Strategic and Regulatory Pathways for Launching High-Value Complex Generics
The standard generic drug business is a race to the bottom. File an ANDA, prove bioequivalence on a straightforward oral solid, survive a few patent challenges, and watch your margins compress the moment a second or third filer gets approved. That model still works at scale, but it no longer drives the growth targets that large generics manufacturers and mid-size specialty pharma companies need to justify their pipelines.
Complex generics are different. A company that successfully launches a generic version of a branded inhalation product, a transdermal system, a liposomal injectable, or a locally acting topical drug does not simply share a market. It frequently controls it for two to four years before a second generic arrives, and sometimes much longer. The regulatory and scientific barriers that delayed its own approval become, once cleared, the same barriers that slow every competitor behind it.
This is the complexity premium: the combination of durable market exclusivity, elevated average selling prices, and compressed generic competition that makes complex generics structurally more valuable than conventional oral solids. Quantifying it requires understanding the mechanics of how the FDA defines, reviews, and approves these products, and how patent strategy, bioequivalence science, manufacturing requirements, and market positioning all interact.
This article covers the full picture. It examines how the FDA classifies complex drug products, what each classification means for development timelines and capital requirements, how to read the patent landscape using tools like DrugPatentWatch before committing resources, which regulatory pathways exist beyond the standard ANDA route, and how companies at the leading edge of this space actually execute launches.
The data throughout this article draws on FDA guidance documents, published literature, IQVIA market analysis, and case studies from companies including Mylan (now Viatris), Hikma, Amneal, Perrigo, and several specialty originators who have defended complex products against generic entry. Where relevant, it cites regulatory dockets and patent filings directly.
Defining the Territory: What Makes a Drug “Complex”
The FDA’s Working Definition
The FDA does not use a single statutory definition of “complex drug product.” Instead, the agency has built its understanding of complexity through a combination of guidance documents, program designations, and formal policy statements issued primarily since 2017, when the Drug Competition Action Plan gave complexity a formal place in FDA’s generic drug strategy.
The most operationally useful definition comes from the FDA’s own list of complex products maintained by the Office of Pharmaceutical Quality (OPQ). That list organizes complexity into four categories: complex active ingredients, complex formulations, complex routes of delivery, and complex drug-device combination products. Each category carries different development implications.
Complex Active Ingredients
This category includes peptides, proteins, oligonucleotides, and polymeric molecules where the active moiety itself presents characterization and bioequivalence challenges. It also includes naturally derived ingredients where batch-to-batch variability is intrinsic, such as heparins, complex mixtures like coal tar, and certain iron complexes.
The analytical challenge here is substantial. Demonstrating that a complex active ingredient is the same as the reference listed drug (RLD) requires advanced analytical methods, including mass spectrometry, NMR, X-ray crystallography, and increasingly, cryo-electron microscopy. For polymer-based molecules like low-molecular-weight heparins (LMWHs), the “sameness” standard becomes difficult to meet using traditional equivalence frameworks because the molecule itself is not a single defined chemical entity.
Enoxaparin sodium, the LMWH sold as Lovenox by Sanofi, took the FDA more than a decade to develop a workable approval pathway. When Sandoz finally received approval for its generic version in 2010, it did so by demonstrating physicochemical equivalence through multiple characterization methods, not just biological assay equivalence. The FDA’s guidance for enoxaparin, published in 2011, required applicants to characterize the heparin source material, the depolymerization process, the molecular weight distribution, specific disaccharide sequences, and anti-Xa and anti-IIa activity ratios [1]. That level of characterization adds two to three years to a development timeline and costs tens of millions of dollars before a single clinical study begins.
Complex Formulations
Complex formulations include liposomes, nanoparticles, microspheres, microemulsions, emulsions, gels, and depot formulations. The complexity here lies primarily in the relationship between formulation characteristics and pharmacokinetics. Two products may contain identical active ingredients but release and distribute them very differently based on particle size distribution, encapsulation efficiency, surface charge, and excipient composition.
Doxorubicin hydrochloride liposome injection (Doxil/Caelyx) is the reference case. After Ortho Biotech’s exclusivity expired, multiple companies attempted generic development. The FDA’s product-specific guidance for this product, updated in 2018 and again in 2022, requires applicants to characterize liposome morphology, lipid composition, encapsulation efficiency, drug release in simulated physiological conditions, and pharmacokinetic parameters through comparative clinical studies [2]. Sun Pharma received the first generic approval in 2013, but the path took years of iterative FDA feedback, and only a small number of generics are approved despite market entry occurring over a decade ago.
Microsphere injectables present similar challenges. Risperidone long-acting injection (Risperdal Consta) is a polymer microsphere product where the drug release profile over two to four weeks determines clinical performance. Demonstrating bioequivalence for a product like this requires understanding polymer degradation kinetics, in vitro-in vivo correlations, and the interaction of particle size with tissue pharmacokinetics. The FDA did not approve a generic for Risperdal Consta until 2023, roughly fifteen years after the branded product launched [3].
Complex Routes of Delivery
Inhalation products, both metered-dose inhalers (MDIs) and dry powder inhalers (DPIs), sit at the center of this category. Inhalation bioequivalence is a genuinely unsolved scientific problem. The FDA’s current thinking requires a weight-of-evidence approach that combines in vitro aerodynamic particle size distribution (APSD) characterization, pharmacokinetic studies, pharmacodynamic studies, and sometimes clinical endpoint studies.
The practical consequence is that bioequivalence demonstration for an MDI product like an albuterol or fluticasone/salmeterol inhaler requires multiple studies costing between $30 million and $80 million, depending on the complexity of the device, the particle formulation, and the therapeutic category. Teva’s ProAir HFA generic to Ventolin did not receive FDA approval until 2020, more than a decade after Teva filed its application [4].
Transdermal drug delivery systems (TDDS) sit in the same category. Bioequivalence for transdermal patches involves demonstrating equivalent drug delivery through skin, which depends on adhesive formulation, patch architecture, drug-in-adhesive versus reservoir designs, and the interaction of all these with individual patient skin characteristics. Dermal pharmacokinetics are notoriously variable, and FDA guidance for many transdermal products requires both in vitro membrane permeation studies and in vivo pharmacokinetic studies.
Topical products on nonintact skin or products intended for local rather than systemic action represent yet another subcategory. For these, the FDA has developed the concept of dermal bioequivalence, which relies on methods like the pharmacodynamic vasoconstrictor assay for corticosteroids or, more recently, dermatopharmacokinetic (DPK) methods that measure drug concentration in skin tape strips. Neither method is universally accepted, and product-specific guidance varies widely.
Drug-Device Combination Products
Combination products that combine a pharmaceutical with a delivery device fall under the jurisdiction of both CDER and CDRH (Center for Devices and Radiological Health). This dual oversight adds a regulatory dimension that pure drug generics do not face. The device component of an inhaler, autoinjector, or transdermal patch may itself be subject to 510(k) clearance requirements if the device design differs meaningfully from the RLD.
The autoinjector category is a good example. Adalimumab (Humira) biosimilars face biosimilarity requirements for the biologic itself and device comparability requirements for the autoinjector. For small-molecule drugs delivered by autoinjector, the device design must not differ in ways that affect drug delivery performance. FDA’s guidance on combination product bioequivalence describes a complex equivalence assessment that covers delivered dose, injection force, and residual volume [5].
The Market Opportunity: Size, Growth, and Concentration
A Market Worth Fighting For
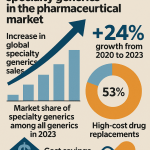
The total U.S. generic pharmaceutical market generated approximately $106 billion in dispensed prescriptions at wholesale acquisition cost in 2023, according to IQVIA data [6]. Complex generics represent a disproportionate share of that value. The top fifty generic molecules by revenue are dominated by products in the complex categories: inhaled corticosteroids, topical immunosuppressants, ophthalmic emulsions, long-acting injectable suspensions, and transdermal systems.
Glatiramer acetate (Copaxone), a complex polypeptide mixture used in multiple sclerosis, generated peak U.S. revenues of approximately $4.2 billion annually before generic entry. When Mylan and Sandoz received approvals in 2017, the branded product’s price declined but not as fast as conventional generic markets might suggest, partly because the complex manufacturing requirements limited new entrants [7]. Teva continued to generate significant revenues from both the brand and its authorized generic for several years post-entry.
The inhaled corticosteroid market tells a similar story. Advair Diskus (fluticasone/salmeterol), which had U.S. revenues exceeding $3 billion at peak, did not see a generic approved until Mylan’s Wixela Inhub received clearance in 2019, roughly four years after the core patents expired. The FDA’s rigorous bioequivalence requirements for DPIs delayed competition for years, and even post-approval, generic substitution rates remained well below the 90 percent levels seen in simple oral solid markets [8].
Why Margins Hold
The economic structure of complex generic markets differs from conventional generics in three measurable ways. First, the number of generic competitors at any given time is lower. In simple oral solid markets, five or more generics often compete within twelve months of the first approval. In complex drug markets, two or three competitors over a three-to-five year horizon is common, and in some categories, the first generic maintains effective market exclusivity for longer.
