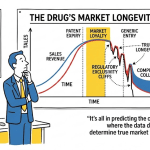
The countdown is relentless. For every blockbuster drug that reaches the market, a clock starts ticking, marking the finite years of patent-protected revenue. This period of market exclusivity is the economic engine of the entire pharmaceutical industry, the reward for a decade or more of high-risk, capital-intensive research and development (R&D) that costs, on average, over $2.2 billion per approved medicine.1 But this engine has a built-in kill switch: patent expiration. When that switch is flipped, the precipitous drop in sales that follows—aptly and ominously termed the “patent cliff”—can feel like falling off the edge of the world.
For companies heavily reliant on a single product, this is an existential threat. For the industry as a whole, it is a recurring, predictable, and market-shattering phenomenon that represents a massive, multi-billion-dollar transfer of wealth from innovators to generic and biosimilar manufacturers.4 The most successful organizations, however, don’t see the patent cliff as an endpoint. They understand that the loss of exclusivity (LOE) is not a catastrophe but a transition point—a strategic inflection that separates the proactive from the reactive.5 They have mastered the art of the second act.
This is the domain of Pharmaceutical Lifecycle Management (LCM). Far more than a collection of defensive, last-minute tactics, true LCM is a holistic, forward-looking discipline. It encompasses all strategies and activities designed to maximize a drug’s value—both therapeutic and commercial—throughout its entire lifespan, from the earliest stages of clinical development to the challenging post-exclusivity era.6 As pharmaceutical consultant Dr. Sarah Johnson aptly puts it, “Late-stage lifecycle management is about squeezing every ounce of value from a drug while ensuring it continues to meet patient needs. It’s a delicate balance of commercial strategy and medical responsibility”.5
This report is a comprehensive, expert-level framework for mastering that second act. It is a strategic manual for the business development, R&D, intellectual property, and commercial teams tasked with navigating the most treacherous phase of a product’s life. We will move beyond theory to provide a data-driven playbook of 15 distinct LCM strategies, grounded in real-world case studies of both landmark successes and cautionary failures. The goal is to provide an actionable guide for turning a potential free-fall into a “controlled descent,” preserving significant value long after the primary patents have expired and, in some cases, creating entirely new trajectories for growth.5 Organizations that wait until the final years of a product’s patent life to consider their defensive strategy are not just late to the game; they are playing a different, far less profitable one, risking immense value left on the table.5 This is the playbook for winning.
Part I: Understanding the Precipice – The Modern Patent Cliff
Before delving into the strategic countermeasures, it is essential to grasp the full scale and evolving nature of the threat. The patent cliff is not a static concept; its contours are constantly being reshaped by the types of drugs losing protection, the shifting regulatory landscape, and the powerful psychological impact it has on market valuation long before the first dollar of revenue is lost.
The Inescapable Gravity of Patent Expiry: Quantifying the Threat
The term “patent cliff” is a colloquialism, but one that aptly captures the phenomenon: a sharp, sudden, and often catastrophic decline in revenue that a company experiences when a blockbuster drug loses its legal monopoly and faces a flood of generic or biosimilar competition.9 The moment a patent expires, the market dynamics shift from monopolistic to intensely competitive, triggering a rapid price war and a dramatic erosion of the originator’s market share.12
The financial impact is staggering. It is not uncommon for a blockbuster drug’s revenue to plummet by 80% to 90% within the first year of generic entry.9 This is not a hypothetical risk; it is a well-documented historical pattern. When Pfizer’s cholesterol-lowering drug Lipitor—once the best-selling drug in the world—lost its patent protection in 2011, its worldwide revenues fell an astonishing 59%, from $9.5 billion in 2011 to $3.9 billion in 2012.9 Similarly, Plavix, an anti-platelet drug from BMS and Sanofi, experienced a comparable drop upon its 2012 expiration.9
This is not a historical anomaly. The industry is currently staring down the most severe patent cliff in its history.
Between 2025 and 2030, nearly 200 blockbuster drugs will lose patent protection, putting approximately $400 billion in annual revenue at risk. This impending wave of expirations is forcing companies to aggressively restock their pipelines and master the art of lifecycle management to survive. 5
This looming cliff is of a different magnitude than previous ones. The wave of expirations in the early 2010s, which included Lipitor, eroded an estimated $100 billion in sales.18 The current cycle, however, puts over $300 billion in sales at risk between 2023 and 2028 alone.18 For individual companies, the exposure can be immense, with potential losses ranging from $6 billion to $38 billion, and five of the top 10 pharmaceutical firms face a potential hit exceeding 50% of their current revenue.17
However, the true impact of the patent cliff begins long before the loss of exclusivity. The phenomenon exerts a powerful psychological and financial pressure on a company from the moment a blockbuster drug becomes a significant portion of its revenue. Financial markets are forward-looking, and a looming, unaddressed patent cliff is a massive red flag for investors and analysts. The threat of losing a primary revenue stream, even years in the future, leads to a discounting of a company’s future earnings potential. This can erode investor confidence, depress stock prices, and significantly limit a company’s access to the capital needed for future innovation.9
This creates a dangerous feedback loop. The very activities required to solve the patent cliff problem—intensive R&D to build a new pipeline or large-scale mergers and acquisitions (M&A) to buy new assets—are funded by the company’s market capitalization and access to debt markets. When a depressed stock price makes it more expensive to raise capital or use stock for acquisitions, the company’s ability to navigate the cliff is severely hampered. This transforms the patent cliff from a future operational challenge into a present-day strategic and financial crisis, forcing companies to act with urgency years before the actual patent expiry date.
More Than a Monolith: The Evolving LOE Landscape for Biologics
The current patent cliff is not just larger than its predecessors; it is fundamentally different in its composition. The wave of expirations in the early 2010s primarily involved small-molecule, chemical-based drugs like Lipitor.19 The current wave, however, is dominated by complex biologic drugs—therapies derived from living cells, such as monoclonal antibodies and other proteins.18 This list includes some of the most successful medicines in history, such as Merck’s Keytruda, BMS’s Opdivo, J&J’s Stelara, and Regeneron’s Eylea.19
This distinction is critically important because the competitive dynamics for biologics are different from those for small molecules. A generic version of a small-molecule drug is a perfect chemical copy, bioequivalent and fully interchangeable with the original. This allows for rapid substitution at the pharmacy level and leads to the precipitous 80-90% revenue drop.
Competitors to biologic drugs, known as “biosimilars,” are not perfect copies. Due to the inherent variability of manufacturing processes that use living cells, a biosimilar is only “highly similar” to the originator product, with no clinically meaningful differences in terms of safety, purity, and potency.21 They are not always considered automatically interchangeable, and their manufacturing process is vastly more complex and expensive than that of a small-molecule generic.19
This complexity has a profound effect on the post-LOE landscape. The entry of biosimilars tends to lead to a slower, more gradual erosion of the originator’s market share and revenue compared to the sheer cliff faced by small molecules.18 The case of AbbVie’s Humira, one of the first mega-blockbuster biologics to face biosimilar competition in the U.S., is instructive. In the first nine months after biosimilar entry in 2023, Humira’s sales fell by a significant but not catastrophic 30.8%—a steep decline, but far from the 80% cliff seen with drugs like Lipitor.9
This transforms the “patent cliff” metaphor into something more akin to a “patent slope” for biologics. This shift has critical strategic implications. The extended decline period provides a longer window for post-LOE lifecycle management strategies to take hold and fight for market share. Because a biosimilar is not an identical copy, it creates an opportunity for the originator company to compete on factors beyond price.
The strategic calculus must therefore evolve. For small molecules, the battle is often an all-out legal and regulatory war fought before the patent expires, because the commercial fight is largely lost on day one of generic entry. For biologics, while pre-LOE strategies remain vital, the post-LOE commercial battle is just as important. Originator companies can leverage the trust and brand equity built over years of safe and effective use. They can emphasize their vast repository of real-world evidence, their established patient support programs, and the subtle (or perceived) differences between their product and the new biosimilar entrants. This makes investments in generating long-term real-world data and building robust “beyond the pill” patient services not just value-added marketing tools, but core defensive assets in a prolonged war of attrition fought on the patent slope.
Part II: The LCM Playbook – 15 Strategies for Value Creation and Defense
Confronting a multi-hundred-billion-dollar revenue threat requires more than a single solution; it demands a sophisticated, multi-layered playbook. Pharmaceutical Lifecycle Management (LCM) is that playbook. It is the systematic process of managing a drug’s entire journey—from conception through design, manufacture, service, and disposal—to maximize its value and strategically delay market competition.6 Effective LCM is not a reactive defense mounted in the final years of patent life. It is a proactive, integrated strategy that should ideally begin during the R&D phase, weaving together developmental, commercial, and legal initiatives into a coherent, long-term plan.8
The following 15 strategies are the core plays in the modern LCM playbook. They are categorized into three fundamental pillars: (A) Developmental & Clinical Strategies, which focus on enhancing the core asset itself; (B) Commercial & Market-Facing Strategies, which reshape the competitive environment; and (C) Legal & Regulatory Strategies, which leverage the intellectual property and regulatory frameworks to protect value.
To provide a strategic overview, the following matrix summarizes these 15 strategies, outlining their primary objectives, typical timing, potential value, and key risks. This serves as a high-level guide for prioritizing and selecting the most appropriate tactics for a given asset and market situation.
Table 1: The Pharmaceutical LCM Strategy Matrix
| Strategy | Primary Objective | Typical Implementation Phase | Potential ROI / Value Driver | Key Risks & Challenges |
| A. Developmental & Clinical | ||||
| 1. Indication Expansion | Expand patient pool, enter new markets | Mid-Lifecycle | High – New revenue streams, market leadership | High clinical trial cost/risk, regulatory uncertainty |
| 2. Next-Gen Formulations | Improve patient experience, new patents | Mid- to Late-Lifecycle | Medium to High – Patent extension, brand loyalty | High R&D/manufacturing complexity, bioequivalence challenges |
| 3. Dosing Frequency Optimization | Enhance convenience and adherence | Mid- to Late-Lifecycle | Medium – Improved compliance, competitive differentiation | Formulation challenges, PK/PD hurdles |
| 4. Side Effect Profile Reduction | Improve tolerability, differentiate on safety | Mid- to Late-Lifecycle | Medium – Increased adherence, physician preference | Difficult to prove superiority, may require large trials |
| 5. Combination Therapies | Enhance efficacy, create new standard of care | Mid-Lifecycle | High – New patent, clinical superiority | High clinical trial failure rate, complex development |
| 6. “Encore” Product (2nd Gen) | Switch patients to new, patented drug | Late-Lifecycle | High – Extends franchise life | Risk of no clinical advantage, cannibalization, payer pushback |
| B. Commercial & Market-Facing | ||||
| 7. Rx-to-OTC Switch | Access mass consumer market, extend brand life | Late-Lifecycle / Post-LOE | High – New, large volume market | Cannibalization of Rx sales, high marketing costs, regulatory hurdles |
| 8. Geographical Expansion | Capture growth in emerging markets | Mid- to Late-Lifecycle | High – Long-term revenue growth | Regulatory complexity, IP risk, infrastructure gaps |
| 9. Strategic Alliances/JVs | Share risk/cost, amplify commercial reach | All Phases | Variable – Depends on deal structure and execution | Loss of control, partner misalignment, cultural clashes |
| 10. Post-Expiry Pricing Warfare | Slow generic erosion, retain brand share | Post-LOE | Medium – Brand revenue preservation | Margin erosion, potential antitrust scrutiny |
| 11. Digital Health Integration | Create “beyond the pill” value, increase stickiness | Mid-Lifecycle to Post-LOE | Medium to High – Differentiation, improved outcomes | Tech development cost, data privacy, regulatory uncertainty |
| C. Legal & Regulatory | ||||
| 12. Authorized Generic Gambit | Capture a share of the generic market | Post-LOE | Medium – Mitigates revenue loss | Can accelerate price erosion, complex logistics |
| 13. Patent Thickets/Evergreening | Delay and deter generic/biosimilar entry | Throughout Lifecycle | High – Monopoly extension | High legal costs, significant antitrust litigation risk |
| 14. Orphan Drug Designation | Gain 7-year market exclusivity for an indication | All Phases | High – Exclusivity independent of patents | Small patient population, high R&D risk for rare diseases |
| 15. Pediatric Exclusivity | Gain 6 months of additional market exclusivity | Late-Lifecycle | High – Significant revenue from 6-month extension | Cost of pediatric trials, risk of negative findings |
A. Developmental & Clinical Strategies: Reinventing the Core Asset
The most durable lifecycle management strategies are those that create genuine, demonstrable value for patients and physicians. Developmental and clinical strategies focus on enhancing the core product itself—making it more effective, safer, more convenient, or applicable to a wider range of medical needs. These are not mere marketing tactics; they are substantial R&D efforts that can result in new intellectual property and a fundamentally stronger value proposition.
