1. Executive Summary and Key Takeaways

The FDA’s Product-Specific Guidance (PSG) program is now the most consequential publicly available dataset in the generic pharmaceutical industry. A PSG does three things at once: it defines the bioequivalence (BE) standard for a specific Reference Listed Drug (RLD), it signals FDA’s willingness to accept applications, and it converts a previously speculative scientific path into a bounded, quantifiable development problem.
As of October 2025, FDA’s Office of Generic Drugs (OGD) has published more than 2,300 PSGs. Each one represents a distinct market entry signal. The companies that systematically treat PSG publication as a trigger for portfolio action — rather than a compliance checkbox — consistently produce higher first-cycle ANDA approval rates, shorter development timelines, and better capital efficiency.
Key Takeaways:
- A published PSG is not documentation. It is the starting gun for a time-sensitive market race driven by aggressive post-entry price erosion — five competitors knock the price down roughly 85% from brand levels.
- PSG type directly encodes development risk. An in vitro/BCS-based biowaiver path is a low-cost green light; a comparative clinical endpoint study mandate is a high-cost gate that demands exceptional commercial justification before proceeding.
- Under GDUFA III (October 2022 to September 2027), FDA must issue PSGs for 90% of non-complex New Chemical Entities within two years of brand approval, and for 75% of complex products within three years. This commitment schedule is a plannable, forward-looking pipeline that most generic companies under-exploit.
- The ‘Upcoming PSGs’ page on FDA.gov is the single most underutilized competitive intelligence source in the industry. Monitoring it and acting before formal publication puts a team months ahead of competitors who only react to the Federal Register notice.
- IP valuation of a generic drug program shifts materially when a PSG exists. The increase in technical probability of success (PTRS) — from roughly 50% without guidance to 85-90% with a clear PSG — can convert a negative risk-adjusted NPV into a compelling investment thesis.
- GDUFA III introduced PSG Teleconferences, pre-submission PSG Meetings, and post-submission PSG Meetings as formal mechanisms to manage the risk of guidance revision mid-development. Teams that do not use these tools are leaving material risk-reduction on the table.
2. What a PSG Actually Is — and Why Most Teams Read It Wrong
The Technical Definition
A Product-Specific Guidance is a document issued by FDA’s Office of Generic Drugs describing the agency’s current thinking on the evidence required to demonstrate that a generic drug product is therapeutically equivalent to its RLD. Each PSG addresses a single drug product, identified by active ingredient, dosage form, route of administration, and RLD application number (an NDA or ANDA number listed in the Orange Book).
PSGs are not regulations. They do not carry the force of law. But in practice, an ANDA that diverges from a PSG’s recommendations without a thoroughly documented scientific rationale will receive a Complete Response Letter (CRL). The agency is explicit: the recommendations in a PSG represent ‘the most accurate, sensitive, and reproducible approach’ to demonstrating bioequivalence for that product. Ignoring them is a near-certain path to deficiency.
What most teams miss is the inverse: a PSG that recommends an in vitro dissolution method or a BCS-based biowaiver is not merely telling you what the FDA will accept — it is telling you that the FDA has already done the scientific legwork to validate that lighter pathway. The research is done. The risk of a method-validity dispute at review is eliminated. That scientific pre-clearance has direct financial value.
The Strategic Misreading
The most common misreading is treating PSGs as a post-decisional resource — something to consult after a target has been selected and a team has started formulation work. This reverses the correct sequence. The PSG should be the first document reviewed in the target selection process, because it defines whether the development pathway is technically and commercially viable before a single dollar of R&D is committed.
The second misreading is treating the absence of a PSG as a neutral signal. It is not. An approved drug without a PSG either means the product is commercially unattractive enough that FDA has not prioritized it, the science for demonstrating bioequivalence is still unresolved, or a PSG is in development and will appear on the Upcoming PSGs page. The first scenario argues against the project. The second creates an entry barrier that protects early movers who can tolerate higher scientific risk or who have proprietary characterization capabilities. The third represents a time-sensitive opportunity to begin pre-development planning before peers who are waiting for the formal publication.
3. The GDUFA Engine: How User Fees Became the Generic Industry’s R&D Budget
From Ad Hoc Advisory to Contractual Obligation
The FDA formally launched the PSG program in 2007, publishing guidance documents for individual drug products on an as-available basis. Early PSGs were useful but the program was inconsistent. There was no publication schedule, no commitment to volume, and no transparent pipeline. Companies planning multi-year development programs could not rely on guidance appearing before they needed it.
The Generic Drug User Fee Amendments of 2012 (GDUFA I) changed that structure fundamentally. Congress authorized the FDA to collect user fees from ANDA applicants and generic drug manufacturers, creating a dedicated revenue stream — roughly $1.6 billion across the GDUFA I cycle — specifically to fund the OGD’s review and research capacity. In exchange, FDA accepted binding performance commitments documented in a ‘goals letter’: ANDA review timelines, first-cycle approval targets, and, crucially, PSG issuance commitments.
GDUFA II (2017-2022) deepened these commitments. The agency promised PSGs for 90% of non-complex NCEs at least two years before the earliest lawful ANDA submission date — the four-year point from brand approval for Hatch-Waxman NCE exclusivity products. For the first time, a generic development team could look at a newly approved brand drug and know, with high probability, that a detailed regulatory roadmap would be published before the filing window even opened.
GDUFA III: The Current Framework (October 2022 to September 2027)
GDUFA III introduced specific PSG commitments for complex products for the first time. The commitment letter requires FDA to issue PSGs for 50% of newly approved complex products within two years of brand approval and 75% within three years. This commitment directly addressed the longest-standing complaint from complex generic developers: that scientific uncertainty persisted for too long, making it rational to delay investment and wait for a competitor to absorb the early-stage risk.
The GDUFA III framework also expanded the pre-ANDA meeting program in ways directly relevant to PSG-driven development. Four new or enhanced meeting types govern the PSG interaction specifically: the PSG Teleconference (for applicants whose active in vivo BE studies may be affected by a newly issued or revised PSG), the pre-submission PSG Meeting (for in-depth scientific discussion of a proposed alternative approach before filing), the post-submission PSG Meeting (for resolving PSG-related deficiencies during review), and the post-CRL Scientific Meeting (for structured discussion of how to address PSG-related complete response items). Each mechanism represents a formal, documented interaction with FDA that shapes the scientific record and reduces the probability of a subsequent deficiency on the same point.