Second, brand-to-generic price erosion is shallower. For a simple oral solid, brand prices can fall 80 to 90 percent within two years of generic entry. For complex generics, the decline is typically 30 to 60 percent, and it happens more slowly. Patients and prescribers often have higher switching reluctance for inhaled, transdermal, or injectable products, partly because these products require patient training and partly because prescribers are cautious about substituting products where perceived differences in device design or formulation might affect outcomes.
Third, and most importantly from a strategic standpoint, the barriers to subsequent generic entry that the first approved company already overcame remain just as high for everyone who comes after. The first filer in a complex ANDA market does not need exclusivity provisions from Hatch-Waxman to maintain pricing power the way the first filer in a simple oral solid market does, though those provisions still help. The science and manufacturing requirements provide durable protection.
| Product Category | Typical Dev. Cost | Avg. Time to 1st Generic | Price Erosion (Yr 1) |
| Simple Oral Solid | $2M-$5M | 24-36 months post-patent | 60-80% |
| Complex Topical/Transdermal | $15M-$40M | 48-72 months post-patent | 30-50% |
| MDI/DPI Inhaler | $40M-$80M | 60-120 months post-patent | 20-40% |
| Liposomal Injectable | $30M-$60M | 48-84 months post-patent | 25-45% |
| Complex Polypeptide/LMWH | $50M-$120M | 72-144 months post-patent | 20-35% |
Table 1. Development economics comparison across generic drug complexity categories. Cost estimates based on published industry data and FDA meeting summaries. Timelines measured from first major patent expiry. Sources: IQVIA [6], FDA Generic Drug Program Reports [9], published industry surveys.
The Concentration Paradox
Despite the outsized opportunity, complex generics development is concentrated among a handful of companies. Teva, Hikma, Amneal, Perrigo, Sun Pharma, and Viatris collectively account for a large majority of approved complex generic applications. Smaller generics companies rarely have the financial capacity to fund the development programs required, and many early-stage specialty pharma companies lack the manufacturing infrastructure.
This concentration creates opportunity for companies that can build the required capabilities. A mid-size generics company that develops genuine scientific expertise in one complex category (say, topical semisolid bioequivalence or long-acting injectable microsphere manufacturing) can build a defensible franchise in that category that larger but less specialized competitors struggle to replicate quickly.
The capital requirements for complex generic development are substantial but not prohibitive for well-capitalized players. A company that secures $50 million to $100 million in development capital, allocates it to two or three programs in the same technical category, and builds a regulatory track record in that category can establish a competitive position that delivers premium economics for a decade or more.
Reading the Patent Landscape Before You Commit
Why Patent Analysis Comes First
The single most common strategic mistake in complex generic development is committing development capital before understanding the patent situation. Development programs for complex generics take four to eight years and cost tens of millions of dollars. A company that initiates development on a product protected by a deep patent estate with no viable challenge strategy may spend five years and $60 million only to discover that it cannot file a Paragraph IV certification that would survive litigation, or that the earliest plausible market entry date is a decade away.
Patent analysis for complex generics is not simple, partly because the relevant patents are not always limited to Orange Book-listed patents. A branded inhaler product may have Orange Book patents covering the active ingredient composition, the device design, and specific formulation claims. But it may also have non-Orange Book patents covering manufacturing processes, device components, or related formulations that a generic company cannot simply ignore even if they do not trigger mandatory 30-month stays.
Tools like DrugPatentWatch aggregate patent data, regulatory filings, and market intelligence into a searchable database that allows development teams to map the full patent landscape for a complex product before committing to a program. DrugPatentWatch tracks not only Orange Book listings but also patent expiry dates, exclusivity periods, ANDA filing histories, and the outcome of Paragraph IV certifications for thousands of drug products. For complex generics, where the patent landscape often involves dozens of patents across multiple portfolios, this kind of systematic mapping is not optional; it is the starting point.
Orange Book vs. Non-Orange Book Patents
The Orange Book (officially, the Approved Drug Products with Therapeutic Equivalence Evaluations) lists patents submitted by NDA holders that claim the drug substance, drug product, or method of use for approved products. When a generic company files an ANDA with a Paragraph IV certification challenging an Orange Book-listed patent, the NDA holder can sue within 45 days and trigger an automatic 30-month stay of FDA approval.
For complex drug products, the Orange Book listing is often only part of the picture. NDA holders routinely hold patents covering manufacturing processes, device engineering, secondary formulation features, and in some cases, specific patient populations or treatment protocols. These patents are not Orange Book-listed if they do not meet the statutory criteria for listing, but they can still be asserted in litigation after ANDA approval, exposing the generic company to infringement claims.
The litigation over Symbicort (budesonide/formoterol) illustrates this dynamic. AstraZeneca held Orange Book patents covering the drug combination and the aerosol formulation. It also held non-listed patents on device component design and on specific methods of propellant blending. When generic companies filed ANDAs, AstraZeneca’s litigation strategy included both Orange Book-triggered suits and pre-launch threatened litigation based on non-listed patents [10]. Generic companies that did not map the full patent portfolio before filing were caught off guard by claims they had not initially prepared to challenge.
Patent Expiry Calendars and Market Entry Windows
Complex products often have multiple patents with staggered expiry dates. A strategic analysis needs to identify the last-to-expire patent that covers a commercially relevant claim, because that patent determines the earliest market entry date absent a successful Paragraph IV challenge.
A hypothetical analysis of a transdermal fentanyl product might reveal: a composition patent expiring in 2025, a device design patent expiring in 2027, a method-of-use patent expiring in 2029, and a manufacturing process patent expiring in 2031. The generic company cannot launch before 2025 based on the first patent alone; it needs a strategy for all four. Whether it challenges all four in Paragraph IV certifications, designs around the device and process patents, or accepts a later-than-2025 entry window is a strategic choice with major financial implications.
DrugPatentWatch’s patent calendars allow development teams to model these scenarios systematically. By mapping every patent associated with a reference product, listing their expiry dates and claim scopes, and identifying which patents are likely vulnerable to invalidity or non-infringement arguments, a company can model the range of plausible market entry dates and assign probability weights to each scenario. That probability-weighted entry date, combined with projected market size and generic market share assumptions, drives the NPV calculation that should govern development decisions.
The average complex generic ANDA takes 53 months from submission to approval, compared to 37 months for a non-complex ANDA, and first-cycle approval rates for complex products are significantly lower. Companies that have not resolved patent issues before filing face a compounded delay risk that can add years to a program timeline.
— FDA Generic Drug Program: Fiscal Year 2024 Report, Office of Generic Drugs [11]
The Paragraph IV Certification Strategy
Paragraph IV certifications, which challenge Orange Book-listed patents as invalid, unenforceable, or not infringed by the proposed generic product, remain the primary tool for early market entry in patent-protected markets. For complex generics, the Paragraph IV strategy requires specialized analysis that goes beyond the invalidity and non-infringement arguments used for simple oral solid challenges.
In an inhaler product challenge, non-infringement arguments often center on device design differences. If the generic company’s inhaler delivers the same drug with comparable aerosol performance but uses a different actuation mechanism, valve design, or formulation process, it may have strong non-infringement arguments against device-related patents even while conceding composition claims have expired.
Invalidity arguments in complex generics cases often hinge on prior art that the PTO examiner did not consider, enablement issues (whether the patent specification teaches one skilled in the art how to make and use the claimed invention, which is often genuinely uncertain for complex formulations), and obviousness based on combinations of prior art references. The complexity of the technology cuts both ways: it means the inventions were genuinely difficult, making obviousness arguments harder, but it also means the scientific literature is deep enough that skilled patent litigators can often find prior art that undermines the novelty or non-obviousness of specific claims.
Inter Partes Review as a Pre-ANDA Tool
Inter partes review (IPR) at the Patent Trial and Appeal Board (PTAB) offers a faster and less expensive path to challenging patent validity than district court litigation. An IPR petition can be filed before or during ANDA litigation, and if instituted, it stays the district court case in many circuits. A successful IPR can invalidate claims that would otherwise block market entry, potentially years before a district court trial would conclude.
For complex generics with broad formulation patents, IPR petitions based on prior art references have an uneven but meaningful track record. PTAB instituted institution rates for pharmaceutical patents have varied considerably by patent type and technology area. Composition-of-matter claims with deep prior art histories in academic literature tend to be more vulnerable than method-of-use claims tied to specific clinical outcomes.
Companies like Mylan, Teva, and Amneal have used IPR petitions strategically, often filing petitions for the most defensible patents in a complex product’s portfolio while pursuing Paragraph IV certifications for others. This parallel track approach maximizes the chances of achieving early entry in at least some of the claim areas, even if not all.
Bioequivalence Science: Where Complex Generics Programs Live or Die
The Core Challenge
Bioequivalence for conventional oral solid generics is well-understood. Measure plasma concentrations after single-dose administration in fasting healthy subjects, calculate Cmax and AUC, demonstrate that both fall within 80 to 125 percent of the reference standard, and the science is done. The statistics are well-established, the studies are relatively inexpensive, and hundreds of CROs worldwide can run them efficiently.
