The Patent Cliff: Scope, Mechanics, and What’s Different This Cycle
The pharmaceutical industry will lose exclusivity on products generating an estimated $236 billion in annual revenue between 2025 and 2030. That figure, cited by GeneOnline and corroborated by IQVIA modeling, covers nearly 70 high-revenue products spanning oncology, immunology, cardiovascular, and diabetes franchises. It is the largest single wave of loss of exclusivity (LOE) in industry history, and it arrives with a structural composition that prior cycles did not face: a heavy weighting toward biologics.
The 2008-2012 patent cliff was predominantly a small-molecule event. Lipitor, Plavix, Singulair — large oral brands with well-understood Hatch-Waxman generic entry mechanics. The current cliff is different. Keytruda (pembrolizumab), Dupixent (dupilumab), Stelara (ustekinumab), Skyrizi (risankizumab), Tremfya (guselkumab) — the products anchoring revenue at Merck, Regeneron, J&J, AbbVie, and others — are large-molecule biologics whose post-LOE erosion follows a slower, but still structurally damaging, curve than small molecules.
Small Molecule vs. Biologic LOE: Erosion Mechanics
For a small-molecule oral drug, the Hatch-Waxman Act’s Abbreviated New Drug Application (ANDA) pathway allows generic manufacturers to establish bioequivalence without repeating full clinical trials. Upon LOE, generic entrants typically achieve price points 80-90% below the reference listed drug (RLD) within 12 months. Branded market share collapses accordingly. NBER research shows branded oral drugs retain roughly 25% price premium after generic entry, while physician-administered drugs (largely injectables) see price declines between 38% and 48%. Market share tells a starker story: generics capture up to 90% of unit volume within months.
Biologic erosion is measurably slower, though no less inevitable. The Biologics Price Competition and Innovation Act (BPCIA) created the biosimilar approval pathway (351(k)), but the evidentiary requirements are more demanding than ANDA. A biosimilar sponsor must demonstrate analytical similarity, pharmacokinetic/pharmacodynamic similarity, and immunogenicity comparability. Achieving the ‘interchangeable biosimilar’ designation, which grants automatic pharmacy-level substitution rights comparable to a generic, requires an additional switching study under FDA’s guidance. Only a subset of approved biosimilars carry that designation. The result: biologics lose 30-70% of revenue in the first post-LOE year, not 80-90%, and the decline extends over a longer curve.
The distinction matters for IP valuation and revenue modeling. A biologic franchise with four to six biosimilar entrants in year two post-LOE behaves differently than an oral drug facing 12 ANDA filers on day one. Portfolio managers should model both scenarios separately, not apply a uniform LOE haircut across a pipeline.
The Regulatory Architecture Driving Generic Entry Speed
The FDA’s Competitive Generic Therapy (CGT) designation, created under FDASIA 2017, accelerates review for generic drug applications where there is insufficient generic competition. A drug with fewer than three approved generics may qualify, giving first applicants eight months of exclusivity on top of whatever Hatch-Waxman 180-day exclusivity applies from a Paragraph IV filing. Generic manufacturers treat CGT designations as early movers’ advantages, filing ANDAs years before LOE in anticipation.
For brands, this means competitive intelligence on ANDA filing activity is a leading indicator of how early and how aggressively generic entry will hit. The Orange Book lists all patents and exclusivities associated with each NDA. Paragraph IV certifications (challenging a listed patent as invalid or not infringed) trigger automatic 30-month stays and signal which products generic manufacturers are targeting most aggressively. Any IP team not monitoring Paragraph IV activity against its own portfolio is operating blind.
The Keytruda Problem: IP Valuation at Scale
Keytruda’s situation is worth examining in detail because it illustrates the structural complexity of biologic IP at the enterprise level. Pembrolizumab generated approximately $25 billion in 2023 revenue, making it the best-selling drug in the world. Its core composition-of-matter patent (US 8,354,509) covers the antibody itself and is listed in the Purple Book (the biologic equivalent of the Orange Book). That patent expires in 2028. Merck has built secondary patent protection around specific formulations, manufacturing processes, dosing regimens, and combination uses — a standard biologic patent thicket designed to extend effective market exclusivity beyond the primary compound patent.
The IP valuation question for analysts: what portion of Keytruda’s $25 billion revenue base remains defensible post-2028? The answer is not binary. Biosimilar entry will be staggered across indications and geographies. Markets with biosimilar interchangeability frameworks (the US, post-FDA designation) will erode faster. Markets without automatic substitution policies will erode more slowly. Japan, South Korea, and several EU member states have distinct biosimilar uptake rates that differ materially from US patterns. A geography-stratified LOE model is the only analytically defensible approach.
