The path from discovery to commercial dominance has never been more expensive, more legally treacherous, or more dependent on intelligence quality. Between regulatory divergence, a looming biosimilar wave, unresolved AI inventorship law, and a digital threat landscape that most biotech security teams are spectacularly unprepared for, the 2025-2026 operating environment is a pressure test for every IP, R&D, and BD function in the industry.
This analysis does not cover the surface. It goes deep into the six core structural challenges reshaping pharmaceutical biotech — and for each one, maps the specific, data-driven IP and commercial response that turns threat into defensible advantage. The intended audience is pharma and biotech IP teams, portfolio managers, R&D leads, and institutional investors who need technical density, not bullet-pointed reassurance.
Issue 1: The Regulatory Maze — From Compliance Hurdle to IP Asset
Why FDA/EMA Divergence Is a Patent-Generation Machine
Regulatory divergence across major markets — the U.S., EU, China, and Japan — is routinely framed as a cost problem. That framing is incomplete. The deeper, more strategically useful truth is that divergent regulatory requirements force companies to develop jurisdiction-specific solutions, and those solutions are often independently patentable.
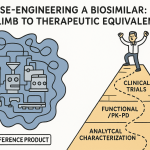
The gap between FDA and EMA expectations is widest in cell and gene therapies (CGTs). The FDA’s accelerated approval pathway, which accepts surrogate endpoints for early market access, has no reliable EMA equivalent. The EMA’s conditional marketing authorization pathway demands a different evidentiary standard — often longer-duration safety follow-up, distinct patient selection criteria, and risk management protocols that the FDA does not require. For a company running a single global trial design, that divergence adds years and capital to a European launch.
But here is what most companies miss: the solution to that divergence is frequently a new patent. A dosing regimen developed specifically to satisfy EMA’s risk management requirements — lower starting dose, modified titration schedule, toxicity monitoring protocol — can be novel, non-obvious, and patentable as a method-of-use claim. A drug-device combination designed to meet different administration requirements in Europe than in the U.S. can generate a new, jurisdiction-differentiated formulation patent. The regulatory hurdle, once cleared, produces an IP artifact that is entirely independent of the original composition of matter (CoM) patent. Senior IP teams exploit this systematically. Junior teams just clear the hurdle and move on.
The same logic applies to China’s National Medical Products Administration (NMPA), which has been accelerating its approval timelines under Priority Review designation — analogous to FDA’s Breakthrough Therapy designation — while maintaining domestic clinical data requirements that frequently differ from Western trial designs. Any company modifying its clinical protocol for NMPA submission should be asking its IP counsel, in real time, whether that modification constitutes an independent invention.
The Composite Shield: What ‘Patent Protection’ Actually Means
The industry’s most persistent misconception is the ‘twenty-year monopoly.’ A drug patent’s statutory term begins on the application filing date, not the approval date. Given that average drug development plus regulatory review consumes ten to fifteen years, most drugs reach market with fewer than ten years of effective patent life remaining. The raw statutory clock is almost irrelevant to commercial strategy.
What actually protects a drug’s revenue is a layered structure of two separate legal systems running concurrently — patents and regulatory exclusivities — administered by two different federal agencies under two different statutes.
Patents are granted by the USPTO under the Patent Act. They confer the negative right to exclude others from making, using, or selling the claimed invention. Regulatory exclusivities are granted by the FDA under the FD&C Act and, for biologics, under the BPCIA. They are affirmative rights that block the FDA itself from accepting or approving a competitor’s abbreviated application — an ANDA for small molecules, a 351(k) biosimilar application for biologics — for defined periods.
The full picture for a single drug asset looks like this:
| Protection Type | Governing Authority | Duration | Operative Effect |
|---|---|---|---|
| Patent Term | USPTO / Patent Act | 20 years from filing | Excludes infringers from making/using/selling the claimed invention |
| New Chemical Entity (NCE) Exclusivity | FDA / FD&C Act Sec. 505(c)(3)(E)(ii) | 5 years from NDA approval | Blocks FDA from accepting an ANDA for 4 years; approving it for 5 years |
| New Clinical Investigation Exclusivity | FDA / FD&C Act Sec. 505(c)(3)(E)(iii) | 3 years from sNDA approval | Blocks FDA approval of a generic for the specific approved change (new indication, new dosage form, OTC switch) |
| Orphan Drug Exclusivity (ODE) | FDA / Orphan Drug Act | 7 years from approval | Blocks FDA approval of same drug for same rare disease |
| Pediatric Exclusivity | FDA / BPCA | 6-month add-on | Attaches to all existing patents and exclusivities; extends them by 6 months |
| Biologic Data Exclusivity | FDA / BPCIA Sec. 351(k)(7) | 12 years from reference product approval | Blocks FDA from approving a 351(k) biosimilar application |
| Patent Term Extension (PTE) | USPTO / Hatch-Waxman Act Sec. 156 | Up to 5 years added | Compensates for regulatory review time lost during FDA approval process |
These clocks run simultaneously and expire on different dates. A CoM patent may expire in 2029 while an ODE runs through 2030 and a pediatric exclusivity add-on from a 2025 study extends all remaining protections to mid-2031. The ‘true’ loss-of-exclusivity (LOE) date — the date on which a generic or biosimilar can realistically enter the market — is not any single date. It is the latest date on which the final piece of the composite shield expires.
Any analysis that looks only at the primary CoM patent expiry understates protection duration. Any analysis that looks only at regulatory exclusivity and ignores the patent estate understates litigation risk for generic entrants. Only integrated analysis — tracking both systems simultaneously — produces an accurate LOE date.
Key Takeaways — Issue 1
Regulatory divergence is a patent-generation opportunity that most IP teams fail to monetize. Every jurisdiction-specific solution is a potential independent invention. Effective LOE analysis requires simultaneous tracking of the patent estate and all active regulatory exclusivities, because neither alone produces an accurate market entry forecast. FDA/EMA misalignment in CGTs is particularly acute, with different evidentiary standards for surrogate endpoints creating meaningfully different development timelines and formulation requirements.