Complex generics break this model at multiple points. Some complex products deliver drugs locally rather than systemically, so plasma concentration measurements do not capture the therapeutic equivalence question. Some products have nonlinear pharmacokinetics where standard two-period crossover designs give misleading results. Some products’ performance depends on patient technique, device characteristics, or site of delivery in ways that single-dose crossover studies cannot capture.
The FDA has responded to these challenges by developing product-specific bioequivalence guidance documents (PSGs) for over 2,000 products, with particularly detailed guidance for complex products. These documents, available on the FDA’s website and tracked systematically through resources like DrugPatentWatch’s regulatory intelligence database, specify the exact studies, methods, and statistical approaches required for each product. Reading a PSG carefully is both the starting point of a development program and a competitive intelligence tool: the studies described define the scientific barriers every competitor must clear.
In Vitro Methods and Their Limitations
For many complex products, the FDA’s PSGs begin with in vitro characterization requirements that establish the physicochemical equivalence of the generic to the RLD. These requirements vary enormously by product type.
For transdermal patches, in vitro permeation testing (IVPT) through human skin membranes under controlled conditions provides data on drug flux rates and cumulative delivery profiles. The FDA’s 2023 guidance on IVPT methodology emphasizes the importance of skin donor selection, skin preparation, receptor fluid composition, and temperature control [12]. A generic patch that shows equivalent IVPT performance has cleared a necessary but not sufficient hurdle; it still needs in vivo pharmacokinetic equivalence for most products.
For inhaled products, in vitro aerodynamic particle size distribution (APSD) testing using cascade impactors measures the size distribution of aerosol particles produced by the inhaler. This is directly relevant to lung deposition because only particles below 5 microns typically reach the lower airways; larger particles deposit in the throat. The FDA’s approach requires APSD equivalence across multiple device orientations and flow rates, reflecting real-world use conditions.
For topical dermatological products intended for local skin action, the FDA has moved toward accepting dermatopharmacokinetic (DPK) studies as the primary bioequivalence method for many products. DPK studies measure drug concentrations in successive layers of stratum corneum collected by sequential tape-stripping, providing a direct measure of drug penetration into the target tissue. This method is more sensitive and specific than plasma pharmacokinetic measurements for locally acting products, but it requires specialized methodology and is subject to significant variability.
Clinical Endpoint Studies: When They’re Required and Why They’re Expensive
For the most challenging complex products, the FDA requires clinical endpoint studies, which are essentially replications of the pivotal trials that supported the brand’s approval but designed to demonstrate equivalent outcomes between the generic and the RLD. These studies are expensive and slow, typically costing $20 million to $50 million and taking two to five years depending on the therapeutic area.
Ophthalmic products for glaucoma represent one category where clinical endpoint studies are sometimes required, particularly for products like prostaglandin analogs where the primary efficacy endpoint (intraocular pressure reduction) can be measured objectively but where small formulation differences might affect performance. The FDA’s PSGs for latanoprost ophthalmic solution and bimatoprost ophthalmic solution have historically required comparative clinical endpoint data for generic applications [13].
Nasal sprays for allergic rhinitis present a similar challenge. The FDA’s PSG for triamcinolone acetonide nasal spray (Nasacort AQ) requires a battery of in vitro tests including spray pattern, plume geometry, droplet size distribution, and drug content uniformity, followed by in vivo pharmacodynamic studies measuring nasal symptom response [14]. For fluticasone propionate nasal spray, the FDA added clinical endpoint study requirements after early generics raised questions about whether in vitro equivalence adequately predicted clinical performance.
Modeling and Simulation as Development Accelerators
Physiologically based pharmacokinetic (PBPK) modeling has emerged as a tool for reducing the number of in vivo studies required in some complex generic programs. The FDA has accepted PBPK models as supporting evidence for certain complex formulation approvals, particularly for extended-release products where the relationship between dissolution and plasma concentration can be modeled with reasonable confidence.
For more complex products like inhalers and transdermals, computational lung deposition models and skin permeation models are active research areas but have not yet achieved regulatory acceptance as substitutes for in vivo data. Several research groups, including those at the University of Maryland’s School of Pharmacy, have published work on physics-based lung deposition models that may eventually support more efficient bioequivalence demonstrations for inhaled products [15]. Companies that invest in these modeling capabilities now are building tools that may significantly reduce development costs in five to ten years.
Regulatory Pathways Beyond the Standard ANDA
The 505(b)(2) Pathway as Strategic Tool
The 505(b)(2) pathway allows an applicant to rely on published literature or the FDA’s findings of safety and effectiveness for a previously approved drug in a new drug application. Unlike an ANDA, which must demonstrate pharmaceutical equivalence and bioequivalence to an RLD without any claimed clinical improvements, a 505(b)(2) application can support modifications to formulation, delivery system, or indication that differentiate the product from the reference drug.
For complex drug development, 505(b)(2) is often the right pathway for a product that addresses the same clinical need as a complex branded drug but through a meaningfully different formulation or delivery approach. A company developing a microsphere injectable formulation of a drug currently delivered as a daily oral tablet would likely file under 505(b)(2), relying on existing safety data for the drug substance while generating new data on the modified delivery system’s pharmacokinetics, safety, and efficacy.
The 505(b)(2) pathway also allows applicants to claim new Orange Book patents for their modified formulation, potentially building a proprietary position in the new delivery format. This is the pathway by which many specialty pharma companies have created complex products that themselves become the reference standard for subsequent generic competition. NovaBay Pharmaceuticals, Jazz Pharmaceuticals, and numerous other specialty pharma companies have used 505(b)(2) approvals to establish market positions in complex drug niches.
The 505(b)(2) pathway has Orange Book implications that require careful management. If a 505(b)(2) applicant lists patents in the Orange Book for a new formulation of an existing drug, it creates the possibility of being challenged by Paragraph IV certifications from generic companies. But it also means the applicant holds the patents and controls the defense. Companies that successfully navigate this cycle, using 505(b)(2) to establish a complex formulation and then defending it through Orange Book patents, can maintain pricing power for years beyond the original drug’s patent life.
The BLA Pathway for Complex Biologics and Biosimilars
Some products that sit at the boundary between complex small molecules and biologics require a Biologics License Application (BLA) rather than an NDA. Products like glatiramer acetate are legally treated as drugs under the FD&C Act despite their biological complexity, but products like growth hormones, insulins, and complex cytokines require BLA approval.
For biosimilar development, the FDA’s 351(k) pathway provides a route to approval by demonstrating biosimilarity to a reference biologic. Biosimilarity does not require identical characterization to the reference product (which would often be impossible given batch-to-batch variability) but does require a demonstration of no clinically meaningful differences in safety, purity, and potency. Interchangeability, a higher standard, requires evidence that the product can be substituted for the reference without the intervention of the prescribing physician and produces the same clinical result.
The distinction between complex small-molecule generics and biosimilars matters for market strategy. Generic drugs are automatically substitutable at the pharmacy in most U.S. states under standard therapeutic equivalence ratings. Biosimilars require either interchangeability designation or physician authorization for substitution in most states, making market penetration more dependent on active prescriber adoption. This difference in substitution dynamics is one reason biosimilar market shares often plateau well below the 90 percent levels seen for simple generic oral solids.
The NDA Suitability Petition: Expanding the Reference Product Base
An NDA suitability petition allows an applicant to petition the FDA to confirm that a new drug application for a modified version of an approved drug would be suitable for ANDA processing. This mechanism is rarely used for complex products but can be strategically valuable in situations where the modified product differs from the RLD in ways that might otherwise require a full NDA.
For example, a company developing a modified-release version of a drug currently approved only as an immediate-release product might petition the FDA for an ANDA suitability determination, arguing that the modified release profile represents a permissible difference under ANDA regulations rather than a substantive new drug requiring full NDA review. If the petition is granted, the company benefits from the streamlined ANDA review process rather than the full NDA pathway, saving several years of development time and tens of millions of dollars.
Citizen Petitions and Their Strategic Misuse
Citizen petitions allow any person to request FDA action, including requests that the agency set specific bioequivalence standards before approving complex generic applications. Brand-name companies have used citizen petitions strategically to delay generic approvals by filing petitions that require FDA response before it can approve pending ANDAs, effectively adding months of delay to competitor timelines.
The FDA Reauthorization Act of 2017 and subsequent FDA guidance have tightened the rules around delay-motivated citizen petitions, but they remain a tool in the competitive toolkit. Generic companies need to anticipate the possibility of citizen petitions from brand manufacturers when developing complex product entry timelines, and they should build contingency time into their launch planning to account for the possibility of petition-driven delays.
Generic companies can also use citizen petitions constructively, petitioning the FDA to issue or update product-specific guidance for products where existing guidance is insufficient for a generic program to proceed. Several generic companies have used petitions to accelerate FDA’s issuance of PSGs for products where scientific consensus on bioequivalence methodology was lacking. This strategy benefits the entire industry but can be particularly advantageous for companies that have already begun development under their own interpretation of what the FDA might require.