Merck’s own hedge is Keytruda’s subcutaneous formulation, which is under regulatory review. If approved, the SC formulation carries new IP and potentially new exclusivity periods independent of the IV formulation’s patent expiry. That is evergreening in its most clinically grounded form — a delivery innovation that generates genuine patient benefit while extending IP protection.
Key Takeaways: The Patent Cliff Context
The $236 billion figure is the headline, but the strategic implication is the composition shift toward biologics with slower but prolonged erosion curves. Companies that model post-LOE revenue using small-molecule decay rates on biologic franchises will systematically underestimate residual value. IP teams should track Purple Book biosimilar application filings and Orange Book Paragraph IV activity as real-time indicators of competitive intent. Analysts pricing LOE risk into valuations need geography-stratified models that account for biosimilar interchangeability status and local substitution policy.
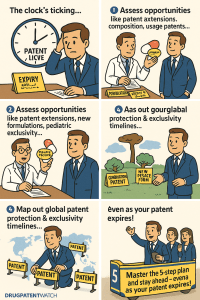
Step 1: Build Your Patent Expiration Strategy 3-5 Years Out
The most common mistake pharma companies make when facing patent expiration is treating it as an event rather than a process. By the time a patent’s expiry date appears on an investor relations slide, the commercially viable response window has largely closed. Effective LOE strategy requires a planning horizon of at least three to five years, and for complex biologic franchises managing biosimilar interchangeability risk, five to seven years is more defensible.
The LOE Strategy Workstream: What It Actually Covers
An LOE strategy is not a single plan. It is a set of parallel workstreams that each operate on different timelines and require different organizational capabilities. IP and legal teams need to audit the full patent portfolio against every listed NDA and BLA, mapping compound patents, formulation patents, method-of-use patents, and process patents to their individual expiry dates and assess the realistic litigation risk of each. Commercial teams need to model how quickly payer formularies will shift to generic or biosimilar alternatives after LOE, which is a function of the drug’s therapeutic category, payer mix, and existing rebate contracts. R&D needs to assess whether next-generation compounds or formulation innovations are sufficiently advanced to hold market share during the transition. Manufacturing needs to evaluate whether post-LOE cost structures are competitive enough to survive price compression.
None of these workstreams can substitute for the others. A company with a bulletproof patent thicket but an uncompetitive manufacturing cost structure will still see margin collapse. A company with best-in-class next-generation compounds but no payer transition strategy will lose formulary position to biosimilars before the next-gen product launches.
The Cross-Functional LOE Team: Structure and Authority
The LOE response team needs genuine cross-functional authority, not advisory status. The most functional models give the LOE team a dedicated budget, executive sponsorship at the C-suite level, and clear decision rights over product lifecycle investments. This team typically draws from R&D, commercial, legal and IP, manufacturing and supply chain, regulatory affairs, and finance. The team needs a program management office capable of tracking interdependencies between workstreams, because delays in regulatory submissions for next-generation formulations, for example, directly affect the commercial transition timeline.
A common structural failure is subordinating the LOE team to the brand team managing the at-risk product. Brand teams are incentivized to maximize near-term revenue, which can conflict with LOE strategy decisions like pricing down to defend volume, launching authorized generics that cannibalize branded sales, or accelerating promotion of the next-generation compound at the expense of the base product.
Patent Portfolio Audit: Mapping Expiry Dates to Revenue
The first technical output from an LOE strategy process is a patent expiry map that correlates each listed patent with its associated revenue protection. This is more complex than it appears. A single NDA may have 20 or more patents listed in the Orange Book, with expiry dates ranging over a decade. The relevant question is not when the last patent expires but when the portfolio’s collective strength becomes insufficient to prevent commercially viable generic entry.
The analysis requires an assessment of each patent’s litigation durability. Formulation patents and method-of-use patents are, on average, more vulnerable to invalidity challenges than composition-of-matter patents. A generic manufacturer filing a Paragraph IV certification on a formulation patent is making a calculated bet that the patent will not survive a district court challenge, either on obviousness grounds or because the specification fails to provide adequate written description support. IP teams should maintain internal ratings for each listed patent’s litigation durability, updated as relevant case law evolves at the Federal Circuit.
Scenario Modeling for LOE Revenue Curves
Quantitative scenario modeling should drive the LOE strategy, not vice versa. The modeling framework needs at least three scenarios: a base case assuming an orderly generic entry at primary patent expiry, a bear case assuming a successful Paragraph IV challenge that accelerates LOE by two to three years, and a bull case assuming litigation success that holds off generic entry until the last listed patent expires. Each scenario maps to different revenue curves, different investment thresholds for lifecycle management tactics, and different M&A urgency levels.
