-a-year product approaches $25 billion at peak sales rates, making calculation accuracy a financial-critical function. The sequential layering of COM, formulation, manufacturing, and method-of-use patents is what enables lifecycle management strategies to function; understanding the filing dates and expiration dates of each layer is the starting point for any competitive intelligence analysis.
Part II: The Regulatory Fortress: FDA Exclusivity Architecture
Patents vs. Regulatory Exclusivity: Two Separate Systems
Patents and FDA regulatory exclusivity are distinct mechanisms that operate on different legal bases, administered by different agencies, and breachable by different means. Patents are property rights granted by the USPTO; they can be challenged through inter partes review (IPR) at the Patent Trial and Appeal Board (PTAB), through Paragraph IV certifications at district court, or through reexamination. They can be invalidated.
Regulatory exclusivity is a statutory right granted by the FDA as a policy incentive for specific types of drug development. It cannot be invalidated by a court ruling on patent validity. If a drug has five-year New Chemical Entity (NCE) exclusivity, the FDA cannot physically accept an Abbreviated New Drug Application (ANDA) for a generic version until four years have elapsed (or five years if no Paragraph IV challenge is filed), regardless of what happens to the patents. This distinction matters enormously for forecasting actual generic entry dates.
The two systems often run in parallel, and the operative constraint on generic entry is whichever one expires later. In some cases, notably for older drugs that lost their patents years ago but still hold orphan drug exclusivity for a narrow indication, regulatory exclusivity is the only barrier remaining.
New Chemical Entity (NCE) Exclusivity: The Five-Year Fortress
NCE exclusivity attaches to drugs containing an active moiety never before approved by the FDA. ‘Active moiety’ is defined as the molecule or ion responsible for the drug’s physiological action. Salt forms, esters, and chelates of a previously approved moiety do not qualify; the active moiety itself must be novel. This exclusivity blocks FDA acceptance of any ANDA or 505(b)(2) application for four years (creating the window for Paragraph IV challenges) and blocks FDA approval for five full years.
For drug valuation purposes, NCE exclusivity functions as a floor on market exclusivity. Even if the COM patent is challenged and invalidated on day one of approval, NCE exclusivity provides five years of protection. The practical value of this floor depends on whether the effective patent life, after PTE, extends beyond five years. For drugs with unusually long development timelines, NCE exclusivity can actually be the binding constraint, outlasting even the PTE-extended patent.
Orphan Drug Exclusivity (ODE): The Seven-Year Monopoly
The Orphan Drug Act grants seven years of market exclusivity to drugs treating rare diseases, defined as conditions affecting fewer than 200,000 patients in the United States. During this period, the FDA cannot approve the same drug for the same orphan indication. ODE is narrowly scoped: it blocks the same drug, not structurally distinct drugs that happen to treat the same condition.
The commercial value of ODE depends heavily on the therapeutic area and pricing environment. For ultra-orphan drugs at prices of $300,000 to $500,000 per patient year, seven years of exclusivity on a 3,000-patient market can generate more than $1 billion in cumulative revenue. For drugs in moderately rare conditions with competitive pressure from structurally distinct molecules, the practical barrier may be weaker than the statutory term suggests.
ODE stacks with patent protection but also with NCE exclusivity and pediatric exclusivity add-ons. The interaction of multiple exclusivity types creates compound barriers to entry that can push the effective generic entry date years beyond what any single exclusivity term would suggest.
New Clinical Investigation (NCI) Exclusivity: The Three-Year Line Extension Tool
NCI exclusivity, sometimes called ‘clinical investigation exclusivity,’ attaches to approved changes to previously approved drugs when those changes required new clinical investigations essential to approval. New indications, new dosage forms, new formulations, and new patient populations can each qualify. The exclusivity lasts three years and applies specifically to the approved change, not to the drug as a whole.
The practical mechanism matters: NCI exclusivity does not block generic entry for the previously approved uses of the drug. It forces the generic to file an ANDA with a ‘carved-out’ label that omits the newly protected indication. This skinny label construct, which is discussed in the lifecycle management section, has generated significant litigation about whether a generic bearing a skinny label can be held liable for inducing infringement of the protected use in real-world prescribing environments.
For lifecycle management purposes, NCI exclusivity is the mechanism that gives commercial value to indication expansion programs. A drug with a core oncology indication that obtains approval for a cardiovascular use gains three years of exclusivity for that cardiovascular indication, during which time sales in that indication contribute to total revenue without generic competition. Stacking multiple NCI exclusivities through sequential indication expansions is a core component of the product life-cycle roadmaps that mature brands execute.
Biologic Exclusivity Under the BPCIA: The 12-Year Standard
Under the Biologics Price Competition and Innovation Act (BPCIA), reference biological products receive 12 years of exclusivity from approval, during which biosimilar applications cannot receive FDA approval. An additional four-year window at the front prevents the FDA from even accepting a biosimilar application. This 12-year standard was a legislative compromise; the branded industry sought 14 years, and biosimilar advocates pushed for seven.
The commercial rationale for longer biologic exclusivity reflects the genuine complexity of biologic manufacturing. Unlike small-molecule synthesis, which produces a chemically identical product regardless of manufacturer, biologic production involves living cell lines, fermentation conditions, and purification steps that make absolute structural identity impossible. The FDA defines biosimilar interchangeability as requiring a higher standard than mere similarity: an interchangeable biosimilar must produce the same clinical result as the reference product in any given patient, and for products administered more than once, the risk of switching must be no greater than continuing on the reference product.
This distinction between ‘biosimilar’ and ‘interchangeable biosimilar’ has direct commercial implications. Interchangeable biosimilars can be substituted at the pharmacy level without physician intervention, in states that permit automatic substitution. Non-interchangeable biosimilars require an explicit prescriber switch. The FDA approved its first interchangeable biosimilar, Cyltezo (adalimumab-adbm), in July 2021, and the category has grown since but remains operationally more difficult to achieve than basic biosimilar approval.
Pediatric Exclusivity: The Six-Month Add-On
Pediatric exclusivity is not a standalone exclusivity period. It is an add-on that attaches to existing protections, extending all existing patents and regulatory exclusivities by six months. The mechanism: if the FDA issues a Written Request for pediatric studies of a drug and the sponsor completes those studies (regardless of outcome), six months attach to every existing patent and exclusivity.
For a drug with a late-expiring formulation patent and NCE exclusivity both expiring in December of a given year, pediatric exclusivity moves both expiration dates to June of the following year. The value is precisely calculable: six months of net revenues from the drug in question, minus the cost of the pediatric trial program, which typically runs $20 million to $100 million depending on therapeutic area and patient population. For any drug generating more than $500 million annually, the pediatric exclusivity calculation is almost always positive.
QIDP Designation: The Antibiotic Premium
The Generating Antibiotic Incentives Now (GAIN) Act created the Qualified Infectious Disease Product (QIDP) designation for antibiotics and antifungals that target serious or life-threatening infections. QIDP adds five years to existing NCE exclusivity, NCI exclusivity, or other applicable exclusivity periods. Combined with NCE exclusivity, QIDP can provide 10 years of exclusivity for a first-in-class antibiotic, a critically important incentive for an antibiotic pipeline that has been commercially unviable for decades without such policy support.
Key Takeaways: Regulatory Exclusivity
Regulatory exclusivity is separate from, and sometimes more durable than, patent protection. NCE exclusivity provides a five-year floor regardless of patent outcomes. ODE’s seven-year term can exceed effective patent life for orphan drugs. NCI exclusivity is the mechanism that makes indication expansion commercially valuable. Biologic exclusivity at 12 years reflects the structural complexity of large-molecule manufacturing and the higher development cost of biologics. Pediatric exclusivity’s six-month add-on produces a positive ROI for essentially any drug generating above $200 million annually. The IRA’s Medicare negotiation timeline interacts with exclusivity periods in ways that are just beginning to affect corporate decision-making.