Strategy 1: Indication Expansion – Unlocking New Patient Populations
Perhaps the most powerful developmental LCM strategy is indication expansion, also known as drug repurposing or repositioning. This involves the rigorous process of gaining regulatory approval to use an existing drug for new medical conditions beyond its original, approved use.24 For a drug company, this is akin to discovering a new oil field right next to a producing well.
The strategic rationale is compelling and multi-faceted. First and foremost, it dramatically expands the addressable market by unlocking entirely new patient populations.24 Second, a new indication is often treated as a new invention, allowing the company to secure new method-of-use patents and, in some jurisdictions, reset the clock on regulatory exclusivities for that specific use, thereby extending the drug’s protected commercial life.8 Finally, a new indication in an area of high unmet need can justify premium pricing and open access to previously restricted formularies.8
However, implementation is a complex strategic exercise, not a simple matter of finding a new use. A successful indication expansion program requires a disciplined assessment framework that systematically balances three critical dimensions: patient value (the severity of the disease and the level of unmet need), commercial value (revenue potential, competitive landscape, market access dynamics), and scientific fit (clinical confidence in the mechanism of action and the compound’s suitability for the new disease).26
Once potential new indications are identified, a company faces a fundamental strategic choice in its clinical development and launch sequencing: the “narrow first” versus the “broad first” approach.27
- Narrow First: This strategy involves launching first in a smaller, well-defined patient sub-population where the drug shows the highest efficacy. This allows the company to build a strong base of compelling clinical evidence, reassure regulators and payers about outcomes and budget impact, and potentially secure a favorable price that can be leveraged in future negotiations for broader indications.27
- Broad First: This approach aims to launch first in the largest possible patient population to maximize early revenue and establish a dominant market position before competitors can enter.27 However, this carries the risk of payer pushback due to budget impact concerns and potential questions about consistent efficacy across a heterogeneous population.27
Case Study: The Masterclass of Keytruda (pembrolizumab)
Merck’s Keytruda, an immuno-oncology agent, is the modern textbook example of a masterful indication expansion strategy. Instead of a “broad first” approach, Merck executed a brilliant “narrow first” strategy. It initially focused on a small, well-defined subset of patients: those with second-line non-small cell lung cancer (NSCLC) whose tumors had high expression of the PD-L1 biomarker.27 In this niche, Keytruda demonstrated superior outcomes, establishing a clear and defensible value proposition.
From this beachhead, Merck systematically and relentlessly expanded. It moved into first-line NSCLC for high PD-L1 expressers, then expanded to all NSCLC patients regardless of PD-L1 status, and then methodically marched across dozens of other cancer types, from melanoma to head and neck cancer to gastric cancer. Each expansion was backed by rigorous clinical data, transforming Keytruda from a niche product into one of the best-selling drugs in history, with sales exceeding $29 billion in 2023.9 This deliberate, evidence-based sequencing built a durable blockbuster franchise and serves as the gold standard for indication expansion.
Strategy 2: Next-Generation Formulations – Improving the User Experience
Beyond finding new uses for a drug, significant value can be created by finding better ways to deliver it. Developing next-generation formulations is a cornerstone of developmental LCM. This involves creating improved versions of an existing drug, such as an extended-release (ER) tablet, a new delivery system (e.g., a transdermal patch instead of an injection), or a more patient-friendly dosage form (e.g., an orally disintegrating tablet for patients with difficulty swallowing).6
The strategic goal is twofold. First, these improvements address real-world patient needs, enhancing convenience, improving adherence, and potentially reducing side effects.8 A patient who can take a pill once a day instead of three times, or use a patch instead of giving themselves an injection, is more likely to stay on therapy and remain loyal to the brand. Second, and crucially from a commercial perspective, a new formulation is often considered a distinct invention and can be protected by a new set of patents.8 This can add years of market exclusivity long after the original composition-of-matter patent has expired, effectively building a new patent wall around the franchise.
This strategy, however, is far from a simple repackaging exercise. It is a significant R&D endeavor that requires deep expertise in formulation science, polymer chemistry, and advanced manufacturing processes.
Case Study: The Convenience of Boniva (ibandronate)
Roche’s lifecycle management of the osteoporosis drug Boniva provides a clear example of successful reformulation driven by patient needs.28 Oral bisphosphonates, the class of drugs to which Boniva belongs, have notoriously strict administration requirements: patients must take them with a full glass of water on an empty stomach and remain upright for at least 30-60 minutes to avoid esophageal irritation. This regimen can be a significant burden and a barrier to adherence.
Recognizing this, Roche first reformulated the original once-daily Boniva tablet into a much more convenient once-monthly tablet. This was a major step forward, making Boniva the first oral treatment for a chronic disease to be administered monthly.28 But they didn’t stop there. Acknowledging that even the monthly oral regimen was difficult for some patients, they developed a third formulation: a quarterly intravenous injection administered by a healthcare professional.28 Each step in this reformulation journey addressed a specific patient friction point, providing a more convenient and user-friendly option that helped defend Boniva’s market share against competitors.
Case Study: The Complexity of Metoprolol Succinate ER
While the benefits of reformulation are clear, the technical hurdles can be immense. The development of a generic version of Metoprolol Succinate ER tablets serves as a powerful case study in the complexities involved.31 The innovator product, Toprol-XL, uses a sophisticated, patented drug delivery system. It is not a simple monolithic tablet; it is a multi-particulate system where the active drug is contained within thousands of tiny pellets. Each individual pellet is coated with a polymer to control the release rate, and these pellets are then compressed into a final tablet. This design achieves a consistent, 24-hour release of a highly water-soluble drug—a significant formulation challenge akin to “trying to build a dam out of sand”.31
For a generic manufacturer, simply matching the active ingredient is not enough. They must reverse-engineer and replicate this entire complex delivery mechanism to prove bioequivalence. This requires advanced analytical techniques to identify every excipient, deep expertise in polymer science to select the right hydrophilic matrix (like HPMC) with the correct viscosity and molecular weight, and precise control over manufacturing processes like wet granulation and compression.31 This case demonstrates that a well-designed formulation is not a trivial modification but a formidable technological barrier that can, in itself, be a powerful tool for lifecycle management.
Strategy 3: Optimizing Dosing Frequency – The Power of Convenience
A specific and highly effective subset of reformulation strategy is the deliberate focus on optimizing dosing frequency. Reducing the number of times a patient must take their medication—for example, moving from a three-times-daily regimen to once-daily—is one of the most impactful ways to improve the patient experience.23 In a world of busy schedules and complex treatment regimens for chronic diseases, the simplicity and convenience of a once-daily pill can be a powerful driver of both patient adherence and brand preference.32
The scientific challenge lies in creating a formulation that can maintain a drug’s concentration in the blood within its therapeutic window (the range where it is effective but not toxic) over a longer period. This requires a sophisticated understanding of the drug’s pharmacokinetics (PK), particularly its absorption, distribution, metabolism, and elimination half-life.33
Implementation typically involves advanced drug delivery technologies. For oral drugs, this often means creating an extended-release (ER) or modified-release (MR) formulation. This is frequently achieved by embedding the active drug within a hydrophilic polymer matrix, such as hydroxypropyl methylcellulose (HPMC). When the tablet is ingested, the polymer hydrates and forms a gel layer. The drug then slowly diffuses out of this gel layer over many hours, providing a smooth and sustained release profile instead of the sharp peaks and troughs seen with an immediate-release tablet.31 Successfully developing such a system can provide a strong competitive advantage and is often patentable.
Case Study: Xeljanz XR (tofacitinib)
A clear, modern example of this strategy is Pfizer’s management of its rheumatoid arthritis drug, Xeljanz. The original product was an immediate-release 5 mg tablet taken twice daily. Recognizing the value of a more convenient regimen, Pfizer developed Xeljanz XR, an 11 mg modified-release tablet designed for once-daily administration.28 The key to regulatory approval was a clinical pharmacology program that successfully demonstrated pharmacokinetic equivalence in key parameters between the new once-daily formulation and the original twice-daily version.28 This allowed Pfizer to offer patients a more convenient option, strengthening the Xeljanz brand and creating a new, patent-protected product line to help defend the franchise against future competition.
Strategy 4: Reducing Side Effect Profiles – A Better Tolerability Proposition
In many chronic diseases, patients may be on therapy for years or even decades. In this context, even seemingly minor side effects can have a major impact on quality of life and long-term adherence to treatment. A lifecycle management strategy focused on improving a drug’s safety and tolerability profile can therefore be a powerful differentiator, particularly in competitive therapeutic areas where multiple effective options exist.5
This strategy is often born not from initial clinical trials, but from the vast amount of data gathered during a product’s time on the market. Post-market surveillance and the growing universe of real-world evidence (RWE) are invaluable for identifying the real-world friction points that patients experience.5 Pharmacovigilance, often seen as a mere regulatory compliance function, can be transformed into a strategic asset.5 By systematically analyzing patient-reported outcomes, adverse event databases, and electronic health records, companies can identify patterns of persistent, low-grade side effects—such as nausea, headache, or dizziness—that may not have been prominent in the original, highly controlled clinical trials but significantly affect real-world patient experience.35
Once an issue is identified, reformulation can provide a solution. For example, if a side effect is linked to the high peak plasma concentration (Cmax) that occurs shortly after taking an immediate-release tablet, developing an extended-release formulation that provides a smoother, lower peak concentration can mitigate that side effect while maintaining overall therapeutic exposure (AUC).8 This creates a product with a superior tolerability proposition, which can be a compelling message for both physicians and patients.
