A technically dense deep dive for pharma IP teams, R&D leads, and institutional investors, covering the full financing architecture, patent valuation mechanics, evergreening roadmaps, and AI-driven discovery pipelines for generic repurposing.
01. The Economic Case for Generic Repurposing
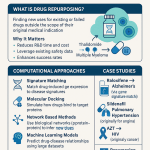
Drug repurposing, the systematic identification of new therapeutic uses for compounds that already carry an established safety record, is not a new idea. Sildenafil reached patients for pulmonary arterial hypertension only after its initial angina program failed and its erectile dysfunction market matured. Aspirin’s antiplatelet mechanism was characterized decades after its analgesic use was routine. What has changed is the rigor with which the pharmaceutical industry now pursues these second and third lives for existing molecules, driven by a convergence of deteriorating de novo R&D productivity, AI-driven target identification, and an accumulating generics estate whose IP has lapsed but whose safety dossiers remain intact.
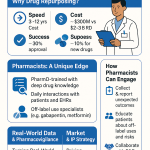
For generic compounds specifically, the arithmetic is difficult to argue with. A novel small molecule entering Phase I clinical trials carries roughly a 90% probability of failing to reach approval. A repurposed generic entering a new efficacy study for an indication with mechanistic plausibility starts from a radically different baseline: ADME data, toxicology packages, manufacturing processes, and years of post-marketing pharmacovigilance are already in hand. Phase I is, in most cases, either unnecessary or abbreviated. The development timeline compresses from the 10 to 17 years typical for a new molecular entity to somewhere between 3 and 12 years. All-in development costs fall from the $2 to $3 billion range to roughly $300 million.
~30%Phase I to Approval Rate, Repurposed Drugs
~10%Phase I to Approval Rate, NMEs
$300MAvg. All-In Repurposing Cost
$2-3BAvg. NME Development Cost
50-60%Cost Reduction vs. De Novo
$59.3BProjected Global Market by 2034
The COVID-19 pandemic stress-tested this framework in real time. Dexamethasone, a corticosteroid off patent since the 1950s, was repurposed under the Oxford RECOVERY trial and became the first treatment shown to reduce mortality in severe COVID-19 patients. Remdesivir, though not a generic, entered emergency use authorization within months of pandemic declaration, drawing on existing safety data from its Ebola development program. Both examples confirmed the hypothesis that speed of response scales with the depth of prior characterization.
The problem is not scientific viability. It is money. The same attributes that make generics attractive for repurposing, established safety, off-patent status, low cost of goods, also strip away the commercial incentive that drives private capital into drug development. Method-of-use exclusivity is typically capped at three years in the United States and one year in most European Union jurisdictions. That window rarely supports the full cost of Phase II and Phase III trials. This is the structural contradiction that every innovative financing model discussed below is designed to solve.
Key Takeaways — Section 01
- Generic repurposing reduces development cost by 50 to 60% and compresses timelines by 5 to 14 years relative to new molecular entity development.
- Phase I to approval success rates run approximately three times higher for repurposed drugs than for novel compounds, reflecting the value of pre-existing safety and pharmacokinetic data.
- The core barrier is not scientific or regulatory but economic: short method-of-use exclusivity windows cannot support the capital required for late-stage clinical trials.
- COVID-19 demonstrated that pre-characterized compounds, including off-patent corticosteroids, can reach clinical validation in months rather than years when funding and regulatory fast-tracking align.
02. IP Valuation: The Asset at the Center of Every Repurposing Decision
Before any financing conversation can begin, an IP valuation must anchor the deal. For generic repurposing, this means mapping the full patent estate of the compound in question and determining what, if any, new exclusivity can be constructed around a novel indication. The residual IP position determines whether royalty financing is structurable, whether venture philanthropy can expect a return, and whether a public-private partnership will face competitive dilution before the investment pays off.
Sildenafil: The Canonical IP Valuation Case Study
Pfizer’s sildenafil offers the most instructive lesson in repurposing IP value. The original composition-of-matter patent, US 5,250,534, expired in 2012 for erectile dysfunction. Pfizer had, however, filed a separate use patent covering the treatment of pulmonary arterial hypertension (PAH), which supported the 2005 FDA approval of Revatio. That use patent, US 6,469,012, provided meaningful exclusivity for the PAH indication well past the base patent cliff. The market separation between a low-cost oral tablet for erectile dysfunction and an intravenous formulation for PAH patients in specialized centers created a defensible commercial moat despite the compound’s generic status. The IP valuation lesson: a repurposed generic’s commercial value is not a function of the base molecule’s patent life, but of how many method-of-use and formulation patents can be constructed around the new indication, and whether those patents can be enforced against a generic challenger given the specificity of the prescribing population.
IP Spotlight: Sildenafil / Pfizer
Composition-of-matter patent US 5,250,534 expired 2012. PAH use patent US 6,469,012 extended commercial exclusivity for Revatio beyond the base cliff. The formulation patent for intravenous sildenafil added a further layer. Net lesson: a three-layer patent stack, composition, use, and formulation, is the minimum defensible architecture for a repurposed generic targeting a specialty indication.
Estimated additional IP value from PAH indication relative to a purely generic sildenafil estate: analysts valued Revatio at approximately $1.2B in peak annual revenue at its height, against a base generic market where per-unit prices had collapsed by 98%.
Remdesivir: Emergency-Use IP and the Limits of Crisis Pricing
Gilead’s remdesivir entered COVID-19 treatment under an Emergency Use Authorization that relied partly on its prior Ebola safety dossier, a structure that resembles the 505(b)(2) pathway in its reliance on existing data. The composition-of-matter patents, primarily US 9,724,360 and related family members, were still in force, which allowed Gilead to price Veklury at approximately $3,100 per treatment course for commercially insured patients in the United States. The IP valuation here depends heavily on jurisdiction: Gilead issued voluntary licenses to generic manufacturers in low-income countries through the Medicines Patent Pool, effectively bifurcating the commercial and humanitarian markets. For repurposing analysts, remdesivir illustrates that when a compound is still under composition-of-matter protection, repurposing for an emergency indication does not follow the same economics as repurposing a generic. The financing models discussed below apply specifically to compounds where the base composition patent has expired.
Dexamethasone: The Off-Patent Reference Point
Dexamethasone is the cleaner archetype for generic repurposing IP. The compound has been off patent for decades, manufactured as a commodity, and the Oxford RECOVERY trial cost approximately £1.7 million in total, funded publicly through NIHR. No commercial entity took the indication through approval. No method-of-use patent was pursued at scale. The result: a treatment that reduces mortality in severe COVID-19 patients by roughly one third costs about £5 per course and carries no meaningful IP protection. This outcome illustrates both the public health strength of the generic repurposing model and its commercial weakness. The IP valuation for dexamethasone’s COVID-19 indication is, effectively, zero. That zero is precisely why the financing models in this article exist.
The absence of IP protection for dexamethasone’s COVID-19 use is not a failure of the patent system. It is the patent system working as designed. Generic repurposing’s challenge is constructing an economic architecture that rewards innovation in the absence of exclusivity, not forcing a patent structure onto science that does not support it.
