Every year, the pharmaceutical industry discards hundreds of compounds with known safety profiles, established pharmacokinetics, and years of preclinical data. Drug repositioning is the discipline that turns those abandoned assets into approved drugs — faster, cheaper, and with a measurably higher probability of success than any new chemical entity (NCE) program. This guide covers the full stack: discovery methodology, IP architecture, regulatory pathway selection, competitive intelligence tools, market sizing, and the AI disruption reshaping who wins.
Section I: The Strategic Case — Why Repositioning Is Now Core R&D Strategy
1.1 Eroom’s Law and the Productivity Crisis That Made Repositioning Inevitable

The numbers are not ambiguous. Since the mid-1990s, the number of new drugs approved per billion US dollars of R&D spending has declined by roughly half every nine years — a trend identified by Jack Scannell and colleagues in 2012 and named Eroom’s Law (Moore’s Law inverted). The de novo discovery process now requires an average of 10 to 17 years and approximately $2.6 billion per approved NCE, a figure that accounts for the cost of failures across the entire portfolio, not just successful programs. Clinical attrition rates consistently exceed 90%. That means nine out of every ten programs that enter the clinic will fail to generate an approved drug.
The systemic causes of this failure rate are well-characterized: target validation errors, poor translational models, safety signals that appear only at scale in Phase III, and the persistent difficulty of demonstrating efficacy in complex, heterogeneous patient populations. None of these problems are easily solved by spending more on Phase I. They are structural features of a discovery paradigm built around testing new biology in human beings for the first time.
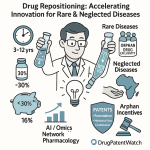
Drug repositioning attacks this problem by starting at a different point on the risk curve. A compound with approved or extensively tested human safety data is not a new hypothesis about human biology — it is de-risked infrastructure. The most failure-prone stage of development, Phase I safety testing, can be compressed or bypassed entirely. The average repositioning program takes 3 to 12 years to approval and costs approximately $300 million, roughly 85% less than the average NCE program. The probability of approval is reported at approximately 30%, against the 10% baseline for new drug applications. These figures are not marketing — they reflect the practical elimination of the single largest source of clinical failure, which is safety signals that arise in human subjects for the first time.
The strategic implication is clear. Repositioning has moved from an opportunistic tactic — something companies did when a lucky clinical observation fell into their lap — to a deliberate, systematic function that any serious pharmaceutical portfolio management operation should run continuously.
1.2 The ‘Valley of Death’ Is a Library, Not a Graveyard
The pharmaceutical industry’s abandoned compounds constitute one of the most underutilized asset classes in R&D. Compounds fail clinical trials for many reasons that have nothing to do with human toxicity: inadequate efficacy in a specific indication, a competitive landscape that shifted mid-program, a corporate merger that changed strategic priorities, or a negative result in a trial that was underpowered or enrolled the wrong patient population. Every one of these compounds has a safety file. Most have pharmacokinetic data. Many have formulation work, dose-escalation results, and biomarker studies.
This accumulated data has real dollar value. A compound that spent $150 million in preclinical and Phase I development before being shelved is not a write-off for the purposes of a repositioning program — it is a starting point. The new sponsor inherits the safety profile without paying for it. This reframing is what makes the economics of repositioning so attractive: the sunk costs of one program’s failure become the de-risking premium of another program’s success.
Large pharmaceutical companies have recognized this dynamic and increasingly use it as a mechanism for portfolio optimization, licensing shelved assets to smaller biotechs that have the focus and flexibility to pursue narrower indications. For the acquiring company, the transaction provides validated chemistry at a fraction of discovery cost. For the licensor, it generates milestone revenue from an asset that would otherwise generate nothing.
1.3 The Numbers in Context
| Metric | De Novo NCE | Drug Repositioning |
|---|---|---|
| Average Development Time | 10-17 years | 3-12 years |
| Average Development Cost | ~$2.6B (portfolio-adjusted) | ~$300M |
| Clinical Probability of Success | ~10% | ~30% |
| Primary Failure Mode | Efficacy and Safety | Efficacy |
| IP Anchor | Composition-of-Matter Patent | Secondary Patents + Regulatory Exclusivity |
| Primary Value Driver | Novelty | De-risked Development Efficiency |
Source: Compiled from published literature including Wouters et al. (JAMA, 2020), DiMasi et al., and Pushpakom et al. (Nature Reviews Drug Discovery, 2019)
Repurposed products account for an estimated 30% to 40% of all FDA-approved drugs and biologics in any given year, and a separate analysis found that 35% of drugs classified as ‘transformative’ by independent clinical reviewers were repurposed products. The category is not a niche. It is a substantial fraction of approved medicine.
Key Takeaways: Section I
The R&D productivity crisis created the conditions under which repositioning became economically rational. The specific mechanism is simple: safety attrition accounts for roughly 30% of all clinical failures. Repositioning eliminates most of that risk category by starting with compounds that have already been in humans. The average 85% cost reduction and threefold improvement in success rates both flow directly from that one structural advantage. For portfolio managers evaluating early-stage assets, the relevant comparison is not ‘repositioning versus blockbuster discovery’ but ‘repositioning versus the 90% failure rate of the alternative.’
Section II: Discovery Methodology — From Serendipity to Systems Biology
2.1 The Three Strategic Frameworks
Every repositioning program begins with a choice of starting point, and that choice shapes the entire downstream development strategy.
The disease-centric approach starts with an unmet medical need and screens a library of existing compounds against it. It accounts for over 60% of repositioning projects and is the dominant framework in rare and orphan disease programs, where the unmet need is clear and regulatory incentives are substantial. The practical advantage of this approach is that it aligns directly with payer logic: a drug that treats a disease with no approved therapy has a defined commercial destination from day one.
The drug-centric approach inverts the logic. It starts with a specific compound — typically one that is off-patent, nearing patent expiry, or was discontinued for non-safety reasons — and systematically screens it against disease models and target panels. This is the framework most commonly used in lifecycle management and in programs targeting polypharmacology, where a drug’s interactions with multiple biological targets are treated as assets rather than liabilities.
The target-centric approach links a disease to a specific, druggable molecular target and then searches existing drugs known to modulate that target. This can proceed in two directions: ‘on-target’ repositioning applies a drug’s known mechanism of action to a new disease that shares the same pathway, while ‘off-target’ repositioning exploits a previously unknown interaction with a different target. The latter is particularly powerful when combined with proteomic target identification techniques, as it can reveal mechanisms of action that were not understood even during the drug’s original development.
2.2 Computational Methods: The Engine of Modern Repositioning
The transformation of repositioning from opportunistic to systematic has been driven almost entirely by computational advances. In silico methods allow researchers to analyze datasets of a scale and complexity that wet-lab work alone cannot match, generating ranked hypotheses that experimental work then validates.
Network-based methods construct biological interaction graphs — nodes representing genes, proteins, diseases, and drugs; edges representing known relationships between them. By applying graph-based inference algorithms, including ‘guilt-by-association’ principles and graph neural networks (GNNs), these models predict novel drug-disease connections across the entire network. The sophistication of modern implementations extends to capturing the polarity and directionality of relationships: whether Protein A negatively regulates Pathway B, or whether Drug X activates Target Y, rather than treating all connections as equivalent.