Case Study: The Evolution of Abilify (aripiprazole)
The lifecycle of Otsuka’s atypical antipsychotic, Abilify, demonstrates how new formulations can address tolerability and adherence challenges in a difficult-to-treat patient population.37 The original product was an oral tablet for schizophrenia and bipolar disorder. While effective, ensuring daily adherence in this population can be a significant clinical challenge, and fluctuations in drug levels can impact both efficacy and side effects.
To address this, the company developed several new formulations. First came an oral solution, which offered improved bioavailability compared to the tablet.38 More significantly, they developed a ready-to-use intramuscular injection for controlling acute agitation, which provided 100% bioavailability and a much faster onset of action than the oral tablet.38 The culmination of this strategy was Abilify Maintena, a long-acting injectable (LAI) formulation administered once monthly. The LAI formulation provides consistent therapeutic levels of the drug over a prolonged period, which helps overcome the issue of daily non-adherence and can lead to a more stable clinical course with a potentially improved side effect profile compared to the peaks and troughs of oral dosing.37 This series of reformulations provided clinicians and patients with a range of options to better manage a complex chronic illness.
Strategy 5: Strategic Combination Therapies – Creating a New Standard of Care
Why offer one drug when you can offer a superior, integrated solution? A strategic combination therapy involves combining two or more distinct active pharmaceutical ingredients (APIs) into a single, synergistic product. This can be done as a fixed-dose combination (FDC), where both drugs are in a single pill, or as co-packaged products intended to be used together.6
The strategic value of this approach is immense. From a clinical perspective, a well-designed combination can offer superior efficacy by targeting a disease through multiple biological pathways simultaneously.39 It can also dramatically simplify treatment regimens for patients, reducing their daily “pill burden” and improving adherence, which is a significant clinical benefit in itself.5 From a commercial and legal standpoint, an FDC is considered a new product. It can be protected by a new set of patents, creating a fresh period of market exclusivity and effectively building a new franchise that can succeed the original single-agent products.5
This strategy is particularly prevalent in chronic diseases like hypertension, diabetes, asthma, and HIV, where multi-drug regimens are the standard of care. However, it is also one of the riskiest LCM strategies. The biological rationale for combining two drugs may be sound, but clinical development is fraught with challenges, including unexpected toxicities, negative drug-drug interactions, and a high rate of failure. In oncology, for example, combination trials now account for more than 25% of all clinical trials, yet the vast majority fail to demonstrate sufficient safety and efficacy to advance to later phases.41 The success rate for early-phase combination trials achieving regulatory approval is a sobering 12.4%.41
Success Case Study: Advair (fluticasone/salmeterol)
Advair, for the treatment of asthma and chronic obstructive pulmonary disease (COPD), is a landmark example of a successful combination therapy. It combines an inhaled corticosteroid (fluticasone propionate) to reduce inflammation with a long-acting beta-agonist (salmeterol) to open the airways.42 Numerous studies, including the large-scale TORCH trial, demonstrated that the combination was more effective at reducing the frequency of exacerbations, improving lung function, and enhancing quality of life than either of its components administered alone.43 This synergistic effect established Advair as a new standard of care and a multi-billion dollar blockbuster, fundamentally changing the treatment paradigm for respiratory diseases.
Success Case Study: Janumet (sitagliptin/metformin)
In the management of type 2 diabetes, Janumet is a prime example of a combination strategy focused on complementary mechanisms and patient convenience.45 It combines metformin, a first-line therapy that primarily reduces glucose production by the liver, with sitagliptin (Januvia), a DPP-4 inhibitor that increases insulin secretion in a glucose-dependent manner. By targeting two different aspects of the disease’s pathophysiology, the combination provides superior glycemic control compared to monotherapy.46 Just as importantly, it combines two pills into one, simplifying the regimen for patients who are often managing multiple medications. This dual benefit of enhanced efficacy and improved convenience has made Janumet a market leader in its class.45
Failure Case Study: Nivolumab + Relatlimab in Adjuvant Melanoma
The RELATIVITY-098 trial serves as a critical cautionary tale.47 This Phase 3 study tested the combination of two immune checkpoint inhibitors—nivolumab (an anti-PD-1 antibody) and relatlimab (an anti-LAG-3 antibody)—against nivolumab alone as an adjuvant (post-surgery) treatment for patients with resected melanoma. Despite the strong biological rationale and the success of the combination in advanced, metastatic melanoma, the trial failed to meet its primary endpoint. The combination did not significantly improve recurrence-free survival compared to nivolumab monotherapy.47
The potential reason for this failure highlights the nuances of drug development: the investigators hypothesized that in the adjuvant setting, where there is no visible tumor, the immune system may lack the necessary target to be fully activated by the dual checkpoint blockade. The presence of a tumor may be essential for the combination to exert its full effect.47 This case underscores the immense scientific risk of combination strategies; even a biologically plausible and previously successful combination can fail when moved into a different clinical setting, after an investment of hundreds of millions of dollars.
Strategy 6: The “Encore” Product – Developing Second-Generation Drugs
The “encore” or second-generation product strategy is one of the most direct, and most controversial, forms of lifecycle management. It involves developing a new, distinct molecular entity that is closely related to a successful first-generation drug. This new molecule is typically an active metabolite, a purified single isomer (enantiomer) of a racemic mixture, or a slightly modified analog of the original drug.48
The strategic goal is to launch this “new and improved” product shortly before the patent on the first-generation drug expires. The company then puts its full marketing muscle behind the new product, often promoting it as having superior efficacy, a better safety profile, or a more convenient dosing regimen, with the explicit aim of switching as many patients as possible from the old drug to the new, patent-protected one.48 If successful, this “product hop” can transfer the market share of the expiring franchise to a new one with a fresh lease on patent life.
This strategy is fraught with challenges. First, the second-generation product must offer a genuine, demonstrable clinical advantage to convince physicians, payers, and patients to switch. Without a clear benefit, it will be seen as a transparent attempt at “evergreening” and will face significant pushback. Second, the timing is critical; the new product must be approved and on the market with enough time to establish itself before the first-generation drug faces generic competition. Finally, this approach attracts intense legal and regulatory scrutiny, with critics arguing that it often involves patenting trivial modifications to stifle competition rather than fostering true innovation.49
Case Study: Claritin (loratadine) to Clarinex (desloratadine)
This is a classic example of a second-generation strategy that largely failed to meet expectations.51 Loratadine (Claritin) was a highly successful non-sedating antihistamine. Desloratadine (Clarinex) is its principal active metabolite. Schering-Plough launched Clarinex as a follow-on product, positioning it as a more refined version of the original. However, clinical studies failed to demonstrate any significant clinical advantage of desloratadine over its parent drug, loratadine.52 When Claritin made its highly successful switch to OTC status and then became available as a cheap generic, there was little compelling reason for patients or doctors to use the more expensive, prescription-only Clarinex. The lack of clear differentiation doomed the strategy.
Case Study: Zyrtec (cetirizine) to Xyzal (levocetirizine)
This case represents a more successful execution of the encore strategy.53 The original drug, cetirizine (Zyrtec), is a racemic mixture, meaning it contains equal amounts of two mirror-image molecules, or enantiomers: the levorotatory (left-handed) and dextrorotatory (right-handed) forms. Levocetirizine (Xyzal) is the purified, single levorotatory enantiomer, which is the more active form of the drug.53
The marketing and clinical argument for Xyzal was based on this scientific distinction. Because it contains only the active component, Xyzal is more potent than Zyrtec, allowing for a lower dose (5 mg for Xyzal vs. 10 mg for Zyrtec) to achieve a similar effect.54 Furthermore, some evidence suggested that by removing the less active dextro-enantiomer, Xyzal might be less likely to cause drowsiness, a key concern with all antihistamines.54 This provided a clearer and more scientifically grounded differentiation story than the Claritin/Clarinex case, allowing Xyzal to carve out a distinct and successful market position as a refined, second-generation option.
B. Commercial & Market-Facing Strategies: Reshaping the Battlefield
While developmental strategies focus on improving the product, commercial strategies focus on reshaping the market environment in which the product competes. These strategies are about positioning, access, and expansion—finding new customers, new channels, and new ways to communicate value in the face of mounting competitive pressure.
Strategy 7: The Rx-to-OTC Switch – Unlocking Mass-Market Potential
For the right product, the switch from prescription-only (Rx) to over-the-counter (OTC) status is one of the most powerful and transformative lifecycle management strategies available.23 It involves a rigorous regulatory process to prove to agencies like the FDA that a drug is safe and effective enough for consumers to self-diagnose their condition, self-select the product, and use it appropriately without the supervision of a healthcare professional.57
The strategic rationale is compelling. An Rx-to-OTC switch can be a lifeline for a product facing patent expiration. Instead of competing with low-cost generics in the prescription market, the brand can pivot to the massive consumer healthcare market, leveraging its established brand recognition and trust directly with consumers.57 This move opens up entirely new sales channels—supermarkets, convenience stores, online retailers—and a much larger potential customer base. Financially, the OTC market is substantial, with the value of switched products reaching around $35 billion in 2021 and projected to grow to $58 billion by 2031.58 Furthermore, the FDA may grant a three-year period of market exclusivity for a newly switched OTC product, providing a valuable buffer against private-label (generic OTC) competition.58
However, the switch is not without risks and challenges. The company loses the promotional power of physicians writing prescriptions. It must invest heavily in direct-to-consumer advertising to build and maintain brand awareness. There is also the risk of cannibalizing the remaining sales of the prescription version if a partial switch occurs.
Success Case Study: Claritin (loratadine)
The switch of Claritin is a landmark case in pharmaceutical history, not least because it was initiated against the manufacturer’s will.59 In 1998, the health insurer Blue Cross of California filed a citizen petition with the FDA to switch Claritin and two other non-sedating antihistamines to OTC status, arguing it would lower costs for the healthcare system.59 After a lengthy process, the FDA’s advisory committee agreed in 2001, and Schering-Plough, facing the inevitable, submitted its own application.59 The switch, which occurred in 2002, was a phenomenal success. Claritin leveraged its powerful brand name and its key differentiator—being non-drowsy compared to older OTC antihistamines like Benadryl—to become a dominant force in the consumer allergy market, extending the franchise’s life for many years.62
Challenges Case Study: The Prilosec (omeprazole) Precedent and the Zegerid Hurdle
Prilosec was the first proton pump inhibitor (PPI) to make the Rx-to-OTC switch in 2003 for the treatment of frequent heartburn.63 Its success established a new, highly profitable OTC category and gave it a six-year head start before the next PPI, Prevacid, made the switch.63 The Prilosec OTC approval became the benchmark against which subsequent PPI switches were measured.
