A deep-dive for pharmaceutical IP teams, R&D leads, and institutional investors on intellectual property architecture, regulatory pathways, exclusivity mechanics, and competitive intelligence in drug repurposing.
Market Reality: Size, Growth, and What the Numbers Actually Mean
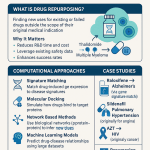
Drug repurposing – the systematic identification and development of new therapeutic indications for existing drug molecules – is no longer a portfolio curiosity. It is a $34.98 billion market segment as of 2024 that accounts for an estimated 25% of the pharmaceutical industry’s annual global revenue. Consensus projections place that figure at $59.30 billion by 2034, implying a CAGR of 5.42%. North America holds roughly 47% of current market share, with the fastest incremental growth anticipated from the Asia-Pacific region as Chinese and South Korean pharma companies adopt computational screening at scale.
That headline growth figure, however, understates the strategic weight of repurposing within R&D budgets. The correct frame is not ‘how large is the market’ but ‘what proportion of late-stage pipeline value is now derived from repurposed or repositioned assets.’ By that measure, the shift is more dramatic: the 505(b)(2) pathway – the primary U.S. regulatory vehicle for repurposed drugs – accounted for 40% of all FDA new drug approvals in 2024, more than any other single NDA category. That figure alone explains why every major pharma company now runs a formal lifecycle management program.
Three structural forces are driving this shift. First, the per-NCE cost of bringing a genuinely new chemical entity to market – accounting for the cost of failures across the portfolio – has pushed past $2 billion in most published estimates, with some IQVIA analyses placing the fully-loaded figure closer to $2.6 billion. That cost compresses returns on invested capital to the point where only a handful of therapeutic categories can justify pure greenfield discovery. Second, the patent cliff on blockbuster biologics is accelerating biosimilar erosion across oncology, immunology, and metabolics, forcing companies to find new revenue streams within existing molecular franchises. Third, AI-driven target discovery has compressed the timeline for generating credible repurposing hypotheses from years to months, reducing the speculative capital required to initiate a program.
The result is a market where repurposing has moved from opportunistic to structural – not a fallback when NCE pipelines run dry, but a parallel, capital-efficient engine running alongside primary discovery.
Key Takeaways: Market Reality
The drug repurposing market at $34.98 billion (2024) reflects genuine commercial momentum, not definitional inflation. The 40% share of FDA approvals via 505(b)(2) in 2024 is the clearest indicator that this is now a mainstream development strategy, not a niche. Investors should track 505(b)(2) filing rates as a leading indicator of near-term NDA approvals within a company’s pipeline, since the pathway’s median approval timeline is materially shorter than a full 505(b)(1) NDA.
The Economic Case: Quantifying the De-Risking Premium
The three-variable economic argument for repurposing – faster, cheaper, higher success rate – is well-documented. The analytical work lies in understanding how these variables interact, and where they break down.
Timeline Compression: Where the 5-7 Year Savings Come From
A repurposed drug’s timeline advantage is not uniformly distributed across all development stages. The bulk of the savings are concentrated in two areas: preclinical development (typically 3-4 years for an NCE) and Phase I safety trials (6-18 months). When a compound has an established human safety dossier from prior clinical work, both stages can be compressed or eliminated entirely, depending on the degree of similarity between the original indication and the new use.
The caveat that IP teams and R&D leads need to hold onto is the ‘bridging study’ problem. The FDA’s 505(b)(2) pathway does not grant a blanket pass on preclinical work. It requires the applicant to provide a scientific justification – a ‘bridge’ – that links the existing safety data to the new product. If the new formulation, route of administration, or patient population differs materially from the reference drug, the FDA will require pharmacokinetic bridging studies, modified toxicology packages, or both. These can add 18-36 months and $30-80 million to the development budget. Companies that model ‘5-7 years faster’ without scoping the bridging requirement are building their business cases on sand.
The actual timeline advantage, properly scoped, ranges from 18 months to seven years depending on: (a) the degree of regulatory reliance justified by the scientific bridge, (b) whether the new indication requires new Phase II or Phase III data, and (c) whether the FDA grants Breakthrough Therapy, Fast Track, or Accelerated Approval designation, which can each shave 6-18 months from the review timeline.
Cost Structure: The $300 Million Figure and Its Limits
The frequently cited $300 million median development cost for a repurposed drug versus $2-3 billion for an NCE is accurate at the median but misleading as a planning figure. The distribution is bimodal. Simple reformulation or dosage-change projects can be executed for $30-80 million. Programs requiring a full Phase III trial in a new indication – which many orphan and oncology repurposing programs do – can cost $200-600 million, well within the NCE range once you account for trial complexity.
The more analytically useful framing is the cost relative to the probability-adjusted expected value of the asset. A repurposed drug entering Phase II with prior human safety data has a probability of reaching market approval roughly three times higher than an NCE at the same stage (approximately 30% versus less than 10%). That probability difference has a computable dollar value. For a drug in a market with $500 million in peak annual sales, a 20-percentage-point improvement in Phase II-to-approval probability is worth approximately $100 million in net present value, before accounting for the time savings. This ‘de-risking premium’ is the correct unit of value for licensing negotiations – not the raw dollar cost of development.
Comparative Development Profile
| Metric | NCE (505(b)(1)) | Repurposed Drug (505(b)(2)) | Notes |
|---|---|---|---|
| Median time to market | 10-15 years | 3-12 years | Range reflects bridging complexity |
| Fully-loaded development cost | $2-3B | $30M-$600M | Bimodal distribution |
| Phase I-to-approval success rate | <10% | ~30% | Post-human safety data established |
| Preclinical investment required | Full | Partial to none | Dependent on FDA bridge scope |
| Primary IP protection | Composition of matter | Method of use; formulation | Key vulnerability distinction |
| U.S. market exclusivity (base) | 5 years (NCE) | 3 years (new use) or 7 years (orphan) | Patent term separate |
| Regulatory pathway | 505(b)(1) NDA | 505(b)(2) NDA | Both require full safety/efficacy showing |
Key Takeaways: Economics
The ‘$300 million’ figure needs contextual adjustment before any investment model is built. The true cost depends on bridging study scope, trial size, and indication complexity. The analytically correct valuation metric is the de-risking premium: the NPV gain from improved probability of success, not just the savings on eliminated trials. That premium is often worth $75-200 million on mid-sized assets, which explains why in-licensing prices for late-preclinical repurposing candidates have risen materially over the past five years.
The IP Playbook: Building a Multi-Layered Patent Fortress
The central IP problem in drug repurposing is structural: the active pharmaceutical ingredient (API) is already in the public domain. Composition-of-matter protection – the strongest form of pharmaceutical IP, capable of creating a 20-year moat around a novel molecule – is unavailable. Everything else must be built from the secondary patent toolkit, and that toolkit requires both architectural thinking and relentless attention to claim drafting.
Method-of-Use Patents: The Necessary Foundation
A method-of-use (MoU) patent – also called a ‘new use’ or ‘Swiss-type’ patent – claims the specific therapeutic application of a known compound rather than the compound itself. The canonical claim structure is: ‘A method of treating [Disease X] comprising administering a therapeutically effective amount of [Compound Y] to a patient in need thereof.’
MoU patents are essential but inherently vulnerable on two fronts. First, the non-obviousness bar is high. A patent examiner will scrutinize the prior art aggressively: if the drug’s known mechanism of action is directly relevant to the new disease, or if published scientific literature has speculated about the connection, the application faces a substantial obviousness rejection under 35 U.S.C. § 103. The strongest MoU applications are those where the therapeutic link was discovered through a non-linear pathway – a computational prediction based on off-target binding profiles, an RWE signal from insurance claims data, or an unexpected pharmacological observation during a clinical trial for an unrelated condition. The nature of the discovery process is, itself, evidence of non-obviousness.
Second, even a granted MoU patent is commercially leaky. The ‘skinny label’ mechanism – formally, a Section viii carve-out under Hatch-Waxman – allows a generic manufacturer to launch with a label that omits the patented indication, covering only the original, off-patent use. Physicians then prescribe the cheaper generic off-label. The Pfizer v. Teva litigation over pregabalin (Lyrica) in the UK confirmed this vulnerability: the UK Supreme Court in 2019 held that the NHS’s generic prescribing practices could potentially lead to infringement, but the line between direct and induced infringement in method-of-use cases remains contested across jurisdictions. In the U.S., the Federal Circuit’s 2021 decision in Amarin Pharma v. Hikma clarified that a ‘skinny label’ launch without active inducement does not, by itself, constitute infringement – leaving MoU patent holders with a significant commercial leak unless the product is differentiated at the formulation level.
