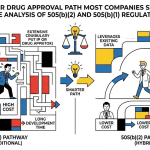
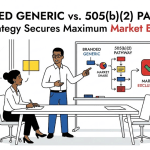
Generic drug development past the ANDA filing date is where most companies either build durable competitive moats or bleed out on legal fees and price erosion. This guide is for IP teams, portfolio managers, R&D leads, and institutional investors who need to move beyond surface-level Hatch-Waxman literacy and into the tactical specifics: which patent challenges win, which formulation strategies create protectable IP, how 505(b)(2) exclusivity compounds returns, and how to build a patent intelligence function that actually predicts competitor moves before they happen.
The generic pharmaceutical market fills roughly 90% of all U.S. prescriptions but accounts for only 26% of total drug spending. That ratio is the whole problem. Volume without margin forces companies to either commoditize toward zero or move up the value chain toward differentiated, hard-to-copy products. Every strategy in this guide is oriented toward that second path.
I. The ANDA Pathway: What ‘Abbreviated’ Actually Means for Strategy
The Regulatory Architecture of an ANDA
The Abbreviated New Drug Application is the primary U.S. regulatory mechanism for generic drug approval, established under the Drug Price Competition and Patent Term Restoration Act of 1984 (the Hatch-Waxman Act). The FDA’s Center for Drug Evaluation and Research governs the process. ‘Abbreviated’ refers specifically to the waiver of duplicative clinical safety and efficacy trials, not to any reduction in technical rigor. The burden simply shifts from proving that a molecule is safe and effective to proving that the generic version performs identically to the Reference Listed Drug (RLD).
That proof requires demonstrating sameness across active ingredients, conditions of use, route of administration, dosage form, strength, labeling (with narrow permissible deviations), and bioequivalence. Bioequivalence studies are the scientific core of most ANDAs: they document comparable absorption, distribution, metabolism, and excretion through pharmacokinetic parameters, primarily Cmax and AUC, within the FDA’s accepted 80-125% confidence interval window.
Current Good Manufacturing Practices (cGMP) compliance sits alongside bioequivalence as a foundational requirement. An application can be scientifically flawless and still receive a Complete Response Letter if the manufacturing site fails inspection.
The ANDA Review Timeline: Where Competitive Advantage Is Made and Lost
The FDA review cycle for a standard ANDA runs 8 to 12 months for well-constructed, deficiency-free submissions. That timeline stretches considerably for applications that require multiple review cycles, with some complex generics accumulating review periods exceeding 30 months. Priority generic designations, which the FDA grants to generics addressing drug shortages or products with no current generic competition, carry expedited review tracks.
The practical implication: a company that files a complete, deficiency-free ANDA with robust bioequivalence data and clean manufacturing documentation gets to market 12 to 18 months ahead of a competitor whose application triggers a major amendment request. That gap, in the context of first-mover pricing dynamics, is worth tens of millions of dollars in incremental margin.
Pre-ANDA preparation is therefore not administrative overhead. It is a direct profit driver. Comprehensive analysis of the RLD, anticipatory review of FDA Product-Specific Guidances (PSGs), and early engagement with FDA on complex product submissions all compress the review cycle.
ANDA vs. 505(b)(2): Choosing the Right Pathway Before You Start Development
The choice between ANDA and 505(b)(2) is one of the highest-leverage decisions a pharmaceutical portfolio team makes, and it should happen at project initiation, not after bioequivalence data is already in hand.
An ANDA applies when the product is an identical version of the RLD, relying on the agency’s prior findings and supported by bioequivalence data. A 505(b)(2) New Drug Application is the hybrid route: the applicant relies, in whole or in part, on existing FDA findings of safety and efficacy for a previously approved active ingredient, or on published literature, but the product itself differs from the RLD in a legally and clinically meaningful way.
Differences that qualify for 505(b)(2) include new dosage forms, new routes of administration, new combinations of active ingredients, new indications, and new patient populations. These modifications can support periods of market exclusivity that no ANDA can provide: three years for new clinical investigations essential to approval, five years for new chemical entity exclusivity, and seven years for orphan drug designations.
The exclusivity question is the critical filter. If the modified product can earn three or more years of exclusivity through a 505(b)(2) route, the economics almost always favor that pathway over an ANDA, even accounting for the additional clinical work required. The ANDA route makes sense when the product is truly identical to the RLD, when the company is targeting first-filer 180-day exclusivity under a Paragraph IV certification, or when development timelines are the primary competitive constraint.
Key Takeaways: ANDA Pathway
- ‘Abbreviated’ means no duplicative clinical trials, not reduced technical scrutiny. Bioequivalence data and cGMP compliance carry the evidentiary burden.
- Review timelines range from 8 months (clean applications) to 30-plus months (deficiency-heavy submissions). That gap is a direct competitive variable.
- The ANDA vs. 505(b)(2) decision should be made at project initiation based on whether the product modification can support market exclusivity. This decision is irreversible once development begins.
- First-generic market entry confers advantages that persist years past the 180-day exclusivity window. Filing speed and application quality both drive this outcome.
II. Hatch-Waxman Patent Certifications: The Full Tactical Map
The Four Certifications and What Each One Signals
Every ANDA must include a patent certification for each patent listed in the FDA Orange Book against the RLD. The certification selected determines the competitive and legal posture of the filing.
A Paragraph I certification states that no patent has been filed for the RLD. A Paragraph II certification states that all listed patents have expired. Both allow immediate approval if other requirements are met, and neither triggers litigation.
A Paragraph III certification commits the filer to waiting for patent expiration before commercial launch, often the default choice for companies that want regulatory approval in advance of a known exclusivity cliff without the expense of patent litigation.