Investment Strategy
For portfolio managers evaluating branded pharma assets, the primary valuation error is using a single patent expiry date as the LOE proxy. True LOE modeling requires layered exclusivity analysis. Assets with stacked ODE plus pediatric exclusivity plus active process patents frequently have 24-36 months of additional commercial runway beyond what headline patent expiry dates suggest. This gap is most common in rare disease and pediatric oncology assets — exactly the categories where biosimilar development costs are highest and branded price protection most durable.
Issue 2: The Capital Crunch — IP as the Only De-Risking Tool That Works
What R&D Actually Costs: The $708 Million Figure Investors Need
For decades, the pharmaceutical industry has cited a headline cost-of-development figure that has inflated progressively toward and past $2 billion per approved drug. The Deloitte 2025 R&D returns report puts the average at $2.23 billion per asset. These figures include the cost of failure — the capital deployed on programs that do not reach approval — which is the correct economic basis for the fully-loaded cost.
The problem with the $2.23 billion figure is not accuracy. The problem is that it is driven by a small number of extraordinary outliers. A 2025 RAND analysis of 38 recently approved drugs found a mean adjusted R&D cost of $1.3 billion — already well below the industry-cited figure — but, critically, a median of $708 million. That median is the appropriate statistic for characterizing a ‘typical’ drug development investment, because it is not inflated by the handful of programs that cost $5 billion or more to develop.
For a founder constructing an investor pitch, or a BD team justifying a licensing deal, the $708 million median is the more intellectually honest and commercially useful number. It reframes the investment from ‘impossible bet’ to ‘quantifiable, high-stakes capital allocation’ — exactly the framing a sophisticated investor needs to begin constructing a risk-adjusted return model.
What Investors Are Actually Checking in IP Due Diligence
When a biotech raises a Series B or enters a licensing negotiation with a large pharmaceutical partner, the investor or counterparty will conduct IP due diligence. This is not a box-checking exercise. It is a structured adversarial search for vulnerabilities that a future generic challenger or litigation opponent could exploit.
The due diligence checklist, executed by patent counsel working for the counterparty, covers four areas that frequently surface deal-ending problems.
Chain of title is the first and most common failure point. Every inventor listed on every patent must have executed a valid assignment agreement transferring their rights to the company. Academic collaborators, contract research organization (CRO) scientists who contributed to key experiments, and former employees who left before the company formalized its IP assignments are all potential gaps. A broken chain of title means the company does not fully own its primary asset — a deal-breaker in any transaction.
Freedom-to-Operate (FTO) is the second checkpoint. Does the company have documented legal analysis confirming it can commercialize its lead asset without infringing any in-force third-party patents? For a small molecule, this covers the molecule, its synthesis, its formulation, and its primary method of use. For a biologic or CGT, as discussed in depth below, the FTO must cover the entire manufacturing and delivery platform. A company that cannot produce an FTO opinion is signaling to the counterparty that it either has not looked for blocking patents — naivety — or has found them and is hoping no one notices, which is worse.
Prior art completeness is the third area of scrutiny. The investor’s patent attorney will search for ‘knockout’ prior art: a published scientific paper, a conference abstract, a foreign patent application, or any public disclosure that clearly anticipated the claimed invention before the filing date. If that prior art exists and the patent examiner missed it, the patent is likely invalid under 35 U.S.C. § 102 and can be challenged through inter partes review (IPR) at the PTAB or in district court litigation. A company whose core patent survived prosecution does not necessarily have a valid patent; it has a patent that has not yet been challenged with the right prior art.
Prosecution history estoppel is the fourth area, and the most technically complex. During prosecution, a patent applicant often narrows claims in response to USPTO rejections. Those narrowing amendments create ‘estoppel’ — the applicant is legally barred from later arguing, in infringement litigation, that the claim covers territory it explicitly gave up during prosecution. A competitor’s patent counsel reads the prosecution history of every patent they are accused of infringing, looking for claim scope surrendered by estoppel. A founder who has not read their own prosecution history with this adversarial lens is not prepared for the questions they will receive in a serious due diligence process.
Key Takeaways — Issue 2
The $708 million RAND median is the correct reference figure for single-asset R&D cost discussions with investors — not the $2.23 billion Deloitte mean, which is inflated by outliers. IP due diligence failures that kill deals most often involve broken chain of title (solvable with standard assignment hygiene), absent FTO opinions (solvable with qualified IP counsel), and undisclosed prosecution history limitations (solvable with transparent portfolio review). Companies that proactively address all four areas before a process begins close transactions faster and at better terms.
Investment Strategy
For institutional investors and strategic acquirers, a rapid FTO screen and prosecution history review on target company patents before entering a formal data room provides significant negotiating leverage. Patent counsel with pharmaceutical prosecution experience can complete a preliminary risk assessment on a three-to-five patent estate in under two weeks. This pre-data-room intelligence often identifies leverage points — or genuine show-stoppers — that can be used to structure a lower initial valuation with milestone-contingent payments tied to successful IPR challenge defense.
Issue 3: The $400 Billion Patent Cliff — How Keytruda, Eliquis, and Opdivo Are Reshaping the Entire Competitive Landscape
The Scale of the Revenue Exposure and Why Biosimilars Amplify It
Between 2025 and 2033, the pharmaceutical industry faces loss-of-exclusivity events on a scale without historical precedent. The headline figure — over $400 billion in aggregate revenue exposure — encompasses some of the highest-grossing drugs in history.
Merck’s pembrolizumab (Keytruda), the world’s best-selling drug, had 2024 revenues of approximately $25 billion. Its core formulation patents begin expiring in 2028, with U.S. composition-of-matter protection running to 2028 on the antibody itself and method-of-use patents on its PD-1 checkpoint inhibitor mechanism extending into the early 2030s. The Keytruda patent estate is substantial, but no patent fortress is impenetrable at scale.