Formulation Patents: Closing the Skinny Label Loophole
The most effective single move in the repurposing IP playbook is pairing the MoU patent with a formulation patent that is both novel and clinically necessary for the new indication. The commercial logic is precise: if the patented formulation is required for therapeutic equivalence in the new indication, a generic with the old immediate-release formulation cannot be safely substituted. This eliminates the skinny label problem, because a pharmacist dispensing the immediate-release generic for the new indication would not be providing a therapeutically equivalent product.
Patentable formulation innovations in the repurposing context include:
Extended-release oral formulations that maintain therapeutic blood levels with lower peak concentration, reducing toxicity or improving tolerability in a patient population that differs from the original indication. Nanoparticle delivery systems – liposomal, polymeric, or lipid nanoparticle – that achieve tissue-specific distribution required for a new indication. Topical or transdermal formulations converted from oral systemic administration. Fixed-dose combinations that pair the repurposed drug with a standard-of-care agent for the new indication. Aqueous injectable formulations for drugs originally approved as oral solids, where the new indication (e.g., acute care or a population unable to swallow tablets) requires parenteral delivery.
Each of these creates a distinct, protectable invention. Critically, a formulation patent covers a physical product, not a method, making it far more resistant to the skinny label carve-out. A generic must replicate the formulation to be substitutable, and doing so constitutes direct infringement of the formulation patent – a cleaner legal claim than induced infringement under a method patent.
Combination Patents: Engineering Non-Obviousness
Combination patents protect a fixed-dose formulation or co-administration regimen of the repurposed drug with one or more other agents. For a combination patent to be non-obvious, the applicant must demonstrate unexpected synergy – a result that could not be predicted from the activity of either component alone. This is a demanding standard, but when met, it produces extremely strong IP.
The strategic value of a combination patent goes beyond legal protection. It creates a clinical differentiation story. A single-agent repurposed drug occupying a crowded therapeutic category has limited pricing power. The same drug in a patented fixed-dose combination with a standard-of-care agent, backed by Phase III data showing superior outcomes, can command premium pricing and accelerate formulary access. The patent and the clinical narrative reinforce each other.
Dosing Regimen and Therapeutic Index Patents
In some repurposing contexts, the therapeutic innovation lies in the dosing architecture. A specific dose level that achieves efficacy in the new indication without the toxicity seen at doses used for the original indication – a narrowed therapeutic window – can be patentable if the result is unexpected. Weekly versus daily dosing for a drug originally administered multiple times per day is similarly protectable if the regimen is both novel and non-obvious, and if clinical data supports the efficacy claim.
These patents are narrower than formulation patents and face a higher obviousness challenge – clinical dose-ranging is considered routine experimentation in many contexts. They are most valuable as supplementary layers in a patent thicket rather than standalone protection.
Building the Patent Thicket: Architectural Design
A single patent, regardless of quality, is a fence. The effective IP strategy for a repurposed drug is architectural – designing a patent thicket that creates multiple, overlapping legal barriers to generic entry. The goal is not to make generic competition impossible, but to raise the legal cost, time, and risk of attempting it to the point where generic manufacturers redirect their Paragraph IV challenges toward softer targets.
A well-designed patent thicket for a repurposed small molecule might include:
A MoU patent covering the new indication with the earliest possible priority date. A formulation patent covering the delivery system specific to the new indication, filed as clinical data on the formulation’s superiority emerges. A combination patent covering co-administration with the most likely standard-of-care partner, backed by PK/PD or Phase II data demonstrating interaction. A dosing regimen patent covering the specific titration schedule found to optimize the safety-efficacy profile. A process patent covering any novel synthesis route for the formulation component (not the API itself, which is off-patent, but the novel excipient or delivery matrix).
Each of these patents has a different expiration date, forcing a generic challenger to navigate multiple validity and infringement analyses simultaneously. The cumulative deterrent effect is disproportionate to the sum of the individual patents. This is the ‘thicket’ dynamic: not just multiple barriers, but multiple barriers that each require separate litigation.
Key Takeaways: IP Playbook
The MoU patent is the starting point, not the finish line. The commercially defensible IP position in repurposing requires a minimum of a MoU patent plus a formulation patent that closes the skinny label gap. The strongest positions combine four or more patent types timed to sequential expiration, creating a rolling exclusivity that extends commercial protection well beyond any single patent term. IP teams should run a Paragraph IV risk assessment for each layer at the time of filing, since the sequence of likely generic challenges will determine the defensive litigation budget.
Investment Strategy: IP Architecture
For institutional investors, the key due diligence question on any repurposed drug asset is: ‘What is the product, not just the method?’ A pure MoU patent is a one-star IP position – legally valid but commercially fragile. A MoU patent paired with a proprietary formulation patent that is clinically essential to the new indication is a three-star position. A full patent thicket with rolling expirations, a registered Paragraph IV litigation history showing prior successful defenses, and Orange Book listings across all relevant patents is a five-star position that justifies premium valuation multiples. Acquirers in the 2022-2025 wave of repurposing asset M&A have consistently paid 30-45% higher acquisition multiples for assets with multi-layer IP positions versus those with MoU patents alone.
IP Valuation Deep Dives: Asset-Level Analysis
Sildenafil (Pfizer): The $4.7 Billion IP Architecture Case Study
Sildenafil’s IP portfolio is the best-documented and most analytically instructive case in repurposing history. Pfizer’s IP strategy for this asset did not resemble a single patent; it resembled a corporate treasury instrument – a structured financial product designed to generate predictable cash flows at precisely timed intervals.
The foundational patent, US5250534, covered sildenafil as a PDE-5 inhibitor for cardiovascular indications and expired in 2012. This was the ‘base position,’ largely a commodity by the time repurposing became commercially relevant. The critical asset was US6469012, the method-of-use patent covering the treatment of erectile dysfunction, which carried an initial expiration of 2019. This second patent was filed after Pfizer’s clinical team observed the drug’s effect in Phase I volunteers – a direct example of how clinical observation generates patentable IP in real time, provided the IP team is monitoring trial results as they emerge.
Pfizer then executed two distinct exclusivity extensions that pushed the effective commercial life of the Viagra franchise beyond what either patent alone could achieve. First, pediatric exclusivity: Pfizer conducted studies of sildenafil (marketed as Revatio) in pediatric patients with pulmonary arterial hypertension (PAH). Under the Best Pharmaceuticals for Children Act (BPCA), completion of FDA-requested pediatric studies grants a six-month exclusivity extension that is appended to any unexpired patent listed in the Orange Book for that drug, including the Viagra ED patent. This moved the core Viagra patent expiration from April 2020 to October 2020. For a drug generating approximately $1.7 billion in annual sales at peak, a six-month extension represented roughly $850 million in protected revenue – a return of several hundred to one on the cost of the pediatric trial.
Second, Pfizer used Paragraph IV litigation strategically. When Teva filed an ANDA with a Paragraph IV certification against the US6469012 patent in 2011, Pfizer sued, triggering an automatic 30-month stay on Teva’s approval. Rather than pursue the litigation to verdict – a path that would have maintained the patent’s full term but carried the risk of an adverse ruling invalidating the patent entirely – Pfizer settled in 2013. The settlement granted Teva a license to launch a generic in December 2017, two years ahead of the patent’s expiration, in exchange for royalties. This trade-off is the critical IP valuation insight: Pfizer accepted a shorter monopoly period in exchange for eliminating the binary invalidation risk of a full Paragraph IV trial, and locked in a royalty stream that partially offset the revenue loss from early generic entry.
The authorized generic launch on the same day as Teva’s entry – executed through Pfizer’s Greenstone subsidiary – then compressed Teva’s 180-day market exclusivity advantage, ensuring that Pfizer captured a large share of the price-sensitive generic market from day one.
IP asset valuation assessment for sildenafil at the time of the Teva settlement: the core Viagra patent (US6469012) carried an estimated market value of $3.2-4.7 billion in NPV terms, discounted at a 10% cost of capital and incorporating the royalty income from the settled Teva agreement. The PAH indication, covered by Revatio and a separate set of formulation and method patents, added another $400-700 million in protected revenue over the same period. Total IP estate value at peak: approximately $4.1-5.4 billion, making sildenafil’s IP portfolio one of the most valuable secondary patent positions in pharmaceutical history.