This created significant hurdles for Zegerid (omeprazole with sodium bicarbonate), which sought to switch years later.65 The FDA’s primary concern was that Zegerid’s formulation resulted in a higher peak drug concentration (
Cmax) and greater overall exposure (AUC) than the benchmark Prilosec OTC.65 The agency issued a Complete Response letter, stating that the manufacturer had not provided adequate data to demonstrate that this higher exposure did not pose a safety risk, or alternatively, that it provided a corresponding increase in benefit to justify that risk.65 This forced the company into a lengthy and expensive process of conducting new pharmacokinetic studies to prove that Zegerid’s exposure, while higher than Prilosec OTC 20 mg, was still lower than the prescription 40 mg dose of Prilosec, a process that significantly delayed its potential switch and highlighted the stringent data requirements for this LCM strategy.65
Strategy 8: Geographical Expansion – Conquering New Frontiers
As growth slows and markets become saturated in the traditional strongholds of North America, Western Europe, and Japan, geographical expansion has become a critical imperative for long-term survival and growth.67 The primary focus of this expansion is on the so-called “pharmerging” markets—a group of high-growth nations including the BRICS (Brazil, Russia, India, China, South Africa) and MIST (Mexico, Indonesia, South Korea, Turkey) countries.67
The strategic rationale is grounded in undeniable macroeconomic and demographic shifts. These markets are the primary engines of global pharmaceutical volume growth. Between 2017 and 2022, the pharmaceutical markets in Brazil and India grew at staggering rates of 13.0% and 11.0%, respectively—nearly double the 7.1% growth of the U.S. market and the 6.6% average of the top five EU markets during the same period.67 This explosive expansion, fueled by rising incomes, growing middle classes, aging populations, and increased healthcare spending, has reshaped the competitive landscape. In just five years, the BRICS and MIST countries doubled their pharmaceutical sales to capture a remarkable 20% of the entire global market share.67 For a global pharmaceutical company, participation in these markets is no longer a “nice to have”; it is an essential counterbalance to patent cliffs and stagnation in their home markets.67
However, winning in emerging markets requires a fundamental shift in strategy. A one-size-fits-all approach imported from the West is destined for failure. These markets are not a monolith; they are a complex and fragmented mosaic of diverse regulatory systems, intellectual property risks, pricing pressures, cultural norms, and infrastructure gaps.67 Success requires a granular, localized approach. This often involves:
- Customer Clustering: Grouping consumers based on common health needs within regions, rather than by national boundaries, to tailor product offerings.69
- Strategic Partnerships: Forming joint ventures or alliances with local companies to navigate complex regulatory pathways, leverage established distribution networks, and gain invaluable local market insights.68
- Tiered Pricing and Access Models: Developing flexible pricing strategies that reflect local economic realities and high out-of-pocket spending burdens.67
- Digital Health Integration: Using telemedicine and digital health platforms to overcome infrastructure limitations and reach underserved populations in remote areas.68
The return on investment (ROI) for geographical expansion is a long-term proposition. While the initial costs of market entry, regulatory compliance, and building local infrastructure can be substantial, the strategic prize is immense. The companies that successfully establish a strong foothold in these high-growth regions today are positioning themselves to be the market leaders of tomorrow, securing revenue streams that will be crucial for funding the next generation of innovation long after their current blockbusters have gone off-patent in the West.26
Strategy 9: Strategic Alliances & Joint Ventures – Sharing Risk, Amplifying Reach
The journey of a drug from lab to market is long, expensive, and fraught with risk. Strategic alliances and joint ventures (JVs) are powerful LCM tools that allow companies to navigate this journey more effectively by sharing the burdens and rewards.71 These partnerships can take many forms, from co-development agreements where two companies pool R&D resources, to co-marketing or co-promotion deals where one company’s sales force helps to sell another’s product.72
The strategic rationale is clear. Alliances allow companies to:
- Share Costs and Risks: The enormous cost of late-stage clinical trials and global product launches can be shared, de-risking the investment for each partner.73
- Access Complementary Expertise: A partnership can combine the strengths of different organizations. A small, innovative biotech with a promising molecule can partner with a large pharmaceutical company that has the global infrastructure, regulatory expertise, and commercial muscle to bring it to market.73
- Amplify Market Reach: Two companies’ sales forces working together can achieve broader and deeper market penetration than either could achieve alone, which is especially important for launching a new drug into a competitive market.75
- Accelerate Timelines: Collaboration can speed up everything from clinical trial recruitment to market access negotiations, helping to get a drug to patients faster.68
While the potential benefits are significant, so are the risks. Misaligned objectives, cultural clashes between organizations, and disagreements over strategy or profit-sharing can derail a partnership. Success requires clear governance, shared goals, and a strong commitment to collaboration from both sides.75
Case Study: The BMS/Pfizer Alliance for Eliquis (apixaban)
The collaboration between Bristol Myers Squibb (BMS) and Pfizer to develop and commercialize the anticoagulant Eliquis is a textbook example of a highly successful pharmaceutical joint venture.76 BMS, which discovered the molecule, brought the R&D innovation. Pfizer brought its massive global commercialization infrastructure and agreed to fund 50-60% of the development costs. The partners share profits and losses equally on a global basis.77
Their shared challenge was immense: to unseat warfarin, the standard of care in anticoagulation for decades, which was effective and extremely cheap.78 The Alliance’s strategy was a masterclass in evidence-based marketing. They invested heavily in a wide-ranging program of real-world evidence studies, going beyond the pivotal clinical trials to demonstrate Eliquis’s performance in everyday clinical practice.78
These studies consistently showed two things. First, Eliquis was associated with a lower risk of stroke and fewer incidents of major bleeding compared to warfarin, especially in high-risk patient groups.79 Second, they made a compelling economic case: while the list price of Eliquis was much higher than warfarin, its use resulted in lower overall medical costs by avoiding expensive hospitalizations for major bleeds.78 By demonstrating both superior clinical outcomes and a strong economic value proposition, the BMS/Pfizer Alliance successfully established Eliquis as a new standard of care and a multi-billion dollar global blockbuster, showcasing the power of a well-executed strategic alliance.
Strategy 10: Post-Expiry Pricing & Rebate Warfare – Defending the Brand
The moment a blockbuster drug loses patent protection, the clock starts on a rapid and brutal price war. However, originator companies are not powerless bystanders. In the immediate post-LOE period, they can deploy aggressive and sophisticated pricing, rebate, and contracting strategies to defend the brand’s market share and slow the erosion caused by generics.81
This is a form of commercial hand-to-hand combat, leveraging the deep relationships and contractual power that the originator has built with payers, pharmacy benefit managers (PBMs), and distributors over the years of market exclusivity. The goal is to make it financially advantageous for the key players in the supply chain to continue favoring the branded product, even when a cheaper generic is available.83
Key tactics in this strategy include:
- Pre-Expiry “Surge” Pricing: In the 12-18 months leading up to patent expiry, some companies will implement a series of price increases on the branded drug. This maximizes revenue during the final period of monopoly and sets a higher baseline from which future generic discounts will be calculated.83
- Aggressive Rebate Contracts: The originator can offer deep rebates to PBMs and health plans in exchange for keeping the branded drug in a preferred or exclusive position on their formularies. In some cases, the net cost of the branded drug to the payer (after the rebate) can be made lower than the cost of the first generic, effectively blocking the generic from gaining traction.9
- Direct-to-Patient Discount Programs: With payers shifting more costs to patients through high co-pays and deductibles, originators can bypass the insurance system and offer discount cards or co-pay assistance programs directly to patients. These programs can lower the patient’s out-of-pocket cost for the brand to a level that is competitive with, or even lower than, the co-pay for the generic.9
Case Study: Pfizer’s Defense of Lipitor
Pfizer’s strategy following the patent expiration of Lipitor is the canonical example of post-expiry commercial warfare.9 Faced with generic competition from Ranbaxy, Pfizer unleashed a multi-pronged assault. The most famous component was the “Lipitor-For-You” rebate program. This was a direct-to-patient discount card that allowed many privately insured patients to get a month’s supply of branded Lipitor for a co-pay as low as $4—often less than the typical co-pay for a generic drug.9
Simultaneously, Pfizer went to war on the payer front. They offered massive rebates to insurance plans and PBMs that made the net cost of Lipitor lower than the generic. This was particularly effective in the mail-order pharmacy channel, where Pfizer was able to maintain a near-monopoly for a significant period.81 While these tactics were controversial and ultimately could not stop the eventual decline of Lipitor’s sales, they were highly effective at slowing the erosion, preserving billions of dollars in revenue for Pfizer and demonstrating that the post-expiry period can be a fiercely contested battleground rather than an immediate surrender.84
Strategy 11: Digital Health Integration – Creating Value “Beyond the Pill”
In an increasingly crowded and competitive market, one of the most forward-looking LCM strategies is to create value that goes “beyond the pill.” This involves integrating a pharmaceutical product with a digital health technology (DHT)—such as a smart sensor, a mobile application, a wearable device, or a data analytics platform—to create a holistic therapeutic ecosystem.29
The strategic rationale is to shift the basis of competition. When a drug goes off-patent, generic competitors can replicate the molecule, but they cannot easily replicate the data, software, and patient engagement ecosystem that has been built around it. A successful DHT integration creates a “sticky” product that is differentiated by its ability to improve patient outcomes, provide valuable data to clinicians, and enhance the overall patient experience.86 This builds a competitive moat based on data and user engagement, not just on the chemical compound itself.
The potential benefits are numerous. For patients, DHTs can provide medication reminders, track symptoms, offer personalized feedback, and improve their ability to self-manage a chronic condition.86 For healthcare providers, these tools can offer real-time insights into a patient’s adherence and disease status between office visits, enabling more proactive and data-driven care.86
However, this is a complex strategy to execute. It requires pharmaceutical companies to develop new core competencies in areas like software engineering, data science, cybersecurity, and human factors design.86 It also involves navigating a rapidly evolving regulatory landscape for software as a medical device (SaMD) and ensuring seamless interoperability with existing health IT systems like electronic health records (EHRs).86
Case Study: Propeller Health and Respiratory Inhalers (e.g., Symbicort)
Propeller Health provides a leading example of a successful digital health integration in the respiratory space.89 The company developed a small, FDA-cleared sensor that attaches to a patient’s existing asthma or COPD inhaler, including widely used products like AstraZeneca’s Symbicort.90
The sensor automatically records the time and location of each medication use and sends this data via Bluetooth to a companion app on the patient’s smartphone. The app provides patients with personalized insights, progress reports, and reminders. It also shares the data with the patient’s physician through a clinical dashboard, allowing the care team to monitor adherence patterns and identify patients who may be at risk of an exacerbation.89
The results have been clinically and commercially significant. Multiple clinical studies have shown that the Propeller platform can increase medication adherence by up to 58%, improve asthma control by up to 63%, and reduce asthma-related emergency room visits and hospitalizations by as much as 57%.90 By demonstrating a tangible improvement in patient outcomes, Propeller provides a powerful value proposition that differentiates the connected inhaler from a non-connected generic alternative. This transforms the product from a simple drug delivery device into an integrated disease management solution.
C. Legal & Regulatory Strategies: Mastering the Rules of Engagement
The third pillar of lifecycle management involves the masterful navigation of the complex legal and regulatory frameworks that govern the pharmaceutical industry. These strategies are rooted in a deep understanding of intellectual property law and regulatory pathways, and they are designed to maximize the duration and strength of a product’s market exclusivity.
