Key Takeaways (Executive Summary)
- Drug repurposing costs roughly $300M versus $2–3B for a novel compound and reaches market approval in 6–12 years rather than 10–15. The approval rate runs near 30% versus ~10% for new molecular entities.
- Pharmacists occupy a structurally unique position in the repurposing discovery chain — they generate real-world evidence daily without labeling it as such, and their pharmacovigilance data can feed directly into AI-driven candidate screens.
- The global drug repurposing market is forecast to reach $51.8–59.3B by 2033–2034, growing at a CAGR of 4.1–5.4%, driven by patent cliff pressure and biosimilar erosion.
- IP protection for repurposed compounds relies primarily on method-of-use, formulation, and combination patents rather than composition-of-matter claims. Patent landscape intelligence tools like DrugPatentWatch are necessary for competitive positioning.
- Regulatory pathways — specifically the 505(b)(2) NDA route and Orphan Drug Designation — provide tangible incentives: reduced clinical data requirements, extended exclusivity, and tax credits on qualifying R&D spend.
- AI/ML platforms (network pharmacology, knowledge graph mining, EHR signal detection) have become the dominant discovery method, outpacing the serendipity-driven model. Pharmacists are the clinical validation layer that keeps these AI hypotheses grounded.
- Off-label prescribing in oncology, psychiatry, and rare disease is informal drug repurposing already in progress. Systematic pharmacist surveillance of these patterns is an underexploited pipeline source.
Part I: What Drug Repurposing Actually Is — and Why the Economics Changed
Defining the Strategy: Repositioning, Reprofiling, and Repurposing Are Not Interchangeable
The industry uses three terms loosely, but each has a distinct regulatory and commercial implication.
Drug repurposing refers to identifying a new therapeutic indication for an approved compound. Regulatory agencies already recognize the safety profile; the development question is efficacy in the new context. Drug repositioning covers a slightly broader territory — it includes approved drugs, but also investigational compounds that failed Phase II or III for their original indication. The molecule has human safety data, but no approval exists yet. Drug reprofiling, used less frequently, describes the identification of new mechanisms of action for an already-marketed drug, sometimes leading to formulation or combination strategies rather than a new indication per se.
The practical difference matters enormously in IP strategy. A repurposed approved drug faces generic competition on the active molecule from day one. The innovator’s protection derives entirely from the new use patent, any novel formulation, or a proprietary combination. A repositioned investigational compound may still have patent life remaining on the active pharmaceutical ingredient, giving the developer a more defensible position. Understanding which category a candidate falls into should shape the business case before any clinical spend.

The Cost-Risk-Time Triangle: Why the Math Favors Repurposing
Traditional de novo drug development runs through five sequential stages: target identification and validation, lead optimization, IND-enabling preclinical studies, Phase I–III clinical trials, and post-market surveillance. The attrition at each gate is punishing. By the time a program exits Phase I, it has already cost $300–500M. The full pipeline to approval runs $2–3B per asset when accounting for failures, and the average cycle time is 10–15 years from first synthesis to label.
Drug repurposing bypasses the first two stages entirely and often compresses Phase I. Since an approved compound already carries an established human safety database, Phase I is either omitted or reduced to a dose-finding study for the new indication. The effective starting point is Phase II efficacy testing. That difference alone cuts development cost to roughly $300M and shrinks the timeline to 6–12 years, with some programs moving significantly faster when prior clinical data is directly applicable.
The probability of technical and regulatory success shifts accordingly. Industry data puts the probability of approval for de novo candidates at roughly 10%. For repurposed compounds with strong mechanistic rationale and existing safety data, that figure rises to approximately 30%. Combined with the lower capital at risk, the expected value per program improves by a factor of three to six depending on indication and competitive landscape.
For portfolio managers evaluating a biotech’s pipeline quality, the presence of validated repurposing programs alongside de novo assets is a material signal. It suggests capital efficiency, shorter time-to-revenue windows, and a hedge against the typical preclinical failure modes that destroy NCE programs early.
IP Valuation of a Repurposed Asset: What the Patent Estate Actually Protects
This is where many pharma business development teams undervalue or overvalue repurposed compounds. The composition-of-matter patent — which protects the molecule itself — is almost always expired or near expiration for a repurposed drug. The innovator therefore relies on a different suite of protections.
Method-of-use patents protect the new therapeutic indication. They are granted when the new use is novel, non-obvious, and adequately described. For example, sildenafil’s use in pulmonary arterial hypertension was separately patentable even after the erectile dysfunction patents issued, because the PAH indication was distinct and not obvious from prior art. The enforceability of method-of-use patents varies by jurisdiction: in the US, they can be enforced against generic manufacturers through the carve-out process (skinny labeling), though this has faced pressure. In Europe, the second medical use can be claimed under EPC Article 54(5), giving somewhat stronger protection.
Formulation patents cover novel delivery mechanisms, dosing regimens, or excipient compositions that improve efficacy or tolerability for the new indication. These are often the most commercially durable protection when the new indication requires a different dose form — an extended-release version for a chronic condition, or a subcutaneous formulation of an IV drug.
Combination patents protect the new use in combination with another agent, where the combination itself is inventive. These are common in oncology repurposing, where a known cytotoxic compound is repurposed as a sensitizer in combination with a novel checkpoint inhibitor.
Orphan Drug Exclusivity provides seven years of market exclusivity in the US (ten years in Europe) for any compound, including a known generic, if approved for a qualifying rare disease. This is the most powerful non-patent protection mechanism available in repurposing. It cannot be “designed around” the way a method-of-use patent can.
Data exclusivity under the 505(b)(2) pathway gives three years of exclusivity when new clinical investigations are essential for approval, and five years for new chemical entities — though repurposed drugs qualifying as new chemical entities are rare.
For IP teams conducting freedom-to-operate analysis or pre-licensing due diligence, the practical question is not whether the molecule is off-patent but which of these protections the developer has secured, and whether those protections are enforceable in the target markets. DrugPatentWatch’s integrated patent database maps all registered patents, Orange Book listings, patent challenge litigation (Paragraph IV filings), and expiration dates, giving analysts a complete view of the exclusivity stack for any given compound.
Key Takeaways — Part I
- Distinguish repurposing (approved drug, new indication), repositioning (failed investigational compound, new indication), and reprofiling (new MOA or formulation strategy). Each has a different IP position.