Liraglutide and the GLP-1 Repurposing Frontier
Novo Nordisk’s liraglutide presents a more complex case. As a biologic GLP-1 receptor agonist with composition-of-matter protection through various formulation and device patents (Victoza patents run in a dense cluster through the late 2020s, with biosimilar interchangeability designations expected to become commercially relevant around 2026 to 2028), its repurposing into Alzheimer’s disease, addiction treatment, and NASH is occurring while the base IP is still at least partially intact. The ADDF has funded trials of liraglutide for Alzheimer’s disease. The IP valuation question for any investor considering royalty financing or a venture philanthropy investment in this indication is multidimensional: How much exclusivity remains on the existing formulations? Can a new use patent for Alzheimer’s be prosecuted and defended against a biosimilar liraglutide entrant? What is the dose equivalence between the metabolic and neurological indications, and does a different dosing regimen support a patentably distinct product profile?
IP Spotlight: Liraglutide / Novo Nordisk
Core composition-of-matter patents for liraglutide expired in the EU around 2023. US patent protection via device and formulation claims extends further, with key expiries clustered between 2026 and 2032 depending on jurisdiction and challenge history. Biosimilar semaglutide and liraglutide entrants are in active development across India, China, and established generic manufacturers in the US.
Any method-of-use patent for Alzheimer’s filed on liraglutide will face a prior art challenge given the volume of published mechanistic literature on GLP-1 receptors in the CNS. Prosecuting a formulation-based distinction (e.g., CNS-optimized delivery, modified dosing schedule) offers a more defensible path to exclusivity than pure indication patenting.
Key Takeaways — Section 02
- IP valuation for a repurposed generic is not a single-layer analysis. Composition-of-matter, method-of-use, formulation, and device patents must all be mapped before deal structuring begins.
- Sildenafil’s PAH trajectory demonstrates that a three-layer patent stack can generate $1B+ annual revenue from a compound otherwise trading as a commodity generic.
- Dexamethasone’s zero-IP COVID-19 outcome is the structural model that requires alternative financing architectures; it cannot be solved through better patent prosecution.
- GLP-1 biosimilar interchangeability timelines will materially affect the investability of liraglutide repurposing programs for CNS and other indications. Track ANDA filing activity and Paragraph IV certifications against Novo Nordisk’s device patents.
03. The Evergreening Technology Roadmap
Evergreening refers to the suite of IP strategies through which pharmaceutical companies extend the effective market exclusivity of a drug beyond its original patent cliff. Critics frame it as rent extraction; defenders frame it as the natural economic response to innovation incentives. Both characterizations contain truth. For repurposing analysts, the evergreening toolkit is relevant in two distinct directions: it is the mechanism through which a successful repurposing program can be commercially protected, and it is the mechanism through which an originator can inadvertently (or deliberately) obstruct a generic repurposing effort through dense patent thickets.
The Full Evergreening Toolkit
01
Formulation Patents
Extended-release formulations, novel salt forms, polymorphs, and particle-size modifications can each carry independent patent protection. A repurposed generic targeting a new indication can differentiate through formulation, potentially generating 10 to 20 years of additional exclusivity on a dosage form distinct from the commodity generic. Example: methylphenidate’s transition from immediate-release to Concerta’s OROS osmotic delivery platform generated substantial exclusivity well past the base patent.
02
Method-of-Use Patents
Protecting the specific indication, dosing regimen, patient subpopulation, or co-administration protocol rather than the molecule itself. These are the primary IP tools for generic repurposing but are difficult to prosecute where prior art is dense. The narrower the claim, the more defensible it is, but the smaller the commercial moat. A method-of-use patent claiming treatment of a molecularly defined glioblastoma subtype, for instance, is more prosecutable than one claiming treatment of cancer broadly.
03
Combination Patents
Fixed-dose combinations of a generic compound with a second agent can generate new patent coverage even when each component is individually off patent. The FDA’s 505(b)(2) pathway accommodates this by allowing reliance on the existing safety data of each component. Combination patents are increasingly relevant for repurposing programs in oncology and CNS, where additive or synergistic mechanisms can be characterized and claimed.
04
Prodrug and Metabolite Patents
Chemical modification of a generic compound to a prodrug form or active metabolite can, in some cases, support a composition-of-matter patent on the modified entity while drawing on the originator compound’s safety data. Valdecoxib-to-parecoxib and codeine-to-morphine pathways illustrate the category, though regulatory and toxicological hurdles for this strategy are nontrivial.
05
Device and Delivery System Patents
Particularly relevant for biologics and inhaled or injectable generics. The auto-injector patent portfolio for Humira’s adalimumab is the most-cited example: AbbVie accumulated over 130 patents covering devices, formulations, and manufacturing processes, delaying biosimilar market entry in the US by years after composition-of-matter expiry. A repurposing program that redesigns the delivery system for a new indication, such as a CNS-targeted nanoparticle formulation of an existing anti-inflammatory, can layer device patents onto a method-of-use position.
06
Pediatric Exclusivity Extensions
The Pediatric Research Equity Act (PREA) and Best Pharmaceuticals for Children Act (BPCA) can grant six months of additional market exclusivity for conducting FDA-requested pediatric studies. For a repurposed generic targeting a pediatric indication, this six-month extension applies to all approved indications of the compound, not just the pediatric one, creating disproportionate commercial value relative to the cost of the pediatric study.
Patent Thickets and the Obstruction Problem
The same toolkit that protects a legitimate repurposing investment can also obstruct a generic repurposing program when held by an originator seeking to prevent a therapeutic area competitor. Researchers pursuing low-cost repurposing for neglected diseases routinely encounter broad method-of-use claims filed during the original development program that were never pursued commercially but nonetheless require a freedom-to-operate opinion before any clinical work can begin. This is the Material Transfer Agreement problem at scale: a company sitting on dormant use patents for compounds it has no intention of developing can extract licensing fees or delay timelines for any third party attempting a repurposing program, even when the compound is formally off patent on composition-of-matter grounds.
Freedom-to-operate analysis is not optional for generic repurposing. It is the precondition for any financing conversation. A royalty financing term sheet built on a compound with an unresolved patent thicket is an unsecured liability, not an asset. IP due diligence must map both expired and active claims, including abandoned applications that may have been revived or continued.
Key Takeaways — Section 03
- A commercially viable repurposed generic requires at minimum a method-of-use patent anchored by a formulation or delivery system patent to create a layered exclusivity position that can support the economics of late-stage clinical development.
- Combination patents and pediatric exclusivity extensions offer overlooked pathways to additional market protection at relatively low incremental cost.
- Patent thickets on dormant use claims are a material risk in freedom-to-operate analysis, particularly in therapeutic areas with extensive originator patent portfolios. Map the full claim family, not just issued and active composition patents.
- Biosimilar interchangeability timelines for biologic generics (particularly GLP-1s) require ongoing monitoring through Paragraph IV filings and Purple Book activity, as these affect the commercial horizon for any repurposing investment in the class.
04. Why Generic Repurposing Is a Structural Market Failure
The term “financial orphan” entered the repurposing lexicon because it precisely describes the economic position of a generic compound with a promising new indication and no viable commercial sponsor. The generic manufacturer has no exclusivity to protect. The branded originator has moved on. Academic researchers can generate the hypothesis and perhaps Phase II proof-of-concept data, but Phase III randomized controlled trials require an organization with regulatory sophistication, pharmacovigilance infrastructure, and commercial manufacturing capacity that most academic medical centers do not possess. Contract research organizations can fill some of those gaps, but they do not provide funding.