Part III: Small Molecules – The Hatch-Waxman Litigation Engine
The Orange Book: Public Notice as Legal Architecture
The Orange Book, formally ‘Approved Drug Products with Therapeutic Equivalence Evaluations,’ is the FDA publication that lists all patents a drug company certifies as covering an approved drug. Under Hatch-Waxman, brand companies are required to list qualifying patents within 30 days of patent issuance or drug approval, whichever is later. Generic manufacturers must engage with every listed patent before they can receive approval for a competing product.
The Orange Book serves as public notice and as litigation choreography. It defines the battlefield. Every patent listed in the Orange Book must receive a certification from a generic applicant: Paragraph I (patent expired), Paragraph II (patent invalid), Paragraph III (applicant agrees to wait for patent expiration), or Paragraph IV (patent invalid or not infringed). Most commercially significant generic challenges use Paragraph IV.
The FTC has scrutinized Orange Book listings for years, particularly for device patents on inhalers and auto-injectors. In 2023 and 2024, the FTC sent letters to drug manufacturers challenging dozens of Orange Book listings as potentially improper, arguing that device patents that do not ‘claim’ the drug itself are ineligible for listing. If the courts adopt the FTC’s reading broadly, it would meaningfully shorten the effective exclusivity of many inhalation and injectable drug products by removing patents that currently support 30-month stays.
The Paragraph IV Filing: Economics and Mechanics
When a generic manufacturer files a Paragraph IV certification, it must notify the patent holder and NDA holder within 20 days. The innovator then has 45 days to file an infringement suit. If it does, the FDA is automatically barred from approving the generic for 30 months from the date of notification, unless the court rules before that period ends. This automatic 30-month stay is the single most powerful tool in the branded company’s arsenal for managing generic entry timing. It provides approximately 2.5 years of additional exclusivity with no judicial proceeding required.
The economics on the generic side are structured to incentivize early challenges. The first applicant to file a substantially complete ANDA with a Paragraph IV certification, the ‘First-to-File’ filer, receives 180 days of generic market exclusivity. During that window, no other generic can launch. On a drug generating $3 billion annually, the 180-day exclusivity for the first-to-file generic can translate to revenues of several hundred million dollars, depending on the discount to brand price and the market penetration rate. That prize creates enormous pressure to file early and litigate aggressively.
Studies of Paragraph IV outcomes consistently show that generic challengers succeed in invalidating or designing around patents roughly 70 to 80 percent of the time when cases go to final judgment. The branded company wins more often at the preliminary injunction stage, where the standard is likelihood of success on the merits, but final validity rulings favor challengers. Many cases settle before final judgment through authorized generic agreements, pay-for-delay arrangements (now subject to antitrust scrutiny after FTC v. Actavis), or entry date agreements.
Authorized Generics and the 180-Day Calculus
An authorized generic (AG) is a version of the branded drug that the innovator itself licenses to a generic manufacturer, or sells under its own name at generic prices, during the 180-day exclusivity window. The AG strategy allows the innovator to capture some of the generic revenue during the exclusivity period and simultaneously splits market share with the first-to-file generic, reducing the value of the 180-day period to the challenger.
The AG strategy is controversial. Generic industry groups argue it devalues the 180-day exclusivity reward and therefore weakens the incentive to challenge weak patents. The FTC has studied the issue; some legislative proposals would bar AGs during the 180-day period. For now, AGs remain a standard tool in the branded company’s LOE defense playbook.
Pfizer deployed the AG strategy aggressively after Lipitor lost exclusivity in November 2011. It supplied Watson Pharmaceuticals with an authorized generic version during the 180-day period, splitting the market and capping Ranbaxy’s (the first-to-file generic) share at levels below what an exclusive 180-day window would have produced. Ranbaxy’s Lipitor AG revenues were substantially lower than initial projections precisely because of Pfizer’s AG move.
The 30-Month Stay: Strategic Use and Limitations
The 30-month stay does not attach to every listed patent. It attaches once per NDA for the first Paragraph IV challenge. A generic manufacturer filing Paragraph IV certifications against multiple listed patents in the same ANDA does not generate multiple stays; the 30 months runs from the first notification. If a second ANDA for the same drug with new Paragraph IV certifications is filed by the same or a different generic after the original stay has expired, no new stay attaches.
Brand companies have attempted to extend stay protection by listing new patents after the original ANDA is filed and then suing on those new listings. Courts have been skeptical, and some circuits have held that late-listed patents do not generate new stays when the generic application was already pending at listing. The operational takeaway: the timing of patent prosecution relative to the first ANDA filing date determines the scope of available stay protection.
Key Takeaways: Hatch-Waxman and Small Molecules
The Paragraph IV filing rate is the single most predictive variable for generic entry timing. The 30-month stay provides roughly 2.5 years of post-challenge exclusivity for branded drugs if the innovator sues promptly. Generic challengers win on validity roughly 70 to 80 percent of the time at final judgment. Authorized generics compress the value of the 180-day exclusivity but capture revenue for the innovator. FTC scrutiny of Orange Book listings for device patents could shorten the effective exclusivity of hundreds of inhaler and injectable products if courts adopt a narrow reading of patent listing eligibility.
Part IV: Biologics – The BPCIA, the Patent Dance, and Biosimilar Interchangeability
Why Biologics Are Different: The Manufacturing Identity Problem
Small molecules are defined by their chemical structure. A molecule of atorvastatin, made in any facility using the appropriate synthesis pathway, is chemically identical to every other molecule of atorvastatin. Generic manufacturers can demonstrate bioequivalence with a relatively standardized pharmacokinetic study in healthy volunteers, and the FDA can rely on the innovator’s clinical data for safety and efficacy.
Biologics do not work this way. A monoclonal antibody like adalimumab (Humira) is a protein approximately 150,000 daltons in molecular weight, produced in CHO (Chinese hamster ovary) cells through a fermentation process. The protein’s three-dimensional structure, its glycosylation pattern (the sugar modifications attached to specific amino acid residues), and its aggregation state are all functions of the exact cell line, culture conditions, and purification sequence used. Two different manufacturers using the same DNA sequence will produce molecules that are structurally similar but not identical. These differences can affect immunogenicity, half-life, and clinical efficacy.
The FDA’s biosimilar pathway, established under the BPCIA, requires extensive analytical characterization, animal studies, human pharmacokinetic and pharmacodynamic data, and in some cases clinical efficacy trials to demonstrate biosimilarity. The total regulatory package for a biosimilar typically costs $100 million to $300 million, compared to the $1 million to $5 million cost of a small-molecule ANDA, which is why the biosimilar market has developed more slowly than the generic small-molecule market and remains concentrated among large, well-capitalized manufacturers.
The Patent Dance: Mandatory Steps, Optional Participation
The BPCIA’s information-exchange mechanism, universally called the ‘patent dance,’ was designed to replicate the Orange Book/Paragraph IV framework for biologics but was adapted to the fact that biologic patents are not publicly listed in a binding manner. The dance requires the biosimilar applicant to share its full application and manufacturing information with the reference product sponsor (RPS) within 20 days of FDA acceptance of the BLA. The RPS then has 60 days to identify patents it believes are infringed. The biosimilar applicant has another 60 days to respond with invalidity or non-infringement positions. The parties then have 15 days to agree on a list of patents to litigate in the ‘first phase,’ with remaining disputes going to a ‘second phase.’