Signature-based methods compare the transcriptional ‘fingerprint’ of a disease state — the pattern of gene expression that characterizes it — against a library of drug-induced transcriptional signatures. The conceptual logic is reversal: a drug that induces the opposite transcriptional pattern to a disease might normalize it. The Connectivity Map (CMap), developed at the Broad Institute and expanded into the LINCS program, is the primary public resource for this approach, with drug-induced expression profiles across multiple cell lines.
Molecular docking is a structure-based technique that simulates the physical interaction between a small molecule and a protein target’s three-dimensional binding site. It allows virtual screening of large compound libraries against disease-relevant targets to generate ranked lists of predicted binders. The limitation is that it requires a high-quality crystal structure or reliable computational model of the target protein — not always available, particularly for structurally complex disease targets.
Machine learning and deep learning methods integrate all of these data types simultaneously. Support vector machines (SVMs), random forests, and variational autoencoders have all been applied to drug-target interaction prediction, with the best-performing models trained on combinations of chemical structure, bioactivity data, gene expression, phenotypic information, and clinical side-effect profiles. The consistent finding across the literature is that multi-modal models outperform single-source approaches, because the signal for a novel drug-indication pair rarely exists cleanly in any one data type.
2.3 Experimental Validation: Phenotypic Screening and Target Deconvolution
Computational predictions require experimental confirmation before any development decision is made. The two main experimental paradigms — phenotypic screening and target-based assays — differ fundamentally in their epistemological assumptions.
Phenotypic screening tests compounds in biologically relevant disease models (cell lines, patient-derived organoids, whole organisms) and identifies those that produce a desired change in cell or organism behavior, without requiring prior knowledge of the molecular target. It is target-agnostic by design. The advantage is that it can identify drugs that work through novel mechanisms that no computational model would have predicted. The disadvantage is that the mechanism of action (MOA) remains unknown until target deconvolution work — proteomics, CRISPR screens, or chemical biology approaches — identifies the relevant target. That gap between phenotypic effect and mechanistic understanding has practical consequences for patent strategy, as discussed in Section III.
Target-based assays screen compounds against specific, pre-validated molecular targets in biochemical or cell-based formats. They provide mechanistic clarity from the outset and generate data that directly supports patent claims. Their limitation is that they can only find compounds that work through known mechanisms — they cannot discover entirely new biology.
High-throughput screening (HTS) is the enabling technology for both approaches. Automation, robotics, and miniaturized assay formats allow hundreds of thousands of compounds to be tested per day, which is necessary for screening against large, structurally diverse compound libraries.
The most productive modern repositioning workflows combine both paradigms. A phenotypic screen identifies a compound-disease connection. Target deconvolution identifies the mechanism. That mechanistic understanding then enables structure-activity relationship (SAR) optimization, IP protection, and predictive toxicology work. This sequence — functional observation first, mechanistic understanding second — has produced some of the most valuable repositioning programs in recent years, precisely because the initial hit could not have been predicted from first principles.
2.4 Real-World Data as a Discovery Engine
Electronic health records (EHRs) and insurance claims databases now contain longitudinal health data for tens of millions of patients. Applied to drug repositioning, these datasets allow researchers to conduct large-scale observational analyses that function as natural experiments: comparing the disease outcomes of patients who happened to take Drug X for one indication against matched patients who did not, looking for statistically significant differences in the incidence or progression of other diseases.
This approach is not hypothesis-free. Confounding is a genuine analytical challenge — patients who take a specific drug often differ systematically from those who do not, in ways that correlate with disease risk. Sophisticated causal inference methods, including propensity score matching, instrumental variable analysis, and target trial emulation frameworks, are required to produce interpretable results from observational data. When applied rigorously, however, RWD analysis can effectively emulate hundreds of randomized trials simultaneously, providing a population-scale signal that is both generative (identifying new hypotheses) and validating (confirming signals from other methods).
The FDA has formally incorporated real-world evidence (RWE) into its evidentiary standards through the 21st Century Cures Act, opening a regulatory pathway for using RWD to support new indication applications in specific circumstances. This regulatory shift has increased the commercial value of RWD analysis by creating a route from observational finding to regulatory approval that does not require a full Phase III program in every case.
Key Takeaways: Section II
Modern repositioning discovery is a multi-layer process. Computational methods — network analysis, signature reversal, molecular docking, multi-modal ML — generate ranked hypotheses at scale. Experimental methods validate and mechanistically characterize the most promising ones. Real-world data provides both population-scale signals and, increasingly, regulatory-grade evidence. No single method dominates. Programs that integrate all three layers consistently outperform those that rely on any one approach.
Section III: IP Architecture — Building a Defensible Moat Without a Composition-of-Matter Patent
3.1 The Core IP Problem: Novelty Without Chemistry
The fundamental IP challenge of drug repositioning is structural. The active pharmaceutical ingredient (API) is already known. Composition-of-matter protection — the strongest form of pharmaceutical IP, covering the molecule itself regardless of use — is unavailable because the compound lacks novelty. Any patent must rest on something genuinely new: the new therapeutic use, the new formulation, the new dosing regimen, or the new combination. Each of these secondary patent categories provides a different level of protection and faces a different set of prosecution hurdles.
Understanding the hierarchy of protection strength is not an academic exercise — it directly determines whether a repositioning program can generate returns sufficient to justify the clinical investment. A program protected only by a method-of-use patent that covers a single indication faces systematic risk of generic erosion through the ‘skinny label’ mechanism. A program that generates a new patented formulation creates a physically distinct product that generics cannot automatically substitute. The IP strategy decision is, in practice, a commercial strategy decision.
3.2 Method-of-Use Patents: Necessary But Insufficient
A method-of-use (or method-of-treatment) patent protects the specific therapeutic application of a known drug. For the thalidomide example, the claim is structured as: ‘A method of treating multiple myeloma comprising administering a therapeutically effective amount of thalidomide to a patient in need thereof.’ These patents are the foundational IP tool for any repositioned drug and are relatively straightforward to prosecute when the indication is clearly distinct from prior uses.
The prosecution challenge is non-obviousness. Patent examiners will frequently argue that using a drug with known anti-inflammatory properties to treat another inflammatory condition is obvious to a person having ordinary skill in the art (PHOSITA). The most reliable rebuttal is ‘unexpected results’ — data showing that the drug worked at a dose, in a patient population, or with an effect magnitude that could not have been predicted from existing knowledge. This means the development program must be designed with prosecution strategy in mind: dose-response data, biomarker correlations, and mechanistic studies that document genuine surprise are not just scientifically interesting, they are legally necessary.
The commercial limitation of method-of-use patents is the skinny label. A generic manufacturer can launch a copy of the off-patent drug with a product label that simply omits the patented indication — what regulatory practitioners call ‘carving out’ the protected use. Because pharmacists can substitute any therapeutically equivalent generic for a branded product regardless of the indication for which it was prescribed, the innovator who funded the new indication can see their market eroded by off-label dispensing of the cheaper generic. Courts have addressed this inconsistently; the Hatch-Waxman framework does not provide a clean mechanism for preventing it.
3.3 Formulation Patents: The Strongest Secondary IP
A new formulation tailored to the new indication is the most commercially robust form of IP protection available to a repositioning program. The logic is mechanical: a new extended-release tablet, a new transdermal patch, a new long-acting injectable, or a new nanoparticle formulation is a physically distinct product. A generic manufacturer cannot substitute the original oral tablet for a transdermal patch. Automatic substitution is impossible. The innovator’s product is, in practical terms, protected regardless of the skinny label problem.