The exclusivity periods available through existing regulatory mechanisms compound the problem. Three years of new clinical investigation exclusivity under the Hatch-Waxman Act in the United States sounds adequate until one calculates the actual cost of the Phase III trial that earned it, which might run $150 to $400 million depending on indication complexity and required sample size. A generic drug selling at $0.30 per tablet in a competitive market will not generate $400 million in net present value from three years of exclusivity even with complete market share. The economics break before the first trial is enrolled.
Orphan Drug Designation offers a more attractive window, seven years of market exclusivity in the United States and ten years in the European Union, plus a 25% tax credit on qualified clinical trial expenses under the Orphan Drug Tax Credit Act. For a repurposed generic with a mechanistically plausible rare disease indication and a patient population below 200,000 in the US, ODD is often the most commercially defensible regulatory strategy. The complication: if the generic is already commercially available at commodity pricing for its original indication, ODD exclusivity for the new indication does not prevent off-label prescribing, which can neutralize commercial exclusivity in practice. Physicians treating patients with the rare disease can simply prescribe the cheap generic off-label, extracting the clinical benefit without compensating the developer who funded the trial.
This is the market failure in its most precise form: the social value of a new indication for a safe, cheap, established compound can be substantial, potentially billions of dollars in quality-adjusted life years, but the private investor who bears the clinical development cost cannot capture that value because the product cannot be priced above commodity levels when a therapeutically identical generic is simultaneously on pharmacy shelves.
Key Takeaways — Section 04
- Three years of US new clinical investigation exclusivity cannot support a Phase III trial costing $150 to $400 million. The math does not close without additional financing mechanisms.
- Orphan Drug Designation is commercially attractive for rare disease repurposing but is undermined by off-label prescribing of the same molecule at commodity prices for the non-orphan indication.
- The structural failure is a mismatch between social value (high) and private capturable value (low), not a failure of scientific feasibility or regulatory willingness.
05. Venture Philanthropy: Mission Capital and Its Real Limits
Venture philanthropy applies the structural discipline of venture capital, milestone-gated tranches, convertible notes, equity positions, royalty agreements, to organizations whose primary objective is disease impact rather than return on capital. The financial returns generated by any successful investment are recycled into the philanthropic mission rather than distributed to shareholders. This structure allows these organizations to accept risk-adjusted returns that would be unacceptable to a commercial fund, specifically the low or uncertain ROI profile of a repurposed generic where full commercial exclusivity is not available.
The ADDF Architecture
The Alzheimer’s Drug Discovery Foundation is the most sophisticated example of venture philanthropy in the repurposing space. The ADDF deploys capital through convertible notes, equity stakes in early-stage companies, and royalty and milestone agreements with terms benchmarked against commercial venture investors. This benchmarking matters: it ensures that ADDF-funded companies do not accept below-market financial terms simply because the funder is a non-profit, which would create adverse selection in the companies they attract. The ADDF’s focus on IND-enabling studies and Phase I and early Phase II trials targets the precise funding gap that commercial capital systematically ignores for Alzheimer’s repurposing programs.
The ADDF’s AI-driven screening effort, which analyzed electronic health records to identify associations between existing medications and Alzheimer’s risk reduction, generated the finding that sildenafil use correlates with a roughly 70% reduction in Alzheimer’s incidence in retrospective analysis. That finding does not establish causation, and the ADDF is explicit about this, but it generated sufficient scientific interest to support a Phase II/III trial design. The IP position for any sildenafil Alzheimer’s use patent is weak given the prior art, but the venture philanthropy model does not require IP-backed exclusivity to justify the investment. The social return on a successful proof-of-concept is the metric that governs ADDF’s capital allocation, not peak commercial revenues.
Cures Within Reach and the Proof-of-Concept Engine
Cures Within Reach operates at a smaller check size than the ADDF but with a broader therapeutic mandate, funding investigator-initiated proof-of-concept trials across any disease with high unmet need. Its track record of leveraging initial grants into follow-on capital from commercial and governmental sources is notable: a $200,000 CWR grant supporting a Phase IIa study of a generic anti-inflammatory in a rare pediatric condition has, in documented cases, attracted a subsequent $5 to $10 million NIH NCATS award to fund Phase IIb work. This capital multiplication effect is central to the venture philanthropy model’s strategic value: it de-risks projects just enough to move them past the threshold at which commercial or government funders will engage.
CWR’s partnership with Innoplexus to develop AI-powered screening specifically for cancer repurposing candidates reflects the field’s current direction. Combining a systematic computational screening layer with a funding mechanism that can move quickly on low-cost proof-of-concept trials creates a genuinely efficient pipeline, particularly for academic investigators who have compound access and clinical relationships but no commercialization experience.
Investment Strategy — Venture Philanthropy
For institutional investors with ESG mandates or impact allocation targets, co-investment alongside venture philanthropies in late-stage proof-of-concept trials offers a specific entry point. By the time an ADDF or CWR grantee has completed a positive Phase IIa study on a repurposed generic, the asset has undergone de-risking that a commercial investor would typically need to fund entirely. The remaining capital need, a Phase IIb/III trial, is still substantial, but the probability-weighted cost is lower than a clean-sheet development investment.
Royalty agreements on successful outcomes, rather than equity, are often the preferred instrument for co-investors at this stage, given the low IP exclusivity available. Structuring a royalty at a percentage of net sales across a defined geographic territory for a defined indication, with a cap linked to the trial funding contribution, creates a return profile that is positive even on relatively modest commercial uptake.
Key Takeaways — Section 05
- Venture philanthropy accepts lower financial returns in exchange for social impact, making it the natural capital source for repurposed generics where commercial exclusivity is thin or absent.
- The ADDF’s AI-driven sildenafil/Alzheimer’s finding demonstrates that systematic computational screening can generate high-value clinical hypotheses even from deeply characterized compounds; the IP implications of such findings require careful analysis before clinical programs are built around them.
- Cures Within Reach’s capital multiplication model, using small grants to unlock larger government and commercial investment, is the most operationally efficient version of the venture philanthropy structure for generic repurposing.
06. Public-Private Partnerships: Architecture, Mechanics, and Pitfalls
Public-private partnerships in pharmaceutical development are not a single instrument. They range from loose data-sharing consortia between academic medical centers and industry to fully integrated joint ventures with shared governance, equity participation, and commercial rights structures. The common thread is risk distribution across parties with different capital bases, different risk tolerances, and different definitions of success.
The IRDiRC Framework and What It Actually Delivers
The International Rare Diseases Research Consortium launched in 2011 with a mandate to develop 200 new rare disease therapies and generate diagnostic tools for most rare diseases within a decade. Its PPP structure aggregates funding from NIH, the European Commission, patient advocacy organizations, and pharmaceutical companies, with shared data norms and regulatory engagement protocols that reduce the friction cost of multi-site clinical programs. For repurposing programs specifically, IRDiRC’s value lies in its established framework for sharing pre-competitive data: genetic registries, natural history studies, and biomarker datasets that would take any single repurposing developer years and tens of millions of dollars to generate independently.