The Supreme Court’s 2017 decision in Amgen v. Sandoz held that participation in the dance is optional: a biosimilar applicant that declines to share its application faces the consequence that the RPS can seek an immediate injunction for infringement of all of its patents, not just those on the negotiated first-phase list. Participation narrows litigation to the agreed subset. The strategic calculation depends on the specific patent landscape and the biosimilar applicant’s confidence in its non-infringement or invalidity positions.
Biosimilar Interchangeability: The Substitution Premium
The FDA has two tiers of biosimilar approval: biosimilar (similar enough to rely on the reference product’s safety and efficacy data) and interchangeable (the higher standard that permits automatic pharmacy substitution in states that allow it). As of early 2026, the FDA has approved more than a dozen interchangeable biosimilars across multiple reference products. All interchangeable biosimilars approved in the U.S. bear reference to a small number of high-value products: adalimumab, insulin glargine, and a handful of others.
The commercial importance of the interchangeability designation depends on state pharmacy practice acts, formulary design, and payer incentives. In states that permit automatic substitution of interchangeable biosimilars and where payers have erected formulary incentives for biosimilar use, the interchangeable product can capture market share faster and at higher volume than a non-interchangeable competitor that requires an explicit prescriber switch. The price discount required to achieve formulary positioning also varies: interchangeable biosimilars have sometimes achieved formulary placement at lower discounts because the payer values the operational ease of pharmacy-level substitution.
The Humira Biosimilar Experience: What Happened and Why
Humira’s U.S. LOE in January 2023 was the most scrutinized drug patent expiration in the modern era, and the results surprised most analysts. Despite the launch of eight biosimilars within the first six months, Humira retained substantial unit market share through 2023 because AbbVie had pre-negotiated deep rebate arrangements with PBMs and insurers that effectively paid for exclusive or preferred formulary placement. The biosimilars launched at 5 to 85 percent discounts to Humira’s list price, but net prices, after rebates, converged in ways that made the branded product competitive on a net-cost basis for many payers.
AbbVie’s global Humira revenues did fall: the company reported a 41 percent year-over-year drop in Q4 2023 revenues for the product. But the stock performance told a different story. AbbVie’s shares outperformed the S&P 500 from the January 2023 LOE through year-end 2023 because the market was pricing the success of Skyrizi (risankizumab) and Rinvoq (upadacitinib), which together generated over $10 billion in revenue in 2023 and were growing rapidly. The stock market was not valuing Humira; it was valuing the bridge.
The IP valuation lesson here is significant. AbbVie’s corporate value through the Humira cliff was maintained not by the residual Humira patent estate, but by the accumulated clinical and commercial data supporting Skyrizi and Rinvoq, each of which has its own IP stack. Rinvoq’s composition-of-matter patent runs through approximately 2028, with formulation and method-of-use patents extending the thicket further. Skyrizi’s core patent protection extends into the early 2030s. These assets were, in IP valuation terms, the replacement for the depreciating Humira estate.
Key Takeaways: Biologics and the BPCIA
Biologics’ structural complexity means that biosimilar development costs $100 million to $300 million versus under $5 million for a small-molecule ANDA. The 12-year exclusivity standard reflects this investment barrier. Biosimilar interchangeability designations create a substitution premium that affects formulary positioning and market share dynamics. The Humira LOE demonstrated that rebate architecture, not patent barriers, can be the most effective short-term defense against biosimilar erosion. The long-term lesson from AbbVie’s experience is that market value through a major LOE event requires a successor asset with its own durable IP estate, not just lifecycle management of the expiring product.
Investment Strategy: Biologics LOE
For institutional investors, the analytical question at a biologic LOE is not ‘how much will biosimilars capture’ but rather: (1) what is the net price convergence trajectory between the reference product and biosimilar competitors under real-world formulary conditions, (2) does the innovator have pre-negotiated rebate contracts that lock in formulary position for 12 to 24 months post-launch, (3) what is the IP stack on the successor asset, and (4) how far along is the clinical conversion to a reformulated or combination version that carries fresh exclusivity. AbbVie answered questions 2 through 4 correctly in the Humira transition. The stock rewarded the preparation.
Part V: Lifecycle Management Tactics
The Patent Thicket: Architecture and Limits
A patent thicket is a collection of overlapping patents covering a single drug product, constructed to create so many litigation risks for a potential generic entrant that the cost of clearing the IP landscape exceeds the expected commercial value of entry. The thicket does not need to be legally unassailable; it needs to be expensive and time-consuming enough to deter or delay.
AbbVie’s Humira portfolio, with over 130 patents covering formulation, concentration, syringe design, and manufacturing processes, is the most-cited example. The core composition-of-matter patent for adalimumab expired in the U.S. in December 2016. AbbVie sustained U.S. market exclusivity until January 2023 by threatening biosimilar entrants with multi-patent infringement suits and by executing settlement agreements that specified 2023 entry dates in exchange for AbbVie dropping litigation. The thicket was not a legal fortress; it was a financial deterrent that worked because the cost of litigating 130 patents across multiple district courts exceeded the expected value of earlier entry for most potential entrants.
The FTC and Congress have taken notice. The FTC’s 2021 report on pharmaceutical patent thickets documented the pattern across multiple large biologics and called for restrictions on Orange Book listings of device patents. Senator Amy Klobuchar’s letters to major drug manufacturers in 2024 specifically called out what the agency termed ‘improper and inaccurate’ patent listings. The trend is toward more scrutiny, not less, which means thicket strategies will face increasing legal risk going forward.
The Full Thicket Roadmap: What a Complete Portfolio Looks Like
A mature thicket for a biologic product typically contains layers that can be mapped onto a timeline. Layer one is the composition-of-matter patent on the molecule, filed at discovery (year 0 in the roadmap, expires year 20). Layer two consists of formulation patents covering concentration, buffer systems, and preservatives, filed at Phase II (year 5 to 7, expires year 25 to 27). Layer three covers manufacturing process patents filed when the production process is locked (year 6 to 8, expires year 26 to 28). Layer four consists of device patents for auto-injectors or prefilled syringes filed at product design (year 8 to 10, expires year 28 to 30). Layer five includes method-of-use patents filed at Phase III completion or at approval for each indication (year 10 to 15, expires year 30 to 35). Each layer has a different expiration date, a different vulnerability profile to PTAB challenge, and a different level of relevance to biosimilar manufacturers.
An entrant attempting to launch a biosimilar must clear or design around each layer independently. Designing around a manufacturing process patent may require a different cell line or purification strategy, which could affect product quality attributes and require additional analytical work. Designing around a device patent may require an alternative delivery device, which requires FDA approval. The cumulative cost of these workarounds is the effective ‘toll’ the thicket imposes.
Product Hopping: The Clinical Conversion Strategy
Product hopping involves reformulating a drug to create a new version with clinically meaningful advantages, launching that version with fresh IP protection, and migrating patients to the new formulation before the original goes generic. The commercial defense depends on making the new version preferred by prescribers and payers on clinical grounds, so that when generic versions of the original formulation launch, they address an increasingly thin slice of the market.
The strategy works best when the reformulation provides a genuine clinical benefit, not merely a convenience difference. Extended-release formulations, subcutaneous versions of intravenous drugs, and combination products that eliminate a separate pill are the most defensible versions. Formulation changes that are purely administrative, moving from a capsule to a tablet without meaningfully different pharmacokinetics, have been challenged as anticompetitive when paired with promotional strategies to discourage generic substitution of the original formulation.