Thalidomide / Lenalidomide (Celgene / BMS): The IP-Linked Franchise Value
Thalidomide’s commercial renaissance was not a clean repurposing story – it was the foundation of a franchise that Celgene built into a $20+ billion revenue operation through disciplined IP stacking across a structural analogue series. The thalidomide-to-lenalidomide-to-pomalidomide progression illustrates how a repurposing discovery, when IP-managed correctly, can seed an entire molecular franchise.
Thalidomide received FDA approval for ENL in 1998 and for multiple myeloma in 2006. The original thalidomide IP was long expired by that point – the molecule dates to 1957. Celgene’s commercial moat came entirely from secondary IP: the S.T.E.P.S. Risk Evaluation and Mitigation Strategy (REMS) program, proprietary manufacturing processes, and, critically, the composition-of-matter patents on lenalidomide (Revlimid), a structural analogue of thalidomide with substantially improved potency and reduced teratogenicity. Lenalidomide was not a pure repurposing play – it was a new chemical entity – but its discovery was enabled by the mechanistic understanding gained from thalidomide repurposing, demonstrating how a repurposed drug creates the scientific foundation for follow-on NCE development.
Revlimid’s composition-of-matter patent expired in January 2022, but Celgene had structured its generic entry agreements with extraordinary specificity: multiple settlement agreements with generic manufacturers that allowed limited-volume generic entry in years one and two post-expiration, with full volume generic availability phased in over 2023-2026. This ‘managed entry’ approach, negotiated in advance and structured via Paragraph IV settlements, is a direct application of the same principles Pfizer used with sildenafil – trading monopoly duration for reduced invalidation risk and predictable revenue. BMS, which acquired Celgene in 2019 for $74 billion, paid a significant portion of that premium for the IP management architecture around the immunomodulatory imide drugs (IMiD) franchise.
IP asset valuation note for the Celgene franchise: at acquisition, the Revlimid patent estate (including U.S. composition-of-matter patents, method patents for myeloma and MDS, and international counterparts) carried an estimated NPV of $14-18 billion, representing the single largest component of the acquisition price.
Esketamine (Janssen/J&J): Formulation Patent as the Moat
Spravato (esketamine nasal spray) is the clearest recent example of a formulation patent creating defensible value from a repurposed molecule. Ketamine, a Schedule III controlled substance approved as a general anesthetic in 1970, has been used off-label for treatment-resistant depression for years. J&J’s contribution was not discovering the antidepressant effect – that was already documented in academic literature – but developing a proprietary nasal spray formulation of esketamine (the S-enantiomer of ketamine) with a specific pharmacokinetic profile optimized for outpatient psychiatric use under REMS supervision.
The method-of-use patent covering ketamine’s antidepressant effect would have been almost impossible to enforce against off-label ketamine infusions. J&J’s commercial position rests primarily on the formulation patent for the nasal delivery system and the Spravato REMS, which restricts dispensing to certified healthcare settings and requires in-office monitoring for two hours post-administration. Generics cannot replicate the Spravato REMS-constrained commercial access model, and the specific nasal formulation patent provides the legal basis for blocking any direct competitor from the same delivery route.
Spravato generated approximately $650 million in 2023 sales, growing at 50%+ annually. IP asset valuation: the nasal formulation patent estate and REMS-based market access position carry an estimated NPV of $4-7 billion over the patent life, assuming continued label expansion into major depressive disorder and other psychiatric indications.
Evergreening: Strategy, Controversy, and the Full Technology Roadmap
‘Evergreening’ is a contested term. Its critics use it to describe trivial patent filings designed to delay generic competition without clinical benefit. Its practitioners call it lifecycle management and describe it as legitimate protection of follow-on innovation. The analytical reality is that both descriptions apply to real cases, and the IP strategist’s job is to execute legitimate lifecycle management that can withstand both legal and political scrutiny.
The Evergreening Technology Roadmap: 12 Tactics
The following represents a comprehensive taxonomy of lifecycle management tactics used in pharmaceutical practice, ordered from those generating clear clinical value to those most vulnerable to legal and regulatory challenge.
Tier 1: High Clinical Value, Strong Legal Defense
New indication discovery (genuine repurposing): Filing new method-of-use patents for a second or third therapeutic indication based on substantive clinical trial data. The classic case is a cardiovascular drug subsequently approved in oncology based on an AI-identified mechanistic link. Clinical value is clear, and the patent term on the new use typically extends protection by 3-7 years beyond the original composition patent.
Proprietary formulation development: Developing an extended-release, nanoparticle, or targeted delivery version that demonstrably improves outcomes (reduced side effects, improved dosing convenience, superior PK profile) in the original or new indication. When clinical trials confirm the superiority of the new formulation over the original, both the patent and the regulatory case are strong.
Fixed-dose combination with novel synergy: Creating a fixed-dose combination product where the two agents demonstrate genuine pharmacological synergy – measured as a statistically significant improvement over either component alone in a randomized trial. The combination patent is among the most defensible in the lifecycle management toolkit.
Pediatric indication extension: Conducting FDA-requested pediatric trials under PDUFA/BPCA, earning the six-month patent extension while genuinely expanding the drug’s utility. The pediatric extension has the highest benefit-to-cost ratio of any lifecycle management tactic: a pediatric trial costing $30-80 million can extend exclusivity on a $1+ billion product.
Tier 2: Moderate Clinical Value, Context-Dependent Defense
Salt or polymorph patents: Filing patents on specific crystalline forms, salts, or polymorphs of the API that offer improved stability, bioavailability, or manufacturability. These are strong when the polymorph confers a measurable clinical benefit, weak when the clinical distinction is minimal.
Metabolite patents: Patenting the pharmacologically active metabolite of a parent compound, potentially with its own composition-of-matter protection if the metabolite is a distinct chemical entity never previously disclosed. Armodafinil (the R-enantiomer of racemic modafinil) and esomeprazole (the S-enantiomer of omeprazole) are the most commercially significant examples. These face vigorous generic and academic criticism but have generally withstood Paragraph IV challenges when clinical differentiation data is available.
Process patents: Protecting a novel, superior manufacturing process for the API or a key intermediate, without necessarily claiming the compound itself. Process patents do not block a generic from making the same compound by a different route, but they add to the overall litigation burden and can prevent a generic from using the most efficient manufacturing method.
Tier 3: Low Clinical Value, Legally and Politically Vulnerable
Minor formulation changes without clinical differentiation: Filing formulation patents for changes that offer no measurable patient benefit – a new tablet color, a marginal change in excipient composition, or a film coating on an already-approved tablet. These patents are often rejected during prosecution and routinely invalidated during Paragraph IV litigation. They generate significant negative press.
Dosage strength proliferation: Adding new dosage strengths of an approved drug without clinical data justifying the new strengths, with the primary goal of ensuring Orange Book coverage at multiple dose points. FDA has been increasingly resistant to approving dosage strengths whose primary purpose is defensive IP filing.
Disease sub-classification patents: Filing method-of-use patents that claim the same treatment in a slightly narrower or differently defined patient population than the approved indication – for example, moving from ‘Type 2 diabetes’ to ‘Type 2 diabetes in patients with ASCVD’ – without substantive new trial data. These face a high obviousness rejection risk.
The Regulatory Response to Aggressive Evergreening
The FDA, the EMA, and national health technology assessment bodies have all implemented structural responses to aggressive lifecycle management. The FDA’s Purple Book and Orange Book are subject to active scrutiny by the FTC, which has pursued multiple pharmaceutical companies for maintaining overbroad or improperly listed patents in the Orange Book. A 2023 proposed FDA rule would tighten the criteria for Orange Book patent listing, requiring a direct connection between the listed patent and the approved drug product.
The IRA’s (Inflation Reduction Act) drug price negotiation provisions, while targeted at high-cost therapeutics, are creating structural pressure on lifecycle management strategies that rely on minor innovations to extend pricing power – a trend that will materially affect the commercial return on Tier 2 and Tier 3 tactics.
Key Takeaways: Evergreening
The commercial and legal sustainability of a lifecycle management program correlates directly with the clinical quality of the underlying innovation. Tier 1 tactics – genuine repurposing, superior formulations, synergistic combinations – generate defensible IP, pass regulatory scrutiny, and support the payer value narrative. Tier 3 tactics are increasingly costly to execute given FTC oversight, Orange Book reform, and IRA pressure, and the return on defensive patent filing without clinical substance is declining. IP teams advising executive leadership should recalibrate lifecycle management budgets away from tactical patent proliferation and toward funded clinical programs that generate both IP and clinical differentiation simultaneously.