The Paragraph IV certification is where strategy diverges sharply from simple market access. The filer asserts that the listed patent is either invalid, unenforceable, or will not be infringed by the generic product. This triggers a 45-day window during which the patent holder can file an infringement suit in federal district court. If the holder files within that window, FDA approval is automatically stayed for up to 30 months, or until the litigation is resolved by court judgment, whichever comes first.
The Section viii statement, colloquially called the ‘skinny label,’ is a carve-out mechanism. The filer certifies that a method-of-use patent does not cover the indications for which the generic seeks approval. The ANDA labeling must omit the patented uses, creating a product approved only for non-patented indications. The legal risk embedded in this approach is real: a generic company that actively promotes a skinny-label product for the carved-out patented indication can face liability for induced infringement, even without directly marketing for that use. The GSK v. Teva litigation, decided by the Federal Circuit in 2021, made that exposure concrete.
The 180-Day Exclusivity Mechanic: IP Valuation Implications
The 180-day exclusivity period granted to the first ANDA filer with a Paragraph IV certification is the most valuable single asset a generic company can hold. During this window, the first filer faces no other generic competition. The economic literature on this period is consistent: generic companies capture 60 to 80% of total generic profits on a given drug during the first six months post-launch.
From an IP valuation standpoint, the 180-day exclusivity functions as a time-limited monopoly with quantifiable cash flow. Valuing it requires estimating the branded drug’s revenue at the time of generic entry, applying standard generic pricing discounts at entry (typically 20 to 30% off the brand price in the absence of other generics), and projecting how rapidly additional generics erode that price after the exclusivity period ends. On drugs with pre-patent-expiry revenues exceeding $500 million annually, the 180-day exclusivity alone can generate $75 to $200 million in incremental margin for the first filer.
The exclusivity triggers and forfeiture events are also critical to model. First-filer exclusivity is forfeited if the generic fails to achieve commercial marketing within 75 days of FDA approval (or a court judgment of non-infringement), or if a court determines that the patent claims are valid and infringed. Monitoring these trigger events is an active portfolio management function, not a legal technicality.
Investment Strategy: Hatch-Waxman Exclusivity Assets
Portfolio managers evaluating generic companies should treat the pipeline of Paragraph IV filings as a structured asset schedule. Each filing with first-filer status represents a time-limited revenue stream with a definable risk profile: litigation outcome probability, expected approval date, commercial readiness, and competitive response from the brand (authorized generics, authorized generic agreements, product hopping). Discounted cash flow models for these assets should incorporate at minimum a 30 to 40% probability-weighted haircut for litigation risk on mature molecule patents, with adjustment upward for clearly weak secondary patents and downward for well-defended composition-of-matter claims.
The 30-Month Stay: What Brand Companies Actually Do With It
The automatic 30-month stay is not simply a delay. For brand companies, it is a structured litigation window, and understanding how they use it informs generic strategy at every stage.
Brand companies routinely use the 30-month stay period to attempt at-risk launch pressure on the generic, to negotiate settlement terms including authorized generic agreements, and to pursue parallel IPR proceedings at the Patent Trial and Appeal Board against their own listed patents as defensive intelligence gathering. Some brands use the period to accelerate lifecycle management activities, reformulating the branded product and shifting prescriber and payer behavior toward the new formulation before the generic launches.
Generic companies that understand this behavioral pattern prepare for launch 12 to 18 months before the stay expires, not at expiration. Commercial launch readiness, including manufacturing scale-up, supply agreements, and managed care contracts, needs to be in place before the legal resolution, not dependent on it.
Reverse Payments and the Actavis Standard
Pay-for-delay settlements, in which the branded company pays the first-filing generic to delay market entry, were effectively subjected to antitrust scrutiny by the Supreme Court’s 2013 FTC v. Actavis ruling. The Court held that large reverse payments are subject to ‘rule of reason’ antitrust analysis, overturning the per se legality standard some circuits had previously applied.
In practice, Actavis moved the settlement dynamic toward non-cash consideration (authorized generic licenses, side agreements on other products, co-promotion arrangements) that are harder to quantify for antitrust regulators. The ten-plus years of post-Actavis litigation have produced a body of case law that sophisticated pharma counsel tracks closely. For portfolio managers, any generic company disclosing a large-value settlement with a brand company in a Paragraph IV context requires careful analysis of what the generic received and whether those terms could face FTC challenge.
Key Takeaways: Hatch-Waxman Certifications
- Paragraph IV filings with first-filer status are structured financial assets. Model them with explicit probability weighting for litigation outcomes.
- The 180-day exclusivity is worth 60 to 80% of total generic profits on that molecule. Its forfeiture conditions deserve as much legal attention as the patent challenge itself.
- The 30-month stay is a commercial and legal window, not merely a delay. Generic commercial readiness preparation should begin 12 to 18 months before stay expiration.
- Reverse payment settlements must be analyzed for Actavis exposure. Non-cash consideration does not eliminate antitrust risk.
III. Complex Generics: The High-Margin Product Strategy
What Makes a Generic ‘Complex’
The FDA classifies complex generics as products whose complexity derives from the active ingredient (peptides, polymeric molecules, complex mixtures), the formulation (liposomes, microspheres, emulsions), the route of administration (inhalation, transdermal, nasal, ophthalmic), the drug-device combination (auto-injectors, inhalers, transdermal patches), or the complexity of establishing bioequivalence. The key commercial feature of this category is competitive scarcity: fewer companies have the technical capability to develop these products, so even late entrants capture meaningful market share rather than fighting for commodity-level margins.