- The economic case rests on three verifiable advantages: $300M vs. $2–3B cost, 6–12 vs. 10–15 year timeline, 30% vs. 10% approval probability.
- IP protection for repurposed compounds is layered: method-of-use patents, formulation patents, combination patents, Orphan Drug Exclusivity, and data exclusivity. Composition-of-matter claims are almost always unavailable.
- Orphan Drug Designation is the single most commercially durable protection mechanism for repurposed drugs targeting rare disease populations.
Part II: The Pharmacist as Repurposing Asset — Clinical Knowledge, RWD, and Discovery
Why Pharmacists Occupy a Structurally Unique Position in the Discovery Chain
The standard drug repurposing discovery pipeline runs roughly as follows: computational screen identifies candidate, medicinal chemistry confirms selectivity for the new target, in vitro models validate mechanism, animal studies test efficacy, clinical trials confirm safety and efficacy in patients. At every stage, the hypothesis originates in silico or in the laboratory. The patient observation that often triggers the most durable repurposing hypotheses — the serendipitous clinical signal — has no formal place in this pipeline.
Pharmacists sit at the interface between the pharmaceutical sciences and the patient. In a clinical pharmacy setting, a single pharmacist may review 200–400 medication regimens per month across a complex patient population. In a retail or community setting, that number is higher. Each interaction generates an observation: this patient on Drug A for indication X also has condition Y that appears improved; this patient discontinued Drug B due to effect Z that, pharmacologically, looks more beneficial than adverse in the context of their comorbidity; this drug combination produces an unexpected synergy that the prescriber noted informally.
These signals are almost never systematically captured. They disappear into informal clinical conversation or, at best, a case report. The gap between what pharmacists observe and what feeds into formal repurposing pipelines is one of the most significant underexploited information asymmetries in drug development.
Pharmacotherapy Depth: The Mechanistic Foundation
A clinical pharmacist’s training covers pharmacokinetics, pharmacodynamics, drug-receptor interaction, metabolic pathways, enzyme induction and inhibition, receptor selectivity, and drug-disease interaction across a full breadth of therapeutic areas. This is not generalist clinical knowledge. It is the same mechanistic substrate that computational repurposing methods draw on when building target-disease networks.
When a pharmacist observes that Drug A, approved for neurological condition X, appears to modulate an inflammatory marker in a patient with autoimmune condition Y, they are making a hypothesis that a knowledge-graph algorithm would also generate — if it had access to that observation as a data point. The difference is that the pharmacist can weight the hypothesis with clinical context (patient’s age, comorbidities, concomitant medications, adherence pattern, timing of effect) that the algorithm never sees.
Knowledge-based repurposing methods — which start from a drug’s known mechanism and search for diseases with overlapping molecular pathology — depend on exactly this kind of mechanistic reasoning. Pharmacists perform this reasoning routinely, embedded in patient care.
Polypharmacy and Off-Target Effects
Patients on five or more concurrent medications are common in pharmacist practice, particularly in geriatric, oncology, and chronic disease populations. Managing these regimens requires a working model of each drug’s full pharmacological profile, including off-target receptor binding, metabolic interactions via CYP450 isoforms, and transporter-mediated interactions (P-gp, BCRP, OATP).
Off-target pharmacology is one of the primary mechanisms by which repurposed drugs achieve their new therapeutic effect. Sildenafil’s PDE5 inhibition was an off-target effect relative to its original cardiovascular indication. Thalidomide’s immunomodulatory activity — the basis of its use in multiple myeloma — operates through cereblon binding, not the sedative mechanism for which it was originally developed. The pharmacist reviewing a complex polypharmacy regimen is, functionally, a detector of off-target pharmacology. No current computational system can replicate the clinical judgment required to distinguish a clinically meaningful off-target signal from noise.
Comprehensive Medication Management as a Repurposing Data Source
Comprehensive medication management (CMM) involves systematic review of a patient’s full regimen: indication, efficacy, safety, and adherence for every drug on the list. CMM programs embedded in health systems or PBMs generate structured clinical data at scale. Across a network of pharmacists performing CMM, the aggregate dataset contains:
- Drug-disease co-occurrence patterns at population level
- Observed response rates for off-label uses not captured in claims data
- Adverse event patterns, including unusual beneficial effects documented as clinical notes
- Drug discontinuation reasons, which often encode efficacy signals (discontinued because the patient no longer needed the drug for their primary condition, sometimes because an unexpected benefit resolved a secondary condition)
This data is not well-integrated into drug discovery pipelines. Most of it sits in EHR clinical notes in unstructured text, or in PBM claims data at insufficient clinical granularity to support repurposing analysis. However, where pharmacist-led CMM programs have been connected to research infrastructure, they have generated actionable repurposing signals. The University of Florida’s AI-augmented pharmacy research program, which uses causal and counterfactual prediction models on large EHR datasets, demonstrates what structured pharmacist data can do when connected to the right analytical tools.
Off-Label Prescribing: The Informal Repurposing Pipeline Already Running
Off-label use — prescribing an FDA-approved drug for an indication, patient population, or dose not included in the approved labeling — is legal, common, and clinically often well-supported. Estimates place off-label use at 20–60% of all prescriptions in some specialty areas, with oncology, psychiatry, pediatrics, and rare disease running at the high end.
From a drug development perspective, widespread off-label use constitutes informal clinical evidence of a drug’s activity in the new context. It is not controlled trial data, but it generates a real-world signal that can support a formal repurposing hypothesis, reduce the prior probability of clinical failure, and in some cases support a 505(b)(2) application when the off-label use is documented with sufficient rigor.
Pharmacists sit at the center of this. Under ASHP guidelines, clinical pharmacists conducting order verification are expected to critically evaluate medications for appropriate use, including off-label use, on a case-by-case basis. They communicate with prescribers when off-label use is identified, assess supporting evidence, document their evaluation, and in many health systems contribute to pharmacy and therapeutics committee criteria that govern institutional off-label prescribing.
Every one of these interactions generates structured data that is relevant to formal repurposing: the drug, the off-label indication, the prescriber’s clinical rationale, the observed outcome, the dose used, and any adverse effects. Currently, almost none of this data flows systematically into drug development pipelines. Building that connection — through structured EHR fields, pharmacist-led registries, or AI-assisted signal extraction from clinical notes — is one of the most cost-effective ways a pharmaceutical company can enhance its repurposing intelligence.