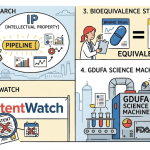
The GDUFA Research-to-PSG Pipeline
GDUFA user fees do not only fund review capacity. A dedicated portion funds the OGD’s Science and Research Program, which commissions and conducts laboratory research on complex BE methodologies. The outputs of this research — validated in vitro release methods, statistical frameworks for bioequivalence of locally acting drugs, physicochemical characterization protocols for nanomaterials — translate directly into new or revised PSGs.
This pipeline creates a specific competitive dynamic. When the FDA announces a research priority at its annual GDUFA Science and Research public workshop, industry participants gain early visibility into which complex products are likely to receive actionable PSGs over the following 12-36 months. A team that monitors these workshops and cross-references the topics with the Upcoming PSGs page can identify high-value targets well before a formal PSG publication — and before most competitors have recognized the opportunity.
4. Anatomy of a PSG: A Field-by-Field Decoding for Strategists
The Bioequivalence Recommendation: The Core Risk Signal
Every PSG leads with bioequivalence recommendations, and the type of BE study recommended is the most important single data point for a strategic risk assessment.
An in vivo pharmacokinetic (PK) study in healthy volunteers is the baseline for systemic drugs. The PSG specifies whether the study must be conducted fasting, fed, or both, and whether a crossover (same subjects receive both test and reference) or parallel design is required. A crossover fasting-only study for a well-characterized oral solid is a manageable, predictable cost. The issuance of the final ICH M13A guidance — which FDA adopted in 2024 — now allows a single BE study under either fasting or fed conditions for many immediate-release oral products, eliminating the prior default two-study requirement. A PSG reflecting this streamlined approach represents a direct cost reduction relative to any study designed before the M13A adoption.
In vitro methods are a distinct and more favorable class of recommendation. Dissolution testing under specified conditions (apparatus type, medium pH and composition, rotation speed, sampling intervals) is the standard in vitro tool for oral solid dosage forms. For complex formulations, the PSG may specify more demanding in vitro tests: the In Vitro Permeation Test (IVPT) for topical drug products, in vitro drug release testing under physiologically relevant conditions for depot injectables, or cascade impactor measurements for orally inhaled drug products (OIDPs). A PSG that recommends a validated in vitro path — particularly one that substitutes for a previously required in vivo or clinical study — can eliminate millions of dollars from the development budget and take years off the timeline.
BCS-based biowaivers occupy a separate category. The Biopharmaceutics Classification System categorizes drugs by aqueous solubility and intestinal permeability. Class I drugs (high solubility, high permeability) are eligible for a waiver of the in vivo BE study entirely, provided the generic formulation is qualitatively and quantitatively (Q1/Q2) similar to the RLD and passes comparative in vitro dissolution testing. A PSG confirming biowaiver eligibility for a target product makes the development path primarily a formulation and analytical chemistry problem, with no clinical site costs, no subject recruitment, and no bioanalytical outsourcing. The ICH M13B guideline, finalized in 2024, extends additional strengths biowaiver criteria for immediate-release solid oral dosage forms, allowing a single pivotal in vivo study to support approval of multiple strengths based on in vitro data alone.
Comparative clinical endpoint studies sit at the top of the complexity and cost scale. These are required when the drug acts locally at a site not reflected in systemic plasma concentrations — the skin, the eye surface, the gastrointestinal mucosa. A clinical endpoint study is essentially a truncated efficacy trial: it requires patient enrollment with the target disease, a clinically validated outcome measure (lesion count, visual acuity, symptom score), and statistical powering to demonstrate equivalence on that endpoint. Costs range from $2 million to $6 million per study, depending on indication and enrollment requirements. A PSG that provides a validated in vitro alternative to a clinical endpoint requirement is the single most commercially transformative document the OGD can publish for a complex product.
Waiver Options, Dissolution Methods, and Device Specifications
Beyond the primary BE recommendation, a PSG contains critical ancillary content. The dissolution method specifications — including dissolution medium pH, surfactant concentration and type, apparatus number, rotation speed, and time points — define the in vitro performance target a generic formulation must hit. These specifications are the direct output of FDA analytical research and are validated against the RLD’s in vivo performance data. A formulator who reads the PSG’s dissolution specifications before beginning prototype development can design directly toward the target, rather than iterating toward an unknown acceptance criterion.
For drug-device combination products — metered-dose inhalers (MDIs), dry powder inhalers (DPIs), auto-injectors, prefilled syringes — the PSG addresses device equivalence as a distinct requirement alongside drug BE. For OIDPs specifically, the PSG specifies in vitro device tests including actuator plume geometry, particle size distribution by cascade impaction, dose content uniformity through inhaler life, and delivered dose assessment. It may also require human factors studies demonstrating equivalent device usability between generic and reference, a requirement with distinct regulatory and IP implications given that device design patents are frequently listed separately from drug patents in the Orange Book.
5. The PSG Lifecycle: From Trigger Event to Quarterly Publication
What Initiates a New PSG
PSG development can be initiated by several distinct events, each carrying different strategic timing implications.
NDA approval is the most systematic trigger. GDUFA II and III commit FDA to issuing PSGs for newly approved NCEs and complex products on specific timelines after NDA approval. This creates a predictable queue: a development team following an NDA approval calendar can forecast, with high probability, when a PSG for that product will appear.
Industry request is the second major trigger. Companies can submit a Controlled Correspondence to OGD requesting development of a PSG for a specific product. This pathway is available for any approved drug lacking PSG coverage. The request should document the scientific complexity of the development challenge and ideally propose a BE methodology, which increases the probability that FDA will act. A citizen petition can serve the same function, though it carries higher visibility and may alert competitors to the requesting company’s portfolio interest.
GDUFA-funded research outcomes directly trigger PSG revisions. When an OGD research project validates a new in vitro method for a complex product, the output is a revised PSG incorporating that method. Monitoring the OGD’s annual research workshop presentations is the most direct way to anticipate these revisions before they appear in the Federal Register.
The Quarterly Publication Cycle and Its Strategic Implications
FDA publishes new and revised PSGs in batches, typically in February, May, August, and November. Each batch is announced in the Federal Register and made searchable on FDA’s PSG database. The Upcoming PSGs page is updated simultaneously to remove newly published PSGs and add any newly identified items in the development pipeline.
A team that monitors only the Federal Register notices is always working with published information — meaning every competitor is starting from the same document at the same time. The strategic advantage comes from monitoring the Upcoming PSGs page continuously, which lists specific products, RLD application numbers, and planned publication months 12 months in advance. This data allows a team to begin preliminary API sourcing discussions, IP freedom-to-operate assessments, and financial modeling before the formal PSG is published, compressing the time between PSG publication and a provisional Go/No-Go decision from weeks to days.