The discount rate applied to post-LOE revenue streams is a matter of significant analytical judgment. Many portfolio managers use a step-up in discount rate at LOE, reflecting the shift from monopoly pricing to competitive market dynamics. The appropriate step-up depends on therapeutic category, generic manufacturer filing intensity, payer behavior, and the specific LOE scenario being modeled.
Key Takeaways: LOE Strategy Fundamentals
Start the formal LOE process no later than five years before primary patent expiry, and seven years for biologic franchises managing biosimilar interchangeability risk. The LOE team needs independent decision rights and C-suite sponsorship. Patent portfolio audits should assess litigation durability, not just expiry dates. Revenue scenario models should include Paragraph IV challenge scenarios as standard inputs, not edge cases.
Step 2: Execute a Layered IP Defense Before LOE
IP defense before LOE is the most technically dense area of pharmaceutical strategy and the one where legal and commercial teams most often talk past each other. The goal is to construct a patent thicket — a cluster of overlapping IP covering different aspects of the drug and its use — that collectively extends effective market exclusivity beyond the primary compound patent.
The Patent Thicket: Architecture and Limits
A well-constructed patent thicket for a small-molecule drug covers, at minimum, the active pharmaceutical ingredient (composition of matter), specific polymorphic forms of the API, pharmaceutical formulations (including excipients, particle sizes, and release profiles), methods of manufacture, and methods of treatment for each approved indication. For a biologic, the thicket extends to specific antibody sequences, glycosylation profiles, conjugation chemistry, formulation buffers, device-drug combinations, and dosing regimen patents.
The commercial value of each layer differs significantly. Composition-of-matter patents are the most valuable because they block all generic versions of the molecule, not just specific formulations. When a composition-of-matter patent expires, the effective protection of the thicket shifts to formulation and use patents, which are individually narrower in scope. A generic manufacturer can potentially design around a formulation patent by using different excipients, different release technologies, or a different particle size specification while still achieving bioequivalence.
The Federal Circuit’s evolving case law on obviousness-type double patenting (ODP) has constrained some thicket-building strategies, particularly the use of continuation patents to generate later expiry dates on claims that are not patentably distinct from the parent. Patent prosecutors working on pharma portfolios need to actively model ODP risk for each continuation filing.
Paragraph IV Litigation Strategy: The 30-Month Stay
When a generic manufacturer files an ANDA with a Paragraph IV certification against a listed patent, the brand company has 45 days to file suit. Filing suit triggers an automatic 30-month stay on FDA approval of the ANDA, giving the brand time to litigate. The strategic value of the 30-month stay depends on how early the Paragraph IV is filed relative to LOE, and how many patents are listed in the Orange Book.
A brand company with multiple Orange Book-listed patents can, in theory, trigger multiple 30-month stays in sequence, though the FDA’s regulations and court rulings have constrained daisy-chaining. The practical litigation strategy is to focus resources on defending the highest-value patents, those with the broadest claims and the best litigation record, while using the stays to preserve revenue through the litigation period. Settlement negotiations during the stay period, including authorized generic agreements, are common and are subject to FTC scrutiny under the Actavis framework for reverse payment settlements.
Regulatory Exclusivity: Stacking Independent of Patent Protection
Regulatory exclusivity operates independently of patent protection and is frequently underutilized in LOE planning. New Chemical Entity (NCE) exclusivity grants five years of data exclusivity for a new molecular entity, blocking ANDA filings during that period regardless of patent status. New Clinical Investigation (NCI) exclusivity grants three years for formulation changes or new indications backed by new clinical studies. Orphan Drug Designation provides seven years of market exclusivity for drugs treating rare diseases. Pediatric exclusivity adds six months to both patent terms and regulatory exclusivities for drugs studied in pediatric populations.
The Biologics Price Competition and Innovation Act gives reference biologics 12 years of data exclusivity. This means a biologic can face biosimilar applications 12 years after approval regardless of patent status, with a four-year no-filing period followed by an eight-year application window.
Stacking these exclusivities requires deliberate clinical and regulatory planning, not just patent prosecution. A brand team that secures pediatric exclusivity on top of NCE exclusivity and a strong patent thicket has effectively extended its protected revenue window in ways that are legally bulletproof, because regulatory exclusivities are not subject to Paragraph IV challenges.
The Interchangeable Biosimilar Threat and IP Response
The interchangeable biosimilar designation is the biologic-specific equivalent of generic substitution rights. An interchangeable biosimilar can be dispensed in place of the reference product without prescriber intervention in states that have automatic substitution laws. As of 2025, most US states have enacted such laws for interchangeable biologics, meaning that an interchangeable biosimilar competitor directly erodes volume at the pharmacy level without requiring prescriber adoption.