Specific High-Value Off-Label Categories
Gabapentin is widely prescribed off-label for anxiety disorders, insomnia, and alcohol use disorder. The volume of off-label use in these indications has effectively generated the clinical rationale for multiple formal repurposing programs, some now in Phase II. Metformin’s off-label use for PCOS, pre-diabetes, and obesity predated formal trials in those indications by years. The clinical signal was pharmacist-observable long before it was trial-tested. Propranolol’s repurposing for infantile hemangiomas began with a clinical observation made during routine cardiac pharmacotherapy, not a computational screen.
The pattern repeats across dozens of compounds. The pharmacist is almost always the first clinician to notice and document the signal, because they are the clinician most engaged with the full medication list.
Key Takeaways — Part II
- Pharmacists generate repurposing-relevant clinical signals daily through CMM, off-label use evaluation, and polypharmacy management. Almost none of this data is currently connected to drug development pipelines.
- Off-target pharmacology — the mechanism underlying most successful repurposing stories — is most likely to be observed by the clinician managing complex polypharmacy: the pharmacist.
- Widespread off-label prescribing in oncology, psychiatry, pediatrics, and rare disease constitutes an informal clinical evidence base for repurposing that pharmacist-led documentation could formalize.
- Building data infrastructure to connect pharmacist CMM observations to repurposing research programs is a low-cost, high-leverage investment for pharma R&D organizations.
Part III: Pharmacovigilance as a Repurposing Engine
The Structural Connection Between PV and Discovery
Pharmacovigilance exists to detect, assess, and prevent adverse drug reactions in post-market populations. Its output is primarily safety data. However, the same signal-detection infrastructure that identifies harmful off-target effects is equally capable of identifying beneficial off-target effects — if the analytical lens is applied that way.
The pharmacovigilance community has recognized this explicitly. Regulatory-linked PV databases — WHO’s VigiBase, the FDA Adverse Event Reporting System (FAERS), the European Medicines Agency’s EudraVigilance — collectively contain hundreds of millions of individual case safety reports. Mining these databases for disproportionate reporting of beneficial effects, or for signals that suggest a drug is modifying a disease pathway unrelated to its approved indication, is an established computational approach to repurposing candidate identification.
Thalidomide’s trajectory provides the historical archetype. The drug was withdrawn in 1961 due to teratogenicity. Its immunomodulatory properties, observed through adverse event patterns and case reports in leprosy patients, led to eventual approval for erythema nodosum leprosum in 1998 and multiple myeloma in 2006. The signal existed in the pharmacovigilance record long before it was formally validated. A pharmacist with access to the FAERS data and the analytical tools to query it could, in principle, identify equivalent signals for other compounds today.
Pharmacist Roles in Active PV
Pharmacists contribute to pharmacovigilance through two primary channels. In institutional settings, they operate within hospital-based medication error reporting and adverse drug event surveillance systems, often directly linked to the FDA MedWatch program. In clinical research settings, research pharmacists manage investigational drug accountability, monitor for adverse events and SUSARs (Suspected Unexpected Serious Adverse Reactions), and contribute to safety data management for IND filings.
Both channels generate data relevant to repurposing. A SUSAR reported during a Phase II trial for Indication A may reflect a drug effect that is therapeutically relevant for Indication B. The pharmacist who files the SUSAR is often the first person with the clinical knowledge to recognize this possibility, but no formal mechanism exists to route that insight into the repurposing pipeline.
Advanced pharmacy programs at academic medical centers have begun to address this gap. The University of Florida’s pharmacy AI research program explicitly uses causal AI models to identify heterogeneity in treatment effects within large patient datasets — a methodology directly applicable to identifying patient subgroups where a drug produces unexpected benefit. These programs demonstrate what becomes possible when pharmacist-generated clinical data is connected to sophisticated analytical infrastructure.
AI-Augmented PV: The Emerging Standard
AI is transforming pharmacovigilance in ways that directly amplify the repurposing utility of PV data. Natural language processing (NLP) systems can now extract structured adverse event information from unstructured clinical notes, social media, and published literature at scale. Machine learning classifiers can distinguish true adverse drug reactions from coincidental events in FAERS reports with greater accuracy than manual review. Disproportionality analysis algorithms can identify unexpected drug-event pairs across databases of millions of reports in hours.
For repurposing, the same tools can be reoriented. Instead of asking “which drugs are associated with unexpected harms,” the query becomes “which drugs are associated with unexpected improvements in conditions outside their approved indication.” The data infrastructure is identical; the question is different.
Pharmacists who understand how to interact with these AI-augmented PV systems — framing the clinical question, interpreting the output, and applying clinical judgment to the signal — become high-value contributors to the repurposing discovery process. This requires digital literacy and data interpretation skills beyond traditional pharmacy training, which is why pharmacy schools are increasingly incorporating pharmacoinformatics and AI literacy into their curricula.
Key Takeaways — Part III
- PV databases (FAERS, VigiBase, EudraVigilance) contain hundreds of millions of case reports that can be mined for beneficial off-target signals using the same computational tools used for safety monitoring.
- Pharmacists who file SUSARs and manage adverse event reporting are generating the raw data for repurposing signal detection. No formal mechanism currently connects PV filings to repurposing research pipelines in most organizations.
- AI-augmented PV — using NLP and ML to extract structured signals from unstructured clinical records — represents the next generation of repurposing candidate identification. Pharmacist clinical judgment is the validation layer.
- A dual-purpose PV infrastructure, designed to identify both harmful and beneficial off-target effects, requires pharmacist involvement at the signal-interpretation stage.
Part IV: Pharmacists in Clinical Trials for Repurposed Compounds
Protocol Design: Where Clinical Pharmacy Expertise Changes Trial Outcomes
Clinical trials for repurposed compounds differ from standard trials in several ways that pharmacists are particularly equipped to address. Because the compound’s safety in its approved population is known, trial design can be more aggressive in exploring dose escalation in the new patient population. But “known safety in Population A” does not automatically transfer to Population B — particularly when the new indication involves patients with different comorbidities, different concomitant medications, or different metabolic profiles.
The pharmacist’s role in protocol design centers on three areas:
First, dose selection for the new indication. The approved dose for Indication A may not be the optimal dose for Indication B. Pharmacokinetic modeling based on the new patient population’s metabolic characteristics, renal and hepatic function, and co-medication-driven CYP interactions is required. Clinical pharmacists with pharmacokinetic expertise are the appropriate professionals to conduct this analysis and propose the starting dose range.