Bristol-Myers Squibb’s apixaban (Eliquis), a Factor Xa inhibitor co-marketed with Pfizer, generated approximately $12 billion in 2024 U.S. revenue. Its core patents expired in 2023, but a combination of patent litigation settlements and regulatory exclusivity pushed generic entry into late 2026 and early 2027. Eliquis is the canonical example of the composite shield in action: multiple generic challengers filed Paragraph IV certifications, BMS and Pfizer litigated, and the resulting settlement agreements structured staggered entry dates that preserved branded revenue well past the initial patent expiry.
Bristol-Myers Squibb’s nivolumab (Opdivo), another PD-1 checkpoint inhibitor, faces biosimilar entry pressure from multiple manufacturers who have filed 351(k) applications with the FDA. The 12-year biologic data exclusivity under the BPCIA ran from Opdivo’s 2014 approval, placing the data exclusivity window through 2026. Post-exclusivity, the biosimilar entry timeline depends on patent litigation resolved through the BPCIA’s ‘patent dance’ mechanism — a structured, mandatory exchange of patent and biosimilar product information between the reference product sponsor and the biosimilar applicant.
For branded biologics, the revenue loss trajectory after biosimilar entry is structurally different from small-molecule generic entry. For small molecules, first-generic entry under 30-month stay litigation resolution can erase 80-90% of branded revenue within 12-18 months. For biologics, the erosion is slower but still severe — 30-70% first-year revenue loss is the current market expectation in the U.S., driven by the slower adoption curve for biosimilars among prescribing physicians and payers compared to generic substitution.
The BPCIA ‘Patent Dance’: How Reference Product Sponsors Use It Strategically
The BPCIA’s patent resolution mechanism — the ‘patent dance’ — is a procedural tool that reference product sponsors (the innovator biologic company) can use strategically to extend litigation timelines and delay biosimilar entry beyond the 12-year data exclusivity window.
The dance begins when a biosimilar applicant (the ‘subsection (k) applicant’) submits its 351(k) application to the FDA and, within 20 days, provides the reference product sponsor with a copy of the application and all information describing the manufacturing process. The reference product sponsor then has 60 days to identify patents it believes would be infringed and propose a list for immediate litigation. This exchange goes through multiple rounds before the parties agree on a litigation list and the biosimilar applicant can file its Paragraph IV-equivalent patent infringement declaratory judgment.
The Amgen v. Sandoz litigation, resolved by the U.S. Supreme Court in 2017 (Amgen Inc. v. Sandoz Inc., 137 S. Ct. 1664), clarified that the information exchange steps are not mandatory but that failure to complete them has consequences — the reference product sponsor retains the right to bring a separate infringement action. This ruling gave reference product sponsors a strategic choice: engage the dance and control the litigation list, or wait and sue later with a broader patent list. Most major reference product sponsors engage the dance precisely because it gives them control over which patents go to immediate litigation.
For biosimilar applicants, the dance creates a timing problem: the dance itself consumes months of calendar time, and the 42-day notice requirement before commercial launch (after court resolution or consent) gives reference product sponsors an additional window to seek preliminary injunctions. AstraZeneca used this mechanism aggressively to delay biosimilar entry for its biologic assets, filing for preliminary injunctions based on later-identified manufacturing process patents not included in the original dance exchange.
Lifecycle Management: The Complete IP Architecture
Pharmaceutical lifecycle management is not a single tactic. It is a multi-layer IP architecture built across R&D, regulatory, and commercial functions, executed over the 10-15 year commercial life of a drug.
The composition of matter (CoM) patent — the original patent on the molecule or biologic — is the foundation. Its primary value is the breadth of its claims: it covers the molecule in all uses and all forms, regardless of what was known at filing. But it expires on the earliest possible date in the composite shield timeline, because it was filed first. Every LCM strategy starts from the question: ‘what new, patentable innovations can we generate before this patent expires?’
New indication development is the highest-value LCM play. A Phase II clinical trial proving a drug’s efficacy in a second tumor type, a second inflammatory indication, or a second neurological condition generates both a new method-of-use patent (protecting the specific use claim) and, upon FDA approval of a supplemental NDA (sNDA), a new three-year period of New Clinical Investigation Exclusivity for that specific change. That exclusivity is narrower than NCE exclusivity — it only blocks FDA approval of a generic for the specific approved change — but combined with a new method-of-use patent, it creates meaningful protection for the expanded indication.
Formulation development is the second major LCM pathway. Switching from IV to subcutaneous administration typically requires substantial formulation engineering work: new excipients, new concentration range, new viscosity profile, new stability package. Each of those innovations can generate independent patent claims. More importantly, a successful IV-to-sub-Q switch gives the commercial team a clear rationale for ‘patient switching’ — migrating existing IV patients to the new formulation before generic IV competition begins. The sub-Q formulation has its own patent life clock, its own regulatory exclusivity, and a protected commercial position even after the original IV formulation goes generic.
AbbVie executed this strategy with extraordinary precision on adalimumab (Humira). The original Humira CoM patents began expiring in 2016. AbbVie filed hundreds of patents on formulations, concentrations, dosing schedules, and manufacturing processes, creating the most-cited example of a ‘Patent Fortress’ in pharmaceutical history. The FDA approved Hyrimoz, Cyltezo, Hadlima, and multiple other adalimumab biosimilars beginning in 2018, but U.S. commercial launch was blocked by patent litigation settlement agreements until January 2023 — a commercial protection period that extended Humira’s U.S. exclusivity by approximately six additional years and generated roughly $100 billion in cumulative U.S. revenue between original patent expiry and first biosimilar commercial entry.