Strategy 12: The Authorized Generic Gambit – Competing with Yourself to Win
The Authorized Generic (AG) gambit is a clever and widely used post-LOE strategy where the brand-name manufacturer competes with its own product.9 An AG is a pharmaceutical product that is produced under the original brand’s New Drug Application (NDA) but is marketed and sold as a generic. It is, in essence, the exact same drug as the brand, made on the same manufacturing line, but sold in generic packaging and at a lower price.81
The brand company can launch the AG itself or, more commonly, through a subsidiary or a partnership with an established generic manufacturer. The timing is critical: the AG is typically launched on the very first day that an independent generic competitor enters the market.9
The strategic rationale is multifaceted. First, it allows the originator company to capture a significant share of the generic market revenue that would otherwise be lost entirely to its competitors. Instead of ceding 100% of the generic volume, the brand company can retain a substantial portion of it through its AG sales.81 Second, the presence of an AG can increase price competition in the generic space from day one. This can put pressure on the profits of the first independent generic filer, who under the Hatch-Waxman Act is typically granted a 180-day period of generic exclusivity. By introducing an AG, the brand company can erode the value of that exclusivity period. Finally, it can create confusion in the market and help to maintain a relationship with pharmacies and distributors in the generic channel.
Case Study: Lipitor’s Authorized Generic Play
Pfizer’s defense of Lipitor provides a classic example of the AG strategy in action.9 When Lipitor’s main patent expired, the first independent generic was launched by Ranbaxy. On the very same day, Pfizer, through a pre-arranged deal with Watson Pharmaceuticals, launched an authorized generic version of atorvastatin.50
This move was a crucial part of Pfizer’s financial strategy to soften the blow of the patent cliff. Under the terms of its deal, Pfizer reportedly received approximately 70% of the revenue from Watson’s sales of the AG.50 This provided a vital stream of income that helped to offset the dramatic losses from the branded product. The AG, combined with the aggressive rebate strategies for the brand, allowed Pfizer to retain a much larger share of the total atorvastatin market value than would have been possible otherwise. It demonstrated that by being willing to compete with itself, an originator company can significantly mitigate the financial damage of LOE.
Strategy 13: Building the Fortress – Patent Thickets & Evergreening
Perhaps the most aggressive and controversial LCM strategy is the creation of a “patent thicket.” This involves filing a dense and complex web of dozens, or even hundreds, of secondary patents around a single drug.19 These patents typically do not cover the original active molecule itself, but rather incremental modifications such as new formulations, different dosage strengths, specific manufacturing processes, or new methods of using the drug.5 This practice is often referred to as “evergreening,” as its primary purpose is to extend the product’s effective monopoly well beyond the expiration of the original composition-of-matter patent.29
The strategic rationale is not necessarily to rely on the strength of any single secondary patent, but on the cumulative deterrent effect of the entire thicket. A generic or biosimilar manufacturer wishing to enter the market must navigate this legal minefield. Even if many of the patents are weak and could potentially be invalidated in court, the sheer cost, time, and complexity of challenging dozens of patents simultaneously can be prohibitive.94 The risk of infringing even one patent and facing a crippling lawsuit can be enough to force competitors to delay their launch or, more commonly, to enter into a settlement agreement with the brand manufacturer that allows for market entry at a much later date than would have otherwise been possible.95
This strategy exists in a gray area of law and ethics. Proponents argue that it represents legitimate protection for ongoing, incremental innovation.93 Critics, however, contend that it is an abuse of the patent system that exploits legal loopholes to stifle competition, delay access to affordable medicines, and place an undue burden on the healthcare system.93 This has led to increasing scrutiny from antitrust regulators and courts around the world.
Case Study: The Humira (adalimumab) Patent Fortress
AbbVie’s defense of its mega-blockbuster biologic, Humira, is the canonical example of a patent thicket strategy.92 While the primary patent on the adalimumab molecule expired in the U.S. in 2016, AbbVie was able to prevent any biosimilar competition until 2023. It achieved this by constructing an astonishingly dense patent fortress.
In the United States, AbbVie amassed approximately 136 patents related to Humira.95 Peer-reviewed research has suggested that as many as 80% of these patents were duplicative, covering non-patentably distinct inventions.94 When biosimilar manufacturers sought to enter the market, they were faced with the daunting and astronomically expensive prospect of litigating against this wall of patents. Ultimately, every single biosimilar competitor chose to settle with AbbVie, agreeing to a staggered and delayed market entry beginning in 2023.94
The impact of this strategy is starkly illustrated by comparing the U.S. market to Europe. In Europe, where patent laws are stricter regarding secondary patents, Humira’s patent estate was much smaller. As a result, biosimilars entered the European market in October 2018, more than four years earlier than in the U.S..94 The Humira case has become a focal point in the global debate over patent law, antitrust enforcement, and drug pricing, demonstrating the profound power of a well-constructed patent thicket to extend a product’s lifecycle.
Strategy 14: The Orphan Drug Designation Play – Leveraging Niche Incentives
The Orphan Drug Act of 1983 was designed to encourage the development of drugs for rare diseases, defined in the U.S. as conditions affecting fewer than 200,000 people.96 Because the small patient populations for these “orphan” diseases made it difficult for companies to recoup their R&D investments, the act created a set of powerful incentives to stimulate innovation in this area.96 As a lifecycle management strategy, obtaining an orphan drug designation can be an extremely valuable play.
The incentives are substantial and include tax credits for qualified clinical trials and exemptions from certain FDA user fees.96 However, the most significant benefit is the promise of seven years of market exclusivity for the approved orphan indication.98 This exclusivity is distinct from and runs independently of any patent protection. This means that even if a drug’s patents have expired, it can still be protected from competition in its orphan indication for seven years from the date of its approval for that use.
This creates several strategic opportunities. A company can develop a drug specifically for a rare disease, leveraging the incentives to de-risk development. Alternatively, as an LCM strategy for an existing drug, a company can pursue an orphan indication as a form of indication expansion.99 Securing an orphan approval for a drug that is also used for more common diseases can create a protected revenue stream and add significant value to the overall franchise. Since the legislation was enacted, orphan drugs have grown from a niche area to a major part of the pharmaceutical market, accounting for more than half of new active substance approvals in the U.S. in recent years.96
Case Study: The Orphan Empire of Eculizumab (Soliris)
Alexion Pharmaceuticals’ Soliris is a prime example of a company building a highly successful and durable franchise by strategically leveraging the orphan drug framework.97 Eculizumab is a monoclonal antibody that inhibits a part of the immune system called the complement cascade. Alexion systematically identified a series of rare, life-threatening diseases driven by uncontrolled complement activation and pursued orphan designations and approvals for each one.
Its journey began with an approval for Paroxysmal Nocturnal Hemoglobinuria (PNH), an ultra-rare blood disorder.97 From there, Alexion expanded Soliris’s label to include other rare conditions:
- Atypical Hemolytic Uremic Syndrome (aHUS), a genetic disease that causes kidney failure.103
- Generalized Myasthenia Gravis (gMG), a rare autoimmune neuromuscular disorder.101
- Neuromyelitis Optica Spectrum Disorder (NMOSD), a rare autoimmune disease of the central nervous system.103
For each of these indications, Soliris received an orphan drug designation and a corresponding period of market exclusivity. By “stacking” these exclusivities, Alexion built a multi-billion dollar product line based on a single molecule, demonstrating how a deep understanding of disease biology combined with a savvy regulatory strategy can create immense and lasting value in the rare disease space.
Strategy 15: The Pediatric Exclusivity Extension – A Critical Six Months
One of the most valuable and commonly used regulatory LCM strategies is the pursuit of pediatric exclusivity. Under the Best Pharmaceuticals for Children Act (BPCA) in the United States, the FDA can issue a Written Request to a drug manufacturer to conduct specific studies of its drug in pediatric populations.107 If the company completes these studies to the FDA’s satisfaction and within the specified timeframe, it is granted an additional six months of market exclusivity.107
This six-month extension is incredibly powerful. It is not a patent extension, but a period of marketing exclusivity that “tacks on” to the end of all existing patent and regulatory exclusivities for that drug.107 Crucially, this extension applies not just to the pediatric formulation or indication that was studied, but to
all existing formulations, dosage forms, and indications of the drug that contain the same active moiety.107
For a blockbuster drug with annual sales in the billions of dollars, an extra six months of monopoly pricing can translate into a massive amount of revenue—often one of the highest ROI activities a company can undertake in the late stage of its product’s lifecycle. As of March 2025, the FDA had granted a total of 335 pediatric exclusivity determinations, covering 316 different drugs, underscoring how integral this strategy has become to the industry.108 It serves the dual purpose of generating critical data on the safe and effective use of medicines in children while providing a significant financial incentive for the sponsoring company.
Example: The Value of Six Months for Lyrica (pregabalin)
Pfizer’s successful use of this provision for its nerve pain drug, Lyrica, highlights its strategic importance.107 By completing the requested pediatric studies, Pfizer secured pediatric exclusivity, which extended its U.S. market protection for Lyrica through June 30, 2019. This provided the company with an additional six months of blockbuster sales, a significant financial bridge that helped to offset the impending revenue cliff and provided more time for its newer products to grow. This strategy is a standard part of the late-stage LCM playbook for nearly every major drug launched in the United States.
Part III: Synthesizing the Strategy – Building a Holistic LCM Framework
Having explored 15 distinct strategies, it is crucial to recognize that the most successful lifecycle management programs do not treat these as an à la carte menu of isolated tactics. Instead, they weave them into a single, integrated framework where developmental, commercial, and legal strategies are planned and executed in concert, often from the earliest stages of a product’s development.
From Tactics to Transformation: An Integrated Approach
The true power of LCM lies in the compounding, multiplicative effect of layering multiple strategies over time. A single tactic might extend a product’s life by a few years; a well-orchestrated sequence of tactics can transform its entire value trajectory. This requires a mindset that views LCM not as a series of defensive maneuvers, but as a continuous, dynamic process of value creation and protection.5
Consider a hypothetical blockbuster drug five years away from its primary patent expiration. A siloed, reactive approach might wait until year three to start thinking about a defense. An integrated, proactive approach, however, sees the entire landscape as a chessboard.
- Early- to Mid-Lifecycle (Years 1-10 post-launch): The work begins now. The company initiates clinical trials for Strategy 1: Indication Expansion, targeting a new patient population. Simultaneously, the formulation science team begins work on Strategy 2: A Next-Generation Formulation, such as a once-weekly version to improve convenience. The legal team, in parallel, begins constructing the early stages of Strategy 13: A Patent Thicket, filing patents on every aspect of the new formulation and manufacturing process.
- Late-Lifecycle (5 years to LOE): The new indication is approved, bringing in a new revenue stream and potentially triggering Strategy 14: Orphan Drug Designation with its seven years of exclusivity for that use. The company submits the required studies for Strategy 15: Pediatric Exclusivity, securing an additional six months of protection across the entire franchise. The next-generation formulation is approved and launched, and a major marketing effort begins to switch patients from the original product to the new, patent-protected one (Strategy 6: The “Encore” Product).
- Post-LOE: As the patents on the original formulation finally expire, the company is ready. It immediately launches Strategy 12: An Authorized Generic to capture a share of the generic market. Simultaneously, it deploys Strategy 10: Aggressive Rebates and Co-pay Cards to defend the remaining market share of the branded original product, for which it has built years of physician and patient loyalty.