The 505(b)(2) Pathway: Mechanics, Exclusivities, and Commercial Strategy
Statutory Architecture and the Hatch-Waxman Foundation
The 505(b)(2) pathway was created by Section 101 of the Drug Price Competition and Patent Term Restoration Act of 1984 – the Hatch-Waxman Amendments – and is codified at 21 U.S.C. § 355(b)(2). The pathway permits an NDA applicant to rely, for the purpose of demonstrating safety and/or efficacy, on data from studies not conducted by or for the applicant, provided the applicant has a legal right to reference them. The two primary categories of referenced data are published scientific literature and the FDA’s prior findings of safety and effectiveness for an already-approved drug – the ‘reference listed drug’ (RLD).
The pathway is not a shortcut on efficacy. Every 505(b)(2) application still requires the sponsor to demonstrate that the new drug product is safe and effective for its proposed use. What the pathway eliminates is the obligation to duplicate preclinical and clinical investigations that have already been conducted. The FDA has extensive discretion in determining what studies are required to bridge the existing data to the new product, which creates both opportunity and uncertainty.
The Scientific Bridge: The Core Technical Challenge
The scientific bridge is the evidentiary package that justifies reliance on external data. Its scope varies dramatically by product type:
For a new indication for an approved oral drug at the same dose and formulation, the bridge may require only a targeted review of existing pharmacokinetics and a full Phase II/III efficacy program in the new indication. The safety reliance is strong because the systemic exposure is identical; the new data requirement is confined to proof of efficacy.
For a new formulation (immediate-release to extended-release), the bridge typically requires comparative PK studies demonstrating that the new formulation achieves equivalent or superior drug exposure over a relevant dosing interval, combined with a safety comparison to characterize any new toxicity signals associated with the changed release profile. Efficacy data from the new trial may be required if the PK profile differs substantially from the RLD.
For a new route of administration (oral to injectable), the bridge is most demanding. The FDA will typically require comprehensive PK bridging data, reformulation safety studies, and often a full Phase III efficacy trial, particularly if the disease indication is also changing. In these cases, the 505(b)(2) advantage over a full 505(b)(1) may be limited to reliance on existing preclinical toxicology, saving 2-3 years of discovery work but not the full 5-7 year claim.
The practical error most companies make is treating the bridge design as a regulatory afterthought rather than the central scientific task of the 505(b)(2) program. Early pre-IND meetings with the FDA to align on the scope and acceptability of the proposed bridge are not optional; they are the single highest-return investment in the development program, because misalignment discovered during the NDA review cycle can trigger a Complete Response Letter that costs 18-24 months.
Market Exclusivity: The Full Taxonomy
The 505(b)(2) pathway can generate up to four distinct types of market exclusivity, each operating on different legal grounds and offering different degrees of commercial protection:
3-Year New Clinical Investigation Exclusivity: Granted when the approval relies on new clinical investigations (other than bioavailability studies) conducted by or for the applicant that were essential for the approval. During these three years, the FDA cannot approve a 505(j) ANDA or a 505(b)(2) that relies on the applicant’s data for the same condition of use. This is the standard exclusivity for new indications, new formulations, and new combinations. It does not prevent a competitor from conducting their own independent clinical program and filing their own 505(b)(2).
5-Year New Chemical Entity Exclusivity: Available if the NDA contains an active moiety that has never been approved in any form by the FDA. This is rare in classic repurposing (where the drug is by definition approved) but applies to shelved compounds that never reached market – a biologically active metabolite of an approved drug, or a pure enantiomer of a racemic drug, may qualify. The 5-year NCE exclusivity blocks both ANDA and 505(b)(2) filings that reference the new NCE, though a Paragraph IV challenge can be filed after four years.
7-Year Orphan Drug Exclusivity (ODE): Available when the drug is approved for a designated rare disease indication. ODE is the most powerful exclusivity available on the 505(b)(2) pathway – it blocks approval of ‘the same drug’ for ‘the same rare disease’ for seven years, regardless of patent status. ODE operates independently of the patent system and is conferred by regulatory law, not intellectual property law.
6-Month Pediatric Exclusivity: A statutory extension appended to any existing exclusivity or patent when the sponsor completes FDA-requested pediatric studies. As with Pfizer’s use of pediatric exclusivity on sildenafil, this six-month add-on is one of the highest-return investments in pharmaceutical development when applied to a large-revenue asset.
The 505(b)(2) Landscape: Approval Trends and Therapeutic Distribution
The therapeutic distribution of 505(b)(2) approvals has shifted materially over the past decade. Through the early 2010s, the pathway was dominated by reformulations of established drugs in cardiovascular and CNS indications. By 2024, the mix has broadened: oncology accounts for approximately 22% of approvals, CNS/psychiatry for 18%, and endocrinology/metabolics for 14%. Rare disease and orphan indications collectively represent approximately 31% – a figure reflecting the strategic alignment of 505(b)(2) with Orphan Drug Designation as complementary exclusivity mechanisms.
A critical emerging trend is the use of 505(b)(2) for generic drug repurposing – specifically, the approval of new indications for drugs whose composition patents have already expired. FDA guidance from 2023-2024 has attempted to address the regulatory pathway for non-manufacturer-sponsored applications (academic institutions, non-profits), though the structural barriers discussed in the EU context below apply in modified form in the U.S. system as well.
Key Takeaways: 505(b)(2)
The 505(b)(2) pathway’s commercial value is determined more by exclusivity strategy than by development cost savings. A company that files a 505(b)(2) and earns only 3-year new clinical investigation exclusivity, without orphan designation or pediatric extension, has a relatively narrow commercial window. The highest-return 505(b)(2) programs pair the application with: (a) orphan designation for a rare disease sub-population, securing 7-year ODE; (b) a pediatric program generating an additional 6-month extension; (c) a Breakthrough Therapy or Fast Track designation that accelerates review; and (d) an Orange Book patent listing that requires any ANDA filer to certify against each listed patent. This exclusivity stack, executed correctly, can create 10-12 years of protected commercial life for a drug whose base composition patent has expired.
Investment Strategy: 505(b)(2) Portfolio
Investors screening for 505(b)(2) pipeline value should focus on three indicators. First, is the application paired with orphan designation? The seven-year ODE creates a commercial window that justifies higher revenue multiples regardless of the underlying patent position. Second, has the company completed a pre-NDA meeting with FDA alignment on the bridge scope? Applications lacking documented FDA alignment on the bridge are subject to material CRL risk. Third, does the Orange Book listing include patents with remaining terms longer than the base 3-year exclusivity period? If formulation or combination patents extend beyond the exclusivity window, the effective exclusivity period can be materially longer than the statutory minimum.
The EMA Framework: Structure, Pilot Failures, and the MAH Veto
Directive 2001/83/EC and the EU Regulatory Architecture
The EU’s regulatory basis for drug repurposing is Directive 2001/83/EC on the Community code relating to medicinal products for human use. Unlike the FDA’s single 505(b)(2) vehicle, the EU framework offers multiple procedural routes depending on the drug’s approval status, the nature of the new indication, and whether the applicant is a commercial Marketing Authorisation Holder (MAH) or a non-commercial entity.
The primary commercial pathways for adding a new indication to an existing marketing authorisation are: (a) a Type II variation for a significant change to the authorized terms, including a new indication – this requires submission to the EMA or national authorities and typically takes 12-18 months from submission to decision; (b) a new marketing authorisation application relying on the Established Active Substance (EAS) provision, available when the drug has been in authorized use in the EU for at least 10 years and there is published scientific literature supporting the new application; and (c) the new indication with significant clinical benefit, which triggers the one-year market protection extension under the ‘8+2+1’ framework.
The ‘8+2+1’ Exclusivity Framework: Full Mechanics
The EU data and market exclusivity framework runs on a defined timeline that operates concurrently with, but independently of, patent protection. The three components are:
Eight-year data exclusivity: From the date of initial marketing authorisation, the applicant’s preclinical and clinical data are protected from reference by third parties. A generic manufacturer cannot rely on this data to support its own application during this period. Data exclusivity runs from first authorisation in any EU member state, regardless of the route of application.
Two-year market protection: After the eight-year data exclusivity period, a generic applicant may submit an application referencing the originator’s data, and the EMA may review and grant a marketing authorisation. But the generic product cannot be placed on the EU market until the full 10-year protection period expires. This creates a two-year ‘dossier evaluation window’ in which competitive preparation proceeds but commercial competition cannot begin.