Second, drug interaction assessment for the trial population. Repurposing trials in oncology, for example, almost always involve patients on multiple concurrent therapies. A systematic drug interaction assessment that accounts for the repurposed compound’s metabolic pathway, transporter profile, and pharmacodynamic interactions with common co-medications is essential before trial enrollment. Pharmacists perform this analysis routinely in clinical care; formalizing it as part of protocol development reduces adverse event risk and protocol amendments.
Third, formulation selection. If the approved dose form is not appropriate for the new indication or patient population — for example, an IV formulation being evaluated for an outpatient chronic disease indication — the pharmacist’s formulation expertise informs whether an oral or subcutaneous alternative is feasible and how to handle the pharmacokinetic differences between dose forms.
Research Pharmacist Functions: Investigational Drug Management
Research pharmacists manage the full lifecycle of investigational drug accountability in clinical trials: receipt, storage, dispensing, accountability documentation, and return or destruction of unused drug. For repurposed compounds, this is particularly important when the compound is commercially available but being used at a different dose, via a different route, or in a new formulation for the trial.
Research pharmacists also manage blinding and randomization logistics for double-blind trials, prepare and dispense placebo and active drug according to the randomization schedule, and ensure that the drug’s physical characteristics under the study conditions match the expectations set in the protocol. For repurposed biologics, where stability under novel administration conditions may be untested, this requires expert judgment.
At Mayo Clinic and similar academic research centers, research pharmacists are embedded in the clinical trials unit, attend protocol review meetings, and provide ongoing support for safety data management. Their participation reduces protocol deviations, improves adverse event documentation quality, and accelerates the regulatory submissions that follow trial completion.
Patient Adherence and Retention: The Commercial Consequence
Clinical trial failure due to inadequate adherence or early discontinuation is more common, and more costly, than most trial sponsors acknowledge. In repurposing trials, where patients are often being asked to take a drug they associate with a different condition — sometimes one with stigma, like thalidomide’s history — adherence challenges are compounded by psychological factors.
Pharmacists improve adherence through individualized patient education: explaining the mechanistic rationale for the new indication, setting appropriate expectations for response timelines, managing side effect concerns with evidence-based counseling, and building the trust that encourages patients to stay on study. These are not soft interventions. In a 500-patient Phase II trial with 25% dropout, reducing dropout to 15% through pharmacist-led adherence support can mean the difference between an adequately powered trial and a failed one.
The business case for funding pharmacist-led patient support programs in repurposing trials is straightforward: the cost of a pharmacist-managed adherence program is a fraction of the cost of running an extension study to recover statistical power lost to dropout.
Key Takeaways — Part IV
- Clinical pharmacists contribute to repurposing trial protocol design through dose selection for the new population, drug interaction assessment, and formulation evaluation — not just dispensing.
- Research pharmacists manage investigational drug accountability, blinding logistics, and safety documentation in ways that reduce protocol deviations and accelerate regulatory submissions.
- Pharmacist-led adherence and retention programs address a structurally underappreciated trial failure mode. The ROI on these programs is measurable and favorable relative to extension study costs.
Part V: Real-World Evidence, EHR Data, and the Pharmacist as Data Steward
What Real-World Evidence Actually Means for Repurposing
Real-world data (RWD) encompasses clinical data collected outside the controlled environment of a randomized trial: EHR records, insurance claims, patient registries, wearable device outputs, and pharmacy dispensing records. Real-world evidence (RWE) is the clinical evidence derived from analyzing RWD. The 21st Century Cures Act (2016) expanded FDA’s mandate to consider RWE in drug approval decisions, and the agency has issued a series of guidance documents on RWD standards, EHR suitability, and RWE study design.
For repurposing, RWE occupies a unique position. A drug with extensive off-label use history may have RWD supporting its new indication that, if properly structured and analyzed, reduces the evidentiary burden in a 505(b)(2) application. The FDA has accepted RWE for label expansions in oncology (notably for PD-1/PD-L1 inhibitors across tumor types) and rare disease. For repurposing programs where ethical or practical barriers to randomized trials exist, RWE may be the primary or only feasible path to approval.
The quality of RWE depends on the quality of the underlying RWD. Data completeness, coding consistency, documentation depth, and the accuracy of concomitant medication records all determine whether an RWD dataset supports regulatory-grade inference. Pharmacists directly influence all of these quality dimensions.
Pharmacist Contributions to RWD Quality
In institutional settings, pharmacists perform medication reconciliation at care transitions (admission, discharge, post-discharge follow-up), which is the primary mechanism by which medication errors and documentation gaps in EHRs are corrected. A patient admitted to hospital whose home medication list is inaccurate in the EHR will generate RWD that misattributes drug exposures and confounds any analysis. Pharmacist-led reconciliation corrects these errors before they propagate into the research database.
Pharmacists also contribute to medication documentation completeness by capturing OTC medications, herbal supplements, and over-the-counter dose adjustments that patients typically do not report to physicians. These are significant sources of confounding in RWD analyses of drug effects, particularly for drugs with narrow therapeutic indices or CYP-mediated interactions.
Where health systems have implemented pharmacist-led documentation programs specifically designed to improve RWD quality for research purposes — capturing structured fields for indication, dose rationale, and observed outcomes rather than free text — the resulting datasets have supported repurposing analyses that were not feasible with standard EHR data.
The Digital Health Integration Gap
Most pharmacy management systems do not integrate well with EHRs. Prescription dispensing data sits in PBM systems; clinical pharmacy notes sit in the EHR; pharmacovigilance reports sit in separate safety databases. A pharmacist observing a clinically significant off-label effect has no single platform in which to document that observation in a structured, searchable format that could feed a repurposing screen.
This integration gap is the primary systemic barrier to pharmacist contributions to repurposing research. Addressing it requires coordinated investment from health systems, PBMs, pharmacy software vendors, and pharmaceutical research organizations. Several academic medical centers are building pharmacist-facing AI tools that extract relevant clinical signals from documentation workflows and route them to research registries, but these are early-stage programs.
For pharmaceutical companies building repurposing programs, partnering with health systems that have made this investment is a direct way to access pharmacist-generated RWD at a quality and scale not available elsewhere.
Key Takeaways — Part V
- RWE from pharmacist-generated data (CMM notes, off-label use documentation, medication reconciliation records) can support 505(b)(2) applications and reduce clinical trial scope in repurposing programs.