PSG Revision Categories and Their Portfolio Implications
FDA classifies PSG revisions into four categories. An editorial revision — correcting typos, updating external references — carries no development implication. A minor revision, which may add an alternative BE option or clarify a study design parameter, can be net positive for developers already in-program, since alternative pathways reduce cost or timeline.
An in vivo major revision adds new in vivo BE studies as necessary requirements for approval. This is the revision type that has historically been most disruptive to funded development programs. An in vitro major revision similarly adds in vitro requirements — less costly to address but still capable of creating formulation rework. A critical revision, the most severe category, adds BE evidence requirements reflecting a change in the safety or effectiveness profile of the drug product, affecting not only programs in development but all currently approved ANDAs for that product, including those already on the market.
The GDUFA III PSG Teleconference mechanism was created specifically to manage the in vivo major and critical revision scenarios. An applicant with a signed study protocol for an in vivo BE study that a new or revised PSG renders incomplete or superseded can request a one-hour teleconference with OGD to discuss the impact in real time. This meeting type does not guarantee relief, but it creates a formal documented exchange that may support a scientific justification for treating existing data as sufficient, or that clarifies the minimum additional work required. Teams that do not request this meeting forfeit the only early-stage negotiation point available to them.
6. IP Valuation and the PSG: How Regulatory Clarity Reprices a Drug Asset
The Core Valuation Problem in Generic Development
Generic drug assets are valued primarily on two variables: the revenue opportunity (market size, price, and market share at launch) and the probability of successfully navigating regulatory and legal hurdles. Standard pharma IP valuation frameworks — income approach using discounted cash flows, market comparables, cost approach for established assets — all depend critically on assumptions about the probability of approval and the timeline to market. These two inputs are precisely what a PSG moves most directly.
Before a PSG exists for a complex product, a valuation model must account for the possibility that no scientifically acceptable path to approval exists, that the required BE study design has not been validated by FDA, or that the agency will reject any approach not explicitly pre-agreed. Under these conditions, a conservative analyst assigns a technical probability of regulatory success (PTRS) of 40-60% for complex products. This uncertainty discount can render an otherwise large-revenue opportunity commercially unviable on a risk-adjusted basis.
When a detailed, final PSG is published, several things change simultaneously. The PTRS moves toward 85-90% for a competent development organization. The timeline to market becomes estimable with meaningful precision rather than wide uncertainty bounds. The likely cost of the pivotal BE study is now determinable based on the PSG’s specified study type. Each of these changes affects a different line in the rNPV model, and the combined effect can shift a project’s risk-adjusted net present value from negative to strongly positive — converting a speculative target into a financeable asset.
IP Valuation Framework for PSG-Enabled Generic Assets
The standard framework for valuing a generic drug opportunity in development applies rNPV methodology: project peak-year revenues, build a volume and price erosion model through the product’s competitive lifecycle, discount future cash flows at an appropriate cost of capital, and apply stage-specific probability weights to each cash flow.
The PSG’s contribution to this framework is precise. On the probability axis, the existence of a final PSG with a feasible BE pathway warrants an uplift of approximately 25-40 percentage points in PTRS relative to a complex product without guidance coverage. On the cost axis, the PSG’s study specification allows a more accurate R&D budget — typically $2 million to $10 million for a generic, but compressible toward $1-2 million for a simple oral solid with a biowaiver path, and expandable to $6-10 million for a complex OIDP or long-acting injectable requiring multiple specialized studies. On the timeline axis, a PSG-guided program with a competent CMC team can produce an ANDA-ready submission for a moderate-complexity product in 24-36 months; without guidance, the same program might require 48-72 months of iterative development with no guaranteed outcome.
For assets in licensing discussions or portfolio M&A transactions, the existence of a final PSG should be treated as a valuation premium factor analogous to a granted patent claim — it reduces execution uncertainty and supports a higher purchase price or upfront payment. An ANDA already filed against a PSG-covered product, at a stage with no outstanding CRL, carries materially lower risk than one in early-stage development for an uncovered product. IP teams negotiating deal terms should explicitly model the PSG-driven probability uplift as a separate line item in the valuation worksheet.
Brand Company Perspective: PSG Issuance as an IP Strategy Input
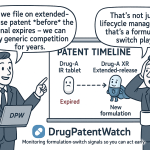
For innovator pharma IP teams, PSG publication is not just a generic industry event. The release of a PSG for a complex product signals FDA’s readiness to accept ANDAs, which directly accelerates the competitive threat calendar. A brand company’s IP lifecycle management strategy — decisions about when to file continuation patents, when to add new Orange Book listings, whether to pursue new formulation patents or method-of-use claims — should be timed partly against PSG publication events.
A PSG that validates an in vitro BE pathway for a previously all-clinical-endpoint product effectively eliminates the barrier that has been protecting the brand’s market position. Brand teams that have been relying on the practical inaccessibility of the development path as a de facto extension of market exclusivity need to recognize that a new PSG resets that calculation. The brand’s remaining protection comes down to the Orange Book patent portfolio, any active regulatory exclusivities, and any REMS programs that might complicate substitution.
7. PSG as Market Signal: The rNPV Math Behind the Starting Gun
Price Erosion Economics and Why Timing Is Everything
The economic logic of generic drug development is built on price erosion curves that are steep, fast, and unforgiving. A single generic entrant typically captures a 30-39% price reduction against the brand. Two or three competitors move that discount to the 50-70% range. Four to six competitors push the discount to roughly 80%. With seven to ten competitors in the market, prices sit at approximately 90% below brand, and gross margins on commodity oral solids fall to 20-35%. At ten or more competitors, the market may become unsustainable for all but the highest-volume, lowest-cost manufacturers.
These dynamics mean that the value of a generic drug program is concentrated in the first 12-24 months of competitive entry. A company that launches six months ahead of its second competitor operates in a near-duopoly during those months, with pricing power and market share capture that may represent the majority of the program’s total lifecycle value. A company that launches six months late may enter a market with three competitors already established and find that the price has eroded past the point of profitability.
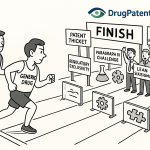
This timing premium transforms PSG publication into a starting gun. From the moment a PSG is published, every month of development time is a month in which competitors are also working. The first mover advantage in generic drug development belongs not to the largest company, but to the most operationally disciplined one — the team that read the PSG first, built its development plan fastest, and executed most cleanly against the FDA’s specified methodology.
First-Cycle Approval Rates and Their Financial Value
Roughly 20% of ANDAs receive first-cycle approval — meaning their first FDA review results in a full approval without a CRL. The remaining 80% require at least one additional review cycle. Each cycle adds, on average, 10-14 months to the clock and carries its own set of amendment costs, response preparation fees, and opportunity costs. The financial value of a first-cycle approval, beyond the direct cost savings, is the timeline compression: a first-cycle approval can bring market launch 18-24 months earlier than a program that cycles twice through deficiencies.