Manufacturing: The Silent Barrier
Why Manufacturing Is a Competitive Moat
Patent strategies and regulatory pathways get most of the attention in complex generics analysis, but manufacturing capability often determines whether a company can actually execute on an approved ANDA. Several complex generic categories require manufacturing processes that most generics companies cannot replicate without major capital investment and years of process development.
Liposomal drug products require specialized lipid processing and extrusion equipment, controlled atmosphere manufacturing, and precise control of particle size distribution throughout the manufacturing process. Small deviations in lipid composition ratios, hydration conditions, or extrusion parameters can produce liposomes with different encapsulation efficiencies, particle sizes, and stability profiles. Building a compliant liposomal manufacturing facility costs $50 million to $150 million and requires process development expertise that takes years to acquire.
Long-acting injectable microspheres require polymer chemistry capabilities, spray-drying or solvent-evaporation processes, and sterile fill-finish manufacturing for parenteral products. The poly(lactic-co-glycolic acid) (PLGA) polymer systems used in products like leuprolide acetate depot (Lupron Depot) and risperidone long-acting injectable must be manufactured within tight specification ranges for molecular weight, composition, and residual solvent content to achieve predictable drug release kinetics. Batch-to-batch consistency in polymer properties is critical and difficult to maintain at commercial scale.
Transdermal patch manufacturing requires coating equipment capable of applying uniform thin films of drug-in-adhesive formulations to release liners, lamination of multiple layers with precise thickness control, and die-cutting of individual patches with consistent adhesive area and drug content uniformity. The adhesive chemistry, coating process, and packaging all interact to determine product stability and performance. Perrigo, Noven (now part of Tesa Labtec), and LTS Lohmann are among the few CDMOs with genuine expertise in commercial-scale transdermal manufacturing.
Process Analytical Technology and Quality by Design
The FDA’s Quality by Design (QbD) initiative, introduced in pharmaceutical development through ICH Q8 and related guidances, has reshaped expectations for complex product manufacturing. QbD requires applicants to understand the relationship between critical material attributes, critical process parameters, and critical quality attributes of the finished product, and to design manufacturing processes that control variability by controlling its root causes.
For complex generics, QbD is not just a regulatory aspiration; it is a practical necessity. A generic inhaler manufacturer that does not understand how variations in excipient particle size, blending time, or filling conditions affect aerosol particle size distribution cannot consistently produce batches within APSD specification. The QbD approach, implemented through process analytical technology (PAT) tools that measure critical process parameters in real time during manufacturing, provides the control mechanisms needed to maintain batch-to-batch consistency at commercial scale.
Companies that have invested in PAT infrastructure for their complex generic manufacturing operations have a measurable advantage over competitors who rely on traditional end-product testing. PAT enables real-time release testing (RTRT), which can dramatically reduce batch testing cycle times and allows tighter process control. The FDA has been actively supportive of RTRT for complex products, recognizing that it provides better quality assurance than traditional sampling-based batch testing.
Scale-Up Challenges and Commercial Readiness
Many complex generic programs that clear the bioequivalence hurdle stall at scale-up. A formulation that performs beautifully in 50-liter batches can fail to meet specification when scaled to 500-liter or 2,000-liter commercial batches because mixing dynamics, heat transfer, and shear forces change with scale. The FDA expects applicants to demonstrate that their commercial-scale manufacturing process produces product equivalent to the batches used in bioequivalence studies, which typically requires manufacturing validation at commercial scale before the ANDA can be approved.
This scale-up requirement creates a capital commitment that occurs before approval and market entry, adding to the financial risk of complex generic programs. A company that completes development, files an ANDA, and then needs to build commercial-scale manufacturing capacity must do so without certainty of approval. Most companies address this through a combination of manufacturing partnerships with experienced CDMOs and phased capital investment tied to regulatory milestones.
Case Studies: Who Got It Right and Why
Mylan’s Glatiramer Acetate: A Multi-Year Campaign Executed Precisely
Glatiramer acetate, the active ingredient in Teva’s Copaxone, is a synthetic polypeptide mixture of four amino acids with variable molecular weight distribution. Demonstrating generic equivalence for this product required overcoming both scientific and regulatory hurdles that had no precedent in the generic drug approval history at the time Mylan began its program.
The FDA’s guidance for glatiramer acetate, developed in collaboration with Mylan and other applicants over many years, ultimately required characterization of amino acid composition, molecular weight distribution, specific optical rotation, nuclear magnetic resonance spectral profiles, circular dichroism spectra, and multiple immunochemical assays demonstrating that the generic stimulated the same immune response patterns as the brand [16]. No single analytical method was sufficient; the totality of the evidence had to establish sameness.
Mylan received tentative FDA approval for its 20 mg/mL glatiramer acetate injection in 2014 and final approval in October 2017 after the relevant patents were addressed. The commercial launch was executed rapidly, with Mylan achieving significant market share within months. Sandoz also received approval simultaneously, creating a two-generic market from day one. Together, the two generics achieved roughly 30 percent market share within the first year, less than most simple oral solid generics achieve in the same timeframe, but representing hundreds of millions of dollars in revenue given the size of the Copaxone market [7].
The lessons from the glatiramer acetate program are clear. First, scientific programs for complex polypeptide generics must engage with the FDA iteratively over many years, using the complex drug substance meeting process to build alignment on characterization requirements before committing to full development. Second, patent strategy must be resolved in parallel with scientific development, not sequentially. Mylan addressed the Paragraph IV litigation while completing its characterization program. Third, manufacturing investment must anticipate commercial needs years before approval.
Hikma’s Long-Acting Injectable Platform
Hikma has built one of the pharmaceutical industry’s more coherent complex generics strategies around long-acting injectables. Rather than treating each product as a standalone development project, Hikma has accumulated manufacturing capabilities, regulatory track records, and scientific expertise in the injectable space that allow it to pursue multiple programs more efficiently than a company approaching each product fresh.
Hikma’s U.S. injectable business, built partly through the acquisition of Boehringer Ingelheim’s Ben Venue facility in Ohio and subsequent investment in its own injectable manufacturing capabilities, processes both complex sterile liquids and suspensions. The company’s generic programs for products like aripiprazole lauroxil extended-release injectable suspension (a LAI antipsychotic) and naltrexone extended-release injectable suspension illustrate how platform-based development works: once the polymer chemistry, manufacturing process, and regulatory approach are established for one product in a category, they transfer more efficiently to the next.
The competitive advantage here is not just cost efficiency. It is speed. A company with established manufacturing processes and regulatory history in long-acting injectable microspheres can move from ANDA filing to approval faster than a competitor learning the technology for the first time. FDA reviewers also develop institutional familiarity with a company’s manufacturing approach, which can smooth the inspection and review process for subsequent products.
Perrigo’s Transdermal Leadership
Perrigo occupies a strong position in the U.S. transdermal generic market, with a portfolio of approved generic patches covering hormonal contraception, smoking cessation (nicotine), pain management (fentanyl, lidocaine), and cardiovascular applications (clonidine, nitroglycerin). This breadth reflects decades of investment in transdermal formulation science and manufacturing.
Perrigo’s approach to transdermal bioequivalence illustrates the platform strategy well. The company has developed internal expertise in IVPT methodology, validated skin testing facilities, and statistical approaches for transdermal bioequivalence that meet current FDA expectations. When the FDA updated its IVPT guidance in 2023, Perrigo was positioned to adapt its existing methodologies rather than building from scratch.
The transdermal contraceptive patch market provides a useful case study in competitive dynamics. Norelgestromin/ethinyl estradiol transdermal system (Xulane, generic for Ortho Evra) was approved as a generic in 2014. Perrigo and Agile Therapeutics are among the companies competing in this space. The technical barriers in transdermal contraceptive development include demonstrating equivalent drug delivery profiles for two hormones simultaneously through skin, managing adhesive performance for a product worn continuously for seven days, and ensuring consistent drug release over the patch wear period. These requirements sustained price premiums and limited competition for years after the brand’s core patents expired [17].
The Advair Diskus Generic: A Regulatory Odyssey Ending in Opportunity
The FDA’s approval of Mylan’s Wixela Inhub (fluticasone propionate/salmeterol inhalation powder) as the first generic for Advair Diskus in January 2019 concluded one of the most prolonged complex ANDA review processes in the FDA’s history. Mylan had first filed its application in 2008, and the approval came eleven years later after multiple Complete Response Letters, extensive Q&A meetings with the FDA, and major scientific breakthroughs in inhaler bioequivalence methodology.
The key scientific challenge was demonstrating that a generic dry powder inhaler could produce equivalent aerosol performance to Advair Diskus when patients used it under the range of real-world inhalation conditions. GSK’s DISKUS device uses a specific multidose blister mechanism that generates aerosol characteristics directly tied to the device’s air pathway geometry and blister foil tear force. Mylan could not use an identical device without infringing device patents, so it developed a device that produced equivalent aerosol performance through a different mechanical design.
The FDA required Mylan to demonstrate equivalence across device resistance, APSD at multiple flow rates, delivered dose uniformity, and in vivo pharmacokinetic and pharmacodynamic comparisons. The pharmacodynamic comparison used both a cortisol suppression study (for the corticosteroid component) and a bronchodilator response study (for the salmeterol component) in addition to standard PK studies [18].