- Pharmacist medication reconciliation at care transitions is the primary correction mechanism for EHR drug exposure errors that would otherwise confound RWD analyses.
- The absence of integrated platforms connecting pharmacy management systems to EHRs and research databases is the main systemic barrier to pharmacist-generated RWD feeding drug repurposing programs. This is a solvable infrastructure problem.
Part VI: Computational Methods, AI Platforms, and the Pharmacist Interface
The Major Computational Repurposing Strategies
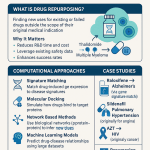
Drug repurposing computational methods fall into five broad categories, each with different data requirements and different roles for pharmacist input.
Target-based methods identify diseases that share molecular targets with a drug’s known mechanism of action. The underlying assumption is that if Drug A inhibits Enzyme X, and Enzyme X is also pathogenic in Disease B, Drug A may be effective in Disease B. These methods depend on the quality of the target-disease association databases they query (DisGeNET, OMIM, DrugBank). Pharmacist knowledge of a drug’s full receptor binding profile, including secondary and tertiary targets, directly enriches this analysis.
Network pharmacology maps drug-target interactions onto protein-protein interaction networks and identifies disease modules that overlap with the drug’s network neighborhood. It produces multi-target repurposing hypotheses — compounds that may affect a disease through simultaneous action on multiple nodes in a disease network. This approach has been particularly productive in complex diseases like Alzheimer’s and metabolic syndrome, where single-target strategies have failed consistently.
Transcriptomics-based methods compare a drug’s gene expression signature (using datasets like LINCS L1000) against disease gene expression signatures and identify compounds whose transcriptional effects reverse the disease state. This approach was behind the identification of itraconazole as a potential anti-cancer agent and has generated multiple repurposing hypotheses now in clinical trials.
Electronic health record mining uses large-scale EHR data to identify statistical associations between drug exposures and disease outcomes outside the drug’s approved indication. These analyses require large patient cohorts, careful confounder adjustment, and replication across independent datasets. The signal quality depends heavily on the accuracy and completeness of the EHR data — which is where pharmacist documentation practices have direct impact.
Knowledge graph mining and large language models represent the newest class of methods. Large biomedical knowledge graphs (Hetionet, OpenBioLink, DRKG) connect drugs, targets, diseases, pathways, and clinical phenotypes into a traversable network. Graph neural network methods can predict drug-disease links not present in the training data by learning from the graph topology. LLMs fine-tuned on biomedical literature can generate repurposing hypotheses directly from text. Both approaches are increasingly being integrated into early drug discovery workflows at major pharmaceutical companies and AI-first drug discovery startups.
Where Pharmacist Expertise Intersects with Computational Methods
Computational methods generate candidates. Clinical judgment validates or refutes them. This distinction matters practically: AI platforms can screen millions of drug-disease pairs and return a ranked list of candidates, but the clinical plausibility of the top candidates requires expert human review before any development spend is committed.
Pharmacists with expertise in the therapeutic area under investigation are natural validators for computationally generated hypotheses. They can assess whether the proposed mechanism makes clinical sense given the disease’s presentation and typical patient population, whether known drug interactions or patient population characteristics would complicate clinical testing, whether the dose and formulation assumed by the hypothesis are clinically realistic, and whether informal clinical observations support or contradict the hypothesis.
At institutions where AI-driven repurposing platforms have been deployed alongside clinical pharmacy teams, the iterative loop between computational hypothesis generation and pharmacist clinical validation has accelerated candidate prioritization and reduced false positive rates. The AI generates the hypothesis space; the pharmacist narrows it to the clinically credible candidates.
Pharmacogenomics and Precision Repurposing
Pharmacogenomic data — specifically, the mapping of drug response variation to genetic polymorphisms — adds a precision dimension to repurposing that is increasingly tractable as population-scale genomic databases (UK Biobank, All of Us, FinnGen) become available for drug-target analysis.
The concept of precision repurposing applies a drug to a genetically defined patient subgroup in which the new indication is driven by a specific mutation or pathway variant. For example, a drug that inhibits a kinase mutated in a subset of cancer patients may produce responses in that subset that are not visible in unselected populations. Identifying these genetic biomarkers of response in repurposing programs requires integrating genomic data with the clinical phenotype data that pharmacists help generate.
Clinical pharmacists with pharmacogenomics training can implement pharmacogenomic-guided prescribing protocols (already standard practice for clopidogrel, warfarin, and several psychiatric medications), which generates structured pharmacogenomic data that can inform precision repurposing analyses. Several academic health systems are building pharmacist-led pharmacogenomics programs explicitly aimed at generating this data at scale.
Key Takeaways — Part VI
- The five major computational repurposing strategies (target-based, network pharmacology, transcriptomics, EHR mining, knowledge graph) each have different data quality requirements that pharmacist documentation practices directly affect.
- AI platforms generate ranked candidate lists. Pharmacist clinical validation is the necessary filter between AI hypothesis generation and development spend commitment.
- Precision repurposing — matching a drug to a genetically defined patient subgroup — represents the frontier of the field. Pharmacist-led pharmacogenomics programs are generating the data that makes this feasible at scale.
Part VII: Regulatory Pathways, Patent Strategy, and Market Entry
The 505(b)(2) Pathway: How It Works and When to Use It
The 505(b)(2) NDA pathway allows applicants to rely, at least in part, on published literature or the FDA’s previous findings of safety and efficacy for an approved drug to support their new indication, dose, dosage form, route of administration, or formulation. The applicant still needs to submit clinical data demonstrating safety and efficacy for the new use, but can reference the existing safety record rather than conducting a full de novo preclinical and Phase I program.
For repurposed drugs, this pathway is the standard route to approval. Its practical advantages are substantial: the IND application can reference existing safety data, Phase I can often be limited to pharmacokinetic bridging in the new population, and the total data package required is smaller than a full 505(b)(1) application. Approval timelines for 505(b)(2) applications run roughly 60% of those for standard NDA applications.
The pathway also creates a specific IP consideration. When a 505(b)(2) applicant relies on another company’s data for the safety foundation, the listed drug owner may have Orange Book-listed patents that create Paragraph IV certification obligations. Managing this exposure — through careful patent landscape analysis, timing of the Paragraph IV certification, and litigation strategy — is a core function of pharma IP teams handling repurposing programs. The DrugPatentWatch database’s full integration of Orange Book listings, Paragraph IV filings, and litigation records makes it the standard tool for this analysis.
