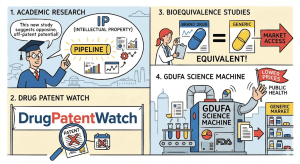
Generic drug development runs on borrowed science. The molecule has already been discovered, the clinical benefit already proven. The scientific burden shifts entirely to a different set of disciplines: analytical chemistry, pharmaceutical engineering, formulation science, and the regulatory expertise required to satisfy an FDA review that scrutinizes every step. Academic research supplies most of that burden, operating as the sector’s de facto R&D utility. This pillar page maps every dimension of that relationship, from the foundational IP asymmetries that shape it to the specific methodologies being built in university labs that will determine who captures the next wave of complex generics revenue.
I. Two Industries, One Science Base: Rethinking Academia’s Pharmaceutical Role
Pharmacy schools and pharmaceutical sciences departments produce two very different kinds of value for the drug industry. The version most people know is target-to-molecule discovery: NIH-funded basic research that identifies a disease pathway, generates a novel compound, and eventually feeds an IND filing at a major pharma company. The second version, less discussed but economically enormous, supplies the technical infrastructure that generic manufacturers need to prove therapeutic equivalence to already-approved drugs. These two functions require entirely different institutional capabilities and produce entirely different intellectual property profiles.
The Innovator Pipeline: Discovery as the Core IP Asset
For brand pharmaceutical companies, academic collaboration is primarily a source of novel composition-of-matter patents. A university lab identifies a new biological target, publishes the discovery, and either licenses the underlying IP to a pharma company through its technology transfer office or spins out a biotech that is eventually acquired. The patent covering that new molecular entity (NME) then anchors years of market exclusivity, typically 20 years from filing, though effective exclusivity is substantially shorter once you net out development time.
The economics are extreme in both directions. Development costs for a single NME regularly exceed $2.5 billion when accounting for failure rates that run roughly 90% through Phase III. The successful fraction commands premium pricing backed by that patent protection. The core IP asset is the molecule itself, and universities that produce it through publicly funded research capture value through licensing royalties, milestone payments, and equity stakes in spinouts.
The entire innovator IP valuation framework, as applied to academic-generated discoveries, rests on composition-of-matter exclusivity. Method-of-use patents and formulation patents layer on top, but the foundational value sits in the composition claim. Patent term extensions under Hatch-Waxman Section 156 can add up to five years to this exclusivity, and Paragraph III and IV certifications filed by generic challengers mark the moment the exclusivity structure begins to fracture.
The Generic Pathway: IP as Obstacle, Not Asset
Generic development inverts this relationship. The generic manufacturer’s IP challenge is not creating a new monopoly but safely navigating an existing one. That means conducting a thorough freedom-to-operate analysis against the innovator’s Orange Book-listed patents before a single gram of API is ordered for development batches. The Hatch-Waxman Act (formally the Drug Price Competition and Patent Term Restoration Act of 1984) created the ANDA framework specifically for this purpose: an abbreviated pathway that lets generic applicants rely on the FDA’s prior safety and efficacy findings for the Reference Listed Drug (RLD), replacing full clinical trial requirements with demonstration of pharmaceutical equivalence and bioequivalence (BE).
Pharmaceutical equivalence requires identical active pharmaceutical ingredient (API), dosage form, strength, and route of administration. Bioequivalence requires proof that the rate and extent of absorption, characterized primarily by Cmax and AUC in pharmacokinetic (PK) studies, fall within the 80-125% confidence interval window relative to the RLD. Meeting that standard is where academic science enters the generic pipeline at every stage.
The IP landscape for a generic developer looks nothing like a traditional pharmaceutical company’s IP portfolio. Rather than owning blockbuster composition-of-matter patents valued in the hundreds of millions, a generic company’s IP assets are primarily enabling technologies: validated analytical methods, proprietary formulation approaches, process patents for non-infringing manufacturing routes. These are valued on a cost-to-replicate basis rather than a discounted cash flow of future exclusivity, making them structurally cheaper to license but also far more numerous and modular.
Key Takeaways: The Structural Divide
Academic collaboration in the innovator sector centers on discovery and patent creation. In the generic sector, it centers on analytical problem-solving and regulatory de-risking. The same university pharmaceutical sciences department can serve both functions, but the outputs, the IP terms, and the commercial logic are categorically different. Generic companies pay for solutions to defined technical problems, not for the right to own new molecules. Understanding this distinction is the starting point for any rational assessment of how academic research generates value in the generic market.
II. The Analytical Infrastructure: How University Labs Decode Innovator Products
Before a generic developer formulates a single tablet, it needs a complete physicochemical portrait of the RLD. The innovator’s manufacturing data, excipient grades, particle size specifications, and process parameters are proprietary trade secrets. Nothing in the Hatch-Waxman framework compels disclosure of that information. The generic applicant has to reconstruct an equivalent functional profile from the outside using analytical methods that can distinguish, quantify, and characterize every relevant attribute of the finished product. University analytical chemistry programs build those methods.
Mass Spectrometry, Chromatography, and the Fingerprinting Problem
High-performance liquid chromatography (HPLC) and gas chromatography (GC) are the workhorses for separating and quantifying API content, impurity profiles, and excipient identification. Academic research pushes these platforms toward greater sensitivity and selectivity. Coupled LC-MS and GC-MS systems developed and refined in university settings allow impurity profiling at sub-ppm concentrations, which matters considerably when the FDA’s impurity thresholds under ICH Q3B(R2) require identification of any degradation product above 0.1% of the drug substance. For genotoxic impurities subject to ICH M7, the threshold drops to parts per million, and detection requires validated methods that most generic companies license or adopt from academic literature rather than develop independently.
Mass spectrometry imaging (MSI), pioneered in academic programs at institutions including the University of Warwick and MIT, takes this further by enabling spatial mapping of drug distribution within a tablet or granule. This matters for modified-release formulations where drug distribution through a polymer matrix directly determines the release rate profile. If the generic developer needs to understand how the innovator achieved a specific dissolution curve, MSI provides a non-destructive cross-sectional map without requiring full reverse engineering of the manufacturing process.