Adherence to PSG recommendations is the most direct and controllable driver of first-cycle approval probability. An ANDA that follows the PSG’s BE methodology, dissolution specifications, and device testing requirements to the letter removes the largest class of technical deficiencies — bioequivalence study design disputes — from the review conversation. The remaining potential deficiency areas (CMC completeness, facility inspection readiness, patent certification accuracy) are separately manageable. A team that treats the PSG as a checklist to be executed perfectly, rather than a starting point for creative interpretation, materially increases its first-cycle probability.
8. Integrating PSG Intelligence with Patent and Competitive Data
The Orange Book as the Foundational Legal Layer
The FDA’s ‘Approved Drug Products with Therapeutic Equivalence Evaluations’ — the Orange Book — lists every patent and exclusivity period associated with each approved brand drug. It specifies four types of patent certification an ANDA filer must make: Paragraph I (patent already expired), Paragraph II (no relevant patent listed), Paragraph III (the applicant will wait for patent expiration before launching), or Paragraph IV (the listed patent is invalid, unenforceable, or not infringed by the proposed generic).
The Orange Book patent listing is the legal clock that governs when a generic can launch. A Paragraph III certification sets a hard launch date, the patent expiration date, with no legal risk but significant financial opportunity cost. A Paragraph IV certification initiates the most high-stakes process in the generic industry: it is deemed an act of infringement under 35 U.S.C. § 271(e)(2), giving the brand company 45 days to file a patent infringement suit and triggering an automatic 30-month stay on FDA final approval if they do.
The Orange Book does not capture all relevant IP. Method-of-use patents, manufacturing process patents, and formulation patents are sometimes listed; device patents for combination products may not be. Freedom-to-operate analysis by qualified IP counsel must cover not just Orange Book listings but the full patent landscape around the RLD, including CPC-classified patent family analysis for related inventions.
The Integrated Portfolio Workflow
The optimal generic drug portfolio selection process runs four intelligence streams simultaneously, each informing the others before a Go/No-Go decision is reached.
The first stream is commercial market intelligence: brand drug revenue, patient population size, formulary positioning, payer mix, and projected generic penetration rate. This stream defines the gross revenue ceiling for the generic opportunity.
The second stream is regulatory intelligence, centered on the PSG. The PSG defines the technical pathway, the cost of the pivotal BE study, the minimum CMC investment, and the likely timeline to an approvable submission. It sets the denominator in the return-on-investment calculation.
The third stream is IP intelligence. This covers the Orange Book patent estate for the RLD, the broader landscape of unlistable patents that might support a design-around strategy, the history of previous Paragraph IV litigation involving the brand company, and the outcome of any inter partes review (IPR) proceedings challenging listed patents.
The fourth stream is competitive intelligence: how many ANDAs have been filed or approved for the same RLD, who the filers are, which have already received tentative approval, and whether any first-filer exclusivity arrangements are in place. Platforms like DrugPatentWatch aggregate ANDA application status, Paragraph IV certifications, patent challenge litigation records, and patent expiration calendars into a single queryable dataset, which makes this stream materially faster to construct than it was a decade ago when the data was distributed across multiple FDA public databases.
The integrated decision matrix scores each target on all four streams. A product that is commercially large, has a clear and low-cost PSG pathway, faces a weak patent portfolio with credibly challengeable claims, and has limited ANDA competition represents the canonical high-value opportunity. Any one dimension being unfavorable does not necessarily kill the project — a strong commercial case can justify a difficult PSG pathway, and a weak patent portfolio may support a Paragraph IV challenge even when the development path is technically demanding — but the scoring of all four dimensions simultaneously forces explicit trade-off discussions rather than defaulting to single-dimension analysis.
9. The Paragraph IV Gambit: How PSGs Underwrite the First-to-File Decision
The 180-Day Exclusivity Mechanism
The Hatch-Waxman Act grants the first ANDA filer to include a Paragraph IV certification a 180-day period of market exclusivity from the date of first commercial marketing. During this window, the FDA cannot grant final approval to any other ANDA for the same drug. The result is a temporary duopoly — the brand and the first generic — during which the first-filer can price substantially above where the eventual fully-competitive market will settle.
The financial value of 180-day exclusivity is a function of the brand’s revenue size and the first-filer’s ability to convert brand market share during the window. For a blockbuster drug with $1-2 billion in annual brand sales, 180-day exclusivity can generate $150-400 million in gross margin for the generic first-filer, depending on the brand’s defense strategy (authorized generics, patient loyalty programs, and DTC marketing all reduce but rarely eliminate first-filer value). For smaller products, the exclusivity value may not justify the litigation cost and the development risk.
The PSG’s role in this calculation is structural. No rational capital allocator will commit $5-10 million in expected patent litigation costs — and potentially $30-50 million over a protracted case — without high confidence that the drug can be successfully developed and approved. A Paragraph IV filing is a two-front commitment: scientific and legal. The PSG resolves the scientific front. It validates that a developable, approvable path exists and allows the development budget to be forecasted with accuracy. This lets the decision-maker isolate and assess the legal risk cleanly, rather than having to price both scientific uncertainty and legal uncertainty simultaneously.
The NCE-1 Filing Window and GDUFA PSG Timing
For drugs protected by the five-year New Chemical Entity (NCE) exclusivity, the earliest lawful ANDA submission date with a Paragraph IV certification is four years after approval — the ‘NCE-1’ window. GDUFA II and III committed FDA to publishing PSGs for 90% of non-complex NCEs at least two years before this window opens.
This commitment produces a defined sequence. Brand drug approved at Year 0. PSG published at no later than Year 2. Development program initiated in Year 2 based on the PSG. ANDA filed in Year 4 at the NCE-1 opening. Review clock runs for approximately 12 months under GDUFA III targets. Tentative approval at approximately Year 5. Full approval at Year 5 if patent litigation resolves, or launch at risk upon court determination. This structured timeline — with PSG publication built into the sequence as a contractual obligation — makes long-range Paragraph IV strategy plannable in a way that was not possible before GDUFA.
10. Complex Generics Deep Dive: OIDP, Topicals, Long-Acting Injectables, and Combo Products
The Structural Under-Representation of Complex Generics
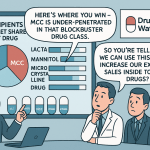
Complex drug products account for roughly a quarter of all approved brand drugs but only 13% of approved generics. The gap exists because demonstrating therapeutic equivalence for locally acting, non-oral, or drug-device combination products requires scientific approaches that cannot be borrowed directly from the standard oral solid BE playbook. Each complex product category has its own methodological challenges, and until GDUFA-funded research generates validated methods for those challenges, viable PSGs cannot be written.