Orphan Drug Designation: The Most Commercially Underutilized Mechanism in Repurposing
Orphan Drug Designation (ODD) is available for any drug intended to treat a disease affecting fewer than 200,000 people in the US. For repurposed compounds, this includes many approved drugs being studied in rare subtypes of common diseases — rare genetic metabolic disorders, pediatric cancers, rare autoimmune conditions — not just conditions that are rare overall.
The benefits of ODD are substantial and compounding:
- Seven years of market exclusivity upon approval, regardless of patent status. This exclusivity applies to the specific approved indication and cannot be circumvented by a generic or biosimilar manufacturer filing for the same indication.
- A 25% tax credit on qualifying clinical research expenses. For a repurposing program with $50–100M in clinical development costs, this credit materially improves program economics.
- Direct access to FDA staff for guidance, through the Office of Orphan Products Development.
- Waiver of PDUFA application fees, which currently run approximately $4M for standard NDA applications.
For pharmaceutical companies evaluating repurposing candidates, the first analytical step should be a systematic check against orphan disease prevalence data. Many compounds have potential indications that qualify for ODD without the company having formally pursued designation. The combination of ODD exclusivity and method-of-use patent protection can create a commercially viable exclusivity window even for drugs on which composition-of-matter patents have long expired.
European Pathways: Article 8(3) and Repurposing in the Hybrid Application
In Europe, repurposed drugs typically pursue approval via the hybrid application procedure under Article 8(3) of Directive 2001/83/EC. This allows reference to the originator’s dossier for the safety data while requiring independent evidence for the new therapeutic indication. The EMA’s scientific advice service provides pre-submission guidance on what data package is required, which is particularly valuable for repurposing programs where the clinical development strategy is non-standard.
Europe also offers Orphan Medicinal Product Designation (OMPD) for conditions affecting fewer than 5 per 10,000 persons in the EU, with 10 years of market exclusivity upon approval. The combined breadth of qualified rare conditions across the US and EU provides substantial opportunity for repurposing programs targeting smaller patient populations.
Evergreening and Its Limits in Repurposing
Evergreening — the practice of filing new patents covering minor modifications to extend a drug’s effective commercial life — is a genuine strategy in pharmaceutical IP management, though its use in repurposing is more constrained than in primary patent protection. A method-of-use patent for a new indication does not extend exclusivity for the original indication, which remains subject to generic competition. Formulation patents on novel dose forms may exclude generics from the new formulation but not from the original.
The criticism of evergreening centers on whether new filings represent genuine innovation or minor modifications that add limited therapeutic value. For repurposing, the new indication is the innovation — the clinical work required to establish efficacy in the new population is real development spend, not a trivial formulation change. Method-of-use patents filed after genuine clinical development of a new indication are defensible as legitimate innovation.
For IP teams, the practical issue is not whether evergreening is ethically acceptable but whether the new patents will withstand challenge. Method-of-use patents in the US face Paragraph IV certifications in which generic applicants argue that the new indication patent is invalid or not infringed through skinny labeling. Litigation outcomes in these cases are fact-specific, but companies with strong clinical differentiation data and clear evidence of the new indication’s novelty and non-obviousness have prevailed consistently.
Key Takeaways — Part VII
- The 505(b)(2) NDA pathway reduces clinical data requirements by allowing reference to existing safety records. It is the standard approval route for repurposed drugs and requires systematic Orange Book/Paragraph IV analysis by IP teams.
- Orphan Drug Designation provides seven years of US market exclusivity upon approval — the most commercially durable protection mechanism for repurposed drugs and available for any drug in a qualifying rare indication, regardless of molecule age.
- The combination of ODD exclusivity and method-of-use patent protection is the standard exclusivity strategy for repurposed compounds where composition-of-matter patents have expired.
- Evergreening through method-of-use and formulation patents is defensible as legitimate IP protection when it follows genuine clinical development. Patent validity depends on the strength of the new indication’s novelty and non-obviousness.
Part VIII: Market Dynamics, Investment Thesis, and Competitive Intelligence
Market Size and Growth Drivers
The global drug repurposing market was valued at approximately $29.4B in 2024. Projections from multiple independent research firms converge on a range of $51–59B by 2033–2034, representing a CAGR of 4.1–5.4%. This growth is driven by four converging pressures:
Patent cliff exposure across major pharmaceutical companies. The period from 2025–2030 includes expiry of composition-of-matter patents on blockbuster biologics and small molecules generating billions in annual revenue. Repurposing existing assets in new indications, or new formulations, is the fastest way to replace eroding revenue without the lead time of a de novo program.
Biosimilar competition accelerating revenue erosion. As biosimilars enter markets previously protected by biologic exclusivity, originator companies are under increasing pressure to demonstrate differentiation through new clinical data. Repurposing into new indications with distinct clinical value is one route to this differentiation.
Rare disease and pediatric policy incentives. The Orphan Drug Act, PREA, and equivalent European legislation have created a system of financial incentives specifically designed to route drug development resources toward underserved populations. Repurposing is economically better suited to rare disease development than de novo drug discovery, and the market is responding.
AI-driven reduction in discovery costs. As computational methods reduce the cost of identifying high-confidence repurposing candidates, the economics of early-stage repurposing programs improve. Companies that build or license AI-enabled repurposing platforms can screen candidates at a fraction of the cost of traditional medicinal chemistry programs.
Investment Strategy for Institutional Investors
For biotech analysts and portfolio managers evaluating drug repurposing exposure, the risk-adjusted investment thesis differs from standard drug development in several respects.
The primary risk in repurposing programs is not safety — that has already been characterized — but efficacy in the new indication. Phase II failure rates in repurposing are still meaningful (roughly 40–50% of programs that enter Phase II do not proceed to Phase III), but the reasons for failure are different: the mechanism assumed by the repurposing hypothesis does not apply in the new disease, or the patient population needs to be more genetically defined for response. These are answerable questions with relatively small Phase II studies, reducing the capital at risk per program.
Repurposing programs also tend to have faster clinical milestones, generating value-accretive data points for portfolio companies on shorter timescales than de novo programs. A company with a diversified portfolio of three to five repurposing programs across different therapeutic areas and indications can reasonably expect multiple Phase II readouts within a 24–36 month window.
The IP risk — specifically, the risk that generic manufacturers challenge method-of-use patents through skinny labeling — is real and should be assessed as part of due diligence. The strength of the method-of-use patent (specificity of the indication claim, non-obviousness relative to prior art, enforceability in key jurisdictions) and the availability of Orphan Drug Exclusivity as a backstop are the key IP risk factors to evaluate.