Merck’s pembrolizumab (Keytruda) conversion to the subcutaneous formulation is the highest-stakes current example of this strategy. The IV formulation’s core patents face expiration around 2028. Merck received FDA approval in September 2025 for Keytruda Qlex, the subcutaneous version co-formulated with the hyaluronidase enzyme berahyaluronidase alfa. The clinical advantage is concrete: subcutaneous administration takes approximately 30 minutes, compared to 30 to 60 minutes for IV infusion, reducing chair time in infusion centers and potentially enabling administration in less-equipped settings. Merck has filed patents on the co-formulation, the specific dosing regimen, and the combination device, all of which will expire in the mid-2030s.
Keytruda IP Valuation: What the Franchise Is Actually Worth
Keytruda generated $29.5 billion in revenue in fiscal 2024 across more than 40 approved indications. The core pembrolizumab composition-of-matter patent expires in 2028, but the franchise’s full IP estate is materially more complex.
Merck’s Orange Book and USPTO filings show pembrolizumab-specific patents extending across formulation and method-of-use claims into the early 2030s. The Keytruda Qlex approval comes with its own IP stack, covering the subcutaneous formulation, the berahyaluronidase co-formulation, and specific dosing protocols. Assuming a 30 percent market penetration of the subcutaneous formulation within two years of launch, and a 20 percent price premium for Qlex over the IV formulation on a per-dose basis, the incremental revenue from the conversion program could reach $3 billion to $6 billion annually by 2027. Against a background of IV biosimilar competition post-2028 that could erode IV pembrolizumab revenues by 60 to 80 percent over three years, the subcutaneous franchise represents the primary IP-protected revenue stream for the Keytruda franchise in the 2028 to 2035 period.
Merck’s pipeline of combination regimens, including pembrolizumab plus the TIGIT inhibitor vibostolimab (MK-7684A) and pembrolizumab plus the LAG-3 antibody favezelimab, each carry independent IP estates with composition-of-matter filings from the 2017 to 2020 period, expiring in the late 2030s. If any of these combinations achieve regulatory approval and clinical differentiation from IV pembrolizumab monotherapy, they create a second product-hopping opportunity: prescribers transition to the combination, which has its own exclusivity, rather than to IV pembrolizumab biosimilars. The IP architecture is designed with this transition in mind.
Method-of-Use Expansion and the Skinny Label Risk
Each new approved indication for a drug can generate NCI exclusivity for three years. Generic manufacturers seeking to launch before the new indication’s exclusivity expires must file an ANDA with a carved-out label (the ‘skinny label’) that omits the protected use. The question courts have struggled with is whether a generic bearing a skinny label can be held liable for induced infringement if real-world prescribing patterns result in off-label use for the protected indication.
GSK v. Teva, a case involving the cardiovascular drug carvedilol, produced a Federal Circuit ruling in 2021 that found generic manufacturers could face induced infringement liability even under a skinny label if their promotional or marketing activities (including Dear Healthcare Provider letters, press releases, and labeling guidance) communicated an intent to encourage use for the protected indication. The decision was controversial, and on remand the case produced mixed results, but the practical effect has been to make skinny labeling a higher-stakes strategy for generic manufacturers. The threat of induced infringement liability has deterred some at-risk launches and strengthened the commercial value of method-of-use patents that would otherwise be easily designed around.
Key Takeaways: Lifecycle Management
Patent thickets work by imposing clearing costs on entrants, not by being legally unassailable. The FTC’s escalating scrutiny of thicket strategies and Orange Book listings is the primary legal risk to this approach over the next five years. Product hopping’s commercial success depends on the clinical credibility of the reformulation; purely cosmetic reformulations face antitrust and regulatory resistance. The Keytruda subcutaneous conversion is the most consequential product-hopping play in the current cycle, with potential to sustain billions in IP-protected revenue past the 2028 IV expiration. Skinny labeling is operationally riskier post-GSK v. Teva; generic manufacturers now face induced infringement exposure that did not meaningfully exist before 2021.
Part VI: The 2025-2030 Patent Cliff – Asset-by-Asset Intelligence
Scale and Composition of the Current Wave
The 2025 to 2030 patent cliff differs from prior cycles in three respects. First, it involves a higher proportion of biologics, which face biosimilar competition rather than generic competition, producing slower and less complete revenue erosion. Second, it includes the two largest single-product revenue streams ever to face LOE in a short time window, Keytruda and Eliquis, within approximately the same 36-month period. Third, it unfolds against the backdrop of IRA-mandated price negotiation, which is compressing the commercial opportunity on the front end of the exclusivity period even before LOE occurs.
Keytruda (Pembrolizumab) – Merck – LOE 2028
Covered in detail in the product-hopping section above. The 2028 LOE event will be the largest single LOE in pharma history measured by pre-LOE sales. The subcutaneous conversion, combination pipeline, and new indication filings are Merck’s primary defenses. Analysts at JPMorgan and Goldman Sachs have modeled Merck’s post-2028 Keytruda revenues using scenarios ranging from 40 percent IV market share erosion (bull case) to 75 percent erosion (bear case) within three years of biosimilar launch. The Qlex conversion rate is the key swing variable.
Eliquis (Apixaban) – Bristol Myers Squibb / Pfizer – LOE 2026-2029
Eliquis is a BMS/Pfizer co-promotion. Patent litigation has produced a complex settlement landscape with multiple generic manufacturers entering at staggered dates. The compound patent expires in 2026, but BMS and Pfizer have defended formulation patents through 2028-2029 for major markets. BMS’s strategic position is particularly exposed: Eliquis represented over 30 percent of its net revenues in recent years, and the LOE arrives before the company’s pipeline assets (Opdualag, Camzyos, Cobenfy) are at sufficient scale to replace the lost cash flow.
Eliquis IP Valuation
The Orange Book listing for apixaban includes the compound patent (estimated expiry 2026 after PTE), two formulation patents with estimated expiry in 2028, and a method-of-use patent for atrial fibrillation. Multiple generic manufacturers have filed Paragraph IV certifications. Settlement agreements have been reached with most challengers specifying entry dates in the 2028 to 2029 range. The present value of the formulation patent protection from 2026 to 2028 amounts to approximately $18 billion in protected revenue at current sales rates, making the litigation defense of those formulation patents among the highest-ROI IP activities in the current pharmaceutical cycle.
Stelara (Ustekinumab) – Johnson & Johnson – LOE 2025
J&J’s ustekinumab faced biosimilar competition beginning in 2025 after Paragraph IV settlements with multiple biosimilar applicants. The product generated approximately $10.8 billion globally in its final full year of exclusivity. J&J has attempted a partial conversion strategy toward Tremfya (guselkumab) in psoriasis, which targets IL-23p19 specifically rather than the IL-12/IL-23 dual mechanism of ustekinumab. Tremfya’s IP estate runs through the early 2030s. The clinical differentiation argument is not always compelling, because both drugs work well in psoriasis, but guselkumab has shown superiority in some head-to-head data.
Opdivo (Nivolumab) – Bristol Myers Squibb – LOE 2028
BMS’s PD-1 checkpoint inhibitor generated approximately $9 billion in 2024. The compound patent expires in 2028. BMS has multiple combination regimens approved or in late-stage development, including nivolumab plus relatlimab (Opdualag) and nivolumab plus ipilimumab (Opdivo Yervoy), each carrying independent IP. The conversion strategy mirrors Merck’s Keytruda playbook: migrate patients to protected combination regimens before nivolumab monotherapy goes off-patent.
BMS’s financial situation makes the timing of Opdivo’s LOE particularly important. The company faces concurrent LOE pressure from both Eliquis and Opdivo in the same 2026-2028 window, with no single replacement asset at the scale of either. The company’s pipeline bets on cardiovascular (Camzyos, mavacamten) and neuroscience (Cobenfy, xanomeline-trospium) are growing but are not currently at the scale needed to replace $35 to $40 billion in combined Eliquis/Opdivo revenues.