The practical limitation of IRDiRC-style large-scale PPPs is timeline. Building the legal framework for a consortium, negotiating data use agreements, resolving IP ownership for any discoveries made using shared data, and establishing governance structures that satisfy both academic publication norms and commercial confidentiality requirements typically takes 18 to 36 months before a single clinical experiment is run. For programs targeting urgent unmet needs, this is often an unacceptable delay.
The ‘In-Kind’ Cost Problem
PPPs for generic repurposing face a specific accounting challenge that is frequently underestimated in early-stage planning: in-kind contributions from pharmaceutical company partners, primarily active pharmaceutical ingredient, placebo comparator, and Good Manufacturing Practice documentation, are often carried at internal cost rather than market value, creating misaligned expectations about the total financial exposure each party is accepting. A pharma company contributing $3 million in internal cost of goods may be providing material with a market value of $15 million, substantially shifting the economic burden relative to cash contributions from public funders. Structuring agreements that account for in-kind contributions at market value, rather than book cost, is essential for maintaining equitable risk distribution and avoiding partnership dissolution mid-trial.
Fifty1 AI Labs and the Technology-Enabled PPP
The partnership between Fifty1 AI Labs and BioSpark AI Technologies illustrates a newer PPP model in which the resource being pooled is not cash or drug supply but proprietary data and computational infrastructure. Fifty1’s clinical dataset combined with BioSpark’s AI architecture creates a repurposing screening capacity that neither party could build cost-effectively alone. This asset-light PPP model, where the shared resource is data rather than capital, may prove more scalable and faster to implement than traditional consortium structures, particularly for the hypothesis-generation phase of repurposing work. The commercial IP questions it raises are, if anything, more complex than traditional PPPs: who owns the AI model trained on jointly contributed data, and how are royalties allocated when the model identifies a compound-indication pair that one partner had already partially explored in internal research?
Investment Strategy — PPPs
Corporate partners entering pharmaceutical PPPs for generic repurposing should seek early clarity on three specific terms: commercial rights structure for any approved new indication (exclusive license, co-development rights, or royalty share), data ownership for pre-competitive datasets generated during the collaboration, and exit mechanics if the clinical program fails or if a partner’s strategic priorities shift. Agreements that defer these questions until Phase III completion routinely end in litigation or forced dissolution.
From a portfolio perspective, PPP participation generates value that does not appear on conventional balance sheets: access to regulatory master files, safety data packages, and manufacturing documentation for compounds that would otherwise require expensive re-creation. These assets have real economic value for any downstream royalty financing or out-licensing transaction.
07. Social Impact Bonds and Crowdfunding: The ‘Pay for Success’ Stack
Social Impact Bonds are outcome-based financing contracts in which private investors fund a social program, and a government or institutional payer reimburses those investors only if pre-specified outcomes are achieved. Their application to pharmaceutical development is conceptually elegant and operationally difficult. The basic structure for a generic repurposing SIB runs as follows: impact investors capitalize a Phase II/III randomized controlled trial for an off-patent therapy. If the trial produces results meeting pre-agreed efficacy and cost-effectiveness thresholds, a healthcare payer, whether NHS, Medicare, Medicaid, or a large insurer, pays out an outcome-based fee to the investors. If the trial fails, investors lose their principal.
Quantifying the ‘Success’ Metric
The most technically demanding component of a pharma SIB is defining the outcome metric. Quality Adjusted Life Years gained per patient treated are a natural unit, but converting QALY estimates to a cash payment requires agreement on a QALY value threshold, typically $50,000 to $150,000 in the United States and £20,000 to £30,000 in the UK under NICE guidance. For a repurposed generic where the drug cost is near zero and the treatment effect is moderate, the health system savings argument can be strong: if a $0.30-per-day generic reduces hospital admissions by 20% in a high-burden chronic disease, the net present value of those avoided hospitalizations at, say, $15,000 per admission can generate an outcome payment that adequately compensates trial investors even without IP exclusivity.
Crowd Funded Cures has built the most developed operational framework for this structure. Their model targets Phase II/III trials for off-patent therapies in high-burden diseases, specifically those where the cost-savings argument to payers is numerically clear, such as mental illness, addiction, and infectious disease, where hospitalization rates are high and per-episode costs are well-characterized. The investor repayment mechanism is tied to a percentage of documented cost savings, not to sales revenue, which is the key distinction from royalty financing: the payer is paying for demonstrated value to its own budget, not for the commercial success of a product.
The RDDR SIB: What Happened and Why
The Rare Disease Drug Repurposing SIB piloted by Beacon (formerly Findacure) in the UK reached the structuring phase and demonstrated theoretical NHS cost savings from several rare disease repurposing programs but did not proceed to implementation. The primary obstacles were not conceptual but institutional: NHS England’s procurement and contracting frameworks were not designed to accommodate outcome-based payments for clinical trial costs, and the political cycle created enough uncertainty around NHS budget commitments to make long-term payment guarantees unfeasible for institutional investors. The RDDR SIB experience produced a detailed playbook for how not to structure these instruments, which is itself valuable: future iterations must secure payer commitment earlier, use shorter outcome measurement windows, and incorporate government budget cycle risk into the investor return calculations.
Investment Strategy — SIBs and Crowdfunding
Impact investors evaluating a pharma SIB should demand, before commitment: a signed outcome payment agreement with the payer (not an indication of interest), clearly defined and independently auditable outcome metrics, a trial design powered to detect the minimum effect size that generates a positive outcome payment, and a failure mechanism that clearly specifies at what point investor principal is written off. Structures that leave outcome measurement to post-trial negotiation carry significant basis risk.
For payers, the SIB model is economically rational only when the cost savings from a successful new indication are large enough to generate an outcome payment that exceeds the trial cost plus investor return. High-burden, high-hospitalization chronic diseases meet this threshold more reliably than rare diseases with small patient populations.
08. Royalty Financing: Non-Dilutive Capital Against Revenue Streams
Royalty financing works by selling a defined percentage of a specific product’s net sales to a capital provider in exchange for upfront funds. It is non-dilutive in the equity sense: the company retains ownership, the royalty seller retains operating control, and there is no board seat, no warrant coverage, and no conversion mechanism changing the cap table. The capital provider’s return is entirely a function of how well the product sells.
Royalty Pharma’s Model and What It Means for Generic Repurposing
Royalty Pharma is the largest entity in the pharmaceutical royalty market, with a portfolio generating over $2 billion in royalty receipts annually. Its 2024 deal structure with Revolution Medicines, providing up to $2 billion in committed funding against royalties on RAS-targeted oncology assets, illustrates the scale at which royalty financing now operates in the biopharma sector. The Royalty Pharma model requires: a product with a defined, protectable revenue stream; a royalty basis (typically net sales at rates ranging from 4% to 12% depending on commercial stage and exclusivity remaining); and a term structure that balances investor payoff period against product lifecycle economics.
For generic repurposing, the royalty financing model runs into the same core problem as every other private financing mechanism: low or absent exclusivity generates low and uncertain revenue projections, which generate low royalty values, which cannot support the upfront capital required for late-stage trials. The cases where royalty financing has worked for repurposed assets generally involve either Orphan Drug Designation (which provides sufficient market exclusivity to project revenue streams) or a combination of a new indication with a novel delivery system that carries its own patent protection.