Authorized generic launches represent a separate LCM tool. An innovator can elect to launch its own ‘authorized generic’ — produced from the branded drug’s approved NDA — simultaneously with or shortly after first generic entry. Authorized generics do not require a new NDA; they are covered by the original approval. They allow the innovator to participate in the lower-priced generic market, maintain manufacturing scale, and erode the exclusivity value of the first generic filer (who, under Hatch-Waxman, typically receives 180 days of generic exclusivity). BMS used authorized generic launches effectively on several small-molecule assets to compress first-generic market share during the exclusivity period.
Debunking ‘Patent Thickets’: What the Data Actually Shows
The political and media characterization of LCM strategies as ‘patent evergreening’ or ‘patent thickets’ is widespread and requires a direct, data-grounded response for any executive who will face this narrative in a stakeholder or policy context.
The core empirical claim in the ‘thicket’ argument is that more patents on a drug product translate to longer market exclusivity. A 2024 USPTO study focused specifically on Orange Book-listed patents — the patents that a drug company registers as directly relevant to a branded product — found no correlation between the number of Orange Book patents and the actual length of market exclusivity. This is not a peripheral finding. It directly refutes the central claim of the ‘thicket’ narrative.
The second empirical point is that follow-on pharmaceutical patents are not ‘junk.’ To receive a patent grant, each application must independently satisfy the USPTO’s requirements for novelty (35 U.S.C. § 102), non-obviousness (35 U.S.C. § 103), and enablement/written description (35 U.S.C. § 112). A patent on a new crystalline polymorph of a drug molecule is not ‘junk’ — it represents a genuine discovery about the molecule’s solid-state chemistry, which has real implications for manufacturing stability, bioavailability, and shelf life. A patent on a new subcutaneous formulation is not ‘junk’ — it required substantial scientific work to achieve therapeutic equivalence with a different dosage form.
The third point is definitional. ‘Evergreening’ implies an extension of the original patent, which is legally impossible. The original CoM patent expires on its scheduled date. At that point, generic manufacturers are legally free to copy and sell the original formulation of the drug. The follow-on patents only protect their specific innovations. A generic of the original IV formulation competes freely after the CoM expiry. Only the new sub-Q formulation — which required real R&D to develop — retains independent patent protection.
In technology sectors with analogous complexity, far higher patent volumes per product are the norm. The 2023 USPTO data showed biopharma comprising approximately 2% of top U.S. patentees, compared to nearly one-third from technology. The narrative that pharmaceutical companies file uniquely aggressive volumes of follow-on patents does not survive comparison to adjacent industries.
Key Takeaways — Issue 3
The $400 billion patent cliff is the single largest driver of large-cap pharma M&A through 2030. Keytruda, Eliquis, and Opdivo collectively represent over $45 billion in annual revenue at immediate LOE risk. For biosimilars specifically, the BPCIA patent dance is a strategic tool, not merely a procedural requirement — reference product sponsors who engage it proactively control the litigation list and timing. AbbVie’s Humira strategy remains the definitive case study in lifecycle management, having extended effective U.S. commercial exclusivity by approximately six years through a multi-layer patent fortress that no single strategy alone could have achieved.
Investment Strategy
The patent cliff creates a predictable, data-driven M&A acquisition cycle. The most attractive acquisition targets for cash-rich pharma companies facing LOE events are late-stage assets (Phase III or NDA-filed) in adjacent therapeutic areas that can be plugged into existing commercial infrastructure. The deal rationale is revenue replacement, not pipeline building, which means acquirers will pay premium multiples for de-risked assets with clean IP estates and short timelines to revenue. For biotech companies with Phase III assets in oncology, immunology, or rare disease, the 2026-2029 window is structurally the best environment for M&A exits since the post-pandemic biotech boom of 2020-2021.
Issue 4: AI Drug Discovery and CRISPR — The IP Chaos That Needs Immediate Legal Attention
The CRISPR Patent War: Discovery vs. Invention in Federal Court
The dispute over foundational CRISPR-Cas9 patents is now a decade-long case study in the most consequential distinction in patent law: the difference between discovery and invention.
The CVC group — University of California-Berkeley, the University of Vienna, and Emmanuelle Charpentier — identified CRISPR-Cas9 as a programmable molecular scissor and demonstrated its function in biochemical (cell-free) systems. Their work, published in the 2012 Doudna-Charpentier paper in Science, established the mechanism. The 2020 Nobel Prize in Chemistry recognized this discovery.
The Broad Institute — MIT, Harvard, and Feng Zhang — filed patent applications, including the now-central U.S. 8,697,359, demonstrating for the first time that CRISPR-Cas9 could be delivered and functionally expressed inside eukaryotic cells: the complex cells that comprise animals, plants, and humans. This is the commercially critical jump. A molecular tool that works only in a test tube has limited therapeutic value. A tool that functions inside living human cells is the foundation of an entire therapeutic modality.
The U.S. Patent Trial and Appeal Board (PTAB) and the Federal Circuit, in a series of proceedings from 2017 through 2022, consistently ruled that Broad’s eukaryotic application was patentably distinct from CVC’s cell-free demonstration. The legal standard applied was ‘reasonable expectation of success’ — whether a person of ordinary skill would have expected CVC’s biochemical system to function in a eukaryotic environment without further inventive work. The courts found they would not. That finding, which many in the scientific community disputed, determined the ownership of patents underlying a $10+ billion therapeutic industry.
The commercial consequence: Broad Institute licensees — including Editas Medicine, Beam Therapeutics, and Prime Medicine — hold rights to the therapeutically critical eukaryotic application patents. CVC licensees — including Intellia Therapeutics and CRISPR Therapeutics — hold rights to the biochemical mechanism patents. Cross-licensing between these camps is ongoing and complex, and the full patent landscape for any CRISPR therapeutic program now requires a multi-party FTO analysis across both estates.
For R&D teams outside this litigation: the CRISPR story teaches that the commercially valuable patent is not the one on the discovery. It is the one on the first enabling application of that discovery in a therapeutically relevant context.