The commercial implication of this gap is significant. Complex generic markets typically have two to four competitors at launch rather than eight to twelve, because the barriers to entry filter out all but the most technically capable applicants. Gross margins on approved complex generics commonly run 60-75% at steady state, versus 20-35% for conventional oral solids. The reward for navigating the complexity is sustained pricing power, not just the first-mover window available in commodity generics.
Orally Inhaled Drug Products (OIDPs)
OIDPs represent the most technically demanding class of complex generics. Products in this category include MDIs, DPIs, and nebulized solutions. The BE standard for OIDPs requires demonstration of both systemic bioequivalence (PK equivalence in healthy volunteers for the systemic component of the drug) and local equivalence (equivalence in drug delivery to the lungs). The FDA’s OIDP BE framework is a ‘totality of the evidence’ approach, requiring a concordant battery of in vitro device performance tests plus an in vivo PK study as the primary pivotal evidence.
Device equivalence for OIDPs adds a distinct layer of complexity. The generic device must produce aerosol performance characteristics — aerodynamic particle size distribution (APSD) measured by multi-stage cascade impaction, fine particle fraction, mass median aerodynamic diameter — that are within specified tolerances of the RLD device throughout the product’s labeled dose count range. Meeting these tolerances often requires reverse-engineering the device to a degree that approaches independent mechanical design, which in turn raises infringement exposure on device design patents not listed in the Orange Book.
The PSG for an OIDP specifies all of these requirements in full: the number and type of in vitro tests, the statistical approach for APSD equivalence, whether a single-dose or multiple-dose PK study is required, and any device human factors study requirements. A team designing an OIDP development program without current review of the PSG risks building a device that passes internal testing criteria but fails the FDA’s specified in vitro equivalence standard.
Topical Drug Products
Topical generics have historically required comparative clinical endpoint studies because systemic plasma concentrations do not reflect local drug activity at the skin. A clinical endpoint study for a topical corticosteroid, antifungal, or acne product typically requires enrollment of 200-600 patients with the relevant dermatological condition, measured against a clinically validated endpoint, with a two-arm parallel design comparing test and reference products.
GDUFA-funded research has progressively validated in vitro alternatives for topical BE. The IVPT, which measures drug flux through excised skin or reconstructed human epidermis under conditions that mimic in vivo exposure, has been validated for several active ingredient classes. Dermatopharmacokinetics (DPK) methods, measuring drug concentration in the stratum corneum by tape-stripping, have been validated for others. A PSG that specifies an IVPT or DPK pathway in lieu of a clinical endpoint study converts a $2-6 million clinical program into a $300,000-600,000 in vitro study, fundamentally changing the commercial viability threshold for the project.
Long-Acting Injectables (LAIs) and Microspheres
Depot injectables and microsphere formulations present BE challenges that standard PK comparisons cannot resolve. The release profile from a depot injection can span days to months. The FDA requires characterization of particle size distribution (volume-weighted, by laser diffraction and dynamic light scattering), encapsulation efficiency, and in vitro drug release rate under physiologically relevant conditions in addition to in vivo PK studies for many LAI products.
For microsphere formulations, PSGs typically require a comprehensive physicochemical characterization package demonstrating sameness of the drug substance within the matrix: polymer molecular weight distribution, drug loading, residual solvent levels, and release kinetics that match the RLD across multiple dissolution time points. The in vitro release method specification in the PSG defines the dissolution apparatus, medium composition, temperature, and sampling schedule. Matching the specified in vitro release profile is both a regulatory requirement and a formulation target that guides the entire development program.
11. Case Study: Advair Diskus and the Multi-Decade OIDP Playbook
The Product and the Patent Position
GlaxoSmithKline’s Advair Diskus (fluticasone propionate/salmeterol xinafoate inhalation powder) reached peak global sales exceeding $8 billion annually, making it one of the most valuable pharmaceutical products in history. The combination DPI for asthma and COPD was protected by an extensive patent portfolio covering the active ingredients, the combination, the formulation, and the proprietary Diskus device. From a generic development perspective, it was simultaneously the most attractive and most technically formidable target in the industry.
IP Valuation Context: The Advair IP estate illustrates the concept of ‘layered exclusivity.’ By the time the primary compound patents expired, GSK had filed continuation patents covering specific formulation ratios, lactose carrier characteristics, and dose delivery parameters. Device design patents on the Diskus covered the inhaler’s internal air dispersion mechanism and foil strip construction. None of these continuation or device patents altered the basic chemical structure of the drugs, but each created a potential infringement theory for a generic developer attempting to replicate Diskus device performance. The Orange Book listed multiple patents with different expiration dates, creating a staggered exclusivity runway that extended the effective period of reduced competition well beyond any single expiration date.
The Development Challenge
Replicating Advair Diskus required solving three simultaneous problems: a compatible micronized powder blend of two active ingredients with specified particle size distributions, a blending process with a lactose carrier that reproducibly delivers the correct fine particle fraction to the lung, and a device that produces in vitro APSD equivalence to the Diskus across its labeled 60-dose range under the conditions specified in the FDA’s PSG.
The PSG for fluticasone propionate/salmeterol xinafoate inhalation powder specified a multi-step totality of evidence approach: a battery of in vitro device performance tests (APSD by cascade impaction, delivered dose uniformity through inhaler life, device resistance) and a pivotal in vivo PK study demonstrating systemic bioequivalence. Device human factors evaluation was required to demonstrate equivalent usability between the proposed generic device and the Diskus.
Mylan (now Viatris) initiated a large-scale clinical equivalence study in asthma patients as early as 2014 as part of its development program, before the PSG had evolved to its current in vitro-plus-PK structure. After multiple development cycles and PSG updates over nearly a decade, the FDA approved Mylan’s Wixela Inhub as the first generic Advair Diskus in January 2019. Hikma and Teva received subsequent approvals in late 2020 and 2021, respectively.
Lessons for Portfolio Teams
The Advair case demonstrates that a PSG for a complex OIDP can be executed — but the development timeline is measured in years, not quarters. The PSG defines the finish line, but the technical distance to that line for a device-dependent product may require iterative device engineering over 4-8 years. Portfolio teams should model realistic development timelines for OIDP targets using the PSG requirements as the input, not a generic ‘complex product’ timeline assumption. The financial model must accommodate the possibility that the PSG will be revised during the development period, requiring PSG Teleconference engagement to assess impact.