The FDA’s Drug Competition Action Plan (DCAP), active since 2017, specifically accelerates the regulatory pathway for complex generics. Under DCAP, the agency publishes Product-Specific Guidances at scale, conducts early meetings with manufacturers to discuss development challenges, and has established a dedicated team within CDER’s Office of Pharmaceutical Quality to resolve complex generic bioequivalence questions. Companies that engage with PSGs early and request Type B pre-ANDA meetings with FDA materially reduce development risk, because the ‘known unknowns’ about what FDA will accept as sufficient bioequivalence evidence get resolved before expensive pivotal studies are run.
IP Valuation of Complex Generic Assets
A complex generic in late-stage development, particularly one with no approved generic equivalent and a pending ANDA with acceptable bioequivalence data, is a fundamentally different asset class than a conventional generic filing. Several valuation factors differentiate it.
First, the barrier to entry is technical rather than purely legal. Even after ANDA approval, competitors face the same formulation and bioequivalence hurdles. That means the first complex generic entrant is likely to face one or two competitors over a five-year horizon rather than the five to ten entrants that hit most conventional generic markets within 24 months of first generic launch. The pricing durability is correspondingly better: complex generics often hold 40 to 60% of the brand price rather than the 20 to 30% typical of conventional generics.
Second, some complex generics require ancillary IP (proprietary manufacturing process patents, device patents for drug-device combinations) that extends protection beyond the primary composition-of-matter patent. This creates a layered IP structure analogous to what brand companies build through evergreening, except the generic company controls it.
Third, manufacturing complexity makes authorized generics harder for brands to execute. An innovator company can rapidly authorize a generic partner to launch under the NDA when a Paragraph IV challenge succeeds, effectively diluting the 180-day exclusivity. For complex generics, manufacturing a compliant authorized generic on short notice requires capabilities the brand may not have contracted for, giving the first-filing generic a longer window of effective exclusivity.
The FDA approved the first generic Vivitrol (naltrexone extended-release injectable suspension) in July 2023, four years after the first ANDA submission. That gap illustrates both the development difficulty and the reward: the single approved generic captures the full benefit of a market that had been a brand-only franchise for years.
Formulation Technology Roadmap for Complex Generics
Generic companies building complex generic pipelines should map their formulation capabilities against the following technology platforms, in order of regulatory approval precedent and development risk.
Extended-release oral solid dosage forms represent the most established complex generic category. Osmotic-pump systems (as in Concerta/methylphenidate ER), multilayer tablet technology, and reservoir-membrane coating systems all carry extensive bioequivalence precedent. The primary challenge is reverse-engineering the release profile without access to the innovator’s proprietary coating or granulation process. QbD approaches using in vitro dissolution profiling and population PK modeling reduce the number of human bioequivalence studies needed.
Inhalation products (MDIs, DPIs, nasal sprays) remain among the hardest categories. The FDA currently requires both pharmacokinetic bioequivalence and in vitro aerodynamic particle size distribution testing for most inhaled generics. For DPIs, a device-specific approach is often required because dose delivery depends on the inhaler device’s resistance characteristics. Teva’s generic Advair (fluticasone/salmeterol) application illustrates the complexity: the FDA rejected multiple attempts before approving Wixela in January 2019, roughly 16 years after the reference product launched.
Microspheres and liposomal products (e.g., generic Lupron Depot, generic Doxil) require demonstrating equivalence in both drug release kinetics and, for liposomes, particle morphology. The FDA’s PSG for liposomal products requires a comprehensive physicochemical characterization package alongside in vitro release testing. No purely in vivo bioequivalence approach has been accepted as sufficient for complex liposomal generics.
Drug-device combinations for injectable products, particularly auto-injectors and prefilled syringes, involve both pharmaceutical and device regulatory pathways. The FDA’s 2019 draft guidance on combination products for ANDAs clarified that the device constituent must be evaluated for safety and function, and that human factors studies may be required if the device design differs meaningfully from the RLD.
Transdermal systems (patches) require in vitro permeation testing and often comparative clinical endpoint studies when the membrane and adhesive system differs. The FDA has accepted Q1/Q2 sameness (identical qualitative and quantitative formulation) arguments for some transdermal generics, but this approach only works when the manufacturer can replicate the reference formulation precisely.
Sandoz/Novartis as a Case Study in Complex Generic IP Strategy
Sandoz, Novartis’s generics division, made a deliberate strategic pivot toward biosimilars and complex pharmaceutical generics when conventional generic margins compressed. The rationale was explicit in company filings: complex products generate higher margins, attract fewer competitors, and create defensible IP positions that persist past initial approval. Sandoz’s biologic portfolio includes Zarxio (filgrastim), the first FDA-approved biosimilar in the U.S. (March 2015), and Hyrimoz (adalimumab biosimilar), approved in July 2023.
The IP architecture around each product illustrates the strategy. Zarxio’s Biologics License Application relied on demonstrating biosimilarity to Amgen’s Neupogen. Sandoz secured no patent exclusivity on the molecule (the composition-of-matter patent had expired), but held manufacturing process IP and device-level patents on the prefilled syringe presentation that deterred some follow-on entrants. Hyrimoz competes in a market where Abbvie’s Humira generated $21.2 billion in 2022 global revenues, making even a small market share extraordinarily valuable.
Key Takeaways: Complex Generics
- The commercial value of complex generics comes from technical barriers that limit competition even after ANDA approval. Pricing durability is structurally better than in conventional generic markets.