Solid-state characterization presents a separate layer of complexity. Powder X-ray diffraction (PXRD), differential scanning calorimetry (DSC), and solid-state NMR are standard tools in academic materials science labs that transfer directly to pharmaceutical characterization. Polymorphic form identification is not an academic curiosity: a different crystal polymorph can exhibit dramatically different solubility and dissolution kinetics, changing the bioavailability profile enough to fail a BE study. The most commercially consequential polymorph disputes in pharmaceutical history, including litigation over ranitidine’s Form 1 and Form 2, rosiglitazone crystalline forms, and the cefdinir Form A/B distinction, illustrate that polymorph control is as much an IP challenge as a scientific one. Academic crystallography research provides the analytical tools to identify, characterize, and ultimately design around innovator polymorph patents.
Near-Infrared and Raman Spectroscopy: Non-Destructive Process Analytics
Near-infrared (NIR) and Raman spectroscopy have matured from niche academic techniques into routine process analytical technology (PAT) tools under the FDA’s PAT initiative. Academic groups at the University of Innsbruck, Duquesne University, and Purdue have driven much of the method development that allowed these techniques to move from laboratory curiosity to GMP-compliant manufacturing floor applications. For generic developers, NIR blend uniformity monitoring and Raman-based raw material identification reduce in-process testing burden and provide the real-time release testing data that supports Quality by Design (QbD) submissions.
The IP valuation of these analytical platforms within a generic company’s asset base is primarily as enablers of development efficiency. A proprietary analytical method that can characterize a complex RLD faster, more completely, or at lower cost than competitors represents a competitive advantage in time-to-ANDA-submission that translates directly to first-filer status under 180-day market exclusivity provisions for Paragraph IV certifications. The company that files first collects that exclusivity; the company that files three months later does not. Academic analytical method development, when licensed or co-developed through sponsored research, shortens the characterization timeline and moves the ANDA clock forward.
IP Valuation Framework for Analytical Method Assets
For IP teams assessing the value of analytical method assets developed in academic collaboration, the appropriate framework is not traditional NPV of future royalties. Analytical methods rarely command royalties across a product’s entire commercial life. The value is primarily a risk-adjusted time-to-market acceleration. If a validated method reduces characterization time by six months on a product with $500 million in annual US generic market revenue at anticipated market share, and first-filer exclusivity is worth 180 days of substantially higher margins, the method’s economic value can be calculated with reasonable precision. That calculation should drive licensing negotiation with university technology transfer offices, not comparables from biotech drug discovery licensing benchmarks.
Key Takeaways: Analytical Science as Competitive Infrastructure
University analytical chemistry provides the decoding toolkit for RLD characterization. The outputs, validated HPLC methods, solid-state characterization protocols, spectroscopic fingerprinting techniques, are not glamorous, but they are the rate-limiting step in early-stage ANDA development for products where the innovator’s formulation is opaque. Academic publication of these methods in journals like the Journal of Pharmaceutical and Biomedical Analysis and Analytical Chemistry creates a public domain knowledge base that the entire generic sector can access, reducing redundant development work industry-wide.
III. Bioequivalence Science: The Methodological Frontier That Determines Market Access
The 80-125% confidence interval for Cmax and AUC in a standard two-way crossover PK study is deceptively simple as a regulatory standard. For oral immediate-release solid dosage forms with well-characterized systemic pharmacokinetics, it is straightforward to execute. For the growing share of the market that consists of locally acting drugs, complex delivery systems, highly variable drugs, and drug-device combinations, it is either insufficient or technically inapplicable. Academic research has spent the past two decades building the alternative methodological toolkit that makes generic competition possible for these harder products.
In Vitro-In Vivo Correlation (IVIVC): The Dissolution Bridge
For modified-release oral products, the dissolution profile, how rapidly the drug releases from the formulation under specified conditions, is the primary in vitro quality attribute. FDA dissolution guidance for immediate-release products typically requires a single-point test at a specified pH. For extended-release formulations, a multi-point dissolution profile across multiple pH conditions is required, and the relationship between that dissolution profile and the in vivo PK profile must be established through IVIVC.
IVIVC development is fundamentally an academic exercise. It requires designing dissolution methods that are discriminating at the critical quality attribute level, generating in vivo PK data from multiple formulations with intentionally different release rates, and fitting a mathematical model that predicts in vivo performance from in vitro data with sufficient precision to satisfy FDA Level A correlation criteria. The FDA’s 1997 Guidance on Extended Release Oral Dosage Forms defines three correlation levels (A, B, C), with Level A being the only one acceptable for biowaivers, meaning regulatory approval of additional strengths without in vivo BE studies.
Academic pharmacokinetics groups, particularly at the University of Maryland, the University of Michigan, and the University of North Carolina, have produced the foundational IVIVC modeling work that the agency has relied on to develop this policy framework. When a generic company submits a Level A IVIVC as part of a biowaiver request, the underlying scientific validity of that approach rests on peer-reviewed academic literature, not on industry-sponsored studies alone.
The commercial value of a validated IVIVC is substantial. An IVIVC that supports biopredictive dissolution testing can replace costly in vivo BE studies for multiple strengths and potentially for post-approval manufacturing changes. For a complex extended-release product with four available strengths, a successful IVIVC biowaiver strategy can eliminate three separate BE studies at $2-5 million each, while also dramatically accelerating post-approval scale-up and site-transfer submissions.
The Vasoconstriction Assay and Topical Product Equivalence
Topical corticosteroids represent one of the clearest examples of academic-regulatory collaboration producing a workable BE methodology for a class of drugs where blood-level measurements are scientifically meaningless. Topical corticosteroids act locally on skin, and their systemic absorption is both variable and clinically irrelevant to their efficacy.
The chromameter-measured vasoconstriction (skin blanching) assay, developed through collaborative work between academic dermatologists and FDA pharmacologists in the late 1980s and validated over subsequent years, became the accepted surrogate for BE demonstration for topical corticosteroids. The assay quantifies the degree of skin blanching induced by a topically applied corticosteroid using chromametry, using that physiological response as a PD surrogate for drug activity. FDA’s 2012 draft and 2018 final guidance for topical corticosteroids formalized this approach into Product-Specific Guidances (PSGs).