The IP dimension of the Advair case also illustrates why patent thicket analysis cannot be delegated to a single search. The relevant IP for a complex combination OIDP spans compound patents, formulation patents, device design patents, and method-of-use patents, each with distinct expiration dates, strength profiles, and challenge strategies. The PSG’s publication confirmed the regulatory path; the legal team’s patent-by-patent analysis determined whether that path was legally traversable.
12. Case Study: Restasis and the GDUFA Research-to-PSG Pipeline
The Product and the Scientific Barrier
Allergan’s Restasis (cyclosporine ophthalmic emulsion, 0.05%) generated approximately $1.5 billion annually at peak and had no generic competition for nearly two decades after its 2003 approval. The active ingredient, cyclosporine, is a calcineurin inhibitor that reduces ocular surface inflammation in patients with chronic dry eye disease. It acts locally on the conjunctival epithelium; plasma concentrations after topical ophthalmic administration are typically undetectable. This meant that a standard systemic PK bioequivalence study was not only scientifically inappropriate — it was methodologically impossible.
The only available path to generic approval, at the time Restasis was approved, was a comparative clinical endpoint study measuring improvement in a validated dry eye disease endpoint (e.g., corneal staining score, conjunctival goblet cell density). A clinical endpoint study of this type requires enrollment of several hundred patients with confirmed aqueous-deficient dry eye, a placebo-controlled or head-to-head design with the RLD, and a primary endpoint sensitive enough to detect equivalence. Cost estimates for such a study ran $3-5 million or more, and the scientific uncertainty around endpoint selection and responder rate made the probability of study success difficult to estimate — particularly because Restasis’s own pivotal trials showed a relatively modest treatment effect, raising questions about whether a generic BE study would be powered adequately.
IP Valuation Context: Allergan’s IP strategy for Restasis became one of the most scrutinized patent docket disputes in pharmaceutical history. The company attempted in 2017 to assign six Restasis formulation patents to the Saint Regis Mohawk Tribe to exploit tribal sovereign immunity from inter partes review proceedings at the Patent Trial and Appeal Board (PTAB). A federal district court subsequently found the patents invalid on obviousness grounds in October 2017, and the Federal Circuit affirmed. The PTAB proceedings and litigation generated substantial IP valuation uncertainty: the formulation patents were being challenged while the real barrier to generic entry was not legal (the patents were being cleared) but scientific (no validated BE pathway existed). This separation of the legal exclusivity question from the scientific access question is characteristic of complex generics, where patent cliffs and PSG issuance are independent events that must be tracked separately.
The GDUFA Research Investment
Recognizing that the Restasis problem was too large and too scientifically pre-competitive for individual companies to solve, OGD dedicated GDUFA research resources to developing validated methods for cyclosporine ophthalmic emulsion characterization and bioequivalence. FDA supported 16 separate research projects on this product over approximately a decade, covering emulsion physicochemical characterization (globule size distribution by dynamic light scattering, viscosity, zeta potential, surface tension), in vitro drug release using modified United States Pharmacopeia (USP) apparatus, and statistical frameworks for bioequivalence determination based on in vitro data.
The PSG for cyclosporine ophthalmic emulsion, 0.05%, went through multiple draft and revision cycles during this period. Each revision reflected new research outputs, progressively building a more complete in vitro BE framework. The final PSG replaced the clinical endpoint requirement with a totality-of-evidence approach combining comprehensive physicochemical characterization with in vitro drug release testing. This approach eliminated the need for a patient enrollment study, reducing the pivotal study cost by roughly an order of magnitude.
Viatris (formed by the 2020 merger of Mylan and Pfizer’s Upjohn division) received FDA approval for the first generic Restasis in February 2022, with an immediate commercial launch. FDA’s approval announcement credited the GDUFA science and research program directly for making the approval possible. The approval arrived years after the primary Restasis patents had been adjudicated — illustrating that the scientific barrier to complex generic entry can persist long after the legal barrier falls, and that PSG-enabling research is the mechanism by which this gap closes.
13. Navigating PSG Revisions Mid-Development: The GDUFA III Rescue Toolkit
Why Revision Risk Is a Real Portfolio Problem
A funded generic development program is not immunized against regulatory change. When FDA publishes a revised PSG that adds new BE study requirements — a major in vivo revision or a critical revision — programs already in clinical or in vitro studies may face a choice between continuing under an approach FDA has superseded or stopping to conduct additional work before filing. Before GDUFA III, there was no formal mechanism for managing this scenario. Companies either filed anyway and addressed the deficiency in a CRL cycle or absorbed the cost of stopping and restarting.
The financial exposure from a mid-development PSG revision is material. If a $2 million in vivo PK study is already complete and a new PSG requires a second, differently designed study, the program incurs roughly $4 million in study costs for studies that might each have cost $2 million if the final PSG had been available at program initiation. If the program is 24 months into development when the revision occurs, the additional time required to design, conduct, and report the new study may delay filing by 12-18 months — representing a timeline hit with direct NPV consequences.
The GDUFA III Toolkit
GDUFA III created three specific mechanisms to address this scenario.
The PSG Teleconference is available to any applicant or prospective applicant that has commenced an in vivo BE study (protocol signed by study sponsor and/or CRO) when a new or revised PSG is published. This one-hour meeting provides a structured forum for discussing the PSG’s impact on the existing program. The applicant presents the study design, the data generated to date, and its scientific rationale for why existing data may satisfy the new or revised requirements. FDA provides real-time feedback. The meeting is not a binding commitment by either party, but the scientific discussion it enables — and the meeting record it creates — provides the evidentiary foundation for a subsequent scientific justification in a controlled correspondence or ANDA submission.
If the teleconference identifies substantive open issues, the applicant can escalate to a pre-submission or post-submission PSG Meeting. These are more formal scientific meetings with broader FDA reviewer participation, intended for cases where a company is proposing an alternative scientific approach not described in the PSG and needs in-depth technical feedback before committing to the approach in a filing. The meeting record from a post-submission PSG Meeting may support the company’s scientific justification in response to a CRL deficiency, creating a stronger documented basis for the alternative approach than a statement in the ANDA itself.
Teams whose development programs are far advanced at the time of a PSG revision should also evaluate whether an ANDA filing based on the original PSG methodology is defensible if accompanied by a comprehensive scientific bridge argument explaining why the pre-revision methodology is consistent with the regulatory standard. FDA has accepted such arguments in some cases, particularly where the substantive scientific standard has not changed and the revision reflects a preference for an alternative method rather than a correction of an identified deficiency in the previous approach.