Brands facing BPCIA biosimilar entry should assess the interchangeability risk for each biosimilar in development. Not all biosimilar sponsors pursue the interchangeability designation, because the switching study requirement adds cost and time. Sponsors focused on hospital and clinic channels — where pharmacist substitution is less relevant because a clinician administers the product — may not seek interchangeability. Sponsors targeting retail or specialty pharmacy channels for self-administered biologics (such as subcutaneous formulations) have stronger incentives to pursue the designation.
The IP response to interchangeable biosimilar entry includes asserting device and delivery system patents, which cover autoinjectors, prefilled syringes, and pen devices used for subcutaneous administration. These device patents may have expiry dates well beyond the biologic molecule’s primary patent, and their validity is generally stronger than formulation patents because they protect proprietary engineering, not chemistry.
Key Takeaways: Layered IP Defense
The patent thicket’s commercial value depends on the litigation durability of its component patents, not just their nominal expiry dates. Paragraph IV litigation strategy should focus on defending high-value patents through the 30-month stay and structured settlements. Regulatory exclusivity stacking — NCE, NCI, orphan, pediatric — provides protection independent of patent validity. Interchangeable biosimilar risk requires specific assessment, since it drives pharmacy-level substitution without prescriber action.
Step 3: Run Product Lifecycle Extension — The Full Evergreening Toolkit
Evergreening — the practice of extending effective market exclusivity through successive product modifications, new formulations, and new indications — has been the subject of considerable policy debate and litigation. The term carries negative connotations in some quarters, but the underlying activities range from genuine clinical innovation (a new pediatric formulation with real dosing advantages) to legally dubious tactics (minor reformulations with no meaningful patient benefit that courts may find obvious). This section addresses the full toolkit as it actually exists, including the risks.
Next-Generation Molecular Entities: The Cleanest LOE Hedge
The highest-value lifecycle extension is a genuinely differentiated successor molecule that patients and prescribers prefer over generics of the original product. This is not evergreening in the pejorative sense but rather what the patent system is designed to incentivize. AstraZeneca’s esomeprazole (Nexium) followed omeprazole (Prilosec) as the S-enantiomer with a demonstrably different pharmacokinetic profile. The medical community debated whether the clinical benefits justified the price differential, but the underlying chemistry was novel and the IP was legally sound.
The challenge for most pharma R&D programs is timing. A next-generation compound needs to reach regulatory approval at least two to three years before the original product’s LOE to capture meaningful market share during the transition. Compounds entering Phase II trials four years before LOE are unlikely to make that window. R&D teams need to carry next-generation programs as dedicated lifecycle management investments with aggressive development timelines, not as standard pipeline assets following conventional phase durations.
Formulation Innovation: Modified Release, New Routes, Novel Delivery
Modified-release formulations represent the most commonly used lifecycle extension tool because they require less clinical development than new molecular entities while generating genuine patient benefits in many cases. A once-daily extended-release version of a twice-daily immediate-release drug reduces pill burden and can improve adherence. If the pharmacokinetic profile achieves better peak-to-trough ratios, there may also be tolerability advantages.
From an IP standpoint, a modified-release formulation generates a new NDA (505(b)(2) pathway, which leverages the original product’s safety data), new Orange Book patent listings, and potentially NCI exclusivity if new clinical studies demonstrate clinical benefit. The new NDA is a distinct regulatory entity from the original product. Generic manufacturers must file against it separately, with separate Paragraph IV certifications and separate litigation risk.
The technology roadmap for formulation innovation includes several distinct platforms. Osmotic release oral system (OROS) technology, long used for extended-release formulations, is mature and widely available to generic manufacturers. Newer platforms, including mucoadhesive delivery systems, prodrug approaches that convert to the active molecule in vivo, and nanoparticle formulations that improve bioavailability for poorly soluble compounds, offer more defensible IP because the underlying technology is newer and the manufacturing complexity is higher.
For biologics, subcutaneous formulation development is the most commercially significant delivery innovation. IV-to-SC transitions require co-formulation with hyaluronidase or development of high-concentration formulations capable of subcutaneous delivery, both of which generate new IP. Roche’s SC formulations of MabThera/Rituxan (rituximab) and Herceptin (trastuzumab), developed in partnership with Halozyme’s ENHANZE technology, represent the most commercially significant examples. The SC formulations generated new exclusivity periods, new device patents on the co-packaged administration devices, and meaningful clinical differentiation in terms of administration time.