BMS IP Valuation: The Double-Cliff Problem
BMS’s IP estate through 2030 can be mapped as follows. Eliquis protection extends through 2028-2029 under formulation and settlement terms. Opdivo’s compound patent expires 2028. Opdualag’s relatlimab component carries a composition-of-matter patent through approximately 2032. Camzyos (mavacamten) has NCE exclusivity through 2026 and patent protection extending to approximately 2033. Cobenfy (xanomeline-trospium) received FDA approval in 2023 with patent protection into the early 2030s. The gap between the revenue base today ($50+ billion annually) and the revenue base that these successor assets will generate by 2030 is the central analytical challenge for BMS investors.
Entresto (Sacubitril/Valsartan) – Novartis – LOE Mid-2025
Novartis received an adverse ruling in July 2025 when a U.S. district court denied a preliminary injunction against a generic manufacturer’s at-risk launch of sacubitril/valsartan. The denial did not adjudicate the ultimate validity of the patents, but it found that Novartis failed to demonstrate a likelihood of success on the merits sufficient to justify an injunction. The practical effect was to expose the product to generic competition sooner than Novartis had projected.
Entresto’s base case, absent patent protection, generates approximately $6 billion annually at risk of erosion to 15 to 25 cents on the dollar within 18 months of full generic penetration. Novartis has filed no meaningful conversion or product-hopping strategy for Entresto, making it a clean cliff rather than a managed LOE event.
Eylea (Aflibercept) – Regeneron – LOE 2025-2027
Regeneron’s Eylea, the vascular endothelial growth factor (VEGF) trap for wet AMD and diabetic macular edema, generated approximately $5.9 billion in the U.S. in its peak year. Regeneron has executed a partial conversion to Eylea HD (8 mg aflibercept, versus 2 mg in the original), approved in 2023 with a dosing interval advantage that allows less frequent injections for many patients. Eylea HD carries a fresh IP estate with key patents extending into the early 2030s.
The Eylea HD conversion faces genuine clinical competition from Apellis’s Syfovre (pegcetacoplan) and from anti-VEGF/anti-angiopoietin-2 combination products including Vabysmo (faricimab, Roche). These competitors have their own IP estates and are not limited by Regeneron’s patent clock. The ophthalmology market is becoming a multi-asset competitive landscape, which means Regeneron’s Eylea HD IP estate is valuable but not monopolistic.
Trulicity (Dulaglutide) – Eli Lilly – LOE 2027
Eli Lilly’s GLP-1 receptor agonist dulaglutide faces LOE around 2027, but Lilly’s position in the GLP-1 space has been substantially repositioned by the success of tirzepatide (Mounjaro, Zepbound), a dual GIP/GLP-1 agonist with a superior efficacy profile in clinical trials. Tirzepatide’s composition-of-matter patent runs through approximately 2036. Lilly’s strategic exposure from Trulicity’s LOE is substantially cushioned by tirzepatide’s commercial scale: Mounjaro plus Zepbound generated over $12 billion in combined revenues in 2024 and are growing rapidly.
Key Takeaways: The 2025-2030 Cliff
The 2025-2030 cliff is the largest in pharma history by pre-LOE revenue at risk. Biologics face slower, less complete erosion than small molecules, but the magnitude of Keytruda and Eliquis LOE is unprecedented in absolute dollar terms. BMS faces the most concentrated two-year cliff exposure of any major company, with Eliquis and Opdivo both losing exclusivity in the 2026-2028 window. Companies with successful conversion strategies (Merck with Keytruda Qlex, Regeneron with Eylea HD, Lilly with tirzepatide) face a materially better outcome than those with clean cliffs (Novartis/Entresto, BMS absent successful ramp of pipeline assets).
Investment Strategy: Positioning for the Cliff
The patent cliff creates both long and short opportunities across the pharma and generic/biosimilar sectors. On the long side, companies with fully-funded bridge strategies and IP-protected successor assets trading at multiples that do not yet reflect the successor assets’ peak revenue potential are the primary candidates. AbbVie post-2019, when the Skyrizi/Rinvoq buildout was underway but not yet commercially visible, is the archetype. The question is identifying which company today is in the pre-AbbVie phase of that transition.
On the short side, companies with concentrated LOE exposure, limited pipeline visibility, and high current multiples relative to post-cliff earnings power are the most exposed. The analytical work involves building a product-by-product revenue bridge from current revenues to post-cliff revenues under three scenarios (managed transition, partial transition, clean cliff), applying a realistic multiple to post-cliff earnings, and comparing to current enterprise value.
For generics and biosimilar manufacturers, the cliff represents the opposite opportunity. Companies with ANDA or biosimilar BLA approvals for the major 2027-2029 expirations, robust manufacturing scale, and proven formulary access strategies will generate the highest returns. In biosimilars specifically, scale matters: the economics favor manufacturers capable of competing on both price and supply reliability simultaneously, because payers and PBMs will not accept single-source biosimilar supply after watching supply disruptions across the generic small-molecule market.
Part VII: IP Valuation Frameworks
The Net Present Value of Patent Protection
IP valuation in pharma is ultimately a cash flow problem. The patent estate’s value is the present value of the incremental cash flows attributable to exclusivity, compared to a counterfactual world in which the product faces generic or biosimilar competition from the current date.
The calculation requires four inputs: annual net revenues under exclusivity for each remaining year, post-LOE revenue trajectory (typically modeled as a percentage of pre-LOE revenues declining on a defined schedule), the date of LOE for each IP protection layer, and the discount rate. The last variable is contested. Some analysts use the company’s WACC; others use a risk-adjusted discount rate that reflects litigation probability, regulatory risk, and IRA negotiation exposure.
For Eliquis, at $12 billion in annual U.S. revenues with LOE in 2028-2029 and assuming 80 percent revenue erosion over three years post-LOE, the NPV of the formulation patent protection from 2026 to 2028 (the period beyond the compound patent expiry) is approximately $16 billion to $20 billion at a 10 percent discount rate. This is the reason BMS and Pfizer have been willing to spend hundreds of millions in litigation defense costs to protect those formulation patents. The ROI on the defense is highly positive even at low probability of winning.
Transaction Multiples and the LOE Discount
When a drug with near-term LOE is acquired, the transaction multiple reflects the residual patent life. Industry data shows that drugs with more than 10 years of exclusivity remaining typically transact at 5x to 8x peak sales. Drugs with 5 to 10 years remaining typically transact at 3x to 5x. Drugs with less than 5 years remaining or with contested IP transact at 1x to 3x, reflecting the high probability of near-term revenue erosion.
This LOE discount creates acquisition opportunities. If a patent-cliff candidate has strong conversion or lifecycle management optionality that the market is not pricing, an acquirer with the execution capability to execute the conversion can acquire the asset at a cliff discount and realize value from the conversion. Bristol Myers Squibb’s acquisition of Celgene in 2019, which brought Revlimid into the portfolio, was partially justified by the view that the tiered generic entry settlement schedule would allow time to ramp replacement assets. The execution has been difficult, but the analytical framework was sound.
Key Takeaways: IP Valuation
Patent estate value is the NPV of exclusivity-protected cash flows. Formulation and method-of-use patents can carry substantial NPV even after the compound patent expires, which is why their defense is worth the litigation cost. LOE discounts in M&A transactions reflect residual exclusivity duration and IP integrity. Conversion optionality (the ability to execute a product-hopping strategy) is not always priced into LOE-discounted acquisition targets, creating potential for acquirers with strong lifecycle management capabilities. The IRA’s price negotiation timeline is beginning to appear in transaction modeling as a discounting factor for small-molecule assets with fewer than 13 years of exclusivity remaining.