The commercial result of this eleven-year investment was significant. Wixela Inhub launched with effectively no generic competition, and Mylan achieved market shares in the inhaled corticosteroid category that generated hundreds of millions in annual revenues. Companies that followed with their own generic Advair approvals (including Prasco’s authorized generic and eventually other ANDA holders) entered a market that Mylan had already organized around the generic product, with formulary positions established and supply chain relationships in place.
Building a Complex Generics Pipeline: Strategic Prioritization
The Product Selection Framework
Selecting complex generic programs to pursue requires a structured analysis that integrates market opportunity, patent vulnerability, scientific feasibility, manufacturing requirements, and competitive dynamics. Companies that make these decisions informally, based on intuition or opportunistic tip, consistently underperform those that apply systematic frameworks.
The framework has four analytical dimensions. Market opportunity quantifies the current U.S. brand revenue for the RLD, the likely market share capture for a generic entrant based on comparable product category dynamics, the expected number of generic competitors at launch and over the following three years, and the price erosion trajectory. This analysis should use current market data, ideally from sources like IQVIA’s MIDAS or similar market research databases, and should model scenarios from optimistic (first and only generic for two-plus years) to conservative (three generics at simultaneous launch).
Patent vulnerability quantifies the probability and timing of a successful patent challenge or design-around. It requires a detailed review of every Orange Book-listed patent and relevant non-Orange Book patent, an assessment of claim scope and prior art exposure, an understanding of the brand company’s litigation history and settlement behavior, and a realistic view of the costs and timelines of Paragraph IV litigation in relevant districts. The Southern District of New York and the District of Delaware handle the majority of ANDA patent litigation; their specific judicial cultures, discovery timelines, and bench strength in pharmaceutical patent law matter to this analysis.
Scientific feasibility assesses whether the company has or can acquire the scientific capabilities to develop and validate a bioequivalence methodology for the product. It requires reviewing the FDA’s PSG if one exists, understanding the state of the scientific literature on bioequivalence methodology for the product category, and honestly evaluating the company’s internal capabilities versus what would need to be acquired through CDMO partnerships, licensing, or hiring.
Competitive intelligence maps the current development landscape. How many companies have filed ANDAs or published development programs for the product? Where are they in their development timelines? What has the FDA’s interaction history with applicants in this category revealed about the regulatory hurdles? Resources like DrugPatentWatch and FDA’s ANDA filing data provide the foundation for this analysis, though it must be supplemented with primary research through conference monitoring, patent application tracking, and industry contacts.
Building Versus Buying Capability
For companies without existing complex generics capabilities, the build-versus-buy decision is central to pipeline strategy. Building internal capabilities takes five to ten years and requires sustained capital investment in equipment, facilities, and scientific talent. Acquiring a company or platform with existing capabilities can accelerate the timeline by several years but typically requires paying a premium over intrinsic asset value.
The CDMO partnership model offers a middle path. A company that partners with an experienced CDMO for manufacturing and with specialized CROs for bioequivalence studies can develop complex generic programs without owning the underlying technical infrastructure. The risks of this model are real: CDMO partnerships can be slow, knowledge transfer is imperfect, and the company does not build proprietary manufacturing expertise that would benefit future programs. But the capital efficiency of the CDMO model makes it the right choice for companies testing their first foray into complex generics.
Licensing is another option. Some companies with approved complex generic ANDAs have licensed manufacturing rights or commercialization rights to partners, particularly in international markets. A company building a complex generics portfolio can sometimes license an approved product from a development-stage company, capturing the commercial opportunity without the development risk, though at a lower margin than a self-developed product would generate.
International Markets: The Regulatory Multiplier
Complex generic strategies in the United States often have natural extensions to international markets, though the regulatory landscape differs materially. The EMA’s decentralized procedure and mutual recognition procedure allow generic companies to file in multiple EU member states based on a single reference member state review. But EMA’s bioequivalence requirements for complex products sometimes differ from FDA’s requirements, meaning that a generic developed for the U.S. market may not automatically satisfy European standards.
Japan, Canada, and Australia all have their own complex generic approval pathways with requirements that partially overlap with FDA’s but differ in important details. A company that builds a complex generic program with international strategy in mind from the beginning can design development programs that generate data packages satisfying multiple regulatory agencies simultaneously, rather than running separate programs for each market. This regulatory efficiency can dramatically improve the economics of complex generic development for products with large international markets.
FDA’s Current Priorities: Where the Agency Is Focused
The Generic Drug Program’s Complex Drug Initiatives
The FDA’s Office of Generic Drugs (OGD) has maintained complex drug products as a strategic priority since the Drug Competition Action Plan of 2017. The Complex Drug Substances and Products (CDSP) team within OGD coordinates product-specific guidance development, complex drug substance characterization programs, and scientific conferences that address unresolved bioequivalence methodology questions.
The FDA’s published list of complex drugs without approved generics, updated periodically, identifies products where the scientific community has not reached consensus on how to demonstrate bioequivalence. This list is strategically valuable because it identifies market opportunities where early movers who help develop the methodology can establish significant lead times. When the FDA works collaboratively with one or two generic applicants to develop a new bioequivalence approach, those applicants understand the regulatory expectations more deeply than later entrants, and their ANDA submissions are better aligned with what reviewers expect.
The FDA’s Critical Path Initiative and subsequent programs have supported research to develop bioequivalence methodologies for specific complex product categories. FDA has funded research on in vitro skin permeation models, lung deposition simulation, and in vitro-in vivo correlations for modified-release products. These research programs, tracked through the FDA’s Science and Research page and published in peer-reviewed journals, provide advance signals about where regulatory thinking is heading.
Draft and Final Guidances to Watch
Several FDA draft guidances issued since 2022 will shape complex generic development for the next five to ten years. The 2023 draft guidance on product-specific bioequivalence recommendations for ophthalmic products addressed long-standing uncertainties about bioequivalence for ophthalmic suspensions, nanosuspensions, and emulsions, introducing a tiered approach that allows sponsors to use in vitro methods as the primary basis for bioequivalence in products where systemic absorption is minimal and the drug product characteristics can be fully characterized analytically [19].
The FDA’s ongoing development of a weight-of-evidence framework for complex inhalation products represents another significant evolution. Rather than specifying fixed study requirements for every inhalation product, the weight-of-evidence approach allows sponsors to propose study designs based on the characteristics of their specific product and device, with FDA evaluating the totality of evidence rather than checking off a fixed list of required studies. This approach gives development teams more flexibility but also more responsibility for justifying their study choices.
The FDA’s 2022 guidance on locally acting gastrointestinal drugs addressed another complex product category that had lacked clear bioequivalence standards. Products like mesalamine delayed-release capsules, sucralfate oral suspension, and cholestyramine powder for oral suspension present unique bioequivalence challenges because their mechanisms of action involve local gut tissue rather than systemic absorption. The FDA’s guidance introduced a combination of in vitro dissolution studies, pharmacokinetic studies, and in some cases pharmacodynamic endpoints to address these products [20].
User Fee Goals and Review Timelines
GDUFA (Generic Drug User Fee Amendments) sets performance goals for FDA review of generic drug applications, including complex ANDAs. Under GDUFA III, which covers fiscal years 2023 through 2027, the FDA committed to reviewing 90 percent of original ANDA submissions within 10 months and 90 percent of complete responses within 6 months, with separate goals for complex and expedited applications [21].
In practice, complex ANDA review times continue to exceed these goals for many products. Complete Response Letters requesting additional data on bioequivalence, manufacturing, or labeling restart the review clock, and for complex products that require multiple cycles of FDA feedback, total review times of 48 to 60 months from original submission are common. Companies should build these extended timelines into their financial models and avoid situations where commercial launch plans depend on first-cycle approval of a complex ANDA.
The FDA’s PDUFA VII and GDUFA III agreements also include enhanced provisions for pre-ANDA meetings with OGD. Complex drug substance meetings, product development meetings, and controlled correspondence (written Q&A) processes allow applicants to resolve scientific and regulatory questions before filing, reducing the likelihood of receiving a Complete Response Letter on issues that could have been resolved in advance. Maximizing use of these pre-submission interactions is one of the highest-ROI activities available to complex generic development teams.
The Authorized Generic Counterstrategy
How Brand Companies Use Authorized Generics
An authorized generic (AG) is a copy of a branded drug that the brand company (or a licensee) markets under a generic name, often at a price discount to the brand but above the price of a Paragraph IV first-filer generic. AGs do not generate Paragraph IV litigation; they are simply marketed under the brand’s ANDA or as a sub-license of the brand’s NDA.
Brand companies use AGs strategically to limit the commercial value of Paragraph IV victories. Under the Hatch-Waxman framework, the first generic filer to challenge a patent earns 180 days of market exclusivity during which no other ANDA-based generics can enter. But an AG can enter during this exclusivity period because it is not an ANDA-based product. A first filer that anticipated a 180-day duopoly (two products: the brand and its generic) instead faces a triopoly (brand, AG, and first-filer generic) with substantially compressed economics.