One-year new indication extension: The 10-year period extends to 11 years if the marketing authorisation holder obtains one or more new therapeutic indications during the first eight years of the drug’s authorisation that, in the view of the scientific assessment, bring a ‘significant clinical benefit’ compared to existing therapies. This extension applies once, regardless of how many new indications are approved. The ‘significant clinical benefit’ threshold is assessed by the CHMP and requires either a clear improvement in clinical outcomes (survival, response rate, quality of life) or a meaningful advance for patients who have no adequate existing treatment options.
For a repurposing strategist, the one-year extension is the EU’s primary commercial incentive for indication expansion. Its limitations are significant compared to the U.S. orphan drug exclusivity: it is only one year (versus seven in the U.S.), it requires the benefit assessment to meet a ‘significant’ threshold rather than just demonstrating effectiveness, and it only applies during the first eight years of the drug’s authorized life.
The EMA Pilot Program: What the 2025 Report Actually Found
The EMA/HMA pilot program for repurposing, launched in 2021, was designed to test whether non-commercial champions (academic institutions, patient advocacy organizations, research hospitals) could navigate the EU regulatory system to obtain a marketing authorisation for a new indication of an off-patent, genericized medicine, with agency support.
The program’s July 2025 report is candid about the outcome. Of the applications that entered the pilot, a meaningful proportion failed to reach the submission stage, and none had obtained final marketing authorisation at the time of reporting. The EMA’s own assessment identified several primary failure modes:
The scientific evidence package problem: Academic champions consistently struggled to translate their trial data into a regulatory-standard benefit-risk dossier. The scientific literature that demonstrates a drug’s activity in a new disease is not the same as a regulatory submission. Synthesizing heterogeneous trial data, addressing confounders in retrospective analyses, and constructing a formal risk management plan require skills that academic institutions generally do not have in-house.
Clinical trial design deficiencies: Multiple programs in the pilot had executed trials that lacked the endpoints or patient stratification criteria required for a regulatory benefit-risk assessment. Primary endpoints that are academically accepted (biomarkers, surrogate endpoints without established regulatory precedent) are often rejected as inadequate bases for a marketing authorisation. This reflects a structural gap between what academic researchers design trials to demonstrate and what regulators require.
The MAH engagement failure: This is the structural issue. Under current EU law, only the MAH – the commercial entity holding the marketing authorisation – can submit a variation to add a new indication to the authorised terms. Academic champions cannot submit independently. In the pilot, engaging MAHs of generic medicines proved extremely difficult: generic manufacturers have no commercial incentive to fund the Type II variation process (estimated cost: €500,000 – €2 million per application) for an indication where the drug is off-patent and any competitor can benefit from the label change. The MAH’s investment, if successful, would immediately become a public good.
The MAH Veto: Structural Problem and Proposed Solutions
The ‘MAH Veto’ – the inability of non-commercial sponsors to submit applications for new indications without MAH cooperation – is the single most significant structural barrier to publicly-funded drug repurposing in the EU. An academic team may hold Phase III data demonstrating efficacy, have received favorable scientific opinions from CHMP, and still be legally unable to change the drug’s label.
Several proposed solutions are under active discussion in EU pharmaceutical legislation reform, including: creating a ‘non-commercial authorisation’ pathway that allows academic sponsors to obtain a separate, parallel marketing authorisation for the new indication without relying on the existing MAH; establishing a compulsory variation mechanism under which the EMA or national competent authorities can require an MAH to submit a variation when there is strong public health evidence supporting a new indication; and creating a government-funded filing intermediary that acts as a de facto MAH for off-patent repurposing applications.
As of 2025, none of these solutions are codified in EU law, though the European Medicines Legislation revision process (2023-2026) includes active proposals on some of these mechanisms. The resolution of the MAH veto question is the single most important regulatory development to track for anyone invested in academic-led or non-profit-funded repurposing programs in Europe.
EMA vs. FDA: Side-by-Side Strategic Comparison
| Dimension | FDA | EMA |
|---|---|---|
| Primary repurposing pathway | 505(b)(2) NDA | Type II variation; EAS pathway |
| Base exclusivity for new indication | 3-year new clinical investigation | 1-year extension of 10-year protection |
| Orphan exclusivity | 7 years (same drug, same indication) | 10 years (orphan medicines) |
| Non-commercial sponsor pathway | No formal mechanism; commercial partner required | Pilot program (limited success); reform proposals pending |
| MAH requirement | No formal barrier; any sponsor can file a 505(b)(2) | MAH must submit variation; non-MAH sponsors legally blocked |
| Scientific bridge concept | Explicit; required for reliance on RLD data | Less explicitly defined; literature-based applications under EAS |
| Pediatric extension | 6 months (BPCA) | 2 years Paediatric Regulation, varies by product |
| Regulatory timeline (typical) | 10-12 months (standard); 6 months (priority review) | 12-18 months for Type II variation |
Key Takeaways: EMA Framework
For companies pursuing a global repurposing strategy, the U.S. 505(b)(2) approval is typically the faster and more commercially significant pathway. EU authorization should proceed in parallel but requires engagement with an EU MAH from the outset – either the company itself holds the EU marketing authorisation, or a commercial partner must be secured. For off-patent drugs where no EU MAH has commercial incentive to file, the MAH veto creates a structural dead end unless EU legislative reform creates an alternative pathway. Non-profit sponsors considering EU-based repurposing programs should factor the cost of MAH engagement – including, potentially, the cost of establishing a commercial entity to hold the EU authorization – into their planning assumptions.
Orphan Drug Act: The Patent-Independent Monopoly
The ODA’s Commercial Logic: Converting Public Health Policy Into Market Exclusivity
The Orphan Drug Act of 1983 was enacted to correct a documented market failure: the pharmaceutical industry had no financial incentive to develop treatments for diseases affecting fewer than 200,000 U.S. patients. The Act created that incentive by granting a seven-year market exclusivity upon FDA approval – a government-authorized monopoly that operates entirely outside the patent system.
For repurposing strategy, this is the critical insight: Orphan Drug Exclusivity (ODE) does not require patent protection. A company can take a generic molecule with zero remaining patent life, demonstrate its effectiveness in a rare disease, obtain FDA approval, and receive seven years during which the FDA legally cannot approve another application for ‘the same drug’ for ‘the same rare disease.’ For the strategist working with off-patent assets – where the patent toolkit is unavailable or inadequate – ODE is the primary commercial mechanism, and the ODA is the most consequential piece of legislation in the repurposing field.
Qualifying Criteria and the Prevalence Threshold
A disease qualifies for orphan designation under the ODA if it affects fewer than 200,000 patients in the United States, or if it affects a larger population but there is no reasonable expectation that sales will recover the costs of development and marketing. The 200,000-patient threshold is stricter than the EU’s equivalent (affecting fewer than 5 in 10,000 EU residents, approximately 250,000 patients), which means certain diseases qualify for EU orphan designation but not U.S. ODD.
Prevalence data for the designation application comes from multiple sources: National Institutes of Health databases, disease registries (both FDA-supported and patient advocacy-managed), published epidemiological studies, and de-identified insurance claims databases. The quality and recency of prevalence data matter: the FDA’s OOPD will scrutinize prevalence estimates that appear to have been constructed to fall below the 200,000 threshold. Applications relying on narrow disease sub-definitions to hit the prevalence cutoff – for example, defining a common cancer type by a specific genetic sub-variant rather than the full indication – are subject to enhanced scrutiny.
The Full Incentive Package
ODD from the FDA’s OOPD provides five categories of benefit prior to approval and upon approval:
Seven-year market exclusivity upon approval: The crown incentive. The FDA cannot approve another sponsor’s application for the same drug for the same rare disease for seven years from the original approval date. ‘Same drug’ is defined as the same active moiety; enantiomers, metabolites, and structural analogues are generally considered the ‘same drug’ unless the sponsor can demonstrate clinical superiority. ‘Clinical superiority’ requires proof of greater effectiveness, greater safety, or a major contribution to patient care compared to the previously approved orphan drug.
50% tax credit for qualified clinical testing expenses: Expenses incurred for clinical trials testing the orphan drug in the U.S. qualify for a tax credit of up to 50% (currently reduced from the original 50% to 25% under the Tax Cuts and Jobs Act of 2017, then restored to 25%). For a $50 million Phase III program, this represents up to $12.5 million in direct tax recovery – meaningful but not the primary financial driver.
Waiver of PDUFA application fees: The NDA user fee for a standard review application in fiscal year 2025 is approximately $4.3 million. Orphan drugs are exempt. For small companies filing their first NDA, this waiver is significant.