Formulation patents face their own prosecution challenges. The formulation itself must be novel and non-obvious — a simple reformulation that any experienced pharmaceutical scientist would have made is not patentable. The strongest formulation patents combine the physical innovation with functional data: a controlled-release formulation that achieves a plasma concentration profile specifically required for efficacy in the new indication, or a new dosage form that eliminates a safety concern that was present with the original formulation at the doses needed for the new use. This framing — formulation as the solution to a clinical problem specific to the new indication — is both scientifically meaningful and legally powerful.
The development implication is that formulation work should begin early in a repositioning program, not as a late-stage commercial consideration. The formulation strategy is an IP strategy decision, and the data generated during formulation development becomes the evidentiary basis for patent prosecution.
3.4 Dosage and Regimen Patents, Combination Patents
A specific dosage or dosing schedule required for the new indication can be patented when it is genuinely non-obvious. The clearest case is when the efficacious dose for the new indication is dramatically lower or higher than the original use, or when a novel dosing schedule (e.g., intermittent dosing, drug holidays) is required to achieve efficacy or manage safety in the new patient population. These patents are moderately protective — they deter direct competitive programs that would need to prove efficacy at the same dose, but they do not prevent off-label use.
Combination patents protect a fixed-dose combination of the repositioned drug with one or more other APIs. Prosecuting a combination patent requires demonstrating synergy or additive effects that are not obvious from the individual drugs’ known pharmacology. When that data exists, combination patents are highly protective because they create a new therapeutic product with a unique clinical profile. A generic manufacturer cannot substitute the individual components for the fixed-dose combination without regulatory approval for the combination itself.
3.5 The Integrated IP-R&D Model
The operational implication of all of the above is that IP strategy and R&D strategy must be unified from the program’s inception, not sequenced. The R&D plan should be explicitly designed to generate data that supports a multi-layered patent portfolio: method-of-use claims supported by unexpected efficacy data, formulation claims supported by clinical pharmacology, dosage claims supported by dose-finding studies, and combination claims supported by mechanistic or synergy data.
This integrated approach transforms what might otherwise be separate legal and scientific processes into a single coordinated program. The goal is a patent thicket: overlapping IP protection across multiple claim types, creating a competitive moat that generics and biosimilar manufacturers cannot breach without substantial legal exposure. In the repositioning context, this is not evergreening in the pejorative sense — it is the foundational commercial architecture that makes clinical investment in an off-patent compound economically rational at all. Without it, no rational capital allocator will fund the Phase II and Phase III trials required for a new indication.
| Patent Type | Prosecution Challenge | Protection Strength vs. Generics | Skinny Label Vulnerability |
|---|---|---|---|
| Method-of-Use | Non-obviousness; unexpected results required | Moderate | High — carve-out is straightforward |
| New Formulation | Novelty of formulation; functional advantage required | High — distinct product, no auto-substitution | None — different product category |
| New Dosage/Regimen | Non-obvious dosing; clinical necessity data required | Moderate | Moderate — off-label dosing possible |
| Combination (Fixed-Dose) | Synergy or additive effect data required | High — new product, independent approval required | Low — generics need separate approval |
| Pediatric Exclusivity | Not a patent; FDA grants 6 additional months | Regulatory, not patent-based | N/A — applies to all approved uses |
Key Takeaways: Section III
Method-of-use patents are necessary but commercially fragile. The skinny label mechanism systematically transfers value from the innovator to generic manufacturers unless the program generates a physically distinct product protected by formulation or combination IP. The decision about which type of secondary patent to pursue is not made at the filing stage — it is made in the R&D program design, which must produce the data that supports prosecution. Programs that integrate IP strategy from day one consistently generate more defensible portfolios than those that address patent strategy after the clinical data exists.
Section IV: Case Studies in IP Valuation — Thalidomide, Sildenafil, and What They Actually Teach
4.1 Thalidomide: From Regulatory Catastrophe to Billion-Dollar IP Franchise
Thalidomide’s history in pharmaceutical IP is one of the most instructive case studies in secondary patent construction. The compound was withdrawn from the European market in 1961 after causing severe birth defects in children whose mothers took it during pregnancy for morning sickness. Its US return began in 1998, when the FDA approved it for erythema nodosum leprosum (ENL), a complication of leprosy. The approval was under the FDA’s highly restricted REMS (Risk Evaluation and Mitigation Strategy) program, which required stringent pregnancy prevention protocols.
The IP architecture Celgene built around thalidomide, and later its structural analog lenalidomide (Revlimid), became a case study in systematic secondary patent construction. The core claims covered method-of-use in multiple myeloma, specific dosing regimens, combination with dexamethasone, and the REMS system itself. The commercial result was remarkable: Revlimid alone generated over $12 billion in annual global sales at its peak, sustained by a patent portfolio that covered not just the molecule but an entire therapeutic ecosystem around it.
For IP and portfolio teams, the Celgene model illustrates a principle that applies directly to repositioning programs: the composition-of-matter patent (which Celgene had for lenalidomide, though not for thalidomide) is less important than the totality of the IP ecosystem. Secondary patents covering the clinical use, the formulation, the dosing protocol, and the safety management system collectively create a moat that is, in some respects, more defensible than a simple composition-of-matter claim.
The IP valuation lesson for analysts: when assessing a repositioning program, the question is not ‘does the company have a patent on the molecule’ but ‘what is the total patent estate, what is the layering of expiry dates, and which claims are most likely to survive Paragraph IV challenge.’
4.2 Sildenafil: When a Safety Signal Becomes a $20 Billion Franchise
Sildenafil was originally developed by Pfizer as a treatment for angina pectoris and hypertension, targeting phosphodiesterase type 5 (PDE5). Phase I trials in the late 1980s showed modest cardiovascular effects, but male trial participants reported a consistent and unexpected side effect: erections. Pfizer’s clinical team recognized the commercial significance and redirected the program.
The IP story of sildenafil is a study in the commercial leverage that a well-timed method-of-use patent can generate when combined with a genuine first-mover advantage. Pfizer’s US Patent 5,250,534, covering the use of sildenafil for erectile dysfunction (ED), was filed in 1993 and granted in 1996. Viagra launched in 1998 and generated $1.9 billion in its first year — a single-year revenue figure that exceeded the entire de novo cost of many drug development programs.
The subsequent competitive and legal history of sildenafil illustrates both the commercial power and the limitations of method-of-use IP. Generic manufacturers filed Paragraph IV certifications challenging the ED use patent before its scheduled 2012 expiry. Pfizer successfully defended the patent in litigation, preserving exclusivity until the patent’s original term. The key legal argument was that the specific use of sildenafil as a PDE5 inhibitor for ED was not predictable from the prior art about PDE5 biology — satisfying the non-obviousness standard.
The analyst takeaway from Viagra’s IP history: a method-of-use patent in a high-volume indication with no therapeutic alternatives can generate disproportionate commercial returns even without composition-of-matter protection. But the commercial ceiling is constrained by the patent’s Paragraph IV vulnerability, and the skinny label problem means that even during the exclusivity period, off-label generic substitution erodes the branded product’s market share over time.
4.3 Evergreening vs. Genuine Innovation: Where the Line Is Drawn
The regulatory and legal system draws a distinction between secondary patents that reflect genuine pharmaceutical innovation and those that extend exclusivity through trivial modifications. US courts and the USPTO have increasingly scrutinized secondary patent claims, and the AIA’s inter partes review (IPR) process has made it substantially easier for generic manufacturers to challenge secondary patents at the Patent Trial and Appeal Board (PTAB) without full district court litigation.