Part VIII: The Inflation Reduction Act – Policy Rewrote the Lifecycle
Medicare Price Negotiation: The Mechanism
The IRA authorized CMS to negotiate the prices of a subset of high-expenditure Medicare drugs, beginning with 10 drugs in 2026 (negotiated in 2023), escalating to 15 drugs per year by 2029, and eventually covering a broader pool. The negotiated ‘Maximum Fair Price’ (MFP) applies to Medicare Part D and Part B drug purchases. It does not, under current law, apply to commercial markets, though there is active policy debate about whether commercial payers will contractually link their rates to MFP.
Drugs become eligible for negotiation based on how much Medicare spends on them, whether they have generic or biosimilar competition, and their time since FDA approval. The eligibility timeline differs by molecule type: small molecules become negotiation-eligible nine years after approval, while biologics become eligible at 13 years. This differential was a deliberate policy choice to reflect the lower barriers to small-molecule generic competition, but it has produced an unintended consequence that is reshaping R&D allocation.
The Small Molecule Penalty: Evidence of R&D Shift
The IRA’s 9-year versus 13-year differential, which some have called the ‘small molecule penalty,’ has generated documented changes in R&D investment allocation within approximately 24 months of the law’s passage. Multiple companies have announced or disclosed internal shifts away from small-molecule oncology programs toward biologics and cell and gene therapies.
A 2025 analysis in the Journal of Clinical Oncology found that post-approval oncology clinical trial initiations for small molecules declined relative to biologics in the two years following IRA enactment, controlling for pipeline composition at the time of the law’s passage. The effect was concentrated in indications with large Medicare populations (lung cancer, colorectal cancer) where the negotiation risk was highest. These are precisely the indications where small molecules have historically delivered some of the most cost-effective therapies, creating a policy paradox: the law designed to reduce drug prices may be diverting innovation away from the most cost-effective modalities.
MFP as a De Facto LOE
For drugs already in the Medicare negotiation pool, the MFP implementation date functions commercially as a secondary LOE. When CMS negotiates a 60 percent discount to the drug’s non-federal average manufacturer price (a discount that has historically been applied in early negotiation rounds), the effective commercial value of the remaining patent life drops dramatically. A drug with four years of patent life remaining and MFP in effect from year two of that period is not a four-year patent estate; it is a two-year estate followed by two years of government-price sales.
IQVIA’s analysis of IRA commercial impact shows that the net present value of a small-molecule drug’s commercial opportunity declines by an estimated 40 to 60 percent relative to the pre-IRA environment, depending on indication, Medicare share of revenues, and time to negotiation eligibility. This has direct implications for how pharma companies price their assets in early-stage licensing transactions, how they value pipeline candidates in internal hurdle rate calculations, and how they structure milestone payments in co-development agreements.
Investment Strategy: Positioning Under the IRA
For investors, the IRA creates several actionable portfolio implications. Companies with pipelines concentrated in biologics, cell therapies, and gene therapies have a structural advantage under the 13-year eligibility standard relative to small-molecule-heavy portfolios. Companies in rare diseases, where orphan drug populations are typically too small to generate the Medicare spending levels that trigger negotiation eligibility, face less IRA exposure. Companies in large-population indications (cardiovascular, diabetes, oncology) with small-molecule pipelines face the highest IRA discount to future commercial value.
The market has not fully priced these distinctions. Small-molecule cardiovascular and metabolic programs at mid-cap companies are being valued on commercial peak-sales assumptions that predate the IRA’s practical impact on negotiation-eligible drugs. As the first round of MFP implementation data becomes available in 2026, the re-pricing of small-molecule commercial assets is likely to become more visible and more rapid.
Part IX: The Global Chessboard
Europe: Supplementary Protection Certificates and the Unitary SPC
The European Union does not replicate the U.S. Orange Book/Hatch-Waxman framework. Instead, patent protection for pharmaceuticals is extended through national Supplementary Protection Certificates (SPCs), which can add up to five additional years of protection beyond the patent term to compensate for regulatory delay. An additional six months is available through a Paediatric Extension, analogous to the U.S. pediatric exclusivity add-on, for completion of a Paediatric Investigation Plan (PIP) per EMA requirements.
The maximum total SPC duration is five years, and the total protection period from the first EU marketing authorization cannot exceed 15 years. The calculation is based on the date of the first EU authorization (not national authorizations), which creates planning considerations for companies that launch in some EU member states before others.
The ongoing development of the Unitary SPC, which would provide a single SPC valid across all EU member states that have ratified the Unified Patent Court (UPC) Agreement, is the most significant structural change to European pharmaceutical IP in two decades. Under the current fragmented system, a company must file for SPCs in each EU member state separately, pay separate fees, and manage separate expiration dates that can differ by months due to national procedural variations. A Unitary SPC eliminates this complexity but also creates a single point of failure: a successful challenge in the Unitary Patent Court invalidates protection across all participating states simultaneously.
Japan: Re-examination Period and the Generics Push
Japan’s pharmaceutical regulatory system uses a ‘Re-examination Period’ (sai-shinsa-kikan) that functions as robust data exclusivity. For standard new drugs, this period runs eight years from approval. For orphan drugs, it extends to ten years. During the Re-examination Period, the PMDA continues monitoring the drug’s safety through post-marketing surveillance, and generic manufacturers cannot receive approval relying on the innovator’s data until the period ends.
The Japanese government has been pushing aggressively toward higher generic utilization rates, targeting an 80 percent generic share of the volume market. This push has created pricing pressure on long-listed branded drugs whose Re-examination Periods have expired. Annual price revisions under Japan’s NHI pricing system, which apply discounts to drugs with high-volume generic competition, have compressed the commercial tails of Japanese branded drug revenues significantly. Companies dependent on Japan for more than 15 percent of their revenue need to model Japanese price erosion independently of patent expiration dates, because the NHI revision mechanism can compress revenues even while a drug is technically protected.
China: Patent Linkage 2.0 and the Data Exclusivity Build
China’s pharmaceutical IP environment has modernized substantially since the 2017 Drug Administration Law amendment and the 2021 introduction of a patent linkage system. The 2021 system established a database of drug patents (analogous to the Orange Book) and a mechanism by which generic applicants must certify their relationship to listed patents. A drug patent holder can file suit within a specified window after receiving certification, triggering a nine-month stay on generic approval.
China’s nine-month stay is shorter than the U.S. 30-month stay, and the overall framework is less litigant-friendly to innovators than the U.S. system, but it represents a major improvement over the pre-2021 environment in which there was no linkage mechanism at all. Importantly, China’s system includes a first-to-challenge exclusivity period of 12 months for the generic manufacturer that successfully invalidates a listed patent, twice the U.S. 180-day period, creating a significant incentive for domestic generic challengers.
The NMPA released draft data exclusivity regulations in 2025 that, if finalized as proposed, would provide six years of data exclusivity for innovative small-molecule drugs and 12 years for biologics. These standards, which align with international norms under TRIPS-Plus frameworks, are essential for multinational companies evaluating China-first development strategies for novel molecules. Without data exclusivity, the commercial case for China registration of truly novel drugs is weakened by the risk of immediate domestic generic competition upon approval.