Fast Track and Accelerated Approval eligibility: Many orphan drugs qualify for Fast Track designation (rolling review of NDA sections as completed), which can reduce the cumulative review timeline by 6-12 months.
OOPD grant funding: The FDA administers a grant program specifically for orphan drug clinical development. Grant awards range from $200,000 to $500,000 per year for up to four years. These are non-dilutive capital sources that, while modest relative to full development costs, meaningfully offset early Phase II expenses for small biotechs or academic teams.
‘Salami Slicing’ and Strategic Sub-Indication Management
Because ODE is indication-specific, it is legally possible to obtain multiple seven-year exclusivity periods for the same drug by developing it in multiple distinct rare diseases. Critics call this ‘salami slicing’ – deliberately pursuing narrow, related indications to accumulate sequential ODE periods rather than seeking a single broader approval.
The practice has generated congressional scrutiny and multiple reform proposals. The 2017 FDA Reauthorization Act included provisions requiring the FDA to clarify when related indications would be considered the ‘same’ disease for ODE purposes. In practice, the FDA’s approach has been case-specific: the same drug can obtain separate ODE for Type 1 and Type 2 variants of a rare disease if the clinical presentations, disease mechanisms, and trial populations are genuinely distinct. If a company files for ‘aggressive B-cell lymphoma’ and separately for ‘diffuse large B-cell lymphoma’ – a histological subtype of aggressive B-cell lymphoma – the FDA is likely to treat these as the same disease.
The ‘Bridge Drug’ Strategy: From Orphan to Blockbuster
The most commercially ambitious application of the ODA is the orphan-to-mainstream sequence: obtain ODE for a rare disease sub-indication, use the exclusivity window to generate safety and commercial infrastructure, then conduct trials in the larger indication and pursue label expansion without needing ODE renewal for the mainstream use.
Ibrutinib (Imbruvica) is the defining case. Initial FDA approval came in 2013 for mantle cell lymphoma (MCL), a rare lymphoma with approximately 4,000 new U.S. cases annually – comfortably within orphan prevalence thresholds. Ibrutinib subsequently received approvals for chronic lymphocytic leukemia (CLL), the most common adult leukemia, and for several additional indications. CLL alone generates over 20,000 new U.S. cases annually and contributes the majority of ibrutinib’s approximately $9 billion in peak annual global sales. The ODA incentives were awarded for a genuinely rare disease application, but the commercial outcome was a near-blockbuster.
This sequence is legal and has generated significant patient benefit by funding development that might not have been commercially viable starting from a CLL indication alone. Its critics argue that it is contrary to the ODA’s intent to redirect incentives toward commercially non-viable diseases.
Key Takeaways: Orphan Drug Act
ODE is the most powerful exclusivity mechanism available to repurposing programs working with off-patent molecules. The seven-year term provides commercial certainty that no patent can match for generic APIs. IP teams should routinely screen any new repurposing target against the 200,000-patient prevalence threshold before committing to a commercial strategy: a rare disease sub-population identification can transform a commercially marginal project into an investable asset. The ‘salami slicing’ risk is manageable with careful disease definition and early engagement with OOPD on the scope of the proposed indication.
Investment Strategy: Orphan Drug Assets
Investors should apply two filters to orphan-designated repurposing assets. First: what is the probability that the same drug achieves approval in a common disease indication within the seven-year ODE window, and has the sponsor already filed an IND for the common disease trial? If yes, the ODE period is funding the commercial build for a substantially larger market opportunity. Price the asset accordingly. Second: how tightly defined is the rare disease indication? Narrowly defined indications with strong patient registry data and clear clinical endpoints represent lower ODE invalidation risk and higher probability of approval within the ODE window.
Case Studies: Three Lessons in IP Execution
Sildenafil: The Full IP Timeline
[See detailed IP valuation in Section 4. The key analytical lesson is the managed patent cliff: Pfizer engineered the generic entry timeline rather than surrendering to it. The Paragraph IV settlement with Teva, the pediatric exclusivity extension on the Revatio program, and the authorized generic launch via Greenstone were not independent tactical moves but a sequenced strategy designed to maximize total franchise NPV across a 15-year period following the original patent filing.]
What the case demonstrates for IP practitioners: the patent is not the commercial asset – the managed exclusivity timeline is. A sophisticated IP team treats each patent as a lever, not a wall. The settlement value of a Paragraph IV dispute is the probabilistic average of two outcomes: full patent life if the patent survives challenge, versus invalidation and immediate generic entry if it does not. When the risk-adjusted value of the settlement (early generic entry plus royalties) exceeds the expected value of full patent life less litigation cost and invalidation risk, settlement is the economically correct decision. Pfizer’s Teva settlement is a textbook example of this calculation.
Thalidomide: Regulatory Infrastructure as the Moat
Thalidomide’s commercial success in multiple myeloma was not built on IP. It was built on the S.T.E.P.S. REMS program – a mandatory risk management architecture that functions as a regulatory moat independent of patents. No generic manufacturer can distribute thalidomide without implementing a REMS program that satisfies the FDA’s requirements, and the FDA requires the REMS program to be shared between the innovator and any generic entrants. In practice, the administrative cost of REMS implementation, combined with Celgene’s willingness to negotiate access agreements rather than litigate, created a commercial structure that delayed meaningful generic erosion for several years.
The thalidomide case is also instructive for the discovery-to-IP pipeline. Dr. Jacob Sheskin’s 1964 clinical observation of ENL improvement was not patented because there was no commercial framework at the time to do so. Decades of academic use of thalidomide for leprosy generated published literature that established prior art for the ENL indication – making a method-of-use patent for that application essentially unobtainable by the time Celgene sought FDA approval. Celgene’s commercial position in thalidomide therefore rested entirely on: (a) the REMS moat; (b) the orphan drug exclusivity for ENL and then myeloma; and (c) the composition-of-matter patents on the structural analogues lenalidomide and pomalidomide, which were genuine NCEs and which carried the franchise’s primary patent value.
Lesson: when primary IP is unavailable, regulatory infrastructure (REMS, manufacturing requirements, specialized distribution networks) can provide commercial protection that is, in some market contexts, more durable than a patent.
Losartan for DMD: The Preclinical Translation Failure
The failed attempt to repurpose losartan for skeletal muscle preservation in Duchenne muscular dystrophy (DMD) offers the most specific preclinical validity lesson in the repurposing literature. The program’s failure was not random – it was predictable in retrospect from the specific limitations of the mdx mouse model used to generate the initial efficacy data.
The mdx mouse has a dystrophin gene mutation analogous to DMD and develops skeletal muscle pathology, but it has a significantly milder clinical course than human DMD. In young mdx mice, the TGF-β pathway targeted by losartan is a dominant driver of early fibrosis. In aged mdx mice, representing the chronic disease state that corresponds to the patient population in a clinical trial, the fibrotic disease had progressed past the therapeutic window for TGF-β inhibition: redundant fibrotic pathways (CTGF, lysyl oxidase, galectin-3 upregulation) had become dominant, and losartan’s mechanistic target was no longer rate-limiting.
The clinical and IP lesson is direct. Every repurposing program that relies on animal model efficacy data should, before Phase I filing, conduct an explicit therapeutic window analysis: at what stage of human disease is the targeted mechanism most active, and does the proposed patient population correspond to that stage? Programs that enroll patients beyond the therapeutic window of their mechanism will fail regardless of how clean the earlier data looked. IP teams should factor this risk into Paragraph IV and licensing valuation models: a preclinical package based exclusively on young-animal data, for a chronic progressive disease, deserves a material validity discount.
Competitive Intelligence: Patent Data as a Strategic Weapon
The 18-Month Disclosure Window: Trading in Future Knowledge
Patent applications are published 18 months after their earliest priority date as a matter of law, under 35 U.S.C. § 122(b). This creates a predictable, legally mandated disclosure timeline that pharmaceutical competitive intelligence functions can exploit systematically. A competitor’s new MoU patent application, published 18 months after filing, reveals the existence of a repurposing program that will not be publicly disclosed through any other channel for potentially another two to three years.
For the monitoring team, this 18-month disclosure window is the primary source of pre-competitive signal in pharmaceutical R&D. A company that builds an automated surveillance system on patent publication feeds for relevant therapeutic areas, biological targets, and competitor assignee names will consistently have 18 months of advance notice on competitor program initiation – enough time to run a FTO analysis, adjust in-licensing priorities, and, if warranted, initiate a competing program with a parallel filing.