The vasoconstriction assay illustrates a general principle: for locally acting drugs, a pharmacodynamic or clinical endpoint surrogate must replace the PK approach, and developing and validating those surrogates is academic work. The FDA cannot develop these methods internally at scale; it relies on published university research to establish scientific legitimacy before issuing a PSG.
For IP teams and portfolio managers, the PSG database is one of the most strategically important public documents in generic drug development. A PSG specifying an in vitro BE approach, a clinical endpoint study, or a PD surrogate method provides a defined regulatory pathway that can be translated directly into development cost and timeline estimates. Products with PSGs that allow in vitro approaches have dramatically lower barriers to entry than those requiring clinical endpoint studies. Academic research that generates the scientific evidence supporting a new in vitro PSG for a drug class with no current generic competition can unlock an entirely new competitive space.
Physiologically-Based Pharmacokinetic (PBPK) Modeling: In Silico Bioequivalence
PBPK models are multi-compartment mathematical representations of human physiology, parameterized with drug-specific physicochemical data (solubility, permeability, protein binding, metabolic clearance) and population-level physiological characteristics (gastrointestinal transit times, organ blood flows, enzyme expression). A PBPK model can simulate the entire ADME behavior of a drug across patient populations, fed/fasted states, drug-drug interaction scenarios, and formulation variations.
For generic development, PBPK modeling has three primary applications. First, it can be used to support biowaivers under the Biopharmaceutics Classification System (BCS) framework by predicting in vivo absorption from in vitro solubility and permeability data without requiring a human PK study. Second, for highly variable drugs, PBPK models can help identify the sources of variability and support the design of replicate crossover BE study designs that the FDA accepts under its 2020 guidance on highly variable drugs. Third, for complex formulations like long-acting injectables (LAIs), PBPK models linked to in vitro release testing data can provide mechanistic predictions of in vivo drug release profiles that support the design of BE studies or, in some cases, justify in vitro BE approaches.
Academic pharmaceutical sciences programs are the primary developers of the PBPK platform knowledge that the generic industry uses. GastroPlus, Simcyp, and PK-Sim, the three dominant commercial PBPK software platforms, all incorporate mechanistic equations and parameter databases that are rooted in decades of academic pharmacokinetics research. FDA’s Center for Drug Evaluation and Research now accepts PBPK analyses as part of ANDA submissions, a policy explicitly enabled by the scientific validation work done in university settings and documented in guidance documents like the 2018 Physiologically Based Pharmacokinetic Analyses framework.
The IP implications of in silico BE approaches are significant. A validated PBPK model that supports a biowaiver for a specific product is an asset. It reduces development cost, it may be licensable to other generic companies developing the same product (creating a licensing revenue stream), and it represents proprietary know-how that is difficult for competitors to replicate without the underlying model architecture and calibration datasets.
Key Takeaways: Alternative BE Methodologies as Market Access Enablers
Every validated alternative to a standard human PK crossover study represents a reduction in development cost, timeline risk, and the barriers to generic entry for a specific product category. Academic research produces these alternatives. The FDA formalizes them in PSGs. Generic developers who track the academic literature in bioequivalence science have advance visibility into which product classes will become accessible to ANDA development before the formal guidance documents are issued, which is a material competitive intelligence advantage.
IV. Quality by Design: The Academic Framework Behind Modern ANDA Submissions
The FDA’s Quality by Design initiative, first articulated in the ICH Q8(R2), Q9, and Q10 guidelines developed between 2005 and 2008, represents a fundamental shift in how regulatory agencies think about pharmaceutical manufacturing. Rather than accepting a fixed manufacturing process with end-product testing as the quality assurance mechanism, QbD requires developers to demonstrate systematic understanding of the relationship between process parameters and product performance. This is material science and physical pharmacy research, and it is produced predominantly in academic laboratories.
Design Space, Control Strategy, and Critical Quality Attributes
Under QbD, a developer must define a design space: the combination of input material attributes (particle size distribution of API, moisture content of excipients, grade of polymers) and process parameters (mixing time, granulation endpoint, tablet compression force) within which the product consistently meets its critical quality attributes (CQAs). CQAs for a generic oral solid dosage form typically include dissolution rate, content uniformity, hardness, friability, and disintegration time.
The intellectual work of defining this design space requires understanding the mechanistic relationships between each input variable and each CQA. Academic pharmaceutical sciences research generates exactly this knowledge. Studies on the effect of HPMC viscosity grade on drug release rate from matrix tablets, the impact of microcrystalline cellulose grade on tablet compaction properties, and the relationship between particle size distribution of API and dissolution rate in immediate-release formulations fill the journals of pharmaceutical technology and provide the scientific basis for rational formulation design.
For generic developers, this academic knowledge base translates into a Design of Experiments (DoE) approach to formulation development, where the number of trial batches required to reach an acceptable formulation is dramatically reduced. Instead of empirically testing 30 formulation variants, a QbD-informed developer can use a DoE matrix of perhaps eight to twelve runs, guided by mechanistic understanding from the literature, to map the design space efficiently. This reduction in experimental burden directly reduces development costs and timelines.
Process Analytical Technology and Real-Time Release Testing
The FDA’s PAT framework, issued in 2004, encouraged the use of in-process measurement tools to monitor and control manufacturing in real time. NIR spectroscopy for blend uniformity, Raman for API identification during granulation, acoustic emission monitoring for granule endpoint detection, and focused beam reflectance measurement (FBRM) for particle size monitoring during wet granulation are all PAT tools developed and validated in academic settings before transfer to GMP manufacturing environments.
Real-time release testing (RTRT), the regulatory mechanism that allows a manufacturer to replace end-product dissolution testing with in-process PAT measurements correlated to dissolution performance, is available only for products where an IVIVC or equivalent predictive model has been established. The academic work that validates PAT-dissolution correlations, and that provides the statistical frameworks for acceptable RTRT control limits, is directly incorporated into regulatory submissions for products seeking this manufacturing flexibility.