The Remedy Pharmaceuticals / Biogen Transaction
Remedy Pharmaceuticals’ sale of its CNS orphan drug program, CIRARA (intravenous glyburide), to Biogen for $120 million upfront plus milestones and royalties provides a relevant case study. Glyburide is a sulfonylurea antidiabetic that has been generic for decades. Remedy’s repurposing program targeted cerebral edema following large hemispheric infarction, using a specifically formulated intravenous version. The key IP was not the molecule but the IV formulation and its dosing protocol, which supported a defensible patent position and an orphan disease designation for a patient population that could not self-administer an oral tablet. The $120 million upfront valuation reflects: orphan exclusivity duration, the protected formulation IP, clinical proof-of-concept data from Phase II, and Biogen’s platform premium for neurological assets. Without the formulation patent layered onto the orphan designation, the IP estate would have supported a fraction of that valuation.
IP Spotlight: CIRARA (Glyburide) / Remedy Pharmaceuticals → Biogen
Base compound: glyburide, off patent as an oral antidiabetic since the 1990s. Repurposing value derived from: IV formulation patent protecting a specific administration protocol, orphan drug designation for large hemispheric infarction providing 7-year US market exclusivity, and Phase II data demonstrating a mortality reduction signal. Deal value: $120M upfront, milestones, and royalties on net sales, structuring a royalty component appropriate for a late-stage asset with defined exclusivity windows.
The Aspreva / Roche Mycophenolate Structure
Aspreva Pharmaceuticals’ licensing of Cellcept (mycophenolate mofetil) from Roche for lupus nephritis is an earlier example of royalty-based deal structuring for a repurposed application. Mycophenolate had been used off-label for lupus nephritis for years by the time Aspreva completed the randomized trials needed for a labeled indication. Roche’s royalty position reflected its contribution of the existing safety dossier and manufacturing infrastructure. The deal structure compensated the originator for the value of its prior investment while allowing Aspreva to capture the new indication premium through an exclusive license with royalty obligations. The practical lesson: when an originator holds safety data that a repurposing company needs for a 505(b)(2) filing, that data access is a licensable asset, and royalty terms on future sales are the standard compensation mechanism.
Investment Strategy — Royalty Financing
Royalty Pharma and peer royalty aggregators focus on late-stage assets with defined exclusivity periods, limiting their relevance for most generic repurposing programs. The more relevant royalty structure for this segment is a synthetic royalty, where a company raises capital against anticipated sales from a Phase III outcome, rather than against established product revenues. Synthetic royalty rates for repurposed generics with orphan designation in the 4 to 8% range on net sales, combined with a royalty cap at 2 to 2.5x the funded amount, represent a reasonable risk-adjusted structure.
Royalty financing is unsuitable for repurposed generics targeting broad therapeutic areas without exclusivity protection. It is appropriate for programs with orphan designation, a novel formulation patent, or a combination IP position that generates projectable exclusivity of at least five years post-approval.
09. Government Programs: ARPA-H, NCATS, and the Pull-Incentive Architecture
Government investment in generic drug repurposing is the most reliable source of capital for programs that fail all commercial attractiveness tests. NCATS, established within NIH in 2012 specifically to address translational bottlenecks, has funded everything from high-throughput screening of approved compound libraries against neglected disease targets to late-stage investigational new drug application support for academic repurposing programs. Its Rare Diseases Clinical Research Network provides the infrastructure for multi-site trials that individual academic centers cannot sustain alone.
ARPA-H and the MATRIX Platform
The Advanced Research Projects Agency for Health represents a higher-risk-tolerance, faster-moving model than NIH’s traditional grant mechanisms. ARPA-H’s September 2023 award of $48.3 million to Every Cure for the MATRIX platform is the largest single government commitment to AI-driven generic repurposing to date. MATRIX’s design is ambitious: an open-source machine learning platform trained on electronic health records, claims data, pharmacogenomic databases, and published clinical literature, designed to identify compound-indication pairs meeting pre-defined clinical plausibility thresholds, then fund validation studies for the top-ranked matches.
Every Cure’s structure as a non-profit operating under an ARPA-H contract, rather than a commercial licensee, means any discoveries made on MATRIX will be published and freely available rather than proprietary. This is either the model’s greatest strength or its greatest commercial limitation, depending on your perspective. For the field, open-source discovery reduces duplication. For the individual repurposing developer, a MATRIX-identified compound-indication pair enters the public domain immediately, requiring rapid clinical execution and IP strategy to establish any commercial position before competitors do.
NCATS and the Rare Disease Drug Repurposing Portal
NCATS operates the National COVID Cohort Collaborative and the NCATS Pharmaceutical Collection, an annotated library of approximately 2,600 approved drugs available for systematic screening. Its Discovering New Therapeutic Uses for Existing Molecules program provides academic researchers with access to pharmaceutical company investigational compounds plus scientific support, regulatory guidance, and clinical trial infrastructure. The model has funded over 30 disease area collaborations and generated several IND filings for repurposed compounds in rare diseases. The primary limitation is that NCATS’ funding does not extend through Phase III: programs that succeed in NCATS-funded Phase II work face the same financing gap on Phase III that affects all generic repurposing.
Investment Strategy — Government Programs
Companies and academic groups should treat government grants as a first-in capital mechanism that de-risks assets to the point where commercial or philanthropic capital will engage. An NCATS-funded Phase II dataset is a fundable asset for royalty financing or venture philanthropy investment in a way that a purely computational hypothesis is not. The strategic objective for any repurposing program is to use public capital to generate the clinical evidence needed to cross the commercial investor’s minimum evidentiary threshold, then transition to private financing for Phase III.
Monitor ARPA-H program announcements actively. Its funding model, outcome-based contracts rather than grants, creates commercial pathways that are structurally different from NIH mechanisms. ARPA-H contracts can include milestone payments tied to specific clinical or regulatory outcomes, which makes them compatible with commercial timelines in a way that standard NIH grants are not.
10. Interventional Pharmacoeconomics + Advance Market Commitments
The University of Chicago Market Shaping Accelerator’s 2025 white paper on generic drug repurposing introduced a specific architecture for combining Interventional Pharmacoeconomics (IVPE) with Advance Market Commitment (AMC) structures to create a self-sustaining financing mechanism for generic repurposing programs. The proposal addresses the core market failure directly rather than working around it.
How the IVPE + AMC Structure Works
Interventional Pharmacoeconomics starts from a cost-effectiveness analysis: what is the incremental cost-effectiveness ratio of a repurposed generic in its proposed new indication versus standard of care? If the ICER is below the prevailing willingness-to-pay threshold, say $50,000 per QALY in a Medicaid context, then the healthcare system stands to gain value from widespread adoption of the repurposed generic. IVPE quantifies that gain as a dollar value per patient treated over a defined time horizon. That quantified savings number becomes the basis for the AMC.