AI Inventorship: The Legal Vacuum Threatening an Entire Business Model
Artificial intelligence platforms now participate meaningfully in drug discovery at multiple stages: target identification and validation, de novo molecular design, ADMET property prediction, synthetic route planning, and clinical trial design optimization. Companies including Exscientia, Recursion Pharmaceuticals, Insilico Medicine, and Evotec have advanced AI-designed drug candidates into human clinical trials. By 2025, the FDA has received IND applications for compounds where AI contributed substantially to molecular design.
This creates an immediate legal problem. Under settled U.S. law — confirmed by the Federal Circuit in Thaler v. Vidal (43 F.4th 1207, Fed. Cir. 2022) — an inventor must be a natural person. The court was unambiguous: ‘we hold that “inventors” as used in the Patent Act must be human beings.’ The USPTO’s February 2024 Inventorship Guidance for AI-Assisted Inventions formalized the analytical framework: AI output is not inventive contribution, but a human who makes a ‘significant contribution’ to the conception of an AI-assisted invention can qualify as an inventor.
The legal line runs through ‘conception,’ the classic patent law standard for inventorship. Conception is ‘the formation in the mind of the inventor of a definite and permanent idea of the complete and operative invention.’ For a drug discovered through AI, the question is: at what point did a human scientist form that ‘definite and permanent idea’ — and what specifically was their contribution?
The USPTO Guidance identifies multiple ways human scientists can make significant contributions in AI-assisted discovery contexts. Designing and training a specialized AI model to solve a specific, non-obvious drug design problem can constitute inventive contribution, particularly if the model architecture itself embodies novel scientific insights. Providing a complex, scientifically specific prompt that meaningfully constrains the AI’s output — a prompt that required expertise and judgment, not merely instruction — may constitute contribution depending on the specificity and scientific content of the guidance. Selecting a specific lead candidate from AI-generated output, based on independent scientific analysis and judgment, can be an inventive act when the selection itself required non-obvious insight. Materially modifying an AI-generated molecular structure through wet lab work — improving binding affinity in vivo, reducing toxicity, enhancing bioavailability — almost certainly constitutes significant contribution because the modification requires original scientific work.
What the Guidance expressly excludes: merely recognizing that an AI tool might solve a class of problems, owning or operating the AI platform without contributing to specific outputs, and post-hoc selection of candidates without documented scientific judgment.
The Human-in-the-Loop R&D Protocol: A Legal Necessity
For any company whose drug discovery pipeline relies substantially on AI platforms, the immediate operational priority is redesigning R&D documentation protocols to capture human inventive contribution in real time. This is not a retrospective legal exercise. Retroactive documentation of ‘what the scientist was thinking’ is nearly worthless in litigation and will not survive challenge in an IPR or district court validity proceeding.
The protocol requires four structural changes to standard R&D operating procedures.
Contemporaneous AI interaction logs must capture every material human input to the AI discovery process: model architecture decisions, training data design choices, prompt engineering, parameter selection, and the scientific rationale behind each. These logs must be timestamped, attributed to specific named scientists, and maintained with the same rigor as a laboratory notebook. They become the primary inventorship documentation.
Lead candidate selection must be documented with explicit scientific reasoning. When a scientist reviews 500 AI-generated molecules and selects ten for further development, the selection criteria — binding affinity thresholds, predicted ADMET profiles, synthetic accessibility scores, structural novelty considerations — must be recorded. The scientist must articulate why their selection required non-obvious scientific judgment, not just rule application.
Wet-lab modification records must link AI-generated structures to human-designed analogs with explicit documentation of what was changed, why, and what scientific insight drove the modification. A medicinal chemist who takes an AI-generated scaffold and adds a fluorine substituent to improve metabolic stability has made a potentially significant inventive contribution — but only if the reasoning for that specific modification is documented at the time it was made.
IP counsel must be embedded in the AI discovery workflow, not consulted after a candidate is selected. The inventorship determination cannot wait until an IND is filed. By that point, the documentation that would support a strong inventorship argument may no longer exist.
Key Takeaways — Issue 4
The Broad Institute’s CRISPR victory established that the commercially valuable patent is the first enabling application in a therapeutically relevant system — not the underlying discovery. Any R&D team entering a CRISPR program now needs a multi-estate FTO spanning both Broad and CVC patent families. For AI drug discovery, Thaler v. Vidal and the February 2024 USPTO Inventorship Guidance create a clear legal standard: human inventive contribution requires ‘significant contribution to conception,’ and that contribution must be documented contemporaneously. Companies that do not embed IP counsel in their AI discovery workflow are building pipelines on legally fragile foundations.
Investment Strategy
Before committing capital to an AI-first drug discovery company, due diligence must include a specific review of the company’s inventorship documentation protocols. Ask to see a sample AI interaction log from a current program. Ask how the company distinguishes ‘inventive prompting’ from ‘operational prompting’ in its recordkeeping. Ask when IP counsel is first consulted in the discovery workflow. A company that cannot answer these questions precisely has a systemic IP validity risk across its entire pipeline — a risk that is material, not theoretical, given the current state of the law.
Issue 5: Digital and Physical IP Security — The Open Doors in Your Infrastructure
Cybersecurity as an IP Protection Function, Not Just a Compliance Function
Most biotech security programs are organized around HIPAA compliance and the protection of patient health information (PHI). This is the wrong primary frame for an industry where the most valuable assets are digital representations of drug discovery data — preclinical packages, clinical trial results, manufacturing process documentation, and patent filing strategies.
The 2025 Biotech Cybersecurity Report from Sekurno, which reviewed 50 biotech platforms across the U.S., provides the most granular current picture of this exposure. The findings are not about sophisticated nation-state intrusion techniques. They are about basic infrastructure failures that create open access. Thirty-six percent of the reviewed platforms had leaked credentials — employee or system account credentials discoverable through public breach databases or dark web sources. Thirty-four percent had insecure APIs — application programming interfaces exposing backend data without proper authentication or authorization controls. Twenty percent had misconfigured cloud environments — storage buckets, database instances, or compute resources accessible to unauthenticated external parties. Over fifty percent had system information leaks — server configurations, software versions, or infrastructure details visible in HTTP response headers or error messages, providing attackers with reconnaissance data.