14. When a Clear PSG Is Not Enough: Pitfalls That Sink Funded Programs
Formulation and Manufacturing Failures
A PSG tells you what to prove; it does not tell you how to make the product. The formulation challenge for a complex generic can be enormous even when the BE standard is well defined. Replicating the drug release profile of an extended-release oral solid requires understanding the RLD’s polymer matrix composition — information not disclosed in the package insert. Replicating the particle size distribution of a nanosuspension ophthalmic requires milling equipment and process controls that may not be available at pilot scale and must be validated at commercial scale before filing.
Scale-up failures are a common cause of development program delay even in PSG-covered products. FDA’s 2011 process validation guidance requires commercial-scale manufacturing data in the ANDA. A company that optimizes its formulation at 10-kg lab batches and then encounters a manufacturing divergence at 200-kg commercial batches must return to formulation development, rerunning in vitro characterization and potentially the pivotal BE study against a newly manufactured batch. Process analytical technology (PAT) and quality-by-design (QbD) approaches reduce this risk but require investment in analytical infrastructure that smaller generic developers sometimes defer.
API Supply Chain Constraints
The active pharmaceutical ingredient for a complex generic may be chemically accessible but commercially unavailable. Cyclosporine is commercially synthesized by a small number of API manufacturers globally. Glatiramer acetate — a complex mixture of polypeptides for which multiple PSGs have been issued — requires specialized polymerization and fractionation process knowledge that is effectively proprietary to a handful of manufacturers. An ANDA applicant that cannot secure a reliable API supply from a qualified Drug Master File (DMF) holder cannot submit a complete application regardless of how good its formulation and BE data are.
For complex APIs in this category, API supply strategy is a pre-development decision, not a development-phase logistics question. A team that identifies a commercially attractive PSG-covered target should perform API supply chain diligence — auditing available DMF holders, assessing process capability and GMP compliance, and potentially contracting API supply before finalizing the development decision — before committing the full development budget.
Political and Administrative Disruptions to PSG Publication
The GDUFA PSG publication schedule is contractual but not immune to disruption. Early 2025 saw a material slowdown in FDA guidance publication activity across all centers, attributed to staffing reductions, administrative reorganization, and budget pressure in the first months of the new administration. The quarterly PSG batches that generic developers rely on for pipeline planning were delayed, creating uncertainty for teams whose development timelines were synchronized to expected PSG publication dates.
This administrative risk is a real factor in portfolio planning. A team whose development initiation depends on an upcoming PSG that is delayed by one or two quarterly publication cycles faces a corresponding delay in its filing timeline. Risk-adjusted portfolio models for complex generics should include a PSG publication delay scenario with appropriate probability weight, particularly in periods of administrative transition or budget constraint at FDA.
15. Investment Strategy for Institutional Analysts
Screening Generic Drug Equities Using PSG Intelligence
Institutional analysts covering generic pharmaceutical equities — Teva Pharmaceuticals, Viatris, Hikma, Amneal, Sun Pharma, Dr. Reddy’s — can use public PSG data as a forward-looking signal for product pipeline value. A generic company with a large proportion of its filed ANDA pipeline in PSG-covered complex products has a structurally higher-quality pipeline than one dependent primarily on commodity oral solids, because the complex products face fewer competitors at launch and sustain pricing longer.
The Upcoming PSGs page on FDA.gov, cross-referenced against publicly available ANDA filing data, allows an analyst to identify which companies have pending applications for products that are about to receive final PSG coverage. A company holding a first-to-file Paragraph IV ANDA for an RLD that is about to receive a PSG that validates a previously unclear BE pathway is potentially holding a significantly undervalued asset — the PSG publication may be the event that converts a tentatively approved or pending application into a commercially launchable product.
Key metrics to monitor in this framework: the number of complex ANDA approvals as a percentage of total approvals (a quality indicator), the company’s reported Paragraph IV first-filer pipeline count, the share of the pipeline in PSG-covered therapeutic categories (inhalers, topicals, LAIs), and management commentary on the timing of upcoming complex generic launches relative to PSG publication dates.
M&A and Licensing Deal Considerations
Licensing deals and M&A transactions involving generic drug portfolios should include explicit PSG due diligence as a standard component. For each ANDA or development-stage asset in the target portfolio, the buyer’s team should assess: whether a final or draft PSG exists, when it was last revised, whether the development program’s BE methodology matches the current PSG, whether any pending PSG revisions are listed on the Upcoming PSGs page that could affect the program, and whether any PSG Teleconferences or PSG Meetings have been requested or held for the program.
A development-stage ANDA for a complex product without current PSG coverage should be assigned a material risk discount in a deal valuation, since a future PSG may specify methodology inconsistent with the work already done. An ANDA in late-stage development that follows a recently revised PSG with no further revisions pending commands a premium — it represents a fully de-risked regulatory path.
Key Investment Risk Factors Specific to PSG-Driven Development
Regulatory methodology risk — the possibility that a PSG revision will require additional studies — remains real even under GDUFA III. Companies that do not actively monitor the Upcoming PSGs page or attend GDUFA research workshops are the most exposed to surprise revision risk.
Competition concentration risk in complex generics is real in both directions. Low initial competition protects pricing in the launch window, but a market with only two or three competitors is also one where a single additional approval can compress margins significantly. Track ANDA filing pipelines for competing products, not just market launch timelines.
API supply concentration creates systemic risk for certain complex active ingredients. An FDA warning letter or import alert affecting a key API manufacturer can simultaneously affect multiple ANDA holders dependent on that supplier, creating short-term pricing recoveries and long-term supply uncertainty.
16. The Future Roadmap: ICH M13A/B, PBPK Modeling, and Propellant Transitions
ICH M13A and M13B: Global Harmonization of the BE Standard
The International Council for Harmonisation ICH M13A guideline — on bioequivalence for immediate-release solid oral dosage forms — was finalized in 2024 and adopted by FDA, EMA, and Health Canada simultaneously. Its primary practical effect is to eliminate the default dual fasting-and-fed BE study requirement for many immediate-release products, replacing it with a single study under either condition where the scientific rationale supports it. For generic developers with global programs, the adoption of M13A into regulatory practice means a single BE study design can satisfy both FDA and EMA requirements, eliminating the cost and timeline of running separate studies for each jurisdiction.
ICH M13B, finalized in the same period, extends biowaiver criteria for additional strengths of immediate-release solid oral dosage forms. A company that conducts a pivotal in vivo BE study on the primary strength can support approval of two, three, or four additional strengths using in vitro dissolution data alone, provided the criteria specified in M13B are met. For a multi-strength product, this biowaiver provision can eliminate two to four additional in vivo studies from the development program — a cost saving that is directly quantifiable from the PSG’s strength-specific recommendations.