An Advance Market Commitment is a legally binding commitment by a payer, a government agency, a large insurer, or a coalition of both, to purchase a defined quantity of a product at a pre-agreed price if that product meets specified clinical performance criteria. AMCs were used successfully in the vaccine market to accelerate pneumococcal vaccine development for low-income countries, where GAVI committed $1.5 billion to purchase qualifying vaccines at a price above the marginal cost of production, creating the demand signal that justified manufacturer investment in production scale-up. The same structure, applied to a repurposed generic’s new indication, tells a potential clinical trial sponsor: if your trial succeeds and the drug meets the ICER threshold, we will pay a defined price for a defined quantity of treatment, generating a return that justifies the trial investment.
The Financial Architecture in Detail
For a concrete illustration: a repurposed generic antifungal for a rare systemic mycosis has commodity drug costs of approximately $0.20 per dose. A randomized trial demonstrating a 30% reduction in 30-day mortality relative to amphotericin B would generate an IVPE value of approximately $28,000 per QALY gained (based on avoided ICU admissions and mortality costs in a 200-patient population). An AMC committing CMS or a state Medicaid program to purchase treatment courses at $800 each, rather than $0.20, for a defined period following approval creates a revenue stream against which a small specialty company or a non-profit clinical development organization can structure royalty financing for the Phase III trial. The AMC functions as the IP substitute: it creates the exclusivity premium that the patent system cannot generate for an off-patent compound, but it generates it through a payer commitment rather than a legal monopoly.
This model is at the proposal stage as of early 2026. No large-scale pharmaceutical AMC for a repurposed generic has been fully implemented in the United States. CMS’s existing mechanisms for value-based contracts and indication-specific pricing are the closest operational analogs, and their use for repurposed generics remains limited by regulatory complexity and payer risk aversion.
Investment Strategy — IVPE + AMC
This is an emerging mechanism that requires policy development before it is commercially operational. The investment priority now is advocacy and pilot structuring: engaging with CMS, CMMI, and state Medicaid agencies to design AMC pilot programs for 2 to 4 high-value generic repurposing candidates where the IVPE analysis is clear and the trial cost is bounded. Proving the mechanism works at a small scale, say a single rare disease indication with a documented 40% reduction in expensive hospitalizations, creates the template for broader adoption.
Companies and health systems that lead the structuring of these pilots will have first-mover commercial advantage when the mechanism scales. The relevant skill set is at the intersection of health economics, regulatory policy, and corporate finance, a rare combination that commands a premium in the current talent market.
11. AI and Computational Repurposing: Full Technology Roadmap
Computational drug repurposing is not a single technology. It is a layered stack of analytical approaches applied sequentially from hypothesis generation through clinical validation. Each layer has a different cost profile, data requirement, and predictive accuracy, and each maps onto a different stage of the development and financing pipeline.
Layer 1: Chemoinformatic Similarity and Pharmacophore Mapping
The foundational layer. Computational tools compare the three-dimensional pharmacophore of a known active compound against a library of approved drugs, identifying structural matches that suggest shared receptor interactions. This layer costs very little, processes thousands of compounds in hours, and generates a long list of hypotheses with low individual probability of clinical success. Its primary value is candidate generation for further filtering, not prioritization. DrugBank, ChEMBL, and the NCATS Pharmaceutical Collection provide the compound libraries. The IP relevance: chemoinformatic similarity data can provide evidence in support of an obviousness challenge against a method-of-use patent claiming a new indication, if the structural similarity to a compound already used in that indication is demonstrable.
Layer 2: Network Pharmacology and Knowledge Graphs
Network-based approaches map drug-protein-disease interaction networks derived from genomic, transcriptomic, and proteomic databases. A drug that hits protein A, which interacts with proteins B and C in a pathway dysregulated in disease X, is identified as a repurposing candidate for disease X regardless of structural similarity to existing disease X treatments. Graph neural networks trained on these interaction networks can rank candidates by biological plausibility with substantially higher precision than chemoinformatic similarity alone. The ARPA-H MATRIX platform uses a variant of this approach, drawing on EHR data to identify real-world compound-outcome associations as additional training signal.
Layer 3: In Silico Clinical Simulation and Electronic Health Record Mining
Electronic health record databases, particularly large multi-site systems such as the Veterans Affairs Corporate Data Warehouse (14 million patients) and the PCORnet distributed network (70 million patients), allow retrospective analysis of medication exposure and clinical outcomes at population scale. A repurposed generic candidate identified at Layer 2 can be subjected to a propensity-score-matched retrospective analysis of EHR data to estimate real-world effect size before a single prospective patient is enrolled. The sildenafil-Alzheimer’s association identified by ADDF’s computational program used this approach, mining an EHR cohort of approximately 7.2 million patients. These retrospective analyses are not clinical trial evidence, but they shift the prior probability of clinical success substantially and provide critical input for phase II trial design and power calculations.
Layer 4: Wet Lab Validation and Organoid Models
Before human studies, AI-identified candidates require wet lab confirmation of the proposed mechanism. Patient-derived organoids, three-dimensional tissue constructs grown from disease-relevant cell types, have shortened this validation step substantially for oncology and rare genetic diseases. A compound identified computationally as active against a cancer driver mutation can be tested in patient-derived tumor organoids in 8 to 12 weeks, providing mechanistic confirmation before an IND is written. The cost of this validation step has dropped from hundreds of thousands of dollars to tens of thousands over the past decade, making it a routine pre-IND component rather than a major capital commitment.
Layer 5: Adaptive Trial Design and Bayesian Optimization
Modern Phase II and III trial designs for repurposed generics increasingly use adaptive randomization, seamless Phase II/III transitions, and Bayesian statistical frameworks that allow early stopping for efficacy or futility without the alpha-inflation problems of frequentist interim analyses. For a repurposed generic where the budget is constrained and the evidence prior is moderate (positive EHR signal, organoid validation, plausible mechanism), an adaptive design can reduce the required sample size by 20 to 40% relative to a conventional fixed design, directly reducing trial cost and therefore financing need.
Table: AI/Computational Repurposing Technology Stack
| Layer | Methodology | Data Input | Cost Range | Output / Use Case |
|---|---|---|---|---|
| 1 — Chemoinformatic | Pharmacophore mapping, QSAR models | ChEMBL, DrugBank, PubChem | $5K–$50K | Long-list candidate generation |
| 2 — Network Pharmacology | Graph neural networks, PPI network analysis | STRING, BioGRID, GTEx, OMIM | $50K–$500K | Mechanistically ranked candidate shortlist |
| 3 — EHR Mining | Propensity-matched retrospective cohort, NLP | VA CDW, PCORnet, TriNetX, Optum | $200K–$2M | Real-world effect size estimate, trial design input |
| 4 — Wet Lab Validation | Patient-derived organoids, target engagement assays | Disease-specific cell lines, primary tissue | $50K–$300K | Mechanistic confirmation, IND-enabling package |
| 5 — Adaptive Trials | Bayesian adaptive randomization, seamless Phase II/III | Prospective clinical enrollment | $5M–$150M | Regulatory-grade efficacy evidence, NDA/sNDA support |
Key Takeaways — Section 11
- AI-driven repurposing is a five-layer process from cheminformatic screening through adaptive clinical trials; investors need to understand where in this stack any given program sits before assigning development risk.
- EHR mining at scale (ARPA-H MATRIX, VA Corporate Data Warehouse) now provides real-world effect size estimates that materially de-risk Phase II trial design and reduce required sample sizes.