- Companies building complex generic pipelines should sequence their technology platform development: oral extended-release first (deepest regulatory precedent), then transdermal, then inhalation, then injectables and liposomials (highest development risk but also highest barriers to entry for competitors).
- Authorized generic risk is lower for complex products due to manufacturing barriers. This makes the 180-day exclusivity more durable.
- IP valuation for complex generic assets should reflect lower competitor count, better pricing dynamics, and the presence of ancillary manufacturing or device patents.
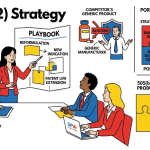
IV. The 505(b)(2) Strategy: Building Exclusivity Where ANDAs Cannot
The Regulatory Mechanics of 505(b)(2)
The 505(b)(2) NDA is authorized by Section 505(b)(2) of the Federal Food, Drug, and Cosmetic Act. It allows the applicant to rely on data that the applicant did not develop: the FDA’s own findings of safety and efficacy for a previously approved drug (the reference product), or published literature establishing safety and efficacy for the relevant active ingredient. The sponsor must then conduct whatever additional studies are necessary to support the specific differences in the new product.
The FDA evaluates 505(b)(2) applications under the same safety and efficacy standard as full NDAs, but the evidentiary burden is lower because the agency already has an established safety profile for the active ingredient. What the sponsor must prove is that the modified product’s differences (new form, new delivery, new combination) do not introduce new safety risks and do achieve the clinical effect claimed.
The result is a hybrid economics of drug development. The sponsor pays for the incremental clinical work associated with the modification, not the full safety and efficacy trial program of a novel molecular entity. For many modified products, that incremental program consists of one to three Phase 1 pharmacokinetic studies and one Phase 3 efficacy study for the new indication or new patient population. Total development costs for well-chosen 505(b)(2) candidates typically fall in the $5 to $50 million range, compared to $100 to $500 million for a full NDA and $1 to $2.5 billion for a novel molecular entity.
Exclusivity Periods as Standalone IP Assets
The exclusivity periods available under 505(b)(2) are the strategic justification for the entire pathway. They are independent of patents and stack on top of any patent-based exclusivity the applicant holds.
Three-year exclusivity applies to 505(b)(2) applications that rely on at least one new clinical investigation essential to approval (conducted or sponsored by the applicant). This exclusivity protects against the filing of any ANDA or 505(b)(2) application that relies on the same finding for the same condition of use. It does not prevent the FDA from approving an NDA for the same drug.
Five-year new chemical entity (NCE) exclusivity applies when the active moiety has never been approved in any form. For 505(b)(2) applications, this is uncommon, but it can apply when the modification involves a truly novel salt form, ester, or polymorph that qualifies as a new chemical entity.
Seven-year orphan drug exclusivity applies to products designated and approved for rare diseases affecting fewer than 200,000 people in the U.S. This exclusivity is absolute: the FDA cannot approve a competitor application for the same drug for the same orphan indication during the seven-year window, regardless of whether the competitor holds patents.
These exclusivity periods are not merely regulatory artifacts. They are balance-sheet items. A 505(b)(2) product with seven-year orphan exclusivity and a strong market position is worth more than a conventional generic with six months of 180-day exclusivity and immediate post-exclusivity price erosion. The NPV differential is often an order of magnitude.
Reimbursement and the J-Code Strategic Variable
The commercial success of a 505(b)(2) product in the physician-administered (buy-and-bill) market depends critically on reimbursement code assignment. Prior to January 2022, many 505(b)(2) drugs were grouped under shared J-codes with therapeutically equivalent generics, effectively treating them as commodity products for reimbursement purposes regardless of their distinct clinical profile.
CMS’s 2022 policy change altered this dynamic. When the FDA has determined that a 505(b)(2) drug is not therapeutically equivalent to the reference drug, CMS now assigns a unique J-code to that product. A unique J-code means the drug is reimbursed as a sole-source product, at ASP plus the applicable markup, without competition from lower-priced generics sharing the same code.
Securing a non-equivalent determination from FDA is not automatic. It requires the applicant to explicitly request it, and FDA grants it only when the product’s differences from the RLD are clinically meaningful in a way that precludes substitution. This means the therapeutic equivalence determination strategy must be planned during product development, not after approval.
Portfolio managers evaluating 505(b)(2) assets should model two reimbursement scenarios: shared J-code (effectively generic pricing) and unique J-code (brand-like pricing). The difference in NPV between these scenarios for a mid-sized physician-administered oncology or rheumatology product commonly exceeds $100 million.
Successful 505(b)(2) Products: IP Architecture Examples
Suboxone film (buprenorphine/naloxone) illustrates how a 505(b)(2) modified formulation can dominate a market established by the original innovator product. Reckitt Benckiser’s film formulation relied on the FDA’s prior approval of Suboxone tablets, then added clinical data demonstrating improved dissolution rates and reduction in pediatric accidental exposure risk. The FDA approved the film in 2010. By 2012, the film formulation held roughly 60% of the buprenorphine/naloxone market. The IP portfolio around the film included several formulation patents, none of which survived challenge in subsequent litigation, but the regulatory data exclusivity and market positioning built during the exclusivity window created durable commercial advantage.
Bendeka (bendamustine) entered the market as a 505(b)(2) product with a reformulated, ready-to-dilute presentation (50 mL, lower volume) versus the reference Treanda (500 mL). Eagle Pharmaceuticals secured three-year exclusivity based on new clinical investigations demonstrating the pharmacokinetic equivalence of the new formulation. The unique J-code assignment, which Eagle actively pursued, gave Bendeka a pricing advantage over Treanda that was structurally independent of patents. The commercial strategy was explicit: use regulatory exclusivity and reimbursement architecture to insulate the product from generic pressure on the reference formulation.