The result of this integrated campaign is not a single extension of value, but a complex, overlapping web of clinical, commercial, and legal protections that extends the franchise’s profitability far beyond the original patent cliff date. This demonstrates that world-class LCM is a cross-functional discipline that requires seamless integration of R&D, commercial, legal, and regulatory strategies from the very beginning of a product’s journey.5
The Central Role of Patent Intelligence
Data is the lifeblood of this integrated approach. To make strategic decisions about which LCM strategies to pursue and when, teams must have an unflinchingly honest and deeply detailed map of the present and a predictive model of the future. This requires a continuous, 360-degree analysis of the market landscape, which forms the bedrock of every subsequent decision.5
This analysis has two core components: understanding the voice of the customer and understanding the competitive landscape.
- Voice of the Customer: This involves deep research into patient and physician needs that go beyond the primary clinical endpoints of the original trials. Are there real-world friction points? Is the dosing schedule inconvenient? Are there persistent, low-grade side effects that impact quality of life? Is the administration method difficult for certain patient populations?5 Answering these questions reveals opportunities for value-creating reformulations or new patient support programs.
- Competitive Intelligence: This requires a granular scrutiny of competitors’ entire strategic posture—mapping their portfolios, dissecting their pricing strategies, and, most critically, monitoring their R&D pipelines and patent filings for future threats.5
This is where sophisticated patent intelligence platforms become indispensable. Tools like DrugPatentWatch allow LCM teams to move from a reactive to a proactive stance. By systematically monitoring patent expirations, new filings, and litigation across the industry, teams can anticipate competitive moves, identify “white space” opportunities for their own R&D, and conduct the critical Freedom-to-Operate (FTO) analysis needed before investing hundreds of millions in a new formulation or indication.1
The convergence of these data streams is remarkably powerful. Imagine market research reveals that patients find a daily oral tablet burdensome. Simultaneously, the competitive intelligence team, using a platform like DrugPatentWatch, flags a new patent filing from a key competitor for an extended-release, once-weekly formulation of a similar compound. The threat is no longer hypothetical; it is a clear and present danger that demands an immediate strategic response.5 This ability to connect the dots between patient needs, competitive actions, and the IP landscape is the hallmark of a modern, data-driven LCM framework.
Conclusion: Thriving in the Post-Exclusivity Era
The patent cliff is one of the most formidable and unforgiving features of the pharmaceutical landscape. The loss of exclusivity on a blockbuster drug represents a moment of profound vulnerability, threatening to erase billions of dollars in revenue and destabilize even the largest of companies. Yet, as this report has demonstrated through 15 distinct strategies and numerous real-world examples, the cliff is not an inevitable endpoint. It is a predictable, manageable business challenge that can be navigated, mitigated, and in some cases, transformed into an opportunity for strategic renewal.
Thriving in the post-exclusivity era is the art of the second act. It is an art grounded in the science of proactive, data-driven, and deeply integrated Pharmaceutical Lifecycle Management. It requires a fundamental shift in mindset: from viewing a product’s life as a finite sprint to the patent expiry finish line, to seeing it as a long-distance marathon of continuous innovation and value creation.
The companies that succeed will be those that start planning early, viewing LCM not as a late-stage defense but as a core component of strategy from the moment a drug enters Phase 3. They will be the ones who listen intently to the voice of the patient, using insights about unmet needs to drive meaningful improvements in formulations and delivery systems. They will be the ones who relentlessly explore the full potential of their molecules through indication expansion and combination therapies. They will master the complex interplay of commercial and legal tactics, from aggressive pricing strategies to the construction of formidable patent fortresses. And they will underpin every decision with a rigorous, 360-degree analysis of the market, leveraging powerful patent intelligence tools like DrugPatentWatch to anticipate threats and seize opportunities before their competitors.
The pressures on the industry are only intensifying. The window for a new drug to achieve peak sales is shrinking, a phenomenon known as life cycle compression.5 New policy pressures, such as the U.S. Inflation Reduction Act, are further complicating the pricing and reimbursement landscape.5 In this environment, the discipline of lifecycle management is no longer just a source of competitive advantage; it is a prerequisite for survival and sustained success. The playbook has been written. The challenge lies in its execution.
Key Takeaways
- The Scale of the Threat is Unprecedented: The pharmaceutical industry faces a patent cliff that puts an estimated $300-$400 billion in annual revenue at risk through 2030, a scale that dwarfs previous waves of patent expirations.
- LCM is a Proactive, Not Reactive, Discipline: Effective Lifecycle Management begins early in a drug’s development, not in the final years before patent expiry. It requires the seamless integration of R&D, commercial, legal, and regulatory strategies.
- The Landscape is Evolving with Biologics: The current patent cliff is dominated by complex biologic drugs. Competition from biosimilars leads to a more gradual “patent slope” rather than a sharp “cliff,” shifting the strategic focus to a prolonged, post-LOE commercial battle based on brand trust and value-added services.
- Developmental Strategies Create Durable Value: The most powerful LCM strategies are those that enhance the core product itself. Indication expansion, next-generation formulations, combination therapies, and second-generation products can create genuine clinical benefits and new, patent-protected revenue streams.
- Commercial Strategies Reshape the Market: Aggressive commercial tactics like Rx-to-OTC switches, geographical expansion into emerging markets, and sophisticated post-expiry pricing and rebate strategies are essential for defending market share and unlocking new avenues for growth.
- Legal and Regulatory Mastery is Non-Negotiable: A deep understanding of the IP and regulatory landscape is critical. Strategies like building patent thickets, launching authorized generics, and leveraging orphan drug and pediatric exclusivities can add billions of dollars to a product’s lifetime value.
- Success Lies in Layering Strategies: The most effective LCM programs do not rely on a single tactic but layer multiple strategies over time to create a compounding, multiplicative effect that extends a franchise’s value far beyond its original patent life.
- Patent Intelligence is the Foundation: All effective LCM is built on a foundation of data. Continuous, 360-degree market and competitive analysis, powered by tools like DrugPatentWatch, is essential for making informed, proactive strategic decisions.
Frequently Asked Questions (FAQ)
1. What is the single most impactful LCM strategy a company can pursue?
There is no single “most impactful” strategy, as the optimal choice depends heavily on the specific drug, its therapeutic area, the competitive landscape, and the company’s risk tolerance. However, for a blockbuster small-molecule drug, securing the six-month Pediatric Exclusivity extension is often the highest ROI activity in the late lifecycle, potentially adding billions in revenue for a relatively modest investment in clinical trials. For a biologic with a broad mechanism of action, a well-executed Indication Expansion strategy, as exemplified by Keytruda, has the potential to transform a single product into a multi-billion dollar franchise that dominates an entire therapeutic area.
2. How early should a company start planning its LCM strategy?
Ideally, foundational LCM planning should begin during Phase 2 or early Phase 3 of clinical development. This is the point at which a company has a clearer picture of the drug’s clinical profile, potential market, and competitive positioning. Early planning allows for the strategic design of Phase 3 trials to potentially support future indication expansions. It provides ample time to begin the complex R&D work for new formulations or combination therapies, ensuring they are ready for launch before the original patent expires. Waiting until a product is on the market, or worse, until a few years before patent expiry, severely limits the available strategic options and is a common cause of value destruction.
3. Isn’t “evergreening” through patent thickets just an anti-competitive abuse of the patent system?
This is one of the most contentious issues in pharmaceutical law and policy. Critics argue that patent thickets often involve patenting trivial or non-inventive modifications with the sole purpose of creating legal barriers to deter generic and biosimilar competition, thereby harming public health by keeping drug prices high. This view has led to increased antitrust scrutiny and litigation. Proponents, typically innovator companies, argue that these secondary patents protect genuine, incremental innovations that improve a product’s safety, efficacy, or convenience, and that they are entitled to protect this ongoing R&D investment. The legal reality is complex and varies by jurisdiction. While strategies like AbbVie’s for Humira have been highly effective commercially, they also carry a significant and growing risk of legal challenges and reputational damage.
4. How does the U.S. Inflation Reduction Act (IRA) impact LCM strategy?
The IRA introduces a new and powerful dynamic into LCM planning. By allowing Medicare to negotiate prices on top-selling drugs after a certain period of market exclusivity (9 years for small molecules, 13 for biologics), the IRA effectively shortens the period of free-market pricing, regardless of patent life. This “negotiation cliff” may arrive years before the “patent cliff.” This reality forces companies to re-evaluate the ROI of long-tail LCM strategies. For example, a strategy that extends a patent by a few years might be less valuable if those years fall within the post-negotiation period where prices are already significantly reduced. It places an even greater premium on strategies that can maximize revenue in the first 9-13 years and on developing truly innovative follow-on products rather than just incremental improvements.
5. With the rise of AI, how will pharmaceutical LCM evolve in the next decade?
Artificial intelligence is poised to revolutionize LCM in several key ways. In developmental LCM, AI can accelerate the identification of new indications by analyzing vast datasets of genomic, proteomic, and clinical data to find novel drug-disease connections. It can also be used to design and optimize new formulations and drug delivery systems in silico, reducing trial-and-error lab work. In commercial LCM, AI will enable hyper-personalized marketing and patient support programs, using real-world data to predict patient adherence issues and deliver targeted interventions. For legal and regulatory strategies, AI can enhance patent intelligence by analyzing global patent landscapes to identify threats and opportunities with greater speed and accuracy. Overall, AI will make LCM more predictive, precise, and data-driven, allowing companies to make smarter, faster decisions across a product’s entire lifecycle.
Works cited
- Maximizing ROI on Drug Development by Monitoring Competitive …, accessed August 18, 2025, https://www.drugpatentwatch.com/blog/maximizing-roi-on-drug-development-by-monitoring-competitive-patent-portfolios/
- Measuring the return from pharmaceutical innovation 2025 | Deloitte Switzerland, accessed August 18, 2025, https://www.deloitte.com/ch/en/Industries/life-sciences-health-care/research/measuring-return-from-pharmaceutical-innovation.html
- Measuring the return from pharmaceutical innovation 2024 | Deloitte US, accessed August 18, 2025, https://www.deloitte.com/us/en/Industries/life-sciences-health-care/articles/measuring-return-from-pharmaceutical-innovation.html
- The Multi-Billion Dollar Countdown: Decoding the Patent Cliff and Seizing the Generic Opportunity – DrugPatentWatch, accessed August 18, 2025, https://www.drugpatentwatch.com/blog/patent-expirations-seizing-opportunities-in-the-generic-drug-market/
- The Art of the Second Act: A Six-Step Framework for Mastering Late-Stage Drug Lifecycle Management – DrugPatentWatch, accessed August 18, 2025, https://www.drugpatentwatch.com/blog/6-steps-to-effective-late-stage-lifecycle-drug-management/
- Lifecycle Management – Zamann Pharma Support GmbH, accessed August 18, 2025, https://zamann-pharma.com/glossary/lifecycle-management/
- www.drugpatentwatch.com, accessed August 18, 2025, https://www.drugpatentwatch.com/blog/how-pharmaceutical-life-cycle-management-strategies-are-evolving/#:~:text=Life%20Cycle%20Management%20in%20pharmaceuticals,value%20throughout%20its%20commercial%20lifetime.