Companies building AI-enabled repurposing platforms with proprietary clinical data assets — large-scale EHR data, pharmacovigilance databases, pharmacist-generated CMM data — represent a differentiated investment case relative to companies relying solely on public databases. The proprietary data generates candidates that competitors cannot easily replicate, and the platform can generate multiple pipeline programs from a single data infrastructure investment.
Competitive Intelligence: Using Patent Landscape Analysis
For pharma and biotech business development teams, the competitive intelligence function in repurposing centers on three questions: which compounds have available repurposing opportunity (expired composition-of-matter patents, unpatented indications, orphan-qualified populations), which competitors have filed method-of-use or formulation patents in the indications under evaluation, and which Paragraph IV certifications have been filed that signal competitive entry.
DrugPatentWatch provides integrated access to all three dimensions: expiration dates for composition-of-matter and formulation patents, method-of-use patent filings organized by indication and compound, and Paragraph IV certification records with litigation outcomes. The platform’s biopharmaceutical forecasting tools also support identification of future therapeutic indications being pursued by competitors, enabling early-stage competitive positioning.
For an IP team conducting a landscape analysis on a repurposing candidate, the standard workflow is: confirm composition-of-matter patent expiration date, map all issued and pending method-of-use and formulation patents in the target indication, identify Paragraph IV certifications filed against the originator compound, and assess orphan disease qualification for the new indication. This analysis, completed before first clinical investment, determines whether the commercial opportunity justifies the development spend.
Key Takeaways — Part VIII
- The global drug repurposing market grows to $51–59B by 2033–2034, driven by patent cliff pressure, biosimilar competition, rare disease policy incentives, and AI-driven reduction in discovery costs.
- For institutional investors, repurposing programs offer faster clinical milestones, lower capital at risk per program, and more predictable failure modes than de novo drug development.
- Companies with proprietary clinical data assets (large-scale EHR data, pharmacist-generated CMM data, pharmacovigilance databases) have durable competitive advantages in AI-driven repurposing that public-database-only competitors cannot replicate.
- Standard competitive intelligence workflow for a repurposing candidate: confirm molecule patent expiry, map method-of-use and formulation patents in the target indication, identify Paragraph IV certifications, assess orphan qualification. DrugPatentWatch integrates all of this.
Part IX: Building Organizational Capability — Integrating Pharmacists into Repurposing Programs
Current Organizational Barriers
Most pharmaceutical companies have not formalized a pharmacist role in their drug repurposing programs. Pharmacists contribute at discrete points — clinical trial operations, pharmacovigilance — but are typically not embedded in the repurposing discovery team that generates and evaluates candidate hypotheses. This is partly structural (discovery teams are predominantly composed of medicinal chemists, computational scientists, and disease biologists) and partly a legacy of how the pharmacist profession has been positioned relative to drug development.
The consequence is that the most valuable pharmacist contributions — real-world signal generation, off-label use documentation, clinical validation of computational hypotheses — occur outside the formal program structure and do not feed into development decisions in any systematic way.
Recommended Organizational Models
Several models for integrating pharmacist expertise into repurposing programs have been demonstrated at academic medical centers, specialized biotech companies, and a small number of large pharma organizations.
The embedded clinical pharmacist model places one or more clinical pharmacists with appropriate therapeutic area expertise in the discovery team, with a mandate to review computationally generated candidates from a clinical plausibility perspective, maintain ongoing surveillance of off-label prescribing patterns in the relevant indication, and maintain relationships with health system pharmacy networks that generate real-world data. This model works best in organizations with a defined therapeutic area focus.
The pharmacist-led RWE generation model formalizes the connection between health system pharmacy programs and pharmaceutical research organizations. The health system pharmacy team, operating under an appropriate data governance framework, generates structured CMM and off-label use documentation that is shared with the pharmaceutical partner for repurposing signal analysis. Several academic medical centers have built this model, and it provides access to pharmacist-generated real-world data that is not available from commercial data vendors.
The pharmacovigilance-to-repurposing routing model creates a formal process by which beneficial off-target effects identified in post-market surveillance are routed to the repurposing discovery team for evaluation. This requires a classification system for PV signals that distinguishes safety-relevant adverse events from pharmacologically interesting effects, which in turn requires pharmacist clinical judgment in the triage process.
Pharmacist Education and Skill Development for Repurposing Roles
Clinical pharmacists taking on repurposing-focused roles require skills beyond standard clinical pharmacy training. Specifically: biomedical data literacy (ability to query and interpret EHR databases, PV databases, and clinical literature databases), basic familiarity with computational repurposing methods (what the major platforms do, what their output means, what their limitations are), and understanding of the regulatory framework for repurposing approvals (505(b)(2), ODD, RWE standards).
Postgraduate residency programs at academic medical centers are beginning to incorporate these competencies, but coverage is inconsistent. For pharmaceutical companies looking to hire or partner with pharmacists for repurposing roles, PharmD programs with pharmacoinformatics tracks, or candidates with post-residency research fellowships at repurposing-focused programs, represent the most relevant talent pool.
Key Takeaways — Part IX
- Most pharmaceutical companies have not formalized pharmacist roles in repurposing discovery programs, leaving the most valuable pharmacist contributions (real-world signal generation, clinical validation) disconnected from development decisions.
- Three organizational models have been demonstrated: embedded clinical pharmacist in the discovery team, pharmacist-led RWE generation in partnership with health systems, and formal pharmacovigilance-to-repurposing routing.
- Clinical pharmacists in repurposing roles require biomedical data literacy, familiarity with computational repurposing methods, and understanding of the regulatory framework. These are teachable skills not yet consistently covered in standard PharmD training.
Appendix A: Canonical Drug Repurposing Case Studies with IP and Commercial Analysis
Sildenafil (Pfizer): From Cardiovascular Failure to Two Blockbuster Indications
Sildenafil was developed by Pfizer scientists as a treatment for hypertension and angina, targeting phosphodiesterase type 5 (PDE5) as a mechanism for smooth muscle relaxation in coronary vasculature. Phase II results were poor for the cardiovascular indication. During trial closeout, clinical investigators observed a consistent, unexpected effect: male patients were reluctant to return unused medication, and self-reported a previously undisclosed sexual side effect.