Building the Surveillance Architecture
An effective patent intelligence function for repurposing programs requires four components:
Automated search and alert infrastructure: Subscriptions to patent database platforms capable of monitoring publication feeds across USPTO, EPO, WIPO, and national patent offices in relevant markets. Search parameters should be built around multiple axes simultaneously: therapeutic area keywords, IPC/CPC classification codes specific to relevant drug classes, competitor assignee names, and target molecule names. DrugPatentWatch provides curated pharmaceutical patent data with structured expiration tracking and Orange Book integration, enabling rapid correlation of patent filings with regulatory submissions.
Expert claim analysis: Automated monitoring generates raw signal; turning that signal into intelligence requires expert claim analysis. When a new application appears for a competitor’s established small molecule in a novel indication context, a patent attorney with pharmaceutical experience needs to assess: the breadth of the claims, the likely prosecution history, the quality of the enablement, and the probability that the claims as drafted will survive examination. A broadly drafted, poorly enabled application is a weaker competitive signal than a narrow but well-supported one.
Cross-source triangulation: Patent filings become actionable intelligence when triangulated with other data sources. A competitor’s new MoU patent application for Compound X in Indication Y, if followed within six months by a ClinicalTrials.gov registration of a Phase II trial for that indication, is a confirmed program. If accompanied by an SEC Form 10-Q reference to a ‘lifecycle management initiative’ and a partnership announcement with an academic medical center in that disease area, it becomes a confirmed, well-resourced program – a five-alarm competitive signal.
Failure landscape mapping: Competitor patent applications that are followed by abandonment, or that are not accompanied by clinical trial registration within three to five years, map the failure landscape. The experimental data disclosed in abandoned applications represents negative evidence: the approaches that did not work, the dose ranges that proved toxic, the patient populations that did not respond. This negative data is freely available to any researcher reading the published application and can save substantial research budget by eliminating failed approaches before they are repeated.
Freedom-to-Operate Analysis: Non-Negotiable Pre-Investment Work
Freedom-to-operate (FTO) analysis for a repurposing program requires mapping not only the patents directly claiming the new use, but also the entire landscape of potentially blocking IP across five categories: method-of-use patents for the same or overlapping disease indications, formulation patents that cover any contemplated delivery system, combination patents that include the API as a component, process patents that cover manufacturing steps, and diagnostic or companion diagnostic patents that may be required for patient selection in the new indication.
The last category is frequently overlooked. In oncology repurposing programs where the target patient population is defined by a biomarker (e.g., a specific mutation or protein expression level), the diagnostic test required to identify that patient population may itself be covered by a patent that requires licensing. CDx patents in oncology have become a significant FTO factor, particularly as precision medicine sub-population targeting becomes standard in regulatory strategy.
AI and Computational Repurposing: From Signal to Patent
The Four Core Computational Platforms
Computational repurposing discovery platforms operate across four primary methodological categories, each with distinct data requirements, output types, and patent implications:
Transcriptomic signature inversion (Connectivity Map / CMAP methodology): This approach compares drug-induced gene expression profiles (‘drug signatures’) against disease-associated gene expression profiles. If a drug induces a gene expression pattern that is the inverse of a disease’s signature, the drug may restore a diseased cell state toward normal. The methodology was pioneered by the Broad Institute and is now implemented by multiple commercial platforms (Recursion Pharmaceuticals, BioMap/Chemspace) at genome-scale. The IP implication of signature-inversion discoveries is strong: the biological pathway connection identified by the algorithm is genuinely non-obvious because it depends on the global pattern of thousands of gene expression changes, not a linear mechanism-of-action argument. This multi-dimensional, algorithm-derived evidence base supports non-obviousness claims in patent prosecution.
Network biology and protein interaction network analysis: Disease targets rarely operate in isolation. Network-based platforms (notably the work of Albert-László Barabási’s group at Northeastern and its commercial successors) model the protein-protein interaction network of a disease module and identify existing drugs that hit key nodes within that network. The IP value here depends on whether the network connection was previously described in literature. If a drug’s known targets are already published as part of the disease pathway, the network finding may face an obviousness challenge even if the computational approach is novel. Patent applications based on network analysis require careful prior art analysis of published pathway literature.
Deep learning for drug-target interaction prediction: Structure-based deep learning models (AlphaFold-integrated platforms, Schrödinger’s FEP+ pipeline, Insilico Medicine’s generative chemistry tools) predict interactions between a drug’s 3D structure and target proteins in the disease-relevant proteome. When such a model predicts an interaction between a known drug and a previously unidentified target relevant to a new disease, the off-target binding hypothesis is the source of patentable novelty. The patent strategy here focuses on the specific drug-target binding interaction and its therapeutic consequence, not the general repurposing concept.
Real-world evidence mining: EHR and insurance claims datasets (IQVIA’s MIDAS, Optum’s Clinformatics, IBM MarketScan) contain longitudinal treatment and outcome data for tens of millions of patients. Statistical algorithms that identify unexpected treatment associations – for example, a significantly lower incidence of a specific disease in patients chronically taking a drug approved for a different indication – generate real-world hypothesis signals that are both clinically credible and highly non-obvious. FDA and EMA have both issued guidance accepting RWE as supporting evidence in certain regulatory contexts, though RWE alone is never sufficient for approval.
AI as a Non-Obviousness Engine: The Patent Application Strategy
The computational source of a repurposing discovery is directly relevant to patent prosecution. U.S. patent law under 35 U.S.C. § 103 requires that an invention not be obvious to ‘a person having ordinary skill in the art’ (PHOSITA) at the time of the invention. The PHOSITA standard is a hypothetical construct that patent examiners and courts use to assess whether the claimed invention would have been predictable from the existing knowledge base.
An AI-generated hypothesis that connects a drug to a disease through a mechanism identified by pattern recognition in a multi-million-data-point dataset is, by its nature, non-obvious. The PHOSITA could not have arrived at the same hypothesis through routine experimentation or through reading the existing literature, because the connection only becomes visible through large-scale computational analysis. This constitutes strong evidence of non-obviousness.
The patent application strategy for AI-driven repurposing discoveries should therefore include: a detailed description of the computational method that generated the hypothesis, as part of the specification; experimental validation data (cell assay, animal model, or early clinical data) that confirms the predicted therapeutic activity and provides the ‘unexpected results’ evidence that strengthens the non-obviousness argument; and claims that specifically cover the therapeutic use identified by the AI analysis, drafted narrowly enough to be enabled by the validation data but broadly enough to capture the commercial value.
Personalized Repurposing: The Biomarker-Companion Diagnostic Pathway
The next generation of repurposing strategy moves beyond ‘new indication for old drug’ to ‘new indication in biomarker-defined sub-population.’ AI platforms trained on multi-omics patient data (genomics, transcriptomics, proteomics, metabolomics combined) can identify specific molecular signatures that predict response to a drug in a sub-population of patients with a common disease.
This precision repurposing approach changes the regulatory and IP strategy in two important ways. Clinically, it allows smaller, faster trials (enrolling only biomarker-positive patients) with higher response rates, reducing the cost and risk of Phase II/III. Commercially, it creates a co-development opportunity for a companion diagnostic (CDx) that identifies the biomarker-positive patient population. The CDx patent estate becomes a second, separate IP asset that must be licensed by any competitor seeking to use the biomarker for patient selection.
The FDA’s approval framework for CDx-linked drugs under the Breakthrough Therapy and BLA pathways is now well-established in oncology (EGFR testing for erlotinib in NSCLC, PD-L1 testing for pembrolizumab, BRCA testing for olaparib). The same framework is being extended to repurposing programs. A repurposed drug plus CDx combination that receives FDA approval with a biomarker-restricted label creates a differentiated product with both a drug IP position and a diagnostic IP position – a significantly stronger commercial structure than a drug alone.
Key Takeaways: AI and Computation
Computational repurposing platforms generate the three things a viable repurposing program requires: a non-obvious discovery (supporting IP); a biological mechanism (supporting clinical development rationale); and patient stratification insight (enabling precision trial design and CDx co-development). Companies that deploy these platforms as integrated R&D tools – not just hypothesis generators requiring validation years later – will have a structural advantage in both speed-to-IND and strength of IP position. The patent filing should follow within weeks of the first experimental validation of an AI-generated hypothesis, using the computational provenance as evidence of non-obviousness in the prosecution record.