- Adaptive trial designs can reduce Phase III sample size requirements by 20 to 40%, directly lowering the capital threshold that makes generic repurposing economically viable.
- AI companies active in this space, including Healx, SOM Biotech, AI Therapeutics, and Innoplexus, each occupy different layers of the stack. Due diligence should map their specific technological positioning rather than treating ‘AI for drug repurposing’ as a homogeneous category.
12. Market Size, Regional Dynamics, and Investment Trends
The global drug repurposing market was valued at approximately $34.98 billion in 2024 across all compound types and is projected to reach $59.30 billion by 2034 (Precedence Research, 5.42% CAGR). Alternative sizing from Roots Analysis sets the market at $29.4 billion in 2024 growing to $37.3 billion by 2030 at 4.1% CAGR. The variance between these estimates reflects methodological differences in how generic repurposing is distinguished from branded repurposing, and how compassionate use and off-label markets are treated. For investment purposes, the direction of travel is unambiguous even if the absolute numbers are debated.
Table: Global Drug Repurposing Market Projections (Selected Sources)
| Source | 2024 Value | Projected Value | CAGR | Dominant Region |
|---|---|---|---|---|
| Precedence Research | $34.98B | $59.30B (2034) | 5.42% | North America (47%) |
| Roots Analysis | $29.4B | $37.3B (2030) | 4.1% | North America |
| Business Research Insights | — | $56.25B (2033) | 11% | Asia Pacific (fastest growth) |
| U.S. Submarket (Precedence) | $12.49B | $21.55B (2034) | 5.60% | — |
| China Submarket | — | $7.6B (2030) | 7.5% | — |
North America’s 47% market share reflects the US regulatory environment’s relative accommodation of 505(b)(2) approvals, the density of academic medical centers generating repurposing hypotheses, and the concentration of venture philanthropy and specialized life science funds. Asia Pacific’s faster projected growth reflects lower R&D cost structures in India and China, growing domestic generics industries seeking new commercial differentiation, and rapidly expanding healthcare infrastructure that creates patient access markets for repurposed therapies at price points that are commercially irrelevant in the US.
The Contract Research Organization outsourcing segment is anticipated to grow at 20 to 25% annually within the repurposing market, driven by academic investigators and small biotechs contracting out clinical operations, biostatistics, and regulatory affairs for Phase II studies. This creates a second-order investment opportunity in specialized CROs with repurposing-specific capabilities, particularly those with experience in adaptive trial design and rare disease clinical networks.
Investment Strategy — Market Dynamics
For institutional investors, the repurposing market’s growth is less relevant as a direct investment target than as a signal of deal flow and exit environment. What matters operationally: the increasing number of NCATS-funded Phase II datasets creates a pipeline of de-risked assets that are potentially financeable through royalty or SIB structures at costs well below fully capitalized Phase III programs. Monitoring NCATS grantee publications and IND filings is a low-cost deal sourcing mechanism for this segment.
Asia Pacific manufacturing partnerships offer a cost reduction pathway for generic repurposing programs where drug supply cost is a constraint on trial feasibility. Indian API manufacturers can produce clinical-grade material for many repurposing candidates at 5 to 15% of US or European sourcing costs, directly reducing the capital requirement for Phase III and commercial launch.
13. Patent Intelligence Infrastructure: DrugPatentWatch
Every repurposing decision begins with a patent landscape analysis. The question is whether that analysis is performed manually, incompletely, and weeks after the clinical hypothesis was formed, or whether it is integrated into the hypothesis generation process itself through a purpose-built intelligence platform. These two approaches produce different outcomes in competitive timing, IP strategy, and deal structure.
The Core Capabilities Relevant to Repurposing Teams
DrugPatentWatch provides patent coverage across 134 countries, with integration of Orange Book listing data, paragraph IV certification filings, regulatory approval status, and litigation history for each tracked compound. For a repurposing team, the combination of these data layers in a single searchable interface solves what would otherwise be a multi-week, multi-database research exercise into a query that returns actionable intelligence in hours.
The patent expiration calendar is operationally critical for opportunistic repurposing programs: it allows a systematic screen of compounds whose composition-of-matter protection is expiring or recently expired, filtered by therapeutic category, mechanism of action, and disease area, identifying windows where a new indication could be pursued without triggering composition-of-matter litigation from an originator. Layered against the regulatory status database, this identifies compounds that are both off-patent and already commercially available as generics, meaning API supply chains and manufacturing documentation exist.
The Paragraph IV filing tracker is equally important for risk management. A Paragraph IV certification against a patent that covers a repurposing program’s proposed new indication is an early warning signal that another party has assessed the same IP as challengeable, which affects both freedom-to-operate analysis and the strategic timing of clinical programs. If a Paragraph IV filer is 30 months into an ANDA litigation cycle against a key method-of-use patent, the commercial exclusivity that anchors a royalty financing term sheet may be shorter than the base term suggests.
AI Research Assistant and Portfolio Forecasting
DrugPatentWatch’s AI research assistant synthesizes patent landscapes, competitive analyses, and regulatory timelines in response to natural language queries, allowing R&D teams and IP counsel to conduct preliminary freedom-to-operate assessments and competitive intelligence reviews without requiring a full external search. For portfolio management teams allocating development budgets across multiple repurposing candidates, the forecasting tools quantify budget requirements tied to specific patent expiration scenarios, license fee obligations, and generic entry timing, making capital allocation decisions more precise.
Patent intelligence is not a post-hoc legal checkmark. For generic repurposing, it is the precondition for every financing conversation. A venture philanthropist, SIB investor, or royalty financier will perform their own IP due diligence before committing capital. Teams that arrive with a fully mapped patent landscape, including active claims, expired claims, pending applications, and Paragraph IV activity, compress due diligence timelines by weeks and signal the operational competence that sophisticated capital providers require.
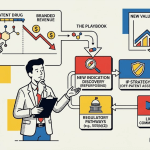
14. Master Investment Framework for Analysts
The financing model that works for a given generic repurposing program depends on five variables: the strength of the IP position available for the new indication; the stage of clinical evidence already generated; the disease area’s unmet need and healthcare system cost burden; the commercial market size for the new indication; and the timeline to cash flow that any investor must accept given the clinical stage. These variables interact, and the analyst’s task is to map their specific combination onto the financing architecture that can bridge the current gap.