Indication Expansion: Clinical and IP Strategy
Seeking regulatory approval for new indications is one of the most defensible forms of lifecycle extension because it requires actual clinical evidence. Each new indication approved on the basis of new clinical investigations qualifies for three-year NCI exclusivity. For an orphan disease indication, seven-year orphan exclusivity applies. For a pediatric indication with a Written Request from FDA, six-month pediatric exclusivity extends both patent protection and regulatory exclusivity.
The clinical strategy for indication expansion should prioritize indications where the drug’s mechanism of action has a scientifically grounded rationale, where the patient population has genuine unmet need, and where the regulatory pathway offers the most exclusivity. Rare disease indications are particularly attractive from a lifecycle management perspective because they combine orphan exclusivity with the commercial dynamics of a specialty or ultra-specialty product — higher pricing, more concentrated prescriber bases, and lower generic substitution pressure.
From an IP perspective, method-of-use patents covering the new indications are listed in the Orange Book (or Purple Book) and must be certified against by any generic or biosimilar applicant seeking to market for those indications. Skinny labeling — where a generic manufacturer carves out the patented indication from its label to avoid infringement — is legally available under the Hatch-Waxman Act. The Amarin v. Hikma litigation over icosapentaenoic acid (Vascepa) explored the boundaries of skinny labeling claims in detail. IP teams should monitor skinny labeling filings in ANDA applications against indication-specific method-of-use patents.
Combination Products: The Franchise Architecture
Fixed-dose combination (FDC) products, which combine two or more active pharmaceutical ingredients in a single dosage form, represent one of the most durable lifecycle extension strategies when the combination has genuine clinical rationale. The HIV antiretroviral market provides the clearest large-scale example. Gilead’s progression from single-agent antiretrovirals to two-drug, then three-drug, then four-drug FDCs, each with new IP and new regulatory exclusivities, created a franchise architecture that extended revenue well beyond any single compound’s patent life. The clinical rationale — simplifying regimens to improve adherence, reducing pill burden, optimizing pharmacokinetic interactions — was real and documented.
FDC IP involves a combination product patent protecting the specific combination and ratio of active ingredients, potentially new formulation patents, and new regulatory exclusivities associated with the NDA filing. Generic manufacturers must bioequivalence-test the combination as a whole, not just individual components, which adds complexity. If one component of the FDC is still under patent protection, the FDC itself benefits from that protection as well.
The risk is clinical relevance. Regulators in the EU, and increasingly in the US, require that FDC products demonstrate benefit relative to concurrent use of the individual components. An FDC where the combination offers no measurable clinical advantage over the component drugs taken separately faces regulatory challenges and payer pushback on premium pricing.
Key Takeaways: Lifecycle Extension
The evergreening toolkit includes strategies that range from genuine clinical innovation to legally vulnerable minor modifications. Next-generation molecular entities offer the cleanest LOE hedge but require a five-to-seven-year development lead time. Modified-release formulations and new delivery systems generate defensible IP and regulatory exclusivity when built on non-obvious technology platforms. Indication expansion is the most legally sound tactic when supported by clinical evidence and paired with orphan or pediatric exclusivity where applicable. FDC franchise architectures provide durable protection when the combination has documented clinical rationale.
Step 4: Deploy Strategic Business Adaptations (Authorized Generics, Licensing, M&A)
Beyond IP defense and lifecycle extension, the commercial and corporate structure of a company facing LOE needs to adapt. The three primary tools are authorized generic programs, licensing and partnership transactions, and portfolio-diversifying M&A.
Authorized Generics: Mechanics and Strategic Purpose
An authorized generic is a version of a brand-name drug sold under the generic drug’s regulatory approval but manufactured or authorized by the innovator company. The authorized generic is legally and pharmaceutically identical to the brand product, sold at a generic price. Innovators launch authorized generics to capture a portion of the volume that will shift to generic alternatives after LOE, preserving manufacturing utilization and distribution relationships.
The most strategically important timing for an authorized generic launch is during the 180-day exclusivity period that Hatch-Waxman grants to the first Paragraph IV filer. During this window, only the first ANDA filer and any authorized generic can market generic versions of the product. A brand company that launches an authorized generic during this window splits the first-generic exclusivity period’s economics with the Paragraph IV filer, reducing the financial reward for challenging the patent in the first place. This has a prospective deterrent effect: generic manufacturers aware that they will share the exclusivity period with an authorized generic may price their Paragraph IV litigation investment differently.
The FTC has studied authorized generic competition extensively. The empirical evidence shows that authorized generics during 180-day exclusivity lower prices faster than single-generic competition, benefiting payers and patients. From the innovator’s perspective, the authorized generic also generates continuous manufacturing volume data, which supports cost structure optimization for the post-LOE period.