- How Pharmaceutical Life Cycle Management Strategies Are Evolving – DrugPatentWatch, accessed August 18, 2025, https://www.drugpatentwatch.com/blog/how-pharmaceutical-life-cycle-management-strategies-are-evolving/
- The End of Exclusivity: Navigating the Drug Patent Cliff for …, accessed August 18, 2025, https://www.drugpatentwatch.com/blog/the-impact-of-drug-patent-expiration-financial-implications-lifecycle-strategies-and-market-transformations/
- www.investopedia.com, accessed August 18, 2025, https://www.investopedia.com/terms/p/patent-cliff.asp#:~:text=Patent%20cliff%20refers%20to%20a,may%20begin%20grabbing%20market%20share.
- Patent Cliff: What It Means, How It Works – Investopedia, accessed August 18, 2025, https://www.investopedia.com/terms/p/patent-cliff.asp
- Understanding Patent Expiries and Their Impact on Drug Prices – East Street Pharmacy, accessed August 18, 2025, https://eaststreetpharmacy.com/understanding-patent-expiries-and-their-impact-on-drug-prices.html
- The Patent Cliff: From Threat to Competitive Advantage – Esko, accessed August 18, 2025, https://www.esko.com/en/blog/patent-cliff-from-threat-to-competitive-advantage
- The Impact of Patent Expirations on the Pharmaceutical Industry – JOCPR, accessed August 18, 2025, https://www.jocpr.com/articles/the-impact-of-patent-expirations-on-the-pharmaceutical-industry-10233.html
- Pharmaceutical Lifecycle Management Strategies in 2017: Comprehensive Assessment of Strategies Being Implemented by Pharmaceutical Companies Around the World – Research and Markets – PR Newswire, accessed August 18, 2025, https://www.prnewswire.com/news-releases/pharmaceutical-lifecycle-management-strategies-in-2017-comprehensive-assessment-of-strategies-being-implemented-by-pharmaceutical-companies-around-the-world—research-and-markets-300452376.html
- What is a patent cliff, and how does it impact companies? – Patsnap Synapse, accessed August 18, 2025, https://synapse.patsnap.com/article/what-is-a-patent-cliff-and-how-does-it-impact-companies
- The $400 Billion Patent Cliff: Big Pharma’s Revenue Crisis, accessed August 18, 2025, https://americanbazaaronline.com/2025/08/04/the-400-billion-patent-cliff-big-pharmas-revenue-crisis-465788/
- How Pfizer, Bristol Myers Squibb and Johnson & Johnson Are Confronting Patent Cliffs, accessed August 18, 2025, https://www.biospace.com/how-pfizer-bristol-myers-squibb-and-johnson-and-johnson-are-confronting-patent-cliffs
- The Impact of Patent Cliff on the Pharmaceutical Industry – Bailey Walsh, accessed August 18, 2025, https://bailey-walsh.com/news/patent-cliff-impact-on-pharmaceutical-industry/
- Navigating the oncology patent cliff: Strategic imperatives for big pharma | BioPharma Dive, accessed August 18, 2025, https://www.biopharmadive.com/spons/navigating-the-oncology-patent-cliff-strategic-imperatives-for-big-pharma/756120/
- Innovative Formulation Strategies for Biosimilars: Trends Focused on Buffer-Free Systems, Safety, Regulatory Alignment, and Intellectual Property Challenges – PMC – PubMed Central, accessed August 18, 2025, https://pmc.ncbi.nlm.nih.gov/articles/PMC12196224/
- Pharmaceutical Product Lifecycle Management | ISPE, accessed August 18, 2025, https://ispe.org/topics/lifecycle-management
- Life Cycle Management Strategies More Crucial than Ever for …, accessed August 18, 2025, https://drug-dev.com/life-cycle-management-strategies-more-crucial-than-ever-for-pharmaceutical-success/
- Drug Indication Expansion: Revolutionizing the Pharma Landscape – Delta4 | AI, accessed August 18, 2025, https://delta4.ai/drug-indication-expansion/
- Knowledge Graphs for Indication Expansion: An Explainable Target-Disease Prediction Method – PMC – PubMed Central, accessed August 18, 2025, https://pmc.ncbi.nlm.nih.gov/articles/PMC8963915/
- Pharma: Expansion Strategy (Case Study) | PwC Switzerland, accessed August 18, 2025, https://www.pwc.ch/en/insights/transformation/pharma-expansion-strategy.html
- Success Multiplied: Launch Excellence for Multi-Indication … – IQVIA, accessed August 18, 2025, https://www.iqvia.com/-/media/iqvia/pdfs/library/white-papers/iqvia-launch-excellence-for-multi-indication-assets-02-23-forweb.pdf
- Stretching Product Value through Reformulation Strategies, accessed August 18, 2025, https://www.pharmtech.com/view/stretching-product-value-through-reformulation-strategies-0
- Ultimate Guide to Pharmaceutical Product Life Cycle Management …, accessed August 18, 2025, https://www.tikamobile.com/resources/blog/ultimate-guide-to-pharmaceutical-product-life-cycle-management
- Benefits of reformulation strategies – Recipharm, accessed August 18, 2025, https://www.recipharm.com/resources/benefits-reformulation-strategies
- Overcoming Formulation Challenges in Generic Drug Development …, accessed August 18, 2025, https://www.drugpatentwatch.com/blog/overcoming-formulation-challenges-in-generic-drug-development-a-case-study/
- Factors to Consider in Designing the Drug Dosage Regimen – Longdom Publishing, accessed August 18, 2025, https://www.longdom.org/open-access/factors-to-consider-in-designing-the-drug-dosage-regimen-102275.html
- Reach Steady State in Pharmacokinetics – BioPharma Services, accessed August 18, 2025, https://www.biopharmaservices.com/blog/phase-1-exploring-the-importance-and-ways-to-achieve-steady-state-in-pharmacokinetics/
- Understanding Repeat Dosing & Steady-State Concentration – Allucent, accessed August 18, 2025, https://www.allucent.com/resources/blog/pharmacokinetic-considerations-repeat-dosing
- Finding better ways to reduce serious drug side effects – UCSF School of Pharmacy, accessed August 18, 2025, https://pharmacy.ucsf.edu/news/2017/08/finding-better-ways-reduce-serious-drug-side-effects
- Top Pharma Product Life Cycle Management Strategies – Within3, accessed August 18, 2025, https://within3.com/blog/life-cycle-management-pharma
- Reformulation-Focused Life Cycle Management of the FDA-Approved Drugs, accessed August 18, 2025, https://www.iomcworld.org/articles/reformulationfocused-life-cycle-management-of-the-fdaapproved-drugs.pdf
- Reformulation-Focused Life Cycle Management of the FDA …, accessed August 18, 2025, https://www.iomcworld.org/articles/reformulationfocused-life-cycle-management-of-the-fdaapproved-drugs-53091.html
- Combine and conquer: challenges for targeted therapy combinations in early phase trials – PMC, accessed August 18, 2025, https://pmc.ncbi.nlm.nih.gov/articles/PMC6135233/
- The regulatory challenges of innovative customized combination products – PMC, accessed August 18, 2025, https://pmc.ncbi.nlm.nih.gov/articles/PMC9354569/
- Factors Affecting Combination Trial Success (FACTS … – Frontiers, accessed August 18, 2025, https://www.frontiersin.org/journals/medicine/articles/10.3389/fmed.2019.00122/full
- Fluticasone and salmeterol (inhalation route) – Side effects & dosage – Mayo Clinic, accessed August 18, 2025, https://www.mayoclinic.org/drugs-supplements/fluticasone-and-salmeterol-inhalation-route/description/drg-20063110
- The role of fluticasone propionate/salmeterol combination therapy in …, accessed August 18, 2025, https://pmc.ncbi.nlm.nih.gov/articles/PMC2898089/
- Combination therapy with the single inhaler salmeterol/fluticasone propionate versus increased doses of inhaled corticosteroids in patients with asthma – NCBI, accessed August 18, 2025, https://www.ncbi.nlm.nih.gov/books/NBK74327/
- What are the market competitors for Januvia? – Patsnap Synapse, accessed August 18, 2025, https://synapse.patsnap.com/article/what-are-the-market-competitors-for-januvia
- Sitagliptin/Metformin (Janumet) as Combination Therapy In the Treatment of Type-2 Diabetes Mellitus – PMC, accessed August 18, 2025, https://pmc.ncbi.nlm.nih.gov/articles/PMC3541863/
- Fallout From Failed Phase 3 Trial: Adjuvant Therapy “Not the Most …, accessed August 18, 2025, https://www.oncologynewscentral.com/melanoma/fallout-from-failed-phase-3-trial-adjuvant-therapy-not-the-most-appropriate-option-for-all-stage-iii-melanomas
- Battling Maturity in the Pharma Product Life Cycle – VCL Solutions, accessed August 18, 2025, https://vcl.solutions/battling-maturity-in-the-pharma-product-life-cycle/
- The Treatment of Pharmaceutical Life Cycle Management Strategies In the European Commission’s Pharmaceutical Sector Inquiry F – Sidley Austin LLP, accessed August 18, 2025, https://www.sidley.com/~/media/files/publications/2009/08/the-treatment-of-pharmaceutical-life-cycle-manag__/files/view-article/fileattachment/the-treatment-of-pharmaceutical-l.pdf
- Managing the challenges of pharmaceutical patent expiry: a case study of Lipitor, accessed August 18, 2025, https://www.researchgate.net/publication/309540780_Managing_the_challenges_of_pharmaceutical_patent_expiry_a_case_study_of_Lipitor
- Loratadine – LiverTox – NCBI Bookshelf, accessed August 18, 2025, https://www.ncbi.nlm.nih.gov/books/NBK548831/
- Desloratadine for Allergic Rhinitis | AAFP, accessed August 18, 2025, https://www.aafp.org/pubs/afp/issues/2003/1115/p2015.html
- Cetirizine – LiverTox – NCBI Bookshelf, accessed August 18, 2025, https://www.ncbi.nlm.nih.gov/books/NBK548420/
- Xyzal vs. Zyrtec: How Do They Compare for Allergies?, accessed August 18, 2025, https://www.verywellhealth.com/xyzal-vs-zyrtec-8784438
- Xyzal vs. Zyrtec and Other Common Allergy Medications: How Do They Compare? – GoodRx, accessed August 18, 2025, https://www.goodrx.com/levocetirizine/allergy-medicine-alternatives-everything-you-need-to-know-about-xyzal
- Rx-to-OTC switches: trends and factors underlying success – PubMed, accessed August 18, 2025, https://pubmed.ncbi.nlm.nih.gov/16604099/
- Rx-to-OTC Switches: Growth, Drivers & The Role of Patients – Lubrizol, accessed August 18, 2025, https://www.lubrizol.com/health/blog/2020/11/rx-to-otc-switches
- How to Select Drugs to Switch from Rx to OTC – Premier Research, accessed August 18, 2025, https://premier-research.com/perspectives/how-to-select-drugs-to-switch-from-rx-to-otc/
- Pharmaceutical Switching | Stanford Graduate School of Business, accessed August 18, 2025, https://www.gsb.stanford.edu/faculty-research/case-studies/pharmaceutical-switching