For repositioning programs, this means that the data supporting secondary patent claims must be genuinely robust. A new formulation that does not demonstrably improve clinical outcomes is vulnerable to IPR challenge on non-obviousness grounds. A dosage regimen that simply uses a lower dose of the same drug for the same class of disease, without evidence of unexpected clinical benefit, is similarly at risk. The PTAB’s track record in pharma IPR proceedings shows a high invalidation rate for secondary claims that rest on thin clinical evidence.
The practical implication: R&D programs designed to generate strong secondary patents need to produce data that would be publishable in a major clinical journal on its own merits. The clinical data and the IP data are the same data. This alignment between scientific rigor and legal defensibility is not coincidental — it is the predictable consequence of an IP system that requires objective indicia of non-obviousness.
Key Takeaways: Section IV
Thalidomide/lenalidomide shows that a multi-layered secondary patent estate can generate billion-dollar franchises on off-patent molecules. Sildenafil shows that a well-prosecuted method-of-use patent in a high-volume indication with no competition generates returns out of proportion to its apparent IP strength. Both cases demonstrate that the commercial question is not the patent’s nominal strength but its practical enforceability and the availability of therapeutic alternatives that generics can offer. PTAB’s IPR track record is a material risk factor for any repositioning program that relies on secondary patents — which is every repositioning program.
Section V: The 505(b)(2) Playbook — Regulatory Strategy as Competitive Weapon
5.1 The 505(b)(2) Pathway: Structure and Strategic Logic
The 505(b)(2) New Drug Application pathway, established under the Hatch-Waxman Amendments of 1984, is the primary regulatory tool for repurposed drugs in the United States. Its defining feature is that it allows an applicant to rely, in part, on safety and efficacy data they do not own — specifically, the FDA’s previous findings for a reference listed drug (RLD) and published scientific literature — to support a new drug application.
This ‘hybrid NDA’ sits between the full 505(b)(1) NDA (required for NCEs, where the applicant owns all supporting data) and the 505(j) ANDA (the generic pathway, which requires demonstration of bioequivalence to an RLD). The 505(b)(2) applicant must conduct whatever new studies are necessary to bridge their product to the existing safety and efficacy data. For a new indication, that typically means new Phase II and Phase III clinical trials demonstrating efficacy in the new disease, along with any additional safety data required given the new patient population. For a new formulation, it may require only pharmacokinetic (PK) bridging studies to demonstrate bioavailability comparable to or demonstrably improved over the RLD.
The pathway’s growth as a share of total FDA approvals reflects its strategic attractiveness. In 2024, 505(b)(2) approvals accounted for approximately 40% of all new FDA approvals, a number that exceeded generic drug approvals and represented a major fraction of total pharmaceutical innovation output. This is not a niche pathway — it is the mainstream route for reformulation, indication expansion, and repurposing work.
5.2 Exclusivity Architecture: Stacking Regulatory and Patent Protection
The 505(b)(2) pathway generates multiple overlapping periods of market exclusivity that can be strategically stacked.
A 505(b)(2) application approved on the basis of new clinical investigations (not bioavailability studies) receives three years of market exclusivity for the new conditions of approval. If the repurposed drug qualifies as a new chemical entity under FDA definitions — specifically, if it is a new ester, salt, or other non-covalent derivative of a previously approved drug — it may qualify for five years of exclusivity. During these periods, the FDA will not approve a competing generic of the same product for the same indication, irrespective of patent status.
Orphan Drug Designation (ODD) is the single most powerful exclusivity mechanism for repositioning programs targeting rare diseases (US prevalence below 200,000 patients). Upon approval in the orphan indication, the drug receives seven years of market exclusivity for that specific use. ODD also provides a 50% tax credit for qualified clinical trial expenses and a waiver of the Prescription Drug User Fee Act (PDUFA) application fee. For a repositioning program with a limited remaining patent life, seven years of regulatory exclusivity on a drug that commands orphan pricing (typically $50,000 to $500,000 per patient per year for serious conditions) can generate commercial returns that dwarf those achievable through patent protection alone.
Pediatric exclusivity adds six months to any existing patent or regulatory exclusivity period when the sponsor conducts pediatric studies under a Written Request from the FDA. This extension applies to all of the drug’s formulations and indications, creating a modest but real commercial incentive for pediatric repositioning work.
5.3 The 505(b)(2) Approval Process: Key Decision Points
The critical early decision in a 505(b)(2) program is the selection of the RLD. The RLD’s labeling, manufacturing standards, and approval basis determine the studies that will be required to bridge the new product. A poorly chosen RLD can require substantially more bridging work than an RLD that closely matches the new product’s intended clinical profile. Pre-IND meetings with FDA are standard practice and essential for establishing agreement on the bridging package before significant clinical investment is made.
The filing strategy also determines the competitive dynamics at approval. A 505(b)(2) application that lists patents in the Orange Book establishes the terms under which generic manufacturers can file Paragraph IV certifications. The timing of those listings, the scope of the listed claims, and the anticipated Paragraph IV litigation timeline all affect the commercial horizon for the branded product. For repositioning programs with novel formulations, Orange Book patent listings are particularly important because they may trigger the 30-month stay of generic approval that gives the innovator time to litigate the patent before facing generic competition.
5.4 The Generic Repositioning Gap and Proposed Solutions
The current regulatory framework has a documented gap that affects non-commercial repositioning. When an academic research group or non-profit organization successfully demonstrates that a cheap, off-patent generic drug has a new therapeutic use in a clinical trial, there is no straightforward mechanism for that finding to be incorporated into the drug’s official labeling. Generic manufacturers have little incentive to fund the application process themselves; they profit from the existing generic market regardless of whether the new indication is labeled.
A ‘labeling-only’ 505(b)(2) pathway has been proposed and discussed at the FDA, under which a non-manufacturer sponsor could submit new clinical evidence, and the FDA would update the established name labeling to reflect the new indication for all therapeutically equivalent generic products. The non-manufacturer would assume responsibility for indication-specific post-marketing surveillance. This proposal addresses a real gap, particularly for neglected tropical diseases and rare conditions where no commercial sponsor has financial incentive to pursue labeled repositioning. Implementation faces unresolved questions about liability, funding mechanisms, and the practical enforceability of pharmacovigilance requirements on non-manufacturer sponsors.
Key Takeaways: Section V
The 505(b)(2) pathway is not a regulatory convenience — it is a competitive architecture. The decision about whether to pursue a new formulation, a new indication, or a combination product determines which exclusivity periods are available, which Orange Book listings are possible, and what the Paragraph IV litigation exposure will be. For any repositioning program, regulatory strategy should be developed in parallel with clinical and IP strategy, not after it. Orphan Drug Designation, when available, frequently provides more certain and more valuable market exclusivity than any secondary patent — and for programs targeting small patient populations with premium pricing, it is the primary commercial moat.
Investment Strategy Note: When evaluating a repositioning-stage company, the exclusivity stack is more important than the nominal patent life. A program with three years of 505(b)(2) exclusivity, seven years of ODD exclusivity, and a well-defended formulation patent can have an effective commercial horizon that extends 12-15 years from approval — comparable to a new NCE program. The analysis should map each layer explicitly and assign probability weights to Paragraph IV challenge outcomes.