PSGs for products newly covered or revised in light of M13A/B should be read in the context of these harmonized standards. A PSG published before M13A adoption may still specify a dual fasting-and-fed study design by default; current FDA practice may allow a single-study approach under the M13A rationale. Applicants planning development programs for these products should confirm current FDA thinking via Controlled Correspondence before finalizing study protocols, since the PSG may not yet have been revised to reflect the M13A adoption.
Physiologically Based Pharmacokinetic Modeling and the Model-Integrated Evidence Pathway
FDA’s Office of Generic Drugs has been building the scientific basis for model-integrated evidence (MIE) — the use of physiologically based pharmacokinetic (PBPK) models and other quantitative methods to generate or supplement BE evidence. PBPK models simulate drug absorption, distribution, metabolism, and elimination across virtual patient populations, allowing prediction of bioequivalence under conditions that would be impractical to study in actual clinical trials: extreme pH conditions, drug-drug interactions, pediatric or geriatric populations.
The regulatory application of MIE in generic drug development remains at an early stage, but the trajectory is clear. FDA has used PBPK models to support biowaiver requests for specific strengths, to justify study design simplifications (e.g., eliminating fed-state studies for BCS Class I drugs with low food effect), and to characterize the clinical significance of in vitro dissolution differences. Future PSGs for appropriate product classes may explicitly list PBPK-supported approaches as acceptable alternatives to specific in vivo studies.
For complex products where conventional BE studies are expensive, scientifically ambiguous, or ethically problematic, the MIE pathway represents the most significant pending improvement in development economics. The companies best positioned to exploit this pathway are those with established PBPK modeling capabilities — either in-house or via qualified academic or CRO partners — and with the regulatory affairs experience to document model validation and uncertainty assessment to FDA’s expected standard.
MDI Propellant Transition: A Structural PSG Revision Wave
The phaseout of hydrofluorocarbon (HFC) propellants in metered-dose inhalers — driven by the Kigali Amendment to the Montreal Protocol and its adoption into domestic environmental policy — is generating a wave of PSG revisions for OIDP products currently formulated with HFC-134a. The replacement propellant, HFC-152a, and future low-GWP propellants (including HFO-1234ze) change the physical properties of the aerosol plume, particle size distribution, and dose delivery characteristics relative to HFC-134a formulations.
For generic OIDP developers, this transition creates both a risk and an opportunity. The risk: a generic OIDP approved against an HFC-134a RLD may need to be reformulated as the RLD transitions to a new propellant, requiring new in vitro and potentially in vivo equivalence data. The opportunity: a brand RLD that transitions to a new propellant formulation may functionally reopen the generic development timeline, since the generic developer’s previously approved product may qualify for its own supplemental application ahead of new competitors rather than having to begin development from scratch.
The FY2025 GDUFA Science and Research workshop identified the propellant transition as an active research priority. PSG revisions for affected products are expected in the 2025-2027 period, and teams with pending OIDP programs should monitor the Upcoming PSGs page for revision notices affecting their target products specifically.
17. FAQ for Regulatory, IP, and Portfolio Teams
Q: A PSG was published two years ago for our target product and we have not yet filed. Should we re-check for a revision before finalizing our study protocol?
Yes. Access the current PSG directly from FDA’s database and compare it to the version your team reviewed during program initiation. The Upcoming PSGs page may also list a revision in progress for the product. If a revision is listed but not yet final, contact your regulatory affairs counsel about submitting a Controlled Correspondence to FDA asking whether it is advisable to proceed with the current study design before the revision is published, or whether a PSG Meeting might be appropriate.
Q: Our target product has no PSG listed in FDA’s database and nothing on the Upcoming PSGs page. How should we assess the development risk?
The absence of a PSG creates undifferentiated scientific risk — any BE methodology you develop may or may not satisfy FDA’s expectations. Evaluate whether the product fits within a general BE guideline (e.g., the 2003 Guidance for Industry on Bioavailability and Bioequivalence Studies for Orally Administered Drug Products), whether comparable products have PSGs from which you can extrapolate, and whether there is a scientific basis for a BCS biowaiver. If none of these applies, consider submitting a Controlled Correspondence requesting PSG development, or a formal request via the pre-ANDA meeting program. Factor the absence of a PSG into your PTRS estimate with a significant downward adjustment.
Q: How should the discovery of a competitive ANDA filing via DrugPatentWatch change the priority of a PSG-covered target in our portfolio?
It depends on first-filer status. If the competitor has filed a Paragraph IV certification and you have not, they are potentially in line for 180-day exclusivity. This does not necessarily kill the opportunity — many profitable generics are approved outside the 180-day exclusivity window — but it changes the financial model materially. Update your revenue projection for the product to reflect reduced first-mover pricing power and accelerated price erosion timing. If the product’s rNPV is still positive under these revised assumptions and you have the formulation and regulatory capacity to execute quickly, proceeding may still be rational. If the market is small enough that the exclusivity difference is decisive, redeploy resources to a target where first-filer status is still achievable.
Q: We received a CRL citing our BE study design as not consistent with the PSG. The study was designed before the PSG’s most recent minor revision. What is the most effective path to resolution?
Request a post-CRL Scientific Meeting with FDA. Prepare a detailed scientific bridge argument demonstrating that your study design — while not identical to the current PSG recommendation — generates data that meets the regulatory standard the PSG is designed to achieve. If the revision was minor and added an alternative BE option rather than changing the core methodology, the case for your existing data should be strong. If the revision changed the primary methodology in ways that create a genuine scientific gap, assess whether a bridging study is possible — a smaller, targeted study designed to address the specific gap identified in the CRL — rather than a full repeat. Document the timeline and cost of both options for the Go/No-Go decision.
Q: How do we handle a complex product where the PSG exists but was written based on research conducted before recent advances in our in vitro characterization capability? We believe our methodology is superior.
Submit a Controlled Correspondence outlining your proposed alternative methodology, the scientific basis for your belief that it is equivalent or superior to the PSG’s recommendation, and any supporting validation data. If OGD agrees in principle, request a pre-ANDA product development meeting to present the full data package and document FDA’s feedback before proceeding to a pivotal study. If FDA disagrees, you can still proceed with the PSG-recommended methodology while preserving the alternative approach for a future PSG comment period. Under no circumstances should you file an ANDA based solely on a non-PSG-consistent methodology without prior OGD feedback — the CRL risk is high and the review delay costly.
This article is intended for regulatory, IP, and portfolio strategy professionals. It does not constitute legal or investment advice. Patent analysis and investment decisions should be reviewed with qualified IP counsel and financial advisors. All FDA data referenced is public and available at fda.gov.