Glumetza (extended-release metformin, Santarus/Valeant) used a gastric-retentive osmotic pump formulation to achieve once-daily dosing with reduced GI side effects compared to immediate-release metformin. The 505(b)(2) approval rested on new clinical data demonstrating the distinct pharmacokinetic profile and tolerability benefit. The formulation patents and regulatory exclusivity created a window of profitability before conventional metformin generics began capturing the managed care formulary position.
Investment Strategy: 505(b)(2) Pipeline Valuation
When evaluating a pharma company’s 505(b)(2) pipeline, the relevant diligence questions are: What exclusivity type is available, and has the company confirmed that determination with FDA? Is the product modification clinically meaningful enough to support a non-equivalence determination and unique J-code? How defensible are the formulation or use patents beyond the regulatory exclusivity period? What is the company’s strategy for the post-exclusivity period, when competition from ANDAs or other 505(b)(2) filings begins?
Companies with multiple 505(b)(2) products in the pipeline, particularly in physician-administered markets where J-code assignments are material, warrant a valuation premium over pure-play conventional generic companies. The combination of regulatory exclusivity, potential unique J-code, and lower development cost relative to novel molecular entities creates a risk-adjusted return profile that is often undervalued in generic peer group multiples.
Key Takeaways: 505(b)(2) Strategy
- The three strategic advantages of 505(b)(2) over ANDA are: access to market exclusivity periods (3, 5, or 7 years), protection from automatic generic substitution during those periods, and eligibility for unique J-code assignment in physician-administered markets.
- Orphan drug designation stacks with 505(b)(2) approval to deliver seven-year market exclusivity. For rare disease applications, this is the most defensible market position available to a modified product.
- The J-code determination strategy must be incorporated into clinical development planning. The FDA’s non-equivalence determination requires specific supporting data; it cannot be retroactively engineered post-approval.
- NPV modeling for 505(b)(2) assets should include a scenario analysis across J-code outcomes. The reimbursement architecture drives commercial value more than the exclusivity period in physician-administered markets.
V. Paragraph IV Challenges: Executing the Patent Attack
Target Selection: Which Patents Are Worth Challenging
Not all Orange Book patents are equally vulnerable. The return on a Paragraph IV challenge depends on two things: whether the patent can be invalidated or circumvented, and whether winning the challenge opens a market worth the litigation expense. A rigorous target selection process precedes any Paragraph IV filing.
Composition-of-matter patents on a novel active ingredient are the hardest to invalidate. These patents, particularly those issued in the 1980s and 1990s before prior art searches became computationally comprehensive, occasionally contain invalidating prior art. But the baseline assumption should be that core API patents will be defended aggressively and often successfully.
Secondary patents are more fertile ground. Formulation patents (claiming specific excipient combinations, particle sizes, coating systems), method-of-use patents, and process patents are all vulnerable to prior art attacks and obviousness arguments. Orange Book listings frequently include patents that, on their face, appear to limit generic entry but contain claims drafted broadly enough to allow design-around without infringement, or narrowly enough that a generic with a different excipient profile never infringes in the first place.
Manufacturing patents and metabolite patents have been challenged on Orange Book listing eligibility grounds. The FDA’s Orange Book listing rules require that listed patents claim the drug or its method of use. Manufacturing process patents do not qualify for listing, and their presence in the Orange Book can be challenged directly through an administrative dispute resolution process or in district court litigation. Challenging an improper listing is cheaper than litigating infringement and, when successful, eliminates the 30-month stay for the associated patent.
Prior Art Analysis and PTAB as Parallel Tracks
The standard invalidity toolkit for Paragraph IV challenges draws on prior art searches, obviousness arguments, and claim construction disputes. Prior art analysis requires comprehensive searching of patent databases (USPTO, EPO, Derwent), scientific literature (PubMed, chemical databases), and foreign patent filings. The goal is identifying publications, patents, or public disclosures predating the challenged patent’s priority date that disclose the claimed invention, or that render it obvious by obvious combination.
Patent Trial and Appeal Board proceedings, specifically Inter Partes Review (IPR), run parallel to district court litigation and provide a faster, cheaper forum for invalidity challenges. PTAB IPR petitions must be filed within one year of service of a complaint alleging infringement of the challenged patent. The IPR process runs approximately 18 months from institution to final written decision. Institution rates on IPR petitions have hovered around 55 to 65% in recent years, with claim cancellation rates (full or partial) in instituted proceedings around 60 to 70%.
The tactical value of IPR in Hatch-Waxman litigation is threefold. First, it creates a parallel proceeding that increases litigation costs for the brand, potentially accelerating settlement discussions. Second, if the PTAB cancels the challenged claims, the district court litigation resolves (or the stay expires without further legal basis). Third, the IPR creates a public record of prior art arguments that can inform the district court proceedings even if the IPR is not fully decided within the 30-month stay window.
The limitation of IPR in the Hatch-Waxman context is the estoppel. Once a final written decision is issued in IPR, the petitioner cannot argue in district court that the surviving patent claims are invalid on any ground that was raised or reasonably could have been raised in the IPR. That estoppel must be factored into the IPR petition strategy: identify the strongest invalidity arguments and determine whether they are better preserved for district court or exhausted in IPR.
Venue Selection and Litigation Dynamics
The majority of Hatch-Waxman patent cases are filed in the District of Delaware and the District of New Jersey. Both districts have dense case law on pharmaceutical patent issues, and judges in these districts have technical familiarity that accelerates case management. Delaware, in particular, handles a disproportionate share of pharmaceutical patent litigation because a large fraction of branded pharmaceutical companies are incorporated there.