For complex generics, the AG strategy matters differently. Complex products with limited generic competition for several years after the first approval present a prolonged window during which the brand company can deploy an AG. If the brand company prices its AG aggressively, it can prevent the first generic company from achieving the market share needed to justify its development investment. This risk is most acute for products where a single generic company has invested heavily to be first and where the brand company retains substantial manufacturing capacity for the product even as brand revenues decline.
Generic companies managing AG risk for complex products should model the AG scenario explicitly in their commercial projections, negotiate supply contracts that provide downside protection in the event of AG competition, and pursue market share through formulary positioning and patient access programs that build switching inertia before the AG can gain traction.
Settlement Strategies and Authorized Generic Provisions
Patent settlement agreements in Hatch-Waxman litigation frequently include provisions that give the settling generic company an authorized generic license in exchange for a delayed market entry date. These settlements, reviewed by the Federal Trade Commission under the “reverse payment” standards established by FTC v. Actavis (2013), represent an alternative to full patent challenges for generic companies that prefer commercial certainty over the risks of litigation.
For complex generics, settlement structures often include supply agreements where the brand company supplies the active ingredient or finished product to the generic licensee at defined prices and volumes. This is particularly common for complex active ingredients that the generic company cannot yet manufacture independently, or for device-based combination products where the brand company owns key manufacturing assets.
The Hatch-Waxman 180-day exclusivity period for complex products is less reliably valuable than for simple oral solids because, as discussed above, the patent litigation timeline for complex products can extend beyond the point at which the underlying patent would have expired anyway. A first-filer generic company that wins a Paragraph IV case for a complex product after six years of litigation may find that its 180-day exclusivity delivers less commercial value than expected if the brand patent would have expired within two years of the litigation victory regardless.
Building Your Regulatory Intelligence Infrastructure
Tracking the Pipeline Before it Becomes the Market
Competitive intelligence in complex generics is not a one-time exercise; it is a continuous monitoring function. Patent filings, ANDA submissions, clinical trial registrations, FDA meeting announcements, and competitive company financial disclosures all contain signals about where the competitive landscape is moving. A company that monitors these signals systematically has a substantial advantage over one that relies on periodic research reports.
The FDA’s ANDA filing data, published quarterly with a lag, shows the number of applications submitted for each product and their status. While the FDA does not identify ANDA applicants by name in most public disclosures, the numbers of applications filed and approved for each RLD drug provide a measure of competitive pressure. A product with twelve ANDAs pending approval and only three approved will face rapid price erosion when approvals accelerate; a product with two ANDAs pending has much better economics for both applicants.
Patent databases, including the USPTO’s Patent Full-Text Database, Google Patents, and commercial platforms like Derwent Innovation, allow development teams to track new patent filings by brand companies for complex products under development or recently approved. Early-stage patent applications that publish eighteen months after filing often reveal the technological direction of a brand company’s formulation development years before an NDA is filed, giving sophisticated generic developers advance insight into future target products.
DrugPatentWatch provides an integrated platform that combines Orange Book patent data, patent expiry calendars, ANDA application data, and regulatory intelligence for thousands of U.S. drug products. For complex generic development teams, the platform’s ability to track multiple data streams simultaneously, including patent listings, paragraph IV filings, court decisions, and exclusivity determinations, reduces the analytical burden of monitoring competitive developments across a pipeline of active programs. Teams that establish systematic workflows using regulatory intelligence platforms like DrugPatentWatch can identify emerging competitive threats or opportunities months or years before they become apparent to competitors relying on less structured monitoring approaches.
The Role of FDA Meeting Requests and Correspondence
FDA meeting requests and controlled correspondence submissions for complex products are public after a delay, through Freedom of Information Act (FOIA) releases. Monitoring FOIA disclosures related to complex product categories reveals what scientific questions other applicants are raising with the FDA, what guidance the agency is providing in response, and whether the FDA is developing consistent positions on bioequivalence methodology that will benefit all applicants or raising new requirements that will complicate existing development programs.
FOIA requests for FDA meeting minutes and correspondence related to specific complex products are a legitimate competitive intelligence tool that is underutilized by most generic development teams. The turnaround time for FOIA requests can be long, but the information obtained is often more specific and actionable than publicly available guidance documents. Companies that have built systematic FOIA monitoring into their regulatory intelligence programs accumulate a body of institutional knowledge about FDA’s thinking on complex product bioequivalence that is genuinely proprietary even though the underlying information is technically public.
Leveraging Scientific Publications
The scientific literature on complex drug bioequivalence is active and rich. Journals including the Journal of Pharmaceutical Sciences, the AAPS Journal, Pharmaceutical Research, and the European Journal of Pharmaceutics and Biopharmaceutics regularly publish research on bioequivalence methodology for complex product categories. Regulatory scientists at the FDA, European Medicines Agency, and Health Canada publish their own research and perspective papers that provide advance signals about regulatory thinking.
Tracking this literature systematically, using automated search alerts and structured review processes, is part of a well-functioning complex generic development operation. When FDA scientists publish papers suggesting that a particular in vitro method shows good in vivo correlation for a specific product category, it often presages the inclusion of that method in future PSG updates. Generic companies that track this signal and incorporate it into their development programs before the PSG is formally updated can be further along in their development when the PSG publishes, reducing the time from PSG publication to ANDA filing.
Financial Modeling for Complex Generic Programs
Building the NPV Model
The net present value model for a complex generic program must account for development costs, timeline uncertainty, regulatory outcome probability, patent challenge risk, competitive entry timing, and market dynamics in a way that simple generic models do not require. A robust model for a complex generic program typically has at least three scenarios: an optimistic case where the Paragraph IV challenge succeeds, FDA approval comes in one cycle, and the product launches as the first or second generic; a base case with one complete response letter, a settled patent case with a defined entry date, and three generic competitors at launch; and a pessimistic case where FDA requires clinical endpoint studies, patent litigation is lost, and market entry occurs several years later than originally planned.
The discount rate applied to complex generic programs should reflect the higher risk profile of these products relative to simple oral solid generics. Most sophisticated generic pharmaceutical companies use discount rates of 12 to 18 percent for complex programs, compared to 8 to 12 percent for conventional generics, reflecting the greater timeline uncertainty and capital intensity.
Development cost modeling for complex generic programs must account for the probability of requiring additional studies beyond the initial development plan. For inhaler products, development plans that assume a single round of bioequivalence studies often underestimate actual costs by 40 to 60 percent once the iterative process of FDA feedback and study redesign is accounted for. Building contingency budgets of 30 to 50 percent above the base development plan is standard practice among experienced complex generic developers.
Milestone-Based Capital Deployment
Structuring capital deployment around development milestones rather than committing the full budget upfront is critical for managing the financial risk of complex generic programs. Early milestones might include successful formulation development (proof-of-concept scale), positive FDA response to a controlled correspondence on bioequivalence methodology, a successful pilot bioequivalence study, and ANDA filing. Later milestones include FDA’s first-cycle review outcome, patent litigation outcomes, and commercial manufacturing validation.
At each milestone, the development team should re-evaluate the program’s expected value and decide whether to continue, pivot the development strategy, or terminate the program. This structured approach allows capital to be redeployed from programs where unexpected obstacles have materially reduced expected value to programs where the risk-adjusted return is better.
Staged financing through milestone-linked tranches is also common in complex generic programs funded by venture capital or private equity. Investors who provide development capital in tranches tied to successful completion of defined scientific and regulatory milestones limit their downside exposure while maintaining the option to increase investment in programs that demonstrate strong probability of success.
Partnership Economics
Complex generic programs frequently involve partnerships between developers (who own the scientific and regulatory expertise) and manufacturers (who provide manufacturing infrastructure) and commercializers (who own the sales force and market access capabilities). These partnerships require careful structuring to ensure that each party captures value proportional to its contribution.
For a developer-manufacturer-commercializer structure, typical economic splits might allocate 20 to 30 percent of net revenues to the developer for its scientific work and regulatory investment, 15 to 25 percent to the manufacturer for technology transfer and dedicated manufacturing capacity, and the balance to the commercializer for market development and ongoing operations. These splits vary significantly based on the relative difficulty of each contribution and the bargaining power of each party.
Royalty structures versus profit-share structures have different risk profiles. Royalties paid as a percentage of net revenues provide the developer with revenue regardless of the commercializer’s cost structure but may disincentivize the commercializer from aggressive price competition if the royalty erodes margin. Profit shares align incentives around profitability but expose the developer to the risk that the commercializer’s cost structure is higher than anticipated.
Looking Ahead: Emerging Categories and Unmet Opportunities
RNA-Based Therapeutics and Oligonucleotide Generics
The growing market for RNA-based therapeutics, including antisense oligonucleotides (ASOs), small interfering RNAs (siRNAs), and mRNA therapeutics, is creating the next generation of complex drug substance challenges for generic developers. The first ASO products have been on the market for over a decade (mipomersen, approved in 2013; various orphan ASOs from Ionis Pharmaceuticals), and as these products approach patent expiry, generic developers must solve characterization and bioequivalence challenges that are even more demanding than those faced for peptide generics.