From an IP perspective, a proprietary PAT control strategy that enables RTRT is a manufacturing process patent opportunity. Generic companies that develop and patent novel PAT-based manufacturing approaches can defend their process against competitor ANDAs, even when the formulation itself is commodity. Academic collaborators who help develop and validate these PAT systems, typically through sponsored research agreements, often negotiate co-inventorship positions that give universities a stake in the resulting process patents.
Key Takeaways: QbD as the Scientific Language of Modern ANDAs
The FDA increasingly expects QbD-informed submissions for complex products. ANDAs that demonstrate design space understanding and contain robust process validation data receive fewer complete response letters and move through review more efficiently. The academic knowledge base that enables QbD is available in peer-reviewed literature, but the companies that have internal capability to apply it systematically, often by hiring from PhD programs at the universities that produce it, develop a structural submission quality advantage.
V. Complex Generics: Where Academic Research Becomes Indispensable
The market segment that has absorbed most of the generic industry’s strategic attention since approximately 2015 is complex generics. These products command significantly higher entry barriers, sustain fewer competitors post-approval, and consequently maintain much more favorable pricing dynamics than commodity oral solids. They also require scientific capabilities that most generic companies do not have in-house, which is why academic collaboration has moved from peripheral to central in their development.
Defining ‘Complex’ and What That Means for IP Valuation
The FDA does not have a single formal definition of ‘complex generic,’ but its Office of Generic Drugs consistently applies the term to products where demonstrating therapeutic equivalence requires non-standard approaches. The key categories include products with complex active ingredients (peptides, oligonucleotides, complex drug substances such as ferumoxytol or sodium hyaluronate), complex formulations (liposomes, emulsions, microspheres, nanoparticles), complex routes of administration (topical, inhaled, ophthalmic, nasal, intravitreal), and complex drug-device combinations (metered dose inhalers, auto-injectors, transdermal patches, nasal sprays).
The IP valuation of a complex generic pipeline looks very different from a simple oral solid portfolio. A company holding an approved ANDA for a product like glatiramer acetate injection (the generic for Copaxone) has an asset whose value is primarily determined by competitive moat depth, the difficulty for subsequent entrants to navigate the BE pathway, and the revenue durability that follows from a thin competitive set. Mylan and Sandoz each spent over a decade and well over $100 million in development costs to generate the analytical characterization, clinical BE data, and manufacturing validation required for glatiramer acetate approval. That investment created a formidable barrier to entry and sustained a market where, years after generic approval, prices have not collapsed to the levels seen in commodity oral solid markets.
For portfolio managers evaluating complex generic companies, the relevant metric is not just pipeline count but the scientific credibility of the BE strategy for each product in development. Products where the FDA has no clear PSG, where the BE pathway requires extensive in vitro-in vivo correlation work or comparative clinical endpoint studies, and where the developer has academic partnerships capable of generating the required data carry substantially different risk profiles than products with clear, validated PSG pathways.
Long-Acting Injectables: The De Novo Formulation Challenge
Long-acting injectable (LAI) microsphere formulations represent perhaps the most technically demanding category of complex generics. The innovator products, risperidone LAI (Risperdal Consta, J&J), naltrexone LAI (Vivitrol, Alkermes), and leuprolide acetate microspheres (Lupron Depot, AbbVie), rely on biodegradable poly(lactic-co-glycolic acid) (PLGA) polymer microspheres that encapsulate the API and release it over weeks to months as the polymer degrades.
The innovator’s specific PLGA molecular weight, copolymer ratio, end-cap chemistry, and microsphere fabrication process (typically a solvent evaporation or spray drying technique) are trade secrets protected by manufacturing process patents that often survive long after the original composition-of-matter patents expire. This is a deliberate evergreening strategy: as the base compound patent expires, the innovator maintains market exclusivity through a thicket of manufacturing patents covering the specific microsphere production process, excipient grade, and sterilization approach.
A generic developer cannot simply copy these process patents. It must independently develop a PLGA microsphere formulation using a non-infringing manufacturing approach that nevertheless produces a product with an in vivo release profile that satisfies the FDA’s BE criteria. This task requires deep expertise in polymer science, particularly the relationships between PLGA degradation kinetics and drug release, between microsphere morphology and encapsulation efficiency, and between in vitro release testing conditions and in vivo performance. That expertise lives primarily in academic polymer science and pharmaceutical sciences departments.
Academic groups at Purdue, MIT, the University of Texas at Austin, and Johns Hopkins have produced the foundational polymer science literature that generic developers use as their design guide for LAI microsphere development. The CRCG has made LAI formulation one of its primary research focus areas, recognizing that the scientific and regulatory pathway for these products remains inadequately defined compared to what the market opportunity warrants.
The IP strategy for an LAI generic is layered. The developer must clear the innovator’s process patent estate through a Paragraph IV certification and litigation strategy or by designing a sufficiently distinct process that avoids infringement. It may then develop proprietary process patents on its own manufacturing approach. The analytical methods used to characterize the microspheres, particularly in vitro drug release testing, particle size distribution measurement, and surface morphology characterization by scanning electron microscopy (SEM), may generate additional IP. Academic collaborators who develop validated in vitro release test methods for specific LAI products generate assets that are independently valuable, either for use in ANDA submissions or for licensing to other developers.
Inhaled Products: Particle Engineering and Device-Formulation Coupling
Generic inhalers, including dry powder inhalers (DPIs), metered dose inhalers (MDIs), and nasal sprays, present a distinct category of complexity rooted in the inseparability of the drug formulation from the drug delivery device. For an MDI, the delivered dose, particle size distribution of the aerosol, and regional deposition in the lung are all determined by the interaction between the formulation (drug concentration, propellant type, cosolvent, surfactant) and the device (actuator orifice dimensions, valve geometry, can material). A generic product requires demonstrating bioequivalence across all of these device-formulation coupled attributes.
FDA’s BE recommendations for orally inhaled and nasal drug products require a ‘weight of evidence’ approach combining in vitro aerodynamic particle size distribution testing (typically using a Next Generation Impactor or Andersen Cascade Impactor), in vitro plume geometry, in vitro emitted dose consistency, and for MDIs with spacers or valved holding chambers, compatibility testing. For some products, a comparative human pharmacokinetic study or a clinical endpoint study measuring lung function is required on top of the in vitro package.