The Federal Circuit, which has exclusive jurisdiction over appeals in patent cases, has produced a substantial body of Hatch-Waxman-specific doctrine. Key decision areas include obviousness analysis for secondary patents (particularly the teaching-away doctrine as applied to pharmaceutical formulations), claim construction for method-of-use patents, and the standard for granting preliminary injunctions in at-risk launch scenarios.
Generic companies launching at-risk (before the district court resolves the patent dispute) take on the risk of being enjoined and ordered to pay damages measured by the brand’s lost profits during the at-risk period. The decision to launch at-risk requires a rigorous assessment of the likelihood of success on the merits, the magnitude of the bond that may be required, and the commercial value of the early launch relative to waiting.
Design-Around as a Non-Litigation Alternative
Designing around an existing patent means developing a non-infringing version of a product that achieves the same therapeutic purpose through means not covered by the challenged claims. This is a parallel strategy to direct patent challenge, not a substitute. In some cases, designing around is faster and cheaper than litigation; in others, it is impossible because the claims are written broadly enough to capture any commercially viable approach.
The design-around analysis begins with claim construction: reading each claim element against the proposed generic formulation and manufacturing process to determine whether every element is present. Patent claims use ‘comprising’ language (open-ended, meaning additional elements are permitted) versus ‘consisting of’ language (closed, meaning only the listed elements). A claim that uses ‘consisting of’ for a specific excipient list is easier to design around than one using ‘comprising’ with a broad functional description.
Freedom-to-Operate (FTO) analysis, conducted before any product development investment, maps the entire Orange Book patent landscape for the target RLD, identifies claims that could be asserted against the proposed generic, and assesses design-around feasibility for each. Companies that skip FTO analysis discover infringement risks after bioequivalence studies are complete, at which point the cost of reformulation is maximized.
The FTO analysis also identifies patents not listed in the Orange Book that may nonetheless be asserted against the generic. Method-of-treatment patents, for example, are sometimes not listed but can be asserted if the generic’s label actively encourages infringement of the patented method.
Evergreening: The Brand Playbook and the Generic Counter-Strategy
Evergreening refers to a collection of strategies brand companies use to extend effective market exclusivity beyond the original composition-of-matter patent expiration. Understanding these strategies is as important for generic companies as for brand IP teams, because each evergreening tactic creates a specific countermeasure.
Patent thicketing involves filing multiple overlapping patents on formulations, excipients, particle sizes, manufacturing processes, metabolites, enantiomers, and methods of use. A branded drug with 30 to 40 Orange Book patents forces generic companies to file Paragraph IV certifications against each one and defend against potential infringement claims on all of them. The litigation burden is multiplicative. Generic companies counter by identifying which patents in the thicket are substantively weak (narrow claims, obvious formulation patents, patents with clear prior art) and concentrating challenge resources there while designing around the remainder.
Product hopping is the practice of transitioning a drug from one formulation to another (e.g., tablet to capsule, twice-daily to once-daily) in anticipation of generic entry on the original formulation. The brand uses its prescriber relationships and payer contract leverage to migrate patients to the new formulation before generic entry. The new formulation typically has its own patent protection. Allergan’s Namenda (memantine) product hop to Namenda XR before generic memantine IR entry was litigated by the FTC on antitrust grounds; the Second Circuit blocked the withdrawal of the original formulation. Generic companies facing a product hop should monitor the brand’s REMS programs, promotional spend shifts, and formulary strategies for early signals.
REMS-based sample blocking occurs when a brand company creates a Risk Evaluation and Mitigation Strategy program with restricted distribution and uses that program to deny generic manufacturers access to reference product samples needed for bioequivalence testing. The FDA Safety and Innovation Act of 2012 (FDASIA) prohibits this practice explicitly. The FDA’s 2021 guidance on REMS and generic access formalized the procedures for generic companies to obtain reference samples for development. Generic companies encountering sample access obstruction should file a formal complaint with FDA’s Office of Generic Drugs and document every denial.
Key Takeaways: Paragraph IV Execution
- Secondary formulation and method-of-use patents are the most viable litigation targets. Core composition-of-matter patents on active ingredients are rarely invalidated; the strategy should be design-around rather than head-on challenge.
- IPR and district court litigation should be planned as coordinated tracks. The estoppel implications of IPR final written decisions must inform which arguments are raised there vs. preserved for district court.
- FTO analysis must precede bioequivalence development, not follow it. The cost of discovering infringement risk after pivotal studies is prohibitive.
- Evergreening counter-strategies are specific to tactic: patent thickets require concentrated challenge against the weakest patents; product hops require early market monitoring and potentially antitrust engagement; REMS-based blocking requires FDA administrative process and contemporaneous documentation.
VI. Patent Intelligence as a Core Business Function
Building a Patent Landscape Analysis Capability
Patent landscape analysis is systematic mapping of the patent activity in a therapeutic area or around a specific molecule. It identifies who holds relevant IP, what claims they hold, when those claims expire, where geographic coverage exists and where it does not, and what white spaces remain unprotected.
Generic companies that treat patent landscape analysis as a standalone project, rather than a continuous function, consistently underperform those that institutionalize it. The reason is temporal: patent filings are forward-looking intelligence. A brand company’s continuation application filed today signals the next generation of Orange Book listings, which will govern generic entry timelines three to five years from now. Companies reading that signal have a multi-year head start in development planning.