Section VI: Competitive Intelligence — Patent Databases as a Strategic Map
6.1 Patent Filings as Leading Indicators
Patent applications are filed years before a company’s repositioning program appears in clinical trial registries or press releases. A competitor’s decision to file a method-of-use patent for a new indication, or a formulation patent for a new delivery system, is an early signal of strategic intent that is both specific and verifiable. Any organization conducting serious competitive intelligence in a therapeutic area should treat patent databases as a primary data source, not a secondary one.
The intelligence value of patent monitoring comes from two types of signals. The first is positive: a new patent application from a competitor reveals that they are actively working in a new indication or with a new technology. The second is negative: the absence of patent activity in a white space — a disease area or target class with no existing IP — reveals a potential opportunity for a first-mover program.
6.2 Key Platforms for Drug Repositioning Intelligence
The practical challenge of patent-based intelligence is data integration. A patent filing from the USPTO, disconnected from the corresponding clinical trial registration on ClinicalTrials.gov, the compound’s pharmacology data in DrugBank, and the competitor’s pipeline information in a commercial database, is less informative than the same data points assembled into a coherent picture. The platforms below represent the core infrastructure for that integration.
DrugPatentWatch provides integrated intelligence on drug patents, regulatory exclusivities, Orange Book listings, and Paragraph IV challenge histories. For repositioning programs, its primary value lies in four specific use cases: forecasting the loss of exclusivity (LOE) date for a target compound (which defines the repositioning opportunity window), identifying which generic manufacturers have filed Paragraph IV certifications against a competitor’s repositioned product (which signals imminent legal conflict), conducting prior art searches to assess whether a contemplated secondary patent claim is novel, and monitoring competitor patent filings in therapeutic areas of strategic interest. The platform’s integration of patent data with FDA regulatory data makes it possible to map the complete exclusivity architecture of any branded drug — patent term, regulatory exclusivity periods, pediatric exclusivity, and Paragraph IV challenge status — in a single interface.
Clarivate Cortellis covers the full drug development lifecycle from discovery through post-market, with data on over 100,000 pipeline drugs and six million patents. For repositioning competitive intelligence, its analytical tools allow users to benchmark a candidate’s preclinical and clinical profile against all known competitors in the same indication, access revenue forecasts for drugs in similar market positions, and use probability-of-success models to evaluate the risk-adjusted value of potential acquisition or in-licensing targets. The platform’s deal database is particularly useful for identifying recent transactions in a therapeutic area — both the terms (upfront payments, milestone structures, royalty rates) and the stage at which assets are changing hands provide signal about how the market values repositioning programs in that space.
DrugBank is a public database covering comprehensive pharmacology, mechanism of action, target interactions, metabolic pathways, and product information for approved and investigational drugs. For repositioning specifically, its target and pathway data is the primary resource for generating ‘on-target’ hypotheses: identifying diseases that share a molecular mechanism with a drug’s known indication, or identifying existing drugs known to modulate a target that a new disease has been linked to. The data is free, regularly updated, and well-structured for programmatic integration with internal databases or computational screening platforms.
Open Targets is a public-private consortium platform (partners include GSK, Bayer, and the EMBL-EBI) that integrates genetic association data, functional genomics, and chemical biology to identify and prioritize drug targets. For repositioning, its primary value is target validation: a drug’s known target can be queried against Open Targets’ genetic evidence database to identify other diseases associated with genetic variants in the same target gene. This provides a systematic way to generate target-centric repositioning hypotheses with strong human genetic support — which is both scientifically robust and advantageous in patent prosecution.
ClinicalTrials.gov is the primary public registry for interventional trials globally. Systematic monitoring of trial registrations and status updates for a therapeutic area reveals competitor clinical activity, identifies discontinued programs (potential in-licensing targets), and surfaces adverse event patterns that can generate new indication hypotheses. The registry’s status field distinguishes between completed, terminated, and discontinued trials; terminated and discontinued trials warrant particular attention for in-licensing prospectors.
| Platform | Type | Primary Repositioning Use Cases |
|---|---|---|
| DrugPatentWatch | Commercial | LOE forecasting; Paragraph IV monitoring; prior art search; secondary patent tracking |
| Cortellis (Clarivate) | Commercial | Pipeline benchmarking; deal valuation; competitive landscape mapping; success probability modeling |
| DrugBank | Public | Target-centric hypothesis generation; MOA mapping; polypharmacology analysis |
| Open Targets | Public/Consortium | Genetic target validation; disease-target association evidence scoring |
| ClinicalTrials.gov | Public | Competitor clinical monitoring; discontinued program identification; adverse event mining |
| PubChem | Public | Compound-bioassay linkage; chemical structure-activity data for screening |
| REPO4EU | Public/Private (EU) | European repositioning partnerships; non-commercial trial infrastructure |
6.3 Deconstructing a Competitor’s Strategy: A Worked Example
Consider a realistic scenario. A competitive intelligence team monitoring a therapeutic area notices a new method-of-use patent application filed by a large cardiovascular company covering the use of their marketed beta-blocker for heart failure with preserved ejection fraction (HFpEF). This is the first signal — the company is exploring indication expansion into a disease area with no approved therapy.
Three months later, a second application appears: a new once-daily extended-release formulation of the same compound, at a lower dose than the cardiovascular indication. This second filing is more informative than the first. It confirms that the company is investing in formulation R&D specifically for the new indication, not simply protecting a theoretical use. The lower dose signals that the new indication requires different PK parameters — consistent with HFpEF’s different hemodynamic requirements relative to hypertension. The once-daily formulation suggests patient compliance is a key design criterion, consistent with a chronic disease indication.
Integrating these patent signals with ClinicalTrials.gov reveals a Phase IIa registration for the new formulation in HFpEF. The team now has a complete picture: indication strategy, formulation approach, and clinical timeline — all from public patent and registry data, assembled 18 to 24 months before any press release.
The competitive response options are now concrete: accelerate an internal program in HFpEF using a different mechanism, begin an in-licensing search for a competing asset in the same indication, prepare a freedom-to-operate analysis around the competitor’s formulation claims, or assess whether their method-of-use claim is vulnerable to a Paragraph IV challenge when appropriate.
Key Takeaways: Section VI
Patent databases are the highest-signal competitive intelligence source for repositioning programs because they are filed before public disclosure and are legally required to be specific. An integrated monitoring program that links patent filings to clinical registrations, compound pharmacology, and commercial data can provide 18-24 months of lead time on a competitor’s strategic moves. DrugPatentWatch and Cortellis are the primary commercial tools for this integration. Open Targets and DrugBank provide the scientific substrate for hypothesis generation. The combination is not optional — it is table stakes for any organization operating in a competitive therapeutic area.
Section VII: Market Sizing and Segment Analysis — Where the Money Is
7.1 Global Market Valuation and Growth
The global drug repurposing market carried a 2024 valuation between approximately $29.4 billion and $35.3 billion, depending on the analytical scope and inclusion criteria applied by different research firms. Projections to 2030-2034 range from $37 billion to $59 billion, reflecting a compound annual growth rate (CAGR) between 2.9% and 8.3%. The variance in these estimates reflects genuine methodological differences in what counts as a ‘repositioned’ drug — whether the category includes reformulations, combination products, and indication line extensions, or only programs where the new indication is entirely distinct from the original approval.