- The RX-TO-OTC Switch of Claritin, Allegra, and Zyrtec: An Unprecedented FDA Response to Petitioner – Digital Commons @ American University Washington College of, accessed August 18, 2025, https://digitalcommons.wcl.american.edu/cgi/viewcontent.cgi?referer=&httpsredir=1&article=1146&context=aulr
- 19-658S018 Claritin Medical Review Part 1 – accessdata.fda.gov, accessed August 18, 2025, https://www.accessdata.fda.gov/drugsatfda_docs/nda/2002/19-658S018_Claritin_Medr_P1.pdf
- When Rx-to-OTC Switch Medications Become Generic – U.S. Pharmacist, accessed August 18, 2025, https://www.uspharmacist.com/article/when-rx-to-otc-switch-medications-become-generic
- Recent Rx-to-OTC Product Switches – U.S. Pharmacist, accessed August 18, 2025, https://www.uspharmacist.com/article/recent-rx-to-otc-product-switches
- Rx-to-OTC Switches: How it Works and Popular Examples – GoodRx, accessed August 18, 2025, https://www.goodrx.com/drugs/otc/switch-from-rx
- 022283Orig1s000 – accessdata.fda.gov, accessed August 18, 2025, https://www.accessdata.fda.gov/drugsatfda_docs/nda/2013/022283Orig1s000MedR.pdf
- Summary Review – accessdata.fda.gov, accessed August 18, 2025, https://www.accessdata.fda.gov/drugsatfda_docs/nda/2009/022281s000_SumR.pdf
- The Influence of Emerging Markets on the Pharmaceutical Industry …, accessed August 18, 2025, https://www.drugpatentwatch.com/blog/the-influence-of-emerging-markets-on-the-pharmaceutical-industry/
- Global Market Expansion Strategies for Biopharma Companies | BioBoston Consulting, accessed August 18, 2025, https://biobostonconsulting.com/global-market-expansion-strategies-for-biopharma-companies-bioboston-consulting/
- Big Pharma Strategies for Emerging Markets Pharmaceuticals – Infiniti Research, accessed August 18, 2025, https://www.infinitiresearch.com/thoughts/winning-emerging-markets-big-pharma-companies-must/
- International Strategy for Sustainable Growth in Multinational Pharmaceutical Companies, accessed August 18, 2025, https://www.mdpi.com/2071-1050/12/3/867
- Case Studies – Business Talent Group, accessed August 18, 2025, https://resources.businesstalentgroup.com/btg-case-studies
- Unleashing the Innovation Power of Alliances – Boston Consulting Group, accessed August 18, 2025, https://www.bcg.com/publications/2022/innovation-power-of-alliances
- Case Studies Of Successful Joint Ventures And Affiliated Companies – FasterCapital, accessed August 18, 2025, https://fastercapital.com/topics/case-studies-of-successful-joint-ventures-and-affiliated-companies.html/1
- Pharmaceutical-case-study-2.pdf – Capgemini, accessed August 18, 2025, https://www.capgemini.com/wp-content/uploads/2021/03/Pharmaceutical-case-study-2.pdf
- Joint Venture Workflow Integration: Case Study Insights – Phoenix Strategy Group, accessed August 18, 2025, https://www.phoenixstrategy.group/blog/joint-venture-workflow-integration-case-study-insights
- Bristol Myers Squibb and Pfizer Announce Direct-to-Patient Eliquis® (apixaban) Option, accessed August 18, 2025, https://news.bms.com/news/details/2025/Bristol-Myers-Squibb-and-Pfizer-Announce-Direct-to-Patient-Eliquis-apixaban-Option/default.aspx
- BRISTOL-MYERS SQUIBB COMPANY, accessed August 18, 2025, https://www.bms.com/assets/bms-ar/documents/2017/Bristol-Myers-Squibb-2017-10-K-FINAL.pdf
- How Bristol-Myers and Pfizer are using real-world data to unseat …, accessed August 18, 2025, https://www.biopharmadive.com/news/bristol-myers-eliquis-noac-real-world-data-unseat-warfarin/515516/
- Bristol-Myers Squibb and Pfizer Present Observational Real-World Data Analysis on the Effectiveness and Safety of Eliquis® (apixaban) Compared to Warfarin in Select High-Risk Patients with Non-Valvular Atrial Fibrillation, accessed August 18, 2025, https://www.pfizer.com/news/press-release/press-release-detail/bristol_myers_squibb_and_pfizer_present_observational_real_world_data_analysis_on_the_effectiveness_and_safety_of_eliquis_apixaban_compared_to_warfarin_in_select_high_risk_patients_with_non_valvular_atrial
- Bristol-Myers Squibb and Pfizer Present Large Real-World Observational Analysis of the Effectiveness and Safety of Direct Oral Anticoagulants Compared to Warfarin in Patients with Non-Valvular Atrial Fibrillation, accessed August 18, 2025, https://www.pfizer.com/news/press-release/press-release-detail/bristol_myers_squibb_and_pfizer_present_large_real_world_observational_analysis_of_the_effectiveness_and_safety_of_direct_oral_anticoagulants_compared_to_warfarin_in_patients_with_non_valvular_atrial_fibrillation
- How to own a Market you Don’t Own: Market Access Strategies Post-Patent Expiration, accessed August 18, 2025, https://www.drugpatentwatch.com/blog/how-to-own-a-market-you-dont-own-market-access-strategies-post-patent-expiration/
- The Impact of Patent Expiry on Drug Prices: A Systematic Literature Review – PMC, accessed August 18, 2025, https://pmc.ncbi.nlm.nih.gov/articles/PMC6132437/
- Navigating pharma loss of exclusivity | EY – US, accessed August 18, 2025, https://www.ey.com/en_us/insights/life-sciences/navigating-pharma-loss-of-exclusivity
- Is Pfizer’s Lipitor Strategy Working? – Drug Channels, accessed August 18, 2025, https://www.drugchannels.net/2012/01/is-pfizers-lipitor-strategy-working.html
- Digital Health Technologies (DHTs) for Drug Development – FDA, accessed August 18, 2025, https://www.fda.gov/science-research/science-and-research-special-topics/digital-health-technologies-dhts-drug-development
- INTEGRATING DIGITAL HEALTH SYSTEMS INTO MEDICAL DEVICE ECOSYSTEMS: CONSIDERATIONS & STRATEGIES – ONdrugDelivery, accessed August 18, 2025, https://ondrugdelivery.com/integrating-digital-health-systems-into-medical-device-ecosystems-considerations-and-strategies/
- Digital Health Integration Assessment and Maturity of the United States Biopharmaceutical Industry: Forces Driving the Next Generation of Connected Autoinjectable Devices, accessed August 18, 2025, https://pmc.ncbi.nlm.nih.gov/articles/PMC8088878/
- Asthma and COPD Digital Inhaler Data Into EHR | CommonSpirit Health, accessed August 18, 2025, https://www.commonspirit.org/news-articles/asthma-and-copd-digital-inhaler-data-into-ehr
- Propeller Health Case Study – AWS – Amazon.com, accessed August 18, 2025, https://aws.amazon.com/solutions/case-studies/propeller-health-case-study/
- FDA clears Propeller Health sensor to work with Symbocort inhaler, accessed August 18, 2025, https://www.gsmedtech.com/GS/NewsDetails/FDA-clears-Propeller-Health-sensor-to-work-with-Symbocort-inhaler
- Propeller Health Receives FDA Clearance to Connect Patients Using the Symbicort® Inhaler to its Digital Health Platform – McKesson Ventures, accessed August 18, 2025, https://ventures.mckesson.com/propeller-health-fda-clearance-symbicort-inhaler/
- In the Thick(et) of It: Addressing Biologic Patent Thickets Using the Sham Exception to Noerr-Pennington, accessed August 18, 2025, https://ir.lawnet.fordham.edu/iplj/vol33/iss3/5/
- Patent Evergreening In The Pharmaceutical Industry: Legal …, accessed August 18, 2025, https://ijlsss.com/patent-evergreening-in-the-pharmaceutical-industry-legal-loophole-or-strategic-innovation/
- Biological patent thickets and delayed access to biosimilars, an …, accessed August 18, 2025, https://academic.oup.com/jlb/article/9/2/lsac022/6680093
- Patent Settlements Are Necessary To Help Combat Patent Thickets, accessed August 18, 2025, https://accessiblemeds.org/resources/blog/patent-settlements-are-necessary-to-help-combat-patent-thickets/
- Orphan drugs: a lasting success story – CEPTON Strategies, accessed August 18, 2025, https://ceptonstrategies.com/en/orphan-drugs-a-lasting-success-story-2/
- Dynamics of patents, orphan drug designation, licensing, and revenues from drugs for rare diseases: The market expansion of eculizumab – PMC – PubMed Central, accessed August 18, 2025, https://pmc.ncbi.nlm.nih.gov/articles/PMC7935269/
- Designating an Orphan Product: Drugs and Biological Products – FDA, accessed August 18, 2025, https://www.fda.gov/industry/medical-products-rare-diseases-and-conditions/designating-orphan-product-drugs-and-biological-products
- Orphan Drug Label Expansions: Analysis Of Subsequent Rare And Common Indication Approvals | Health Affairs, accessed August 18, 2025, https://www.healthaffairs.org/doi/10.1377/hlthaff.2023.00219
- From Orphan to Opportunity: Mastering Rare Disease Launch Excellence – IQVIA, accessed August 18, 2025, https://www.iqvia.com/-/media/iqvia/pdfs/library/white-papers/from-orphan-to-opportunity-mastering-rare-disease-launch-excellence.pdf
- EU/3/14/1304 – orphan designation for treatment myasthenia gravis …, accessed August 18, 2025, https://www.ema.europa.eu/en/medicines/human/orphan-designations/eu-3-14-1304
- Pharmacology, Pharmacokinetics and Pharmacodynamics of Eculizumab, and Possibilities for an Individualized Approach to Eculizumab – PMC – PubMed Central, accessed August 18, 2025, https://pmc.ncbi.nlm.nih.gov/articles/PMC6584251/
- SOLIRIS – Orphanet, accessed August 18, 2025, https://www.orpha.net/en/drug/trade_name/82335?name=
- Access and Reimbursement Guide, accessed August 18, 2025, https://alexionaccessnavigator.com/-/media/alexionaccessnavigator/soliris/files/soliris-access-and-reimbursement-guide.pdf
- Search Orphan Drug Designations and Approvals – FDA, accessed August 18, 2025, https://www.accessdata.fda.gov/scripts/opdlisting/oopd/detailedIndex.cfm?cfgridkey=434214
- Search Orphan Drug Designations and Approvals – FDA, accessed August 18, 2025, https://www.accessdata.fda.gov/scripts/opdlisting/oopd/detailedIndex.cfm?cfgridkey=398713
- Benefits of FDA Pediatric Exclusivity – Pharmaceutical Law Group, accessed August 18, 2025, https://www.pharmalawgrp.com/blog/4/benefits-of-fda-pediatric-exclusivity/
- Pediatric Exclusivity Granted – FDA, accessed August 18, 2025, https://www.fda.gov/drugs/development-resources/pediatric-exclusivity-granted
- DrugPatentWatch Highlights 5 Strategies for Generic Drug …, accessed August 18, 2025, https://www.geneonline.com/drugpatentwatch-highlights-5-strategies-for-generic-drug-manufacturers-to-succeed-post-patent-expiration/