India: Section 3(d) as Anti-Evergreening Architecture
India’s Section 3(d) of the Patents Act, 1970, as amended in 2005, prohibits the grant of patents for ‘new forms of known substances’ unless those forms demonstrate a ‘significantly enhanced efficacy’ compared to the known substance. The provision was designed specifically to block the secondary patenting strategies that constitute evergreening in other markets: new salt forms, new polymorphs, new crystal structures, new hydrates, and new dosage forms of previously known molecules are unpatentable in India unless enhanced efficacy is demonstrated.
The Novartis v. Union of India (2013) decision by the Indian Supreme Court confirmed this interpretation and rejected Novartis’s argument that the beta-crystalline form of imatinib (the active ingredient in Glivec) qualified for a patent because it had higher bioavailability than the free base form of the compound. The Court held that enhanced bioavailability did not constitute ‘significantly enhanced efficacy’ within the meaning of Section 3(d).
The operational consequence for multinational pharmaceutical companies is that many secondary patents that provide meaningful exclusivity in the United States and Europe do not exist in India. This means that generics manufactured in India for export to other markets may be able to use non-patentable formulation variants as the basis for their products, potentially accelerating global generic competition for drugs that rely heavily on secondary IP in their home markets.
Key Takeaways: Global IP Geography
European SPC strategy requires country-by-country planning under the current fragmented system, with the Unitary SPC creating efficiency but also single-point-of-failure risk. Japan’s Re-examination Period provides effective eight-to-ten-year data exclusivity but does not substitute for a full patent strategy, and NHI pricing mechanisms can compress revenue independent of patent status. China’s patent linkage system is maturing rapidly, and the 2025 data exclusivity draft regulations represent the most important IP development in the Chinese pharma market in a decade. India’s Section 3(d) remains the most potent anti-evergreening provision in any major pharmaceutical market and directly affects the global generic supply chain for drugs that rely on secondary patents in other jurisdictions.
Part X: At-Risk Launches
The Mechanics and Economics of at-Risk Entry
An at-risk generic launch occurs when a generic manufacturer begins commercial distribution of its product before the resolution of patent litigation, betting that courts will ultimately find the asserted patents invalid or not infringed. The risk is severe: if the courts find for the innovator, the generic manufacturer faces liability for the innovator’s lost profits, which for a blockbuster drug can reach into the billions of dollars. Under 35 U.S.C. Section 284, courts may also award treble damages for willful infringement, which could triple the exposure.
The calculus that drives at-risk launches involves comparing the expected value of early market entry against the probability-weighted cost of an adverse judgment. For a drug generating $3 billion annually, an at-risk launch six months before the court rules generates roughly $1.5 billion in revenue. If the generic sells at a 30 percent discount to brand and captures 50 percent market share, the gross revenue during the at-risk period is approximately $450 million. The question is whether $450 million justifies the litigation exposure.
The Protonix (pantoprazole) at-risk launch by Teva and Sun Pharmaceuticals illustrates the catastrophic downside. Both companies launched pantoprazole before litigation concluded. The court ultimately upheld Wyeth’s formulation patent. The settlement required both generic companies to pay a combined $2.15 billion, one of the largest patent infringement settlements in industry history. The at-risk revenue was a fraction of the settlement cost.
When At-Risk Launches Make Sense: The 2024-2025 FTC Lens
Despite the Protonix example, at-risk launches have increased in frequency in the 2023-2025 period for a specific reason: the FTC’s campaign against allegedly improper Orange Book listings has created a new category of at-risk opportunity. When a court orders delisting of a device patent that a generic manufacturer has challenged as improperly listed, the 30-month stay associated with that patent may be vacated, and the generic can launch without waiting for litigation to conclude on the remaining compound or formulation patents.
For inhalers, auto-injectors, and pre-filled syringe products where device patents have been listed in the Orange Book, the FTC’s position is that those patents do not ‘claim the drug’ as required by statute. If courts agree, the litigation terrain shifts materially: device patents that have been supporting 30-month stays lose that function, and generic manufacturers can enter earlier with lower litigation risk. This has produced a wave of Orange Book delisting motions in 2024 and 2025 that is rewriting the competitive timelines for multiple respiratory and injectable drug categories.
Key Takeaways: At-Risk Launches
At-risk launches require a rigorous probability-weighted cost-benefit analysis. The Protonix settlement demonstrates that even large generic manufacturers can face existential financial exposure from a failed at-risk strategy. The FTC’s Orange Book delisting campaign has created a new category of at-risk opportunity for device-patent-defended products, where the legal risk profile is materially different from traditional compound or formulation patent challenges. For investors in generic manufacturers, positions in at-risk launches are asymmetric: the upside is large but bounded, while the downside can exceed the at-risk revenue by a factor of five or more.
Part XI: Technology Roadmap – Next-Generation Molecules and the New Exclusivity Frontier
New Modalities, New IP Architectures
The pharmaceutical industry’s shift toward novel therapeutic modalities, including mRNA therapeutics, siRNA/antisense oligonucleotides, cell and gene therapies, and antibody-drug conjugates (ADCs), is not merely a scientific development. It is an IP architecture shift that will reshape the nature of pharmaceutical patent protection over the next decade.
Each of these modalities generates a distinct IP portfolio structure. mRNA therapeutics, illustrated by the Moderna and BioNTech COVID-19 vaccines, involve at least four distinct IP layers: the lipid nanoparticle delivery system, the mRNA sequence design (UTR elements, cap analogues, modified nucleotides), the encoded antigen or protein sequence, and manufacturing processes. These layers are owned by different parties, creating the kind of fragmented IP landscape that produces freedom-to-operate (FTO) complexity in ways that small-molecule pharmaceuticals did not.
The Moderna v. Pfizer/BioNTech litigation over mRNA vaccine lipid nanoparticle patents, initiated in August 2022, offers a preview of the IP warfare that will characterize the mRNA therapeutics market. Moderna claims that Pfizer/BioNTech’s LNP formulation used in the Comirnaty vaccine infringes patents filed by Moderna scientists before the pandemic. The case is pending in multiple jurisdictions and will likely produce precedents that define the contours of mRNA IP protection for a generation.
CRISPR: The Platform Patent Dispute and Its Commercial Consequences
CRISPR-Cas9 gene editing technology is subject to one of the most intensely litigated platform patent disputes in history, between the Broad Institute (controlling IP developed in Zhang Feng’s laboratory) and the University of California (controlling IP from Jennifer Doudna and Emmanuelle Charpentier’s work). The fundamental question, which has produced conflicting results in the U.S. and European proceedings, is which party holds priority for CRISPR-Cas9 in eukaryotic cells, the claim that matters commercially for human therapeutics.
The practical consequence for companies developing CRISPR-based medicines is that they must license IP from at least one, and potentially both, of these competing patent estates. The licensing terms, royalty rates, and field-of-use restrictions embedded in CRISPR platform licenses create a layered cost structure that affects the economics of CRISPR therapeutics in ways that traditional small-molecule or biologic drugs do not face. The bluebird bio/CRISPR Therapeutics/Vertex CTX001 (now Casgevy) collaboration is a case study: Vertex paid $900 million to acquire CRISPR Therapeutics, taking on both the clinical and IP exposure simultaneously.
Antibody-Drug Conjugates: The ADC IP Stack
ADCs combine a monoclonal antibody (targeting moiety) with a cytotoxic payload connected by a chemical linker. Each component carries its own IP. The antibody component may be covered by composition-of-matter patents from the original antibody developer. The payload (often an auristatin, maytansine, or camptothecin derivative) is covered by synthesis and method-of-use patents. The linker chemistry is covered by a distinct set of patents, often held by platform companies like ADC Therapeutics or Sutro Biopharma that have built linker portfolios independent of specific antibody-payload combinations.