Oligonucleotide generics require demonstration of sequence identity, backbone chemistry equivalence (phosphorothioate linkages, chemical modifications at specific positions), and equivalence of pharmacokinetic behavior in tissues where the drug accumulates (primarily liver and kidney). The FDA has not yet issued comprehensive guidance on oligonucleotide generic bioequivalence, and the scientific literature on this topic is active but not yet at consensus. Companies that engage with the FDA now on the scientific framework for oligonucleotide generics will have a multi-year advantage when the first commercially significant oligonucleotide patents expire.
Inhaled Drug Delivery Innovation
The inhaled drug delivery space continues to evolve in ways that create new complex generic opportunities. Soft-mist inhalers (SMIs), like the Respimat device used for tiotropium bromide (Spiriva), use aqueous formulations sprayed at low velocity through a mechanical nozzle, producing aerosols with different characteristics from both MDIs and DPIs. Generic development for SMI products requires device characterization and bioequivalence approaches tailored to the SMI technology, and the FDA has been developing product-specific guidance for SMI generics.
Inhaled combination products with three or more active ingredients, like triple therapy ICS/LABA/LAMA inhalers (fluticasone furoate/umeclidinium/vilanterol, marketed as Trelegy Ellipta by GSK), represent the next frontier of inhalation complexity. Demonstrating bioequivalence for three drugs simultaneously through a single inhalation device, with each drug having different aerosol performance requirements, adds a combinatorial complexity to the standard inhaler bioequivalence problem that generic developers are only beginning to address.
Complex Topical Immunomodulators
Topical tacrolimus (Protopic) and pimecrolimus (Elidel) remain markets where generic entry has been limited by bioequivalence challenges. Tacrolimus is a macrolide calcineurin inhibitor with complex skin penetration behavior; pimecrolimus is similarly complex. The FDA’s PSGs for these products require demonstration of equivalent drug concentration in skin via DPK methods, followed by comparative clinical endpoint studies measuring the EASI (Eczema Area and Severity Index) score in atopic dermatitis patients.
The clinical endpoint study requirement adds $30 million to $50 million to the development cost and three to five years to the timeline. Companies willing to make this investment in a product category where the brand has maintained high market share despite generic alternatives being theoretically possible may find the economics highly attractive. The total U.S. market for topical calcineurin inhibitors exceeds $1 billion annually, and generic penetration remains below levels seen in simpler topical categories.
Microbiome-Based Products and Complex Biological Mixtures
Fecal microbiota-based products, recently approved as Rebyota (RBX2660) and Vowst (SER-109) for recurrent Clostridioides difficile infection, represent an entirely new category of complex biological mixture that will eventually face generic competition. These products contain live microbial communities with complex and variable composition, and the framework for demonstrating “sameness” or therapeutic equivalence for a microbial mixture product does not exist yet.
The FDA’s engagement with microbiome product development is at an early stage, with preliminary guidance published in 2022 covering safety considerations for live microbiome-based products [22]. The generic or follow-on product pathway for these products will likely require a new regulatory framework, possibly combining elements of biosimilar pathways, botanical drug frameworks, and novel scientific approaches to demonstrating microbial community equivalence. Companies that engage with this question now, through research partnerships with academic microbiome researchers and early dialogue with the FDA, are positioning for opportunities that may not generate revenue for a decade but could be extremely valuable when the framework matures.
Execution: What Separates Winners from Also-Rans
The Pre-Filing Process as Competitive Weapon
In complex generics, the period between initiating development and filing an ANDA is where competitive positions are won or lost. Companies that use this period to align fully with FDA expectations, resolve patent strategy, and build manufacturing readiness arrive at the filing stage in a fundamentally different position from those who file with unresolved questions.
The pre-filing process should include at minimum: a preliminary bioequivalence strategy review with internal scientific leadership, a formal controlled correspondence or pre-ANDA meeting with FDA to confirm the bioequivalence approach, a detailed patent landscape analysis using platforms like DrugPatentWatch, a manufacturing readiness assessment including scale-up planning and any required facility upgrades, and a commercial launch readiness assessment covering supply chain, distribution agreements, and pricing strategy.
Companies that skip steps in the pre-filing process to reduce upfront costs consistently incur larger costs later in the form of complete response letters, additional studies, and delayed launches. The return on investment from thorough pre-filing preparation is high, particularly for complex products where a single additional bioequivalence study can cost $10 million to $30 million and take two to three years to complete.
Post-Approval Commercial Execution
Receiving FDA approval for a complex generic is not the end of the challenge; it is the beginning of the commercial execution phase. Complex products often require patient training programs, healthcare provider education, and managed care formulary access that simple oral solid generics do not need. An inhaler generic requires patients and caregivers to learn device use. A transdermal patch requires education about application site rotation and disposal. A long-acting injectable requires administration training for healthcare providers and patient scheduling systems.
Companies that treat complex generic launches like simple oral solid launches consistently underperform. The same properties that make these products scientifically complex make them commercially complex. Market access teams need clinical data that supports equivalent outcomes, not just equivalent bioavailability. Managed care formulary committees need to understand the clinical equivalence evidence for products where prescribers have historically been reluctant to switch.
The most successful complex generic launches build relationships with key opinion leaders in the relevant specialty, provide clinical education on the bioequivalence evidence base, and work proactively with pharmacy benefit managers to secure preferred formulary status before product launch. These activities require commercial investment beyond what is typical for simple generic launches, but they pay back through faster formulary adoption and higher market share in the critical first twelve months.
Supply Chain Resilience for Complex Products
Complex generic products frequently have supply chains that are more fragile than those for simple oral solids. A liposomal injectable depends on specialty lipids from a small number of qualified suppliers. A long-acting microsphere injectable depends on pharmaceutical-grade PLGA polymer from a limited supplier base. A transdermal patch depends on specialty adhesives and release liners from highly specialized suppliers.
Supply disruptions for complex products can be catastrophic for commercial operations. A company that cannot supply product to the market for three to six months loses formulary positions and market share that are extremely difficult to recapture. Building supply chain resilience through dual-source qualification for critical materials, safety stock management, and supply agreement structures that provide priority allocation in shortage conditions is an essential component of complex generic commercial strategy.
The COVID-19 pandemic exposed supply chain vulnerabilities across the pharmaceutical industry, but the effects on complex generic products were disproportionate because the specialized supply chains for these products have fewer redundancies. Companies that invested in supply chain resilience before the pandemic maintained product availability while competitors faced shortages. That supply chain reliability translated directly into market share gains that have persisted years after the acute supply disruptions resolved.
Key Takeaways
• Complex generics command structurally higher margins than conventional oral solids because the scientific, regulatory, and manufacturing barriers that delay your own approval become identical barriers for every competitor who follows you.
• The FDA classifies complex products across four categories: complex active ingredients (peptides, LMWHs, polypeptide mixtures), complex formulations (liposomes, microspheres, nanoparticles), complex routes of delivery (inhalers, transdermals, topicals), and drug-device combination products. Each category requires a different development approach.
• Patent analysis must precede development investment. Using tools like DrugPatentWatch to map both Orange Book and non-Orange Book patents, model probabilistic market entry dates, and assess the viability of Paragraph IV certifications or design-around strategies is the foundation of sound complex generic program selection.
• The 505(b)(2) pathway offers a distinct strategic option for complex product developers who want to establish proprietary positions through modified formulations, potentially creating Orange Book patent estates that then attract their own generic challenges years later.
• Bioequivalence science for complex products is specific to the product category: IVPT for transdermals, APSD for inhalers, DPK for locally acting topicals, and multi-method characterization for complex active ingredients. Understanding and building expertise in the relevant methodology before filing is essential.
• Manufacturing capability is often the binding constraint in complex generic development. Platform-based strategies that accumulate expertise in one technical category (long-acting injectables, transdermals, liposomal products) generate compounding returns on manufacturing investment.
• The pre-ANDA meeting process, controlled correspondence program, and other FDA pre-filing interaction mechanisms are among the highest-ROI tools available to complex generic developers. Companies that use these tools to resolve bioequivalence methodology questions before filing dramatically reduce their Complete Response Letter risk.
• Commercial execution for complex generics requires investment in patient education, healthcare provider training, managed care access, and supply chain resilience that exceeds what simple oral solid generics need. Companies that plan for this upfront outperform those that treat complex generic launches as standard generic operations.
FAQ
1. What is the typical return on investment for a complex generic program compared to a conventional oral solid ANDA?
The answer depends heavily on product selection, competitive dynamics, and execution quality, but the economic structure is consistently more favorable for complex generics. A conventional oral solid ANDA typically generates revenues in the range of $5 million to $30 million over its commercial life, with peak revenues concentrated in the first 12 to 24 months before competition compresses margins. A well-executed complex generic program for a product in the $1 billion to $4 billion brand market can generate $150 million to $800 million in cumulative revenues over a three-to-seven-year period of limited competition. The development investment is higher, $30 million to $100 million versus $2 million to $5 million, but the return multiples are substantially better for successful complex programs. The key qualifier is “successful”: the failure rate for complex generic programs, defined as programs that do not achieve approval or that achieve approval after the commercial window has closed, is materially higher than for simple oral solid programs.