The analytical process for a comprehensive landscape involves searching USPTO, EPO’s Espacenet, WIPO’s PatentScope, and commercial databases (Derwent, PatSeer, Clarivate) using structured query strings built from the drug’s CAS number, INN, known synonyms, therapeutic class, and relevant formulation terminology. The resulting patent family set must be deduped, classified by claim type (composition, formulation, use, process, device), and mapped against the Orange Book listings to identify discrepancies between what is listed and what has been filed.
Discrepancies between Orange Book listings and the full patent portfolio are strategically significant in both directions. Brands sometimes fail to list patents they should have listed, inadvertently shortening their effective exclusivity. More commonly, brands list patents that may not meet Orange Book listing criteria, requiring challenge.
Competitive Intelligence: Building a Real-Time Monitoring System
Competitive intelligence in generic pharma draws from patent filings, ANDA tracker publications (the FDA publishes first-time generic approvals and tentative approvals weekly), clinical trial registries, earnings call disclosures, and regulatory submission databases. The integration of these sources into a coherent picture of competitor pipelines and timelines is the function of a formal CI operation.
The FDA’s ANDA approval tracker and the Paragraph IV certification database are public-domain inputs that enable generic companies to track competitor filings against the same targets. A company that files a Paragraph IV certification can quickly determine whether they are the first filer (and therefore hold potential 180-day exclusivity), a subsequent filer (subject to the forfeiture provisions), or entering a market where no exclusivity is available.
Earnings call analysis provides softer intelligence on strategic priorities. When a generic company’s management discusses a specific therapeutic category as a priority for new filings, or when a brand company discloses a REMS program expansion or a new formulation patent filing, both signals are material to competitor pipeline planning.
Clinical trial registry monitoring identifies branded development programs in their early clinical stages, providing three to five years of advance notice of drugs that may lose exclusivity or that may be subject to 505(b)(2) modification strategies by competitors. A Phase 2 study filed today on a novel once-daily formulation of an established drug is a signal that the sponsor intends a 505(b)(2) filing within two to three years, which in turn means the generic company has that window to file its own ANDA on the reference formulation before the brand migrates prescribers.
White Space Identification: Finding Unprotected Opportunities
White spaces are regions of a patent landscape with no, or minimal, patent coverage, representing areas where innovation is possible without infringing existing IP. Identifying them requires not just knowing what is patented but understanding the technical trajectory of the field: what innovations are coming, what prior art exists that would invalidate prospective patents in the space, and whether unmet clinical needs exist that could anchor a development program.
For generic companies, the most actionable white spaces fall into several categories. The first is therapeutic areas where the composition-of-matter patent has expired but no generic exists (often because of REMS restrictions, formulation complexity, or limited market size). The second is patient populations where the branded drug is used off-label without a corresponding approved indication, creating 505(b)(2) opportunity. The third is formulation modifications that offer a documentable clinical benefit (bioavailability improvement, reduced dosing frequency, elimination of food effect) without infringing existing formulation patents.
Drug repurposing is a specialized form of white space analysis. It identifies existing approved drugs with known safety profiles that may have clinical activity in new indications. The canonical examples are well-known: thalidomide in multiple myeloma, sildenafil in pulmonary arterial hypertension. For generic companies, the relevant observation is that a repurposed use of an off-patent molecule, supported by new clinical data, can qualify for 505(b)(2) approval and three-year exclusivity. The clinical investment is smaller than for a novel drug, and the safety risk is already characterized.
Investment Strategy: Patent Intelligence Infrastructure
Institutional investors evaluating generic pharma companies should assess the patent intelligence function as a leading indicator of pipeline quality. Companies with sophisticated patent monitoring capabilities, demonstrated by early and accurate Paragraph IV filings on the highest-value targets, consistent first-filer exclusivity capture, and proactive design-around programs, consistently outperform companies that rely on reactive, project-by-project IP assessments.
The infrastructure cost is modest relative to the return. A dedicated patent analytics function with access to commercial database subscriptions (Derwent Innovation, DrugPatentWatch, Orange Book Plus), two to three specialized patent analysts, and defined processes for new target evaluation and competitor monitoring runs at $1 to $3 million annually. The identification of a single high-value Paragraph IV target with first-filer exclusivity potential can justify that investment for a decade.
Key Takeaways: Patent Intelligence
- Patent landscape analysis is a continuous operational function, not a project. Continuation patent filings today signal Orange Book listings three to five years from now. The companies reading those signals have a multi-year development head start.
- The FDA’s ANDA tracker, Paragraph IV certification database, and clinical trial registries are all public-domain intelligence inputs. Companies not using these sources systematically are operating blind relative to competitors that do.
- White space identification converts patent landscape data into R&D investment targets. The most actionable white spaces are expired composition-of-matter patents without generics (REMS or formulation-complexity barriers), off-label indications without approved generics, and formulation modifications offering documentable clinical benefit.
- Patent intelligence infrastructure costs $1 to $3 million annually. A single first-filer exclusivity capture on a $1 billion-revenue drug generates 30 to 50 times that investment in incremental margin during the exclusivity window.
VII. Lifecycle Management: The Generic Company’s Own Patent Portfolio
From Copycat to IP Holder: Building Proprietary Generic IP
Lifecycle management is traditionally described as a brand company strategy: file continuation patents, develop next-generation formulations, seek new indications, and migrate the market before generic entry. But generic companies can and should build their own lifecycle management programs, creating proprietary IP around the products they develop.
The mechanism is straightforward. When a generic company develops a complex formulation to achieve bioequivalence with a technically challenging RLD, the manufacturing process, excipient system, or particle engineering approach used may itself be novel and patentable. That process patent does not appear in the Orange Book (process patents cannot be listed), but it provides a real competitive barrier to subsequent generic entrants: any competitor seeking to develop the same generic must either design around the process patent or license it.