The particle engineering science underlying this pathway is an active academic research area. Spray drying, jet milling, and supercritical fluid precipitation techniques for producing drug particles with controlled aerodynamic particle size distributions have been extensively studied in pharmaceutical engineering departments. Computational fluid dynamics (CFD) modeling of airflow and drug deposition in realistic airway geometries, developed primarily in academic biomedical engineering programs, is increasingly being incorporated into BE submissions to provide mechanistic justification for the in vitro test methods selected.
The commercial stakes are high. GSK’s Advair Diskus (fluticasone propionate/salmeterol DPI) had US sales exceeding $4 billion annually at its peak, and the absence of approved generic versions for years after patent expiry, due precisely to the difficulty of demonstrating BE for a complex DPI, illustrates the economic protection that formulation complexity provides. The generic versions that eventually reached the market, including Mylan’s Wixela Inhub and Hikma’s version, required development timelines measured in years and collaboration with academic respiratory researchers to validate the analytical approach.
The CRCG: A Pre-Competitive Research Hub
In 2020, the FDA awarded a $5 million GDUFA-funded grant to a consortium led by the University of Maryland School of Pharmacy and the University of Michigan College of Pharmacy to establish the Center for Research on Complex Generics (CRCG). The center’s mandate covers four primary research domains: complex injectables, inhaled and nasal products, topical and ophthalmic products, and quantitative methods and modeling. It operates as a pre-competitive research hub, meaning its scientific outputs are shared across the generic industry rather than held as proprietary assets of individual companies.
The CRCG’s initial industry stakeholder survey, conducted shortly after launch, identified the most pressing scientific needs by sector vote. Complex injectable formulations ranked highest, driven specifically by LAI microsphere and liposomal products. Drug-device combination characterization ranked second. PBPK and MIDD methodology development ranked third, with strong interest in validated modeling approaches that could reduce or replace human PK studies for specific product classes.
By 2025, the CRCG had published more than 80 peer-reviewed papers, hosted 12 workshops with FDA scientists, and trained over 200 graduate students and postdoctoral researchers who have entered the generic drug industry workforce. This talent pipeline is itself a deliverable of GDUFA-funded academic investment, building long-term scientific capacity that individual generic companies could not justify funding independently.
Key Takeaways: Complex Generics as High-Moat, High-Academic-Dependency Assets
Complex generics require de novo formulation innovation, not replication. The science to support that innovation is produced in academic labs. Companies that have established deep academic partnerships in the specific technical areas relevant to their complex generic pipeline, LAI polymer science, inhaled particle engineering, in silico PBPK modeling, have a durable competitive advantage that cannot be quickly replicated by capital alone. For investors, the depth and specificity of a generic company’s academic collaboration portfolio is a leading indicator of pipeline execution probability for complex products.
VI. GDUFA: The Policy Machine Funding the Academic-Generic Partnership
The Generic Drug User Fee Amendments, first enacted in 2012 and reauthorized in 2017 (GDUFA II) and again in 2022 (GDUFA III), created the financial and structural framework for systematic academic engagement with generic drug science. Understanding the GDUFA science and research program is essential for any analyst, IP team, or R&D lead trying to anticipate where regulatory science is heading and which product classes will have clarified development pathways in the near term.
The GDUFA Science Program: Mechanism and Scale
GDUFA user fees, paid by generic drug manufacturers and applicants, fund FDA’s Office of Generic Drugs (OGD) operations including review staff, IT infrastructure, and the regulatory science program. The science program specifically funds external research, primarily at academic institutions, aimed at resolving the scientific knowledge gaps that produce development uncertainty, application failures, and regulatory delays for complex products.
The program operates through two primary mechanisms. GDUFA grants fund open-ended academic research on topics the FDA identifies as high-priority based on its ANDA review experience. GDUFA contracts fund more specific deliverables, often method development or validation studies for defined product types. Since GDUFA I inception, OGD has awarded well over 100 grants and contracts to academic institutions, creating a research network that is effectively a contract R&D arm for the agency on complex generic topics.
The fiscal year 2023 GDUFA science and research report documented concrete regulatory impact: 19 new or revised PSGs informed by GDUFA-funded research in that year alone, 309 Controlled Correspondences answered using data from GDUFA-funded studies, and contributions to 89 pre-ANDA meetings. Those PSGs directly translate to commercial opportunities. A new PSG for a product with no current approved generic, where the lack of regulatory clarity had been suppressing development investment, can unlock ANDA filings within months of publication.
FY2025 GDUFA science priorities, published by OGD, listed complex injectables (focusing on liposomal and microsphere formulations), drug-device combinations, and PBPK modeling for locally acting drugs as the top research areas. Companies monitoring these priorities have an 18-to-24-month lead time on anticipating which PSGs are likely to be issued, time that can be used to advance development programs before competitors who are waiting for the PSG to initiate development.
Product-Specific Guidances as the Commercial Manifestation of Academic Research
PSGs are the most direct commercial output of the GDUFA science program. Each PSG provides route-specific, product-specific recommendations on the recommended BE approach, the preferred test and reference formulation, key in vitro quality attributes, and any specific device or container-closure considerations for drug-device combinations. They exist for approximately 1,600 products as of 2025, with new and revised guidances issued on a rolling basis.
For a product with no PSG, the development pathway is uncertain. A developer must submit a pre-ANDA meeting request, propose a BE approach, and wait for FDA feedback before committing development resources. This process adds six to eighteen months to the development timeline and introduces the risk that the FDA will reject the proposed approach at ANDA submission stage, resulting in a complete response letter. For a product with a clear PSG specifying an in vitro BE approach using validated methods from academic literature, that uncertainty collapses.
The academic research pipeline feeding into future PSG development is visible to anyone who tracks the CRCG publication record and GDUFA grant award lists (both public through FDA’s website). When CRCG researchers publish a validated in vitro release test methodology for a specific LAI formulation type, or when FDA contracts an academic group to develop a PBPK model for a topical drug, those outputs will, within 24-36 months, become the scientific basis for a revised or new PSG. This publication-to-PSG pipeline is trackable and represents genuine competitive intelligence for development portfolio management.