Licensing: In-Licensing to Fill Revenue Gaps
A company facing a major LOE event has two licensing-related priorities: in-licensing late-stage assets that can contribute revenue before the gap hits, and out-licensing declining assets to companies better positioned to maximize their remaining value. Neither strategy is straightforward.
In-licensing late-stage assets to fill an LOE revenue gap requires paying peak valuations for near-launch compounds during a period when the acquiring company’s bargaining position — specifically, its ability to sustain a high deal price using cash flows from the at-risk product — is strongest. Companies that wait until after LOE to in-license, when their revenue base has compressed, will pay with dilutive equity rather than cash, worsening the financial impact.
The deal terms matter as much as the asset. Royalty structures, milestone payments, co-promotion rights, and geographic licensing restrictions all affect the economic value of an in-licensed compound. IP teams reviewing in-licensing deals need to assess the patent durability of the incoming asset with the same rigor they apply to their own portfolio.
Out-licensing products approaching LOE is less common but commercially rational in specific circumstances. A branded product in a therapeutic area where the company has no ongoing R&D commitment, limited commercial infrastructure, or a sales force that is being redeployed to other priorities may generate more value through a royalty stream from a licensee than through continued internal commercialization. The out-licensing price for a product approaching LOE is heavily discounted versus peak-revenue valuations, so these transactions require careful financial modeling.
M&A as LOE Defense: The Merck-Harpoon Model
The most aggressive version of LOE preparation is a targeted acquisition program designed to fill the revenue gap created by a specific expiry event. Merck’s January 2024 agreement to acquire Harpoon Therapeutics for $680 million is an instructive example. The transaction brought Merck a clinical-stage bispecific T-cell engager (BiTE) program in oncology, complementing the pembrolizumab franchise that faces LOE in 2028. The acquisition was explicitly framed in the context of bolstering Merck’s oncology pipeline for the post-Keytruda period.
The IP valuation logic in these transactions: the acquiree’s pipeline assets carry their own patent portfolios with expiry dates that, if development succeeds, will fall after the acquiror’s LOE cliff. Analysts pricing these deals need to assess the technology platform’s IP durability alongside the clinical risk. A BiTE platform with composition-of-matter patents expiring in 2042 offers 14 years of potential exclusivity on any approved product — assuming successful development and no successful Paragraph IV challenge. The net present value of that exclusivity is highly sensitive to peak sales assumptions and discount rates, which is why biotech M&A modeling requires scenario-based valuation, not point estimates.
The acquisition targets most attractive for LOE defense have specific characteristics: Phase II or Phase III assets reducing binary clinical risk, mechanism-of-action differentiation from the acquiror’s current portfolio to limit cannibalization, IP portfolios with primary patent expiry dates at least 10 years from anticipated launch, and therapeutic area alignment that lets the acquiror leverage existing commercial infrastructure.
Key Takeaways: Strategic Business Adaptations
Authorized generics launched during the 180-day first-generic exclusivity period serve a dual purpose: capturing generic volume and diluting the financial incentive for Paragraph IV challenges. In-licensing is most financially efficient when executed before LOE, while operating cash flows are strongest. M&A for LOE defense requires IP due diligence on the target’s own patent portfolio, not just its clinical pipeline, with scenario-based valuation that accounts for Paragraph IV risk on the incoming assets.
Step 5: Restructure Manufacturing and Supply Chain for Post-LOE Margins
Revenue compression after LOE is inevitable. The margin response — which is within operational control — determines whether the post-LOE business is economically viable or a drag on the portfolio. Manufacturing and supply chain optimization is the least glamorous element of LOE strategy and the one most commonly deferred until the revenue decline has already started.
Cost Structure Benchmarking Against Generic Manufacturers
The relevant cost benchmark for a post-LOE branded product’s manufacturing cost is not the company’s prior-year COGS per unit but the generic manufacturer’s estimated COGS per unit. Generic manufacturers operating at scale in cost-efficient geographies — particularly Indian API manufacturers and Chinese contract manufacturers — have cost structures that branded pharma companies cannot match through marginal efficiency improvements. The question is how close the branded product’s cost structure can get, and whether the residual cost gap is covered by brand premium or authorized generic revenue.