The commercial response to this observation generated approximately $1.7B in annual revenue for the erectile dysfunction indication at peak (Viagra). Pfizer secured method-of-use patents on the ED indication, with primary patent expiry in 2012 in the US (extended through additional patent filings). The subsequent repurposing for pulmonary arterial hypertension (Revatio, approved 2005) secured an additional commercial lifecycle with a separate dosing regimen and distinct patient population, supported by new method-of-use patents.
The IP lesson: a molecule with failed composition-of-matter claims in its original indication can generate multiple method-of-use patent families across successive repurposed indications, each with distinct commercial value and different exclusivity windows.
Thalidomide (Celgene): From Withdrawal to Orphan Drug Commercial Success
Thalidomide’s history — teratogenic disaster in the 1960s, withdrawal, eventual repurposing for erythema nodosum leprosum (1998) and multiple myeloma (2006) — is the most instructive case study in how a drug’s benefit-risk ratio is indication-specific, not absolute.
Celgene built a commercial franchise on thalidomide’s immunomodulatory properties through a combination of Orphan Drug Exclusivity (both ENL and MM qualified), aggressive method-of-use patent prosecution, and a proprietary distribution and safety management system (STEPS program) that effectively created a barrier to generic entry beyond the patent and exclusivity protection. The MM approval contributed to Celgene’s eventual acquisition by Bristol-Myers Squibb for $74B in 2019.
The commercial structure of the thalidomide franchise demonstrates that Orphan Drug Exclusivity plus method-of-use patents plus proprietary distribution infrastructure can generate multi-billion-dollar commercial value for a molecule that no one owns at the composition-of-matter level.
Dexamethasone (COVID-19): RWE-Driven Emergency Repurposing
Dexamethasone’s approval for COVID-19 in hospitalized patients requiring supplemental oxygen or ventilation was supported by data from the RECOVERY trial, a large randomized adaptive platform trial conducted in the UK during the acute pandemic phase. The compound was approved for decades as a corticosteroid for multiple indications; its use in COVID-19 was a genuine repurposing on a mechanistic basis (cytokine storm modulation).
The commercial structure of this repurposing differs from the sildenafil or thalidomide models because dexamethasone is a long-off-patent generic, and no commercial entity captured significant revenue from the COVID indication. The public health value was enormous; the commercial return was near zero. This case illustrates the structural gap that the DRUGS Act and similar proposals aim to address: the absence of commercial incentive for repurposing generic drugs in public health emergencies.
For pharmaceutical business development, the dexamethasone case is instructive as a model of what not to pursue: a generic molecule in a short-duration indication with no path to Orphan Drug Exclusivity and no available method-of-use patent protection. The business case for commercial repurposing requires at least one durable exclusivity mechanism.
Appendix B: Repurposing Technology Roadmap — From Serendipity to Systematic AI
Generation 1 (Pre-2000): Serendipitous clinical observation. Repurposing occurs through chance clinical observation, individual investigator intuition, or accidental discovery during trials for other indications. Sildenafil, aspirin, propranolol in hemangiomas. No systematic methodology. Discovery rate low; hit-to-approval rate high when discovery occurs.
Generation 2 (2000–2010): Knowledge-based and literature mining. Systematic literature review and database mining (PubMed, DrugBank, ChEMBL) to identify mechanistic connections between approved drugs and new diseases. First computational repurposing platforms emerge. SIDER database of drug side effect profiles enables systematic off-target hypothesis generation.
Generation 3 (2010–2018): Transcriptomics and signature-based repurposing. LINCS L1000 program generates gene expression signatures for thousands of small molecules, enabling signature reversal approaches. Broad Institute’s Connectivity Map (CMap) becomes the standard tool for transcriptomics-based repurposing. First large-scale EHR mining studies using claims data generate epidemiological repurposing evidence.
Generation 4 (2018–2023): Network pharmacology and knowledge graphs. Graph-based methods on protein-protein interaction networks and biomedical knowledge graphs (Hetionet, DRKG) enable multi-target repurposing hypothesis generation at scale. Graph neural networks predict drug-disease links from graph topology. FAERS mining with ML classifiers generates PV-derived repurposing candidates systematically.
Generation 5 (2023–present): LLM-augmented repurposing and precision subgroup identification. Foundation models trained on biomedical literature generate repurposing hypotheses from text at scale. Multimodal AI systems integrate genomics, proteomics, transcriptomics, EHR, and PV data in unified representation spaces. Precision repurposing identifies genetically defined patient subgroups for targeted clinical development. AI-enabled clinical trial matching connects repurposing hypotheses to specific patient populations in existing registries within weeks rather than months.
Glossary of Technical Terms
505(b)(2) NDA: New Drug Application pathway allowing reliance on existing safety data for an approved drug to support a new indication, dose form, or route of administration.
Composition-of-matter patent (COM): Patent protecting the chemical structure of a drug molecule. Almost always unavailable for repurposed compounds.
Evergreening: The practice of filing additional patents (formulation, method-of-use, combination) to extend a drug’s effective commercial exclusivity beyond the original compound patent.
Knowledge graph: A structured network representation connecting biological entities (drugs, targets, diseases, pathways) that enables computational traversal to identify non-obvious drug-disease associations.
Method-of-use patent: Patent protecting a specific therapeutic use of a known compound, as distinct from the compound itself.
Orphan Drug Designation (ODD): US regulatory designation for drugs treating diseases affecting fewer than 200,000 patients, providing seven-year market exclusivity and additional incentives.
Paragraph IV certification: Certification filed by a generic applicant asserting that a listed Orange Book patent is invalid or not infringed, initiating potential patent litigation under Hatch-Waxman.
Pharmacovigilance (PV): The science of detecting, assessing, and preventing adverse drug reactions in post-market populations.
Real-world data (RWD): Clinical data collected outside randomized trials, including EHR records, claims, registries, and wearable outputs.
SUSAR: Suspected Unexpected Serious Adverse Reaction — an adverse event that is unexpected relative to the investigator’s brochure and serious in severity, requiring expedited reporting during clinical trials.
For patent landscape analysis, method-of-use patent mapping, and Paragraph IV tracking on specific repurposing candidates, DrugPatentWatch provides integrated small molecule and biologic patent intelligence at DrugPatentWatch.com.
Copyright notice: This article is an original analytical work. Source material was drawn from publicly available research, regulatory guidance documents, and the original DrugPatentWatch blog post at drugpatentwatch.com/blog.