IP Positioning Within the GDUFA Ecosystem
Pre-competitive research funded by GDUFA and conducted through academic consortia creates a shared scientific commons. The analytical methods, modeling frameworks, and bioequivalence approaches developed under CRCG projects are published and freely available to all generic developers. This is by design: the goal is to reduce barriers to entry for the entire industry, not to create proprietary advantages for specific companies.
The IP opportunity for individual companies within this ecosystem exists at the product-specific level, not the methodological level. A company that takes a CRCG-developed in vitro release test methodology and applies it first to a specific LAI product, generating the validation data and ANDA submission package, captures first-filer exclusivity for that product. The generic method is publicly available; the application of that method to a specific, commercially important product, done faster and better than competitors, is the source of proprietary value.
Academic collaborations that extend beyond the CRCG’s pre-competitive mandate, for example, sponsored research agreements with specific universities for product-specific formulation work, can generate IP that is more clearly proprietary. The terms under which that IP is owned, licensed, and exercised require careful structuring. Generic companies should negotiate for non-exclusive licenses to platform enabling technologies (ensuring freedom to operate without paying ongoing royalties on broadly applicable methods) while seeking either ownership or exclusive options on product-specific formulation patents developed under sponsored research.
Key Takeaways: GDUFA as a Forward Intelligence Signal
The GDUFA science program is the most important forward indicator of near-term generic market access changes. Academic grants awarded, CRCG research publications, and FDA-issued PSGs form a causal chain with roughly a two-to-three-year lag time. Portfolio teams that treat the GDUFA research pipeline as competitive intelligence, tracking grant awards, CRCG publications, and PSG issuance patterns, can position development programs ahead of the regulatory clarity curve.
VII. Collaboration Structures, IP Terms, and the Technology Transfer Negotiation
The mechanics of how academic science reaches the generic industry, the specific contract structures, IP term allocations, and technology transfer models, determine how much of the value academic research creates is actually captured by the parties involved. These mechanics have evolved considerably as the generic industry’s dependence on academic science has grown.
Sponsored Research Agreements: The One-to-One Model
The traditional sponsored research agreement (SRA) is a bilateral contract between a single company and a university laboratory. The company funds a defined research program, typically for one to three years, in exchange for an option to license IP generated during the project. The key negotiated terms include publication rights (university researchers require the right to publish; companies require a review period, typically 30 to 90 days, to identify patentable inventions before publication), IP ownership (universities typically retain ownership under Bayh-Dole Act provisions, with the company receiving a license), and the scope and exclusivity of that license.
For generic-sector SRAs, the appropriate licensing terms differ from the innovator-sector norm. In innovator drug discovery, a company licensing a new drug molecule from a university typically requires a broad, exclusive, worldwide license across all therapeutic applications, because the entire commercial value of the molecule depends on market exclusivity. In the generic sector, the licensed technology is more often an enabling tool: an analytical method, a formulation platform, or a PBPK modeling framework. Exclusive worldwide rights to such a tool are rarely necessary and are prohibitively expensive to negotiate. Non-exclusive licenses, allowing the university to license the same method to multiple generic companies (or even to the FDA for regulatory use), are typically more appropriate and more commercially efficient.
The University of Wisconsin-Madison’s ‘Badger IP Industry Advantage’ program, launched in 2024, formalizes this approach by offering pre-negotiated, transparent IP license terms that include non-exclusive, royalty-free options in exchange for upfront fees. This model reduces transaction costs for both parties, accelerates collaboration formation, and aligns with the public health rationale for promoting broad access to enabling technologies that increase generic market competition.
Multi-Stakeholder Consortia: Pre-Competitive Science at Scale
When the scientific challenge exceeds what any single company’s sponsored research budget can address, and when the results of the research would benefit all market participants rather than conferring competitive advantage on a single sponsor, the multi-stakeholder consortium model is more efficient. The CRCG is the most prominent generic-sector example, but other consortia address adjacent scientific domains.
The Center for Applied Pharmacokinetic Research (CAPKR) at the University of Manchester pools academic and industry expertise in PBPK modeling and pharmacokinetic simulation, working on problems relevant to both generic and innovator development. Industry consortium members gain access to cutting-edge modeling capabilities and to a forum for direct scientific engagement with academic experts, without the overhead of building equivalent internal expertise.
Governance structures in multi-stakeholder consortia require careful design to manage the tension between pre-competitive collaboration and individual company competitive interests. Consortium members typically agree that research outputs published through the consortium are available to all members on equal terms. Member companies that want product-specific work that builds on consortium methodologies must commission that through separate bilateral agreements outside the consortium framework. This division between pre-competitive platform science (shared) and product-specific application (proprietary) is the operating principle that makes these consortia viable.
Key Takeaways: IP Terms Must Match the Generic Business Model
Technology transfer offices at universities that want productive partnerships with the generic industry need to understand that the generic sector’s IP needs are structurally different from the innovator sector’s. Non-exclusive licenses for enabling technologies, streamlined agreement templates, and reasonable upfront fees without royalty tails that persist through the product’s commercial life are the terms most likely to create productive relationships. Academic institutions that insist on innovator-style exclusive licenses for analytical methods or formulation platform technologies will find generic companies going elsewhere for the enabling science they need.
VIII. Bridging the Translational Gap: Why Most Academic Research Doesn’t Reach ANDAs
Despite the growing institutional infrastructure connecting academic research and generic drug development, a substantial fraction of university-generated pharmaceutical science never reaches commercial application. The reasons are structural, not incidental, and they define the next frontier of improvement in the academic-generic collaboration ecosystem.
The Regulatory Know-How Gap
The most consistent barrier to translation is not scientific quality. It is regulatory expertise. An academic lab may develop a genuinely novel method for characterizing a complex RLD, publish it in a high-impact journal with rigorous experimental design, and receive strong scientific peer review validation. That paper still cannot support an ANDA submission if the method was not developed according to ICH Q2(R1) analytical method validation guidelines, if the reagents and reference standards used are not pharmacopeial grade or fully traceable, or if the experimental conditions do not map onto the GMP testing environment where the method will be applied.