Investment Strategy: Portfolio Construction for Repurposing Assets
Drug repurposing assets require a specific valuation framework that differs materially from standard pipeline analysis. The following represents a structured approach for institutional investors and corporate M&A teams.
The Five-Factor Valuation Model
IP Layer Depth (0-5 scale): Score one point for each of the following present in the asset’s IP estate: a granted MoU patent with a remaining term exceeding five years; a formulation patent covering the specific delivery system used in the repurposed application; a combination patent covering co-administration with a standard-of-care agent; Orange Book listing with Paragraph IV history showing at least one prior successful defense; and a pending or granted pediatric exclusivity extension. Maximum score: 5. An asset scoring 4-5 warrants a premium valuation multiple relative to similar-revenue assets with weaker IP.
Exclusivity Stack Value: Independently calculate the commercial value of each exclusivity mechanism: (a) remaining ODE period if applicable, discounted by the probability that a clinical superiority challenge succeeds; (b) remaining base NDA exclusivity (3-year new clinical investigation); (c) remaining Orange Book patent terms; and (d) REMS or restricted distribution program that adds operational complexity barriers to generic entry. Sum these values with appropriate discounting. A strong exclusivity stack covering 8-12 total years is the primary commercial driver for generic drug repurposing.
Bridging Study Risk: Assess whether pre-NDA FDA alignment on the bridge scope is documented. Undocumented bridge scope is a binary CRL risk. Assign a 20-30% probability reduction to the approval probability for assets without documented FDA alignment. For assets in Phase III with accepted bridge plans, this risk is substantially resolved.
Indication Expansion Optionality: Does the new indication sit within a common disease category where the same drug could pursue label expansion beyond the rare disease or specific sub-indication that anchors the current program? Ibrutinib’s value creation from MCL to CLL to other hematological malignancies is the most extreme case. Value this optionality using a real options framework rather than a simple DCF, since the expansion probability is highly dependent on emerging trial data and FDA labeling decisions that are not fully deterministic.
Competitive Landscape and Paragraph IV Exposure: How many ANDA filers are expected, and what is the typical time from ANDA filing to first generic launch in this therapeutic category? For assets with weak formulation IP and only MoU protection, model immediate generic erosion as the base case and treat the MoU patent as a ‘call option’ that extends commercial life only if litigation is successful.
Acquisition Premium Benchmarks
Based on M&A transactions in the 2020-2025 period involving repurposed drug assets, the following premium structures have been observed: assets with a 5-factor IP score of 4-5 and ODE remaining have traded at 8-12x peak annual revenue; assets with standard 3-year exclusivity and a 3-factor IP score have traded at 4-6x peak revenue; assets with only a MoU patent and no formulation or combination protection have traded at 2-4x peak revenue.
The discount for weak IP is larger than intuition suggests because the revenue volatility associated with early generic entry is highly punished by acquirer DCF models. A drug with predictable 10-year exclusivity and moderate sales has higher M&A value than a drug with large but volatile sales at risk from immediate generic erosion.
Master FAQ for IP and Regulatory Teams
Q: Our company is repurposing an off-patent, generic small molecule for a common disease. No composition patent exists. How do we build a commercially defensible position?
A: The answer is the formulation. If the new indication requires a specific delivery system – extended-release, targeted, or a novel administration route – that offers clinical benefits over the original immediate-release generic, develop that formulation in parallel with the clinical program, file the formulation patent before the Phase III protocol is finalized, and ensure the Phase III design incorporates the proprietary formulation as the investigational product. The clinical trial data will then support both the NDA (establishing efficacy for the new indication) and the formulation patent (demonstrating the formulation’s clinical necessity). A generic competitor’s immediate-release version cannot substitute for the patented formulation for the new indication, which closes the skinny label vulnerability and creates a defensible commercial position. Pair this with an Orphan Drug Designation if any patient sub-population qualifies under the 200,000-patient threshold, and file for 3-year new clinical investigation exclusivity. Total expected exclusivity window: 3 years plus any remaining formulation patent term, potentially 10-15 years if the formulation patent is filed early.
Q: How should a small biotech approach licensing discussions with a large pharma company for an AI-generated repurposing hypothesis with early in vitro validation?
A: At the hypothesis-only stage, the licensing position is weak: the asset has no clinical data, and the discovery is not de-risked. The correct pre-licensing sequence is: file a provisional patent application covering the MoU and any novel formulation concepts identified during the AI analysis (establishing priority date before disclosing to partners); generate in vitro and early in vivo validation data that confirms the AI prediction; conduct a ‘disease biology deep dive’ to identify the therapeutic window and optimal patient population; scope the 505(b)(2) bridge requirements with a contract regulatory consultant and document the findings. With this package in place, the licensing value is based on a de-risked hypothesis with documented IP, a defined regulatory path, and a scoped development budget. The ‘de-risking premium’ in this context is worth $20-80 million in licensing NPV terms on a mid-sized indication, versus $1-5 million for an undocumented hypothesis without validation.
Q: What is the key mistake companies make when designing a 505(b)(2) program?
A: Underinvesting in pre-IND FDA engagement on bridge scope. The FDA’s Type A and Type B meeting processes exist specifically to align on the adequacy of the proposed scientific bridge before significant development capital is committed. A Type B pre-IND meeting that results in written FDA agreement on the reliance strategy for the RLD’s safety data, the scope of required bridging PK studies, and the Phase II/III design requirements is the highest-return investment in any 505(b)(2) program. Companies that skip this step and proceed to NDA submission based on internal assumptions about FDA acceptability consistently receive Complete Response Letters requiring additional bridging studies, adding 18-36 months and $30-100 million to the program cost.
Q: A competitor has filed a MoU patent for the same indication we are targeting. Can we still develop our program?
A: A competitor’s pending or granted MoU patent does not block your development program; it affects your commercial strategy after approval. Run a FTO analysis focused on: the scope of the patent claims (are they limited to a specific dosage, route, or patient population that differs from your proposed product?); the patent’s validity (is it likely to survive a re-examination or IPR challenge on obviousness or prior art grounds?); and whether your intended formulation is covered by a separate formulation patent. If your product is a materially different formulation (extended-release versus immediate-release, for example), you may have freedom to operate commercially, and your own formulation patent can block the competitor from copying your delivery system. If the competitor’s MoU claims are broad and appear valid, consider three options: challenge validity through an IPR petition before the PTAB; design around the claims with a differentiated product; or approach the patent holder for a cross-license. Do not invest in a Phase III program for a commercial indication without a clear FTO position for the post-approval commercial product.
Q: How do we evaluate whether pursuing a Paragraph IV challenge on a repurposed drug’s patents is worth the litigation cost?
A: The standard economic model for Paragraph IV strategy weighs the expected revenue gain from early generic entry against the probability-adjusted cost of litigation and potential damages. For method-of-use patents on repurposed drugs, two factors materially increase the attractiveness of a Paragraph IV challenge relative to composition-of-matter patents: first, MoU patents face higher obviousness risk in litigation than composition patents, because the connection between the drug and the new disease is often traceable to published scientific literature even when the specific clinical application is novel; second, even if the MoU patent survives challenge, a skinny label launch may be commercially viable if a meaningful portion of prescribing physicians will substitute the generic off-label. The economic test for Paragraph IV on a repurposed drug is therefore: (litigation probability of success × early entry revenue) + (skinny label off-label substitution rate × post-launch generic revenue) minus (litigation cost + settlement risk). For formulation patents covering the proprietary delivery system, the economics are less favorable to generic challengers, which is why strong formulation IP deters Paragraph IV filings more effectively than MoU patents alone.
References and Data Sources
Data in this analysis draws on: DrugPatentWatch pharmaceutical patent and exclusivity database; FDA Orange Book, Purple Book, and PDUFA annual reports; EMA EU Repurposing Pilot Report (July 2025); Precedence Research Drug Repurposing Market Report (2024); IQVIA Institute for Human Data Science; published case studies on sildenafil, lenalidomide, esketamine, and losartan/DMD from peer-reviewed pharmacological and legal literature; USPTO and EPO patent prosecution records; FTC pharmaceutical competition reports; Celgene and Pfizer SEC filings; European Commission pharmaceutical legislation review documentation (2023-2026); Yale Journal of Law and Technology repurposing ecosystem analysis; and Duke-Margolis Center working paper on regulatory actions for generic drug repurposing (2025).
This analysis is prepared for pharmaceutical IP teams, R&D leads, and institutional investors. It does not constitute legal advice. Patent strategy, regulatory submissions, and investment decisions should be executed with qualified legal, regulatory, and financial counsel.