The structural growth drivers are durable. Patent cliffs on major blockbusters — including immunology and oncology products generating tens of billions in annual revenue — will erode branded market share and create competitive pressure to replace revenue through lifecycle management, including repositioning. The cost of de novo R&D continues to increase. The FDA’s increased acceptance of RWE and its expansion of the 505(b)(2) pathway’s scope are reducing regulatory barriers for new indication work. These factors collectively make repositioning more attractive on a risk-adjusted basis over time.
7.2 Therapeutic Area Segmentation
Oncology is the largest segment, accounting for approximately 37% of the market. The drivers are the depth of unmet need across cancer subtypes, the well-characterized molecular biology that enables target-centric repositioning, and the regulatory environment that allows accelerated approval for oncology drugs on the basis of surrogate endpoints. The combination of high drug prices in oncology and the multiple indication structure of many cancer drugs (where a single API is approved sequentially for different tumor types) makes oncology the natural home for method-of-use patent strategies.
Rare and orphan diseases are the fastest-growing segment, with a projected CAGR of approximately 15%. The combination of regulatory incentives (ODD’s seven-year exclusivity, fee waivers, tax credits), premium pricing for therapies addressing high unmet need, engaged patient advocacy communities that accelerate trial recruitment, and a biomarker-driven development paradigm that reduces trial size requirements makes orphan repositioning economically attractive at a program cost that de novo programs cannot match. A repositioning program that reaches approval in an orphan indication with a drug that costs $300 million to develop and carries a $150,000-per-year price point can generate a return on invested capital that substantially outperforms an NCE program.
Central nervous system (CNS) diseases represent a large unmet need and a growing segment, though clinical success rates in CNS are lower than in other areas due to the complexity of CNS pharmacology and the difficulty of demonstrating efficacy in heterogeneous patient populations like depression, Alzheimer’s disease, and schizophrenia. Repositioning in CNS benefits particularly from RWD approaches, where large EHR datasets can reveal signal in the patient population before expensive clinical trials are initiated.
7.3 Geographic Analysis
North America accounts for approximately 45-47% of global repositioning market revenue. The US regulatory framework — specifically the 505(b)(2) pathway, ODD, and the established Paragraph IV litigation ecosystem — is the most developed in the world for repositioning programs. US venture capital and institutional investment markets have robust infrastructure for financing repositioning-stage biotech companies. Pricing power in the US, relative to other major markets, means that approval value is highest here.
Europe is the second-largest market and is developing a more structured institutional framework for repositioning through REPO4EU, a public-private platform designed to facilitate mechanism-based repositioning across European academic and industry partners. The European Medicines Agency’s (EMA) equivalent of the 505(b)(2) pathway — the hybrid application under Article 10(3) of Directive 2001/83/EC — provides a comparable legal basis for relying on existing data, though the specific procedures and data requirements differ from the US framework.
Asia-Pacific is the fastest-growing regional segment, driven by healthcare expenditure growth and expanding research infrastructure in China, Japan, South Korea, and Australia. Chinese regulatory authorities have made explicit efforts to align with FDA and EMA frameworks for hybrid applications, which is accelerating the development of a domestic repositioning industry.
Key Takeaways: Section VII
The market’s structure has two important implications for strategy. First, oncology and rare disease together represent the most commercially attractive repositioning opportunities — oncology for volume and the depth of IP protection available around combination regimens, rare disease for regulatory exclusivity, premium pricing, and lower trial cost. Programs targeting other therapeutic areas face more competitive pricing pressure and weaker exclusivity architecture. Second, the US regulatory and investment ecosystem is the primary commercial destination for repositioning programs. European and Asia-Pacific programs typically follow US approval rather than leading it.
Section VIII: The AI Disruption — Techbio Platforms and the New Competitive Landscape {#ai-disruption}
8.1 What AI Actually Does in Repositioning
AI’s practical contributions to drug repositioning fall into four specific functions that correspond to discrete stages of the discovery process. Understanding which function is being served by a specific AI tool is necessary for evaluating both its scientific validity and its commercial implications.
The first function is dataset integration. The datasets relevant to repositioning — chemical structures, protein sequences, gene expression profiles, clinical trial results, adverse event reports, patent literature, EHR data — are enormous, heterogeneous, and stored in different formats across different repositories. AI is the only scalable technology for integrating and normalizing these datasets into a unified representation that can be queried for drug-indication relationships. This is not glamorous, but it is the foundational layer on which everything else depends.
The second function is pattern recognition across the integrated dataset. Machine learning models — including graph neural networks for drug-target interaction prediction, variational autoencoders for generative chemistry, and large language models for scientific literature mining — can identify correlations between compound properties, target biology, disease mechanisms, and clinical outcomes that no human analyst could find manually at scale. The output is a ranked list of compound-indication pairs with associated probability scores and supporting evidence.
The third function is toxicity prediction. One of the most valuable applications of ML in repositioning is early prediction of safety signals that would not be apparent from a compound’s original indication. Models trained on clinical adverse event data, mechanistic toxicology, and structural features can flag potential safety concerns in the new indication’s patient population before a clinical trial begins. This directly addresses the residual safety risk that method-of-use expansion programs face when the new patient population differs substantially from the original.
The fourth function is trial design optimization. ML models trained on historical trial designs and outcomes can identify the enrollment criteria, endpoints, biomarker selection, and statistical design that maximize the probability of demonstrating efficacy in a new indication. This function is newer and less validated than the others, but early evidence suggests that AI-optimized trial designs for repositioning programs can meaningfully improve success rates in Phase II.
8.2 The Techbio Competitors
A distinct class of company has emerged around proprietary AI platforms for drug discovery and repositioning. These ‘techbio’ firms lead with technology rather than specific therapeutic expertise, and their competitive model rests on the claim that their platforms can generate high-quality repositioning candidates faster and cheaper than traditional discovery processes.
Recursion Pharmaceuticals uses automated high-content phenotypic imaging at scale — running millions of cell-based experiments per week — to generate a proprietary dataset of drug-induced cellular phenotypes across hundreds of disease models. Their ML platform then maps compound-phenotype relationships to identify repositioning candidates. The company has described its approach as a ‘cellular cartography’ of drug biology, creating a data asset that compounds in value as more experiments are run.
Exscientia has focused on AI-accelerated medicinal chemistry and drug design, applying generative models to both NCE programs and repositioning work. The company’s approach generates novel candidate structures optimized for specific target profiles, which can be applied to the reformulation and analog programs that often accompany repositioning.
Standigm, a Korean-based AI drug discovery company, has built specific tools for knowledge graph-based repositioning, with a published track record of identifying clinically validated repositioning candidates in oncology and rare diseases. Bullfrog AI focuses explicitly on drug rescue and repurposing, using ML to analyze existing preclinical and clinical datasets to identify repositionable assets among compounds that failed in previous programs.
The competitive threat these companies pose to traditional pharmaceutical organizations is specific. A techbio company running a platform across the entire approved drug universe can generate and prioritize a repositioning candidate in weeks at a cost that is orders of magnitude below a traditional drug screening campaign. This changes the economics of early-stage repositioning to the point where traditional companies that do not build or partner with similar capabilities will be systematically outcompeted in the identification of high-quality candidates.
The strategic response for traditional pharmaceutical companies is not to ignore these platforms but to treat them as partnership targets. The combination of a techbio platform’s candidate generation capability with a large pharma’s clinical development infrastructure, regulatory expertise, and commercial organization is more powerful than either capability alone.