FDA’s ANDA review scrutinizes every analytical method submission against these validation criteria. A method with missing specificity, linearity, precision, or robustness data generates a deficiency letter that delays approval. If the academic publication on which the method is based did not include validation against these specific criteria, the generic company must conduct additional validation studies, adding time and cost to the development program. If those additional studies reveal that the method as published does not meet validation criteria under GMP conditions, the academic work may be scientifically valuable but commercially unusable.
This gap is not an argument against academic collaboration. It is an argument for changing how academic pharmaceutical research is conducted and reported. University programs that train graduate students in ICH validation requirements, that conduct their method development work in ways that generate validation-compatible datasets, and that publish not just the scientific novel finding but the regulatory acceptability framework for their methods, produce work that is far more directly useful to industry and regulators alike.
cGMP Culture and Academic Research Practice
Current Good Manufacturing Practices (cGMP) govern every aspect of manufacturing, testing, and quality control for FDA-regulated drug products. They require documented procedures for every step, validated instruments with calibrated traceability, qualified personnel for all critical operations, and change control processes for any modification to established methods. Academic research labs operate under none of these requirements.
This mismatch means that manufacturing or analytical work conducted at a university, even when scientifically rigorous, typically cannot be directly incorporated into a regulatory submission without substantial additional validation work under GMP conditions. Scale-up from a university bench to a GMP pilot plant often reveals unexpected challenges: particle aggregation behaviors that did not manifest at gram scale, mixing uniformity problems that emerge at kilogram scale, or sterility assurance issues for parenteral products that require controlled cleanroom manufacturing.
The CRCG partially addresses this by housing some research in facilities with higher quality standards than typical academic labs, and by partnering with FDA’s own laboratories for some validation work. Industry-funded translational centers at institutions like the University of Maryland’s School of Pharmacy, which has dedicated GMP-capable pilot manufacturing facilities, represent a more complete solution. Universities willing to invest in this infrastructure attract industry partners who need translational capability, not just scientific novelty.
The Generic Industry’s Risk Profile and Early-Stage Investment Aversion
Generic companies operate on margins that are under constant compression. The post-entry price erosion for oral solid generics can exceed 80% within 18 months of the first generic approval, as subsequent ANDAs are approved and retail pharmacy purchasing programs play manufacturers against each other. This economics forces a discipline of investing only in assets with high probability of regulatory approval and competitive differentiation.
An early-stage academic proof of concept, however scientifically compelling, rarely meets that threshold. A novel PBPK model that predicts LAI release behavior in rats does not tell a generic company whether the FDA will accept a PBPK-supported BE approach for the specific human product it is trying to develop. A new in vitro dissolution methodology published in the Journal of Controlled Release may be scientifically valid but lacks the FDA endorsement, in the form of a PSG or regulatory guidance, that a generic company needs before committing multi-million-dollar development resources to an ANDA program built on that methodology.
This creates a structural investment gap between what academic research produces and what generic companies will pay to develop. The CRCG and the GDUFA grant program partially fill this gap at the methodological level. At the product-specific level, the gap persists. A targeted, publicly funded grant mechanism, perhaps through an NIH-FDA joint program or a BARDA-style advance market commitment for specific underserved complex generic products, could accelerate the translation of academic science into commercially viable ANDA programs for products where market failure has left patients without access to affordable alternatives.
Key Takeaways: Translation Requires Infrastructure, Not Just Funding
The generic sector’s ‘valley of death’ is primarily a capability gap, not a capital gap. The science that academic institutions produce needs to be developed in ways that are compatible with GMP requirements, validated against ICH guidelines, and packaged in a form that FDA reviewers can use. Universities that build this translational capability, through dedicated GMP pilot facilities, regulatory science training programs, and industry-facing technology transfer expertise, become genuine R&D partners rather than upstream science suppliers.
IX. Investment Strategy for Generic Pharma Analysts: Reading the Academic Signal
Academic research activity in pharmaceutical sciences is a leading indicator for generic drug market development. Analysts and portfolio managers who track it systematically can identify competitive dynamics and market access changes 24-36 months before they become visible in ANDA filing databases or product launch announcements.
How to Use the GDUFA Research Pipeline as a Forward Indicator
The FDA publishes the GDUFA science and research priorities annually. These documents name the specific scientific problems the agency has identified as the highest barriers to generic market access for complex products. When the FDA names a problem, it means the agency has already seen enough ANDA submissions for relevant products to know that the scientific knowledge gaps are causing systematic approval delays.
The GDUFA grant award database, available through FDA’s website, lists the academic institutions receiving funding and the broad research areas those grants address. Tracking these awards against the PSG issuance timeline provides a data-driven basis for estimating when regulatory clarity will arrive for specific product categories. For LAI microsphere products, for example, GDUFA-funded research at the University of Maryland and Rutgers focused on in vitro release test method development from 2020 onward. PSG revisions for specific LAI products followed. Companies that began LAI generic development programs in 2020 based on tracking that research pipeline were 18-24 months ahead of competitors who waited for PSG publication to initiate development.
Evaluating Generic Companies Through Their Academic Partnership Depth
For institutional investors and analysts evaluating generic pharmaceutical companies, the depth and specificity of academic partnerships is a material factor in pipeline execution risk for complex products. A company with a sponsored research agreement at a leading pharmaceutical sciences program for each of its top five complex generic pipeline products, with clear milestones tied to the development of validated BE methodologies, has a fundamentally different risk profile from a company claiming the same pipeline without that scientific infrastructure.
Key due diligence questions for evaluating academic partnership quality: Does the sponsored research agreement include co-development of the BE methodology to a regulatory-submission-ready standard, or does it end at scientific proof of concept? Has the academic partner worked with FDA scientists on the relevant product class before? Does the university have GMP-capable pilot manufacturing facilities that can support development batch manufacturing? Are the key academic investigators aligned with FDA’s quantitative methods and modeling priorities, or are they working in basic science areas with limited near-term regulatory application?