Similarly, a generic company developing a 505(b)(2) product has explicit opportunities to file composition, formulation, and method patents on the modified product. Those patents, filed before ANDA or 505(b)(2) submission, can be listed in the Orange Book (for composition and use claims) and will trigger 30-month stays against subsequent generic challengers. The generic company is now on the other side of the Hatch-Waxman dynamic.
Parenteral to Oral Conversion as a 505(b)(2) Pipeline Strategy
Converting a drug from parenteral (injectable) administration to oral delivery is one of the highest-value formulation innovation strategies in pharma. The clinical rationale is clear: oral dosing improves patient compliance, reduces healthcare resource utilization (no infusion center visit), and expands the patient population that can access the drug. The regulatory rationale for 505(b)(2) is equally clear: the conversion requires new clinical studies demonstrating oral bioavailability and PK equivalence to the parenteral form, which qualifies as new clinical investigations essential to approval.
Successful oral conversion programs require resolving the formulation science challenge of achieving adequate and reproducible oral bioavailability for molecules that are typically parenterally administered because oral bioavailability is poor. Technologies that have been applied include lipid-based drug delivery systems (self-emulsifying drug delivery systems, or SEDDS), nanotechnology approaches (nanoparticle formulations to increase surface area), and prodrug strategies that improve intestinal permeability.
The IP protection for a successful oral conversion is layered. The conversion itself may not be patentable if it is obvious in view of prior art (the molecule exists, and oral conversion was a known goal). But the specific formulation enabling adequate bioavailability (the SEDDS composition, the specific nanoparticle engineering approach, the prodrug structure) is often patentable, particularly if it achieves unexpected results relative to what the prior art would have predicted.
New Indication Strategies and Evergreening by Generics
Generic companies with strong clinical capabilities can pursue new indication approvals for off-patent molecules, generating 505(b)(2) exclusivity through a strategy structurally similar to brand company evergreening but applied to off-patent drugs.
The playbook begins with compound repurposing analysis: identifying signals in published literature, case reports, or mechanistic hypotheses that an off-patent molecule may have activity in an indication where it is not approved. The development program then pursues a Phase 2 proof-of-concept study and, if positive, a Phase 3 registration study sufficient to support a 505(b)(2) NDA with a new indication.
This strategy is most economically viable when the off-patent molecule has a well-understood safety profile (reducing Phase 3 safety monitoring costs), when the target indication has an established clinical endpoint (reducing the need for surrogate endpoint development), and when the patient population is small enough to qualify for orphan designation (which delivers seven-year exclusivity rather than three). Companies that combine a new indication 505(b)(2) with orphan designation create the most durable commercial position available on an off-patent molecule.
Key Takeaways: Lifecycle Management for Generics
- Generic companies developing complex products should file patents on novel manufacturing processes, excipient systems, and particle engineering approaches. These process patents do not appear in the Orange Book but create real competitive barriers.
- 505(b)(2) products with patentable formulation innovations can be listed in the Orange Book, triggering 30-month stays against subsequent generic challengers. The company has crossed from generic challenger to IP holder.
- Parenteral-to-oral conversion programs generate 505(b)(2) exclusivity when the conversion requires new clinical studies. The formulation enabling adequate oral bioavailability is often independently patentable.
- New indication programs on off-patent molecules, particularly when combined with orphan designation, create seven-year market exclusivity on products that conventional generics cannot touch during that window.
Conclusion: The Integrated Post-ANDA Operating Model
The companies that win in the post-ANDA market run a fundamentally different business than generic companies operating the way the industry worked in 1995. The conventional model, file ANDAs on straightforward molecules, wait for patent expiration, compete on price, has a terminal economics problem. Commodity generics with six to ten market entrants within two years of first launch generate operating margins in the low single digits. That math does not sustain the R&D investment needed to refresh a pipeline.
The winning operating model integrates five capabilities. First, a patent intelligence function that operates continuously, reads competitor filings as forward-looking intelligence, and updates the product prioritization framework in real time. Second, an R&D operation capable of complex generic development, including the formulation science, bioequivalence design, and manufacturing process development needed for inhalation products, injectables, and drug-device combinations. Third, a regulatory strategy capability that selects between ANDA and 505(b)(2) at project initiation, engages FDA through pre-ANDA and pre-IND meetings, and tracks PSG updates as competitive intelligence. Fourth, a patent litigation and design-around function that runs Paragraph IV challenges against vulnerable secondary patents, coordinates IPR and district court strategy, and maintains current FTO analyses on all active development programs. Fifth, a business development capability that evaluates pipeline assets, partnership structures, and licensing opportunities with the IP valuation rigor the market demands.
No individual capability on that list is novel. What is unusual is the full integration: the patent intelligence feeding the product prioritization, the regulatory strategy informing the litigation planning, the lifecycle management creating new IP from the generic development process itself. Companies that run all five functions at a high level and integrate them into a single commercial decision framework are the ones that consistently capture 180-day exclusivity, build complex generic franchises with durable margins, and convert 505(b)(2) approvals into exclusivity periods that compound returns across multiple product cycles.
That is what winning post-ANDA looks like. It is an operating model, not a tactic.
Data in this article reflects publicly available sources including FDA Orange Book, PTAB statistics, CMS reimbursement guidelines, and company public filings as of the date of publication. This article does not constitute legal or investment advice. Readers should consult qualified legal counsel and financial advisors before making decisions based on the analysis presented.