None of these vulnerabilities require a sophisticated attacker. They require only an attacker who knows how to use freely available scanning tools. The HaveIBeenPwned database, Shodan, and similar public tools will identify most of these exposures in hours.
The consequence of a successful compromise is not primarily a regulatory fine under HIPAA or GDPR, though those are real. The primary consequence is competitive: if a threat actor — nation-state, commercial competitor, or IP theft-focused criminal group — exfiltrates a company’s preclinical data package for a Phase I candidate, that actor can use the data to accelerate their own program, potentially filing a competing patent application before the victimized company files its own, or identifying and targeting specific regulatory weaknesses before the IND is submitted. The average U.S. healthcare data breach cost of $10.22 million is economically trivial compared to the potential loss of a $700 million R&D investment.
API Security as a Literal Drug Supply Problem
The other ‘API’ at risk is the active pharmaceutical ingredient supply chain. The U.S. pharmaceutical industry relies on a geographically concentrated API manufacturing base — predominantly India and China — that is now subject to significant geopolitical and trade policy disruption.
The 2025 tariff environment has restructured the economic calculus for API sourcing. A PwC analysis of pharma executive surveys found that 89% of industry leaders planned changes to supply chain strategy in direct response to U.S. trade policy shifts. For companies sourcing APIs from Chinese manufacturers subject to escalating tariffs, the cost impact is immediate and compounds with each tariff tier escalation.
The IP dimension of this supply chain problem is underappreciated. Many API manufacturing processes are proprietary — covered by process patents, protected as trade secrets, or both. A single-source API manufacturer in a jurisdiction with weak IP enforcement or adversarial geopolitical alignment creates a specific risk: that manufacturer has access to the company’s proprietary synthesis route, formulation chemistry, and quality control specifications. That information is the equivalent of the crown jewel IP in digital form, stored not on the company’s secured servers but on a third-party facility’s systems.
Supply chain risk mitigation for pharma — dual sourcing, near-shoring, qualified supplier diversification — is therefore simultaneously an IP protection strategy. Moving API manufacturing to a qualified supplier in a jurisdiction with strong IP law enforcement (EU, Japan, domestic U.S.) reduces both supply disruption risk and trade secret misappropriation risk.
Key Takeaways — Issue 5
The biotech industry’s cybersecurity posture is structurally insufficient for its IP risk profile. Leaked credentials, insecure APIs, and misconfigured cloud environments — discovered through basic scanning in 50 reviewed companies — represent open access to the industry’s most valuable assets. The primary risk is not regulatory: it is competitive IP theft that can invalidate a patent by enabling a competitor to file first. API supply chain concentration in China and India simultaneously creates supply disruption risk and IP theft risk, because sole-source manufacturers hold proprietary process information. Supply chain diversification and cybersecurity hardening are the same strategic imperative viewed from different angles.
Issue 6: The Competitive Battlefield — Where All Five Threats Converge
The sixth and final structural challenge — competitive intensity — is the convergence point for every issue described above. Competition in 2026 does not come primarily from the company with a structurally similar molecule in Phase III. It comes from the entire competitive intelligence and IP landscape operating simultaneously.
A competitor who masters the regulatory maze generates jurisdiction-specific IP that creates blocking positions in markets where the originator has not yet filed. A competitor who perfects its capital raise with superior IP documentation closes financing that the originator loses. A competitor who executes M&A with disciplined patent due diligence acquires the assets needed to fill its LOE gap before a rival can. A competitor who redesigns its AI discovery R&D protocols to legally secure human inventorship builds a pipeline that is patentable, while the originator’s AI-generated candidates remain in a legal gray zone. A competitor — or nation-state actor — who exploits an insecure API or leaked credentials acquires years of competitive intelligence without conducting any R&D.
In this environment, the company with the best science does not necessarily win. The company with the best intelligence infrastructure does. That infrastructure requires continuous situational awareness across patent data, regulatory exclusivity data, clinical trial data, competitor pipeline data, and cybersecurity monitoring — integrated in a single, queryable system.
The core operational challenge is data quality. Raw patent data is, in the language of the practitioners who work with it daily, ‘notoriously messy.’ Misspellings in assignee names, outdated ownership records that have not tracked M&A activity, machine-translated claims from foreign-language applications, and inconsistent international classification codes make raw database access unreliable for high-stakes decisions. A patent filed by a startup that was subsequently acquired by a mid-size biotech that was then merged into a large pharmaceutical company may still be indexed under the startup’s original name — invisible to any competitor running a standard assignee search for the large pharma.
The value of professional pharmaceutical intelligence platforms — including DrugPatentWatch, Cortellis, Evaluate Omnium, and Citeline — is not data access, which is available for free through USPTO, WIPO, and EPO systems. The value is curation (systematic cleaning and correction of the underlying data, including M&A-based ownership tracking) and integration (merging patent data with regulatory exclusivity data and clinical trial data into a single unified interface). Curated and integrated data, according to practitioners who have quantified the labor impact, saves internal teams more than two working years annually that would otherwise go to manual data cleaning and cross-referencing.
The ROI of that investment is calculable across three dimensions.
An FTO analysis that stops a company from committing $150 million to a program blocked by a competitor’s in-force patent delivers a return orders of magnitude higher than the cost of the analysis. This is loss prevention, and it is the most direct ROI case for pharmaceutical intelligence.
A patent landscape analysis that identifies a credible, uncrowded ‘white space’ — a therapeutic target, a molecular class, or a delivery mechanism with significant clinical potential and limited patent activity — is the foundation for a future billion-dollar program. This is offensive ROI, measured in the pipeline value created by directing R&D toward commercially defensible ground.