These questions separate academic partnerships that are strategically valuable from those that are reputationally convenient but operationally limited.
Complex Generic IP as a Valuation Premium Driver
The sustained price premium that complex generics command relative to commodity oral solids is a function of the depth of the competitive moat created by high development barriers. When that moat is maintained in part by academic partnership-derived scientific capabilities, the valuation multiple applied to complex generic revenue should reflect the durability of that competitive position.
A portfolio with strong positions in three to five complex generic product categories, each supported by proprietary BE methodology development co-owned or exclusively licensed from academic partners, justifies a higher EV/EBITDA multiple than a portfolio of equivalent revenue generated from oral solid generics facing twelve-plus approved competitors. The academic science that enables the complex generic moat is, in this framework, a balance-sheet-worthy intangible asset that current generic company valuations frequently understate.
Key Takeaways: Academic Activity as Intelligence, Collaboration Depth as Risk Metric
Analysts who treat GDUFA grant awards and CRCG publication activity as market intelligence rather than academic noise will systematically anticipate generic market access changes before they are priced into equities. Companies that have operationalized deep academic collaboration for their complex generic pipelines have demonstrably lower development execution risk, shorter time-to-market timelines, and more durable competitive positions in the markets they enter.
X. Strategic Recommendations Across the Stakeholder Map
The academic-generic partnership is productive but not yet optimized. Persistent structural inefficiencies in how academic science is conducted, transferred, and applied to the regulatory pathway leave value on the table for all parties.
For Academic Pharmaceutical Sciences Programs
Regulatory science needs to be core curriculum, not elective enrichment. Graduate students in pharmaceutical sciences who do not understand ICH Q2(R1) validation requirements, the structure of an ANDA submission, or the specific quality standards required for cGMP testing methods are inadequately prepared for the industry positions most of them will hold. Programs that integrate regulatory science training into their doctoral curricula, and that conduct their research in ways designed to produce regulatory-submission-ready datasets, produce graduates who are immediately productive in industry and produce research that translates more efficiently to commercial applications.
University technology transfer offices need to adopt flexible, modular IP models for generic sector engagement. The standard innovator-sector license template, built for exclusive worldwide rights to a novel drug molecule, does not fit the generic sector’s need for non-exclusive, cost-effective access to enabling analytical and formulation technologies. Universities that develop pre-negotiated term sheets for enabling technology licenses, with transparent royalty structures and no exclusivity requirements, will close deals faster and build longer-term industry relationships.
Investment in GMP-capable pilot manufacturing infrastructure is the single largest capability gap in most academic pharmaceutical sciences programs. Without it, even the best academic science cannot be translated into the development batches required for BE studies or ANDA submissions. Joint investments between universities, state governments, and industry sponsors in dedicated translational manufacturing facilities, modeled on programs at the University of Maryland and Rutgers, would dramatically reduce the translational gap.
For Generic Pharmaceutical Companies
The companies that will win disproportionate share in complex generics over the next decade are already building the academic partnerships that will supply their development infrastructure. Waiting for PSG publication to begin academic collaboration is a reactive posture that concedes the development timeline advantage to competitors with earlier engagement. The optimal approach is to identify product classes aligned with GDUFA science priorities, identify the academic groups doing the best work in those areas, and establish sponsored research agreements or consortia memberships before the PSG exists.
Internal MIDD capability, whether built through hiring from academic programs, through licensing academic PBPK models, or through dedicated partnerships with quantitative pharmacology groups, is becoming table stakes for complex generic development. The FDA’s increasing acceptance of PBPK-supported biopredictive dissolution methods and in silico BE approaches for specific product classes means that companies without this capability will face slower development timelines and greater regulatory uncertainty than their MIDD-capable competitors.
For Regulators and Policymakers
GDUFA III, negotiated and enacted in 2022 for the period through 2027, maintained the science and research program but did not substantially expand its scope to address emerging complex generic categories including complex mixture drug substances, oligonucleotide generics, and biosimilar-adjacent complex biologics. Future GDUFA reauthorization negotiations should explicitly expand the research program’s mandate to cover these emerging categories, with targeted funding for the specific scientific problems, characterization methods for complex mixture APIs, in vitro BE approaches for oligonucleotide generics, that will determine whether robust generic competition in these high-cost therapeutic areas develops within the next decade.
A targeted translational grant program, jointly administered by FDA and NIH, specifically designed to fund the gap between academic proof of concept and regulatory-submission-ready data packages for specific under-genericized complex products, would address the structural funding failure that currently leaves promising academic research stranded before it reaches commercial application. This is not a request for general pharmaceutical R&D funding. It is a targeted intervention designed to fix a specific market failure with high public health and public expenditure consequences.
International harmonization of complex generic regulatory standards, particularly between FDA and EMA, would reduce duplicative development investment and accelerate patient access globally. FDA has pursued bilateral scientific exchange with EMA on biosimilars and complex generics through existing international engagement channels, but formal, binding guideline harmonization remains limited. A joint FDA-EMA working group specifically focused on complex generic BE methodology standards, building on the scientific platforms being developed through GDUFA-funded academic research, would benefit developers, regulators, and patients across both markets.
Conclusion
Academic research is not peripheral to generic drug development. It is the infrastructure on which the entire sector’s scientific credibility rests. It decodes innovator products that do not come with instructions. It builds the bioequivalence methodologies that define what regulatory approval requires for each category of complex product. It supplies the formulation science that enables developers to independently invent alternative routes to a bioequivalent outcome when the innovator’s manufacturing process is a trade secret. And through the GDUFA science program, it translates directly into the PSGs that determine whether and when generic competition arrives for the most expensive medicines on the market.
The companies, institutions, and policymakers that treat this relationship strategically, rather than as incidental academic background, will shape the competitive structure of pharmaceutical markets for the decade ahead.
Data sourced from FDA Office of Generic Drugs annual reports, GDUFA science and research outcome publications, CRCG public research outputs, and peer-reviewed literature in pharmaceutical sciences. Patent landscape data from public Orange Book and USPTO records.