8.3 The Limits of AI in Repositioning
The claims made for AI in drug discovery deserve calibration. The fundamental challenge — demonstrating that a drug is safe and effective in humans — cannot be solved computationally. AI can improve the quality and efficiency of candidate identification, but the clinical success rate of AI-generated candidates is not yet demonstrably higher than historically observed rates for repositioning programs broadly. The literature on AI drug discovery contains many papers reporting high predictive accuracy on held-out test sets, but the translational track record — how many AI-generated candidates have reached approved drug status — remains limited.
The specific risk for repositioning programs is that AI-generated hypotheses are only as good as the data they are trained on. If the training data systematically underrepresents certain patient populations, disease subtypes, or drug classes, the model’s predictions will be biased in ways that are not apparent from standard validation metrics. Prospective validation in independent datasets and robust clinical design remain the irreplaceable validators of any AI-generated repositioning hypothesis.
Key Takeaways: Section VIII
AI is a genuine productivity amplifier for the hypothesis generation and prioritization stages of repositioning. The techbio companies have built data assets and platform capabilities that traditional pharmaceutical organizations cannot easily replicate without substantial investment or partnership. The risk is that AI-generated candidates carry hidden biases from training data limitations. The appropriate framework is to treat AI platforms as hypothesis generators that compress the time and cost of candidate identification, while maintaining rigorous clinical and IP standards for the programs that advance. Organizations that treat AI as a decision-maker rather than a hypothesis generator will encounter avoidable failures.
Section IX: Precision Medicine Intersection — Biomarker-Stratified Repositioning {#precision-medicine}
9.1 Biomarker Stratification as a Commercial Strategy
Precision medicine — the use of genomic, proteomic, or other molecular biomarkers to define patient subpopulations with different treatment responses — changes the economic logic of drug repositioning in a specific and important way. A drug that failed to demonstrate efficacy in an unselected patient population with a broad indication may be highly effective in a molecularly defined subpopulation. Repositioning with biomarker stratification converts a Phase III failure in 1,000 patients into a potential Phase II success in 150 patients who carry the relevant biomarker.
This reframing has three commercial implications. First, it reduces clinical trial size and cost, making it feasible to pursue indications that would be economically unviable without stratification. Second, it creates a companion diagnostic co-development opportunity — a diagnostic test that identifies the responding subpopulation has independent commercial value and strengthens the drug’s reimbursement profile by enabling precision prescribing. Third, and most importantly for IP strategy, it often supports a new patent claim. A method-of-use claim covering the use of a drug in a biomarker-selected population (‘a method of treating non-small cell lung cancer in patients expressing biomarker X, comprising administering a therapeutically effective amount of compound Y’) is substantially stronger than a broad indication claim because the biomarker specificity is itself a novel and non-obvious limitation.
9.2 Pharmacogenomics in Repositioning: Translating Genetic Association to Clinical Program
Genome-wide association studies (GWAS) have generated thousands of validated genetic associations between specific variants and disease susceptibility. For repositioning, these associations are actionable in two directions. A GWAS finding that a disease is associated with a variant in a gene encoding a drug target identifies a genetically validated target for repositioning programs. A drug known to modulate that target now has genetic support for its use in the disease — a substantially stronger evidence base than a computational prediction alone.
The reverse direction is also informative: pharmacogenomic data on drug response can identify patient subgroups who are, for genetic reasons, likely to respond to a repositioned drug. Variants in CYP450 enzymes that affect drug metabolism can predict whether a patient will achieve therapeutic plasma concentrations at a standard dose. Variants in the drug’s known target can predict receptor sensitivity. These pharmacogenomic factors define the stratified population in which a precision repositioning program should be tested.
9.3 The Acquired Resistance Problem
The intersection of repositioning with precision medicine also imports one of precision oncology’s persistent clinical problems: acquired drug resistance. When a molecularly targeted drug is effective in a biomarker-selected population, the selection pressure it exerts drives the emergence of resistant clones. This is not a failure of the drug — it is a predictable biological consequence of targeted therapy in heterogeneous tumors or disease states.
For repositioning programs, the resistance problem creates a research imperative to develop combination strategies from early in the program. Identifying resistance mechanisms before they emerge clinically — through CRISPR screens, patient-derived organoid models, or ctDNA monitoring in early trials — and designing combination regimens that address those mechanisms is both good science and good IP strategy. A combination patent that covers the repositioned drug together with a resistance-breaking agent is one of the strongest secondary patent types available.
Key Takeaways: Section IX
Biomarker-stratified repositioning reduces clinical trial size and cost, improves the probability of demonstrating efficacy, creates companion diagnostic co-development opportunities, and generates stronger secondary patent claims. The practical challenge is identifying the right biomarker early enough to incorporate it into the trial design. Programs that invest in translational biomarker work in Phase I and II consistently generate more prosecutable IP and more defensible regulatory submissions than programs that treat biomarker selection as a late-stage decision.
Section X: Investment Strategy — Evaluating Repositioning Assets {#investment-strategy}
10.1 What to Look for in a Repositioning-Stage Company
Institutional investors evaluating repositioning programs need a different analytical framework than they apply to NCE programs. The key variables are not the same.
The compound’s safety history is the starting asset, and its quality determines how much Phase I work can be avoided or compressed. A compound with IND-enabling studies completed, Phase I data in humans at the target dose range, and a well-characterized safety profile in a relevant patient population can reach Phase II proof-of-concept studies in 12 to 18 months. A compound with only animal safety data requires the full Phase I program, eroding the timeline advantage of repositioning.
The IP landscape is more complex than in NCE programs, but the key question is the same: what is the effective exclusivity horizon for the product in the target indication? This requires mapping every relevant patent (method-of-use, formulation, dosage, combination), assessing the probability of surviving Paragraph IV challenge for each, and mapping the regulatory exclusivity periods (505(b)(2) exclusivity, ODD, pediatric). The commercial horizon is the longest defensible combination of these layers, risk-adjusted for litigation outcomes.
The indication selection is the most important variable that management controls. The same compound repositioned into an indication with ODD eligibility, a small well-defined patient population, and premium pricing potential generates a fundamentally different financial profile than the same compound repositioned into a large-market indication with intense generic competition and managed care pricing pressure.
10.2 Valuation Framework: Risk-Adjusted NPV for Repositioning Programs
Standard risk-adjusted net present value (rNPV) models apply well to repositioning programs, with three modifications specific to the category.
The probability of technical success (PTS) at each clinical phase should be higher than the NCE baseline — 30% overall versus 10%, reflecting the safety de-risking. But this uplift should be applied specifically to the Phase I success probability, not uniformly across the clinical program. Phase II and Phase III efficacy failures are as common in repositioning as in NCE programs. The rNPV model should reflect this by using NCE-level probability assumptions for Phase II and Phase III efficacy outcomes while using elevated probability assumptions for Phase I safety outcomes.
The commercial projection should be built from the exclusivity architecture, not from top-down market share estimates. The exclusivity periods define when generic competition begins. The reimbursement environment in the target indication defines pricing. The patient population size and treatment duration define peak sales. A bottom-up commercial model that starts with the exclusivity map is more accurate than a top-down share estimate because it correctly identifies the commercial ceiling imposed by generic entry.
The risk of Paragraph IV challenge should be modeled explicitly. For any branded product with secondary patent protection, the probability that a generic manufacturer will file a Paragraph IV certification within 24 months of approval is historically high (above 70% for products with significant commercial potential). The probability that the innovator wins the subsequent litigation, and the timing of resolution, should both be modeled as scenario variables. Many repositioning-stage acquisitions and licensing deals undervalue this risk because the patent portfolio looks strong on paper — but PTAB’s track record on secondary patent challenges is sobering.