Process chemistry optimization, continuous manufacturing adoption, and active pharmaceutical ingredient (API) resourcing from qualified low-cost suppliers are the primary levers for COGS reduction in small-molecule post-LOE programs. For biologics, the COGS reduction opportunity is different. Biologic manufacturing at commercial scale involves high fixed costs in cell culture, purification, and fill-finish capacity. Post-LOE biologic COGS reduction comes from utilization management — keeping existing facilities running at optimal batch efficiency — and from biosimilar-level process improvements achieved through years of accumulated process characterization data. An innovator biologic manufacturer with 15 years of process development history has a manufacturing cost structure that biosimilar entrants, building from the initial 351(k) analytical comparability packages, are still working toward.
Demand Forecasting and Capacity Rightsizing
Post-LOE volume trajectories are not linear, and manufacturing capacity planning needs to account for scenario variability. A demand forecast built solely on the base-case LOE scenario will result in either excess capacity that generates fixed-cost drag or insufficient capacity that leaves the authorized generic or residual branded business unable to supply market demand. The appropriate manufacturing planning model uses probability-weighted demand scenarios aligned with the IP litigation scenarios from the LOE strategy: orderly expiry, accelerated Paragraph IV entry, extended litigation holding off generics.
Capacity rightsizing may require divestiture of manufacturing assets that are efficient at high utilization rates but uneconomic at post-LOE volumes. Contract manufacturing organization (CMO) relationships provide a flexible capacity buffer — a post-LOE supply strategy that maintains a baseline owned capacity with CMO overflow capacity can reduce fixed-cost exposure while preserving supply reliability.
Supply Chain Resilience: API Sourcing and Concentration Risk
Drug shortages in the post-LOE environment, which may seem counterintuitive given increased supply from multiple generic manufacturers, are more common than they appear because many generics rely on the same small pool of API suppliers. A brand company maintaining post-LOE manufacturing for a residual branded or authorized generic business that sources API from a diversified supplier base has a reliability advantage over generics sourcing from concentrated Asian API supply chains subject to regulatory action risk (FDA warning letters, import alerts).
Documenting and publicizing supply chain reliability is a legitimate commercial differentiation argument in hospital and health system contracting, where buyers have experienced supply disruptions from generic manufacturers and place real value on supply continuity guarantees.
Manufacturing Expertise as a Barrier to Entry
For products with complex manufacturing characteristics — sterile injectables, products requiring specialized containment, biologics with demanding cold-chain requirements, or drugs with active ingredient stability challenges — manufacturing expertise constitutes a genuine, albeit non-IP, barrier to entry. Generic manufacturers seeking to enter these markets face a steeper regulatory and operational path than they do for standard oral solid dosage forms.
FDA’s complex drug review process for complex injectables, locally acting drugs, and drug-device combination products is more demanding than standard ANDA review. The regulatory complexity translates into fewer ANDA filers and less aggressive price competition. Brand companies in these categories should track the number of ANDA filers against their complex products separately from their standard-formulation products, and price post-LOE strategy accordingly.
Key Takeaways: Manufacturing and Supply Chain
Manufacturing strategy for LOE preparation is fundamentally a cost structure exercise benchmarked against generic competitor economics, not against prior-year internal COGS. Capacity rightsizing should use probability-weighted demand scenarios from the IP litigation model, not a single base-case forecast. API supplier diversification is an underutilized supply chain competitive advantage in post-LOE markets where generic concentration risk creates periodic shortages. Complex manufacturing requirements — sterile injectables, biologics, drug-device combinations — reduce the pool of ANDA/biosimilar filers and moderate post-LOE price erosion.
Post-LOE Performance Measurement Framework
Running LOE strategy without a measurement framework is operationally incoherent. The KPI set for post-LOE performance needs to cover revenue retention, market share dynamics, lifecycle extension returns, and manufacturing efficiency, each against the scenario baselines established during pre-LOE planning.
Revenue Retention and Market Share Metrics
The primary revenue metric is not total revenue but revenue retention rate — the percentage of peak annual revenue retained in years one, two, and three post-LOE. Industry benchmarks for small-molecule oral drugs suggest 15-25% revenue retention at year two under orderly generic entry. Biologics retain 45-65% at year two under typical biosimilar entry patterns. Products with successful lifecycle extension to a successor compound or new formulation should measure successor revenue separately and track the transition rate from original to successor.
Market share measurement post-LOE requires tracking brand, authorized generic, and successor product volume together as an ‘extended franchise share.’ The goal is not necessarily to retain branded market share — which will fall regardless — but to retain franchise revenue across the full product family.
Lifecycle Extension ROI
The ROI calculation for each lifecycle extension investment needs to be prospective (estimated before the investment) and retrospective (measured against actual revenue outcomes). A modified-release formulation development program costing $150 million that generates two years of additional effective exclusivity on a $2 billion-per-year product is straightforwardly accretive — the net present value of incremental exclusivity revenue exceeds the development cost by a wide margin. A program with the same cost generating six months of additional exclusivity on a $400 million product is marginal.