Patent due diligence in an M&A context that identifies a fatal validity flaw or an FTO-blocking third-party patent — and supports a $300-500 million reduction in acquisition price — delivers a return that can fund the entire intelligence function for a decade. This is transactional ROI, measured in purchase price saved on a single deal.
Key Takeaways — Issue 6
Competitive advantage in 2026 derives from intelligence quality, not scientific quality alone. The six structural challenges described in this analysis are not independent threats — they are interconnected pressure points where the same integrated patent and regulatory intelligence infrastructure provides the primary response. ‘Dirty’ patent data is a multi-million-dollar business risk, not a minor inconvenience, because incorrect ownership records or missed blocking patents translate directly to flawed R&D investment and M&A valuation decisions. Professional intelligence platforms are cost-justified on loss prevention alone before the offensive and transactional ROI is counted.
The Full IP Playbook: Integrated Execution Across R&D, BD, and the C-Suite
Patent Landscape Analysis as R&D Infrastructure
Patent Landscape Analysis (PLA) is systematic, structured analysis of patent databases to map the IP topology of a technology field. It is not a one-time deliverable. For pharmaceutical and biotech R&D, it is ongoing infrastructure — as fundamental to the research process as the laboratory information management system (LIMS).
The four outputs of a PLA — white space identification, competitor technology tracking, trend detection, and litigation minefield mapping — each directly inform R&D resource allocation decisions that collectively determine whether a $700 million development investment ends in approval and revenue or in litigation and write-off.
White space identification is the primary offensive value. A well-executed PLA maps not just where current patent activity is concentrated, but where it is absent. A therapeutic target with strong preclinical validation and limited patent coverage is the pharmaceutical equivalent of a strategic acquisition before the market prices in the value. R&D teams that use PLA to identify these uncrowded areas systematically build pipelines with higher expected commercial exclusivity and lower expected litigation cost.
Competitor technology tracking through PLA is near-real-time competitive intelligence. Patent applications publish 18 months after filing. A company that monitors competitor patent filings in its therapeutic area will learn about new molecular modalities, new formulation approaches, and new combination therapy strategies 18 months before they appear in a press release, a publication, or a conference presentation. This lead time is strategically material.
Emerging technology convergence is detectable through PLA before it becomes visible in clinical or commercial data. The convergence of antibody engineering with oligonucleotide chemistry — the foundation of antibody-oligonucleotide conjugates (AOCs) — was visible in the patent literature two to three years before AOC programs entered broad clinical discussion. Companies that track patent filing trends across adjacent technology areas get that two-to-three-year window to build their own positions or identify acquisition targets.
Minefield mapping prevents the most catastrophic form of R&D waste: investing $50-150 million in IND-enabling studies and early Phase I for a program that is blocked by a competitor’s in-force patent on a critical method of use. A PLA conducted before IND-enabling studies begin costs a fraction of one week of clinical trial operations. An FTO opinion based on that PLA costs a fraction of one day of Phase III operations. The cost-risk math for conducting these analyses early is so favorable that their absence in an R&D program represents not strategic judgment but systematic negligence.
Biologic and CGT FTO: A Platform-First Analysis
Freedom-to-Operate analysis for a small-molecule drug is (relatively) tractable: clear the molecule, its synthesis, its formulation, and its method of use across the major commercial jurisdictions. For a biologic — a monoclonal antibody, an antibody-drug conjugate, a cell therapy, a gene therapy — the FTO scope is fundamentally different because the ‘product’ is inseparable from its manufacturing and delivery platform.
A CAR-T cell therapy program, for example, requires FTO clearance across at minimum six distinct patent domains: the CAR construct itself (antigen binding domain, hinge, transmembrane domain, costimulatory domain, signaling domain), the T cell activation and expansion protocol, the viral vector used for construct delivery (lentiviral, gammaretroviral, or non-viral), the specific vector manufacturing cell line if proprietary, the cryopreservation and formulation technology for the final product, and any conditioning regimen or combination therapy required for clinical efficacy.
Kymriah (tisagenlecleucel), developed by the University of Pennsylvania and commercialized by Novartis, and Yescarta (axicabtagene ciloleucel), developed by Kite Pharma (acquired by Gilead), have overlapping patent estates that cover multiple domains in the CAR-T manufacturing and delivery space. New entrants into CAR-T must conduct FTO analysis across both estates, plus the foundational CAR construct patents held by St. Jude Children’s Research Hospital (licensed by multiple parties), plus vector patents held by entities including Oxford Biomedica and Lentigen Technology.
A new CAR-T program that selects its vector, cell line, and cryopreservation technology before conducting this FTO analysis — choosing platform components based on scientific performance alone — risks building an entire program on a foundation that requires licensing at terms the IP holder can dictate, or that is blocked entirely.
The practical implication: biologic and CGT FTO analysis is a platform selection input, not a program clearance step. It must happen before the manufacturing platform is chosen, not after the clinical product design is locked.
M&A Patent Due Diligence: The Three-Phase Playbook
For BD teams executing pharmaceutical M&A, patent due diligence is the primary financial valuation tool, not a supporting legal function. The IP estate is the asset being acquired. The lab equipment, the real estate, and the headcount are incidental.
Phase one — the pre-data-room assessment — uses publicly available patent databases and commercial intelligence platforms to build a foundational IP inventory on the target before entering the formal data room process. This assessment maps all patents assigned to the target, all pending applications, the legal status of each (granted, published, pending, abandoned), the expiry dates of granted patents, the geographic coverage across key commercial jurisdictions, and the corporate family tree to catch patents assigned to subsidiaries or predecessor entities. A pre-data-room assessment typically takes two to four weeks with experienced patent counsel and a good data platform. Its value is in giving the acquirer a baseline against which to measure the disclosures made in the data room, and in identifying questions to prioritize before the formal process begins.