Table: Financing Model Selection Framework
| Program Profile | IP Position | Recommended Financing Stack | Key Risk |
|---|---|---|---|
| Rare disease, preclinical hypothesis | Weak (no exclusivity available) | Government grant (NCATS/ARPA-H) + Venture philanthropy | Proof-of-concept failure; no capital transition path to Phase III |
| Rare disease, Phase II data, Orphan Designation | Moderate (ODD + formulation patent) | Royalty financing or venture philanthropy convertible note + PPP for Phase III | Off-label prescribing undercutting ODD commercial exclusivity |
| High-burden chronic disease, clear ICER savings | Weak to none | Social Impact Bond + AMC commitment from payer | SIB structuring complexity; payer commitment not secured pre-trial |
| Specialty indication, novel delivery system | Strong (formulation + use patents stacked) | Commercial VC + Synthetic royalty financing | Formulation patent challenge; Paragraph IV ANDA filing |
| Global health / neglected disease, no commercial market | None required | PPP + Advance Market Commitment + Philanthropic capital | AMC funding commitment not legally binding; payer priority shift |
A few structural observations for analysts building deal screening frameworks. First, the financing model is not independent of the regulatory strategy: programs pursuing 505(b)(2) with reliance on originator safety data need the originator’s right of reference or a published literature package that substitutes for it. The 505(b)(2) pathway’s value as a cost-reduction mechanism only materializes if the data reliance is clean; if the originator challenges the right of reference, legal costs can eliminate the savings. Second, the decision to pursue Orphan Drug Designation must account for the off-label prescribing risk before the designation is used as the primary commercial protection justification in a financing pitch. Third, any royalty financing structure for a repurposed generic should include an explicit scenario analysis for generic entry into the new indication before the royalty cap is reached, with a floor payment mechanism or alternative repayment pathway in that scenario.
Master Key Takeaways
- Generic repurposing’s market failure is structural, not incidental. Solving it requires a purpose-built financing architecture, not a larger budget allocated to conventional development models.
- IP valuation must precede financing conversations. The available exclusivity period determines which financing instrument is structurable and at what cost of capital.
- Venture philanthropy funds the hypothesis-to-Phase-IIa gap. Government programs (NCATS, ARPA-H) fund the Phase IIa-to-Phase IIb gap. Commercial capital, royalty financing, or SIBs fund Phase III. Mapping this capital cascade correctly at the program outset determines whether a repurposing program reaches patients or dies at the Phase II transition.
- AI computational stacks have compressed the hypothesis generation cost by two orders of magnitude over the past decade. The binding constraint is no longer finding candidates; it is financing their clinical validation.
- Adaptive trial designs should be standard for generic repurposing programs, not aspirational. A 25% sample size reduction on a $100M Phase III trial is $25M in saved capital that does not need to be raised.
- The IVPE + AMC model from the University of Chicago Market Shaping Accelerator is the most conceptually complete solution to the generic repurposing market failure. It is policy-stage today, but analysts should position for its eventual implementation in US federal healthcare programs.
- DrugPatentWatch and analogous patent intelligence platforms convert what would be multi-week, multi-database IP research into deal-stage input, enabling faster screening of compound estates and earlier identification of competitive risks in the financing timeline.
15. FAQ
What is the difference between a 505(b)(1) and 505(b)(2) NDA for a repurposed generic, and when does the choice affect financing?
A 505(b)(1) application requires the applicant to own or have right of reference to all safety and efficacy data supporting the application, meaning entirely original clinical trials. A 505(b)(2) application allows reliance on published literature or FDA’s findings from a previously approved product, meaning the applicant can cite the originator’s approved safety package without owning or licensing it directly, provided the data is publicly available or the FDA’s prior finding is explicitly incorporated. The 505(b)(2) pathway reduces trial cost and timeline by enabling a more targeted efficacy package, which directly affects how much capital needs to be raised and therefore which financing instruments are viable. For a repurposed generic targeting a new indication, 505(b)(2) is almost always the preferred regulatory route.
How does biosimilar interchangeability designation affect repurposing economics for biologic generics like GLP-1 agonists?
Biosimilar interchangeability designation from the FDA means a pharmacist can substitute the biosimilar for the reference biologic without a physician’s intervention, which substantially expands biosimilar market penetration relative to a non-interchangeable designation. For a biologic compound being repurposed into a new indication, an interchangeable biosimilar entering the reference product’s existing indication simultaneously creates commodity pricing pressure that can eliminate the commercial margin supporting a royalty financing structure for the new indication, unless the new indication is covered by a separate formulation patent or a use patent that the biosimilar does not automatically carry. Tracking Purple Book listings and interchangeability applications from FDA is essential for any biologic repurposing program financing analysis.
Why do Social Impact Bonds for pharmaceutical development require pre-committed payer agreements rather than post-trial negotiation?
A SIB’s risk transfer mechanism, in which investors bear trial failure risk in exchange for an outcome payment, only functions if the outcome payment is certain when the outcome is achieved. If payers retain discretion over whether to pay after a successful trial, investors are bearing both clinical risk and payer political risk. Healthcare budget cycles, administrative changes, and shifting policy priorities all affect the payer’s willingness to honor a non-legally-binding commitment. Structuring the outcome payment as a contractually binding obligation at the SIB’s inception, with specific outcome metrics, payment amounts, and enforcement mechanisms, is the technical requirement that separates a financeable SIB from a conceptual exercise.
What does Paragraph IV litigation history on a compound tell a repurposing investor?
A Paragraph IV certification is a generic manufacturer’s challenge claiming that a listed patent is either invalid or will not be infringed by the generic’s product. A successful Paragraph IV challenge demonstrates that the specific patent in question was unable to withstand judicial scrutiny, which weakens any repurposing program’s reliance on that patent for commercial exclusivity. Conversely, a Paragraph IV challenge that was settled with a reverse payment (originator pays the generic to delay market entry) and is subsequently challenged under antitrust law signals a weak patent position that an originator chose to buy out rather than defend. Full Paragraph IV litigation history on any patent being used to justify commercial exclusivity in a royalty financing term sheet is mandatory due diligence.
How should an R&D portfolio team prioritize which generic compounds to screen for repurposing potential given limited resources?
Prioritization should run through four filters in sequence. First, established safety profile depth: compounds with extensive post-marketing safety data in large patient populations carry lower Phase I equivalence risk than compounds with limited real-world exposure. Second, mechanistic plausibility in the target indication: computational screening (network pharmacology or EHR mining) should confirm a positive signal before any resources are committed to wet lab work. Third, IP landscape feasibility: a freedom-to-operate analysis should confirm that a defensible exclusivity position is constructable for the new indication, whether through method-of-use, formulation, or ODD, before clinical planning begins. Fourth, payer value alignment: the ICER for the proposed new indication should be below prevailing willingness-to-pay thresholds, and the healthcare system savings should be large enough to support an AMC or SIB structure if traditional exclusivity is unavailable. Compounds passing all four filters are fundable. Those failing the third or fourth are candidates for government grant funding rather than commercial development.
SOURCE ARTICLE: DrugPatentWatch.com — ‘Innovative Financing Models for Repurposing Generic Drugs’ (July 2025) / drugpatentwatch.com
ADDITIONAL SOURCES CITED IN ORIGINAL: PMC/Pushpakom et al. (PMC9336118) • PMC/Kesselheim et al. (PMC10627937) • FDA Generic Drug FAQs • Precedence Research Drug Repurposing Market 2025 • ARPA-H MATRIX Award (Sept 2023) • University of Chicago Market Shaping Accelerator (2025) • Royalty Pharma / Revolution Medicines (2024) • Crowd Funded Cures • Debevoise Royalty Financing Overview • Covington & Burling Synthetic Royalty Study • Duke Health Policy Drug Repurposing for Pandemic Innovation
DISCLAIMER: This document is for informational and analytical purposes only. Nothing herein constitutes investment, legal, or regulatory advice. Patent landscapes and market data are subject to ongoing change; verify all claims against current primary sources before acting on them.