10.3 Common Valuation Errors
Three specific errors recur in institutional analysis of repositioning programs.
The first is treating the compound’s historical safety data as a blanket guarantee. Repositioning into a different disease may involve a different patient population, longer treatment duration, different concomitant medications, and different dose levels than the original indication. All of these differences can surface safety signals that were not apparent in the original program. The Phase I program for a repositioned drug should be designed to specifically address the safety questions posed by the new context, not simply to replicate the historical data.
The second error is conflating IP breadth with IP strength. A patent with 40 claims is not necessarily more defensible than a patent with 10 claims. What matters is whether the key claims — the ones that would block a competing generic from reaching the market — are novel, non-obvious, and supported by robust data. An IP review that simply counts patents without assessing claim-level validity is not useful for commercial decision-making.
The third error is ignoring the skinny label problem in method-of-use-only programs. If the entire IP moat rests on a single method-of-use patent, the commercial projection needs to model the market share erosion that will occur through off-label generic substitution even during the exclusivity period. Historical experience with method-of-use-protected repositioned drugs shows that branded market share can erode by 30-50% within 24 months of generic entry into the original indication, regardless of the method-of-use patent’s validity. This is not a legal outcome — it is a commercial reality driven by prescriber and payer behavior.
Key Takeaways: Section X
Repositioning investment analysis requires a different analytical lens than NCE programs. The key value drivers are the exclusivity architecture (not just patent count), the indication selection (small-market ODD opportunities frequently outperform large-market generics-exposed opportunities on a risk-adjusted basis), and the quality of the safety heritage (which determines how much Phase I work can be compressed). The most common analytical error is treating secondary IP as uniformly strong without assessing claim-level Paragraph IV vulnerability and the real-world impact of the skinny label problem.
Section XI: Operational Blueprint — Building the Program {#operational-blueprint}
11.1 The Integrated Intelligence Function
The first operational requirement for a systematic repositioning program is an integrated intelligence function — a cross-functional team with access to patent databases, clinical registries, pharmacological databases, and commercial intelligence platforms, with the mandate to continuously monitor and synthesize intelligence from all sources. This is not a function that can be adequately performed by a single department. Patent monitoring requires IP counsel. Clinical trial monitoring requires regulatory and medical science expertise. Commercial intelligence requires business development and market access input. Computational hypothesis generation requires bioinformatics and data science capability.
The team’s outputs should include a continuously updated patent landscape for each therapeutic area of strategic interest, a ranked list of competitor repositioning programs by indication and development stage, a library of potential in-licensing candidates from discontinued programs, and a map of ‘white space’ indications where repositioning candidates could achieve first-mover IP positioning.
11.2 The Discovery-to-Development Handoff
The handoff from computational hypothesis to development program is where many repositioning programs lose value. Computational tools generate candidates with probability scores and supporting evidence, but translating that output into a development decision requires clinical, regulatory, and commercial judgment that the algorithm cannot provide.
A structured Stage Gate process adapted for repositioning should include: a computational screening gate (ranked candidates with supporting evidence), a feasibility gate (assessment of compound availability, safety history quality, and IP landscape), a proof-of-concept gate (early experimental validation in a disease-relevant model), a program initiation gate (full clinical, IP, regulatory, and commercial assessment), and a Phase III entry gate (complete data package review and financing assessment). Each gate should produce a documented go/no-go recommendation with explicit criteria, enabling consistent decision-making across the portfolio.
11.3 Building the Compound Library
For organizations building an internal repositioning capability, the compound library is the fundamental asset. A library of off-patent drugs with characterized safety profiles, known pharmacokinetics, and commercial GMP manufacturing processes is the raw material from which repositioning candidates are identified. The library should be curated to maximize chemical and mechanistic diversity while prioritizing compounds with human safety data at doses relevant to potential new indications.
External compound libraries are available through several mechanisms. Academic medical centers that conducted investigator-initiated trials with off-patent drugs often have excess drug supply and extensive safety and PK data. Companies divesting therapeutic area assets as part of portfolio rationalization will often license or transfer compound libraries along with the associated data packages. The NIH’s National Center for Advancing Translational Sciences (NCATS) maintains a collection of compounds available for repositioning research, including approved drugs, failed drugs, and drugs approved outside the United States.
Key Takeaways: Section XI
The organizational infrastructure for systematic repositioning — the intelligence function, the Stage Gate process, the compound library — is a material competitive asset. Organizations that have built this infrastructure consistently identify candidates faster, make better-informed go/no-go decisions, and build stronger IP portfolios than those that treat repositioning as a series of ad hoc projects. The investment in the infrastructure is modest relative to the clinical development costs it is guiding.
Appendix: Glossary of Key Terms
505(b)(2) NDA: An FDA New Drug Application that relies, in part, on safety and efficacy data not owned by the applicant, including the FDA’s findings for a reference listed drug and published literature. The primary regulatory pathway for repositioned drugs in the US.
Composition-of-Matter Patent: A patent covering a chemical compound itself, regardless of its use. The strongest form of pharmaceutical IP protection. Not available to repositioning programs because the API is already known.
Eroom’s Law: The observation that the number of new drugs approved per billion dollars of R&D spending has declined by roughly half every nine years since the mid-1950s, when adjusted for inflation. Named as an inversion of Moore’s Law.
Evergreening: The practice of filing secondary patents on existing drugs to extend market exclusivity beyond the original patent’s expiration. In repositioning, the term also describes the legitimate practice of building IP around genuinely new clinical uses.
Loss of Exclusivity (LOE): The date on which all patent and regulatory exclusivity protections for a branded drug expire, after which generic or biosimilar manufacturers can enter the market.
Method-of-Use Patent: A patent covering the specific therapeutic application of a known drug to treat a new disease or condition. The foundational IP tool for repositioning programs.
Orphan Drug Designation (ODD): An FDA designation for drugs targeting rare diseases (US prevalence below 200,000 patients) that provides seven years of market exclusivity upon approval, tax credits for clinical trial costs, and fee waivers.
Paragraph IV Certification: A certification filed by a generic drug applicant asserting that one or more patents listed in the FDA’s Orange Book for a branded drug are invalid, unenforceable, or will not be infringed by the generic product.
Phenotypic Screening: An experimental drug screening approach that measures compound effects on cell or organism behavior without requiring prior knowledge of the molecular target. Contrasted with target-based screening.
Polypharmacology: The interaction of a single drug with multiple biological targets. Historically viewed as a source of off-target side effects; in repositioning strategy, treated as a map of potential new therapeutic applications.
Reference Listed Drug (RLD): The branded drug whose FDA approval provides the regulatory foundation for a 505(b)(2) NDA.
Skinny Label: A product label used by a generic manufacturer that omits one or more patented indications of the branded reference drug, allowing the generic to be marketed for the non-patented uses while not directly infringing the method-of-use patent covering the excluded indication.
Target-Centric Repositioning: A repositioning approach that begins with a specific molecular target known to be relevant to a disease, then identifies existing drugs known to modulate that target.
This document is for informational purposes only and does not constitute legal, regulatory, or investment advice. Patent and regulatory landscapes are subject to change. Consult qualified legal and regulatory counsel before making IP or development decisions.