Phase two — the in-data-room deep dive — requires a genuinely cross-functional team. Patent counsel reviews claim scope, prosecution history, and chain of title. R&D scientists assess technical validity: does the claimed invention work as described? Are the disclosed examples reproducible? Is there ‘hidden prior art’ that the company’s own internal scientists know about but has not been published? BD and finance translate legal and technical findings into financial model inputs: probability of challenge success, expected litigation timeline and cost, impact of a validity finding on revenue projections across different scenarios.
Phase three — risk quantification and valuation adjustment — converts all findings into a structured, scenario-based financial model. The base case uses the most likely IP outcome: patents valid, no blocking FTO issues, clear chain of title. The downside scenario incorporates the probability-weighted cost of identified risks: a 40% probability that a key patent is challenged through IPR and invalidated, translated into expected revenue impact and modeled across years three through seven of the deal. The upside scenario captures optionality: additional unpatented innovations or trade secrets that are not yet in the patent estate but represent future patentable value.
This three-scenario model is what gives a BD executive the quantitative basis for a negotiated price adjustment: ‘Our base-case valuation is $1.8 billion. Our diligence has identified a 35% probability of invalidation on your primary method-of-use patent, which accounts for 60% of the projected revenue in years four through seven. Our risk-adjusted valuation is $1.4 billion, and this 120-page legal and technical report is the basis.’
Key Takeaways — Full Playbook
Patent Landscape Analysis is R&D infrastructure, not a one-time legal deliverable. It must run continuously to track competitor technology, identify white space, and map litigation risk before programs commit capital to clinical development. FTO for biologics and CGTs must be conducted at the platform selection stage, covering vector, cell line, culture medium, and cryopreservation technology — not just the final product. M&A due diligence on pharmaceutical assets is fundamentally an IP valuation exercise. The three-phase playbook — pre-data-room assessment, cross-functional deep dive, risk-quantified valuation adjustment — gives acquirers the factual basis to negotiate price adjustments on specific, documented risks rather than arguing general ‘uncertainty.’
Frequently Asked Questions
What is the actual effective patent life of a pharmaceutical drug after approval?
For most drugs, seven to twelve years. The statutory patent term is twenty years from the application filing date, but given average development timelines of ten to fifteen years, the majority of the patent term is consumed before approval. Patent Term Extension under Hatch-Waxman (35 U.S.C. § 156) can add up to five years of term to compensate for FDA review time, but PTE is capped and subject to complex calculation rules. The effective patent life is also not the same as effective market exclusivity, because regulatory exclusivities under the FD&C Act and BPCIA may extend protection beyond the last patent expiry.
When should an FTO analysis be conducted for a biologic program?
Before platform selection. For a biologic or CGT program, the manufacturing and delivery platform — vector, cell line, culture medium, formulation technology — is covered by a separate and complex patent landscape from the therapeutic product itself. Selecting a platform based on scientific performance and then conducting FTO is the wrong sequence. The FTO must inform the platform selection, because choosing a patented platform without a clear licensing path creates a blocking IP problem that may be unsolvable without abandoning the program or paying licensing fees at terms the IP holder dictates.
How does the BPCIA ‘patent dance’ actually work in practice?
When a biosimilar applicant files a 351(k) application, it must provide the reference product sponsor with a copy of the application and manufacturing process information within 20 days of FDA acceptance. The reference product sponsor then identifies patents it believes would be infringed. The parties negotiate a list of patents for immediate litigation through a structured exchange. After the Federal Circuit’s Amgen v. Sandoz ruling, completing the dance is not strictly mandatory, but reference product sponsors who engage it gain control over the initial litigation list and force the biosimilar applicant into a defined procedural timeline. The 42-day notice requirement before commercial launch gives reference product sponsors a final window to seek preliminary injunctions.
Is a drug discovered primarily by an AI platform patentable?
Under current U.S. law, only if a human made a ‘significant contribution to conception’ — the standard set by Thaler v. Vidal (Fed. Cir. 2022) and operationalized by the USPTO’s February 2024 Inventorship Guidance. Significant contribution can include designing and training a specialized AI model to solve a specific drug design problem, providing scientifically complex and specific prompting that guided the AI’s output, selecting a lead candidate based on documented non-obvious scientific judgment, or materially modifying the AI-generated structure through wet-lab work. What does not qualify: general supervision of the AI platform, ownership of the platform without contribution to specific outputs, or post-hoc selection without documented scientific reasoning.
What is the difference between a patent and regulatory exclusivity, and why does it matter?
A patent is granted by the USPTO under the Patent Act and gives the holder the right to exclude others from the claimed invention. It expires on the patent’s term end date, regardless of commercial status. Regulatory exclusivity is granted by the FDA under the FD&C Act or BPCIA and blocks the FDA from approving a competitor’s abbreviated application for a defined period after the innovator’s approval. The two systems are independent: a patent can expire while a regulatory exclusivity remains in force, and vice versa. True loss-of-exclusivity modeling requires tracking both systems simultaneously to identify the latest date on which a generic or biosimilar can realistically enter the market.
Why does pharmaceutical patent data quality matter for business decisions?
Raw patent databases contain systematic errors: misspellings in assignee names, outdated ownership records that have not tracked M&A activity, and inconsistent international classifications. A patent filed by a startup that was subsequently acquired and merged into a large pharmaceutical company may still be indexed under the startup’s original name. An analyst who searches for a competitor’s patent estate and misses that patent because of an outdated ownership record has a materially incomplete picture of the competitive landscape. Professional intelligence platforms that curate data — correcting misspellings, tracking M&A to update ownership records, normalizing classification codes — eliminate this class of error. The cost of professional data is trivial compared to the cost of an M&A valuation or R&D investment decision made on incomplete data.
This analysis draws on publicly available data from the USPTO, FDA, PTAB, and federal court records, supplemented by published research from RAND, Deloitte, PwC, and Sekurno. All drug names, company names, litigation citations, and regulatory events referenced are real. No financial advice is expressed or implied. IP strategy decisions require qualified legal counsel.