The result is that an ADC manufacturer must typically navigate multiple third-party patent estates to bring a product to market, and the FTO analysis for an ADC is substantially more complex than for either a naked antibody or a small-molecule drug. As ADCs become one of the most active areas of pharma M&A (there were more than $50 billion in ADC-focused transactions in 2023-2024), the quality of the FTO analysis on both the acquirer’s and the target’s IP estates is a critical diligence factor.
The Regulatory Exclusivity Pathway for Gene Therapies
Gene therapies occupy a complex regulatory position. One-time treatments that correct a genetic defect are classified as biologics under the BPCIA, entitling them to 12 years of exclusivity. The FDA has also indicated that gene therapies may qualify for orphan drug designation in most of the genetic conditions currently being targeted, adding seven years of ODE on top of biologic exclusivity. For ultra-rare pediatric conditions, the Rare Pediatric Disease designation can generate a Priority Review Voucher (PRV) that can be sold to another company for $100 million to $200 million, creating a near-term revenue event independent of the drug’s commercial launch.
The combination of biologic exclusivity, ODE, and PRV monetization means that a gene therapy approved for a rare pediatric condition can generate IP-protected commercial revenue plus a substantial cash payment from a PRV sale before a single patient is treated. The IP architecture for these products is uniquely favorable, which is a primary reason that rare pediatric genetic diseases have attracted disproportionate pipeline investment.
Final Key Takeaways: The Full Picture
On Patent Mechanics. The statutory 20-year term is the starting point, not the answer. Effective commercial life runs 5 to 12 years after approval. PTEs under Section 156 can restore up to five years but require precise calculation and active prosecution. The sequential layering of composition, formulation, manufacturing, and method-of-use patents is the primary tool for extending the enforceable IP envelope beyond the compound patent expiration date.
On Regulatory Exclusivity. NCE, ODE, NCI, biologic, and pediatric exclusivities operate independently of patents and cannot be invalidated through litigation. The operative LOE date is the later of patent expiration and regulatory exclusivity expiration. For valuation and competitive forecasting purposes, both must be calculated for each approved indication, not just the primary indication.
On the 2025-2030 Cliff. The current wave is the largest in pharma history by pre-LOE revenue at risk. Keytruda’s 2028 LOE is the single largest revenue-erosion event ever. Biologics will face slower erosion than small molecules, but the formulary contracting dynamics, not just the legal patent status, will determine the actual revenue trajectory. BMS faces the most concentrated cliff exposure among major companies.
On Lifecycle Management. Patent thickets are legally opaque deterrents, not unassailable fortresses. FTC scrutiny is tightening. Product hopping’s value depends on clinical credibility of the reformulation. Merck’s Keytruda Qlex is the most consequential product-hopping execution in the current cycle. Skinny labeling carries induced infringement exposure that has grown materially since GSK v. Teva.
On the IRA. The nine-year Medicare negotiation eligibility for small molecules is a second commercial cliff, layered on top of patent expiration. Companies and investors who model drug value on the assumption that patent protection equals commercial exclusivity are overstating NPV for small-molecule assets. The modality shift toward biologics and cell/gene therapies is partly a rational response to the IRA’s differential treatment.
On Global IP. European SPC plus paediatric extension can provide up to 15.5 years of total protection from first EU authorization. Japan’s Re-examination Period provides eight-to-ten-year data exclusivity regardless of patent status. China’s maturing patent linkage and draft data exclusivity regulations are the most important IP development in the global emerging-market pharma landscape. India’s Section 3(d) remains the world’s most powerful single statutory barrier to secondary pharmaceutical patenting.
On New Modalities. mRNA, CRISPR, ADC, and cell/gene therapy IP architectures are fundamentally different from small-molecule and antibody portfolios. Platform patent disputes (Moderna v. Pfizer, the Broad v. UC CRISPR proceedings) will define commercial rights for entire therapeutic categories. FTO analysis for these modalities requires specialized expertise that most pharma IP teams are still building.
FAQ
Q: What is the practical difference between patent expiration and regulatory exclusivity expiration?
A: A patent can be challenged and invalidated through Paragraph IV litigation, inter partes review at the PTAB, or inequitable conduct findings. Regulatory exclusivity cannot. If a drug’s Orange Book patents are all invalidated by a court, but the drug still holds NCE exclusivity, the FDA cannot approve a generic for five years from drug approval regardless of the patent outcome. In competitive intelligence, the two dates must be tracked independently because either can be the binding constraint on generic entry.
Q: How does the IRA’s small molecule penalty change drug valuation models?
A: Pre-IRA, a drug’s commercial NPV was modeled as: annual revenues under exclusivity discounted at WACC, multiplied by years of exclusivity. Post-IRA, for small molecules in large Medicare-covered populations, the model must include a negotiation haircut beginning at year nine. If CMS historically negotiates discounts of 40 to 60 percent, the revenue in years nine through exclusivity expiration is reduced by that amount. For a drug with 15 years of exclusivity from approval, the last six years of that period face negotiated price compression. This substantially reduces modeled NPV and affects deal pricing, milestone structures, and R&D hurdle rates for small-molecule programs.
Q: What triggers a 30-month stay, and can a brand company get more than one?
A: A 30-month stay attaches when the NDA holder or patent owner files an infringement suit against a Paragraph IV ANDA filer within 45 days of receiving the Paragraph IV notice. Only one stay per NDA is standard, attaching to the first Paragraph IV challenge received. Patents listed after the ANDA is filed generally do not generate new stays in most circuits. Some brand companies have attempted to generate second stays by filing new listings and new suits on new ANDAs from the same generic, but courts scrutinize this as a potential abuse of the stay mechanism.
Q: How does biosimilar interchangeability differ from basic biosimilar approval, and why does it matter commercially?
A: A biosimilar demonstrates sufficient structural and functional similarity to the reference product to rely on the reference product’s safety and efficacy data. An interchangeable biosimilar additionally demonstrates that it can be substituted for the reference product without increased risk to the patient, even for patients who may be switched back and forth between the reference product and the biosimilar. Commercially, interchangeable biosimilars can be substituted at the pharmacy level in states that permit automatic substitution, without requiring an explicit prescriber switch. This enables faster and deeper market penetration because it removes the prescriber step from the substitution workflow.
Q: What is India’s Section 3(d) and why does it matter for global generic strategy?
A: Section 3(d) of the Indian Patents Act prohibits patenting of new forms of previously known pharmaceutical substances, including salts, esters, polymorphs, and crystal forms, unless they show significantly enhanced therapeutic efficacy. It blocks the secondary patents that form the second, third, and fourth layers of patent thickets in U.S. and European jurisdictions. Because India is the world’s largest exporter of generic pharmaceuticals, drugs that rely on secondary patents for exclusivity in the U.S. may be manufactured in India using unpatentable formulation variants and exported, potentially accelerating global generic competition even for drugs still under secondary patent protection in other markets.
Q: What is ‘patent dance’ in the context of biosimilar approvals?
A: The patent dance is the multi-step information-exchange process mandated by the BPCIA between biosimilar applicants and reference product sponsors. The applicant shares its full biologics license application and manufacturing information; the RPS identifies relevant patents; the applicant responds with invalidity or non-infringement positions; the parties negotiate which patents to litigate in the first phase. The Supreme Court’s Amgen v. Sandoz ruling held that participation is optional, though declining to dance allows the RPS to sue immediately on all patents rather than a negotiated subset. The dance can narrow and sequence litigation but does not eliminate it.
Drug patent expiration dates and regulatory exclusivity periods are subject to change through litigation outcomes, regulatory actions, and statutory amendments. For real-time expiration data, Paragraph IV filing tracking, and competitive intelligence on specific assets, consult DrugPatentWatch.