2. How should a company decide whether to pursue a Paragraph IV challenge or a design-around strategy for a complex generic?
The decision framework compares the probability-weighted value of each path. A Paragraph IV challenge is valuable when one or more key Orange Book patents have material invalidity exposure based on prior art, the brand company has a history of settling Paragraph IV cases on commercially reasonable terms, and the generic company has the litigation budget to sustain a multi-year district court case. A design-around strategy is preferable when the patents are well-crafted and difficult to challenge on invalidity grounds, the generic company’s scientific team can credibly develop a product that does not infringe the key claims, and the cost of designing around the patents is less than the expected cost of litigation. For complex inhalation products, design-around strategies based on alternative device designs have been successful for companies like Mylan (Wixela versus Advair DISKUS) and Cipla (Dulera/formoterol/mometasone MDI generics). For complex polypeptide generics where the patent covers the active ingredient composition broadly, Paragraph IV challenges are often the only viable path to early entry.
3. How do authorized generic agreements affect the economics of Paragraph IV first-filer exclusivity for complex products?
Authorized generics can substantially erode the commercial value of 180-day Paragraph IV exclusivity for complex products, just as they do for conventional generics. The economics are particularly sensitive for complex products because the 180-day exclusivity window may be the only period of limited competition before multiple generics enter simultaneously. A first filer that anticipated exclusive market access for six months (brand plus one generic) and instead faces an authorized generic from day one may see revenue projections reduced by 40 to 60 percent during the exclusivity period. The FTC has studied authorized generic competition extensively and found that AGs reduce the first-filer’s revenues by an average of roughly 50 percent during the exclusivity period [23]. Companies modeling complex generic program NPVs should use the AG scenario as their base case for products where the brand company has maintained manufacturing capacity and has financial incentives to protect market share through AG deployment.
4. What are the most common reasons complex ANDA programs fail, and how can they be avoided?
The most common failure modes in complex generic programs fall into four categories. First, bioequivalence methodology misalignment: applicants design and execute studies without adequate pre-ANDA FDA alignment, then receive Complete Response Letters requiring different studies. Prevention requires systematic use of FDA’s pre-submission meeting processes. Second, patent strategy gaps: applicants file Paragraph IV certifications on Orange Book patents without adequately assessing non-Orange Book patent risk, then face post-approval litigation on non-listed patents. Prevention requires comprehensive patent landscape analysis using all available tools, including commercial patent databases and platforms like DrugPatentWatch. Third, manufacturing scale-up failure: formulations that perform well at development scale fail to meet specification at commercial scale, triggering manufacturing-related CRLs or post-approval compliance actions. Prevention requires early investment in scale-up activities and QbD-based process understanding. Fourth, competitive timing miscalculation: programs are initiated and funded for products where the development timeline extends beyond the commercially viable window because multiple competitors achieve approval before the applicant does. Prevention requires rigorous competitive intelligence and honest assessment of development timelines before committing capital.
5. How is the FDA’s evolving guidance on weight-of-evidence approaches for inhalation bioequivalence changing the economics of inhaler generic development?
The shift toward weight-of-evidence approaches for inhaler bioequivalence has two competing economic effects. On the positive side, it potentially reduces the rigid requirement for clinical endpoint studies in some cases where strong in vitro equivalence data can be supplemented with PK/PD studies that fall short of full clinical endpoint study requirements. If a generic inhaler developer can demonstrate equivalence through a well-justified combination of in vitro APSD, PK, and PD studies without a full multi-arm clinical trial, the development cost for that product might decrease by $15 million to $40 million. On the negative side, the weight-of-evidence framework increases the regulatory uncertainty of individual programs because the outcome depends on FDA’s subjective assessment of the evidence package rather than a checklist of required studies. Companies that build strong scientific justifications for their study designs, engage with the FDA iteratively through the development process, and document their weight-of-evidence rationale carefully are better positioned to benefit from this flexibility than those who treat it as permission to do less science. The economics improve for companies with genuine scientific depth and become more uncertain for those without it.
References
1. U.S. Food and Drug Administration. (2011). Draft Guidance on Enoxaparin Sodium. Office of Generic Drugs. https://www.fda.gov/media/75286/download
2. U.S. Food and Drug Administration. (2022). Product-specific guidance for doxorubicin hydrochloride (liposomal). Office of Generic Drugs. https://www.accessdata.fda.gov/scripts/cder/psg/index.cfm
3. U.S. Food and Drug Administration. (2023). ANDA approval letter: Risperidone extended-release injectable suspension. Drugs@FDA. https://www.accessdata.fda.gov/drugsatfda_docs/appletter/2023
4. U.S. Food and Drug Administration. (2020). First generic drug approvals: Albuterol sulfate inhalation aerosol. FDA Drug Approvals and Databases. https://www.fda.gov/drugs/first-generic-drug-approvals
5. U.S. Food and Drug Administration. (2019). Use of International Standard ISO 11608-5 “Needle-Based Injection Systems for Medical Use” as a Consensus Standard for Combination Products (Guidance for Industry). https://www.fda.gov/regulatory-information/search-fda-guidance-documents
6. IQVIA Institute for Human Data Science. (2024). The Use of Medicines in the U.S. 2024: Usage and Spending Trends and Outlook to 2028. IQVIA. https://www.iqvia.com/insights/the-iqvia-institute/reports
7. Mylan N.V. (2018). Annual Report 2017: Generic glatiramer acetate commercial performance. Mylan Investor Relations. https://investor.mylan.com
8. GlaxoSmithKline plc. (2020). Annual Report: Advair market dynamics and generic competition. GSK Investor Relations. https://www.gsk.com/en-gb/investors
9. U.S. Food and Drug Administration. (2024). Generic Drug Program: Fiscal Year 2024 Report. Office of Generic Drugs. https://www.fda.gov/drugs/generic-drugs/generic-drug-program-updates
10. Shire Pharmaceuticals v. Barr Laboratories, No. 05-cv-0206 (D. Del. 2007). AstraZeneca LP v. Breath Ltd, No. 09-cv-01249 (D.N.J. 2013).
11. U.S. Food and Drug Administration. (2024). Fiscal Year 2024 Generic Drug Program Performance Report. Office of Generic Drugs. https://www.fda.gov/drugs/generic-drugs
12. U.S. Food and Drug Administration. (2023). In vitro permeation test methodology for topical products: Guidance for industry. Office of Pharmaceutical Quality. https://www.fda.gov/regulatory-information/search-fda-guidance-documents
13. U.S. Food and Drug Administration. (2022). Product-specific guidance for latanoprost ophthalmic solution, 0.005%. Office of Generic Drugs. https://www.accessdata.fda.gov/scripts/cder/psg/index.cfm
14. U.S. Food and Drug Administration. (2019). Product-specific guidance for triamcinolone acetonide nasal spray. Office of Generic Drugs. https://www.accessdata.fda.gov/scripts/cder/psg/index.cfm
15. Borghardt, J. M., Kloft, C., & Sharma, A. (2018). Inhaled therapy in respiratory disease: The complex interplay of pulmonary kinetic processes. Scientific Reports, 8, 9739. https://doi.org/10.1038/s41598-018-27786-3
16. U.S. Food and Drug Administration. (2014). Draft Guidance for Industry: Glatiramer Acetate Injection; 20 mg/mL and 40 mg/mL. Office of Generic Drugs. https://www.fda.gov/media/90979/download
17. Perrigo Company plc. (2020). Annual Report 2019: Prescription segment generic transdermal portfolio performance. Perrigo Investor Relations. https://investor.perrigo.com
18. U.S. Food and Drug Administration. (2018). Product-specific guidance for fluticasone propionate; salmeterol xinafoate inhalation powder. Office of Generic Drugs. https://www.accessdata.fda.gov/scripts/cder/psg/index.cfm
19. U.S. Food and Drug Administration. (2023). Draft Guidance: Product-specific bioequivalence recommendations for ophthalmic products using the locally acting NDA framework. Office of Generic Drugs. https://www.fda.gov/regulatory-information/search-fda-guidance-documents
20. U.S. Food and Drug Administration. (2022). Bioequivalence Guidance for Locally Acting Gastrointestinal Drug Products. Office of Generic Drugs. https://www.fda.gov/regulatory-information/search-fda-guidance-documents
21. U.S. Food and Drug Administration. (2022). Generic Drug User Fee Amendments III (GDUFA III) Commitment Letter. FDA-2022-N-0553. https://www.fda.gov/industry/fda-user-fee-programs/generic-drug-user-fee-amendments
22. U.S. Food and Drug Administration. (2022). Early Clinical Trials with Live Biotherapeutic Products: Chemistry, Manufacturing, and Control Information (Guidance for Industry). https://www.fda.gov/regulatory-information/search-fda-guidance-documents
23. Federal Trade Commission. (2023). Authorized Generic Drugs: Short-Term Effects and Long-Term Impact. FTC Bureau of Economics. https://www.ftc.gov/sites/default/files/documents/reports