Pre-LOE, these calculations require conservative revenue assumptions and probability discounts for regulatory approval and Paragraph IV litigation outcomes. Post-LOE, actual performance against pre-investment projections provides the most valuable data for calibrating future lifecycle management investment decisions.
Key Takeaways: Performance Measurement
Revenue retention rate, measured as a percentage of peak annual revenue at years one through three post-LOE, is the single most actionable top-line metric. Market share tracking should cover the extended franchise — brand, authorized generic, and successor — not just the original branded product. Lifecycle extension investments require prospective ROI calculations with regulatory and litigation probability discounts, measured against actual outcomes to calibrate future planning.
Investment Strategy for Analysts
For institutional investors and sell-side analysts, the patent cliff presents both risks and identifiable mispricings.
Pricing LOE Risk into Valuation
Most sell-side models apply a binary LOE discount — revenue falls to zero at patent expiry. This is analytically wrong for biologics and directionally wrong for small-molecule drugs with significant lifecycle management programs. A more defensible model runs a probability-weighted NPV across three scenarios (orderly expiry, Paragraph IV acceleration, extended litigation), applies a step-up discount rate at LOE reflecting the shift from monopoly to competitive pricing, and separately models successor product revenue with its own peak-sales and adoption assumptions.
The most common mispricing in pharma equities around LOE events comes from the market underestimating the revenue durability of biologic franchises post-LOE (because analysts apply small-molecule erosion rates to biologics) and from the market failing to value the optionality embedded in mid-stage lifecycle management programs that are not yet included in consensus models.
Monitoring Signals for LOE Event Timing
Paragraph IV filing activity, tracked through ANDA databases and FDA’s Orange Book updates, is the earliest available signal that generic manufacturers are targeting a specific product. A product with five or more Paragraph IV filers is facing aggressive competitive intent; the financial market often has not fully priced that intent if the primary patent expiry date is still three or more years away.
Biosimilar 351(k) application filings, tracked through the Purple Book, are the biologic equivalent. The filing date and the complexity of the biosimilar’s regulatory pathway — including whether the sponsor is pursuing interchangeability — directly affect LOE timing and erosion severity.
M&A Signals and Patent-Driven Deal Thesis
Patent data is a leading indicator of M&A activity. A company with a primary LOE event within three years and insufficient late-stage pipeline to cover the revenue gap has identifiable M&A pressure. The targets it is most likely to pursue are late-stage clinical assets in aligned therapeutic areas with primary patent expiry dates 10 or more years out. Screening for these targets using patent data, pipeline databases, and financial modeling of the acquiror’s LOE gap can generate actionable investment hypotheses ahead of deal announcements.
Master Key Takeaways
The $236 billion patent cliff running from 2025 to 2030 is not a uniform event. It is a heterogeneous set of LOE scenarios across small-molecule and biologic products, each with distinct erosion mechanics, IP durability profiles, and lifecycle management optionality.
Effective LOE strategy starts no later than five years before primary patent expiry for small-molecule products and seven years for biologics managing biosimilar interchangeability risk. The patent portfolio audit — assessing litigation durability, not just nominal expiry dates — is the first technical deliverable and the foundation for every subsequent strategic decision.
The evergreening toolkit is not monolithic. Next-generation molecular entities, modified-release formulations, new delivery systems, indication expansions backed by clinical evidence, and fixed-dose combination franchise architectures each carry distinct IP durability profiles, clinical development requirements, regulatory exclusivity opportunities, and commercial risk profiles. Selecting the right toolkit components requires mapping each option’s expected ROI against the specific product’s revenue base and LOE timeline.
Authorized generic programs, in-licensing, out-licensing, and M&A each operate on different capital requirements and time horizons. The authorized generic is the fastest to deploy and most directly tied to LOE timing. In-licensing and M&A require lead times of two to four years to generate revenue before the LOE gap hits.
Manufacturing and supply chain restructuring is the most consistently underinvested area of LOE planning. Post-LOE margin defense is a manufacturing cost structure problem, not primarily an IP or commercial problem, and it requires its own dedicated planning workstream benchmarked against generic competitor economics.
For investors, the key analytical edge is applying biologic-specific erosion rates to biologic LOE events, tracking Paragraph IV and 351(k) filing activity as early warning signals, and screening for M&A-driven companies using patent expiry gap analysis to identify deal thesis candidates ahead of announcements.
Data sources: IQVIA, GeneOnline, NBER, FDA Orange Book and Purple Book, SEC filings. Patent data and expiry information sourced from DrugPatentWatch.